Professional Documents
Culture Documents
SUPER Multiplanar CT and MRI of Collections in The Retropharyngeal Space Is It An Abcess
SUPER Multiplanar CT and MRI of Collections in The Retropharyngeal Space Is It An Abcess
Uploaded by
punct_org3256Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
SUPER Multiplanar CT and MRI of Collections in The Retropharyngeal Space Is It An Abcess
SUPER Multiplanar CT and MRI of Collections in The Retropharyngeal Space Is It An Abcess
Uploaded by
punct_org3256Copyright:
Available Formats
N e u r o r a d i o l o g y / H e a d a n d N e c k I m a g i n g • P i c t o r i a l E s s ay
Hoang et al.
Multiplanar Imaging of Retropharyngeal Space
Neuroradiology/Head and Neck Imaging
Pictorial Essay
Downloaded from www.ajronline.org by 92.83.161.47 on 03/28/23 from IP address 92.83.161.47. Copyright ARRS. For personal use only; all rights reserved
Multiplanar CT and MRI of
Collections in the Retropharyngeal
Space: Is It an Abscess?
Jenny K. Hoang1 OBJECTIVE. The purpose of this article is to describe a practical imaging approach to
Barton F. Branstetter IV2 evaluating collections in the retropharyngeal space.
James D. Eastwood1 CONCLUSION. The differential diagnoses for fluid in the retropharyngeal space in
Christine M. Glastonbury 3 clude both noninfectious and infectious processes. The multiplanar capabilities of CT and
MRI are ideal for characterizing and delineating collections. In this pictorial essay, we de
Hoang JK, Branstetter BF IV, Eastwood JD, scribe the anatomy of the retropharyngeal space and offer a four-step approach to evaluating
Glastonbury CM retropharyngeal collections on multiplanar imaging.
T
he retropharyngeal space spans The alar fascia, a deep layer of the deep
the skull base to the mediasti cervical fascia, divides the retropharyngeal
num and normally contains fat space into two components: the true retropha
and lymph nodes. The main ryngeal space and the danger space (Fig. 1).
causes of fluid expanding the retropharyn The anterior true retropharyngeal space ex
geal space can be divided into noninfectious tends from the clivus to a variable level from
retropharyngeal edema and retropharyngeal T1 to T6 vertebrae, where the alar fascia fuses
Keywords: retropharyngeal abscess, retropharyngeal infection, including suppurative retrophar with the visceral fascia to obliterate the true
cellulitis, retropharyngeal edema, retropharyngeal yngeal nodes and retropharyngeal abscess. retropharyngeal space [2]. The posteriorly lo
nodes, retropharyngeal space The multiplanar capabilities of CT and MRI cated danger space, however, extends further
are ideal for characterizing and delineating inferiorly into the posterior mediastinum and
DOI:10.2214/AJR.10.5116
collections. In this pictorial essay, we present to the level of the diaphragm. Because the
Received June 8, 2010; accepted after revision the anatomy of the retropharyngeal space alar fascia is very thin, the danger space and
August 23, 2010. and offer a practical approach to evaluating true retropharyngeal space cannot be distin
retropharyngeal collections on multiplanar guished on imaging in a healthy patient.
C. M. Glastonbury is an investor and consultant for
Amirsys.
imaging. Important points to remember are The normal contents of the retropharynge
that one, a suppurative retropharyngeal node al space include fat, small vessels, and lymph
J. K. Hoang is a GE-AUR fellow for 2010–2011. is contained by the nodal capsule; two, a ret nodes. The retropharyngeal nodes drain the na
1
ropharyngeal space abscess is contained sopharynx, oropharynx, nasal cavity, parana
Department of Radiology, Division of Neuroradiology,
only by the fascia of the retropharyngeal sal sinuses, middle ears, and prevertebral space.
