Professional Documents
Culture Documents
GIT Lec 4
GIT Lec 4
Uploaded by
Kim Sa-bu0 ratings0% found this document useful (0 votes)
6 views36 pagesPepsin is secreted as pepsinogen and activated by hydrochloric acid in the stomach. Pepsin can further activate pepsinogen in an autocatalytic process. Optimal pH for pepsin activity is 2, while it is blocked at pH 5. Gastric secretion is regulated by both nervous and hormonal mechanisms, including gastrin which stimulates parietal cells to secrete acid. The presence of food and distention of the stomach stimulate gastrin release. Acid and other factors in the intestine provide feedback inhibition of gastric secretion. Total gastrectomy can lead to deficiencies in vitamin B12, iron, and issues with dumping syndrome.
Original Description:
Original Title
GIT lec 4
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentPepsin is secreted as pepsinogen and activated by hydrochloric acid in the stomach. Pepsin can further activate pepsinogen in an autocatalytic process. Optimal pH for pepsin activity is 2, while it is blocked at pH 5. Gastric secretion is regulated by both nervous and hormonal mechanisms, including gastrin which stimulates parietal cells to secrete acid. The presence of food and distention of the stomach stimulate gastrin release. Acid and other factors in the intestine provide feedback inhibition of gastric secretion. Total gastrectomy can lead to deficiencies in vitamin B12, iron, and issues with dumping syndrome.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
6 views36 pagesGIT Lec 4
GIT Lec 4
Uploaded by
Kim Sa-buPepsin is secreted as pepsinogen and activated by hydrochloric acid in the stomach. Pepsin can further activate pepsinogen in an autocatalytic process. Optimal pH for pepsin activity is 2, while it is blocked at pH 5. Gastric secretion is regulated by both nervous and hormonal mechanisms, including gastrin which stimulates parietal cells to secrete acid. The presence of food and distention of the stomach stimulate gastrin release. Acid and other factors in the intestine provide feedback inhibition of gastric secretion. Total gastrectomy can lead to deficiencies in vitamin B12, iron, and issues with dumping syndrome.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 36
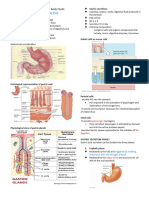
PEPSIN:
▣ secreted as pepsinogen and activated
by HCL.
▣ pepsin itself can activate pepsinogen
into pepsin → autocatalytic positive
feedback process.
▣ Optimum PH for pepsin is 2, At PH 5
it will be blocked.
▣ Group I pepsinogen: only present in acid
secreting region i.e. secreted by peptic and
mucus neck cells of the oxyntic gland.
▣ Group II pepsinogen: from pyloric,
Brunner’s and oxyntic gland.
▣ Maximal acid secretion correlates with
pepsinogen I level. Patients with
congenitally elevated circulating pepsinogen
I levels have a 5 folds greater incidence of
peptic ulcer than normal levels.
▣ Gastric lipase: weak lipolytic enzyme
acts mainly on butter fat.
▣ Gelatinase: liquefies the protein gelatin.
▣ Intrinsic factor: secreted by the parietal
cells, it’s a glycoprotein that combines
firmly with vitamin B12→protect vitamin
B12 from digestion and also this complex
will become bound to specific receptors
in the ileum and from there vitamin B12
is absorbed by endocytosis.
REGULATION OF GASTRIC SECRETION
▣ The regulation of the gastric secretion is by both
nervous and hormonal mechanisms.
▣ it is different from that of salivary secretion
which is controlled by nervous mechanism only.
▣ Gastric secretion associated with a meal can be
divided into 3 phases:-
1. Cephalic phase.
2. Gastric phase.
3. Intestinal phase.
1) Cephalic phase: also called nervous or
appetite phase. Gastric secretion can occur
even before the food reaches the stomach
and it is controlled by the vagus nerve. It
can be divided into to 2 types:
A-unconditioned reflex: the secretion
results from the taste of the food. The
presence of food in the mouth will
stimulate gastric secretion after five
minutes and the secretion may persist for
half to two hours.
