Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
12 viewsPyloric Stenosis
Pyloric Stenosis
Uploaded by
fdgrgPyloric stenosis is a condition in infants where the pyloric sphincter muscle thickens, preventing food from exiting the stomach. This causes projectile vomiting and leads to dehydration and malnutrition. While the exact cause is unknown, it often involves genetic and environmental factors. Diagnosis involves physical exam finding an olive-shaped stomach mass and ultrasound or barium imaging. Treatment is pyloromyotomy surgery to cut the thickened muscle. With fluid resuscitation pre-op and careful post-op care, outcomes are typically good.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You might also like
- Detailed Lesson Plan in English IV - COMPOUND SENTENCEDocument12 pagesDetailed Lesson Plan in English IV - COMPOUND SENTENCEMadhie Gre Dela Provi94% (16)
- Talal Asad - Anthropology and The Colonial EncounterDocument4 pagesTalal Asad - Anthropology and The Colonial EncounterTania Saha100% (1)
- Pyloric Stenosis: CLASS:-B.Sc. Nursing 3 YearDocument38 pagesPyloric Stenosis: CLASS:-B.Sc. Nursing 3 YearshikhaNo ratings yet
- Part 11 Metal Detector Manual PDFDocument24 pagesPart 11 Metal Detector Manual PDFOrlando Melipillan100% (1)
- Y8 Textiles WorkbookDocument68 pagesY8 Textiles WorkbookCharlene Joy100% (1)
- Pyloric Stenosis: CLASS:-B.Sc. Nursing 3 YearDocument38 pagesPyloric Stenosis: CLASS:-B.Sc. Nursing 3 Yearshikha100% (2)
- Pyloric StenosisDocument47 pagesPyloric StenosisgeethsreesatNo ratings yet
- GI DisordersDocument80 pagesGI DisordersjoycechicagoNo ratings yet
- Pyloric Stenosis OriginalDocument66 pagesPyloric Stenosis OriginalNITHA KNo ratings yet
- Pyloric Stenosis Case StudyDocument37 pagesPyloric Stenosis Case StudyFaith Torralba100% (3)
- Hypertrophic Pyloric StenosisDocument17 pagesHypertrophic Pyloric StenosisMohammed Fareed100% (1)
- Pediatric Care Online AAPDocument18 pagesPediatric Care Online AAPNikola StojsicNo ratings yet
- Emesis in The NewbornDocument34 pagesEmesis in The NewbornVasishta NadellaNo ratings yet
- Congenital Anomalies of GiDocument94 pagesCongenital Anomalies of GiPadmaNo ratings yet
- Pyloric Stenosis: Supervisor: DR NTAGANDA Edmond, Consultant Ped SurgDocument21 pagesPyloric Stenosis: Supervisor: DR NTAGANDA Edmond, Consultant Ped SurgJames NTEGEREJIMANANo ratings yet
- Hirschsprung Disease PPTDocument48 pagesHirschsprung Disease PPTKathleen BalauagNo ratings yet
- Pyloric StenosisDocument3 pagesPyloric Stenosismagisasamundo100% (1)
- Pyloric Stenosis WDocument11 pagesPyloric Stenosis WKlaue Neiv CallaNo ratings yet
- 20 PediatricDocument31 pages20 PediatricMahmoud AbuAwadNo ratings yet
- Canine PyometraDocument5 pagesCanine Pyometrammary09No ratings yet
- Pyloric Stenosis PDFDocument3 pagesPyloric Stenosis PDFKiiza AloysiusNo ratings yet
- NCM 109 High Risk PregnancyDocument11 pagesNCM 109 High Risk PregnancyLea BorceNo ratings yet
- Textbook DiscussionDocument6 pagesTextbook DiscussionHahak UkukNo ratings yet
- Nursing Care of The Child With A Gastrointestinal DisordersDocument46 pagesNursing Care of The Child With A Gastrointestinal Disorderstalaekrema01No ratings yet
- In Partial Fulfillment For The Requirements in R.L.E: Submitted By: Elaine Blanche R. GonzalezDocument6 pagesIn Partial Fulfillment For The Requirements in R.L.E: Submitted By: Elaine Blanche R. GonzalezBlanche GonzalezNo ratings yet
- 8. Care of Child With GI Dysfunction (1) ءءءءDocument44 pages8. Care of Child With GI Dysfunction (1) ءءءءNuhaNo ratings yet
- C. Disorders of The Lowel BowelDocument69 pagesC. Disorders of The Lowel BowelJmarie Brillantes PopiocoNo ratings yet
- Pyloric StenosisDocument4 pagesPyloric StenosisAaliyaan KhanNo ratings yet
- Hirschsprung'S Disease OR Congenital Aganglionic MegacolonDocument59 pagesHirschsprung'S Disease OR Congenital Aganglionic MegacolonHarshika KDGNo ratings yet
