Professional Documents
Culture Documents
Asma 5
Asma 5
Uploaded by
abdi syahputraOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Asma 5
Asma 5
Uploaded by
abdi syahputraCopyright:
Available Formats
Journal of Asthma and Allergy
ISSN: (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/djaa20
Organization, Clinical and Management Indicators
on the First Year of Activity of an Outpatient Clinic
Dedicated to the Diagnosis and Treatment of
Severe Asthma in Italy
Silvia Tognella, Claudio Micheletto, Alessandro Roggeri, Guido Polese, Denise
Artioli, Gianenrico Senna, Marco Caminati & Daniela Paola Roggeri
To cite this article: Silvia Tognella, Claudio Micheletto, Alessandro Roggeri, Guido Polese,
Denise Artioli, Gianenrico Senna, Marco Caminati & Daniela Paola Roggeri (2021) Organization,
Clinical and Management Indicators on the First Year of Activity of an Outpatient Clinic
Dedicated to the Diagnosis and Treatment of Severe Asthma in Italy, Journal of Asthma and
Allergy, , 1011-1018, DOI: 10.2147/JAA.S309740
To link to this article: https://doi.org/10.2147/JAA.S309740
© 2021 Tognella et al. Published online: 30 Nov 2022.
Submit your article to this journal Article views: 9
View related articles View Crossmark data
Citing articles: 1 View citing articles
Full Terms & Conditions of access and use can be found at
https://www.tandfonline.com/action/journalInformation?journalCode=djaa20
Journal of Asthma and Allergy Dovepress
open access to scientific and medical research
Open Access Full Text Article
ORIGINAL RESEARCH
Organization, Clinical and Management Indicators
on the First Year of Activity of an Outpatient
Clinic Dedicated to the Diagnosis and Treatment
of Severe Asthma in Italy
Silvia Tognella 1 Purpose: A Regional Technical Commission was set in 2017 by Veneto region (Italy) to
Claudio Micheletto 2 provide opinions and recommendations on drug prescriptions and to implement treatment-
Alessandro Roggeri 3 pathway guidelines for severe asthma. In this observational study, we describe the first structured,
Guido Polese 4 integrated, multidisciplinary, patient-centered outpatient clinic for the care of severe-asthma
patients in Italy, and characterize patients referring to the center for specialist visits.
Denise Artioli 1
Patients and Methods: To characterize patients that accessed the outpatient clinic in 2018,
Gianenrico Senna 5
data on demographic characteristics, treatments, severity of asthma, phenotypes, and relevant
Marco Caminati 5,6
comorbidities by phenotype were collected. Use of biologic agents and indicators of the
Daniela Paola Roggeri 3 performance of the outpatient clinic were described.
1
Pulmonology Unit, Mater Salutis Results: A structured multidisciplinary outpatient pathway for taking charge of patients and
Hospital, Legnago (Verona), Italy;
2 for administration and monitoring of biological agents was developed. A total of 146 patients
Pulmonology Unit, Azienda Ospedaliera
Universitaria Integrata, Verona, Italy; accessed the outpatient clinic in 2018: 62.3% had uncontrolled asthma upon admission and
3
ProCure Solutions, Nembro, Bergamo, 27.4% were already being treated with biologic agents. Among patients with uncontrolled
Italy; 4Pulmonology Unit, Magalini
Hospital, Villafranca (Verona), Italy;
asthma, 66% had severe uncontrolled asthma, 22% had moderate–severe uncontrolled
5
Asthma Center and Allergy Unit, Verona asthma, and 12% had mild–moderate uncontrolled asthma. Main asthma phenotypes in
University Hospital, Verona, Italy; uncontrolled-asthma patients were allergic (58% of patients), eosinophilic (22%), allergic
6
Department of Medicine, Allergy and
Clinical Immunology Section, University plus eosinophilic (10%) and non-atopic asthma (10%). Among patients affected by severe
of Verona and Verona University asthma, 47% had allergic asthma, 28% had eosinophilic asthma, 13% had allergic plus
Hospital, Verona, 37134, Italy eosinophilic asthma, and 12% had non-atopic asthma. Nasal polyps were more frequent in
eosinophilic and allergic plus eosinophilic asthma, while gastro-esophageal reflux disease
was more frequent in non-atopic asthma.
Conclusion: This structure of an outpatient clinic for the treatment of severe asthma, with
its dedicated pathway and multidisciplinary approach, may allow a stricter control of asthma
and optimization of therapies, as well as minimization of drug misuse.
Keywords: asthma, severe, multidisciplinary, outpatient
Introduction
Asthma, a major noncommunicable disease, affected in 2019 262 million persons and is
Correspondence: Alessandro Roggeri responsible of 461,000 deaths. Asthma affects both children and adults and represents
ProCure Solutions, Via Camozzi 1/C,
Nembro, 24027, BG, Italy the most frequent chronic disease in children.1,2 It is a chronic inflammatory disorder of
Tel +39 035 521121 the airways caused by an interaction between genetic factors and environmental factors.
Email alessandro.
roggeri@procuresolutions.it Asthma is characterized by widespread, variable, and reversible airflow obstruction,
Journal of Asthma and Allergy 2021:14 1011–1018 1011
Received: 18 May 2021 © 2021 Tognella et al. This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.
Accepted: 27 July 2021 php and incorporate the Creative Commons Attribution – Non Commercial (unported, v3.0) License (http://creativecommons.org/licenses/by-nc/3.0/). By accessing the
work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For
Published: 13 August 2021 permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms (https://www.dovepress.com/terms.php).
