Professional Documents
Culture Documents
Prevalence of Primary Dysmenorrhea Its Intensity A
Prevalence of Primary Dysmenorrhea Its Intensity A
Uploaded by
milionCopyright:
Available Formats
You might also like
- Bio Signature Modulation ExplainedDocument4 pagesBio Signature Modulation ExplainedChris Gregory100% (4)
- Tantra For MenDocument18 pagesTantra For MenDeba Brata100% (1)
- Gynecologic Problems of Childhood: Anne Margrette C. VelasquezDocument46 pagesGynecologic Problems of Childhood: Anne Margrette C. VelasquezAnne Margrette Velasquez100% (1)
- Ijwh-14-517 TiruyeDocument11 pagesIjwh-14-517 TiruyeDaraaswanNo ratings yet
- FRPH 04 939035Document7 pagesFRPH 04 939035DaraaswanNo ratings yet
- Determinants of Female Genital Mutilation Among Under Five-Year Children in Motta Town, Northwest Ethiopia, 2022: Unmatched Case Control StudyDocument11 pagesDeterminants of Female Genital Mutilation Among Under Five-Year Children in Motta Town, Northwest Ethiopia, 2022: Unmatched Case Control StudysamsiebopNo ratings yet
- Wong2010Document4 pagesWong2010dara intanNo ratings yet
- Prevalence of Dysmenorrhea and Its Effects On SchoDocument7 pagesPrevalence of Dysmenorrhea and Its Effects On SchoMarilyn RebatoNo ratings yet
- Epidemiology of Dysmenorrhea Among University of Dschang Students (West Region, Cameroon) : A Cross-Sectional StudyDocument6 pagesEpidemiology of Dysmenorrhea Among University of Dschang Students (West Region, Cameroon) : A Cross-Sectional StudyInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Ijwh 287715 Teenage Pregnancy and Its Associated Factors in Eastern EthiDocument12 pagesIjwh 287715 Teenage Pregnancy and Its Associated Factors in Eastern EthiJinky Mendoza CalingasanNo ratings yet
- Dude Ja 2016Document5 pagesDude Ja 2016Mushfiqur RahmanNo ratings yet
- BacaDocument9 pagesBacaLivianadrNo ratings yet
- Dysmenorrhoea Among Adolescent Girls - Characteristics and Symptoms Experienced During MenstruationDocument8 pagesDysmenorrhoea Among Adolescent Girls - Characteristics and Symptoms Experienced During MenstruationUlfa Diya AtiqaNo ratings yet
- Problem Pada MenstruasiDocument8 pagesProblem Pada MenstruasiInna MeratiNo ratings yet
- 1-S2.0-S1110569017302935-MainDocument5 pages1-S2.0-S1110569017302935-Maindara intanNo ratings yet
- Undernutrition Among Pregnant Women in Rural Communities in Southern EthiopiaDocument7 pagesUndernutrition Among Pregnant Women in Rural Communities in Southern EthiopiaJenny Rose PangdaoNo ratings yet
- JournalDocument5 pagesJournalNatalia ChandraNo ratings yet
- Prevalence of Dysmenorrhoea and Its Associated Factors Among Female Medical Students at Kampala International University Western CampusDocument15 pagesPrevalence of Dysmenorrhoea and Its Associated Factors Among Female Medical Students at Kampala International University Western CampusKIU PUBLICATION AND EXTENSIONNo ratings yet
- Prevalence and Pattern of Dysmenorrhea Among SeconDocument6 pagesPrevalence and Pattern of Dysmenorrhea Among SeconmilionNo ratings yet
- Jkachn 24 3 264.ko - enDocument9 pagesJkachn 24 3 264.ko - enSonali DakhoreNo ratings yet
- Explore The Knowledge and Impact On Dysmenorrhea Among Nursing Students of Selected CollegeDocument5 pagesExplore The Knowledge and Impact On Dysmenorrhea Among Nursing Students of Selected CollegeEditor IJTSRDNo ratings yet
- JMDH 16 2271Document8 pagesJMDH 16 2271fatcaterpillarNo ratings yet
- Prevalence and Factors Affecting Enuresis Amongst Primary School ChildrenDocument5 pagesPrevalence and Factors Affecting Enuresis Amongst Primary School ChildrenAshu SharmaNo ratings yet
- Prevalence and Predictors of Dysmenorrhea Among STDocument6 pagesPrevalence and Predictors of Dysmenorrhea Among STAngel 冯晓君No ratings yet
- 1 SMDocument6 pages1 SMedi_wsNo ratings yet
- 10 1 1 976 384 PDFDocument7 pages10 1 1 976 384 PDFAdam RiskyNo ratings yet
- Menstrual Disorders Among Zagazig University Students, Zagazig, EgyptDocument6 pagesMenstrual Disorders Among Zagazig University Students, Zagazig, EgyptErsi Dwi Utami SiregarNo ratings yet
- SouthwestDocument7 pagesSouthwestDamesa MiesaNo ratings yet
- Jurnal Vulva HygienDocument10 pagesJurnal Vulva HygienDinaMerianaVanrioNo ratings yet
- Research ArticleDocument11 pagesResearch ArticleJabou NjieNo ratings yet
- Severity of Primary DysmenorrheaDocument7 pagesSeverity of Primary Dysmenorrheasfs_idxNo ratings yet
- Effectiveness of Audio Drama On Menstrual Hygiene and Management of Minor Ailments of Menstruation Upon Knowledge and Practice Among Visually Challenged GirlsDocument5 pagesEffectiveness of Audio Drama On Menstrual Hygiene and Management of Minor Ailments of Menstruation Upon Knowledge and Practice Among Visually Challenged GirlsInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Research ArticleDocument9 pagesResearch ArticleshahrasyiddNo ratings yet
- Prevalency DismenoireDocument8 pagesPrevalency DismenoireFatiya MuthmainnahNo ratings yet
- Effect of Health Education Program For Mothers of Children With Enterobius Vermicularis at Assiut University Children HospitalDocument30 pagesEffect of Health Education Program For Mothers of Children With Enterobius Vermicularis at Assiut University Children HospitalancillaagraynNo ratings yet
- Use OnlyDocument4 pagesUse OnlyDavid AyibonteyNo ratings yet
- A Study To Identify Premenstrual Syndrome and Their Management Adopted by Adolescent Girls Studying in Selected High School at Jabalpur M.PDocument4 pagesA Study To Identify Premenstrual Syndrome and Their Management Adopted by Adolescent Girls Studying in Selected High School at Jabalpur M.PEditor IJTSRDNo ratings yet
- 80 ArticleText 355 1 10 20190816 PDFDocument8 pages80 ArticleText 355 1 10 20190816 PDFnay laNo ratings yet
- Depression Among University Students in Kenya: Prevalence and Sociodemographic CorrelatesDocument7 pagesDepression Among University Students in Kenya: Prevalence and Sociodemographic CorrelatesDani AnyikaNo ratings yet
- RRTM 327129 Isolation of Escherichia Coli and Its Associated Risk FactorDocument8 pagesRRTM 327129 Isolation of Escherichia Coli and Its Associated Risk FactorAssefa AlemuNo ratings yet
- PembahasanDocument7 pagesPembahasanDini LianiNo ratings yet
- Jurnal DysmenorrheaDocument10 pagesJurnal Dysmenorrheaanisah tri agustiniNo ratings yet
- IJWH 352348 Determinants of Premature Rupture of Membrane Prom Among PDocument12 pagesIJWH 352348 Determinants of Premature Rupture of Membrane Prom Among PCitaNo ratings yet
- 1000-Article Text-3267-1-10-20221210Document6 pages1000-Article Text-3267-1-10-20221210Jasmine Hasna N RNo ratings yet
- 357 1278 1 PBDocument7 pages357 1278 1 PBPika RahayuNo ratings yet
- EN Epidemiology of Dysmenorrhea Among FemalDocument6 pagesEN Epidemiology of Dysmenorrhea Among FemalRuth RachmawatyNo ratings yet