- G.I Disorders Part 2Document53 pagesG.I Disorders Part 2شبلي غرايبهNo ratings yet
- Patient Scenario, Chapter 45, Nursing Care of A Family When A Child Has A Gastrointestinal DisorderDocument93 pagesPatient Scenario, Chapter 45, Nursing Care of A Family When A Child Has A Gastrointestinal DisorderDay MedsNo ratings yet
- Parrish July 2013Document7 pagesParrish July 2013Tada MinionNo ratings yet
- Nursing Care of The Child With Gastrointestinal DisordersDocument50 pagesNursing Care of The Child With Gastrointestinal Disordersمهند الرحيليNo ratings yet
- Approach To The Child With Nausea and Vomiting: by DR - Ryan Al - GhanemiDocument50 pagesApproach To The Child With Nausea and Vomiting: by DR - Ryan Al - GhanemiyusufharkianNo ratings yet
- Gastro - NelsonDocument14 pagesGastro - NelsonGemma OrquioNo ratings yet
- PBL No Bowel Output in NeonatesDocument24 pagesPBL No Bowel Output in NeonatesOTOH RAYA OMARNo ratings yet
- MCN Report Polyhydramnios 1Document24 pagesMCN Report Polyhydramnios 1Vincent CuyucaNo ratings yet
- Common Diseases of The InfantDocument131 pagesCommon Diseases of The Infanthed-janquillanoNo ratings yet
- FinalsDocument6 pagesFinalsjcmrtrzNo ratings yet
- Pyloric StenosisDocument20 pagesPyloric Stenosisjohnfoday2022No ratings yet
- Alteration in MetabolismDocument26 pagesAlteration in MetabolismAileen MonaresNo ratings yet
- Omphalocelevsgastroschisis 160810122732Document23 pagesOmphalocelevsgastroschisis 160810122732LNICCOLAIO100% (1)
- Competency Appraisal 1 Reviewer-1Document53 pagesCompetency Appraisal 1 Reviewer-1Paolo Carubio100% (1)
- Acute Appendicitis: History and ExaminationDocument6 pagesAcute Appendicitis: History and ExaminationPraktek Dokter Umum drjosefdrelsyNo ratings yet
- Feeding ProblemsDocument33 pagesFeeding ProblemsuouoNo ratings yet
- Acute Abdominal Pain in ChildrenDocument53 pagesAcute Abdominal Pain in ChildrenSutapa PawarNo ratings yet
- Infantile Pyloric StenosisDocument6 pagesInfantile Pyloric StenosisAksha PraiselinNo ratings yet
- APSA Gastroschisis Brochure FNLDocument5 pagesAPSA Gastroschisis Brochure FNLFarzana AhmedNo ratings yet
- Pyloric StenosisDocument5 pagesPyloric Stenosisensoooooooooo100% (1)
- Gastrointestinal System Symptoms and Signs of Gastrointes Tinal ProblemsDocument77 pagesGastrointestinal System Symptoms and Signs of Gastrointes Tinal ProblemsSindhu BabuNo ratings yet
- Chronic Constipation in Children: BMJ (Online) December 2006Document6 pagesChronic Constipation in Children: BMJ (Online) December 2006Residen KardiologiNo ratings yet
- Congenital Development Disorder of Esophagus, Stomach, Duodenum, Abdomen Wall, Anus and RectumDocument56 pagesCongenital Development Disorder of Esophagus, Stomach, Duodenum, Abdomen Wall, Anus and RectumSarah Nabella PutriNo ratings yet
- Week 8 Pedia Pediatric GI DisturbancesDocument110 pagesWeek 8 Pedia Pediatric GI DisturbancesJaja ManezNo ratings yet
- Gastro NephroDocument93 pagesGastro Nephrohasanatiya41No ratings yet
- Imperforate AnusDocument17 pagesImperforate AnusNalzaro Emyril100% (1)
- Common GI DiseasesDocument116 pagesCommon GI DiseasesmeleseNo ratings yet
- Pedia GiDocument10 pagesPedia GiCam IbardolasaNo ratings yet
- Case Presentation 4 AGEDocument33 pagesCase Presentation 4 AGERoselyn VelascoNo ratings yet
- Constipation - Emergency Management in - Children 2018Document10 pagesConstipation - Emergency Management in - Children 2018Alma Rebeca Mota NovaNo ratings yet
- Abdominal Wall Defects: Omphalocele and Gastroschisis: DR - Enono Yhoshu Department of Pediatric SurgeryDocument42 pagesAbdominal Wall Defects: Omphalocele and Gastroschisis: DR - Enono Yhoshu Department of Pediatric SurgeryYogi drNo ratings yet
- Abdominal Pain and Vomiting in ChildrenDocument18 pagesAbdominal Pain and Vomiting in ChildrenSimon Ganesya RahardjoNo ratings yet
- Prelim 01Document6 pagesPrelim 01labilabi labNo ratings yet
