Professional Documents
Culture Documents
08 CLS 382 443 Enzymes Pancreas FINAL
08 CLS 382 443 Enzymes Pancreas FINAL
Uploaded by
amal0 ratings0% found this document useful (0 votes)
16 views8 pagesThe pancreas has both exocrine and endocrine functions. The exocrine pancreas produces enzymes that digest nutrients, while the endocrine pancreas produces hormones like insulin that regulate blood sugar. Pancreatitis occurs when digestive enzymes inside the pancreas become activated and cause inflammation. Acute pancreatitis develops quickly but resolves in weeks, while chronic pancreatitis causes long-lasting inflammation and scarring. Gallstones and alcohol abuse are the main causes. Diagnosis involves blood tests of pancreatic enzymes and imaging of the abdomen.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe pancreas has both exocrine and endocrine functions. The exocrine pancreas produces enzymes that digest nutrients, while the endocrine pancreas produces hormones like insulin that regulate blood sugar. Pancreatitis occurs when digestive enzymes inside the pancreas become activated and cause inflammation. Acute pancreatitis develops quickly but resolves in weeks, while chronic pancreatitis causes long-lasting inflammation and scarring. Gallstones and alcohol abuse are the main causes. Diagnosis involves blood tests of pancreatic enzymes and imaging of the abdomen.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
16 views8 pages08 CLS 382 443 Enzymes Pancreas FINAL
08 CLS 382 443 Enzymes Pancreas FINAL
Uploaded by
amalThe pancreas has both exocrine and endocrine functions. The exocrine pancreas produces enzymes that digest nutrients, while the endocrine pancreas produces hormones like insulin that regulate blood sugar. Pancreatitis occurs when digestive enzymes inside the pancreas become activated and cause inflammation. Acute pancreatitis develops quickly but resolves in weeks, while chronic pancreatitis causes long-lasting inflammation and scarring. Gallstones and alcohol abuse are the main causes. Diagnosis involves blood tests of pancreatic enzymes and imaging of the abdomen.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 8
CLS 382 - Lecture 8
Clinical Enzymology – Pancreas
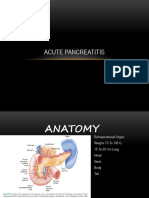
Pancreatic tissue
• The pancreas consists of two kinds
of tissues that perform different
functions:
➢ The exocrine pancreas:
- makes, stores and releases powerful
enzymes (in an inactive form to the
small intestine) to digest fats, proteins,
and carbohydrates.
- makes and releases bicarbonate to
neutralize stomach acids and allow for
the activation of pancreatic enzymes
once needed.
➢ The endocrine pancreas:
- produces hormones that help
maintain normal blood sugar levels by
regulating glucose transport into the
body's cells, where it is used for energy
(e.g. insulin and glucagon)
• Pancreatitis may occur when digestive
enzymes become activated while still
inside the pancreas, causing irritation
and injury to pancreatic tissue and
leading to inflammation.
• In acute pancreatitis, inflammation develops quickly and then goes away after a few
days to weeks.
• The main causes are gallstones (block the pancreatic duct) and long-term alcohol
abuse.
• Moderate to severe attacks may require a long hospital stay to monitor for and treat
serious complications.
• With treatment, mild attacks may get better after a few days. In mild cases, your
pancreas may return to normal once it has healed.
• Recurrent attacks of acute pancreatitis can lead to chronic pancreatitis.
• Chronic pancreatitis is long-lasting inflammation in the pancreas.
• Long-term alcohol abuse is the main cause. Smoking cigarettes also increases risk.
• It can lead to the formation of scar tissue in the pancreas that keeps it from working
properly.
• A pancreas that does not work properly can lead to digestive problems and diabetes.
• Pancreatitis occurs more often in men than in women. It is becoming more common,
though the reasons for this aren't clear.
• For instance, in the US, nearly 275,000 people are hospitalized with acute
pancreatitis each year. Chronic pancreatitis is less common, with about 86,000
people hospitalized.
