Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
18 viewsPediatric Hematologic Disorders
Pediatric Hematologic Disorders
Uploaded by
candiaangeltherese1318238This document discusses hematologic disorders in children. It provides an overview of the hematologic system including the types of blood cells produced in the bone marrow - red blood cells, white blood cells, and platelets. It then describes common disorders that can affect these cells such as anemias that impact red blood cell counts, bleeding disorders like hemophilia, and cancers of the blood cells known as leukemias and lymphomas. The summary concludes by outlining some of the signs and symptoms clinicians examine for when evaluating a child for a potential hematologic condition.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You might also like
- ATLSPracticeTest2 With AnswersDocument10 pagesATLSPracticeTest2 With Answersemad mohamed100% (1)
- Hematologic Disorders NotesDocument19 pagesHematologic Disorders Notesmikkagreen95% (22)
- 4b7c36 PDFDocument56 pages4b7c36 PDFsgoranksNo ratings yet
- Ghid Plante Medicinale Flora SpontanaDocument52 pagesGhid Plante Medicinale Flora Spontanaa100% (4)
- Sodium Lauryl Sulfate - WebDocument2 pagesSodium Lauryl Sulfate - WebMatea MareljaNo ratings yet
- What Is Desoxy DHEA and How Does It WorkDocument2 pagesWhat Is Desoxy DHEA and How Does It WorkdenovonutritionNo ratings yet
- Hematologic DisordersDocument8 pagesHematologic DisordersCorpus, Irene Zen P.No ratings yet
- Blood and LymphaticDocument4 pagesBlood and LymphaticCKNo ratings yet
- Hematologic DisorderDocument7 pagesHematologic Disordermawel100% (2)
- Anaphy Chapter 11 BloodDocument4 pagesAnaphy Chapter 11 BloodJohnNo ratings yet
- CARDIOVASCULARDocument20 pagesCARDIOVASCULARpriya garciaNo ratings yet
- (Hema) 1.1 Intro To Hema (Perez) - PANDADocument6 pages(Hema) 1.1 Intro To Hema (Perez) - PANDATony DawaNo ratings yet
- Child With Hematologic DisordersDocument5 pagesChild With Hematologic Disordersjadengg.pandak014No ratings yet
- Blood - Complete NotesDocument5 pagesBlood - Complete NotesLance CarandangNo ratings yet
- Blood SBDocument20 pagesBlood SBnoshNo ratings yet
- Circulatory System Reviewer - BAYLONDocument33 pagesCirculatory System Reviewer - BAYLONElijah Joaquin Payumo BaylonNo ratings yet
- BLOODDocument4 pagesBLOODcarolNo ratings yet
- Blood: HematopoiesisDocument6 pagesBlood: HematopoiesisMary Rose T. RecientesNo ratings yet
- HEMATOPOESISDocument71 pagesHEMATOPOESISHussenNo ratings yet
- Hematopoiesis ErythropoiesisDocument8 pagesHematopoiesis ErythropoiesisASHLEY ALEXIS GUEVARRANo ratings yet
- Types:: Precursor CellsDocument4 pagesTypes:: Precursor CellsGrace UrbanoNo ratings yet
- Cardiovascular System - BloodDocument8 pagesCardiovascular System - BloodVernice LopezNo ratings yet
- CBC Reviewer Anaphy LabDocument9 pagesCBC Reviewer Anaphy LabARVINE JUSTINE CORPUZNo ratings yet
- Hema Quiz 1Document8 pagesHema Quiz 1Shianne RacadioNo ratings yet
- CHAPTER 2 HematopoiesisDocument7 pagesCHAPTER 2 HematopoiesisAMELIA DALE MARQUEZNo ratings yet
- Module 2 PPT NOTES HematopoiesisDocument8 pagesModule 2 PPT NOTES HematopoiesisMohammad MasacalNo ratings yet
- Blood 2Document4 pagesBlood 2Jhes D.No ratings yet
- Blood Chapter 11Document4 pagesBlood Chapter 11James CastroNo ratings yet
- Hemolytic Anemia IntrinsicDocument14 pagesHemolytic Anemia IntrinsicSophia Gail ChingNo ratings yet
- Group1 Hematology Prelim Learning SummaryDocument22 pagesGroup1 Hematology Prelim Learning Summarylai cruzNo ratings yet
- vt59.2708-21242375124 394146998891967 4683953301704066077 n.pdfHEMA-HANDOUTS-1.pdf NC Cat 106&ccb 1-7&Document15 pagesvt59.2708-21242375124 394146998891967 4683953301704066077 n.pdfHEMA-HANDOUTS-1.pdf NC Cat 106&ccb 1-7&jasminemuammilNo ratings yet
- Chapter 11 - BloodDocument33 pagesChapter 11 - BloodCORONEL, SOPHIANo ratings yet
- Blood (Anaphy)Document8 pagesBlood (Anaphy)CORONEL, SOPHIANo ratings yet
- Hema 1A Lec 1 Shift Reviewer Hematopoiesis Prepared By: C Hematopoiesis DefinedDocument7 pagesHema 1A Lec 1 Shift Reviewer Hematopoiesis Prepared By: C Hematopoiesis DefinedMarc ViduyaNo ratings yet
- Body Fluids and Circulation: BloodDocument2 pagesBody Fluids and Circulation: Bloodswayam bhosaleNo ratings yet
- Blood PPT NotesDocument7 pagesBlood PPT NotesArce JohnsonNo ratings yet
- Bloodandcoagulation 171230045036Document85 pagesBloodandcoagulation 171230045036Parmarkeval PravnibhaiNo ratings yet
- BloodDocument5 pagesBloodChelsie NicoleNo ratings yet
- Blood and Lymph (Autosaved)Document46 pagesBlood and Lymph (Autosaved)Shaikh SaqibNo ratings yet
- Development of Blood Cells 2019Document31 pagesDevelopment of Blood Cells 2019Muhammad Anas Abbal100% (1)
- RBC MorphologyDocument9 pagesRBC MorphologybiancsNo ratings yet
- Red Cell Physiology HemaDocument12 pagesRed Cell Physiology HemaIya BangalanNo ratings yet
- Blood Cells: By, Shobhana PandianDocument60 pagesBlood Cells: By, Shobhana PandianhrishikeshanandNo ratings yet
- 2014 Curs Hematologie - FinalDocument333 pages2014 Curs Hematologie - FinalRamona Andreea ConstantinNo ratings yet
- The Blood System: Arteries VeinsDocument17 pagesThe Blood System: Arteries VeinsØmNo ratings yet
- Module 2: Hematopoiesis I. General Principles of HematopoiesisDocument13 pagesModule 2: Hematopoiesis I. General Principles of HematopoiesisJane JapoleNo ratings yet
- Hematology Module 2 and 3Document11 pagesHematology Module 2 and 3SEAN MELNOR LOSBAÑESNo ratings yet
- Blood AnalysisDocument89 pagesBlood AnalysisRiddhi JaganiNo ratings yet
