Professional Documents
Culture Documents
Urinary System
Urinary System
Uploaded by
Tana Oquendo0 ratings0% found this document useful (0 votes)
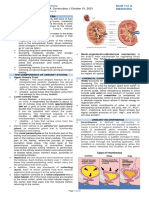
9 views8 pagesThe urinary system is composed of the kidneys, ureters, urinary bladder, and urethra. The kidneys filter the blood to remove wastes and excess water to produce urine. The urine contains substances like urea, creatinine, and ions that are filtered out of the blood. It then travels through the ureters to the bladder where it is stored until elimination through the urethra.
The kidneys are bean-shaped organs located along the posterior abdominal wall, with one on each side. Each kidney contains nephrons, which are the functional filtering units of the kidney that remove wastes from the blood to form urine. The urine is then transported through a series
Original Description:
Original Title
URINARY-SYSTEM
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe urinary system is composed of the kidneys, ureters, urinary bladder, and urethra. The kidneys filter the blood to remove wastes and excess water to produce urine. The urine contains substances like urea, creatinine, and ions that are filtered out of the blood. It then travels through the ureters to the bladder where it is stored until elimination through the urethra.
The kidneys are bean-shaped organs located along the posterior abdominal wall, with one on each side. Each kidney contains nephrons, which are the functional filtering units of the kidney that remove wastes from the blood to form urine. The urine is then transported through a series
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
9 views8 pagesUrinary System
Urinary System
Uploaded by
Tana OquendoThe urinary system is composed of the kidneys, ureters, urinary bladder, and urethra. The kidneys filter the blood to remove wastes and excess water to produce urine. The urine contains substances like urea, creatinine, and ions that are filtered out of the blood. It then travels through the ureters to the bladder where it is stored until elimination through the urethra.
The kidneys are bean-shaped organs located along the posterior abdominal wall, with one on each side. Each kidney contains nephrons, which are the functional filtering units of the kidney that remove wastes from the blood to form urine. The urine is then transported through a series
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 8
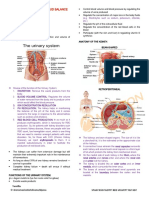
URINARY SYSTEM T- Toxin removal
The nitrogenous waste products are poorly
Composed of the two kidneys which is reabsorbed, so tubules cells have few
the right and the left kidneys, two ureters, membranes carrier to reabsorb these
urinary bladder and urethra substances because we do not need them, so
A large volume of blood flows through they tend to remain in the filtrate and they are
the kidney which remove substances found in high concentrations in the urine
from the blood to form urine. excreted from the body. Various ions are
The urine contains excess water and ions, reabsorbed and allowed to go out in the urine,
metabolic wastes like urea, creatinine and and according to what is needed at a particular
toxic substances consumed with the food. time to maintain the proper pH and the
The urine produced by the kidneys flow electrolyte composition of the blood.
through the ureters, and the urinary Common nitrogenous waste includes:
bladder where it is stored until it is
eliminated through the urethra.
Urea which is formed by the liver as an
end product of protein breakdown when
KIDNEYS (“A WET BED”) amino acids are used to produce energy.
Uric acid which is released when nucleic
A – Acid base balance
acids are metabolized
The kidney secretes variable amount of Creatinine which is associated with
hydrogen to help regulate the extracellular creatinine metabolism and the muscle
fluid ph. The ph determines the acidity or tissue.
alkalinity of the fluid. (THE blood pH is 7.35-
B - BP control
7.45;normal. Low; acid :: High; alkaline)
RAAS is an important mechanism that
W- Water removal
regulate the blood pressure.
We know that the kidneys are the major
E - Electrolyte Balance
excretory organ in our body, that removes
excess water. The kidneys help regulate the concentration of
major molecules and ions like the glucose,
Note: Water is not always excreted via the
sodium, chloride, potassium, calcium,
renal system. It can be also eliminated through
bicarbonate and phosphate.
the GIT, respiratory system, or through our
perspiration D - Vitamin D activation
E – Erythropoiesis The kidneys convert vitamin D from the
supplements that we take or from the food we
Erythropoietin is a hormone primarily
eat, to the active form of vitamin D that is
produced by the kidneys. This hormone plays
needed by our body.
a key role in the production of red blood cells,
and the process is known as erythropoiesis.