Duke University Medical Center, Box 3808, Erwin Rd,
Durham, NC 27710. Address correspondence to space and has the potential for devastating Retropharyngeal nodes are often large in chil
J. K. Hoang (jenny.hoang@duke.edu). complications from mass effect and the dren and begin to atrophy before puberty.
spread of infection; and three, retropharyn
2
Department of Radiology, University of Pittsburgh, geal space edema is noninfectious and re Imaging Approach
Pittsburgh, PA.
solves spontaneously as its cause is treated. We recommend that the interpretive ap
3
Departments of Radiology and Biomedical Imaging, proach to a retropharyngeal space collection
Otolaryngology–Head and Neck Surgery, and Radiation Normal Anatomy include an evaluation of multiplanar imaging
Oncology, University of California, San Francisco, Understanding the anatomy of the retro for four characteristics: distribution of fluid,
San Francisco, CA.
pharyngeal space is the key to appreciating configuration and mass effect, presence or
WEB the spread of infection and formation of a absence of a thick enhancing wall, and ancil
This is a Web exclusive article. retropharyngeal abscess [1] (Fig. 1). The ret lary findings (Table 1).
ropharyngeal space is posterior to the phar
AJR 2011; 196:W426–W432
ynx and esophagus and anterior to the pre Retropharyngeal Edema
0361–803X/11/1964–W426 vertebral muscles. It is bound by the visceral Retropharyngeal edema is the presence of
fascia anteriorly, the prevertebral fascia pos nonpurulent fluid in the retropharyngeal space.
© American Roentgen Ray Society teriorly, and the carotid sheaths laterally. The accumulation of fluid is thought to be due
W426 AJR:196, April 2011
Multiplanar Imaging of Retropharyngeal Space
TABLE 1: Four-Step Interpretive Approach to Retropharyngeal Space Collection on Multiplanar Imaging
Step Retropharyngeal Edema Suppurative Retropharyngeal Node Retropharyngeal Abscess
Fluid distribution Fills the retropharyngeal space from Unilateral Fills the retropharyngeal space from
side to side side to side
Configuration and mass effect Axial images show ovoid, rectangular, Rounded or ovoid configuration; mass Rounded or ovoid configuration;
or “bow-tie” configuration; sagittal effect varies moderate-to-marked mass effect
Downloaded from www.ajronline.org by 92.83.161.47 on 03/28/23 from IP address 92.83.161.47. Copyright ARRS. For personal use only; all rights reserved
images show diffuse configuration
with tapered inferior and superior
margins; mild mass effect
Thick enhancing wall No Can have an enhancing wall Most have an enhancing wall
Ancillary findings Neck infection adjacent to the Primary infectious source such as otitis Primary infectious source such as otitis
retropharyngeal space or suppurative media or tonsillitis; retropharyngeal media or tonsillitis; presence of a
retropharyngeal node; internal jugular edema is a common associated foreign body in traumatic causes;
vein thrombosis; focal calcification finding complications in the airway,
anterior to C1–C2; other inflammatory mediastinum, or vessels
signs of radiotherapy
to altered lymphatic drainage or excess lymph the prevertebral space. As infection drains to CT of 4.4 cm3 [6]. Patients without purulence
production. There are multiple causes of retro the retropharyngeal node, the node enlarges at surgery were grouped with those who re
pharyngeal edema, including radiotherapy, in as the result of proliferation and invasion of sponded to medical therapy. This group had
ternal jugular vein (IJV) thrombosis (Fig. 2), inflammatory cells (i.e., reactive lymphade CT scans with a smaller mean volume in the
and retropharyngeal calcific tendinitis (Fig. 3). nopathy). Next, the node can become edem low-attenuation focus (2.2 cm3). The current
The latter is an inflammatory condition due to atous and this is referred to as the presup treatment for suppurative retropharyngeal
calcium hydroxyapatite deposition in the lon purative phase [6]. Finally, necrosis and pus nodes is a trial of IV antibiotics if the patient’s
gus colli tendons [3]. Rupture of crystal de formation occur to create a suppurative ret condition is stable [9, 10]. Surgical drain
posits provokes an inflammatory response and ropharyngeal node. Such infections are most age is considered if there is progression after
results in acute neck pain and retropharyn commonly seen in early childhood before the medical therapy or if the suppurative node is
geal space edema. Another common cause of retropharyngeal nodes atrophy. large at presentation.
