Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
39 viewsEndocrine System
Endocrine System
Uploaded by
Roeisa SalinasThe document discusses the anatomy and functions of various endocrine glands. It describes the pituitary gland as having two lobes - the anterior pituitary gland which produces several hormones including growth hormone and prolactin, and the posterior pituitary gland which stores hormones produced in the hypothalamus. The thyroid gland produces thyroid hormones that regulate metabolism. The parathyroid glands regulate calcium levels through parathyroid hormone. Other glands discussed include the adrenal glands, pancreas, gonads, thymus, and pineal gland.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You might also like
- Lesson Plan Diabetes MellitusDocument6 pagesLesson Plan Diabetes MellitusClaire100% (4)
- Endocrine SystemDocument20 pagesEndocrine SystemSheena Pasion100% (2)
- A Simple Guide to The Pineal Gland (The Third Eye) And Its FunctionFrom EverandA Simple Guide to The Pineal Gland (The Third Eye) And Its FunctionRating: 5 out of 5 stars5/5 (1)
- Endocrine ReviewDocument9 pagesEndocrine ReviewSpencer ThomasNo ratings yet
- Somatic Nervous SystemDocument4 pagesSomatic Nervous SystemGuenNo ratings yet
- Anaphy LecDocument5 pagesAnaphy Lecmelbertconag1973No ratings yet
- AnaPhy Lec - Endocrine SystemDocument2 pagesAnaPhy Lec - Endocrine SystemReigh DakotaNo ratings yet
- 22 Chemical Co-OrdinationDocument47 pages22 Chemical Co-OrdinationRachna JaiswalNo ratings yet
- Script For Midterm VRDocument5 pagesScript For Midterm VRDanica MerinNo ratings yet
- Endocrine System Animal ScienceDocument15 pagesEndocrine System Animal ScienceJairus LampanoNo ratings yet
- Chemical Co Ordination and Integration - 434dea34 f494 4704 A8c9 6876397e324eDocument53 pagesChemical Co Ordination and Integration - 434dea34 f494 4704 A8c9 6876397e324epcgurukotari9No ratings yet
- Genbio2 ReviewerDocument4 pagesGenbio2 ReviewerLovely QuezonNo ratings yet
- Quick Study Guide To The Endocrine SystemDocument11 pagesQuick Study Guide To The Endocrine SystemMc Luis Glen AserdanoNo ratings yet
- Endocrine Glands - 1st - ChapterDocument12 pagesEndocrine Glands - 1st - Chaptervarun kumarNo ratings yet
- Endocrine System NotesDocument8 pagesEndocrine System NotesShiela Mae SagayoNo ratings yet
- Endokrinologi Reproduksi: Bayu Kurniawan, DRDocument48 pagesEndokrinologi Reproduksi: Bayu Kurniawan, DRdocbay100% (1)
- Animal Hormones PDFDocument11 pagesAnimal Hormones PDFAin HusnaNo ratings yet
- ANATOMY Endocrine TranscribedDocument9 pagesANATOMY Endocrine TranscribedYanyan PanesNo ratings yet
- EndocrineDocument49 pagesEndocrineHerbert DelacruzNo ratings yet
- Endocrine System (Zoology)Document3 pagesEndocrine System (Zoology)Cheska de GuzmanNo ratings yet
- Endocrine SystemDocument43 pagesEndocrine SystemnandaNo ratings yet
- Endocrine System PTT FinalDocument56 pagesEndocrine System PTT FinalVenice GalleneroNo ratings yet
- Chemical Coordination and IntegrationDocument3 pagesChemical Coordination and Integrationakhil01ajNo ratings yet
- Reproduction & Endocrinology 1: Hypothalamus and PituitaryDocument41 pagesReproduction & Endocrinology 1: Hypothalamus and PituitaryabdulNo ratings yet
- The Nervous and The Endocrine SystemsDocument9 pagesThe Nervous and The Endocrine SystemsluciaarecesdiazNo ratings yet
- Endocrine Glands and Their FunctionsDocument31 pagesEndocrine Glands and Their FunctionsAfrina Asmi MINo ratings yet
- Endocrine SystemDocument7 pagesEndocrine SystemClyde CapapasNo ratings yet
- Physio 1Document6 pagesPhysio 1amjadNo ratings yet
- Endocrine SystemDocument4 pagesEndocrine Systemden mNo ratings yet
- Notes in Science LT 10 - Endocrine SystemDocument3 pagesNotes in Science LT 10 - Endocrine SystemAlven ReyNo ratings yet
- The Endocrine Glands and The Nervous SystemDocument5 pagesThe Endocrine Glands and The Nervous SystemLyanna MormontNo ratings yet
- Endocrine SystemDocument7 pagesEndocrine SystemMikaella Viador100% (2)
- Endocrine System NotesDocument23 pagesEndocrine System NoteslacyNo ratings yet
- Med Surg EndocrineDocument13 pagesMed Surg EndocrineTeresa TorreonNo ratings yet
- OhohohDocument34 pagesOhohohuriNo ratings yet
- Topic 3 THE ENDOCRINE SYSTEMDocument41 pagesTopic 3 THE ENDOCRINE SYSTEMIreneNo ratings yet
- Chemical Coordination & Integration PowernotesDocument3 pagesChemical Coordination & Integration PowernotesSushmit SrivastavaNo ratings yet
- Endocrine SystemDocument14 pagesEndocrine SystemElaine Victoria ElizanNo ratings yet
