Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
13 viewsGIB Report
GIB Report
Uploaded by
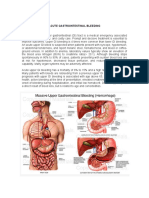
Rani Gayle RiveraUpper gastrointestinal bleeding can originate from the esophagus, stomach, or duodenum. The most common causes are peptic ulcers, accounting for around 50% of cases, and variceal hemorrhaging. Peptic ulcers are defined as disruptions in the stomach or duodenal mucosa due to inflammation. Hemorrhoids and colonic diverticula are the most frequent sources of lower gastrointestinal bleeding. Diverticula bleeding typically occurs abruptly from the right colon in older patients, while hemorrhoids usually cause painless bright red bleeding.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You might also like
- Quick Review/Pearl Sheet: These Are in Random Order To Help You Prepare For You NBME ExamDocument19 pagesQuick Review/Pearl Sheet: These Are in Random Order To Help You Prepare For You NBME ExamWyoXPat100% (12)
- Management of Patient With Gastrointestinal BleedingDocument14 pagesManagement of Patient With Gastrointestinal BleedingPulkit MandalNo ratings yet
- Acute Gastrointestinal Bleeding Upper GI BleedingDocument18 pagesAcute Gastrointestinal Bleeding Upper GI BleedingAldwin AyuyangNo ratings yet
- Case Study Medical WardDocument4 pagesCase Study Medical WardFrancis Antonio Llenaresas QuijanoNo ratings yet
- Diverticular Disease of The ColonDocument38 pagesDiverticular Disease of The Colonapi-19641337No ratings yet
- Causes of Upper Gastrointestinal Bleeding in Adults UpToDateDocument37 pagesCauses of Upper Gastrointestinal Bleeding in Adults UpToDateJodene Rose RojasNo ratings yet
- HEMATOCHEZIADocument26 pagesHEMATOCHEZIAAlvin HartantoNo ratings yet
- Upper Gastrointestinal Bleeding: EL IlcoxDocument1 pageUpper Gastrointestinal Bleeding: EL IlcoxdaisyNo ratings yet
- Gastro Intestinal Bleeding DR - muayAD ABASSDocument59 pagesGastro Intestinal Bleeding DR - muayAD ABASSMAFADHELNo ratings yet
- DiverticulitisDocument15 pagesDiverticulitisElisabeth MelisaNo ratings yet
- CholangitisDocument15 pagesCholangitisFaye TanNo ratings yet
- Causes of Upper Gastrointestinal Bleeding in Adults - UpToDateDocument37 pagesCauses of Upper Gastrointestinal Bleeding in Adults - UpToDateAline MoraisNo ratings yet
- ICC2 (103) GIT BleedingDocument68 pagesICC2 (103) GIT Bleedingabdulrhman essamNo ratings yet
- Gastro Intestinal Disorders: Assessment, Conditions, & ManagementDocument84 pagesGastro Intestinal Disorders: Assessment, Conditions, & ManagementBryan GrafftNo ratings yet
- Upper Gi Bleed: History, Pe, Pathophysiology, Diagnostics and TreatmentDocument6 pagesUpper Gi Bleed: History, Pe, Pathophysiology, Diagnostics and TreatmentJennicaNo ratings yet
- Diverticular Disease: Diverticulitis, Bleeding, and FistulaDocument8 pagesDiverticular Disease: Diverticulitis, Bleeding, and FistulaakashkumarpanwarNo ratings yet
- Peptic Ulcer Disease: by Parthevan RajasingamDocument33 pagesPeptic Ulcer Disease: by Parthevan RajasingamNinaNo ratings yet
- Peptic UlcerDocument4 pagesPeptic UlcerEris Abdul AzizNo ratings yet
- Upper Gastrointestinal BleedingDocument46 pagesUpper Gastrointestinal BleedingRashed ShatnawiNo ratings yet
- Lower GI Bleeding SlideDocument29 pagesLower GI Bleeding Slideraed faisalNo ratings yet