retropharyngeal edema is infection in spaces Our four-step approach for evaluating suppu
surrounding the retropharyngeal space. In an rative retropharyngeal nodes is as follows: first, Retropharyngeal Abscess
adult, the prevertebral space is the most com with regard to fluid distribution, such nodes are Retropharyngeal abscess is most common
mon source of infection (Fig. 4), compared laterally located. Second, these nodes have a ly due to rupture of a suppurative retrophar
with the pharynx in children (Figs. 5 and 6). rounded or oval configuration, and the mass yngeal node into the retropharyngeal space
Our four-step approach for evaluating ret effect varies depending on the degree of nod (Fig. 7) and is contained only by the fascia
ropharyngeal edema is as follows: first, with al enlargement. Third, with regard to the wall, surrounding the retropharyngeal space. Oth
regard to fluid distribution, edema uniformly a thin hyperdense or enhancing rim may be er less common causes of a retropharyngeal
fills the retropharyngeal space from side to found around this low-density node [7, 8]; an abscess are spread of infection from contig
side. Second, edema has a smooth ovoid, rect edematous node in the presuppurative phase uous spaces across the fascial boundaries
angular, or “bow-tie” configuration on axial can also be low density. Fourth, ancillary or direct inoculation from penetrating trau
imaging and a diffuse craniocaudal distribu findings include evidence of the primary in ma (Fig. 8). Before infection evolves into a
tion on sagittal images, with tapered inferi fectious source, such as otitis media or tonsil walled abscess, it is known as retropharyn
or and superior margins; there is only mild litis. Retropharyngeal edema is a common as geal cellulitis or phlegmon. This condition
mass effect. Third, there is no wall thicken sociated finding. can be difficult to differentiate from retro
ing or enhancement. Fourth, ancillary find There is confusion in the literature about pharyngeal edema. The typical clinical pre
ings include IJV thrombosis, adjacent neck the terms “suppurative retropharyngeal node” sentation of retropharyngeal abscess is acute
infection, and focal calcification anterior to and “retropharyngeal abscess.” Suppurative to subacute onset of neck pain, dysphagia or
C1–C2 in the longus colli tendons [4, 5]. retropharyngeal node, or adenitis, is regard odynophagia, and a low-grade fever.
Retropharyngeal edema does not require ed as a more accurate description for infection Our four-step approach for evaluating ret
surgical drainage. Most cases resolve as the contained by the nodal capsule. The distinc ropharyngeal abscess is as follows: first, with
cause of edema is treated. tion from abscess is important because many regard to fluid distribution, a retropharyngeal
cases do not have purulent material at surgery abscess fills the retropharyngeal space from
Suppurative Retropharyngeal Node and can be successfully managed medically. side to side [7, 8]. Second, retropharyngeal
A suppurative retropharyngeal node is a re The sign of rim enhancement and a low-den abscesses have an oval or rounded configura
active lymph node that has undergone lique sity center is less than 57% specificity for pu tion; moderate-to-marked mass effect can pro
factive necrosis but is contained by the nodal rulent material at surgery [6]. Shefelbine et al. duce anterior displacement of the pharynx and
capsule (also known as retropharyngeal ad [6] found that the volume of the hypodense flattening of prevertebral muscles. Third, retro
enitis or intranodal abscess) (Figs. 5 and 6). focus is a better predictor of pus at surgery. pharyngeal abscess usually has a thick enhanc
The process begins as a bacterial infection in In that study, patients with purulence present ing wall. Fourth, ancillary findings include
the pharynx, paranasal sinuses, middle ear, or at surgery had a mean hypodense volume on evidence of primary infection or presence of a
AJR:196, April 2011 W427
Hoang et al.
