Professional Documents
Culture Documents
Syndrome of Contractures
Syndrome of Contractures
Uploaded by
raquelbibiCopyright:
Available Formats
You might also like
- Treatment of Massive Obesity With Ricereduction Diet Program. An Analysis of 106 Patients With at Least A 45-kg Weight LossDocument10 pagesTreatment of Massive Obesity With Ricereduction Diet Program. An Analysis of 106 Patients With at Least A 45-kg Weight LossJéssica Moreira100% (2)
- Animal-Assisted TherapyDocument196 pagesAnimal-Assisted Therapyraquelbibi100% (3)
- Asian Studies Major For College Ancient History of East AsiaDocument64 pagesAsian Studies Major For College Ancient History of East AsiaApaaNo ratings yet
- Raoul Tubiana - Jean-Michel Thomine - Evelyn Mackin - F Brunelli - Examination of The Hand and Wrist-CRC PressDocument406 pagesRaoul Tubiana - Jean-Michel Thomine - Evelyn Mackin - F Brunelli - Examination of The Hand and Wrist-CRC PressMaricruzhdezaNo ratings yet
- Vestax VCI-380 Midi Mapping v3.4Document23 pagesVestax VCI-380 Midi Mapping v3.4Matthieu TabNo ratings yet
- A.D. Pearle - Surgical Technique and Anatomic Study of Latissimus Dorsi and Teres Major Transfers (2006)Document9 pagesA.D. Pearle - Surgical Technique and Anatomic Study of Latissimus Dorsi and Teres Major Transfers (2006)João Pedro ZenattoNo ratings yet
- Post-Traumatic Elbow Stiffness - Arthrolysis and Mechanical DistractionDocument31 pagesPost-Traumatic Elbow Stiffness - Arthrolysis and Mechanical DistractionAna-Maria ȘtefanNo ratings yet
- The Origin and Evolutionary Biology of Pinnipeds Seals, Sea Lions, and WalrusesDocument26 pagesThe Origin and Evolutionary Biology of Pinnipeds Seals, Sea Lions, and WalrusesMaya D.No ratings yet
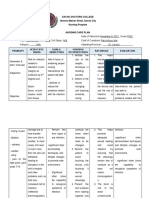
- Davao Doctors College General Malvar Street, Davao City Nursing ProgramDocument5 pagesDavao Doctors College General Malvar Street, Davao City Nursing ProgramJhoneric Vencer EscultorNo ratings yet
- The Multisensory HandbookDocument177 pagesThe Multisensory Handbookraquelbibi100% (3)
- MycologyDocument129 pagesMycologyPriyanka Rajput100% (4)
- Amlodipine Drug StudyDocument1 pageAmlodipine Drug StudyElleNo ratings yet
- Neuromuscular Diseases and RehabilitationDocument41 pagesNeuromuscular Diseases and RehabilitationraquelbibiNo ratings yet
- Levucell SB Research BibliographyDocument23 pagesLevucell SB Research BibliographyrubenriveraNo ratings yet
- Kinesiology of The Musculoskeletal System 3rd Edition (Donald A. Neumann) Capitulo Ombro ComplexoDocument57 pagesKinesiology of The Musculoskeletal System 3rd Edition (Donald A. Neumann) Capitulo Ombro ComplexoMurilo PinzNo ratings yet
- Assessment of OrthopedicVersus Neurologic Causes of Gait Change in Dogs and CatsDocument9 pagesAssessment of OrthopedicVersus Neurologic Causes of Gait Change in Dogs and CatsAristoteles Esteban Cine VelazquezNo ratings yet
- Thoracic IncisionsDocument10 pagesThoracic IncisionsRadioputro WicaksonoNo ratings yet
- Hemorrhoidal Laser Procedure - Short - and Long-Term Results From A Prospective StudyDocument5 pagesHemorrhoidal Laser Procedure - Short - and Long-Term Results From A Prospective StudyagusNo ratings yet
- Strategy of The Netherlands in The Field of Rare DiseasesDocument20 pagesStrategy of The Netherlands in The Field of Rare DiseasesGehd JdifkNo ratings yet
- Biomechanics of Cervical SpineDocument58 pagesBiomechanics of Cervical SpinesanavoraNo ratings yet
- Skeletal SystemDocument64 pagesSkeletal SystemGem Rose UretaNo ratings yet
- Pain Education For Physiotherapists Is It Time For C - 2011 - Journal of PhysioDocument2 pagesPain Education For Physiotherapists Is It Time For C - 2011 - Journal of PhysioCông Tác Xã Hội Phòng100% (1)
- Far Lateral Vs Extreme Lateral AproachDocument14 pagesFar Lateral Vs Extreme Lateral AproachcristianescNo ratings yet
- Vertebral ColumnDocument84 pagesVertebral ColumnGenesis GeronagaNo ratings yet
- Damage Control Orthopaedics in Spinal Trauma JAAOSDocument12 pagesDamage Control Orthopaedics in Spinal Trauma JAAOSAzmi FarhadiNo ratings yet
- Human Postural ControlDocument9 pagesHuman Postural Controlelbueno21No ratings yet
- AOTrauma Elastic Stable IntramedullaryDocument249 pagesAOTrauma Elastic Stable IntramedullaryVivek ChNo ratings yet
- 2011fetal Brain Function Jaypee Journal-AnnotatedDocument7 pages2011fetal Brain Function Jaypee Journal-AnnotatedDamara Gardel100% (1)
- Early Total Care To Early Appropriate Care What.2Document8 pagesEarly Total Care To Early Appropriate Care What.2ChrisNo ratings yet
- Effect of Heat Treatment On Edible Yam (Dioscorea Activity: Kinetic and Thermodynamic AnalysisDocument10 pagesEffect of Heat Treatment On Edible Yam (Dioscorea Activity: Kinetic and Thermodynamic Analysisاجي تقرى100% (1)
- High Median Nerve InjuriesDocument10 pagesHigh Median Nerve InjuriesKarime TapiaNo ratings yet
- .1 Arthritides-P1Document14 pages.1 Arthritides-P1ELIZABETH GRACE AMADORNo ratings yet
- Introduction To FranchisingDocument23 pagesIntroduction To FranchisingJuzer RampurawalaNo ratings yet
- Portal Vein Thrombosis 2021Document175 pagesPortal Vein Thrombosis 2021haitham aloolNo ratings yet
- Protocol For The Examination of Specimens From Patients With Plasma Cell NeoplasmsDocument12 pagesProtocol For The Examination of Specimens From Patients With Plasma Cell NeoplasmsMaikka IlaganNo ratings yet
- Diabetic Neuropathy: DR Shahjada SelimDocument129 pagesDiabetic Neuropathy: DR Shahjada SelimmadboyNo ratings yet
- PFO UpdateDocument33 pagesPFO UpdateMitesh PatelNo ratings yet
- AAOS Clinical Practice Guideline Summary .10Document9 pagesAAOS Clinical Practice Guideline Summary .10mukhlis akmalNo ratings yet
- Bacteriological Spectrum and Antibiogram of Isolates Obtained From Smoked Fish Sold in Federal Capital Territory, Abuja, NigeriaDocument10 pagesBacteriological Spectrum and Antibiogram of Isolates Obtained From Smoked Fish Sold in Federal Capital Territory, Abuja, NigeriaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Umbilicalherniarepair: Overview of Approaches and Review of LiteratureDocument16 pagesUmbilicalherniarepair: Overview of Approaches and Review of LiteratureVictor Matias BarriosNo ratings yet
- Dermatology NLC DR Manish Soni 2021Document94 pagesDermatology NLC DR Manish Soni 2021akashineeNo ratings yet
- Iqvia Institute Biosimilars in The United States 2023 Usl Orb3393Document41 pagesIqvia Institute Biosimilars in The United States 2023 Usl Orb3393Igor IlievskiNo ratings yet
- Devil-Fictions by Lance Phillips Book Preview-AfDocument20 pagesDevil-Fictions by Lance Phillips Book Preview-AfBlazeVOX [books]No ratings yet
- Posture Dr. Dr. MY, SP KFR-KDocument67 pagesPosture Dr. Dr. MY, SP KFR-KCikupaNo ratings yet
- 15 Gene Expression Translation SDocument6 pages15 Gene Expression Translation SHelp Me Study TutoringNo ratings yet
- Modul Hip Disarticulation ProstheticsDocument67 pagesModul Hip Disarticulation ProstheticsCapt KidsNo ratings yet
- Attock Refinery Limited: Low Gravity Residual Fuel OilDocument7 pagesAttock Refinery Limited: Low Gravity Residual Fuel OilshahNo ratings yet
- Surpass 1Document13 pagesSurpass 1Fernando DominguezNo ratings yet
- Acl Injury & Acl Protocol Melbourne GuidelineDocument36 pagesAcl Injury & Acl Protocol Melbourne GuidelineCrunchy Cacao100% (1)
- Interdigital (Morton's) Neuroma - Foot & Ankle - OrthobulletsDocument3 pagesInterdigital (Morton's) Neuroma - Foot & Ankle - OrthobulletsEmiel AwadNo ratings yet
- Thy ReviewerDocument229 pagesThy ReviewerKimberly Anne OjedaNo ratings yet
- Pedicle Screw Fixation in Fracture of Thoraco-Lumbar SpineDocument21 pagesPedicle Screw Fixation in Fracture of Thoraco-Lumbar SpineNiyati SharmaNo ratings yet
- Nexus ICSIDocument114 pagesNexus ICSIDr.Pratixa JoshiNo ratings yet
