Professional Documents
Culture Documents
Fournier S Gangrene
Fournier S Gangrene
Uploaded by
reza arnediCopyright:
Available Formats
You might also like
- NCM 117 Psychiatric Nursing MODULE 7Document27 pagesNCM 117 Psychiatric Nursing MODULE 7Meryville JacildoNo ratings yet
- 01-ACMC Case Study ReferenceDocument8 pages01-ACMC Case Study ReferenceJean Sunny100% (1)
- Blood AnalysisDocument4 pagesBlood AnalysisSuman Malik SehrawatNo ratings yet
- Jurnal MenagementDocument5 pagesJurnal Menagementelsy oktaviaNo ratings yet
- SepsisDocument9 pagesSepsisLeón TorresNo ratings yet
- 1 Elassmy2016Document5 pages1 Elassmy2016aldillawrNo ratings yet
- Surgical Management of Fourniers Gangrene A Seven Year Experience at The Philippine General HospitalDocument6 pagesSurgical Management of Fourniers Gangrene A Seven Year Experience at The Philippine General HospitalGian PagadduNo ratings yet
- A Study On Fournier's Gangrene: Original ResearchDocument5 pagesA Study On Fournier's Gangrene: Original Researchzetta369No ratings yet
- Prognostic Factor Fournier GangreneDocument7 pagesPrognostic Factor Fournier GangreneRaeni Dwi PutriNo ratings yet
- Postoperative Nausea and Vomiting: Retrospective Comparative Statistical StudyDocument19 pagesPostoperative Nausea and Vomiting: Retrospective Comparative Statistical StudyIJAR JOURNALNo ratings yet
- Cureus 0013 00000015301Document5 pagesCureus 0013 00000015301Abdunur MusemakweliNo ratings yet
- 55-Article Text-103-1-10-20200408Document7 pages55-Article Text-103-1-10-20200408Kshitiz112No ratings yet
- The Study of Epidemiological, Clinical and Biochemical Characteristics of Covid 19 Non Survivors in A Tertiary Care Hospital of Southern IndiaDocument6 pagesThe Study of Epidemiological, Clinical and Biochemical Characteristics of Covid 19 Non Survivors in A Tertiary Care Hospital of Southern IndiaIJAR JOURNALNo ratings yet
- Ioi80197 463 473Document11 pagesIoi80197 463 473Phạm LinhNo ratings yet
- Fourniers Gangrene and Its Management A Prospective StudyDocument12 pagesFourniers Gangrene and Its Management A Prospective StudyAthenaeum Scientific PublishersNo ratings yet
- Founier GangrenDocument5 pagesFounier GangrenJohannes MarpaungNo ratings yet
- Postoperative Infection and Mortality Following Elective Surgery in The International Surgical Outcomes Study (ISOS)Document32 pagesPostoperative Infection and Mortality Following Elective Surgery in The International Surgical Outcomes Study (ISOS)Antonio Carlos Betanzos PlanellNo ratings yet
- NF UkDocument7 pagesNF UkMax FaxNo ratings yet
- 1 LRDocument12 pages1 LRaoonNo ratings yet
- Full TextDocument32 pagesFull TextHam FGNo ratings yet
- Necrotising Fasciitis or Pyoderma Gangrenosum: A Fatal DilemmaDocument8 pagesNecrotising Fasciitis or Pyoderma Gangrenosum: A Fatal DilemmayuktianaNo ratings yet
- Jurnal PatogenesisDocument6 pagesJurnal PatogenesisErmiati EmhyNo ratings yet
- The Surgical Management of Parasitic Diseases: George Tsoulfas Jamal J. Hoballah George C. Velmahos Yik-Hong HoDocument366 pagesThe Surgical Management of Parasitic Diseases: George Tsoulfas Jamal J. Hoballah George C. Velmahos Yik-Hong HoEsdinawan Carakantara SatrijaNo ratings yet
- LancetDocument11 pagesLancetvieira.beatrizNo ratings yet
- Fernandez Alcaraz2019Document5 pagesFernandez Alcaraz2019ARQ. HernandezNo ratings yet
- 1-s2.0-S1201971212000264-main_2Document7 pages1-s2.0-S1201971212000264-main_2lee zaraNo ratings yet
- A Retrospective Analysis of Fourniers Gangrene at A TertiaryGovernment Hospital in The PhilippinesDocument3 pagesA Retrospective Analysis of Fourniers Gangrene at A TertiaryGovernment Hospital in The PhilippinesGian PagadduNo ratings yet
- The Epidemiology, Antibiotic Resistance and Post-Discharge Course of Peritonsillar Abscesses in London, OntarioDocument7 pagesThe Epidemiology, Antibiotic Resistance and Post-Discharge Course of Peritonsillar Abscesses in London, OntarioMaharaniNo ratings yet
- Chen 2018Document5 pagesChen 2018Teja Laksana NukanaNo ratings yet
- 150-Final Document To Be Uploaded-1966-1-10-20230110Document5 pages150-Final Document To Be Uploaded-1966-1-10-20230110M Hassan RafiqNo ratings yet
- The Presentation, Management and Outcomes of Fournier's Gangrene at A Tertiary Urology Referral Centre in South AfricaDocument6 pagesThe Presentation, Management and Outcomes of Fournier's Gangrene at A Tertiary Urology Referral Centre in South AfricaAngeel GomezNo ratings yet
- Clinical Characteristics, Laboratory Abnormalities and Outcome of Covid-19 Positive Patients Admitted in Tertiary Care Hospital of KarachiDocument8 pagesClinical Characteristics, Laboratory Abnormalities and Outcome of Covid-19 Positive Patients Admitted in Tertiary Care Hospital of KarachiIJAR JOURNALNo ratings yet
- INSULINOMADocument6 pagesINSULINOMASaifullah NaseerNo ratings yet
- Horne, A. W., & Missmer, S. A. (2022) - Pathophysiology, Diagnosis, and Management of Endometriosis. BMJ, 379.Document19 pagesHorne, A. W., & Missmer, S. A. (2022) - Pathophysiology, Diagnosis, and Management of Endometriosis. BMJ, 379.Hernando Rivera-DuqueNo ratings yet
- 01singh PDFDocument9 pages01singh PDFTri Santi InggianyNo ratings yet
- Pathophysiology, Diagnosis, and ManagementDocument19 pagesPathophysiology, Diagnosis, and Management1832303aNo ratings yet
- CC 12570Document9 pagesCC 12570Kornelis AribowoNo ratings yet
- Candidiasis in PICUDocument6 pagesCandidiasis in PICUMeirinda HidayantiNo ratings yet
- Study of The Prevalence of Nosocomial Infections in The University Hospital Center of Béni-Messous, Algiers in 2023 - AlgeriaDocument6 pagesStudy of The Prevalence of Nosocomial Infections in The University Hospital Center of Béni-Messous, Algiers in 2023 - AlgeriaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Fournier's Gangrene: An Experience in Tertiary Care HospitalDocument9 pagesFournier's Gangrene: An Experience in Tertiary Care HospitalKriti KumariNo ratings yet
- Envenimations ViperinesDocument6 pagesEnvenimations ViperinesIJAR JOURNALNo ratings yet
- Fungal Endocarditis Current ChallengesDocument5 pagesFungal Endocarditis Current ChallengesmarnixvonkempNo ratings yet
- Clinical Trends of Ectopic Pregnancy - A Study in A Tertiary Care Hospital of West Bengal, IndiaDocument7 pagesClinical Trends of Ectopic Pregnancy - A Study in A Tertiary Care Hospital of West Bengal, IndiaIJAR JOURNALNo ratings yet
- 2021 Amaylia Oehadian - Putri - Uun - Bahti - Evan - Jeffery (U) - Erythropoiesis Differences in Various ClinicalDocument6 pages2021 Amaylia Oehadian - Putri - Uun - Bahti - Evan - Jeffery (U) - Erythropoiesis Differences in Various ClinicalEvan SusandiNo ratings yet