- University of Mosul / College of Nursing Child and Adolescent Health NursingDocument11 pagesUniversity of Mosul / College of Nursing Child and Adolescent Health NursingRayan AhmedNo ratings yet
- Dysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandDysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Marfan Syndrome Marfan Syndrome Is A Degenerative Generalized Disorder of The Connective Tissue With An InciDocument2 pagesMarfan Syndrome Marfan Syndrome Is A Degenerative Generalized Disorder of The Connective Tissue With An IncifdgrgNo ratings yet
- Substance Abuse Handout MCHDocument5 pagesSubstance Abuse Handout MCHfdgrgNo ratings yet
- Local Media4906741505093406640Document7 pagesLocal Media4906741505093406640fdgrgNo ratings yet
- Coral Reefs in The PhilippinesDocument2 pagesCoral Reefs in The PhilippinesfdgrgNo ratings yet
- MARFANDocument17 pagesMARFANfdgrgNo ratings yet
- What Is An STIDocument7 pagesWhat Is An STIfdgrgNo ratings yet
- CHE2Document1 pageCHE2fdgrgNo ratings yet
- rs2 AssDocument1 pagers2 AssfdgrgNo ratings yet
- Cleft Lip and PalateDocument1 pageCleft Lip and PalatefdgrgNo ratings yet
- Neuraltube DefectsDocument3 pagesNeuraltube DefectsfdgrgNo ratings yet
- Ai-Ai ResumeDocument3 pagesAi-Ai ResumeNeon True BeldiaNo ratings yet
- Relatorio Mano JulioDocument7 pagesRelatorio Mano JulioProGeo Projetos AmbientaisNo ratings yet
- N. Mixture, CombinationDocument2 pagesN. Mixture, CombinationYareniNo ratings yet
- Alarm Security Pic - Google ShoppingDocument1 pageAlarm Security Pic - Google Shoppingleeleeleebc123No ratings yet
- Peptides and Proteins: M.Prasad Naidu MSC Medical Biochemistry, PH.DDocument30 pagesPeptides and Proteins: M.Prasad Naidu MSC Medical Biochemistry, PH.DDr. M. Prasad NaiduNo ratings yet
- Getting The Most From Lube Oil AnalysisDocument16 pagesGetting The Most From Lube Oil AnalysisGuru Raja Ragavendran Nagarajan100% (2)
- Padiernos vs. PeopleDocument22 pagesPadiernos vs. PeopleMariel ManingasNo ratings yet
- Synchronous Alternators: Three-Phase BrushlessDocument5 pagesSynchronous Alternators: Three-Phase BrushlessĐại DươngNo ratings yet
- DMX DC Motor ControllerDocument23 pagesDMX DC Motor ControlleromargarayNo ratings yet
- Themelis Ulloa LandfillDocument15 pagesThemelis Ulloa LandfillHenry Bagus WicaksonoNo ratings yet
- Name:: Nyoman Gede Abhyasa Class: X Mipa 2 Absent: 25 AnswersDocument2 pagesName:: Nyoman Gede Abhyasa Class: X Mipa 2 Absent: 25 AnswersRetrify - Random ContentNo ratings yet
- Taylor Swift LyricsDocument2 pagesTaylor Swift LyricsElsie DomeNo ratings yet
- Service Manual - NEC Versa 2700 Series LaptopDocument130 pagesService Manual - NEC Versa 2700 Series LaptopToan NguyenNo ratings yet
- MAD Practical 6Document15 pagesMAD Practical 6DIVYESH PATELNo ratings yet
- Ethical Considerations Dissertation ExampleDocument7 pagesEthical Considerations Dissertation ExampleBuyPapersOnlineCanada100% (1)
- Inactive Volcanoes in The Philippine SDocument6 pagesInactive Volcanoes in The Philippine SChristian ParadoNo ratings yet
- Bstem-5 4Document61 pagesBstem-5 4G-SamNo ratings yet
- Autumn Activity BookDocument33 pagesAutumn Activity Bookbuzuleacnadya100% (3)
- 2.20 Optimizing Control: F. G. Shinskey C. G. Laspe B. G. Lipták M. RuelDocument10 pages2.20 Optimizing Control: F. G. Shinskey C. G. Laspe B. G. Lipták M. RueljigjigawNo ratings yet
- Ballistic - August September 2021Document168 pagesBallistic - August September 2021andrewrowe100% (2)
- Bydf3 ElectricDocument61 pagesBydf3 ElectricIvan Avila100% (1)
- 044.QTRE409 - International Human Resource ManagementDocument11 pages044.QTRE409 - International Human Resource ManagementDo Minh Gia AnNo ratings yet
- Biogas ProductionDocument7 pagesBiogas ProductionFagbohungbe MichaelNo ratings yet
- Maunakea Brochure C SEED and L Acoustics CreationsDocument6 pagesMaunakea Brochure C SEED and L Acoustics Creationsmlaouhi MajedNo ratings yet
- Guru ShishyaDocument3 pagesGuru ShishyacktacsNo ratings yet
