Professional Documents
Culture Documents
(02.12) CM Valvular Heart Diseases (TG20) - Anne Gabrielle Liu
(02.12) CM Valvular Heart Diseases (TG20) - Anne Gabrielle Liu
Uploaded by
Mikmik DGCopyright:
Available Formats
You might also like
- Pamphlet 80 - Edition 4 - August 2014Document33 pagesPamphlet 80 - Edition 4 - August 2014Reza AranNo ratings yet
- KP 238 Tahun 2018 PDFDocument298 pagesKP 238 Tahun 2018 PDFAviation MedicineNo ratings yet
- Head and Neck AnatomyDocument115 pagesHead and Neck AnatomyMobarobber100% (11)
- Medicine Clinics Guide: Summary of Bates Tables From DR DominguezDocument226 pagesMedicine Clinics Guide: Summary of Bates Tables From DR DominguezSaf DicamNo ratings yet
- All ORE OSCEs PDFDocument123 pagesAll ORE OSCEs PDFAna100% (1)
- Nursing Care Plan PIHDocument2 pagesNursing Care Plan PIHLei Ortega100% (7)
- Pocket Reference For ECGs Made Easy 5th EditionDocument133 pagesPocket Reference For ECGs Made Easy 5th EditionSylvia Loong100% (2)
- Ecls GuidDocument24 pagesEcls GuidHanafieHeluthNo ratings yet
- Endogenous Cardiotonic SteroidsDocument30 pagesEndogenous Cardiotonic SteroidsSebastian NemethNo ratings yet
- (MED-HO) 02 Aplastic Anemia, AIHA, PVDocument23 pages(MED-HO) 02 Aplastic Anemia, AIHA, PVJolaine ValloNo ratings yet
- ESVS Thoracic Ds PDFDocument49 pagesESVS Thoracic Ds PDFFredy CarolNo ratings yet
- DHS Austere EMS Field GuideDocument298 pagesDHS Austere EMS Field GuideRicardo Luis Martin Sant'Anna100% (2)
- Infectious DiseasesDocument356 pagesInfectious DiseasesNormala Macabuntal SaripadaNo ratings yet
- Medical Science IDocument80 pagesMedical Science I常靓No ratings yet
- Screening For Aspiration Risk Associated With Dysphagia in Acute StrokeDocument105 pagesScreening For Aspiration Risk Associated With Dysphagia in Acute StrokealexandraNo ratings yet
- S16427e PDFDocument356 pagesS16427e PDFhuda ifandaNo ratings yet
- Macrolídeo e Ação ImunomoduladoraDocument30 pagesMacrolídeo e Ação ImunomoduladorajanainaNo ratings yet
- MMS Internal Medicine Treatment & ProtocolsDocument248 pagesMMS Internal Medicine Treatment & ProtocolsVeselin PapazovNo ratings yet
- Murillo de Oliveira Antunes 2020Document15 pagesMurillo de Oliveira Antunes 2020Asisten Lab TLPNo ratings yet
- Chronic PainDocument237 pagesChronic PainLeigh SalesNo ratings yet
- Epidemiology Lecture NoteDocument118 pagesEpidemiology Lecture Notepushpa devkotaNo ratings yet
- Classical Osteopathy PDFDocument400 pagesClassical Osteopathy PDFAnonymous yvlCvHw100% (6)
- 5 A4 Critical Care and Hospitalist Medicine Made Ridiculously SimpleDocument390 pages5 A4 Critical Care and Hospitalist Medicine Made Ridiculously Simpleepic sound everNo ratings yet
- Venous Thrombosis Guidelines 2021 1Document74 pagesVenous Thrombosis Guidelines 2021 1Mendoza Calderon DiegoNo ratings yet
- GOLD 2023 Ver 1.3 17feb2023 - WMV (008 008)Document1 pageGOLD 2023 Ver 1.3 17feb2023 - WMV (008 008)dian handayaniNo ratings yet
- Asthama in ElderlyDocument72 pagesAsthama in ElderlyboyzonerajNo ratings yet
- Guia Esvs Manejo Evc 2015Document60 pagesGuia Esvs Manejo Evc 2015Steeven Ruilova Valle100% (1)
- (DERMA) 01 Introduction To Dermatology (History and PE)Document8 pages(DERMA) 01 Introduction To Dermatology (History and PE)Jolaine ValloNo ratings yet
- ESC Guidance COVID 19 PandemicDocument119 pagesESC Guidance COVID 19 PandemicReka DrincalNo ratings yet
- 2018 SAM Protocol EnglishDocument166 pages2018 SAM Protocol EnglishMurtaza HamdardNo ratings yet
- Carotid ESVS 2018Document79 pagesCarotid ESVS 2018Ahmed ElmallahNo ratings yet
- FA ManualDocument346 pagesFA ManualbabudevanandNo ratings yet
- 051-Anaesthesia, Pharmacology, Intensive Care and Emergency a.P.I.C.E. - 23rd Annual Meeting-AntoDocument396 pages051-Anaesthesia, Pharmacology, Intensive Care and Emergency a.P.I.C.E. - 23rd Annual Meeting-AntoDita Retno Wulandari100% (1)
- Final Thesis. CWs - En.de - De.fr - Fr.enDocument81 pagesFinal Thesis. CWs - En.de - De.fr - Fr.enBeera InstituteNo ratings yet
- 1 Aa Tesis Aravena Roman Maximiliano 2015Document339 pages1 Aa Tesis Aravena Roman Maximiliano 2015iqyuwidya100% (1)
- Si 67-02 KP 238 Tahun 2018 Manual of Civil Aviation Medicine 1Document300 pagesSi 67-02 KP 238 Tahun 2018 Manual of Civil Aviation Medicine 1tan.mongieNo ratings yet
- 2014 Mrcs Osce RECALLDocument85 pages2014 Mrcs Osce RECALLIdo EgaziNo ratings yet
- ECG Measurements and Interpretation Programs: Physician's GuideDocument52 pagesECG Measurements and Interpretation Programs: Physician's GuideAnand M SNo ratings yet
- Training Guide To Trainers: Training Manual On Training of CahwsDocument69 pagesTraining Guide To Trainers: Training Manual On Training of CahwsDvm Abdi BuraaleNo ratings yet
- AHA ACC Test Ergo Met RicoDocument56 pagesAHA ACC Test Ergo Met RicoValentina VaccaroNo ratings yet
- History of MedicineDocument108 pagesHistory of MedicineAlexandra Constantin100% (2)
- Ingles 4 Tesis Abayomi SorinolaDocument154 pagesIngles 4 Tesis Abayomi SorinolaThe Almighty BelugaNo ratings yet
- CD 004929Document41 pagesCD 004929DylanNo ratings yet
- Cumulative Trauma Disorder (CTD) Medical Treatment GuidelinesDocument43 pagesCumulative Trauma Disorder (CTD) Medical Treatment GuidelinesAarthi ArumugamNo ratings yet
- Geophysical Methods To Detect Stress in Underground Mines: Report of Investigations/2004Document23 pagesGeophysical Methods To Detect Stress in Underground Mines: Report of Investigations/2004wypoNo ratings yet
- LabmanDocument754 pagesLabmanpsalminaNo ratings yet
- Flee Nor 2015Document67 pagesFlee Nor 2015Cosmin AndreiNo ratings yet
- Cardiovascular ImagingDocument401 pagesCardiovascular ImagingRani Mulia100% (5)
- Daftar IsiDocument1 pageDaftar IsiHiz AnNo ratings yet
- Borderline Manual Ol enDocument72 pagesBorderline Manual Ol enbasakerpolatNo ratings yet
- Lung CancerDocument31 pagesLung CancerFarhat KhanNo ratings yet
- 2023 CPG On The Management of Atherosclerotic Carotid and Vertebral Artery DiseaseDocument105 pages2023 CPG On The Management of Atherosclerotic Carotid and Vertebral Artery DiseaseElisa NovaesNo ratings yet
- Virulence: Factors in Escherichia Coli Urinary Tract InfectionDocument49 pagesVirulence: Factors in Escherichia Coli Urinary Tract InfectionD Wisam NajmNo ratings yet
- Finalversion 091105 RFDocument135 pagesFinalversion 091105 RFAbdulai FofanaNo ratings yet
- CDC 52472 DS1Document164 pagesCDC 52472 DS1Lorens LaubanNo ratings yet
- Saggital Module Skull BaseDocument84 pagesSaggital Module Skull BaseAnoop SinghNo ratings yet
- Timothy Report AttachmentDocument25 pagesTimothy Report AttachmentFrancis OtienoNo ratings yet
- On-X® Mitral Heart ValveDocument20 pagesOn-X® Mitral Heart ValveChaitanya Sai TNo ratings yet
- Labour LawDocument135 pagesLabour LawSathish ChokkalingamNo ratings yet
- Handbook of Dental Hygienist (PDFDrive)Document523 pagesHandbook of Dental Hygienist (PDFDrive)neetika guptaNo ratings yet
- (02.05) CM Cardiovascular Nutrition (TG13) - FINAL - Andrea Maxine CajucomDocument14 pages(02.05) CM Cardiovascular Nutrition (TG13) - FINAL - Andrea Maxine CajucomMikmik DGNo ratings yet
- (02.29) Pediatric Cardiac Catheterization (TG16) - Noelle Jiyana SingsonDocument9 pages(02.29) Pediatric Cardiac Catheterization (TG16) - Noelle Jiyana SingsonMikmik DGNo ratings yet
- (02.02) CM Diagnosis of Cardiovascular Disease (TG10) - Jonaz NazarenoDocument15 pages(02.02) CM Diagnosis of Cardiovascular Disease (TG10) - Jonaz NazarenoMikmik DGNo ratings yet
- (02.28) PD Cyanotic Congenital Heart Diseases (Tg15) Final - Matthew Ethan AngDocument13 pages(02.28) PD Cyanotic Congenital Heart Diseases (Tg15) Final - Matthew Ethan AngMikmik DGNo ratings yet
- (02.18) SU Surgical Diseases of The Pericardium - Neil Andrew AliazasDocument8 pages(02.18) SU Surgical Diseases of The Pericardium - Neil Andrew AliazasMikmik DGNo ratings yet
- (02.09) CM Ventricular Tachyarrhythmias (TG17) - Rene Martin ElefanteDocument10 pages(02.09) CM Ventricular Tachyarrhythmias (TG17) - Rene Martin ElefanteMikmik DGNo ratings yet
- (02.23) CM Peripheral Arterial Occlusive Disease (Tg9) - Final - Navin John Pasia - Navin John PasiaDocument19 pages(02.23) CM Peripheral Arterial Occlusive Disease (Tg9) - Final - Navin John Pasia - Navin John PasiaMikmik DGNo ratings yet
- (02.22b) CM Diseases of The Aorta 2 (TG8) - Morvenn Chaimek C. BertizDocument5 pages(02.22b) CM Diseases of The Aorta 2 (TG8) - Morvenn Chaimek C. BertizMikmik DGNo ratings yet
- (02.21b) Im Congestive Heart Failure 2 (Tg6) - Arielle Dana YaoDocument7 pages(02.21b) Im Congestive Heart Failure 2 (Tg6) - Arielle Dana YaoMikmik DGNo ratings yet
- (02.31) PA Introduction and Physiology of Pain (TG18) Final - Martin DionesDocument13 pages(02.31) PA Introduction and Physiology of Pain (TG18) Final - Martin DionesMikmik DGNo ratings yet
- (02.27) PD Acyanotic Congenital Heart Disease (Tg14) - Final - Janel Zahra RasulDocument8 pages(02.27) PD Acyanotic Congenital Heart Disease (Tg14) - Final - Janel Zahra RasulMikmik DGNo ratings yet
- (02.21a) CM Congestive Heart Failure 1 (TG 5) - Ervin Kyle CerezoDocument9 pages(02.21a) CM Congestive Heart Failure 1 (TG 5) - Ervin Kyle CerezoMikmik DGNo ratings yet
- (02.20) CM Cardiomyopathy and Myocarditis (TG4) - ANA CARMINA LIBERATODocument12 pages(02.20) CM Cardiomyopathy and Myocarditis (TG4) - ANA CARMINA LIBERATOMikmik DGNo ratings yet
- (02.22a) CM Diseases of The Aorta 1 (TG7) - Jose Gabriel OrdinalDocument13 pages(02.22a) CM Diseases of The Aorta 1 (TG7) - Jose Gabriel OrdinalMikmik DGNo ratings yet
- (02.14) SU Surgical Management of Valvular Heart Disease (TG 22) - Joseph Paul RiveraDocument15 pages(02.14) SU Surgical Management of Valvular Heart Disease (TG 22) - Joseph Paul RiveraMikmik DGNo ratings yet
- (02.30) SU Surgical Management of Congenital Heart Diseases (TG17) - Rene Martin ElefanteDocument12 pages(02.30) SU Surgical Management of Congenital Heart Diseases (TG17) - Rene Martin ElefanteMikmik DGNo ratings yet
- (02.16) PC SGD Anti-Hypertensives (TG24) - MA. GLORIA SALAPANTANDocument7 pages(02.16) PC SGD Anti-Hypertensives (TG24) - MA. GLORIA SALAPANTANMikmik DGNo ratings yet
- (02.03) RD Cardiovascular Radiology (TG11 - John Edward BallelosDocument22 pages(02.03) RD Cardiovascular Radiology (TG11 - John Edward BallelosMikmik DGNo ratings yet
- (06.08) Quantitative Study Designs Observational Studies (TG18-CG6) - FINAL - Martin DionesDocument11 pages(06.08) Quantitative Study Designs Observational Studies (TG18-CG6) - FINAL - Martin DionesMikmik DGNo ratings yet
- (02.07) CM Bradycardias (Tg15) - Matthew Ethan AngDocument10 pages(02.07) CM Bradycardias (Tg15) - Matthew Ethan AngMikmik DGNo ratings yet
- 01.25.01 Principles of Pharmacokinetics - Absorption and DistributionDocument10 pages01.25.01 Principles of Pharmacokinetics - Absorption and DistributionMikmik DGNo ratings yet
- (06.05) Data Privacy Act and Its Implication To Research (TG15-CG3) - Final - MATTHEW ETHAN ANGDocument7 pages(06.05) Data Privacy Act and Its Implication To Research (TG15-CG3) - Final - MATTHEW ETHAN ANGMikmik DGNo ratings yet
- (06.01) Introduction To Statistics and Statistical Inference (TG11-CG23) - Final - Deanna Flor LimDocument11 pages(06.01) Introduction To Statistics and Statistical Inference (TG11-CG23) - Final - Deanna Flor LimMikmik DGNo ratings yet
- 01.20.01 Pharmacodynamics 2 - Mechanisms of Drug ActionDocument11 pages01.20.01 Pharmacodynamics 2 - Mechanisms of Drug ActionMikmik DGNo ratings yet
- 01.24.01 SIM On Mechanisms of Drug ActionDocument13 pages01.24.01 SIM On Mechanisms of Drug ActionMikmik DGNo ratings yet
- (06.07) Principles of Validity and Reliability (TG17-CG5) FINAL - SHEREE BIANNE-THA NOLEEN MENDEZDocument6 pages(06.07) Principles of Validity and Reliability (TG17-CG5) FINAL - SHEREE BIANNE-THA NOLEEN MENDEZMikmik DGNo ratings yet
- 01.22.01 General Overview To RadiologyDocument11 pages01.22.01 General Overview To RadiologyMikmik DGNo ratings yet
- (06.12) Data Management and Analysis (TG22-CG10) - Final - Mikaela Kate RamirezDocument15 pages(06.12) Data Management and Analysis (TG22-CG10) - Final - Mikaela Kate RamirezMikmik DGNo ratings yet
- FinMan - Dionisio - DavidEmmanuel - Midterm PaperDocument2 pagesFinMan - Dionisio - DavidEmmanuel - Midterm PaperMikmik DGNo ratings yet
- 01.19.01 General Concepts in Parasitology 1-4Document7 pages01.19.01 General Concepts in Parasitology 1-4Mikmik DGNo ratings yet
- Heart and Circulation ExercisesDocument3 pagesHeart and Circulation ExercisesHanaOmarNo ratings yet
- Ninja NerdDocument3 pagesNinja NerdSalsabila HMNo ratings yet
- Preoperative Cardiac Risk Assessment in Noncardiac SurgeryDocument6 pagesPreoperative Cardiac Risk Assessment in Noncardiac SurgeryOgbonnaya IfeanyichukwuNo ratings yet
- Chapter 2 - Clinical Cardiovascular Examination-2Document43 pagesChapter 2 - Clinical Cardiovascular Examination-2sarahya.medinaNo ratings yet
- Abdominal Aortic Aneurysm 2Document22 pagesAbdominal Aortic Aneurysm 2Kendy Rizky HadyanNo ratings yet
- Lecture On Hemodynamic and Thromboembolic DisordersDocument77 pagesLecture On Hemodynamic and Thromboembolic DisordersCharmaine Torio PastorNo ratings yet
- Reversible Cerebral Vasoconstriction SyndromeDocument6 pagesReversible Cerebral Vasoconstriction SyndromeKashifNo ratings yet
- Peripheral Arterial DiseaseDocument40 pagesPeripheral Arterial Diseaseuseofforcelaw100% (1)
- (UMA) ERBA XL-640 Basic Performance DataDocument38 pages(UMA) ERBA XL-640 Basic Performance DataKo KyoNo ratings yet
- Lippincott Antiarrhythmics 7Document2 pagesLippincott Antiarrhythmics 7Wijdan HatemNo ratings yet
- Manajemen Perioperatif Pada Hipertensi WORDDocument16 pagesManajemen Perioperatif Pada Hipertensi WORDIan MatatulaNo ratings yet
- Myocardial Infarction. BPTDocument62 pagesMyocardial Infarction. BPTAanchal GuptaNo ratings yet
- Myocardial Infarction Midterm Case StudyDocument24 pagesMyocardial Infarction Midterm Case StudyReizel GaasNo ratings yet
- Pengetahuan, Sikap, Dan Perilaku Terhadap Pencegahan Serta Penanggulangan Hipertensi Di Kabupaten BogorDocument9 pagesPengetahuan, Sikap, Dan Perilaku Terhadap Pencegahan Serta Penanggulangan Hipertensi Di Kabupaten BogorIntan OktavianiNo ratings yet
- Heart AttackDocument18 pagesHeart AttackKhalifullahNo ratings yet