- GIN L9 Shabot 0708Document53 pagesGIN L9 Shabot 0708api-3799874No ratings yet
- Angio Displa SiaDocument4 pagesAngio Displa SiaBelaFawziaNo ratings yet
- 2009 Pearl SheetDocument19 pages2009 Pearl Sheetmikez100% (1)
- Clinical-Manifestations-Diagnosis and Prognosis of Crohn DiseaseDocument46 pagesClinical-Manifestations-Diagnosis and Prognosis of Crohn DiseasejzainounNo ratings yet
- Causes of Upper Gastrointestinal Bleeding in Adults - UpToDate PDFDocument55 pagesCauses of Upper Gastrointestinal Bleeding in Adults - UpToDate PDFKristell LópezNo ratings yet
- Liver Abscess: Key PointsDocument5 pagesLiver Abscess: Key PointsVanadia Nurul MetaNo ratings yet
- Uppergastrointestinalbleeding: Marcie Feinman,, Elliott R. HautDocument11 pagesUppergastrointestinalbleeding: Marcie Feinman,, Elliott R. HautjoseNo ratings yet
- Boala Crohn Clinical ManifestationsDocument16 pagesBoala Crohn Clinical ManifestationsEdith CroitoruNo ratings yet
- Abdomen AgudoDocument38 pagesAbdomen AgudoJeslia TorresNo ratings yet
- Amoebic Liver Abscess: Clinical MedicineDocument5 pagesAmoebic Liver Abscess: Clinical MedicineAizat KamalNo ratings yet
- Gastrointestinal Tract Bleeding: DR Stefanus Nangoi, M.Biomed, SPBDocument29 pagesGastrointestinal Tract Bleeding: DR Stefanus Nangoi, M.Biomed, SPBNindyNo ratings yet
- Causes of Sis and Management of A CaseDocument26 pagesCauses of Sis and Management of A CaseEmmanuelLazarusNo ratings yet
- Upper Gastrointestinal Bleeding.Document13 pagesUpper Gastrointestinal Bleeding.Gieselle Scott100% (1)
- Diverticular DiseaseDocument2 pagesDiverticular DiseaseMemMed Administrator100% (2)
- Complications of CholelithiasisDocument25 pagesComplications of CholelithiasisGibson RamseyNo ratings yet
- Pathogenesis of Diseases of The Gallbladder and Biliary TractDocument28 pagesPathogenesis of Diseases of The Gallbladder and Biliary TractMuhammad MakkiNo ratings yet
- Portal HypertensionDocument13 pagesPortal HypertensionCiprian BoesanNo ratings yet
- Acute GI Bleeding: Louis Chaptini MDDocument67 pagesAcute GI Bleeding: Louis Chaptini MDSiti RahayuNo ratings yet
- Management of Upper Gi BleedingDocument41 pagesManagement of Upper Gi Bleedingkaukab azimNo ratings yet
- Chylous, Bloody, and Pancreatic Ascites - UpToDateDocument26 pagesChylous, Bloody, and Pancreatic Ascites - UpToDateAndrea RodríguezNo ratings yet
- Cholecystitis: David R. Elwood, MDDocument12 pagesCholecystitis: David R. Elwood, MDJefferson Candela RadaNo ratings yet
- AscitesascitesDocument15 pagesAscitesascitesKevinJuliusTanadyNo ratings yet
- Inflammatory Bowel DiseaseDocument19 pagesInflammatory Bowel Diseasenathan asfahaNo ratings yet
- 01 Gastritis & PUDxxDocument51 pages01 Gastritis & PUDxxTor Koang ThorNo ratings yet
- CholecystitisDocument12 pagesCholecystitisMariela HuertaNo ratings yet
- Perforated Peptic UlcerDocument68 pagesPerforated Peptic UlcerSaibo BoldsaikhanNo ratings yet
- Mallory Weiss Syndrome - StatPearls - NCBI BookshelfDocument9 pagesMallory Weiss Syndrome - StatPearls - NCBI BookshelfDaniela EstradaNo ratings yet
- Pyogenic Liver AbscessDocument10 pagesPyogenic Liver AbscessErnesto Sebastian GarcíaNo ratings yet
- ULGIBDocument31 pagesULGIBEzraNo ratings yet
- Background: Pediatric AppendicitisDocument15 pagesBackground: Pediatric AppendicitisnikkitaihsanNo ratings yet
- Liver Abscess Modul 2Document3 pagesLiver Abscess Modul 2ras emil sazuraNo ratings yet