Causes of pancreatitis
• Gallstones and long-term alcohol abuse are the main causes of pancreatitis. Others include:
➢ Medications (e.g.) valproic acid (for seizure or bipolar disorders)
estrogen (menopause or osteoporosis)
➢ Viral infections such as mumps and Epstein-Barr virus
➢ Very high blood triglyceride level (hypertriglyceridemia)
➢ high blood calcium level (hypercalcemia)
➢ Cystic fibrosis (or being a carrier of a gene that causes cystic fibrosis)
➢ Inherited defects that result in early activation of digestive enzymes
➢ Pancreatic cancer
➢ Certain autoimmune conditions
➢ Injury (trauma) to the pancreas
• Some cases of acute and chronic pancreatitis have no clear cause
• Pancreatitis can cluster in some families, and there are several known genes that contribute
to increased risk for pancreatitis.
• In children, cystic fibrosis is a major cause of chronic pancreatic failure.
• It is usually suspected clinically in infancy as the children present with chronic refractory foul
stools, recurrent chest infections and failure to thrive.
• It is diagnosed by confirming an increased concentration of chloride in the sweat.
• Genetic confirmation is usually made, but the condition can be caused by a large number of
mutations in the CFTR gene.
Diagnosis
• Pancreatitis is diagnosed with physical exam/medical history, blood tests, and imaging
• At least 2 of the 3 following criteria must be present to diagnose acute pancreatitis:
i. Abdominal pain that is "consistent with the disease"
ii. Levels of lipase or amylase (pancreatic enzymes) that are 3x higher than the ULN
iii. "Characteristic" abdominal imaging results
Laboratory Tests
1- Lipase (preferred); as it is more specific than amylase for diseases of the pancreas,
particularly for acute pancreatitis and for acute alcoholic pancreatitis.
• Levels start to rise within (4-8) hrs of the onset of pancreatitis symptoms and typically return
to normal within a week.
• Acute pancreatitis is diagnosed if the lipase level reaches 3 times above the upper limit of
normal. As chronic pancreatitis gets worse, lipase levels may return to normal or decrease.
2- Amylase; while the amylase test is sensitive for pancreatic diseases, it is not specific.
• An elevated amylase level may indicate a problem, but the cause may not be related to the
pancreas.
• Levels start to rise (2-12) hrs after the onset of acute pancreatitis symptoms and typically
return to normal within a week.
• Acute pancreatitis is likely if the level reaches 3 times above the upper limit of normal.
• Amylase also may be monitored in people with chronic pancreatitis. It will often be
moderately elevated until the cells that make it become damaged, at which point blood
levels of amylase may be decreased.
• The pancreas is the major source of digestive enzymes. Deficiency of these enzymes causes
profound maldigestion, and subsequently malabsorption.
• In suspected enzyme deficiency, a therapeutic trial of oral enzyme replacement with food
will usually confirm the diagnosis.
• Fecal elastase or chymotrypsin are occasionally measured to confirm the presence of
residual pancreatic function.
• Quantitative measurements of pancreatic enzymes in intestinal secretions are no longer
performed in routine clinical practice.
Other tests
• To help diagnose or detect complications of • To help diagnose and evaluate chronic
acute pancreatitis pancreatitis
➢ Complete blood count –CBC- ➢ Pancreatic enzymes elastase (reduced) and
(WBC count could point to infection) chymotrypsin (absent) in stool in pancreatic
➢ Triglycerides insufficiency (which could be caused by chronic
pancreatitis). Both are occasionally measured to
➢ Liver panel (including bilirubin and confirm the presence of residual pancreatic
liver enzymes) function
➢ Glucose ➢ Fecal fat (fat in the stool) as excess fat in stool is
often the first sign of pancreatic insufficiency
➢ Calcium (largely replaced now by fecal elastase).