- 01 Critical Care IV Drug Infusions - AdultDocument33 pages01 Critical Care IV Drug Infusions - Adultdoc_gelo100% (1)
- NSG 6001 Final Exam 1 - Question and AnswersDocument49 pagesNSG 6001 Final Exam 1 - Question and AnswersDAVIDNo ratings yet
- Health Talk On HypertensionDocument8 pagesHealth Talk On HypertensionSHUBHENDU SHANDILYANo ratings yet
- Workbook - A Guide To The Vascular SystemDocument202 pagesWorkbook - A Guide To The Vascular SystemDenis PogoreviciNo ratings yet
- Uptodates1748681521000243 Pdfdownload True PDFDocument17 pagesUptodates1748681521000243 Pdfdownload True PDFAhmad AshammeryNo ratings yet
- Graphic OrganizerDocument1 pageGraphic OrganizerKenshin MedinaNo ratings yet
- Pathology of Blood VesselsDocument80 pagesPathology of Blood VesselsiqiqiqiqiqNo ratings yet
- Labelling The Human HeartDocument6 pagesLabelling The Human Heartchinpy088464No ratings yet
- CIRCULATORYDocument20 pagesCIRCULATORYDannica Trisha CrisostomoNo ratings yet
- Programbook IsicamDocument36 pagesProgrambook Isicamadi bestaraNo ratings yet
- Nihms 1931223Document17 pagesNihms 1931223reymistery10No ratings yet
- Heart PDFDocument48 pagesHeart PDFdr.chetan2385No ratings yet
- Bio Lab 11Document5 pagesBio Lab 11Sarah JaglalNo ratings yet
(02.12) CM Valvular Heart Diseases (TG20) - Anne Gabrielle Liu
(02.12) CM Valvular Heart Diseases (TG20) - Anne Gabrielle Liu
Uploaded by
Mikmik DGOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
(02.12) CM Valvular Heart Diseases (TG20) - Anne Gabrielle Liu
(02.12) CM Valvular Heart Diseases (TG20) - Anne Gabrielle Liu
Uploaded by
Mikmik DGCopyright:
Available Formats
MODULE 02: CARDIOLOGY
Valvular Heart Diseases
ADRIEL E. GUERRERO, MD, FPCP, FPCC
09/03/2021
CLINICAL MEDICINE
TABLE OF CONTENTS I. INTRODUCTION
A. REVIEW OF HEART SOUNDS
I. INTRODUCTION..........................................................................................................1
A. REVIEW OF HEART SOUNDS ...............................................................................1
B. MURMURS ..........................................................................................................2
[VIDEO] REVIEW OF HEART SOUNDS
C. SYSTOLIC MURMURS ..........................................................................................2
D. DIASTOLIC MURMURS ........................................................................................2
II. AORTIC STENOSIS (AS) ..............................................................................................3
A. CAUSE AND PATHOLOGY ....................................................................................3
B. PATHOPHYSIOLOGY ............................................................................................3
C. CLINICAL PRESENTATION ....................................................................................4
D. PHYSICAL EXAMINATION ....................................................................................4
E. AUDIO DEMO ......................................................................................................4
F. LABORATORY EXAMINATION ..............................................................................4
G. DIFFERENTIAL DIAGNOSES .................................................................................5
H. MEDICAL TREATMENT ........................................................................................5
I. SURGICAL TREATMENT ........................................................................................5
III. AORTIC REGURGITATION (AR) .................................................................................6
A. CAUSE AND PATHOLOGY ....................................................................................6
B. PATHOPHYSIOLOGY ............................................................................................6 • NOTE: Please scan this QR code to hear the review of the heart sounds
C. CLINICAL PRESENTATION ....................................................................................6 • When a healthy heart beats, it makes a lub dub sound
D. PHYSICAL EXAMINATION ....................................................................................7 • S1
E. LABORATORY EXAMINATION ..............................................................................7 o The first heart sound, “lub”
F. DIFFERENTIAL DIAGNOSIS ...................................................................................7 o Caused by the closing of the atrioventricular (AV1) valves after the
G. MEDICAL TREATMENT ........................................................................................7
atria have pumped blood into the ventricles
H. SURGICAL TREATMENT ......................................................................................7
IV. MITRAL STENOSIS (MS) ...........................................................................................8 • S2
A. INTRODUCTION ..................................................................................................8 o The second heart sound, “dub”
B. RHEUMATIC FEVER .............................................................................................8 o Originates from the closing of the aortic and pulmonary valves, right
C. PATHOPHYSIOLOGY AND SYMPTOMATOLOGY ..................................................9 after the ventricles have ejected the blood
D. DIAGNOSTIC FEATURES ......................................................................................9 • Systole: the time interval between S1 and S2 when the ventricles
E. CONSEQUENCES OF UNTREATED MITRAL STENOSIS ........................................10
contract
F. DIFFERENTIAL DIAGNOSIS OF MITRAL STENOSIS..............................................10
TREATMENT ..........................................................................................................10 • Diastole: the time interval between S2 and the next S1 when the
V. MITRAL REGURGITATION (MR)...............................................................................12 ventricles relax and are filled with blood
A. COMMON ETIOLOGIES OF MITRAL REGURGITATION ......................................12 o Longer than systole
B. DIFFERENTIAL DIAGNOSIS OF MITRAL REGURGITATION ..................................12
C. SYMPTOMATOLOGY OF MITRAL REGURGITATION ..........................................12
D. LABORATORY EXAMINATIONS .........................................................................13
[VIDEO] REVIEW OF HEART SOUNDS – continuation
E. TREATMENT ......................................................................................................13
VI. MITRAL VALVE PROLAPSE......................................................................................13
A. OVERVIEW ........................................................................................................13
B. LABORATORY EXAMINATIONS..........................................................................14
C. TREATMENT ......................................................................................................14
VII. TRICUSPID STENOSIS (TS) .....................................................................................14
A. HISTORY ............................................................................................................14
B. PHYSICAL FINDINGS ..........................................................................................14
C. LABORATORY FINDINGS ...................................................................................14
D. TREATMENT .....................................................................................................14
VIII. TRICUSPID REGURGITATION (TR) ........................................................................14
A. CAUSES .............................................................................................................14
B. MECHANISMS ...................................................................................................14
C. TREATMENT CONSIDERATIONS ........................................................................14
IX. PULMONIC VALVE DISEASE ....................................................................................15
QUICK REVIEW ............................................................................................................15
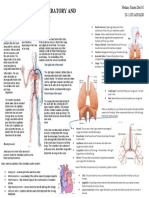
SUMMARY OF CONCEPTS .....................................................................................15 Figure 1. Heart sounds auscultation sites
SUMMARY OF NEED-TO-KNOWS (NDTK) .............................................................17
SUMMARY OF PROCESSES ....................................................................................17 • Heart sounds are auscultated at 4 different sites on the chest wall, which
SUMMARY OF MEMORY AIDS ..............................................................................17 correspond to the location of blood flow as it passes through the:
SUMMARY OF EQUATIONS ...................................................................................17
o Aortic area in the right 2nd intercostal space
REVIEW QUESTIONS .............................................................................................17
REFERENCES................................................................................................................18 o Pulmonic area in the left 2nd intercostal space
REQUIRED .............................................................................................................18 o Tricuspid area in the left 4th intercostal space
SUPPLEMENTARY..................................................................................................18 o Mitral area at the apex or the left 5th intercostal space
FREEDOM SPACE.........................................................................................................18 (midclavicular)
• This is how similar defects associated with different valves are
differentiated
The left atrium (LA1) is normal
1 AV: Atrioventricular
YL7: 02.12 Transcribed by TG 20: Dee, Garrido, Liu, Molen, Punzalan 1 of 18
B. MURMURS Pulmonic Stenosis
[VIDEO] HEART MURMURS [VIDEO] PULMONIC VALVE STENOSIS
• NOTE: Sample audio at 2:13 of the video linked in the QR code • Same characteristics as the aortic valve stenosis, however, is best heard
• Whooshing sounds produced by turbulent blood flow at the pulmonic area
• Diagnosed based on: o Does not radiate to the neck
o Time they occur in the cardiac cycle
§ Systolic or diastolic
o Shape: Their changes in intensity over time Ventricular Septal Defect (VSD2) and Mitral Valve Prolapse (MVP3)
o Location: Auscultation site where they are best heard 2 Ventricular Septal Defect: Holosystolic murmur over the 3rd intercostal
§ Aortic, pulmonic, tricuspid, or mitral areas space, left parasternal border (Erb’s point)
2 Mitral Valve Prolapse: Early to mid-type of systolic murmur
2 Best heard over the apex or mitral area
C. SYSTOLIC MURMURS
D. DIASTOLIC MURMURS
[VIDEO] SYSTOLIC MURMURS
• Examples of conditions associated with common systolic murmurs [VIDEO] DIASTOLIC MURMURS
include: • Examples of conditions associated with diastolic murmurs include:
o Mitral valve regurgitation o Aortic valve regurgitation
o Tricuspid valve regurgitation o Pulmonic valve regurgitation
o Aortic stenosis o Mitral stenosis
o Pulmonic stenosis o Tricuspid stenosis
Mitral Valve Regurgitation Aortic Valve Regurgitation
LA4
[VIDEO] MITRAL VALVE REGURGITATION [VIDEO] AORTIC VALVE REGURGITATION
• NOTE: sample audio at 2:50 of the video linked in the QR code • NOTE: sample audio at 4:52 of the video linked in the QR code
• Occurs when the mitral valves does not close properly and blood surges • Occurs when the aortic valve doesn’t close properly, resulting to blood
back to the left atrium during systole flowing back to the left ventricle (LV4) during diastole (or the filling
• The murmur starts at S1 when the AV valves close phase)
o Maintains the same intensity through the entire duration of systole • Best heard along the left sternal border
• Best heard at the mitral region, the apex • Peaks at the beginning of diastole, when pressure differences are
o Radiates to the left axilla highest
• Then rapidly decreases when the equilibrium is reached
Tricuspid Regurgitation
Pulmonic Regurgitation
[VIDEO] TRICUSPID VALVE REGURGITATION : Occurs when the pulmonic valve is incompetent which results in the
abnormal reversal of blood flow from the pulmonary artery into the right
• Has similar timing and shape with mitral valve regurgitation, but occurs
ventricle
on the other side of the heart
2 Most common acquired abnormality of the pulmonic valve, secondary to
• Loudest in the tricuspid area
the dilation of the pulmonary valve ring as a consequence of pulmonary
o Radiates up along the left sternal border
hypertension
Aortic Valve Stenosis Mitral Stenosis
2 Inability of the mitral valve to open during diastole due to obstruction in
left ventricular inflow
[VIDEO] AORTIC VALVE STENOSIS
• NOTE: sample audio at 3:50 of the video linked in the QR code
Tricuspid Stenosis
• Occurs when the aortic valve does not open properly and blood is forced
through a narrow opening 2 Have the same diastolic murmur as mitral stenosis but on the right side
• Crescendo-decrescendo or diamond shaped murmur
o Formed due to: TIP: Three important things to remember whenever you do cardiac
§ The blood flow starting small auscultation:
§ Then rising to a maximum mid-systole at the peak of ventricular • Determine the timing whether it is systolic or diastolic
contraction • Determine the changes in intensity of the murmur
§ Then attenuating towards the end of systole o If it’s diamond shaped or holosystolic
o Starts a short moment after S1 • Determine the location you would hear the murmur best
o Often preceded by an ejection click caused by the opening of the
stenotic valve
• Loudest in the aortic area ACTIVE RECALL
o Radiates to the carotid arteries in the neck Which among the following is not a diastolic murmur?
§ Following the direction of blood flow a) Aortic Valve Regurgitation
b) Aortic Stenosis
c) Mitral Stenosis
d) Tricuspid Stenosis
T/F. The diagnosis of murmurs is based on time, shape, and location.
