Professional Documents
Culture Documents
MCN Lec M1L3B Reviewer
MCN Lec M1L3B Reviewer
Uploaded by
Emily Bernat0 ratings0% found this document useful (0 votes)
18 views6 pagesThe document summarizes the processes of spermatogenesis and oogenesis. Spermatogenesis is the process by which sperm are produced in the testes over 65-75 days, beginning at puberty. It involves the differentiation of stem cells into sperm through meiosis and spermiogenesis. Oogenesis begins before birth as primordial follicles form in the ovaries. At puberty, oogenesis involves the maturation of ova through meiotic divisions within developing follicles under the influence of hormones like FSH and LH, potentially culminating in ovulation. The menstrual cycle is regulated by changes in these hormone levels across its four phases.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe document summarizes the processes of spermatogenesis and oogenesis. Spermatogenesis is the process by which sperm are produced in the testes over 65-75 days, beginning at puberty. It involves the differentiation of stem cells into sperm through meiosis and spermiogenesis. Oogenesis begins before birth as primordial follicles form in the ovaries. At puberty, oogenesis involves the maturation of ova through meiotic divisions within developing follicles under the influence of hormones like FSH and LH, potentially culminating in ovulation. The menstrual cycle is regulated by changes in these hormone levels across its four phases.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
18 views6 pagesMCN Lec M1L3B Reviewer
MCN Lec M1L3B Reviewer
Uploaded by
Emily BernatThe document summarizes the processes of spermatogenesis and oogenesis. Spermatogenesis is the process by which sperm are produced in the testes over 65-75 days, beginning at puberty. It involves the differentiation of stem cells into sperm through meiosis and spermiogenesis. Oogenesis begins before birth as primordial follicles form in the ovaries. At puberty, oogenesis involves the maturation of ova through meiotic divisions within developing follicles under the influence of hormones like FSH and LH, potentially culminating in ovulation. The menstrual cycle is regulated by changes in these hormone levels across its four phases.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 6
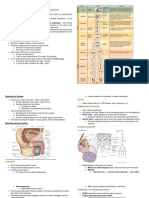
M1 : Lesson 3B: Menstrual Cycle Spermatogenesis
• The process by which the seminiferous
Menstrual cycle tubules of the testes produce sperm.
• A menstrual cycle is a periodic uterine • Begins in males at puberty.
bleeding in response to cyclical • 65 to 75 days.
hormones beginning at puberty and • Begins with spermatogonia (stem
ending at menopause. cells)with diploid (2n) number of
• Menstrual cycles are possible because chromosomes.
of the interplay between the • Some spermatogonia lose contact with
hypothalamus, pituitary, ovaries and the basement membrane and undergo
uterus. developmental changes.
• The cycle varies in length from 23 to 35 • Differentiate into primary
days, averaging 28 days (from the spermatocytes (2n) 46 chromosomes.
beginning of one menstrual flow to the • Each primary spermatocytes replicates
beginning of the next). its DNA and meiosis begins.
• The menstrual cycle is divided into four • 2 Secondary spermatocytes are formed
phases that are characterized by by meiosis I.
changes in the uterine endometrium: • Each secondary spermatocytes 23
(Silbert-Flagg and Pillitteri, 2018) chromosomes, haploid number.
o (1) the proliferative • No further replication occurs in the
o (2) the secretory, secondary spermatocytes.
o (3) the ischemic • Spermiogenesis – final stage of
o (4) Menses spermatogenesis.
• Development of haploid spermatids
into sperm.
• No cell division occurs in
spermiogenesis.
• Spermatids transform into elongated,
slender sperm.
• •Sperm
o 300 million sperm complete the
process of spermatogenesis each
day.
o 60 um long
o Structures that are highly adapted
for reaching and penetrating
secondary oocytes.
o Once ejaculated, most sperm do
not survive more than 48 hours
within the female reproductive
organ.
o Parts of the sperm:
▪ Head
➢ contains nucleaus with 23
chromosomes
▪ Acrosome
➢ covers the anterior two o Germ cells differentiate within the
thirds of the nucleus. ovary into oogonia diploid (2n).
