Professional Documents
Culture Documents
ACSM Diabetes
ACSM Diabetes
Uploaded by
jrice003Copyright:
Available Formats
You might also like
- Endocrine DisordersDocument28 pagesEndocrine DisordersRhitzle Ann50% (2)
- CH1Document46 pagesCH1Muhammad FahmiNo ratings yet
- Metabolic Syndrome Thesis PDFDocument5 pagesMetabolic Syndrome Thesis PDFafknawjof100% (2)
- Adult Obesity CausesDocument9 pagesAdult Obesity CausesAntoNo ratings yet
- Heart Disease Term PaperDocument5 pagesHeart Disease Term Paperafmzxppzpvoluf100% (1)
- Overweight and Obesity CDC 2019Document6 pagesOverweight and Obesity CDC 2019Evi BaeNo ratings yet
- Clinical Guideline: Annals of Internal MedicineDocument8 pagesClinical Guideline: Annals of Internal MedicineYulias YoweiNo ratings yet
- AQ FamilyMedicine 06Document12 pagesAQ FamilyMedicine 06Eduardo OrtizNo ratings yet
- Term Paper Heart DiseaseDocument7 pagesTerm Paper Heart Diseasec5p0cd99100% (1)
- Exercise Can Help Tame Type 2 DiabetesDocument2 pagesExercise Can Help Tame Type 2 DiabetesAfifah WidyadhariNo ratings yet
- Diabetes and Exercise ThesisDocument7 pagesDiabetes and Exercise Thesistonyacartererie100% (2)
- Exercise and Diabetes: A Clinician's Guide to Prescribing Physical ActivityFrom EverandExercise and Diabetes: A Clinician's Guide to Prescribing Physical ActivityNo ratings yet
- DiabetesDocument5 pagesDiabetesJayson TrajanoNo ratings yet
- Chronic DiseaseDocument6 pagesChronic DiseasekksNo ratings yet
- Determinants of Public HealthDocument6 pagesDeterminants of Public HealthMissy OrgelaNo ratings yet
- Exercise - Physical Activity in Individuals With Type 2 Diabet... - Medicine & Science in Sports & ExerciseDocument51 pagesExercise - Physical Activity in Individuals With Type 2 Diabet... - Medicine & Science in Sports & ExerciseRicardo Arellano GarcíaNo ratings yet
- PHD Thesis Metabolic SyndromeDocument5 pagesPHD Thesis Metabolic Syndromejanchampagnefargo100% (2)
- Questionnaire Questions - ScrapDocument9 pagesQuestionnaire Questions - ScrapNaomi JohnsonNo ratings yet
- Week 4 & 5Document27 pagesWeek 4 & 5Ali HaiderNo ratings yet
- Heex4400aacvpr PhysiciansDocument24 pagesHeex4400aacvpr PhysiciansSuganya BalachandranNo ratings yet
- Tugas Pengganti Uts (Summary)Document12 pagesTugas Pengganti Uts (Summary)Uni TyasNo ratings yet
- Diabetes Educational Program in ElderlyDocument9 pagesDiabetes Educational Program in ElderlyJaveria KhawarNo ratings yet
- Health - Diabetes Research PaperDocument7 pagesHealth - Diabetes Research Paperapi-299727107No ratings yet
- Diabetes AAG 2011 508Document4 pagesDiabetes AAG 2011 508Shams HassanNo ratings yet
- Diabetes in SportsDocument11 pagesDiabetes in SportsstefanNo ratings yet
- The Problem and It'S Background: World Health OrganizationDocument26 pagesThe Problem and It'S Background: World Health OrganizationGio LlanosNo ratings yet
- Metabolic Syndrome: Pennington Biomedical Research CenterDocument17 pagesMetabolic Syndrome: Pennington Biomedical Research CenterJhay-arr HernandezNo ratings yet
- Diabetes No Atleta CompetitivoDocument7 pagesDiabetes No Atleta CompetitivojosiNo ratings yet
- Insulin TherapyDocument55 pagesInsulin TherapyShriyank BhargavaNo ratings yet
- Dissertation On Metabolic SyndromeDocument4 pagesDissertation On Metabolic SyndromeWhereToBuyResumePaperCanada100% (1)
- Dental Hygienists Against Heart DiseaseDocument26 pagesDental Hygienists Against Heart Diseaserajdeep_pavaskarNo ratings yet
- ANNALS-Diabetes Tipo IIDocument16 pagesANNALS-Diabetes Tipo IIewb100% (2)
- AGNG 320 Tak1Document8 pagesAGNG 320 Tak1mutiso mutieNo ratings yet
- Risk Factors: Tobacco UseDocument9 pagesRisk Factors: Tobacco UseLester Patalinghug BernardinoNo ratings yet
- Metabolic Syndrome - Symptoms, Diagnosis, and CausesDocument7 pagesMetabolic Syndrome - Symptoms, Diagnosis, and CausesdrmuratNo ratings yet
- Meeting the American Diabetes Association Standards of Care: An Algorithmic Approach to Clinical Care of the Diabetes PatientFrom EverandMeeting the American Diabetes Association Standards of Care: An Algorithmic Approach to Clinical Care of the Diabetes PatientNo ratings yet
- Dodging Diabetes ComplicationsDocument20 pagesDodging Diabetes ComplicationsUlises MatiasNo ratings yet
- CVD Effects of ExerciseDocument11 pagesCVD Effects of ExerciseAboobacker SabithNo ratings yet
- Obesity Care in DiabetsDocument1 pageObesity Care in DiabetsTanzer BalkırNo ratings yet
- Fitness and DiseaseDocument25 pagesFitness and Diseaseapi-309742389No ratings yet
- Type 1 Delay Living Update Press Release - FinalDocument2 pagesType 1 Delay Living Update Press Release - FinalMelchor Alcántara BarreraNo ratings yet
- DR KessyDocument8 pagesDR KessyAnitha OnesmoNo ratings yet
- Abstract 1AND2 SetDocument11 pagesAbstract 1AND2 Setmarina20240015829No ratings yet
- High Blood Pressure and Cholesterol: 39 1 in 2 2 in 3Document4 pagesHigh Blood Pressure and Cholesterol: 39 1 in 2 2 in 3annyzaukNo ratings yet
- Weight Management Program 2015Document14 pagesWeight Management Program 2015api-284569489No ratings yet
- Heart Disease and Stroke Scientific ReviewDocument6 pagesHeart Disease and Stroke Scientific Reviewapi-371380624No ratings yet
- Disease Diabetes Health ArticlesDocument3 pagesDisease Diabetes Health ArticlesarmanNo ratings yet
- Coronary Artery Disease Cad2Document182 pagesCoronary Artery Disease Cad2Mamot Mot0% (1)
- DiabetesDocument8 pagesDiabetessahakumarsayanNo ratings yet
- Prevention: Can Prediabetes, Type 2 Diabetes and Gestational Diabetes Be Prevented?Document9 pagesPrevention: Can Prediabetes, Type 2 Diabetes and Gestational Diabetes Be Prevented?BethChay LacsonNo ratings yet
- Harmonizing The Metabolic SyndromeDocument7 pagesHarmonizing The Metabolic SyndromeCarlos_RuedasNo ratings yet
- Term Paper DiabetesDocument8 pagesTerm Paper Diabetesea5zjs6a100% (1)
- AAA_Type_2_Diabetes_Annals_of_Internal_MedicineDocument19 pagesAAA_Type_2_Diabetes_Annals_of_Internal_MedicineCelebfan BoyNo ratings yet
- Chair Master-Exercise-Instructor-Manual-with-pictures PDFDocument64 pagesChair Master-Exercise-Instructor-Manual-with-pictures PDFonix2000100% (1)
- E147 Full PDFDocument21 pagesE147 Full PDFcahyatiNo ratings yet
- Dissertation On Diabetes Type 2Document4 pagesDissertation On Diabetes Type 2PaperWritingHelpCanada100% (1)
- Misclassification of Cardiometabolic Health When Using Body Mass Index Categories in NHANES 2005-2012Document5 pagesMisclassification of Cardiometabolic Health When Using Body Mass Index Categories in NHANES 2005-2012Maria Ignacia MacariNo ratings yet
- Insurance: Vivek College of CommerceDocument26 pagesInsurance: Vivek College of CommerceprasadNo ratings yet
- Diabetes Mellitus by DR RelliqueteDocument5 pagesDiabetes Mellitus by DR RelliqueteKenneth Jed M. RobentaNo ratings yet
- Diabetes Knowledge TestDocument1 pageDiabetes Knowledge TestNadira Farah PrayogoNo ratings yet
- Diabetis-Metabolic DisordersDocument358 pagesDiabetis-Metabolic DisordersHampson MalekanoNo ratings yet
- DM Guidelines CCPDocument87 pagesDM Guidelines CCPfuad20No ratings yet
- Nursing ProcessDocument12 pagesNursing ProcessArif AshariNo ratings yet
- Short Guide Clinical NutritionDocument30 pagesShort Guide Clinical Nutritiontopiq100% (1)
- Health Tips For Ramad - 1Document9 pagesHealth Tips For Ramad - 1Syahrizul Fadly MadelliNo ratings yet
- Pone 0163350Document14 pagesPone 0163350alifandoNo ratings yet
- Dka 31-05-11Document52 pagesDka 31-05-11Hussain AzharNo ratings yet
- FORA G31 Manual EngDocument48 pagesFORA G31 Manual EngAdriana IacobNo ratings yet
- Section 504 Plan: Form 4 St. Michael-Albertiville Public SchoolsDocument10 pagesSection 504 Plan: Form 4 St. Michael-Albertiville Public Schoolsapi-314180367No ratings yet
- Clinical Chemistry Review NotesDocument54 pagesClinical Chemistry Review NotesALEONA AMON ARANTENo ratings yet
- TeneligliptinDocument17 pagesTeneligliptintarun956519No ratings yet
- Surya VigyanDocument41 pagesSurya Vigyanpradeepnagda100% (2)
- AdknowlDocument21 pagesAdknowlBie JhingcHayNo ratings yet
- Diabetes Management: OverviewDocument20 pagesDiabetes Management: Overviewlaloo01No ratings yet
- UntitledDocument1 pageUntitledapi-134347145No ratings yet
- Crossfit NutritionDocument16 pagesCrossfit Nutritionscribd94100% (1)
- Self Efficacy Theory - Case StudiesDocument13 pagesSelf Efficacy Theory - Case StudiesPetros Akin-Nibosun0% (1)
- Pathophysiology of DiabetesDocument3 pagesPathophysiology of DiabetesJeffrey Ramos GironNo ratings yet
- Enzymes Questions For AQA AS BiologyDocument67 pagesEnzymes Questions For AQA AS Biologyjames75% (4)
- Blood Sugar TestDocument4 pagesBlood Sugar TestanisyaNo ratings yet
- DM DR Osama Mahmoud PDFDocument27 pagesDM DR Osama Mahmoud PDFRaouf Ra'fat Soliman100% (1)
- Part I - Sample Questions: COMPETENCY 1: Patient CareDocument20 pagesPart I - Sample Questions: COMPETENCY 1: Patient CareAbdallah ElmenshawyNo ratings yet
- Invisible Minerals Part II by DR Carolyn DeanDocument46 pagesInvisible Minerals Part II by DR Carolyn Deanlihu74100% (1)
- NCP DM 1Document6 pagesNCP DM 1Shin AblangNo ratings yet
- Diabetes FreeDocument166 pagesDiabetes FreeTerry D Barone100% (1)
- NAT Reviewer in EnglishDocument9 pagesNAT Reviewer in Englishleomille250% (2)
ACSM Diabetes
ACSM Diabetes
Uploaded by
jrice003Original Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
ACSM Diabetes
ACSM Diabetes
Uploaded by
jrice003Copyright:
Available Formats
IN THIS ISSUE
News You Need Diabetes Mellitus: An Overview Overview of Type 2 Diabetes Type 1 Diabetes and Exercise Coaching News Avoiding Possible Interactions Between Exercise and Diabetic Medications Self-Tests 1 1 3 5 7 8 11
ACSMs
Certified News
JULY-SEPTEMBER 2007 VOLUME 17, ISSUE 3
News You Need
Certification Updates
Summer 2007
by: Mike Niederpruem, National Director of Certification and Registry Programs
Diabetes Mellitus: An Overview
Larry S. Verity, Ph.D., FACSM, Professor of Exercise Physiology, School of Exercise & Nutritional Sciences, San Diego State University As an overview, diabetes mellitus is a group of diseases marked by elevated blood glucose levels resulting from defects in insulin production, insulin action, or both. Overall, diabetes can lead to serious complications and premature death, yet those with Diabetes can take action to control their disease and lower their risk of complications. In the United States, the prevalence of diabetes is about 20.8 million people1,2. The significance and burden of diabetes towards the heath care system is reflected in the following1,2: Diabetes is one of the most common chronic diseases affecting people in the United States. More than 1.5 million new cases are diagnosed annually. Diabetes has a major impact on the health of the U.S. population. It is the leading cause of new blindness, endstage renal disease, and nontraumatic amputations in adults. Direct medical costs and indirect costs of diabetes total $132 billion annually (based on 2002 estimates). Sixth leading cause of death in U.S. (fifth leading cause of death for women) Overall, the risk of death among people with diabetes is about twice that of people without diabetes of similar age. Cardiovascular disease 2 to 4-fold in cardiovascular disease About 73 percent of adults with diabetes have a blood pressure greater than or equal to 130/80 mm Hg
