Professional Documents
Culture Documents
AACPDM Dystonia CP
AACPDM Dystonia CP
Uploaded by
Karen AngOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
AACPDM Dystonia CP
AACPDM Dystonia CP
Uploaded by
Karen AngCopyright:
Available Formats
CARE PATHWAYS
DYSTONIA
Bottom Line ‘Evidence-Informed’ Recommendations for the Management
of Dystonia in Individuals with Cerebral Palsy
Authors (AACPDM Dystonia Care Pathway Team): D Fehlings (team lead),
L Brown, A Harvey, K Himmelmann, JP Lin, A MacIntosh, J Mink, E Monbaliu, J Rice, J Silver, L Switzer, I Walter.
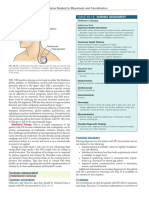
DEFINITIONS tion, determine if the dystonia is generalized or focal and
Dystonia is a movement disorder in which involuntary sus- assess the severity (can use a standardized scale such
tained or intermittent muscle contractions cause twisting as the Barry Albright Dystonia Scale outlined in Section
and repetitive movements, abnormal postures, or both. 3). Assess the impact of the dystonia on function, pain/
Dystonia in cerebral palsy (CP) presents as hypertonia, in- comfort (including sleep), and care-giving and whether
voluntary postures and movements, or a combination. Dys- management is required.
tonia occurs in dyskinetic CP but also is commonly presentIf dystonia is present, assess whether the neurologic
in spastic CP. presentation is consistent with CP (risk factors, brain
WHY IS DYSTONIA IN CEREBRAL PALSY imaging, and family history) or if additional work-up is
required. An important masquerader of CP-related
IMPORTANT? dystonia is Dopamine Responsive Dystonia. Consider the
• Dystonia can impede motor function through involuntary need for a trial of levodopa and/or a referral to a neu-
muscle contractions, limitations in muscle relaxation, rologist/geneticist for additional diagnostic work-up.
and overflow, which is the association of involuntary
movement with intended movement which spreads to MANAGEMENT
surrounding or distant muscles It is important to note that much of this Dystonia Care
• Dystonia can interfere with positioning for sitting Pathway is based on expert opinion, as the evidence for
and lying dystonia management in CP is currently limited.
• Dystonic postures and movement can be painful • Rehabilitation Strategies: Rehabilitation strategies used
by physiotherapists, occupational therapists and speech
• Dystonia can interfere with sleep pathologists are generally considered cornerstones in
• Dystonia can result in high energy expenditure and mal- the management of dystonia in CP. General principles
nutrition include: 1) ensuring therapy is goal-directed, 2) avoiding
asymmetry and aiming for symmetrical positioning to en-
• Dystonic postures/hypertonia can create challenges
hance motor control, 3) optimizing seating and position-
with care-giving
ing with good stability/support, 4) considering orthoses
Target Population: Individuals with dystonia in CP where and splints to increase stability and coordination, and 5)
the dystonia interferes with function, positioning or causes considering the need for communication supports.
pain and disrupted sleep.
• Generalized Dystonia Management: With increasing
Target Clinical Providers: Physicians/Nurses/Therapists severity of dystonia, additional interventions may be
caring for individuals with dystonia in CP. required beginning with oral medications. Oral baclofen
is considered a first line medication for the management
ASSESSMENT of dystonia in CP. Common indications include pain or
ACPDM-0218-424
Dystonia is a frequently overlooked element of the neuro-
difficulty sleeping associated with dystonia in CP. If the
logical presentation of CP. Therefore, it is recommended
individual does not respond well to oral baclofen, trihexy-
that a ‘dystonia’ assessment be routinely included in
phenidyl can be used as a second line medication. Other
your neurological examination (assessing for fluctuating
oral medications should be considered for specific indi-
hypertonia, and using tactile stimulation or voluntary
cations. For example, the intermittent use of benzo-
movement to trigger dystonia). More informa-
diazepines is helpful for dystonic storms or
tion can be found in Section 3 of this
disturbed sleep, and gabapentin for
pathway in the HAT tool link.
dystonia associated with
On your examina-
pain.
© September 2016, AACPDM Care Pathways, for review 2019
CARE PATHWAYS
DYSTONIA
Bottom Line ‘Evidence-Informed’ Recommendations for the Management
of Dystonia in Individuals with Cerebral Palsy
Authors (AACPDM Dystonia Care Pathway Team): D Fehlings (team lead),
L Brown, A Harvey, K Himmelmann, JP Lin, A MacIntosh, J Mink, E Monbaliu, J Rice, J Silver, L Switzer, I Walter.
