Professional Documents
Culture Documents
Diverticular Disease-1
Diverticular Disease-1
Uploaded by
عبد الله مازن موسى عبد0 ratings0% found this document useful (0 votes)
14 views26 pagesThis document summarizes intestinal and colonic diverticula. It describes that diverticula are out-pouchings that can occur in the digestive tract. There are two types: congenital, which involve all bowel wall layers; and acquired, which lack a muscular layer. Specific types discussed include jejunal, Meckel's, and sigmoid diverticula. Meckel's diverticulum is a remnant of the vitelline duct and can cause bleeding or obstruction. Complications of sigmoid diverticula include inflammation, perforation, bleeding, and fistula formation. Treatment involves antibiotics for acute diverticulitis and possible surgery for complications or recurrent issues.
Original Description:
Lecture in general
surgery
Original Title
diverticular disease-1 (1)
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document summarizes intestinal and colonic diverticula. It describes that diverticula are out-pouchings that can occur in the digestive tract. There are two types: congenital, which involve all bowel wall layers; and acquired, which lack a muscular layer. Specific types discussed include jejunal, Meckel's, and sigmoid diverticula. Meckel's diverticulum is a remnant of the vitelline duct and can cause bleeding or obstruction. Complications of sigmoid diverticula include inflammation, perforation, bleeding, and fistula formation. Treatment involves antibiotics for acute diverticulitis and possible surgery for complications or recurrent issues.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
14 views26 pagesDiverticular Disease-1
Diverticular Disease-1
Uploaded by
عبد الله مازن موسى عبدThis document summarizes intestinal and colonic diverticula. It describes that diverticula are out-pouchings that can occur in the digestive tract. There are two types: congenital, which involve all bowel wall layers; and acquired, which lack a muscular layer. Specific types discussed include jejunal, Meckel's, and sigmoid diverticula. Meckel's diverticulum is a remnant of the vitelline duct and can cause bleeding or obstruction. Complications of sigmoid diverticula include inflammation, perforation, bleeding, and fistula formation. Treatment involves antibiotics for acute diverticulitis and possible surgery for complications or recurrent issues.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 26
BOWEL DIVERTICULA
Dr. SAHAL KRAIDY
M.B.CH.B F I C M S DR
INTESTINAL DIVERTICULA Diverticula
(hollow out-pouchings) are a common structural
abnormality that can occur from the oesophagus
to the rectosigmoid junction (but not usually in
the rectum).
They can be classified as:
• Congenital. All three coats of the bowel are
present in the wall of the diverticulum, e.g.
Meckel’s diverticulum.
• Acquired. There is no muscularis layer present in
the diverticulum, e.g. sigmoid diverticula.
Jejunal diverticula
Jejunal diverticula These arise from the mesenteric side
of the bowel as a result of mucosal herniation at the
point of entry of the blood vessels.
they can result in malabsorption, as a result of bacterial
stasis, or present as an acute abdominal emergency if
they become inflamed or perforate. Bleeding from a
jejunal diverticulum is a rare complication.
Elective resection of an affected small bowel segment
that is causing malabsorption can be effective.
Meckel’s diverticulum
A Meckel’s diverticulum is a persistent remnant
of the vitellointestinal duct, It is found on the
antimesenteric side of the ileum
Vitellointestinal duct appearing in the beginning of
embryonic life as a long tubular structure, connects
the midgut to the yolksac. It regresses during fifth to
ninth week of fetal development . If the lumen does
not completely obliterate, it can result in patent
vitellointestinal duct
A Meckel’s diverticulum contains all three coats of the
bowel wall and has its own blood supply. It is
vulnerable to obstruction and inflammation in the
same way as the appendix; indeed, when a normal
appendix is found at surgery for suspected
appendicitis, a Meckel’s diverticulum should be
looked for by examining the small bowel particularly
if free fluid or pus is found
Features of Meckel’s diverticulum
■ Remnant of vitellointestinal duct
■ Occurs in 2 per cent of patients, 2 inches (5 cm long), 2 feet
(60 cm) from the ileocaecal valve, 20 per cent heterotopic,
twice common in male epithelium.
■ Should be looked for when a normal appendix is found at
surgery for suspected appendicitis
■ If a Meckel’s is found incidentally at surgery, it can be left
provided it has a wide mouth and is not thickened
■ Can be source of gastrointestinal bleeding if it contains ectopic
gastric mucosa
In around 20 per cent of cases, the mucosa of a Meckel’s
diverticulum contains heterotopic epithelium of gastric,
colonic or pancreatic type.