Diabetes Mellitus... Continued on Page 2
ACSMs Committee on Certification and Registry Boards, 2006-07 Milestones
Each year, the ACSM Committee on Certification and Registry Boards (CCRB) provides an annual update on CCRB activity at a public colloquium that takes place during the ACSM Annual Meeting. There is always great news to share, and this year in New Orleans was no exception. As a result of all the hard work of our CCRB volunteers over the last year, here are a few of our accomplishments: Achieved Successful Accreditation from the National Commission for Certifying Agencies (NCCA) ACSM Certified Personal TrainerSM ACSM Health/Fitness Instructor ACSM Exercise Specialist ACSM Registered Clinical Exercise Physiologist Released the Following New Publications ACSMs Resources for the Personal Trainer, Second Edition ACSMs Health/Fitness Facility Standards and Guidelines, Third Edition ACSMs Health-Related Physical Fitness Assessment Manual, Second Edition ACSMs Metabolic Calculations Handbook, First Edition Established Partnership with National Intramural-Recreational Sports Association (NIRSA) Launched the ACSM Club Connection Program Developed a Free Interactive Exam Tutorial Completed Successful Job Task Analyses for All Certification Programs Launched a New CEC course: Behavior Change Strategies for Optimal Client Outcomes
News You Need... Continued on Page 12
In this themed issue of ACSMs Certified News, experts provide an overview and recommendations for fitness practitioners to improve awareness and development of exercise programs for those with Type 1 and Type 2 Diabetes. Marialice Kern, Ph.D., addresses exercise recommendations for Type 1 Diabetes Mellitus (T1DM), while Larry S. Verity, Ph.D., reviews exercise recommendations for Type 2 Diabetes Mellitus (T2DM). Lastly, Sheri Colberg-Ochs, Ph.D., highlights the interaction of exercise with common diabetes medications. Each of these three authors are professionals in the field of diabetes and have lived with T1DM for 25 years or more.
ACSMs Certified News
AMERICAN COLLEGE OF SPORTS MEDICINE | (317) 637-9200
ACSMS CERTIFIED NEWS
EDITORS Paul Sorace, M.S. Larry S. Verity, Ph.D., FACSM
COMMITTEE CHAIR Dino Costanzo, M.A., FACSM CCRB PUBLICATIONS SUBCOMMITTEE CHAIR Jonathan N. Myers, Ph.D., FACSM ADMINISTRATION PRESIDENT Robert E. Sallis, M.D., FACSM PUBLICATIONS COMMITTEE CHAIR Jeffrey L. Roitman, Ed.D., FACSM EXECUTIVE VICE PRESIDENT James R. Whitehead NATIONAL CENTER NEWSLETTER STAFF NATIONAL DIRECTOR OF CERTIFICATION AND REGISTRY PROGRAMS Mike Niederpruem ASSISTANT DIRECTOR OF CERTIFICATION Hope Wood MANAGER, CERTIFICATION PROGRAMS Traci Rush CERTIFICATION PROGRAM COORDINATOR Beth Muhlenkamp
Diabetes Mellitus... Continued from Page 1
Leading cause of: Non-traumatic amputations (82,000/ year or 224/day) More than 60 percent of nontraumatic lower-limb amputations occur in people with diabetes. Blindness (~20,000/year or 60/day) End stage renal disease (38,000/year or 104/day) Neural Defects: About 60-70 percent of people with diabetes have mild to severe forms of nervous system damage. Almost 30 percent of people with diabetes aged 40 years or older have impaired sensation in the feet (i.e., at least one area that lacks feeling). Based on these disease-related consequences of diabetes, it is imperative for health fitness practitioners to understand exercise risks, benefits, and precautions for those with diabetes. Although there are three main types of Diabetes Mellitus1, we focus only on T1DM and T2DM in this issue. Gestational Diabetes Mellitus (GDM) is not addressed; however, many GDM strategies align closely with those for T2DM. Briefly, T1DM develops when the bodys immune system destroys insulin-producing cells that regulate blood glucose. To survive, people with T1DM must have insulin delivered by injection or a pump, while some do use inhaled insulin. This form of diabetes usually strikes children and young adults, although disease onset can occur at any age. T1DM accounts for 5-10 percent of all diagnosed cases of diabetes1. Risk factors for T1DM may be autoimmune, genetic, or environmental. Presently, there is no known way to prevent T1DM, even though there are known biologic markers increasing risk for T1DM. T2DM is the most common form of diabetes and accounts for about 90-95 percent of all diagnosed cases1. It usually begins as insulin resistance, a disorder in which insulin receptor sites on the target cell are impaired.
As the need for insulin rises, the pancreas gradually loses its ability to produce it. T2DM is associated with older age, obesity, family history of diabetes, history of GDM, impaired glucose metabolism, physical inactivity, and race/ethnicity. Moreover, T2DM in children and adolescents is more commonly diagnosed, particularly in American Indians, African Americans, and Hispanic/Latino Americans. Treating diabetes requires timely medication(s) use, proper nutrition, and regular physical activity/exercise to aid in regulating blood glucose. Diabetes self-management education (DMSE) is an integral component of medical care, especially routine glucose monitoring, which aids in glucose control and benefits both T1DM and T2DM. To avoid acute risks of exercise (e.g., high or low blood glucose), it is strongly recommended that blood glucose monitoring be performed before/after each exercise/physical activity session. Health fitness practitioners need to know the role of exercise in diabetes risks, benefits, and precautions. Overall, if a client with diabetes does not have disease-related complications (e.g., heart and vessel, eye, kidney, or nerve), then the recommendations put forth in this themed issue are prudent for the health fitness practitioner. If there are known complications, physician-directed exercise and/or physical activity planning and development is warranted.
PROFESSIONAL EDUCATION COORDINATOR Gretchen Dovenmuehle DIRECTOR OF PROFESSIONAL EDUCATION AND DISTANCE LEARNING Karen J. Pierce ASSISTANT EXECUTIVE VICE PRESIDENT, GROUP PUBLISHER D. Mark Robertson SENIOR DIRECTOR OF PUBLICATIONS AND MARKETING Jeff Richardson PUBLICATIONS MANAGER David Brewer FOR MORE CERTIFICATION RESOURCES CONTACT THE ACSM CERTIFICATION RESOURCE CENTER: 1-800-486-5643 INFORMATION FOR SUBSCRIBERS CORRESPONDENCE REGARDING EDITORIAL CONTENT SHOULD BE ADDRESSED TO: Certification & Registry Department E-mail: certification@acsm.org Tel.: (317) 637-9200, ext. 121 CHANGE OF ADDRESS OR MEMBERSHIP INQUIRIES MEMBERSHIP AND CHAPTER SERVICES TEL.: (317) 637-9200, EXT. 139 OR EXT. 136. ACSMs Certified News (ISSN# 1056-9677) is published quarterly by the American College of Sports Medicine Committee on Certification and Registry Boards (CCRB). All issues are published electronically and in print. The articles published in ACSMs Certified News have been carefully reviewed, but have not been submitted for consideration as, and therefore are not, official pronouncements, policies, statements, or opinions of ACSM. Information published in ACSMs Certified News is not necessarily the position of the American College of Sports Medicine or the Committee on Certification and Registry Boards. The purpose of this newsletter is to inform certified individuals about activities of ACSM and their profession and about new information relative to exercise and health. Information presented here is not intended to be information supplemental to the ACSMs Guidelines for Exercise Testing and Prescription or the established positions of ACSM. ACSMs Certified News is copyrighted by the American College of Sports Medicine. No portion(s) of the work(s) may be reproduced without written consent from the Publisher. Permission to reproduce copies of articles for noncommercial use may be obtained from the Rights and Permissions editor. ACSM NATIONAL CENTER
References
1. American Diabetes Association: Standards of Medical Care in Diabetes: Position Statement. Diabetes Care, 30 (suppl 1):S4S41, 2007. 2. U.S. Centers for Disease Control and Prevention. National diabetes fact sheet: general information and national estimates on diabetes in the United States, 2005. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2005.
SELF-TEST ANSWER KEY FOR PAGE 11 QUESTION 1 2 3 4 5 TEST #1: C B B A C TEST #2: B D D A E TEST #3: A A E B D
401 WEST MICHIGAN ST. INDIANAPOLIS, IN 46202-3233. TEL.: (317) 637-9200 FAX: (317) 634-7817
2007 American College of Sports Medicine. ISSN # 1056-9677
JULY/AUGUST/SEPTEMBER 2007 | VOLUME 17; ISSUE 3
ACSMs Certified News
Overview of Type 2 Diabetes
Larry S. Verity, Ph.D., FACSM Professor of Exercise Physiology School of Exercise & Nutritional Sciences San Diego State University cose in the liver and skeletal muscle12,16. Reduced insulin receptor binding at target tissues and impaired post-binding activities related to intracellular insulin action result in insulin resistance. Interestingly, these abnormalities are reversible with weight loss, diet, and physical activity12. Elevated blood glucose, or hyperglycemia in T2DM suggests that insulin release is inadequate to compensate for the insulin resistance. At diagnosis, T2DM have significantly elevated levels of insulin, which contributes to insulin resistance. Over time, the pancreas loses its ability to produce insulin, and the need for exogenous insulin to control blood glucose increases. Thus, T2DM is a progressive disease occurring in a gradual succession of stages of increasing glucose intolerance and insulin resistance6. Onset of T2DM is associated with genetic, environmental, and cultural factors5. The risk of disease rises with family history, age, obesity, and inactivity7,9. About 80 percent of adults with T2DM are obese and physically inactive, both of which are related to increased insulin resistance6. Lifestyle interventions focusing on weight loss and physical activity are essential strategies to not only manage glucose levels and lessen the onset of disease-related complications, but also to prevent the onset of T2DM1,11,12. Moreover, aggressive lifestyle intervention can actually reduce the amount of medication (e.g., oral drugs and exogenous insulin) required to manage T2DM. Blood glucose control for T2DM is crucial in managing the disease and lessening the onset of cardiovascular disease and diabetesrelated complications (DRCs)4. Because diabetics are two to four times more likely than nondiabetics to suffer a fatal heart attack or stroke6,7, the health fitness practitioner should ensure that their client with T2DM monitors his/her blood glucose and manages CVD risk factors. Overall glycemic control is routinely assessed using glycosylated hemoglobin (A1c). A1c gives a measure of average glucose over the preceding two to three months and the goal for diabetes from the American Diabetes Association (ADA) is to have an A1c value < 7.0 percent6; however, the American Association of Clinical Endocrinologist (AACE) has recommended an A1c value <6.5 percent .