- Body Fluids and Circulation - NotesDocument12 pagesBody Fluids and Circulation - NotesSaloni GuptaNo ratings yet
- Lecture 14Document30 pagesLecture 14MOHAMMED ELNAGGARNo ratings yet
- Hematology 1 L1 Introduction To Hematology 1 LectureDocument2 pagesHematology 1 L1 Introduction To Hematology 1 LectureChelze Faith DizonNo ratings yet
- Human Histology Midterms: Blood and HemopoesisDocument3 pagesHuman Histology Midterms: Blood and Hemopoesisabi dimatulacNo ratings yet
- HO Notecards 1Document12 pagesHO Notecards 1MrSomnambululNo ratings yet
- Chapter 8 - Transport in MammalsDocument119 pagesChapter 8 - Transport in Mammalsapi-3728508100% (1)
- Blood Part 1Document35 pagesBlood Part 1Keziah TampusNo ratings yet
- ErythropoisisDocument47 pagesErythropoisisDisha SuvarnaNo ratings yet
- BloodDocument4 pagesBloodA R F I J U LNo ratings yet
- Introduction To HematologyDocument19 pagesIntroduction To HematologyDr Deepshikha ParakhNo ratings yet
- Lesson 3 Blood Updated 2020Document29 pagesLesson 3 Blood Updated 2020Waliid Khan 5SNo ratings yet
- Human Blood - English - 1561800335 - English - 1579005206Document9 pagesHuman Blood - English - 1561800335 - English - 1579005206Rahul Dev PNo ratings yet
- Assessment and Management of Patients With Hematologic DisordersDocument20 pagesAssessment and Management of Patients With Hematologic Disorderschristine mercado100% (1)
- Anatomy and Physiology With PhatophysiologyDocument6 pagesAnatomy and Physiology With PhatophysiologyJustine Mae OyongNo ratings yet
- 1.07 - The BloodDocument5 pages1.07 - The Blood13PLAN, SENTH RUEN, ANo ratings yet
- Blood: Blood Is Made Up ofDocument5 pagesBlood: Blood Is Made Up ofNatasha JeanNo ratings yet
- TRANSES ANAPHY Male Reproductive SystemDocument6 pagesTRANSES ANAPHY Male Reproductive SystemPia LouiseNo ratings yet
- Environmental Studies - Question Bank Multidisciplinary Nature of Environmental StudiesDocument6 pagesEnvironmental Studies - Question Bank Multidisciplinary Nature of Environmental StudiesAditya KapoorNo ratings yet
- Scientific Validation of Standardization of Narayana Chendrooram (Kannusamy Paramparai Vaithiyam) Through The Siddha and Modern TechniquesDocument12 pagesScientific Validation of Standardization of Narayana Chendrooram (Kannusamy Paramparai Vaithiyam) Through The Siddha and Modern TechniquesBala Kiran GaddamNo ratings yet
- B05 QuestionsDocument5 pagesB05 QuestionsMauriya SenthilnathanNo ratings yet
- 16 Psychological Tricks To Make People Like You Immediately - The IndependentDocument23 pages16 Psychological Tricks To Make People Like You Immediately - The IndependentMohammed SalihNo ratings yet
- Spotting: Class 12Document51 pagesSpotting: Class 12Ritik Kumar NayakNo ratings yet
- BP605T Unit 4-6Document482 pagesBP605T Unit 4-6Gyampoh SolomonNo ratings yet
- Bagaimana Petani Di Malaysia Mempunyai Pabrik PupukDocument14 pagesBagaimana Petani Di Malaysia Mempunyai Pabrik PupukShamNo ratings yet
- Oral MucosaDocument40 pagesOral MucosaLobna ElkilanyNo ratings yet
- Flik Silverpen's Guide ToDocument9 pagesFlik Silverpen's Guide ToSonny3091100% (1)
- Ecology NotesDocument13 pagesEcology NotesAndy TonNo ratings yet
- 96-117+Grima+2023+Article +paper-2Document22 pages96-117+Grima+2023+Article +paper-2Girma TimerNo ratings yet
- Myeloid Series Demonstration SlidesDocument30 pagesMyeloid Series Demonstration SlidesOsannah Irish InsongNo ratings yet
- Kebt108 PDFDocument16 pagesKebt108 PDFAdrija DasNo ratings yet
- All India Institute of Medical Sciences Nagpur Department of Obstetrics and GynecologyDocument19 pagesAll India Institute of Medical Sciences Nagpur Department of Obstetrics and GynecologySugan GavaskarNo ratings yet
- Master Your Research Skills A Practical IEP Approach GuideDocument45 pagesMaster Your Research Skills A Practical IEP Approach GuideSandeep SpNo ratings yet
- Paper of Lower Plant TaxonomyDocument35 pagesPaper of Lower Plant TaxonomyMuthiaranifsNo ratings yet
- Mituru Lova Vol V Issue 01Document20 pagesMituru Lova Vol V Issue 01Ravi PalihawadanaNo ratings yet
- 8 Muscular System Med TerminologyDocument30 pages8 Muscular System Med TerminologyKavita MahaseNo ratings yet
- The Champion Text Book On Embalming 1908Document712 pagesThe Champion Text Book On Embalming 1908Ocean100% (3)
- Transport of Lipids in The Body FluidsDocument1 pageTransport of Lipids in The Body FluidsZeedan MohammedNo ratings yet
- Edexcel Intl A Levels Biology Unit 3 Wbi13 v1Document6 pagesEdexcel Intl A Levels Biology Unit 3 Wbi13 v1seif nimer100% (1)
- Defler Et Al., 2001 PDFDocument60 pagesDefler Et Al., 2001 PDFANDRES HUMBERTO CARDONA CARDONANo ratings yet
- 2.2.56. Amino Acid Analysis PDFDocument7 pages2.2.56. Amino Acid Analysis PDFliska ramdanawatiNo ratings yet
- DAFTAR PUSTAKA - Docx2Document2 pagesDAFTAR PUSTAKA - Docx2AQ GhesTyNo ratings yet
Pediatric Hematologic Disorders
Pediatric Hematologic Disorders
Uploaded by
candiaangeltherese13182380 ratings0% found this document useful (0 votes)
18 views8 pagesThis document discusses hematologic disorders in children. It provides an overview of the hematologic system including the types of blood cells produced in the bone marrow - red blood cells, white blood cells, and platelets. It then describes common disorders that can affect these cells such as anemias that impact red blood cell counts, bleeding disorders like hemophilia, and cancers of the blood cells known as leukemias and lymphomas. The summary concludes by outlining some of the signs and symptoms clinicians examine for when evaluating a child for a potential hematologic condition.