- Endocrine Manifestations of Systemic Autoimmune Diseases, Volume 9 (Handbook of Systemic Autoimmune Diseases) (PDFDrive)Document352 pagesEndocrine Manifestations of Systemic Autoimmune Diseases, Volume 9 (Handbook of Systemic Autoimmune Diseases) (PDFDrive)Laura Diana BarthaNo ratings yet
- Protocol: Percutaneous Tibial Nerve StimulationDocument8 pagesProtocol: Percutaneous Tibial Nerve StimulationAléssio NovaisNo ratings yet
- Levin1981Document11 pagesLevin1981luis sanchezNo ratings yet
- 05 Fetal Development 1Document4 pages05 Fetal Development 1Gwen CastroNo ratings yet
- Philippine PanDocument82 pagesPhilippine PanJ. G. CheockNo ratings yet
- GOLD For COPD Pocket GuideDocument30 pagesGOLD For COPD Pocket Guideraul sinatoNo ratings yet
- Deep Tendon Reflex Steps On How To Assess The DTR: Normal Response: DTR GradingDocument2 pagesDeep Tendon Reflex Steps On How To Assess The DTR: Normal Response: DTR GradingElla EvangelistaNo ratings yet
- 7the Axis VertebraDocument151 pages7the Axis VertebraAminou MounirouNo ratings yet
- Centrally Mediated Abdominal Pain SyndromesDocument4 pagesCentrally Mediated Abdominal Pain SyndromesPolo Good BoyNo ratings yet
- Lingaya University ProspectusDocument27 pagesLingaya University ProspectusChalla RamanamurtyNo ratings yet
- Foot and Ankle Injuries and Pain: Indranil Neel' Kushare, MDDocument55 pagesFoot and Ankle Injuries and Pain: Indranil Neel' Kushare, MDrizwan.mughal1997No ratings yet
- Evaluation of A Paediatric Early Warning System Pews Score On Admission To A Paediatric Intensive Care Unit To Predict Mortality Risk in A Low Resource Setting Guinea BissauDocument6 pagesEvaluation of A Paediatric Early Warning System Pews Score On Admission To A Paediatric Intensive Care Unit To Predict Mortality Risk in A Low Resource Setting Guinea BissauHerald Scholarly Open AccessNo ratings yet
- Syndrome of Contractures and Deformities SofCD Dysplasia of Hips Varus Deformity of Shanks Wry Neck So Called Idiopathic Scoliosis Causes Clinic Prophylaxis TherapyDocument15 pagesSyndrome of Contractures and Deformities SofCD Dysplasia of Hips Varus Deformity of Shanks Wry Neck So Called Idiopathic Scoliosis Causes Clinic Prophylaxis TherapyAthenaeum Scientific PublishersNo ratings yet
- Neuromuscular Diseases and RehabilitationDocument41 pagesNeuromuscular Diseases and RehabilitationraquelbibiNo ratings yet
- Patterns of Postural Assymetry in InfantsDocument7 pagesPatterns of Postural Assymetry in InfantsraquelbibiNo ratings yet
- Global Postural Reeducation For Patients With Musculoskeletal Conditions. A Systematic Review of Randomized Controlled TrialsDocument12 pagesGlobal Postural Reeducation For Patients With Musculoskeletal Conditions. A Systematic Review of Randomized Controlled TrialsraquelbibiNo ratings yet
- Comprehensive Psychoneuroendocrinology: Jennifer W. Applebaum, Evan L. Maclean, Shelby E. McdonaldDocument12 pagesComprehensive Psychoneuroendocrinology: Jennifer W. Applebaum, Evan L. Maclean, Shelby E. McdonaldraquelbibiNo ratings yet
- Treatments For Infantile Postural AsymmetryDocument7 pagesTreatments For Infantile Postural AsymmetryraquelbibiNo ratings yet
- Barroqueiro2014 - The Effects of A Global Postural Reeducation Program On An Adolescent Handball Player With Isthmic SpondylolisthesisDocument15 pagesBarroqueiro2014 - The Effects of A Global Postural Reeducation Program On An Adolescent Handball Player With Isthmic SpondylolisthesisraquelbibiNo ratings yet
- Effectiveness of Global Postural Re-Education For Treatment of Spinal Disorders A Meta-AnalysisDocument10 pagesEffectiveness of Global Postural Re-Education For Treatment of Spinal Disorders A Meta-AnalysisraquelbibiNo ratings yet
- Cerebral Palsy An Information Guide For ParentsDocument36 pagesCerebral Palsy An Information Guide For Parentsraquelbibi100% (1)
- What Is MDocument2 pagesWhat Is MkasjdkasNo ratings yet
- Dyspepsia LectureDocument2 pagesDyspepsia LectureDaneva Reyes0% (1)
- Practice of Medicine - by Balaram JanaDocument93 pagesPractice of Medicine - by Balaram JanaFarhana V PNo ratings yet
- Red Biotechnology ProjectDocument5 pagesRed Biotechnology ProjectMahendrakumar ManiNo ratings yet
- 125 - 187 - Benny Tjan - GalleyDocument5 pages125 - 187 - Benny Tjan - GalleyZihan ZetiraNo ratings yet
- Thoracic and Neck TraumaDocument13 pagesThoracic and Neck Traumahatem alsrourNo ratings yet
- Diseases Associated With The Various Organ SystemsDocument10 pagesDiseases Associated With The Various Organ SystemsKimh SampagNo ratings yet
- Meninges - Steven McGee - Evidence-Based Physical Diagnosis-Elsevier (2017)Document8 pagesMeninges - Steven McGee - Evidence-Based Physical Diagnosis-Elsevier (2017)Victor MejiaNo ratings yet
- Office Of: The SecretaryDocument44 pagesOffice Of: The Secretarypaomillan0423No ratings yet
- Pathology: Tutorial 5Document18 pagesPathology: Tutorial 5Salma AshrafNo ratings yet
- Hepatic EncephalopathyDocument5 pagesHepatic Encephalopathyliveconnectionz282No ratings yet
- PE M2 Dance Injuries and First AidDocument22 pagesPE M2 Dance Injuries and First AidKeith Emerich FermaNo ratings yet
- Basic First Aid 0808Document72 pagesBasic First Aid 0808BS AnilKumarNo ratings yet
- Pengetahuan Dan Sikap Masyarakat Terhadap Penyakit Malaria Di Desa Kolongan Kecamatan Talawaan Kabupaten Minahasa UtaraDocument6 pagesPengetahuan Dan Sikap Masyarakat Terhadap Penyakit Malaria Di Desa Kolongan Kecamatan Talawaan Kabupaten Minahasa Utarasri humaerahNo ratings yet
- Abinash em Gi SurDocument72 pagesAbinash em Gi Sursapkota18No ratings yet
- When To Use Deprogramming Splint and WhyDocument2 pagesWhen To Use Deprogramming Splint and WhyJustin KimberlakeNo ratings yet
- 04 SPS SAINS TG2-Nota Grafik B4Document6 pages04 SPS SAINS TG2-Nota Grafik B4AZAMOLLYNo ratings yet
- Pediatric Cholestasis: Epidemiology, Genetics, Diagnosis, and Current ManagementDocument5 pagesPediatric Cholestasis: Epidemiology, Genetics, Diagnosis, and Current ManagementAnnisa SusiloNo ratings yet
- Sulfamethoxazole Trimethoprim PDFDocument10 pagesSulfamethoxazole Trimethoprim PDFAsi SyyffaNo ratings yet
- Dissociative Amnesia Case ReportDocument3 pagesDissociative Amnesia Case ReportJon MaciejewskiNo ratings yet
- Miasm ConsolidatedDocument72 pagesMiasm ConsolidatedSatyendra RawatNo ratings yet
- S19 FullDocument11 pagesS19 FullDiana AmpulembangNo ratings yet
- FilariasisDocument8 pagesFilariasisTheeya QuigaoNo ratings yet
- 1 s2.0 S0165032721002366 MainDocument7 pages1 s2.0 S0165032721002366 Mainana cristina brazNo ratings yet
- Control of Diarrheal Diseases (CCD) Definition of DiarrhoeaDocument27 pagesControl of Diarrheal Diseases (CCD) Definition of Diarrhoeaإحسان ماجد محمدNo ratings yet
- Ozone Therapy and Uv Blood Irradiation: What It Helps TreatDocument8 pagesOzone Therapy and Uv Blood Irradiation: What It Helps TreatsumanNo ratings yet
Syndrome of Contractures
Syndrome of Contractures
Uploaded by
raquelbibiOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Syndrome of Contractures
Syndrome of Contractures
Uploaded by
raquelbibiCopyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/330587250
“Syndrome of Contractures” According to Prof. Hans Mau; Problems of
Shanks, Knees, Hips, Pelvis and Spine; Children, Adolescents, Adults,
Diagnosis, Treatment
Article in Surgical Science · January 2019
DOI: 10.4236/ss.2019.101004
CITATIONS READS
2 6,044
3 authors, including:
Jacek Karski
Medical University of Lublin
25 PUBLICATIONS 130 CITATIONS
SEE PROFILE
Some of the authors of this publication are also working on these related projects:
AARD A case report View project
DDH developmental dysplasia of the hip - View project
All content following this page was uploaded by Jacek Karski on 31 July 2020.