Type 2 Diabetes Mellitus (T2DM) is a significant health burden in the United States due to increased morbidity and mortality associated with macrovascular and microvascular diabetes complications9. The rate of growth in T2DM both nationally9 and globally10 is projected to double by 2050 and 2025, respectively. One in three people born in the United States in 2000 are projected to develop diabetes in their lifetime13. While the prevalence of T2DM is common among all elderly and obese, selected minority and ethnic groups are disproportionately affected6,8,9. Moreover, persons with diabetes suffer disproportionately from physical and cognitive disability9. Usually, T2DM afflicts adults over 30 years and is directly related to co-existing conditions, such as obesity, hypertension, dyslipidemia, and insulin resistance6,7. Alarmingly, the incidence of T2DM in children and adolescents has significantly increased over the past 20 years, presumably related to increased levels of obesity secondary to excess caloric intake and too little caloric expenditure6. About 85 percent of children diagnosed with T2DM are overweight or obese at diagnosis5. The inextricable relationship between T2DM and obesity in adults and youth has prompted the development of the term Diabesity which is trademarked by Shape Up America. Diabesity refers to the link between obesity and T2DM the most prevalent form of diabetes in America14. Although T2DM displays varying degrees of insulin production (e.g., normal or elevated), the disease is characterized by insulin resistance. Insulin resistance is considered a peripheral defect because of a decrease in insulin-mediated uptake and storage of glu-
In addition to elevated blood glucose, multiple co-existing risk factors for heart disease are typically present in T2DM including obesity, hypertension, dyslipidemia, and physical inactivity6,8. Obesity predominates in T2DM with body mass index (BMI) often exceeding 30 kgm2 and abdominal girth being quite large. This type of morphology places many with T2DM at high risk for heart disease and cancer5,8. Therefore, weight loss is a primary treatment goal to improve insulin action in persons with T2DM6,7,8. The primary goal of therapy for all diabetics focuses on Diabetes Self Monitoring Education (DSME) and Self Blood Glucose Monitoring (SBGM) to achieve acceptable blood glucose control (HbA1c < 7.0 percent) based upon ADA guidelines, thereby limiting the development and progression of diabetesrelated complications6. Persons with T2DM show reduced risk for retinopathy, nephropathy, and neuropathy with intensive therapy and the potential for a reduction of cardiovascular disease with improved glycemic control4. Glycemic control is best achieved through DSME and SBGM combined with nutrition, adjustment of diabetes medications, and regular physical activity6,15. Cardiovascular risk factors, along with symptomatic and asymptomatic coronary heart disease, are far too common in T2DM6,7,8. Recently, a call to action was put forth by the ADA and AHA to prevent cardiovascular disease and diabetes8. Diagnosis of macrovascular disease and co-morbid conditions of diabetes coupled with aggressive intervention is crucial in minimizing progression of this disease8.
Table 1: Indications For Stress Testing with Diabetes6,15
Known or suspected cardiovascular disease (e.g., CAD, PAD) Age > 35 years Age > 25 years if duration of diabetes > 10 years for type 2 or > 15 years for type 1 Presence of any additional risk factors for cardiovascular disease Microvascular disease Proliferative retinopathy Nephropathy, including microalbuminuria Peripheral Vascular Disease Autonomic neuropathy
CAD = coronary artery disease; PAD = peripheral arterial disease
Pre-Activity Screening
A thorough pre-activity screening of the patients clinical status is recommended to ensure safe and effective participation1,2,11,15. Before commencing exercise, prudent screening for vascular and neurological complications, including silent ischemia, are warranted, along with identification of the presence of cardiovascular disease risk factors15. Coexisting morbidities in the diabetes health profile are important for the health fitness
Type 2 Diabetes... Continued on Page 4
ACSMs Certified News
AMERICAN COLLEGE OF SPORTS MEDICINE | (317) 637-9200
practitioner to determine whether the client status is acceptable for safely engaging in exercise and to determine the need for monitoring of each session. Use of the PAR-Q and PARMedX questionnaires are helpful screening tools for the health fitness practitioner to ensure medical oversight in evaluating the clients health profile. Persons with diabetes are stratified in the high-risk category, according to recommended guidelines3, and a stress test is strongly advised before initiating moderate to vigorous exercise irrespective of the patients cardiac risk profile3,6,15. Specific indications for a stress test to be administered include the presence of one or more of the criteria shown in Table 1.6,15
Table 2: Comparing Aerobic and Resistance Training Recommendations for Type 2 Diabetes
Aerobic Training Recommendations GETP7 - Diabetes Current Type 2 Diabetes Recommendations 3-7 days/week 40-60% HRR* > 60% HRR** > 150 minutes/week* > 90 minutes/week** aerobic Resistance Training Recommendations ACSM Position Stand (2000) > 2 days/week 10-15 repetitions 8-10 exercises > 1 set per exercise Current Type 2 Diabetes Recommendations > 3 days/week 8-10 repetitions > 8 exercises up to 3 sets per exercise
Frequency Intensity Time Type or Mode
3-4 days/week 50-80% HRR 20-60 minutes aerobic
*Moderate intensity; ** Vigorous intensity
Exercise: Benefits for Type 2 Diabetes
The benefits of regular exercise for T2DM are significant and over the past 20 years the powerful role of exercise and physical activity has become more fully appreciated in treating and preventing T2DM1,2,12,15,16. The molecular understanding of exercise in relation to T2DM is evolving, as is knowledge regarding the optimal mode, frequency, and duration of exercise to treat and prevent this disorder1,2,6,1115. In addition, there is a growing appreciation for the role of aerobic exercise, as well as resistance training, in T2DM1,6,15. Although DRCs have been the premise to discourage exercise participation, there are a variety of activities that allow for safe exercise in a supervised setting to oversee diabetes and DRCs. Individualized exercise training needs to be an integral part of the treatment plan for the management of T2DM. It is important for the health fitness practitioner to ensure the development of a safe and effective program for the client with T2DM through physician interaction.
Exercise Program for Type 2 Diabetes:
Current exercise recommendations for T2DM attempt to enhance the volume of weekly aerobic physical activity, along with increasing the quantity and quality of resistance training sessions6,15. These recommendations address important outcomes aimed at improved glucose management, reduced heart disease risk, and favorable psychoemotional changes that lessen/delay progression of the disease. Proper precaution of exercise participation is prudent with T2DM clientele, especially, monitoring blood glucose before/after exercise. Finally, the recommendations put forth in this article are limited to persons with T2DM who do not have DRCs. If DRCs are part of a clients health profile, it is important for the health fitness practitioner to have medical oversight in developing a safe and effective exercise program for those with T2DM, and maybe recommend clinical supervision for safe participation.
The aerobic exercise recommendations presented in ACSMs Guidelines for Exercise Testing and Prescription, Seventh Edition. (GETP7) for all diabetes needs to be modified to meet specific needs of the client with T2DM3. As presented in Table 2, the FITT recommendations in GETP7 are compared with current recommendations for T2DM3,15. The more current aerobic activity is recommended not only to improve glucose metabolism and glucose control, but also to aid in weight management and cardiovascular risk prevention6,15. Coupled with obesity, health fitness professionals should strive to have their client with T2DM achieve at least 150 minutes of moderate intensity physical activity each week, and may need to increase the amount of time in physical activity/resistance training to aid in weight management15. In addition to aerobic exercise, resistance training is strongly recommended for T2DM. In recent years, many studies have examined the benefits, effectiveness, and safety of resistance training in T2DM. The current guidelines (see Table 2) recommend that resistance training be performed up to three times per week for clients with T2DM6,15. Moreover, eight or more exercises should be included in this training with eight to ten repetitions (e.g., 8-10 RM) of each exercise performed per set, while the number of sets should progress from one to three. Most importantly, health fitness practitioners must supervise and assess their clients with T2DM to ensure the proper safety, progression, and effectiveness of the training program. Irrespective of aerobic or resistance training, the health fitness practitioner should design an exercise program to accommodate the clinical status of the patient\client and specify the type and intensity of activity as well as duration and frequency. In summary, the health fitness practitioner can safely and effectively accomplish exercise program development for T2DM. It is important to consider current health and DRC status before physical activity participation. Participation in physical activity affords critical benefits for those with T2DM, while health fitness practitioners need to keep close
scrutiny over the intensity of the exercise program to yield both safe and effective outcomes for this clientele.
References
1. Albright, A., M. Franz, G. Hornsby, A. Kriska, D. Marrero, I. Ulrich, and L.S. Verity. American College of Sports Medicine. Exercise and Type 2 Diabetes. Position Stand. Medicine & Science in Sports & Exercise, 32:13451360, 2000. 2. American College of Sports Medicine and American Diabetes Association. Diabetes Mellitus and Exercise: A joint position statement of the American College of Sports Medicine and The American Diabetes Association. Medicine & Science in Sports & Exercise, 29:ivi, 1997. 3. American College of Sports Medicine. ACSMs Guidelines for Exercise Testing and Prescription, 7th ed. Philadelphia:Lippincott, Williams & Wilkins, 2006. 4. American Diabetes Association: Implications of the United Kingdom Prospective Diabetes Study: Position Statement. Diabetes Care, 26(suppl 1):S28S32, 2003. 5. American Diabetes Association (2000). Type 2 diabetes in children and adolescents (Consensus Statement, 2000). Diabetes Care, 23(3): 381389. 6. American Diabetes Association: Standards of Medical Care in Diabetes: Position Statement. Diabetes Care, 30 (suppl 1):S4S41, 2007. 7. Centers for Disease Control and Prevention. National diabetes fact sheet: general information and national estimates on diabetes in the United States, 2005. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, 2005. 8. Eckel, R.H., R. Kahn, R.M. Robertson, and R.A. Rizza. Preventing Cardiovascular Disease and Diabetes: A Call to Action From the American Diabetes Association and the American Heart Association. Circulation, 113:2943-2946, 2006. 9. Engelgau, M.M., L.S. Geiss, J.B. Saaddine, J. Boyle, S. Benjamin, E. Gregg, E.Tierney, N. Rios-Burrows, A.H. Mokdad, E.S. Ford, G. Imperatore, and K. Venkat Narayan. The Evolving Diabetes Burden in the United States. Annals of Internal Medicine, 140(11):945-950, 2004. 10. Green, A., N.C. Hirsch, and S.K. Pramming. The Changing World Demography of Type 2 Diabetes. Diabetes/Metabolism Research and Reviews, 19:3-7, 2003. 11. Hornsby W.G. and A.L. Albright. Diabetes (pp. 13341). In: ACSMs Exercise Management for Persons with Chronic Disease and Disabilities, 2nd ed., Durstine L and G Moore (Editors), Champaign, IL: Human Kinetics; 2003. 12. Ivy, J.L., T.W. Zderc, and D.L. Fogt (1999). Prevention and Treatment of Non-Insulin Dependent Diabetes Mellitus. (pp. 135). In: Exercise and Sport Science Reviews, vol. 27, J.O. Holloszy (Editor). Lippincott Williams & Wilkins: Philadelphia, PA. 13. Narayan, K.M., J. Boyle, T. Thompson, S.W. Sorensen, and D. F. Williamson. Lifetime Risk for Diabetes Mellitus in the United States. Journal of the American Medical Association, 290:1884-1890, 2003. 14. Shape Up America! Healthy Weight For Life [http://www.shapeup.org/prof/diabesity.php] 15. Sigal, R.J., G.P. Kenny, D.H. Wasserman, and C. CastanedaSceppa. Physical Activity/Exercise and Type 2 Diabetes: Technical Review. Diabetes Care, 27 (10): 2518-2539, 2004. 16. Riddell M.C., N. Ruderman, M. Berger, and M. Vranic: Exercise physiology and diabetes: From antiquity to the age of the exercise sciences (pp. 315). In: Handbook of Exercise in Diabetes, 2nd ed., Ruderman N, J Devlin, S Schneider, and A Kriska,(Editors). Alexandria, VA: American Diabetes Association; 2002.