B-conditioned reflex: the cephalic phase of
gastric secretion can be brought about not
only by the taste of the food but also by the
sight, smell or thought of food that’s to say
by conditioned reflex.
▣ The neural pathway for the cephalic phase
is the vagus
Gastric secretion in response to this vagal
stimulation is highly acidic and high in
pepsin. Cephalic phase accounts for 1/3 to ½
of total gastric acid secretion associated with
a meal.
▣ Emotional states: anger and hostility is
associated with hyper secretion of the
gastric mucosa. This is mediated
principally by the vagi.
▣ Fear and depression decrease gastric
secretion.
2) Gastric phase: presence of food in the
stomach stimulates gastric secretion by both
A-Nervous. B-Hormonal.
A-Nervous:
1-Local reflexes in the intrinsic nerve plexus of
the stomach (chemoreceptor and stretch).
2-Vago vagal reflexes that passes from the
stomach to the brainstem and back to the
stomach.
B-Hormonal: →Gastrin
▪ Gastrin is produced by G-cells in the antrum.
A second type of gastrin producing cells the
TG-cells found throughout the stomach and
small intestine.
▪ The G-cells are flask shaped and have a
small apex which contains micro villi which
is in contact with the lumen. This apical
portion may serve some type of receptor
function.
The presence of food in the stomach causes the
release of gastrin by:
1-distention→the bulk of food distends the
pyloric antrum and this causes the release of
gastrin
2-certain substances such as peptides and
amino acids (meat extract-partially digested
proteins)
3- gastrin is also released in response to vagal
stimulation which release gastrin-releasing
peptide (GRP) or Bombesin to produce gastrin.
Vagal nerve stimulation will inhibit
somatostatin which inhibits the G-cells. Thus
the nervous and hormonal stimulation of
gastric secretion interact and are not merely
additive but are markedly synergistic.
▣ Gastrin stimulates gastric juice highly acidic
but it does not contain high peptic activity.
The gastric phase of secretion accounts for ½
-2/3 of total gastric acid secretion associated
with a meal.
ROLE OF HISTAMINE IN ACID SECRETION
▣ Histamine is a powerful stimulant of acid
secretion. There are 3 receptors for histamine
▣ H1 – H2 – H3
▣ H2-receptors mediate the stimulatory effect
of histamine on acid secretion. So H2-
receptors antagonist such as cimitidine –
ranitidine – famotidine – e.t.c. are very
useful drugs in the treatment of peptic ulcer.
▣ It is believed that there are separate
receptors for acetylcholine-gastrin and
histamine but they interact synergistically i.e.
histamine facilitate the action of gastrin and
acetylcholine.
▣ It is believed that the stimulatory effect of
gastrin on acid secretion is mediated by the
release of histamine which in turn
stimulates the oxyntic cells to produce acid
secretion.
▣ ECL (Enterochromaffin like cells or
chromaffin)
▣ Present in acid-secreting part of the
stomach. Gastrin acts mainly by
stimulating these cells to release histamine
which acts quickly to stimulate gastric acid
secretion.
FEEDBACK INHIBITION OF GASTRIC ACID
SECRETION BY ANTRAL FACTORS:
▣ If the PH in the antrum falls to 1.5 or 2
(highly acidic) then there will be
inhibition of the gastrin mechanism and
thus there will be inhibition of acid
secretion induced by gastrin.
▣ This will protect the stomach against very
high acid secretion. When the PH rises
gastrin will be secreted again. Acid in the
antrum inhibit gastric secretion partly by
direct inhibition of the G-cells and partly
by somatostatin which inhibits the G-cells
3) Intestinal phase:
▣ The presence of certain substances in the
upper small intestine will stimulate the
secretion of gastric acid. Certain food in the
small intestine will cause small release of
enteric or intestinal gastrin from duodenal
mucosa which will cause small increase in
acid secretion. The intestinal phase accounts
for the least of the total acid gastric secretion.