foreign body in traumatic causes. In addition, differentiate between noninfectious and in pharynx. Neuroimaging Clin N Am 2003; 13:393–
the radiologist should search carefully for fectious causes. 410 [ix]
complications [10, 11]. 8. Hudgins PA. Nodal and nonnodal inflammatory
The mortality rate for retropharyngeal ab Acknowledgment processes of the pediatric neck. Neuroimaging
scess is less than 1% [12] and has declined in We thank Roxana Gafton for her editorial Clin N Am 2000; 10:181–192 [ix]
the last 50 years because of the availability of assistance in preparing the manuscript. 9. Craig FW, Schunk JE. Retropharyngeal abscess
antibiotics and early diagnosis with CT. The in children: clinical presentation, utility of imag
Downloaded from www.ajronline.org by 92.83.161.47 on 03/28/23 from IP address 92.83.161.47. Copyright ARRS. For personal use only; all rights reserved
most urgent complication is airway compres References ing, and current management. Pediatrics 2003;
sion from mass effect on the larynx and phar 1. Branstetter BF 4th, Weissman JL. Normal anatomy 111:1394–1398
ynx. Airway compromise is suggested in up to of the neck with CT and MR imaging correlation. 10. Johnston D, Schmidt R, Barth P. Parapharyngeal
3% of patients by the clinical symptom of stri Radiol Clin North Am 2000; 38:925–940 [ix] and retropharyngeal infections in children: argu
dor [12]. The other feared complications are 2. Davis WL, Harnsberger HR, Smoker WR, Wa ment for a trial of medical therapy and intraoral
rare and documented in the literature as case tanabe AS. Retropharyngeal space: evaluation of drainage for medical treatment failures. Int J Pe-
reports and case series. Infection can spread in normal anatomy and diseases with CT and MR diatr Otorhinolaryngol 2009; 73:761–765
feriorly via the danger space to the mediasti imaging. Radiology 1990; 174:59–64 11. Page NC, Bauer EM, Lieu JE. Clinical features
num, where it can result in mediastinitis, peri 3. Ring D, Vaccaro AR, Scuderi G, Pathria MN, and treatment of retropharyngeal abscess in chil
carditis, pleuritis, and empyema [13] (Fig. 9). Garfin SR. Acute calcific retropharyngeal tendi dren. Otolaryngol Head Neck Surg 2008; 138:
Infection can also break through the surround nitis: clinical presentation and pathological char 300–306
ing fascial planes and cause infection in the air acterization. J Bone Joint Surg Am 1994; 76:1636– 12. Coulthard M, Isaacs D. Retropharyngeal abscess.
way, spine, or carotid space. Vascular compli 1642 Arch Dis Child 1991; 66:1227–1230
cations of carotid space infection include IJV 4. Kanzaria H, Stein JC. A severe sore throat in a 13. Papalia E, Rena O, Oliaro A, et al. Descending
thrombosis, carotid artery rupture, and pseudo middle-aged man: calcific tendonitis of the longus necrotizing mediastinitis: surgical management.
aneurysm [14–16]. Finally, the infection itself colli tendon. J Emerg Med 2008 [epub ahead of Eur J Cardiothorac Surg 2001; 20:739–742
can evolve into necrotizing fasciitis and sepsis print] 14. Beningfield A, Nehus E, Chen AY, Yellin S.
[13]. Because these complications are associ 5. Eastwood JD, Hudgins PA, Malone D. Retrophar Pseudoaneurysm of the internal carotid artery af
ated with significant morbidity and mortality, yngeal effusion in acute calcific prevertebral ten ter retropharyngeal abscess. Otolaryngol Head
a true retropharyngeal abscess usually requires dinitis: diagnosis with CT and MR imaging. Neck Surg 2006; 134:338–339
prompt surgical drainage. AJNR 1998; 19:1789–1792 15. Hudgins PA, Dorey JH, Jacobs IN. Internal ca
6. Shefelbine SE, Mancuso AA, Gajewski BJ, Ojiri rotid artery narrowing in children with retro
Conclusion H, Stringer S, Sedwick JD. Pediatric retropharyn pharyngeal lymphadenitis and abscess. AJNR
The accurate diagnosis of retropharynge geal lymphadenitis: differentiation from retro 1998; 19:1841–1843
al collections will help triage patients for ap pharyngeal abscess and treatment implications. 16. Ide C, Bodart E, Remacle M, De Coene B, Nisolle
propriate management. A four-step imaging Otolaryngol Head Neck Surg 2007; 136:182–188 JF, Trigaux JP. An early MR observation of ca
assessment with multiplanar imaging will 7. Branstetter BF 4th, Weissman JL. Infection of the rotid involvement by retropharyngeal abscess.
help to recognize key imaging findings that facial area, oral cavity, oropharynx, and retro AJNR 1998; 19:499–501
A B C
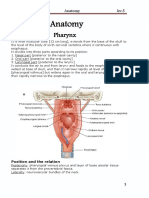
Fig. 1—Normal anatomy of retropharyngeal space.