- Journal AslinyaDocument11 pagesJournal AslinyainNo ratings yet
- Clinical Clerk Seminar Series: Approach To Gi BleedsDocument11 pagesClinical Clerk Seminar Series: Approach To Gi BleedsAngel_Liboon_388No ratings yet
- Stomach and DuodenumDocument84 pagesStomach and DuodenumDhanush PillaiNo ratings yet
- GIT DisordersDocument28 pagesGIT Disordersbpt2100% (1)
- Upper and Lower GI Bleeding Differential DiagnosesDocument3 pagesUpper and Lower GI Bleeding Differential DiagnosesKEn PilapilNo ratings yet
- Gallstone Disease: Types of Gall Stone and AetiologyDocument6 pagesGallstone Disease: Types of Gall Stone and AetiologyEileen MartinNo ratings yet
- Esophageal Varices, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandEsophageal Varices, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Portal Vein Thrombosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandPortal Vein Thrombosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Diverticulitis Cure: The Ultimate Diverticulitis Diet: Diverticulitis Recipes: Your Ultimate Diverticulitis CookbookFrom EverandDiverticulitis Cure: The Ultimate Diverticulitis Diet: Diverticulitis Recipes: Your Ultimate Diverticulitis CookbookNo ratings yet
GIB Report
GIB Report
Uploaded by
Rani Gayle Rivera0 ratings0% found this document useful (0 votes)
13 views2 pagesUpper gastrointestinal bleeding can originate from the esophagus, stomach, or duodenum. The most common causes are peptic ulcers, accounting for around 50% of cases, and variceal hemorrhaging. Peptic ulcers are defined as disruptions in the stomach or duodenal mucosa due to inflammation. Hemorrhoids and colonic diverticula are the most frequent sources of lower gastrointestinal bleeding. Diverticula bleeding typically occurs abruptly from the right colon in older patients, while hemorrhoids usually cause painless bright red bleeding.
Original Description:
GI bleeding
Original Title
GIB report
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentUpper gastrointestinal bleeding can originate from the esophagus, stomach, or duodenum. The most common causes are peptic ulcers, accounting for around 50% of cases, and variceal hemorrhaging. Peptic ulcers are defined as disruptions in the stomach or duodenal mucosa due to inflammation. Hemorrhoids and colonic diverticula are the most frequent sources of lower gastrointestinal bleeding. Diverticula bleeding typically occurs abruptly from the right colon in older patients, while hemorrhoids usually cause painless bright red bleeding.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
13 views2 pagesGIB Report
GIB Report
Uploaded by
Rani Gayle RiveraUpper gastrointestinal bleeding can originate from the esophagus, stomach, or duodenum. The most common causes are peptic ulcers, accounting for around 50% of cases, and variceal hemorrhaging. Peptic ulcers are defined as disruptions in the stomach or duodenal mucosa due to inflammation. Hemorrhoids and colonic diverticula are the most frequent sources of lower gastrointestinal bleeding. Diverticula bleeding typically occurs abruptly from the right colon in older patients, while hemorrhoids usually cause painless bright red bleeding.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 2
Good day Doctors, This is PGI Rivera and to hospitalizations.