Inhibition of gastric secretion by intestinal
factors:
▣ gastric secretion can be inhibited also by
certain substances in the upper small
intestine for e.g. 1-Acid. 2-Fat. 3-Hyper/
Hypo-osmotic fluids. 4-Any irritating
substance in the upper small intestine.
The inhibition of gastric secretion can be
brought about in 2 ways:
1. Enterogastric reflex: reflex nervous
signals are transmitted from the duodenum
back to the stomach to cause inhibition of
gastric secretion and gastric emptying.
▣ This reflex is stimulated by many factors
for e.g. acid in the duodenum will
stimulate this reflex. If the PH in the
duodenum falls to 3.5 or 4 this will
stimulate this reflex to inhibit gastric
secretion and thus protects the duodenal
mucosa from high acidity.
2. Inhibitory hormones:
the presence of acids, fat, hypo/hyper
osmotic fluids, e.t.c. causes the release of
several intestinal hormones that are:
-Secretin.
-Gastric inhibitory peptide (GIP).
-Vasoactive intestinal polypeptide (VIP).
-Somatostatin.
-Peptide YY.
Enterogastrone:
▣ refers to the inhibitory hormones that
inhibit gastric acid secretion. Peptide YY
is a good candidate to be Enterogastrone.
Fat causes its release from the jejunum
and it is an effective inhibitor of gastrin-
stimulated acid secretion.
▣ Gastric secretion is increased following the
removal of a large part of the small intestine,
due to the removal of the source of these
inhibitory hormones. The purpose of
inhibition of gastric secretion and emptying
is to slow the release of chyme from the
stomach to the small intestine when the
small intestine is already filled. So high
acidity reduces gastric secretion and motility
and high fat reduce gastric secretion and
emptying and so on.
Secretion of stomach during the interdigestive
period
▣ The stomach secrets only a few milliliters of
gastric juice per hour during the interdigestive
phase when little or no digestion is occurring
anywhere in the gut. The secretion is usually of
the non-oxyntic type i.e. composed mainly of
mucus, little pepsin and almost no acid and
sometimes it is usually slightly alkaline with
sodium bicarbonate.
▣ During emotional stress there will be an
increase of the interdigestive secretion up
to 50 ml. or more per hour like that of the
cephalic phase. So emotional stimuli is
believed to be one of the factors for the
development of peptic ulcer.
Total Gastrectomy and its effect:
1. Intrinsic factor deficiency which leads to
megaloblastic anemia, so it is compensated
by parenteral injection of cyanocobalamine
(vit.B12).
2. Protein digestion still normal in the absence
of pepsin, because of the presence of other
pancreatic proteolytic enzymes.
3. Iron deficiency anemia will occur. Gastric
secretions dissolve the iron and permit it to form
soluble complexes with ascorbic acid (vit. C)
and other substances that aid its reduction to the
fe⁺⁺ ferrous form.
❑ That’s why iron deficiency anemia is a
troublesome and frequent complication of
Gastrectomy
4. They must eat small, frequent meals
because of the dumping syndrome.
❑ Dumping syndrome occurs due to:
A-Rapid absorption of glucose from the
intestine and the resulted hyperglycemia and
abrupt rise in insulin secretion will cause in
turn hypoglycemic symptoms about 2 hours
after a meal.