The user has requested enhancement of the downloaded file.
Surgical Science, 2019, 10, 24-38
http://www.scirp.org/journal/ss
ISSN Online: 2157-9415
ISSN Print: 2157-9407
“Syndrome of Contractures” According to Prof.
Hans Mau; Problems of Shanks, Knees, Hips,
Pelvis and Spine; Children, Adolescents,
Adults, Diagnosis, Treatment
Karski Tomasz1, Karski Jacek2, Domagała Marian3
1
Vincent Pol University, Lublin, Poland
2
Medical University, Lublin, Poland
3
Medical Centre, Laszczów, Poland
How to cite this paper: Tomasz, K., Jacek, Abstract
K. and Marian, D. (2019) “Syndrome of
Contractures” According to Prof. Hans The problems of movement apparatus in children, youth and even adoles-
Mau; Problems of Shanks, Knees, Hips, cents aren’t connected with “a weakness of muscles” but with a shortening of
Pelvis and Spine; Children, Adolescents, muscles, tendons, and capsules which in orthopaedic literature is called “con-
Adults, Diagnosis, Treatment. Surgical
tracture” [1] [2] [3] [4]. The older way of thinking about the problem was
Science, 10, 24-38.
https://doi.org/10.4236/ss.2019.101004 based on the conviction that “weak muscles” cause and make problems; we,
however, present on many examples that “restriction of movements” doing
Received: December 17, 2018 by shortening of soft tissues makes contracture and incorrect position of
Accepted: January 21, 2019 joints, body parts, the serious and frequent clinical problems.
Published: January 24, 2019
Copyright © 2019 by author(s) and Keywords
Scientific Research Publishing Inc. Contracture, Incorrect Position of Body, Influence on Shanks, Hips, Pelvis,
This work is licensed under the Creative
Neck, Spine, Physiotherapy
Commons Attribution International
License (CC BY 4.0).
http://creativecommons.org/licenses/by/4.0/
Open Access
1. Causes of the “Syndrome of Contractures” (SofC)
The “syndrome of contractures” (Figures 1-3) has been described with all details by
Prof. Hans Mau—as Siebener [Kontrakturen] Syndrom” (syndrome of seven con-
tractures). In 2006 in Lublin we added to “the Syndrome of Contracture” the eighth
deformity—bigger than normal “varus of shanks” (Figures 13-15). Now, we de-
scribe this syndrome as the “Syndrome of Contractures and Deformities” (SofCD).
In literature we find that this syndrome has been described also by: Hensinger,
Howorth, Green & Griffin, Dega, Vizkelety, Karski J., T. Karski & M. Frelek-Karska
and colleagues [1] [3]-[13]. The causes of the “Syndrome of Contractures and
DOI: 10.4236/ss.2019.101004 Jan. 24, 2019 24 Surgical Science
Karski Tomasz et al.
Figure 1. Three month old child; “Syndrome of Contractures and Deformities”. 1. Pla-
giocephalia. 2. Right sided wry neck. 3. Limited abduction of the left hip as a symptom of
dysplasia in form of DDH. 4. Infantile scoliosis left convex. 5. Moderate varus of shanks.
Figure 2. Two month old child, “Syndrome of Contractures and Deformities”. 1. Plagio-
cephalia. 2. Torticollis sinister. Head turned to the right. 3. Restricted abduction of left
hip. 4. Varus of shank.
Deformities” are: higher weight, greater length of the fetus’s body and from the
mother side: small abdomen during pregnancy, lack of amniotic fluids (oligohy-
dramnios) and inconvenient, “androidal” or “platypelloid” pelvic bone anatomy.
Asymmetrical contractures of joints imply discrepancies in ranges of movements
of separate joints (hip: left: right, knee: left: right, left: right sides of spine).
DOI: 10.4236/ss.2019.101004 25 Surgical Science
Karski Tomasz et al.
Figure 3. Typical “Syndrome of Contractures and Deformities”. Child 1 month old.
Changed axis of spine (scoliosis infantilis). Limited abduction of the left hip as symptom
of dysplasia (DDH).
They can be additionally influenced by Minimal Brain Dysfunctions (MBD).
MBD—means sub-spasticity of various groups of muscles—mostly flexors of
hip, flexors of knees, and flexors of feet.
The “left sided SofCD” is more common, as a result of the first position of the
fetus during pregnancy, when the fetus is placed on his back on the left side of
the mother’s uterus. Such pregnancies occur in 85% - 95% of all cases [14] [15].
From the orthopaedic point of view, children with “Syndrome of Contractures
and Deformities” has the dispositions to: infantile scoliosis, torticollis (wry
neck), and dysplasia of the hip in form of development dysplasia of hip (DDH)
according Klisic, mostly of the left hip because of the limited abduction of this
joint (Figure 3(b)). In SofCD limited adduction of the right hip in their “exten-
sion position”, in some cases even abduction contracture of this joint, play role
in the development of the so-called idiopathic scoliosis, through “gait” and
“permanent standing “at ease” on the right leg” (Figures 9-12).
Clinical symptoms of the “Syndrome of Contractures” are according Prof.
Hans Mau [5] [7]-[13] [16] [17] [18]. There are asymmetrical position of various
parts of the child’s body and asymmetrical range of movements of joints
(Figures 1-3):
1) Scull deformity (plagiocephaly);
2) Wry neck (torticollis muscularis);
DOI: 10.4236/ss.2019.101004 26 Surgical Science
Karski Tomasz et al.
3) Infantile scoliosis (scoliosis infantilis)—other than idiopathic scoliosis;
4) Limited abduction of the left hip. Untreated, can lead to development of
dysplasia. According to Prof. P. Klisic there is DDH (Developmental Dysplasia
of the Hip [DDH]), which was mentioned earlier;
5) Contracture (shortening) of abductor muscles and soft tissues of the right
hip (according to T. Karski), described as Haltungsschwäche (“weak posture”)
by H. Mau—is the cause of oblique position of pelvis and through func-
tion—“standing” and “gait” is the cause of scoliosis;
6) Pelvic bone asymmetry, described by Prof. Mau—according ours observa-
tions is caused by shortening (contracture) of adductors of the left hip and by
shortening (contracture) of abductors of the right hip (explanation of T, Karski);
7) Foot deformities—such as: pes equino-varus, pes equino-valgus, pes cal-
caneo-valgus.
In Lublin, in 2006 (T. Karski) we added to the “Syndrome of Contractures” in
newborns and babies, as the eighth deformity, the excessive shank deformity
(crura vara) which later can lead, under special conditions, to Blount disease [see
literature—article published in German and in USA—Karski T. and co-authors,
and T. Karski & J. Karski]. Since 2006 we talk about the “Syndrome of Contrac-
tures and Deformities” (SofCD) what we described in chapter earlier.
2. Material
During 8 years (2009-2017) authors examined 922 newborns and babies with
symptoms of the SofCD. The diagnosis criteria were similarly like using by Prof.
Hans Mau—the registration of clinical symptoms of asymmetries in position
and in movement of head, neck, pelvis, hips, knees, feet. The control group con-
sisted of 263 children presented by parents for examination, with no sign of the
SofCD, but with others problems. In 2018 the material gathers 1033 cases.