- Endorine SystemDocument4 pagesEndorine SystemMichaela Shianne E. MatituNo ratings yet
- Endo Reviewer 1Document8 pagesEndo Reviewer 1ANA DelafuenteNo ratings yet
- The Endocrine System: Properties: Mechanisms of Hormone ActionDocument5 pagesThe Endocrine System: Properties: Mechanisms of Hormone ActionaudreyNo ratings yet
- PNKND Les 0 V 9 VWR60 B RCNDocument4 pagesPNKND Les 0 V 9 VWR60 B RCNaadeshthite476No ratings yet
- Module 5Document9 pagesModule 5CamilleCalmaLenonNo ratings yet
- EndocrineDocument5 pagesEndocrineShem DelolaNo ratings yet
- Endocrine Histology NotesDocument5 pagesEndocrine Histology NotesJulie TranNo ratings yet
- Unit 8: Endocrine System: Hormones Because Lipids Fear Water That's WhyDocument7 pagesUnit 8: Endocrine System: Hormones Because Lipids Fear Water That's WhyFaoloPanganNo ratings yet
- Endocrine System NotesDocument6 pagesEndocrine System Noteshannah pelonia100% (1)
- Endocrine SystemDocument4 pagesEndocrine SystemJames Castro100% (1)
- Endo ReviewerDocument5 pagesEndo ReviewerZIAN LABADIANo ratings yet
- Science: Endocrine & Nervous SystemDocument5 pagesScience: Endocrine & Nervous SystemLUISE DANIELLA DELOS REYES DOLOTALLASNo ratings yet
- MC1 REVIEWER (Endocrine System) - MIDTERMSDocument6 pagesMC1 REVIEWER (Endocrine System) - MIDTERMSFrancine Dominique CollantesNo ratings yet
- Endocrine DisordersDocument12 pagesEndocrine DisordersTrix Angelo S StacruzNo ratings yet
- Endocrine System Reviewer LecDocument3 pagesEndocrine System Reviewer LecNOELLE LAURAINNE TANZONo ratings yet
- The Endocrine System: Presented By: 5th Group Feby Amalia Hardianty Suryana Syuaib Andi Nurul Virninda Debby Trisia SariDocument24 pagesThe Endocrine System: Presented By: 5th Group Feby Amalia Hardianty Suryana Syuaib Andi Nurul Virninda Debby Trisia SariAndi Nurhidayah100% (1)
- Endocrine NotesDocument1 pageEndocrine NotesShivraj singh RajputNo ratings yet
- Hsslive Xi Zoology CH 22Document4 pagesHsslive Xi Zoology CH 22Ashly Santhosh KNo ratings yet
- Endo AnaphysioDocument9 pagesEndo AnaphysioShelley Jade MenorNo ratings yet
- Excretory Products and Their EliminationDocument12 pagesExcretory Products and Their EliminationPoorva NaikNo ratings yet
- Estrutura e Função Do Sistema Hipófise-HipotálamoDocument49 pagesEstrutura e Função Do Sistema Hipófise-HipotálamoMicheli CastroNo ratings yet
- Endocrine System TransesDocument5 pagesEndocrine System Transesadrielvamos28No ratings yet
- Endrocrine NotesDocument5 pagesEndrocrine NoteskatNo ratings yet
- Endocrine PhysiologyDocument79 pagesEndocrine PhysiologyCHALIE MEQUNo ratings yet
- Hormone Levels & Fertility Bloodwork - Fertility PlusDocument7 pagesHormone Levels & Fertility Bloodwork - Fertility PlusUtomo Budidarmo100% (1)
- AcromegalyDocument24 pagesAcromegalycsngiuNo ratings yet
- DX Test de GNRH 2011Document6 pagesDX Test de GNRH 2011Sheyla Alegre ParionaNo ratings yet
- Pituitary Gland IntroDocument40 pagesPituitary Gland IntroSaif AliNo ratings yet
- Clinical Case Diabetes Insipidus-2Document11 pagesClinical Case Diabetes Insipidus-2Marga Koury100% (1)
- Insulin in Pregnancy: Dr. Kyar Nyo Soe Myint Consultant Endocrinologist University of Medicine 2, NOGTHDocument39 pagesInsulin in Pregnancy: Dr. Kyar Nyo Soe Myint Consultant Endocrinologist University of Medicine 2, NOGTHYadanar KyawNo ratings yet
- Bio-Identical Hormones - New Beginnings-Half P VertDocument1 pageBio-Identical Hormones - New Beginnings-Half P VertsafinditNo ratings yet
- Indonesian Pediatric Endocrinology 4thDocument14 pagesIndonesian Pediatric Endocrinology 4thGendis Ayu ArdiasNo ratings yet
- 11th STD - Class-1 - Chemical Coordination and Integration - NotesDocument7 pages11th STD - Class-1 - Chemical Coordination and Integration - Notesdisha shuklaNo ratings yet
- Pedendo Proceedings Book Foutput Ok 2019 Permasalahan Dalam Skrining Hipotiroid Kongenital DiDocument186 pagesPedendo Proceedings Book Foutput Ok 2019 Permasalahan Dalam Skrining Hipotiroid Kongenital DiDamar Prasetya, Sp.ANo ratings yet
- Drugs Acting ON THE Endocrine SystemDocument81 pagesDrugs Acting ON THE Endocrine SystemLuis WashingtonNo ratings yet
- Hormone/Contraceptive Use in O&G: Provera Acute Maintena NceDocument2 pagesHormone/Contraceptive Use in O&G: Provera Acute Maintena Ncekhangsiean89No ratings yet
- Cockrem 2005 Conservation and Behavioral NeuroendocrinologyDocument10 pagesCockrem 2005 Conservation and Behavioral NeuroendocrinologyAmanda WerneckNo ratings yet
- Laboratory Diagnostics of (Selected) Endocrine DisordersDocument48 pagesLaboratory Diagnostics of (Selected) Endocrine DisordersPaulina PaskeviciuteNo ratings yet