This is the process of producing red blood
KIDNEY
cells via the stimulation of the bone marrow
by the erythropoietin.
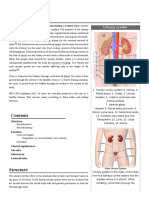
A pair of bean-shaped organ found along the Renal Fascia – A thin layer of connective
posterior wall of the abdominal cavity, with tissue encircling the kidneys.
one kidney on the either side of the vertebral
Anchors the kidney to the peritoneum
column.
and the abdominal wall.
Note: Renal; Latin word for kidney
The fat surrounding the kidneys is
The left kidney is higher than the right
important in holding them in their normal
kidney due to that larger size of the liver
body position. If the amount of fatty
on the right side of our body.
tissue dwindles like as with rapid weight
Each kidney approximately weighs 125
loss, the kidneys may drop to a lower
to 170 g in males. And 115 to 155 g in
position. The condition is called ptosis.
females.
Ptosis creates problems if the ureter
The kidney is located posterior to the
become kinked.
peritoneum and they touch the muscles of
If the ureters become kinked, the urine
the back. It’s located is called
can no longer pass through it, and the
retroperitoneal.
urine backs up and exerts pressure on the
Our kidneys are also surrounded by a
kidney tissue. This condition is called
layer of adipose tissue that holds them in
hydronephrosis, which can severely
place and protects them from physical
damage the kidney.
damage.
STRUCTURE OF THE KIDNEYS
HILUM - on the medial side of every kidney
The kidney structure has two layers:
there is a hilum, where the renal arteries and
the nerves enter, and where the renal veins - Outer (renal cortex): contains many
and the ureter exit capillaries and is made up of renal
corpuscles (part of the nephron which is
made of glomerulus and bowman’s
3 LAYERS OF THE FATTY POUCH capsule) and renal tubules.
- Inner (renal medulla): contains many
Renal Capsule (Fibrous capsule) – A fibrous
blood vessels and tubules. Triangle
layer of connective tissue covering the kidney
sections of tissues can be found in the
parenchyma.
renal medulla.
The innermost layer. This is strong and - These triangular sections of tissue that
fibrous. And it’s attached to the kidneys, constitutes the medulla is called the renal
and prevents infection. pyramids. There are 8-18 renal pyramids
in every kidney. The structure that
Perirenal Fat (or adipose capsule) – A separates the pyramids are called the renal
region of adipose against the kidney (in which columns and they also transmits blood
the adrenal glands are embedded) vessels.
A protective layer that protects the - When you look at closely, we can find
kidneys from injury. tubules or tubes. The tips of the tubes are
what we call the renal papilla or renal
papillae.
- The renal papillae are considered the apex 9. Peritubular capillaries/vasa recta are
of the renal pyramid. They are projecting specialized portion of peritubular capillaries
toward the center of the kidneys, and they that extends deep into the medulla of the
are surrounded by a funnel- shaped kidney and surround the loops of Henle and
structure which we call as the minor the collecting ducts.
calyx.
10. Blood coming from the peritubular
- These minor calyxes will join together to
capillaries including the vasa recta enters the
form the major calyx.
interlobular veins, and the veins of the kidney
- The major calyxes will join together to
run parallel to the arteries and they have
form the renal pelvis. The renal pelvis is
similar names but in reverse.
the large funnel wherein the major
calyxes from all the renal pyramids join to 11. Arcuate veins
form this structure.
12. Interlobar veins
- These renal pelvis narrows to form a
small tube called as the ureter, wherein 13. Segmental veins
the ureter exits the kidney and is
14.Renal veins which exit our kidneys.
connected to the urinary bladder.