Original Description:
Original Title
pediatric hematologic disorders
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses hematologic disorders in children. It provides an overview of the hematologic system including the types of blood cells produced in the bone marrow - red blood cells, white blood cells, and platelets. It then describes common disorders that can affect these cells such as anemias that impact red blood cell counts, bleeding disorders like hemophilia, and cancers of the blood cells known as leukemias and lymphomas. The summary concludes by outlining some of the signs and symptoms clinicians examine for when evaluating a child for a potential hematologic condition.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
18 views8 pagesPediatric Hematologic Disorders
Pediatric Hematologic Disorders
Uploaded by
candiaangeltherese1318238This document discusses hematologic disorders in children. It provides an overview of the hematologic system including the types of blood cells produced in the bone marrow - red blood cells, white blood cells, and platelets. It then describes common disorders that can affect these cells such as anemias that impact red blood cell counts, bleeding disorders like hemophilia, and cancers of the blood cells known as leukemias and lymphomas. The summary concludes by outlining some of the signs and symptoms clinicians examine for when evaluating a child for a potential hematologic condition.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 8
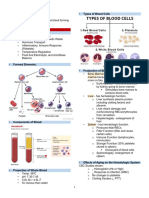
The Child with Hematologic Disorders 4.
Red blood cells
- Also called erythrocytes
Contents - Life span of 120 days
1. Review of the hematologic system - Transports oxygen & CO2 to & from the
2. Disorders of the red blood cells tissues
a. Anemia - Hemoglobin
i. Iron deficiency anemia o Molecule responsible for carrying O2
ii. Sickle cell anemia to the tissues
iii. Thalassemia o Somewhat affected by age
iv. Aplastic anemia ▪ 15-20 g/dL in neonates
3. Defects on hemostasis ▪ 12-15 g/dL in >2 mos
a. Hemophilia o Heme = iron
4. Neoplastic disorders o Globin = protein that attracts oxygen
a. Leukemia - Hematocrit
b. Lymphoma o Times 3 the amount of hemoglobin
i. Hodgkin’s disease o Normal 35-45%
ii. Non-Hodgkin’s lymphoma o Affected by hydration
▪ Elevated if px is dehydrated
▪ Decreased if fluid overload
The Hematologic System - Bilirubin is the waste product
- Interrelated w/ immune system in fighting off - Decreased RBC is manifested by fatigue since
infection there is an impairment in the oxygen-carrying
- Rises from the bone marrow capacity of the blood
- Stem cell - Erythropoietin
o Also called as pluripotent stem cells o Hormone produced by the kidney
o Has the ability to transform into any o Stimulates the production of RBCs in
type of cell the bone marrow
- Hematopoiesis - Lead can replace iron in the cells, causing
o The process of blood formation toxicity
o Occurs mainly in the liver and spleen 5. White blood cells
during intrauterine life - Also called leukocytes
o Red bone marrow is the main site - Fights off infection
after birth - Types
▪ As the child approaches o Granulocytes
adolescence, bone growth ▪ Neutrophils
ceases • Fight off acute
▪ Bone marrow in many bones infections or invading
can’t fr microorganisms
1. Bone marrow • Phagocytosis effect
- Red bone marrow is the main site of (engulfing the foreign
hematopoiesis after birth body)
- As the child approaches adolescence, the red • Remove dead cells
bone marrow can’t form blood cells since it has ▪ Eosinophils
transformed into the yellow bone marrow • Acts in allergic
o This is due to the cessation of bone reactions
growth • Defends against
- Creates the primitive form of blood cells called parasites & lung &
the blast cells skin infections
o Blast cells are the most immature form ▪ Basophils
of blood cells • Releases heparin &
o The precursor to RBCs, WBCs, & histamine
platelets • Protects against
2. Yellow bone marrow infections via
- Is made of fat deposits inflammation
3. Blood
• Also known as mast
- Composed of plasma & cells
cells
o Plasma is the fluid portion
o Agranulocytes
o Blood cell types originate from blast
▪ Lymphocytes
cells
• Main cells that fight
▪ RBC
infections
▪ WBC
• “natural killer cells”
▪ Platelets
• T cells & B cells - Physical examination
o B cells produce o Cardinal S&S
immunoglobulins ▪ Fatigue
▪ Monocytes ▪ Headache
• Help w/ neutrophils ▪ Vertigo
• Form macrophages in ▪ Irritability
the body tissues ▪ Depression
6. Platelets ▪ Anorexia & weight loss
- Also called thrombocytes ▪ Bleeding, bruising
- Coagulation or clotting process ▪ Heavy menstrual flow
o Adhere to one another & plug holes in ▪ Epistaxis
the tissues where there is bleeding ▪ Recurrent infections
- Releases serotonin ▪ Bone & joint pain
o Vasoconstrictor o Vital signs
o Decreases blood flow to the injured ▪ Tachycardia
area ▪ Tachypnea
- Normal: 150 – 450 x10^9 g/dL o Inspection
o Low levels manifest as abnormal ▪ Bruising
bleeding ▪ Pallor or flushing
7. Antibodies ▪ Jaundice (skin & eyes)
- Immunoglobulin A (IgA) ▪ Purpura
o Found in the linings of respi & GI tract • Blood spots or skin
o Also found in breastmilk hemorrhages
o Prevents large foreign bodies from • <4 mm are called
