Professional Documents
Culture Documents
Essential Paediatrics Course Book 2023
Essential Paediatrics Course Book 2023
Uploaded by
alextkijiji_81403773Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Essential Paediatrics Course Book 2023
Essential Paediatrics Course Book 2023
Uploaded by
alextkijiji_81403773Copyright:
Available Formats
Essential Paediatrics
E-coursebook
About Dr Clarke
Dr Clarke’s passion is medical education. For
twenty years he was Associate Dean in the London
Deanery, helping clinicians in both primary and
secondary care improve their teaching skills.
With a background in both hospital medicine and
general practice, Dr Clarke is a Fellow of the Royal
College of Physicians and of the Royal College of
General Practitioners. His most recent clinical work
was in general practice in North London and
Hertfordshire.
As an independent provider of medical education,
his main focus has been on helping students
prepare for their final examinations. Although Bob
formally retired in 2021, he continues to provide
occasional revision courses.
About the paediatrics course team
Bob has collaborated with a team of consultants and registrars in developing and
delivering this course. All members of the teaching team have been selected because
of their track record of excellence in teaching. On the January 2023 course, Bob will be
teaching with two consultant paediatricians: Dr Hannah Jacob and Dr Gareth Lewis.
This e-coursebook is provided for the individual personal use of students
who have booked the “Essential Paediatrics” on-line course.
It must not be distributed or shared with others in any format and must not
be uploaded to any other part of the internet.
Ask Doctor Clarke
Ask Doctor Clarke Revision Courses
• Essential Medicine
• Essential Surgery
• Essential Paediatrics
The Ask Doctor Clarke team has been providing the UK's most popular and highly
acclaimed revision courses for many years. Each course is high yield, covering the
most popular examination topics in a single day. The lecturers, who have collaborated
with Dr Clarke in developing and evaluating the course materials, have been selected
for their track record of excellence in teaching.
After your exams
• Please email support@askdoctorclarke.com
• What were your clinical cases?
• What questions were you asked?
• Your report will help to ensure the courses are fully up to date
Images credits and copyright
Where no attribution is made, images and illustrations are © Dr R Clarke. Most of the remaining images
are in the public domain, mainly from Wikimedia, but occasionally from Pixabay and Flickr. Creative
commons licensing details can be found at: https://creativecommons.org/licenses/by/4.0/ Authorship is
shown alongside the images. Links to the originals and details of any editing are given on page 85. We
have tried to trace and request permission from all authors of copyright images, whom we have
acknowledged, but in some cases this may not have been feasible. If contacted, we will be pleased to
rectify any errors or omissions as soon as possible.
Important note
These notes are presented in good faith and every effort has been taken to ensure their accuracy.
Nevertheless, it is possible that some errors may have been overlooked. It is always important to check
such information, particularly drug indications, contraindications and dosages, with your clinical teachers
and with other reliable sources such as the BNF for Children. Disclaimer: no responsibility can be taken
by Doctor Clarke or his co-lecturers for any loss, damage or injury occasioned to any person acting or
refraining from action as a result of this information. Please give feedback on this document and report
any inaccuracies or ambiguities to the email address above.
Ask Doctor Clarke
Essential Paediatrics
Essential Paediatrics
Programme
Page
08.30 Registration
09.00 Paediatric Cardiology 4
10.30 Emergencies in Children 20
11.10 Coffee
11.30 Two Cases 27
12.00 Gastroenterology 35
13.00 Lunch
13.45 Respiratory Disease 47
14.45 Three Cases 59
15.30 Tea
15.45 Neonates 67
16.40 Neurology and Development 74
17.30 Close
Important Note
This e-coursebook is provided for the individual personal use of students
who have booked the “Essential Paediatrics” on-line course.
It must not be distributed or shared with others in any format and must not
be uploaded to any other part of the internet.
© Dr R Clarke 2023 support@askdoctorclarke.com 3
Essential Paediatrics
Paediatric Cardiology: Quiz
Question 1
Down syndrome: what abnormalities are shown in this picture?
What cardiac abnormalities are typically associated?
V Miles: with permission
Question 2
What features would suggest that a murmur is innocent?
Question 3
What are the physical signs of a small VSD?
Question 4
What are the four components of Fallot’s tetralogy?
© Dr R Clarke 2023 support@askdoctorclarke.com 4
Essential Paediatrics
Introduction
Course aims
• Cover the essentials of paediatrics in a single day
• Focus on areas popular in exams
• Make sense of areas that most people find difficult
• Quizzes and question stops
• Opportunities for questions during breaks
• Buzz words
Memory aids
• Deep understanding plus
• Repetition, songs, poems, mnemonics
• For example: pyloric stenosis buzz words:
hypokalaemic, hypochloraemic metabolic
alkalosis
Bronchiolitis poem
In kids under one, there’s a common disease
With cough, snotty nose, crackles and wheeze
Always record the respiratory rate
If it’s severe, they’ll desaturate
Signs of shock: “I SHOCKS” Normal respiratory and heart rates for children (APLS 2016)
I Increased respiratory rate
S sinus tachycardia
H hypotension
O oliguria
C cold
K klammy
S slow capillary refill
Clinical exams: student report
“My case was a 6 year old boy with a VSD. I found this quite challenging and the little boy was very
sweet but wanted to tell me all about his problem so I couldn’t go through my usual routine with his
mother with the history but it didn’t seem to matter as I passed anyway. I think it’s more about having a
good rapport with the child and being child friendly!”
History taking: don’t forget
• To talk to the child as well as the parent
• Birth history and developmental history
• Social history
• Family history
Examination
• Examination starts from the moment you walk into the room
• Observation while taking the history gives lots of information about a child’s clinical condition
Top tips
• Leave the child on the parent’s knee if that is where they are most comfortable
• Always explain what you are going to do
• Use one of the parents as a “dummy” eg listen to the parent’s heart first
• Be systematic, yet opportunistic i.e auscultate before they start crying, look into the throat when
they’re screaming!
• Examiners will understand if a child has been difficult to examine
© Dr R Clarke 2023 support@askdoctorclarke.com 5
Essential Paediatrics
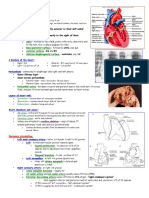
Paediatric Cardiology
Paediatric cardiology
• Examination of the cardiovascular system
• Acyanotic congenital heart disease: ventricular septal defect, atrial septal defect and patent ductus
arteriosus
• Cyanotic congenital heart disease: Fallot’s tetralogy, transposition of the great arteries
• Down syndrome and the heart
Examination of the Cardiovascular System
Approach to examination
M Radford: with permission
• Wash hands, introduce yourself and ask
permission
• Look: scars, clubbing, oxygen, breathlessness,
cyanosis, respiratory rate, activity, JVP
• Feel: pulses, praecordium, liver
• Listen: heart, lung bases
• Finally thank child and parents and wash hands
Please note
• It is reasonable to perform auscultation first while the child is quiet
• “Babies don’t have a neck” so check for enlargement of liver instead of assessing the JVP
Auscultation: question stop
What causes the first and second heart sounds?
Normal heart sounds
lub dub
ventricular systole diastole
© Dr R Clarke 2023 support@askdoctorclarke.com 6
Essential Paediatrics
Normal splitting of the second heart sound
• During inspiration, there is an increase in the negative intra-thoracic pressure
• This increases venous return from the body into the right atrium
• And therefore increases the volume of blood to be ejected by the right ventricle
• Causing a slight delay in the closure of the pulmonary valve (P2)
Lub dub Lub de
A2 P2
Inspiration Expiration
Wide fixed splitting of the second heart sound with an atrial septal defect (ASD)
Lub splat Lub splat
Inspiration Expiration
Splitting of the second sound in atrial septal defect
• Wide: due to shunting, with increase flow to right side of heart, delaying closure of pulmonary valve
• Fixed: no variation with respiration because of “common atrium”. (Due to the defect, changes with
respiration affect both sides of the heart equally)
Please note
• You are not expected to diagnose wide fixed splitting of the second sound
• It is a subtle sign and many paediatricians have never heard it
• This is why it is much harder to diagnose ASDs compared with VSDs
• But it is still useful to be aware of this sign as it is often asked about in exams
Pansystolic murmur: “burrr”
no gap between murmur and HS2
lub dub
Pansystolic murmur diastole
© Dr R Clarke 2023 support@askdoctorclarke.com 7
Essential Paediatrics
Differential diagnosis of a pansystolic mumur
• Ventricular septal defect (at lower left sternal edge, often with a thrill)
• Mitral regurgitation (loudest at apex and radiates to axilla)
• Tricuspid regurgitation (with pulsatile hepatomegaly and V waves in JVP)
Ejection systolic murmur: “burr de”
audible gap between
mumur and HS2
lub dub
ventricular systole diastole
Murmurs: above or below the nipple line?
Radiates to neck
Radiates to back
PDA
machinery
murmur
Aortic stenosis Pulmonary stenosis
Ejection systolic above
VSD (MR)
Pansystolic below
The nipple line
Continuous murmur: BurrrDurrr
lub dub
diastole
© Dr R Clarke 2023 support@askdoctorclarke.com 8
Essential Paediatrics
Four useful sounds
• ASD (Lub splat)
• Pansystolic murmur (Burrr)
• Ejection systolic murmur (Burr de)
• Machinery murmur (BurrrDurrr)
Innocent murmurs
• Heard at some time in about 25% of children
• Soft ejection systolic murmur at left sternal edge
• May occasionally sound harsh
• No radiation to carotids and no thrills
• No symptoms
• Often heard with fever (tachycardia with increased cardiac output)
The 7 S’s
• Short
• Soft
• Systolic
• S1 & S2 normal
• Standing and sitting variation
• Symptomless and
• Special tests normal (ECG, CXR, Echo)
Fetal circulation
The unfolded heart
SVC Pulmonary veins SVC Pulmonary veins
IVC IVC
Foramen ovale Crosses
Foramen ovale
Right Left
atrium atrium
Right Left
ventricle ventricle Oxygenated blood
Ductus from umbilical vein Ductus
arteriosus (via ductus venosus
and IVC)
arteriosus
Aorta Aorta
Pulmonary artery Pulmonary artery
Fetal circulation
• In utero, oxygenated blood is provided by placenta
• Fetal lung is bypassed by most circulating blood
• High pulmonary resistance means blood follows alternate path via:
• Foramen ovale (from RA to LA)
• Ductus arteriosus (from PA to aorta)
© Dr R Clarke 2023 support@askdoctorclarke.com 9
Essential Paediatrics
Normal transition SVC Pulmonary veins
At birth first breath triggered by
• Hypoxia secondary to cord clamping IVC
• Stimulation
RA LA
Air drawn into lungs
• Oxygen is powerful pulmonary vasodilator
• Large drop in pulmonary resistance RV LV
Blood redirected through lungs
Ductus closes within a day or two due to Pulmonary artery
Aorta
withdrawal of placental prostaglandins
Systemic circulation and ductus Pulmonary circulation
Oxygen- vasoconstriction Oxygen- vasodilation
Hypoxia- vasodilation Hypoxia- vasoconstriction
Prostaglandins and the ductus arteriosus
Congenital heart disease (CHD)
• Commonest congenital malformation
• Approx 1% of live births
• 10% of stillbirths have cardiac lesions
• VSD and PDA are the commonest abnormalities
Classification of CHD
• Acyanotic: ASD, VSD, PDA, pulmonary stenosis, aortic stenosis, co-arctation
• Cyanotic: tetralogy of Fallot, transposition of the great arteries
Central cyanosis
J Peterson: with permission
Blueness occurs when there is more than 50g/l de-
oxygenated haemoglobin
If not anaemic, this will usually occur with an
oxygen saturation of 85% or less
© Dr R Clarke 2023 support@askdoctorclarke.com 10
Essential Paediatrics
Acyanotic Congenital Heart Disease
Three left-to-right shunts
• VSD
• ASD
• PDA
Ventricular septal defect (VSD) SVC Pulmonary veins
• Common: 30% of CHD
• Sometimes diagnosed antenatally if a good four IVC
chamber view is obtained on ultrasound
• Variable size
• Loudness of murmur inversely related to size of
shunt VSD
Buzz words
If large, a VSD may cause
“A left to right shunt at ventricular level”
Aorta
Pulmonary artery
Student report
“My case was examination of a 3 year old with a VSD”
Small VSD
• High velocity jet with loud “blowing” or “rasping” pansystolic murmur
• May have a thrill (palpable murmur), but no significant left to right shunt
• Increased risk of endocarditis
• Often close spontaneously before age 5
• Differential diagnosis: other pansystolic murmurs eg mitral and tricuspid regurgitation
A large shunt can cause heart failure
• Sheer volume of traffic can slow down traffic flow on a motorway even without an obstruction such as
road works
• With a big VSD there is volume overload of the ventricles because of the shunting
• This leads to heart failure
Shunting of blood with a VSD
Lungs
RA RV LA LV Body
Volume and pressure overload
• Large shunt increases blood flow to lungs: volume overload
• Pulmonary venous congestion causes breathlessness and/ or chest infections
• Eventually pulmonary arterial hypertension develops with pressure overload of RV
• Signs then include: left parasternal heave, loud P2 and pulmonary ejection murmur
Large VSD
• Typically presents with heart failure at 4-6 weeks
• Breathless and sweaty on feeding or crying
• May also be a cause of faltering growth or
• Recurrent chest infections
© Dr R Clarke 2023 support@askdoctorclarke.com 11
Essential Paediatrics
Typical case: small VSD
• Blowing pansystolic murmur at lower left sternal edge
• With an associated thrill
• But no right ventricular heave or signs of heart failure
Large VSD: on examination
• Left parasternal heave (due to right ventricular hypertrophy)
• Quiet or absent pansystolic murmur
• Pulmonary ejection murmur
• In other words, signs of pulmonary hypertension
VSD investigations
• ECG- right ventricular hypertrophy (dominant R wave in V1)
• CXR- cardiomegaly, prominent pulmonary artery and plethoric lung fields
• Echo- shows size of lesion and doppler flow may indicate size of shunt
VSD treatment
• None if small
• Antibiotic prophylaxis not recommended (NICE 2008 and 2018)
• Diuretics and ACEI for heart failure
• Repair if large defect with risk of pulmonary hypertension
Atrial septal defect
• May be asymptomatic
• Recurrent chest infections or heart failure
• Arrhythmias common in 30s and 40s (SVT and AF)
• Flow across the defect itself does not create a murmur (as low pressures in atria)
• Isolated ASD: low risk of endocarditis and antibiotic prophylaxis not needed (NICE 2008)
Buzz words Wide fixed splitting of the second sound
If large, an ASD may cause
“A left to right shunt at atrial level” Delayed P2
SVC Pulmonary veins
IVC Lub splat Lub splat
ASD
Aorta
Pulmonary artery
Inspiration Expiration
ASD treatment
• Trans-catheter closure (via femoral vein and IVC to right atrium) or
• Open heart surgery with patch repair before 5th birthday
Notes on video
https://www.youtube.com/watch?v=I5sRAcOVGiU
Trans-catheter closure using a double-umbrella occluder device (“Amplatzer septal occluder”)
© Dr R Clarke 2023 support@askdoctorclarke.com 12
Essential Paediatrics
Patent ductus arteriosus (PDA) SVC Pulmonary veins
• 12% of CHD cases IVC
• Second commonest after VSD
• Commoner in premature babies (kept open by
hypoxia)
• Normally closes within a day or two of birth
• If persists, left to right shunt occurs as right
sided pressures fall with lung expansion Patent ductus
arteriosus
Buzz words Pulmonary artery
Aorta
“A left to right shunt at ductal level”
PDA and prematurity
• Preterm heart less sensitive to reduction in prostaglandin levels at birth
• Expanded lungs are main site of prostaglandin breakdown
• Lung immaturity may result in slower decline in PG levels
• Hypoxia more common in preterm infants: contributes to keeping duct open
• PDA occurs in up to 60% of infants <28 weeks gestation
PDA: on examination
• Collapsing or “bounding” pulses: the shunting leads to extra blood flow through the lungs and hence
extra blood returning to the left of the heart (volume overload)
• Extra blood ejected from LV causes high systolic pulse pressure
• Rapid “run-off” through the ductus leads to low diastolic pressure
• Auscultation: continuous “machinery” murmur
• Loudest below left clavicle and radiates to back
BurrrrDurrr
lub dub
diastole
Presentation depends on degree of shunting
• Small shunt: well neonate with a machinery murmur
• Larger shunt: heart failure or recurrent chest infections
PDA: treatments
• Prostaglandin inhibitors to close duct
• Transcatheter occlusion
• Surgical ligation
© Dr R Clarke 2023 support@askdoctorclarke.com 13
Essential Paediatrics
Cyanotic Congenital Heart Disease
Fallot’s tetralogy
P pulmonary stenosis causing
R right ventricular hypertrophy
O over-riding aorta; R to L shunt across
V VSD
E ejection systolic murmur- pulmonary
Embryology of Fallot’s: unequal partitioning of the truncus arteriosus
Anterior
Normal
PA
m
Truncus tu
S ep Right Ao Left
arteriosus
Posterior
Fallot’s
PA
Ao
Week 4 Week 5 of intrauterine development
Viewed as though looking up from ventricle
Transverse section through chest
Aorta displaced
to the right
LA
Pulmonary
stenosis VSD
RA
LV
RV
RV hypertrophy
“Unfolded” “Folded”
On examination Buzz words
• Clubbing and cyanosis “Right ventricular outflow tract obstruction”
• Right ventricular hypertrophy “Infundibular pulmonary stenosis”
• Ejection systolic murmur ie not just the valve that is narrow, the outflow tract
just below the valve is affected
Squatting posture
• Partially occludes femoral arteries
• Increases systemic vascular resistance
• More blood flows across ductus into PA
• Improves oxygenation
© Dr R Clarke 2023 support@askdoctorclarke.com 14
Essential Paediatrics
Squatting poem
Fallot was squatting down low
His ductus assisting the flow
After it closed, he went quite cyanosed
But Blalock helped him to grow
Patent ductus in Fallot’s SVC Pulmonary veins
• Cyanotic spells often become apparent around
IVC
day 2 or day 3 when the ductus closes
• In 1944 Dr Helen Taussig noted that babies
with a persistent patent ductus lived longer
than those without
• She thought an operation to create a similar
shunt into the pulmonary artery would help
• She persuaded Alfred Blalock to perform the Right to left shunt
through VSD due to
first shunt operation pulmonary stenosis Patent ductus
Pulmonary stenosis
bypasses
obstruction
Blalock-Taussig shunt Surgery
• Usually a two-stage procedure
• Shunt operation to increase pulmonary flow in
Right subclavian order to help develop the pulmonary arteries,
artery which have been “starved” of blood flow by the
stenosis; improves oxygenation
Pulmonary • Followed by definitive correction
artery • Latest evidence: betablockers prevent
infundibular spasm and reduce cyanotic spells
www.wikipedia.com
Transposition of the great arteries
• Associated with diabetes in pregnancy
• Aorta comes off RV and PA comes off LV: circulation with two separate loops
• Only the PDA allows some oxygenated blood to reach systemic circulation
• Cyanotic from birth
• Prostaglandin infusion to keep duct open (“duct dependent lesion”)
• Atrial septostomy to encourage further mixing
• Then definitive “switch” operation
Lungs SVC Pulmonary veins
IVC
Atrial septostomy
LA LV PA allows further
mixing
PDA
RA RV
Ao
Patent ductus
arteriosus allows
some oxygenated
Body blood to reach body
Pulmonary
Aorta
artery
Two separate loops linked by patent ductus Atrial septostomy improves oxygenation
© Dr R Clarke 2023 support@askdoctorclarke.com 15
Essential Paediatrics
Down Syndrome and the Heart
Down syndrome
R Round face
O Occipital flattening (& nasal flattening)
S Speckled iris (Brushfield spots)
E Epicanthic folds
O Open mouth with protruding tongue
L Low set ears
A Almond (oval) upward slanting eyes
Roseola
• Is just a mnemonic
• No more common in Down syndrome
• Mild viral infection due to herpesvirus 6
• Affects babies and toddlers 6/12- 2 years
• 3 days of fever followed by up to 3 days of viral macules on chest
• Sixth disease 3+3= 6
Hands: single transverse
Strabismus (squint) palmar crease, short
fingers, curved little finger
(clinodactyly)
Feet: sandal gap between
Brushfield big toe and other digits
spots
Epicanthic fold on iris
Flat bridge of nose
Open mouth
Protruding tongue Duodenal atresia
“Double bubble”
Down syndrome
• Hands: single transverse palmar crease, short fingers, curved little finger (clinodactyly)
• Feet: sandal gap between big toe and other digits
• Increased risk of: duodenal atresia, coeliac disease, Hirschprung’s, squint, leukaemia, hypothyroidism
• 40-50% have a cardiac abnormality: all should have an echo at time of diagnosis
Down syndrome associated with
• ASD
• VSD
• Atrioventricular canal defect (low ASD and high VSD)
• Mitral and tricuspid valve regurgitation
Buzz words
• “Endocardial cushion defect”
RA LA
• Leads to “failure of septation” of the heart
• “AVSD”
v
RV LV
Endocardial Cushions divide the heart into
left and right; and into atria and ventricles
NB Notes on Turner’s syndrome on p34 Coronal view of heart
Student report
“Examine this child’s cardiovascular system. He was aged 2, with a systolic murmur. I was asked about
Eisenmenger’s syndrome.”