A Meckel’s diverticulum can present clinically in the following
ways:
• Haemorrhage. If gastric mucosa is present, peptic ulceration
can occur and present as painless maroon rectal bleeding
or melaena. If the stomach, duodenum and colon are
cleared by endoscopy, radioisotope scanning with
technetium-99m may demonstrate a Meckel’s. (A Meckel’s
is notoriously difficult to see with contrast radiology.)
• Diverticulitis. Meckel’s diverticulitis presents like
appendicitis, although if perforation occurs the
presentation may resemble a perforated duodenal ulcer.
• Intussusception. A Meckel’s can be the lead point
for ileoileal or ileocolic intussusception.
Chronic ulceration. Pain is felt around the umbilicus,
as the site of the diverticulum is midgut in origin.
• Intestinal obstruction. A band between the apex
of the diverticulum and the umbilicus (also part
of the vitellointestinal duct) may cause
obstruction directly or by a volvulus around it.
• Perforation. The vast majority of Meckel’s are
asymptomatic.
When found in the course of abdominal surgery,
a Meckel’s can safely be left alone provided it
has a wide mouth and is not thickened. When
there is doubt, it can be resected. The finding
of a Meckel’s diverticulum in an inguinal or
femoral hernia has been described as Littre’s
hernia
Diverticular disease of the large intestine
Diverticula are found in the left colon in around 75 per cent
of over 70 year olds in the Western world.
Epidemiology supports the widely held view that diverticular
disease is a consequence of a refined Western diet deficient
in
dietary fibre. The combination of altered collagen structure
with ageing, disordered motility and increased intraluminal
pressure most notably in the narrow sigmoid colon results in
herniation of mucosa, protruding through the circular muscle
at the points
where blood vessels penetrate the bowel wall. The rectum
has
a complete muscular coat and a wider lumen and is thus very
rarely affected
Complications of diverticular disease
The majority of patients with diverticula are asymptomatic;
historical studies suggest somewhere between 10 and 30 per cent
will have symptomatic complications
These complications are:
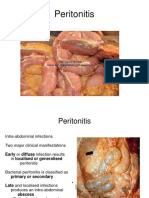
*Pain and inflammation (diverticulitis).
*Perforation: most often contained leading to pericolic
*abscess formation, but occasionally free leading to generalised
peritonitis.
*Intestinal obstruction: progressive fibrosis can cause stenosis
of the sigmoid and large bowel obstruction or loops of small
intestine can adhere to an inflamed sigmoid resulting in small
bowel obstruction.
*Haemorrhage: diverticulitis may present with profuse colonic
haemorrhage.
*Fistula formation: (colovesical, colovaginal, enterocolic,
colocutaneous) occurs in 5 per cent of cases, colovesical
Gangrenous Meckel’s diverticulitis. fistulation is most common.
Hinchey classification of complicated
diverticulitis.
I Mesenteric or pericolic abscess
II Pelvic abscess
III Purulent peritonitis
IV Faecal peritonitis
Clinical features
In mild cases, symptoms such as distension,
flatulence and a sensation of heaviness in the
lower abdomen may be indistinguishable from
those of irritable bowel syndrom
Diverticulitis typically presents as persistent
lower abdominal pain, usually in the left iliac
fossa accompanied by loose stools or indeed
constipation. Fever, malaise and leukocytosis
can differentiate diverticulitis from painful
diverticulosis.
Generalised peritonitis as a result of free
perforation presents in the typical manner
with systemic upset and generalised tenderne
Haemorrhage from colonic diverticula is typically
painless and profuse.
The presentation of a fistula resulting from
diverticular disease depends on the site. The
most common colovesical fistula results in
recurrent urinary tract infections and
pneumaturia (flatus in the urine) or even faeces
in the urine. Colovaginal fistulae are more
common in patients who have had a
hysterectomy. Colocutaneous fistulation is rare in
the absence of prior intervention (e.g. radiologi
Work up
Plain chest and abdominal radiographs can
demonstrate a pneumoperitoneum.
Where available, spiral CT has excellent
Colonoscopy is normally deferred until 6 weeks
after an acute attack of diverticulitis. It may
demonstrate the necks of diverticula within
the bowel lumen
Barium enema showing sigmoid diverticular •
disease ‘sawteeth’ and diverticula
Treatment
* Management Patients are frequently recommended to take a high-
fibre diet and bulk-forming laxatives,
although the evidence for the effectiveness of these in diverticulosis or
after an attack of diverticulitis is limited.