- EndocrinologyDocument50 pagesEndocrinologyCut TirayaNo ratings yet
- Insulin IssuesDocument6 pagesInsulin Issuesdoctorzo0% (1)
- Thyroid DisorderDocument2 pagesThyroid Disordermaulikmd21No ratings yet
- Endocrine System QuizDocument4 pagesEndocrine System QuizIrams KitchenNo ratings yet
- Types of Diabetes MellitusDocument5 pagesTypes of Diabetes MellitusKlinik MaleoNo ratings yet
- Target BeneficiariesDocument6 pagesTarget BeneficiariesTommy SoleraNo ratings yet
- JurdingDocument10 pagesJurdingRuth Astry EvangeliaNo ratings yet
- Depot-Ped: 3 Months: 11.25 MG or 30 MG Q12weeks. (SQ) Lupron: Children: Initially, 50Document3 pagesDepot-Ped: 3 Months: 11.25 MG or 30 MG Q12weeks. (SQ) Lupron: Children: Initially, 50thuey epeNo ratings yet
- Hormonal Control ExerciseDocument32 pagesHormonal Control ExerciseamirNo ratings yet
- Animal Endocrine SystemDocument9 pagesAnimal Endocrine SystemAaron ZNo ratings yet
- MUL, Dick PDFDocument240 pagesMUL, Dick PDFNursyamsuddin MoganaNo ratings yet
- Hypothyroidism In Pregnancy The title page of the diploma thеsisDocument56 pagesHypothyroidism In Pregnancy The title page of the diploma thеsisEcaterina GorganNo ratings yet
- Case Ana - CC - Primary HyperthyroidismDocument15 pagesCase Ana - CC - Primary HyperthyroidismKatrina CanlapanNo ratings yet
- Glands and HormonesDocument1 pageGlands and HormonesRussel Dave ValenzuelaNo ratings yet
Endocrine System
Endocrine System
Uploaded by
Roeisa Salinas0 ratings0% found this document useful (0 votes)
39 views7 pagesThe document discusses the anatomy and functions of various endocrine glands. It describes the pituitary gland as having two lobes - the anterior pituitary gland which produces several hormones including growth hormone and prolactin, and the posterior pituitary gland which stores hormones produced in the hypothalamus. The thyroid gland produces thyroid hormones that regulate metabolism. The parathyroid glands regulate calcium levels through parathyroid hormone. Other glands discussed include the adrenal glands, pancreas, gonads, thymus, and pineal gland.
Original Description:
Anatomy and Physiology - Endocrine System transes by Roeisa Salinas
Original Title
ENDOCRINE SYSTEM
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe document discusses the anatomy and functions of various endocrine glands. It describes the pituitary gland as having two lobes - the anterior pituitary gland which produces several hormones including growth hormone and prolactin, and the posterior pituitary gland which stores hormones produced in the hypothalamus. The thyroid gland produces thyroid hormones that regulate metabolism. The parathyroid glands regulate calcium levels through parathyroid hormone. Other glands discussed include the adrenal glands, pancreas, gonads, thymus, and pineal gland.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
39 views7 pagesEndocrine System
Endocrine System
Uploaded by
Roeisa SalinasThe document discusses the anatomy and functions of various endocrine glands. It describes the pituitary gland as having two lobes - the anterior pituitary gland which produces several hormones including growth hormone and prolactin, and the posterior pituitary gland which stores hormones produced in the hypothalamus. The thyroid gland produces thyroid hormones that regulate metabolism. The parathyroid glands regulate calcium levels through parathyroid hormone. Other glands discussed include the adrenal glands, pancreas, gonads, thymus, and pineal gland.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 7
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
ENDOCRINE SYSTEM Gross Anatomy & Basic Function of Endocrine
Glands
Functional Anatomy of the Endocrine Glands
PITUITARY GLAND (hypophysis)
• 2nd major control system of body
• Coordinate and integrate body activities • in the sella turcica of sphenoid bone
• Hormone = Greek “to arouse” • 2 lobes: Adenohypophysis (APG) &
• Target Organs – respond to particular hormone Neurohypophysis (PPG) + infundibulum
• Cells have nuclei, mitochondria, ER, Golgi
bodies, secretory vesicles
4 main chemical groups that act as hormones:
1. Protein & glycoprotein molecules – insulin, GH,
PTH
2. Small peptide molecules – vasopressin, prods of
enteroendocrine cells
3. AA derivatives – thyroxine, adrenaline/epi,
noradrenaline/nore
4. Steroids from cholesterol – adrenal cortical
hormones, ovarian/testicular hormones
• Endocrine function – anterior P.G., thyroid,
adrenals, parathyroids