FUNCTIONAL UNIT OF THE KIDNEYS
BLOOD FLOW THROUGH THE
KIDNEY Nephron
1. Renal Artery - Branch off from the Functional unit of the kidney
abdominal aorta and enter the kidneys. They Produce urine
give rise to several branches Nephron is made up of many tubules
2. Segmental arteries Over 1 million nephrons in every kidney.
Each nephron is composed of the renal
3. Interlobar arteries pass between the renal corpuscle which is made up of the
pyramids glomerulus and the bowman’s capsule.
4. Arcuate arteries arch between the cortex
and the medulla
5. Interlobular arteries branch off the
arcuate arteries to project into the cortex.
6. The afferent arterioles arise from the
branches of the interlobular arteries and
extend to the glomerular capillaries.
7. Glomerular capillaries
8. Efferent arterioles extend from the
glomerular capillaries and then going to the
peritubular capillaries which surrounds the
proximal and distal tubules and the loops of Proximal Convoluted tubule
Henle.
Loop of Henle composed of the Note: proteinuria; protein in urine, hematuria;
descending limb and ascending limb. blood in urine
o The descending limb: the
Proximal Convoluted tubule (PCT) – Lined
substances travel going
with cuboidal cells with brush border or
downward.
microvilli. The cells reabsorb substances from
o The ascending limb: the
the filtrate as well as secrete substances into
substances travel going the filtrate
upward.
Distal Convoluted tubule Loop of Henle – Composed of the descending
limb and ascending limb.
o The descending limb: substance
TWO TYPES OF NEPHRONS going downward, the descending limb
Cortical is made up of thin segment of simple
squamous epithelium and is highly
Account to 80 -85% of the total permeable to water.
nephron o The ascending limb: upward,
More abundant compare to juxta contains thick segment, and is
medullary impermeable to water.
Have shorter nephron loop
The loop of Henle of the cortical
nephron does not extend deep into the Distal Convoluted tubule (DCT) – lines with
medulla and they are only located in cuboidal cells, and the cells are thinner. These
the renal cortex (outer layer of the cells play a role in secreting substances into
kidney) the filtrate rather than removing substances
from it.
Juxta Medullary
There are two types of cells:
Account for the 15-20% of the
1. Intercalated cells with microvilli:
nephrons
Function is for the acid-base balance of the
Have longer nephron loops
blood.
The renal corpuscles are located in the
cortex yet very near the cortex 2. Principal cells: Do not have microvilli.
medulla junction. Function is for the sodium and water balance.
They have loops of Henle that extend
Collecting duct – not part of the nephron.
deep into the medulla of the kidney.
Passes through the renal pyramids which are
That is why it is called juxta medulla
located in the renal medulla and ends in the
renal papillae where it empties into a minor
calyx.; surrounds the tips of the tubules/renal
PARTS OF THE NEPHRON
papillae that join together to form a major
Glomerulus – Tuft of capillaries with calyx; joined together to form the renal
fenestrations or pores. These fenestrations pelvis; narrows down to form the ureter; tube
allow the filtrate to pass through except for that delivers the urine from the kidney going
the majority of the proteins and blood cells to the urinary bladder.
Review: Henle, and 19% in the DCT and
collecting duct.
From the afferent arteriole, the blood goes to
3. Tubular secretion – Movement of
the glomerulus, and the blood is filtered. The
substances from the blood into the
filtered substances which are called the
tubular fluid. In tubular secretion, all
filtrate, will proceed to the bowman’s capsule
the undesirable substances are excreted
(glomerular capsule). Both the glomerulus
in the urine.
and the glomerular capsule compose the renal
corpuscle. These bowman’s capsule surrounds
the glomerulus, and the filtrate is caught by
Micturition / Voiding / Urination - Is a
the glomerular capsule.