➢ Filled with enzymes that o Diploid oogonia divide mitotically to
help a sperm penetrate a produce millions of germ cells.
secondary oocytes for o Most of the germ cells degenerate ,
fertilization. process known as atresia.
➢ Hyaluronidase and o Few, develops into larger cells
proteases. called primary oocytes.
▪ Tail o Primary oocytes enter prophase of
➢ • Neck – constricted region meiosis I during fetal development
just behind the head that but do not complete that phase
contains centrioles. until after puberty.
➢ Middle piece – contains the o During the arrested meiosis I, each
mitochondria which provide primary oocyte is surrounded by a
the energy (ATP) for single layer of follicular cell.
locomotion of sperm. o Primordial follicle.
➢ Principal piece – longest o Between 5-7 million ova are form in
portion. utero
➢ End piece – terminal, o At birth - 2M primary oocytes
tapering portion of the tail. remain in each ovary.
o By age 7 – 500,000 are present in
each ovary
HORMONAL CONTROL & SEXUAL
o By 22 years – 300,000are present
DEVELOPMENT
o By menopause – none are left
• Androgens – male sex hormones , o The remainder of the primary
produced in testes and adrenal glands oocytes undergo atresia.
• For devt of male sex organs and o Primordial follicle starts to grow,
secondary sex characteristics, developing into primary follicles
spermatogenesis stimulated by the gonadotropins
• Testosterone is one major androgen (FSH and LH) secreted by the
• Leydig cells ( located in testes) secretes anterior pituitary.
testosterone o Primary follicles consists of a
primary oocytes is surrounded by
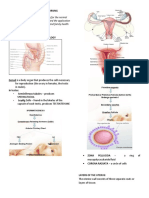
OOGENESIS AND FOLLICULAR DEVELOPMENT granulosa cells.
• Oogenesis o As the primary follicle grows, it
o formation of gametes in the forms a cleart glycoprotein layer
ovaries. called zona pellucida between the
o Begins in females before they are primary oocytes and the granulosa
born. cells.
o Same manner as spermatogenesis; ▪ Theca folliculi – encircles the
meiosis takes place. basement membrane of the
o Fetal development granulosa cells.
primordial(primitive) germ cells ▪ Theca interna – vascularized
migrate from the yolk sac to the internal layer
ovaries. ▪ Theca externa – outermost
layer.
o Secondary follicle becomes larger (FSH) and luteinizing hormone (LH)
turning into a mature (graafian) from the anterior pituitary.
follicle. • Involved mainly in ovarian functions.
o While in this follicle, the diploid • Follicle Stimulating Hormone (FSH)
primary oocytes completes meiosis o Released from the anterior pituitary
I, producing two haploid cells of gland
unequal size – each with 23 o Initiates follicular growth.
chromosomes. o Receptors of FSH exist primarily on
o First polar body the cell membrane of the granulosa
▪ Smaller cell produced By cells of the ovarian follicle
meiosis I. • Luteinizing Hormone (LH).
o Secondary oocytes o Stimulates androgen synthesis by
▪ Begins meiosis II Then stops in the theca cells.
Metaphase. o Progesterone synthesis by the
o Mature (graafian) Follicle soon corpus luteum.
ruptures And releases its Secondary o Stimulates prostaglandin synthesis
oocytes then ovulation by intracellular production of cAMP.
▪ Secondary oocyte is expelled o Triggers ovulation and formation of
into the pelvic cavity together corpus luteum.
with first polar body. • Estrogen
▪ Swept into the uterine tube. o Secreted by ovarian Follicles.
o If fertilization does not occur, it • Progesterone
degenerates. o Secreted mainly by cells of the
o If sperms are present In the uterine corpus luteum.
tube and one penetrates the
secondary oocytes, meiosis II MENSTRUATION
resumes.