• Endo & Exocrine function – pancreas and Anterior Pituitary Gland (Adenohypophysis)
gonads • Epithelial upgrowth from roof of primitive oral
• Both gland types are derived from epithelium cavity – Rathke’s pouch (R’sP)
• Endocrine glands (EnG) – release hormones in • Contain a cleft/group of cyst-like spaces w/c
ECF/blood represent vestigial lumen of R’sP
• Exocrine glands (ExG) – release at body • Remnant of R’sP divides major part of APG from
surface/ducts thin zone of tissue, between APG & PPG – pars
intermedia
• Extension surrounds the neural stalk – pars
tuberalis
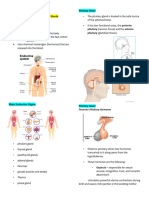
Posterior Pituitary Gland (Neurohypophysis/pars
nervosa)
• Downgrowth of nervous tissue from
hypothalamus, joined by pituitary stalk –
infundibulum
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
1. Oxytocin – produced in paraventricular nuclei,
“swift birth”
2. Antidiuretic hormone (ADH) –
vasopressin/arginine vasopressin, in supraoptic
nuclei; conserve water in distal convoluted tubules
of kidneys & collecting tubules reabsorb water by
sodium
PINEAL GLAND
• Small cone-shaped gland in rood of 3rd ventricle
• Major endo product is melatonin – diurnal
cycle/sleep-wake cycle
Anterior Pituitary Hormones: • Melatonin - peaks at night/lowest at noon; effect
on reprod. system that prevents precocious
• Target organ is another endoc. gland; secrete sexual maturation; changing level may affect
hormone in response to stimulation biological rhythms: body temp, sleep, appetite
• “master gland” – controls activity of many other
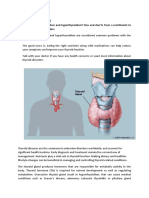
THYROID GLAND
endoc. Gland
1. Gonadotropins – regulate gamete production & • 2 lobes joined by a central mass – isthmus
hormonal activity (ovaries/testes) • Located in throat, inferior to larynx
• Epithelial downgrowth from fetal tongue
o Follicle-stimulating hormone (FSH) • C cells are from ultimobranchial element of 4th
o Luteinizing hormone (LH) branchial pouch
2. Adrenocorticotropic hormone (ACTH) – • Also part of normal brain development
endocrine activity of adrenal cortex • Cretinism – like dwarfism + affected brain,
3. Thyroid-stimulating hormone (TSH) – influence absence of thyroxine
growth and activity of thyroid gland 1. Thyroid hormone (TH) – 2 active hormones,
2 hormones not directly involved in EnG regulation: control rate of body metabolism and cellular
oxidation
4. Growth Hormone (GH) – determine body size,
growth of muscle/long bones o T4 (thyroxine/tetraiodothyronine)
o T3 (triiodothyronine) – more active
5. Prolactin (PRL) – milk production by breasts
2. Calcitonin – released in response to high blood
• Ventral hypothalamic hormones control Ca level
production/secretion of tropic hormones, GH,
PARATHYROID GLANDS
PRL
• Hypothalamic hormones reach cells of APG via • Embedded on posterior surface of thyroid gland
hypophyseal portal system (2nd image) • 2 small oval glands on each lobe
Posterior Pituitary Hormones: • Secrete parathyroid hormone (PTH) – most
important regulator of calcium balance of blood
• Not an EnG, does not synthesize hormones • Stimulate kidneys to convert vit D to active D3
• Storage area for 2 neurohormones transported form (Calcitriol)
to it via axons of neurons in paraventricular &
supraoptic nuclei of hypothalamus THYMUS
• Cell body (producer, in hypothalamus), • Bilobed gland in superior thorax, posterior to
infundibulum (long axon), herring bodies sternum, anterior to heart/lungs
(ends of PPG, storage of secretory vesicles) • Visible in infant, begins to thin at puberty, almost
invisible at old age
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
• Produces families of hormones: thymulin, THE GONADS
thymosin, thymopoietin
• Ovaries – paired, almond-sized organs in pelvic
• Involved in maturation of T lymphocytes/T cells cavity, produce female sex cells (ova); EnG and
and immune response ExG functions only begin at puberty; 2 steroid
• Act locally as paracrines (affect nearby cells) hormone groups
ADRENAL (SUPRARENAL) GLANDS 1. Estrogens
• At the top of kidneys - development of secondary sex charac.: maturation
• Triangle, “kidney party hats” of reprod. system and development of the breasts
• Adrenal medulla develops from neural crest - act w/ progesterone to bring cyclic changes of the
tissue uterine lining – menstrual cycle
• Directly controlled by SNS - prepare mammary gland for lactation
• Adrenal medulla – act w/ SNS, fight-or-flight
2. Progesterone
response
- uterine musculature in quiescent state
1. Epinephrine – 80%
- Helps prepare breast tissue for lactation