➢ Magnesium ➢ Immunoreactive trypsinogen (IRT):
trypsinogen, an inactive precursor produced by
➢ C-reactive protein (CRP is a measure of the pancreas that is converted to the enzyme
inflammation) trypsin; the pancreatic enzyme that digests
proteins. IRT may be elevated with pancreatitis
➢ Sweat (chloride) test for diagnosis of CF
➢ Tests for genetic mutations such as those
associated with CF (CFTR Gene Mutation
Testing) or other causes of hereditary
pancreatitis
You might also like
- Acute PancreatitisDocument31 pagesAcute PancreatitisAmoroso, Marian Corneth D.No ratings yet
- Create Your Concept Map of Chronic Pancreatitis: Diagnostic TestDocument2 pagesCreate Your Concept Map of Chronic Pancreatitis: Diagnostic TestAnne B. BuenvenidaNo ratings yet
- Case Write Up Acute PancreatitisDocument25 pagesCase Write Up Acute PancreatitislunaNo ratings yet
- All Therapy 200 RATOS 2010Document284 pagesAll Therapy 200 RATOS 2010Bhargavi SunkiNo ratings yet
- Acute PancreatitisDocument35 pagesAcute PancreatitisJerson Ingno100% (4)
- PancreatitisDocument26 pagesPancreatitisJnah Macs100% (2)
- By: Mark Benjamer R. CarganillaDocument22 pagesBy: Mark Benjamer R. CarganillahabibikoNo ratings yet
- Acute PancreatitisDocument7 pagesAcute PancreatitisVytheeshwaran Vedagiri100% (9)
- 4-Hepatobiliary DiseaseDocument22 pages4-Hepatobiliary Diseaseabdalmajeed alshammaryNo ratings yet
- Acute PancreatitisDocument79 pagesAcute Pancreatitiszaiba0786No ratings yet
- PancreatitisDocument6 pagesPancreatitisMahaNo ratings yet
- Acute and Chronic PancreatitisDocument13 pagesAcute and Chronic PancreatitisZeinab AmerNo ratings yet
- 3-Pancreas-SG-2022-After Class-FinalDocument20 pages3-Pancreas-SG-2022-After Class-FinalTyler YounNo ratings yet
- Pancreatitis: What Is The Pancreas and What Does It Do?Document5 pagesPancreatitis: What Is The Pancreas and What Does It Do?NonameNo ratings yet
- By DR.: Haitham Mokhtar Mohamed Abd AllahDocument101 pagesBy DR.: Haitham Mokhtar Mohamed Abd AllahMohamed ElkadyNo ratings yet
- Pancreas - Enzyme and FunctionDocument18 pagesPancreas - Enzyme and FunctionLisa PalabaoNo ratings yet
- 24+pancreas Pancreatitis+-+updateDocument27 pages24+pancreas Pancreatitis+-+updateMinh Nguyễn Phương HồngNo ratings yet
- Pancreatitis PresentationDocument41 pagesPancreatitis Presentationak2621829No ratings yet
- Welcome To The Morning Session: Dr. Sadia AfrinDocument37 pagesWelcome To The Morning Session: Dr. Sadia AfrinGENERAL sharpNo ratings yet
- Pancreatitis Definition of TermsDocument6 pagesPancreatitis Definition of TermsDonna Marie Arguelles AmpaNo ratings yet
- Pancreatitis: Def Pancreatitis (Inflammation of The Pancreas) Is A Serious Disorder. The Most Basic Classification SystemDocument5 pagesPancreatitis: Def Pancreatitis (Inflammation of The Pancreas) Is A Serious Disorder. The Most Basic Classification SystemSanthu Su100% (2)
- Acute PancreatitisDocument19 pagesAcute PancreatitisFloida Rose KatterNo ratings yet
- PANCREASDocument74 pagesPANCREASzaiba0786No ratings yet
- Acute Pancreatitis by Yuvaraj BSC Nursing Sec YearDocument9 pagesAcute Pancreatitis by Yuvaraj BSC Nursing Sec Yearvidhyasagar754No ratings yet
- Askep PankreatitisDocument48 pagesAskep PankreatitisYeni DwiNo ratings yet
- Acute PancreatitisDocument64 pagesAcute PancreatitisOleksandr RotarNo ratings yet
- Pancreatitis: Pancreatitis Is Inflammation of The Pancreas. It Occurs When Pancreatic Enzymes (Especially Trypsin)Document6 pagesPancreatitis: Pancreatitis Is Inflammation of The Pancreas. It Occurs When Pancreatic Enzymes (Especially Trypsin)tianallyNo ratings yet