▪ Ovum or mature egg unite with • Is an episodic uterine bleeding in
response to cyclic hormonal changes
sperm cell forming diploid (2n),
zygote. • The purpose is to bring an ovum to
o Corpus luteum maturity and renew a uterine tissue bed
▪ contains the remnants of a that will be responsible for the ova’s
mature follicle after ovulation. growth should it be fertilized
▪ Produces progesterone, • That allows for conception and
estrogens, relaxin and inhibin implantation of a new life
until it degenerates into fibrous • Menarche
scar tissue called corpus o first menstrual period in girls.
albicans. o May occur as early as 9 years old or
as late as 17 years old.
HYPOTHALAMIC o Average onsest at 12.4 years
PITUITARYOVARIAN/TESTICULAR AXIS • Normal menstrual Cycle: 23 to 35 days,
average of 28 days.
Gonadotrophin Releasing Hormone (GnRH) • Length/duration: 2 to 7 days, ranges of
• Secreted by the hypothalamus. 1-9 days
• Controls the ovarian and uterine cycles. • Average amount blood loss of 30 to 80
• Stimulates the release, synthesis and ml
storage of follicle stimulating hormone
• Color of menstrual flow: Dark red; a ➢ Follicle that begins to
combination of blood, mucus and develop at the beginning of
endometrial cells. a particular menstrual cycle
• Odor: Similar to marigolds. may not reach maturity and
• Teaching about Menstrual Health ovulate until several
o 1. Exercise – moderate exercise menstrual cycles later.
o 2. Sexual relations- not ➢ Menstrual flow from the
contraindicated uterus
o 3. Activities of daily living- nothing ➢ 50-150 ml of blood, tissue
is contraindicated fluid, mucus and epithelial
o 4. Pain relief- Prostaglandin cells shed from the
inhibitors, applying local heat endometrium.
o 5. Rest – more rest if dysmenorrhea ▪ Events in the Uterus
is present ➢ Decrease estrogen and
o 6. Nutrition- iron supplementation progesterone stimulate the
• Four body structures involved release of prostaglandins.
o 1. Hypothalamus ➢ Prostaglandins causes
o 2. Pituitary gland uterine spiral arterioles to
o 3. Ovaries constrict
o 4. Uterus ➢ cells they supply become
• 4 Phases: oxygen deprived
o Menstrual phase ➢ starts to die
▪ Episodic uterine bleeding in ➢ stratum functionalis sloughs
response to cyclic hormonal off
changes. ➢ menstrual flow passes from
▪ Cyclic monthly changes in the uterine cavity through
ovaries and endometrium in the cervix and vagina
preparations for ovulation. o Preovulatory phase (proliferative)
▪ Monthly shedding off uterine ▪ Time between the end of
lining in response to drop in menstruation and ovulation.
estrogen and progesterone ▪ Events in the Ovaries:
level ➢ Secondary follicles in the
▪ Purpose: ovaries begin to secret
➢ To bring an ovum to estrogen and inhibin.
maturity ➢ A single secondary follicle in
➢ Renew uterine tissue bed one of the two ovaries
that will be responsible for become dominant follicle.
its growth should it be ➢ Dominant follicle secretes
fertilized. estrogen and inhibin which
▪ • Events in the Ovaries: will decrease the secretion
➢ Under the influence of FSH of FSH.
– primordial follicles ➢ Decrease of FSH will cause
develop into primary other less well developed
follicles then into secondary follicles to stop growing and
follicles. undergo atresia.
➢ Takes several months to ➢ One dominant follicle
occur. becomes the mature
(graafian follicle) and ovulation preceded by
continues to enlarge and sudden drop.
ready for ovulation. ➢ Cervical mucous under the
➢ During the final maturation influence of estrogen is
process, the mature follicle favorable to spermatozoa.
continues to increase its ➢ Fern test:
estrogen production. o Cervical mucus forms
➢ Follicular Phase because fernlike patterns when
ovarian follicles are growing placed on a glass slide
and developing. and allowed to dry.
▪ Events in the Uterus o Caused by
➢ Estrogens secreted by the crystallization of
growing ovarian follicles sodium chloride on
stimulate the repair of the mucus fibers known as
endometrium. arborization or ferning.