Question: Eisenmenger’s syndrome refers to the process of shunt reversal- why does this happen?
© Dr R Clarke 2023 support@askdoctorclarke.com 16
Essential Paediatrics
Post Course Notes
Case history: Kawasaki’s disease
This 3 year old has had a prolonged fever. She has developed a rash on her hands and feet which is
now starting to peel. What is the likely diagnosis? What cardiac complication may occur?
Kawasaki’s disease: febrile mucocutaneous syndrome
Diagnosis: fever for 5 days plus 4 out of 5 of the following
• Conjunctivitis
• Lymphadenopathy
• Rash
• Lips- redness, cracking or strawberry tongue
• Extremity changes
Mnemonic: clear
C Conjunctivitis
L Lymphadendopathy and lips
E Extremity changes
A Aneurysms
R Rash
? Bacterial toxin
Acute phase response Prolonged fever >5 days
Raised WCC, ESR, CRP
T cell stimulation & cytokine release
Thrombocytosis
Conjunctivitis without pus
Early mucocutaneous Red cracked lips / strawberry tongue
Polymorphous rash on trunk
syndrome Redness around BCG scar
Hands and feet- red and then peeling
20% develop coronary aneurysms
Best detected on echo
Small risk of thrombosis and death
Late vasculitis Early immunoglobulin prevents
Aspirin continued for at least 6 weeks
Heart failure
• Symptoms: poor feeding, sweating, poor weight gain, breathlessness, recurrent chest infections
• Signs: tachypnoea, tachycardia, extra heart sounds (“gallop rhythm”), cardiomegaly (displaced apex),
hepatomegaly
• Important causes in neonate: hypoplastic left heart or co-arctation
• VSD or PDA in infant, particularly the first few weeks when pulmonary vascular resistance is falling
(left to right shunts therefore increase)
© Dr R Clarke 2023 support@askdoctorclarke.com 17
Essential Paediatrics
Rheumatic fever
• Occurs after the usual immunological 2-6 week gap following infection with Strep. pyogenes (Group A
beta-haemolytic Streptococcus)
• >50% of cases associated with an acute carditis
• Antibodies cross react with bacterial cell wall and heart antigens (“molecular mimicry”)
• Chronic rheumatic heart disease: recurrent episodes, often subclinical, damage heart valves
• Typically leads to mitral stenosis or aortic regurgitation years later
• Diagnosis based on evidence of Strep. (Throat swab or ASO titre) plus major and minor criteria
Duckett Jones’ major criteria: “Carey’s red nodule ruined Arthur’s career”
• Carey’s: Carey Coombs mitral diastolic murmur
• Red: erythema marginatum
• Nodule (painless, subcutaneous, rare)
• Ruined (just a verb)
• Arthur- arthritis (typically medium and large joints)
• Career- chorea (abnormal movements of Sydenham’s chorea- St Vitus’ dance)
Minor criteria
• Arthralgia
• Fever
• Raised ESR
• Heart block
Co-arctation of the aorta
• Narrowing usually just below origin of left subclavian: “juxta-ductal”
• Associated with Turner’s syndrome
• May present with shock in neonatal period when ductus closes (if severe narrowing)
• Or later with heart failure or hypertension
• Weak femoral pulses with radio-femoral delay
• Arm BP > leg BP (Four-limb BP measurement)
• Systolic murmur over back
• Rib notching due to collaterals on CXR >age 7
Infective endocarditis
• 2 signs in the hands: clubbing and splinter haemorrhages
• 1 in the heart: variable murmurs
• 2 in the abdomen: splenomegaly and microscopic haematuria
• May complicate any congenital heart defect
• Usual organism is Strep. Viridans (dental)
• Antibiotics for 6 weeks if strep. on a native valve
Eisenmenger syndrome: shunt reversal
• Large shunt leads to pulmonary artery hypertension
• As this develops, the degree of left to right shunting gets less which may lead to initial improvement in
heart failure symptoms
• Finally, the right sided pressures are so high that right to left shunting occurs causing cyanosis
• This is called the “Eisenmenger syndrome”, causing acquired cyanotic heart disease
• Only treatment option at this stage is heart-lung transplantation
© Dr R Clarke 2023 support@askdoctorclarke.com 18
Essential Paediatrics
Post Course Notes: Paediatric Basic Life Support
Always check the latest guidelines at www.resus.org.uk
Four favourite questions
Q: How long would you continue before going for help?
A:
5 cycles or 1 minute
Carry an infant with you if alone when going for help
Q: How long would you continue CPR
A:
Until further help arrives
Until signs of life are noted
Until you are exhausted
Q: When would you perform CPR in the presence of a pulse?
A:
Bradycardia <60,
Thready pulse in collapsed child or
No signs of life
Q: What are signs of life?
A:
Spontaneous movement
Spontaneous breathing
Response to stimulation
© Dr R Clarke 2023 support@askdoctorclarke.com 19
Essential Paediatrics
Emergencies in Children
First: call for help, check for danger, evaluate responsiveness
Checks & vital signs Examples of intervention
Airway Treat choking and maintain airway patency
Call anaesthetist
Breathing- O2 sats. and respiratory rate High flow oxygen
Circulation- pulse, BP, temperature, CRT IV access and fluid bolus for shock
Disability- AVPU* or Paed. GCS; moving all 4 Check capillary glucose, treat hypoglycaemia
limbs? Treat seizures
Exposure- check mucous membranes and Check for urticaria and for non- blanching or evolving rash
entire skin Preserve patient dignity. Repeat checks if initially normal
*AVPU: Alert, responds to Voice, responds to Pain, Unresponsive
Intravenous fluids in children
• Fluid resuscitation in a shocked patient
• Replacement of a fluid deficit
• Maintenance fluids Total fluid requirement
• Accounting for ongoing losses
Bolus IV fluids for shock
• Initial bolus of 10ml/kg 0.9% sodium chloride solution over 5-10 minutes
• Call for senior help and consider repeating if necessary
• Same initial dose used for shock in sepsis, severe D&V and diabetic ketoacidosis (DKA)
• In ketoacidosis, bolus given over 15 minutes
Case history
Sam is a 6 year old boy who normally weighs 20kg. He has a two day history of severe diarrhoea and
vomiting. On examination he is shocked.
• What are the signs of shock?
• After assessing ABCDE and summoning senior help, how much IV fluid would you give him as an
initial bolus?
After correction of shock, Sam is assessed as 5% dehydrated: correction of fluid deficit
• Calculate volume in ml using % dehydration x weight (kg) x 10
• Replace over 24 hours (48 hours in DKA)
• Sam is 5% dehydrated, so his deficit is 20 x5 x10= 1000ml
Maintenance fluids / 24 hours Or use 4-2-1 rule for hourly rate
100ml/ kg/ 24hrs for first 10kg 4ml/ kg/ hour for first 10kg
50ml/ kg/ 24hrs for next 10kg 2ml/ kg/ hour for next 10kg
20ml/ kg/ 24hrs for remaining kg 1ml/ kg/ hour for further kg
Sam’s fluids in first 24 hours, after correction of shock
Deficit 1000ml
Maintenance 1500ml
Ongoing loss 800ml (estimate or measure volume of diarrhoea)
Total 3300ml (ie 137ml/ hour)
Special circumstance: diabetic ketoacidosis (BSPED 2021)
• Significant risk of cerebral oedema, so after initial resuscitation, deficit replaced slowly over 48 hours
• Use pH to assess severity and as a guide to the degree of dehydration
• Mild: pH > 7.2: assume 5% dehydration
• Moderate: pH 7.1- 7.19: assume 5% dehydration
© Dr R Clarke 2023 support@askdoctorclarke.com 20
Essential Paediatrics
• Severe: pH <7.1: assume 10% dehydration
Diabetic ketoacidosis initial management
Two Emergencies: Test Yourself
Case 1: Hayden y
History
• 4 years old
• Known eczema, hayfever,
asthma
• Sudden onset difficulty in
breathing
Examination
• Heart rate 180bpm
• RR 60bpm
• Sats 87%
• BP unrecordable
Questions: What does the picture show? What is the diagnosis?
After checking ABCDE, what emergency medication would you give?
Case 2: Matt
History
7 years old
1 day history fever, lethargy
Examination
Temp 39.2
HR 170bpm
RR 25
BP 70/30
CRT 5 seconds
Questions
• What is the likely diagnosis?
• After checking ABCDE, what emergency treatment would you give?
© Dr R Clarke 2023 support@askdoctorclarke.com 21
Essential Paediatrics
Case 1: Hayden (Image by Anaphylaxis Australia with permission)
Anaphylaxis
• Immune mediated, life-threatening allergic reaction
• Exposure to an allergen precipitates release of histamine, leukotrienes and prostaglandins
• Swelling of mucous membranes, increased bronchial smooth muscle tone, loss of vascular tone and
increased capillary permeability
• Urticarial / erythematous / itchy rash, lip/ tongue/ facial swelling, wheeze, stridor
Anaphylaxis algorithm
Based on Resuscitation UK Guidelines 2008 and NICE 2011: check latest at www.resus.org.uk
Adrenaline
• Give IM adrenaline (under 6 years, give 0.15ml of ‘1 in 1000’= 150microgm; 6-12years, give 0.3ml)
• Consider Nebulised adrenaline (5ml ‘1 in 1000’)
Poem
Up to six, with intramuscular pricks
In it goes swiftly, a hundred and fifty
Whatever the brand, one in a thousand
Alternatively: Remember IM: M is Latin symbol for millennium (1000)
© Dr R Clarke 2023 support@askdoctorclarke.com 22
Essential Paediatrics
Following initial resuscitation
• Antihistamine eg chlorphenamine (“Piriton”)
• IV hydrocortisone (4mg /kg)
• Observation for rebound symptoms – “biphasic anaphylaxis”
• Education re basic life support and use of an adrenaline
autoinjector
• Blood (IgE panel) and/ or skin prick testing
• Referral to dieticians for advice re allergen avoidance
Case 2: Matt- Meningococcal sepsis
Invasive meningococcal disease
Meningococcal sepsis
• Life-threatening gram negative infection: Neisseria meningitidis
• 1 in 10 mortality, significant morbidity
• Infection causes systemic inflammatory response with leaking capillaries and deranged clotting
• Serious risk of multi-organ failure
• Immunisation against serogroup C routine for many years – 90% UK cases serogroup B
• Meningitis B vaccine offered for routine use since 2016
Early management of suspected meningococcal disease in children >3 months
Based on NICE Guideline (2010 updated 2022), HPSC Guideline (ROI 2016)
© Dr R Clarke 2023 support@askdoctorclarke.com 23
Essential Paediatrics
Intravenous antibiotics
• Severe meningococcal sepsis typically treated with ceftriaxone (80mg/kg – 100mg/kg) IV over 30
minutes
• Cefotaxime used instead if patient being given balanced electrolyte solution such as Hartmann’s
• Always check latest guidance in BNF for Children
Typical CSF findings
• Cloudy CSF
• White cell count >10 per microml
• Polymorphs ++
• Gram negative diplococci
• Low glucose (<50% of serum level)
• High protein (>400mg/l)
Student report
Initial assessment of 8 year old child with "rash" - was meningococcal sepsis - was shown picture when
exposing dummy. Request all relevant investigations, start appropriate management etc. Was asked
what else I needed to do - totally forgot to say I would inform public health!
Public health aspects
• Notifiable disease
• Only offer prophylactic antibiotics to close household contacts (sharing kitchen, bathroom etc)
• Single dose oral ciprofloxacin used
• Information and advice sheet for other contacts
Status epilepticus (based on APLS 2021 and NICE 2022)
Mnemonic for 6 stage approach
Oh my Lord, let’s phone the anaesthetist! (See pre-course work)
Oh Oxygen (after checking ABC)
My Midazolam (buccal; or rectal diazepam; or IV lorazepam)
Lord Lorazepam (IV)
Let’s Levetiracetam (IV infusion)
Phone the Phenytoin (or phenobarbitone IV infusion)
Anaesthetist Rapid induction anaesthesia
Summary
• A number of different illnesses can present as emergencies in children
• The approach to all paediatric emergencies is to assess ABCDE
• Always call for senior help when faced with a paediatric emergency
© Dr R Clarke 2023 support@askdoctorclarke.com 24
Essential Paediatrics
Post Course Notes: Replacement of Ongoing Fluid Losses
Ongoing losses (such as from surgical drains or ongoing watery stools)
These are measured in mls and replaced “ml for ml” (for example if a child loses 200mls fluid via watery
stools over a 4 hr period then 50 extra ml per hour additional fluid will be needed for 4 hrs to replace
this).
Typically a bag of “0.45% sodium chloride solution and 5% glucose” is used when giving maintenance IV
fluids to children. Pre-prepared bags containing 10 or 20mmol potassium chloride are available and
should be used unless there is a history of hyperkalaemia, anuria or renal failure.
Once a child has been started on IV fluids close attention should be paid to:
• Their hydration and circulatory status (heart rate, blood pressure, cap refill, urine output and weight).
This is to ensure that the child is neither being “under” or “over” filled with IV fluids.
• Electrolyte balance, in particular serum sodium and potassium levels
Post Course Notes: Adrenaline Auto-injectors
How to use an adrenaline auto-injector eg “Emerade”
• Remove the safety cap
• Place the device against the outer thigh and press it firmly in until it clicks (see diagram)
• Hold it against the thigh for 5 seconds
• Remove the unit & lightly massage the injection site
• Call 999 and state “Anaphylaxis”. Take the used Emerade device with you to hospital.
Note
Children should have 2 devices available at all times. It should not be injected into the buttock. It is
designed to work through clothing. After it has worked, the needle shield remains locked and extended. If
you peel back the label, you will see that the inspection window has become coloured after successful
administration.
After use
• Be prepared to inject a second time with another unused device in 5-10 minutes if necessary
Post course note:
Traffic light system for children with fever or unwell (NICE 2013, reviewed 2017)
© Dr R Clarke 2023 support@askdoctorclarke.com 25
Essential Paediatrics
Post Course Notes: UK Vaccination Schedule
Age 2/12 3/12 4/12 12/12 Pre- 12-13 14 years
school years
booster
DTPP+ HiB DTPP + Hib DTPP + Hib Hib + Men.C DTTP HPV x2 DTP
+ Hep B = + Hep B = + Hep B = “4 in 1” “3 in 1”
“6 in 1” “6 in 1” “6 in 1” Teenage
booster
Pneumo. Pneumo.
Men.B Men.B Men.B
Rotavirus Rotavirus
(oral)
Men.ACW
Y
MMR MMR
Notes Plus
annual flu
vaccine
age 2-10
Vaccinations
For latest details, check www.nhs.uk/Conditions/vaccinations/ (Accessed December 2022)
2 months: 6-in-1 plus rotavirus and meningitis B
3 months: 6-in-1 plus pneumococcal and rotavirus (second dose)
4 months: 6-in-1 plus pneumococcal (second dose) and men B (second dose)
12 months: MMR, Hib/Men C booster (Men C second dose, Hib fourth dose), pneumococcal (third dose)
and Men B (third dose)
Pre-school booster
3 years 4 months: 4-in1 pre-school booster with MMR (second dose)
Notes
6-in-1: diphtheria, tetanus, pertussis, polio, haemophilus influenzae B, hep B
4-in-1: diphtheria, tetanus, pertussis, polio
Plus Covid vaccination
See https://www.nhs.uk/conditions/vaccinations/nhs-vaccinations-and-when-to-have-them/
© Dr R Clarke 2023 support@askdoctorclarke.com 26
Essential Paediatrics
Two Cases
Case one: Luke
Luke is a five year old boy, previously fit and well. He has been looking increasingly pale over the last
few weeks. He now has a temperature of 38.5 and is feeling very tired. On examination, he is pale with
bruises on his shins, arms and abdomen. There is hepatosplenomegaly and multiple lymph nodes in the
neck and groin.
Single best answer questions:
Choose one investigation to help you make a diagnosis
a) Full blood count with film
b) Clotting screen
c) Serum iron levels / TIBC
d) CRP
e) Blood culture
What is the most likely diagnosis?
a) Idiopathic thrombocytopaenic purpura
b) Non-accidental injury
c) Severe iron deficiency anaemia
d) Acute leukaemia
e) Haemophilia
Case two: suspected child abuse
You are a junior doctor in the emergency department. You have just taken a history from a mother who
brought in her 1 year old daughter with burns to the arms and legs after “falling into the bath” while being
looked after by the mother’s boyfriend. You are concerned that the burns may be the result of child
abuse.