Clonidine can also be considered for disturbed sleep as- • Focal Dystonia Management: For individuals with focal
sociated with dystonia. or segmental dystonia associated with persisting pos-
In the presence of severe generalized dystonia associated tures causing pain or impacting on function/care-giving,
with significant impact on care/comfort, more aggres- periodic injections of Botulinum toxin can be undertaken.
sive management can be undertaken. This may include Consider targeting both the agonist/antagonist muscles
intrathecal baclofen (ITB) or deep brain stimulation around the joint(s) involved with the dystonic posture.
(DBS). These strategies require a referral to a special-
ist team. Individuals with severe generalized hypertonia
with a combination of dystonia and spasticity may trial
intrathecal baclofen. Other considerations of whether to
choose ITB or DBS can be based on the cerebral anatomy
and whether placement of the stimulator in the globus
pallidus is possible. ITB should be used with caution in
the presence of nocturnal respiratory compromise.
A classic feature of dystonia in CP is a fluctuation in the
severity of the dystonia. For this reason it is important to
periodically re-evaluate the individual and adjust the in-
terventions as required. For some individuals with severe
dystonia, a personalized plan for managing increasing
dystonia can be developed and includes increasing the
dose of current oral medications or introducing a second
medication (e.g. clonidine or gabapentin). The use of the
Dystonia Severity Action Plan (DSAP) may be helpful for
monitoring unstable dystonia and is outlined in Section 3.
A rapid and severe increase in dystonia is termed ‘Peri-
odic Status Dystonicus’. It can be life-threatening and
requires urgent treatment often with a combination of
benzodiazepines and clonidine (enteral, intravenous, or
transdermal) (see Section 3 for a management protocol
for ‘Status Dystonicus’). Another important issue is the
triggering of dystonia from secondary health conditions
including gastrointestinal disorders such as reflux or
constipation. The overall general health of the individual
ACPDM-0218-424
should be carefully monitored and secondary health is-
sues actively addressed.
© September 2016, AACPDM Care Pathways, for review 2019
CARE PATHWAYS
ACPDM-0218-424
The purpose of this document is to provide health care professionals with key facts and recommendations for the assessment and treatment of dystonia in children
and youth with cerebral palsy. This summary was produced by the AACPDM Dystonia Care Pathway Team (D Fehlings (team lead), L Brown, A Harvey, K Himmelmann,
JP Lin, A MacIntosh, J Mink, E Monbaliu, J Rice, J Silver, L Switzer, I Walters). The summary is based on a systematic review being submitted for peer-
reviewed publication. However, health care professionals should continue to use their own judgement and take into account additional
relevant factors and context. The AACPDM is not liable for any damages, claims, liabilities, or costs arising from the use of
these recommendations including loss or damages arising from any claims made by a third party.
© September 2016, AACPDM Care Pathways, for review 2019
You might also like
- Psychiatric Nursing Ebook 8th Edition Ebook PDFDocument61 pagesPsychiatric Nursing Ebook 8th Edition Ebook PDFcarey.sowder235100% (46)
- 4 - 5774129521364043804-Compressed (1) - Compressed PDFDocument809 pages4 - 5774129521364043804-Compressed (1) - Compressed PDFMichelle100% (9)
- Drug Information - A Guide For Pharmacists (PDFDrive)Document907 pagesDrug Information - A Guide For Pharmacists (PDFDrive)Nikitha Gunnala100% (3)