Syndrome of contractures and its influence are on locomotors system [1] [2]
[3] [4] [7] [9] [11] [16]-[24]. In article we present the cases of SofCD and its in-
fluence on:
1) dysplasia of the hip;
2) wry neck (torticollis);
3) biomechanical etiology of the so-called idiopathic scoliosis;
4) Blount disease [19] [20] [21] [22].
Hips [1] [3] [4] [8] [10] [11] [13] [19] [20] [25] [26]: The dysplasia of the hips
can be connected with 1) the Syndrome of Contractures and Deformities
(SofCD), with 2) laxity of joints and with 3) disorders of the central nerve system
witch influence the movement of hips. The dysplasia of the hips in babies with
the SofCD shows a deficit of abduction of hips, mostly on the left hip (Figure
3(b)). The physiological treatment in this group of deformation is simple, easy
and gives good results in relative short time. In therapy, as always, it is important
to carry the child in full abduction and flexion of hips for over one year, as well to
use orthopedic abduction devices (Figures 4-6). Unfortunately, in opposition to
our recommendations, “wrongly educated” physiotherapists and rehabilitation
DOI: 10.4236/ss.2019.101004 27 Surgical Science
Karski Tomasz et al.
Figure 4. Improper way of carrying the child recommended by poorly educated orthope-
dic surgeons, physiotherapist, pediatricians (a). Proper way of carrying the child. Full
abduction of the hips—the best prophylaxis for dysplasia (b).
Figure 5. Two month old child with typical Syndrome of Contractures and Deformities.
Carrying the child in full abduction of the hips is the prophylaxis for dysplasia. Twisting
child’s head to the left side is the best therapy of left sided wry neck (b).
Figure 6. One year old child. Syndrome of Contracture and Deformities. Proper way of
carrying the child in full abduction of the hips—the best method of therapy for dysplasia.
Permanent rotation position of the head to the left side is the best method of therapy for
the left sided wry neck.
DOI: 10.4236/ss.2019.101004 28 Surgical Science
Karski Tomasz et al.
doctors—in Poland as well as also in abroad—recommend carrying children in a
way they are facing to the front, to streets, to shops (Figure 4(a)).
In some patients we use orthopedic abduction devices. For successful treat-
ment and for full “restitutio ad integrum” we need months or sometimes years.
Children with dysplasia and laxity of joints need an especially long therapy. We
let the child stand and walk at the age of one year, if in this moment the hips are
healthy in a clinical and radiological examination. It is forbidden to stand and walk
earlier and if it happens it is a mistake of therapy—by also such recommendation
is giving by some pediatricians doctors. If the dysplasia of the hips has not been
cured sufficiently during the first year of child’s life, for prolonged therapy, we use
a spongy triangle for walking or Weickert treasures—model for walking (Figure
7(a), Figure 7(b)).
Neck [2] [4] [5] [7] [13] [19] [20] [21] [23] [27] [28]: Very frequently (6% to
8% of the Polish population) in newborns and babies occurs a wry neck—in
Latin—torticollis muscularis or torticollis myogenes. There are three forms of
such a deformity:
1) Torticollis connected with SofCD;
2) Torticollis after traumatic delivery;
3) Congenital wry neck with tumor neonatorum.
Until now in Poland, wry neck is treated in many Medical Centres with old
methods of physiotherapy by stimulations, frequent, repeated movements, by
Vojta method. This kind of therapy never gives sufficient results. Only perma-
nent “rotation stretching position” in the direction of the torticollis side give a
good result (Figure 5(b), Figure 6, Figure 8). This method of therapy was intro-
duced in Lublin in July 1974 (44 years ago—T. Karski) and give success in all
cases in age from 1 to 3 year-old patients. Here I would like to remind, that be-
fore 1974 in the Pediatric Orthopedic and Rehabilitation Department of Medical
Figure 7. Two methods of treatment of hip dysplasia. (a) child with Weickert’s trousers
for walking. (b) child with spongy triangle. Walking in abduction is the best method for
therapy of dysplasia in older children. The presented methods are better than orthopedic
devices used when the child is laying down.
DOI: 10.4236/ss.2019.101004 29 Surgical Science
Karski Tomasz et al.
Figure 8. Three year old child. Stretching-rotation treatment to the left side for left sided
wry neck is successful even for older children. At this age a successful therapy needs more
time, even 2 - 3 years, if the time of the stretching lasts 1 - 2 hours every day.
University in Lublin we had operated many patients, even 2 - 3 cases per week.
From 1974 to 1995 the number operated patients was significantly smaller. In
years 1995-2009 (in this time Prof. T. Karski was the head of the Department),
we operated only 3 - 5 patients per year, commonly coming from the far regions
of ours country.
Spine, scoliosis [7] [12] [13] [19] [21] [25] [29]-[36]: The biomechanical etiol-
ogy of the so-called idiopathic scoliosis (“so-called”—because the etiology has been
discovered and explained, 1995—T. Karski and J. Karski) is based on the asymme-
try of movements of hips and on the asymmetry of functioning—“standing” and
“gait”. The history of Lublin discoveries are the following:
1995—First presentation of the biomechanical etiology during Orthopedic
Congress in Szeged (Hungary);
1996—First publication in Germany;
1997—Confirmation that the “standing ‘at ease’ on the right leg” is an impor-
tant cause in two groups of scoliosis;
2001—Description of the new classification—first and second group of scoliosis;
2004—Description of the third group of scoliosis;
2006—Ultimate description of the “model of the movement of the hips” and
type of scoliosis (three groups and four types—see classification);
2007—Explanation why blind children do not have scoliosis (gait is without
lifting of legs, standing is safe on both legs) and describing the “indirect, addi-
tional influences” in development of scoliosis, coming from Central Nerve Sys-
tem (CNS) in children with Minimal Brain Dysfunction (MBD). In children with
MBD there are: 1) anterior tilt of pelvis, 2) extension contracture of the spine, 3)
laxity of joints.
We present the following stages in the development of the so-called idiopathic
DOI: 10.4236/ss.2019.101004 30 Surgical Science
Karski Tomasz et al.
scoliosis:
1) Asymmetry of position and range of movements of the hips resulting from
the “Syndrome of Contracture and Deformities” (SofCD);
2) Limited movements of right hip: restricted adduction in strait position of
joint, restricted internal rotation, frequent limited extension of both hip joints;
3) Next influences are connected with the function—“gait” and “standing”.
Here we explain: during walking, restricted movement—not presented in the
right hip is transmitted to the pelvis and to the spine as compensatory move-
ment, which causes rotation distortion of inter-vertebral joints and stiffness of
the spine;
4) The next cause is connected with permanent standing “at ease” on the right
leg. As a result, appear the left convex lumbar curve in scoliosis II-nd epg and in
I-st epg type.
In the new classification of the so-called idiopathic scoliosis there are three
groups and four types of spine deformities (Figures 9-12). Distinguishing types
of scoliosis is important for the therapy. Here we explain: in every type of scolio-
sis, stretching exercises for spine, for hips and for proper position of pelvis are
the only correct therapies. They should lead to a full and symmetrical movement
of spine—flexion, deviation, rotation, the same in hips—full and symmetrical
adduction, internal rotation and extension. In our program of therapy we never
recommend strengthening exercises, but we recommend such sport arts as ka-
rate, taekwondo, aikido, yoga.
Shank, Blount disease [13] [19] [20] [21] [22]: The varus deformity of shank
was added to the “Syndrome of Contractures” in 2006 [T. Karski] (Figures
13-15). In many newborns, as a result of adapting to mother’s uterus, develop
varus deformity of shanks. In some cases, varus deformity is bigger than “normal”,
Figure 9. New classification. 15 year old patient. “S” scoliosis in I epg, 3D. Primary dou-
ble curves. Connection with gait & standing “at ease” on the right leg. Specific model of
hips movements. In development—first rotation deformity, next curves. Stiffness of
spine. Progression.
DOI: 10.4236/ss.2019.101004 31 Surgical Science
Karski Tomasz et al.
Figure 10. New classification. 10 year old patient. “C” scoliosis in II/A epg. 1D. Connec-
tion with standing “at ease” on the right leg. Specific model of hips movements. Flexible
spine. No progression.
Figure 11. New classification. 13 year old patient. “S” scoliosis in II/B epg. 2D or mix.
Thoracic curve secondary. Connection with standing “at ease” on the right leg plus laxity of
joints or wrong exercises in previous therapy. Flexible spine. No progression or a small one.
Figure 12. New classification. Two patients aged 18 and 20. Scoliosis “Ist” in IIIrd epg.
Specific model of hips movements. Connection with gait only. 2D or mix. Stiffness of
spine. No curves or a small one.
DOI: 10.4236/ss.2019.101004 32 Surgical Science
Karski Tomasz et al.