Tognella et al Dovepress
airway inflammation, excessive production of mucus, and asthma a common pathophysiological mechanism, affect
airway hyper-responsiveness. These features lead to recurrent the control of the pathology, its phenotype and treatment
episodes of wheezing, breathlessness, chest tightness, and response. The most frequent co-morbidities are rhinitis,
coughing.3 sinusitis, gastroesophageal reflux disease, obstructive
Asthma can have several phenotypes4,5 driven by mul sleep apnea, hormonal disorders, and
tiple underlying disease processes. A different etiology of psychopathologies.23,24
inflammation in asthma can be associated with a different Long-term use of OCs is associated, in addition to
response to asthma treatments.6 psychological side-effects, with adverse effects: obesity,
Asthma presents with varying degrees of severity, ran diabetes mellitus, osteoporosis, cataracts, hypertension,
ging from mild, intermittent disease to severe presenta and adrenal suppression,25,26 Even short-term use of OCs
tions with debilitating (even life-threatening) symptoms. can lead to sleep disturbance, increased risk of infection,
Asthma is considered to be “severe” if it is uncontrolled bone fracture, and thromboembolism.27,28 Strategies to
despite adherence to maximal therapy or worsened with minimize OC need are, therefore, a high priority.
step-down of high-dose treatments.7 Severe asthma affects An outpatient clinic structured with a dedicated path
only a minority of all asthma patients, and prevalence can way and multidisciplinary team for the treatment of severe
vary from country-to-country, due largely to variation asthma can provide complete services and allow the opti
between clinical and epidemiological definitions.8,9 mization of asthma treatment and outcomes. Besides the
To be classified as having “severe asthma”, patients adequate clinical control of severe asthma, in order to meet
treated with the maximum dose of inhalation therapy patient needs and optimization of management within
should be assessed appropriately in a specialist setting to a landscape of limited resources, a specific pathway for
confirm the diagnosis, evaluate comorbidities and their the care of adult patients affected by severe bronchial
management, as well as to assess the level of adherence asthma was implemented in the Local Health Unit
to therapy and inference of environmental factors.7,10–12 “ULSS9 Scaligera” in Veneto, Italy.
Severe asthma is estimated to affect about 3–10% of Foreseeing the evolution of therapeutic approaches
asthma patients: despite such a small percentage of the against severe asthma and upcoming marketing authorization
population, total expenditure accounts for >60% of the of a new class of monoclonal antibodies, in 2016 the Veneto
total costs attributed to asthma.7,13,14 Most asthma Region highlighted the need for pharmacological manage
patients can be cared for adequately based on global ment of severe asthma to define (i) therapeutic alternatives
guidelines (ie, Global Initiative for Asthma (GINA); according to the literature; (ii) criteria for selecting patients
Global Strategy for Asthma Management and who could benefit from new drug therapies; (iii) indicators
Prevention). Nevertheless, a subpopulation of patients for monitoring the appropriateness of prescriptions.
with severe asthma will not be treated adequately with In this observational study, we aimed to describe the first
the current standard of care despite the availability of structured, integrated, multidisciplinary, patient-centered
therapies reported as being “highly efficacious” in clinical outpatient clinic for the clinical management of severe
trials,15,16 and their treatment remains an important unmet asthma in Italy. We also aimed to characterize severe-
need.17 asthma patients referred to the outpatient clinic for specialist
Observational studies carried out in Italy have esti visits. The purpose of the outpatient clinic was to create an
mated suboptimal control of asthma to affect ~35% of optimized treatment pathway for the entire ULSS (local
asthma patients.18–20 Two real-world studies in Italy Health Unit) to meet regional goals. The treatment pathway
revealed that the prevalence of severe uncontrolled asthma was approved by the General Manager Health and Social
ranged from 0.025% (Veneto Region, based on Care Veneto Region and the results of the first year of
a population aged >6 years)20 to 0.04% (based on an activity are presented here following.
adult subpopulation).21 Patients with severe uncontrolled
asthma carry a high risk of severe exacerbations and Materials and Methods
mortality, and are often dependent upon oral corticoster This was a retrospective cohort study based on real-world,
oids (OCs).22 patient-level results from the database of asthma outpatient
Asthma is frequently associated with several comorbid clinics of ULSS 9 Scaligera. We evaluated the organiza
ities and concomitant conditions that may share with tion of the Pulmonology Unit of Bussolengo/Villafranca in
1012 https://doi.org/10.2147/JAA.S309740 Journal of Asthma and Allergy 2021:14
DovePress
Powered by TCPDF (www.tcpdf.org)
Dovepress Tognella et al
Verona Azienda (ULSS 9 Scaligera) and its performance hypothesis was not specified because this was not an
for the first year of activity (2018). The innovative struc analytical study. General descriptive statistics for contin
ture of the ambulatory unit and specific pathways for new uous numerical variables were the number of observations,
and consolidated patients are described. the mean, and the standard deviation. For categorical vari
We wished to characterize patients who accessed the ables, the proportion of patients with a certain event/char
outpatient clinic during 2018. Hence, data on demographic acteristic are presented.
characteristics (age, sex), treatments, asthma severity, spe
cific phenotypes according to the assessment of the treat Results
ing physician (allergic asthma, eosinophilic asthma, non- The outpatient clinic aimed, through a multidisciplinary
allergic asthma, mixed phenotype) and relevant comorbid and integrated approach, to (i) provide the correct diagno
ities by phenotype were collected. Moreover, the origin of sis; (ii) identify the most suitable pharmacological therapy;
the patients accessing the outpatient clinic is reported (eg, (iii) undertake specialist monitoring personalized accord
Emergency Room, Intensive Care Unit). ing to the need of each adult patient with severe asthma.
To describe ambulatory activities in 2018, the health
care resources analyzed were specialist visits, diagnostic
examinations, and drug prescriptions. Patients with uncon
Outpatient Pathways and Organization
The outpatient clinical pathway for a patient with severe
trolled asthma accessed the outpatient clinic irrespective of
asthma, and the clinical pathway for the administration
asthma severity, so the overall population and population
and monitoring of biological therapies for a patient with
of patients with severe asthma are described separately.
severe asthma, are described in Figures 1 and 2,
Finally, use of biologic agents and indicators of perfor
respectively.
mance are described.