- Treatment of Childhood DystoniaDocument8 pagesTreatment of Childhood DystonialhnguNo ratings yet
- Develop Med Child Neuro - 2013 - Allen - Status Dystonicus A Practice GuideDocument8 pagesDevelop Med Child Neuro - 2013 - Allen - Status Dystonicus A Practice Guidef.cohenneurologiaNo ratings yet
- Jankovic 2013Document12 pagesJankovic 2013Roberta Lessa RibeiroNo ratings yet
- Nihms 1901086Document52 pagesNihms 1901086cfernandfuNo ratings yet
- BMJ 2020 062659.fullDocument6 pagesBMJ 2020 062659.fullSrhappy FaceNo ratings yet
- Therapeutic Interventions in Vertigo ManagementDocument9 pagesTherapeutic Interventions in Vertigo ManagementtamiNo ratings yet
- DistoniasDocument14 pagesDistoniasFrancisco GonzalezNo ratings yet
- Distonia CervicalDocument12 pagesDistonia CervicalcarolinafspintoNo ratings yet
- Cuando Hay Dificultad para Tragar. El Rol Del LogopedaDocument4 pagesCuando Hay Dificultad para Tragar. El Rol Del LogopedaPaula San José CascónNo ratings yet
- ScienceDocument3 pagesScienceAmal DavisNo ratings yet
- Delirium Pathway - OTLPCM002-3Document1 pageDelirium Pathway - OTLPCM002-3Iftida YatiNo ratings yet
- Therapeutic Interventions in Vertigo Management: Review ArticleDocument12 pagesTherapeutic Interventions in Vertigo Management: Review ArticleAdityaNo ratings yet
- Pysche OSCE - EPSE ExaminationDocument1 pagePysche OSCE - EPSE ExaminationAmber WangNo ratings yet
- Pharmacologic Treatment of Vestibular Disorders: Surgical Treatments - in Less FrequentDocument8 pagesPharmacologic Treatment of Vestibular Disorders: Surgical Treatments - in Less FrequentRay MaudyNo ratings yet
- Piis2212440318300592 PDFDocument3 pagesPiis2212440318300592 PDFUmer HussainNo ratings yet
- MNT StrokeDocument29 pagesMNT Strokemangalik100% (1)
- Dystonia ChapterDocument33 pagesDystonia Chapteraria tristayanthiNo ratings yet
- Management of Hoarseness-JUL 2018Document2 pagesManagement of Hoarseness-JUL 2018wiwiNo ratings yet
- Extra Pyramidal Side EffectsDocument27 pagesExtra Pyramidal Side EffectsChisco OKabsNo ratings yet
- Ad, TD, Akathisia 120454Document20 pagesAd, TD, Akathisia 120454watch itNo ratings yet
- Assessment of Infantile DystoniaDocument75 pagesAssessment of Infantile Dystoniaahmed12mohamed12hNo ratings yet
- Parkinsons DiseaseDocument2 pagesParkinsons Diseaseapi-621761287No ratings yet
- Pediatrictone Management: Sathya Vadivelu,, Anne Stratton,, Wendy PierceDocument10 pagesPediatrictone Management: Sathya Vadivelu,, Anne Stratton,, Wendy PierceDeborah SalinasNo ratings yet
- Kinesiotape en DisfoniaDocument5 pagesKinesiotape en DisfoniaingridspulerNo ratings yet
- JNNP 2013 305532Document12 pagesJNNP 2013 305532Yanina Pérez de VillarrealNo ratings yet
- NIH Public Access: Treatment Strategies For DystoniaDocument21 pagesNIH Public Access: Treatment Strategies For DystoniaRoro Khairiyah AmaliaNo ratings yet
- Endocrine DisorderDocument5 pagesEndocrine DisorderMenly SusadaNo ratings yet
- Pe 2 3 36Document6 pagesPe 2 3 36Oslo SaputraNo ratings yet
- V. Mark Durand, David H. Barlow, Stefan G. Hofmann - Essentials of Abnormal PsycDocument13 pagesV. Mark Durand, David H. Barlow, Stefan G. Hofmann - Essentials of Abnormal Psyca.utiashviliNo ratings yet
- 03 2010 Bare Essentials - Hyperkinetic Movement DisordersDocument10 pages03 2010 Bare Essentials - Hyperkinetic Movement DisordersadsfdhNo ratings yet
- Pelosin 2013Document10 pagesPelosin 2013QuocNo ratings yet
- Pharmacological ManagementDocument14 pagesPharmacological ManagementMiran Miran Hussien Ahmed Hassan El MaghrabiNo ratings yet