reflex action. The process of releasing urine
Glomerular Filtration Rate (GFR) – the from the urinary bladder through the urethra
amount of filtrate being made by the kidney. and out of the body. The process of urination
begins when the muscles of the urethral
125 mL/min (normal GFR)
sphincter relax, allowing the urine to pass
180 L/day (1 day) through the urethra. At the same time that the
Out of 180 Liters, the kidney only sphincter is relax, the smooth muscle in the
produces 1-2 liters of urine per day or walls of the urinary bladder contract to expel
only 1% of the 180. the urine from the bladder. The stretch
receptors activate the detrusor muscle, and
relax the internal urethral sphincter and the
URINE FORMATION: 3 MAJOR URINE external urethral sphincter is under voluntary
PROCESS control after approximately 2 years old and
this has to do with the growth of the spinal
1. Glomerular formation - There is a
cord and the appropriate nerves.
movement of substances from the blood
within the glomerulus into the capsular Urine - 1-2 L produced a day. If the
space or the bowman’s capsule. In amount of urine in the urinary bladder is
glomerular filtration, the blood is 150 mL, that is the time we can feel the
filtered in the glomerulus. The water urge to urinate.
and the solutes which are smaller than Around 500 mL – When a person can no
proteins are forced through the capillary longer hold the urine.
walls and the pores of the glomerular
capsule into the renal tubule.
2. Tubular reabsorption – Movement of Note:
substances from the tubular fluid back
into the blood. Almost all desirable The bladder can actually hold 1 L of urine.
organic substances are reabsorbed like
The normal yellow color of the urine is
water, glucose, amino acids and the
due to urochrome which is a pigment
needed ions. They are transported out of
arising from the body’s breakdown of
the filtrate into the tubule cells and enter
hemoglobin. And as a rule, the greater
the capillary blood. 99% of the filtrate
the solute concentration, the deeper the
is reabsorbed. 65 % is reabsorb in the
yellow color. Abnormal yellow color
PCT, 15% in the descending loop of
may also be due to certain foods as well
as to various drugs like vitamin C, and ABNORMAL URINARY
also due to bile or blood.
The odor of the freshly voided urine is
slightly aromatic, but bacterial action
gives it an ammonia like odor when left
standing. Certain diseases may also alter
the characteristic odor of the urine.
pH level of the urine ranges from 4.5 to
8. But its average value is 6, which is
slightly acidic. The food that we eat may
CONSTITUENTS
influence the pH of our urine.
Specific gravity is the relative weight of a
specific volume of a liquid compared
with an equal volume of distilled water. PROTEINURIA
Specific gravity of distilled water is 1 - In pregnancy, urinary protein excretion
because 1mL weighs 1g, and because normally increases substantially.
urine contains many dissolved solutes it However, urinary protein excretion is
weighs more than water. Its customary considered abnormal when the level
specific gravity ranges from 1.001 – 1.03. exceeds 300 mg a day. In many pregnant
Urine with a specific gravity of 1.001 women, proteinuria appears to increase
contains few solutes and is very dilute. further at the time of labor and delivery.
Dilute urine is common when a person
drinks large amount of water, uses
diuretics, or suffers from chronic renal HEMOGLOBINURIA
failure.
Conditions that produce urine with a high - Hemolytic anemia is a condition
specific gravity include limited fluid characterized by the rapture of red
intake, fever, and kidney inflammation. blood cells.
If urine becomes excessively
concentrated, some of the solutes begin
to precipitate or crystalize forming RAAS (Renin Angiotensin Aldosterone
kidney stones or what we call as the renal System) - A mechanism that is extremely
calculi. important for regulating the blood pressure.
As well as the amount of blood volume.
TWO FACTORS THAT TRIGGERS THE
RAAS:
1.Hypovolemia – Decreased blood volume
2.Hypotension – Decreased blood pressure
Either way, the cells of the juxta glomerular - The ends of the ureters extend slightly
cells of the kidneys are stimulated either by into the urinary bladder and are sealed at
LBP in the afferent arteriole/changes in the the point of entry to the bladder by the
solute content to filtrate they respond by ureterovesical valve. These valves prevent
releasing the enzyme renin; This renin acts on the urine from flowing back towards the
the protein called as the angiotensinogen kidneys.