Organization of the diagnostic, therapeutic, and medi
Three main indicators allowed evaluation of the degree
cal-assistance pathways involved the outpatient clinic of
of achievement with respect to the declared objective.
the Pulmonology Unit, Respiratory Pathophysiology Unit,
Indicator 1 was (number of patients taken in charge/total
Allergy Unit, as well as the hospital pharmacy, booking
number of patients evaluated) × 100; the expected value
center of the outpatient clinic.
was ≥70%. Indicator 2 was (number of patients treated
To manage the associated diseases, the following
with biologic agents/total number of patients taken in
departments were involved (if needed): Ear, Nose and
charge) × 100; the expected value was ≥50%. Indicator 3
Throat; Gastrointestinal; Rheumatology; Laboratory
was (number of patients with suspension of OC use/num
Testing. Outpatient clinics from the Department of
ber of patients treated with biologic agents) × 100; the
Clinical Psychology and dietary services were available
expected value was ≥50%.
on demand to offer additional support to patients.
This manuscript reviewed and describe the center
During 2018, the outpatient clinic of Pulmonology Unit
activities in order to present the new organization of the
of Bussolengo/Villafranca undertook: 424 visits by pneu
outpatient clinic that was established by a Veneto Regional
mologists to control asthma; four first visits by pneumol
Law (Law Decree n.54 2018 and Law Decree n.85 2018).
ogists; three evaluations of exhaled gas; 393
All patients accessing the outpatient ambulatory signed the
measurements of simple/global spirometry; 649 adminis
informed consent to the treatment and collection of sani
trations of biologic agents (at the moment of starting this
tary routine data as forecasted by the European General
outpatient structure only omalizumab and mepolizumab
Data Protection Regulation (GDPR) (2016/679), Law
were available and reimbursed by Italian National Health
Decree 196/2003 (Italian legal rules regarding the protec
Service (NHS)).
tion of personal data that specifically includes the manage
ment and evaluation of activities of the outpatient clinic
and epidemiology and scientific research activities) inte Description of Outpatient Clinic
grated with Law Decree 10/08/2018 nr 101; only data Activities
covered by reported laws were collected and presented in A total of 146 patients accessed the outpatient clinic in
aggregated and anonymous way. 2018. Among them, 91 (62.3%) had uncontrolled asthma
All patients who accessed Pulmonology Unit of upon admission, 40 (27.4%) were already being treated
Bussolengo/Villafranca in 2018 were evaluated. A formal with biologic agents, and 10 (10.3%) were discharged with
Journal of Asthma and Allergy 2021:14 https://doi.org/10.2147/JAA.S309740
1013
DovePress
Powered by TCPDF (www.tcpdf.org)
Tognella et al Dovepress
Figure 1 Outpatient clinical pathway for a patient with severe asthma.
a different diagnosis. The average age of patients with asthma, and 11 (12%) had mild–moderate uncontrolled
uncontrolled asthma was 53.8 ± 16.9 years, and 64.5% asthma.
were men. Among patients with uncontrolled asthma, 76 (84%)
Following GINA definitions, out of the 91 patients were referred from a first-level outpatient clinic, four (4%)
with uncontrolled asthma who accessed the outpatient from the intensive care unit (after hospital admission
clinic, 60 (66%) were affected by severe uncontrolled caused by atopic uncontrolled asthma), six (7%) from
asthma, 20 (22%) had moderate–severe uncontrolled hospital admission due to respiratory failure, and four
1014 https://doi.org/10.2147/JAA.S309740 Journal of Asthma and Allergy 2021:14
DovePress
Powered by TCPDF (www.tcpdf.org)
Dovepress Tognella et al
Figure 2 Clinical pathway for the administration and monitoring of biological therapies for a patient with severe asthma.
(4%) from the Emergency Department; one patient was 28 (47%) had allergic asthma, 17 (28%) had eosinophilic
pregnant. asthma, eight (13%) had allergic plus eosinophilic asthma,
The most frequently reported diagnosis was allergic and seven (12%) had non-atopic asthma.
asthma in 53 (58%) cases (average age, 49 ± 17.5 years), Nasal polyps were more frequent in eosinophilic and
eosinophilic asthma in 20 (22%) patients (58.8 ± 13.7 allergic plus eosinophilic asthma, while gastro-esophageal
years), allergic plus eosinophilic asthma in nine (10%) reflux disease was more frequent in non-atopic asthma.
cases (60.8 ± 10.1 years) and non-atopic asthma in nine Overall, 36.6% of cases with severe asthma met the
(10%) patients (69 ± 10.5 years). The prevalence of criteria for use of biologic agents: 29% had the allergic
comorbidities by asthma phenotype is described in phenotype, 53% had the eosinophilic phenotype, and 63%
Figure 3. had the allergic plus eosinophilic phenotype. Among
Among the 60 patients affected by the “severe” phe patients treated with biologic agents, 86.2% discontinued
notype (61.6% females; average age, 56.2 ± 15.2 years), OC use.
Journal of Asthma and Allergy 2021:14 https://doi.org/10.2147/JAA.S309740
1015
DovePress
Powered by TCPDF (www.tcpdf.org)
Tognella et al Dovepress
Figure 3 Prevalence of comorbidities by asthma phenotype.
Abbreviations: GERD, gastro-esophageal reflux disease; COPD, chronic obstructive pulmonary disease, COPD.