- Rock Mass Characterization by High-Resolution SoniDocument17 pagesRock Mass Characterization by High-Resolution SoniJose AleNo ratings yet
Pyloric Stenosis
Pyloric Stenosis
Uploaded by
fdgrg0 ratings0% found this document useful (0 votes)
12 views5 pagesPyloric stenosis is a condition in infants where the pyloric sphincter muscle thickens, preventing food from exiting the stomach. This causes projectile vomiting and leads to dehydration and malnutrition. While the exact cause is unknown, it often involves genetic and environmental factors. Diagnosis involves physical exam finding an olive-shaped stomach mass and ultrasound or barium imaging. Treatment is pyloromyotomy surgery to cut the thickened muscle. With fluid resuscitation pre-op and careful post-op care, outcomes are typically good.
Original Description:
fffjglgh
Original Title
PYLORIC STENOSIS
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentPyloric stenosis is a condition in infants where the pyloric sphincter muscle thickens, preventing food from exiting the stomach. This causes projectile vomiting and leads to dehydration and malnutrition. While the exact cause is unknown, it often involves genetic and environmental factors. Diagnosis involves physical exam finding an olive-shaped stomach mass and ultrasound or barium imaging. Treatment is pyloromyotomy surgery to cut the thickened muscle. With fluid resuscitation pre-op and careful post-op care, outcomes are typically good.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
12 views5 pagesPyloric Stenosis
Pyloric Stenosis
Uploaded by
fdgrgPyloric stenosis is a condition in infants where the pyloric sphincter muscle thickens, preventing food from exiting the stomach. This causes projectile vomiting and leads to dehydration and malnutrition. While the exact cause is unknown, it often involves genetic and environmental factors. Diagnosis involves physical exam finding an olive-shaped stomach mass and ultrasound or barium imaging. Treatment is pyloromyotomy surgery to cut the thickened muscle. With fluid resuscitation pre-op and careful post-op care, outcomes are typically good.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 5
LET’S DEFINE
Pylorus- The part of the stomach that connects to the
duodenum (first part of the small intestine). It is a valve
that opens and closes during digestion.
Pyloric Sphincter- a ring of smooth muscle that
regulates release of gastric contents into the
duodenum.
Stenosis- it means “narrowing”
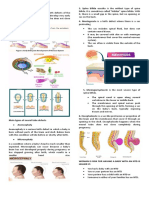
The stomach is an organ in the upper abdomen. It can
Duodenum- it is first part of the small intestine.
be divided into fundus, body, antrum and pylorus.
Hyperplasia- the increase (in mass) of an organ or Pylorus connects the stomach to the duodenum (the 1
tissue. st section of the small intestine). It is a valve that opens
and closes during digestion. Together, the pylorus and
Hypertrophy- is an increase in the size of cells or tissues. duodenum play an important role in helping to move
Pyloromyotomy- an incision in the wall of the pylorus. the food through the digestive system.
Laparoscopy- is a type of surgical procedure that allows
a surgeon to access the inside of the abdomen and
pelvis without having large incision in the skin.
PYLORIC STENOSIS
-A condition wherein the muscles of the pylorus are
abnormally thickened, which prevents the stomach
from emptying into the small intestine, and food backs
up into the esophagus.
➢This type of blockage is also referred to as a gastric
\
outlet obstruction. Wherein hypertrophy and
hyperplasia occurs in the muscles surrounding the PATHOPHYSIOLOGY
sphincter. Resulting in elongation and narrowing of
pyloric channel
➢ Muscles in the pyloric sphincter may thickened to as
twice its size, with a consistency similar to a cartilage.
➢ This condition usually develops in the first few weeks
of life (4-6 weeks).
➢ The exact cause is unknown but multifactorial
inheritance is most likely the cause of this condition.