- The Magnitude of Failed Induction of Labor and Associated Factors Among Women Delivered at Public Hospitals of Arsi Zone Southeast Ethiopia 2020 ADocument14 pagesThe Magnitude of Failed Induction of Labor and Associated Factors Among Women Delivered at Public Hospitals of Arsi Zone Southeast Ethiopia 2020 ABeti yemaneNo ratings yet
- The Prevalence and Risk Factors of Dysmenorrhea - Dyto Prasetya BuwanaDocument10 pagesThe Prevalence and Risk Factors of Dysmenorrhea - Dyto Prasetya Buwana0406 Dyto Prasetya BuwanaNo ratings yet
- Prevalence of Anaemia and Dysmenorrhoea Among Adolescent GirlsDocument5 pagesPrevalence of Anaemia and Dysmenorrhoea Among Adolescent GirlssafiraNo ratings yet
- BMC Public Health: Intestinal Parasites Prevalence and Related Factors in School Children, A Western City Sample-TurkeyDocument6 pagesBMC Public Health: Intestinal Parasites Prevalence and Related Factors in School Children, A Western City Sample-TurkeyVelazquez Rico Cinthya MontserrathNo ratings yet
- Prevalence of Dysmenorrhea Associated Factors PainDocument23 pagesPrevalence of Dysmenorrhea Associated Factors PainDaraaswanNo ratings yet
- Depression Among Pregnant Women and Associated Factors in Hawassa City, Ethiopia: An Institution-Based Cross-Sectional StudyDocument6 pagesDepression Among Pregnant Women and Associated Factors in Hawassa City, Ethiopia: An Institution-Based Cross-Sectional Studyevita juniarNo ratings yet
- PRBM 13 1365Document8 pagesPRBM 13 1365Dewi Utami IrianiNo ratings yet
- Hubungan Peran Keluarga Dengan Harga Diri Pada Penderita Penyakit KustaDocument10 pagesHubungan Peran Keluarga Dengan Harga Diri Pada Penderita Penyakit KustaEnggar RahmanNo ratings yet
- Parker2009 - Menstruasi PDFDocument8 pagesParker2009 - Menstruasi PDFtiaraNo ratings yet
- Epidemiology of Dysmenorrhea Among Female Adolescents in CentralDocument7 pagesEpidemiology of Dysmenorrhea Among Female Adolescents in CentralRuth RachmawatyNo ratings yet
- Awareness On Menstrual Hygiene Among Deaf Mute Adolescents With Special Reference To in Thrissur District, KeralaDocument5 pagesAwareness On Menstrual Hygiene Among Deaf Mute Adolescents With Special Reference To in Thrissur District, KeralaEditor IJTSRDNo ratings yet
- FileDocument19 pagesFileTanushikha SangwanNo ratings yet
- Jurnal Tentang Asfiksia-DikonversiDocument12 pagesJurnal Tentang Asfiksia-DikonversiLaila Al-GifariahNo ratings yet
- The Impact of Menstrual Symptoms On Everyday LifeDocument7 pagesThe Impact of Menstrual Symptoms On Everyday LifeEiman Khowaja (22GJKB-CLSTEC)No ratings yet
- Premenstrual Syndrome Frequency, Premenstrual Syndrome Coping Strategies and Factors Affecting Premenstrual Syndrome in University Students in TurkeyDocument18 pagesPremenstrual Syndrome Frequency, Premenstrual Syndrome Coping Strategies and Factors Affecting Premenstrual Syndrome in University Students in TurkeyGlobal Research and Development ServicesNo ratings yet
- MafraDocument33 pagesMafrayvette kinyuyNo ratings yet
- Acne: Current Concepts and ManagementFrom EverandAcne: Current Concepts and ManagementDae Hun SuhNo ratings yet
- Uterine FibroidsDocument47 pagesUterine FibroidsMoh Aldhy HusaintNo ratings yet
- Project Work: InvestigatoryDocument16 pagesProject Work: InvestigatoryRahul DasNo ratings yet
- Legalization Abortion in IndiaDocument13 pagesLegalization Abortion in IndiaNeetish Kumar HandaNo ratings yet
- 9th - Cystic OvariesDocument25 pages9th - Cystic Ovariesnoor aineNo ratings yet
- 4.2 Deviations From The Mendelian InheritanceDocument62 pages4.2 Deviations From The Mendelian InheritancejiaenNo ratings yet
- Mark SchemeDocument9 pagesMark SchemeJanani MNo ratings yet
- Comprehensive Examination: Assumption Montessori SchoolDocument9 pagesComprehensive Examination: Assumption Montessori Schoolshincee23No ratings yet
- Artificial Insemination ProcedureDocument9 pagesArtificial Insemination ProcedureJyotiNo ratings yet
- Med Trans ReviewerDocument1 pageMed Trans ReviewerDenise CerdaNo ratings yet
- Alchemical Taoism: Five Element TheoryDocument13 pagesAlchemical Taoism: Five Element Theoryמיקי קליין יוגהNo ratings yet
- Causes of Maternal Mortality and MorbidityDocument20 pagesCauses of Maternal Mortality and MorbidityRaNa MaYaaNo ratings yet
- Spontaneous AbortionDocument17 pagesSpontaneous Abortionanon_985338331No ratings yet
- 3893 ID Faktor Risiko Yang Mempengaruhi Kejadian Dismenore PrimerDocument8 pages3893 ID Faktor Risiko Yang Mempengaruhi Kejadian Dismenore PrimerNur lailah sakinahNo ratings yet
- Jadwal Semester 2 Februari - Juli 2020: Hari Tanggal JAM KelompokDocument30 pagesJadwal Semester 2 Februari - Juli 2020: Hari Tanggal JAM KelompokFelicia AcraminNo ratings yet
- Congenital Adrenal HyperplasiaDocument28 pagesCongenital Adrenal HyperplasiaWindelyn Gamaro0% (1)
- DR Stephen Chang - Deer ExerciseDocument1 pageDR Stephen Chang - Deer ExerciseDolf Cheng100% (2)
- 3 Placenta Previa Nursing Care PlansDocument7 pages3 Placenta Previa Nursing Care PlansAjay RajpootNo ratings yet
- Sterilization of DogsDocument18 pagesSterilization of Dogsjo12joseNo ratings yet
- Ms Sabiha ReportDocument4 pagesMs Sabiha Reportzafir alamNo ratings yet
- Sakila MurmuDocument47 pagesSakila MurmuSakila murmuNo ratings yet
- The Ultimate Male Orgasm PDFDocument4 pagesThe Ultimate Male Orgasm PDFDavid Hosam50% (2)
- Biology SSC - Ii: SECTION - B (Marks 30)Document2 pagesBiology SSC - Ii: SECTION - B (Marks 30)Bushra BushraNo ratings yet
- BIO220Document6 pagesBIO220imma haznaNo ratings yet
- Geself Midterms ReviewerDocument13 pagesGeself Midterms ReviewerKim OpenaNo ratings yet
- Gonorrhea: by Siena Kathleen V. Placino BSN-IV Communicable Disease Nursing C.I.: Dr. Dario V. SumandeDocument38 pagesGonorrhea: by Siena Kathleen V. Placino BSN-IV Communicable Disease Nursing C.I.: Dr. Dario V. SumandeSiena100% (1)
- Biology Rose 09Document68 pagesBiology Rose 09kukaraja77No ratings yet
- Stamina Guide Orgasm Top TipsDocument26 pagesStamina Guide Orgasm Top TipsJames Jameson57% (7)
Prevalence of Primary Dysmenorrhea Its Intensity A
Prevalence of Primary Dysmenorrhea Its Intensity A
Uploaded by
milionOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Prevalence of Primary Dysmenorrhea Its Intensity A
Prevalence of Primary Dysmenorrhea Its Intensity A
Uploaded by
milionCopyright:
Available Formats
International Journal of Women’s Health Dovepress
open access to scientific and medical research
Open Access Full Text Article
ORIGINAL RESEARCH
Prevalence of Primary Dysmenorrhea, Its Intensity
and Associated Factors Among Female Students
at High Schools of Wolaita Zone, Southern
International Journal of Women's Health downloaded from https://www.dovepress.com/ on 10-Nov-2022
Ethiopia: Cross-Sectional Study Design
Mesfin Mammo*, Mihiretu Alemayehu *, Gizachew Ambaw *
School of Public Health, College of Health Science and Medicine, Wolaita Sodo University, Wolaita Sodo, Ethiopia
*These authors contributed equally to this work
Correspondence: Gizachew Ambaw, Wolaita Sodo, Ethiopia, Tel +251918556340, Email gizachewambawkase@gmail.com
For personal use only.