ANSWERS: 1B, 2T
2 VSD: Ventricular Septal Defect 4 LV: Left Ventricle
3 MVP: Mitral Valve Prolapse
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 2 of 18
II. AORTIC STENOSIS (AS5) B. PATHOPHYSIOLOGY
• Left-sided valvular pathologies, particularly those involving the aortic and
mitral valves, seem to be more important clinically than those of the right-
sided valves
o In terms of hemodynamic changes, they greatly influence the natural
history or management of these diseases
• A systolic murmur
A. CAUSE AND PATHOLOGY
• Has 3 principal causes:
o Congenital bicuspid valve with superimposed calcification
§ If it’s congenital, the most common valvular pathology that reaches
to adulthood involves the bicuspid valve
o Calcification of a normal trileaflet valve
Figure 3. (Left) Normal LV with a normal cardiac output and normal aortic
§ Occurs more commonly in degenerative diseases (particularly aortic
valve, (Right) Aortic Stenosis
stenosis and aortic sclerosis)
o Rheumatic diseases • Figure 3:
o Left: Normal LV with a normal cardiac output and normal aortic valve
NOTE: Doc emphasizes that these pathologies are in relation to adult § In systole, a LV pressure of 120/10 produces an output of 120/80
cardiology as there will be a separate lecture on pediatric cardiology. Þ Produces the same systolic pressure
§ Diastolic pressure is generated upon closure of the aortic valve
§ The left atrium (LA6) is normal
Þ Has a pressure of 10 which is also normal
o Right: Aortic Stenosis
§ Due to the difficulty of opening the aortic valve, the LV has to go
under hypertrophy for it to generate a higher pressure to push
blood forward past the aortic stenosis
Þ This only produces an output of 110/75
Þ There is a difference of 90 mmHg in pressure between the LV
systolic pressure and the aortic output
Þ The pressure in LV, which is now high, will cause the LA pressure
to increase as well
- Most of the time, this causes LA enlargement as a
consequence
Figure 2. Major types of aortic valve stenosis. (A) Normal aortic valve, (B)
Congenital bicuspid aortic stenosis with a false raphe present at 6 o’clock, (C)
Rheumatic aortic stenosis with its commissures fused with a fixed central
orifice, and (D) Calcific degenerative aortic stenosis
• Figure 2:
o A: Normal trileaflet aortic valve
§ A cusp rather than a true leaflet with chordae and papillary muscles
§ Aortic and pulmonic valves are cuspids
o B: Congenital bicuspid aortic stenosis with a false raphe present at 6
o’clock
§ Looks like a fish mouth
§ Looks bicuspid
§ Has an anterior and posterior leaflet due to the failure of separation
the medial raphe
Þ This was supposed to be an aortic tricuspid valve
Þ Further restricts the opening of that valve
o C: Rheumatic aortic stenosis with its commissures fused with a fixed
central orifice and D: Calcific degenerative aortic stenosis
§ Both will cause narrowing of the aortic valves as well
§ C is a pathologic feature of patients with rheumatic heart disease Figure 4. Aortic Stenosis Hemodynamic Changes
§ Whereas in D, it is more of a degenerative type • Figure 4:
§ Distinguishing between the two: 1) All hemodynamic changes in aortic stenosis are related to left
Þ In rheumatic disease: inflammation, which extensively involves ventricular outflow obstruction
the commissures, causes their fusion which then results into the 2) LV outflow obstruction causes 4 differences in terms of pressure:
narrowing of the orifice § Elevation of LV systolic pressure
Þ In degenerative types: calcification starts at the base of the cusp, Þ Therefore, it takes time for blood to be injected out
producing restriction § This increases left ventricular ejection time (LEVT7)
- Commissures are not fused, but are thickened and calcified § Elevation of LV diastolic pressure
• The differences in pathologies are important in terms of etiology in the § Aortic pressure decreases
diagnosis of the cause of aortic stenosis Þ Aortic pressure: the pressure beyond the aortic stenosis
3) All of those will lead to:
§ Hypertrophy
§ Dysfunction
§ Increased myocardial oxygen consumption
§ Decreased diastolic time
5 AS: Aortic Stenosis 7 LEVT: Left Ventricular Ejection Time
6 LA: Left Atrium
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 3 of 18
4) This all then subsequently leads to a disproportion in supply and o Expected finding for patients with severe AS:
demand of myocardial oxygen consumption § Pulsus parvus et tardus carotid impulse: slow-rising, late-peaking,
5) Then may eventually end in LV failure low-amplitude carotid pulse
C. CLINICAL PRESENTATION E. AUDIO DEMO
• Patients demonstrate 4 important principal clinical manifestations:
o Exertional dyspnea
[VIDEO] AORTIC STENOSIS
§ Represent patients with decreased oxygen demand and decreased
cardiac output
o Angina
o Syncope
o Heart failure
[MEMORY AID] CLINICAL PRESENTATION OF AORTIC STENOSIS: ASH
• Angina
• Syncope
• Heart failure
• To listen to the audio demo for aortic stenosis provided in the lecture
video, please scan this QR code. You may also opt to open this in Valvular
Heart Disease Guerrero Part 1 of 2 at 19:35! J
• Notes on the video:
o Best heard along the right sternal boarder in the 2nd intercoastal
space
o Described as a crescendo-decrescendo systolic ejection murmur
o The murmur classically radiates to the carotids
o Common causes include calcified and bicuspid aortic valves
o S2 is often diminished
§ In severe AS, it may be absent
Figure 5. Aortic Stenosis Latent Period
F. LABORATORY EXAMINATION
• Figure 5: • These laboratory exams could be a verification of pathophysiologic
o In aortic stenosis, there is a very long latent period from the time it changes related to AS
starts to happen • Classic change: LV hypertrophy is the key finding
§ Example: In rheumatic or degenerative diseases, despite the
o Can be demonstrated by:
increasing obstruction or narrowing of the aortic valve and the
§ Electrocardiogram (ECG8)
consequent overload of the myocardium, there is a latent period
§ 2D Echo: estimates valve area, LV size, and LV function
wherein patients are not symptomatic for so many years
• If patients have a cardiac catheterization, the following must be
o For about 20 to 40 years, patients are asymptomatic
documented:
o However, based on the graph, once patients develop these symptoms
o The differential pressure from the LV to the aorta
(ASH), patients consequently deteriorate rapidly
§ If you’re planning an operation, also document the presence or
o Subsequently, survival also decreases:
absence of concomitant coronary artery disease (CAD9)
§ Presentation of heart failure has an average survival of 2 years
§ Presentation of syncope has an average survival of about 3 years
§ Presentation of angina has an average survival of about 5 years Radiograph Findings
o Understanding and memorizing this graph is crucial to recognize if
patients need an intervention
NDTK: The onset of symptoms for AS is very important to recognize because
patients deteriorate so rapidly once they develop.
ACTIVE RECALL
T/F. Right-sided valve pathologies seem to be more important clinically
than left-sided valve pathologies.
Among the following, which hemodynamic change is NOT among the
changes that occur in AS?
a) Increased diastolic time
b) Elevation of LV systolic pressure
c) Elevation of LV diastolic pressure
d) Decrease in aortic pressure
e) AOTA
Figure 6. X-ray presentation of aortic stenosis
ANSWERS: 3F, 4A
• Figure 6:
o There is a cardiac silhouette resembling a LV hypertrophy
D. PHYSICAL EXAMINATION o The apex is displaced laterally and downward
• Palpation of carotid upstroke o The outlet of the LV, which is the aorta, is displaying tortuosity, bulging,
o For the: and showing stiffness
§ Evaluation of the systolic murmur as a result of a radiating AS
§ Examination for signs of heart failure
o The normal carotid pulse is a rapid upstroke and gradual downstroke
8 ECG: Electrocardiogram 9 CAD: Coronary Artery Disease
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 4 of 18
ECG Findings Pharmacologic Therapies
• Diuretics and digitalis in congestive heart failure
o Caution must be exercised since patients already have a low cardiac
output due to a fixed obstruction.
§ Recall: Computation formula for Cardiac output (see Equation 1)
§ The formula does not work in this case due to an obstruction
§ No matter how much the patient increases their HR, this will not
increase cardiac output.
o Administering diuretics can induce hypotension
o The use of digoxin must also be cautioned because it increases
myocardial oxygen demand, resulting in more angina.
• Nitroglycerin can help to relieve angina
o Can also decrease blood pressure like the previously mentioned drugs.
• Statins (HMG CoA reductase inhibitors) can help to slow down progression
of calcification, but this involves a long process
Figure 7. ECG exhibiting AS findings • No effect on long term survival
• ECG changes will reflect the electrical changes related to hypertrophy 𝐶𝑂 = 𝑆𝑉 𝑥 𝐻𝑅
• Classically presents with tall R waves over the left sided leads, V5 and V6
o V5 and V6 strained pattern or T-wave inversions related to the decrease Equation 1. Cardiac output
or disproportion in oxygen supply and demand, which in turn, is related • Where:
to hypertrophy o CO = Cardiac output
o SV = Stroke volume
G. DIFFERENTIAL DIAGNOSES o HR = Heart rate
• Differential diagnosis of AS can be centered into:
o Hemodynamic changes in AS I. SURGICAL TREATMENT
§ If you have angina, you have to rule out acute coronary syndrome • Recall: The main method of treatment for aortic stenosis is surgery
(ACS10) • Indications for Surgery:
o Blood pressure of the patient will be relative low considering the o Severe Aortic Stenosis (<0.6 cm2/m2) even if asymptomatic
inability of the aortic valve to open o Symptomatic with left ventricular dysfunction (LV Ejection fraction of
§ Hence, the need to rule out hypovolemic shock < 50)
o Timing of the murmur o Expanding post-stenotic aortic root (even if asymptomatic) which
§ Hence, consideration of mitral regurgitation and mitral valve dilates due to pressure differences
prolapse o Those who undergo coronary artery bypass grafting (CABG) even if
Þ Obviously, these are best heard at the mitral area on the apex asymptomatic
Þ The murmur of aortic stenosis is located over the right 2nd o Consequent mitral stenosis
intercostal space • Operative risk of Aortic Valve Replacement in asymptomatic severe aortic
§ The location of the murmur will be important in these differentials stenosis is 4%
• In frank CHF (Chronic Heart Failure) – 15 to 20%
Table 1. Summary of Differential Diagnoses for AS o 4-5x increase in risk if you time the surgery when the patient is in heart
DIFFERENTIAL DIAGNOSIS REASON FOR CONSIDERATION failure
• Due to the hemodynamic changes in AS o 10-year survival rate of patients with aortic valve replacement is 60%
Acute Coronary Syndrome
• Angina § 30% biosynthesis fail in 10 years
The blood pressure of the patient will be § Mechanical prosthesis: hemorrhage fm anticoagulation
Hypovolemic Shock relatively low considering the inability of the • The selection on bioprosthesis or mechanical prosthesis (metal valve)
aortic valve to open depends on the timing of surgery
Mitral Regurgitation • Similar timing of the murmur o Patients who are >65 years old can have a bioprosthesis
• However, both of these are both heard o Younger patients can have a mechanical prosthesis
Mitral Valve Prolapse
better at the mitral area on the apex § Patients using mechanical prosthesis will require longer use of
anticoagulant drugs
H. MEDICAL TREATMENT
• Medical management does not influence or prolong the survival of Non-Surgical Treatment
patients
o Surgery is the preferred mode of treatment
§ Almost all patients with AS are recommended for surgery
o Should patients refuse consent to surgery, medical management can
still be done to tide over patients
Management of Severe Aortic Stenosis
NOTE: Severe AS is defined as an opening less than 0.5 cm2/m2.
• Avoid strenuous physical activities even if asymptomatic Figure 8. Percutaneous Transcatheter Placement of AV Prosthesis
o Angina is more prominent when physically straining oneself • Percutaneous Transcatheter Placement of AV Prosthesis
o Physical activities cause further reduction of blood pressure and o Uses a retroflex 2 catheter
differential changes in pressure o Inserted percutaneously into the aortic valve
• Dietary Changes: Sodium Restriction (to lessen heart failure o Highly specialized and highly precise method
symptomatology) § Dependent on the expertise of the transcatheter team to place the
transcatheter in the exact location of the aortic valve
§ Indications will probably be given by the interventional cardiologist
10ACS: Acute Coronary Syndrome
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 5 of 18
III. AORTIC REGURGITATION (AR11) § Leads to prolapsing and primary aortic regurgitation
A. CAUSE AND PATHOLOGY
• Aortic Regurgitation is a diastolic event Aortic Root Diseases
• Arises due to the failure of the aortic valves to close • Basic defect is dilatation of aortic root, causing a separation of the cusp
• Upon diastole, blood is dumped back into a supposed closed aortic valve o They will be improperly coarctated, causing aortic regurgitation
o Blood flows back from the aorta and back into the left ventricle o Age-related (degenerative) aortic dilation
o Due to insufficiency, volume now accumulates into the LV o Cystic medial necrosis of the aorta
o This causes a net increased pressure in the left ventricle in both acute § Isolated or associated with classic Marfan syndrome
and chronic aortic regurgitation • Aortic dilatation related to the following conditions:
o Bicuspid valves, aortic dissection
o Osteogenesis imperfecta
Symptomatology of Aortic Regurgitation
o Syphilitic aortitis
o Ankylosing spondylitis
o Behcet syndrome
o Psoriatic arthritis
o Arthritis with ulcerative colitis
o Relapsing polychondritis
o Reactive arthritis
o Giant cell arteritis
o Systemic hypertension
NOTE: Doc does not expound on the list of diseases relating to aortic root
dilatation.