The most important cause of
continue. Gastrointestinal bleeding may be gastric and duodenal erosions is NSAID use: where
categorized by the source or the site of the ~50% of patients who chronically ingest NSAIDs
bleeding. may have gastric erosions. Other potential causes
include alcohol intake, H. pylori infection, and
Generally, this may be classified into 3 namely stress related mucosal injury. // Less common
upper gastrointestinal sources, small intestinal causes of UGIB include neoplasms, vascular
sources, and colonic sources. ectasias (including hereditary hemorrhagic
telangiectasias or Osler Weber Rendu and gastric
Upper gastrointestinal causes include Peptic ulcers, antral vascular ectasia, Dieulafoy’s lesion in which
the most common cause of UGIB which account for an aberrant vessel in the mucosa bleeds from a
~50% of UGIB hospitalizations (this will be pinpoint mucosal defect, prolapse gastropathy
discussed further later), // Mallory Weiss Tears (prolapse of proximal stomach into esophagus with
accounting for ~2-10% of UGIB hospitalizations retching, especially in alcoholics, aortoenteric
presenting with classic history of vomiting, fistulas, and hemobilia or hemosuccus pancreatus
retching, or coughing preceding hematemesis or bleeding from the bile duct or pancreatic duct.
especially in an alcoholic patient. Bleeding from
these tears, which are usually on the gastric side of Focusing on the most common cause of UGIB,
the gastroesophageal junction, stops Peptic ulcers account for ~50% of UGIB
spontaneously in ~80-90% of patients and recurs hospitalizations. A peptic ulcer is defined as
only in 0-10%. // On the other hand, the proportion disruption of the mucosal integrity of the stomach
of UGIB hospitalizations due to varices varies and/or duodenum leading to a local defect or
widely from ~2-40%, depending on the population. excavation due to active inflammation. Although
Patients with variceal hemorrhage often have burning epigastric pain exacerbated by fasting and
poorer outcomes than patients with other sources improved with meals is a symptom complex
of UGIB. Approximately 5–15% of cirrhotics per associated with peptic ulcer disease, it is now clear
year develop varices, and it is estimated that the that >90% patients with this symptom complex
majority of patients with cirrhosis will develop (dyspepsia) do not have ulcers and that the
varices over their lifetimes. Furthermore, it is majority of patients with peptic ulcers may be
anticipated that roughly one-third of patients with asymptomatic. Ulcers occur within the stomach
varices will develop bleeding. Several factors and/or duodenum and are often chronic in nature.
predict the risk of bleeding, including the severity
of cirrhosis (Child-Pugh class, Model for End-Stage Patients without a source of GIB identified on
Liver Disease [MELD] score); the height of wedged- upper endoscopy and colonoscopy were previously
hepatic vein pressure; the size of the varix; the labeled as having obscure GIB but with the advent
location of the varix; and certain endoscopic of improved diagnostic modalities, ~75% of GIB
stigmata, including red wale signs, hematocystic previously labeled as obscure is now estimated to
spots, diffuse erythema, bluish color, cherry red originate in the small intestine beyond the extent
spots, or white-nipple spots. Patients with tense of a standard upper endoscopic exam. Small
ascites are also at increased risk for bleeding from intestinal GIB may account for ~5% of GIB cases.
varices. // Lastly, erosions are endoscopically The most common causes in adults include vascular
visualized breaks that are confined to the mucosa ectasias, neoplasm like gastrointestinal stromal
and do not cause major bleeding because arteries tumor, carcinoid, adenocarcinoma, lymphoma,
and veins are not present in the mucosa. Erosions metastases, and NSAID induced erosions and
in the esophagus, stomach, or duodenum ulcers. Other less common causes of small
commonly cause mild UGIB, with erosive gastritis intestinal GIB include Crohn’s disease, infection,
and duodenitis accounting for ~10-15% and erosive ischemia, vasculitis, small bowel varices,
esophagitis (primarily due to gastroesophageal diverticular, intussusception, Dieulafoy’s lesions,
reflux disease) accounting for ~1-10% of UGIB aortoenteric fistulas, and duplication cysts.