Introduction: Primary dysmenorrhea is a highly prevalent gynecological problem and one of the most common causes of school
absenteeism among school adolescents. Nearly, half of females with primary dysmenorrhea missed school or work at least once per
cycle. Therefore, this study aimed to assess the prevalence of primary dysmenorrhea and its associated factors among female students
in Wolaita soddo town high schools.
Methods: An institution-based cross-sectional study was conducted among female students at Wolaita soddo town high schools from
October 1–30/2021. A total of 733 students were selected using a simple random sampling technique. The data were entered using Epi
data version 3.1 and exported to SPSS version 25 for analysis. Binary logistic regression analysis was used. Variables with a p-value of
<0.05 in the multivariable logistic regression analysis model were considered statistically significant.
Results: The prevalence of primary dysmenorrhea was 70% (95% CI (66.6%, 73.4%)). Factors such as age <18 years (AOR 2.55;
95% CI (1.77, 3.68)), long duration of menstrual flow (AOR 2.72; 95% CI (1.42, 5.17)), irregular menstrual cycle (AOR 2.39; 95% CI
(1.68, 3.41)), family history of dysmenorrhea (AOR 2.46; 95% CI (1.67, 3.64)) and skipping breakfast (AOR 1.62; 95% CI (1.13,
2.33)) were associated with primary dysmenorrhea.
Conclusion: The prevalence of primary dysmenorrhea was high among high school students in the study area. Being younger age,
long menstrual flow duration, irregular monthly menstrual cycle, family history of dysmenorrhea, and skipping breakfast were
determinants of primary dysmenorrhea.
Keywords: primary dysmenorrhea, prevalence, adolescents, menstruation, Ethiopia
Introduction
Dysmenorrhea is defined as the presence of painful cramps of uterine origin that occur during menstruation.1
Dysmenorrhea can be divided into two broad categories of primary and secondary. Primary dysmenorrhea is described
as recurrent, cramping pain occurring with menses in the absence of identifiable pelvic pathology. Secondary dysmenor
rhea is menstrual pain associated with underlying pelvic pathologies such as endometriosis, uterine myomas, pelvic
inflammatory disease, ovarian cyst, intra-uterine adhesions and cervical stenosis. The most common symptoms of
dysmenorrhea are cramps lower abdominal pain, back pain, nausea/vomiting and headache.2
The cause of primary dysmenorrhea is not well established. However, the responsible cause has identified on the
hyper-production of uterine prostaglandins, thus resulting in increased uterine one and high amplitude contractions.
Women with dysmenorrhea have higher levels of prostaglandins, which are highest during the first two days of menses.
Prostaglandin production is controlled by progesterone; when progesterone levels drop, immediately prior to
International Journal of Women’s Health 2022:14 1569–1577 1569
Received: 29 July 2022 © 2022 Mammo et al. This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.
Accepted: 4 November 2022 php and incorporate the Creative Commons Attribution – Non Commercial (unported, v3.0) License (http://creativecommons.org/licenses/by-nc/3.0/). By accessing the
work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For
Published: 9 November 2022 permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms (https://www.dovepress.com/terms.php).
Mammo et al Dovepress
menstruation prostaglandin level increase. These increase in prostaglandin level cause muscles contraction in uterus,
which cause pain during menstrual flow.1,2
Primary dysmenorrhea is the most commonly reported gynecological and menstrual disorder. It affects a large
proportion of women of reproductive ages. It affects millions of women during their reproductive year.1,3 Globally,
the previous epidemiological investigations have reported that the magnitudes of dysmenorrhea ranges from 41.7% to
94%.4,5 In sub-Saharan Africa, the prevalence of primary dysmenorrhea ranges also from 51.1% to 88.1%.6,7 In Ethiopia
the prevalence of primary dysmenorrhea ranges from 62.3% to 85,4%.3,8 The common risk factors for primary
dysmenorrhea are a positive family history of dysmenorrhea, obesity, being younger age, shorter or longer menstrual
cycle interval, stress, menstrual cycle irregularity, early menarche before 12 years and circumcision.11,12
Primary dysmenorrhea is a significant contributor to approximately 10% of incapacitating severe menstrual pain
among females during adolescence and early adulthood. In addition, it is severe enough to result in a significant socio-
economic dysfunction and disability particularly in adolescents and young women.9 In United-States an estimated
600 million work hours and 2 billion dollars of economic loss are associated with dysmenorrhea. It has a significant
negative impact on students’ academic performance.7 Several studies have stated that primary dysmenorrhea usually
affects relationships, functioning, and productivity, contributes to absenteeism in class/work and reduces day-to-life
activities.10 In despite this, the problem is considered to be underestimated and untreated as most women do not seek
medical treatment because they commonly perceive that pain is an expected part of menstruation. For example, about
85.8% of females do not seek medical care/advice which indicates that screening all adolescent girls for primary
dysmenorrhea is important.28 So that findings can guide to design an effective menstrual health education program
and to develop strategies to compensate lost classes and improve poor academic performance.
Developing appropriate management and preventive strategies is important to reduce the health impact of dysmenor
rhea among adolescent girls.9 However, studies on the status of dysmenorrhea and associated factors among female high
school students are scarce in southern Ethiopia. Therefore, this study aimed to determine the prevalence of primary
dysmenorrhea and its associated factors among female students at Wolaita soddo town high schools, southern Ethiopia.
Methods
Study Setting and Period
A cross-sectional study was conducted among female students at Wolaita soddo town high schools from October 1–30/
202. Wolaita Soddo town is the capital city of Wolaita zone found southern nation nationalities people regional state of
Ethiopia. It is about 320 km away from Addis Ababa the capital of Ethiopia. There are seven public and four private high
schools in the town serving for a total of 12,792 students of which 6580 are female.
Source Population and Study Population
All female high school students attending their education in Wolaita Soddo town were used as source populations. On the
other hand, all randomly selected female high school students who were present in the four selected high schools during
the data collection period were taken as the study population.
Inclusion and Exclusion Criteria
Female students who undergo their education in the selected high schools in Soddo town were included in the study. On the
other hand, female students who had a known diagnosed medical history of pelvic pathology were excluded from the study.
Sample Size Determination
The required sample size was computed using Open Epi V.3.03 statistical software. The following assumptions were
considered; a confidence level of 95%, marginal error of 5%, design effect = 2 and the prevalence of primary
dysmenorrhea from previous study as 64.7%.13 Based on this assumption the required sample size was 660. Finally,
considering a 10% non-response rate, the required sample size was 733.
1570 https://doi.org/10.2147/IJWH.S384275 International Journal of Women’s Health 2022:14
DovePress
Powered by TCPDF (www.tcpdf.org)
Dovepress Mammo et al
Sampling Technique and Procedure
Study participants were selected from all Soddo town high schools using a multistage stratified sampling technique. First,
the eleven schools were stratified into seven public and four private schools. Then, three schools were selected from the
public and one from the private by using simple random sampling. The selected schools were stratified and proportion
ally allocated to their grades from 9 to 12 and the list of female students from each grade was used as a sampling frame.
Finally, the study participants were selected using a simple random sampling technique after the required sample size was
proportionally allocated to each grade.