B. PATHOPHYSIOLOGY
Figure 9. Comparison of Acute vs Chronic Aortic Regurgitation
Acute AR
• LV and LA are not prepared for the influx of blood and fails to expand
o LV is not prepared and is normal, therefore there is no time for the
heart to compensate
• As blood rushes back into the left ventricle, pressure increases since there’s
no change in size of these chambers (and there is no time for the heart to
compensate)
• Subsequently this causes an increase in pressure in the left atrium, which
can present as early pulmonary congestion
o Acute Aortic Regurgitation can lead to:
§ Pulmonary Congestion
§ Acute Heart Failure
§ Decreased Oxygenation
§ Death
Chronic AR Figure 10. Pathophysiology of Aortic Regurgitation
• The LV is able to dilate and subsequently compensate for the increase in
• Unlike AS (which involves changes in pressure), AR involves an increase in
pressure
volume
• There is an increase in the volume, which leads to the dilatation of both LV
o Blood backflows into the LV as compared to stenosis which is the
and LA increase in pressure since the blood cannot escape the LV
o Symptomatology would be on a longer basis
• Increased LV volume then causes and increase in LV mass in order to
maintain a normal pressure
Primary Valvular Causes • However, the increase in mass causes a disproportionate oxygen demand,
• Unlike aortic stenosis, there are many etiologies to consider such as: heart failure, dyspnea, and ultimately left ventricular failure
o Degenerative Causes • Increase in stroke volume will lead to a decrease in diastolic time
§ Degeneration leading to fibrous thickening of the cusps causing
improper closure are still the most common causes “Mahina yung puso” –Dr Guerrero
§ Manifests as improper closure of the aortic valves
C. CLINICAL PRESENTATION
o Infective Endocarditis
§ Can occur whether infective endocarditis is active or healed • Symptoms:
§ Due to vegetation of bacteria on the valves leading to perforation o Prominent heart failure
and loss of tissue o Exertional dyspnea
o Aortic Tears or Lacerations o Orthopnea
§ Tears proximal to the cusps of the valve (proximal aorta) can o Paroxysmal Nocturnal Dyspnea (PND12)
consequently involve injuries of the coronary artery leading to o Angina (disproportion of oxygen supply and demand)
hemorrhage and sudden death o Diaphoresis (poor cardiac output)
§ When you have a dissection root to the arch, they can involve the o Palpitations (tachycardia to compensate for the low cardiac output)
cusp which is the origin of coronary arteries
o Congenitally Bicuspid Valves
§ Causes inadequate opening (stenosis) and closing (regurgitation of
the valves)
o Rheumatic causes
11AR: Aortic Regurgitation 12PND: Paroxysmal Nocturnal Dyspnea
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 6 of 18
D. PHYSICAL EXAMINATION • Figure 11:
o Chronic AR presents with the following findings on the chest x-ray
• Aortic Regurgitation is best heard over the left parasternal border
§ Left ventricular hypertrophy
• One can also auscultate the murmur when the carotid is auscultated
§ Prominent outlet of aorta
o The upstroke of the carotid will reflect systolic timing
§ Wide mediastinum (caused by the dilatation of the aortic root)
Þ Recall: the mediastinum is wider in AR (contrary to AS where the
Table 2. Peripheral Signs of Aortic Regurgitation (In Decongested Patients)
mediastinum is narrow)
SIGN DESCRIPTION
o Acute AR presents with a normal sized heart and some degree of
Corrigan’s Pulse • Pulses with abrupt distention and quick
pulmonary vascular congestion (cloudy appearance in the lungs)
collapse
§ Recall: LV is normal and has no time to enlarge
o Rapid, strong upstroke with very brisk
Þ Hence, blood volume immediately enters the pulmonary
downstroke
circulation causing pulmonary congestion
• Water-hammer pulse
§ The CXR of acute AR shows a rare instance wherein congestion is
De Musset’s Sign • Head bobbing observed in a normal ventricle
Traube’s Sign • Pistol shot sound on the femoral artery • Figure 12:
Duroziez’s sign • Systolic murmur heard over the femoral artery o LV hypertrophy may also present with findings on the ECG
when compressed proximally o Strain changes related to AR are typically not observed on the ECG
Muller’s Sign • Systolic pulsation of the uvula § What is really seen are the changes in volume and voltages
Quincke’s Sign • Capillary pulsation of the fingers Þ Volume and voltages are notably very tall
Hill’s Sign • Popliteal cuff systolic BP > brachial cuff systolic Þ ST-segment depression and T-wave inversion in leads I, aVL, V5
BP by 60 mmHg and V6 (LV strain)
E. LABORATORY EXAMINATION F. DIFFERENTIAL DIAGNOSIS
• 2D-echocardiogram • PE of widened pulse pressure suggests the following possible differentials:
o Includes the assessment myocardial contractility and function o Thyrotoxicosis
o LV hypertrophy is manifested on the 2D-echo o Severe anemia
§ Like AS, AR also involves an overburdened left ventricular o AV fistula/malformations
hypertrophy (what differs between AS and AR is the § Applies to patients who undergo dialysis
pathophysiology) • PE and timing of diastolic murmur suggests the following possible
Þ AS causes LV hypertrophy by pressure, while AR causes LV differentials:
hypertrophy by volume o Mitral stenosis
• Lab exams are also indicated for patients who will undergo definite § Presents as a rumbling sound instead of a decrescendo type of
surgery (cardiac catherization and angiography) murmur
o Includes the assessment of the magnitude of AR and the status of LV o Ruptured coronary sinus of Valsalva (RCSOV)
function § Usually preceded by chest pain and a diastolic murmur of AR
G. MEDICAL TREATMENT
• Main goal is to unload or decrease volume (since AR is a volume problem)
through the following interventions:
o Salt restriction and diuretics
§ By decreasing the amount of fluids and sodium, the preload is
effectively minimized, and therefore reduces the strain on the
patient’s heart
§ Indicated for patients with chronic AR
Þ Patients with chronic AR have narrower pulse pressures and are
more symptomatic (increased volume and congestion)
Þ Patients with clinically significant AR actually feel more
Figure 11. (Left) Chronic Aortic Regurgitation: Note the enlargement of the comfortable once they have widened pulse pressures
left ventricle and atria, (Right) Acute Aortic Regurgitation: Normal sized o Vasodilators (ACE Inhibitors)
heart, with some degree of pulmonary congestion - cloudy appearance in the § Decreases the afterload
lungs § Improves the forward flow of the cardiac output
Þ Nitrates are not as helpful in relieving angina
o Penicillin
§ Treatment for syphilitic aortitis
H. SURGICAL TREATMENT
• Surgery is the definitive therapy
o Best performed before the onset of overt heart failure
§ Beyond this point (once heart failure occurs, it becomes difficult to
reverse the effects on the LV)
• Operation should be carried out even in asymptomatic patients with either
of the criteria applying a rule of 50
o Rule of 50
§ Summarizes the indications for surgery even for asymptomatic AR
patients
Þ Progressive left ventricular dysfunction and ejection fraction of
< 50%
Figure 12. ECG of Aortic Regurgitation
Þ Large left ventricular end-systolic diameter of > 50 mL/m2
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 7 of 18
Aortic Valve Replacement (AVR13) B. RHEUMATIC FEVER
• May use either a mechanical prosthesis and bioprosthesis Connection to Mitral Valve Damage
• Considerations • Predominant cause of mitral stenosis
o There is no percutaneous intervention for AR compared to AS o Dominant in females – 2/3 are rheumatics
o Timing is important o Only 25% have isolated MS and 40% have MS and mitral regurgitation
§ Operative mortality is 4.3% § Because of the inflamed and disfigured mitral valve (see Figure. 13)
§ Operative mortality increases to 10% if the patient already has LV o More common in developing countries
enlargement and dysfunction
ACTIVE RECALL
Aortic regurgitation can be managed by medical means. The best
treatment for AR is still surgery.
a) First sentence is true
b) Second Sentence is true
c) Both sentences are true
d) Neither are true
T/F: Aortic regurgitation is a problem of pressure.
ANSWERS: 5C, 6F - volume not pressure.
Figure 13. 2D-echo showing (Left) disfigured mitral valve leading to a (Right)
IV. MITRAL STENOSIS (MS14) fish-mouth appearance of the valve due to restricted opening
A. INTRODUCTION
• Figure 13:
• One of the most important valvular dysfunction or pathology especially in o Disfigured mitral valve leads to poor opening during diastole
the Philippine setting o Causes a “fish-mouth appearance” of the mitral valve
o High importance and frequency • 38% of cases: multi-valve involvement
o Potential cause of death if improperly diagnosed and improper o Aortic valve (AV) is 35% > tricuspid valve (TV) 6% > pulmonic valve
intervention timing
Diagnostic Features
Definition
• Thickening of the leaflet edges
• Defined as narrowing of mitral valve orifice • Fusion of the commissures
o Recall: mitral valve opens during diastole o Always a feature of rheumatic conditions
§ Systole (S1) closes mitral and tricuspid valve and opens aortic and
• Chordal thickening and fusion
pulmonic valve
o Consequence of antibody-antigen inflammatory reaction
Þ Mitral valve closes first since the left side of the heart has higher
o Recall: mitral and tricuspid valves are like parachutes with chordae,
pressure while aortic and pulmonic are cuspids
§ Diastole: opening of mitral and tricuspid; closing of aortic and
• Hallmark of rheumatic disease: Aschoff bodies
pulmonic valve
o Seen in pathology
o In mitral stenosis, the valve fails to open during diastole
o Seen in myocardium and not valve tissue
• When the stenotic mitral valve opens, it causes a rumble
o Due to a very big difference in the left atrium and left ventricle pressure
Natural History
Cause
• Most common cause: rheumatic condition
o More common in females
o Recall: AS is commonly caused by degenerative conditions
Symptoms
• Dyspnea and fatigue
o Due to poor emptying of left ventricle
• Decreased exercise tolerance
o This symptom is more evident when the heart rate is fast
§ During a fast heart rate, there is less time for the left ventricle to fill
because of the narrowed mitral valve
§ Less filled up left ventricle → lower cardiac output in systole
• Thus, patients must have a controlled heart rate
o Slow down the heart rate in order to prolong the diastolic phase and
give the LV more time to fill
Figure 14. Flowchart showing the natural history of rheumatic heart disease.
Complications
• Recall:
• Atrial fibrillation
o In aortic stenosis, intervene when symptomatic because patients
o Due to dilatation of left atrium
deteriorate fast
• Systemic embolism
o In aortic regurgitation, prior to heart failure, surgery must happen
o As part of atrial fibrillation
• In mitral stenosis, you have quite some time
• Infective endocarditis
o Patients have an immune reaction to repeated group A streptococcus
o May be easily infected
infections commonly seen in the Philippines
§ So, doctors in the US have not encountered many MS patients
• After a precipitating event, patient has first episode of rheumatic fever
• Repeated episodes of rheumatic fever will deform the valves
o Causing rheumatic heart disease
13AVR: Aortic Valve Replacement 14MS: Mitral Stenosis
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 8 of 18
TIP: Rheumatic heart disease already involves valvular pathology while D. DIAGNOSTIC FEATURES
rheumatic fever involves fever and inflammatory reactions. History and PE findings
• Common complaints
C. PATHOPHYSIOLOGY AND SYMPTOMATOLOGY o Exertional dyspnea
o paroxysmal nocturnal dyspnea (PND)
o Orthopnea
o Hemoptysis
• Recall: prevalence and risk factors for MS
o 2/3 are females
o Pure MS are generally from a rheumatic cause
• Pertinent findings at PE
o Opening snap
o Loud S1
o Diastolic rumble at the apex
[VIDEO] MITRAL STENOSIS
Figure 15. Flowchart showing pathophysiology of mitral stenosis. • To listen to the audio demo for mitral stenosis provided in the lecture
video, please scan this QR code. You may also opt to open this in Valvular
• In mitral valve stenosis, pressure changes are important Heart Disease Guerrero Part 2 of 2 at 14:49 to 16:38! J
• Mitral valve fails to open in diastole → increased left atrial pressure →
causes hypertrophy of left atrium → transmits pressure to pulmonic
circulation Radiologic Findings
o The increased pressure and blood in the pulmonic circulation leads to • ECG and CXR
hemoptysis o Evidence of left atrial enlargement with normal left ventricular size (in
§ Hemoptysis is more commonly a manifestation of MS compared to pure mitral stenosis)
other valvular diseases § Presence of enlarged left ventricle: suspect other valvular lesions
• Relatively, LV is normal because it is underfilled. (mitral regurgitation, aortic stenosis, etc.)
o Because the pressure is accumulating in left atrium • 2D-echo
o So, in pure mitral stenosis, left ventricle is normal
• Yet, because of dilated LA pressure into the lungs, there are manifestations
of left-sided heart failure → pulmonary congestion, orthopnea, dyspnea,
PND
o Recall: right-sided failure involves engorged neck veins, hepatomegaly,
bipedal edema, ascites
§ Symptoms of right-sided failure can also happen in the later stages
of MS as pulmonary hypertension worsens
TIP: Mitral stenosis patients manifest with left-sided heart failure first
then eventually, right-sided heart failure. Figure 16. Chest X-ray showing mitral stenosis. LAA: Left atrial appendage,
MPA: main pulmonary artery, LPA: left pulmonary artery, RPA: right
pulmonary artery, Ao: Aorta
• Recall: left recurrent laryngeal nerve hooks on the left main stem bronchus,
which is the roof of the left atrium • Figure 16:
• Compression of that nerve causes hoarseness, called Ortner’s syndrome o Left ventricle is preserved: level of mid-clavicular line and 5th intercostal
o Sometimes are referred to ENT for hoarseness but in fact, they have space
mitral stenosis o Four bumps on the left cardiac border: aorta, main pulmonary artery,
• Hypertrophy and dilatation will lead to: left atrial appendage, and normal left ventricle
o Atrial fibrillation causing decreased cardiac output o Sometimes, can appreciate prominent right and left pulmonary artery
o Atrial fibrillation along with stasis leads to: § Also findings related to pulmonary congestion such as prominent
§ Thromboembolism from the left atrium fissures and pulmonary circulation
§ Stroke o Other findings not appreciable in the figure:
§ Pulmonary emboli § Double contracture of the right cardiac border (manifestation of left
§ Myocardial infarction (MI15) atrial enlargement)
§ Uplifting of the left main stem bronchus (the roof of the left atrium)
Þ So, the angle of the carina is widened to more than 90 degrees
TIP: The main symptomatology of MS includes embolism, heart failure,
and poor cardiac output. Þ Obtuse carinal angle: contributory radiologic finding in dilated
left atrium
15MI: Myocardial Infarction
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 9 of 18
ACTIVE RECALL
Identify. Three common symptoms of mitral stenosis.
Identify. The type of heart failure that occurs first in mitral stenosis.
Identify. Hoarseness from mitral stenosis is called _____________
because the ____________ is compressed by the enlarged left atrium.
Identify. The four differential diagnoses for mitral stenosis.
Identify. Difference of the murmur in mitral stenosis and mitral
regurgitation.
ANSWERS: 7 dyspnea, fatigue, decreased exercise tolerance. 8 left-sided
HF. 9 Ortner’s syndrome, left recurrent laryngeal nerve. 10 atrial septal
Figure 17. ECG findings showing mitral stenosis. defect, left atrial myxoma, mitral regurgitation, aortic regurgitation. 11 MS
• Figure 17: murmur is a diastolic murmur while MR murmur is systolic.