- Examination of Ulcero-Proliferative Lesions of Oropharynx and Oral Cavity - A Clinical PerspectiveDocument7 pagesExamination of Ulcero-Proliferative Lesions of Oropharynx and Oral Cavity - A Clinical PerspectiveInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Analysis of Mortality in Covid 19 Patients - A Study in A District Covid Hospital in Andhra Pradesh During The First WaveDocument6 pagesAnalysis of Mortality in Covid 19 Patients - A Study in A District Covid Hospital in Andhra Pradesh During The First WaveIJAR JOURNALNo ratings yet
- Management of Fournier GangrenDocument4 pagesManagement of Fournier GangrenArby ShafaraNo ratings yet
- Fournier Gangrene Pictorial ReviewDocument11 pagesFournier Gangrene Pictorial ReviewKristell PérezNo ratings yet
- Jurnal 3 Abses Leher DalamDocument6 pagesJurnal 3 Abses Leher DalamRohayu AsnawiNo ratings yet
- Prospective Cohort StudyDocument6 pagesProspective Cohort StudyMãnoj MaheshwariNo ratings yet
- Journal Homepage: - : IntroductionDocument8 pagesJournal Homepage: - : IntroductionIJAR JOURNALNo ratings yet
- Fournier's Gangrene. A Clinical ReviewDocument9 pagesFournier's Gangrene. A Clinical ReviewJohannes MarpaungNo ratings yet
- Odontogenic Necrotizing Fasciitis: A Systematic Review of The LiteratureDocument7 pagesOdontogenic Necrotizing Fasciitis: A Systematic Review of The LiteratureDenta HaritsaNo ratings yet
- Assessment of Postoperative Anaesthetic Incidents in The Recovery RoomDocument5 pagesAssessment of Postoperative Anaesthetic Incidents in The Recovery RoomIJAR JOURNALNo ratings yet
- Fournier's Gangrene. A Clinical Review: ArticleDocument9 pagesFournier's Gangrene. A Clinical Review: ArticleMichael Stevent Cuellar RodriguezNo ratings yet
- JC On StenoDocument5 pagesJC On StenotanviaggrawalNo ratings yet
- 4 SaDocument6 pages4 SaRizqi AmaliaNo ratings yet
- Efficacy of Corticosteroids in Non-Intensive Care Unit Patients With COVID-19 Pneumonia From The New York Metropolitan RegionDocument14 pagesEfficacy of Corticosteroids in Non-Intensive Care Unit Patients With COVID-19 Pneumonia From The New York Metropolitan RegionicarosalernoNo ratings yet
- Morra 2018Document9 pagesMorra 2018Distro AwanNo ratings yet
- The Incidence and Risk Factors of Ventilator-Associated Pneumonia in ICUDocument6 pagesThe Incidence and Risk Factors of Ventilator-Associated Pneumonia in ICUWentiNo ratings yet
- Mudança Epidemiológica Gonococo FrançaDocument4 pagesMudança Epidemiológica Gonococo FrançaEliseu AmaralNo ratings yet
- Community-Acquired Pneumonia: Strategies for ManagementFrom EverandCommunity-Acquired Pneumonia: Strategies for ManagementAntoni TorresRating: 4.5 out of 5 stars4.5/5 (2)
- Method of Statement PCDocument8 pagesMethod of Statement PCAbada SaadNo ratings yet
- Clinical Leadership Development and Education For NursesDocument10 pagesClinical Leadership Development and Education For NursesVia Eliadora TogatoropNo ratings yet
- Ecm 216 Building Services Bab 3.2 Water Supply PDFDocument6 pagesEcm 216 Building Services Bab 3.2 Water Supply PDFAZUAN BIN AHMAD FAUZI100% (8)
- Shell Helix Ultra Professional AJ-L 0W-20: Main Applications Specifications, Approvals & RecommendationsDocument2 pagesShell Helix Ultra Professional AJ-L 0W-20: Main Applications Specifications, Approvals & RecommendationsMuhNo ratings yet
- Fed BatchDocument3 pagesFed BatchKrishnadev Madhavan NairNo ratings yet
- Guidelines For Open Plant StructuresDocument6 pagesGuidelines For Open Plant StructuresIndrawNo ratings yet
- 2024 MSDocument38 pages2024 MS6vnh5z7fnjNo ratings yet
- Msds For Skim CoatDocument8 pagesMsds For Skim Coatlovely palomaNo ratings yet
- Homework 2Document9 pagesHomework 2Alexis R. CamargoNo ratings yet
- AHA Anderson StudyDocument8 pagesAHA Anderson Studykaren lilianaNo ratings yet
- NestleDocument12 pagesNestleParadoxNo ratings yet
- Day 1 Menu: BreakfastDocument11 pagesDay 1 Menu: BreakfastAndrew HubbardNo ratings yet
- WSNZ 1311 Construction Machinery Fact Sheet v5Document4 pagesWSNZ 1311 Construction Machinery Fact Sheet v5Gemunu WeerethungaNo ratings yet
- Home Remedies To Treat Dupuytren S Disease OrthoBethesda .G-Job 84Document15 pagesHome Remedies To Treat Dupuytren S Disease OrthoBethesda .G-Job 84paulsub63No ratings yet
- Herbalife SurveyDocument1 pageHerbalife Surveyrhymes2u100% (1)
- Antibiotic Microbial Resistance (AMR) Removal Efficiencies by 2019 PDFDocument13 pagesAntibiotic Microbial Resistance (AMR) Removal Efficiencies by 2019 PDFdebleenaNo ratings yet
- AFD Runs End JanuaryDocument3 pagesAFD Runs End Januarylarry_kelley_1No ratings yet
- Abortion Pro Life Vs Pro ChoiceDocument6 pagesAbortion Pro Life Vs Pro Choiceapi-356865000No ratings yet
- PE 12 HOPE 3 Q2 Module 3 Lesson 6 7 by FarrahDocument33 pagesPE 12 HOPE 3 Q2 Module 3 Lesson 6 7 by Farrahricsha masanayNo ratings yet
- Parental Substance AbuseDocument10 pagesParental Substance Abuseapi-360330020No ratings yet
- Daftar Pustaka-MendeleyDocument3 pagesDaftar Pustaka-Mendeleynurafiat175No ratings yet
- Visa Invitation LettersDocument6 pagesVisa Invitation LettersPrince SharmaNo ratings yet
- Monthly AUGUST 2015 REPOKHNDocument13 pagesMonthly AUGUST 2015 REPOKHNAkash PGNo ratings yet
- ITRC 2009 - LNAPL Guidance DocumentDocument157 pagesITRC 2009 - LNAPL Guidance DocumentFelipe NaretaNo ratings yet
- Umer Mehmood: Personal ProfileDocument3 pagesUmer Mehmood: Personal ProfileMuhammad sufyan Muhammad sufyanNo ratings yet
- Psychology Test 2 Practice QuestionsDocument15 pagesPsychology Test 2 Practice Questionsshamim3261100% (3)
- Makassar Workshop - BeneFusion 5 Series 20190626Document49 pagesMakassar Workshop - BeneFusion 5 Series 20190626wahyu bunha rNo ratings yet
Fournier S Gangrene
Fournier S Gangrene
Uploaded by
reza arnediOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Fournier S Gangrene
Fournier S Gangrene
Uploaded by
reza arnediCopyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/283817497
Analysis of prognostic factors affecting mortality in Fournier’s gangrene: A
study of 72 cases
Article in Canadian Urological Association journal = Journal de l'Association des urologues du Canada · November 2015
DOI: 10.5489/cuaj.3192
CITATIONS READS
26 1,581
9 authors, including:
Mohamed Tarchouli Ahmed Bounaim
First Medical and Surgical Center of Royal Armed Forces. Agadir. Morocco Mohammed V University of Rabat
34 PUBLICATIONS 140 CITATIONS 110 PUBLICATIONS 251 CITATIONS
SEE PROFILE SEE PROFILE
Mohamed Essarghini Abdelhak Bensal
Military Hospital Mohammed V, Rabat Military Hospital Mohammed V, Rabat
19 PUBLICATIONS 72 CITATIONS 4 PUBLICATIONS 32 CITATIONS
SEE PROFILE SEE PROFILE
Some of the authors of this publication are also working on these related projects:
General surgery View project
Hepatobiliary View project
All content following this page was uploaded by Mohamed Tarchouli on 08 July 2016.