2. Norepinephrine – 20%
• Testes – paired oval suspended in pouchlike sac
• Adrenal cortex – 3 major groups of steroid (scrotum) outside pelvic cavity; produce male
hormones (corticosteroids) sex cells (sperm); EnG and ExG begin at
1. Mineralocorticoids (aldosterone) – zona puberty
glomerulosa, regulate water and electrolyte balance 1. Testosterone – maturation of reprod. system,
in ECFs by Na ion reabsorption in kidney tubules male secondary charac, sexual drive/libido
2. Glucocorticoids (cortisol (hydrocortisone),
cortisone, corticosterone) – z. fasciculata, resist
Microscopic Anatomy of Endocrine Glands
long-term stressors by increasing blood glucose
levels Anterior Pituitary Gland
3. Gonadocorticoids (sex hormones) – z. 2 main cells population based on color:
reticularis, androgens (male), estrogens (female) • Chromophils – w/ color
PANCREAS o Basophils – Violet/blue
o Acidophils – orange
• Partially behind stomach in abdomen
Note: Eosinophils - pink
• EnG and ExG functions
• Chromophobes – w/o color
• Produce digestive enzymes, insulin, glucagon
• Pancreatic islets/islets of Langerhans secrete
the hormones
1. Insulin – decrease blood sugar levels, accelerate
transport of glucose in body cells (oxidized for
energy/converted to glycogen or fat for storage);
from alpha cells
2. Glucagon – increase blood sugar level,
stimulates liver to break down glycogen stores to
glucose, synthesize glucose by gluconeogenesis, Other cells involved in secretion:
release glucose to blood; from beta cells
• Somatotrophs – GH secretion, 50%
• Mammotrophs – lactotrophs, PRL, 20%
• Corticotrophs – secrete ACTH, 20%
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
• Thyrotrophs – TSH (thyrotrophin), 5% Thyroid Gland
• Gonadotrophs – FSH and LSH, 5% • Follicles – spherical sacs w/ pink-stained
Pars intermedia material (colloid); stored T3 & T4 attached to
protein colloidal material stored in follicles as
• Derived embryologically from R’Sp
thyroglobulin; formed by simple
• Basophilic cells lying in irreg clusters between
cuboidal/squamous epithelial cells that
APG and PPG
synthesize products
• Contain small cystic spaces filled with
eosinophilic material
• Contain secretory granules like corticotrops
• Produce alpha-MSH from POMC at low levels
• Inactive – thyroid epithelial cells are simple
flat/cuboidal cells
• Active – tall and columnar
• Scalloped pale edge of colloid is where the
colloid has been removed from follicle lumen
(bitten off to release stored hormones)
Posterior Pituitary Gland
• Non-myelinated axons of specialized neurons
(neurosecretory activity)
• Cell bodies are in supraoptic (ADH) &
paraventricular nuclei (oxytocin) of
hypothalamus
• Hormones are passed down to axons in
neurosecretory granules, accumulate in
• Parafollicular or C cells – 2nd type of endoc cell
distended terminations of axons where contact
w/ neuroendocrine cells structure; found as
w/ capillaries happen – Herring bodies
scattered cells in the follicle lining/small clumps
• Pituicytes – specialized highly branched glial
in interstices between follicles; secrete
cells, supports axons
calcitonin
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
Parathyroid Glands - aldosterone secretion is independent of ACTH
control
2 major cell types:
• Chief cells – small w/ round central nuclei and
pale eosinophilic/clear cytoplasm; secrete and
synthesize PTH
• Oxyphil cells – occur in nodules; copious
eosinophilic cytoplasm seen packed with
mitochondria
2. Zona fasciculata – middle and broadest of the
cortical zones; w/ narrow columns and cords of cells,
1 cell thick, separated by fine strands of collagen and
wide-bore capillaries; abundant cytoplasm and pale
staining due to many lipid droplets; abundant
mitochondria and smooth ER
Adrenal (Suprarenal) glands - secretes glucocorticoid hormones (cortisol) w/
• Small, flat endoc glands closely applied to upper many metabolic effects:
pole of each kidney o Raise blood glucose level, increase cellular
2 types with diff functions and origin: synthesis of glycogen
• Adrenal cortex – similar embryological origin to o Increase rate of CHON breakdown and rate
gonads; secrets various steroid hormones; of liberation of lipid from tissue stores
adrenal steroids divided to 3:
o Mineralocorticoids – z.g. - cortisol secretion is controlled by hypothalamus
o Glucocorticoids – z.f. via APG tropic hormone ACTH
o Sex hormones – z.r.
Adrenal glands layers: 3 zonas + top & bottom layer
• Capsule
• Zona glomerulosa (z.g.)
• Zona fasciculata (z.f.)
• Zona reticularis (z.r.)