Discussion patients with suspected severe asthma operating with phy
Severe uncontrolled asthma carries a substantial burden in sicians and nurses already trained in the management of
terms of severely impaired quality of life and a significant this pathology allowing patients a dedicated access to the
economic impact. A real-world study in Italy recently structure and reduction of waiting lists.
showed the average cost per patient per year (excluding Within the population that was followed in the
pharmacological treatments) to be €3701; pharmacological first year of the clinic, the allergic phenotype is con
treatments costs range from €138 to >€17,000.29 firmed to be predominant (58%), and with an appar
Moreover, corticosteroids shadow costs, due to OCs- ently lower average age than the other phenotypes.
induced morbidity, range from 45% to 30%.30 Persistent and significant eosinophilia was found in
Maintenance of asthma control is expected to reduce the only 10% of patients suffering of allergic asthma,
overall economic impact of asthma as well as the indirect while 22% of patients affected by non-allergic asthma
costs associated with decreased productivity of the could be diagnosed as an eosinophilic phenotype.
affected patients. A small proportion of subjects (9/91 patients) were
The innovative structure of the outpatient clinic found to be affected by non-allergic asthma and with
described here allowed a dedicated treatment pathway for out eosinophils, thus being able to fall into the more
each specific phenotype of severe asthma. It allowed dif generic category of “intrinsic” asthma, characterized by
ferent modalities to be used and scheduling of clinical a significantly higher average age of allergic asth
evaluations compared with that observed in most outpati matics. The importance of evaluating the nasal poly
ent clinics in Italy. Particularly, compared with the stan posis-asthma association is confirmed which was found
dard pulmonology outpatient clinics of the Italian NHS, to be mainly associated with the eosinophilic pheno
the one presented in this manuscript is dedicated only to type compared to the purely atopic one.
1016 https://doi.org/10.2147/JAA.S309740 Journal of Asthma and Allergy 2021:14
DovePress
Powered by TCPDF (www.tcpdf.org)
Dovepress Tognella et al
A small percentage of patients (12%) was diagnosed personalization of pharmacological treatment thanks to iden
with mild-moderate asthma and the inclusion in the dedi tification of the asthma phenotype. This strategy avoided
cated pathway made it possible to achieve control of inappropriate immediate use of biologic agents, chronic
asthma symptoms and to return the patient to the first use of high doses of OCs, and allowed optimization of
level outpatient clinic. pharmacological treatment. Even for severe-asthma patients,
The assessment of the first year of activity of the clinic identification of the phenotype and regular follow-up
showed a substantial adequacy of the referral of patients allowed correct decisions on initiation of biologic-agent
by the referring specialists; in fact, only 15 patients were therapy (as per GINA recommendations) to be made.
discharged from the clinic with another diagnosis and 91 Moreover, patients had regular contact with specialist
patients had uncontrolled asthma at the time of the first physicians and dedicated nurses. This availability contrib
assessment in the clinic. uted to improvement in compliance with treatment and the
Most (77/91 patients) of the patients came from first possibility of step-down of supportive treatment (eg, OCs).
level specialist outpatient clinics. The other patients were In the future, optimization of use of healthcare resources
referred for evaluation at the outpatient clinic after serious can be estimated to evaluate the performance of the inte
acute events requiring hospitalization in intensive care unit grated and multidisciplinary approach of this outpatient
(4 patients, all subjects with uncontrolled atopic bronchial clinic.
asthma), after an ordinary hospitalization due to respira
tory failure (6 patients) and after accessing to emergency Conclusion
department (4 patients). All this confirms, once again, that The new structure of the outpatient clinic ULSS 9
despite the wide availability of treatments, and the ease of Scaligera for the treatment of severe asthma is based on
access to treatment in Italy, asthma remains a potentially a dedicated pathway and a multidisciplinary approach.
life-threatening pathology. This structure allowed strict control of patients and opti
For 60 patients (66%) it was possible to conclude the mization of pharmacological treatment with the potential
course proposed by the guidelines during the year of of better control of asthma and minimization of drug
observation and to effectively diagnose severe asthma, misuse.
while 20 subjects (22%) remained under close monitoring
with a diagnosis of moderate asthma-severe “difficult to
Funding
control”
Financial support for manuscript preparation was provided
In the organizational reality of first level clinic, waiting
by AstraZeneca. The latter had no role in the study design,
lists and booking difficulties would not have allowed the
collection/analysis/interpretation of data, writing of the
above results to be achieved. Thanks to the project
report, or the decision to submit the manuscript for
described here, with the use of dedicated medical and
publication.
nursing staff, it was possible to guarantee access to spe
cific planning for patients in the clinic, to closely monitor
subject in times established by the therapeutic changes but
Disclosure
AR and DPR are consultants for AstraZeneca. ST is
also to quickly guarantee re-evaluations if exacerbations
speaker for and reports personal fees from Chiesi and
occur.
GSK, outside the submitted work. CM received fees as
This type of structure permitted correct identification
a speaker in local, national and international congress by
of severe-asthma patients and enabled their evaluation
GSK, AstraZeneca, Sanofi, and Novartis. DA reports
through specific indicators. Once a patient had been diag
grants from Aipo Ricerche, Chiesi, and Menarini, during
nosed with severe asthma and the specific phenotype had
the conduct of the study. The authors report no other
been identified though characterization, the most appropri
conflicts of interest in this work.
ate treatment (according to GINA recommendations) was
prescribed. Subsequently, patients were re-evaluated peri
odically for dose adjustments/changes and check on con References
trol of comorbidities. 1. Vos T, Lim SS, Abbafati Cet al. Global burden of 369 diseases and
injuries in 204 countries and territories, 1990–2019: a systematic
The outpatient clinic also accepted patients with uncon analysis for the global burden of disease study 2019. Lancet.
trolled asthma of different severity. It allowed 2020;396(10258):1204–1222.
Journal of Asthma and Allergy 2021:14 https://doi.org/10.2147/JAA.S309740
1017
DovePress
Powered by TCPDF (www.tcpdf.org)
Tognella et al Dovepress
2. World Health Organization.WHO factsheets on Asthma. Available 19. Bettoncelli G, Magnoni MS, Fassari C, et al. Il controllo dell’asma in
from https://www.who.int/news-room/fact-sheets/detail/asthma. Italia misurato con ACT (Asthma Control Test). Società Italiana di
Accessed July 29, 2021. Medicina Generale. 2006;6:10–17.
3. Pascual RM, Peters SP. Airway remodeling contributes to the progressive 20. Vianello A, Caminati M, Andretta M, et al. Prevalence of severe
loss of lung function in asthma: an overview. J Allergy Clin Immunol. asthma according to the drug regulatory agency perspective: an
2005;116(3):477–486;quiz 487. doi:10.1016/j.jaci.2005.07.011 Italian experience. World Allergy Organ J. 2019;12(4):100032.