- Pain Agitation and Delirium (PAD) UHL Critical Care GuidelineDocument35 pagesPain Agitation and Delirium (PAD) UHL Critical Care GuidelineLollapallooza 23No ratings yet
- Murphy Et Al 2012 IPT EDDocument9 pagesMurphy Et Al 2012 IPT EDCésar BlancoNo ratings yet
- 245 FTPDocument2 pages245 FTPEdwin Mmaitsi KodiaNo ratings yet
- Patho NotesDocument4 pagesPatho Notesapi-676469437No ratings yet
- Insomnia in Older AdultsDocument2 pagesInsomnia in Older AdultssavitageraNo ratings yet
- MEDICAL SURGICAL NURSING ASSESSMENT AND MANAGEMENT OF CLINICAL PROBLEMS 9th EditionDocument1 pageMEDICAL SURGICAL NURSING ASSESSMENT AND MANAGEMENT OF CLINICAL PROBLEMS 9th EditionMeryPinkihanNo ratings yet
- MEDICAL SURGICAL NURSING ASSESSMENT AND MANAGEMENT OF CLINICAL PROBLEMS 9th EditionDocument1 pageMEDICAL SURGICAL NURSING ASSESSMENT AND MANAGEMENT OF CLINICAL PROBLEMS 9th EditionMeryPinkihanNo ratings yet
- 2010 Bare Essentials - Hyperkinetic Movement DisordersDocument10 pages2010 Bare Essentials - Hyperkinetic Movement DisordersValentina RomeroNo ratings yet
- Conscious Sedation PaediatricsDocument44 pagesConscious Sedation PaediatricsReeta TaxakNo ratings yet
- Emergencies in Palliative CareDocument3 pagesEmergencies in Palliative CareJorge Cortina GonzalesNo ratings yet
- ABCDEF Bundle WebcastDocument42 pagesABCDEF Bundle WebcastsoulstakersNo ratings yet
- Parkinson19 PDFDocument6 pagesParkinson19 PDFLorenaNo ratings yet
- AJGP 12 2019 Focus Patel Palliative Sedation WEB PDFDocument8 pagesAJGP 12 2019 Focus Patel Palliative Sedation WEB PDFFrancisco Rodriguez de NarvaezNo ratings yet
- 6 Various Treatment Modalities in TMJ Disorders (Autosaved)Document52 pages6 Various Treatment Modalities in TMJ Disorders (Autosaved)Supriya ShuklaNo ratings yet
- Drug-Induced Sleep Endoscopy (DISE)Document4 pagesDrug-Induced Sleep Endoscopy (DISE)Luis De jesus SolanoNo ratings yet
- Movement Disorders Overview and Treatment OptionsDocument15 pagesMovement Disorders Overview and Treatment OptionsDitaris Galih ImanNo ratings yet
- Trastornos Del Movimiento Articulo 2Document7 pagesTrastornos Del Movimiento Articulo 2cfernandfuNo ratings yet
- Congential 3 Musculoskeletal 3 Neurological 3 Abusive DisordersDocument7 pagesCongential 3 Musculoskeletal 3 Neurological 3 Abusive DisordersNichole CollinsNo ratings yet
- 10 Consejos en La SedacionDocument3 pages10 Consejos en La SedacionAntonio AlonsoNo ratings yet
- A Video Atlas of Levodopa Induced DyskinesiaDocument9 pagesA Video Atlas of Levodopa Induced DyskinesiaserhatNo ratings yet
- Thoracic Outlet SyndromeDocument6 pagesThoracic Outlet SyndromeCharles MitchellNo ratings yet
- Tos Part 2 B Jam 2017Document6 pagesTos Part 2 B Jam 2017Charles MitchellNo ratings yet
- Activity#2: Assessment Diagnosis Planning Intervention Rationale Evaluation IndependentDocument4 pagesActivity#2: Assessment Diagnosis Planning Intervention Rationale Evaluation IndependentCLOYD JHON OBISPONo ratings yet
- Protocol 010Document12 pagesProtocol 010hatem newishyNo ratings yet
- Care Management of The Agitation or Aggressiveness Crisis in Patients With TBI. Systematic Review of The Literature and Practice RecommendationsDocument10 pagesCare Management of The Agitation or Aggressiveness Crisis in Patients With TBI. Systematic Review of The Literature and Practice RecommendationsNers EducationNo ratings yet
- Jall Jsot Dap PresentationDocument13 pagesJall Jsot Dap Presentationapi-383172592No ratings yet
- Psy PRBLM 2 EsrdDocument5 pagesPsy PRBLM 2 EsrdNoreen ChoudhriNo ratings yet
- A Simple Guide to Parkinson's Disease and Related Brain ConditionsFrom EverandA Simple Guide to Parkinson's Disease and Related Brain ConditionsNo ratings yet