(already present in the blood) which is
produced by the liver. The amino acids are
removed leaving only angiotensin I. The URINARY BLADDER
angiotensin I is rapidly converted to a smaller
peptide called as angiotensin II by the - Sac-like hallow organ for the urine
angiotensin converting enzyme or A.C.E. The storage
A.C.E is secreted into the lungs and kidneys - Located along the body’s midline at the
by cells in the endothelium or inner layer of inferior end of the pelvis. You can find
the blood vessels. here the trigone which is a triangular
section of the bladder that is outlined by
Angiotensin II in return, acts on the three openings. (2 ureteric orifices: where
blood vessels causing the BV to constrict. ureters enter and 1 urethral orifice)
Vasoconstriction is the medical term for
the constrictions of the blood vessels.
Vasodilation which is the dilation of the URETHRA
blood vessels. This vasoconstriction leads
to an increase in the peripheral resistance - The urethra carries the urine from the
which could increase the blood pressure. urinary bladder going to the exterior of
The Angiotensin II also acts on the the body.
adrenal cortical cells to promote the - The urethral orifice or meatus is the
release of a hormone known as external opening of the urethra where the
aldosterone. Aldosterone is a hormone urine comes out.
that promotes water and sodium
retention. And as a result, the blood
volume increases as well as the blood FEMALE URETHRA
pressure.
- Shorter than the male. Around 2 in in
length
- The opening is located below the clitoris
URETERS
and above the vaginal opening
- A pair of tubes that carry the urine from - The shorter urethra is one of the reasons
the kidneys going to the urinary bladder. why women get UTI more often. The
- Ureters are 10-12 inches long and they shorter urethra makes it easier for the
run on the left and right sides of the body bacteria to get into the bladder.
parallel to the vertebral column.
- Gravity and peristalsis of the smooth
muscle tissue in the walls of the ureters MALE URETHRA
moves the urine toward the urinary
bladder. Around 8-10 in length and ends at the tip
of the penis.
Because of the length, the male urethra is 3. The hormone produced by the kidney
divided into three regions. that plays an important role in RBC
production
4. Give 2 layers of the kidney structure
1. Prostatic: passes through the prostate gland
5. The innermost layer of the fatty pouch
2. Membranous: passes through the that protects the kidney
urogenital diaphragm. Urogenital diaphragm 6. The parts of nephron
is a double layer of pelvic fascia with its 7. The major functions of nephron
included muscle that is situated between the 8. The pair of tubes that carry the urine
ischial and pubic rami, and supports the from the kidney to the urinary bladder
prostate in the male, and gives passage to the 9. The average GFR in a day: how many
membranous part of the urethra. % becomes urine
10. What type of kidney stones are
2. Penile/spongy: passes through the length of radiopaque in x-ray?
the penis.
The flow of urine in the urethra is
controlled by the internal and external
urethral sphincter muscles.
The internal urethral sphincter is made of
smooth muscle, and opens involuntarily
when the bladder reaches a certain set
level of distention. The opening of the
internal sphincter which results in the
sensation of “needing to urinate”.
The I.S is made up of skeletal muscle and
may be opened to allow the urine to pass
through the urethra or may be held close
to the delay urination.
KIDNEY STONES (nephrolithiasis; renal
calculi)
- Hard deposits made of minerals and salts
that is formed inside our kidneys.