The user has requested enhancement of the downloaded file.
Original research
Analysis of prognostic factors affecting mortality in Fournier’s
gangrene: A study of 72 cases
Mohamed Tarchouli, MD;* Ahmed Bounaim, MD;* Mohamed Essarghini, MD;* Moulay Brahim Ratbi, MD;*
Mohamed Said Belhamidi, MD;* Abdelhak Bensal, MD;* Adil Zemmouri, MD;† Abdelmounaim Ait Ali, MD;*
Khalid Sair, MD*
Department of Digestive Surgery, Mohammed V Military Hospital, Faculty of Medicine and Pharmacy, Mohammed V University, Rabat, Morocco; †Department of Anesthesiology and Intensive Care,
*
Mohammed V Military Hospital, Faculty of Medicine and Pharmacy, Mohammed V University, Rabat, Morocco
Cite as: Can Urol Assoc J 2015;9(11-12):E800-4. http://dx.doi.org/10.5489/cuaj.3192 by the French dermatologist Jean-Alfred Fournier in 1883.1
Published online November 4, 2015. He described a fulminant gangrene of the scrotum and penis
observed especially in healthy young men without appar-
Abstract ent etiologic factors. Presently, the disease mainly affects
men in the fifth to seventh decades of life, with associated
Introduction: Fournier’s gangrene is a rapidly progressing necro- predisposing factors and an identifiable etiology. The gan-
tizing fasciitis of the perineum and genital area associated with a grene is considered the result of a polymicrobial aerobic and
high mortality rate. We presented our experience in managing this
anaerobic synergistic infection originating from a colorec-
entity and identified prognostic factors affecting mortality.
tal, genitourinary or skin infection site. It can progress to a
Methods: We carried out a retrospective study of 72 patients treated
for Fournier’s gangrene at our institution between January 2005 fulminant soft tissue infection and spread rapidly along the
and December 2014. Patients were divided into survivors and non- fascial planes to the abdominal wall and even the thorax.
survivors and potential prognostic factors were analyzed. Early diagnosis with fast and adequate treatment, includ-
Results: Of the 72 patients, 64 were males (89%) and 8 females ing aggressive surgical debridement, hemodynamic stabiliza-
(11%), with a mean age of 51 years. The most common predis- tion and broad-spectrum antibiotic-therapy, are the mainstay
posing factor was diabetes mellitus (38%). The mortality rate was of successful management. However, despite advances in
17% (12 patients died). Statistically significant differences were surgical technique and critical care, the mortality rate is still
not found in age, gender, and predisposing factors, except in heart high, between 20% and 50% in most contemporary series.2
disease (p = 0.038). Individual laboratory parameters significantly In this study, we presented our experience in managing
correlating with mortality included hemoglobin (p = 0.023), hema-
Fournier’s gangrene during a 10-year period and we ana-
tocrit (p = 0.019), serum urea (p = 0.009), creatinine (p = 0.042),
lyzed different factors affecting its outcome and mortality.
and potassium (p = 0.026). Severe sepsis on admission and the
extent of affected surface area also predicted higher mortality.
Others factors, such as duration of symptoms before admission, Methods
number of surgical debridement, diverting colostomy and length
of hospital stay, did not show significant differences. The median We conducted a retrospective study of 72 patients diagnosed
Fournier’s Gangrene Severity Index (FGSI) was significantly higher with Fournier’s gangrene and undergoing surgical treatment at
in non-survivors (p = 0.002). Mohammed V Military Hospital of Rabat, Digestive Surgery
Conclusion: Fournier’s gangrene is a severe surgical emergency Department, Morocco during the 10-year period between
requiring early diagnosis and aggressive therapy. Identification of January 2005 and December 2014. The diagnosis was based
prognostic factors is essential to establish an optimal treatment and on the patient’s medical history and physical examination.
to improve outcome. The FGSI is a simple and valid method for
Data were collected for age, gender, etiology, risk factors,
predicting disease severity and patient survival.
duration of symptoms before admission, physical examina-
tion, laboratory findings, total extent of affected body surface,
antibiotic therapy, surgical treatment and number of sub-
Introduction sequent debridement, requirement for intestinal diversion,
length of hospital stay, and outcome. Mortality was defined
Fournier’s gangrene is a rapidly progressive necrotizing fas- as disease-related death during the hospital stay. Patients with
ciitis of the perineal, perianal and genital area, first described incomplete medical records were excluded from the study.
E800 CUAJ • November-December 2015 • Volume 9, Issues 11-12
© 2015 Canadian Urological Association
Prognostic factors affecting mortality in Fournier’s gangrene
The extent of gangrene was measured using nomograms Results
routinely used to assess the extent of burn injuries, accord-
ing to which penis, scrotum and perineum each account Of the 72 patients, 64 were males (89%) and 8 were females
for 1% surface area, and each ischiorectal fossa accounts (11%), with a median age of 51 years (range: 23–75), and a
for 2.5%.3,4 medical history of Fournier’s gangrene in 49 (68%) patients.