Data Collection Tools and Procedures
Data were collected using a pretested structured self-administered questionnaire developed based on review of the related
literature. The questionnaire contained items on socio-demographic and economic factors, menstrual characteristics of
respondents, lifestyle and behavioral related factors, menstrual characteristics and severity of dysmenorrhea was
measured using a 10-point visual analogue scale (VAS).13 The tool was first developed in English and translated into
Amharic, and then translated back to English for consistency. Three BSc nurses and one MPH level health professional
were recruited and trained as data collectors and supervisors, respectively.
Operational Definition
Primary dysmenorrhea: - Students who had pain in the abdomen, thighs and lower back one day before and/or the first to
third day of menstruation in the last 3 months.14
To measure the intensity of primary dysmenorrhea; a 10-point numerical rating scale (NRS) was used to represent the
continuum of girls’ student perception of degree of pain and classified as mild 1–3, moderate 4–7 and severe 8–10.13
Data Processing and Analysis
The collected questioners first manually checked for completeness, and then the data was coded and entered using Epi
data version 3.1 and exported to SPSS version 26 for data analysis. The descriptive statistics, such as frequency,
percentage, mean, standard deviation were performed to describe study population. Bi-variable binary logistic regression
model was computed to test the presence of crude association between primary dysmenorrhea and independent variables
and to identify candidate variables for multivariable analysis. All variables in bi-variable analysis with p < 0.25 were
included in multivariable binary logistic regression analysis. Significance factors were identified based on p-value <0.05.
Finally, text, tables and graphs were used to present the result.
Results
Socio Demographic Characteristics of the Participant and Their Parents
A total of 707 female students participated in the study with a response rate of 96.4%. The mean (SD) age was 16.7 ±
1.32 years with the minimum age of 14 and the maximum age of 19 years. About nine tenth of 636 (90%) of the study
participants were Wolaita by ethnicity. Of the respondents, majority 600 (84.9%) were urban dwellers and nearly two-
third 482 (68.2%) lived with their parents. Regarding parents’ educational status, more than half of the fathers 413
(58.4%) had an educational status of secondary or higher (Table 1).
Obstetric and Gynecological Related Characteristics
Two-third of the participants 478 (67.6%) started menarche at 13–14 years with a mean age of menarche at 13.39 years.
More than half 398 (56.3%) reported a menstrual duration of 3–7 days, and more than three-fourth of them 568 (80.3%)
reported a normal amount of menstrual flow. Nearly, one-tenth 70 (9.9%) of the study participants had ever used
hormonal contraceptives. Moreover, 282 (39.9%) of students reported a family history of dysmenorrhea (Table 2).
International Journal of Women’s Health 2022:14 https://doi.org/10.2147/IJWH.S384275
1571
DovePress
Powered by TCPDF (www.tcpdf.org)
Mammo et al Dovepress
Table 1 Socio- Demographic Characteristics of Female Students at Wolaita Soddo Town High School
Southern Ethiopia, 2021, (n=707)
Variables Category Frequency Percent (%)
Age in years 14–17 481 68
18–19 226 32
Religion Protestant 552 78.1
Orthodox 125 17.7
Muslim 17 2.4
Catholic 9 1.3
Others 4 0.6
Ethnicity Wolaita 636 90
Amhara 31 4.4
Guragie 13 1.8
Gamo 14 2.0
Others 13 1.8
Place of residence Urban 600 84.9
Rural 107 15.9
Living with parents Yes 482 68.2
No 225 31.8
Mothers education Unable to read and write 116 16.4
Read and write 235 33.2
Primary 157 22.2
Secondary 118 16.7
Tertiary 81 11.5
Fathers education Unable to read and write 48 6.8
Read and write 115 16.3
Primary 131 18.5
Secondary 207 29.3
Tertiary 206 29.1
Family size <=4 189 26.7
5–8 456 64.5
≥9 62 8.8
Life Style and Behavioral Characteristics
More than half 417 (59.0%) of the respondents were not involved in regular physical activity. Almost all of the
participants, 690 (97.6%) did not smoke cigarettes. There were 71 (10.0%) participants consumed alcohol and 495
(70.0%) consumed chocolate. Approximately, 397 (56.2%) of them took three or fewer glasses of tea per day.
Approximately 475 (67.2%) and 369 (52.2%) students skipped breakfast and did not get adequate sleep per night,
respectively (Table 3).
Prevalence of Primary Dysmenorrhea and Its Intensity
According to this study, 495 (70.0%) with CI (66.6–73.4%) of the students reported that they were suffering from
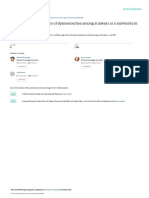
primary dysmenorrhea. According to the numeric rating scale (NRS) experienced mild pain 203 (41.0%), moderate pain
181 (36.6%) and severe pain 111 (22.4%) (Figure 1). More than two-thirds of students 338 (68.3%) had pain that started
a few days before menstrual flow and in almost half of the students 245 (49.5%) pain lasts within one day of menstrual
flow. The location of this pain varies among students and was mostly reported in the lower abdomen 341 (68.9%),
followed by the lower back 103 (20.8%), and abdominal pain that extended to thighs (10.1%). Backache and fatigue were
the most common symptoms associated with primary dysmenorrhea and drinking coffee or tea and getting rest were the
most preferable management options used by students during menstrual pain.
1572 https://doi.org/10.2147/IJWH.S384275 International Journal of Women’s Health 2022:14
DovePress
Powered by TCPDF (www.tcpdf.org)
Dovepress Mammo et al
Table 2 Obstetric and Gynecological Related Characteristics of Female Students at Wolaita Soddo
Town High School Southern Ethiopia, 2021, (n=707)
Variables Categories Frequency Percent (%)
Age at menarche <= 12 133 18.8
13–14 478 67.6
≥ 15 96 13.6
Duration of menstrual flow < 3 days 206 29.1
3–7 days 398 56.3
>7 days 103 14.6
Amount of blood flow <= 1 pad/day 33 4.7
2–4 pads/day 568 80.3
≥ 5 pads/day 106 15.0
Length of menstrual cycle < 21 days 45 6.4
21–35 days 653 92.4
>35 days 9 1.3
Menstrual cycle regularity Yes 298 42.1
No 409 57.9
Hormonal contraceptive use Yes 70 9.9
No 637 90.1
Circumcision history Yes 487 68.9
No 220 31.1
Child birth Yes 26 3.7
No 681 96.3
Family history Yes 282 39.9
No 425 60.1
Table 3 Life Style and Behavioral Characteristics of Female Students at Wolaita Soddo Town High
School Southern Ethiopia, 2021, (n=707)
Variables Categories Frequency Percent (%)
Physical activity Yes 290 41.0
No 417 59.0
Cigarette smoking Yes 17 2.4
No 690 97.6
Alcohol consumption Yes 71 10.0
No 636 90.0
Chocolate consumption Yes 495 70.0
No 212 30.0
Coffee intake in cups Not at all 290 41.0
< 3 cups 257 36.4
≥ 3 cups 160 22.6
Tea drinking Not at all 119 16.8
< 4 glasses 397 56.2
≥ 4 glasses 191 27.0
Sugar intake Not at all 65 9.2
Minimal 312 44.1
Moderate 281 39.7
Excessive 49 6.9
Skipping breakfast Yes 475 67.2
No 232 32.8
Sleeping pattern in hours < 7hrs 369 52.2
≥ 7hr 338 47.8
Sexual activity Yes 290 41.0
No 417 59.0
International Journal of Women’s Health 2022:14 https://doi.org/10.2147/IJWH.S384275
1573
DovePress
Powered by TCPDF (www.tcpdf.org)
Mammo et al Dovepress
Figure 1 Pie chart for intensity of menstrual pain among female students at Wolaita soddo town high school southern Ethiopia, 2021.