- Chronic Pancreatitis DR AhsanDocument46 pagesChronic Pancreatitis DR Ahsanahsanshabbir1111No ratings yet
- Blood Urea Nitrogen (BUN) Measures The Amount of Urea Nitrogen, ADocument15 pagesBlood Urea Nitrogen (BUN) Measures The Amount of Urea Nitrogen, ArayevieNo ratings yet
- SESSION 4 - Acute PancreatitisDocument27 pagesSESSION 4 - Acute Pancreatitisndunguruyovin29No ratings yet
- 8 Pancreatic Disease 2slidesDocument32 pages8 Pancreatic Disease 2slidesOmar khalidNo ratings yet
- PancreatitisDocument59 pagesPancreatitisrimsha waseemNo ratings yet
- Acute Pancreatitis by DR DilmoDocument50 pagesAcute Pancreatitis by DR Dilmosinan kNo ratings yet
- PancreatitisDocument18 pagesPancreatitisDr.Gutale AlmuqdishawiNo ratings yet
- Acute PancreatitisDocument40 pagesAcute PancreatitisAbdulsalam DostNo ratings yet
- Pancreatitis PDFDocument19 pagesPancreatitis PDFSidraNo ratings yet
- Acute Pancreatitis SymptomsDocument12 pagesAcute Pancreatitis SymptomsUthraa SalvatoreNo ratings yet
- Case Concept Acute PrancreatitisDocument8 pagesCase Concept Acute PrancreatitisGio GallegoNo ratings yet
- Acute Pancreatitis: Dr. Ali Raza Dr. Talha Javed CHDocument31 pagesAcute Pancreatitis: Dr. Ali Raza Dr. Talha Javed CHahmad frazNo ratings yet
- Chronic DiarrheaDocument66 pagesChronic DiarrheaJulita Yanti100% (1)
- Pancreatitis Group 5Document25 pagesPancreatitis Group 5Mark Jefferson LunaNo ratings yet
- Chronic PancreatitisDocument48 pagesChronic Pancreatitismolinbenisto100No ratings yet
- Clinicopathological Conference CPC #6: 45 Y/o Male With Intermittent Abdominal Pain, Nausea, and DiarrheaDocument24 pagesClinicopathological Conference CPC #6: 45 Y/o Male With Intermittent Abdominal Pain, Nausea, and DiarrheaElaine June FielNo ratings yet
- Diseases of Pancreas Ug ClassDocument107 pagesDiseases of Pancreas Ug ClassSrinivas PamarthiNo ratings yet
- Chronic PancreatitisDocument47 pagesChronic PancreatitismalekNo ratings yet
- Chronic PancreatitisDocument51 pagesChronic PancreatitisAli Nawaz khanNo ratings yet
- Acute PancreatitisDocument40 pagesAcute PancreatitisMustafa HusainNo ratings yet
- Acute Pancreatitis - IanDocument21 pagesAcute Pancreatitis - Ianhandrian rahmanNo ratings yet
- PancreATITIS OCT. 21, 2021Document33 pagesPancreATITIS OCT. 21, 2021Alyssa NicoleNo ratings yet
- Acutep 1Document45 pagesAcutep 1api-19916399No ratings yet
- Chapter - 2 - C - II Liver CirrhosisDocument39 pagesChapter - 2 - C - II Liver CirrhosisEmmaNo ratings yet
- NCM 30 Study Guide On The ChildDocument6 pagesNCM 30 Study Guide On The ChildJai - HoNo ratings yet
- Acute Pancreatitis (Acute Pancreatic Necrosis)Document12 pagesAcute Pancreatitis (Acute Pancreatic Necrosis)sosotarab2No ratings yet
- Chemical Pathology of The Stomach PancreasDocument92 pagesChemical Pathology of The Stomach Pancreasallenshanique1999No ratings yet
- PancreasDocument78 pagesPancreasabdirahiim ahmedNo ratings yet
- Nephrology - Proteinuria - SOAP Note - Manish Suneja PDFDocument4 pagesNephrology - Proteinuria - SOAP Note - Manish Suneja PDFΝίκος ΣυρίγοςNo ratings yet
- Physiology of PancreaticDocument61 pagesPhysiology of PancreaticMuhammad AbdullahNo ratings yet
- Acute PancreatitisDocument40 pagesAcute PancreatitisSiddarth KumarNo ratings yet
- Gall Bladder Diseases by - DR Arun Aggarwal GastroenterologistDocument53 pagesGall Bladder Diseases by - DR Arun Aggarwal GastroenterologistDr. Arun Aggarwal GastroenterologistNo ratings yet