right colon; chronic or occult bleeding is not
Lastly, for the colonic causes. characteristic. Patients at increased risk for
bleeding tend to be hypertensive, have
Hemorrhoids are probably the most common cause atherosclerosis, and regularly use antithrombotic
of LGIB; anal fissures also cause minor bleeding and therapy and nonsteroidal anti-inflammatory
pain. If these local anal processes, which rarely agents. Additional risk factors include obesity and a
require hospitalization, are excluded, the most history of diabetes mellitus. Most bleeds are self-
common cause of LGIB in adults would be limited and stop spontaneously with bowel rest.
diverticulosis. Other causes include vascular The lifetime risk of rebleeding is 25%
ectasias (especially in the proximal colon of
patients >70 years), neoplasms (primarily
adenocarcinoma), colitis (ischemic, infectious,
Crohn’s or ulcerative colitis, NSAID induced colitis
or ulcers), postpolypectomy bleeding, and radiation
proctopathy. Rarer causes include solitary rectal
ulcer syndrome, varices (most commonly rectal),
lymphoid nodular hyperplasia, vasculitis, trauma,
and aortocolic fistulas.
Focusing on the most common ones we have
Hemorrhoids: Hemorrhoidal cushions are a normal
part of the anal canal. The vascular structures
contained within aid in continence by preventing
damage to the sphincter muscle. Engorgement and
straining lead to prolapse of this tissue into the
anal canal. Over time, the anatomic support system
of the hemorrhoidal complex weakens, exposing
this tissue to the outside of the anal canal where it
is susceptible to injury. Patients with hemorrhoidal
disease commonly present in the clinics for two
reasons: bleeding and protrusion. Pain is less
common than with fissures and if present, is
described as dull ache from engorgement of the
hemorrhoidal tissue. Severe pain may indicate a
thrombosed hemorrhoid. Hemorrhoidal bleeding is
described as painless bright red blood seen either
in the toilet or upon wiping. Occasional patients
can present with significant bleeding, which may be
a cause of anemia; however, the presence of a
colonic neoplasm must be ruled out in anemic
patients.
Hemorrhage from a colonic diverticulum is the
most common cause of hematochezia in patients
>60 years, yet only 20% of patients with
diverticulosis will have gastrointestinal bleeding.
Diverticular bleeding is abrupt in onset, usually
painless, sometimes massive, and often from the
You might also like
- Quick Review/Pearl Sheet: These Are in Random Order To Help You Prepare For You NBME ExamDocument19 pagesQuick Review/Pearl Sheet: These Are in Random Order To Help You Prepare For You NBME ExamWyoXPat100% (12)
- Management of Patient With Gastrointestinal BleedingDocument14 pagesManagement of Patient With Gastrointestinal BleedingPulkit MandalNo ratings yet
- Acute Gastrointestinal Bleeding Upper GI BleedingDocument18 pagesAcute Gastrointestinal Bleeding Upper GI BleedingAldwin AyuyangNo ratings yet
- Case Study Medical WardDocument4 pagesCase Study Medical WardFrancis Antonio Llenaresas QuijanoNo ratings yet
- Diverticular Disease of The ColonDocument38 pagesDiverticular Disease of The Colonapi-19641337No ratings yet