➢ Stratum basalis undergo ➢ Spinnbarkeit Test :
mitosis and produces a new o Cervical mucus
stratum functionalis. becomes thin and
➢ The thickness of the watery and can be
endometrium doubles to 4 stretched into long
to 10 mm. strands.
➢ Termed as Proliferative ➢ Midmenstrual pain
phase because the ➢ Breast tenderness
endometrium is o Postovulatory phase (secretory)
proliferating. ▪ Time between ovulation and
o Ovulation onset of the next menses.
▪ The rupture of the mature ▪ It is the most constant part of
(graafian) follcile. the female reproductive cycle.
▪ Release of the secondary ▪ Last 14 days in a day cycle, from
oocyte into the pelvic cavity day 15 to day 28.
▪ Occurs on day 14 in a 28 day ▪ Events in one ovary
cycle. ➢ After ovulation, the mature
▪ High levels of estrogens during follicle collapses.
the last part of the preovulatory ➢ A blood clot forms from
phase exerts a positive minor bleeding of the
feedback. ruptured follicle – corpus
▪ Secrete LH and GnRH and hemorrhagicum Corpus
causes ovulation. luteum.
▪ Mittelschmerz – the small ➢ Corpus luteum secretes
amount of blood that leaks into progesterone, estrogen,
the pelvic cavity from the relaxin and inhibin under
rupture follcile can cause pain. the influence of LH.
▪ Signs and symptoms of ➢ Termed as Luteal Phase.
ovulation: ➢ Oocyte is not fertilized –
➢ Basal body temperature the corpus luteum has a
slightly increase 0.2 to 0.5 lifespan of 2 weeks.
˚C on the day following
➢ Its secretory activity
declines
➢ Degenerates into corpus
albicans.
➢ Decrease progesterone,
estrogen, and inhibin
causes loss of negative
feedback suppression Rise
of GnRh, FSG,LH
➢ If the secondary oocyte is
fertilized and begins to
divide.
➢ Corpus luteum persist for 2
weeks.
➢ Chorion of the embryo after
8 days of fertilization will
produce human chorionic
gonadotropin (hCG).
➢ hCG like LH, stimulates the
secretory activity of the
corpus luteum.
▪ Events in the Uterus
➢ Progesterone and estrogens
produced by the corpus
luteum promote growth
and coiling of the
endometrial glands.
➢ Vascularization of the
endometrium.
➢ Thickening of the
endometrium to 12 to 18
mm.
➢ Secretory Period –
secretory activity of the
endometrial glands,
You might also like
- Anatomy of The DogDocument226 pagesAnatomy of The DogAlina Ioana100% (26)
- SpermatogenesisDocument33 pagesSpermatogenesisSalman Xahir100% (1)
- 2 Spermatogenesis DR - GosaiDocument31 pages2 Spermatogenesis DR - GosaiDr.B.B.GosaiNo ratings yet
- Gametogenesis: Mrs Madhu Mishra Associate Professor Department of Lifescience (Zoology) RNTU, BhopalDocument21 pagesGametogenesis: Mrs Madhu Mishra Associate Professor Department of Lifescience (Zoology) RNTU, Bhopalmadhu dwivediNo ratings yet
- Reproductive System Reviewer - BAYLONDocument16 pagesReproductive System Reviewer - BAYLONElijah Joaquin Payumo BaylonNo ratings yet
- Male Reproductive OrganDocument43 pagesMale Reproductive OrganIsrahia CopiocoNo ratings yet
- Human Reproduction - L2Document28 pagesHuman Reproduction - L2israrmarwat6100No ratings yet
- EOT StructureDocument27 pagesEOT StructureNKANo ratings yet
- Gonad & GametogenesisDocument40 pagesGonad & GametogenesisAnggita DaniellaNo ratings yet