Factors Associated with Primary Dysmenorrhea
Participants whose age 14–17 years were 2.55 times more likely to experience primary dysmenorrhea than those aged
≥18 years (AOR 2.55; 95% CI (1.77, 3.68)). Long duration of menstrual flow was 2.72 times more likely to develop
primary dysmenorrhea compared to shorter duration (AOR 2.72; 95% CI (1.42, 5.17)). Students who had irregular
menstruation were 2.39 times more likely to have primary dysmenorrhea compared to students who had regular
menstruation (AOR 2.39; 95% CI (1.68, 3.41)), and participants who had a family history of dysmenorrhea were 2.46
times more likely to have primary dysmenorrhea than those who did not had a family history of dysmenorrhea (AOR
2.46; 95% CI (1.67, 3.64)). Students who skipped breakfast were 1.62 times more likely to develop primary dysmenor
rhea compared with those who ate breakfast (AOR 1.62; 95% CI (1.13, 2.33)) (Table 4).
Discussion
Adolescence is the transition period from puberty to early adulthood during which physical, emotional and psychological
changes occur in the body. Menarche is a significant landmark of adolescence that prepares girls for future motherhood.
The present study was conducted to assess one of the menstrual problems; associated with primary dysmenorrhea among
adolescent girls.
The prevalence of primary dysmenorrhea among the study participants was 70%. Of these, 203 (41.0%), 181 (36.6%),
and 111 (22.4%) rated their pain intensity as mild, moderate, and severe respectively. The findings of this study were
comparable with those of previous studies reported in Debre Markos (69.3%),9 Hararegie (69.26%),15 Ghana (68.1%)16
and Brazil 73%.17 However, the prevalence in this study was relatively lower than that, reported in Egypt 76.1%,18 Benin
78.3%,19 Oman 94%,4 Kuwait 85.6%20 and Romania 78.4%.29 The possible reasons for the discrepancies in the
estimated prevalence may be the socio-cultural differences of the study participants in pain perception during menstrua
tion and lifestyle differences.
In contrast, the prevalence was relatively higher than that reported in studies conducted among university students in
Hawassa 51.5%,11 Nigeria 51.1%,6 China 41.7%,5 South Korea 58.8%,21 Georgia 52%.22 This inconsistency is probably
because the prevalence of primary dysmenorrhea is higher among adolescents and decreases with increasing age,
whereas in studies performed among university students age range between 18 and 29 years.
In this study, younger age was significantly associated with primary dysmenorrhea. Participants aged <14–17 years
were 2.55 times more likely to experience primary dysmenorrhea than those aged ≥18 years. This finding was in line
with those of the studies conducted in Benin,19 Nigeria6 and Iran.23 This may be because primary dysmenorrhea is
more frequent in young virgin girls and those who have not given birth and its prevalence decreases with increas
ing age.
1574 https://doi.org/10.2147/IJWH.S384275 International Journal of Women’s Health 2022:14
DovePress
Powered by TCPDF (www.tcpdf.org)
Dovepress Mammo et al
Table 4 Factors Associated with Primary Dysmenorrhea Among Female Students at Wolaita Soddo Town High School Southern
Ethiopia, 2021, (n=707)
Variables Categories Primary Dysmenorrhea COR (95% CI) AOR (95% CI)
Yes No
Age in years 14–17 368 113 2.54 (1.81–3.56) 2.55 (1.77–3.68) **
18–19 127 99 1 1
Fathers education Unable to read and write 34 14 0.86 (0.43–1.73) 0.83 (0.39–1.75)
Read and write 76 39 0.69 (0.42–1.14) 0.75 (0.44–1.28)
Primary 83 48 0.61 (0.38–0.98) 0.64 (0.38–1.07)
Secondary 150 57 0.93 (0.60–1.44) 0.92 (0.57–1.48)
Tertiary 152 54 1 1
Family size <= 4 141 48 1 1
5–8 308 148 0.70 (0.48–1.03) 0.98 (0.64–1.49)
≥9 46 16 0.98 (0.50–1.88) 1.67 (0.81–3.42)
Duration of menstrual flow < 3 days 134 72 1 1
3–7 days 275 123 1.20 (0.84–1.72) 1.18 (0.79–1.74)
>7 days 86 17 2.71 (1.50–4.92) 2.72 (1.42–5.17) **
Cycle regularity Yes 178 120 1 1
No 317 92 2.32 (1.67–3.22) 2.39 (1.68–3.40) **
Family history Yes 225 57 2.27 (1.59–3.22) 2.46 (1.67–3.64) **
No 270 155 1 1
Sugar intake Not at all 50 15 1 1
Minimal 210 102 0.62 (0.33–1.15) 0.53 (0.26–1.05)
Moderate 195 86 0.68 (0.36–1.28) 0.63 (0.31–1.26)
Excessive 40 9 1.33 (0.53–3.36) 1.12 (0.42–3.01)
Breakfast skipping Yes 353 122 1.83 (1.31–2.56) 1.62 (1.13–2.33) **
No 142 90 1 1
Note: ** Indicates variables significant at p-value <0.01.
Abbreviations: COR, crude odds ratio; AOR, adjusted odds ratio; CI, confidence interval.
A longer duration of menstrual bleeding (>7 days) was an important risk factor for primary dysmenorrhea; and long
duration of menstrual flow (>7) was 2.72 times more likely to develop primary dysmenorrhea. This finding is supported
by studies from Mekele,12 Nigeria,6 South Korea,21 Italy,24 and India.25 Menstrual irregularity was also one of the
contributing factors for primary dysmenorrhea. Those students who had irregular menstruation were 2.39 times more
likely to have primary dysmenorrhea. This finding was consistent with a study in Debre Tabor,3 Gondar,13 Hawassa,11
Ghana16 and Egypt.18 The possible explanation might be due to an immature hypothalamopituitary- ovarian axis or it
may be due to changing trends of lifestyle, changing dietary habits and tough competition which is responsible for
psychological stress among adolescents and also the irregularity of menstruation which could fluctuate steroid hormones
and might lead to primary dysmenorrhea.26
Family history of dysmenorrhea was another predictor for the presence of primary dysmenorrhea. It was found that
primary dysmenorrhea was 2.4 time more prevalent among those respondents who have family history of dysmenorrhea.
This was supported by a study in Hawassa,11 Debre Tabor,3 Gondar,13 Benin,19 India25 and Georgia secondary school
students;22 this could be related to behaviors that girls learn from their mothers for the possibility of societal reward or
that control pain. It might have also a psychological impact such as daughters may react to menstruation similarly like
their mothers and they may share the same attitude and taboos towards menses.27
Our study demonstrated that breakfast skipping significantly increases the prevalence of primary dysmenorrhea.
Students who skipped their breakfast were 1.62 times more likely to develop primary dysmenorrhea. This finding is
compatible with studies done in India,25 Georgia,22 and China;9 but contrasts with studies done in Hawassa University
that breakfast skipping preventive rather than risk.11 Nevertheless, it has been demonstrated that diet can influence
International Journal of Women’s Health 2022:14 https://doi.org/10.2147/IJWH.S384275
1575
DovePress
Powered by TCPDF (www.tcpdf.org)
Mammo et al Dovepress
menstrual regularity. Specific dietary nutrients may have direct effects or exert their effects by altering the status of
circulating sex steroids. So, as inadequate nutrition is a cause of low energy availability and can alter hormonal status.22
Limitation of the Study
The limitation of this study is the fact that temporal relations could not be established, since the study design was a cross-
sectional study. Since the study variables were measured by the participant self-reporting, and there could be a recall bias
as the students were asked for events within the last three months. However, this study still provides important insights
regarding primary dysmenorrhea, and associated risk factors among female secondary school students.
Conclusions
A high proportion of female secondary school students were suffered from primary dysmenorrhea. Students with younger
age, long duration of menstrual flow, irregular cycle, family history of dysmenorrhea, and breakfast skipping were more
likely to develop primary dysmenorrhea.
Abbreviations
AOR, adjusted odd ratio; CI, confidence interval; COR, crude odd ratio; SD, standard deviation; SPSS, Statistical
Package for Social Science; VAS, visual analogue scale.
Data Sharing Statement
All the minimal data sets used to reach the conclusions drawn in the manuscript are included within the manuscript.