What would you say in discussing your concerns regarding non-accidental injury with the parent? Please
specify some of the phrases you would use.
© Dr R Clarke 2023 support@askdoctorclarke.com 27
Essential Paediatrics
Case One: Luke
Best investigation to make a diagnosis Blood film shows blasts
Full blood count and film
Image by A Christaras at Wikimedia
Hb 63 g/l, WBC 65 x 109 /l, Plt 35 x 109 /l
What is the most likely diagnosis?
a) Idiopathic thrombocytopaenic purpura
b) Non-accidental injury
c) Severe iron deficiency anaemia
d) Acute leukaemia
e) Haemophilia
Leukaemia
• Acute lymphoblastic leukaemia (ALL) is the commonest childhood cancer
• Peak incidence 2-5 years
• Malignant disease of the bone marrow
• Lymphoid precursors (blasts) proliferate and replace normal haematopoetic cells
• Underlying cause unknown
• Diagnosis is confirmed by bone marrow aspirate
• Buzzwords: testes and CNS are “sanctuary sites”
Clinical features
• Bone pain
• Lymphadenopathy, hepatosplenomegaly
• Bone marrow failure (anaemia, neutropaenia, thrombocytopaenia)
Managing ALL
• Induction chemotherapy at tertiary centre
• Shared-care with local hospital for consolidation and maintenance: 2 years in girls, 3 years in boys
• Examples of drugs used include vincristine, methotrexate and steroids
• Additional treatments include bone marrow transplantation if poor response or relapse
• Radiotherapy rarely required for sanctuary sites
Buzz words: minimal residual disease burden
• Induction chemotherapy for 4 weeks
• Repeat bone marrow aspirate
• Good prognosis if no circulating blasts on blood film and less than 5% blasts in marrow
Key complications of ALL
Pathophysiology Treatment
BONE MARROW Malignant infiltration of Transfusion of blood
FAILURE bone marrow products
Chemotherapy drugs Granulocyte colony
stimulating factor
SEPSIS Low WBC count Broad spectrum
(“febrile neutropenia”) antibiotics
Renal failure secondary
TUMOUR LYSIS to increased levels of Hyperhydration
SYNDROME urate, phosphate and Allopurinol or
potassium at initiation of Rasburicase
chemotherapy Dialysis
© Dr R Clarke 2023 support@askdoctorclarke.com 28
Essential Paediatrics
Outcomes in ALL
• Variable prognosis based on variety of clinical and laboratory findings
• Best prognosis: Age 1-10 years, lower WBC at diagnosis (under 50 x 109/l), good response to
induction chemotherapy with minimal residual disease burden
• Overall cure rate around 90%
Case Two: Suspected Child Abuse
You are a junior doctor in the emergency department. You have just taken a history from a mother who
brought in her 1 year old daughter with burns to the arms and legs after “falling into the bath” while being
looked after by the mother’s boyfriend. You are concerned that the burns may be the result of child
abuse.
What would you say in discussing your concerns regarding non-accidental injury with the parent? Please
specify some of the phrases you would use.
Video
Watch the following video of a junior doctor sharing these concerns with the parent.
Make a note of any phrases that may be useful for you to use in similar situations in exams / clinical
practice
General principles
• Remain calm and polite
• Acknowledge concerns and questions
• Emphasise that the child’s welfare is your priority
• Admit when you don’t know the answer and offer to contact a senior
A useful phase for difficult scenarios
“I understand you must be very worried about your child. I assure you we are doing everything we can to
help her. Her well-being is our absolute priority”
Student report
We had to take a history from mother about a 4 year old girl who was overheard talking to dolls about
inappropriate behaviour by the child's uncle. We were asked about the immediate management of the
situation.
Student report
There was a question on our short answer paediatrics paper about non-accidental injury. We weren't
asked anything specifically about the procedures, just asked what we would do in the situation (ie get
senior review, document everything, get a witness/chaperone).
© Dr R Clarke 2023 support@askdoctorclarke.com 29
Essential Paediatrics
Outline of usual process
Junior has concern
Discussion with senior
Paediatric assessment
Ongoing concern
No further concern
Refer to social care
+/- Police
Strategy meeting
Child protection investigation
Child protection conference
Child Protection Plan
Post course resources: country specific information (All accessed December 2022)
Useful short summaries for England, Wales, Scotland and Northern Ireland at NSPCC website:
https://learning.nspcc.org.uk/child-protection-system
Child abuse guidelines for Northern Ireland (2017): available at
https://www.proceduresonline.com/sbni/
Child abuse guidelines for Scotland (2021); download guidance from
https://www.gov.scot/publications/national-guidance-child-protection-scotland-2021/
Child abuse guidelines for Wales (2016)
https://gov.wales/safeguarding-children-guidance-child-practice-reviews
Children First guidelines for Republic of Ireland (2019, updated 2021): download guidance from
https://www.gov.ie/en/policy-information/d1b594-children-first/
© Dr R Clarke 2023 support@askdoctorclarke.com 30
Essential Paediatrics
Post Course Notes: Safeguarding Children
NSPCC study: child cruelty in the UK (2011)
On asking 18 -24 year olds:
• 1 in 4 were severely abused during childhood
• 1 in 9 experienced severe physical violence at the hands of an adult
• 1 in 9 experienced contact sexual abuse
• 1 in 10 severely neglected
Implications
• You WILL see a case of child abuse during your first 5 years of clinical practice
• Will you recognise it? Will you know what to do?
Four types of abuse
• Physical (non-accidental injury)
• Emotional
• Sexual
• Neglect
Physical abuse
• Bruises
• Bites
• Lacerations eg torn frenulum
• Burns
• Fractures
• Abusive head trauma
• Fabricated and induced illness (FII)
Suspicions raised if
• Delay in presentation
• Vague, elusive or changing history
• Angry or abusive parents even when gently
questioned
• Discrepancy between witnesses
• Discrepancy between history and findings
• Injuries in very young pre-mobile children
Spiral fracture of femur
Risk factors
• Previous episode of abuse
• Abuse in sibling
• Single poorly supported parent
• Conflict between parents
• Alcohol and drug use by parent
• Stress, anger, poor parenting
• Child with disability
• Not all cases have risk factors
© Dr R Clarke 2023 support@askdoctorclarke.com 31
Essential Paediatrics
Differential diagnosis
• Accidental injury
• Osteogenesis imperfecta
• Coagulation disorders eg idiopathic thrombocytopaenic purpura
• Mongolian blue spot
• Scalded skin syndrome
Investigations
Reason for Investigations Investigations Investigations to
Investigation related to needed to exclude look for associated
presenting injury other differential injuries
or illness diagnoses
Relevant e.g. suspected History of easy or Children aged <2y
presentation fracture florid bruising (at increased risk
of severe abuse)
Investigations e.g. limb X-ray FBC Skeletal survey
Clotting screen CT head (<1yr)
Ophthalmology
Typical examination questions
• What would you do if you had concerns about a child’s welfare?
• Take a history from this parent whose child has presented with burns
Two student reports
“Non accidental injury - child “fell off sofa” and has bruising and scratches on face. The questions were
on how to manage this.”
“Non accidental injury viva: I was shown a picture and asked how to deal with the case”
History taking in suspected child abuse
• Try to obtain a detailed account of what has happened
• Check whether other agencies are already involved in supporting the family
• Check exactly who was present and who lives in the household
Management
S afety of the child is absolute priority
M anage presenting medical problem appropriately
A lways discuss concerns with a senior paediatrician
C ontact Social Care
K eep clear and contemporaneous notes
Additional notes on differential diagnosis
Student report
“Fracture: I was asked about the differential diagnosis and what I would suspect if the child had blue
sclerae”
Osteogenesis imperfecta
• Hereditary condition, often autosomal dominant
• Mutation in gene coding for type 1 collagen
• Variable severity
• Child born with blue sclerae
• Mum may be in a wheelchair
• Associated with otosclerosis (conductive deafness) in 50%
• Associated with aortic regurgitation
• X-ray shows osteopaenia and multiple healed fractures
© Dr R Clarke 2023 support@askdoctorclarke.com 32
Essential Paediatrics
Mongolian blue spot
• Blue / grey discolouration present from birth
• “Dermal melanocytosis”: clusters of melanocytes deep in dermis
• Usually in Asian and Afro-Caribbean infants
• Disappear by 4 years of age
• Typically at base of spine and buttocks
• Also on legs and near wrists
• Main implication is that they can be confused with bruises
Scalded skin syndrome
• Superficial staphylococcal infection of skin
• With thin walled bullae that rapidly burst
• Leaving moist erythematous base- look like scalds
• Exfoliating toxin damages intercellular glycoprotein
responsible for epidermal cell adhesion (desmoglein 1)
• Typically affects skin folds and axillae
© Dr R Clarke 2023 support@askdoctorclarke.com 33
Essential Paediatrics
Post Course Notes: Turner Syndrome
Incidence: 1 in 2500 live born girls
Aetiology: Complete or partial absence of one of the X chromosomes
Diagnosis: Karyotype analysis
Clinical features: 1. Short stature
2. Non functioning ovaries
3. Abnormal appearance
Girls with Turner syndrome may have few clinical features, but short stature and infertility are nearly
always present. Therefore ALL girls presenting with short stature or delayed puberty should have their
karyotype checked.
Phenotypic features:
• Short stature (often normal growth until 3-4 years then slows)
• Low hairline
• Neck webbing
• Broad chest (widely spaced nipples)
• Increased carrying angle (cubitus valgus)
Associated features:
• Cardiac defects (e.g coarctation of the aorta)
• Renal anomalies
• Autoimmune thyroiditis
• Diabetes
• Middle ear disease
• Learning difficulties
• Hypertension
Management:
• Multidisciplinary, including a paediatric endocrinologist
• Growth hormone to optimize final height
• Sex hormone replacement (oestrogen to induce secondary sexual characteristics, progesterone to
induce menstruation)
• Monitor blood pressure
• Monitor for thyroid disease and diabetes
• Monitor for hearing loss
• IVF for fertility (using donor eggs)
• Family support: check www.tss.org.uk
© Dr R Clarke 2023 support@askdoctorclarke.com 34
Essential Paediatrics
Gastroenterology
Question 1
A baby boy is born prematurely at 34 weeks gestation. His birth weight is 2.00kg. Aged 8 weeks, his
weight is 3.40kg and at 12 weeks, it is 4.00kg. Plot these figures on the chart below, correcting for
gestational age where appropriate. What centile is he on at 12 weeks? What is a centile?
Question 2: What is the typical abnormality seen on blood gas analysis in pyloric stenosis?
Question 3: Watch the video. What is the most likely diagnosis? (Single best answer)
a) Gastroenteritis
b) Haemolytic uraemic syndrome
c) Intussusception
d) Necrotising enterocolitis
e) Urinary tract infection
Question 4: Sophie
3 year old Sophie has a 3 day history of fever, vomiting and diarrhoea. She is unwell and requires
intravenous fluids. The day after admission, you find that Sophie has passed no urine for 22 hours. She
has a GCS of 13/15 and appears slightly jaundiced. Haemolytic uraemic syndrome is suspected.
Which one of the following investigations would be the most likely to confirm the diagnosis?
a) Blood Culture
b) Clotting screen
c) FBC & blood film
d) Stool culture
e) Urine Culture
Question 5
A 4 year old girl has faltering growth. She has no immunodeficiency. The recommended initial test for
coeliac disease is
a) IgA anti-gliadin antibodies
b) HLA DQ 2 status
c) IgA anti-tissue transglutaminase antibodies
d) HLA DQ2 and DQ8 status
e) IgA anti-endomysial antibodies
© Dr R Clarke 2023 support@askdoctorclarke.com 35
Essential Paediatrics
Growth Charts
Student report
“The paediatric part of my osce was about faltering growth. We had to plot the boy’s weight on a growth
chart, and state what centile he was on.”
Paediatric growth charts
• Allow health professionals and parents to see whether a child is following an expected growth pattern
• Compiled using measurements from a cohort of many children
• Plotting on a centile chart shows how one child compares to others of same age and sex
Using a growth chart
• Select the right chart for the child’s sex
• Special charts for very premature babies <32/40 and for Down syndrome and cerebral palsy
• Use a single solid dot, not a cross or circle
• Serial measurements are key: crossing two or more centile lines should raise concerns
Plotting premature babies born from 32 weeks to 36+6
• Mark the birth weight at gestation in the left hand box and use this box until 42 weeks
• After this, use the 0-1 year graph with gestational correction
• Plot measurements at the child’s actual age and then draw a line back the number of weeks the infant
was preterm. Mark the spot with an arrow.
• Apply correction until at least 1 year of age
Example from question 1
Check your understanding
A baby girl is born at 30 weeks gestation. What is her corrected age at 12 weeks and 20 weeks old?
Answer to quiz question: centiles
At 12 weeks, he is on the 9th centile after correction for 6 weeks’ prematurity. A centile line defines the
weight below which a given percentage of a large population of children will be. Being on the 9th centile
line means that 9% of children of any given age will be lighter.
Student report (continued)
“We then got new information: the boy had GORD. We had to explain this condition to the father and
suggest appropriate non-drug measures that might help.”
© Dr R Clarke 2023 support@askdoctorclarke.com 36
Essential Paediatrics
Gastro-Oesophageal Reflux Disease (GORD)
Posseting vs GORD (NICE 2015)
• 40% of otherwise healthy babies have effortless regurgitation due to normal reflux after feeds
• Usually starts before 8 weeks and self-limiting by 12 months in 90%
• Many babies pull their legs up, arch their backs and scream after feeds (“Colic”)
• Only if the child is constantly miserable, coughing or wheezing after feeds or failing to put on weight is
the term GORD used
Red flags for alternative diagnosis
• Projectile vomiting (? pyloric stenosis)
• Green, bile-stained vomit (? obstruction)
• Chronic diarrhoea (? cow’s milk protein allergy)
• Haematemesis or melaena (? cause of bleeding)
• Persists beyond 1 year (? UTI or other cause)
• Acutely unwell with vomiting (? sepsis)
Simple posseting
Complications of GORD
• Problems related to vomiting milk
– Faltering growth, failure to thrive
• Problems related to acidity in oesophagus
– Oesophageal stricture
• Respiratory complications
– Apnoeic episodes
– Recurrent micro-aspiration with wheeze / pneumonitis
Note
• Oesophageal pH study rarely needed
• Significant GORD when acid present for >4% of day
• Refer for specialist assessment if complications develop or high-risk group (ex–prem or
neurodisability)
Explain to a mother what reflux is and what simple measures can help
© Dr R Clarke 2023 support@askdoctorclarke.com 37
Essential Paediatrics
Explain reflux
• The muscle ring at the lower end of the gullet isn’t as well developed as it is in older children
• Buzz words for a paediatrician: immaturity of the lower oesophageal sphincter
Simple measures
• Smaller more frequent feeds
• Wind baby during feeds
• Keep baby upright eg papoose sling
• Add thickeners to feeds (eg carob seed flour “Carobel” + wide teat)
Stepwise approach (Based on NICE 2015)
NB Risk of obstruction if concurrent use of thickened milk and alginate
Gastroenteritis and Haemolytic Uraemic Syndrome
Gastroenteritis
• Very common
• Commonly viral – Adenovirus, Enterovirus, Rotavirus (less common since vaccination)
• Less commonly bacterial – Salmonella, Campylobacter, E. coli O157
• Most cases self-limiting
• Some children require admission for rehydration
Clinical assessment (based on NICE 2009 and RCPI/ HSE 2014)
Favourite question: What are the signs of haemodyamic shock?
Answer: I-shocks
© Dr R Clarke 2023 support@askdoctorclarke.com 38
Essential Paediatrics
Treatment
Key principles
1) Use the nasogastric route to give fluids if the child is not shocked and not vomiting
2) If giving IV fluids use an isotonic crystalloid such as 0.9% sodium chloride solution
3) The amount of fluid to give is calculated by adding maintenance and the estimated deficit (and
sometimes ongoing losses)
4) Always discuss route, volume and rates of rehydration with a senior
5) Isolate children with diarrhoea and vomiting
Gastroenteritis: case history
Question 4: Sophie
3 year old Sophie has a 3 day history of fever, vomiting and diarrhoea. She is unwell and requires
intravenous fluids. The day after admission, you find that Sophie has passed no urine for 22 hours. She
has a GCS of 13/15 and appears slightly jaundiced. Haemolytic uraemic syndrome is suspected.
Haemolytic uraemic syndrome (HUS)
• Commonest cause of acute kidney injury in children
• Typically 1-2 days after onset of diarrhoea due to E. Coli O157
• Only 1 in 20 children with E Coli O157 get it
• Occasionally follows campylobacter or shigella
Triad
• Acute kidney injury
• Low platelets
• Haemolyic anaemia
Single best answer question:
Which one of the following investigations would be the most likely to confirm the diagnosis?
a) Blood culture
b) Clotting screen
c) FBC & blood film
d) Stool culture
e) Urine culture
© Dr R Clarke 2023 support@askdoctorclarke.com 39
Essential Paediatrics
Haemolytic uraemic syndrome: answer FBC and film
Low haemoglobin, low platelets, film will show fragmented red cells (“schistocytes”)
Red cells passing through fibrin mesh in arteriole Fragmented red cells result: schistocytes or helmet cells
Haemolytic uraemic syndrome: treatment
• Supportive +/- blood transfusion if needed
• Dialysis for acute kidney injury
• Antibiotics make it worse
• Significant morbidity and mortality
Pyloric Stenosis
Case history
• 4 week old baby boy
• 1 week history of vomiting
• Birth weight 3.2kg, current weight 2.9kg
On examination
• Scrawny
• Hungry
• Scaphoid abdomen
• Olive shaped mass right upper quadrant
Archie
Pyloric mass Distended stomach
© Dr R Clarke 2023 support@askdoctorclarke.com 40
Essential Paediatrics
Favourite questions
• Describe the presentation
• What investigations would you perform?
• Explain the acid base and electrolyte abnormalities
Hypertrophy of
sphincter
Pyloric stenosis
• Commonest surgical emergency of infancy
• Hypertrophy of the muscle in the gastric pylorus
• Progressive projectile vomiting secondary to gastric outflow obstruction
• Presents at 3-12 weeks of age
• Commoner in first-born males
Bilious vomiting (green) in neonates & infants Non-bilious vomiting (yellow)
Intestinal obstruction Pyloric stenosis
eg volvulus, duodenal or jejunal atresia, intussusception
Necrotising enterocolitis Gastro-oesophageal reflux
Gastroenteritis (severe) Gastroenteritis (mild)
Assess ABC: test feed if stable
• Observe a feed
• Witness a projectile vomit!
• Vomit is yellow not green as it is non-bilious
Further investigations
• Capillary blood gas – metabolic alkalosis
• Ultrasound: thickened and lengthened pyloric muscle
• U&Es may show raised sodium, urea, creatinine and a low potassium and chloride
Question 2: What is the typical abnormality seen in blood gas analysis in pyloric stenosis?