o Right ventricular hypertrophy manifests on the ECG
§ Seen in tall R waves in V1 and right axis deviation and right
ventricular hypertrophy
TREATMENT
o LV is normal Goals of Medical Treatment
§ Unlike AS and AR that present with LV hypertrophy, the left ventricle • The definitive treatment for mitral stenosis is surgical
is normal in MS o However, medical treatment may be done if it is caught earlier
§ What may occur in MS is right ventricular hypertrophy • Goals of medical treatment for mitral stenosis
o P-mitrale not clearly seen here but may be appreciated in an ECG for o To reduce the recurrence of rheumatic fever
MS patients § Recall: repeated bouts of RF will lead to further inflammation and
o Appreciate left atrial enlargement in V1: the terminal deflection of the narrowing of the valves
P wave is downward o To provide prophylaxis for infective endocarditis
§ Indicated for patients with mitral stenosis who will be undergoing
E. CONSEQUENCES OF UNTREATED MITRAL STENOSIS any type of surgery (e.g. when undergoing dental procedures)
• Pulmonary hypertension § Patients must be protected from possible surgical infections
o Chronic congestion of the lungs → fibrous thickening of alveolar and o To reduce symptoms of pulmonary congestion
pulmonary capillary walls § Examples: orthopnea, paroxysmal nocturnal dyspnea
• Thrombi and emboli in the left atrial appendage § Pulmonary congestion is a permanent manifestation of mitral
o Because of atrial fibrillation stenosis
o More common in older patients and in reduced cardiac output Þ The goal here is only to reduce the severity of the symptoms and
• Pulmonary infections and infective endocarditis not to remove them
§ Avoid over diuresis of patients as these further decreases cardiac
output
F. DIFFERENTIAL DIAGNOSIS OF MITRAL STENOSIS
o To control the ventricular rate (if atrial fibrillation is present)
• Four considerations from murmur and anatomic differences § Treatment must give allowance for ventricular rate control
Þ Recall: MS patients inherently already have a low cardiac output
Atrial Septal Defect and low blood pressure
• Can have right ventricular enlargement and right atrial enlargement § Use of beta-blockers to control for the ventricular rate might further
• But no left atrial enlargement since the pressure is increased on the right aggravate hypotension
side in left-to-right shunts Þ Over diuresis of patients (in an attempt to relieve pulmonary
• Fixed splitting in ASD which can be misdiagnosed or compared to the congestion) will lead to low cardiac output states and high
opening snap ventricular rates
o But opening snap appreciated in the mitral valve area - This is a difficult state to pull patients out of
o Wide splitting is over the left para-sternal border § Therefore, beta-blockers must be used with caution
Þ It is a delicate balance between controlling the ventricular rate
and blood pressure
Left Atrial Myxoma
o To prevent thromboembolic complications
• Similar to a mitral stenosis murmur is a tumor-plop sound § Done by giving anticoagulant therapy
• In myxomatous tumors over the left atrium where it is attached in the
interatrial septum:
o In diastole and because of pressure difference, the myxoma tries to
Pharmacologic Treatment
obstruct the flow of the mitral valve opening • Treatment options are summarized below (see Table 3)
o Causing syncope because of decreased cardiac output and the tumor-
flop sound resembling the opening snap Table 3. Summary of Drug Examples Used in the Treatment of Mitral Stenosis
• 2D echo is used to differentiate the myxoma from MS TREATMENT ACTION/INDICATION CLINICAL NOTES
• Prophylactic
Mitral Regurgitation treatment for • Still the gold standard
RF and IE pharmacologic treatment
• Murmur: in the mitral area as well but during systole, so it is MR
Penicillin • Acts against beta- to prevent (prophylaxis)
o But this can be part of an MS
hemolytic rheumatic fever and
• MR involves left ventricular hypertrophy
Streptococcal infective carditis
o Recall: In pure MS conditions, the left ventricle is spared
infections
• Must be used with caution
Aortic Regurgitation (Austin Flint) o Recall: risk of severe
• Austin-Flint: apical mid-diastolic murmur from AR hypotension due to
Oral diuretics
o Caused by a vibration of the chordae when blood is pushed back to the over diuresis
(and sodium -
left ventricle and hits the chordae • Giving diuretics is
restrictions)
• Becomes louder on handgrip and decreases with amyl nitrate conditional if the patients
typically have low cardiac
output
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 10 of 18
TREATMENT ACTION/INDICATION CLINICAL NOTES § Also a deciding factor on whether to do a normal spontaneous
• Main drug used is still delivery (NSD17) or to perform a cesarean section
warfarin
• Indicated for
o Newer oral General Procedure
patients with atrial
anticoagulants have not
fibrillation
Oral been studied on
o Recall: given to
anticoagulant patients with moderate
prevent
s (Warfarin) to severe MS
thrombo-
• Target an INR of 2 to 3.1
embolic
o Prevents embolization
complications
and permanent atrial
fibrillation
• Acts to lengthen
diastolic LV filling
o Gives the left • Specific drug example Figure 18. (Left) Percutaneous transseptal mitral commissurotomy in early
ventricle administered depends on inflation, note the waistline of the balloon (black arrowheads) representing
enough time to the needs and therapeutic the location of the orifice before undergoing (Right) full expansion to force
fill to improve goals of the patient* the valve open
Heart rate
cardiac output o Beta-blockers
controlling
• Recall: Treatment o Digitalis • Insert a deflated balloon over the right femoral vein à inferior vena cava
drugs
involves a very o Non-dihydropyridine à right atrium à puncture the interatrial septum à to get into the left
delicate balance calcium antagonists side of the heart and into the mitral valve
between low § Diltiazem • Full inflation forces the valve to open (see Figure 18)
cardiac output and § Verapamil o Recall: patients with mitral regurgitation will not be able to control the
compensatory cracking of the fused commissures leading to increased deterioration
tachycardia
Mitral Valve Replacement
• Indications for the different heart rate controlling drugs*
o Beta-blockers
§ Indicated for MS patients in sinus rhythm
§ Indicated for MS patients with atrial fibrillation as long as the blood
pressure is allowable (Systolic blood pressure (SBP16) greater than or
equal to 100) just to slow down the heart rate
o Digitalis
§ Indicated for MS patients with atrial fibrillation and low cardiac
output (SBP is low at around 90)
§ Not indicated (no role) for MS patients in sinus rhythm
o Non-dihydropyridine calcium antagonists Figure 19. (Left) St. Jude Bileaflet Valve and the (Right) Carpentier Edwards
§ Indicated for MS patients who cannot tolerate beta-blockers Pericardial Valve
Þ Patients allergic to beta-blockers
Þ Patients with COPD or severe asthma) • Use of either a bioprosthesis or mechanical prosthesis to replace the mitral
valve (see Figure 19)
Surgical Treatment o St. Jude Bileaflet Valve: commonly used mechanical prosthesis
• Recall: Surgery is the definitive treatment for mitral stenosis nowadays due to its greater durability
o Carpentier Edwards Pericardial Valve: type of pericardial or
bioprosthesis valve
Mitral Valvotomy
• Done for patients who are not good candidates for mitral valvotomy
• Also known as balloon valvuloplasty or percutaneous balloon o MS patients with mitral regurgitation
valvuloplasty o MS patients with distorted valves from previous transcatheter or
• Indications and contraindications operative manipulation
o Indicated in symptomatic patients with severe and isolated MS • Statistics
§ Severe: defined as MS with a mitral valve orifice less than 1.0 cm2 / o 6% operative mortality due to incidence of stroke
m2 o 70% overall 10-year survival rate
§ Ideal for patients with the following three characteristics: § Poor recovery for patients of old age, with marked disability, and/or
Þ Mobile, thin leaflets with little to no calcium deposits AND depressed cardiac index (especially those with heart failure
Þ Without extensive subvalvular thickening AND symptoms)
Þ With no or mild mitral regurgitation only Þ Old age: rheumatic patients get into problems at 40 years of age
o Contraindicated for patients with mitral regurgitation and usually opt out of surgery if they have been tolerating their
§ Recall: only patients with isolated MS are good candidates for this symptoms for that long
intervention • Other considerations
§ Performing this surgery risks worsening the mitral regurgitation and o Long-term complications of valve replacement depend on the valve
increasing congestion for the patient used
Þ Dilation of the mitral valve risks cracking or opening the valve o Use of bioprosthesis instead of a mechanical prosthesis for women of
using the balloon (there is lack of control to avoid this event from reproductive or menstruating age
happening) § Mechanical prosthesis will require long term anticoagulation
• Open valvotomy: not done anymore due to mortality rate (2%) therapy using warfarin (has risks of teratogenicity and abortion in
• Other considerations pregnancy)
o 50% of patients require reoperation after 10 years
§ There is a recurrence of narrowing usually in 10 years’ time
o Only carried out in pregnant women if pulmonary congestion occurs
despite intensive medical treatment
§ Used as an alternative to open surgery (not possible for pregnant
patients)
16SBP: Systolic Blood Pressure 17 NSD: Normal Spontaneous Delivery
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 11 of 18
ACTIVE RECALL B. DIFFERENTIAL DIAGNOSIS OF MITRAL REGURGITATION
Which of the following is a contraindication to perform mitral • Recall: MR presents with a systolic murmur near the apex (observed during
valvotomy? the auscultation stage of PE)
a) Patient has mitral regurgitation • Specifically, MR presents with a holosystolic murmur
b) Patient is pregnant with persistent pulmonary congestion o The murmur is not a diamond-shaped or harsh-sounding murmur
c) Patient is obese • Differentials may be formed based on the type of systolic murmur and its
d) AOTA location (see Table 4)
Identify. Gold standard prophylaxis for rheumatic fever and infective
endocarditis Table 4. Auscultatory Findings for the Four Main Differentials of MR
DIFFERENTIAL CHARACTERISTICS
CLINICAL NOTES
ANSWERS: 12A, 13 Penicillin DIAGNOSIS (SOUND, LOCATION)
• Holosystolic murmur at the
Tricuspid Increases with
4th intercostal space, left
V. MITRAL REGURGITATION (MR18) Regurgitation inspiration
parasternal border
• Marked by a systolic murmur heard best at the apex (see QR code below) • Harsh, holosystolic murmur at Murmurs are
• Regurgitation involves pathologic changes related to volume Ventricular the 3rd intercostal space, left shorter with
Septal Defect parasternal border (Erb’s elevated PA
point) pressures
[VIDEO] MITRAL REGURGITATION HEART SOUNDS
• Holosystolic murmur (harsh
ejection murmur) at the 2nd
intercostal space, right
• Gallavardin phenomenon of
Aortic aortic stenosis Radiation to the
Stenosis o Musical component (not carotid arteries
holosystolic sounding)
may be transmitted from
this location to the apex
through solid tissues
• Systolic murmur
o Not holosystolic (click-type
Mitral Valve
• To listen to the audio demo for mitral stenosis provided in the lecture sound) -
Prolapse
video, please scan this QR code. You may also opt to open this in Valvular o Usually an early- to mid-
Heart Disease Guerrero Part 2 of 2 at 39:50 onwards! J type systolic murmur
• Video notes:
o Patient had a normal S1 and S2 but had a remarkable systolic murmur C. SYMPTOMATOLOGY OF MITRAL REGURGITATION
over the apex
A. COMMON ETIOLOGIES OF MITRAL REGURGITATION
• Causes of MR not only involves the valve but may also involve the root or
the apparatus attached to the valve
Mitral Valve Leaflet Abnormality
• Rheumatic heart disease: still the most common cause (similar to MS)
• Myxomatous alteration: includes MVP
• Infective endocarditis: destroys the valve leading to insufficiency or
improper mitral valve coaptation
Mitral Annulus Dilatation of Any Cause Figure 20. Diagram comparing a normal systole to acute and chronic MR.
• Secondary cause of MR
o The annulus (where the valve lies) dilates, leading to forced separation • Similar to AR, mitral regurgitation may be acute or chronic
of the mitral leaflet, ultimately causing MR • Manifestations of MR depends on the acuteness of the condition (the time
• Particularly seen in heart failure it takes for the heart to compensate) (see Figure 20)
o Dilated cardiomyopathy
o Ischemic Heart Disease (IHD19) with dilated LV Acute MR
• Problem is that there is no time for the heart to compensate for the
Ruptured Chordae Tendinae increased pressure (see Figure 20)
• Trauma o Blood back flows into the LA à No time for LA to dilate à High LA
• Rupture is common in cases of mitral valve prolapse pressure transmitted to the lungs à Early pulmonary edema
• Myocardial infarction • Typical manifestations of impaired LV function:
o Patients may experience a rupture of the chordae usually 7 days o Dyspnea
following an anterior wall MI (post-MI) o Fatigue
o Manifests as sudden heart failure o Orthopnea
o Early pulmonary edema
§ May be life-threatening
Papillary Muscle Disorder § Usual initial manifestation because of the rapid volume overload on
• Ischemic Heart Disease the LA and the pulmonary venous system
o Papillary muscles are supplied by the anterior descending artery and as • Occurs in the setting of CAD and acute MI (usually in the inferior wall)
such may be affected (experience a rupture) by a large anterior wall MI o These events cause a papillary muscle rupture or dysfunction
§ Patient with a large anterior MI à papillary muscle rupture à LV is
not prepared to accommodate the increased pressure à Acute MR
o Immediate surgery is needed to repair the ruptured papillary muscle or
chordae tendineae
18MR: Mitral Regurgitation 19 IHD: Ischemic Heart Disease
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 12 of 18
Chronic MR • Beta-blockers and biventricular pacing
o Only indicated for primary treatment of severe LV dysfunction in
• Problem involves a long-term and repeated inflammatory process in the
functional MR
mitral valve
o Beta-blockers are given to override the rate of the heart of patients with
o There is time for the LV and LA to dilate and accommodate and
pacemakers
normalize the pressure respectively to lessen congestion (see Figure 20)
§ This is so they can time the sequence of activation of the atrium and
o Subsequent progressive enlargement of the left atrium and ventricle
ventricle, to improve mitral regurgitation and consequent cardiac
• Typical manifestations
output as well as to lessen congestion
o Patients may remain asymptomatic for years
• If atrial fibrillation is encountered, maintenance of a normal ventricular
o Patients may have normal exercise tolerance until the systolic
response with beta-blockers, calcium channel blockers, and/or digitalis
dysfunction of the LV develops
therapy is considered
§ Once LV systolic dysfunction occurs, symptoms of reduced cardiac
o Be very careful with calcium channel blockers because in MR, the LV is
output may be observed
already dilated
Þ Fatigue, dyspnea on exertion, shortness of breath
§ Non-dihydropyridines such as Diltiazem and Verapamil can further
o Over time, patients may feel chest palpitations if AF develops due to
aggravate heart failure
chronic atrial dilatation
o Beta-blockers or digitalis therapy are preferred over calcium-channel
§ Sometimes with further AF, one can lose the "kick" of the atrium
blockers
which contributes 30% of the cardiac output and further contributes
§ Start with digitalis therapy in patients with AF, dilated LV, and
to fatigue and dyspnea
congestion
§ This further progresses to pulmonary congestion and edema
• Anticoagulation is considered for patients who develop atrial fibrillation or
o Symptoms may progress to symptomatic congestive heart failure with
have had mitral valve replacement surgery
pulmonary congestion and edema
o Recall: Warfarin is indicated because the new anti-coagulants in the
§ True for patients with LV enlargement and more severe diseases
market have not been tested in sever valvular hear disease
§ At this stage of LV dilatation, the myocardial dysfunction often
becomes irreversible • Antibiotics are recommended prior to any dental procedure that involves
manipulation of gingival tissue, the periapical region of the tooth, or
Þ Pulmonary congestion is a late symptom
perforation of oral mucosa
D. LABORATORY EXAMINATIONS
Surgical Treatment
• Recall: Changes are related to increased volume in LV
• Non-surgical candidates include patients who are:
• Diagnostic Features:
o Asymptomatic
o LA enlargement
o Have the ability to exercise (limited to strenuous exertion)
§ Rarely do you have right atrial enlargement, but RAE may be present
o Have normal LV function
if pulmonary hypertension is severe or if with a concomitant MS
• Surgery for severe MR even if asymptomatic or when LV dysfunction is
murmur
progressive (declining <60%) and/or LV ESD on echo is >45mm
o Atrial Fibrillation will further aggravate cardiac output
o Rule of 50 similar to that in AR can also be applied here
o Left ventricular hypertrophy
§ Involves determining the ejection fraction and ESD
• Laboratory examinations/techniques
• MV total replacement is indicated for severely/markedly shrunken,
o 2D Echo – most accurate non-invasive technique
deformed, calcified leaflets
o Chest X-ray – demonstrate LA enlargement and LV enlargement
• MV repair (reconstruction) with annuloplasty
o ECG
o Lessen problem on long term anticoagulation and thromboembolism
§ Done for patients in sinus rhythm, provided they meet the
criteria/indications for repair
§ In patients already in AF, repair is no longer indicated and total
replacement is done
o For ruptures chordae, annular dilatation, and IE
o Not suitable for MR due to myxomatous degeneration and patients with
calcified leaflets
2 As long as the ejection fraction is still good, when the LV is not yet dilated,
you can postpone surgery
2 The type of surgery will depend on the degree of destruction of the valve
Figure 21. Mitral Regurgitation CXR ACTIVE RECALL
• Figure 21: Which of the following cardiovascular disorders risks destroying the
o Displaced apex laterally and downward at 7th intercostal space mitral valve leaflet, leading to insufficiency and improper mitral valve
§ Signifying left ventricular hypertrophy coaptation?