To assess the severity of infection, we used the Fournier’s Diabetes mellitus coexisted in 27 patients (38%), high blood
Gangrene Severity Index (FGSI) described by Loar and col- pressure in 21 (29%), heart disease in 16 (22%), lung disease
leagues in 1995, and the presence of sepsis, severe sepsis or in 5 (7%), liver disease in 6 (8%), kidney disease in 8 (11%),
septic shock on admission. FGSI was obtained by combining and vascular disease in 10 (14%). Nine patients (13%) pre-
admission clinical (temperature, heart and respiratory rates) sented immunodepression with 5 malignant neoplasms, 2
and laboratory parameters (hematocrit and leukocyte count, chemotherapeutic treatments, and 2 chronic corticosteroid
serum sodium, potassium, creatinine and bicarbonate).5 In use. Chronic alcoholism was detected in 4 patients (6%)
this index, each parameter is given 0 to 4 points, and FGSI and smoking habit in 14 patients (19%).
is calculated by adding the points of each parameter. The An etiological factor was identified in 67 (93%) cases;
cut-off point is 9, meaning that when FGSI is >9, the prob- therefore, only 5 (7%) patients had idiopathic Fournier’s
ability of death is 75%, and when it is ≤9, the probability gangrene. The most common source of sepsis was anorec-
of survival is 78% (Table 1). Sepsis is defined as infection tal, especially anal suppurations. No statistical significant
with systemic inflammatory response syndrome, which is difference in etiologic factor was found between survivors
manifested with two or more of the following findings: body and non-survivors (Table 2).
temperature <36 °C or >38 °C, heart rate >90 beats/min, The most common clinical signs at the time of admis-
respiratory rate >20 breaths/ min or PaCO2<32 mmHg, and sion were perineal necrosis (n = 67; 93%), perineal pain
leukocyte count >12 000 cells/mm3, <4000 cells/mm3, or (n = 61; 85%), fever (n = 38; 53%), and poor general con-
>10% of immature forms. Severe sepsis is defined as sepsis dition (n = 27; 38%). All patients underwent wide debride-
combined with organ dysfunction, hypotension or tissue ment of necrotic tissue under the cover of broad spectrum
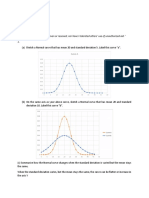
hypoperfusion. Septic shock is defined as sepsis with refrac- antibiotics (Fig. 1). Treatment was continued with sequential
tory arterial hypotension or signs of systemic hypoperfusion debridement until the wound showed healthy granulation
in spite of fluid resuscitation.3,4 tissue. Intestinal diversion and hyperbaric oxygen therapy
Statistical analysis was performed using SPSS program were applied, in addition to surgical debridement when
version 13.0. Qualitative variables were defined by frequen- required. Therefore, adjunctive hyperbaric oxygen thera-
cy and percentage, and quantitative variables were defined py was used in 56 patients (78%) and prevention of fecal
by the median value and the 25th to 75th percentiles. The contamination was attempted by diverting-colostomy in 14
statistical tests employed in the univariate analysis were patients (19%). Patients with severe sepsis, requiring vaso-
the chi-square test and Fisher’s exact test for the qualitative pressors or mechanical ventilation support were treated in
variables and the Mann-Whitney test for the quantitative the intensive care unit.
variables. Statistical significance was set at p < 0.05. Of the 72 patients, 60 (83%) survived and 12 (17%) died.
The etiology in mortality cases was colorectal in 7 cases
(13%), genitourinary in 3 (38%), traumatic in 2 (50%). The
Table 1. Fournier’s Gangrene Severity Index
High abnormal values Low abnormal values
Variables
+4 +3 +2 +1 0 +1 +2 +3 +4
Temperature, °C >41 39–40.9 – 38.5–38.9 36–38.4 34–35.9 32–33.9 30–31.9 <29.9
Heart rate >180 140–179 110–139 – 70–109 – 55–69 40–54 <39
Respiration rate >50 35–49 – 25–34 12–24 10–11 6–9 – <5
Serum Na, mmol/L >180 160–179 155–159 150–154 130–149 – 120–129 111–119 <110
Serum K, mmol/L >7 6–6.9 – 5.5–5.9 3.5–5.4 3–3.4 2.5–2.9 – <2.5
Serum creatinine, mg/100 ml,
>3.5 2–3.4 1.5–1.9 – 0.6–1.4 – <0.6 – –
×2 for acute renal failure
Hematocrit, % >60 – 50–59.9 46–49.9 30–45.9 – 20–29.9 – <20
White blood cell count,
>40 – 20–39.9 15–19.9 3–14.9 – 1–2.9 – <1
×1000/mm3
Serum bicarbonate, mmol/L >52 41–51,9 – 32–40.9 22–31.9 – 18–21.9 15–17.9 <15
CUAJ • November-December 2015 • Volume 9, Issues 11-12 E801
Tarchouli et al.
Table 2. Sources of Fournier’s gangrene
Etiology Patients (n) (%)
Colorectal 54 (75%)
Genitourinary 8 (11%)
Retroperitoneal (psoas abscess) 1 (1%)
Traumatic 4 (6%)
Unknown 5 (7%)
causes of death were: multiple organ failure in 10 (83%),
acute myocardial infarction in 1 and pulmonary thrombo-
embolism in 1. Microbiological cultures were done in 44
patients (61%). A single microorganism was isolated in 7
patients (16%), and multiple microorganisms were found
in 37 patients (84%). The most frequent bacterial agents
cultured from the necrotic tissue were Escherichia coli (83%)
and Streptococcus spp (35%). Analyses of different prog-
nostic factors according to survivors and non-survivors are
shown in Table 3 and Table 4.
Discussion
In the past, Fournier’s gangrene was thought to affect young
men only. Currently, the reported age of patients has pro-
gressively increased, as was shown in our study with a
median age of 51.6,7 Some authors do not report significant
differences of age between survivors and non-survivors.7,8
Conversely, a growing number of studies show that surviv- Fig.1. Fournier’s gangrene located to the perineum and scrotum after surgical
ing patients were significantly associated with a younger debridement.
age.9,10 The same was true in our series, but without sta-
tistical significance. With regard to gender, male predomi- ma.15,16 These conditions are associated with reduced cell-
nance has also been reported in previous studies.11 Czymek mediated immune response, which favours the development
and colleagues described the female gender as a risk factor of the infection. Some authors have reported an associa-
associated with a higher mortality; however, we could not tion between these predisposing factors and mortality.17,18
demonstrate similar findings.12
Despite the development of treatment modalities, anti-
Table 3. Analysis of prognostic factors (qualitative
biotic therapy, and intensive care techniques, Fournier’s variables)
gangrene is still a fatal disease with high mortality rate Survivors Non-survivors
(20%–50%).3,13,14 A mortality rate of 17% was detected at Variables p value
(n = 60) n (%) (n = 12) n (%)
our centre, that is 14% (8/56) in the hyperbaric oxygen Male/female 54/6 10/2 NS
therapy group and 25% (4/16) in the non-hyperbaric oxy- Diabetes 20 (33.3) 7 (58.3) NS
gen therapy group. Our good results may be explained by Hypertension 16 (26.7) 5 (41.7) NS
the relative young age of our patients and especially the Heart disease 8 (13.3) 8 (66.7) 0.038
improvement of treatment options (adjunctive hyperbaric Lung disease 4 (6.7) 1 (8.3) NS
oxygen therapy to radical surgical debridement, regularly Liver disease 5 (8.3) 1 (8.3) NS
wound debridement and dressings, and broad spectrum anti- Kidney disease 6 (10.0) 2 (16.7) NS
biotic coverage). Hyperbaric oxygen therapy is particularly vascular disease 8 (13.3) 2 (16.7) NS
helpful in increasing oxygen tension in infected tissue and Malignant disease 2 (3.3) 3 (25.0) NS
in killing anaerobic bacteria limiting the extent of necrosis Severe sepsis on
6 (10.0) 9 (75.0) 0.027
and improving wound healing.6 admission
Multiple predisposing factors for Fournier’s gangrene Septic shock on
0 (0.0) 2 (16.7) NS
include diabetes mellitus, arterial hypertension, chronic admission
renal failure, systemic disorders, malignant neoplasms, Diverting colostomy 10 (16.7) 4 (33.3) NS
chronic alcoholism, immunosuppression, and local trau- NS: nonsignificant (p > 0.05).