• Adrenal medulla
3. Zona reticularis – thin, innermost layer, lies next
1. Zona glomerulosa - cells arranged in irreg ovoid
to adrenal medulla; irreg network of branching cords
clusters separated by delicate fibrous trabeculae;
and clusters of glandular cells separated by wide
round nuclei, less cytoplasm than cells in z.f.;
diameter capillaries; cells are smaller than z.f. w/
cytoplasm with many smooth ER and mitochondria
less cytoplasm but darker staining because of fewer
w/ scanty lipid droplets
lipid droplets
- secretes mineralocorticoid hormones
(aldosterone) controlled by the RA system - brown lipofuscin pigment is seen, secretes small
- aldosterone acts directly on renal tubules to quantities of androgens and glucocorticoids
increase Na and water retention
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
2. Glucagon – metabolic effects that oppose insulin
Other cells present in the islets:
• Somatostatin – released by delta cells
• Vasoactive intestinal peptide (VIP)
• Pancreatic polypeptide (PP)
Enterochromaffin (EC) Cells:
• Motilin
• 5-hydroxytryptamine (5-HT, serotonin)
• Substance P
• Adrenal medulla – similar origin to SNS, highly
specialized add-on of this system; secretes • Islet of Langerhans – groups of up to 3000
catecholamine hormones under control of secretory cells supported by a fine collagenous
preganglionic neurons of SNS: network w/ fenestrated (tiny openings/pores)
o Adrenaline (epinephrine) capillary; delicate capsule surrounds each islet;
o Noradrenaline (norepinephrine) cells are small w/pale-stained granular
- clusters of cells w/ granular, faintly basophilic cytoplasm
cytoplasm, w/ many capillaries in their fine
supporting stroma
- acute physical and psychological stresses
initiate the release of these hormones
- released catecholamines act on adrenergic
receptors: heart/BVs, bronchioles, visceral
muscle, skeletal muscle
- adrenaline also has potent metabolic effects
(glycogenolysis)
- Insulin-producing beta cells over 60%
distributed in islet
- Glucagon-producing alpha cells about
25% arranged around periphery
Pineal Gland
2 main cell types:
• Pinealocytes (pineal chief cells) – highly
modified neurons in clusters and cords
surrounded by fenestrated capillaries; round
nuclei w/ prominent nucleoli and granular
Endocrine Pancreas cytoplasm; cytoplasmic granules w/ melatonin
and precursor 5-HT
• embryonic epithelium of the pancreatic ducts
• Neuroglial cells – like astrocytes of CNS;
consists of both exocrine and endocrine cells
dispersed between clusters of pinealocytes and
• during development, endocrine cells migrate in association w/ capillaries
from duct system and aggregate around
capillaries = isolated clusters of cells – islets of
Langerhans
• main secretory products:
1. Insulin – promotes uptake of glucose by most
cells (liver, skeletal muscle, adipose tissue)
MTY1102 Anatomy & Physiology Laboratory Salinas, Roeisa A.
You might also like
- Lesson Plan Diabetes MellitusDocument6 pagesLesson Plan Diabetes MellitusClaire100% (4)
- Endocrine SystemDocument20 pagesEndocrine SystemSheena Pasion100% (2)
- A Simple Guide to The Pineal Gland (The Third Eye) And Its FunctionFrom EverandA Simple Guide to The Pineal Gland (The Third Eye) And Its FunctionRating: 5 out of 5 stars5/5 (1)
- Endocrine ReviewDocument9 pagesEndocrine ReviewSpencer ThomasNo ratings yet
- Somatic Nervous SystemDocument4 pagesSomatic Nervous SystemGuenNo ratings yet
- Anaphy LecDocument5 pagesAnaphy Lecmelbertconag1973No ratings yet
- AnaPhy Lec - Endocrine SystemDocument2 pagesAnaPhy Lec - Endocrine SystemReigh DakotaNo ratings yet
- 22 Chemical Co-OrdinationDocument47 pages22 Chemical Co-OrdinationRachna JaiswalNo ratings yet
- Script For Midterm VRDocument5 pagesScript For Midterm VRDanica MerinNo ratings yet
- Endocrine System Animal ScienceDocument15 pagesEndocrine System Animal ScienceJairus LampanoNo ratings yet
- Chemical Co Ordination and Integration - 434dea34 f494 4704 A8c9 6876397e324eDocument53 pagesChemical Co Ordination and Integration - 434dea34 f494 4704 A8c9 6876397e324epcgurukotari9No ratings yet
- Genbio2 ReviewerDocument4 pagesGenbio2 ReviewerLovely QuezonNo ratings yet
- Quick Study Guide To The Endocrine SystemDocument11 pagesQuick Study Guide To The Endocrine SystemMc Luis Glen AserdanoNo ratings yet