Figure 13. Varus deformity of shanks—typical Blount disease.
Figure 14. Varus deformity of shanks—Blount disease plus rickets.
Figure 15. Varus deformity of shanks—one-sided Blount disease. Left leg self corrected.
Treatment of children aged 1 - 3 years only by physiotherapy (look text). Older child-
ren—surgery.
DOI: 10.4236/ss.2019.101004 33 Surgical Science
Karski Tomasz et al.
and then, it can trigger, under special conditions to Blount disease. These condi-
tions are following:
1) premature, too early standing and walking, under the age of 1;
2) vitamin D deficiency.
In such situations Blount disease can develop, it means varus in proximal part
of shanks, in place of epiphysis and methaphysis. Primary Blount disease in
every case is bilateral. In later years, one of the shanks, usually the left one, can
correct itself spontaneously. The deformation of the right shank is durable and
becomes bigger with time. Thus, one-sided deformity can be noticed in cases
with the “Syndrome of Standing ‘at ease’ on the Right Leg” (new syndrome—see
Literature).
All cases of Blount disease until 1981 in our Department had been operated.
In the 80’ we found the conservative method of therapy. We “use” for this ther-
apy, the Heuter-Volkmann law. According to this law, pathological changes of
axes of lower extremities develop when “existing loading bigger than normal and
primary varus of shanks is observed”. If loading or overloading is not present
spontaneously appears correction of axis. Since 1981 we recommended parents
to carry children with varus deformity 10 or even 20 degrees for 2 - 3 months, in
some cases 4 months, until the shanks regain their normal axes. In this period
the child shouldn’t stand nor walk. To all cases of Blount disease we add vitamin
D. After introducing such a conservative treatment, from 1981 until now, in all
cases, in children aged from 1 to 2.5, the axes of legs come to normal. We em-
phasize that the age for such treatment is 1 to 2.5, in some cases—3 years. Older
children have to be operated on, like before.
3. Discussion
In etiology of deformities and illnesses of movement apparatus can play role the
following causal influences: congenital, hormonal, coming from Central Nerve
System—in children with MBD, but we must remember about very frequent in-
fluences going from the “Syndrome of Contractures and Deformities” (SofCD).
The asymmetries in SofCD—in position of part of the body of newborn and ba-
bies, in range of movement of joints can influence the development and growth
of the child body [8] [9] [13] [19] [20] [23] [24] [29] [30] [32] [34] [35]. They
can changed function—“standing” and “gait”. Non treated can even influenced
the function of hips, knee, feet, spine in adult period of life. So regarding to
proper treatment of newborns, babies and youth persons we should see as pro-
phylaxis management for the older people.
4. Conclusions
1) Every orthopedic surgeon and pediatric doctor, as well every physiothera-
pist, should be familiarized with the knowledge about the “Syndrome of Con-
tractures and Deformities” (SofCD) based on Prof. Hans Mau’s (Germany) ex-
perience.
DOI: 10.4236/ss.2019.101004 34 Surgical Science
Karski Tomasz et al.
2) Every newborn and baby with the SofCD should be treated very early by
proper nursing and using of orthopedic devices, older children by stretching ex-
ercises in order to reach symmetry of joint movements of hips, knees, feet, and
spine.
3) Only symmetry of movements and of function enables proper body growth.
This rule is especially important in prophylaxis of hip dysplasia and of scoliosis.
4) Effective treatment of small children with residual changes of SofCD should
be considered an effective prophylaxis of insufficiency of the movement appara-
tus and as an important procedure against arthrosis of hips, knees, spine in older
patients.
5) The aim of physiotherapy is to achieve symmetry of position, symmetry of
movements of joints as well symmetry in development and growth.
6) For the treatment of older children we should use the stretching exercises
to heal contracted (shortened) side or part of the body, and of region of joints
but we never recommend strengthening exercises.
7) In therapy and prophylaxis of the so-called idiopathic scoliosis we recom-
mend the stretching exercises for right hips to obtain full movement, flex-
ion-rotation exercises for spine, embryo position for rest and sleeping in the
nights, and standing “et ease” only on the left leg, sport, especially exercises like
karate, taekwondo, aikido, kung fu.
8) Additionally, in treatment we can use thermotherapy, magnetic fields, bio-
dynamic (diadynamic), laser, and massages. Exercises in geothermal water are
especially useful.
Acknowledgements
1) Many thanks to Honorata Menet for correction of English text.
2) All patients—adults and children—are agree to reproduce the figures in the
scientific publication, in Surgical Science Journal, in USA.
Conflicts of Interest
The authors declare no conflicts of interest regarding the publication of this pa-
per.
References
[1] Dega, W. (1932) Badania z dziedziny etiologii wrodzonego zwichnięcia biodra [Re-
search on the Subject of the Congenital Dysplasia of the Hip]. Chirurgia Narządu
Ruchu, 144-151.
[2] Golden, K.A., Beals, S.P., Littlefield, T.R., et al. (1999) Sternocleidomastoid Imbal-
ance versus Congenital Muscular Torticollis: Their Relationship to Positional Pla-
giocephaly. The Cleft Palate-Craniofacial Journal, 36, 256-261.
https://doi.org/10.1597/1545-1569_1999_036_0256_sivcmt_2.3.co_2
[3] Hensinger, R.N. (1979) Congenital Dislocation of the Hip. Clinical Symposium,
31-35.
[4] Howorth, B. (1977) The Etiology of Congenital Dislocation of the Hip. Clinical Or-
DOI: 10.4236/ss.2019.101004 35 Surgical Science
Karski Tomasz et al.
thopedics, 29, 164-179.
[5] Cheng, J.C., Tang, S.P., Chen, T.M., et al. (2000) The Clinical Presentation and
Outcome of Treatment of Congenital Muscular Torticollis in Infants: A Study of
1,086 Cases. Journal of Pediatric Surgery, 35, 1091-1096.
https://doi.org/10.1053/jpsu.2000.7833
[6] Watson, G.H. (1971) Relation between Side of Plagiocephaly, Dislocation of Hip,
Scoliosis, Bat Ears, and Sternomastoid Tumour. Archives of Disease in Childhood,
46, 203-210. https://doi.org/10.1136/adc.46.246.203
[7] Karski, T. (1996) Kontrakturen und Wachstumsstörungen im Hüft- und Beckenbereich
in der Ätiologie der sogenannten “Idiopathischen Skoliosen”—Biomechanische
Überlegungen [The Contracture and Growth Abnormalities in Hip and Pelvis
Region in the Etiology of So-Called Idiopathic Scoliosis—Biomechanical Conside-
rations]. Orthopädische Praxis, 32, 155-160.
[8] Karski, T., Kałakucki, J. and Karski, J. (2006) Syndrome of Contractures (According
to Mau) with the Abduction Contracture of the Right Hip as Causative Factor for
Development of the So-Called Idiopathic Scoliosis. Studies in Health Technology
and Informatics, 123, 34-39.
[9] Malawski, S. (1994) Własne zasady leczenia skolioz niskostopniowych w świetle
współczesnych poglądów na etiologię i patogenezę powstawania skolioz [Own Prin-
ciples of the Therapy of Beginnings Scoliosis in Actually Point of View to Etiology
and Pathogenesis of Scoliosis]. Chirurgia Narządów Ruchu i Ortopedia Polska, 59,
3, 189-197.
[10] Barlow, T.G. (1962) Early Diagnosis and Treatment of Congenital Dislocation of the
Hip. Journal of Bone and Joint Surgery, 44-B, 292-3012.
[11] Green, N.E. and Griffin, P.P. (1982) Hip Dysplasia Associated with Abduction
Contracture of the Contra Lateral Hip. The Journal of Bone and Joint Surgery, 64,
1273-1281.
[12] Tomasz, K., Kałakucki, J. and Karski, J. (2007) Relationship of “Syndrome of Con-
tractures” in Newborns with the Development of the So-Called Idiopathic Scoliosis.
World Journal of Pediatrics, 3, 254-259.
[13] http://www.ortopedia.karski.lublin.pl/
[14] Oleszczuk, J., Szymański, W. and Wilczyński, B. (1999) Patologia Ciąży (Pathological
Pregnancy). In: Rudolf, K., Ed., Położnictwo, Dream Publ., Kraków, 395-499.
[15] Oleszczuk, J., Chazan, B., Kamiński, K., Leszczyńska-Gorzelak, B., Skręt, A. and
Szymański, W. (1999) Poród Patologiczny (Pathological Childbirth/Delivery). In:
Rudolf, K., Ed., Położnictwo, Dream Publ., Kraków, 291-337.