* Antispasmodics may have a role if recurrent pain is a problem.
*Acute diverticulitis is treated by intravenous antibiotics (to cover
Gram-negative bacilli and anaerobes) alongside appropriate
resuscitation and analgesia.
*Nil by mouth to ‘rest the bowel’ and catheterisation to reduce the
risk of colovesical fistulation are often advocated, but there is little
evidence to support these practices.
A CT scan can confirm the diagnosis and assess for complications.
After the acute attack
Principles of surgical management of
diverticular disease
■ Hartmann’s procedure is the safest option in
emergency
surgery
■ Primary anastomosis can be considered in selected
patients
■ Elective resection may be offered for recurrent attacks
■ Definitive treatment of colovesical fistula will require
resection
THANK YOU
You might also like
- UW (Step 1) GIT - Educational Objectives PDFDocument69 pagesUW (Step 1) GIT - Educational Objectives PDFDrbee10No ratings yet
- Single Best Answer (SBA) QuestionsDocument16 pagesSingle Best Answer (SBA) QuestionsKrairat Komdee67% (3)
- Meckels DiveritulumDocument30 pagesMeckels DiveritulumFrancis Adrian O. LadoresNo ratings yet
- Meckel's DiverticulumDocument4 pagesMeckel's DiverticulumKlaue Neiv CallaNo ratings yet
- Bowel Obstruction and Tumors SheetDocument19 pagesBowel Obstruction and Tumors SheetAbu Ibtihal OsmanNo ratings yet
- Diverticular DiseaseDocument8 pagesDiverticular Diseasenurizzah_885541100% (1)
- Diverticulum DiseaseDocument6 pagesDiverticulum Diseasen_robinNo ratings yet
- Small Intestine - (UPTODATE)Document4 pagesSmall Intestine - (UPTODATE)Ha Jae kyeongNo ratings yet
- Diverticular Diseases of ColonDocument22 pagesDiverticular Diseases of ColonGyan Prakash BhartiNo ratings yet
- Small Bowel: Alaa MaaliDocument78 pagesSmall Bowel: Alaa MaaliHalima AssiNo ratings yet
- DIVERTIKULOSISDocument28 pagesDIVERTIKULOSISAndrie WigunaNo ratings yet
- Diverticular Disease: Diverticulitis, Bleeding, and FistulaDocument8 pagesDiverticular Disease: Diverticulitis, Bleeding, and FistulaakashkumarpanwarNo ratings yet
- Pediatrics Meckel'S DiverticulumDocument15 pagesPediatrics Meckel'S Diverticulum906 SoNo ratings yet
- Diverticular Disease of The ColonDocument3 pagesDiverticular Disease of The ColonaliceNo ratings yet
- Abdominal X-Rays PT 1Document20 pagesAbdominal X-Rays PT 1sb medexNo ratings yet
- Surgical Acute Abdomen in Pediatric 2Document23 pagesSurgical Acute Abdomen in Pediatric 2Fahad HasanNo ratings yet
- Colonic and Small Intestine Disorders-1Document28 pagesColonic and Small Intestine Disorders-1YIKI ISAACNo ratings yet
- Ipi 82603Document18 pagesIpi 82603Megawati LiwangNo ratings yet
- Esophageal DiverticulaDocument18 pagesEsophageal DiverticulaAbigail BascoNo ratings yet
- EsophagealDiverticula StatPearls NCBIBookshelfDocument9 pagesEsophagealDiverticula StatPearls NCBIBookshelfInês PriorNo ratings yet
- IntussusceptionDocument10 pagesIntussusceptionshenlie100% (1)
- Acquiredintestinalileus 131003164413 Phpapp01Document53 pagesAcquiredintestinalileus 131003164413 Phpapp01fandiroziNo ratings yet
- PeritonitisDocument33 pagesPeritonitisnurulamaliahnutNo ratings yet
- Anatomy Atresia, Volvulus, Meckel's Diverticulum: BowelDocument45 pagesAnatomy Atresia, Volvulus, Meckel's Diverticulum: BowelkedokterankeluargaNo ratings yet