E802 CUAJ • November-December 2015 • Volume 9, Issues 11-12
Prognostic factors affecting mortality in Fournier’s gangrene
Table 4. Analysis of prognostic factors (quantitative body surface was significantly higher in non-survivors than
variables)
in survivors (p = 0.033), as confirmed in other studies.8,27
Survivors (min, Non-survivors
p Consequently, we believe that the extent of necrosis is
Variables max) (min, max)
(n = 60) (n = 12)
value one of the most important prognostic factors in Fournier’s
Age 50 (40, 59) 63 (51, 70) NS gangrene. Furthermore, most authors advocate that intestinal
Heart rate, bpm 88 (80, 103) 91 (81, 112) NS diversion should be used in cases of colorectal perforation or
Respiration rate, rpm 19 (17, 21) 20 (18, 22) NS anal sphincter involvement, or simply to prevent fecal con-
Temperature, °C 37.7 (37.0, 38.4) 38.6 (36.6, 39.0) NS tamination of the wound. In our study, diverting colostomy
Hemoglobin, (g/dL) 13 (10.5, 14.1) 10.8 (8.6, 12.0) 0.023 was done in 14 patients, but did not show any prognostic
Hematocrit, % 38.2 (30.4, 41.1) 30.4 (27.1, 35) 0.019 value.28,29 In addition, wound cultures were mostly poly-
White blood cell microbial in our patients, and the isolated microorganisms
15.7 (14.3, 21.5) 22.8 (15.6, 33.1) NS were not significantly different between survivors and non-
count, 103 cells/mm3
Urea 57 (36, 74) 103 (86, 147) 0.009 survivors, concurrent with other reports.3,4
Creatinine, mg/dL 1.2 (1.0, 1.7) 1.8 (1.1, 4.5) 0.042 Some laboratory parameters, such as low levels of hema-
Sodium, mmol/L 134 (131, 136) 135 (129, 138) NS tocrit and albumin, or high levels of urea, creatinine, leu-
Potassium, mmol/L 3.8 (3.5, 4.3) 4.4 (3.9, 5.6) 0.026 kocyte count, sodium, potassium, alkaline phosphatase and
GGT, IU/L 58 (34, 90) 52 (44, 68) NS lactate dehydrogenase, have been shown to have a prognostic
Alkaline phosphatase, value.4,6,13 In our study, mortality was significantly higher in
91 (57, 146) 130 (96, 237) NS
IU/L patients with low levels of hemoglobin (p = 0.023) and hema-
Venous bicarbonate,
22.4 (20.1, 23.7) 21.6 (18.8, 24.2) NS
tocrit (p = 0.019), as well as elevated levels of serum urea
mmol/L (p = 0.009), creatinine (p = 0.042) and potassium (p = 0.026).
Duration of These biologic disorders reflect renal dysfunction probably
3 (3, 5) 4 (2, 5) NS
symptoms, days
related to septic shock and may be the initial stage of a multi-
Affected surface, % 3(2, 5) 6(4, 13) 0.033
organ failure. Reduced hemoglobin and hematocrit levels
No. debridements 3(3, 4) 4(3, 5) NS
showed an altered general status in the patient. This alteration
Length of hospital
32(15, 62) 12(3, 25) NS was also related to the sepsis from Fouriner’s gangrene. In
stay, days
addition, severe sepsis on admission was also predictive for
FGSI score 5(3, 7) 10(7, 12) 0.002
Min: minimum; max: maximum; bpm: beats per minute; rpm: breaths per minute; GGT:
higher mortality in our patients (p = 0.027).
gamma-glutamyl transpeptidase; FGSI score: Fournier’s Gangrene Severity Index Score; Laor and colleagues developed a prognostic index (FGSI)
NS: nonsignificant (p > 0.05).
to determine the severity of infection and prognosis of patients
with Fournier’s gangrene, by using vital signs and laboratory
Diabetes mellitus is the most common predisposing factor, data.5 In this system, a FGSI of 9 was used as a threshold
but does not affect the prognosis and clinical outcome.19,20 parameter to predict outcome. FGSI ≥9 had a 75% probability
The most common concomitant disease in our study was of death and FGSI <9 had a 78% probability of survival. The
also diabetes (38%), but it was not significantly related to cut-off point and its predictive value have been validated
mortality. Only the mortality rate in heart disease was signifi- in other current series.15,30 In our case, the FGSI was signifi-
cantly higher (p = 0.038), similar to reports by García Marín cantly higher in non-surviving patients with an acceptable
and Jiménez-Pacheco and their respective colleagues.6,17 discriminatory capacity (p = 0.002). Such results support the
Given the severity of symptoms and the rapid progression established threshold value of 9 and the validity of the FGSI.
of necrosis, it is important to recognize Fournier’s gangrene Recently, Yilmazlar and colleagues suggested a new scoring
early, when cutaneous manifestations are minimal. Delay in system, the Uludag FGSI (UFGSI), adding 2 parameters (age
surgical debridement can increase the extent of the necrosis, and disease extension) to the classic FGSI score.31
and lead to a worse prognosis.21,22 Early admission, rapid Based on the results of our study, we concluded that
diagnosis, and adequate surgical treatment are crucial com- the use of a prognostic scoring system is important to iden-
ponents in achieving a successful outcome. The median tify patients with a greater risk of major complications or
duration of symptoms before admission was a day longer in death. Extra attention is required to manage these patients.
non-survivors (4 vs. 3), but this was not predictive for mortal- A more aggressive treatment with extensive surgical debride-
ity in our study. Moreover, Chawla and colleagues reported ment, appropriate antibiotic and adequate fluid resuscitation
that the number of surgical debridement negatively affected should be started at admission. A careful follow-up must be
mortality since it might reflect a greater extent of disease.23 In performed in the intensive care unit to reduce mortality and
our series, there were no differences regarding this parameter to improve outcome.
between survivors and non-survivors, consistent with other Major limitations of this study include its retrospective
studies.24-26 In contrast, we found that the extent of affected design and small sample size, a common limitation due to
CUAJ • November-December 2015 • Volume 9, Issues 11-12 E803
Tarchouli et al.
10. Sorensen MD, Krieger JN, Rivara FP, et al. Fournier’s gangrene: Management and mortality predictors in
the rarity of Fournier’s gangrene. A multi-institutional pro- a population based study. J Urol 2009;182:2742-7. http://dx.doi.org/10.1016/j.juro.2009.08.050.
spective study is needed to accrue the number of patients 11. Eke N. Fournier’s gangrene: A review of 1726 cases. Br J Surg 2000;87:718-28. http://dx.doi.
necessary to further validate the prognostic factors of this org/10.1046/j.1365-2168.2000.01497.x.
entity. 12. Czymek R, Frank P, Limmer S, et al. Fournier’s gangrene: Is the female gender a risk factor? Langenbecks
Arch Surg 2010;395:173-80. http://dx.doi.org/10.1007/s00423-008-0461-9.
13. Corcoran AT, Smaldone MC, Gibbons EP, et al. Validation of the Fournier’s gangrene severity index in a
Conclusion large contemporary series. J Urol 2008;180:944-8. http://dx.doi.org/10.1016/j.juro.2008.05.021.