A, Diagram of fascial layers of retropharyngeal space (double-headed arrow). True retropharyngeal space is between visceral fascia and alar fascia of deep layer of deep
cervical fascia. Danger space is between alar and prevertebral layers of deep cervical fascia. These two components cannot be distinguished on MRI and CT in healthy patient.
B and C, Axial enhanced CT (B) and T2-weighted MRI (C) images show normal thin fat-containing retropharyngeal space (arrowheads, B; single arrowhead, C). Anterior
visceral fascia surrounds pharynx and esophagus. Posterior prevertebral fascia invests longus colli and other prevertebral muscles. Carotid spaces form lateral walls
of retropharyngeal space and contain internal or common carotid artery (CCA) and internal jugular vein (IJV). Lymph nodes lie in true retropharyngeal space and are
subdivided into lateral and medial groups. Lateral lymph nodes are located lateral to longus colli and capitis muscles and extend from skull base to C3.
(Fig. 1 continues on next page)
W428 AJR:196, April 2011
Multiplanar Imaging of Retropharyngeal Space
Fig. 1 (continued)—Normal anatomy of
retropharyngeal space.
D and E, Sagittal enhanced CT (D) and T1-weighted
MRI (E) images show normal thin fat-containing
retropharyngeal space (arrowheads, D and E). Fascial
layers that form anterior and posterior walls attach
to clivus. Danger space of retropharyngeal space
extends from clivus to mediastinum.
Downloaded from www.ajronline.org by 92.83.161.47 on 03/28/23 from IP address 92.83.161.47. Copyright ARRS. For personal use only; all rights reserved
D E
A B
Fig. 2—32-year-old man with retropharyngeal edema
due to internal jugular vein (IJV) thrombophlebitis.
Infected catheter used for renal dialysis was
removed 3 weeks earlier. New subclavian catheter
was placed. One week later, patient presented with
fever and right neck tenderness.
A and B, Axial unenhanced CT images show
collection (arrowheads, A and B) filling from side to
side in retropharyngeal space, with mild mass effect.
This is consistent with retropharyngeal edema. There
is high-density thrombosis in right IJV (arrow, A and
B) and edema in surrounding carotid space.
C, Sagittal unenhanced reformatted CT image
shows fluid expanding in retropharyngeal space
(arrowheads).
D, Axial enhanced CT image performed 10 hours later
shows reduction in amount of retropharyngeal edema
(arrowheads). There is contrast-filling defect (arrow)
in thrombosed IJV.
C D
AJR:196, April 2011 W429
Hoang et al.
Downloaded from www.ajronline.org by 92.83.161.47 on 03/28/23 from IP address 92.83.161.47. Copyright ARRS. For personal use only; all rights reserved
A B C
Fig. 3—26-year-old man with retropharyngeal edema secondary to calcific tendinitis. He presented with 2-day history of neck pain, stiffness, and tenderness.
A and B, Axial unenhanced (A) and sagittal reformatted (B) CT images show diffuse low attenuation collection (arrowheads, A and B) in retropharyngeal space with mild
mass effect and tapered margins. These findings are in keeping with retropharyngeal edema.
C, Parasagittal reformatted CT image in bone windows shows focal calcification (arrow) in right longus colli tendon at C1–C2 level. (Courtesy of Everton KL, Durham, NC)
A B C
Fig. 4—47-year-old man with retropharyngeal edema due to cervical spine epidural abscess. Patient had history of IV heroin use and presented with 1-week history of
neck pain.
A, Axial fat-suppressed gradient-echo MRI scan shows fluid collection (arrowheads) filling retropharyngeal space from side to side with mild mass effect. There is also
hyperintensity in right longus colli muscle and other prevertebral muscles (curved arrow). CCA = common carotid artery, IJV = internal jugular vein, LC = longus collis.