Ethical Approval and Consent to Participants
Ethical clearance letter was obtained from Wolaita Soddo University, College of Health Sciences; School of Public
Health institutional review board (IRB) (Ref. No. CRCSD9/03/2014). Official letter was received from the school of
public health and submitted to Soddo town education office in order to get official letter of permission for data collection.
Informed consent was obtained for respondents above 18 years of old and for those who are under 18 year’s oral assent
from them and consent obtained from parents before collecting the data. All relevant ethical principles under the Helsinki
declaration were followed and respected.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design,
execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically
reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article
has been submitted; and agree to be accountable for all aspects of the work.
Disclosure
The authors declare that no one has competing interests in this work.
References
1. Bernardi M, Lazzeri L, Perelli F, Reis FM, Petraglia F. Dysmenorrhea and related disorders. F1000Research. 2017;6:1645. doi:10.12688/
f1000research.11682.1
2. Lefebvre G, Pinsonneault O, Antao V, et al. Primary dysmenorrhea consensus guideline. J Obstet Gynaecol Can. 2005;27(12):1117–1146.
3. Giletew A, Bekele W. Prevalence and associated factors of primary dysmenorrhea among Debre Tabor University students, north Central Ethiopia.
Int J Biomed Eng Clin Sci. 2019;4(4):70–74.
4. Al-Kindi R, Al-Bulushi A. Prevalence and impact of dysmenorrhoea among Omani high school students. Sultan Qaboos Univ Med J. 2011;11
(4):485.
5. Hu Z, Tang L, Chen L, Kaminga AC, Xu H. Prevalence and risk factors associated with primary dysmenorrhea among Chinese female university
students: a cross-sectional study. J Pediatr Adolesc Gynecol. 2020;33(1):15–22. doi:10.1016/j.jpag.2019.09.004
6. Onu A, Aluh D, Ikehi M Prevalence and management of dysmenorrhea among secondary school adolescents in Enugu state, Nigeria; 2020.
1576 https://doi.org/10.2147/IJWH.S384275 International Journal of Women’s Health 2022:14
DovePress
Powered by TCPDF (www.tcpdf.org)
Dovepress Mammo et al
7. Dengeingei T, Uusiku L, Tuhadeleni ON, Lifalaza A. Assessing knowledge and practice regarding the management of dysmenorrhea among
students at university of Namibia Rundu campus. Glob J Health Sci. 2020;12(9):105. doi:10.5539/gjhs.v12n9p105
8. Assefa N, Demissie A, Hailemeskel S. Primary dysmenorrhea magnitude, associated risk factors, and its effect on academic performance: evidence
from female university students in Ethiopia. Int J Womens Health. 2016;8:489. doi:10.2147/IJWH.S112768
9. Muluneh AA, Gebreslasie KZ, Anteneh KT, Kassa ZY. Prevalence and associated factors of dysmenorrhea among secondary and preparatory
school students in Debremarkos town, North-West Ethiopia. BMC Womens Health. 2018;18(1):1–8. doi:10.1186/s12905-018-0552-x
10. Sukalingam K, Ganesan K. Health-related quality of life in young adult girls with dysmenorrhea among university medical students in Shah Alam,
Malaysia: a cross-sectional study. Recent Adv Biol Med. 2016;2(2016):968. doi:10.18639/RABM.2016.02.343082
11. Tadese M, Kassa A, Muluneh AA, Altaye G. Prevalence of dysmenorrhoea, associated risk factors and its relationship with academic performance
among graduating female university students in Ethiopia: a cross-sectional study. BMJ open. 2021;11(3):e043814. doi:10.1136/bmjopen-2020-043814
12. Yesuf TA, Eshete NA, Sisay EA. Dysmenorrhea among university health science students, northern Ethiopia: impact and associated factors.
Int J Reprod Med. 2018;2018:23.
13. Azagew AW, Kassie DG, Walle TA. Prevalence of primary dysmenorrhea, its intensity, impact and associated factors among female students’ at
Gondar town preparatory school, Northwest Ethiopia. BMC Womens Health. 2020;20(1):1–7. doi:10.1186/s12905-019-0873-4
14. Sahin S, Ozdemir K, Unsal A, Arslan R. Review of frequency of dysmenorrhea and some associated factors and evaluation of the relationship
between dysmenorrhea and sleep quality in university students. Gynecol Obstet Invest. 2014;78(3):179–185. doi:10.1159/000363743
15. Mohammed H, Hassen N, Musa A. Dysmenorrhea and associated factors among secondary school students in East Hararghe Zone, Eastern
Ethiopia. East Afr J Health Biomed Sci. 2019;3(1):39–48.
16. Acheampong K, Baffour-Awuah D, Ganu D, et al. Prevalence and predictors of dysmenorrhea, its effect, and coping mechanisms among
adolescents in Shai Osudoku District, Ghana. Obstet Gynecol Int. 2019;2019:23.
17. Pitangui ACR, Gomes MR, Lima AS, Schwingel PA, Albuquerque AP, de Araújo RC. Menstruation disturbances: prevalence, characteristics, and
effects on the activities of daily living among adolescent girls from Brazil. J Pediatr Adolesc Gynecol. 2013;26(3):148–152. doi:10.1016/j.
jpag.2012.12.001
18. Mohamed EM. Epidemiology of dysmenorrhea among adolescent students in Assiut City, Egypt. Life Sci J. 2012;9(1):348–353.
19. Sidi I, Hounkpatin B, Obossou A, et al. Primary dysmenorrhea in the schools of Parakou: prevalence, impact and therapeutic approach. Gynecol
Obstet. 2016;6(376):2161–0932.1000376.
20. Al-Matouq S, Al-Mutairi H, Al-Mutairi O, et al. Dysmenorrhea among high-school students and its associated factors in Kuwait. BMC Pediatr.
2019;19(1):1–12. doi:10.1186/s12887-019-1442-6
21. Jang IA, Kim MY, Lee SR, Jeong KA, Chung HW. Factors related to dysmenorrhea among Vietnamese and Vietnamese marriage immigrant
women in South Korea. Obstet Gynaecol Sci. 2013;56(4):242–248. doi:10.5468/ogs.2013.56.4.242
22. Gagua T, Tkeshelashvili B, Gagua D. Primary dysmenorrhea: prevalence in adolescent population of Tbilisi, Georgia and risk factors. J Turk Ger
Gynecol Assoc. 2012;13(3):162. doi:10.5152/jtgga.2012.21
23. Habibi N, Huang MSL, Gan WY, Zulida R, Safavi SM. Prevalence of primary dysmenorrhea and factors associated with its intensity among
undergraduate students: a cross-sectional study. Pain Manag Nurs. 2015;16(6):855–861. doi:10.1016/j.pmn.2015.07.001
24. Grandi G, Ferrari S, Xholli A, et al. Prevalence of menstrual pain in young women: what is dysmenorrhea? J Pain Res. 2012;5:169. doi:10.2147/
JPR.S30602
25. Kural M, Noor NN, Pandit D, Joshi T, Patil A. Menstrual characteristics and prevalence of dysmenorrhea in college going girls. J Fam Med Prim
Care. 2015;4(3):426. doi:10.4103/2249-4863.161345
26. Montoya JS, Cabezza AH, Rojas OM, Navarrete RC, Keever M. Menstrual disorders in adolescents. Bol Med Hosp Infant Mex. 2012;69(1):60–72.
27. Shiferaw MT, Wubshet M, Tegabu D. Menstrual problems and associated factors among students of Bahir Dar University, Amhara National
Regional State, Ethiopia: a cross-sectional survey. Pan Afr Med J. 2014;17:67.
28. Omidvar S, Bakouei F, Amiri FN, et al. Primary dysmenorrhea and menstrual symptoms in Indian female students: prevalence, impact and
management. Glob J Health Sci. 2016;8:135. doi:10.5539/gjhs.v8n8p135
29. Sima RM, Sulea M, Radosa JC, et al. The prevalence, management and impact of dysmenorrhea on medical students’ lives—A multicenter study.