- Fertilization and Implantation-1Document9 pagesFertilization and Implantation-1hussain AltaherNo ratings yet
- General Embryology 2022Document130 pagesGeneral Embryology 2022KAMAL ALSOFIANYNo ratings yet
- AndrologyDocument57 pagesAndrologyaginche amareNo ratings yet
- Apigo 3Document11 pagesApigo 3Ms. Jia Mae CasimoNo ratings yet
- Lesson 2 Reproductive StrategiesDocument62 pagesLesson 2 Reproductive StrategiesJeestin Kent GabineraNo ratings yet
- A Gametogenesis 16 12 14 PDFDocument20 pagesA Gametogenesis 16 12 14 PDFDidiNo ratings yet
- Male SubfertilityDocument41 pagesMale SubfertilityIshaThapaNo ratings yet
- EM2.Gametogenesis (At)Document52 pagesEM2.Gametogenesis (At)MUDIN ABDELLANo ratings yet
- Fertilization - CCRGDocument27 pagesFertilization - CCRGTushar AgrawalNo ratings yet
- Spermatogenesis: Feriha Ercan, Ph.D. Dept. Histology and EmbryologyDocument41 pagesSpermatogenesis: Feriha Ercan, Ph.D. Dept. Histology and EmbryologyErdem AltunNo ratings yet
- Gametogenesis: by Anagha Jose Class - Xii Reg ScienceDocument16 pagesGametogenesis: by Anagha Jose Class - Xii Reg ScienceanaghaNo ratings yet
- Gametogenesis by Anagha JoseDocument16 pagesGametogenesis by Anagha JoseanaghaNo ratings yet
- EMBRYOLOGY: Gametogenesis, Fertilization in Details.Document46 pagesEMBRYOLOGY: Gametogenesis, Fertilization in Details.Mercy AdeolaNo ratings yet
- 11 MaleDocument14 pages11 MaleJasmine KaurNo ratings yet
- Gametogenesis p1 PDFDocument13 pagesGametogenesis p1 PDFLiane LomioNo ratings yet
- ANAT0001 Fertilisation and CleavageDocument7 pagesANAT0001 Fertilisation and CleavageOmed ZarifiNo ratings yet
- OogenesisDocument18 pagesOogenesisgvantsaNo ratings yet
- Spermatogenesis & Sperm Maturation : Dr. Amin JanDocument33 pagesSpermatogenesis & Sperm Maturation : Dr. Amin JanSalman XahirNo ratings yet
- AndrologyDocument57 pagesAndrologyyomifgaramuNo ratings yet
- Ana 213 PuhDocument23 pagesAna 213 PuhPRINCE ADEWUMI JONATHANNo ratings yet
- LESSON 9 GametogenesisDocument20 pagesLESSON 9 GametogenesisMelissa ColosagaNo ratings yet
- WWW - Studyguide.pk: Aspects of Human Reproduction Key ObjectivesDocument9 pagesWWW - Studyguide.pk: Aspects of Human Reproduction Key ObjectivesP.P.KarthikeyanNo ratings yet
- Sexual ReproductionDocument26 pagesSexual ReproductionRicky SalazarNo ratings yet
- EMBRYOLOGY - First Week of Human DevelopmentDocument7 pagesEMBRYOLOGY - First Week of Human DevelopmentMeow CattoNo ratings yet
- Human Reproduction SpermatogenesisDocument8 pagesHuman Reproduction SpermatogenesisDEIRDRE ANGELIQUE MURILLONo ratings yet
- Game To GenesisDocument20 pagesGame To GenesisPriya KashyapNo ratings yet
- Group 1 - Male Reproductive TransesDocument8 pagesGroup 1 - Male Reproductive Transesategwen20No ratings yet
- Embryology: by Dr. Manish SataniDocument47 pagesEmbryology: by Dr. Manish SataniDhaval ChauhanNo ratings yet
- SpermatoDocument8 pagesSpermatoabdullahishtiaq8908No ratings yet
- MCN HandoutsDocument22 pagesMCN HandoutsFRANCYM PRINCESSRICH BATENGANo ratings yet
- Chapter 12 Conception and Fetal DevelopmentDocument17 pagesChapter 12 Conception and Fetal DevelopmentRoneshia Michelle Rudolph100% (1)