being absorbed in the GI tract petechiae
o Prevents adherence of pathogens to • >1 cm are called
mucosal cells ecchymoses
- Immunoglobulin G (IgG) ▪ Pruritus
o Most frequently occurring antibody in ▪ Cyanosis
plasma ▪ Retinal hemorrhage
o Neutralizes bacterial toxins ▪ Blurred vision
o Activates phagocytosis ▪ Lymphadenopathy
- Immunoglobulin M (IgM) ▪ Tachypnea, orthopnea, or
o Agglutinates antigens dyspnea
o Lyses cell walls ▪ Impaired thought process
o Discovered early in the course of an ▪ Lethargy
infection in the bloodstream ▪ Bone or joint swelling
- Immunoglobulin E (IgE) ▪ Hematuria
o Involved in immediate hypersensitivity ▪ Heavy menstruation
reactions o Palpation
o Bound to mast cells on tissue surfaces ▪ Decreased CRT
o Associated w/ allergy & parasitic ▪ Tenderness over lymph nodes
infections ▪ Hepatomegaly
- Immunoglobulin D (IgD) ▪ Splenomegaly
o Found in plasma ▪ Decreased muscle mass
o Receptor that binds antigens to ▪ Bone & joint tenderness
lymphocyte surfaces o Auscultation
▪ Heart murmurs
Nursing Process ▪ Abnormal lung sounds
1. Assessment - Diagnostic tests
- Health history o CBC w/ differential count
o History of present illness ▪ One of the most general
o Prenatal & family history screening test for hematologic
▪ Blood type & immune system problems
▪ Prematurity ▪ Differential count determines
▪ Low birth weight percentage of WBC present
▪ Diet & diet behaviors ▪ RBC count is the total # of
▪ Menstrual flow RBCs found in a cm3 of blood
▪ Exposure to infections ▪ WBC count is the total # of
▪ Fam history of bleeding circulating leukocytes
disorders
▪ Hemoglobin helps diagnosis o Chronic blood loss
of anemia ▪ Heavy menstrual flow
▪ Hematocrit measurement of ▪ GI bleeding
the state that PRBCs & o OTC drugs
measurement of RBC mass ▪ Long-term use (>3 mos) of
▪ MCV (mean corpuscular aspirin
volume) is the measurement o Celiac disease
of individual RBC size o Surgical removal of a part of the GI
▪ MCH (mean corpuscular tract
hemoglobin) measures the o Parasite infestations
average weight of hemoglobin ▪ Tapeworms
in the RBC ▪ Round worms
▪ MCHC (mean corpuscular - Body’s capacity to transport O2 is impaired
hemoglobin concentration) - IDA during pregnancy is associated w/ low
measures the average fetal BW & preterm birth
concentration of hemoglobin - Sa
in the RBC o Folic acid
o Bone marrow biopsy ▪ Used as supplementation
▪ Aspiration of bone marrow ▪ Synthetic
sample ▪ Can help prevent neural tube
▪ Aids in diagnosis of aplastic defects
anemia, leukemia, etc. o Folate
▪ Sedation is needed ▪ Naturally found in food
(Benadryl) ▪ Best source of vitamin B9
▪ Bleeding & hematoma ▪ Can help prevent neural tube
formation may occur upon defects
aspiration ▪ Do not overcook vegetables to
2. Nursing Diagnosis get the most folate
- Risk for deficient fluid volume - S&S
- Activity intolerance o Fatigue
- Fatigue o Pallor
- Risk for infection o Hypoxia
- Ineffective tissue perfusion o Weakness
- Risk for tissue injury o Activity intolerance
- Delayed growth & development o Poor weight gain
3. Planning o Overweight
4. Implementation o Infections
5. Evaluation o Hemorrhage
o Epistaxis
Disorders of the Red Blood Cells o Bruising
Anemia o Mucosal bleeding (oral, GI, vagina)
- Occurs when there is a low RBC count, - Risk factors
hematocrit, or hemoglobin o Prematurity
- Results in poorly oxygenated cells and - Complications (neural tube defects):
malfunction of the body organs & systems o Anencephaly
- Causes ▪ Parts of the brain & skull are
o Damage in the bone marrow missing
o Suppressed production of o Spina bifida
erythropoietin in the kidney ▪ Spine & spinal column doesn’t
o Nutritional component needed to form develop properly during
blood (iron) is insufficient intrauterine development
o Blood cells produced are poorly ▪ There is a gap in the spin
structured o Encephalocele
▪ Sac-like protrusion of the brain
Iron Deficiency Anemia & its membranes through an
- Hemoglobin synthesis is deficient opening in the skull
- Amount of hemoglobin circulating in the blood - Nursing management
is inadequate o Educate the parents about the diet &
- Caused by insufficient iron in the blood (heme treatment regimen:
component of hemoglobin is primarily iron) ▪ Prescribed iron supplement
o Inadequate iron intake therapy
o Malabsorption of iron in the GI tract
▪ Iron fortified milk, cereal, or o Fatigue
formula o Fever
▪ Avoid fresh cow’s milk to o Hematuria
avoid allergies & GI irritation o Swollen abdomen
▪ Food rich in iron o Painful erection
▪ Iron therapy may cause o Organ damage
constipation & dark green or o Pooling of blood
black stools o Growth retardation
▪ Safe storing of iron o Crisis episodes
▪ Take iron supplement w/ ▪ Caused by obstruction of
vitamin c sources to aid iron blood flow due to sickled cells
absorption or vaso-occlusion
o Administer vitamin B12 IM to treat o Sequestration
deficiency due to failure of gastric ▪ Aplastic crisis due to an
mucosa to secrete the intrinsic factor extreme drop of RBCs
needed to absorb vitamin B12 o Megaloblastic anemia
▪ Injected into the ventrogluteal ▪ Excess need for folic acid or
muscle vitamin B12
▪ Using z-track method o Hyper hemolytic crisis
o Assist in blood transfusion (PRBC) ▪ Rapid RBC destruction