Capillary Blood Gas
pH 7.54 (7.25 -7.35) Alkalosis
pCO2 5.3 (4.5 – 6.0)
pO2 11 (10 -13)
HCO3 39 (22 – 26)
Metabolic alkalosis
BE + 12 (-2 to +2)
Na 149 (135 – 145)
K 2.9 (3.5 – 4.5) Hypokalaemic
Cl 89 (96 -106) Hypochloraemic
Hypokalemic, hypochloraemic metabolic alkalosis
Metabolic alkalosis
• With gastroenteritis, there is loss of acidic stomach juices together with alkaline small bowel
contents
• In pyloric stenosis, the vomiting is non-bilious: only acidic stomach juices are lost
• This results in a metabolic alkalosis with a raised bicarbonate level
• Buzz words: hypokalaemic, hypochloraemic, metabolic alkalosis
© Dr R Clarke 2023 support@askdoctorclarke.com 41
Essential Paediatrics
Raised bicarbonate
H2CO3 H+ + HCO3-
Lost due to vomiting Raised levels
of gastric juices Metabolic alkalosis
Two main reasons for hypokalaemia
• Potassium lost as KCl in vomit
• Dehydration activates renin-angiotensin-aldosterone system, resulting in renal sodium retention with
potassium loss in the urine (Na+/K+ exchange)
Hypochloraemia
• Loss of chloride along with hydrogen ions in gastric secretions
Management
• ABC and nil by mouth
• Nasogastric tube on free drainage
• IV access for fluid and electrolyte resuscitation and maintenance
• Surgery – Ramstedt’s pyloromyotomy
Yellow
I puked it up and though it was vile
It didn’t contain bile
So it was all yellow
I puked it up and though I was so small
It nearly hit the wall
And it was all yellow
I heaved with all my might
An olive on the right
And it was all yellow
My tongue, my tongue don’t look so well
Depressed, depressed fontanelle
Do you know: I’ve just puked myself dry, I’ve just puked myself dry
I puked it up: that acid was all mine
Now I’ve gone alkaline
My milk is all yellow
Look my chloride, now it has gone so low
Because of blocked outflow
And it was all yellow
High renin and high aldosterone
They make, they make my tubules moan
Do you know that my potassium’s low, that my potassium’s low
It’s true: hypochloraemia too, hypokalaemia too
Hypochloraemia
It’s true: hypokalaemia too, hypochloraemia too
© Dr R Clarke 2023 support@askdoctorclarke.com 42
Essential Paediatrics
Intussusception
Question 3
Watch the video. Single best answer: what is the most likely diagnosis?
c) Intussusception
Intussusception
• A paediatric surgical emergency
• Age 6 months to 2 years
• Characteristically episodic pain with screaming, drawing up legs and pallor
• Caused by one section of intestine “telescoping” into another
• Preceding viral illness – lymph node “lead point”
• Recurrent episodes may suggest a polyp or Meckel’s diverticulum
Bowel obstruction
• Causes fluid shifts and ischaemia
• “Redcurrant jelly stool” (stool mixed with blood and pus) is a late sign
Management: emergency
• Airway and breathing
• Circulation: IV access; fluid resuscitation
• Diagnosis: Ultrasound
• Treatment: Air enema reduction or surgery
Target or doughnut sign
© Dr R Clarke 2023 support@askdoctorclarke.com 43
Essential Paediatrics
Coeliac Disease
Coeliac disease: history On examination
• 3 years old • Distended abdomen
• Smallest in her class • Thin skin with loss of subcutaneous fat
• 5-6 loose stools per day • Wasted buttocks with reduced muscle bulk
• Difficulty weaning • Pallor (due to anaemia)
• Short stature
www.rcpch.ac.uk
www.rcpch.ac.uk
Height Weight
Coeliac disease
• Autoimmune disease triggered by gluten in cereals (wheat, barley and rye)
• Progressive flattening of the small bowel mucosa results in malabsorption with steatorrhoea
• Undiagnosed it can result in faltering growth, iron deficiency anaemia and osteopaenia
Pathophysiology
© Dr R Clarke 2023 support@askdoctorclarke.com 44
Essential Paediatrics
Serology (NICE 2015; ICGP 2015)
• Check total IgA: 2% have deficiency which can cause false negatives
• Check that child is on normal diet- gluten avoidance leads to disappearance of IgA antibodies
• This means at least one slice of bread per day for at least three weeks prior to test
• First line: IgA anti-tissue transglutaminase antibodies (tTG)
• If borderline, check IgA anti-endomysial antibodies (EMA)
HLA testing
• 95% of patients have DQ2 genotype and most of the rest express DQ8
• However, 30% of Caucasians have DQ2 and the vast majority do not have coeliac disease (CD)
• NICE (2015) recommend that HLA testing should not be performed routinely
• Occasionally specialists use a negative test to confirm that symptoms are unlikely to be due to CD
Diagnosis
• Duodenal or jejunal biopsy while on a normal
diet containing gluten (otherwise false negative
test result)
Buzz words: triad
• Crypt hypertrophy
• Lymphocytic infiltrate
• Subtotal villus atrophy
Normal Subtotal villus atrophy
Associated with
• Dermatitis herpetiformis
• Autoimmune disorders such as vitiligo,
pernicious anaemia, Hashimoto’s disease, type
1 diabetes (annual blood test for antibodies)
• Late development of small bowel lymphoma
Dermatitis herpetiformis
Treatment
• Lifelong gluten free diet
• Involve the paediatric dieticians
• Gluten re-challenge if diagnosed before two years old or diagnostic uncertainty eg cow’s milk
intolerance can occasionally cause sub-total villus atrophy
Post Course Note: Explaining CD to a patient and/ or parent: suggestions
• Autoimmune disease where the body attacks part of the gut
• Triggered by a protein called gluten which is found in cereals and flour
• The lining of part of the gut becomes sore/ inflamed and the normal finger-like projections get
flattened: this leads to difficulty absorbing food. Here’s a diagram…
• This can lead to tummy pain, diarrhoea, weight loss and tiredness
• Lifelong condition which gets better if you stop eating foods that contain gluten completely and forever
• There’s lots of help available from dieticians and also from self-help groups
• I’ll get an information leaflet for you….
© Dr R Clarke 2023 support@askdoctorclarke.com 45
Essential Paediatrics
Post Course Notes: Inflammatory Bowel Disease
Crohn’s and ulcerative colitis
• Chronic inflammatory bowel diseases of unknown aetiology
• Inappropriate activation of the mucosal immune system
• May present with abdominal pain and diarrhoea
• May cause total colitis, which may present acutely with a toxic megacolon (toxic dilatation)
Symptom severity grading
• Mild- less than 4 stools per day and systemically well
• Moderate- more than 4 stools per day and systemically well
• Severe- more than 6 stools per day or systemically unwell
• Systemically unwell: eg tachycardia, fever, anaemia, hypoalbuminaemia
Crohn’s disease
• A quarter of cases present in childhood and adolescence
• Commoner than UC in this age group
• Chronic, relapsing remitting inflammatory bowel disorder
• Can affect anywhere from mouth to anus: remember to look for mouth ulcers and to ask to check for
anal skin tags, fistulae and fissures
Pathology
• Typically affects terminal ileum; may extend into colon; skip lesions
• Terminal ileum involvement may lead to malabsorption- due to loss of bile salts
• Transmural inflammation with non-caseating granulomas
• May cause strictures, adhesions, fistulae and abscesses
Presentation
• Weight loss with diarrhoea and abdominal pain; bloody diarrhoea with colitis
• Growth failure with delayed puberty
• Systemic features: anaemia, fever, poor appetite
• Extra-intestinal: uveitis, arthritis, erythema nodosum, pyoderma gangrenosum
• Toxic megacolon
Investigations
• FBC may show evidence of anaemia (of chronic disease, or due to blood loss from colitis)
• Raised CRP and ESR
• Stool cultures negative; faecal calprotectin raised
• Barium follow-through: thickening of bowel wall, strictures, cobblestone mucosa, rose thorn ulcers
• Colonoscopy and biopsy
Treatment options
• Elemental diet for 6 weeks sometimes used to induce remission
• Anti-inflammatory aminosalicylates: sulfasalazine and mesalizine
• Steroids for relapses
• Azathioprine can be used to maintain remission in colitis and is “steroid sparing”
• Infliximab and other anti-TNF drugs
• Surgery
• See latest NICE guidance (2019)
See also notes on Functional Abdominal Pain (p84)
© Dr R Clarke 2023 support@askdoctorclarke.com 46
Essential Paediatrics
Respiratory Disease
Question 1
Watch the following video. List your clinical observations.
Question 2
What clinical signs would indicate a child was having a life-threatening asthma attack?
Question 3
You are called urgently to the emergency department by a nurse who is concerned about 3 year old
Jamie’s breathing. Jamie’s mother tells you he has had a cold for the last few days. Overnight he
developed a harsh cough and noisy breathing. He has a temperature of 37.9. The rest of the
observations are normal.
What sign of acute respiratory difficulty is being shown in this video clip? Select one answer only
a) Grunting
b) Head bobbing
c) Stertor
d) Stridor
e) Wheeze
Question 4
What is the most likely diagnosis?
a) Acute anaphylaxis
b) Epiglottitis
c) Inhaled foreign body
d) Severe quinsy
e) Viral croup
Question 5
Watch the video clip. What is the most likely diagnosis?
Name 5 key professionals involved in this child’s management.
© Dr R Clarke 2023 support@askdoctorclarke.com 47
Essential Paediatrics
Respiratory illness in children
Neonates Infants Under 5s Over 5s
Respiratory distress Bronchiolitis Viral induced wheeze Asthma
syndrome Pneumonia Croup Pneumonia
Pneumonia Croup Pneumonia Cystic fibrosis
Chronic lung disease Cystic fibrosis Cystic fibrosis
Congenital lung Chronic lung disease Epiglottitis
malformations Epiglottitis
Favourite exam topics
• Respiratory signs
• Bronchiolitis
• Asthma
• Viral induced wheeze
• Croup and epiglottitis
• Cystic fibrosis
NB Respiratory distress syndrome discussed later; plus post course notes on pneumonia
Respiratory Signs
Important clues on examination
• Agitated, distressed child or quiet, tired child
• Respiratory distress: head bobbing, nasal flaring, tracheal tug, tachypnoea, recessions, use of
accessory muscles, abdominal breathing
• Buzz words: increased work of breathing
Four important respiratory noises
• Stridor, stertor, grunting, wheeze
Stridor
• Sounds like ……………………………..
• Uniphasic, heard on inspiration
• A low to medium-pitched sound that signifies upper airway obstruction
• Croup, epiglottitis, bacterial tracheitis, severe tonsillitis, foreign body aspiration and anaphylaxis
Stertor
• Sounds like ……………………………..
• Noisy, snoring-type breathing that results from airflow obstruction higher up: in the nose,
nasopharynx or oropharynx
• Viral URTI (snotty nose!), obstructive sleep apnoea and craniofacial abnormalities.
Grunting
• Sounds like ………………………………….
• End-expiratory sound due to closure of glottis
• Self-induced positive end-expiratory pressure to keep airways open (“Self-PEEP”)
• Equivalent to “pursed lips expiration” in an adult with emphysema
• Severe respiratory distress
Wheeze
• Sounds like …………………………………
• A whistling sound on expiration: flow of high-velocity air through narrowed airways
• Asthma, viral induced wheeze, anaphylaxis and foreign body aspiration
© Dr R Clarke 2023 support@askdoctorclarke.com 48
Essential Paediatrics
Bronchiolitis
Student report
“We were shown a video of an infant in respiratory distress- to comment upon signs”
Bronchiolitis
• Usually occurs in children under 1 year old
• 1 in 3 infants will get it: only 2% need admission
• Seasonal: September/ October to February/ March
• Viral infection causes small airways obstruction
• 80% caused by respiratory syncytial virus (RSV)
• 20% due to adenovirus, influenza and parainfluenza viruses
Bronchiolitis
• Typically a 9 day illness
• 3 day prodrome with “cold” and harsh cough
• 3 days ill with fever, high-pitched wheeze and breathlessness
• 3 days recovering
Severity of Illness
0 3 6 9
Source: www.uptodate.com
Used with permission Days of Illness
On examination
• Low grade fever (<39 degrees) and tachycardia
• Increased respiratory rate
• Nasal flaring, harsh cough, wheeze
• Subcostal and intercostal recession
• Assess for cyanosis
• Auscultation: fine inspiratory crackles and expiratory wheezes
Investigation
• None in mild cases – clinical diagnosis based on symptoms and signs
• More severe cases:
• Capillary blood gas (looking for respiratory acidosis)
• CXR: not routine- only performed if diagnosis uncertain
• Nasal swab or nasopharyngeal aspirate for respiratory viruses
Admission indicated if DRAMAS (NICE 2021, RCPI/ HSE 2014)
• Dehydration
• Respiratory rate >70 (or marked recession or grunting)
• Apnoeic episodes
• Milk intake <50% of normal
• Appearance: ill or exhausted in view of health professional
• Saturations less than 90% on air or presence of cyanosis
Quality standards (NICE 2016 and RCPI/ HSE 2014)
• Do not give antibiotics, salbutamol or ipratropium
• Do not give inhaled or oral corticosteroids
• Do give fluids, oxygen and respiratory support
© Dr R Clarke 2023 support@askdoctorclarke.com 49
Essential Paediatrics
Management of bronchiolitis
Favourite exam question: which children are at risk of severe bronchiolitis?
At risk (DOH guideline 2015, RCPI/ HSE 2014)
• Infants born at or before 35 weeks gestation up to 6 months old
• Chronic lung disease in first 2 years
• Significant congenital heart disease in first two years
Palivizumab
• Given to premature babies with chronic lung disease
• Also those with cystic fibrosis and congenital heart disease
• Appears to make illness less severe
• Monoclonal antibody to RSV surface protein
• Passive immunity- not a vaccine
• Monthly IM injections for 6 months
• Costs > £500 for one 100mg ampoule
Bronchiolitis summary
In kids under one, there’s a common disease
With cough, snotty nose, crackles and wheeze
Always record the respiratory rate
If it’s severe, they’ll desaturate
Fluids, oxygen and feeding go in
But no antibiotics and no ventolin
And if you’re a prem or have lung or heart reasons
You’ll get pali injections during the season
© Dr R Clarke 2023 support@askdoctorclarke.com 50
Essential Paediatrics
Asthma
Asthma
• Chronic inflammatory disorder characterized by reversible airflow obstruction
• Hard to diagnose under 3 years old
• Typically associated with history of atopy (eczema, allergy, hay fever)
• Ask about previous prolonged / PICU admissions or IV therapy
Clinical assessment of acute asthma (Based on BTS/ SIGN 2019, RCPI/ HSE 2014)
Five PROPS for asthma assessment Severe asthma in a child over 5 years:
any one of
P- peak flow* 33% - 50% of best / predicted
R- respiratory rate More than 30/ min
O- oxygen saturations Less than 92%
P- pulse rate More than 125/ min
S- sentences Too breathless to talk or using accessory neck muscles
* PFR can usually be measured from aged 7 years
Life threatening features: “33, 92, CHEST”
33 PFR <33% of best or predicted
92 Oxygen saturations less than 92% with any one of:
C Cyanosis
H Hypotension
E Exhaustion with poor respiratory effort
S Silent chest
T Tired and confused (ie reduced conscious level)
Clinical case study
6 year old Adil presents to the emergency department at 05.00hrs with difficulty in breathing that has got
worse over night. He is known to have eczema and also has a blue inhaler prescribed by his GP. His
parents have tried two puffs but this has not helped. On examination he looks unwell and is using
accessory muscles of respiration. Afebrile, heart rate 150bpm, respiratory rate 50 bpm with expiratory
wheeze and he is too breathless to speak. O2 saturation: 87% in air. Auscultation: reduced air entry
bilaterally, with barely audible wheeze.
Asthma task
• Decide whether Adil is most likely to be having a severe or life-threatening attack
• Outline how you would manage Adil initially
© Dr R Clarke 2023 support@askdoctorclarke.com 51
Essential Paediatrics
Treatment of mild/ moderate asthma
• Often managed in the community
• Inhaled beta2 agonist via spacer: up to 10 puffs 30 seconds apart; repeated every 4 hours
• Oral prednisolone
• Admit if not responding quickly or out of hours presentation
Treatment of severe asthma
• Transfer to hospital urgently
• If SpO2 is less than 94%, give high flow oxygen
• Nebulised beta2 agonists (eg salbutamol 2.5mg under 5 years; 5mg over 5 years)
• “Burst therapy”: repeated every 20-30 minutes if needed, checking PFR
• Add nebulised ipratropium (250microgram) if not improving after initial nebuliser
• IV hydrocortisone 4mg/kg every 4 hours
Severe and not improving or life threatening
• Senior review and high dependency/ PICU
• Consider second line treatments (IV therapy) in addition to treatments above
• Magnesium sulphate used first
• Aminophylline or salbutamol by infusion if still not improving
Acute severe asthma: summary of treatment options
O = Oxygen if saturations below 94%
S = Salbutamol (via oxygen driven nebulizer)
H = Hydrocortisone (if can’t take oral prednisolone)
I = Ipratropium bromide nebulised
T = Theophylline (IV aminophylline)
Me = Magnesium sulphate (nebulised or IV)
Adil has a life threatening attack
• SpO2 of 87% and a relatively silent chest
• Initial treatment as for acute severe asthma
• Consider early IV therapy if not responding
• Get early assessment by seniors and anaesthetists
Peak flow rate
• Children aged over 7 can use a meter
• Encourage to keep a peak flow diary
• Twice daily to help make a diagnosis- looking for “morning dips”
• Sometimes used to monitor control
• Obtain early warning of an exacerbation
• A “fast blast” is better than a “slow blow”
See also: post course notes on chronic asthma p56
Viral Induced Wheeze
Viral induced wheeze
• Wheezing episode associated with viral URTI
• Typically children <5 years old
• Absence of strong history of eczema / hay fever (atopy suggests asthma)
• Previous episodes of wheeze, but PICU / prolonged admissions unlikely
• Buzz words: no interval symptoms
Management of viral induced wheeze (See NICE CKS 2017)
• Assess and manage acute cases as you would a child with asthma
• Steroids not effective in pre-school children with wheeze
• Only give steroids if pre-existing or suspected asthma
© Dr R Clarke 2023 support@askdoctorclarke.com 52
Essential Paediatrics
Croup and Epiglottitis
Quiz question 3
You are called urgently to the emergency department by a nurse who is concerned about 3 year old
Jamie’s breathing. Jamie’s mother tells you he has had a cold for the last few days. Overnight he
developed a harsh cough and noisy breathing. He has a temperature of 37.9. The rest of the
observations are normal.
Croup
• Acute viral laryngotracheobronchitis
• Commonest cause of stridor in children
• Coryzal illness (a “cold” with nasal discharge ) for a few days followed by
• Mild fever, hoarse voice, barking seal-like cough +/- respiratory distress
• Age 6 months to 6 years
• Parainfluenza virus (occasionally RSV / influenza)
Croup Epiglottitis
Very common Rare due to Hib vaccine
Mild to severely unwell Very unwell and toxic
Drooling not usually seen Drooling
Managed with steroids +/- adrenaline nebs Leave well alone. Get ENT and anaesthetist.