o Prominent left atrium a) Rheumatic fever
o Flat pulmonary artery and small/normal aorta b) Infective endocarditis
o Prominent pulmonary vessels (congestion) c) Ischemic heart disease with LV dilatation
d) Dilated cardiomyopathy
T/F. Pulmonary congestion manifests early on for patients with chronic
E. TREATMENT MR.
Medical Treatment
• Restriction of activity and salt intake ANSWERS: 14B, 15F
o Regurgitations are volume-related pathophysiologic changes
o Management for all regurgitations include reduction of salt and diuresis
• Afterload-reducing agents
VI. MITRAL VALVE PROLAPSE
o Nitrates and anti-hypertensive drugs A. OVERVIEW
§ Reduction of pre-load and afterload • Same causing as MR, but different in character
§ Anti-hypertensive medications (ACE inhibitors and ARBs) are • Also known as: Barlow’s syndrome, floppy valve-syndrome, systolic click-
afterload unloaders murmur syndrome, and billowing mitral leaflet
o Diuretics • Excessive or redundant mitral leaflet tissue
o Helpful in dilating afterload and maintaining the forward cardiac output o Most common is the posterior MV leaflet (more affected than the
in persons with MR with symptoms and/or LV dysfunction anterior mitral valve leaflet)
• May lead to excessive stress on the papillary muscles leading to
dysfunction or rupture of the chordae
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 13 of 18
o Rupture of chordae tendineae with progressive annular dilatation and D. TREATMENT
calcification
• Patients can be prone to ventricular arrythmia Medical Treatment
o Manifested as palpitations • Intensive salt restriction
• Diuretic treatment
Clinical Features Surgical Treatment
• Females (14-30 years old) • Definitive treatment
• Clinical course is often benign • Diastolic pressure gradient >4mmHg
• Increased familial incidence – autosomal dominant • Tricuspid orifice , 1.5 to 2.0 cm
• Most common cause of isolated severe MR requiring surgical treatment in • With open heart repair/prosthesis/tricuspid valve replacement, a large
North America bioprosthetic valve is preferred
o Severe cases would already require intervention o A bioprosthetic valve is more durable over the right as it is not pressure
• Palpitations, lightheadedness, and syncope related to arrythmias (PVCs, dependent, and is a better option because it withholds long-term
SVTs, VTs) can still be treated with medical therapy anticoagulation
o Sudden death is rare § Unless the patient is already in atrial fibrillation
• Chest pain – substernal, prolonged, unrelated to exertion
o Consequent to either increased PA pressure or problems with chordae VIII. TRICUSPID REGURGITATION (TR21)
elasticity A. CAUSES
Anatomically Abnormal Valve
B. LABORATORY EXAMINATIONS
• Rheumatic
• Non-rheumatic
Table 5. Laboratory Exams for MVP
o Infective endocarditis
ECG ECHO
o Ebstein anomaly
More definitive; demonstrates
Non-specific ST-segment and T- o Floppy (prolapse)
systolic displacement of mitral
wave changes o Congenital (non-Ebstein)
valve leaflet o Carcinoid
Pre-ventricular contractions Quantifies MR and LV function o Papillary muscle dysfunction
o Trauma
C. TREATMENT o Connective tissue disorders (Marfan)
• IE prophylaxis o Rheumatoid arthritis
o For patients undergoing surgery and pregnant women o Radiation injury
• Beta-blockers
o For benign cases Anatomically Normal Valve (Functional)
o Sometimes relieve chest pain • Elevated right ventricular systolic pressure (dilated annulus)
• MV repair or replacement o If surgery is indicated, they are usually with a consequent mitral valve
o For severe symptomatic MR replacement and a tricuspid valve annuloplasty
o Replacement is rarely indicated
• Antiplatelets
B. MECHANISMS
o For patients with transient ischemic attacks
• Anticoagulation
Table 6. Mechanisms of Tricuspid Regurgitation
o If recurrent transient ischemic attacks
ANNULAR LEAFLET
CONDITION LEAFLET AREA
CIRCUMFERENCE INSERTION
NOTE: The sections on right-sided valves were not discussed extensively. Floppy Increased Increased Normal
Ebstein
Increased Increased Abnormal
Anomaly
VII. TRICUSPID STENOSIS (TS20)
Pulmonary RV
A. HISTORY Normal Increased Normal
Systolic HPN
• Progressive fatigue, edema, anorexia Papillary
• Minimal orthopnea, paroxysmal nocturnal dyspnea Muscle Normal Normal Normal
• Rheumatic fever in two thirds of patients Dysfunction
• Female preponderance Carcinoid Decreased/Normal Normal Normal
• Pulmonary edema and hemoptysis are rare Rheumatic Decreased/Normal Normal Normal
Infective
Decreased/Normal Normal Normal
B. PHYSICAL FINDINGS Endocarditis
• Signs of multivalvular involvement
• Diastolic rumble at lower left sternal border, increasing in intensity with C. TREATMENT CONSIDERATIONS
inspiration • Isolated TR, in the absence of pulmonary hypertension
• Often confused with mitral stenosis o Well tolerated and does not require operation
• Peripheral cyanosis • Functional TR (secondary to pulmonary hypertension with MV disease)
• Neck vein distention, with prominent v waves and slow y descent o Resolves with effective correction of the MV disease
• Absent right ventricular lift • Annuloplasty
• Associated murmurs of mitral and aortic valve disease o Procedure usually performed
• Hepatic pulsation • Tricuspid valve replacement
• Ascites, peripheral edema o For severely deformed valves
C. LABORATORY FINDINGS
• ECG: tall right atrial P waves and no right ventricular hypertrophy
• Chest roentgenogram: dilated right atrium without an enlarged pulmonary
artery segment
• Echo: diastolic doming of tricuspid valve leaflet
20TS: Tricuspid Stenosis 21TR: Tricuspid Regurgitation
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 14 of 18
IX. PULMONIC VALVE DISEASE • Clinical Presentation
o Exertional dyspnea
• Pulmonic Regurgitation
o Angina
o Most commonly acquired abnormality of the PV
o Syncope
o Secondary to dilatation of the PV ring as a consequence of pulmonary
o Heart failure
hypertension
• Laboratory Examinations
• Elicits a typical Graham Steell murmur
o LV hypertrophy is the key finding demonstrated by
o High-pitched decrescendo
§ ECG
o Diastolic blowing murmur
§ 2D Echo
o Along the left sternal border similar to aortic regurgitation
o Radiograph findings:
• Of little hemodynamic significance
§ Cardiac silhouette resembling a LV hypertrophy
§ Apex is displaced laterally and downward
HOW’S MY TRANSING? § The aorta is displaying tortuosity, bulging, and showing stiffness
Feedback Form: https://tinyurl.com/2024YL7HMTForm o ECG findings: presents with tall R waves over the left sided leads, V5
Errata Tracker: https://tinyurl.com/2024YL7ET02 and V6
• Differential diagnoses
o Acute coronary syndrome (ACS): Due to the hemodynamic changes in
QUICK REVIEW AS and angina
SUMMARY OF CONCEPTS o Hypovolemic Shock: The blood pressure of the patient will be relatively
REVIEW OF HEART SOUNDS low considering the inability of the aortic valve to open
• S1: The first heart sound, “lub” caused by the closing of AV valves after the o Mitral regurgitation and mitral valve prolapse: Similar timing of the
atria have pumped blood into the ventricles murmur
• S2: The second heart sound, “dub” which originates from the closing of • Treatment of Aortic Stenosis
the aortic and pulmonary valves, right after the ventricles have ejected the o Medical Management: Generally does not improve outcomes or
blood survivability and is only given to patients who refuse consent for surgery
• Systole: the time interval between S1 and S2 when the ventricles contract o Surgical Management: Preferred mode of treatment via a valve
• Diastole: the time interval between S2 and the next S1 when the ventricles replacement
relax and are filled with blood § Patients > 65 years old can receive bioprosthesis
• 4 Different sites on the chest wall where heart sounds are auscultated: § Younger patients receive mechanical prosthesis, but must be given
o Aortic area: In the right 2nd intercostal space anti-coagulants
o Pulmonic area: In the left 2nd intercostal space
o Tricuspid area: In the left 4th intercostal space AORTIC REGURGITATION
o Mitral area: At the apex or the left 5th intercostal space (midclavicular) • Overview
o It is a diastolic event
MURMURS o Unlike stenosis, AR is a volume-related problem
• Murmurs: Whooshing sounds produced by turbulent blood flow o Due to valvular insufficiency, blood flows back into the LV
o Diagnosed based on: o It is best heard in the left parasternal border
§ Time • Acute AR vs Chronic AR
§ Shape o Acute: The heart has not adapted yet and cannot compensate for the
§ Location increase in blood volume in the LV, thus causing an increase in LA
• Systolic Murmurs pressure and subsequently leading to pulmonary congestion
o Mitral valve regurgitation: Occurs when the mitral valves does not o Chronic: The LV is dialated, and enlarged, and therefore can
close properly and blood surges back to the left atrium during systole compensate for the increase volume of blood without increasing
o Tricuspid valve regurgitation: Has similar timing and shape with mitral pressure in the LA
valve regurgitation, but occurs on the other side of the heart • Treatment of Aortic Regurgitation
o Aortic valve stenosis: Occurs when the aortic valve doesn’t open o Medical Management: Unlike aortic stenosis, medical treatment has
properly and blood is forced through a narrow opening value since AR can be treated by reducing preload via the
o Pulmonic valve stenosis: Same characteristics as the aortic valve administration of diuretics
stenosis, however, is best heard at the pulmonic area o Surgical Management: Similar to surgical management, valve
2 Ventricular Septal Defect: Holosystolic murmur over the 3rd intercostal replacement is still the mainstay treatment.
space, left parasternal border (Erb’s point)
2 Mitral Valve Prolapse: Early to mid-type of systolic murmur MITRAL STENOSIS
• Diastolic Murmurs • Defined as narrowing of the mitral valve orifice
o Aortic valve regurgitation: Occurs when the aortic valve doesn’t close • Fish-mouth appearance: characteristic of affected mitral valve on 2D echo
properly, resulting to blood flowing back to the left ventricle (LV) during • Aschoff bodies: characteristic pathologic finding in the myocardium
diastole (or the filling phase) • Most common cause: rheumatic conditions
: Pulmonic valve regurgitation: Occurs when the pulmonic valve is • Symptoms: dyspnea, fatigue, decreased exercise tolerance
incompetent which results in the abnormal reversal of blood flow from • Complications: atrial fibrillation, systemic embolism, infective endocarditis
the pulmonary artery into the right ventricle • MS and Rheumatic Heart Disease:
2 Mitral stenosis: Inability of the mitral valve to open during diastole due o Mostly in females and in developing countries
to obstruction in left ventricular inflow o 25%: isolated MS and 40%: MS and mitral regurgitation (MR)
2 Tricuspid stenosis: Have the same diastolic murmur as mitral stenosis o Repeated group A strep infection leads to disfigurement of mitral valve
but on the right side • Key characteristics: fish-mouth appearance and Aschoff bodies
• Diagnostics and Natural History
AORTIC STENOSIS o History: Exertional dyspnea, paroxysmal nocturnal dyspnea, orthopnea,
• Aortic stenosis: a systolic murmur and hemoptysis
• 3 Principal causes: o PE findings: Opening snap, loud S1, diastolic rumble at the apex
o Congenital bicuspid valve with superimposed calcification o Chest X-Ray main finding: LA enlargement with normal LV size
o Calcification of a normal trileaflet valve § Enlarged LV: suspect involvement of other valvular lesions
o Rheumatic diseases Þ Other findings: pulmonary congestion (prominent fissures and
• Pathophysiology pulmonary circulation), double contracture of the right cardiac
o Due to the difficulty of opening the aortic valve, the LV has to go under border, uplifting of the left main stem bronchus (carinal
hypertrophy for it to generate a higher pressure to push blood forward widening)
past the aortic stenosis o ECG findings: Left atrial enlargement
o The pressure in LV, which is now high, will cause the LA pressure to § Tall R waves in V1, right axis deviation, RV hypertrophy
increase which causes LA enlargement § P-mitrale
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 15 of 18
§ Downward terminal deflection of the P wave Þ Pulmonary edema: Usual initial manifestation because of the
o Natural history: pulmonary hypertension, thrombi and emboli, rapid volume overload on the LA and the pulmonary venous
pulmonary infections, infective endocarditis system
• Four Differential for Mitral Stenosis o Chronic MR: Involves a long-term and repeated inflammatory process
o Atrial Septal Defect: Rule out because: in the mitral valve
§ The wide splitting sound is different from the opening snap § Patients may remain asymptomatic for years
§ ASD has right atrial and ventricular enlargement but no left atrial § Patients may have normal exercise tolerance until the systolic
enlargement (which is characteristic of mitral stenosis) dysfunction of the LV develops (leading to symptoms of reduced
o Left Atrial Myxoma: has a similar “tumor-plop” sound but this is ruled cardiac output)
out using a 2D echo Þ Fatigue, dyspnea on exertion, shortness of breath
o Mitral Regurgitation: has a murmur but rule out because: § Overtime, patients may feel chest palpitations if AF develops due to
§ Murmur occurs during systole while MS occurs in diastole chronic atrial dilatation
§ MR has LV hypertrophy while pure MS does not have it § Symptoms may progress to symptomatic congestive heart failure
o Aortic regurgitation (Austin Flint): apical mid-diastolic murmur with pulmonary congestion and edema
§ Louder on handgrip and decreases with amyl nitrate • Diagnostic Features
• Goals of medical treatment: o LA enlargement
o To reduce the recurrence of rheumatic fever o Atrial Fibrillation will further elevate cardiac output
o To provide prophylaxis for infective endocarditis o Left ventricular hypertrophy
o To reduce symptoms of pulmonary congestion • Laboratory examinations/techniques
o To control the ventricular rate (if atrial fibrillation is present) o 2D Echo – most accurate non-invasive technique
o To prevent thromboembolic complications o Chest X-ray – demonstrate LA enlargement and LV enlargement
• Pharmacologic treatment: o ECG
o Penicillin: Still the gold standard pharmacologic treatment to prevent • Medical Treatment
(prophylaxis) rheumatic fever and infective carditis o Restriction of activity and salt intake
o Oral diuretics (and sodium restrictions): Giving diuretics is conditional o Afterload-reducing agents
if the patients typically have low cardiac output § Nitrates and anti-hypertensive drugs
o Oral anticoagulants (warfarin): Indicated for patients with atrial § Diuretics
fibrillation o Beta-blockers and biventricular pacing
§ Target INR of 2 to 3.1 § Only indicated for primary treatment of severe LV dysfunction in
o Heart rate controlling drugs: Lengthens diastolic LV filling to improve functional MR
cardiac output § Beta-blockers are given to override the rate of the heart of patients
§ Beta-blockers with pacemakers
§ Digitalis o If atrial fibrillation is encountered, maintenance of a normal ventricular
§ Non-dihydropyridine calcium antagonists response with beta-blockers, calcium channel blockers, and/or
Þ Diltiazem digitalis therapy is considered
Þ Verapamil o Anticoagulation is considered for patients who develop atrial
• Surgical treatment: fibrillation or have had mitral valve replacement surgery
o Mitral valvotomy: Also known as balloon valvuloplasty or percutaneous § Warfarin is indicated
balloon valvuloplasty o Antibiotics are recommended prior to any dental procedures
§ Indicated in symptomatic patients with severe and isolated MS (less • Surgical Treatment
than 1.0 cm2 / m2) o Non-surgical candidates:
§ Contraindicated for patients with mitral regurgitation § Asymptomatic
o Mitral valve replacement: Use of either a bioprosthesis or mechanical § Exercise limited to strenuous exertion
prosthesis to replace the mitral valve § Normal LV function
§ Done for patients who are not good candidates for mitral valvotomy o Surgery for severe MR even if asymptomatic or when LV dysfunction is
(patients with MR or grossly distorted valves) progressive (declining <60%) and/or LV ESD on echo is >45mm
o MV total replacement is indicated for severely/markedly shrunken,
MITRAL REGURGITATION deformed, calcified leaflets
• Marked by a systolic murmur heard best at the apex (see QR code below) o MV repair (reconstruction) with annuloplasty
• Regurgitation involves pathologic changes related to volume § Lessen problem on long term anticoagulation and
• Common etiologies of MR: thromboembolism
o Mitral valve leaflet abnormality: due to rheumatic heart disease, § For ruptures chordae, annular dilatation, and IE
myxomatous alteration, or infective endocarditis § Not suitable for MR due to myxomatous degeneration and patients
o Mitral annulus dilatation of any cause: due to dilated cardiomyopathy with calcified leaflets
or IHD with dilated LV
o Rupture of the chordae tendinea: due to trauma, MVP, MI MITRAL VALVE PROLAPSE
o Papillary muscle disorder: due to IHD • Also known as: Barlow’s syndrome, floppy valve-syndrome, systolic click-
• Differential diagnosis of MR: murmur syndrome, and billowing mitral leaflet
o Tricuspid regurgitation: Holosystolic murmur at the 4th intercostal • Excessive or redundant mitral leaflet tissue
space, left parasternal border o Most common is the posterior MV leaflet (more affected than the
o Ventricular septal defect: Harsh, holosystolic murder at the 3rd anterior mitral valve leaflet)
intercostal space, left parasternal border (Erb’s point) • May lead to excessive stress on the papillary muscles leading to
o Aortic stenosis: Holosystolic murmur (harsh ejection murmur) at the dysfunction or rupture of the chordae
2nd intercostal space, right • Patients can be prone to ventricular arrythmia
§ Gallavardin phenomenon of aortic stenosis: Musical component o Manifested as palpitations
(not holosystolic sounding) may be transmitted from this location to • Clinical Features
the apex through solid tissues o Females (14-30 years old)
o Mitral valve prolapse: Systolic murmur; not holosystolic (click-type o Clinical course is often benign
sound) o Increased familial incidence – autosomal dominant
• Symptomatology of MR: o Most common cause of isolated severe MR requiring surgical treatment
o Acute MR: There is no time for the heart to compensate for the in North America
increased pressure o Palpitations, lightheadedness, and syncope related to arrythmias
§ Typical manifestations of impaired LV function (PVCs, SVTs, VTs) can still be treated with medical therapy
Þ Dyspnea § Sudden death is rare
Þ Fatigue o Chest pain – substernal, prolonged, unrelated to exertion
Þ Orthopnea
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 16 of 18
• Laboratory Examination PULMONIC VALVE DISEASE
o ECG – Non-specific ST-segment and T-wave changes; pre-ventricular • Pulmonic Regurgitation
contractions o Most commonly acquired abnormality of the PV
o Echo – More definitive; demonstrates systolic displacement of mitral o Secondary to dilatation of the PV ring as a consequence of pulmonary
valve leaflet; quantifies MR and LV function hypertension
• Treatment • Elicits a typical Graham Steell murmur
o IE prophylaxis • Of little hemodynamic significance
§ For patients undergoing surgery and pregnant women
o Beta-blockers SUMMARY OF NEED-TO-KNOWS (NDTK)
§ For benign cases
• The onset of symptoms for AS is very important to recognize because
§ Sometimes relieve chest pain
patients deteriorate so rapidly once they develop.