4. Simpson JL, Scott R, Boyle MJ, Gibson PG. Inflammatory subtypes in doi:10.1016/j.waojou.2019.100032
asthma: assessment and identification using induced sputum. 21. Pedrini A, Rossi E, Calabria S, et al. Current management of severe
Respirology. 2006;11(1):54–61. doi:10.1111/j.1440-1843.2006.00784.x refractory asthma in Italy: analysis of real-world data. Glob Reg
5. Hancox RJ, Cowan DC, Aldridge RE, et al. Asthma phenotypes: Health Technol Assess. 2017;4(1):e216–e220. doi:10.5301/
consistency of classification using induced sputum. Respirology. grhta.5000273
2012;17(3):461–466. doi:10.1111/j.1440-1843.2011.02113.x 22. Accordini S, Bugiani M, Arossa W, et al. Poor control increases the
6. Douwes J. Non-eosinophilic asthma: importance and possible economic cost of asthma. A multicentre population-based study.
mechanisms. Thorax. 2002;57(7):643–648. doi:10.1136/thorax.57.7.643 Int Arch Allergy Immunol. 2006;141(2):189–198. doi:10.1159/
7. Chung KF, Wenzel SE, Brozek JR, et al. International ERS/ATS 000094898
guidelines on definition, evaluation and treatment of severe asthma. 23. Poddighe D, Brambilla I, Licari A, Marseglia GL. Pediatric rhinosi
Eur Respir J. 2014;43:343–373. doi:10.1183/09031936.00202013 nusitis and asthma. Respir Med. 2018;141:94–99. PMID: 30053979.
8. Wenzel S. Severe asthma: epidemiology, pathophysiology and
doi:10.1016/j.rmed.2018.06.016
treatment. Mt Sinai J Med. 2003;70:185–190.
24. Lefebvre P, Duh MS, Lafeuille MH, et al. Acute and chronic systemic
9. Engelkes M, de Ridder MAJ, Svensson E, et al. Multinational,
corticosteroid-related complications in patients with severe asthma. J
database cohort study to assess severe exacerbation rate in asthma.
Allergy Clin Immunol. 2015;136(6):1488–1495. doi:10.1016/j.
Respir Med. 2020;165:105919. doi:10.1016/j.rmed.2020.105919
jaci.2015.07.046
10. Bel EH, Sousa A, Fleming L, et al. Diagnosis and definition of severe
25. Lefebvre P, Duh MS, Lafeuille MH, et al. Acute and chronic systemic
refractory asthma: an international consensus statement from the
corticosteroid-related complications in patients with severe asthma.
innovative medicine initiative (IMI). Thorax. 2011;66(10):910–917.
J Allergy Clin Immunol. 2015;136(6):1488–1495. doi:10.1016/j.
doi:10.1136/thx.2010.153643
11. Chanez P, Wenzel SE, Anderson GP, et al. Severe asthma in adults: jaci.2015.07.046
what are the important questions? J Allergy Clin Immunol. 2007;119 26. Foster JM, McDonald VM, Guo M, Reddel HK. “I have lost in every
(6):1337–1348. doi:10.1016/j.jaci.2006.11.702 facet of my life”: the hidden burden of severe asthma. Eur Respir J.
12. Global Initiative for Asthma. Difficult-to-treat & severe asthma in 2017;50(3):1700765. doi:10.1183/13993003.00765-2017
adolescent and adult patients. diagnosis and management. A GINA 27. Waljee AK, Rogers MAM, Paul L, et al. Short term use of oral
pocket guide for health professionals; 2018. Available from: https:// corticosteroids and related harms among adults in the United States:
ginasthma.org/wp-content/uploads/2018/11/GINA-SA-FINAL-wms. population based cohort study. BMJ. 2017;357:j1415. doi:10.1136/
pdf. Accessed July 29, 2021. bmj.j1415
13. Hekking PP, Wener RR, Amelink M, et al. The prevalence of severe 28. Global Initiative for Asthma.Difficult-to-treat & severe asthma in
refractory asthma. J Allergy Clin Immunol. 2015;135:896–902. adolescent and adult patients. diagnosis and management. A GINA
doi:10.1016/j.jaci.2014.08.042 pocket guide for health professionals; 2018. Available from https://
14. Sadatsafavi M, Lynd L, Marra C, et al. Direct health care costs ginasthma.org/wp-content/uploads/2018/11/GINA-SA-FINAL-wms.
associated with asthma in British Columbia. Can Respir J. pdf. Accessed July 29, 2021.
2010;17:74–80. doi:10.1155/2010/361071 29. Colombo GL, Di Matteo S, Heffler E, et al. Risultati dello studio
15. Braido F, Brusselle G, Guastalla D, et al. Determinants and impact of HERCULES: valutazione economica dell’impiego di risorse sanitarie
suboptimal asthma control in Europe: the international cross-sectional e descrizione del profilo clinico del paziente con asma grave non
and longitudinal assessment on asthma control (LIAISON) study. Respir controllato in Italia secondo dati di real-world. [Results of the
Res. 2016;17(1):51. doi:10.1186/s12931-016-0374-z HERCULES study: economic evaluation of healthcare resources
16. Bateman ED, Boushey HA, Bousquet J, et al. Can guideline-defined use and description of the clinical profile of the patient with severe
asthma control be achieved? The gaining optimal asthma control uncontrolled asthma in Italy according to real-world data]. Clin Econ
study. Am J Respir Crit Care Med. 2004;170:836–844. doi:10.1164/ Italian Articles Outcomes Res. 2020;15:63–78. Italian.
rccm.200401-033OC 30. Canonica GW, Colombo GL, Bruno GM, et al. Shadow cost of oral
17. Gauthier M, Ray A, Wenzel SE. Evolving concepts of asthma. Am corticosteroids-related adverse events: a pharmacoeconomic evalua
J Respir Crit Care Med. 2015;192(6):660–668. doi:10.1164/ tion applied to real-life data from the severe asthma network in Italy
rccm.201504-0763PP (SANI) registry. World Allergy Organ J. 2019;12(1):100007.