- CYTOGEN: Chapter 3 Meiosis, Development, and AgingDocument6 pagesCYTOGEN: Chapter 3 Meiosis, Development, and AgingpangetkoNo ratings yet
- Reproductive SystemDocument11 pagesReproductive SystemgabbybibobuNo ratings yet
- GametogenesisDocument35 pagesGametogenesisJason TulipatNo ratings yet
- Reproduction Student MaterialDocument27 pagesReproduction Student MaterialEsosa OdighizuwaNo ratings yet
- GametogenisisDocument43 pagesGametogenisisaimi BatrisyiaNo ratings yet
- SpermatogenesisDocument27 pagesSpermatogenesisSabio DenmenNo ratings yet
- Formation of GametesDocument27 pagesFormation of GametesKalo kajiNo ratings yet
- Lesson4 FertilizationDocument33 pagesLesson4 Fertilizationy041087No ratings yet
- Male Reprroductive FinalsDocument6 pagesMale Reprroductive Finalserikamayranoa14No ratings yet
- The Human Reproductive SystemDocument7 pagesThe Human Reproductive SystemAlloiza CaguiclaNo ratings yet
- Human Reproduction - Male Reproductive SystemDocument15 pagesHuman Reproduction - Male Reproductive Systemafrinadewan683No ratings yet
- Anbt - 608: Submitted ToDocument50 pagesAnbt - 608: Submitted ToMayuriGulhaneNo ratings yet
- Cell Cycle & Gametogenesis: DR Sharifa Abdul Aziz FPSK, Usim 2008/2009Document37 pagesCell Cycle & Gametogenesis: DR Sharifa Abdul Aziz FPSK, Usim 2008/2009Jessica PachecoNo ratings yet
- ReproductionDocument82 pagesReproductionBIJAY GAUTAMNo ratings yet
- SpermatogenesisDocument16 pagesSpermatogenesisFazilaNo ratings yet
- Chapter 15 Sexual Reproduction, Development and Growth in HumansDocument38 pagesChapter 15 Sexual Reproduction, Development and Growth in HumansYiHui SiaNo ratings yet
- Human Reproduction Unit Review WorksheetDocument25 pagesHuman Reproduction Unit Review Worksheetmofid monirNo ratings yet
- Human Life Cycle & Male Reproductive System: Dr. Muhjah Falah Hasan PH.D in Infertility & Clinical ReproductionDocument32 pagesHuman Life Cycle & Male Reproductive System: Dr. Muhjah Falah Hasan PH.D in Infertility & Clinical Reproductionsuad aliNo ratings yet
- Anaphy Reviewer FINALSDocument4 pagesAnaphy Reviewer FINALSim. EliasNo ratings yet
- Chapter XII ReproductiveDocument17 pagesChapter XII ReproductiveHannah DiñosoNo ratings yet
- M3 Pre TaskDocument1 pageM3 Pre TaskEmily BernatNo ratings yet
- CHN Lab Retdem With RationaleDocument7 pagesCHN Lab Retdem With RationaleEmily BernatNo ratings yet
- MCN Lec M1L3A ReviewerDocument10 pagesMCN Lec M1L3A ReviewerEmily BernatNo ratings yet
- MCN Lec M1L1 ReviewerDocument4 pagesMCN Lec M1L1 ReviewerEmily BernatNo ratings yet
- MCN LectureDocument8 pagesMCN LectureEmily BernatNo ratings yet
- CHN RevsDocument25 pagesCHN RevsEmily BernatNo ratings yet
- MCN Lec M8 TransesDocument9 pagesMCN Lec M8 TransesEmily BernatNo ratings yet
- MCN Lec M1L2 ReviewerDocument10 pagesMCN Lec M1L2 ReviewerEmily BernatNo ratings yet
- MCN Lec M7 TransesDocument8 pagesMCN Lec M7 TransesEmily BernatNo ratings yet
- Pharmacology 1 4Document61 pagesPharmacology 1 4Emily BernatNo ratings yet
- Nursing Practice 1: PhilippinesDocument25 pagesNursing Practice 1: PhilippinesEmily BernatNo ratings yet
- NCM 102 - M3-Post TaskDocument8 pagesNCM 102 - M3-Post TaskEmily BernatNo ratings yet
