Professional Documents
Culture Documents
Medical Surgerical Nursing: Lecture / Nurs 13 Ppts / Book
Medical Surgerical Nursing: Lecture / Nurs 13 Ppts / Book
Uploaded by
cheskalyka.asiloOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Medical Surgerical Nursing: Lecture / Nurs 13 Ppts / Book
Medical Surgerical Nursing: Lecture / Nurs 13 Ppts / Book
Uploaded by
cheskalyka.asiloCopyright:
Available Formats
MEDICAL SURGERICAL NURSING
LECTURE / NURS 13
PPTS / BOOK
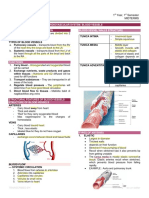
PERIPHERAL VASCULAR DISEASES • Structurally analogous to the arterial system
• Venules = arterioles, veins = arteries, and the vena cava = aorta
OUTLINE • Walls of the veins, in contrast to those of the arteries, are thinner
I Anatomy of Vascular System and considerably less muscular
II Pathophysiology of the Vascular System • The thin, less muscular structure of the vein wall allows these
III Physical Assessment of Vascular System vessels to distend more than arteries
IV Diagnostic Evaluation → Greater distensibility and compliance permit large volumes
V Peripheral Vascular Diseases of blood to remain in the veins under low pressure
VI Arterial Disorders → Veins are referred to as capacitance vessels
VII Venous Disorders • Contraction of skeletal muscles in the extremities creates the
primary pumping action to facilitate venous blood flow back to
I. ANATOMY OF VASCULAR SYSTEM the heart
• Major veins, particularly in the lower extremities, have one-way
valves that allow blood to flow against gravity
• Valves allow blood to be pumped back to the heart but prevent it
from draining back into the periphery
LYMPHATIC VESSELS
• Complex network of thin-walled vessels similar to the blood
capillaries
• Collects lymphatic fluid from tissues and organs and transports
the fluid to the venous circulation
• Converge into two main structures: the thoracic duct and the
right lymphatic duct
→ Ducts empty into the junction of the subclavian and the
internal jugular veins
ARTERIES • Right lymphatic duct: conveys lymph primarily from the right
side of the head, neck, thorax, and upper arms
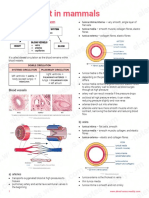
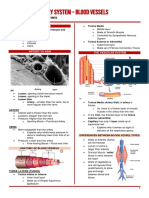
• Thick-walled structures that carry blood from the heart to the
tissues • Thoracic duct: conveys lymph from the remainder of the body
• Aorta: gives rise to numerous branches, which continue to divide • Peripheral lymphatic vessels: join larger lymph vessels and
into progressively smaller arteries pass-through regional lymph nodes before entering the venous
circulation
• Arterioles: smallest arteries, generally embedded within the
tissues • Lymph nodes: play an important role in filtering foreign particles
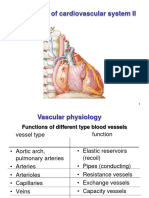
Walls of Arteries FUNCTION OF VASCULAR SYSTEM
• → Inner endothelial cell layer Functions
Tunica • → Very thin layer → Circulatory needs of tissue →
• Blood flow
intima • → Provides a smooth surface for contact with the
→ Blood pressure •
→ Capillary filtration and
flowing blood
reabsorption
•→ A middle layer of smooth muscle and elastic
→ Hemodynamic resistance •
→ Peripheral vascular
tissue
regulating mechanisms
Makes up most of the vessel wall in the aorta
→
and other large arteries of the body II. PATHOPHYSIOLOGY
Tunica Composed chiefly of elastic and connective • Reduced blood flow through peripheral blood vessels
media tissue fibers that give the vessels considerable characterizes all peripheral vascular diseases
strength and allow them to constrict and dilate
→ to accommodate the blood ejected from the
• The physiologic effects of altered blood flow depend on the
heart during each cardiac cycle (stroke extent to which tissue demands exceed the supply of oxygen and
nutrients available
volume) and maintain an even, steady flow of
blood • If tissue needs are high, even modestly reduced blood flow may
→ Outer layer of connective tissue be inadequate to maintain tissue integrity
Tunica
→ Layer of connective tissue that anchors the • Tissues then fall prey to ischemia, become malnourished, and
adventitia ultimately die unless adequate blood flow is restored
vessel to its surroundings
PUMP FAILURE
Note: • Inadequate peripheral blood flow occurs when the heart’s
The intima and the inner third of the smooth muscle layer of the pumping action becomes inefficient
media are in such close contact with the blood that the blood • Left-sided heart failure (Left Ventricular Failure)
vessels receive their nourishment by direct diffusion. The → Causes an accumulation of blood in the lungs and a
adventitia and the outer media layers have a limited vascular reduction in forward flow or cardiac output, which results
system for nourishment and require their own blood supply to meet in inadequate arterial blood flow to the tissues
metabolic needs.