Healthcare. 2022;10(1):157. doi:10.3390/healthcare10010157
International Journal of Women’s Health Dovepress
Publish your work in this journal
The International Journal of Women’s Health is an international, peer-reviewed open-access journal publishing original research, reports,
editorials, reviews and commentaries on all aspects of women’s healthcare including gynecology, obstetrics, and breast cancer. The manuscript
management system is completely online and includes a very quick and fair peer-review system, which is all easy to use. Visit http://www.
dovepress.com/testimonials.php to read real quotes from published authors.
Submit your manuscript here: https://www.dovepress.com/international-journal-of-womens-health-journal
International Journal of Women’s Health 2022:14 DovePress 1577
Powered by TCPDF (www.tcpdf.org)
You might also like
- Bio Signature Modulation ExplainedDocument4 pagesBio Signature Modulation ExplainedChris Gregory100% (4)
- Tantra For MenDocument18 pagesTantra For MenDeba Brata100% (1)
- Gynecologic Problems of Childhood: Anne Margrette C. VelasquezDocument46 pagesGynecologic Problems of Childhood: Anne Margrette C. VelasquezAnne Margrette Velasquez100% (1)
- Ijwh-14-517 TiruyeDocument11 pagesIjwh-14-517 TiruyeDaraaswanNo ratings yet
- FRPH 04 939035Document7 pagesFRPH 04 939035DaraaswanNo ratings yet
- Determinants of Female Genital Mutilation Among Under Five-Year Children in Motta Town, Northwest Ethiopia, 2022: Unmatched Case Control StudyDocument11 pagesDeterminants of Female Genital Mutilation Among Under Five-Year Children in Motta Town, Northwest Ethiopia, 2022: Unmatched Case Control StudysamsiebopNo ratings yet
- Wong2010Document4 pagesWong2010dara intanNo ratings yet
- Prevalence of Dysmenorrhea and Its Effects On SchoDocument7 pagesPrevalence of Dysmenorrhea and Its Effects On SchoMarilyn RebatoNo ratings yet
- Epidemiology of Dysmenorrhea Among University of Dschang Students (West Region, Cameroon) : A Cross-Sectional StudyDocument6 pagesEpidemiology of Dysmenorrhea Among University of Dschang Students (West Region, Cameroon) : A Cross-Sectional StudyInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Ijwh 287715 Teenage Pregnancy and Its Associated Factors in Eastern EthiDocument12 pagesIjwh 287715 Teenage Pregnancy and Its Associated Factors in Eastern EthiJinky Mendoza CalingasanNo ratings yet
- Dude Ja 2016Document5 pagesDude Ja 2016Mushfiqur RahmanNo ratings yet
- BacaDocument9 pagesBacaLivianadrNo ratings yet
- Dysmenorrhoea Among Adolescent Girls - Characteristics and Symptoms Experienced During MenstruationDocument8 pagesDysmenorrhoea Among Adolescent Girls - Characteristics and Symptoms Experienced During MenstruationUlfa Diya AtiqaNo ratings yet
- Problem Pada MenstruasiDocument8 pagesProblem Pada MenstruasiInna MeratiNo ratings yet
- 1-S2.0-S1110569017302935-MainDocument5 pages1-S2.0-S1110569017302935-Maindara intanNo ratings yet
- Undernutrition Among Pregnant Women in Rural Communities in Southern EthiopiaDocument7 pagesUndernutrition Among Pregnant Women in Rural Communities in Southern EthiopiaJenny Rose PangdaoNo ratings yet
- JournalDocument5 pagesJournalNatalia ChandraNo ratings yet
- Prevalence of Dysmenorrhoea and Its Associated Factors Among Female Medical Students at Kampala International University Western CampusDocument15 pagesPrevalence of Dysmenorrhoea and Its Associated Factors Among Female Medical Students at Kampala International University Western CampusKIU PUBLICATION AND EXTENSIONNo ratings yet
- Prevalence and Pattern of Dysmenorrhea Among SeconDocument6 pagesPrevalence and Pattern of Dysmenorrhea Among SeconmilionNo ratings yet
- Jkachn 24 3 264.ko - enDocument9 pagesJkachn 24 3 264.ko - enSonali DakhoreNo ratings yet
- Explore The Knowledge and Impact On Dysmenorrhea Among Nursing Students of Selected CollegeDocument5 pagesExplore The Knowledge and Impact On Dysmenorrhea Among Nursing Students of Selected CollegeEditor IJTSRDNo ratings yet
- JMDH 16 2271Document8 pagesJMDH 16 2271fatcaterpillarNo ratings yet
- Prevalence and Factors Affecting Enuresis Amongst Primary School ChildrenDocument5 pagesPrevalence and Factors Affecting Enuresis Amongst Primary School ChildrenAshu SharmaNo ratings yet
- Prevalence and Predictors of Dysmenorrhea Among STDocument6 pagesPrevalence and Predictors of Dysmenorrhea Among STAngel 冯晓君No ratings yet
- 1 SMDocument6 pages1 SMedi_wsNo ratings yet
- 10 1 1 976 384 PDFDocument7 pages10 1 1 976 384 PDFAdam RiskyNo ratings yet
- Menstrual Disorders Among Zagazig University Students, Zagazig, EgyptDocument6 pagesMenstrual Disorders Among Zagazig University Students, Zagazig, EgyptErsi Dwi Utami SiregarNo ratings yet
- SouthwestDocument7 pagesSouthwestDamesa MiesaNo ratings yet
- Jurnal Vulva HygienDocument10 pagesJurnal Vulva HygienDinaMerianaVanrioNo ratings yet
- Research ArticleDocument11 pagesResearch ArticleJabou NjieNo ratings yet
- Severity of Primary DysmenorrheaDocument7 pagesSeverity of Primary Dysmenorrheasfs_idxNo ratings yet
- Effectiveness of Audio Drama On Menstrual Hygiene and Management of Minor Ailments of Menstruation Upon Knowledge and Practice Among Visually Challenged GirlsDocument5 pagesEffectiveness of Audio Drama On Menstrual Hygiene and Management of Minor Ailments of Menstruation Upon Knowledge and Practice Among Visually Challenged GirlsInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Research ArticleDocument9 pagesResearch ArticleshahrasyiddNo ratings yet
- Prevalency DismenoireDocument8 pagesPrevalency DismenoireFatiya MuthmainnahNo ratings yet
- Effect of Health Education Program For Mothers of Children With Enterobius Vermicularis at Assiut University Children HospitalDocument30 pagesEffect of Health Education Program For Mothers of Children With Enterobius Vermicularis at Assiut University Children HospitalancillaagraynNo ratings yet
- Use OnlyDocument4 pagesUse OnlyDavid AyibonteyNo ratings yet
- A Study To Identify Premenstrual Syndrome and Their Management Adopted by Adolescent Girls Studying in Selected High School at Jabalpur M.PDocument4 pagesA Study To Identify Premenstrual Syndrome and Their Management Adopted by Adolescent Girls Studying in Selected High School at Jabalpur M.PEditor IJTSRDNo ratings yet
- 80 ArticleText 355 1 10 20190816 PDFDocument8 pages80 ArticleText 355 1 10 20190816 PDFnay laNo ratings yet
- Depression Among University Students in Kenya: Prevalence and Sociodemographic CorrelatesDocument7 pagesDepression Among University Students in Kenya: Prevalence and Sociodemographic CorrelatesDani AnyikaNo ratings yet
- RRTM 327129 Isolation of Escherichia Coli and Its Associated Risk FactorDocument8 pagesRRTM 327129 Isolation of Escherichia Coli and Its Associated Risk FactorAssefa AlemuNo ratings yet