B-Rapid entry of hyper osmotic meals to the
intestine, this provokes the movement of so
much water into the gut and this will cause
hypovolemia and hypotension
▣
You might also like
- Ielts (Sample Answers Writing)Document101 pagesIelts (Sample Answers Writing)Dang Thuy Lieu100% (6)
- Lecture-5 Hormonal Regulation of Intestinal MotilityDocument4 pagesLecture-5 Hormonal Regulation of Intestinal Motilityمرتضى حسين عبدNo ratings yet
- Unit 7 Physiology Lec.3Document4 pagesUnit 7 Physiology Lec.3Akeil AkeilNo ratings yet
- Control of DigestionDocument5 pagesControl of DigestionMichael NyaongoNo ratings yet
- Physio 6. Digestive System 6Document21 pagesPhysio 6. Digestive System 6Xena XenaNo ratings yet
- Clinical BiochemistryDocument56 pagesClinical Biochemistrysoumya palavalasa100% (1)
- PSG 252 Lecture 3 The StomachDocument5 pagesPSG 252 Lecture 3 The StomachMichael TobilobaNo ratings yet
- Cpy 521 - 122630Document41 pagesCpy 521 - 122630onyibor joshuaNo ratings yet
- Git Lecture 3Document30 pagesGit Lecture 3sandhiya.peetamberNo ratings yet
- Physiology, Lecture 8, GIT 2 (Stomach) (Slides)Document24 pagesPhysiology, Lecture 8, GIT 2 (Stomach) (Slides)Ali Al-Qudsi100% (2)
- GIT Lect A2Document43 pagesGIT Lect A2Ayurveda PgNo ratings yet
- Gastric Secretions MineDocument27 pagesGastric Secretions MinesasamaterasuNo ratings yet
- GIT Lect A2Document45 pagesGIT Lect A2Aira Jill PadernillaNo ratings yet
- Git HormonesDocument36 pagesGit Hormoneserereegbeji2005No ratings yet
- Gastric SecretionDocument36 pagesGastric SecretionammuNo ratings yet
- StomachDocument14 pagesStomachMajd HusseinNo ratings yet
- Gastric SecretionDocument45 pagesGastric SecretionAzeeza Elya100% (1)
- Lecture 10: Gastric Secretion & Its Regulation: Functions of StomachDocument8 pagesLecture 10: Gastric Secretion & Its Regulation: Functions of StomachBoody KhalilNo ratings yet
- Digestive System - 2Document4 pagesDigestive System - 2Sherida GibbsNo ratings yet
- Gastric Juice RegulationDocument22 pagesGastric Juice Regulationjanuian75% (4)
- Digestive System 2 (2) (1) - 061351Document39 pagesDigestive System 2 (2) (1) - 061351virajmore6222No ratings yet
- MBBS Lecture 1 Gastrointestinal HormonesDocument5 pagesMBBS Lecture 1 Gastrointestinal Hormonessamueltoluwabori360No ratings yet
- Hormonal Control of GitDocument42 pagesHormonal Control of GitM. Shahin Uddin KazemNo ratings yet
- Dr. ChintanDocument60 pagesDr. ChintanWaqar AhmedNo ratings yet
- Gastric Juice (Autosaved)Document15 pagesGastric Juice (Autosaved)ZahidKhanNo ratings yet
- Physio 5 From A.S#Document8 pagesPhysio 5 From A.S#Ahmed AmarNo ratings yet
- Gastrointestinal HormonesDocument5 pagesGastrointestinal Hormonesanjali.jha1909No ratings yet
- Gastric SecretionDocument50 pagesGastric SecretionYanglem AmarjitNo ratings yet
- Physiology Lecture 2Document32 pagesPhysiology Lecture 2Gracen33No ratings yet
- DigestionDocument187 pagesDigestionJane Andrea Christiano Djianzonie100% (1)
- Gi Hormones: Dr. Sharon M. PDocument50 pagesGi Hormones: Dr. Sharon M. PAleenaNo ratings yet
- Salivary SecretionDocument10 pagesSalivary SecretionMahadi Hasan KhanNo ratings yet
- Drugs Acting On GITDocument131 pagesDrugs Acting On GITmaxwell amponsahNo ratings yet