18. Allegra L, Cremonesi G, Girbino G, et al; PRISMA (PRospectIve doi:10.1016/j.waojou.2018.12.001
Study on asthMA control) Study Group. Real-life prospective study
on asthma control in Italy: cross-sectional phase results. Respir Med.
2012;106:205–214. doi:10.1016/j.rmed.2011.10.001
Journal of Asthma and Allergy Dovepress
Publish your work in this journal
The Journal of Asthma and Allergy is an international, peer-reviewed new therapies. The manuscript management system is completely
open-access journal publishing original research, reports, editorials online and includes a very quick and fair peer-review system, which
and commentaries on the following topics: Asthma; Pulmonary is all easy to use. Visit http://www.dovepress.com/testimonials.php
physiology; Asthma related clinical health; Clinical immunology and to read real quotes from published authors.
the immunological basis of disease; Pharmacological interventions and
Submit your manuscript here: https://www.dovepress.com/journal-of-asthma-and-allergy-journal
1018 DovePress Journal of Asthma and Allergy 2021:14
Powered by TCPDF (www.tcpdf.org)
You might also like
- Water Cures - Drugs Kill - How Water Cured Incurable Diseases (PDFDrive)Document244 pagesWater Cures - Drugs Kill - How Water Cured Incurable Diseases (PDFDrive)Mohammad0% (1)
- ACTIVITY 3 Identifying Sentence ErrorsDocument4 pagesACTIVITY 3 Identifying Sentence ErrorsApril MasongNo ratings yet
- My Lesson PlanDocument8 pagesMy Lesson Planapi-29785663293% (15)
- Oral Health in Asthmatic Patients: A Review: Clinical and Molecular AllergyDocument8 pagesOral Health in Asthmatic Patients: A Review: Clinical and Molecular AllergyJOSE VALDEMAR OJEDA ROJASNo ratings yet
- Endotype-Driven Treatment in Chronic Upper Airway DiseasesDocument14 pagesEndotype-Driven Treatment in Chronic Upper Airway DiseaseslockyNo ratings yet
- Articol Coacaz Negru PDFDocument5 pagesArticol Coacaz Negru PDFManu MandaNo ratings yet
- Effectiveness of FeNO Guided Treatment in Adult Asthma Patients A Systematic ReviewDocument11 pagesEffectiveness of FeNO Guided Treatment in Adult Asthma Patients A Systematic ReviewFikrieNo ratings yet
- WAO-ARIA Consensus On Chronic Cough - Part 3 Management Strategies in Primary and Cough-Specialty CareDocument20 pagesWAO-ARIA Consensus On Chronic Cough - Part 3 Management Strategies in Primary and Cough-Specialty CareNabilah AnandaNo ratings yet
- FULLTEXT01Document21 pagesFULLTEXT01mason.sadeghiNo ratings yet
- 2022 Lin Sun - Difference of Serum Cytokine Profile in Allergic A RetrieveDocument12 pages2022 Lin Sun - Difference of Serum Cytokine Profile in Allergic A RetrieveSteve aokiNo ratings yet
- The Heterogeneity of Chronic Cough: A Case For Endotypes of Cough HypersensitivityDocument11 pagesThe Heterogeneity of Chronic Cough: A Case For Endotypes of Cough HypersensitivityNadia hasibuanNo ratings yet
- KlasifikasiDocument8 pagesKlasifikasinurul sachrani putriNo ratings yet
- Evaluation of Antibiotics On Chronic Obstructive Pulmonary Disease Patient in Lung Hospital, West Sumatera, IndonesiaDocument4 pagesEvaluation of Antibiotics On Chronic Obstructive Pulmonary Disease Patient in Lung Hospital, West Sumatera, IndonesiaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Jaa 4 001 PDFDocument12 pagesJaa 4 001 PDFRulianti BarantiNo ratings yet
- Cough HipersensitivityDocument21 pagesCough HipersensitivityNabilah AnandaNo ratings yet
- NCM 112 Lec 2Document64 pagesNCM 112 Lec 2JIMENEZ, TRISHA MARIE D.No ratings yet
- Uric Acid, Blood Pressure, and Gout Management (PDFDrive)Document200 pagesUric Acid, Blood Pressure, and Gout Management (PDFDrive)Aurveda SE HealNo ratings yet
- The Prevalence of Allergic Rhinitis in Asthmatics and The Impact On Bronchial Asthma Control: A Single Center ExperienceDocument6 pagesThe Prevalence of Allergic Rhinitis in Asthmatics and The Impact On Bronchial Asthma Control: A Single Center ExperienceangelNo ratings yet
- Mometasone Furoate Nasal Spray-Systemic ReviewDocument5 pagesMometasone Furoate Nasal Spray-Systemic ReviewRobin ScherbatskyNo ratings yet
- Inhaled Corticosteroids Safety and Adverse Effects-DikonversiDocument8 pagesInhaled Corticosteroids Safety and Adverse Effects-DikonversiRachmi MerrinaNo ratings yet
- Treatment Trends in Allergic Rhinitis and Asthma: A British ENT SurveyDocument5 pagesTreatment Trends in Allergic Rhinitis and Asthma: A British ENT SurveyAndra LaszloNo ratings yet
- JurnalDocument8 pagesJurnalhidayatullahNo ratings yet
- 欧洲呼吸学会成人及儿童慢性咳嗽诊治指南Document31 pages欧洲呼吸学会成人及儿童慢性咳嗽诊治指南GaryNo ratings yet
- Asthma Dissertation IdeasDocument6 pagesAsthma Dissertation IdeasPaperWriterServiceSingapore100% (1)