Antibiotics after securing airway.
Management of croup (based on CATS Guideline 2016)
Dexamethasone
• Long half-life: single oral dose usually enough
• Oral dose calculated as 150 micrograms per kg and ideally given prior to admission
• May be repeated on arrival at hospital and again after 12 hours if needed
• Typical 1-2 year old would receive 2mg (5ml of 2mg/5ml solution)
• Typical 3-4 year old would receive 3mg (7.5ml of 2mg/5ml solution)
© Dr R Clarke 2023 support@askdoctorclarke.com 53
Essential Paediatrics
Summary: bronchiolitis, croup and viral induced wheeze
Condition Bronchiolitis Croup Viral induced wheeze
Typical age Usually under 1yr 6/12 to 6 yrs Under 5s
In common, ↑ respiratory rate ↑ respiratory rate ↑ respiratory rate
may have ↑work of breathing ↑work of breathing ↑work of breathing
Typical Inspiratory crackles and Barking cough Expiratory wheeze
differences expiratory wheeze Inspiratory stridor No crackles
No crackles/ wheeze No stridor
Main Supportive Dexamethasone Bronchodilators
management
Cystic Fibrosis
Student report
“I was asked to do a respiratory examination on a 14 year old girl. At the end I was asked what the most
likely diagnosis was and who should be involved in her management”.
Question 5 from the quiz. Watch the video. What is the most likely diagnosis?
Name 5 key professionals involved in this child’s management
Cystic Fibrosis Bedside clues
• Commonest life limiting inherited disease of
Caucasians
• Autosomal recessive inheritance
• 1 in 25 people in the UK are CF carriers
• Commonest mutation is delta F508
• Neonatal screening has been in place since 2006
Pathophysiology
Mutation on chromosome 7
Abnormal transmembrane conductance regulator protein
(CFTR)
Responsible for cellular chloride transport
Thick secretions
Pancreatic insufficiency Recurrent chest infections
Bronchiectasis
Diabetes
mellitus Malabsorption
Faltering growth, chronic poor health
© Dr R Clarke 2023 support@askdoctorclarke.com 54
Essential Paediatrics
Investigations
Investigation Findings
Newborn screening Raised immunoreactive trypsin (IRT) on newborn bloodspot card
Sweat Test Gold standard. High chloride levels – 2 abnormal tests necessary for
diagnosis
Genetics >1600 mutations identified, >98% detectable on genetic testing
Chest x-ray Hyperinflation, peribronchial thickening, bronchiectasis
Lung Function Obstructive ventilatory defect
Sputum Haemophilus influenzae, Staph.aureus, Pseudomonas aeruginosa,
Burkholderia cepacia, E.coli, Klebsiella
Multidisciplinary management of cystic fibrosis
© Dr R Clarke 2023 support@askdoctorclarke.com 55
Essential Paediatrics
Post Course Notes: Pneumonia
Pneumonia: causes
• Up to a third of cases are viral (RSV, Parainfluenza, Adeno, Rhinovirus)
• Bacterial: Strep. pneumoniae, Mycoplasma pneumoniae, Chlamydia pneumoniae,
Staph. aureus, Haemophilus influenzae, Moraxella catarrhalis
Pneumonia: clinical features
• Symptoms: cough, difficulty in breathing, fever, poor feeding, chest pain
• Signs: respiratory distress, wheeze / crackles /reduced air entry on auscultation
• Bronchial breathing uncommon (when present implies consolidation)
• Sometimes upper abdominal tenderness
• Variable clinical severity
“Mild chest infection”
• Generally well child with fever and cough
• No signs respiratory distress
• Sats>93% in air
• Localising unilateral chest signs
• Tolerating oral fluids and passing urine
• No other risk factors
• The term “mild chest infection” is less alarming for parents than “pneumonia”
Management if mild
• At home
• Oral antibiotics (<5s get amoxicillin; >5s get a macrolide for 10 days eg erythromycin)
• Advice about fluids
• Advice about temperature control
• Advice about worrying symptoms and reasons to return
• No follow-up needed
Moderate to severe
• Unwell child
• Respiratory distress
• Oxygen requirement
• Poor fluid intake
Management if moderate to severe
• Admit to the ward
• Oxygen to maintain saturation >92%
• IV antibiotics + / - IV fluids
• Close observation for deterioration
Post Course Notes: Additional Notes On Chronic Asthma
Royal College of Physicians: 3 closed questions to assess control of asthma
• Have you had symptoms during the day?
• Have you had difficulty sleeping because of your symptoms? (Cough or wheeze)
• Does it interfere with normal activities? (Time missed from school, sports etc)
Other methods available, incorporating use of reliever and FEV (eg Asthma control questionnaire)
Preventers: step up and step down (see BTS / SIGN guidelines)
• Consider stepping up if using a reliever at least once per day 3 days per week
• If using one reliever inhaler per month, asthma is poorly controlled and needs review
• Concern that some children are over treated with inhaled corticosteroids (ICS)
• If good control for 3/12, consider slow step down with 25-50% reduction in ICS for 3/12
• Important to monitor growth annually in children with asthma
• Exhaled nitric oxide as measure of airway inflammation: low levels may help decision to step down
© Dr R Clarke 2023 support@askdoctorclarke.com 56
Essential Paediatrics
Chronic asthma aged under 5 years (Based on BTS/ SIGN July 2019)
Notes on children under 5 years
• Avoid long acting beta agonists (LABA: unlicensed and increased toxicity in under 5’s)
• Use very low (paediatric) dose of inhaled corticosteroids: eg beclometasone dipropionate “Clenil
modulite” 50 micrograms, 2 puffs twice daily
• If poor control, consider increasing the dose to low dose: 100 micrograms, 2 puffs twice daily
• If medium dose needed (200 micrograms, 2 puffs twice daily), refer for specialist assessment (step 4)
Montelukast
• Leukotriene receptor antagonist
• Used as a preventer/ controller in chronic asthma
• Single daily dose- granules or cherry flavoured tablet- both well tolerated
• Two thirds of children respond
• Main benefit in under 5’s but can be useful in older children (see notes below)
Chronic asthma aged over 5 years (based on BTS/ SIGN 2019)
Notes on children over 5
Step 2: very low dose ICS is the first line preventer for children
• For example, beclometasone dipropionate 50micrograms two puffs twice daily or
• “Pulmicort turbohaler” 100micrograms one puff twice daily
© Dr R Clarke 2023 support@askdoctorclarke.com 57
Essential Paediatrics
Step 3 often involves use of a combined inhaler with LABA and very low dose ICS
• Combined inhalers seem to improve adherence
• For example, if using dry powder device, “Symbicort turbohaler” (budesonide/ formoterol 100/6) one
puff twice daily
• If using metered dose inhaler, “Seretide evohaler” (fluticasone/ salmeterol 50/25) two puffs twice
daily, preferably with a spacer which improves drug delivery
• Consider stopping LABA if no improvement
• In step 3, a leukotriene receptor antagonist may be added as an alternative to LABA
Step 4
Additional therapy may involve a trial of montelukast or addition of slow release theophylline by mouth. If
medium dose ICS are used (beclometasone 200micrograms two puffs twice daily or equivalent), the
guidelines state:
• The child should be under the care of a specialist paediatrician for the duration of the treatment
• Give specific written advice about steroid replacement in severe intercurrent illness or surgery
All children with asthma should be offered
• A supported, written, self management plan
• Training in inhaler technique and have this checked at regular review
• Advice on weight loss if overweight and avoidance of triggers (eg tobacco smoke)
Older children should have checking of PFR and/ or spirometry when well in addition to when unwell
Post Course Notes: Peak Flow, Spacers and Inhalers
Peak flow meter: instructions
• Stand up when using the meter
• Zero the meter and hold it at the side so your fingers don’t get in the way of the pointer
• Take a big breath, clamp your lips round the mouthpiece and breathe out hard and fast
• “Imagine you’re trying to blow out all the candles on your birthday cake”
• Note the position of the pointer and then return it to zero
• Repeat this three times and record the best of your 3 attempts
Asthma gadgetry that may be presented in the exam
Metered dose inhalers (MDI) Dry powder inhaler(DPI) Spacers
(Example: “Turbohaler”)
Spacers
• Ideal for use with metered dose inhalers
• Bigger ones more efficient but bulky
• Aerochamber: medium: fits any inhaler
• To clean, rinse in warm water and drip dry
• Do not use a cloth: static leads to aerosol deposition on wall
• Used with face mask in pre-school children
© Dr R Clarke 2023 support@askdoctorclarke.com 58
Essential Paediatrics
Three Cases
Case One
Sajida is a 6 year old girl, previously fit and well. Her parents are concerned she may have
developed an allergy as her eyes have become very puffy over the last few days. There are no
associated breathing difficulties. On examination she has puffy ankles and a slightly distended abdomen
with shifting dullness.
Single best answer question: choose one investigation to help you make a diagnosis:
a) Blood culture
b) Serum IgE
c) Dipstick urine
d) Blood sugar
e) Abdominal x-ray
Case Two You are asked to look at this boy’s rash. Describe what you see?
E Warren: with permission
What diagnoses may cause a rash like this?
Case Three
5 year old James presents to the Paediatric Assessment Unit with a 1 day history of limping. There is no
obvious history of trauma and he is otherwise well. On examination James is afebrile with normal
observations. He is reluctant to weight bear on his left leg and there is some pain on internal rotation of
the left hip.
List four possible diagnoses that may explain this presentation
List four investigations useful in making a diagnosis in a child with a limp
© Dr R Clarke 2023 support@askdoctorclarke.com 59
Essential Paediatrics
Case One: Sajida
Urine dipstick shows: Protein ++++, Blood +, Ketones and glucose negative
An additional question might be: what is the most likely diagnosis? (Single best answer)
a) Urinary tract infection
b) Post-streptococcal glomerulonephritis
c) IgA nephropathy
d) Allergic urticaria with incidental proteinuria
e) Nephrotic syndrome
Nephrotic Syndrome
Proteinuria
Nephrotic
Syndrome
Hypoalbuminaemia Oedema
Nephrotic: massive protein leak
• Frothy urine with protein +++
• Hypoalbuminaemia
• Compensatory increase in liver protein synthesis
• Leads to increased lipoproteins & hyperlipidaemia
• Loss of immunoglobulins- risk infection
• Loss of anti-thrombin III- small risk of clotting
Investigations
• FBC- to check haematocrit (intravascular volume depletion) and for infection
• U&E and creatinine- to check renal function
• LFT- to check albumin (typically <25g/l)
Diagnosis and treatment
• From clinical features and confirmed proteinuria
• 95% of cases due to minimal change disease
• Renal biopsy not typically indicated
• ABC: may be fluid depleted. Careful fluid balance and IV albumin if fluids required
• Treatment is with a six week course of steroids (prednisolone)
• Penicillin prophylaxis against streptococcal infection
Classification
• Steroid resistant- 10% (need a biopsy)
• Steroid sensitive- 90%
– 30% resolves
– 30% one relapse
– 30% multiple relapses (steroid dependent)
Excellent prognosis if
• Aged 1 to 12
• No hypertension
• No macroscopic haematuria ie not nephritic
• No impaired renal function
• Normal complement levels
• Good response to steroids within 4 weeks
© Dr R Clarke 2023 support@askdoctorclarke.com 60
Essential Paediatrics
Glomerulonephritis
• Non-proliferative: most glomeruli look normal under the light microscope
• Proliferative: inflammatory cells in the mesangium (the connective tissue that supports the glomerular
capillaries)
Acute nephritic syndrome: abnormal HOST response?
H Hypertension
O Oliguria
S Smoky brown haematuria
T Trace oedema
• Immune complex disease; usually 2 weeks post streptococcal
• Low C3 and C4 and high anti-streptolysin ab
Nephrotic vs nephritic
Post course note: presentations of glomerulonephritis (simplified)
© Dr R Clarke 2023 support@askdoctorclarke.com 61
Essential Paediatrics
Case Two: Describe what you see
Rash affecting both legs with well defined purple round lesions, of varying sizes, some of which coalesce
over the ankles. This is consistent with a petechial / purpuric rash.
E Warren: with permission
Differential diagnosis of a non-blanching rash
• Infection: meningococcal septicaemia; other viral / bacterial infections
• Bleeding disorder: idiopathic thrombocytopaenic purpura, acute leukaemia,
haemolytic uraemic syndrome
• Vasculitis: Henoch-Schonlein purpura
• Mechanical / trauma: recurrent coughing / vomiting; non-accidental injury
Student report
History from a dad whose son had multiple bruises and 6 weeks of being unwell.
I was asked about differentials: HSP, ITP, ALL and NAI.
I discussed the differentials and the examiner seemed happy!
Condition ALL ITP HSP Meningococcal HUS
sepsis
Typical Fever and Well child with Well with Critically ill Unwell
presentation lymph nodes purpura purpura on with shock AKI
buttocks and Widespread Jaundice
lower limbs non blanching
rash
FBC and film Low Hb Normal Variable Low Hb
Blasts on film Schistocytes
High
lymphocytes
Low neutrophils Low platelets Normal Low platelets Low platelets
Low platelets platelets
Henoch-Schonlein purpura / IgA vasculitis
• 3 – 10 years of age
• Often history of recent URTI
• Type of IgA vasculitis
• Multi-system involvement
Henoch-Schonlein purpura
• Clinical diagnosis with “palpable purpura” on extensor surfaces
• Exclude other causes: check blood cultures if child unwell
• Check for hypertension / renal complications and for intussusception
• Symptomatic treatment
• 75% resolve spontaneously; minority develop long term renal complications
Idiopathic thrombocytopaenic purpura
• Petechiae (<3mm) and purpura (3-10mm) in a well child
• Immunologically mediated destruction of platelets, often 1-2 weeks after viral URTI
• Normal Hb and WCC; platelet count typically below 40 x109 /l
• Usually mild and resolves spontaneously in about three weeks
• Avoid NSAIDs and contact sports as 1 in 300 develop intracranial haemorrhage
• If severe with mucosal bleeding, may need treatment with IV immunoglobulin and steroids
• A few get chronic relapsing form; if severe, splenectomy may be needed
Student report
History-taking: "easy bruising". I was then shown FBC, clotting and blood film results. I was asked about
the diagnosis, which was ITP. I was then asked about the treatment. I said that in mild cases, it resolves
spontaneously, but that if more severe, steroids and immunoglobulins might be needed
© Dr R Clarke 2023 support@askdoctorclarke.com 62
Essential Paediatrics
Case Three: James
5 year old James presents to the Paediatric Assessment Unit with a 1 day history of limping. There is no
obvious history of trauma and he is otherwise well. On examination James is afebrile with normal
observations. He is reluctant to weight bear on his left leg and there is some pain on internal rotation of
the left hip. List four possible diagnoses that may explain this presentation. List four investigations useful
in making a diagnosis in a child with a limp.
Causes of a childhood limp
Age Painful limp Painless limp
1-3 Septic Arthritis Developmental dysplasia of hip
Transient Synovitis Congenital causes (e.g. cerebral palsy)
3-10 Transient Synovitis Perthes’ disease (chronic)
Septic Arthritis Juvenile idiopathic arthritis
Juvenile idiopathic arthritis
Perthes’ disease (acute)
Malignancy
10-16 Slipped upper femoral epiphysis (acute) Slipped upper femoral epiphysis (chronic)
Juvenile idiopathic arthritis Juvenile idiopathic arthritis
Septic Arthritis
Malignancy
Transient synovitis
• Commonest cause of acute limp in childhood
• Transiently inflamed synovium of hip
• Underlying cause unclear though often preceded by a viral infection
• Age 2-12 years; M:F = 2:1
• Unilateral sudden onset painful limp
• Pain may be referred to medial thigh or knee
• No pain at rest
Transient synovitis
• Mildly decreased range of movement
• 1/3 no restriction of movement
• Child well, no fever
• FBC, CRP, Blood Culture, X-ray- all normal
• Ultrasound scan shows joint effusion
• Treat with analgesia; NSAIDs reduce duration of symptoms
• Resolves spontaneously within a few days
Septic arthritis
• Acute painful hip with pain at rest
• Child often looks unwell & has fever
• Reluctance to move hip with decreased range of movement
• Neutrophil count & CRP- raised
• Diagnosis confirmed by joint aspirate culture
• Treatment- IV antibiotics & surgical drainage
• Without prompt treatment joint destruction can occur
• Organisms include: staph (75%), strep (20%); rarely (5%) gram negatives and salmonella (sickle)
© Dr R Clarke 2023 support@askdoctorclarke.com 63
Essential Paediatrics
Post Course Notes on Limp
Perthes’ disease
• Idiopathic ischaemia of femoral epiphysis
• Leads to avascular necrosis
• Re-vascularisation and re-ossification follows (over 1.5- 3 years)
• M:F = 5:1, Age 5-10 yrs
• Insidious onset of limp, initially painful
• Decreased range of movement (especially abduction & internal rotation)
Perthes’ disease
• X-ray (initially) - increased density of femoral head
• X-ray (later)- Irregular edge to femoral head
• Good prognosis if less than half of epiphysis involved & under 6 yrs
• Management generally conservative
• If severe, may need surgery
Slipped upper femoral epiphysis
• Displacement of femoral head; usually posteriorly & medially
• Age 10-15 years (coinciding with growth spurt)
• M > F (slight predominance); commoner with obesity
• Acute painful limp often after minor trauma
• Pain may be referred to knee
• Restricted range of movement (esp abduction & internal rotation)
Perthes’ disease (right hip) Slipped upper femoral epiphysis
Post Course Notes: Juvenile Idiopathic Arthritis
Juvenile idiopathic arthritis
• Arthritis for more than 6 weeks before age 16 years
• Rheumatoid factor is usually negative
• Antinuclear antibodies usually present in the commonest form: pauci-articular
• Some older girls with polyarticular disease similar to rheumatoid may be RF positive
Classified by onset
• Pauci-articular or oligoarthritis- 4 or fewer joints in first 6 months (60%)
• Polyarticular- 5 or more joints (20%)
• Systemic: Still’s disease (10%)
• Other: enthesitis related, psoriatic (10%)
Systemic JIA
• Usually before age 5 and affecting boys and girls equally
• Acute illness with high swinging fever and salmon coloured macular rash
• Systemic onset with myalgia may precede arthritis
• Lymphadenopathy and hepatosplenomegaly often present
• Pleurisy and pericarditis may occur; no eye involvement
• Anaemia, raised ESR and CRP typical of acute phase response
• Majority recover; one third progress to severe arthritis
• Differential from other causes of fever and myalgia, arthralgia:
• Rheumatic fever, Kawasaki’s, Leukaemia, SLE, reactive arthritis
© Dr R Clarke 2023 support@askdoctorclarke.com 64
Essential Paediatrics
Pauci-articular JIA
• Young children, typically aged 2-6 years; girls : boys = 4:1
• Medium sized joints- not hips, typically knees, ankles, elbows, wrists
• Asymmetrical oligoarthritis
• One third get chronic eye problems- anterior uveitis (iritis)- usually ANA positive
Polyarticular JIA
• Symmetrical involving any joint, typically hands, wrists knees
• Unlike rheumatoid arthritis, it spares the metacarpo-phalangeal joints (MCPs)
• Neck and temporo-mandibular joints may be involved
• More often progressive if onset in girls over 8years or if rheumatoid factor positive
Management options
• Multi-disciplinary approach including physio, OT and educational input
• Physiotherapy: passive movements, exercises, splints to prevent contractures, hydrotherapy
• Simple analgesia first – paracetamol, ibuprofen
• Steroid injection into joint often used in pauci-articular disease
• Disease modifying: methotrexate, systemic steroids, biologicals: anti-TNF eg infliximab
Post Course Note: Anti-thrombin III and Nephrotic Syndrome
Mechanism of action of anticoagulants
Intrinsic pathway Extrinsic pathway
Contact factor pathway Tissue factor pathway
Contact with damaged endothelium Tissue factors
XI Warfarin
I,
XI Inhibits
,I IX, X,VII
Rivaroxaban inhibits Xa
X,
I
VI
XI Heparin and
II
Fondaparinux
activate ATIII
Factor X Factor Xa
V Antithrombin III
inactivates
Warfarin inhibits II Prothrombin (II) Thrombin
Fibrinogen Fibrin
Loss of ATIII in nephrotic syndrome
Intrinsic pathway Extrinsic pathway
Contact factor pathway Tissue factor pathway
Contact with damaged endothelium Tissue factors
XI
I,
XI ATIII deficiency
,I
X,
I
VI
Inherited or
XI
II Acquired: leaks out
in nephrotic syndrome
Increased risk VTE
Factor X Factor Xa
Factor V Leiden mutation
Activated Antithrombin III
V
Prevents inactivation by aPC protein C inactivates
Factor V more active inactivates V
Increased risk VTE Prothrombin (II) Thrombin
Present in 30% of those with DVT
Fibrinogen Fibrin
© Dr R Clarke 2023 support@askdoctorclarke.com 65
Essential Paediatrics
Post Course Notes: Common Childhood Infectious Diseases
Measles
Incubation period 10 days; infectious until day 5 of rash
Ill child with fever, red eyes and a harsh cough
Koplik spots inside cheek on day 3 or 4 of illness (close to parotid duct)
Maculopapular rash spreading from behind ears to face and trunk becoming confluent
Rash alone not diagnostic as so many infections produce similar (“morbilliform rash”)
Complications more likely in immunosuppressed children: pneumonia, encephalitis
Very rare late complication: subacute sclerosing pan encephalitis
Mumps
Long incubation period 2-3 weeks
Fever typically for 4 days with unilateral parotitis, often becoming bilateral
Infectious for seven days from onset of parotid swelling
Complications: viral meningitis, orchitis
Rubella
Well child with low grade fever and erythematous rash all over body
Lymphadenopathy, particularly posterior auricular and occipital nodes
Risk to fetus if mother catches rubella in pregnancy (congenital rubella syndrome)
Chickenpox
Long incubation period like mumps: 2-3 weeks; then fever with widespread rash
Papules rapidly become vesicles and then form pustules and crusts
Infectious to others for seven days from the start of the rash
Rare complications: secondary bacterial skin infection and chickenpox pneumonia
Very rarely: varicella cerebellitis
Slapped cheek disease / erythema infectiosum
“Fifth disease” due to parvovirus B19
Virus can affect erythroblasts in bone marrow.