• Right-sided heart failure (Right Ventricular Failure)
CAPILLARIES → Causes systemic venous congestion and a reduction in
• The walls of the capillaries are composed of a single layer of forward flow
endothelial cells ALTERATIONS IN BLOOD AND LYMPHATIC VESSELS
→ Thin-walled structure permits rapid and efficient transport ARTERIES
of nutrients to the cells and removal of metabolic wastes
• Arteries can become damaged or obstructed as a result of
VEINS atherosclerotic plaque, thromboemboli, chemical or
• Capillaries join to form larger vessels called venules, which join mechanical trauma, infections or inflammatory processes,
to form veins vasospastic disorders, and congenital malformations
• Thin-walled vesseld that transport deoxygenated blood from the • A sudden arterial occlusion causes profound and often
capillaries bach to the right side of the heart irreversible tissue ischemia and tissue death
ASILO, CHESKA LYKA | BSN 3-1 1
TRANS: MEDICAL SURGICAL NURSING (LECTURE)
• When arterial occlusions develop gradually, there is less risk of • Pulses should be palpated bilaterally and simultaneously,
sudden tissue death because collateral circulation may develop, comparing both sides for symmetry in rate, rhythm, and quality
giving that tissue the opportunity to adapt to gradually decreased
blood flow IV. DIAGNOSTIC EVALUATION
DOPPLER ULTRASOUND FLOW STUDIES
VEINS
• Venous blood flow can be reduced by a thromboembolus CONTINUOUS WAVE (CW) DOPPLER ULTRASOUND
obstructing the vein, by incompetent venous valves, or by a • Device may be used to detect the blood flow in vessels
reduction in the effectiveness of the pumping action of
• Emits a continuous signal through the patient’s tissues
surrounding muscles
• The signals are reflected by (“echo off”) the moving blood cells
• ↓ venous blood flow = ↑ venous pressure
and are received by the device
→ A subsequent increase in capillary hydrostatic pressure,
net filtration of fluid out of the capillaries into the interstitial • Signal is then transmitted to a loudspeaker or headphones
space, and subsequent edema → Because CW Doppler emits a continuous signal, all
vascular structures in the path of the sound beam are
• Edematous tissues cannot receive adequate nutrition from
insonated, and differentiating arterial from venous flow and
the blood and consequently are more susceptible to breakdown,
detecting the site of a stenosis may be difficult
injury, and infection
• The depth at which blood flow can be detected by Doppler is
LYMPHATIC VESSELS determined by the frequency (in megahertz [MHz]) it generates
• Obstruction of lymphatic vessels also results in edema → Lower the frequency, the deeper the tissue penetration
→ A 5- to 10-MHz probe may be used to evaluate the
• Lymphatic vessels can become obstructed by a tumor or by
peripheral arteries
damage from mechanical trauma or inflammatory processes
• Procedure in lower extremities:
CIRCULATORY INSUFFICIENCY OF THE EXTRIMITIES → Patient is placed in the supine position with the head of the
• Peripheral vascular diseases most result in ischemia and bed elevated 20 to 30 degrees
produce some of the same symptoms: pain, skin changes, → Legs are externally rotated to permit adequate access to
diminished pulse, and possible edema the medial malleolus
• The type and severity of symptoms depend in part on the type, → Acoustic gel is applied to the patient’s skin to permit
stage, and extent of the disease process and on the speed with uniform transmission of the ultrasound wave
which the disorder develops → Tip of the Doppler transducer is positioned at a 45- to 60-
degree angle over the expected location of the artery and
III. PHYSICAL ASSESSMENT OF VASCULAR SYSTEM angled slowly to identify arterial blood flow
HEALTH HISTORY • More useful as a clinical tool when combined with ankle blood
• Nurse obtains an in-depth description from the patient with pressures
peripheral vascular disease of any pain and its precipitating
factors
• Peripheral arterial insufficiency: muscular, cramp-type pain,
discomfort, or fatigue in the extremities consistently reproduced
with the same degree of exercise or activity and relieved by rest
• Intermittent claudication: pain, discomfort, or fatigue is caused
by the inability of the arterial system to provide adequate blood
flow to the tissues in the face of increased demands for nutrients
and oxygen during exercise
• Ischemia: aka rest pain, severe degree of arterial insufficiency