o Oxygen supplementation if hypoxia is - Nursing diagnoses
presence o Pain rlt joint swelling
o Give liquid iron w/ a straw to avoid o Knowledge deficit rlt disease,
contact w/ & staining the teeth treatment, & prevention crisis
o Avoid substances that impair iron o Ineffective tissue perfusion rlt vaso-
absorption occlusion
▪ Antacids - Nursing management
▪ Milk o Assess for pain q2-4h
▪ Administer prescribed
analgesics
Sickle Cell Disease ▪ Pain scale <5 is not a priority
- Caused by a mutation in the hemoglobin ▪ Monitor for effectiveness
- Results in the sickle form of the RBC when it is ▪ Apply warm compress to joint
deoxygenated as prescribed
o RBCs have a shorter lifespan (20 ▪ Avoid cold compress bc it may
days) cause vasoconstriction
o Sickled RBCs are stiff and sticky o Provide rest periods
which may cause an obstruction in ▪ Encourage bed rest
smaller blood vessels o Prevent dehydration
o Obstruction causes hypoxia and ▪ Administer fluids
necrosis of the affected tissue ▪ Increase OFI unless
- Autosomal recessive disorder contraindicated
o Genes need to be inherited from both o Assist in BT of PRBC if prescribed
parents o Educate parents on the disease
o Only inheriting one gene result in a process & the prevention of crises
Sickle Cell Trait where a person is ▪ Sickle cell trait
asymptomatic and a carrier ▪ Sickle anemia
▪ Symptoms only present when ▪ Sickling
the O2 demands of the body o Prevent infection
increases ▪ Administer prescribed
o More common in Africans antibiotics
- Factors that trigger sickling ▪ Encourage immunization
o Hypoxia o Administer oxygen supplementation
o Increase in blood viscosity
▪ Due to an increased
concentration of sickle cells Thalassemia
- Clinical manifestations - Autosomal recessive disorder wherein there is
o Acute pain an impaction of the alpha & beta polypeptide
o Swollen, tender hands & feet chains in the hemoglobin A
o Hepatomegaly - Characterized by a deficient synthesis of
o Splenomegaly specific globulin chains of the hemoglobin
o Jaundice molecule
o Results in damaged RBCs o Thrombocytopenia
o Alpha thalassemia is a deficiency in - Also characterized by bone marrow hypoplasia
alpha globulin chains - Types
o Beta thalassemia is a deficiency in o Primary
beta globulin chains ▪ Congenital
- Overproduction of RBCs occur to compensate o Secondary
for hemolysis ▪ Acquired due to autoimmune
o Folic acid deficiency may occur due to disease
increased demands of the bone - Clinical manifestations
marrow o Lack of RBCs
- Types acc to presentation of symptoms ▪ Pallor
o Thalassemia major ▪ Lethargy
▪ Moderate to severe anemia ▪ Tachycardia
▪ Clinical manifestations present ▪ Shortness of breath
around 6 months of age ▪ Decreased hemoglobin
o Thalassemia minor • <5-6 g / 100 mL in
▪ Mild to moderate anemia children
▪ May be asymptomatic o Lack of WBCs
▪ Commonly goes undetected ▪ Recurrent infection
- Clinical manifestations o Lack of platelets
o Early signs ▪ Abnormal bleeding
▪ Insidious onset ▪ Bruising
▪ Anemia - Prognosis
▪ Unexplained fever o Depends on the extent & duration of
▪ Poor feeding the decreased blood cell production
▪ Poor weight gain o Also depends on the client
▪ Enlarged spleen - Diagnostic evaluation
o Later signs o Routine CBC
▪ Chronic hypoxia o Peripheral blood smear
▪ Damage to liver, spleen, ▪ Reveals pancytopenia
heart, pancreas, & lymph o Bone marrow aspiration & biopsy
glands from - Nursing Management
hemochromatosis o Prevent infection
▪ Slight jaundice or bronze skin o Assess for abnormal bleeding
color o Administer prescribed medication &
▪ Thick cranial bones w/ blood products
prominent cheeks & flat nose ▪ Antilymphocyte globulin
▪ Growth retardation (ALG) or Anti-thymocyte
▪ Delayed sexual development globulin (ATG)
- Treatment • Suppresses T cell-
o Bone marrow transplant dependent
o High-iron diet autoimmune
- Nursing management responses w/o
o Prevent infection causing bone marrow
o Avoid activities that may increase the suppression
risk for fractures & injury ▪ Cyclosporine
o Promote rest • Given if ALT or ATG
o Adhere to prescribed diet therapy is ineffective
o Blood transfusion
o Diet as tolerated
Aplastic Anemia ▪ Avoid forcing food if N/V is
- Caused by damage to the bone marrow present
- Bone marrow may be damaged due to: ▪ Liquid or soft diet may be
o Infections (HPV, hepatitis) ordered if N/V is present
o Radiation o Meticulous oral care
o Medications
▪ Immunosuppression
medications used to eliminate Defects on Hemostasis
cancer cells Hemophilia
- Characterized by pancytopenia
o Anemia
o Granulocytopenia
- X-linked recessive congenital bleeding ▪ Spontaneous prolonged
disorders characterized by a deficiency in bleeding
specific coagulation protein • Gums
- Found dominantly in males • Circumcision
- Common types: • Umbilical cord
o Hemophilia A - Clinical manifestations
▪ Classic hemophilia o Epistaxis
▪ Caused by a deficiency of o Hematoma
clotting factor VIII, which is o Bleeding
necessary for the formation of o
thromboplastin - Nursing Management
▪ Caused by deficiency of o Assess for acute or chronic bleeding
antihemophilic globulin C, ▪ Assess skin, joint, muscles,
which is necessary for blood gums, rectum, mouth
clotting o Administer the missing clothing factor