14. Sorensen MD, Krieger JN, Rivara FP, et al. Fournier’s gangrene: Population based epidemiology and
Despite overall improvement in the antibiotic spectrum and outcomes. J Urol 2009;181:2120-6. http://dx.doi.org/10.1016/j.juro.2009.01.034.
surgical techniques, Fournier’s gangrene continues to be 15. Lujan Marco S, Budia A, Di Capua C, et al. Evaluation of a severity score to predict the prognosis of Fournier’s
a serious pathology with a high mortality rate. Early rec- gangrene. BJU Int 2010;106:373-6. http://dx.doi.org/10.1111/j.1464-410X.2009.09075.x.
16. Shyam DC, Rapsang AG. Fournier’s gangrene. Surgeon 2013;11:222-32. http://dx.doi.org/10.1016/j.
ognition of infection with prompt radical debridement is surge.2013.02.001.
the mainstays of successful management. Comprehensive 17. Jimenez-Pacheco A, Arrabal-Polo MA, Arias-Santiago S, et al. Fournier gangrene: Description of 37 cases
evaluation of metabolic status and physiological parameters, and analysis of associated health care costs. Actas Dermosifiliogr 2012;103:29-35. http://dx.doi.
predisposing factors, and the extent of necrosis may help org/10.1016/j.adengl.2011.04.007.
determine mortality risk and establish an optimal treatment. 18. Torremadé Barreda J, Millán Scheiding M, Suárez Fernández C, et al. Fournier gangrene. A retrospective
study of 41 cases. Cir Esp 2010;87:218-23. http://dx.doi.org/10.1016/S2173-5077(10)70051-X.
The FGSI score remains a simple and valid method to evalu- 19. Nisbet AA, Thompson IM. Impact of diabetes mellitus on the presentation and outcomes of Fournier’s
ate infection severity and predict outcome in patients with gangrene. Urology 2002;60:775-9.
Fournier’s gangrene. 20. Yanar H, Taviloglu K, Ertekin C, et al. Fournier’s gangrene: Risk factors and strategies for management.
World J Surg 2006;30:1750-4. http://dx.doi.org/10.1007/s00268-005-0777-3.
Competing interests: The authors declare no competing financial or personal interests. 21. Janane A, Hajji F, Ismail TO, et al. Hyperbaric oxygen therapy adjunctive to surgical debridement in
management of Fournier’s gangrene: Usefulness of a severity index score in predicting disease gravity
and patient survival. Actas Urol Esp 2011;35:332-8. http://dx.doi.org/10.1016/j.acuro.2011.01.019.
22. Tuncel A, Keten T, Aslan Y, et al. Comparison of different scoring systems for outcome prediction in patients
This paper has been peer-reviewed. with Fournier’s gangrene: Experience with 50 patients. Scand J Urol 2014;48:393-9. http://dx.doi.org
/10.3109/21681805.2014.886289.
23. Chawla SN, Gallop C, Mydlo JH. Fournier’s gangrene: An analysis of repeated surgical debridement. Eur
Urol 2003;43:572-5.
References 24. Erol B, Tuncel A, Hanci V, et al. Fournier’s gangrene: Overview of prognostic factors and definition of new
prognostic parameter. Urology 2010;75:1193-8. http://dx.doi.org/10.1016/j.urology.2009.08.090.
1. Fournier JA. Jean-Alfred Fournier 1832-1914. Gangrene foudroyante de la verge (overwhelming gangrene). 25. Palmer LS, Winter HI, Tolia BM, et al. The limited impact of involved surface area and surgical debridement
Sem Med 1883. Dis Colon Rectum 1988;31:984-8. on survival in Fournier’s gangrene. Br J Urol 1995;76:208-12.
2. Benjelloun el B, Souiki T, Yakla N, et al. Fournier’s gangrene: Our experience with 50 patients and analysis 26. Roghmann F, von Bodman C, Loppenberg B, et al. Is there a need for the Fournier’s gangrene severity
of factors affecting mortality. World J Emerg Surg 2013;8:13. http://dx.doi.org/10.1186/1749- index? Comparison of scoring systems for outcome prediction in patients with Fournier’s gangrene. BJU
7922-8-13. Int 2012;110:1359-65. http://dx.doi.org/10.1111/j.1464-410X.2012.11082.x.
3. Altarac S, Katusin D, Crnica S, et al. Fournier’s gangrene: Etiology and outcome analysis of 41 patients. 27. Ruiz-Tovar J, Cordoba L, Devesa JM. Prognostic factors in Fournier gangrene. Asian J Surg 2012;35:37-41.
Urol Int 2012;88:289-93. http://dx.doi.org/10.1159/000335507. http://dx.doi.org/10.1016/j.asjsur.2012.04.006.
4. García Marín A, Turégano Fuentes F, Cuadrado Ayuso M, et al. Predictive factors for mortality in 28. Akcan A, Sozuer E, Akyildiz H, et al. Necessity of preventive colostomy for Fournier’s gangrene of the
Fournier’s gangrene: A series of 59 cases. Cir Esp 2015;93:12-7. http://dx.doi.org/10.1016/j. anorectal region. Ulus Travma Acil Cerrahi Derg 2009;15:342-6.
cireng.2014.03.013. 29. Ozturk E, Sonmez Y, Yilmazlar T. What are the indications for a stoma in Fournier’s gangrene? Colorectal
5. Laor E, Palmer LS, Tolia BM, et al. Outcome prediction in patients with Fournier’s gangrene. J Urol Dis 2011;13:1044-7. http://dx.doi.org/10.1111/j.1463-1318.2010.02353.x.
1995;154:89-92. 30. Oymaci E, Coskun A, Yakan S, et al. Evaluation of factors affecting mortality in Fournier’s Gangrene:
6. García Marín A, Martín Gil J, Vaquero Rodríguez A, et al. Fournier’s gangrene: analysis of prognostic Retrospective clinical study of sixteen cases. Ulus Cerrahi Derg 2014;30:85-9. http://dx.doi.
variables in 34 patients. Eur J Trauma Emerg Surg 2011;37:141-5. http://dx.doi.org/10.1007/ org/10.5152/UCD.2014.2512.
s00068-010-0028-7. 31. Yilmazlar T, Ozturk E, Ozguc H, et al. Fournier’s gangrene: An analysis of 80 patients and a novel
7. Tuncel A, Aydin O, Tekdogan U, et al. Fournier’s gangrene: Three years of experience with 20 patients scoring system. Tech Coloproctol 2010;14:217-23. http://dx.doi.org/10.1007/s10151-010-0592-1.
and validity of the Fournier’s Gangrene Severity Index Score. Eur Urol 2006;50:838-43. http://dx.doi.
org/10.1016/j.eururo.2006.01.030.
8. Yeniyol CO, Suelozgen T, Arslan M, et al. Fournier’s gangrene: Experience with 25 patients and use of
Correspondence: Dr. Mohamed Tarchouli, Department of Digestive Surgery, Mohammed V Military
Fournier’s gangrene severity index score. Urology 2004;64:218-22. http://dx.doi.org/10.1016/j. Hospital, Rabat, Morocco; mtarchouli@gmail.com
urology.2004.03.049.
9. Aridogan IA, Izol V, Abat D, et al. Epidemiological characteristics of Fournier’s gangrene: A report of 71
patients. Urol Int 2012;89:457-61. http://dx.doi.org/10.1159/000342407.