Diet, excess body weight, medical
conditions, certain supplements and
medications are among the many causes
of kidney stones
REVIEW:
1. Give the location of the kidneys
2. The functional unit of the kidney
You might also like
- Dr:Khalid MiladDocument27 pagesDr:Khalid MiladMohsen Elzobna0% (1)
- SH Lecture 2018 - Respiratory System DevelopmentDocument23 pagesSH Lecture 2018 - Respiratory System DevelopmentAna-Maria-Cecilia DurduiNo ratings yet
- Urinary SystemDocument9 pagesUrinary SystemMa Ellen LumauagNo ratings yet
- KidneyDocument40 pagesKidneyOlaifa victorNo ratings yet
- Chapter 6Document3 pagesChapter 6John ErickNo ratings yet
- Urinary SystemDocument3 pagesUrinary SystempsychelastwishNo ratings yet
- Understanding Medical Surgical Nursing - 0849-0849Document1 pageUnderstanding Medical Surgical Nursing - 0849-0849Anas TasyaNo ratings yet
- CHAPTER 18 ANAPHY TransesDocument5 pagesCHAPTER 18 ANAPHY TransesHoly HaeinNo ratings yet
- Life Processes - Excretion - Humans & Plants - OriginalDocument36 pagesLife Processes - Excretion - Humans & Plants - Originalnouraft.07No ratings yet
- 6.1 Concepts of UrinaryDocument10 pages6.1 Concepts of UrinaryIvy VillalobosNo ratings yet
- Urinary SystemDocument4 pagesUrinary SystemMohammed Keyarul IslamNo ratings yet
- Kidney: PDF Generated At: Sun, 26 Jan 2014 03:55:26 UTCDocument15 pagesKidney: PDF Generated At: Sun, 26 Jan 2014 03:55:26 UTCVijay RajendiranNo ratings yet
- Urinary System: Nurmila Sari Anatomi FKIK UIN Syarif Hidayatullah JakartaDocument44 pagesUrinary System: Nurmila Sari Anatomi FKIK UIN Syarif Hidayatullah JakartaSeptiara IqraNo ratings yet
- The Urinary System & Fluid BalanceDocument8 pagesThe Urinary System & Fluid BalanceMarianne DugosNo ratings yet
- MIRADOR, Kiana AnaphyAct16Document4 pagesMIRADOR, Kiana AnaphyAct16Kiana MiradorNo ratings yet
- Chapter 18 Anaphy TransesDocument5 pagesChapter 18 Anaphy TransesHoly HaeinNo ratings yet
- Renal FunctionDocument5 pagesRenal Functionchayiezen0301No ratings yet
- Urinary SystemDocument14 pagesUrinary SystemCharli ParachinniNo ratings yet
- What Are The KidneysDocument5 pagesWhat Are The KidneysMary Jane TiangsonNo ratings yet
- Revision Notes: Excretory OrgansDocument4 pagesRevision Notes: Excretory Organskavitaruby1980No ratings yet
- Urinary SystemDocument2 pagesUrinary SystemCharlayne AnneNo ratings yet
- Excretory SystemDocument6 pagesExcretory SystemAiman AfzalNo ratings yet
- Urinary SystemDocument22 pagesUrinary SystemGray Odyssey M.No ratings yet
- PINK Cream and Green Illustrative Science Project PresentationDocument31 pagesPINK Cream and Green Illustrative Science Project Presentationereneovalerozo22No ratings yet
- Renal Physiology 1 1aDocument88 pagesRenal Physiology 1 1afentaw melkieNo ratings yet
- Urinary SystemDocument77 pagesUrinary SystemJushelle Anne Tigoy PilareNo ratings yet
- AnaphyDocument3 pagesAnaphyKenneth DelorinoNo ratings yet
- MLT 1027 Learning Outcome 14 Renal UrinaryDocument94 pagesMLT 1027 Learning Outcome 14 Renal UrinaryMelanie TranNo ratings yet
- Urinary SystemDocument9 pagesUrinary SystemCailah Sofia SelausoNo ratings yet
- The Human Renal SystemDocument8 pagesThe Human Renal SystemRobert CaseyNo ratings yet
- Urinary System (2015 - 06 - 09 22 - 21 - 55 Utc)Document44 pagesUrinary System (2015 - 06 - 09 22 - 21 - 55 Utc)DiazNo ratings yet
- Urinary SystemDocument10 pagesUrinary SystemElyka Alivan Valdez PolonioNo ratings yet