JULY/AUGUST/SEPTEMBER 2007 | VOLUME 17; ISSUE 3
ACSMs Certified News
Type 1 Diabetes and Exercise
Marialice Kern, Ph.D., FACSM, Professor of Exercise Physiology, San Francisco State University
Introduction
Between Type 1 Diabetes Mellitus (T1DM) and Type 2 Diabetes Mellitus (T2DM), T1DM is significantly less prevalent8. T1DM, formerly known as juvenile onset or insulin dependent, afflicts more than one million people in the United States. Though the clinical symptoms for both types are the same (polyuria (excessive urination), polydipsia (excessive drinking/thirst), polyphagia (excessive eating/hunger), blurred vision and/or weight loss), disease etiology for T1DM is based on an autoimmune disorder which results in the destruction of the beta ()-cells of the pancreas8. These cells produce insulin, an anabolic hormone which is necessary for life. Because T1DM lacks insulin production, this hormone must be taken via subcutaneous injection using either a needle (usually several shots/day) or an insulin-pump (continuous insulin infusion, with bolus amounts given with meals). The quantity of insulin each person with T1DM must take per day is dependent on their sensitivity to insulin, and this sensitivity can change significantly depending on an individuals exercise habits. It is important that exercise professionals understand the pathology of diabetes and possible complications, and benefits that are associated with exercise in T1DM if they are going to properly prescribe an exercise program which will help the T1DM have a better quality of life.
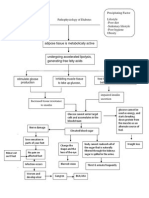
Pathological Physiology of Diabetes
The symptoms and complications associated with T1DM can be attributed to a lack of circulating insulin: (a) decreased utilization of glucose by the body cells, resulting in high blood glucose, (b) increased mobilization and use of fats, resulting in ketoacidosis, and (c) depletion of amino acids. For T1DM, the primary defect is inadequate insulin secretion secondary to progressive destruction of pancreatic -cells via an autoimmune process. There is clinical evidence suggesting that individuals who develop with T1DM are genetically predisposed to this -cell destruction5. This evidence is several fold. At the time of diagnosis, the presence of anti-insulin and antiislet cell antibodies is seen in the blood, along with the presence of inflammatory cells around the islets. T-lymphocytes are also activated. Genes located on chromosome 6, the HLA (Human Leukocyte Antigens) genes, help the immune system to distinguish between ones own cells and foreign cells. There are many different alleles (copies) of the HLA genes. The genetic risk of inheriting T1DM is explained in over 50 percent of the cases by the presence of the genes HLA-DR, HLA-DQ, and HLA-DP10. Specifically, in the general population, only 50 percent of the population inherits a copy of the DR genes DR3 and DR4, and less than three percent have two alleles. But, in
T1DM, at least one allele of DR3 or DR4 is found in 95 percent of caucasians, with the prevalence of developing T1DM even higher if the individual has both DR3 and DR412. Persons with T1DM also have a higher incidence of other known autoimmune diseases (arthritis, Addisons, Hashimoto thyroiditis, and multiple sclerosis)5. Symptoms of T1DM will occur when 80 to 90 percent of the -cell mass is destroyed8. The lack of insulin results in several intracellular abnormalities in both muscle and liver such as excessive hepatic glucose production, decreased muscle glucose uptake, and glucose intolerance11. When insulin is secreted from the pancreas, it is dumped into the venous effluent, where it directly passes through the liver. Normally, 50 percent of the insulin is removed from the circulation on this first pass. If there is no insulin being secreted, there is no cap on the insulin counter-regulatory hormones: glucagon, catecholamines, growth hormone, and glucocorticoids. This results in an increase in hepatic glucose output and a decreased extraction of glucose from the blood by the periphery. If the liver is dumping glucose, and the skeletal muscle is not able to take that glucose inside the cell, high blood glucose levels develop and continue to increase. This is uncontrolled diabetes, and, in its worse form, results in dehydration, loss of acid-base balance, circulatory shock and death. Without the help of insulin, glucose does not diffuse easily across cell membranes. High concentrations of glucose cause a fluid shift as the body tries to equalize the osmotic pressure between the intracellular and extracellular fluid. Both intracellular and extracellular fluids are lost in uncontrolled diabetes. Increased osmotic pressure in the extracellular fluid (where there is a high concentration of glucose) results in a shift of water from the intracellular fluid to the extracellular fluid. When blood glucose levels are greater than ~ 180 mg/dl, glucose spills into the urine7. Extracellular fluid is lost by water following the glucose in the urine (osmotic diuresis). This is due to the osmotic effect of glucose in the renal tubules which greatly decreases tubular reabsorption of water by the kidneys, causing cellular dehydration11. At this point in time, the body is sensing starvation, and shifts its fuel source from glucose to fat and protein. Increased fat metabolism results in increased keto acid levels (acetoacetic and -hydroxybutyric) in the blood, creating diabetic ketoacidosis. When fats are supplying the primary fuel source, concentrations of ketone bodies (ketoacidosis) in the blood may increase tenfold or higher7. To compound the problem, ketone bodies have a low threshold for excretion by the kidneys, and because they are strong acids, they are partially neutralized by sodium ions from the
Type I Diabetes... Continued on Page 6
ACSMs Certified News
Type I Diabetes... Continued from Page 5
AMERICAN COLLEGE OF SPORTS MEDICINE | (317) 637-9200
extracellular fluid. These sodium ions are replaced with hydrogen ions, which make the blood even more acidic. If the mechanisms mentioned above continue for weeks to months, death can occur. First priority for the person with T1DM when admitted to the hospital in diabetic ketoacidosis (diabetic coma), is to normalize his/her electrolytes and bicarbonate stores which will restore the blood pH. This is more important than normalization of the blood glucose. We can see how this explains the previously mentioned symptoms! Polyuria: blood glucose higher than kidney threshold (usually ~180 mg/dl), glucose will spill into the urine. Polydipsia: tissue dehydration triggers the excessive thirst. Weight loss: body is wasting away (melting into the urine), increased fat metabolism and protein breakdown to supply the necessary intermediates to oxidize fat. Polyphagia: constant hunger, as the cells sense lack of fuel.
will help ensure that he/she will not exacerbate any preexisting complications by participating in an exercise program2.
Precautions
There are certain precautions which are helpful when advising an individual with T1DM on an exercise program. Always use adequate warm-up and cool-down periods; if neuropathy is present, avoid high impact activities; for weight bearing activities, wear footwear which is properly fitted, supportive and well cushioned; use proper hygiene, keeping feet dry and clean; and, most importantly, perform regular blood glucose monitoring. To help regulate the glycemic response to exercise several steps can be taken. Remember, everyone is different, and, depending upon how long the individual has had diabetes, how tight their glycemic control, and how well they know their bodys response to a given exercise bout, to a certain quantity of insulin, to a certain quantity of food, some of these recommendations may or may not be applicable2. 1. Metabolic Control Before Exercise Avoid exercise if fasting glucose is >250mg/dl and ketosis is present Use caution if glucose is > 300 mg/dl and no ketosis is present Ingest added carbohydrate if glucose is < 100 mg/dl 2. Blood glucose monitoring before and after exercise Identify when changes in insulin or food intake are necessary Learn the glycemic response to different exercise conditions 3. Food Intake Consume added carbohydrate as needed to avoid hypoglycemia Carbohydrate-based foods should be readily available during and after exercise Use these guidelines to help individuals with T1DM develop a personal history of his/her response. The best way to do this is to monitor blood glucose regularly and keep a written record. Overall, it is the individuals responsibility! The use of an exercise diary is very helpful. Record the blood glucose levels, the amount of insulin taken and when, time of day of usual exercise, what did the last meal consist of and when was it eaten, type of exercise and for how long, along with any special comments (i.e., blood sugar dropped three hours after exercise). The hope is that the individual with T1DM will gain information about his or her response to different activities and conditions and can use that information to plan meals and medications for upcoming activities. Hypoglycemia is most problematic in T1DM. Therefore, a record of the above mentioned parameters can be used to modify insulin regimen. Examples of insulin dose
Exercise and Type 1 Diabetes
Given the scenario depicted above, what are the benefits of maintaining a regular exercise program for persons with T1DM? Regular exercise allows the person with diabetes the same advantages seen in persons without diabetes (e.g., cardiovascular risk focus, metabolic improvements, body weight/fat management), plus a few more. The increase in sensitivity to insulin (needing less insulin to get the same effect), decrease in cardiovascular risk (lowering blood pressure, total cholesterol, increased HDL cholesterol) are common to both populations3. The effect of increased insulin sensitivity results in a decrease in the individuals insulin requirements. If the insulin intake is not decreased or additional carbohydrates (glucose) are not ingested, hypoglycemia may result either during the activity or in the hours following.
modifications are listed below4. 1. Inject > one hour before exercise 2. Decrease intermediate-acting insulin 3. Omit short-acting insulin before exercise 4. Decrease insulin pump setting when exercising around meal times 5. Inject insulin into non-exercising muscleabdominal is preferred These modifications, along with the availability of additional carbohydrates (as needed), should decrease the probability of a hypoglycemic reaction. If you notice the signs of hypoglycemia (trembling, rapid heart rate, profuse sweating, pale skin, confusion or disorientation, and jumbled, slow or slurred speech), give the individual some simple sugar. Many of these symptoms could just be due to a more intense exercise bout than usual, but with a person with T1DM , better to be safe than sorry. There is no reason why persons with T1DM should not be encouraged to participate in regular exercise and gain the benefits that all individuals, with or without diabetes, receive from daily exercise. Though precautions must be taken, through trial and error, the person with T1DM can learn to adjust their insulin dose appropriately. Insulin adjustments and the availability of simple carbohydrates will decrease the risk of a hypoglycemic incident.