and a critical state of persistent pain in the when the patient is
resting, and often worse at night and may interfere with sleep
ANKLE-BRACHIAL INDEX (ABI)
• Ratio of the systolic blood pressure in the ankle to the systolic
blood pressure in the arm
• Objective indicator of arterial disease that allows the examiner to
quantify the degree of stenosis
• Procedure:
→ Patient should rest in a supine position for approximately
5 minutes
PHYSICAL ASSESSMENT → Appropriately sized blood pressure cuff (10-cm cuff) is
INSPECTION OF THE SKIN applied to the patient’s ankle above the malleolus
• Inadequate blood flow results in cool and pale extremities → After identifying an arterial signal (posterior tibial and
dorsalis pedis arteries) the systolic pressures, are
• Reduction of blood flow to tissues lead to pallor obtained in both ankles, while listening to the Doppler
• Rubor: a reddish-blue discoloration of the extremities, may be signal at each artery
observed within 20 seconds to 2 minutes after the extremity is → If pressure in these arteries cannot be measured, pressure
placed in the dependent position can be measured in the peroneal artery, which can also be
• Cyanosis: a bluish tint of the skin, is manifested when the assessed at the ankle
amount of oxygenated hemoglobin contained in the blood is • To calculate ABI, the highest ankle systolic pressure for each
reduced foot is divided by the higher of the two brachial systolic pressures
• Loss of hair, brittle nails, dry or scaling skin, atrophy, and
ulcerations
• Edema may be apparent bilaterally or unilaterally
• Gangrenous changes appear after prolonged, severe ischemia
and represent tissue necrosis
PALPATION OF PULSES
• Use light touch and avoid using only the index finger for palpation
• Absence of a pulse may indicate that the site of stenosis is
proximal to that location
• Occlusive arterial disease impairs blood flow and can reduce
or obliterate palpable pulsations in the extremities
ASILO, CHESKA LYKA | BSN 3-1 2
TRANS: MEDICAL SURGICAL NURSING (LECTURE)
EXERCISE TESTING Often absent or
Pulse Usually, present
• Used to determine how long a patient can walk and to measure diminished
the ankle systolic blood pressure in response to walking • Frequent, especially at
• The patient walks on a treadmill at 1.5 mph with a 12% incline Edema Infrequent the end of the day and in
for a maximum of 5 minutes, or the test can be modified to areas of ulceration
walking a set distance in a hallway
RISK FACTORS
• A normal response to the test is little or no drop in ankle systolic
pressure after exercise • Age (elderly): Blood vessels become less elastic, become thin
walled and calcified
• Patient with true vascular claudication, the ankle pressure drops
→ ↑ PVR = ↑ BP
• Reassure the patient that the treadmill test will not require
running; rather, the test may require walking on a slight incline
• Sex (male)
• Cigarette smoking
DUPLEX ULTRASONOGRAPHY → Nicotine causes vasoconstriction and spasm of the
• Involves B-mode grayscale imaging of the tissue, organs, and arteries = ↓ circulation to the extremities
blood vessels (arterial and venous) and permits estimation of → CO2 inhaled in cigarette smoke reduces O2 transport to
velocity changes by use of a pulsed Doppler tissues
• Color flow techniques: identify vessels, may be used to shorten • Hypertension: cause elastic tissues to be replaced by fibrous
the examination time collagen tissue
• Used to determine the level and extent of venous disease as well → Arterial wall become less distensible = ↑ resistance to
as chronicity of the disease blood flow = ↑ Blood pressure
• Noninvasive and usually requires no patient preparation • Hyperlipidemia: atherosclerotic plaque
• B mode and Doppler: possible to image and assess blood flow, • Obesity: places added burden on the heart and blood vessels
evaluate flow of the distal vessels, locate the disease, and because excess fat contributes to ↑ venous congestion
determine anatomic morphology and the hemodynamic • Lack of physical activity
significance of plaque causing stenosis → Physical activity promotes muscle contraction = ↑ venous
• Patients who undergo abdominal vascular duplex ultrasound return to the heart
NPO for 6 hours before procedure → Aids in development of collateral circulation
• Emotional stress: stimulates sympathetic NS = peripheral
vasoconstriction = ↑ BP
• Diabetes Mellitus: changes in glucose and fat metabolism
promote the atherosclerotic process