o Hemophilia B o Administer Desmopressin to children
▪ Christmas disease w/ mild hemophilia A
▪ Less common type o Prevent or minimize bleeding
▪ Factor IX deficiency o Provide support
o Hemophilia C o Provide child & family teaching
▪ Deficiency of factor XI
o von Willebrand Disease
▪ Deficiency in von Willebrand Neoplastic Disorders
factor, a protein necessary for Leukemia
platelet adhesion - Most common cancer in children
- Common in Africans - Uncontrolled production of deformed or
o May be a genetic adaptation for immature WBCs
protection against malaria - Rapid increase in lymphocytes causes
- Etiology crowding
o Results in decrease of RBC & platelet
production
- Fatigue, susceptibility to infection, &
increased bleeding results from the decreased
normal WBCs, RBCs, & platelets
- Peak onset of 3-5 y/o
- Types
o Acute lymphoid leukemia (ALL)
▪ Most common type in children
• Greatest in 2-6 y/o
▪ More common in males
▪ Involves WBCs from lymphoid
▪ Most curable type
o Acute myelogenous leukemia (AML)
▪ Most common form of
leukemia
▪ More common in adults
- Assessment findings ▪ Curable rate is only 40%
o Mild ▪ Involves WBCs from myeloid
▪ Hemophilia (factor level of 5- • Granulocytes
50%) • Monocytes
▪ Prolonged bleeding only if ▪ Curable rate is only 40%
injury is present - Clinical manifestation
o Moderate o Weight loss
▪ Hemophilia (1-5%) o Anorexia
▪ Prolonged bleeding during o Vomiting
trauma or surgery o Abdominal pain
▪ Episodes of spontaneous o Bone pain
bleeding o Petechiae
o Severe o Purpura
▪ Factor level of <1% o Hematuria
o Epistaxis
o Tarry stools o Nerve irritation in the extremities
o Easy bruising o Non-productive cough
- Diagnostic evaluation ▪ Occurs in 50% of patients
o CBC o Pruritus
o Bone marrow aspiration ▪ Systemic manifestation
o Lumbar puncture o Engorgement of neck veins
▪ Insertion of a needle in the o Edema of face, neck, & right arm
lower spine o Urinary retention
▪ Headache & back pain may o Constipation
occur after the procedure o Compression of the cord
- Nursing Management - Stages
o Prevent infection o Stage I
▪ Pseudomonas is the most ▪ Involves single lymph node
common infectious agent region or lymphoid structure
o Prevent bleeding & injury • Spleen
▪ Use toothbrushes w/ soft • Thymus
bristles • Waldeyer’s ring
o Promote energy conservation o Tonsils
▪ Uninterrupted sleep & rest o Adenoids
o Relieve anxiety o Other
o Promote normal growth & lymphoid
development tissues in
o Promote positive body image URT
o Promote family coping o Stage II
o Prednisone therapy may be prescribed ▪ Involves 2 or more lymph
▪ May cause a moon-shaped node regions on the same
appearance side of the diaphragm
▪ Assure px that side effects ▪ E.g. mediastinum is a single
only temporary site, hilar lymph nodes are
lateralized
o Stage III
Lymphoma ▪ Involves lymph node
- Tumors in the lymphoid system regions/structures on both
o Thymus sides of the diaphragm
o Bone marrow ▪ III1
o Lymph nodes • w/ or w/o involvement
o Spleen of splenic, hilar,
o Tonsils celiac, or portal nodes
o Intestinal lymphoid tissues ▪ III2
- Occur more frequently in males • w/ involvement of
1. Hodgkin’s Disease para-aortic, iliac, or
- Known as cancer of the lymph or lymphoma mesenteric nodes
- Incidence o Stage IV
o Most common in adults ▪ Involvement of extranodial
o Most common in 15-19 y/o sites
- Believed to be caused by Epstein-Barr virus - Treatment
(EBV) o Surgical removal of the tumor
o Associated w/ immunosuppression & ▪ Usually indicated for stage 1
organ transplantation o Chemotherapy
- Mechanism of growth & spread is unknown o Radiotherapy
- Risk factors ▪ May be combined w/
o Family history (1st degree) chemotherapy
- Pathophysiology 2. Non-Hodgkin’s Lymphoma
o Cancerous transformation occurs from - Group of malignancies w/ a common origin in
a particular site in the lymph node the lymphoid cells
o As growth continues, the entire node - 7x more common than HD
becomes replaced w/ zones of - Incidence
necrosis obscuring the normal nodular o Most common in childhood (< 15y/o)
pattern - Risk factors
- Clinical manifestation o No dietary, hereditary, or ethnic risk
o Painless lymphadenopathy factors involved
▪ Clavicles, cervical
o Immunosuppression Review Questions
▪ Autoimmune disorders 1. Why should a client with SCA be concerned if
▪ Infectious, physical, & they marry a person w/ the sickle cell trait?
chemical agents 2. What defect is most commonly caused by
- Major histopathologic patterns anemia?
o Nodular a. Increased RBC count & blood
▪ Well-differentiated viscosity
lymphocytes b. Decreased hematopoietic system &
▪ Nodal & extra nodal sites hyperactivity
o Diffuse c. Increased presence of abnormal
▪ Cell aggregate is not evident, hemoglobin
unlike the nodular pattern d. Decreased capacity of blood to carry
- Pathophysiology O2
o Abnormal proliferation of neoplastic 3. Common symptoms of hemophilia in children
lymphocytes include _________, _________, __________,
o Cells remain fixed at 1 phase of _________.
development & continue to proliferate
o Both T & B lymphocytes mature in the
lymph nodes Answers
o Mechanical obstruction of enlarged 1. Since there is a possibility that their offspring
lymph nodes occur may be a carrier of the sickle cell trait.