References
1. American College of Sports Medicine: ACSMs guidelines for exercise testing and prescription, 7th ed. M.H. Whaley, P.H. Brubaker, R.M. Otto (eds). Philadelphia: Lippincott Williams & Wilkins, 2005. 2. American Diabetes Association: Clinical practice recommendations 2000: diabetes mellitus and exercise. Diabetes Care 23 (suppl 1):S50-S54, 2000. 3. Brooks, G.A., T.D. Fahey, and K.M. Baldwin. Exercise physiology: human bioenergetics and its applications. 4th ed. New York: McGraw-Hill, 2005. 4. Colberg, S.R. and D.P. Swain. Exercise and diabetes control: a winning combination. The Physician & Sports Medicine 28(4): 63-64, 69-72, 77-78, 81, 2000 5. Defranco, S., S. Bonissoni, F. Cerutti, et al. Defective function of Fas in patients with type 1 diabetes associated with other autoimmune diseases. Diabetes 50:483-488, 2001. 6. Devlin, J. Effects of exercise on insulin sensitivity in humans. Diabetes Care 15 (11):1690-1693, 1992. 7. Kitabchi, A. E., G. E. Umpierrez, M. B. Murphy, et al. Management of hyperglycemic crises in patients with diabetes. Diabetes Care 24:131-153, 2001. 8. National Institute of Diabetes and Digestive and Kidney Diseases. National Diabetes Statistics fact sheet: general information and national estimates on diabetes in the United States, 2005. Bethesda, MD: U.S. Department of Health and Human Services, National Institute of Health, 2005. 9. Pollock, M.L., G.A. Gaesser, J.D. Butcher, et al. The recommended quantity and quality of exercise for developing and maintaining cardiorespiratory and muscular fitness and flexibility in healthy adults. Medicine & Science in Sports & Exercise 30(6):975-991, 1998. 10. Todd J.A., J.I. Bell, H.O. McDevitt, et al. HLA-DQ beta gene contributes to susceptibility and resistance to insulin-dependent diabetes mellitus. Nature 329:599-604, 1987. 11. Widermaier, E.P., H. Raff, and K.T. Strang. Vanders human physiology: the mechanisms of body function. 10th ed. New York: McGraw-Hill, 2006. 12. Wolf, E., K.M. Spencer, A.G. Cudworth, et al. The genetic susceptibility to type 1 (insulin-dependent) diabetes: analysis of the HLA-DR association. Diabetologia 24:224-230, 1983.
Exercise Recommendations
Exercise recommendations for T1DM are no different than those without Diabetes1. ACSM recommends aerobic exercise (continuous, rhythmic, prolonged activities using the large muscle groups of the arms and/or legs) three to five days per week, for 20 to 60 minutes at 40 to 85 percent of heart rate reserve or 55 to 90 percent of heart rate maximum9. Resistance and flexibility training are recommended two to three days per week. If the person with T1DM is over 35 years old, or is over 25 years old and has had diabetes for more than 15 years, has any risk factors for coronary heart disease, autonomic neuropathy, or any microvascular disease (proliferative retinopathy or nephropathy), he/she should undergo a medical evaluation before beginning an exercise program. This
JULY/AUGUST/SEPTEMBER 2007 | VOLUME 17; ISSUE 3
ACSMs Certified News
Coaching News
Get out of sales and go fishing!
This is the sixteenth edition of the Coaching News column, sponsored by Wellcoaches Corporation in alliance with ACSM, and it appears regularly in ACSMs Certified News. Our thanks to Robert Rhode, Ph.D., for this title used in his presentation, Coaching Behavior Change Using Motivational Interviewing, at IHRSA 2007. What would happen to your personal training business if you stopped selling training and focused instead on helping your clients clarify their goals, motivations, and the value of becoming fit? Would your business wither or grow? My money is on growth. Im not suggesting that you stop charging for your services or that there is something shameful about selling. I am suggesting that a change in perspectivefrom selling to fishingwill help your clients clarify why they want to be fit and why they train with you. As a result, your clients are more likely to be intrinsically motivated and, therefore, more successful. They will also happily train with you for longer periods of time. So what is fishing and how do you do it? Let me answer this question through the lens of Motivational Interviewing (MI), an evidence-based methodology for helping people change behavior. MI is a client-centered, directive method for enhancing intrinsic motivation to change by exploring and resolving ambivalence.1 Lets explore this further. First, MIs focus is wholly on the client his/her agenda, motivations, perspective. To preserve this focus, its essential to fish for information beyond that needed to create an exercise prescription. Be curious and cultivate a beginners mindno assumptions. Ask questions like, What do you want to accomplish? If your training is successful, what would be different for you a year from now? What motivates you and what gets in your way? These open-ended questions generate thoughtful responses and reveal things about your clients that are important for you to know and use. Curiosity has another benefit as well. It assumes that your clients have the answers and that these answers are correct. Your
clients are, after all, the experts of their own lives and its important that you give them the freedom to completely speak their mind without judgment. What should you do when your client misunderstands the literature or chooses an action based on a popular exercise or nutrition myth? There is, after all, no shortage of diet du jour and fitness by celebrity programs. By all means, speak up if your clients choose goals that are unrealistic or prescriptions not supported by exercise science. Be aware, however, that how you speak up will make all the difference. When your client asks you to endorse something unscientific, harmful, or ineffective, go fishing. This is the perfect time to ask, What do you like about the diet? or, What attracted you to this particular exercise program? Questions like these respect your clients intelligence, are non-threatening, and will provide you with valuable information about your clients agenda and motivations. Once you have clarified whats important to your client, summarize the relevant information and ask permission to share your expertise: Now that I know you dont enjoy cardio exercise, how do you feel about creating a program that integrates shorter bouts of aerobic training with strength training? or I understand your reluctance to strength train because you dont want to develop bulky muscles. May I share with you some of the science that speaks to that concern? My clients always say, yes when I ask permission and I believe yours will as well. Secondly, MI proposes that change occurs naturally and fishing gives you an effective way to encourage this natural human propensity. To do this, listen for change talk. Statements that begin with I want to or I can or I started or I will or I need to give voice to your clients motivations and intention to act. And when you hear change talk, dont just sit there! Reflect it back to your client, reinforce it by asking for more information (Tell me more). Go fishing and keep the lure dangling where your client can see it! Reinforcing your clients change talk is important because people are more persuaded by what they hear themselves say than by what someone tells them.2 In other words, your clients will always be more motivated by what they say themselves than by what you tell them about your service or the promise of exercise. Third, MI assumes that ambivalence is a natural part of the change process. Therefore, dont ignore or diminish your clients ambivalence when you hear it. Instead, embrace it after all, change doesnt happen without it. Help your clients resolve their ambivalence by
amplifying the discrepancy between their present behavior and their goals. In other words, go fishing! When your client misses a workout, rather than reminding them that they cant achieve their goals without putting in the time, say instead: Im curious. How did it feel to not come to the club when you said you would? or What was great about giving yourself an unplanned day off from your workout? These questions are neutral in tone, respectful, non-judgmental, and appreciate that the client has choice about doing or not doing the healthy behavior. You can then ask, What would you do differently next time? or What did you learn? Questions like these help your clients clarify their motivations and reinforce their commitment to their goals. Both outcomes also strengthen the value of the work they do with you. In summary, if you fish effectively you can sell less. You create for your clients a richer training environment by encouraging them to hear their own change talk, explore their goals and motivations, and articulate for themselves all they receive from your service. In short, fishing gives your clients a powerful framework for success. And the greater your clients success, the greater is your reward personally and professionally. Go fishing!
About the Author
Heidi Duskey, MA is ACSM Health/Fitness Instructor Certified and certified wellness coach and has worked in the health club industry in management roles for the past 15 years. Heidi coaches privately, and conducts group coaching programs in a variety of wellness topics and walks the walk as a seasoned racewalker. Heidi can be reached at heidi@coach4zest.com
References
1. Miller, William R., Rollnick, S. (2002). Motivational Interviewing, Second Edition. New York: The Guilford Press. 2. Bem, D.J. (1972). Self-perception theory. In L. Berkowitz (Ed.), Advances in experimental psychology (Vol. 6, pp. 1-62). New York: Academic Press.
The Coaching News column is sponsored by Wellcoaches Corporation, the leader in health, fitness, and wellness coach training and delivery of wellness coaching services, in partnership with ACSM. To learn more about this topic or other topics on coaching health, fitness, and wellness, visit www.wellcoach.com.
ACSMs Certified News
AMERICAN COLLEGE OF SPORTS MEDICINE | (317) 637-9200
Avoiding Possible Interactions Between Exercise and Diabetic Medications
Sheri R. Colberg, Ph.D., FACSM, ACSM Exercise Test Technologist Certified, Associate Professor of Exercise Science, Exercise Science, Sport, Physical Education, and Recreation Department, Old Dominion University, Norfolk, Virginia
The presence of Diabetes Mellitus presents specific challenges with regard to effective maintenance of normal or near normal blood glucose levels before, during, and after physical activity. Given the many health benefits bestowed by exercise, though, it has been and continues to be an integral cornerstone of diabetes management. Certain prescribed medications, including some oral hypoglycemic and other diabetic medications, can affect the bodys metabolic response to exercise, however, frequently causing hypoglycemia (a blood glucose level of less than 70 mg/dl). In order to help diabetic individuals engage in regular exercise with a minimal risk of such potentially negative metabolic changes, it is important for health and fitness professionals to gain a better understanding of the actions of such medications and their potential glycemic effects.
Oral Hypoglycemic and Other Diabetic Medications
To date, there are Food and Drug Administration (FDA) approved oral Diabetic
medications available in six different classes, along with three injectable ones (including insulin). Many oral drugs in the sulfonylurea class (see Table 1) increase the risk of developing hypoglycemia during and after a bout of physical activity. Older-generation sulfonylureas (such as Diabinese and Orinase) cause insulin release from the pancreas and somewhat decrease insulin resistance; due to their longer duration of up to 72 hours, though, gives them a greater potential to cause individuals blood glucose levels to go too low during and/or after any physical activity.13 Secondgeneration sulfonylureas, such as DiaBeta, Micronase, Glynase, Amaryl, and Glucotrol, generally are cleared from the body more quickly (in 24 hours or less) and thereby present a smaller risk of causing exercise-associated hypoglycemia. Among these, DiaBeta, Micronase, and Glynase convey the greatest risk due to their slightly longer duration (24 hours versus only 12 to 16 hours for the other two).6 Individuals will need to check their blood glucose levels more often when exercising (and afterwards) if they take any of these
longer-lasting oral hypoglycemic medications. When exercise becomes regular, they may also benefit from checking with their health care providers about lowering their doses, particularly if they are experiencing more frequent lows with exercise. For the most effective dosage adjustments, diabetic exercisers should document all bouts of hypoglycemia after verifying them with blood glucose monitoring. Most of the medications in the remaining classes, however, are far less likely to affect glycemic responses to exercise. For example, insulin sensitizers like Avandia and Actos mainly improve the action of insulin at rest, not during exercise, so their risk of causing exercise-associated hypoglycemia is almost nonexistent.10 Similarly, Glucophage and Glucophage XR (the extended release form of metformin) are unlikely to cause it because their main action is to lower liver glucose output overnight, which has little effect on exercise responses.12 Prandin or Starlix use potentially increases risk if taken immediately before prolonged exercise as they increase insulin levels temporarily when taken before meals, and postprandial exercise in individuals with Type 2 Diabetes Mellitus (T2DM) lowers blood glucose levels more than the same bout done pre-breakfast (and before insulin is released).9 Medications that slow down the absorption of carbohydrates (Precose and Glyset) do not directly affect exercise, but can delay effective treatment of hypoglycemia during activities by slowing the absorption of carbohydrates ingested to treat this condition. Finally, the newest class of oral diabetic drugs, dipeptidyl peptidase-4 inhibitors (DPP-4 inhibitors), extend the action of insulin, but apparently do not increase the risk of exercise-induced hypoglycemia in individuals with T2DM already being treated with metformin.1 Most of these oral medications are used by individuals with T2DM, who commonly take a combination of two or more of them in an attempt to more effectively control glycemia. Certain medications themselves are already combination drugs; for example, Glucovance is comprised of glyburide and metformin. Some recent research, though, has additionally indicated the use of metformin in insulinresistant individuals with Type 1 Diabetes Mellitus (T1DM) who are experiencing a form of double diabetes with characteristics of both types.4,7 Individuals with either type of diabetes can certainly benefit from the insulin-sensitizing effects of an acute bout of exercise and regular physical training, both of which improve insulin action and generally lower blood glucose levels. There are also two new injectable diabetic medications (listed in Table 1) that can be used by individuals with either T1DM or T2DM: Byetta (exenatide, or extendin-4) and Symlin
Diabetic Medications... Continued on Page 9
JULY/AUGUST/SEPTEMBER 2007 | VOLUME 17; ISSUE 3
ACSMs Certified News
Diabetic Medications... Continued from Page 8
(pramlintide), a synthetic form of amylin, which is a hormone normally co-released from pancreatic beta cells with insulin.5,11 The main exercise-related concern with the use of these medications is that they both delay the emptying of food from the gut after a meal and could, therefore, slow the release of ingested carbohydrates taken to prevent or treat low blood glucose levels during a bout of exercise. Consequently, to err on the side of safety, if hypoglycemia is likely to occur during physical activity, neither Byetta nor Symlin should be injected within two hours prior to scheduled physical activity.