- NCP CompilationDocument29 pagesNCP CompilationEmily BernatNo ratings yet
- Mod 2 CHN Lec 2Document11 pagesMod 2 CHN Lec 2Emily BernatNo ratings yet
- Sample-Pattern Ranking - FNCP Teaching-PLanDocument5 pagesSample-Pattern Ranking - FNCP Teaching-PLanEmily BernatNo ratings yet
- Module4 6fundamentals in NursingDocument14 pagesModule4 6fundamentals in NursingEmily BernatNo ratings yet
- Module 4 Funda LecDocument5 pagesModule 4 Funda LecEmily BernatNo ratings yet
- Module-2-Overview of The Professional Nursing PracticesDocument45 pagesModule-2-Overview of The Professional Nursing PracticesEmily BernatNo ratings yet
- Module-1-Nursing As A Profession1Document48 pagesModule-1-Nursing As A Profession1Emily BernatNo ratings yet
- Module4 6fundamentals in NursingDocument14 pagesModule4 6fundamentals in NursingEmily BernatNo ratings yet
- Module 1 3fundamentals in NursingreviewerDocument20 pagesModule 1 3fundamentals in NursingreviewerEmily BernatNo ratings yet
- Instructional Materials: Dovie Brabante-Ponciano, MAN, RNDocument28 pagesInstructional Materials: Dovie Brabante-Ponciano, MAN, RNEmily BernatNo ratings yet
- Centro Escolar University Makati Audited Summary of Assesment Second Semester Sy 2021-2022 Science Courses Plan ADocument4 pagesCentro Escolar University Makati Audited Summary of Assesment Second Semester Sy 2021-2022 Science Courses Plan AEmily BernatNo ratings yet
- M1-3 RevDocument19 pagesM1-3 RevEmily BernatNo ratings yet
- Lec - M4. Post Task I - Cardiovascular SystemDocument2 pagesLec - M4. Post Task I - Cardiovascular SystemEmily BernatNo ratings yet
- M4 6 Funda Lec ReviewerDocument15 pagesM4 6 Funda Lec ReviewerEmily BernatNo ratings yet
- B3 M2cia2Document2 pagesB3 M2cia2Emily BernatNo ratings yet
- B3 M7posttaskDocument8 pagesB3 M7posttaskEmily BernatNo ratings yet
- Health Education MidtermsDocument9 pagesHealth Education MidtermsEmily BernatNo ratings yet
- Finals: Anatomy and Physiology Lecture: M4: L1. Hematopoeisis Hemopoietic Growth FactorsDocument33 pagesFinals: Anatomy and Physiology Lecture: M4: L1. Hematopoeisis Hemopoietic Growth FactorsEmily BernatNo ratings yet
- Feline AbdominAl Ultrasonography Jounal of Feline Medicine and Surgery 2020Document19 pagesFeline AbdominAl Ultrasonography Jounal of Feline Medicine and Surgery 2020antonio arteagaNo ratings yet
- Miller & Cohen 2001 An Integrative Theory of Prefrontal Cortex FunctionDocument39 pagesMiller & Cohen 2001 An Integrative Theory of Prefrontal Cortex FunctionhoorieNo ratings yet
- Biopsych 02/07/2015: 1. Resting Membrane PotentialDocument2 pagesBiopsych 02/07/2015: 1. Resting Membrane PotentialMarvic SueltoNo ratings yet
- DLL SCI9circulatory3Document3 pagesDLL SCI9circulatory3Mantikar IsmaelNo ratings yet
- Cytokines and Interferons Types and FunctionsDocument25 pagesCytokines and Interferons Types and FunctionsSereen Abd El-rahmanNo ratings yet
- EI2311 Biomedical Instrumentation SyllabusDocument6 pagesEI2311 Biomedical Instrumentation Syllabuspriya0% (1)
- Digestive System: Digestive Glands. Alimentary CanalDocument27 pagesDigestive System: Digestive Glands. Alimentary CanalAnkit NariyaNo ratings yet