➢ Pyloric stenosis occurs in 1 in 500-1000 live births,
affecting 4 males for every 1 female
➢ Usually occurs in first born white (Caucasian) male
infants, seen less frequently in African-American and
Asian infants.
➢ Occurs less frequently in breastfed infants than
formulafed infants.
The cause of pyloric stenosis is unknown, but factors MANIFESTATION
that might play a role are as follows:
❑ Projectile vomiting
✓ Hyperplasia
❑ Persistent-Chronic hunger
✓ Hypertrophy
❑ Decreased urine output
✓ Environmental factors
❑ Constipation
✓ Genetic Factors
❑ Signs of Dehydration and Malnutrition
Assessment and Diagnostic Findings
❑ Weight Loss
• Laboratory studies. Electrolytes, pH, BUN, and
creatinine levels should be obtained at the same time as ❑ Epigastric distension
intravenous access in patients with pyloric stenosis.
❑ Palpable olive-shaped tumor in the epigastrium
• Ultrasonography. If the clinical presentation is typical
and an olive is felt, the diagnosis is almost certain; ❑ Visible gastric peristaltic waves
however formal ultrasonography is still recommended NURSING Assessment in a child with pyloric stenosis
to evaluate the pylorus and confirm the diagnosis. include:
• Radiography. Radiographic studies with barium ➢ Assess the child’s history of vomiting. Ask when the
swallow show an abnormal retention of barium in the vomiting started and determine the character of the
stomach and increased peristalsis. vomiting.
Risk factors for pyloric stenosis include: ➢ Assess for the child’s elimination
✓ Sex of the baby: Full-term, first-born male babies are ➢ Physical exam
at higher risk. It’s less likely in baby girls.
NURSING INTERVENTION
✓ Race: It happens more to white infants, especially of
European descent. • Maintain adequate nutrition and fluid intake
✓ Family history of pyloric stenosis: About 15% of • Provide mouth care
infants with pyloric stenosis have a family history of it.
• Physical exam
The parent who had the condition before also matters.
An infant’s risk is three times higher if the mother had • Promote skin integrity
pyloric stenosis, compared to the father.
• Promote family coping
✓ Smoking: Babies whose mothers smoked during
Medical Treatment
pregnancy are at higher risk.
✓ Surgery called pyloromyotomy treats pyloric stenosis
✓ Antibiotics: Some babies who needed antibiotics
shortly after birth may be at higher risk. Babies whose ✓ Surgery can be performed laparoscopically or through
mothers took certain antibiotics late in pregnancy may a supra-umbilical incision
also have a higher risk. ✓ There’s no way to prevent pyloric stenosis. If you
✓ Approach to feeding: Some studies of babies drinking know pyloric stenosis runs in your family, make sure to
formula show an increased risk for pyloric stenosis. But tell your healthcare provider.
it remains unclear if the risk comes from the bottle or
the formula.
Medical Management (PRE-OPERATIVE) CONCLUSION
• Fluid Regimen and Electrolyte Correction - The baby ✓ Pyloric stenosis is a problem that causes forceful
will not have any surgery until the blood biochemistry is vomiting in babies from birth to 6 months of age. It can
normalized. lead to dehydration. In pyloric stenosis, the muscles in
the stomach that connect to the small intestine thicken.
• Proper Care of Infant
This causes the opening of the pylorus to become
- Monitor vital signs narrow.
- Referral process ✓ Pyloric stenosis is surgically managed, with a
Ramstedt’s pyloromyotomy7 and should not be
- Comfort measures-semi-fowlers or R side lying undertaken until any fluid or electrolyte abnormalities
- Education have been correction. Surgery can be performed
laparoscopically or through a supra-umbilical incision
Postoperative Care
• Monitor IV Fluid
• Provide feeding as prescribed by surgeon
• Document INO
• Monitor surgical site
NURSING DIAGNOSIS
Based on the assessment data, the major nursing
diagnoses are:
• Imbalanced nutrition: less than body requirements
related to inability to retain food.
• Deficient fluid volume related to frequent vomiting.
• Impaired oral mucous membrane related to NPO
status.
• Risk for impaired skin integrity related to fluid and
nutritional deficit.
• Compromised family coping related to seriousness of
illness and impending surgery.