- THE Urinary System: Charlotte R. Espiritu RN. MANDocument25 pagesTHE Urinary System: Charlotte R. Espiritu RN. MANLenny Ronalyn QuitorianoNo ratings yet
- Unit - Ii Human Anatomy and PhysiologyDocument15 pagesUnit - Ii Human Anatomy and PhysiologyRK YeleswarapuNo ratings yet
- Urinary SystemDocument28 pagesUrinary Systemgabanule brandonNo ratings yet
- Anph FinalsDocument42 pagesAnph FinalsVincent BustamanteNo ratings yet
- Urinary System Final PrintDocument9 pagesUrinary System Final Printrussellnicoabendanabendan1234No ratings yet
- Introduction and Assessment of The Renal - Urological SystemDocument182 pagesIntroduction and Assessment of The Renal - Urological SystemValerie Suge-Michieka100% (1)
- Chronic Kidney DiseaseDocument25 pagesChronic Kidney DiseaseZachary CohenNo ratings yet
- Human Anatomy Physiology Chapter 13 Urinary System NotesDocument10 pagesHuman Anatomy Physiology Chapter 13 Urinary System NotesVGH CREATIONS Lucky's.lyrical.statusNo ratings yet
- The Excretory SystemDocument31 pagesThe Excretory Systemapi-3759646100% (12)
- Urinary System, Genital System of Veterinary AnatomyDocument30 pagesUrinary System, Genital System of Veterinary AnatomyRadia RaicyNo ratings yet
- 1 - The Urinary System and Fluid Balance - de Veyra - Silvano&tajalaDocument12 pages1 - The Urinary System and Fluid Balance - de Veyra - Silvano&tajalaMika SaldañaNo ratings yet
- Kidney Anatomy and PhysiologyDocument5 pagesKidney Anatomy and PhysiologyDianne MacaraigNo ratings yet
- Structures and Functions: Chapter 45: Nursing Assessment: Urinary SystemDocument18 pagesStructures and Functions: Chapter 45: Nursing Assessment: Urinary SystemKennette LimNo ratings yet
- Zoo 1 Excretion and OsmoregulationDocument17 pagesZoo 1 Excretion and OsmoregulationMaheshkumar KalalNo ratings yet
- The Human Renal SystemDocument6 pagesThe Human Renal Systemhoneydine_03No ratings yet
- Anatomy of Urinary SystemDocument43 pagesAnatomy of Urinary Systemandrea titus100% (1)
- Topik 2 2021Document26 pagesTopik 2 2021AnnisNo ratings yet
- DR Laxman Khanal Bpkihs 07-06-2013Document86 pagesDR Laxman Khanal Bpkihs 07-06-2013Bilal YimamNo ratings yet
- Urinary System Anatomy and PhysiologyDocument13 pagesUrinary System Anatomy and PhysiologyKBDNo ratings yet
- Anatomy - Kidney'sDocument18 pagesAnatomy - Kidney'sOlivia MorrisonNo ratings yet
- Anatomy and Physiology of The KidneysDocument21 pagesAnatomy and Physiology of The Kidneysccbrown750% (2)
- Anatomy and Physiology - Kidney - ForDocument3 pagesAnatomy and Physiology - Kidney - ForKristelle ModalesNo ratings yet
- Anatomy and Physiology of Urinary SystemDocument5 pagesAnatomy and Physiology of Urinary SystemIan CruzNo ratings yet
- Excretion KDBDocument82 pagesExcretion KDBKiranNo ratings yet
- The Urinary SystemDocument3 pagesThe Urinary SystemDaniel NevadoNo ratings yet
- HemodialysisDocument23 pagesHemodialysisKrishnaBihariShuklaNo ratings yet
- Renal SystemDocument18 pagesRenal SystemS GNo ratings yet
- Kidney Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandKidney Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Renal Reflections: Exploring the Marvels of Nephrology: The Intricate Ballet of Kidney Functions UnveiledFrom EverandRenal Reflections: Exploring the Marvels of Nephrology: The Intricate Ballet of Kidney Functions UnveiledNo ratings yet
- Blood SystemDocument13 pagesBlood SystemTana OquendoNo ratings yet
- Digestive SystemDocument9 pagesDigestive SystemTana OquendoNo ratings yet