- Syphilinum. (Luesinum.) - THE GUIDING SYMPTOMS OF OUR MATERIA MEDICA by CONSTANT PDFDocument24 pagesSyphilinum. (Luesinum.) - THE GUIDING SYMPTOMS OF OUR MATERIA MEDICA by CONSTANT PDFHarrison DavidsonNo ratings yet
- CirculatorySystemSE - Anthony HernandezDocument5 pagesCirculatorySystemSE - Anthony HernandezAnthony Hernandez100% (1)
- Relationship of Tooth Grinding Pattern During Sleep Bruxism and Temporomandibular Joint StatusDocument9 pagesRelationship of Tooth Grinding Pattern During Sleep Bruxism and Temporomandibular Joint StatusJonathan GIraldo MartinezNo ratings yet
- Smile Line and Periodontium Visibility: Clinical and Research ReportDocument9 pagesSmile Line and Periodontium Visibility: Clinical and Research ReportMed-Amine TouloutNo ratings yet
- Group 18 Problem 1B: Thedi Darma Wijaya 405090120Document46 pagesGroup 18 Problem 1B: Thedi Darma Wijaya 405090120mty_aldNo ratings yet
- Winter - 18 Examination Subject Title: Human Anatomy Physiology Subject CodeDocument23 pagesWinter - 18 Examination Subject Title: Human Anatomy Physiology Subject CodeDAMBALENo ratings yet
- Third Quarter Examination Tle 8: Department of EducationDocument3 pagesThird Quarter Examination Tle 8: Department of EducationJaneNo ratings yet
- Laporan Kematian Cianjur AprilDocument9 pagesLaporan Kematian Cianjur AprilTri Utami NingrumNo ratings yet
- Histology of Large IntestineDocument38 pagesHistology of Large IntestinedoyoumatterindeedNo ratings yet
- Case Study - AppendectomyDocument34 pagesCase Study - Appendectomypuchay_chiepipaii100% (2)
- BLOODDocument5 pagesBLOODSora TensaiNo ratings yet
- Glandular EpitheliumDocument5 pagesGlandular EpitheliumNakuru SandwichNo ratings yet
- (Reference Series in Biomedical Engineering) Wolfgang Holnthoner, Andrea Banfi, James Kirkpatrick, Heinz Redl (Eds.) - Vascularization For Tissue Engineering and Regenerative Medicine-Springer InternaDocument231 pages(Reference Series in Biomedical Engineering) Wolfgang Holnthoner, Andrea Banfi, James Kirkpatrick, Heinz Redl (Eds.) - Vascularization For Tissue Engineering and Regenerative Medicine-Springer InternaIsidoro OlveraNo ratings yet
- The Endocrine SystemDocument2 pagesThe Endocrine SystemRenz Carlvince Butihen-Billones0% (1)
- Grand Case PresentationDocument59 pagesGrand Case PresentationRon Lucernas MayugaNo ratings yet
- The Bilingual Brain: Proficiency and Age of Acquisition of The Second LanguageDocument12 pagesThe Bilingual Brain: Proficiency and Age of Acquisition of The Second LanguageAnn KarapNo ratings yet
- Excretory SystemDocument1 pageExcretory SystemMica Dell MartinezNo ratings yet
- Cornell Notes Template Health TemplateDocument3 pagesCornell Notes Template Health TemplateBrittany EncisoNo ratings yet
- 2 B. Inggris Ips Kunci Pembahasan Paket A PDFDocument7 pages2 B. Inggris Ips Kunci Pembahasan Paket A PDFAksanNo ratings yet
- Learn CBSE: Body Movements Class 6 Extra Questions Science Chapter 8Document5 pagesLearn CBSE: Body Movements Class 6 Extra Questions Science Chapter 8Naresh world SinghNo ratings yet
- Difference Between Mast Cell and BasophilDocument3 pagesDifference Between Mast Cell and Basophilponbohacop100% (1)
- Tissues Pre LabDocument43 pagesTissues Pre LabCindy-chan DelfinNo ratings yet