[16] Mau, H. (1983) Powstawanie skoliozy u małych dzieci w: Wczesne wykrywanie i
zapobieganie progresji bocznych skrzywień kręgosłupa (Early Screening and
Prophylaxis of Scoliosis) Materiały z Sesji Naukowej PAN. PZWL, Warszawa,
34-42.
[17] Mau, H. (1979) Zur Ätiopathogenese von Skoliose, Hüftdysplasie und Schiefhals im
Säuglinsalter (Ethiopathogenesis of Scoliosis, Hip Dysplasia and Torticollis in
Infants). Zeitschrift F r Orthop dische Chirurgie, 5, 601-605.
[18] Mau, H. (1982) Die Atiopatogenese der Skoliose (Ethiopathogenesis of Scoliosis).
Bücherei des Orthopäden, Band 33, Enke Verlag Stuttgart, 1-110.
[19] Jacek, K. and Karski, T. (2012) Zespół przykurczów u noworodków i niemowląt
przyczyną odległych dysfunkcji narządu ruchu w tym skolioz tzw. idiopatycznych.
Wykrywanie zagrożeń oraz zasady profilaktyki przez zabiegi fizjoterapeutyczne
[Syndrome of Contractures in Newborns and Babies as a Cause of Deformities in
DOI: 10.4236/ss.2019.101004 36 Surgical Science
Karski Tomasz et al.
Movement Apparatus and in Etiology of the So-Called Idiopathic Scoliosis in Next
Years of Life. New Screening and Treatment by Physiotherapy]. Zesz. Nauk., WSSP
T. 15, S. 11-25, Bibliogr. Poz. 43.
[20] Karski, T. and Jacek, K. (2015) “Syndrome of Contractures and Deformities” ac-
cording to Prof. Hans Mau as Primary Cause of Hip, Neck, Shank and Spine De-
formities in Babies, Youth and Adults. American Research Journal of Medicine and
Surgery, 1, 1-10.
[21] Tibor, V. and Karski, T. (2000) Skoliozy tzw. idiopatyczne-przyczyny, rozwój i
utrwalanie się wady. Profilaktyka i zasady nowej rehabilitacji [The Etiology of the
So-Called Idiopathic Scoliosis. Progress and Fixation of the Spine Disorders. The
Prophylaxis and Principles of the New Rehabilitation Treatment]. KGM, Lublin,
1-143.
[22] Karski, T., Drabik, Z., Karski, J. and Agbemey, E. (1994) Osteotomien in der Be-
handlung von Kindern mit Crura vara (M. Blount) [Surgery in the Treatment of
Children with Crura Vara (Blount Disease) Orthop]. Praxis, Heft 9, 582-585.
[23] Karski, T., Frelek-Kars, M., Karski, J., Madej, J. and Kałakucki, J. (2001) Zespół
przykurczów u noworodków i niemowląt przyczyną odległych dysfunkcji narządu
ruchu w tym tzw. skolioz idiopatycznych. Wykrywanie zagrożeń nieprawidłowego
rozwoju kręgosłupa i zasady nowej profilaktyki skolioz [The Syndrome of Contrac-
tures at Newborns and Babies as a Cause of Dysfunctions of Skeletal System and
among Others of the So-Called Idiopathic Scoliosis. The Discovery of the Danger of
the Oncoming Scoliosis. Rules of New Prophylactics]. Międzynarodowa Konferencja
Naukowa: Uwarunkowania rozwoju sprawności i zdrowia. Częstochowa, 10-11
grudnia. Progr. i streszcz, s. 11-12.
[24] Karski, T., Karski, J., Madej, J. and Latalski, M. (2002) Persönliche Überlegungen
zur Ätiologie der idiopathischen Skoliosen. Praktische Hinweisen zur Entdeckung
beginnender Skoliosen. Möglichkeiten der Prophylaxe [Considerations about Eti-
ology of the Idiopathic Scoliosis. Practical Directions in Discovering of the Begin-
nings Stages of Scoliosis]. Orthopädische Praxis 02/, 38 Jahrgang, Seite 75-83.
[25] Kane, A.A., Mitchell, L.E., Craven, K.P., et al. (1996) Observations on a Recent In-
crease in Plagiocephaly without Synostosis. Pediatrics, 97, 877-885.
[26] Rogers, G.F. and Mulliken, J.B. (2003) The Significance of Torticollis in Deforma-
tional Posterior Plagiocephaly [Abstract]. Proceedings of the Tenth International
Congress of the International Society of Craniofacial Surgery, 21-24 September
2003, 61.
[27] Karski, T. (2002) Etiology of the So-Called “Idiopathic Scoliosis”. Biomechanical
Explanation of Spine Deformity. Two Groups of Development of Scoliosis. New
Rehabilitation Treatment. Possibility of Prophylactics, Studies in Technology and
Informatics. In: Theodoros, B., Ed., Research into Spinal Deformities 4, IOS Press,
Washington, Vol. 91, 37-46.
[28] Karski, T., Karski, J. and Kałakucki, J. (2003) Minimal Incongruence of the Hip
Joint at Youth and Adults Treated and Not-Treated because of DDH in Baby Pe-
riod. 2nd Annual International Conference SICOT/SIROT, Cairo, 10-13 September
2003, SFS8-H.
[29] Karski, T. (2011) Biomechanical Etiology of the So-Called Idiopathic Scoliosis
(1995-2007)—Connection with “Syndrome of Contractures”—Fundamental Infor-
mation for Pediatricians in Program of Early Prophylactics. Journal of US-China
Medical Science, 8, 72-86.
[30] Jacek, K. and Karski, T. (2013) So-Called Idiopathic Scoliosis: Diagnostic Tests;
Examples of Children Incorrect Treated: New Therapy by Stretching Exercises and
DOI: 10.4236/ss.2019.101004 37 Surgical Science
Karski Tomasz et al.
Results. Journal of Novel Physiotherapies, 3, 147.
[31] Karski, T. and Karski, J. (2015) Biomechanical Etiology of the So-Called Idiopathic
Scoliosis (1995-2007). Causative Role of “Gait” and “Permanent Standing “at Ease”
on the Right Leg. New Classification. Principles of New Therapy and Causal Pro-
phylaxis. Canadian Open Medical Science & Medicine Journal, 1, 1-16.
[32] Karski, J., Karski, T., Kandzierski, G., Tarczy, M., Kałakucki, J. and Latalski, M.
(2005) “Zespół przykurczów” u noworodków i niemowląt wg prof. Hansa Mau w
wyjaśnieniu “geografii” i niektórych klinicznych cech skolioz tzw. idiopatycznych.
[“Contracture syndrome” in Newborns and Infants according to Prof. Hans Mau as
an Explanation of the “Geography” and Certain Clinical Features of Idiopathic Sco-
liosis]. Ortopedia, Traumatologia, Rehabilitacja, 23-27.
[33] Karski, T. (2005) Biomechanical Explanation of Etiology of the So-Called Idiopathic
Scoliosis. Two Etiopahtological Groups—Important for Treatment and Neo-Proph-
ylaxis. Pan Arab Journal, 9, 123-135.
[34] Jacek, K., Kalakucki, J., Karski, T. and Dlugosz, M. (2006) “Syndrom kontraktur”
(podle Mau) s abdukční kontrakturou pravého kyčelního kloubu jako příčinného
faktoru vývoje tzv. idiopatické skoliózy [Syndrome of Contractures” (According to
Mau) with the Abduction Contracture of the Right Hip as Causative Factor for De-
velopment of the So-Called Idiopathic Scoliosis]. Pohybove Ustroji (Locomotor
System)/Czech Republic, 81-88.
[35] Karski, T., Kałakucki, J. and Karski, J. (2006) “Syndrome of Contractures” (Ac-
cording to Mau) with the Abduction Contracture of the Right Hip as Causative
Factor for Development of the So-Called Idiopathic Scoliosis. Technology and In-
formatics, Vol. 1, 2, 3, In: Uyttendaele, D. and Dangerfield, P.H., Eds., Research into
Spinal Deformities 5, IOS Press, Washington, 34-39.
[36] Jacek, K., Karski, T. and Kędzierski, Z. (2013) Syndrome of Contractures and De-
formities” in Newborns and Infants according Mau—And Its Influence for Secon-
dary Deformities of Movement Apparatus in Babies, Youth and Adults. Pohybove
Ustroji (Locomotor System), 315-317.