- Causes of Upper Gastrointestinal Bleeding in Adults UpToDateDocument37 pagesCauses of Upper Gastrointestinal Bleeding in Adults UpToDateJodene Rose RojasNo ratings yet
- HEMATOCHEZIADocument26 pagesHEMATOCHEZIAAlvin HartantoNo ratings yet
- Upper Gastrointestinal Bleeding: EL IlcoxDocument1 pageUpper Gastrointestinal Bleeding: EL IlcoxdaisyNo ratings yet
- Gastro Intestinal Bleeding DR - muayAD ABASSDocument59 pagesGastro Intestinal Bleeding DR - muayAD ABASSMAFADHELNo ratings yet
- DiverticulitisDocument15 pagesDiverticulitisElisabeth MelisaNo ratings yet
- CholangitisDocument15 pagesCholangitisFaye TanNo ratings yet
- Causes of Upper Gastrointestinal Bleeding in Adults - UpToDateDocument37 pagesCauses of Upper Gastrointestinal Bleeding in Adults - UpToDateAline MoraisNo ratings yet
- ICC2 (103) GIT BleedingDocument68 pagesICC2 (103) GIT Bleedingabdulrhman essamNo ratings yet
- Gastro Intestinal Disorders: Assessment, Conditions, & ManagementDocument84 pagesGastro Intestinal Disorders: Assessment, Conditions, & ManagementBryan GrafftNo ratings yet
- Upper Gi Bleed: History, Pe, Pathophysiology, Diagnostics and TreatmentDocument6 pagesUpper Gi Bleed: History, Pe, Pathophysiology, Diagnostics and TreatmentJennicaNo ratings yet
- Diverticular Disease: Diverticulitis, Bleeding, and FistulaDocument8 pagesDiverticular Disease: Diverticulitis, Bleeding, and FistulaakashkumarpanwarNo ratings yet
- Peptic Ulcer Disease: by Parthevan RajasingamDocument33 pagesPeptic Ulcer Disease: by Parthevan RajasingamNinaNo ratings yet
- Peptic UlcerDocument4 pagesPeptic UlcerEris Abdul AzizNo ratings yet
- Upper Gastrointestinal BleedingDocument46 pagesUpper Gastrointestinal BleedingRashed ShatnawiNo ratings yet
- Lower GI Bleeding SlideDocument29 pagesLower GI Bleeding Slideraed faisalNo ratings yet
- GIN L9 Shabot 0708Document53 pagesGIN L9 Shabot 0708api-3799874No ratings yet
- Angio Displa SiaDocument4 pagesAngio Displa SiaBelaFawziaNo ratings yet
- 2009 Pearl SheetDocument19 pages2009 Pearl Sheetmikez100% (1)
- Clinical-Manifestations-Diagnosis and Prognosis of Crohn DiseaseDocument46 pagesClinical-Manifestations-Diagnosis and Prognosis of Crohn DiseasejzainounNo ratings yet
- Causes of Upper Gastrointestinal Bleeding in Adults - UpToDate PDFDocument55 pagesCauses of Upper Gastrointestinal Bleeding in Adults - UpToDate PDFKristell LópezNo ratings yet
- Liver Abscess: Key PointsDocument5 pagesLiver Abscess: Key PointsVanadia Nurul MetaNo ratings yet
- Uppergastrointestinalbleeding: Marcie Feinman,, Elliott R. HautDocument11 pagesUppergastrointestinalbleeding: Marcie Feinman,, Elliott R. HautjoseNo ratings yet
- Boala Crohn Clinical ManifestationsDocument16 pagesBoala Crohn Clinical ManifestationsEdith CroitoruNo ratings yet
- Abdomen AgudoDocument38 pagesAbdomen AgudoJeslia TorresNo ratings yet
- Amoebic Liver Abscess: Clinical MedicineDocument5 pagesAmoebic Liver Abscess: Clinical MedicineAizat KamalNo ratings yet
- Gastrointestinal Tract Bleeding: DR Stefanus Nangoi, M.Biomed, SPBDocument29 pagesGastrointestinal Tract Bleeding: DR Stefanus Nangoi, M.Biomed, SPBNindyNo ratings yet
- Causes of Sis and Management of A CaseDocument26 pagesCauses of Sis and Management of A CaseEmmanuelLazarusNo ratings yet