Child with low grade fever for a few days prior to developing bright red cheeks
Fine lace like rash may spread onto truck and limbs; may last several weeks
Can cause aplastic crisis in sickle cell disease
Infection in pregnancy can cause fetal anaemia, heart failure and death
Scarlet fever
Group A beta haemolytic streptococcus (strep. pyogenes) produces erythrogenic toxin
Typically in children aged 2 to 10 years old with high fever and sore throat
2 days later a rough rash starts on face, upper chest and armpits; then spreads to abdomen & limbs
Flushed red cheeks with circum-oral pallor
Swollen strawberry tongue (pale with red spots) with signs of tonsillitis
Mild form often called “scarlatina” with mild sore throat and low grade fever
Treated with penicillin V for 10 days and infectious for one day after course started
Fever usually lasts 4 days; rash typically peels within a week
Complications rare: sinusitis, pneumonia, meningitis
Late complications very rare: post streptococcal acute nephritis, rheumatic fever and invasive group A
streptococcal disease
Invasive group A streptococcal disease
Includes necrotising fasciitis and streptococcal toxic shock
See https://www.esht.nhs.uk/wp-content/uploads/2017/06/0447.pdf
© Dr R Clarke 2023 support@askdoctorclarke.com 66
Essential Paediatrics
Neonates: Test Yourself
1) What does the picture show?
2) What does the picture show?
3) What does the picture show?
4) What test is being performed on the right hip?
5) What does the picture show?
6) What does this picture show?
7) Teddy was born prematurely by emergency c-section at 31/40 and is now 12 hours old.
Observations: HR 195 bpm, RR 80, Sats 83% in 60% oxygen
Examination: Grunting, nasal flaring, intercostal and subcostal recessions, widespread inspiratory
crackles
What is the most likely diagnosis?
a) Tension pneumothorax
b) Meconium aspiration syndrome
c) Patent ductus arteriosus
d) Respiratory distress syndrome
e) Congenital diaphragmatic hernia
Teddy
© Dr R Clarke 2023 support@askdoctorclarke.com 67
Essential Paediatrics
Neonates
Neonates: favourite examination questions
• Neonatal examination findings
• Neonatal jaundice
• Complications of pre-term delivery
• The unwell term baby (pre-course work)
Definitions
Neonate: a baby (term and preterm) up to 28 days of age
Term baby: born between 37 and 42 weeks gestation
Preterm baby: born between 23 weeks and 36+6 weeks gestation
Neonatal Examination Findings
The newborn examination: “The baby check”
• All babies within 48 hours of birth
• Systematic examination to identify congenital anomalies or possible health problems
• “Head to toe” principle
• Be opportunistic – heart sounds before they cry, red reflexes when eyes open
• See helpful summary at http://patient.info/doctor/neonatal-examination
Q1: Facial capillary malformation / naevus
• “Port wine stain”
• Present at birth
• Flat and does not increase in size
• Ophthalmic and maxillary distribution
• Sturge-Weber Syndrome associated with
leptomeningeal angiomas and
• Seizures, glaucoma, hemiparesis
Infantile haemangioma (see pre-course work)
• Raised “strawberry naevus”
• Not present at birth
• Does increase in size
• Due to endothelial proliferation
• Not assoc. intracranial abnormalities
• Fades spontaneously by 5th birthday
Q2: Absent left red reflex
• Congenital cataract or retinoblastoma
Retinoblastoma
• Rare 1:20,000 births
• More commonly picked up later (9-22months)
Bilateral absence of red reflex
• Congenital cataracts eg rubella
• Failure of treatment can lead to amblyopia
Q3: Single transverse palmar crease
• 1 in 30 people
• May be associated with Down syndrome
www.en.wikipedia.com
• Fetal alcohol syndrome
• Other chromosomal abnormalities
© Dr R Clarke 2023 support@askdoctorclarke.com 68
Essential Paediatrics
Q4: Ortolani test right hip
• For developmental dysplasia of the hip
• Combined with Barlow test
• 1-20/1000 births
• Higher incidence in females, positive FH or
breech delivery
Begin with Barlow pushing femoral head
Backward
Q5 Bilateral talipes equinovarus
• Positional or fixed
• Foot flexed, in varus and supinated
Ask Abbie @ wix.com
• Can be associated with chromosomal
syndromes
• Treatment involves physiotherapy +/- surgery
“See sole in supination”
Neonatal Jaundice
Q6) What does this picture show?
A: a neonate with eye protection having phototherapy on a biliblanket
Jaundice in newborns
• 60% of term babies develop jaundice in the first week
• Most of those who develop jaundice longer than 24 hours after delivery are well and have
“physiological jaundice”
• It is important to consider alternative pathological causes of jaundice, particularly prior to 24 hours
• Two key issues: level of bilirubin and cause
Bilirubin metabolism and causes of neonatal jaundice
© Dr R Clarke 2023 support@askdoctorclarke.com 69
Essential Paediatrics
Level of bilirubin
• Unconjugated bilirubin crosses the blood brain barrier
• Damages the basal ganglia (kernicterus= yellow kernel)
• May cause acute encephalopathy (irritability, apnoea, convulsions)
• May also lead to dyskinetic cerebral palsy
Managing significant jaundice
• Adequate hydration through good feeding
• Mothers should continue to breastfeed
• Phototherapy breaks down bilirubin into easily excreted isomers
• Very high levels of jaundice may need an exchange blood transfusion
Phototherapy (NICE 2016 and RCPI/ HSE 2016)
• Check neonates regularly for visible jaundice in natural light: sclerae, gums, blanched skin
• Measure bilirubin urgently if visibly jaundiced
• Three risk factors for kernicterus: level of bilirubin, how fast level is rising, whether features of acute
encephalopathy are present
• Use gestation-specific chart to determine need for phototherapy
Serum bilirubin (SBR) chart for babies born at 38 weeks or later
Causes in those receiving phototherapy
• Idiopathic / “physiological” 50%
• ABO incompatibility 20%
• Rhesus incompatibility 10%
• G6PD deficiency 10%
• Infection 10%
• Other: liver disease, metabolic 10%
© Dr R Clarke 2023 support@askdoctorclarke.com 70
Essential Paediatrics
Investigations
Time frame Causes Investigations
Onset within ABO incompatibility FBC including haematocrit
24 hours Rh haemolytic disease U&E if dehydrated
Sepsis Serum bilirubin
Blood group
Direct antiglobulin test (Coombs test)
CRP and blood culture if suspected sepsis
Onset 24hours As above plus Transcutaneous bilirubin:
to 2/52 Physiological jaundice 80% well below treatment line: observe
Breast milk jaundice 20% close to or above: confirm serum level
Polycythaemia Admit for investigation
Prolonged >2/52 As above plus Check conjugated bilirubin
duration Biliary atresia Liver u/s
Hypothyroidism Urine culture
UTI G6PD levels if appropriate
G6PD deficiency
Liver disease
Physiological jaundice
• Commonest cause of neonatal jaundice
• Onset typically day 2-5 and resolves by 2 weeks
• High red blood cell volume at birth and decreased red blood cell survival
• Immature hepatic enzymes
• Exacerbated by poor feeding
Breast milk jaundice
• Onset at the end of the first week
• Commonest cause of prolonged jaundice beyond 2 weeks
• 10% are still jaundiced at 1/12, but gone by 2/12
• Precise mechanism unclear
• Breast milk may inhibit hepatic enzymes
Complications of Preterm Delivery
Preterm deliveries
Up to 1 in 10 pregnancies deliver before 37 weeks
Risk factors for preterm delivery include;
• Pre-eclampsia
• Multiple pregnancy
• Reduced or increased amniotic fluid
• Cervical insufficiency
• Sepsis - chorioamnionitis
Outcomes in preterm deliveries
• Babies born after 30 weeks typically do very well
• Babies born before 30 weeks (particularly <27 weeks) have lower survival rates and many will have
long term problems such as chronic lung disease / developmental difficulties
© Dr R Clarke 2023 support@askdoctorclarke.com 71
Essential Paediatrics
Complications of preterm delivery Retinitis of prematurity
• Hyperoxia from early resuscitation
releases free radicals which damage
retinal vessels (phase 1)
• Subsequent hypoxia leads to VEGF
production and neo-vascularisation
(phase 2)
• High oxygen and low oxygen levels
both implicated: drives me nuts!
Karaoke
Heads and hearts and lungs and guts, lungs and guts
Heads and hearts and lungs and guts, lungs and guts
And retinitis drives me nuts
Heads and hearts and lungs and guts
Heads
Haemorrhage Hypoxic ischaemic damage
Mainly in premature with very low birth weight Damage to deep white matter
Fragile vessels of germinal matrix Avascular “watershed zone”
Intraventricular haemorrhage Periventricular leucomalacia
If severe, risk of hydrocephalus Usually bilateral
¼ get damage to nearby internal capsule If severe, cysts may occur
“Periventricular haemorrhagic infarction” ¾ develop spastic diplegia
Unilateral: risk of spastic hemiparesis
Bilateral: risk of spastic quadriplegia
Lungs: respiratory distress syndrome eg question 6: Teddy
• Deficiency of surfactant from type 2 pneumocytes
• Production begins between 24-28 weeks and is adequate by 35 weeks
• Antenatal steroids promote production in threatened pre-term labour
Diagnosis and management
M O’Reilly With permission
ET tube
• RDS presents in the first 24 hours of life
• Increased rate and work of breathing, Diffuse
increasing oxygen requirement ground glass
• CXR classically shows ground-glass shadowing shadowing
and air bronchograms
• Respiratory support: oxygen, CPAP, ventilation
• Surfactant (“Curosurf”) via ET tube Air bronchograms
NG tube
Respiratory distress syndrome
© Dr R Clarke 2023 support@askdoctorclarke.com 72
Essential Paediatrics
Guts: necrotising enterocolitis
• Disease of preterms (rarely seen in term babies)
www.radiopaedia.com © Dr Frank Gaillard
• Bowel ischaemia, inflammation, necrosis, perforation
• Poor feed tolerance, abdominal distension and
bloody stools Dilated loops of bowel
• X-ray: air in the intestinal wall (pneumatosis
intestinalis)
• Bowel rest (NBM), total parenteral nutrition (TPN),
antibiotics Dark radiolucent line
• Surgery to remove perforated or necrotic bowel Within bowel wall
Pneumatosis intestinalis
Post Course Notes on Jaundice
Haemolytic jaundice
• Unconjugated bilirubin is produced as a result of haemolysis
• In newborns excessive haemolysis can occur in sepsis, or as the result of:
• Immune destruction – blood group ABO incompatibility, rhesus incompatibility
• Congenital RBC defects – hereditary spherocytosis, G6PD deficiency
• A positive Coomb’s test (direct antiglobulin test) in the presence of unconjugated hyperbilirubinaemia
suggests a haemolytic jaundice.
• Haemolytic jaundice may necessitate exchange transfusion as treatment (which not only removes
high levels of bilirubin, but also some of the pathological antibodies).
Congenital infections
• Maternal infections during pregnancy can have significant impact on the health of the neonate
• “TORCH” is a good way of remembering the list of serious congenital infections
T = Toxoplasmosis
O = Other (HIV, measles, parvovirus, hepatitis)
R = Rubella
C = Cytomegalovirus
H = Herpes Simplex
Congenital infections
• These infections can be associated with a variety of problems including congenital anomalies,
jaundice, anaemia, thrombocytopaenia, blindness, deafness and learning difficulties
NB
• A conjugated hyperbilirubinaemia should always be investigated as it may be the result of congenital
biliary atresia.
Biliary atresia
• Biliary atresia is a congenital abnormality (blockage/absence) of the bile ducts. Untreated it results in
progressive liver failure.
• Clinical signs include jaundice, pale stools, dark urine and a distended abdomen secondary to
hepatomegaly.
• Diagnosis involves imaging of the hepatobiliary system to confirm the presence of abnormal
pathways.
• Treatment is with Kasai hepatoportoenterostomy (if only external bile ducts involved) or liver
transplant (if intra-hepatic duct involvement). For best outcomes surgery should take place within the
first 2 months of life.
© Dr R Clarke 2023 support@askdoctorclarke.com 73
Essential Paediatrics
Neurology and Development
Test yourself
1) Case history Billy
• 2 years old, normally well
• Runny nose for two days
• Temperatures > 39oC
• 4 minute episode initially stiff, then jerking of all 4 limbs
• Now sleepy, but observations normal
• Red tympanic membrane right ear
Single best answer: what is the most likely diagnosis?
a) Meningitis with seizure secondary to cerebral irritation
b) First presentation of epilepsy
c) Febrile convulsion secondary to right otitis media
d) Status epilepticus secondary to viral upper respiratory tract infection
e) Breath holding attack
2) What can you see in this picture? Can you name a neurological condition in which a child may
need one of these?
3) By what age should a child be able to:
1) Walk?
2) Speak in 2 word sentences?
3) Ride a tricycle?
4) Following a febrile seizure, which factor does not predispose to future development of
epilepsy?
a) Family history of epilepsy
b) Febrile seizure lasting more than 15 minutes
c) Febrile seizure recurring several times in first 24 hours
d) Generalised onset of seizure
e) Developmental delay
© Dr R Clarke 2023 support@askdoctorclarke.com 74
Essential Paediatrics
Neurological Disorders
Topics in blue most likely to come up in exams
Symptoms
• Delayed development
- failure to acquire skills
- loss of skills
• Seizures
- obvious
- subtle
• Asymmetrical limb use – early “handedness”
• Problems walking – frequent falls, unsteadiness
• Headaches / vomiting
• Changes in behaviour / behavioural problems
Neurological examination in children
© Dr R Clarke 2023 support@askdoctorclarke.com 75
Essential Paediatrics
Febrile Convulsions
Question 1: Billy
Single best answer: what is the most likely diagnosis?
a. Meningitis with seizure secondary to cerebral irritation
b. First presentation of epilepsy
c. Febrile convulsion secondary to right otitis media
d. Status epilepticus secondary to viral upper respiratory tract infection
e. Breath holding attack
Febrile convulsions
• Commonest seizure disorder of childhood
• Affects approximately 1 in 30 children
• Typically between 6 months and 5 years of age
• A seizure associated with a fever
• Seizures are typically generalised and short in duration
• Fever may be due to UTI, URTI or other infection
• Not CNS infection: only 1% of those with a fit and a fever have meningitis
Billy: continued
Whilst you are examining Billy he has another episode of turning stiff, followed by rhythmic jerking of his
limbs for 2 minutes.