• Family history of atherosclerosis
VI. ARTERIAL DISORDERS
ARTERIOSCLEROSIS OBLITERANS
• Disorder in which there is an atherosclerotic narrowing or
obstruction of the inner and middle later of the artery
• Most common cause of arterial obstructive diseases in the
extremities
• Lowe extremities are involved more than the upper extremities
• Common site of disease: femoral artery, iliac arteries,
popliteal arteries
V. PERIPHERAL VASCULAR DISEASES • In a diabetic person, the disease becomes more progressive
which affects the smaller arteries and often involves vessels
• Characterized by a reduction on the blood flow and hence below the knee
oxygen, through the peripheral vessels • Accumulation of lipids, calcium, blood components,
• When the need of the tissues for oxygen, exceeds the supply, carbohydrates, and fibrous tissue on the intimal layer of the
areas of ischemia and necrosis will develop artery
• Factors that can contribute to the development of PVD → Accumulations are referred to as atheromas or plaques
→ Atherosclerotic changes
→ Thrombus formation
→ Embolization
→ High coagulability of blood
→ Hypertension
→ Inflammatory process or infection
ARTERIAL INSUFFICIENCY
• Decreased blood flow toward the tissues, producing ischemia
• Pulses usually diminished or absent
• Sharp, stabbing pain occurs because of ischemia, particularly
with activity
• There is interference with nutrients and oxygen arriving to the
tissues, leading tot ischemic ulcers and changes in the skin
VENOUS INSUFFICIENCY PATHOPHYSIOLOGY
• Decreased return of blood from the tissues to the heart
• Plaque formation on the intimal wall that causes partial or
• Leads to venous congestion and stasis of blood complete occlusion
• Pulses are present • Calcification of the middle layer and a gradual loss of elasticity
Arterial Disease Venous Disease leads to weakened arterial walls
Cool or cold, hairless, dry, Warm, thickened, • Predisposes to aneurysm, dilation, or thrombus formation
Skin shiny, pallor on elevation, mottled, pigmented → Artery is unable to transport an adequate blood volume to
rubor on dangling areas the tissues during exercise or rest
• Symptoms appear when the blood vessels no longer provide
Aching, cramping, enough blood to supply O2, and nutrients and remove metabolic
Sharp, stabbing, worsens
activity and walking waste products
Pain with activity and walking,
helps, elevating feet
lowering may relieve pain
relieves pain CLINICAL MANIFESTATIONS
Severely painful; pale; Moderately painful, pink • Intermittent claudication
Ulcers gray base; found on heel, base, found on medial → Pain in the extremity that develops in a muscle that has an
toes, dorsum of the foot aspect of the ankle inadequate blood supply during exercise
ASILO, CHESKA LYKA | BSN 3-1 3
TRANS: MEDICAL SURGICAL NURSING (LECTURE)
→ The cramping pain disappear within 1-2 minutes after
stopping the exercise or resting THROMBOANGITIS OBLITERANS
→ The femoral artery is often affected: pain in the calf muscle (BUERGER’S DISEASE)
in the most common symptom • Characterized by acute inflammatory lesions and occlusive
• Pain at rest is indicative of severe disease thrombosis of the arteries and veins
→ Gnawing, burning pain that occur more frequently at night • Has a very strong association with cigarette smoking
• Feelings of coldness • Commonly occurs in male between 20-40 years old
• Numbness or tingling sensation • May involve arteries of the upper extremities (wrist)
• Advanced arteriosclerosis obliterans = ischemia = necrosis, • Usually affect the lower leg, toes, and feet
ulcerations, and gangrene in the toes and distal foot
DIAGNOSTIC TESTS
• Doppler ultrasonography: high frequency sound waves
directed to artery or veins through a hand-held transducer moved
evenly across the skin surface
→ Audible tone produced in proportion to blood velocity
→ Measure blood flow through blood vessels
MANAGEMENT
• Directed toward prevention of vessel occlusion
→ Use of vasodilators
• Surgical Intervention
→ Embolectomy: removal of blood clot, done when large
arteries are obstructed
→ Endarterectomy: removal of blood clot and stripping of CLINICAL MANIFESTATION
atherosclerotic plaque along with the inner arterial wall • Intermittent claudication in the arch of the foot
→ Arterial by-pass surgery: an obstructed arterial segment
• Pain during rest in toes
may be bypassed by using a prosthetic material (Teflon)
or the patient’s own artery or vein (saphenous vein) • Coldness due to persistent ischemia