- By: Abduljabbar Hamid Jabbar: University of Baghdad-College of Medicine M. B. Ch. BDocument14 pagesBy: Abduljabbar Hamid Jabbar: University of Baghdad-College of Medicine M. B. Ch. BXena XenaNo ratings yet
- Git HormonesDocument17 pagesGit HormonesAniket MittalNo ratings yet
- Phys OkDocument7 pagesPhys OkVivek ChaudharyNo ratings yet
- Digestive System 1Document45 pagesDigestive System 1dmutethia68No ratings yet
- Gastric EmptyingDocument30 pagesGastric EmptyingARBIN TABASSUM FNo ratings yet
- All About GIT PhysiologyDocument79 pagesAll About GIT PhysiologyHarshavardhan AmancherlaNo ratings yet
- Digestive Physiology: Movement of MaterialsDocument14 pagesDigestive Physiology: Movement of MaterialsJãçk SparrowNo ratings yet
- DS Phy 7Document15 pagesDS Phy 7Arif NabeelNo ratings yet
- MBBS Lecture 2 Saliva and Gastric SecretionDocument7 pagesMBBS Lecture 2 Saliva and Gastric Secretionsamueltoluwabori360No ratings yet
- Gastric Secretion-FinalDocument107 pagesGastric Secretion-FinalDr.Gomathi sivakumarNo ratings yet
- Physio 5. Digestive System 5Document17 pagesPhysio 5. Digestive System 5Xena XenaNo ratings yet
- Р.8.OPERATION ON THE STOMATH AND DUODENUMDocument47 pagesР.8.OPERATION ON THE STOMATH AND DUODENUMMahmood SalahNo ratings yet
- Ondansetron: Gastric EmptyingDocument4,170 pagesOndansetron: Gastric EmptyingdrsaidumerNo ratings yet
- 1.physiologe Emrcs2016Document117 pages1.physiologe Emrcs2016Farah FarahNo ratings yet
- Pendahuluan Gi SystemDocument21 pagesPendahuluan Gi SystemdeasyahNo ratings yet
- Digestive System and Bioenergetics NotesDocument9 pagesDigestive System and Bioenergetics NotesDestinee LegendsNo ratings yet
- Gastric Juice AnalysisDocument6 pagesGastric Juice Analysismaynard pascualNo ratings yet
- GIDocument7 pagesGIiheart musicNo ratings yet
- 15 Digestive System: Give The Function and Mechanism of Secretion of Salivary Juice?Document24 pages15 Digestive System: Give The Function and Mechanism of Secretion of Salivary Juice?Bhavin ChangelaNo ratings yet
- Git Physiology AnswersDocument53 pagesGit Physiology AnswersSharif ImamNo ratings yet
- Physio. D. NOOR. L4.GITDocument8 pagesPhysio. D. NOOR. L4.GITزين العابدين محمد عويشNo ratings yet
- Regulation of GIT ProcessesDocument16 pagesRegulation of GIT ProcessesMuneeb Ur RehmanNo ratings yet
- Physiology: Stomach by DR Anam IsrarDocument20 pagesPhysiology: Stomach by DR Anam IsrarSaher Yasin100% (1)
- Digestion Physiology A&p IIDocument99 pagesDigestion Physiology A&p IIMonasterio Tan KennethNo ratings yet
- Arrangement by The Nervous System and HormonesDocument5 pagesArrangement by The Nervous System and Hormonesagustin savitryNo ratings yet
- Gastrin From Wikipedia, The Free EncyclopediaDocument23 pagesGastrin From Wikipedia, The Free EncyclopediaVincent Lau Bi ShengNo ratings yet
- Problem 2 - GI TractDocument30 pagesProblem 2 - GI Tractfahmi rosyadiNo ratings yet
- Quick Specs: HP EliteDisplay E222 21.5-Inch MonitorDocument11 pagesQuick Specs: HP EliteDisplay E222 21.5-Inch MonitorRudolph RednoseNo ratings yet
- DMSCO Log Book Vol.8 6/1930-5/1931Document49 pagesDMSCO Log Book Vol.8 6/1930-5/1931Des Moines University Archives and Rare Book RoomNo ratings yet
- Personal Protective EquipmentDocument10 pagesPersonal Protective EquipmentTomislav Panov100% (1)