DOI: 10.4236/ss.2019.101004 38 Surgical Science
View publication stats
You might also like
- Treatment of Massive Obesity With Ricereduction Diet Program. An Analysis of 106 Patients With at Least A 45-kg Weight LossDocument10 pagesTreatment of Massive Obesity With Ricereduction Diet Program. An Analysis of 106 Patients With at Least A 45-kg Weight LossJéssica Moreira100% (2)
- Animal-Assisted TherapyDocument196 pagesAnimal-Assisted Therapyraquelbibi100% (3)
- Asian Studies Major For College Ancient History of East AsiaDocument64 pagesAsian Studies Major For College Ancient History of East AsiaApaaNo ratings yet
- Raoul Tubiana - Jean-Michel Thomine - Evelyn Mackin - F Brunelli - Examination of The Hand and Wrist-CRC PressDocument406 pagesRaoul Tubiana - Jean-Michel Thomine - Evelyn Mackin - F Brunelli - Examination of The Hand and Wrist-CRC PressMaricruzhdezaNo ratings yet
- Vestax VCI-380 Midi Mapping v3.4Document23 pagesVestax VCI-380 Midi Mapping v3.4Matthieu TabNo ratings yet
- A.D. Pearle - Surgical Technique and Anatomic Study of Latissimus Dorsi and Teres Major Transfers (2006)Document9 pagesA.D. Pearle - Surgical Technique and Anatomic Study of Latissimus Dorsi and Teres Major Transfers (2006)João Pedro ZenattoNo ratings yet
- Post-Traumatic Elbow Stiffness - Arthrolysis and Mechanical DistractionDocument31 pagesPost-Traumatic Elbow Stiffness - Arthrolysis and Mechanical DistractionAna-Maria ȘtefanNo ratings yet
- The Origin and Evolutionary Biology of Pinnipeds Seals, Sea Lions, and WalrusesDocument26 pagesThe Origin and Evolutionary Biology of Pinnipeds Seals, Sea Lions, and WalrusesMaya D.No ratings yet
- Davao Doctors College General Malvar Street, Davao City Nursing ProgramDocument5 pagesDavao Doctors College General Malvar Street, Davao City Nursing ProgramJhoneric Vencer EscultorNo ratings yet
- The Multisensory HandbookDocument177 pagesThe Multisensory Handbookraquelbibi100% (3)
- MycologyDocument129 pagesMycologyPriyanka Rajput100% (4)
- Amlodipine Drug StudyDocument1 pageAmlodipine Drug StudyElleNo ratings yet
- Neuromuscular Diseases and RehabilitationDocument41 pagesNeuromuscular Diseases and RehabilitationraquelbibiNo ratings yet
- Levucell SB Research BibliographyDocument23 pagesLevucell SB Research BibliographyrubenriveraNo ratings yet
- Kinesiology of The Musculoskeletal System 3rd Edition (Donald A. Neumann) Capitulo Ombro ComplexoDocument57 pagesKinesiology of The Musculoskeletal System 3rd Edition (Donald A. Neumann) Capitulo Ombro ComplexoMurilo PinzNo ratings yet
- Assessment of OrthopedicVersus Neurologic Causes of Gait Change in Dogs and CatsDocument9 pagesAssessment of OrthopedicVersus Neurologic Causes of Gait Change in Dogs and CatsAristoteles Esteban Cine VelazquezNo ratings yet
- Thoracic IncisionsDocument10 pagesThoracic IncisionsRadioputro WicaksonoNo ratings yet
- Hemorrhoidal Laser Procedure - Short - and Long-Term Results From A Prospective StudyDocument5 pagesHemorrhoidal Laser Procedure - Short - and Long-Term Results From A Prospective StudyagusNo ratings yet
- Strategy of The Netherlands in The Field of Rare DiseasesDocument20 pagesStrategy of The Netherlands in The Field of Rare DiseasesGehd JdifkNo ratings yet
- Biomechanics of Cervical SpineDocument58 pagesBiomechanics of Cervical SpinesanavoraNo ratings yet
- Skeletal SystemDocument64 pagesSkeletal SystemGem Rose UretaNo ratings yet
- Pain Education For Physiotherapists Is It Time For C - 2011 - Journal of PhysioDocument2 pagesPain Education For Physiotherapists Is It Time For C - 2011 - Journal of PhysioCông Tác Xã Hội Phòng100% (1)
- Far Lateral Vs Extreme Lateral AproachDocument14 pagesFar Lateral Vs Extreme Lateral AproachcristianescNo ratings yet
- Vertebral ColumnDocument84 pagesVertebral ColumnGenesis GeronagaNo ratings yet
- Damage Control Orthopaedics in Spinal Trauma JAAOSDocument12 pagesDamage Control Orthopaedics in Spinal Trauma JAAOSAzmi FarhadiNo ratings yet
- Human Postural ControlDocument9 pagesHuman Postural Controlelbueno21No ratings yet
- AOTrauma Elastic Stable IntramedullaryDocument249 pagesAOTrauma Elastic Stable IntramedullaryVivek ChNo ratings yet
- 2011fetal Brain Function Jaypee Journal-AnnotatedDocument7 pages2011fetal Brain Function Jaypee Journal-AnnotatedDamara Gardel100% (1)
- Early Total Care To Early Appropriate Care What.2Document8 pagesEarly Total Care To Early Appropriate Care What.2ChrisNo ratings yet
- Effect of Heat Treatment On Edible Yam (Dioscorea Activity: Kinetic and Thermodynamic AnalysisDocument10 pagesEffect of Heat Treatment On Edible Yam (Dioscorea Activity: Kinetic and Thermodynamic Analysisاجي تقرى100% (1)
- High Median Nerve InjuriesDocument10 pagesHigh Median Nerve InjuriesKarime TapiaNo ratings yet
- .1 Arthritides-P1Document14 pages.1 Arthritides-P1ELIZABETH GRACE AMADORNo ratings yet
- Introduction To FranchisingDocument23 pagesIntroduction To FranchisingJuzer RampurawalaNo ratings yet
- Portal Vein Thrombosis 2021Document175 pagesPortal Vein Thrombosis 2021haitham aloolNo ratings yet
- Protocol For The Examination of Specimens From Patients With Plasma Cell NeoplasmsDocument12 pagesProtocol For The Examination of Specimens From Patients With Plasma Cell NeoplasmsMaikka IlaganNo ratings yet
- Diabetic Neuropathy: DR Shahjada SelimDocument129 pagesDiabetic Neuropathy: DR Shahjada SelimmadboyNo ratings yet
- PFO UpdateDocument33 pagesPFO UpdateMitesh PatelNo ratings yet
- AAOS Clinical Practice Guideline Summary .10Document9 pagesAAOS Clinical Practice Guideline Summary .10mukhlis akmalNo ratings yet
- Bacteriological Spectrum and Antibiogram of Isolates Obtained From Smoked Fish Sold in Federal Capital Territory, Abuja, NigeriaDocument10 pagesBacteriological Spectrum and Antibiogram of Isolates Obtained From Smoked Fish Sold in Federal Capital Territory, Abuja, NigeriaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Umbilicalherniarepair: Overview of Approaches and Review of LiteratureDocument16 pagesUmbilicalherniarepair: Overview of Approaches and Review of LiteratureVictor Matias BarriosNo ratings yet
- Dermatology NLC DR Manish Soni 2021Document94 pagesDermatology NLC DR Manish Soni 2021akashineeNo ratings yet
- Iqvia Institute Biosimilars in The United States 2023 Usl Orb3393Document41 pagesIqvia Institute Biosimilars in The United States 2023 Usl Orb3393Igor IlievskiNo ratings yet
- Devil-Fictions by Lance Phillips Book Preview-AfDocument20 pagesDevil-Fictions by Lance Phillips Book Preview-AfBlazeVOX [books]No ratings yet
- Posture Dr. Dr. MY, SP KFR-KDocument67 pagesPosture Dr. Dr. MY, SP KFR-KCikupaNo ratings yet
- 15 Gene Expression Translation SDocument6 pages15 Gene Expression Translation SHelp Me Study TutoringNo ratings yet
- Modul Hip Disarticulation ProstheticsDocument67 pagesModul Hip Disarticulation ProstheticsCapt KidsNo ratings yet
- Attock Refinery Limited: Low Gravity Residual Fuel OilDocument7 pagesAttock Refinery Limited: Low Gravity Residual Fuel OilshahNo ratings yet
- Surpass 1Document13 pagesSurpass 1Fernando DominguezNo ratings yet
- Acl Injury & Acl Protocol Melbourne GuidelineDocument36 pagesAcl Injury & Acl Protocol Melbourne GuidelineCrunchy Cacao100% (1)