- PembahasanDocument7 pagesPembahasanDini LianiNo ratings yet
- Jurnal DysmenorrheaDocument10 pagesJurnal Dysmenorrheaanisah tri agustiniNo ratings yet
- IJWH 352348 Determinants of Premature Rupture of Membrane Prom Among PDocument12 pagesIJWH 352348 Determinants of Premature Rupture of Membrane Prom Among PCitaNo ratings yet
- 1000-Article Text-3267-1-10-20221210Document6 pages1000-Article Text-3267-1-10-20221210Jasmine Hasna N RNo ratings yet
- 357 1278 1 PBDocument7 pages357 1278 1 PBPika RahayuNo ratings yet
- EN Epidemiology of Dysmenorrhea Among FemalDocument6 pagesEN Epidemiology of Dysmenorrhea Among FemalRuth RachmawatyNo ratings yet
- The Magnitude of Failed Induction of Labor and Associated Factors Among Women Delivered at Public Hospitals of Arsi Zone Southeast Ethiopia 2020 ADocument14 pagesThe Magnitude of Failed Induction of Labor and Associated Factors Among Women Delivered at Public Hospitals of Arsi Zone Southeast Ethiopia 2020 ABeti yemaneNo ratings yet
- The Prevalence and Risk Factors of Dysmenorrhea - Dyto Prasetya BuwanaDocument10 pagesThe Prevalence and Risk Factors of Dysmenorrhea - Dyto Prasetya Buwana0406 Dyto Prasetya BuwanaNo ratings yet
- Prevalence of Anaemia and Dysmenorrhoea Among Adolescent GirlsDocument5 pagesPrevalence of Anaemia and Dysmenorrhoea Among Adolescent GirlssafiraNo ratings yet
- BMC Public Health: Intestinal Parasites Prevalence and Related Factors in School Children, A Western City Sample-TurkeyDocument6 pagesBMC Public Health: Intestinal Parasites Prevalence and Related Factors in School Children, A Western City Sample-TurkeyVelazquez Rico Cinthya MontserrathNo ratings yet
- Prevalence of Dysmenorrhea Associated Factors PainDocument23 pagesPrevalence of Dysmenorrhea Associated Factors PainDaraaswanNo ratings yet
- Depression Among Pregnant Women and Associated Factors in Hawassa City, Ethiopia: An Institution-Based Cross-Sectional StudyDocument6 pagesDepression Among Pregnant Women and Associated Factors in Hawassa City, Ethiopia: An Institution-Based Cross-Sectional Studyevita juniarNo ratings yet
- PRBM 13 1365Document8 pagesPRBM 13 1365Dewi Utami IrianiNo ratings yet
- Hubungan Peran Keluarga Dengan Harga Diri Pada Penderita Penyakit KustaDocument10 pagesHubungan Peran Keluarga Dengan Harga Diri Pada Penderita Penyakit KustaEnggar RahmanNo ratings yet
- Parker2009 - Menstruasi PDFDocument8 pagesParker2009 - Menstruasi PDFtiaraNo ratings yet
- Epidemiology of Dysmenorrhea Among Female Adolescents in CentralDocument7 pagesEpidemiology of Dysmenorrhea Among Female Adolescents in CentralRuth RachmawatyNo ratings yet
- Awareness On Menstrual Hygiene Among Deaf Mute Adolescents With Special Reference To in Thrissur District, KeralaDocument5 pagesAwareness On Menstrual Hygiene Among Deaf Mute Adolescents With Special Reference To in Thrissur District, KeralaEditor IJTSRDNo ratings yet
- FileDocument19 pagesFileTanushikha SangwanNo ratings yet
- Jurnal Tentang Asfiksia-DikonversiDocument12 pagesJurnal Tentang Asfiksia-DikonversiLaila Al-GifariahNo ratings yet
- The Impact of Menstrual Symptoms On Everyday LifeDocument7 pagesThe Impact of Menstrual Symptoms On Everyday LifeEiman Khowaja (22GJKB-CLSTEC)No ratings yet
- Premenstrual Syndrome Frequency, Premenstrual Syndrome Coping Strategies and Factors Affecting Premenstrual Syndrome in University Students in TurkeyDocument18 pagesPremenstrual Syndrome Frequency, Premenstrual Syndrome Coping Strategies and Factors Affecting Premenstrual Syndrome in University Students in TurkeyGlobal Research and Development ServicesNo ratings yet
- MafraDocument33 pagesMafrayvette kinyuyNo ratings yet
- Acne: Current Concepts and ManagementFrom EverandAcne: Current Concepts and ManagementDae Hun SuhNo ratings yet
- Uterine FibroidsDocument47 pagesUterine FibroidsMoh Aldhy HusaintNo ratings yet
- Project Work: InvestigatoryDocument16 pagesProject Work: InvestigatoryRahul DasNo ratings yet
- Legalization Abortion in IndiaDocument13 pagesLegalization Abortion in IndiaNeetish Kumar HandaNo ratings yet
- 9th - Cystic OvariesDocument25 pages9th - Cystic Ovariesnoor aineNo ratings yet
- 4.2 Deviations From The Mendelian InheritanceDocument62 pages4.2 Deviations From The Mendelian InheritancejiaenNo ratings yet
- Mark SchemeDocument9 pagesMark SchemeJanani MNo ratings yet
- Comprehensive Examination: Assumption Montessori SchoolDocument9 pagesComprehensive Examination: Assumption Montessori Schoolshincee23No ratings yet
- Artificial Insemination ProcedureDocument9 pagesArtificial Insemination ProcedureJyotiNo ratings yet
- Med Trans ReviewerDocument1 pageMed Trans ReviewerDenise CerdaNo ratings yet
- Alchemical Taoism: Five Element TheoryDocument13 pagesAlchemical Taoism: Five Element Theoryמיקי קליין יוגהNo ratings yet
- Causes of Maternal Mortality and MorbidityDocument20 pagesCauses of Maternal Mortality and MorbidityRaNa MaYaaNo ratings yet
- Spontaneous AbortionDocument17 pagesSpontaneous Abortionanon_985338331No ratings yet
- 3893 ID Faktor Risiko Yang Mempengaruhi Kejadian Dismenore PrimerDocument8 pages3893 ID Faktor Risiko Yang Mempengaruhi Kejadian Dismenore PrimerNur lailah sakinahNo ratings yet
- Jadwal Semester 2 Februari - Juli 2020: Hari Tanggal JAM KelompokDocument30 pagesJadwal Semester 2 Februari - Juli 2020: Hari Tanggal JAM KelompokFelicia AcraminNo ratings yet
- Congenital Adrenal HyperplasiaDocument28 pagesCongenital Adrenal HyperplasiaWindelyn Gamaro0% (1)
- DR Stephen Chang - Deer ExerciseDocument1 pageDR Stephen Chang - Deer ExerciseDolf Cheng100% (2)
- 3 Placenta Previa Nursing Care PlansDocument7 pages3 Placenta Previa Nursing Care PlansAjay RajpootNo ratings yet
- Sterilization of DogsDocument18 pagesSterilization of Dogsjo12joseNo ratings yet
- Ms Sabiha ReportDocument4 pagesMs Sabiha Reportzafir alamNo ratings yet
- Sakila MurmuDocument47 pagesSakila MurmuSakila murmuNo ratings yet
- The Ultimate Male Orgasm PDFDocument4 pagesThe Ultimate Male Orgasm PDFDavid Hosam50% (2)
- Biology SSC - Ii: SECTION - B (Marks 30)Document2 pagesBiology SSC - Ii: SECTION - B (Marks 30)Bushra BushraNo ratings yet
- BIO220Document6 pagesBIO220imma haznaNo ratings yet
- Geself Midterms ReviewerDocument13 pagesGeself Midterms ReviewerKim OpenaNo ratings yet
- Gonorrhea: by Siena Kathleen V. Placino BSN-IV Communicable Disease Nursing C.I.: Dr. Dario V. SumandeDocument38 pagesGonorrhea: by Siena Kathleen V. Placino BSN-IV Communicable Disease Nursing C.I.: Dr. Dario V. SumandeSiena100% (1)
- Biology Rose 09Document68 pagesBiology Rose 09kukaraja77No ratings yet
- Stamina Guide Orgasm Top TipsDocument26 pagesStamina Guide Orgasm Top TipsJames Jameson57% (7)