- He Notes 8Document20 pagesHe Notes 8Tana OquendoNo ratings yet
- Health Edu-Note 7-MidtermDocument23 pagesHealth Edu-Note 7-MidtermTana OquendoNo ratings yet
- He Notes 9 PDFDocument21 pagesHe Notes 9 PDFTana OquendoNo ratings yet
- Invertebrate Digestive System2019 ModuleDocument11 pagesInvertebrate Digestive System2019 ModuleJeff Bryan Arellano HimorNo ratings yet
- Embryology Revision NotesDocument10 pagesEmbryology Revision NotesvamshidhNo ratings yet
- Uh Ipa explanation-WPS OfficeDocument15 pagesUh Ipa explanation-WPS Officewinda wahyuniNo ratings yet
- Wisdom Teeth RemovalDocument12 pagesWisdom Teeth RemovalDalia Annamelia Fernández PaumierNo ratings yet
- Minimal Invasive Techniques in Porcelain Laminate Veneers: Case SeriesDocument4 pagesMinimal Invasive Techniques in Porcelain Laminate Veneers: Case Seriesfanny rizky andriyaniNo ratings yet
- Cardiovascular RegulationDocument40 pagesCardiovascular RegulationeliseudesafateNo ratings yet
- Unit D - Human Systems Unit PlanDocument4 pagesUnit D - Human Systems Unit Planapi-427321002No ratings yet
- ImmunologyDocument14 pagesImmunologyayeiNo ratings yet
- Anatomy JPDocument15 pagesAnatomy JPSeptimiu TiplicaNo ratings yet
- The Articulatory SystemDocument4 pagesThe Articulatory SystemDianne MaeNo ratings yet
- 2020 Dental-CertificateDocument1 page2020 Dental-CertificateMeach CallejoNo ratings yet
- Blood Physiology 2022Document116 pagesBlood Physiology 2022Gurmessa FekaduNo ratings yet
- EndocrinologyDocument46 pagesEndocrinology[161]Shuaib AktherNo ratings yet
- Histology of The Respiratory System 20152016Document44 pagesHistology of The Respiratory System 20152016mugilanNo ratings yet
- Https://d1c0fc7ib89kee - Cloudfront.net/uploads/attachment/file//7b Knowledge Organiser PFRDocument2 pagesHttps://d1c0fc7ib89kee - Cloudfront.net/uploads/attachment/file//7b Knowledge Organiser PFRAmaya AliNo ratings yet
- Eccrine Glands Are DistributedDocument1 pageEccrine Glands Are DistributedGwenneth BrilloNo ratings yet
- TongueDocument10 pagesTongueBhuwanesh SharmaNo ratings yet
- MCQ - 4th Assessment - Gynae-17-03-16Document4 pagesMCQ - 4th Assessment - Gynae-17-03-16leonNo ratings yet
- KABERIDocument8 pagesKABERIRahulNo ratings yet
- MCQs For LaboratoryDocument42 pagesMCQs For LaboratorySami Khan87% (68)
- Revision Notes Class 11 - Biology Chapter 19 - Excretory Product and Their EliminationDocument9 pagesRevision Notes Class 11 - Biology Chapter 19 - Excretory Product and Their EliminationHarpreetNo ratings yet
- Bams Question PaperDocument7 pagesBams Question Paperwaku74100% (3)
- Chapter 61 LiverDocument1 pageChapter 61 LiverDayane MirandaNo ratings yet
- % Chapter 1: Regulation of Water ContentDocument39 pages% Chapter 1: Regulation of Water ContentK CNo ratings yet
- Neuropati AlkoholDocument4 pagesNeuropati AlkoholNatalia IhalauwNo ratings yet
- Sino Biological Inc. 2013 Product CatalogDocument181 pagesSino Biological Inc. 2013 Product CatalogMegan MckinneyNo ratings yet
- Summerbridge Hong Kong 2019 Lesson Plan Template Teacher: Lizzie Yetman Course: Date: 13 July Aim/Objective: Students Will Be Able To - .Document2 pagesSummerbridge Hong Kong 2019 Lesson Plan Template Teacher: Lizzie Yetman Course: Date: 13 July Aim/Objective: Students Will Be Able To - .Isaac MNo ratings yet
- FCPS Pretest Series Golden File 3Document224 pagesFCPS Pretest Series Golden File 3Marsiano QendroNo ratings yet