E804 CUAJ • November-December 2015 • Volume 9, Issues 11-12
View publication stats
You might also like
- NCM 117 Psychiatric Nursing MODULE 7Document27 pagesNCM 117 Psychiatric Nursing MODULE 7Meryville JacildoNo ratings yet
- 01-ACMC Case Study ReferenceDocument8 pages01-ACMC Case Study ReferenceJean Sunny100% (1)
- Blood AnalysisDocument4 pagesBlood AnalysisSuman Malik SehrawatNo ratings yet
- Jurnal MenagementDocument5 pagesJurnal Menagementelsy oktaviaNo ratings yet
- SepsisDocument9 pagesSepsisLeón TorresNo ratings yet
- 1 Elassmy2016Document5 pages1 Elassmy2016aldillawrNo ratings yet
- Surgical Management of Fourniers Gangrene A Seven Year Experience at The Philippine General HospitalDocument6 pagesSurgical Management of Fourniers Gangrene A Seven Year Experience at The Philippine General HospitalGian PagadduNo ratings yet
- A Study On Fournier's Gangrene: Original ResearchDocument5 pagesA Study On Fournier's Gangrene: Original Researchzetta369No ratings yet
- Prognostic Factor Fournier GangreneDocument7 pagesPrognostic Factor Fournier GangreneRaeni Dwi PutriNo ratings yet
- Postoperative Nausea and Vomiting: Retrospective Comparative Statistical StudyDocument19 pagesPostoperative Nausea and Vomiting: Retrospective Comparative Statistical StudyIJAR JOURNALNo ratings yet
- Cureus 0013 00000015301Document5 pagesCureus 0013 00000015301Abdunur MusemakweliNo ratings yet
- 55-Article Text-103-1-10-20200408Document7 pages55-Article Text-103-1-10-20200408Kshitiz112No ratings yet
- The Study of Epidemiological, Clinical and Biochemical Characteristics of Covid 19 Non Survivors in A Tertiary Care Hospital of Southern IndiaDocument6 pagesThe Study of Epidemiological, Clinical and Biochemical Characteristics of Covid 19 Non Survivors in A Tertiary Care Hospital of Southern IndiaIJAR JOURNALNo ratings yet
- Ioi80197 463 473Document11 pagesIoi80197 463 473Phạm LinhNo ratings yet
- Fourniers Gangrene and Its Management A Prospective StudyDocument12 pagesFourniers Gangrene and Its Management A Prospective StudyAthenaeum Scientific PublishersNo ratings yet
- Founier GangrenDocument5 pagesFounier GangrenJohannes MarpaungNo ratings yet
- Postoperative Infection and Mortality Following Elective Surgery in The International Surgical Outcomes Study (ISOS)Document32 pagesPostoperative Infection and Mortality Following Elective Surgery in The International Surgical Outcomes Study (ISOS)Antonio Carlos Betanzos PlanellNo ratings yet
- NF UkDocument7 pagesNF UkMax FaxNo ratings yet
- 1 LRDocument12 pages1 LRaoonNo ratings yet
- Full TextDocument32 pagesFull TextHam FGNo ratings yet
- Necrotising Fasciitis or Pyoderma Gangrenosum: A Fatal DilemmaDocument8 pagesNecrotising Fasciitis or Pyoderma Gangrenosum: A Fatal DilemmayuktianaNo ratings yet
- Jurnal PatogenesisDocument6 pagesJurnal PatogenesisErmiati EmhyNo ratings yet
- The Surgical Management of Parasitic Diseases: George Tsoulfas Jamal J. Hoballah George C. Velmahos Yik-Hong HoDocument366 pagesThe Surgical Management of Parasitic Diseases: George Tsoulfas Jamal J. Hoballah George C. Velmahos Yik-Hong HoEsdinawan Carakantara SatrijaNo ratings yet
- LancetDocument11 pagesLancetvieira.beatrizNo ratings yet
- Fernandez Alcaraz2019Document5 pagesFernandez Alcaraz2019ARQ. HernandezNo ratings yet
- 1-s2.0-S1201971212000264-main_2Document7 pages1-s2.0-S1201971212000264-main_2lee zaraNo ratings yet
- A Retrospective Analysis of Fourniers Gangrene at A TertiaryGovernment Hospital in The PhilippinesDocument3 pagesA Retrospective Analysis of Fourniers Gangrene at A TertiaryGovernment Hospital in The PhilippinesGian PagadduNo ratings yet
- The Epidemiology, Antibiotic Resistance and Post-Discharge Course of Peritonsillar Abscesses in London, OntarioDocument7 pagesThe Epidemiology, Antibiotic Resistance and Post-Discharge Course of Peritonsillar Abscesses in London, OntarioMaharaniNo ratings yet
- Chen 2018Document5 pagesChen 2018Teja Laksana NukanaNo ratings yet
- 150-Final Document To Be Uploaded-1966-1-10-20230110Document5 pages150-Final Document To Be Uploaded-1966-1-10-20230110M Hassan RafiqNo ratings yet
- The Presentation, Management and Outcomes of Fournier's Gangrene at A Tertiary Urology Referral Centre in South AfricaDocument6 pagesThe Presentation, Management and Outcomes of Fournier's Gangrene at A Tertiary Urology Referral Centre in South AfricaAngeel GomezNo ratings yet
- Clinical Characteristics, Laboratory Abnormalities and Outcome of Covid-19 Positive Patients Admitted in Tertiary Care Hospital of KarachiDocument8 pagesClinical Characteristics, Laboratory Abnormalities and Outcome of Covid-19 Positive Patients Admitted in Tertiary Care Hospital of KarachiIJAR JOURNALNo ratings yet
- INSULINOMADocument6 pagesINSULINOMASaifullah NaseerNo ratings yet
- Horne, A. W., & Missmer, S. A. (2022) - Pathophysiology, Diagnosis, and Management of Endometriosis. BMJ, 379.Document19 pagesHorne, A. W., & Missmer, S. A. (2022) - Pathophysiology, Diagnosis, and Management of Endometriosis. BMJ, 379.Hernando Rivera-DuqueNo ratings yet
- 01singh PDFDocument9 pages01singh PDFTri Santi InggianyNo ratings yet
- Pathophysiology, Diagnosis, and ManagementDocument19 pagesPathophysiology, Diagnosis, and Management1832303aNo ratings yet
- CC 12570Document9 pagesCC 12570Kornelis AribowoNo ratings yet
- Candidiasis in PICUDocument6 pagesCandidiasis in PICUMeirinda HidayantiNo ratings yet
- Study of The Prevalence of Nosocomial Infections in The University Hospital Center of Béni-Messous, Algiers in 2023 - AlgeriaDocument6 pagesStudy of The Prevalence of Nosocomial Infections in The University Hospital Center of Béni-Messous, Algiers in 2023 - AlgeriaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Fournier's Gangrene: An Experience in Tertiary Care HospitalDocument9 pagesFournier's Gangrene: An Experience in Tertiary Care HospitalKriti KumariNo ratings yet
- Envenimations ViperinesDocument6 pagesEnvenimations ViperinesIJAR JOURNALNo ratings yet
- Fungal Endocarditis Current ChallengesDocument5 pagesFungal Endocarditis Current ChallengesmarnixvonkempNo ratings yet