- Interdigital (Morton's) Neuroma - Foot & Ankle - OrthobulletsDocument3 pagesInterdigital (Morton's) Neuroma - Foot & Ankle - OrthobulletsEmiel AwadNo ratings yet
- Thy ReviewerDocument229 pagesThy ReviewerKimberly Anne OjedaNo ratings yet
- Pedicle Screw Fixation in Fracture of Thoraco-Lumbar SpineDocument21 pagesPedicle Screw Fixation in Fracture of Thoraco-Lumbar SpineNiyati SharmaNo ratings yet
- Nexus ICSIDocument114 pagesNexus ICSIDr.Pratixa JoshiNo ratings yet
- Endocrine Manifestations of Systemic Autoimmune Diseases, Volume 9 (Handbook of Systemic Autoimmune Diseases) (PDFDrive)Document352 pagesEndocrine Manifestations of Systemic Autoimmune Diseases, Volume 9 (Handbook of Systemic Autoimmune Diseases) (PDFDrive)Laura Diana BarthaNo ratings yet
- Protocol: Percutaneous Tibial Nerve StimulationDocument8 pagesProtocol: Percutaneous Tibial Nerve StimulationAléssio NovaisNo ratings yet
- Levin1981Document11 pagesLevin1981luis sanchezNo ratings yet
- 05 Fetal Development 1Document4 pages05 Fetal Development 1Gwen CastroNo ratings yet
- Philippine PanDocument82 pagesPhilippine PanJ. G. CheockNo ratings yet
- GOLD For COPD Pocket GuideDocument30 pagesGOLD For COPD Pocket Guideraul sinatoNo ratings yet
- Deep Tendon Reflex Steps On How To Assess The DTR: Normal Response: DTR GradingDocument2 pagesDeep Tendon Reflex Steps On How To Assess The DTR: Normal Response: DTR GradingElla EvangelistaNo ratings yet
- 7the Axis VertebraDocument151 pages7the Axis VertebraAminou MounirouNo ratings yet
- Centrally Mediated Abdominal Pain SyndromesDocument4 pagesCentrally Mediated Abdominal Pain SyndromesPolo Good BoyNo ratings yet
- Lingaya University ProspectusDocument27 pagesLingaya University ProspectusChalla RamanamurtyNo ratings yet
- Foot and Ankle Injuries and Pain: Indranil Neel' Kushare, MDDocument55 pagesFoot and Ankle Injuries and Pain: Indranil Neel' Kushare, MDrizwan.mughal1997No ratings yet
- Evaluation of A Paediatric Early Warning System Pews Score On Admission To A Paediatric Intensive Care Unit To Predict Mortality Risk in A Low Resource Setting Guinea BissauDocument6 pagesEvaluation of A Paediatric Early Warning System Pews Score On Admission To A Paediatric Intensive Care Unit To Predict Mortality Risk in A Low Resource Setting Guinea BissauHerald Scholarly Open AccessNo ratings yet
- Syndrome of Contractures and Deformities SofCD Dysplasia of Hips Varus Deformity of Shanks Wry Neck So Called Idiopathic Scoliosis Causes Clinic Prophylaxis TherapyDocument15 pagesSyndrome of Contractures and Deformities SofCD Dysplasia of Hips Varus Deformity of Shanks Wry Neck So Called Idiopathic Scoliosis Causes Clinic Prophylaxis TherapyAthenaeum Scientific PublishersNo ratings yet
- Neuromuscular Diseases and RehabilitationDocument41 pagesNeuromuscular Diseases and RehabilitationraquelbibiNo ratings yet
- Patterns of Postural Assymetry in InfantsDocument7 pagesPatterns of Postural Assymetry in InfantsraquelbibiNo ratings yet
- Global Postural Reeducation For Patients With Musculoskeletal Conditions. A Systematic Review of Randomized Controlled TrialsDocument12 pagesGlobal Postural Reeducation For Patients With Musculoskeletal Conditions. A Systematic Review of Randomized Controlled TrialsraquelbibiNo ratings yet
- Comprehensive Psychoneuroendocrinology: Jennifer W. Applebaum, Evan L. Maclean, Shelby E. McdonaldDocument12 pagesComprehensive Psychoneuroendocrinology: Jennifer W. Applebaum, Evan L. Maclean, Shelby E. McdonaldraquelbibiNo ratings yet
- Treatments For Infantile Postural AsymmetryDocument7 pagesTreatments For Infantile Postural AsymmetryraquelbibiNo ratings yet
- Barroqueiro2014 - The Effects of A Global Postural Reeducation Program On An Adolescent Handball Player With Isthmic SpondylolisthesisDocument15 pagesBarroqueiro2014 - The Effects of A Global Postural Reeducation Program On An Adolescent Handball Player With Isthmic SpondylolisthesisraquelbibiNo ratings yet
- Effectiveness of Global Postural Re-Education For Treatment of Spinal Disorders A Meta-AnalysisDocument10 pagesEffectiveness of Global Postural Re-Education For Treatment of Spinal Disorders A Meta-AnalysisraquelbibiNo ratings yet
- Cerebral Palsy An Information Guide For ParentsDocument36 pagesCerebral Palsy An Information Guide For Parentsraquelbibi100% (1)
- What Is MDocument2 pagesWhat Is MkasjdkasNo ratings yet
- Dyspepsia LectureDocument2 pagesDyspepsia LectureDaneva Reyes0% (1)
- Practice of Medicine - by Balaram JanaDocument93 pagesPractice of Medicine - by Balaram JanaFarhana V PNo ratings yet
- Red Biotechnology ProjectDocument5 pagesRed Biotechnology ProjectMahendrakumar ManiNo ratings yet
- 125 - 187 - Benny Tjan - GalleyDocument5 pages125 - 187 - Benny Tjan - GalleyZihan ZetiraNo ratings yet
- Thoracic and Neck TraumaDocument13 pagesThoracic and Neck Traumahatem alsrourNo ratings yet
- Diseases Associated With The Various Organ SystemsDocument10 pagesDiseases Associated With The Various Organ SystemsKimh SampagNo ratings yet
- Meninges - Steven McGee - Evidence-Based Physical Diagnosis-Elsevier (2017)Document8 pagesMeninges - Steven McGee - Evidence-Based Physical Diagnosis-Elsevier (2017)Victor MejiaNo ratings yet
- Office Of: The SecretaryDocument44 pagesOffice Of: The Secretarypaomillan0423No ratings yet
- Pathology: Tutorial 5Document18 pagesPathology: Tutorial 5Salma AshrafNo ratings yet
- Hepatic EncephalopathyDocument5 pagesHepatic Encephalopathyliveconnectionz282No ratings yet
- PE M2 Dance Injuries and First AidDocument22 pagesPE M2 Dance Injuries and First AidKeith Emerich FermaNo ratings yet
- Basic First Aid 0808Document72 pagesBasic First Aid 0808BS AnilKumarNo ratings yet
- Pengetahuan Dan Sikap Masyarakat Terhadap Penyakit Malaria Di Desa Kolongan Kecamatan Talawaan Kabupaten Minahasa UtaraDocument6 pagesPengetahuan Dan Sikap Masyarakat Terhadap Penyakit Malaria Di Desa Kolongan Kecamatan Talawaan Kabupaten Minahasa Utarasri humaerahNo ratings yet
- Abinash em Gi SurDocument72 pagesAbinash em Gi Sursapkota18No ratings yet
- When To Use Deprogramming Splint and WhyDocument2 pagesWhen To Use Deprogramming Splint and WhyJustin KimberlakeNo ratings yet
- 04 SPS SAINS TG2-Nota Grafik B4Document6 pages04 SPS SAINS TG2-Nota Grafik B4AZAMOLLYNo ratings yet
- Pediatric Cholestasis: Epidemiology, Genetics, Diagnosis, and Current ManagementDocument5 pagesPediatric Cholestasis: Epidemiology, Genetics, Diagnosis, and Current ManagementAnnisa SusiloNo ratings yet
- Sulfamethoxazole Trimethoprim PDFDocument10 pagesSulfamethoxazole Trimethoprim PDFAsi SyyffaNo ratings yet
- Dissociative Amnesia Case ReportDocument3 pagesDissociative Amnesia Case ReportJon MaciejewskiNo ratings yet
- Miasm ConsolidatedDocument72 pagesMiasm ConsolidatedSatyendra RawatNo ratings yet
- S19 FullDocument11 pagesS19 FullDiana AmpulembangNo ratings yet
- FilariasisDocument8 pagesFilariasisTheeya QuigaoNo ratings yet
- 1 s2.0 S0165032721002366 MainDocument7 pages1 s2.0 S0165032721002366 Mainana cristina brazNo ratings yet
- Control of Diarrheal Diseases (CCD) Definition of DiarrhoeaDocument27 pagesControl of Diarrheal Diseases (CCD) Definition of Diarrhoeaإحسان ماجد محمدNo ratings yet
- Ozone Therapy and Uv Blood Irradiation: What It Helps TreatDocument8 pagesOzone Therapy and Uv Blood Irradiation: What It Helps TreatsumanNo ratings yet