- Endocrine Glands - 1st - ChapterDocument12 pagesEndocrine Glands - 1st - Chaptervarun kumarNo ratings yet
- Endocrine System NotesDocument8 pagesEndocrine System NotesShiela Mae SagayoNo ratings yet
- Endokrinologi Reproduksi: Bayu Kurniawan, DRDocument48 pagesEndokrinologi Reproduksi: Bayu Kurniawan, DRdocbay100% (1)
- Animal Hormones PDFDocument11 pagesAnimal Hormones PDFAin HusnaNo ratings yet
- ANATOMY Endocrine TranscribedDocument9 pagesANATOMY Endocrine TranscribedYanyan PanesNo ratings yet
- EndocrineDocument49 pagesEndocrineHerbert DelacruzNo ratings yet
- Endocrine System (Zoology)Document3 pagesEndocrine System (Zoology)Cheska de GuzmanNo ratings yet
- Endocrine SystemDocument43 pagesEndocrine SystemnandaNo ratings yet
- Endocrine System PTT FinalDocument56 pagesEndocrine System PTT FinalVenice GalleneroNo ratings yet
- Chemical Coordination and IntegrationDocument3 pagesChemical Coordination and Integrationakhil01ajNo ratings yet
- Reproduction & Endocrinology 1: Hypothalamus and PituitaryDocument41 pagesReproduction & Endocrinology 1: Hypothalamus and PituitaryabdulNo ratings yet
- The Nervous and The Endocrine SystemsDocument9 pagesThe Nervous and The Endocrine SystemsluciaarecesdiazNo ratings yet
- Endocrine Glands and Their FunctionsDocument31 pagesEndocrine Glands and Their FunctionsAfrina Asmi MINo ratings yet
- Endocrine SystemDocument7 pagesEndocrine SystemClyde CapapasNo ratings yet
- Physio 1Document6 pagesPhysio 1amjadNo ratings yet
- Endocrine SystemDocument4 pagesEndocrine Systemden mNo ratings yet
- Notes in Science LT 10 - Endocrine SystemDocument3 pagesNotes in Science LT 10 - Endocrine SystemAlven ReyNo ratings yet
- The Endocrine Glands and The Nervous SystemDocument5 pagesThe Endocrine Glands and The Nervous SystemLyanna MormontNo ratings yet
- Endocrine SystemDocument7 pagesEndocrine SystemMikaella Viador100% (2)
- Endocrine System NotesDocument23 pagesEndocrine System NoteslacyNo ratings yet
- Med Surg EndocrineDocument13 pagesMed Surg EndocrineTeresa TorreonNo ratings yet
- OhohohDocument34 pagesOhohohuriNo ratings yet
- Topic 3 THE ENDOCRINE SYSTEMDocument41 pagesTopic 3 THE ENDOCRINE SYSTEMIreneNo ratings yet
- Chemical Coordination & Integration PowernotesDocument3 pagesChemical Coordination & Integration PowernotesSushmit SrivastavaNo ratings yet
- Endocrine SystemDocument14 pagesEndocrine SystemElaine Victoria ElizanNo ratings yet
- Endorine SystemDocument4 pagesEndorine SystemMichaela Shianne E. MatituNo ratings yet
- Endo Reviewer 1Document8 pagesEndo Reviewer 1ANA DelafuenteNo ratings yet
- The Endocrine System: Properties: Mechanisms of Hormone ActionDocument5 pagesThe Endocrine System: Properties: Mechanisms of Hormone ActionaudreyNo ratings yet
- PNKND Les 0 V 9 VWR60 B RCNDocument4 pagesPNKND Les 0 V 9 VWR60 B RCNaadeshthite476No ratings yet
- Module 5Document9 pagesModule 5CamilleCalmaLenonNo ratings yet
- EndocrineDocument5 pagesEndocrineShem DelolaNo ratings yet
- Endocrine Histology NotesDocument5 pagesEndocrine Histology NotesJulie TranNo ratings yet
- Unit 8: Endocrine System: Hormones Because Lipids Fear Water That's WhyDocument7 pagesUnit 8: Endocrine System: Hormones Because Lipids Fear Water That's WhyFaoloPanganNo ratings yet
- Endocrine System NotesDocument6 pagesEndocrine System Noteshannah pelonia100% (1)
- Endocrine SystemDocument4 pagesEndocrine SystemJames Castro100% (1)
- Endo ReviewerDocument5 pagesEndo ReviewerZIAN LABADIANo ratings yet
- Science: Endocrine & Nervous SystemDocument5 pagesScience: Endocrine & Nervous SystemLUISE DANIELLA DELOS REYES DOLOTALLASNo ratings yet
- MC1 REVIEWER (Endocrine System) - MIDTERMSDocument6 pagesMC1 REVIEWER (Endocrine System) - MIDTERMSFrancine Dominique CollantesNo ratings yet
- Endocrine DisordersDocument12 pagesEndocrine DisordersTrix Angelo S StacruzNo ratings yet
- Endocrine System Reviewer LecDocument3 pagesEndocrine System Reviewer LecNOELLE LAURAINNE TANZONo ratings yet
- The Endocrine System: Presented By: 5th Group Feby Amalia Hardianty Suryana Syuaib Andi Nurul Virninda Debby Trisia SariDocument24 pagesThe Endocrine System: Presented By: 5th Group Feby Amalia Hardianty Suryana Syuaib Andi Nurul Virninda Debby Trisia SariAndi Nurhidayah100% (1)