What is your initial management?
a) Give PR paracetamol and diclofenac to treat fever
b) Give buccal midazolam to terminate seizure
c) Assess ABC, give oxygen, call for help
d) Load with IV phenytoin to prevent further seizures
e) Give IV antibiotics to treat ear infection
Management of febrile seizures
• Always remember ABC (+ DEFG- don’t ever forget glucose)
• Symptomatic relief of high fever with anti-pyretics
• Find a focus for the fever, and treat with antibiotics if indicated
• Frightening to witness- it is normal for parents to think their child is dying
• Educate the parents about prognosis and outcomes in febrile seizures
Prognosis
• Febrile convulsions are not epilepsy
• The risk of recurrent febrile seizures during another febrile illness is approximately 30%
• If a child is developmentally normal, has no family history of epilepsy and presents with a simple
febrile seizure, the risk of developing epilepsy is the same as the population risk
Risk of epilepsy is increased if
• There are neurological abnormalities on examination or developmental delay
• Family history of epilepsy
• Presenting with complex febrile seizures (eg lasting longer than 15 minutes, with focal features or
recurring within the same illness)
4) Following a febrile seizure, which factor does not predispose to future epilepsy?
a) Family history of epilepsy
b) Febrile seizure lasting more than 15 minutes
c) Febrile seizure recurring several times in first 24 hours
d) Generalised onset of seizure
e) Developmental delay
Student report
“I was asked to explain a febrile convulsion to a worried mother”
© Dr R Clarke 2023 support@askdoctorclarke.com 76
Essential Paediatrics
Useful phrases
• A seizure which occurs when there is a sudden increase in temperature
• Usually at the start of a simple viral infection
• Affects 1 in 30 children between the age of 6 months and 5 years
• Very frightening to watch, but usually only lasts a few minutes
• Not epilepsy, so the long-term outlook is excellent and does not need regular medication
• May occur again if your child gets another sudden high fever
Epilepsy in Children
Epilepsy in children
• Seizure = a transient clinical event that is the result of abnormal electrical activity in the brain
• Epilepsy = a chronic brain disorder with recurrent (two or more) non-febrile seizures in the absence of
acute cerebral insult
• 75% idiopathic
• 75% well controlled by monotherapy
Classification of seizures
Electroencephalogram (EEG; see NICE 2012, updated 2020)
• Can’t exclude epilepsy- 50% of children with epilepsy have normal EEG
• After a first seizure can help predict risk of recurrence
• Consider sleep deprived EEG if standard EEG normal
• Can sometimes help determine seizure type
• Should not be done if non-epileptic attack disorder is suspected
Three main indications for MRI (NICE 2012, updated 2020)
• Onset before 2 years
• Focal features (from history, examination or EEG)
• Poor control despite first line antiepileptic drugs (AED)
Remember the 6 stage approach to potential status (seizure longer than 5 minutes: see pre-course
work and notes on Emergencies): Oh my Lord, let’s phone the anaesthetist!
Case history
Rory is a 5 year old boy. His teachers at school describe frequent brief episodes of “day-dreaming”.
During these episodes he does not respond to his name being called and cannot remember anything
about them afterwards
What is the most likely explanation?
a) Temporal lobe epilepsy
b) Atonic seizures (drop attacks)
c) Tonic seizures
d) Absence seizures
e) Tonic-clonic seizures
© Dr R Clarke 2023 support@askdoctorclarke.com 77
Essential Paediatrics
Absence epilepsy of childhood
• Children aged 4-10 years
• Transient loss of consciousness - often with open,
blinking eyes or twitching mouth movements
• Can be precipitated by hyperventilation
• Duration <30 seconds
• EEG typically shows 3Hz spike and wave
abnormality
• Treated with an anti-epileptic drug such as
ethosuximide or sodium valproate
• Most children “grow out” of absence epilepsy by
adolescence
Student report
“The child and parent were in the station, I was asked to take a history about the child's seizures, they
were absence seizures. Then I was asked about differentials especially non-epileptic causes in young
children.”
Case history
Maisie is a 5 month old baby girl. She is brought to the GP with recurrent episodes of “colic”. These
episodes involve Maisie crying, curling forward and stretching out her arms. She can do this up to 20
times in a row. These episodes are not associated with feeds or vomiting. She is thriving along the 75th
centile.
What is the most likely explanation?
a) Severe gastro-oesophageal reflux
b) Reflex anoxic seizures
c) Myoclonic seizures
d) Atypical absence seizures
e) Infantile spasms
West’s syndrome
• Onset of infantile spasms in first year of life
• A third have major organic disorder eg
• Underlying tuberous sclerosis or hypoxic
ischaemic encephalopathy
Triad of
1) Infantile spasms (“flexor spasms”)
2) Developmental delay Chaotic EEG: All the time
3) Hypsarrhythmia on EEG (“chaotic” pattern) Not just during an attack
Treatment
• Infantile spasms can be treated with steroids or vigabatrin
• Prognosis is poor with long term developmental and behavioural difficulties
• Most will go on to have other seizure types
Anti-epileptic drugs (See NICE 2012, updated 2020; and ROI HSE 2017)
Type of epilepsy First line drugs include
Generalised tonic-clonic (GTC) Lamotrigine or valproate*
Focal Carbamazepine or lamotrigine
Absence Ethosuximide or valproate*
Infantile spasms Prednisolone or vigabatrin
* Please note Avoid valproate in girls: high risk of
teratogenesis in pregnancy
Levetiracetam (“Keppra”)
• Second line for focal or generalised epilepsy if first line drug unsuitable or not tolerated
• Relatively expensive but generally well tolerated
© Dr R Clarke 2023 support@askdoctorclarke.com 78
Essential Paediatrics
Developmental Paediatrics
Question 3) By what age should a child be able to:
1) Walk? 18 months
2) Speak in 2 word sentences? 2 years
3) Ride a tricycle? Three years
Developmental assessment
Gross Motor Can they control their head? Can they roll? Can they sit? Can they walk or run?
Fine Motor (vision) Do they make eye contact? Do they follow with their eyes?
Can they hold onto big things? Can they hold onto little things?
What can they draw?
Language (hearing) Can they laugh? Can they babble? Do they have any words?
Can they speak in sentences?
Social / behavioural Do they smile? Do they wave goodbye? What do they play?
Can they feed themselves? Are they toilet trained?
Milestones
Age Gross Motor Fine Motor / Vision Language / Hearing Social / personal
3m Raises head and Follows a moving object Vocalises tunefully Smiles socially
chest when prone (6-8 weeks)
6m Rolls over, sits with Transfers objects Babbles Enjoys interaction
some support between hands
12 m Pulls to stand Pincer grasp Says “mama” “dada” Waves bye-bye
18 m Walks well Hand preference 6-12 words Uses spoon
Tower of 2-4 cubes Domestic mimicry
3 yr Rides a tricycle Circular scribbles 3-5 word sentences Make-believe play
Jumps in puddles Copies a circle Puts on clothes
Walks on tip toes Tower of 9 cubes
4 yr Hops on one leg Draws circles and squares Speaks clearly Plays well with other
6-word sentences children
5 yr Stands on one foot Draws triangle, people, Knows name, age Dresses and
for >10 seconds house address undresses self
See also Bellman et al (2013) BMJ 346: 31-35
Poem for some one year milestones Poem for some three year milestones
Now I am one, I have just begun At three I’ll get dressed and seldom depressed
To pull myself up to stand My sentences last all day
And wave “bye bye” with my hand And I’ll scribble and scribble away
For my next trick I’ll use pincer grip My tricycle goes and I’ll walk on tip toes
Which “Mama” and “Dada” think grand As a break from make-believe play
Case history
Timmy is brought to clinic by his parents. He is 2 and a half years old and appears “slower” than the rest
of the children at his nursery. He started walking 6 months ago and still is quite unsteady on his feet. He
tends to fall over to the right side. He is left-handed and doesn’t like to use his right arm. He was a
premature baby born at 32/40 by emergency c-section and needed resuscitation and ventilation at birth.
On examination he walks unsteadily, dragging his right foot along the ground. His right arm and leg are
stiff with brisk reflexes and an upgoing right plantar. The rest of the examination is normal.
• Do you think Timmy’s development is delayed?
• What do the findings on examination suggest?
• What might be the underlying cause for his difficulties?
© Dr R Clarke 2023 support@askdoctorclarke.com 79
Essential Paediatrics
Answers
Do you think Timmy’s development is delayed?
Timmy walked at 24 months – this is delayed
What do the findings on examination suggest?
Timmy has signs of a right sided hemiplegia – weakness with increased tone and reflexes in the
right arm and leg.
What might be the underlying cause for his difficulties?
Cerebral palsy secondary to prematurity and birth asphyxia
Cerebral palsy
• CP is not a single diagnosis: an "umbrella" term describing
• A non-progressive brain lesion that manifests as motor or postural abnormalities
• The lesion can occur at any point between conception and 3 years of age
• Typically presents as hypotonia/ poor feeding/ fits in a neonate and spasticity develops later
• Clinical diagnosis supported by brain MRI findings: eg periventricular leucomalacia
Causes of cerebral palsy
In utero Perinatal After delivery Unknown
Congenital Birth asphyxia Brain injury Common
infections Prematurity Meningitis
Kernicterus Encephalitis
Four common presentations
Spastic diplegia Equinovarus deformity
Spastic diplegic gait
• Equinovarus deformity at both ankles
• Adduction of hips with scissoring
• Associated rotation and swaying of trunk
• See helpful video at www.youtube.com/watch?v=xdMX3_q5NKk
© Dr R Clarke 2023 support@askdoctorclarke.com 80
Essential Paediatrics
Complications and associations
Student report
“There was a young girl in the bed with abnormal movements. She had a PEG tube. I was asked what it
was and what it was used for. I was also asked what I noticed about the girl. Said she had dyskinesia
and was asked about the different types and to differentiate between athetosis (writhing movements) and
chorea (jerky movements).”
Question 2) What can you see in this picture? Can you name a neurological
condition in which a child may need one of these?
This is a PEG – percutaneous endoscopic gastrostomy. Sometimes called a
“button”. Used in children with feeding difficulties or who need supplemental
feeds.
Duchenne muscular dystrophy
X-linked recessive Calf muscles: Complications:
1 in 4000 boys: onset 3-5 years Loss of dystrophin Diaphragmatic weakness
Motor delay & clumsiness Muscle cell damage Cardiomyopathy
Proximal myopathy (Gower) Replaced by fat & fibrous tissue Scoliosis and contractures
Creatine kinase & gene testing Calf pseudohypertrophy Cognitive impairment
© Dr R Clarke 2023 support@askdoctorclarke.com 81
Essential Paediatrics
Developmental assessment: test yourself
• We are going to show you a short video clip of a 3 year old girl.
• After watching the video clip:
• In pairs we’d like you to comment on her neurological and developmental findings
Notes on the video
Single best answer question
Which of the following conditions might best explain your observations?
a) Duchenne muscular dystrophy
b) Cerebellar brain tumour
c) Juvenile myoclonic epilepsy
d) Spina bifida
e) Cerebral palsy
Post Course Notes on Breath Holding Attacks and Reflex Anoxic Seizures
Breath holding attacks
• Common in 6 month to 2 year age group
• Pain or anger followed by brief crying
• Child takes a deep breath and stops breathing
• Turns blue and limbs extend
• Then limp with loss of consciousness
• Sometimes a few convulsive jerks; no post-ictal phase
Reflex anoxic seizures
• Also affect infants and toddlers
• Equivalent to a faint in older child
• Triggers: minor injury, cold food, fright, fever
• Vagal activation causes bradycardia
• Child turns pale and collapses to floor
• May induce tonic-clonic convulsion
Post Course Notes on Child Mental Health
Common child mental health conditions
• One in ten children between the ages of 1 and 15 have a mental health disorder
• Rates of mental health problems increase as children reach adolescence
• Child and adolescent mental health services (aka CAMHS or child psychiatry) are a separate clinical
speciality to Paediatrics. All paediatricians however are trained to recognize the key clinical features
of common mental health disorders in children
• Important mental health diagnoses include; anxiety, depression, conduct disorder, hyperkinetic
disorder (severe ADHD), self-harm, substance misuse and more rarely conditions involving
psychosis.
• Autism, whilst often diagnosed by Child Psychiatrists, is no longer considered a psychiatric disorder
and tends to be categorised with other neurodevelopmental conditions.
Autism and autistic spectrum disorder
• Prevalence of at least 1%
• More commonly diagnosed in boys than girls (ratio approx. 4 to 1)
© Dr R Clarke 2023 support@askdoctorclarke.com 82
Essential Paediatrics
Autism: triad of Impairment
Children typically present with impairment before the age of three years in each of the following
categories:
1. Reciprocal social interaction (features may include poor eye contact, difficulty
establishing/maintaining peer relationships, lack of shared enjoyment)
2. Social communication (including delayed or disordered speech, lack of gestures, absent imaginative
play)
3. Restricted, repetitive, stereotyped interests or behaviours (including preoccupations, adherence to
routines, stereotyped motor mannerisms)
Notes on autism
• Associated difficulties with learning (intellectual disability in 50%), behaviour (including eating and
sleeping), emotional well being
• Clinical picture very variable (dependent on underlying difficulties and environment)
• Diagnosis is usually based on the results of a variety of standardised neuropsychological tests
(ADOS/ADI, DISCO)
• Intervention is supportive and multi-disciplinary (paediatrics, SLT, OT, psychology) and multi-agency
(social care & education)
Attention deficit hyperactivity disorder
• Prevalence approx. 4% of boys and 1% of girls
• A behavioural disorder characterised by
a) Inattentiveness
b) Hyperactivity
c) Impulsiveness
Diagnosis and management
• Symptoms must be present before 7 years of age and observed in more than 1 setting (e.g. home
and school)
• Clinical features may include; “always on the go”, fidgety, noisy, disruptive, excessively chatty,
“doesn’t listen”, “always interrupting”, easily distracted, difficulty finishing tasks
• Diagnosis – not typically given to under 5s (many “symptoms” of ADHD can be confused with normal
variant pre-school child behaviour). A clinical diagnosis is made based on multi-source information
gathering and standardised guidelines.
• Management typically involves a combination of behavioural +/- pharmacological therapies. Drugs
used are typically stimulant medicines such as methylphenidate (Ritalin).
• Prognosis; 1/3 progress into adulthood without ongoing significant difficulties, 1/3 have some
persistent features, and 1/3 remain significantly impaired.
• Important co-morbidities include anxiety and mood disorders, and substance misuse.
Conduct disorder
• A pattern of persistent disruptive behaviour in which the basic rights of others and major age-
appropriate social norms are violated
• 5% of under 15 year olds in the UK have a conduct disorder – again, it is more common in boys
Features of conduct disorder
• Chronic conflict with parents, teachers etc.
• Aggressive behaviour towards people or animals
• Destructive behaviour towards property
• Lying
• Participation in anti-social behaviour such as stealing, truancy, substance misuse, running away
Diagnosis and management
• Diagnosis is based on clinical, psychiatric and psychological assessment
• Management primarily involves psychological therapy such as CBT (to help with problem solving,
anger management and impulse control)
• Co-morbidities include anxiety, depression, ADHD, substance misuse, learning difficulties
© Dr R Clarke 2023 support@askdoctorclarke.com 83
Essential Paediatrics
Post Course Notes: Functional Abdominal Pain
Functional abdominal pain: student report
“History: Functional abdominal pain in a child - I hate paeds. Chronic abdo pain, missing school for 3
months..blah blah blah. Parents just separated. Got asked about differentials and how to get the child
back into school (I was totally clueless...apparently there are co-ordinators). In the end I had to explain
the diagnosis to the father.”
Recurrent abdominal pain: differential
• Functional dyspepsia
• Irritable bowel syndrome
• Abdominal migraine
• Functional abdominal pain syndrome
Functional pain: clinical features
• Child well between attacks
• No weight loss / faltering growth
• No blood in stool or perianal disease
• Examination normal
Investigations
• Urine dipstick and MSU (exclude UTI and renal disease)
• FBC, ESR, CRP (exclude inflammatory bowel disease)
• Stool culture
• Stool microscopy for giardia
• Stool for calprotectin (raised in inflammatory bowel disease)
• Coeliac screen
Explanation
• Never say “It isn’t serious” as this can sound dismissive
• “Serious but not dangerous”: serious as it can interfere with normal activities
• Disturbance of the movement of the bowel which becomes sensitive
• Encourage healthy diet, exercise and school attendance
Reattribution: 3 components
• Acknowledge (“This pain is real”)
• Explain (eg “It is due to spasm of the bowel” or “Sensitive intestines which can feel the food going
round the bends”)
• Make the link (“Even minor stress can release adrenaline which can make the bowel go into spasm
more easily. I wonder if the trouble at school / family problems you told me about might be
contributing..”)
Good notes on this topic at
https://www.bsuh.nhs.uk/library/wp-content/uploads/sites/8/2020/06/Paediatric-Guidelines-Functional-
Abdominal-Pain-2018-2.pdf
© Dr R Clarke 2023 support@askdoctorclarke.com 84
Essential Paediatrics
Essential Paediatrics: Image Credits
Where no attribution is made, images and illustrations are © Dr R Clarke.
Most of the remaining images are in the public domain- mainly from Wikimedia, but occasionally from
Pixabay, Research Gate and Flickr. Creative commons licensing can be found at:
https://creativecommons.org/licenses/by/4.0/
Authorship is shown alongside the images. Links to the originals and details of editing are given below.
Copyright images
We have tried to trace and request permission from all authors of copyright images, but in some cases
this may not have been possible. If contacted, we will be pleased to rectify any errors or omissions as
soon as possible.