- Upper Gastrointestinal Bleeding.Document13 pagesUpper Gastrointestinal Bleeding.Gieselle Scott100% (1)
- Diverticular DiseaseDocument2 pagesDiverticular DiseaseMemMed Administrator100% (2)
- Complications of CholelithiasisDocument25 pagesComplications of CholelithiasisGibson RamseyNo ratings yet
- Pathogenesis of Diseases of The Gallbladder and Biliary TractDocument28 pagesPathogenesis of Diseases of The Gallbladder and Biliary TractMuhammad MakkiNo ratings yet
- Portal HypertensionDocument13 pagesPortal HypertensionCiprian BoesanNo ratings yet
- Acute GI Bleeding: Louis Chaptini MDDocument67 pagesAcute GI Bleeding: Louis Chaptini MDSiti RahayuNo ratings yet
- Management of Upper Gi BleedingDocument41 pagesManagement of Upper Gi Bleedingkaukab azimNo ratings yet
- Chylous, Bloody, and Pancreatic Ascites - UpToDateDocument26 pagesChylous, Bloody, and Pancreatic Ascites - UpToDateAndrea RodríguezNo ratings yet
- Cholecystitis: David R. Elwood, MDDocument12 pagesCholecystitis: David R. Elwood, MDJefferson Candela RadaNo ratings yet
- AscitesascitesDocument15 pagesAscitesascitesKevinJuliusTanadyNo ratings yet
- Inflammatory Bowel DiseaseDocument19 pagesInflammatory Bowel Diseasenathan asfahaNo ratings yet
- 01 Gastritis & PUDxxDocument51 pages01 Gastritis & PUDxxTor Koang ThorNo ratings yet
- CholecystitisDocument12 pagesCholecystitisMariela HuertaNo ratings yet
- Perforated Peptic UlcerDocument68 pagesPerforated Peptic UlcerSaibo BoldsaikhanNo ratings yet
- Mallory Weiss Syndrome - StatPearls - NCBI BookshelfDocument9 pagesMallory Weiss Syndrome - StatPearls - NCBI BookshelfDaniela EstradaNo ratings yet
- Pyogenic Liver AbscessDocument10 pagesPyogenic Liver AbscessErnesto Sebastian GarcíaNo ratings yet
- ULGIBDocument31 pagesULGIBEzraNo ratings yet
- Background: Pediatric AppendicitisDocument15 pagesBackground: Pediatric AppendicitisnikkitaihsanNo ratings yet
- Liver Abscess Modul 2Document3 pagesLiver Abscess Modul 2ras emil sazuraNo ratings yet
- Journal AslinyaDocument11 pagesJournal AslinyainNo ratings yet
- Clinical Clerk Seminar Series: Approach To Gi BleedsDocument11 pagesClinical Clerk Seminar Series: Approach To Gi BleedsAngel_Liboon_388No ratings yet
- Stomach and DuodenumDocument84 pagesStomach and DuodenumDhanush PillaiNo ratings yet
- GIT DisordersDocument28 pagesGIT Disordersbpt2100% (1)
- Upper and Lower GI Bleeding Differential DiagnosesDocument3 pagesUpper and Lower GI Bleeding Differential DiagnosesKEn PilapilNo ratings yet
- Gallstone Disease: Types of Gall Stone and AetiologyDocument6 pagesGallstone Disease: Types of Gall Stone and AetiologyEileen MartinNo ratings yet
- Esophageal Varices, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandEsophageal Varices, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Portal Vein Thrombosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandPortal Vein Thrombosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Diverticulitis Cure: The Ultimate Diverticulitis Diet: Diverticulitis Recipes: Your Ultimate Diverticulitis CookbookFrom EverandDiverticulitis Cure: The Ultimate Diverticulitis Diet: Diverticulitis Recipes: Your Ultimate Diverticulitis CookbookNo ratings yet