- Feno Revision Sistematica Italia 2020Document20 pagesFeno Revision Sistematica Italia 2020Estefania Yu AcevedoNo ratings yet
- Asma RefractarioDocument9 pagesAsma RefractarioFlavio GuillenNo ratings yet
- Actual Concepts in Rhinosinusitis: A Review of Clinical Presentations, in Ammatory Pathways, Cytokine Profiles, Remodeling, and ManagementDocument18 pagesActual Concepts in Rhinosinusitis: A Review of Clinical Presentations, in Ammatory Pathways, Cytokine Profiles, Remodeling, and ManagementAurum MortNo ratings yet
- Allergy - 2008 - Sastre - Ebastine in Allergic Rhinitis and Chronic Idiopathic UrticariaDocument20 pagesAllergy - 2008 - Sastre - Ebastine in Allergic Rhinitis and Chronic Idiopathic UrticariaBabar TayyabNo ratings yet
- Buerger's DiseaseDocument8 pagesBuerger's DiseaseELSA HANA AL MUNAWAROHNo ratings yet
- Pi Is 1323893016301745Document27 pagesPi Is 1323893016301745Afria TikaNo ratings yet
- Asthma Term PaperDocument4 pagesAsthma Term Papereryhlxwgf100% (1)
- Asthma Case PresentationDocument3 pagesAsthma Case Presentationfernandezrachelle44No ratings yet
- Corticosteroids and Steroid Therapy 2015 Carmen Adkins PDFDocument129 pagesCorticosteroids and Steroid Therapy 2015 Carmen Adkins PDFSalahuddin ShikalgarNo ratings yet
- Copd Overlap AsthmaDocument8 pagesCopd Overlap AsthmaYaYakNo ratings yet
- ATCAM - Volume 1 - Issue Issue 1-2 - Pages 12-21 PDFDocument10 pagesATCAM - Volume 1 - Issue Issue 1-2 - Pages 12-21 PDFqalbiNo ratings yet
- A Review of The Metered Dose Inhaler Technique in Asthmatic and COPD PatientsDocument7 pagesA Review of The Metered Dose Inhaler Technique in Asthmatic and COPD PatientsselviaNo ratings yet
- B Russell e 2013Document10 pagesB Russell e 2013Arief Janurachman HakimNo ratings yet
- Diagnosis and Treatment of Chronic CoughFrom EverandDiagnosis and Treatment of Chronic CoughSang Heon ChoNo ratings yet
- 9410 41584 6 PBDocument9 pages9410 41584 6 PBMuzaki AndiyantoNo ratings yet
- Severe Asthma in Primary Care: Identification and ManagementDocument8 pagesSevere Asthma in Primary Care: Identification and ManagementIzza UrfanNo ratings yet
- Dissertation Topics On AsthmaDocument8 pagesDissertation Topics On AsthmaWhereToBuyResumePaperCanada100% (1)
- Factors Related To Severe Acute Asthma Attack and Treatment: IJPSR (2012), Vol. 3, Issue 08 (Research Article)Document4 pagesFactors Related To Severe Acute Asthma Attack and Treatment: IJPSR (2012), Vol. 3, Issue 08 (Research Article)Tanvir HayderNo ratings yet
- Severe and Difficult-to-Treat Asthma in Adults: Review ArticleDocument12 pagesSevere and Difficult-to-Treat Asthma in Adults: Review ArticlePatricio MiguelNo ratings yet
- Rhinosinusitis: Alexi Decastro,, Lisa Mims,, William J. HuestonDocument15 pagesRhinosinusitis: Alexi Decastro,, Lisa Mims,, William J. HuestonkikoNo ratings yet
- Synopsis Submitted To: Application For The Registration of Subjects For Dissertation of TheDocument14 pagesSynopsis Submitted To: Application For The Registration of Subjects For Dissertation of TheAraafathNo ratings yet
- Asthama VireshDocument34 pagesAsthama VireshVarun MahajaniNo ratings yet
- 2023 Risk Factors of NSAID Exacerbated Respiratory DiseaseDocument22 pages2023 Risk Factors of NSAID Exacerbated Respiratory Diseasexiongmao2389No ratings yet
- Exacerbations of CopdDocument10 pagesExacerbations of CopdMelissa PeñataNo ratings yet
- Community-Acquired Pneumonia: Strategies for ManagementFrom EverandCommunity-Acquired Pneumonia: Strategies for ManagementAntoni TorresRating: 4.5 out of 5 stars4.5/5 (2)
- The Burden of Allergic Rhinitis and Asthma: Tunis Ozdoganoglu and Murat SonguDocument13 pagesThe Burden of Allergic Rhinitis and Asthma: Tunis Ozdoganoglu and Murat Songudanaagus81No ratings yet
- Ana Phy RespiratoryDocument5 pagesAna Phy Respiratorydayang ranarioNo ratings yet
- Ra 2 PDFDocument6 pagesRa 2 PDFRikaRistantiNo ratings yet
- BMJ Pediatric Asthma in A NutshellDocument14 pagesBMJ Pediatric Asthma in A NutshellarjumandNo ratings yet
- Treatment Strategies For Asthma: Reshaping The Concept of Asthma ManagementDocument11 pagesTreatment Strategies For Asthma: Reshaping The Concept of Asthma Managementtegarsh321No ratings yet
- Cough Management A Practical ApproachDocument12 pagesCough Management A Practical ApproachYohan YudhantoNo ratings yet
- Japanese Guidelines For Childhood Asthma 2017 PDFDocument15 pagesJapanese Guidelines For Childhood Asthma 2017 PDFcindy315No ratings yet
- Management - of - Chronic - Respiratory - and - Allergic - DisDocument20 pagesManagement - of - Chronic - Respiratory - and - Allergic - DisjoseNo ratings yet