Paediatric Cardiology
Fallot’s tetraology
https://www.123rf.com/photo_35532466_crying-newborn-baby.html
Author: © Samantha Ireland @123rf; edited with addition of cyanosis
Down syndrome
https://www.flickr.com/photos/49428126@N00/240740614/in/album-72157594255900521/
© V Miles, used with permission
Projectile vomiting
https://www.youtube.com/watch?v=PUKMUZ4tlJg
Author: Thinkmodo; with permission
Thoracotomy: © M Radford, used with permission
Pulse oximeter: © J Petersen, used with permission
Traffic jam
https://commons.wikimedia.org/w/index.php?curid=13485990
Author: Andrew Smith @wikimedia
ASD video available to watch at https://www.youtube.com/watch?v=I5sRAcOVGiU
Author: Dr Robert Frankel, Maimonides Health Centre, New York. Also available at:
https://makeagif.com/gif/the-amplatzer-septal-occluder-device-Q7UNA0
Squatting posture
https://www.123rf.com/stock-photo/17343947.html
Author © Photobac @123rf, with license
Blalock shunt
https://commons.wikimedia.org/wiki/File:Blalock_shuntWiki.jpg
Author: Pezard @wikimedia
Duodenal atresia
https://commons.wikimedia.org/wiki/File:DuodAtres.png
Author: Kinderradiologie Stuttgart @wikimedia
Emergencies
Anaphylaxis Image © Anaphylaxis Australia, used with permission
Meningococcal sepsis rash
www.meningitis.org © Meningitis Research Foundation and used with permission
© Dr R Clarke 2023 support@askdoctorclarke.com 85
Essential Paediatrics
Meningitis
https://commons.wikimedia.org/wiki/File:The_diseases_of_infancy_and_childhood_(1910)_(1478386795
3).jpg Author: Internet Book Archive @wikimedia
Emerade diagram © and used with permission from www.emerade.com
Two cases
Blasts
https://commons.wikimedia.org/wiki/File:ALL_-_Peripherial_Blood_-_Diagnosis_-_01.jpg
Author: Author A Christaras @wikimedia
Gastroenterology
Growth charts: © RCPCH; used with permission
Posseting
https://www.123rf.com/stock-photo/141533736.html
Author: © T Amornporn @123rf, with license
Papoose sling
https://www.123rf.com/stock-photo/63154259.html
Author: © Jozef Polc @123rf, with license
Schistocyte
https://commons.wikimedia.org/wiki/File:Thrombi_in_patient_with_thrombotic_thrombocytopenic_purpura_.jpg
Author: Erhabor Osaro @wikimedia
Fibrin mesh and red cells
https://commons.wikimedia.org/wiki/File:Red_Blood_Cells_In_Clot.png
Author: Fuzis @wikimedia; cropped and colourised
Pyloric stenosis: unable to trace author
Doughnut sign diagram
https://www.journalmc.org/index.php/JMC/article/view/402/289
With permission Elmer Press: original article: R Abrahams , A Franco, K Lewis (2012) Pediatric Colocolic
Intussusception With Pathologic Lead Point: A Case Report
Coeliac disease endoscopy
https://commons.wikimedia.org/wiki/File:Celiac_endo.JPG Author: Samir @ wikimedia
Subtotal villus atrophy: © Dr Joseph Murray, Mayoclinic, with permission
Dermatitis herpetiformis: © Anthony J. Mancini MD, with permission
Ann & Robert H. Lurie Children’s Hospital of Chicago
Respiratory
Bronchiolitis- www.uptodate © and used with permission
https://www.uptodate.com/contents/bronchiolitis-and-rsv-in-infants-and-children-beyond-the-basics/print
Peak flow meter
https://commons.wikimedia.org/wiki/File:Treating_Kids_with_Asthma_(5)_(7163885241).jpg
Author FDA/ MJ Ermarth @wikimedia
Dexamethasone ampoule
https://commons.wikimedia.org/wiki/File:Dexamethasone_phosphate_for_injection.jpg
Author: LHcheM @wikimedia
Nebuliser device and creon medication picture: source untraceable
© Dr R Clarke 2023 support@askdoctorclarke.com 86
Essential Paediatrics
Three cases
Rash on legs E Warren @flickr with permission
Glomerulus diagram
https://commons.wikimedia.org/wiki/File:Renal_corpuscle.svg
Author: M Komorniczak @wikimedia; addition of labels and stars in editing
Perthes
https://commons.wikimedia.org/wiki/File:LCPdisease2015.png Author: J Heilman @wikimedia
SUFE
https://commons.wikimedia.org/wiki/File:Epilys.jpg Author: Jochen Lengerke @wikimedia
Neonates
Baby in incubator
https://commons.wikimedia.org/wiki/File:Neonatal_Jacoplane.jpg Author: Jacoplane @wikimedia
Port wine stain
https://commons.wikimedia.org/wiki/File:A_new_born_child_with_m-cm_syndrome..png
Author: ArturroD @wikimedia
Absent red reflex
https://www.pedseye.com/treatment/pediatric-cataracts/ © Dr Mark Steele with permission
Congen cataracts bilat absent red reflex
https://commons.wikimedia.org/wiki/File:Cataracts_due_to_Congenital_Rubella_Syndrome_(CRS)_PHIL_4284_lores.jpg
Author: CDC @wikimedia
Single transverse palmar crease
https://en.wikipedia.org/wiki/File:Simian_crease2.jpg
Author unknown
Talipes equinovarus
https://commons.wikimedia.org/wiki/File:Pied_bot,_varus_%C3%A9quin_(bilateral).jpg
Author: Brachet Youri
Lotus position
http://lia022.wix.com/yoga-with-abbie/apps/blog
© Used with kind permission Abbie Galvin @thestudio.yoga
Biliblanket
https://www.flickr.com/photos/chimothy27/2720183296/in/album-72157606449184104/
With kind permission M Evans
Teddy image
https://commons.wikimedia.org/wiki/File:Premature_infant_with_ventilator.jpg
Author: Ceejayoz @wikimedia
Ortolani diagram
©Prof RM Castelein @NTVG.nl, with permission
And https://dundeemedstudentnotes.wordpress.com/2014/02/
Normal fetal hip
https://commons.wikimedia.org/wiki/SMART-
Servier_Medical_Art#/media/File:Foetus_newborn_baby_4_--_Smart-Servier.png
Ultrasound of hip
https://europepmc.org/article/MED/28372341#free-full-text
Author: Kang YR, Koo J. Ultrasonography of the pediatric hip and spine. Ultrasonography (Seoul,
Korea). 2017 Jul;36(3):239-251.
© Dr R Clarke 2023 support@askdoctorclarke.com 87
Essential Paediatrics
Kernicterus
https://cluelessmedic.tumblr.com/post/82938412958/kernicterus-post-mortem-specimen
Image widely available on the www; original source and author unknown
Neonate outline diagram
Author and source unknown (originally from a blog, now untraceable)
Coronal section through brain
https://epos.myesr.org/esr/viewing/?module=viewing_poster&pi=138118
Open license Authors: I Ciocan, W Pabst, R Wolf @Epos
NEC image
https://commons.wikimedia.org/wiki/File:Neonatal_necrotizing_enterocolitis,_gross_pathology_20G0021
_lores.jpg
Author: CDC @wikimedia
Neurology and Development
Billy
https://www.123rf.com/stock-photo/113896888.html
© Tatiana Foxy @123rf, with license
Pat-a-cake
https://www.flickr.com/photos/jenni_lloyd/4069463804
Author: Jenni Lloyd @flickr
Spike and wave EEG
https://commons.wikimedia.org/wiki/File:Spike-waves.png
Der Lange @wikimedia
Hypsarrhythmia EEG
https://commons.wikimedia.org/wiki/File:Human_EEG_Comparison.jpg
Authors: A Cherninskyi & Ralphelg @wikimedia
Talipes
https://commons.wikimedia.org/wiki/File:Illustration_showing_treatment_of_a_clubfoot_Wellcome_L0066
938.jpg
Author: Wellcome Images @wikimedia; cropped and annotated during editing
Duchenne
https://www.flickr.com/photos/muscular_dystrophy_canada/3250950570/
Author: Muscular Dystrophy Canada @flickr
© Dr R Clarke 2023 support@askdoctorclarke.com 88
You might also like
- Wgu Pathophysiology Study Guide d236 Pathophysiology Exam Questions Completed With Correct AnswersDocument12 pagesWgu Pathophysiology Study Guide d236 Pathophysiology Exam Questions Completed With Correct AnswersAllstudy100% (1)
- NLE EssenceDocument59 pagesNLE EssenceFatima ShahNo ratings yet
- Priscilla's Medicine With Addon FinalDocument432 pagesPriscilla's Medicine With Addon FinalLee100% (1)
- Guyton Physiology Chapter 9 OutlineDocument18 pagesGuyton Physiology Chapter 9 Outlinebahahahah100% (5)
- Physical Medicine and Rehabilitation Oxford 2010Document482 pagesPhysical Medicine and Rehabilitation Oxford 2010montserrat santiago sanchezNo ratings yet
- Sel&Ass&Pae&Lis&Car&1 STDocument198 pagesSel&Ass&Pae&Lis&Car&1 STali tida100% (1)
- Case Presentation PreeclampsiaDocument41 pagesCase Presentation PreeclampsiaJomari Zapanta50% (2)
- The Boy Who Wasn’t Short: human stories from the revolution in genetic medicineFrom EverandThe Boy Who Wasn’t Short: human stories from the revolution in genetic medicineNo ratings yet
- Essentials of Pediatric Emergency MedicineFrom EverandEssentials of Pediatric Emergency MedicineRating: 4.5 out of 5 stars4.5/5 (3)
- Abnormal Heart Sounds: First Heart Sound (S)Document4 pagesAbnormal Heart Sounds: First Heart Sound (S)Faris Mufid MadyaputraNo ratings yet
- (Medbook4u.com) Pedd2897Ped PDFDocument667 pages(Medbook4u.com) Pedd2897Ped PDFkoNo ratings yet
- 1419Document369 pages1419Cảnh HoàngNo ratings yet
- Pediatric Cardiology Thesis TopicsDocument4 pagesPediatric Cardiology Thesis Topicspzblktgld100% (2)
- Birth Asphyxia - Conditions - UCSF Benioff Children's HospitalsDocument5 pagesBirth Asphyxia - Conditions - UCSF Benioff Children's Hospitalsbilalkhan02008No ratings yet
- LP1ncm109 YboaDocument21 pagesLP1ncm109 YboaMargarette GeresNo ratings yet
- Free Sketchy Guide - How To Honor Pediatrics Rotations v.050224Document9 pagesFree Sketchy Guide - How To Honor Pediatrics Rotations v.050224Prasoon KashyapNo ratings yet
- PANCE (Physician Assistant Nat. Cert Exam) Flashcard BookFrom EverandPANCE (Physician Assistant Nat. Cert Exam) Flashcard BookRating: 1.5 out of 5 stars1.5/5 (4)
- Bedside (Pediatrics)Document289 pagesBedside (Pediatrics)tajfaiz779No ratings yet
- Age With Moderate Dehydration New 1Document74 pagesAge With Moderate Dehydration New 1Jhade Relleta100% (1)
- Prenatal Counseling: Ventriculomegaly: and HydrocephalusDocument3 pagesPrenatal Counseling: Ventriculomegaly: and HydrocephalusHendri PrasetyoNo ratings yet
- Compications of Prematurity Wilson PDFDocument51 pagesCompications of Prematurity Wilson PDFMuhammad YaminNo ratings yet
- Congenital Heart Defect: Presented by Abhinay Sharma BhugooDocument46 pagesCongenital Heart Defect: Presented by Abhinay Sharma Bhugooabhinay_1712No ratings yet
- Shock: Recognition Recognition Recognition RecognitionDocument3 pagesShock: Recognition Recognition Recognition RecognitionSuryadi P. Dwipayana, Ida BgsNo ratings yet
- Encephalo CeleDocument11 pagesEncephalo CeleMike Faustino SolangonNo ratings yet
- What Is Hydrocephalus?Document8 pagesWhat Is Hydrocephalus?Urej BandiolaNo ratings yet
- (Mebooksfree - Net) Rev Que Pae Emq Ans 1stDocument142 pages(Mebooksfree - Net) Rev Que Pae Emq Ans 1staeyousefNo ratings yet
- Pediatrics 2005 Trotter 771 83Document16 pagesPediatrics 2005 Trotter 771 83Ligia RiosNo ratings yet
- Pocketbook For Management of Diabetes in Childhood and Adolescence in Under-Resourced CountriesDocument56 pagesPocketbook For Management of Diabetes in Childhood and Adolescence in Under-Resourced Countriesdiabetes asiaNo ratings yet
- Topic 2. BSN 3Document6 pagesTopic 2. BSN 3Anthony jesusNo ratings yet
- Spotlight On HealthDocument40 pagesSpotlight On HealthNCCScribdLoginNo ratings yet
- The Compass 2015Document178 pagesThe Compass 2015Venture Publishing100% (1)
- Letters To The Editor: ReferenceDocument2 pagesLetters To The Editor: ReferenceEvelina Lestari NapitupuluNo ratings yet
- Periventricular Leukomalacia PVLDocument1 pagePeriventricular Leukomalacia PVLJonathan wiradinataNo ratings yet
- Case Study of Chronic Kidney DiseaseDocument54 pagesCase Study of Chronic Kidney DiseaseJomari Zapanta100% (4)
- Understanding Diabetes for Action: Rethinking How You Handle Diabetes a Holistic ApproachFrom EverandUnderstanding Diabetes for Action: Rethinking How You Handle Diabetes a Holistic ApproachNo ratings yet
- 50 Cases in CardiologyDocument253 pages50 Cases in CardiologyEleonora DraganNo ratings yet
- Pediatrics Workbook 2024Document100 pagesPediatrics Workbook 2024CastleKGNo ratings yet
- Textbook Paediatrics A Core Text On Child Health Second Edition Tony Waterston Ebook All Chapter PDFDocument50 pagesTextbook Paediatrics A Core Text On Child Health Second Edition Tony Waterston Ebook All Chapter PDFhelen.black690100% (5)
- To Be ConDocument53 pagesTo Be ConLiza AingelicaNo ratings yet
- Medical Management of Children With Down SyndromeDocument8 pagesMedical Management of Children With Down SyndromeMariana OrozcoNo ratings yet
- Pocketbook For Management of Diabetes in Childhood and Adolescence in Under-Resourced CountriesDocument60 pagesPocketbook For Management of Diabetes in Childhood and Adolescence in Under-Resourced Countriesdiabetes asia100% (1)
- LFAC ISPAD Pocketbook 2nd Edition Low ResDocument60 pagesLFAC ISPAD Pocketbook 2nd Edition Low ResAndreea Katy100% (1)
- Recipe Book For Babies Who Need To Make The Most of Every MouthfulDocument23 pagesRecipe Book For Babies Who Need To Make The Most of Every MouthfulAditya Ikhsan PrasiddhaNo ratings yet
- Thesis On Birth AsphyxiaDocument4 pagesThesis On Birth Asphyxiaimmkhuwhd100% (3)
- Newborn Screening TestDocument29 pagesNewborn Screening Testjinky_bsantos@yahoo.comNo ratings yet
- Hydrocephalus Lesson PlanDocument12 pagesHydrocephalus Lesson PlanUday KumarNo ratings yet
- Pummilli690910 30 10 2010 PDFDocument374 pagesPummilli690910 30 10 2010 PDFJacqline CharlesNo ratings yet
- CyanosisinNewborn NS122142Document25 pagesCyanosisinNewborn NS122142Rosdiana Elizabeth SiburianNo ratings yet
- Congenital MalformationsDocument33 pagesCongenital MalformationsMoumita BatabyalNo ratings yet
- A Premature Infant Is An Infant Born Before 37 WK GestationDocument5 pagesA Premature Infant Is An Infant Born Before 37 WK GestationKamila KawaiiNo ratings yet
- Apnoea Bradycardia PremDocument2 pagesApnoea Bradycardia PremmusafirlautNo ratings yet
- Approach To Acute Diarrhea ScriptDocument11 pagesApproach To Acute Diarrhea ScriptChinenye ModestaNo ratings yet
- Kegawatan Pada AnakDocument80 pagesKegawatan Pada AnakbubujuhumNo ratings yet
- Multimedia: Umbilical HerniaDocument9 pagesMultimedia: Umbilical HerniaPetric Libut PhilanthropiaNo ratings yet
- NICU-by SreedharDocument18 pagesNICU-by SreedharSreedhar Nakka KenniNo ratings yet
- Children With Achondroplasia Guidance For Parents and Health Care ProfessionalsDocument22 pagesChildren With Achondroplasia Guidance For Parents and Health Care Professionalshorace35No ratings yet
- Working with Children Who Need Long-term Respiratory SupportFrom EverandWorking with Children Who Need Long-term Respiratory SupportNo ratings yet
- Top 10 Differential Diagnoses in Family Medicine - CoughDocument2 pagesTop 10 Differential Diagnoses in Family Medicine - CoughTiza OyonNo ratings yet
- Preemie ReferenceDocument22 pagesPreemie ReferenceurhighnxssNo ratings yet
- Practice Test (2014)Document16 pagesPractice Test (2014)Ali GhahremanNo ratings yet
- Child With Gastrointestinal Dysfunction: 1. Intestinal ObstructionDocument12 pagesChild With Gastrointestinal Dysfunction: 1. Intestinal Obstructionمحمد الملكNo ratings yet
- Guideline Rheumatic Disease in Children PDFDocument432 pagesGuideline Rheumatic Disease in Children PDFMada Dobos100% (1)
- Finals Ha Lec Heart and Neck Vessel, Peripheral Vascular Systems, Assessing The AbdomenDocument8 pagesFinals Ha Lec Heart and Neck Vessel, Peripheral Vascular Systems, Assessing The AbdomenNel joy PaurilloNo ratings yet
- Maternal Cardiovascular and Hemodynamic Adaptations To PregnancyDocument13 pagesMaternal Cardiovascular and Hemodynamic Adaptations To PregnancyAnchalia ChandrakumaranNo ratings yet
- Physical Examination Techniques and ManueversDocument160 pagesPhysical Examination Techniques and ManueversMa-anJaneDiamosNo ratings yet
- EI2311-Biomedical Instrumentation Question BankDocument20 pagesEI2311-Biomedical Instrumentation Question BankrajapandiyaNo ratings yet
- Home Work Ni Wayan SutariDocument12 pagesHome Work Ni Wayan SutariMuhammad RihadiNo ratings yet
- Natalya Master CardioDocument71 pagesNatalya Master CardioTaman Hoang100% (1)
- Malaika Ifx DZ SummaryDocument17 pagesMalaika Ifx DZ SummaryZhi Ning CNo ratings yet
- Valvular Heart DiseaseDocument85 pagesValvular Heart DiseaseWilliam Lie100% (2)
- Impaired Verbal CommunicationDocument6 pagesImpaired Verbal CommunicationLaura Sansonetti100% (1)
- Cvs - Clinical NotesDocument38 pagesCvs - Clinical NotessekaralingamNo ratings yet
- 1800 MCQ Revised VersionDocument606 pages1800 MCQ Revised VersionFarah FarahNo ratings yet
- Physical Examination in PaediatricsDocument162 pagesPhysical Examination in PaediatricsUsman Ali100% (1)
- Cor Pulmonale IkaDocument19 pagesCor Pulmonale IkaIka Lukita SariNo ratings yet
- Mastery Question MDFDocument66 pagesMastery Question MDFshaaish100% (1)
- Nursing Health Assessment Exam 2Document45 pagesNursing Health Assessment Exam 2Jennifer Jaworsky100% (3)
- Cardiac Disease in PregnancyDocument44 pagesCardiac Disease in PregnancyNariska Cooper100% (1)
- Health AssessmentDocument35 pagesHealth AssessmentKm GaputanNo ratings yet
- Anatomy and Physiology Ii-Dm Cardiovascular Sys-1Document64 pagesAnatomy and Physiology Ii-Dm Cardiovascular Sys-1Mathews showsNo ratings yet
- Nclex ExamDocument24 pagesNclex ExamJheanAlphonsineT.MeansNo ratings yet
- Wigger's Diagram WorksheetDocument6 pagesWigger's Diagram WorksheetYina BambinaNo ratings yet
- Cardiology Quick Revision Final 3Document215 pagesCardiology Quick Revision Final 3bsjdbd dbNo ratings yet
- Approach To Heart MurmursDocument57 pagesApproach To Heart MurmursRadley Jed PelagioNo ratings yet
- Physiology of The Cardiovascular System-CVSDocument56 pagesPhysiology of The Cardiovascular System-CVSAmanuel MaruNo ratings yet
- Ncert Ans Class 5 Evs ch15 Blow Hot Blow ColdDocument8 pagesNcert Ans Class 5 Evs ch15 Blow Hot Blow ColdPuja DoraNo ratings yet
- 07 - 01 - Assessment of Cardiovascular SystemDocument55 pages07 - 01 - Assessment of Cardiovascular SystemSalman Habeeb50% (2)
- Clinical Assessment of The Cardiac Patient 2 2Document15 pagesClinical Assessment of The Cardiac Patient 2 2Lindsay JohnstonNo ratings yet