- Screenshot 2023-11-26 at 5.15.31 PMDocument39 pagesScreenshot 2023-11-26 at 5.15.31 PMgauravsingh708284No ratings yet
- Obvious Neonatal Anomalies - NewDocument14 pagesObvious Neonatal Anomalies - NewnlwhtdcsnvuvbkxmtpNo ratings yet
- Large Bowel Obstruction by Nic MDocument42 pagesLarge Bowel Obstruction by Nic MRisky OpponentNo ratings yet
- Divertikel - WehrmannDocument36 pagesDivertikel - WehrmannSake Cinema21No ratings yet
- Problem 4 GIT Josephine AngeliaDocument35 pagesProblem 4 GIT Josephine AngeliaAndreas AdiwinataNo ratings yet
- Disorders of EsophagusDocument27 pagesDisorders of EsophagusFranci Kay SichuNo ratings yet
- Pathology of The Digestive System: Presentation by Rowell AngelesDocument25 pagesPathology of The Digestive System: Presentation by Rowell AngelesZEESHAN YOUSUFNo ratings yet
- Small Intestine and ColonDocument9 pagesSmall Intestine and Colonlentini@maltanet.netNo ratings yet
- Lemmel's Syndrome As A Rare Cause of Obstructive JaundiceDocument4 pagesLemmel's Syndrome As A Rare Cause of Obstructive JaundiceKath de L'EnferNo ratings yet
- გაუვალობაDocument37 pagesგაუვალობაMalak A MahadeenNo ratings yet
- Bowel ObstuctionDocument100 pagesBowel ObstuctionRam Kirubakar ThangarajNo ratings yet
- Kelainan Pada Usus HalusDocument28 pagesKelainan Pada Usus HalusClara Shinta AruanNo ratings yet
- Pancreatitis Ercp Pain Amylase Lipase ErcpDocument24 pagesPancreatitis Ercp Pain Amylase Lipase ErcpPerplexed CeleryNo ratings yet
- L08 Diverticular DiseasesDocument11 pagesL08 Diverticular DiseasesS sNo ratings yet
- Disorders of The IntestinesDocument64 pagesDisorders of The IntestinesCharmaine Torio PastorNo ratings yet
- Appendicitis Lec2023Document6 pagesAppendicitis Lec2023Taha MuhammedNo ratings yet
- DiverticulosisDocument9 pagesDiverticulosisSyafiq Shahbudin100% (1)
- Intestinal ObstructionDocument9 pagesIntestinal ObstructionMuhammad Fuad Jaafar100% (1)
- Abdominal - GIT ImagingDocument83 pagesAbdominal - GIT ImagingHala AhmadNo ratings yet
- Acute Cholecystitis:: Etiological TypesDocument5 pagesAcute Cholecystitis:: Etiological Typesvivek yadavNo ratings yet
- Lecture 7 Intussusception 2016Document8 pagesLecture 7 Intussusception 2016Nuukelo ShimbomeNo ratings yet
- ColectomyDocument9 pagesColectomyAgung Choro de ObesNo ratings yet
- SG3 Paediatric Surgical EmergenciesDocument69 pagesSG3 Paediatric Surgical EmergenciesDiyana ZatyNo ratings yet
- Appendicitis 5.9Document50 pagesAppendicitis 5.9Smart SaravanaNo ratings yet
- Gastrointestinal Fistulas - Mousa MashagbahDocument23 pagesGastrointestinal Fistulas - Mousa MashagbahmencarilmuNo ratings yet
- Ulcerative ColitisDocument12 pagesUlcerative ColitisSanthu SuNo ratings yet
- Volvulus & IntussuseptionDocument22 pagesVolvulus & IntussuseptionliaNo ratings yet
- Íleo Biliar - UpToDateDocument19 pagesÍleo Biliar - UpToDateRogelio MoscosoNo ratings yet
- Problem 4 GITDocument94 pagesProblem 4 GITArioNo ratings yet
- Peptic and Other Benign UlcersDocument31 pagesPeptic and Other Benign Ulcersmomi311No ratings yet
- Acute AbdomenDocument7 pagesAcute AbdomenAishaNo ratings yet
- UntitledDocument49 pagesUntitledkedas70No ratings yet
- Intestinal Obstruction: EpidemiologyDocument11 pagesIntestinal Obstruction: EpidemiologyBereket temesgenNo ratings yet
- Pathology of Small & Large Intestine: Developmental LesionsDocument5 pagesPathology of Small & Large Intestine: Developmental LesionsaiadalkhalidiNo ratings yet