- Hepatorenal Syndrome Pathophysiology, Diag-Nosis, and ManagementDocument15 pagesHepatorenal Syndrome Pathophysiology, Diag-Nosis, and Managementwinny kartikaNo ratings yet
- Emergency MedicineDocument6 pagesEmergency MedicineChaht RojborwonwitayaNo ratings yet
- Diagnostic Services:-2D Echo, Audiometry, Bronchoscopy, CTDocument196 pagesDiagnostic Services:-2D Echo, Audiometry, Bronchoscopy, CTLalita NaiduNo ratings yet
- 1 - MCQs Classified اسئله د محمد امامDocument68 pages1 - MCQs Classified اسئله د محمد امامAhmed GaberNo ratings yet
- Benzathine Penicillin, Metronidazole and Benzyl PenicillinDocument5 pagesBenzathine Penicillin, Metronidazole and Benzyl PenicillinJorge Eduardo Espinoza RíosNo ratings yet
- Norepinephrine FinalDocument2 pagesNorepinephrine FinalNelly CruzNo ratings yet
- Care PlanDocument11 pagesCare PlanCathy GewontNo ratings yet
- DR Narendra Kumar Assistant ProfessorDocument16 pagesDR Narendra Kumar Assistant ProfessorAbdiweli AbubakarNo ratings yet
- AROMADocument2 pagesAROMAGlen LozadaNo ratings yet
- Neet AnaesthesiaDocument233 pagesNeet AnaesthesiaASHISHNo ratings yet
- Overview of MicroemulsionDocument13 pagesOverview of MicroemulsionEditor IJTSRDNo ratings yet
- Ebook Techniques in Ophthalmic Plastic Surgery A Personal Tutorial PDF Full Chapter PDFDocument67 pagesEbook Techniques in Ophthalmic Plastic Surgery A Personal Tutorial PDF Full Chapter PDFdonald.lozada63697% (39)
- FAR 381 Adrenocorticosteroids: Shamiso MlamboDocument22 pagesFAR 381 Adrenocorticosteroids: Shamiso MlamboHuzaifa KhanNo ratings yet
- Challenges in Formulation Development of Fast Dissolving Oral FilmsDocument18 pagesChallenges in Formulation Development of Fast Dissolving Oral FilmsKhoa DuyNo ratings yet
- Sabira Sultana REVIEWapjcpDocument11 pagesSabira Sultana REVIEWapjcpDiana RomeroNo ratings yet
- Post-Operative Complications: Hadi Munib Oral and Maxillofacial SurgeryDocument61 pagesPost-Operative Complications: Hadi Munib Oral and Maxillofacial SurgeryAli ahmedNo ratings yet
- Modular Exam: Chemical ReactionsDocument36 pagesModular Exam: Chemical ReactionsMarian Isabel YuNo ratings yet
- Marijuana Is A WellDocument4 pagesMarijuana Is A WellFermin Perez Fidel III100% (1)
- Endodontics Pain Control in Endodontics: Differential Diagnosis of Dental PainDocument4 pagesEndodontics Pain Control in Endodontics: Differential Diagnosis of Dental Painريام الموسويNo ratings yet
- CardiovascularDocument5 pagesCardiovascularVipinNo ratings yet
- Dosage Handouts 2020 2021Document16 pagesDosage Handouts 2020 2021chrystan maconNo ratings yet
- Medicinal Plants Used in The Treatment of Malaria, A Key Emphasis To Artemisia, Cinchona, Cryptolepis, and Tabebuia GeneraDocument14 pagesMedicinal Plants Used in The Treatment of Malaria, A Key Emphasis To Artemisia, Cinchona, Cryptolepis, and Tabebuia GeneraJ Elver SilvaNo ratings yet
- WEEK 3 Module-Psychopathology, Etiology and Psychodynamic of Schizophrenia, Mood and Anxiety DisordersDocument31 pagesWEEK 3 Module-Psychopathology, Etiology and Psychodynamic of Schizophrenia, Mood and Anxiety Disordersbartidoerikarose422No ratings yet
- Healthcare and Pharmacy AfriaDocument6 pagesHealthcare and Pharmacy AfriaAngela DelarmenteNo ratings yet
- 2c-MOLECULAR ASPECTS OF DRUG ACTIONDocument66 pages2c-MOLECULAR ASPECTS OF DRUG ACTIONAlly AbdalahNo ratings yet
- EMA Epar Public Assessment ReportDocument37 pagesEMA Epar Public Assessment ReportOscar Javier EstupiñánNo ratings yet
- Communication With Other Healthcare ProfessionalsDocument16 pagesCommunication With Other Healthcare ProfessionalsSittie Fahieda Aloyodan100% (1)