B and C, T1-weighted (B) and T2-weighted (C) MRI scans show anterior epidural collection (arrow, B and C) extending from C2 to C4 vertebral levels. T1-weighted
image shows hyperintense stripe (arrowheads, B) in keeping with fat-containing true retropharyngeal space. Posterior to fat stripe is thin diffuse T1 isointense and T2
hyperintense signal collection (arrowhead, C) in danger space (asterisks, B and C) from C2 to mediastinum. These findings are consistent with retropharyngeal edema in
danger space secondary to prevertebral space infection.
W430 AJR:196, April 2011
Multiplanar Imaging of Retropharyngeal Space
Fig. 5—3-year-old boy with retropharyngeal
suppurative node and retropharyngeal edema. He
presented with fever and neck pain and 1-week
history of upper respiratory tract infection symptoms.
A, Axial enhanced CT scan at level of nasopharynx
shows unilateral collection in left retropharyngeal
space (arrow). There is mild mass effect and
thin high-density rim. This is consistent with
retropharyngeal suppurative node.
Downloaded from www.ajronline.org by 92.83.161.47 on 03/28/23 from IP address 92.83.161.47. Copyright ARRS. For personal use only; all rights reserved
B, Axial enhanced CT scan at level of oropharynx
shows fluid density bilaterally in retropharyngeal
space (arrowheads) with mild mass effect and no
rim enhancement. This is in keeping with reactive
retropharyngeal edema.
C and D, Coronal (C) and sagittal (D) reformatted
CT images show oval-shaped left retropharyngeal
suppurative node (arrow, C) and retropharyngeal
edema (arrowheads, C and D). Patient improved with
IV antibiotics and did not require surgical drainage.
CCA = common carotid artery, ICA = internal carotid
A B artery, LC = longus collis.
C D
A B C
Fig. 6—10-year-old boy with retropharyngeal suppurative node and retropharyngeal edema. He presented with 1-day history of fever after 3 days of odynophagia and left
neck pain and stiffness.
A and B, Axial enhanced (A) and coronal reformatted (B) CT images show rounded unilateral collection in left retropharyngeal space (straight arrow, A and B). There
is mild mass effect and thin high-density rim. This is consistent with retropharyngeal suppurative node. There is also enlarged right retropharyngeal node without low
density (curved arrow, A and B) in keeping with reactive lymphadenopathy.
C, Axial enhanced CT image at higher level in oropharynx shows collection (arrowheads) filling retropharyngeal space from side to side with mild mass effect and no rim
enhancement. This is in keeping with reactive retropharyngeal edema. Intraoperative examination found patient to have firm palpable mass behind tonsil pillars. From
transoral approach, only tiny amount of pus was expressed. He improved with IV antibiotic therapy and was discharged on oral antibiotics.
AJR:196, April 2011 W431
Hoang et al.
Fig. 7—1-year-old girl with retropharyngeal abscess.
She presented with fever and 1-week history of
worsening stridor. This was preceded by otitis media
treated with oral antibiotics.
A and B, Axial (A) and sagittal reformatted (B)
enhanced CT images show large collection
(arrowheads, A and B) filling both sides of
retropharyngeal space. Collection has marked mass
effect with obliteration of airway (asterisk, A). There
Downloaded from www.ajronline.org by 92.83.161.47 on 03/28/23 from IP address 92.83.161.47. Copyright ARRS. For personal use only; all rights reserved
are enhancing septations and thick enhancing wall.
Endotracheal tube (arrow, A) was required before
CT scan.
A B
Fig. 8—3-year-old girl with retropharyngeal cellulitis
due to penetrating injury to oropharynx, which
resulted from fall while running with stick in her
mouth. She presented 5 days later with fever and
odynophagia.
A and B, Axial (A) and sagittal reformatted (B)
enhanced CT images show large mucosal defect
(arrow, A and B) in posterior oropharyngeal wall and
gas (asterisks, A and B) and fluid (arrowheads, A and
B) in retropharyngeal space. There is mild diffuse
expansion of retropharyngeal space but no wall
thickening or enhancement. On surgical exploration,
breech in mucosa was noted in posterior pharyngeal
wall. There was no purulent material or fluctuant
mass. Patient improved with 2-day course of IV
antibiotics and was discharged with oral antibiotics.