Table 1: Classes of Oral and Other Diabetic Medications
Class of Drug Sulfonylureas Brand Name (Generic Name) Amaryl (glimepiride), DiaBeta, Micronase, and Glynase (glyburide or glibenclamide), Glucotrol (glipizide), Diabinese (chlorpropamide), Orinase (tolbutamide) Avandia (rosiglitazone), Actos (pioglitazone) Mechanism of Action(s) Promote insulin secretion from pancreatic beta cells; some medications may increase insulin sensitivity
Thiazolidenediones Glitazones Biguanides
Increase insulin sensitivity of peripheral tissues, primarily skeletal muscles
Glucophage, Glucophage XR (metformin)
Decrease liver output of glucose while increasing liver and muscle insulin sensitivity; no direct effect on beta cells Stimulate beta cells to increase insulin secretion, but only for a very short duration (unlike sulfonylureas) Work in small intestines to slow digestion of some carbohydrates to control post-meal blood glucose elevations Work by inhibiting DPP-4, an enzyme that breaks down glucagon-like peptide1 (GLP-1); delayed GLP-1 degradation extends insulin action while suppressing glucagon release Helps control glycemic spikes for three hours after meals by delaying gastric emptying Stimulate insulin release; inhibit the livers release of glucose by lowering post-meal glucagon release; delay gastric emptying
Precautions for Insulin Use
Although individuals with T1DM must taken exogenous insulin, supplemental doses are eventually prescribed for up to 40 percent of individuals with T2DM, making insulin use widespread. Insulin users, particularly ones with T1DM, face a potentially more complicated exercise-medication interaction because they must precisely balance insulin and blood glucose levels to avoid both hypoglycemia and possible elevations in glucose levels during exercise.7 Longer duration exercise is more likely to have a glucose-lowering effect (unless insulin is deficient and ketone levels are moderate or higher), but shorter bouts of intense exercise, such as sprinting or heaving weightlifting, can also cause blood glucose levels to rise from the release of exaggerated amount of counterregulatory hormones like epinephrine and glucagon. In spite of the additional challenges involved, one of the best strategies for optimizing management outcomes is to learn the effects of exercise on insulin action and differing insulin regimens on glycemic control. Today, there are many medical options and they are constantly expanding. The majority of T1DM insulin users and some T2DM users requiring insulin choose to utilize a combination of short- and long-acting insulins (varying by time to peak action and total duration) given two to four (or more) times daily.8 Others may receive a continuous infusion of short-acting insulin that follows a basal-bolus regimen by using an insulin pump.3 The goal during exercise is to mimic the metabolic responses of non-diabetic individuals. When no more than minimal (basal) levels of insulin are circulating in the bloodstream during exercise, normoglycemia will be more effectively maintained. Given that both insulin and muscular contractions evoke separate mechanisms that cause muscles to take up glucose from the bloodstream, they additively increase muscle glucose uptake during exercise. Consequently, the type of insulin taken and the timing of its use can have a large effect on glycemic responses to physical activity.2,3,7 The onset, peak and dura-
Meglitinides/ Phenylalanine derivatives
Prandin (repaglinide), Starlix (nateglinide)
Alpha-Glucosidase Inhibitors
Precose (acarbose), Glyset (miglitol)
DPP-4 Inhibitors
Januvia (sitagliptin phosphate), Galvus (vildagliptin) Symlin (pramlintide acetate) Byetta (exenatide)
Amylin (injected) Incretins (injected)
tion of various insulins are listed in Table 2. If an individual exercises when exogenous insulin levels are peaking, the risk of hypoglycemia is greatly increased, particularly when failing to compensate with reduced insulin doses or consumption of additional carbohydrates.2 For instance, intermediateacting N injected at breakfast will peak around noon and exert its effects throughout the afternoon. If exercise is done after lunch without an increased carbohydrate intake at the prior meal or lower morning dose of N being given, blood glucose levels may decrease more rapidly than at other times of day with lower circulating levels of insulin. Exercise done within two hours of the administration of a rapid-acting insulin analog will also require appropriate compensation. Conversely, if only Lantus or Levemir (both of which provide basal insulin coverage for 12 to 24 hours) are circulating during an activity, then hypoglycemia will be much less likely to result.8 Likewise, insulin pump users can normalize their response to exercise by either disconnecting their pumps or reducing programmed basal rates during physical activity, both of which will lower circulating insulin levels closer to non-diabetic levels.3 Some pump users also decrease their basal rates before and/or after the activity, depending on how long it lasts and on their individ-
ual blood glucose responses.
Medications to Control Other Related Health Problems
Besides taking medications for diabetes control, many individuals may also take others to control elevated blood lipids (especially cholesterol levels), hypertension, and other coexisting health problems. Most medications taken for non-diabetic reasons will not affect exercise glycemia or other responses directly, with a few notable exceptions. Use of a class of drugs to treat high cholesterol levels called statins for short (including Lipitor, Mevacor, Pravachol, Crestor, and Zocor) may result in unexplained muscle pain and weakness during physical activity, possibly by compromising the muscles ability to generate energy effectively.14 However, muscle cramps during or after exercise, nocturnal cramping, and general fatigue all resolve after statin use is discontinued. If an individual taking a drug from this class experiences any of these symptoms with exercise, he or she needs to consult with a doctor about possibly switching to another cholesterol-lowering medication. Moreover, any prescribed drugs taken to reduce body water levels (diuretics like Lasix, Microzide, Enduron, and Lozol) and improve blood pressure can lead to dehydration and
Diabetic Medications... Continued on Page 10
ACSMs Certified News
10
AMERICAN COLLEGE OF SPORTS MEDICINE | (317) 637-9200
Diabetic Medications... Continued from Page 9
dizziness from hypotension, but will not likely affect blood glucose levels. Vasodilators such as nitroglycerin increase coronary blood flow during exercise, but can also induce low blood pressure, which increases the risk of fainting during or following an activity. Finally, beta-blockers (e.g., Lopressor, Inderal, Levatol, Corgard, Tenormin, Zebeta, and others) taken to treat heart disease and hypertension lower resting and exercise heart rates. For individuals using such a blocker, their heart rates will not reach age-expected values at any intensity of exercise.15 On the other hand, if taking either ACE inhibitors (Capoten, Accupril, Vasotec, Lotensin, Zestril, etc.) or angiotensin II receptor blockers (ARBs, such as Cozaar, Benicar, and Avapro), which are commonly prescribed for diabetic individuals to reduce blood pressure and/or protect the kidneys, individuals can expect no negative metabolic effects during exercise. In fact, using certain ACE inhibitors may actually lower the risk of untoward cardiovascular events for anyone with pre-existing heart disease. Other medications taken to treat heart disease and hypertension (calcium-channel blockers like Procardia, Sular, Cardene, Cardizem, and Norvasc), depression (Wellbutrin, Prozac, and others), or chronic pain (Celebrex) also have no impact on exercise responses. Aspirin and other blood thinners (such as Coumadin), however, have the potential to make individuals bruise more easily or extensively in response to athletic injuries.
Conclusion
Clearly, the use of various medications to control diabetes (and related health problems) can affect glycemic and other responses to exercise. In order to engage safely in regular physical activity without fear of unbalancing blood glucose levels, persons with diabetes must be willing to check their blood glucose at more frequent intervals than normal to determine their unique metabolic responses and any potential interactions with their prescribed medications. To help them do so, health and fitness professionals need to be aware of these possible effects and prescribe and monitor exercise appropriately.
Recommended Review Articles and Resources:
Albright, A., M. Franz, G. Hornsby, A. Kriska, D. Marrero, I. Ulrich, and L.S. Verity. American College of Sports Medicine. American College of Sports Medicine position stand. Exercise and type 2 diabetes. Medicine & Science in Sports & Exercise, 32:1345?1360, 2000. Colberg, S. The Diabetic Athlete: Prescriptions for Exercise and Sports. Champaigne, IL: Human Kinetics, 2001. Sigal, R., G. Kenny, D. Wasserman, et al. Physical activity/exercise and type 2 diabetes: a consensus statement from the American Diabetes Association. Diabetes Care, 29(6):1433-1438, 2006.