- Endocrine NotesDocument1 pageEndocrine NotesShivraj singh RajputNo ratings yet
- Hsslive Xi Zoology CH 22Document4 pagesHsslive Xi Zoology CH 22Ashly Santhosh KNo ratings yet
- Endo AnaphysioDocument9 pagesEndo AnaphysioShelley Jade MenorNo ratings yet
- Excretory Products and Their EliminationDocument12 pagesExcretory Products and Their EliminationPoorva NaikNo ratings yet
- Estrutura e Função Do Sistema Hipófise-HipotálamoDocument49 pagesEstrutura e Função Do Sistema Hipófise-HipotálamoMicheli CastroNo ratings yet
- Endocrine System TransesDocument5 pagesEndocrine System Transesadrielvamos28No ratings yet
- Endrocrine NotesDocument5 pagesEndrocrine NoteskatNo ratings yet
- Endocrine PhysiologyDocument79 pagesEndocrine PhysiologyCHALIE MEQUNo ratings yet
- Hormone Levels & Fertility Bloodwork - Fertility PlusDocument7 pagesHormone Levels & Fertility Bloodwork - Fertility PlusUtomo Budidarmo100% (1)
- AcromegalyDocument24 pagesAcromegalycsngiuNo ratings yet
- DX Test de GNRH 2011Document6 pagesDX Test de GNRH 2011Sheyla Alegre ParionaNo ratings yet
- Pituitary Gland IntroDocument40 pagesPituitary Gland IntroSaif AliNo ratings yet
- Clinical Case Diabetes Insipidus-2Document11 pagesClinical Case Diabetes Insipidus-2Marga Koury100% (1)
- Insulin in Pregnancy: Dr. Kyar Nyo Soe Myint Consultant Endocrinologist University of Medicine 2, NOGTHDocument39 pagesInsulin in Pregnancy: Dr. Kyar Nyo Soe Myint Consultant Endocrinologist University of Medicine 2, NOGTHYadanar KyawNo ratings yet
- Bio-Identical Hormones - New Beginnings-Half P VertDocument1 pageBio-Identical Hormones - New Beginnings-Half P VertsafinditNo ratings yet
- Indonesian Pediatric Endocrinology 4thDocument14 pagesIndonesian Pediatric Endocrinology 4thGendis Ayu ArdiasNo ratings yet
- 11th STD - Class-1 - Chemical Coordination and Integration - NotesDocument7 pages11th STD - Class-1 - Chemical Coordination and Integration - Notesdisha shuklaNo ratings yet
- Pedendo Proceedings Book Foutput Ok 2019 Permasalahan Dalam Skrining Hipotiroid Kongenital DiDocument186 pagesPedendo Proceedings Book Foutput Ok 2019 Permasalahan Dalam Skrining Hipotiroid Kongenital DiDamar Prasetya, Sp.ANo ratings yet
- Drugs Acting ON THE Endocrine SystemDocument81 pagesDrugs Acting ON THE Endocrine SystemLuis WashingtonNo ratings yet
- Hormone/Contraceptive Use in O&G: Provera Acute Maintena NceDocument2 pagesHormone/Contraceptive Use in O&G: Provera Acute Maintena Ncekhangsiean89No ratings yet
- Cockrem 2005 Conservation and Behavioral NeuroendocrinologyDocument10 pagesCockrem 2005 Conservation and Behavioral NeuroendocrinologyAmanda WerneckNo ratings yet
- Laboratory Diagnostics of (Selected) Endocrine DisordersDocument48 pagesLaboratory Diagnostics of (Selected) Endocrine DisordersPaulina PaskeviciuteNo ratings yet
- EndocrinologyDocument50 pagesEndocrinologyCut TirayaNo ratings yet
- Insulin IssuesDocument6 pagesInsulin Issuesdoctorzo0% (1)
- Thyroid DisorderDocument2 pagesThyroid Disordermaulikmd21No ratings yet
- Endocrine System QuizDocument4 pagesEndocrine System QuizIrams KitchenNo ratings yet
- Types of Diabetes MellitusDocument5 pagesTypes of Diabetes MellitusKlinik MaleoNo ratings yet
- Target BeneficiariesDocument6 pagesTarget BeneficiariesTommy SoleraNo ratings yet
- JurdingDocument10 pagesJurdingRuth Astry EvangeliaNo ratings yet
- Depot-Ped: 3 Months: 11.25 MG or 30 MG Q12weeks. (SQ) Lupron: Children: Initially, 50Document3 pagesDepot-Ped: 3 Months: 11.25 MG or 30 MG Q12weeks. (SQ) Lupron: Children: Initially, 50thuey epeNo ratings yet
- Hormonal Control ExerciseDocument32 pagesHormonal Control ExerciseamirNo ratings yet
- Animal Endocrine SystemDocument9 pagesAnimal Endocrine SystemAaron ZNo ratings yet
- MUL, Dick PDFDocument240 pagesMUL, Dick PDFNursyamsuddin MoganaNo ratings yet
- Hypothyroidism In Pregnancy The title page of the diploma thеsisDocument56 pagesHypothyroidism In Pregnancy The title page of the diploma thеsisEcaterina GorganNo ratings yet
- Case Ana - CC - Primary HyperthyroidismDocument15 pagesCase Ana - CC - Primary HyperthyroidismKatrina CanlapanNo ratings yet
- Glands and HormonesDocument1 pageGlands and HormonesRussel Dave ValenzuelaNo ratings yet