- Children 10 01571Document9 pagesChildren 10 01571billyolivierapattiasina25No ratings yet
- 2000 Journal of The California Dental AssociationDocument20 pages2000 Journal of The California Dental AssociationUnyar LeresatiNo ratings yet
- Ers BeDocument24 pagesErs Bedicky wahyudiNo ratings yet
- EFFICACY OF HOMOEOPATHIC SIMILLIMUM IN TREATING ATOPIC BRONCHIAL ASTHMA WITH AN EVALUATION BASED ON IgEDocument13 pagesEFFICACY OF HOMOEOPATHIC SIMILLIMUM IN TREATING ATOPIC BRONCHIAL ASTHMA WITH AN EVALUATION BASED ON IgEAraafathNo ratings yet
- Primer: BronchiectasisDocument18 pagesPrimer: BronchiectasisAnanta Bryan Tohari WijayaNo ratings yet
- Orr 2019Document15 pagesOrr 2019abdi syahputraNo ratings yet
- Lag Aert 2017Document8 pagesLag Aert 2017abdi syahputraNo ratings yet
- Dyspareunia MacneillDocument14 pagesDyspareunia Macneillabdi syahputraNo ratings yet
- 192 2020 Article 4250Document7 pages192 2020 Article 4250abdi syahputraNo ratings yet
- Evaluation and Differential Diagnosis of DyspareuniaDocument10 pagesEvaluation and Differential Diagnosis of Dyspareuniaabdi syahputraNo ratings yet
- E836 FullDocument1 pageE836 Fullabdi syahputraNo ratings yet
- Asma 6Document39 pagesAsma 6abdi syahputraNo ratings yet
- Status EpilepticusDocument10 pagesStatus Epilepticusabdi syahputraNo ratings yet
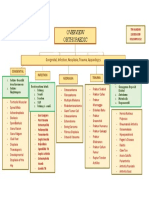
- Orthopaedic: Congenital, Infection, Neoplasia, Trauma, AppandegesDocument1 pageOrthopaedic: Congenital, Infection, Neoplasia, Trauma, AppandegesdinsNo ratings yet
- Ortho-Rheumatology Questions by DR - OkashaDocument136 pagesOrtho-Rheumatology Questions by DR - Okashamohammed okashaNo ratings yet
- Cumulative Lyme Disease (2013-2014) : Jayson Karuna Microbiology 1420-076 CenDocument2 pagesCumulative Lyme Disease (2013-2014) : Jayson Karuna Microbiology 1420-076 CenJayNo ratings yet
- MCN 2Document106 pagesMCN 2Nicole Dela TorreNo ratings yet
- Case Study NCPDocument6 pagesCase Study NCPEarl Joseph DezaNo ratings yet
- Seminar On Antigen-Antibody Reaction and Immunodeficiency DiseasesDocument28 pagesSeminar On Antigen-Antibody Reaction and Immunodeficiency DiseasesDr. Shiny KajalNo ratings yet
- Neurodevelopmental Disorders The History and Future of A Diagnostic ConceptDocument9 pagesNeurodevelopmental Disorders The History and Future of A Diagnostic Conceptmtkeniabianor_409003No ratings yet
- Record of Staff Toolbox Meeting TemplateDocument2 pagesRecord of Staff Toolbox Meeting TemplatemetaNo ratings yet
- De Thi Hoc Sinh Gioi Mon Tieng Anh Lop 9 Nam Hoc 2018 2019 So 12Document6 pagesDe Thi Hoc Sinh Gioi Mon Tieng Anh Lop 9 Nam Hoc 2018 2019 So 12Nhật VyNo ratings yet
- Gram Staining ProcedureDocument3 pagesGram Staining ProcedureCheska SillayuNo ratings yet
- Perdev 00Document2 pagesPerdev 00Nasser GementizaNo ratings yet
- Autosomal Dominant Polycystic Kidney DiseaseDocument11 pagesAutosomal Dominant Polycystic Kidney DiseaserutwickNo ratings yet
- Combining Scalp Acupuncture and Manual Therapy1Document26 pagesCombining Scalp Acupuncture and Manual Therapy1thesantorinimassageNo ratings yet
- An Investegatory Project ReportDocument17 pagesAn Investegatory Project ReportKhushi kapseNo ratings yet
- Deep Mycotic InfectionDocument5 pagesDeep Mycotic InfectionjalalfaizNo ratings yet
- Nosodes and Sarcodes - ClarkeDocument12 pagesNosodes and Sarcodes - Clarkemelos24No ratings yet
- Culture Bound: Illnesses in The PHDocument13 pagesCulture Bound: Illnesses in The PHMichael B.No ratings yet
- Human Cells Journey: Organ Syste MDocument7 pagesHuman Cells Journey: Organ Syste MArina CucuruzaNo ratings yet
- Hand Eczema TreatmentDocument9 pagesHand Eczema TreatmentCharcravorti AyatollahsNo ratings yet
- 50 bài tập Từ trái nghĩa Mức độ thông hiểu - phần 1Document13 pages50 bài tập Từ trái nghĩa Mức độ thông hiểu - phần 1huyentran2771996No ratings yet
- NSTP Notes - From ModuleDocument12 pagesNSTP Notes - From ModuleJulianna Jade Dela CruzNo ratings yet
- The Genetic Spectrum of Congenital OcularDocument12 pagesThe Genetic Spectrum of Congenital OcularKryssiaNo ratings yet
- REP8 Unit 8 Klucz OdpowiedziDocument4 pagesREP8 Unit 8 Klucz Odpowiedzipanna hanna19No ratings yet
- Nursing Case Presentation For A Patient With CABG: Subject: Medical Surgical Nursing-IIDocument10 pagesNursing Case Presentation For A Patient With CABG: Subject: Medical Surgical Nursing-IIanamika sharmaNo ratings yet
- Topic 11 - Certification and Legislation in Food and BeverageDocument35 pagesTopic 11 - Certification and Legislation in Food and BeverageEni Syafina RoslanNo ratings yet
- Final Graphic CommDocument46 pagesFinal Graphic Commatiq jalilNo ratings yet
- Ingles 4Document8 pagesIngles 4denisseNo ratings yet