controlled with metformin alone. Diabetes Care, 29(12):26382643, 2006. 2. Chokkalingam, K., K. Tsintzas, L. Norton, et al. Exercise under hyperinsulinaemic conditions increases whole-body glucose disposal without affecting muscle glycogen utilisation in type 1 diabetes. Diabetologia, 50(2):414-421, 2007. 3. Diabetes Research in Children Network (DirecNet) Study Group; E. Tsalikian, C. Kollman, et al. Prevention of hypoglycemia during exercise in children with type 1 diabetes by suspending basal insulin. Diabetes Care, 29(10):2200-2204, 2006. 4. Hamilton, J., E. Cummings, V. Zdravkovic, et al. Metformin as an adjunct therapy in adolescents with type 1 diabetes and insulin resistance: a randomized controlled trial. Diabetes Care, 26(1):138-143, 2003. 5. Joy, S., P. Rodgers, A. Scates. Incretin mimetics as emerging treatment for type 2 diabetes. Annals of Pharmacotherapy, 39(1):110118, 2005. 6. Larsen, J., F. Dela, S. Madsbad, et al. Interaction of sulfonylureas and exercise on glucose homeostasis in type 2 diabetic patients. Diabetes Care, 22(10):16471654, 1999. 7. Muis, M., M. Bots, H. Bilo, et al. Determinants of daily insulin use in type 1 diabetes. Journal of Diabetes and Its Complications, 20(6):356-360, 2006. 8. Peterson, G. Intermediate and long-acting insulins: a review of NPH insulin, insulin glargine and insulin detemir. Current Medical Research and Opinion, 22(12):2613-2619, 2006. 9. Poirier, P., S. Mawhinney, L. Grondin, et al. Prior meal enhances the plasma glucose lowering effect of exercise in type 2 diabetes. Medicine & Science in Sports & Exercise, 33:12591264, 2001. 10. Reusch, J., J. Regensteiner, P. Watson. Novel actions of thiazolidinediones on vascular function and exercise capacity. American Journal of Medicine, 115:69S74S, 2003. 11. Ryan, G., L. Jobe, R. Martin. Pramlintide in the treatment of type 1 and type 2 diabetes mellitus. Clinical Therapeutics, 27(10):1500-1512, 2005. 12. Schwartz, S., V. Fonseca, B. Berner, et al. Efficacy, tolerability, and safety of a novel once-daily extended-release metformin in patients with type 2 diabetes. Diabetes Care, 29(4):759-764, 2006. 13. Shorr, R., W. Ray, J. Daugherty, et al. Individual sulfonylureas and serious hypoglycemia in older people. Journal of the American Geriatrics Society, 44(7):751-755, 1996. 14. Thompson, P., P. Clarkson, R. Karas. Statin-associated myopathy. Journal of the American Medical Association, 289(13):1681-1690, 2003. 15. Wonisch, M., P. Hofmann, F. Fruhwald, et al. Influence of betablocker use on percentage of target heart rate exercise prescription. European Journal of Cardiovascular Prevention and Rehabilitation, 10(4):296-301, 2003.
of exercise science at Old Dominion University in Norfolk, Virginia. As well as being an American Diabetes Association-funded clinical exercise researcher, she is also the author of numerous articles and four books on diabetes and exercise, including The Diabetic Athlete (2001), The 7 Step Diabetes Fitness Plan (2006), and 50 Secrets of the Longest Living People with Diabetes (November 2007).
Staying up to date with the ACSM Calendar of Events
Whether its upcoming dates, home study opportunities, or upcoming conferences, you will find the latest continuing education information in the ACSM Calendar of Events at www.acsm.org/coe. Calendar entries include conferences endorsed by ACSM that offer continuing education credits, as well as general non-ACSM approved programs that have been submitted to our office. If you would like to have your meeting reviewed for endorsement, select Endorsement Application to access the Guidelines for Endorsement and Continuing Education Credit application. For questions on ACSM continuing education opportunities, the ACSM endorsement process, or to receive the monthly calendar of events e-mail, please contact the education department at education@acsm.org. For questions on nonACSM endorsed continuing education that could be accepted for recertification, please contact Traci Rush at certification@acsm.org.
References
1. Charbonnel, B., A. Karasik, J. Liu, et al. Efficacy and safety of the dipeptidyl peptidase-4 inhibitor sitagliptin added to ongoing metformin therapy in patients with type 2 diabetes inadequately
About the Author:
Sheri R. Colberg, Ph.D., FACSM, is an associate professor
JULY/AUGUST/SEPTEMBER 2007 | VOLUME 17; ISSUE 3
11
ACSMs Certified News
July-September 2007 Continuing Education Self-Tests
Credits provided by the American College of Sports Medicine CEC Credit Offering Expires September 30, 2008
SELF-TEST #1 (1 CEC): The following questions were taken from Overview of Type 2 Diabetes published in this issue of ACSMs Certified News, pages 3-4. 1. For type 2 diabetics, the risk for a fatal heart attack or stroke is increased by over nondiabetics. A. 1-2 times B. 3-5 times C. 2-4 times D. 2-3 times 2. Type 2 diabetics only need to monitor their blood glucose before exercising, while recovery and postexercise is not as important. A. True B. False 3. Current recommended aerobic exercise at a moderate intensity for type 2 diabetes does NOT include _______: A. 3-7 days per week B. At least 90 minutes per week C. 40-60% HR D. At least 150 minutes per week 2.Type 1 diabetes is most commonly seen in A. African Americans B. Obese individuals C. Individuals over the age of 45 D. Individuals who inherit HLA alleles DR3 or DR4 E. A, B, and C only 3. A person with diabetes suffering from ketoacidosis has A. High blood glucose B. High circulating levels of acetoacetic and hydroxybutyric acids C. High blood pH D. A and B only E. All of the above 4. The biggest concern for a person with type 1 diabetes participating in an exercise program is A. Hypoglycemia B. Diabetic coma C. Hyperglycemia D. Improper heart rate response E. Inadequate sweat response 2. Insulin sensitizers like Avandia and Actos mainly improve the action of insulin at rest, not during exercise, so theyre unlikely to cause exercise-associated hypoglycemia. A. True B. False 3. Which of the following diabetic medications has the greatest potential to cause hypoglycemia during or after physical activity? A. Actos B. DPP-4 inhibitors, like Januvia C. Glucophage D. Glyset E. Insulin 4. What is the main concern with the use of either Symlin or Byetta within two hours prior to exercise? A. The injection site used to give either one might still hurt during exercise. B. If hypoglycemia develops during exercise, it may be harder to treat rapidly. C. They are so new to the market that no one knows their exact mechanisms of action. D. Both cause the release of insulin that could cause hypoglycemia during exercise. E. Due to their action, blood glucose levels will likely rise during exercise.
4. Type 2 diabetes can be effectively treated through 5. Testing and recording blood glucose levels before and weight loss, nutrition modifications, and physical activity. after exercise is good practice for the novice exerciser A. True with type 1 diabetes. He/She should also B. False A. Note when and how much insulin was taken B. Note when the last meal was eaten, and the 5. An important tool used to determine long-term composition of the meal 5. Which type of insulin administered two hours before glucose control for diabetes is ____________: C. Time of day the exercise was performed A. A fasting blood glucose the start of exercise is most likely to result in D. Type, intensity and duration of the exercise B. A post-absorptive blood glucose hypoglycemia due to its onset and peak times? E. All of the above C. Glycosylated hemoglobin (A1C) A. Lantus D. All of the above B. N (NPH) SELF-TEST #3 (2 CEC): The following questions were taken from Avoiding Possible Interactions Between C. Basal insulin SELF-TEST #2 (1 CEC): The following questions were Exercise and Diabetic Medications published in this issue D. Humalog or NovoLog taken from Type 1 Diabetes and Exercise published in of ACSMs Certified News, pages 8-10. this issue of ACSMs Certified News, pages 5-6. E. None of these insulins 1. Certain prescribed medications, including some oral 1. Type 1 diabetes is the most prevalent form of diabetes hypoglycemic and other diabetic medications, can affect in the United States. the bodys metabolic response to exercise, frequently A. True causing hypoglycemia. B. False A. True B. False
ACSMs
Certified News
NAME ADDRESS CITY BUSINESS TELEPHONE
To receive credit, circle the best answer for each question, check your answers against the answer key on page 2, and mail entire page with check or money order payable in US dollars to: American College of Sports Medicine, Dept 6022, Carol Stream, IL 60122-6022 ACSM Member (PLEASE MARK BELOW) Please Allow 4-6 weeks for processing of CECs [ ] Yes-$15 TOTAL $_________________ [ ] No- $20 ($25 fee for returned checks) ID # __________________ (Please provide your ACSM ID number)
ACSM USE:
627826
PLEASE PRINT OR TYPE REQUESTED INFORMATION
STATE E-MAIL
ZIP
July-September 2007 Issue EXPIRATION DATE: 09/30/08 SELF-TESTS SUBMITTED AFTER THE EXPIRATION DATE WILL NOT BE ACCEPTED. Federal Tax ID number 23-6390952
Tip: Frequent self-test participants can find their ACSM ID number located on any credit verification letter.
ACSMs Certified News
12
AMERICAN COLLEGE OF SPORTS MEDICINE | (317) 637-9200
News You Need... Continued from Page 1
ACSMs Regional Chapters
Enjoy top-notch educational presentations and unmatched opportunities to network with fellow professionals at ACSMs Regional Chapter meetings. In addition, earn valuable continuing education credits to keep your certification current. Below is a listing of upcoming meetings near you: July 18-21, 2007, Alaska Chapter, Sitka, AK Contact: Litia Garrison, alaska_acsm@yahoo.com, (907) 747-5160 October 4-5, 2007, Northland Chapter, Brookings, SD Contact: John Keener, Ph.D., nacsm@d.umn.edu, (218) 726-8531, www.d.umn.edu/~nacsm October 18-19, 2007, Central States Chapter, Springfield, MO Contact: Joel Cramer, Ph.D., jcramer@ou.edu, (405) 325-1371, www.centralstatesacsm.org October 25-27, 2007, Midwest Chapter, Columbus, OH Contact:Tim Kirby, Ph.D., kirby.1@osu.edu, (614) 292-0664, www.mwacsm.org November 2-3, 2007- Mid-Atlantic Chapter, Harrisburg, PA Contact: W. Craig Stevens, Ph.D., FACSM, cstevens@wcupa.edu, (610) 738-0497, www.marcacsm.org November 9-10, 2007, Southwest Chapter, San Diego, CA Contact: Jack Young, Ph.D., FACSM, jyoung@ccmail.nevada.edu, (702) 895-4626, www.swacsm.org November 15-16, 2007, New England Chapter, Providence, RI Contact: NEACSM Office, neacsm@thocc.org, (860) 224-5888, www.neacsm.org
Completed a Pre-workshop Packet and Study Guide for ACSM Health/Fitness Instructor 2007 workshops Established an Exam Development Team (started at Annual Meeting last year) Launched Item Writing Webinars Launched the ACSM Certified Personal TrainerSM Exam in Spanish Available in June Deployed an ACSM Membership Discount For non-member, ACSM Certified Professionals Our 70+ subject matter experts that comprise the CCRB are volunteers, and they will be as busy as ever in the coming year. Please help us acknowledge their commitment and hard work with a special thank you. Another important function of our annual updates is to disseminate the activity and performance of all our certification programs. Please find the details in the table below,
CCRB Examination Activity: January 1, 2006 December 31, 2006. Also, if you havent noticed already, each issue of ACSMs Certified News is now themed. In other words, each issue is specifically devoted to a single and relevant topic for the health/fitness practitioner. Plus, all CECs available in each issue are now based exclusively on the articles that appear. This makes it easier than ever to accumulate your required CECs to not only maintain your certification status, but continue to develop your knowledge base. Finally, as a reminder for all of you whose recertification window closes on December 31, 2007: You should submit your accumulated CECs (continuing education credits) and accompanying fees as soon as possible, to avoid the last-minute rush as the end of the year approaches. If you have any questions about your recertification status, please contact Traci Rush, ACSMs Certification Manager, at (317) 637-9200, ext. 126.