A B
Fig. 9—37-year-old man with retropharyngeal
abscess and necrotizing fasciitis in neck complicated
by descending mediastinitis.
A, Axial enhanced CT image of neck at level of hyoid
shows collection (arrowheads) filling retropharyngeal
space from side to side. There is only mild mass
effect, but thin wall enhancement is present. Edema
is also noted in pharyngeal mucosal space (asterisk),
parapharyngeal space, and submandibular space
(arrows).
B, Axial enhanced CT image of upper thorax
shows fluid collection (arrowheads) in posterior
mediastinum tracking into right middle mediastinum.
In comparison, there is normal low density fat in
anterior mediastinum (curved arrow). Patient also had
reactive bilateral pleural effusions.
A B
W432 AJR:196, April 2011
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5822)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (898)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (403)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Brainstem MnemonicsDocument2 pagesBrainstem MnemonicsFajar Rudy Qimindra100% (4)
- Notiuni UtileDocument1 pageNotiuni Utilepunct_org3256No ratings yet
- Safety Guidelines For Magnetic Resonance Imaging Equipment in Clinical UseDocument86 pagesSafety Guidelines For Magnetic Resonance Imaging Equipment in Clinical Usepunct_org3256No ratings yet
- Supine Breast MRIDocument6 pagesSupine Breast MRIpunct_org3256No ratings yet
- Spine Imaging A Case Based Guide To ImagingDocument377 pagesSpine Imaging A Case Based Guide To Imagingpunct_org3256100% (1)
- Anatomy of The PharynxDocument11 pagesAnatomy of The Pharynxpunct_org3256No ratings yet
- Dental Disease and RadiologyDocument11 pagesDental Disease and Radiologypunct_org3256No ratings yet
- Recurrence in The Thyroidectomy Bed Sonographic FindingsDocument7 pagesRecurrence in The Thyroidectomy Bed Sonographic Findingspunct_org3256No ratings yet
- Nasal and Paranasal Sinus PathologiesDocument7 pagesNasal and Paranasal Sinus Pathologiespunct_org3256No ratings yet
- Differential Diagnosis Fungal Sinusitis and Odontogenic SinuitisDocument8 pagesDifferential Diagnosis Fungal Sinusitis and Odontogenic Sinuitispunct_org3256No ratings yet
- Fracture HealingDocument6 pagesFracture Healingpunct_org3256No ratings yet
- Chronic Pancreatitis or Pancreatic TumorDocument18 pagesChronic Pancreatitis or Pancreatic Tumorpunct_org3256No ratings yet
- Changes Lungs Plain Radiograph: Vascular The The of The ChestDocument8 pagesChanges Lungs Plain Radiograph: Vascular The The of The Chestpunct_org3256No ratings yet
- Hip Prostethis ComplicationDocument11 pagesHip Prostethis Complicationpunct_org3256No ratings yet
- Oblique MR Imaging of The Anterior Cruciate LigamentDocument5 pagesOblique MR Imaging of The Anterior Cruciate Ligamentpunct_org3256No ratings yet
- Oncrete Design: Péter Leczovics, Erzsébet DomonyiDocument12 pagesOncrete Design: Péter Leczovics, Erzsébet Domonyipunct_org3256No ratings yet
- Abdominal Ultrasound - LiverDocument30 pagesAbdominal Ultrasound - Liverpunct_org3256No ratings yet
- ESR European Training Curriculum Level I-II (2020)Document154 pagesESR European Training Curriculum Level I-II (2020)punct_org3256No ratings yet
- Kuo2017 Article DiagnosisOfBronchiectasisAndAiDocument10 pagesKuo2017 Article DiagnosisOfBronchiectasisAndAipunct_org3256No ratings yet
- Anatomy of Orofacial Structures: For C-II Medical StudentsDocument76 pagesAnatomy of Orofacial Structures: For C-II Medical Studentssamuel mekuriawNo ratings yet