- Сhronic pancreatitis: Lykhatska G.VDocument42 pagesСhronic pancreatitis: Lykhatska G.VOlga CîrsteaNo ratings yet
- PancreatitisDocument13 pagesPancreatitisIbrahim kargboNo ratings yet
- Ulcerative Colitis, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandUlcerative Colitis, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Liver Cirrhosis, A Simple Guide To The Condition, Treatment And Related DiseasesFrom EverandLiver Cirrhosis, A Simple Guide To The Condition, Treatment And Related DiseasesNo ratings yet
- Surgery Oral Exam CASES JMC 12 2008 V2Document17 pagesSurgery Oral Exam CASES JMC 12 2008 V2aaronlhuangNo ratings yet
- Nursing Care PlansDocument10 pagesNursing Care PlansClaire Alcantara50% (2)
- February / March 2010Document16 pagesFebruary / March 2010Instrulife OostkampNo ratings yet
- Chronic PancreatitisDocument23 pagesChronic PancreatitisAlvin YeeNo ratings yet
- Acute PancreatitisDocument66 pagesAcute PancreatitisSamina GulNo ratings yet
- TESTS "STEP-2" Full Base 2014Document57 pagesTESTS "STEP-2" Full Base 2014gauravNo ratings yet
- Book PDF Educational Psychology Developing Learners Loose Leaf Version PDF Full ChapterDocument23 pagesBook PDF Educational Psychology Developing Learners Loose Leaf Version PDF Full Chaptertammy.rankin407100% (15)
- Acute Pancreatitis Part 3Document23 pagesAcute Pancreatitis Part 3Jerome CidNo ratings yet
- Pancreatic PathologyDocument7 pagesPancreatic Pathologyzeroun24100% (1)
- Abdominal Case Study CompiledDocument392 pagesAbdominal Case Study CompiledIshak IzharNo ratings yet
- Gi Exam2016Document28 pagesGi Exam2016Andrea BroccoliNo ratings yet
- (Forensic Pathology Reviews 5) Burkhard Madea, Michael Tsokos, Johanna Preuß (Auth.), Michael Tsokos MD (Eds.) - Forensic Pathology Reviews-Humana Press (2008) PDFDocument289 pages(Forensic Pathology Reviews 5) Burkhard Madea, Michael Tsokos, Johanna Preuß (Auth.), Michael Tsokos MD (Eds.) - Forensic Pathology Reviews-Humana Press (2008) PDFDeo Rafael100% (1)
- Acute AbdomenDocument24 pagesAcute AbdomenGrace SimmonsNo ratings yet
- Acute Abdominal Pain MS LectureDocument63 pagesAcute Abdominal Pain MS LectureRovanNo ratings yet
- DR Is-Acute PancreatitisDocument11 pagesDR Is-Acute PancreatitisSemestaNo ratings yet
- Nodular Fat Necrosis in The Feline and Canine AbdomenDocument5 pagesNodular Fat Necrosis in The Feline and Canine Abdomenludiegues752No ratings yet
- Prostate McqsDocument21 pagesProstate McqsFarah FarahNo ratings yet
- Mcqs IV Year Students SurgeryDocument38 pagesMcqs IV Year Students SurgeryAbdimajiidNo ratings yet
- PANCREATITIS Patient EducationDocument4 pagesPANCREATITIS Patient EducationRomalyn AcquidanNo ratings yet
- Advanced - GIT Block 2 - @eduwaves360Document234 pagesAdvanced - GIT Block 2 - @eduwaves360Anh DungxNo ratings yet
- GI Answer Key Part 1Document5 pagesGI Answer Key Part 1Nom NomNo ratings yet
- Syllabus - DM M CH PDFDocument131 pagesSyllabus - DM M CH PDFDrarfatNo ratings yet
- Hepatobiliary Pancreatic Radiology 1683072599120Document31 pagesHepatobiliary Pancreatic Radiology 1683072599120Shivank RastogiNo ratings yet
- Med Surg SyllabusDocument16 pagesMed Surg SyllabusCrystal AshleyNo ratings yet
- Medical Surgical NursingDocument6 pagesMedical Surgical NursingMariel Febreo MerlanNo ratings yet
- Medsurg P2 Part 1 1 2Document22 pagesMedsurg P2 Part 1 1 2mary ann corsanesNo ratings yet
- Met Caz ClinicDocument57 pagesMet Caz ClinicIndrecan AndreiNo ratings yet