CCRB Examination Activity: January 1, 2006 December 31, 2006
Total Candidates (2006) 1,889 Pass Rate 69% Credentials Awarded 1,303 Number of Operational (Scored) Items 125-150 Number of Experimental (Non-scored) Total Items Items 0-25 125-150 Time Limit 2.5 hours
Credential ACSM Certified Personal Trainer ACSM Health/Fitness Instructor ACSM Exercise Specialist ACSM Registered ClinicalExercise Physiologist
874
67%
585
125-150
0-25
125-150
3.5 hours
280
53%
148
100-135
0-25
100-135
3.5 hours
190
86%
163
125-150
0-25
125-150
3 hours
ACSMs Certified News ISSN # 1056-9677 P.O. Box 1440 Indianapolis, IN 46206-1440 USA
You might also like
- Endocrine DisordersDocument28 pagesEndocrine DisordersRhitzle Ann50% (2)
- CH1Document46 pagesCH1Muhammad FahmiNo ratings yet
- Metabolic Syndrome Thesis PDFDocument5 pagesMetabolic Syndrome Thesis PDFafknawjof100% (2)
- Adult Obesity CausesDocument9 pagesAdult Obesity CausesAntoNo ratings yet
- Heart Disease Term PaperDocument5 pagesHeart Disease Term Paperafmzxppzpvoluf100% (1)
- Overweight and Obesity CDC 2019Document6 pagesOverweight and Obesity CDC 2019Evi BaeNo ratings yet
- Clinical Guideline: Annals of Internal MedicineDocument8 pagesClinical Guideline: Annals of Internal MedicineYulias YoweiNo ratings yet
- AQ FamilyMedicine 06Document12 pagesAQ FamilyMedicine 06Eduardo OrtizNo ratings yet
- Term Paper Heart DiseaseDocument7 pagesTerm Paper Heart Diseasec5p0cd99100% (1)
- Exercise Can Help Tame Type 2 DiabetesDocument2 pagesExercise Can Help Tame Type 2 DiabetesAfifah WidyadhariNo ratings yet
- Diabetes and Exercise ThesisDocument7 pagesDiabetes and Exercise Thesistonyacartererie100% (2)
- Exercise and Diabetes: A Clinician's Guide to Prescribing Physical ActivityFrom EverandExercise and Diabetes: A Clinician's Guide to Prescribing Physical ActivityNo ratings yet
- DiabetesDocument5 pagesDiabetesJayson TrajanoNo ratings yet
- Chronic DiseaseDocument6 pagesChronic DiseasekksNo ratings yet
- Determinants of Public HealthDocument6 pagesDeterminants of Public HealthMissy OrgelaNo ratings yet
- Exercise - Physical Activity in Individuals With Type 2 Diabet... - Medicine & Science in Sports & ExerciseDocument51 pagesExercise - Physical Activity in Individuals With Type 2 Diabet... - Medicine & Science in Sports & ExerciseRicardo Arellano GarcíaNo ratings yet
- PHD Thesis Metabolic SyndromeDocument5 pagesPHD Thesis Metabolic Syndromejanchampagnefargo100% (2)
- Questionnaire Questions - ScrapDocument9 pagesQuestionnaire Questions - ScrapNaomi JohnsonNo ratings yet
- Week 4 & 5Document27 pagesWeek 4 & 5Ali HaiderNo ratings yet
- Heex4400aacvpr PhysiciansDocument24 pagesHeex4400aacvpr PhysiciansSuganya BalachandranNo ratings yet
- Tugas Pengganti Uts (Summary)Document12 pagesTugas Pengganti Uts (Summary)Uni TyasNo ratings yet
- Diabetes Educational Program in ElderlyDocument9 pagesDiabetes Educational Program in ElderlyJaveria KhawarNo ratings yet
- Health - Diabetes Research PaperDocument7 pagesHealth - Diabetes Research Paperapi-299727107No ratings yet
- Diabetes AAG 2011 508Document4 pagesDiabetes AAG 2011 508Shams HassanNo ratings yet
- Diabetes in SportsDocument11 pagesDiabetes in SportsstefanNo ratings yet
- The Problem and It'S Background: World Health OrganizationDocument26 pagesThe Problem and It'S Background: World Health OrganizationGio LlanosNo ratings yet
- Metabolic Syndrome: Pennington Biomedical Research CenterDocument17 pagesMetabolic Syndrome: Pennington Biomedical Research CenterJhay-arr HernandezNo ratings yet
- Diabetes No Atleta CompetitivoDocument7 pagesDiabetes No Atleta CompetitivojosiNo ratings yet
- Insulin TherapyDocument55 pagesInsulin TherapyShriyank BhargavaNo ratings yet
- Dissertation On Metabolic SyndromeDocument4 pagesDissertation On Metabolic SyndromeWhereToBuyResumePaperCanada100% (1)
- Dental Hygienists Against Heart DiseaseDocument26 pagesDental Hygienists Against Heart Diseaserajdeep_pavaskarNo ratings yet
- ANNALS-Diabetes Tipo IIDocument16 pagesANNALS-Diabetes Tipo IIewb100% (2)
- AGNG 320 Tak1Document8 pagesAGNG 320 Tak1mutiso mutieNo ratings yet
- Risk Factors: Tobacco UseDocument9 pagesRisk Factors: Tobacco UseLester Patalinghug BernardinoNo ratings yet
- Metabolic Syndrome - Symptoms, Diagnosis, and CausesDocument7 pagesMetabolic Syndrome - Symptoms, Diagnosis, and CausesdrmuratNo ratings yet
- Meeting the American Diabetes Association Standards of Care: An Algorithmic Approach to Clinical Care of the Diabetes PatientFrom EverandMeeting the American Diabetes Association Standards of Care: An Algorithmic Approach to Clinical Care of the Diabetes PatientNo ratings yet
- Dodging Diabetes ComplicationsDocument20 pagesDodging Diabetes ComplicationsUlises MatiasNo ratings yet
- CVD Effects of ExerciseDocument11 pagesCVD Effects of ExerciseAboobacker SabithNo ratings yet
- Obesity Care in DiabetsDocument1 pageObesity Care in DiabetsTanzer BalkırNo ratings yet
- Fitness and DiseaseDocument25 pagesFitness and Diseaseapi-309742389No ratings yet
- Type 1 Delay Living Update Press Release - FinalDocument2 pagesType 1 Delay Living Update Press Release - FinalMelchor Alcántara BarreraNo ratings yet
- DR KessyDocument8 pagesDR KessyAnitha OnesmoNo ratings yet
- Abstract 1AND2 SetDocument11 pagesAbstract 1AND2 Setmarina20240015829No ratings yet
- High Blood Pressure and Cholesterol: 39 1 in 2 2 in 3Document4 pagesHigh Blood Pressure and Cholesterol: 39 1 in 2 2 in 3annyzaukNo ratings yet
- Weight Management Program 2015Document14 pagesWeight Management Program 2015api-284569489No ratings yet
- Heart Disease and Stroke Scientific ReviewDocument6 pagesHeart Disease and Stroke Scientific Reviewapi-371380624No ratings yet
- Disease Diabetes Health ArticlesDocument3 pagesDisease Diabetes Health ArticlesarmanNo ratings yet
- Coronary Artery Disease Cad2Document182 pagesCoronary Artery Disease Cad2Mamot Mot0% (1)
- DiabetesDocument8 pagesDiabetessahakumarsayanNo ratings yet
- Prevention: Can Prediabetes, Type 2 Diabetes and Gestational Diabetes Be Prevented?Document9 pagesPrevention: Can Prediabetes, Type 2 Diabetes and Gestational Diabetes Be Prevented?BethChay LacsonNo ratings yet
- Harmonizing The Metabolic SyndromeDocument7 pagesHarmonizing The Metabolic SyndromeCarlos_RuedasNo ratings yet
- Term Paper DiabetesDocument8 pagesTerm Paper Diabetesea5zjs6a100% (1)
- AAA_Type_2_Diabetes_Annals_of_Internal_MedicineDocument19 pagesAAA_Type_2_Diabetes_Annals_of_Internal_MedicineCelebfan BoyNo ratings yet
- Chair Master-Exercise-Instructor-Manual-with-pictures PDFDocument64 pagesChair Master-Exercise-Instructor-Manual-with-pictures PDFonix2000100% (1)
- E147 Full PDFDocument21 pagesE147 Full PDFcahyatiNo ratings yet
- Dissertation On Diabetes Type 2Document4 pagesDissertation On Diabetes Type 2PaperWritingHelpCanada100% (1)
- Misclassification of Cardiometabolic Health When Using Body Mass Index Categories in NHANES 2005-2012Document5 pagesMisclassification of Cardiometabolic Health When Using Body Mass Index Categories in NHANES 2005-2012Maria Ignacia MacariNo ratings yet
- Insurance: Vivek College of CommerceDocument26 pagesInsurance: Vivek College of CommerceprasadNo ratings yet
- Diabetes Mellitus by DR RelliqueteDocument5 pagesDiabetes Mellitus by DR RelliqueteKenneth Jed M. RobentaNo ratings yet
- Diabetes Knowledge TestDocument1 pageDiabetes Knowledge TestNadira Farah PrayogoNo ratings yet
- Diabetis-Metabolic DisordersDocument358 pagesDiabetis-Metabolic DisordersHampson MalekanoNo ratings yet
- DM Guidelines CCPDocument87 pagesDM Guidelines CCPfuad20No ratings yet
- Nursing ProcessDocument12 pagesNursing ProcessArif AshariNo ratings yet
- Short Guide Clinical NutritionDocument30 pagesShort Guide Clinical Nutritiontopiq100% (1)
- Health Tips For Ramad - 1Document9 pagesHealth Tips For Ramad - 1Syahrizul Fadly MadelliNo ratings yet
- Pone 0163350Document14 pagesPone 0163350alifandoNo ratings yet
- Dka 31-05-11Document52 pagesDka 31-05-11Hussain AzharNo ratings yet
- FORA G31 Manual EngDocument48 pagesFORA G31 Manual EngAdriana IacobNo ratings yet
- Section 504 Plan: Form 4 St. Michael-Albertiville Public SchoolsDocument10 pagesSection 504 Plan: Form 4 St. Michael-Albertiville Public Schoolsapi-314180367No ratings yet
- Clinical Chemistry Review NotesDocument54 pagesClinical Chemistry Review NotesALEONA AMON ARANTENo ratings yet
- TeneligliptinDocument17 pagesTeneligliptintarun956519No ratings yet
- Surya VigyanDocument41 pagesSurya Vigyanpradeepnagda100% (2)
- AdknowlDocument21 pagesAdknowlBie JhingcHayNo ratings yet
- Diabetes Management: OverviewDocument20 pagesDiabetes Management: Overviewlaloo01No ratings yet
- UntitledDocument1 pageUntitledapi-134347145No ratings yet
- Crossfit NutritionDocument16 pagesCrossfit Nutritionscribd94100% (1)
- Self Efficacy Theory - Case StudiesDocument13 pagesSelf Efficacy Theory - Case StudiesPetros Akin-Nibosun0% (1)
- Pathophysiology of DiabetesDocument3 pagesPathophysiology of DiabetesJeffrey Ramos GironNo ratings yet
- Enzymes Questions For AQA AS BiologyDocument67 pagesEnzymes Questions For AQA AS Biologyjames75% (4)
- Blood Sugar TestDocument4 pagesBlood Sugar TestanisyaNo ratings yet
- DM DR Osama Mahmoud PDFDocument27 pagesDM DR Osama Mahmoud PDFRaouf Ra'fat Soliman100% (1)
- Part I - Sample Questions: COMPETENCY 1: Patient CareDocument20 pagesPart I - Sample Questions: COMPETENCY 1: Patient CareAbdallah ElmenshawyNo ratings yet
- Invisible Minerals Part II by DR Carolyn DeanDocument46 pagesInvisible Minerals Part II by DR Carolyn Deanlihu74100% (1)
- NCP DM 1Document6 pagesNCP DM 1Shin AblangNo ratings yet
- Diabetes FreeDocument166 pagesDiabetes FreeTerry D Barone100% (1)
- NAT Reviewer in EnglishDocument9 pagesNAT Reviewer in Englishleomille250% (2)