EVALUATION
Goals are met as evidenced by:
• Improved nutrition and hydration
• Maintained mouth and skin integrity
• Relieved family anxiety
You might also like
- Detailed Lesson Plan in English IV - COMPOUND SENTENCEDocument12 pagesDetailed Lesson Plan in English IV - COMPOUND SENTENCEMadhie Gre Dela Provi94% (16)
- Talal Asad - Anthropology and The Colonial EncounterDocument4 pagesTalal Asad - Anthropology and The Colonial EncounterTania Saha100% (1)
- Pyloric Stenosis: CLASS:-B.Sc. Nursing 3 YearDocument38 pagesPyloric Stenosis: CLASS:-B.Sc. Nursing 3 YearshikhaNo ratings yet
- Part 11 Metal Detector Manual PDFDocument24 pagesPart 11 Metal Detector Manual PDFOrlando Melipillan100% (1)
- Y8 Textiles WorkbookDocument68 pagesY8 Textiles WorkbookCharlene Joy100% (1)
- Pyloric Stenosis: CLASS:-B.Sc. Nursing 3 YearDocument38 pagesPyloric Stenosis: CLASS:-B.Sc. Nursing 3 Yearshikha100% (2)
- Pyloric StenosisDocument47 pagesPyloric StenosisgeethsreesatNo ratings yet
- GI DisordersDocument80 pagesGI DisordersjoycechicagoNo ratings yet
- Pyloric Stenosis OriginalDocument66 pagesPyloric Stenosis OriginalNITHA KNo ratings yet
- Pyloric Stenosis Case StudyDocument37 pagesPyloric Stenosis Case StudyFaith Torralba100% (3)
- Hypertrophic Pyloric StenosisDocument17 pagesHypertrophic Pyloric StenosisMohammed Fareed100% (1)
- Pediatric Care Online AAPDocument18 pagesPediatric Care Online AAPNikola StojsicNo ratings yet
- Emesis in The NewbornDocument34 pagesEmesis in The NewbornVasishta NadellaNo ratings yet
- Congenital Anomalies of GiDocument94 pagesCongenital Anomalies of GiPadmaNo ratings yet
- Pyloric Stenosis: Supervisor: DR NTAGANDA Edmond, Consultant Ped SurgDocument21 pagesPyloric Stenosis: Supervisor: DR NTAGANDA Edmond, Consultant Ped SurgJames NTEGEREJIMANANo ratings yet
- Hirschsprung Disease PPTDocument48 pagesHirschsprung Disease PPTKathleen BalauagNo ratings yet
- Pyloric StenosisDocument3 pagesPyloric Stenosismagisasamundo100% (1)
- Pyloric Stenosis WDocument11 pagesPyloric Stenosis WKlaue Neiv CallaNo ratings yet
- 20 PediatricDocument31 pages20 PediatricMahmoud AbuAwadNo ratings yet
- Canine PyometraDocument5 pagesCanine Pyometrammary09No ratings yet
- Pyloric Stenosis PDFDocument3 pagesPyloric Stenosis PDFKiiza AloysiusNo ratings yet
- NCM 109 High Risk PregnancyDocument11 pagesNCM 109 High Risk PregnancyLea BorceNo ratings yet
- Textbook DiscussionDocument6 pagesTextbook DiscussionHahak UkukNo ratings yet
- Nursing Care of The Child With A Gastrointestinal DisordersDocument46 pagesNursing Care of The Child With A Gastrointestinal Disorderstalaekrema01No ratings yet
- In Partial Fulfillment For The Requirements in R.L.E: Submitted By: Elaine Blanche R. GonzalezDocument6 pagesIn Partial Fulfillment For The Requirements in R.L.E: Submitted By: Elaine Blanche R. GonzalezBlanche GonzalezNo ratings yet
- 8. Care of Child With GI Dysfunction (1) ءءءءDocument44 pages8. Care of Child With GI Dysfunction (1) ءءءءNuhaNo ratings yet
- C. Disorders of The Lowel BowelDocument69 pagesC. Disorders of The Lowel BowelJmarie Brillantes PopiocoNo ratings yet
- Pyloric StenosisDocument4 pagesPyloric StenosisAaliyaan KhanNo ratings yet
- Hirschsprung'S Disease OR Congenital Aganglionic MegacolonDocument59 pagesHirschsprung'S Disease OR Congenital Aganglionic MegacolonHarshika KDGNo ratings yet
- G.I Disorders Part 2Document53 pagesG.I Disorders Part 2شبلي غرايبهNo ratings yet
- Patient Scenario, Chapter 45, Nursing Care of A Family When A Child Has A Gastrointestinal DisorderDocument93 pagesPatient Scenario, Chapter 45, Nursing Care of A Family When A Child Has A Gastrointestinal DisorderDay MedsNo ratings yet
- Parrish July 2013Document7 pagesParrish July 2013Tada MinionNo ratings yet