- Clinical manifestations 2. D.
o Localized or generalized painless 3. Bleeding
lymphadenopathy Hemarthrosis
▪ Common sites: Joint swelling, pain, & limited ROM
• Cervical Altered neurologic status (caused by
• Axillary intracranial bleeding)
• Inguinal
• Femoral
- Nursing diagnoses
o Altered nutrition rlt anorexia in
chemotherapy
o Risk for ineffective management of
therapeutic regimen
- Treatment
o Combination chemotherapy for
shrinking the tumor & remission
o Cyclophosphamide
o Doxorubicin
- Complications
o Metastasis of the tumor to other parts
of the body
o Thrombocytopenia due to
chemotherapy
You might also like
- ATLSPracticeTest2 With AnswersDocument10 pagesATLSPracticeTest2 With Answersemad mohamed100% (1)
- Hematologic Disorders NotesDocument19 pagesHematologic Disorders Notesmikkagreen95% (22)
- 4b7c36 PDFDocument56 pages4b7c36 PDFsgoranksNo ratings yet
- Ghid Plante Medicinale Flora SpontanaDocument52 pagesGhid Plante Medicinale Flora Spontanaa100% (4)
- Sodium Lauryl Sulfate - WebDocument2 pagesSodium Lauryl Sulfate - WebMatea MareljaNo ratings yet
- What Is Desoxy DHEA and How Does It WorkDocument2 pagesWhat Is Desoxy DHEA and How Does It WorkdenovonutritionNo ratings yet
- Hematologic DisordersDocument8 pagesHematologic DisordersCorpus, Irene Zen P.No ratings yet
- Blood and LymphaticDocument4 pagesBlood and LymphaticCKNo ratings yet
- Hematologic DisorderDocument7 pagesHematologic Disordermawel100% (2)
- Anaphy Chapter 11 BloodDocument4 pagesAnaphy Chapter 11 BloodJohnNo ratings yet
- CARDIOVASCULARDocument20 pagesCARDIOVASCULARpriya garciaNo ratings yet
- (Hema) 1.1 Intro To Hema (Perez) - PANDADocument6 pages(Hema) 1.1 Intro To Hema (Perez) - PANDATony DawaNo ratings yet
- Child With Hematologic DisordersDocument5 pagesChild With Hematologic Disordersjadengg.pandak014No ratings yet
- Blood - Complete NotesDocument5 pagesBlood - Complete NotesLance CarandangNo ratings yet
- Blood SBDocument20 pagesBlood SBnoshNo ratings yet
- Circulatory System Reviewer - BAYLONDocument33 pagesCirculatory System Reviewer - BAYLONElijah Joaquin Payumo BaylonNo ratings yet
- BLOODDocument4 pagesBLOODcarolNo ratings yet
- Blood: HematopoiesisDocument6 pagesBlood: HematopoiesisMary Rose T. RecientesNo ratings yet
- HEMATOPOESISDocument71 pagesHEMATOPOESISHussenNo ratings yet
- Hematopoiesis ErythropoiesisDocument8 pagesHematopoiesis ErythropoiesisASHLEY ALEXIS GUEVARRANo ratings yet
- Types:: Precursor CellsDocument4 pagesTypes:: Precursor CellsGrace UrbanoNo ratings yet
- Cardiovascular System - BloodDocument8 pagesCardiovascular System - BloodVernice LopezNo ratings yet
- CBC Reviewer Anaphy LabDocument9 pagesCBC Reviewer Anaphy LabARVINE JUSTINE CORPUZNo ratings yet
- Hema Quiz 1Document8 pagesHema Quiz 1Shianne RacadioNo ratings yet
- CHAPTER 2 HematopoiesisDocument7 pagesCHAPTER 2 HematopoiesisAMELIA DALE MARQUEZNo ratings yet
- Module 2 PPT NOTES HematopoiesisDocument8 pagesModule 2 PPT NOTES HematopoiesisMohammad MasacalNo ratings yet
- Blood 2Document4 pagesBlood 2Jhes D.No ratings yet
- Blood Chapter 11Document4 pagesBlood Chapter 11James CastroNo ratings yet
- Hemolytic Anemia IntrinsicDocument14 pagesHemolytic Anemia IntrinsicSophia Gail ChingNo ratings yet
- Group1 Hematology Prelim Learning SummaryDocument22 pagesGroup1 Hematology Prelim Learning Summarylai cruzNo ratings yet
- vt59.2708-21242375124 394146998891967 4683953301704066077 n.pdfHEMA-HANDOUTS-1.pdf NC Cat 106&ccb 1-7&Document15 pagesvt59.2708-21242375124 394146998891967 4683953301704066077 n.pdfHEMA-HANDOUTS-1.pdf NC Cat 106&ccb 1-7&jasminemuammilNo ratings yet
- Chapter 11 - BloodDocument33 pagesChapter 11 - BloodCORONEL, SOPHIANo ratings yet
- Blood (Anaphy)Document8 pagesBlood (Anaphy)CORONEL, SOPHIANo ratings yet
- Hema 1A Lec 1 Shift Reviewer Hematopoiesis Prepared By: C Hematopoiesis DefinedDocument7 pagesHema 1A Lec 1 Shift Reviewer Hematopoiesis Prepared By: C Hematopoiesis DefinedMarc ViduyaNo ratings yet
- Body Fluids and Circulation: BloodDocument2 pagesBody Fluids and Circulation: Bloodswayam bhosaleNo ratings yet
- Blood PPT NotesDocument7 pagesBlood PPT NotesArce JohnsonNo ratings yet
- Bloodandcoagulation 171230045036Document85 pagesBloodandcoagulation 171230045036Parmarkeval PravnibhaiNo ratings yet
- BloodDocument5 pagesBloodChelsie NicoleNo ratings yet
- Blood and Lymph (Autosaved)Document46 pagesBlood and Lymph (Autosaved)Shaikh SaqibNo ratings yet
- Development of Blood Cells 2019Document31 pagesDevelopment of Blood Cells 2019Muhammad Anas Abbal100% (1)
- RBC MorphologyDocument9 pagesRBC MorphologybiancsNo ratings yet
- Red Cell Physiology HemaDocument12 pagesRed Cell Physiology HemaIya BangalanNo ratings yet
- Blood Cells: By, Shobhana PandianDocument60 pagesBlood Cells: By, Shobhana PandianhrishikeshanandNo ratings yet
- 2014 Curs Hematologie - FinalDocument333 pages2014 Curs Hematologie - FinalRamona Andreea ConstantinNo ratings yet
- The Blood System: Arteries VeinsDocument17 pagesThe Blood System: Arteries VeinsØmNo ratings yet