o MV repair or replacement
§ For severe symptomatic MR
§ Replacement is rarely indicated SUMMARY OF PROCESSES
o Antiplatelets HEMODYNAMIC CHANGES IN AORTIC STENOSIS
§ For patients with TIA 1) All hemodynamic changes in aortic stenosis are related to left ventricular
o Anticoagulation outflow obstruction
§ If recurrent TIAs 2) LV outflow obstruction causes 4 differences in terms of pressure:
o Elevation of LV systolic pressure
TRICUSPID STENOSIS § Therefore, it takes time for blood to be injected out
• History o This increases left ventricular ejection time (LEVT)
o Progressive fatigue, edema, anorexia o Elevation of LV diastolic pressure
o Minimal orthopnea, paroxysmal nocturnal dyspnea o Aortic pressure decreases
o Rheumatic fever in two thirds of patients § Aortic pressure: the pressure beyond the aortic stenosis
o Female preponderance 3) All of those will lead to:
o Pulmonary edema and hemoptysis are rare o Hypertrophy
• Physical Findings o Dysfunction
o Signs of multivalvular involvement o Increased myocardial oxygen consumption
o Diastolic rumble at lower left sternal border, increasing in intensity with o Decreased diastolic time
inspiration 4) This all then subsequently leads to a disproportion in supply and demand
o Often confused with mitral stenosis of myocardial oxygen consumption
o Peripheral cyanosis 5) Then may eventually end in LV failure
o Neck vein distention, with prominent v waves and slow y descent
o Absent right ventricular lift MITRAL STENOSIS PATHOPHYSIOLOGY
o Associated murmurs of mitral and aortic valve disease 1) Mitral valve fails to open in diastole → increased left atrial pressure →
o Hepatic pulsation causes hypertrophy of left atrium → transmits pressure to pulmonic
o Ascites, peripheral edema circulation → hemoptysis
• Laboratory Findings 2) Dilated LA → left-sided heart failure → pulmonary congestion, orthopnea,
o ECG: tall right atrial P waves and no right ventricular hypertrophy paroxysmal nocturnal dyspnea → eventually right-sided heart failure
o Chest roentgenogram: dilated right atrium without an enlarged 3) Atrial fibrillation → decreased cardiac output
pulmonary artery segment 4) Atrial fibrillation + stasis → thromboembolism in left atrium, stroke, MI
o Echo: diastolic doming of tricuspid valve leaflet
• Treatment SUMMARY OF MEMORY AIDS
o Medical treatment • CLINICAL PRESENTATION OF AORTIC STENOSIS: ASH
§ Intensive salt restriction o Angina
§ Diuretic treatment o Syncope
o Surgical treatment o Heart failure
§ Definitive treatment
§ With open heart repair/prosthesis/tricuspid valve replacement, a
SUMMARY OF EQUATIONS
large bioprosthetic valve is preferred
Equation 1. Cardiac output
TRICUSPID REGURGITATION
𝐶𝑂 = 𝑆𝑉 𝑥 𝐻𝑅
• Causes
• Where:
o Anatomically abnormal valve
§ Rheumatic o CO = Cardiac output
o SV = Stroke volume
§ Non-rheumatic
o HR = Heart rate
Þ Infective endocarditis
Þ Ebstein anomaly
Þ Floppy (prolapse) REVIEW QUESTIONS
Þ Congenital (non-Ebstein) S.M. (29/F) comes to the clinic at 13 weeks AOG complaining of dyspnea,
Þ Carcinoid fatigue, and palpitations. S.M. was previously diagnosed with severe mitral
Þ Papillary muscle dysfunction stenosis secondary to rheumatic fever but has no history of mitral
Þ Trauma regurgitation. She is currently taking medication for her mitral stenosis.
Þ Connective tissue disorders (Marfan) After a thorough PE and additional diagnostic tests, you find S.M. now has
Þ Rheumatoid arthritis pulmonary congestion aggravated by her pregnancy and present condition.
Þ Radiation injury Days passed and S.M.’s respiratory symptoms persisted and worsened.
Which surgical treatment may be done to best manage her current
o Anatomically normal valve (functional)
condition?
§ Elevated right ventricular systolic pressure (dilated annulus)
a) Mitral valvotomy
• Treatment Considerations
b) Mitral valve replacement
o Isolated TR, in the absence of pulmonary hypertension
c) Coronary angioplasty
§ Well-tolerated and does not require operation
d) NOTA
o Functional TR (secondary to pulmonary hypertension with MV disease)
§ Resolves with effective correction of the MV disease
o Annuloplasty
o Tricuspid valve replacement
§ For severely deformed valves
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 17 of 18
Which of the following is false about the etiology of aortic regurgitation. FREEDOM SPACE
a) It can arise from an active or recovered case of infective endocarditis
U can do this!
b) Due to the proximity of the aortic root, disorders of this anatomic
structure can cause aortic valve insufficiency
c) Aortic dissections at the level of the descending aorta can cause a
regurgitation.
d) It can be an age-related disease
Dr. Peppa Pig was checking to see if Ian Veneracion had an aortic stenosis.
What is FALSE about the process of diagnosing him?
a) His radiographic findings can present with a cardiac silhouette
resembling a LV hypertrophy.
b) She can order an ECG or 2D Echo to estimate the LV function and size.
c) It can be due to a congenital tricuspid valve with superimposed
calcification.
d) It is important to recognize when he presents an onset of symptoms
because patients rapidly deteriorate once they develop.
A patient comes to you saying she is often having shortness of breath even
when doing household chores that she had no problems doing before. She
reports frequent bouts of strep throat, especially when she was younger.
Otherwise, her history is unremarkable. Following your history-taking,
which clinical finding will best allow you to favor your initial impression?
a) Hearing a characteristic tumor-plop sound
b) Presence of right atrial and ventricular enlargement
c) Hearing an apical mid-diastolic murmur
d) Hearing a diastolic opening snap in the mitral area
Hearty B. (24/F) is pregnant and comes to the hospital for her routine
prenatal check-up. As she is about to leave her OB/GYN’s clinic, she feels
lightheaded and has to sit down. Dr. Paw, a cardiologist, sees her and asks
her if she is okay. She shares that she has been feeling lightheaded lately
and has been experiencing palpitation more often, as well as chest pains
every now and then. She says her mother has MVP and asks Dr. Paw if she
has it too. Which diagnostic test/s will he recommend Hearty to have done
in order to definitively say she has MVP as well?
a) Chest X-ray
b) ECG
c) Echo
d) AOTA
ANSWERS:
1A, 2C, 3C, 4D, 5C
EXPLANATIONS:
1. A. Mitral valvotomy – Mitral valvotomy is indicated for patients with severe
mitral stenosis with no or mild mitral regurgitation. In the case of the patient,
mitral valvotomy is also indicated for pregnant patients with severe MS when
pulmonary congestion occurs even after medical treatment.
2. C. Aortic dissections at the level of the descending aorta can cause a
regurgitation – For an aortic dissection to cause aortic regurgitation it must be
at the root or at the aortic arch, since those structures are much nearer to the
valve.
3. C. It can be due to a congenital tricuspid valve with superimposed
calcification – A principal cause of AS is a congenital bicuspid valve, not
tricuspid.
4. D. Hearing a diastolic opening snap in the mitral area – This is characteristic
of mitral stenosis, which follows the history and symptoms given. A is for left
atrial myxoma; B is for ASD; and C is for Aortic Regurgitation.
5. C. Echo – Compared to an ECG, An echocardiogram is more definitive and is
able demonstrate systolic displacement of mitral valve leaflets better as well
quantify MR and LV function
REFERENCES
REQUIRED
(1) Adriel E. Guerrero, MD, FPCP, FPCC. 09-03-21. Valvular Heart Disease
[Lecture slides].
2 ASMPH 2023. 02.10: Valvular Heart Disease by Adriel E. Guerrero, MD,
FPCP, FPCC.
SUPPLEMENTARY
: Armstrong, Guy P. “Pulmonic Regurgitation.” MSD Manual,
[https://www.msdmanuals.com/professional/cardiovascular-
disorders/valvular-disorders/pulmonic-regurgitation]. Accessed 02-09-
2021.