- Nursing Care of The Child With Gastrointestinal DisordersDocument50 pagesNursing Care of The Child With Gastrointestinal Disordersمهند الرحيليNo ratings yet
- Approach To The Child With Nausea and Vomiting: by DR - Ryan Al - GhanemiDocument50 pagesApproach To The Child With Nausea and Vomiting: by DR - Ryan Al - GhanemiyusufharkianNo ratings yet
- Gastro - NelsonDocument14 pagesGastro - NelsonGemma OrquioNo ratings yet
- PBL No Bowel Output in NeonatesDocument24 pagesPBL No Bowel Output in NeonatesOTOH RAYA OMARNo ratings yet
- MCN Report Polyhydramnios 1Document24 pagesMCN Report Polyhydramnios 1Vincent CuyucaNo ratings yet
- Common Diseases of The InfantDocument131 pagesCommon Diseases of The Infanthed-janquillanoNo ratings yet
- FinalsDocument6 pagesFinalsjcmrtrzNo ratings yet
- Pyloric StenosisDocument20 pagesPyloric Stenosisjohnfoday2022No ratings yet
- Alteration in MetabolismDocument26 pagesAlteration in MetabolismAileen MonaresNo ratings yet
- Omphalocelevsgastroschisis 160810122732Document23 pagesOmphalocelevsgastroschisis 160810122732LNICCOLAIO100% (1)
- Competency Appraisal 1 Reviewer-1Document53 pagesCompetency Appraisal 1 Reviewer-1Paolo Carubio100% (1)
- Acute Appendicitis: History and ExaminationDocument6 pagesAcute Appendicitis: History and ExaminationPraktek Dokter Umum drjosefdrelsyNo ratings yet
- Feeding ProblemsDocument33 pagesFeeding ProblemsuouoNo ratings yet
- Acute Abdominal Pain in ChildrenDocument53 pagesAcute Abdominal Pain in ChildrenSutapa PawarNo ratings yet
- Infantile Pyloric StenosisDocument6 pagesInfantile Pyloric StenosisAksha PraiselinNo ratings yet
- APSA Gastroschisis Brochure FNLDocument5 pagesAPSA Gastroschisis Brochure FNLFarzana AhmedNo ratings yet
- Pyloric StenosisDocument5 pagesPyloric Stenosisensoooooooooo100% (1)
- Gastrointestinal System Symptoms and Signs of Gastrointes Tinal ProblemsDocument77 pagesGastrointestinal System Symptoms and Signs of Gastrointes Tinal ProblemsSindhu BabuNo ratings yet
- Chronic Constipation in Children: BMJ (Online) December 2006Document6 pagesChronic Constipation in Children: BMJ (Online) December 2006Residen KardiologiNo ratings yet
- Congenital Development Disorder of Esophagus, Stomach, Duodenum, Abdomen Wall, Anus and RectumDocument56 pagesCongenital Development Disorder of Esophagus, Stomach, Duodenum, Abdomen Wall, Anus and RectumSarah Nabella PutriNo ratings yet
- Week 8 Pedia Pediatric GI DisturbancesDocument110 pagesWeek 8 Pedia Pediatric GI DisturbancesJaja ManezNo ratings yet
- Gastro NephroDocument93 pagesGastro Nephrohasanatiya41No ratings yet
- Imperforate AnusDocument17 pagesImperforate AnusNalzaro Emyril100% (1)
- Common GI DiseasesDocument116 pagesCommon GI DiseasesmeleseNo ratings yet
- Pedia GiDocument10 pagesPedia GiCam IbardolasaNo ratings yet
- Case Presentation 4 AGEDocument33 pagesCase Presentation 4 AGERoselyn VelascoNo ratings yet
- Constipation - Emergency Management in - Children 2018Document10 pagesConstipation - Emergency Management in - Children 2018Alma Rebeca Mota NovaNo ratings yet
- Abdominal Wall Defects: Omphalocele and Gastroschisis: DR - Enono Yhoshu Department of Pediatric SurgeryDocument42 pagesAbdominal Wall Defects: Omphalocele and Gastroschisis: DR - Enono Yhoshu Department of Pediatric SurgeryYogi drNo ratings yet
- Abdominal Pain and Vomiting in ChildrenDocument18 pagesAbdominal Pain and Vomiting in ChildrenSimon Ganesya RahardjoNo ratings yet
- Prelim 01Document6 pagesPrelim 01labilabi labNo ratings yet
- University of Mosul / College of Nursing Child and Adolescent Health NursingDocument11 pagesUniversity of Mosul / College of Nursing Child and Adolescent Health NursingRayan AhmedNo ratings yet
- Dysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandDysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Marfan Syndrome Marfan Syndrome Is A Degenerative Generalized Disorder of The Connective Tissue With An InciDocument2 pagesMarfan Syndrome Marfan Syndrome Is A Degenerative Generalized Disorder of The Connective Tissue With An IncifdgrgNo ratings yet
- Substance Abuse Handout MCHDocument5 pagesSubstance Abuse Handout MCHfdgrgNo ratings yet
- Local Media4906741505093406640Document7 pagesLocal Media4906741505093406640fdgrgNo ratings yet
- Coral Reefs in The PhilippinesDocument2 pagesCoral Reefs in The PhilippinesfdgrgNo ratings yet
- MARFANDocument17 pagesMARFANfdgrgNo ratings yet
- What Is An STIDocument7 pagesWhat Is An STIfdgrgNo ratings yet
- CHE2Document1 pageCHE2fdgrgNo ratings yet
- rs2 AssDocument1 pagers2 AssfdgrgNo ratings yet
- Cleft Lip and PalateDocument1 pageCleft Lip and PalatefdgrgNo ratings yet
- Neuraltube DefectsDocument3 pagesNeuraltube DefectsfdgrgNo ratings yet
- Ai-Ai ResumeDocument3 pagesAi-Ai ResumeNeon True BeldiaNo ratings yet
- Relatorio Mano JulioDocument7 pagesRelatorio Mano JulioProGeo Projetos AmbientaisNo ratings yet
- N. Mixture, CombinationDocument2 pagesN. Mixture, CombinationYareniNo ratings yet
- Alarm Security Pic - Google ShoppingDocument1 pageAlarm Security Pic - Google Shoppingleeleeleebc123No ratings yet
- Peptides and Proteins: M.Prasad Naidu MSC Medical Biochemistry, PH.DDocument30 pagesPeptides and Proteins: M.Prasad Naidu MSC Medical Biochemistry, PH.DDr. M. Prasad NaiduNo ratings yet
- Getting The Most From Lube Oil AnalysisDocument16 pagesGetting The Most From Lube Oil AnalysisGuru Raja Ragavendran Nagarajan100% (2)
- Padiernos vs. PeopleDocument22 pagesPadiernos vs. PeopleMariel ManingasNo ratings yet
- Synchronous Alternators: Three-Phase BrushlessDocument5 pagesSynchronous Alternators: Three-Phase BrushlessĐại DươngNo ratings yet
- DMX DC Motor ControllerDocument23 pagesDMX DC Motor ControlleromargarayNo ratings yet
- Themelis Ulloa LandfillDocument15 pagesThemelis Ulloa LandfillHenry Bagus WicaksonoNo ratings yet
- Name:: Nyoman Gede Abhyasa Class: X Mipa 2 Absent: 25 AnswersDocument2 pagesName:: Nyoman Gede Abhyasa Class: X Mipa 2 Absent: 25 AnswersRetrify - Random ContentNo ratings yet
- Taylor Swift LyricsDocument2 pagesTaylor Swift LyricsElsie DomeNo ratings yet
- Service Manual - NEC Versa 2700 Series LaptopDocument130 pagesService Manual - NEC Versa 2700 Series LaptopToan NguyenNo ratings yet
- MAD Practical 6Document15 pagesMAD Practical 6DIVYESH PATELNo ratings yet
- Ethical Considerations Dissertation ExampleDocument7 pagesEthical Considerations Dissertation ExampleBuyPapersOnlineCanada100% (1)
- Inactive Volcanoes in The Philippine SDocument6 pagesInactive Volcanoes in The Philippine SChristian ParadoNo ratings yet
- Bstem-5 4Document61 pagesBstem-5 4G-SamNo ratings yet
- Autumn Activity BookDocument33 pagesAutumn Activity Bookbuzuleacnadya100% (3)
- 2.20 Optimizing Control: F. G. Shinskey C. G. Laspe B. G. Lipták M. RuelDocument10 pages2.20 Optimizing Control: F. G. Shinskey C. G. Laspe B. G. Lipták M. RueljigjigawNo ratings yet
- Ballistic - August September 2021Document168 pagesBallistic - August September 2021andrewrowe100% (2)
- Bydf3 ElectricDocument61 pagesBydf3 ElectricIvan Avila100% (1)
- 044.QTRE409 - International Human Resource ManagementDocument11 pages044.QTRE409 - International Human Resource ManagementDo Minh Gia AnNo ratings yet
- Biogas ProductionDocument7 pagesBiogas ProductionFagbohungbe MichaelNo ratings yet
- Maunakea Brochure C SEED and L Acoustics CreationsDocument6 pagesMaunakea Brochure C SEED and L Acoustics Creationsmlaouhi MajedNo ratings yet
- Guru ShishyaDocument3 pagesGuru ShishyacktacsNo ratings yet
- Rock Mass Characterization by High-Resolution SoniDocument17 pagesRock Mass Characterization by High-Resolution SoniJose AleNo ratings yet