- Module 2: Hematopoiesis I. General Principles of HematopoiesisDocument13 pagesModule 2: Hematopoiesis I. General Principles of HematopoiesisJane JapoleNo ratings yet
- Hematology Module 2 and 3Document11 pagesHematology Module 2 and 3SEAN MELNOR LOSBAÑESNo ratings yet
- Blood AnalysisDocument89 pagesBlood AnalysisRiddhi JaganiNo ratings yet
- Body Fluids and Circulation - NotesDocument12 pagesBody Fluids and Circulation - NotesSaloni GuptaNo ratings yet
- Lecture 14Document30 pagesLecture 14MOHAMMED ELNAGGARNo ratings yet
- Hematology 1 L1 Introduction To Hematology 1 LectureDocument2 pagesHematology 1 L1 Introduction To Hematology 1 LectureChelze Faith DizonNo ratings yet
- Human Histology Midterms: Blood and HemopoesisDocument3 pagesHuman Histology Midterms: Blood and Hemopoesisabi dimatulacNo ratings yet
- HO Notecards 1Document12 pagesHO Notecards 1MrSomnambululNo ratings yet
- Chapter 8 - Transport in MammalsDocument119 pagesChapter 8 - Transport in Mammalsapi-3728508100% (1)
- Blood Part 1Document35 pagesBlood Part 1Keziah TampusNo ratings yet
- ErythropoisisDocument47 pagesErythropoisisDisha SuvarnaNo ratings yet
- BloodDocument4 pagesBloodA R F I J U LNo ratings yet
- Introduction To HematologyDocument19 pagesIntroduction To HematologyDr Deepshikha ParakhNo ratings yet
- Lesson 3 Blood Updated 2020Document29 pagesLesson 3 Blood Updated 2020Waliid Khan 5SNo ratings yet
- Human Blood - English - 1561800335 - English - 1579005206Document9 pagesHuman Blood - English - 1561800335 - English - 1579005206Rahul Dev PNo ratings yet
- Assessment and Management of Patients With Hematologic DisordersDocument20 pagesAssessment and Management of Patients With Hematologic Disorderschristine mercado100% (1)
- Anatomy and Physiology With PhatophysiologyDocument6 pagesAnatomy and Physiology With PhatophysiologyJustine Mae OyongNo ratings yet
- 1.07 - The BloodDocument5 pages1.07 - The Blood13PLAN, SENTH RUEN, ANo ratings yet
- Blood: Blood Is Made Up ofDocument5 pagesBlood: Blood Is Made Up ofNatasha JeanNo ratings yet
- TRANSES ANAPHY Male Reproductive SystemDocument6 pagesTRANSES ANAPHY Male Reproductive SystemPia LouiseNo ratings yet
- Environmental Studies - Question Bank Multidisciplinary Nature of Environmental StudiesDocument6 pagesEnvironmental Studies - Question Bank Multidisciplinary Nature of Environmental StudiesAditya KapoorNo ratings yet
- Scientific Validation of Standardization of Narayana Chendrooram (Kannusamy Paramparai Vaithiyam) Through The Siddha and Modern TechniquesDocument12 pagesScientific Validation of Standardization of Narayana Chendrooram (Kannusamy Paramparai Vaithiyam) Through The Siddha and Modern TechniquesBala Kiran GaddamNo ratings yet
- B05 QuestionsDocument5 pagesB05 QuestionsMauriya SenthilnathanNo ratings yet
- 16 Psychological Tricks To Make People Like You Immediately - The IndependentDocument23 pages16 Psychological Tricks To Make People Like You Immediately - The IndependentMohammed SalihNo ratings yet
- Spotting: Class 12Document51 pagesSpotting: Class 12Ritik Kumar NayakNo ratings yet
- BP605T Unit 4-6Document482 pagesBP605T Unit 4-6Gyampoh SolomonNo ratings yet
- Bagaimana Petani Di Malaysia Mempunyai Pabrik PupukDocument14 pagesBagaimana Petani Di Malaysia Mempunyai Pabrik PupukShamNo ratings yet
- Oral MucosaDocument40 pagesOral MucosaLobna ElkilanyNo ratings yet
- Flik Silverpen's Guide ToDocument9 pagesFlik Silverpen's Guide ToSonny3091100% (1)
- Ecology NotesDocument13 pagesEcology NotesAndy TonNo ratings yet
- 96-117+Grima+2023+Article +paper-2Document22 pages96-117+Grima+2023+Article +paper-2Girma TimerNo ratings yet
- Myeloid Series Demonstration SlidesDocument30 pagesMyeloid Series Demonstration SlidesOsannah Irish InsongNo ratings yet
- Kebt108 PDFDocument16 pagesKebt108 PDFAdrija DasNo ratings yet
- All India Institute of Medical Sciences Nagpur Department of Obstetrics and GynecologyDocument19 pagesAll India Institute of Medical Sciences Nagpur Department of Obstetrics and GynecologySugan GavaskarNo ratings yet
- Master Your Research Skills A Practical IEP Approach GuideDocument45 pagesMaster Your Research Skills A Practical IEP Approach GuideSandeep SpNo ratings yet
- Paper of Lower Plant TaxonomyDocument35 pagesPaper of Lower Plant TaxonomyMuthiaranifsNo ratings yet
- Mituru Lova Vol V Issue 01Document20 pagesMituru Lova Vol V Issue 01Ravi PalihawadanaNo ratings yet
- 8 Muscular System Med TerminologyDocument30 pages8 Muscular System Med TerminologyKavita MahaseNo ratings yet
- The Champion Text Book On Embalming 1908Document712 pagesThe Champion Text Book On Embalming 1908Ocean100% (3)
- Transport of Lipids in The Body FluidsDocument1 pageTransport of Lipids in The Body FluidsZeedan MohammedNo ratings yet
- Edexcel Intl A Levels Biology Unit 3 Wbi13 v1Document6 pagesEdexcel Intl A Levels Biology Unit 3 Wbi13 v1seif nimer100% (1)
- Defler Et Al., 2001 PDFDocument60 pagesDefler Et Al., 2001 PDFANDRES HUMBERTO CARDONA CARDONANo ratings yet
- 2.2.56. Amino Acid Analysis PDFDocument7 pages2.2.56. Amino Acid Analysis PDFliska ramdanawatiNo ratings yet
- DAFTAR PUSTAKA - Docx2Document2 pagesDAFTAR PUSTAKA - Docx2AQ GhesTyNo ratings yet