YL7: 02.12 CARDIOLOGY: Valvular Heart Diseases 18 of 18
You might also like
- Pamphlet 80 - Edition 4 - August 2014Document33 pagesPamphlet 80 - Edition 4 - August 2014Reza AranNo ratings yet
- KP 238 Tahun 2018 PDFDocument298 pagesKP 238 Tahun 2018 PDFAviation MedicineNo ratings yet
- Head and Neck AnatomyDocument115 pagesHead and Neck AnatomyMobarobber100% (11)
- Medicine Clinics Guide: Summary of Bates Tables From DR DominguezDocument226 pagesMedicine Clinics Guide: Summary of Bates Tables From DR DominguezSaf DicamNo ratings yet
- All ORE OSCEs PDFDocument123 pagesAll ORE OSCEs PDFAna100% (1)
- Nursing Care Plan PIHDocument2 pagesNursing Care Plan PIHLei Ortega100% (7)
- Pocket Reference For ECGs Made Easy 5th EditionDocument133 pagesPocket Reference For ECGs Made Easy 5th EditionSylvia Loong100% (2)
- Ecls GuidDocument24 pagesEcls GuidHanafieHeluthNo ratings yet
- Endogenous Cardiotonic SteroidsDocument30 pagesEndogenous Cardiotonic SteroidsSebastian NemethNo ratings yet
- (MED-HO) 02 Aplastic Anemia, AIHA, PVDocument23 pages(MED-HO) 02 Aplastic Anemia, AIHA, PVJolaine ValloNo ratings yet
- ESVS Thoracic Ds PDFDocument49 pagesESVS Thoracic Ds PDFFredy CarolNo ratings yet
- DHS Austere EMS Field GuideDocument298 pagesDHS Austere EMS Field GuideRicardo Luis Martin Sant'Anna100% (2)
- Infectious DiseasesDocument356 pagesInfectious DiseasesNormala Macabuntal SaripadaNo ratings yet
- Medical Science IDocument80 pagesMedical Science I常靓No ratings yet
- Screening For Aspiration Risk Associated With Dysphagia in Acute StrokeDocument105 pagesScreening For Aspiration Risk Associated With Dysphagia in Acute StrokealexandraNo ratings yet
- S16427e PDFDocument356 pagesS16427e PDFhuda ifandaNo ratings yet
- Macrolídeo e Ação ImunomoduladoraDocument30 pagesMacrolídeo e Ação ImunomoduladorajanainaNo ratings yet
- MMS Internal Medicine Treatment & ProtocolsDocument248 pagesMMS Internal Medicine Treatment & ProtocolsVeselin PapazovNo ratings yet
- Murillo de Oliveira Antunes 2020Document15 pagesMurillo de Oliveira Antunes 2020Asisten Lab TLPNo ratings yet
- Chronic PainDocument237 pagesChronic PainLeigh SalesNo ratings yet
- Epidemiology Lecture NoteDocument118 pagesEpidemiology Lecture Notepushpa devkotaNo ratings yet
- Classical Osteopathy PDFDocument400 pagesClassical Osteopathy PDFAnonymous yvlCvHw100% (6)
- 5 A4 Critical Care and Hospitalist Medicine Made Ridiculously SimpleDocument390 pages5 A4 Critical Care and Hospitalist Medicine Made Ridiculously Simpleepic sound everNo ratings yet
- Venous Thrombosis Guidelines 2021 1Document74 pagesVenous Thrombosis Guidelines 2021 1Mendoza Calderon DiegoNo ratings yet
- GOLD 2023 Ver 1.3 17feb2023 - WMV (008 008)Document1 pageGOLD 2023 Ver 1.3 17feb2023 - WMV (008 008)dian handayaniNo ratings yet
- Asthama in ElderlyDocument72 pagesAsthama in ElderlyboyzonerajNo ratings yet
- Guia Esvs Manejo Evc 2015Document60 pagesGuia Esvs Manejo Evc 2015Steeven Ruilova Valle100% (1)
- (DERMA) 01 Introduction To Dermatology (History and PE)Document8 pages(DERMA) 01 Introduction To Dermatology (History and PE)Jolaine ValloNo ratings yet
- ESC Guidance COVID 19 PandemicDocument119 pagesESC Guidance COVID 19 PandemicReka DrincalNo ratings yet
- 2018 SAM Protocol EnglishDocument166 pages2018 SAM Protocol EnglishMurtaza HamdardNo ratings yet
- Carotid ESVS 2018Document79 pagesCarotid ESVS 2018Ahmed ElmallahNo ratings yet
- FA ManualDocument346 pagesFA ManualbabudevanandNo ratings yet
- 051-Anaesthesia, Pharmacology, Intensive Care and Emergency a.P.I.C.E. - 23rd Annual Meeting-AntoDocument396 pages051-Anaesthesia, Pharmacology, Intensive Care and Emergency a.P.I.C.E. - 23rd Annual Meeting-AntoDita Retno Wulandari100% (1)
- Final Thesis. CWs - En.de - De.fr - Fr.enDocument81 pagesFinal Thesis. CWs - En.de - De.fr - Fr.enBeera InstituteNo ratings yet
- 1 Aa Tesis Aravena Roman Maximiliano 2015Document339 pages1 Aa Tesis Aravena Roman Maximiliano 2015iqyuwidya100% (1)
- Si 67-02 KP 238 Tahun 2018 Manual of Civil Aviation Medicine 1Document300 pagesSi 67-02 KP 238 Tahun 2018 Manual of Civil Aviation Medicine 1tan.mongieNo ratings yet
- 2014 Mrcs Osce RECALLDocument85 pages2014 Mrcs Osce RECALLIdo EgaziNo ratings yet
- ECG Measurements and Interpretation Programs: Physician's GuideDocument52 pagesECG Measurements and Interpretation Programs: Physician's GuideAnand M SNo ratings yet
- Training Guide To Trainers: Training Manual On Training of CahwsDocument69 pagesTraining Guide To Trainers: Training Manual On Training of CahwsDvm Abdi BuraaleNo ratings yet
- AHA ACC Test Ergo Met RicoDocument56 pagesAHA ACC Test Ergo Met RicoValentina VaccaroNo ratings yet
- History of MedicineDocument108 pagesHistory of MedicineAlexandra Constantin100% (2)
- Ingles 4 Tesis Abayomi SorinolaDocument154 pagesIngles 4 Tesis Abayomi SorinolaThe Almighty BelugaNo ratings yet
- CD 004929Document41 pagesCD 004929DylanNo ratings yet
- Cumulative Trauma Disorder (CTD) Medical Treatment GuidelinesDocument43 pagesCumulative Trauma Disorder (CTD) Medical Treatment GuidelinesAarthi ArumugamNo ratings yet
- Geophysical Methods To Detect Stress in Underground Mines: Report of Investigations/2004Document23 pagesGeophysical Methods To Detect Stress in Underground Mines: Report of Investigations/2004wypoNo ratings yet
- LabmanDocument754 pagesLabmanpsalminaNo ratings yet
- Flee Nor 2015Document67 pagesFlee Nor 2015Cosmin AndreiNo ratings yet
- Cardiovascular ImagingDocument401 pagesCardiovascular ImagingRani Mulia100% (5)
- Daftar IsiDocument1 pageDaftar IsiHiz AnNo ratings yet
- Borderline Manual Ol enDocument72 pagesBorderline Manual Ol enbasakerpolatNo ratings yet
- Lung CancerDocument31 pagesLung CancerFarhat KhanNo ratings yet
- 2023 CPG On The Management of Atherosclerotic Carotid and Vertebral Artery DiseaseDocument105 pages2023 CPG On The Management of Atherosclerotic Carotid and Vertebral Artery DiseaseElisa NovaesNo ratings yet
- Virulence: Factors in Escherichia Coli Urinary Tract InfectionDocument49 pagesVirulence: Factors in Escherichia Coli Urinary Tract InfectionD Wisam NajmNo ratings yet
- Finalversion 091105 RFDocument135 pagesFinalversion 091105 RFAbdulai FofanaNo ratings yet
- CDC 52472 DS1Document164 pagesCDC 52472 DS1Lorens LaubanNo ratings yet
- Saggital Module Skull BaseDocument84 pagesSaggital Module Skull BaseAnoop SinghNo ratings yet
- Timothy Report AttachmentDocument25 pagesTimothy Report AttachmentFrancis OtienoNo ratings yet
- On-X® Mitral Heart ValveDocument20 pagesOn-X® Mitral Heart ValveChaitanya Sai TNo ratings yet
- Labour LawDocument135 pagesLabour LawSathish ChokkalingamNo ratings yet
- Handbook of Dental Hygienist (PDFDrive)Document523 pagesHandbook of Dental Hygienist (PDFDrive)neetika guptaNo ratings yet
- (02.05) CM Cardiovascular Nutrition (TG13) - FINAL - Andrea Maxine CajucomDocument14 pages(02.05) CM Cardiovascular Nutrition (TG13) - FINAL - Andrea Maxine CajucomMikmik DGNo ratings yet
- (02.29) Pediatric Cardiac Catheterization (TG16) - Noelle Jiyana SingsonDocument9 pages(02.29) Pediatric Cardiac Catheterization (TG16) - Noelle Jiyana SingsonMikmik DGNo ratings yet
- (02.02) CM Diagnosis of Cardiovascular Disease (TG10) - Jonaz NazarenoDocument15 pages(02.02) CM Diagnosis of Cardiovascular Disease (TG10) - Jonaz NazarenoMikmik DGNo ratings yet
- (02.28) PD Cyanotic Congenital Heart Diseases (Tg15) Final - Matthew Ethan AngDocument13 pages(02.28) PD Cyanotic Congenital Heart Diseases (Tg15) Final - Matthew Ethan AngMikmik DGNo ratings yet
- (02.18) SU Surgical Diseases of The Pericardium - Neil Andrew AliazasDocument8 pages(02.18) SU Surgical Diseases of The Pericardium - Neil Andrew AliazasMikmik DGNo ratings yet
- (02.09) CM Ventricular Tachyarrhythmias (TG17) - Rene Martin ElefanteDocument10 pages(02.09) CM Ventricular Tachyarrhythmias (TG17) - Rene Martin ElefanteMikmik DGNo ratings yet
- (02.23) CM Peripheral Arterial Occlusive Disease (Tg9) - Final - Navin John Pasia - Navin John PasiaDocument19 pages(02.23) CM Peripheral Arterial Occlusive Disease (Tg9) - Final - Navin John Pasia - Navin John PasiaMikmik DGNo ratings yet
- (02.22b) CM Diseases of The Aorta 2 (TG8) - Morvenn Chaimek C. BertizDocument5 pages(02.22b) CM Diseases of The Aorta 2 (TG8) - Morvenn Chaimek C. BertizMikmik DGNo ratings yet
- (02.21b) Im Congestive Heart Failure 2 (Tg6) - Arielle Dana YaoDocument7 pages(02.21b) Im Congestive Heart Failure 2 (Tg6) - Arielle Dana YaoMikmik DGNo ratings yet
- (02.31) PA Introduction and Physiology of Pain (TG18) Final - Martin DionesDocument13 pages(02.31) PA Introduction and Physiology of Pain (TG18) Final - Martin DionesMikmik DGNo ratings yet
- (02.27) PD Acyanotic Congenital Heart Disease (Tg14) - Final - Janel Zahra RasulDocument8 pages(02.27) PD Acyanotic Congenital Heart Disease (Tg14) - Final - Janel Zahra RasulMikmik DGNo ratings yet
- (02.21a) CM Congestive Heart Failure 1 (TG 5) - Ervin Kyle CerezoDocument9 pages(02.21a) CM Congestive Heart Failure 1 (TG 5) - Ervin Kyle CerezoMikmik DGNo ratings yet
- (02.20) CM Cardiomyopathy and Myocarditis (TG4) - ANA CARMINA LIBERATODocument12 pages(02.20) CM Cardiomyopathy and Myocarditis (TG4) - ANA CARMINA LIBERATOMikmik DGNo ratings yet
- (02.22a) CM Diseases of The Aorta 1 (TG7) - Jose Gabriel OrdinalDocument13 pages(02.22a) CM Diseases of The Aorta 1 (TG7) - Jose Gabriel OrdinalMikmik DGNo ratings yet
- (02.14) SU Surgical Management of Valvular Heart Disease (TG 22) - Joseph Paul RiveraDocument15 pages(02.14) SU Surgical Management of Valvular Heart Disease (TG 22) - Joseph Paul RiveraMikmik DGNo ratings yet
- (02.30) SU Surgical Management of Congenital Heart Diseases (TG17) - Rene Martin ElefanteDocument12 pages(02.30) SU Surgical Management of Congenital Heart Diseases (TG17) - Rene Martin ElefanteMikmik DGNo ratings yet
- (02.16) PC SGD Anti-Hypertensives (TG24) - MA. GLORIA SALAPANTANDocument7 pages(02.16) PC SGD Anti-Hypertensives (TG24) - MA. GLORIA SALAPANTANMikmik DGNo ratings yet
- (02.03) RD Cardiovascular Radiology (TG11 - John Edward BallelosDocument22 pages(02.03) RD Cardiovascular Radiology (TG11 - John Edward BallelosMikmik DGNo ratings yet
- (06.08) Quantitative Study Designs Observational Studies (TG18-CG6) - FINAL - Martin DionesDocument11 pages(06.08) Quantitative Study Designs Observational Studies (TG18-CG6) - FINAL - Martin DionesMikmik DGNo ratings yet
- (02.07) CM Bradycardias (Tg15) - Matthew Ethan AngDocument10 pages(02.07) CM Bradycardias (Tg15) - Matthew Ethan AngMikmik DGNo ratings yet
- 01.25.01 Principles of Pharmacokinetics - Absorption and DistributionDocument10 pages01.25.01 Principles of Pharmacokinetics - Absorption and DistributionMikmik DGNo ratings yet
- (06.05) Data Privacy Act and Its Implication To Research (TG15-CG3) - Final - MATTHEW ETHAN ANGDocument7 pages(06.05) Data Privacy Act and Its Implication To Research (TG15-CG3) - Final - MATTHEW ETHAN ANGMikmik DGNo ratings yet
- (06.01) Introduction To Statistics and Statistical Inference (TG11-CG23) - Final - Deanna Flor LimDocument11 pages(06.01) Introduction To Statistics and Statistical Inference (TG11-CG23) - Final - Deanna Flor LimMikmik DGNo ratings yet
- 01.20.01 Pharmacodynamics 2 - Mechanisms of Drug ActionDocument11 pages01.20.01 Pharmacodynamics 2 - Mechanisms of Drug ActionMikmik DGNo ratings yet
- 01.24.01 SIM On Mechanisms of Drug ActionDocument13 pages01.24.01 SIM On Mechanisms of Drug ActionMikmik DGNo ratings yet
- (06.07) Principles of Validity and Reliability (TG17-CG5) FINAL - SHEREE BIANNE-THA NOLEEN MENDEZDocument6 pages(06.07) Principles of Validity and Reliability (TG17-CG5) FINAL - SHEREE BIANNE-THA NOLEEN MENDEZMikmik DGNo ratings yet
- 01.22.01 General Overview To RadiologyDocument11 pages01.22.01 General Overview To RadiologyMikmik DGNo ratings yet
- (06.12) Data Management and Analysis (TG22-CG10) - Final - Mikaela Kate RamirezDocument15 pages(06.12) Data Management and Analysis (TG22-CG10) - Final - Mikaela Kate RamirezMikmik DGNo ratings yet
- FinMan - Dionisio - DavidEmmanuel - Midterm PaperDocument2 pagesFinMan - Dionisio - DavidEmmanuel - Midterm PaperMikmik DGNo ratings yet
- 01.19.01 General Concepts in Parasitology 1-4Document7 pages01.19.01 General Concepts in Parasitology 1-4Mikmik DGNo ratings yet
- Heart and Circulation ExercisesDocument3 pagesHeart and Circulation ExercisesHanaOmarNo ratings yet
- Ninja NerdDocument3 pagesNinja NerdSalsabila HMNo ratings yet
- Preoperative Cardiac Risk Assessment in Noncardiac SurgeryDocument6 pagesPreoperative Cardiac Risk Assessment in Noncardiac SurgeryOgbonnaya IfeanyichukwuNo ratings yet
- Chapter 2 - Clinical Cardiovascular Examination-2Document43 pagesChapter 2 - Clinical Cardiovascular Examination-2sarahya.medinaNo ratings yet
- Abdominal Aortic Aneurysm 2Document22 pagesAbdominal Aortic Aneurysm 2Kendy Rizky HadyanNo ratings yet
- Lecture On Hemodynamic and Thromboembolic DisordersDocument77 pagesLecture On Hemodynamic and Thromboembolic DisordersCharmaine Torio PastorNo ratings yet
- Reversible Cerebral Vasoconstriction SyndromeDocument6 pagesReversible Cerebral Vasoconstriction SyndromeKashifNo ratings yet
- Peripheral Arterial DiseaseDocument40 pagesPeripheral Arterial Diseaseuseofforcelaw100% (1)
- (UMA) ERBA XL-640 Basic Performance DataDocument38 pages(UMA) ERBA XL-640 Basic Performance DataKo KyoNo ratings yet
- Lippincott Antiarrhythmics 7Document2 pagesLippincott Antiarrhythmics 7Wijdan HatemNo ratings yet
- Manajemen Perioperatif Pada Hipertensi WORDDocument16 pagesManajemen Perioperatif Pada Hipertensi WORDIan MatatulaNo ratings yet
- Myocardial Infarction. BPTDocument62 pagesMyocardial Infarction. BPTAanchal GuptaNo ratings yet
- Myocardial Infarction Midterm Case StudyDocument24 pagesMyocardial Infarction Midterm Case StudyReizel GaasNo ratings yet
- Pengetahuan, Sikap, Dan Perilaku Terhadap Pencegahan Serta Penanggulangan Hipertensi Di Kabupaten BogorDocument9 pagesPengetahuan, Sikap, Dan Perilaku Terhadap Pencegahan Serta Penanggulangan Hipertensi Di Kabupaten BogorIntan OktavianiNo ratings yet
- Heart AttackDocument18 pagesHeart AttackKhalifullahNo ratings yet
- 01 Critical Care IV Drug Infusions - AdultDocument33 pages01 Critical Care IV Drug Infusions - Adultdoc_gelo100% (1)
- NSG 6001 Final Exam 1 - Question and AnswersDocument49 pagesNSG 6001 Final Exam 1 - Question and AnswersDAVIDNo ratings yet
- Health Talk On HypertensionDocument8 pagesHealth Talk On HypertensionSHUBHENDU SHANDILYANo ratings yet
- Workbook - A Guide To The Vascular SystemDocument202 pagesWorkbook - A Guide To The Vascular SystemDenis PogoreviciNo ratings yet
- Uptodates1748681521000243 Pdfdownload True PDFDocument17 pagesUptodates1748681521000243 Pdfdownload True PDFAhmad AshammeryNo ratings yet
- Graphic OrganizerDocument1 pageGraphic OrganizerKenshin MedinaNo ratings yet
- Pathology of Blood VesselsDocument80 pagesPathology of Blood VesselsiqiqiqiqiqNo ratings yet
- Labelling The Human HeartDocument6 pagesLabelling The Human Heartchinpy088464No ratings yet
- CIRCULATORYDocument20 pagesCIRCULATORYDannica Trisha CrisostomoNo ratings yet
- Programbook IsicamDocument36 pagesProgrambook Isicamadi bestaraNo ratings yet
- Nihms 1931223Document17 pagesNihms 1931223reymistery10No ratings yet
- Heart PDFDocument48 pagesHeart PDFdr.chetan2385No ratings yet
- Bio Lab 11Document5 pagesBio Lab 11Sarah JaglalNo ratings yet