- Cifra Club - Debbie Gibson - Lost in Your EyesDocument3 pagesCifra Club - Debbie Gibson - Lost in Your Eyesnivaldo de oliveira OliveiraNo ratings yet
- Cradles of Early Science Development of Science in Asia IndiaDocument4 pagesCradles of Early Science Development of Science in Asia IndiaAvox EverdeenNo ratings yet
- ALS 204 LH (Top Labelling)Document2 pagesALS 204 LH (Top Labelling)Yashvanth ShettyNo ratings yet
- CG-Full-Note For PU PDFDocument77 pagesCG-Full-Note For PU PDFirusha0% (1)
- Landfill Project Bratislava SlovakiaDocument286 pagesLandfill Project Bratislava SlovakiaaaNo ratings yet
- The New India Assurance Co. LTDDocument3 pagesThe New India Assurance Co. LTDsarath potnuriNo ratings yet
- Catalogue Chiller Carrier 19XRD - 2012Document24 pagesCatalogue Chiller Carrier 19XRD - 2012jimmiilongNo ratings yet
- Jon Krohn Metis Deep Learning 2017-05-01Document107 pagesJon Krohn Metis Deep Learning 2017-05-01Arnaldo Preso De LigaNo ratings yet
- Grand Prairie, TX City Council Meeting Agenda 05-20-2014 (Includes April 15, 2014 Minutes)Document379 pagesGrand Prairie, TX City Council Meeting Agenda 05-20-2014 (Includes April 15, 2014 Minutes)Westchester GasetteNo ratings yet
- Spirited Away - Film of The Fantastic and Evolving Japanese Folk SymbolsDocument25 pagesSpirited Away - Film of The Fantastic and Evolving Japanese Folk Symbolscv JunksNo ratings yet
- What Is Galactic Evolution?: Milky WayDocument12 pagesWhat Is Galactic Evolution?: Milky WayPROF RAJESH DUBEYNo ratings yet
- Analysis of Diaphragm WallDocument6 pagesAnalysis of Diaphragm WallSanthosh BabuNo ratings yet
- # Sample Quotation Copy For Go Kart SparesDocument3 pages# Sample Quotation Copy For Go Kart SparessaqibNo ratings yet
- UF-3000 GI 2004 enDocument86 pagesUF-3000 GI 2004 enjw lNo ratings yet
- Tool Life When High Speed Ball Nose End Milling Inconel 718: Adrian Sharman, Richard C. Dewes, David K. AspinwallDocument7 pagesTool Life When High Speed Ball Nose End Milling Inconel 718: Adrian Sharman, Richard C. Dewes, David K. AspinwallKin HamzahNo ratings yet
- Loughborough Junction Minutes 16 February 2009Document5 pagesLoughborough Junction Minutes 16 February 2009Loughborough JunctionNo ratings yet
- Study of Reweighting Methods Using Single Histogram MethodDocument3 pagesStudy of Reweighting Methods Using Single Histogram Methodt_sairamNo ratings yet
- G5 Q2W7 DLL MathDocument8 pagesG5 Q2W7 DLL MathFloriza MangiselNo ratings yet
- AC 43.13-1B Section 5 Penetrant InspectionDocument8 pagesAC 43.13-1B Section 5 Penetrant Inspection320338100% (1)
- Armstrong AS Process Flow Diagram: ProductDocument26 pagesArmstrong AS Process Flow Diagram: ProductBALACHANDAR SNo ratings yet
- B.ing 2Document3 pagesB.ing 2Dwi purwitasariNo ratings yet
- Q-PCF-12-30-PN 6Document1 pageQ-PCF-12-30-PN 6Camilo Maya PodestaNo ratings yet
- Rocks and Minerals Webquest Justin PowersDocument2 pagesRocks and Minerals Webquest Justin Powersapi-264089789100% (1)
- Chapter 10: Frequency Response Techniques 1Document60 pagesChapter 10: Frequency Response Techniques 1CesarNo ratings yet
- Trade of Export - ImportDocument9 pagesTrade of Export - ImportrahulvaliyaNo ratings yet
- PIIS1098360021012478Document13 pagesPIIS1098360021012478Opale PapaleNo ratings yet