- Clinical Trends of Ectopic Pregnancy - A Study in A Tertiary Care Hospital of West Bengal, IndiaDocument7 pagesClinical Trends of Ectopic Pregnancy - A Study in A Tertiary Care Hospital of West Bengal, IndiaIJAR JOURNALNo ratings yet
- 2021 Amaylia Oehadian - Putri - Uun - Bahti - Evan - Jeffery (U) - Erythropoiesis Differences in Various ClinicalDocument6 pages2021 Amaylia Oehadian - Putri - Uun - Bahti - Evan - Jeffery (U) - Erythropoiesis Differences in Various ClinicalEvan SusandiNo ratings yet
- Examination of Ulcero-Proliferative Lesions of Oropharynx and Oral Cavity - A Clinical PerspectiveDocument7 pagesExamination of Ulcero-Proliferative Lesions of Oropharynx and Oral Cavity - A Clinical PerspectiveInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Analysis of Mortality in Covid 19 Patients - A Study in A District Covid Hospital in Andhra Pradesh During The First WaveDocument6 pagesAnalysis of Mortality in Covid 19 Patients - A Study in A District Covid Hospital in Andhra Pradesh During The First WaveIJAR JOURNALNo ratings yet
- Management of Fournier GangrenDocument4 pagesManagement of Fournier GangrenArby ShafaraNo ratings yet
- Fournier Gangrene Pictorial ReviewDocument11 pagesFournier Gangrene Pictorial ReviewKristell PérezNo ratings yet
- Jurnal 3 Abses Leher DalamDocument6 pagesJurnal 3 Abses Leher DalamRohayu AsnawiNo ratings yet
- Prospective Cohort StudyDocument6 pagesProspective Cohort StudyMãnoj MaheshwariNo ratings yet
- Journal Homepage: - : IntroductionDocument8 pagesJournal Homepage: - : IntroductionIJAR JOURNALNo ratings yet
- Fournier's Gangrene. A Clinical ReviewDocument9 pagesFournier's Gangrene. A Clinical ReviewJohannes MarpaungNo ratings yet
- Odontogenic Necrotizing Fasciitis: A Systematic Review of The LiteratureDocument7 pagesOdontogenic Necrotizing Fasciitis: A Systematic Review of The LiteratureDenta HaritsaNo ratings yet
- Assessment of Postoperative Anaesthetic Incidents in The Recovery RoomDocument5 pagesAssessment of Postoperative Anaesthetic Incidents in The Recovery RoomIJAR JOURNALNo ratings yet
- Fournier's Gangrene. A Clinical Review: ArticleDocument9 pagesFournier's Gangrene. A Clinical Review: ArticleMichael Stevent Cuellar RodriguezNo ratings yet
- JC On StenoDocument5 pagesJC On StenotanviaggrawalNo ratings yet
- 4 SaDocument6 pages4 SaRizqi AmaliaNo ratings yet
- Efficacy of Corticosteroids in Non-Intensive Care Unit Patients With COVID-19 Pneumonia From The New York Metropolitan RegionDocument14 pagesEfficacy of Corticosteroids in Non-Intensive Care Unit Patients With COVID-19 Pneumonia From The New York Metropolitan RegionicarosalernoNo ratings yet
- Morra 2018Document9 pagesMorra 2018Distro AwanNo ratings yet
- The Incidence and Risk Factors of Ventilator-Associated Pneumonia in ICUDocument6 pagesThe Incidence and Risk Factors of Ventilator-Associated Pneumonia in ICUWentiNo ratings yet
- Mudança Epidemiológica Gonococo FrançaDocument4 pagesMudança Epidemiológica Gonococo FrançaEliseu AmaralNo ratings yet
- Community-Acquired Pneumonia: Strategies for ManagementFrom EverandCommunity-Acquired Pneumonia: Strategies for ManagementAntoni TorresRating: 4.5 out of 5 stars4.5/5 (2)
- Method of Statement PCDocument8 pagesMethod of Statement PCAbada SaadNo ratings yet
- Clinical Leadership Development and Education For NursesDocument10 pagesClinical Leadership Development and Education For NursesVia Eliadora TogatoropNo ratings yet
- Ecm 216 Building Services Bab 3.2 Water Supply PDFDocument6 pagesEcm 216 Building Services Bab 3.2 Water Supply PDFAZUAN BIN AHMAD FAUZI100% (8)
- Shell Helix Ultra Professional AJ-L 0W-20: Main Applications Specifications, Approvals & RecommendationsDocument2 pagesShell Helix Ultra Professional AJ-L 0W-20: Main Applications Specifications, Approvals & RecommendationsMuhNo ratings yet
- Fed BatchDocument3 pagesFed BatchKrishnadev Madhavan NairNo ratings yet
- Guidelines For Open Plant StructuresDocument6 pagesGuidelines For Open Plant StructuresIndrawNo ratings yet
- 2024 MSDocument38 pages2024 MS6vnh5z7fnjNo ratings yet
- Msds For Skim CoatDocument8 pagesMsds For Skim Coatlovely palomaNo ratings yet
- Homework 2Document9 pagesHomework 2Alexis R. CamargoNo ratings yet
- AHA Anderson StudyDocument8 pagesAHA Anderson Studykaren lilianaNo ratings yet
- NestleDocument12 pagesNestleParadoxNo ratings yet
- Day 1 Menu: BreakfastDocument11 pagesDay 1 Menu: BreakfastAndrew HubbardNo ratings yet
- WSNZ 1311 Construction Machinery Fact Sheet v5Document4 pagesWSNZ 1311 Construction Machinery Fact Sheet v5Gemunu WeerethungaNo ratings yet
- Home Remedies To Treat Dupuytren S Disease OrthoBethesda .G-Job 84Document15 pagesHome Remedies To Treat Dupuytren S Disease OrthoBethesda .G-Job 84paulsub63No ratings yet
- Herbalife SurveyDocument1 pageHerbalife Surveyrhymes2u100% (1)
- Antibiotic Microbial Resistance (AMR) Removal Efficiencies by 2019 PDFDocument13 pagesAntibiotic Microbial Resistance (AMR) Removal Efficiencies by 2019 PDFdebleenaNo ratings yet
- AFD Runs End JanuaryDocument3 pagesAFD Runs End Januarylarry_kelley_1No ratings yet
- Abortion Pro Life Vs Pro ChoiceDocument6 pagesAbortion Pro Life Vs Pro Choiceapi-356865000No ratings yet
- PE 12 HOPE 3 Q2 Module 3 Lesson 6 7 by FarrahDocument33 pagesPE 12 HOPE 3 Q2 Module 3 Lesson 6 7 by Farrahricsha masanayNo ratings yet
- Parental Substance AbuseDocument10 pagesParental Substance Abuseapi-360330020No ratings yet
- Daftar Pustaka-MendeleyDocument3 pagesDaftar Pustaka-Mendeleynurafiat175No ratings yet
- Visa Invitation LettersDocument6 pagesVisa Invitation LettersPrince SharmaNo ratings yet
- Monthly AUGUST 2015 REPOKHNDocument13 pagesMonthly AUGUST 2015 REPOKHNAkash PGNo ratings yet
- ITRC 2009 - LNAPL Guidance DocumentDocument157 pagesITRC 2009 - LNAPL Guidance DocumentFelipe NaretaNo ratings yet
- Umer Mehmood: Personal ProfileDocument3 pagesUmer Mehmood: Personal ProfileMuhammad sufyan Muhammad sufyanNo ratings yet
- Psychology Test 2 Practice QuestionsDocument15 pagesPsychology Test 2 Practice Questionsshamim3261100% (3)
- Makassar Workshop - BeneFusion 5 Series 20190626Document49 pagesMakassar Workshop - BeneFusion 5 Series 20190626wahyu bunha rNo ratings yet