- What Is Intestinal ObstructionDocument5 pagesWhat Is Intestinal ObstructionmatrixtrinityNo ratings yet
- Lec 3Document56 pagesLec 3zainabd1964No ratings yet
- Diverticulitis Cure: The Ultimate Diverticulitis Diet: Diverticulitis Recipes: Your Ultimate Diverticulitis CookbookFrom EverandDiverticulitis Cure: The Ultimate Diverticulitis Diet: Diverticulitis Recipes: Your Ultimate Diverticulitis CookbookNo ratings yet
- Diverticulosis, A Simple Guide to the Condition, Treatment and Related DiseasesFrom EverandDiverticulosis, A Simple Guide to the Condition, Treatment and Related DiseasesRating: 1 out of 5 stars1/5 (1)
- 8 Disorders of The Umbilical Cord 2018Document12 pages8 Disorders of The Umbilical Cord 2018Yan Zhen YuanNo ratings yet
- Pedia - Comprehensive Exam (Version 2)Document6 pagesPedia - Comprehensive Exam (Version 2)EricNo ratings yet
- Acute Abdominal Pain in ChildrenDocument82 pagesAcute Abdominal Pain in ChildrensameemNo ratings yet
- 2-Acute Abdominal PainDocument24 pages2-Acute Abdominal Painabdalmajeed alshammaryNo ratings yet
- Umbilical GranulomaDocument3 pagesUmbilical GranulomaNina KharimaNo ratings yet
- Surgery Paper 1 Viva QDocument46 pagesSurgery Paper 1 Viva QMusabbirNo ratings yet
- Embryology McqsDocument15 pagesEmbryology McqsDr-Jahanzaib GondalNo ratings yet
- Meckel's DiverticulumDocument8 pagesMeckel's DiverticulumNurul An NisaNo ratings yet
- GI PathologyDocument22 pagesGI Pathologyzeroun24100% (5)
- Part 2 Exam FM - 2021Document70 pagesPart 2 Exam FM - 2021rahafas95No ratings yet
- Test Bank On GI PathologyDocument14 pagesTest Bank On GI PathologySeff CausapinNo ratings yet
- Acute AbdomenDocument69 pagesAcute AbdomenArwa QishtaNo ratings yet
- 194 Surgical Cases PDFDocument160 pages194 Surgical Cases PDFkint100% (4)
- Small IntDocument59 pagesSmall IntCatalin SavinNo ratings yet
- The Pediatric Visit Gastroenterology 1St Edition Leonard G Feld Online Ebook Texxtbook Full Chapter PDFDocument69 pagesThe Pediatric Visit Gastroenterology 1St Edition Leonard G Feld Online Ebook Texxtbook Full Chapter PDFjane.quashie661100% (6)
- A Huge Completely Isolated Duplication CystDocument6 pagesA Huge Completely Isolated Duplication CystNurlyanti RustamNo ratings yet
- DDX of RIF Mass (Syazwani)Document44 pagesDDX of RIF Mass (Syazwani)Nurul Syazwani RamliNo ratings yet
- Minimally Invasive Surgery: Amar Shah and Anirudh ShahDocument5 pagesMinimally Invasive Surgery: Amar Shah and Anirudh ShahKadelsy BristolNo ratings yet
- Thesis Topics of MS General SurgeryDocument20 pagesThesis Topics of MS General SurgeryNaveed Khan75% (12)
- Family Medicine QuizletDocument28 pagesFamily Medicine QuizletNEsreNo ratings yet
- Meckel's Diverticulum: I. EpidemiologyDocument6 pagesMeckel's Diverticulum: I. EpidemiologyAlessandra EndozoNo ratings yet
- GSDocument9 pagesGSSindhiya DurairajanNo ratings yet
- Gastrointestinal Tract PathologyDocument8 pagesGastrointestinal Tract PathologyMiguel Cuevas Dolot100% (2)
- High Yeild Anatomy.Document14 pagesHigh Yeild Anatomy.SHAKEEL1991No ratings yet
- MCQ NasDocument16 pagesMCQ NasDwi HerawatiNo ratings yet
- Acute AbdomenDocument58 pagesAcute AbdomenkharisaNo ratings yet
- Anasurgery MockboardDocument12 pagesAnasurgery MockboardVince CabahugNo ratings yet
- Minimally Invasive SurgeryDocument6 pagesMinimally Invasive SurgerycarmenNo ratings yet