- Thyroid Function Tests: What Is The Thyroid Gland?Document2 pagesThyroid Function Tests: What Is The Thyroid Gland?rastamaneazy269No ratings yet
- Lec.11 Parotid RegionDocument7 pagesLec.11 Parotid RegionothmanNo ratings yet
- Labs24 26SpecialSensesDocument2 pagesLabs24 26SpecialSensesMatt Joseph CabantingNo ratings yet
- Methods of Space GainingDocument34 pagesMethods of Space GainingSasikumar Rasappan0% (1)
- Mcqs 1Document4 pagesMcqs 1Dood100% (1)
- Orthodontics 2: Research Activity Part 3 of 3Document22 pagesOrthodontics 2: Research Activity Part 3 of 3Gem Hanna Callano ParaguaNo ratings yet
- Anatomy of NeckDocument100 pagesAnatomy of NeckdiptidigheNo ratings yet
- Islcollective Worksheets Beginner Prea1 Elementary A1 Students With Special Educational Needs Learning Difficulties Eg 13058306758a823927b7371 03862355Document2 pagesIslcollective Worksheets Beginner Prea1 Elementary A1 Students With Special Educational Needs Learning Difficulties Eg 13058306758a823927b7371 03862355sandronecaNo ratings yet
- The Hypoglossal Nerve CN XII Course Motor TeachMeAnatomyDocument3 pagesThe Hypoglossal Nerve CN XII Course Motor TeachMeAnatomyMohammad HadiNo ratings yet
- Functional and Aesthetic Full Mouth Rehabilitation of A Severely Worn Dentition To Restore Vertical Dimension: A Case ReportDocument5 pagesFunctional and Aesthetic Full Mouth Rehabilitation of A Severely Worn Dentition To Restore Vertical Dimension: A Case ReportSyrk12No ratings yet
- Keyword Ideas On Hair Loss For SEODocument18 pagesKeyword Ideas On Hair Loss For SEOChitrakarudu KalabhimaniNo ratings yet
- Normal Values in OphthalmologyDocument4 pagesNormal Values in OphthalmologyRameshNo ratings yet
- FCPS NOV Paper 2 Oph 2012Document13 pagesFCPS NOV Paper 2 Oph 2012bahaashakirNo ratings yet
- Submental Island FlapDocument20 pagesSubmental Island FlapdrshariquennazirNo ratings yet
- 02-Three-Visit CD PDFDocument20 pages02-Three-Visit CD PDFBernythefly axcNo ratings yet
- Regional Flaps in Head and Neck ReconstructionDocument11 pagesRegional Flaps in Head and Neck ReconstructionBenedetta GuarinoNo ratings yet
- Unit 1 Physical Description and ComparisonDocument7 pagesUnit 1 Physical Description and ComparisonMaría Cecilia CarattoliNo ratings yet
- Case Study TrichoDocument6 pagesCase Study TrichoVisanth KumarNo ratings yet
- Surgically Assisted Rapid Maxillary Expansion (SARME) : A Review of The LiteratureDocument6 pagesSurgically Assisted Rapid Maxillary Expansion (SARME) : A Review of The LiteratureMaria SilvaNo ratings yet
- Articulo 7Document10 pagesArticulo 7Javier CastilloNo ratings yet
- The Facial NerveDocument6 pagesThe Facial NerveRahul Raj SNo ratings yet
- Updated List of Dental Clinics As of September 2021Document4 pagesUpdated List of Dental Clinics As of September 2021Paolo Joshua Abratique0% (1)
- Spear 2008Document9 pagesSpear 2008IlseNo ratings yet
- Wella-Lista de Precios Octubre 2023 SQDocument4 pagesWella-Lista de Precios Octubre 2023 SQGEKO MobiliariosNo ratings yet
- Atlas of Complex Orthodontics PDFDocument564 pagesAtlas of Complex Orthodontics PDFKENAN ABBARANo ratings yet
- BrainstemDocument36 pagesBrainstemSowmya SUmMyNo ratings yet
- What Is An Ear InfectionDocument3 pagesWhat Is An Ear InfectionGladie Ann Dela RosaNo ratings yet
- Anatomy Quiz 7Document7 pagesAnatomy Quiz 7Michael MerlinNo ratings yet