→ Percutaneous transluminal angioplasty • Paresthesia
(atherectomy): balloon tip of the catheter is inflated to • Weak or absent pulsation in posterior tibial or dorsalis pedis
provide compression of the plaque • Extremities are red or cyanotic
→ Amputation: with advanced atherosclerosis and • Ulceration and gangrene are frequent complications
gangrene of the extremities; toes are the most often → Early can occur spontaneously but often follow trauma
amputated part
INTERVENTIONS
NURSING INTERVENTIONS
• Advise person to stop smoking
ASSESS • Vasodilators
• Condition of the skin: shiny, taut, absence of hair growth • Prevent progression of disease
(indicates poor circulation) • Avoid trauma to ischemic tissues
• Ulcerations or necrotic tissues • Relieve pain
• Extremely cold to touch • Provide emotional support
• Peripheral pulses: diminished, weak, absent, bilateral inequality • Advise patient to avoid mechanical, chemical, or thermal injuries
to the feet
Grading Meaning
0 Absent • Amputation of the leg is only done when the following occurs:
1+ Weak and thready → Gangrene extends well into the foot
→ Pain is severe and cannot be controlled
2+ Norrmal
→ Severe infection or toxicity occurs
3+ Ful and bounding
• Prolonged or absent capillary refill of nailbeds
• Loss of muscle tone or weakness
• Prevent further progression of existing disease
ACUTE CARE
• Monitor the limb distal to the affected site for changes in color or
temperature
→ ↓ arterial flow (pale and cool initially) = bluish or darker =
tissue becoming necrotic and black
• Activities that cause pain should be avoided
• Give vasodilators if prescribed: relaxation of vascular smooth
muscle = decreased pain
• Comfort measures: proper body positioning to decrease
pressure on the affected area
REYNAUD’S DISEASE
POST-OPERATIVE CARE FOR ARTERIAL SURGERY • Unknown etiology, may be due to immunologic abnormalities
• Patient is monitored for signs of decreased circulation in the • Common in women between 20-40 years old
affected limb and interventions done to promote circulation and • May be stimulated by emotional stress, hypersensitivity to cold,
comfort alteration in sympathetic innervation
• Assess and report changes in skin color and temperature distal
to the surgical site every 2-4 hours
• Assess peripheral pulses
→ Sudden absence in pulse may indicate thrombosis
→ Mark location of pulse with pen to facilitate frequent
assessment
• Assess wound for redness, swelling, and drainage
• Promote circulation
→ Reposition patient every 2 hours
→ Tell patient not to cross legs
→ Encourage progressive activity when permitted
• Medication with analgesics to reduce pain
ASILO, CHESKA LYKA | BSN 3-1 4
TRANS: MEDICAL SURGICAL NURSING (LECTURE)
REYNAUD’S PHENOMENON TYPES OF ANEURYSMS
• Refers to intermittent episodes during which small arteries
or arterioles of the left and right arm constrict (spasm) SACCULAR ANEURYSM
causing changes in skin color and temperature • Involves only part of the circumference of the artery
• Generally unilateral and may affect only 1-2 fingers • Takes the form of a sac or pouch like dilation attached to the side
• Characterized by reduction of blood flow to the fingers of artery
manifested by cutaneous vessel constriction and resulting in
blanching or pallor FUSIFORM ANEURYSM
• Spindle shaped
• Involves the entire circumference of the arterial wall
DISSECTING ANEURYSM
• Involves hemorrhage into a vessel wall, which splits and dissects
the wall causing a widening of the vessel
• Cause by degenerative defect in the tunica media and tunica
intima
CLINICAL MANIFESTATIONS
• During arterial spasm: slugging blood flow causes pallor,
coldness, numbness, cutaneous cyanosis, and pain
• Following the spasm: involve area become intensely reddened
with tingling and throbbing sensations
• Long-lasting or prolonged Reynaud’s disease: ulcerations DIAGNOSTIC TESTS
can develop on the fingertips and toes • Chest and abdominal x-rays: helpful in preliminary diagnosis
MEDICAL MANAGEMENT of aortic aneurysm
• Ultrasound: useful in determining the size, shape, and location
• Aimed at prevention
od the aneurysm
• Person is advised to protect against exposure to cold
• Quit smoking THORACIC AORTIC ANEURYSM
• Drug therapy: calcium channel blockers, vascular smooth • Aneurysm in the thoracic area
muscle relaxants, vasodilators - promote circulation and • Occur most frequently in hypertensive men between 40-70 years
reduce pain old
• Sympathectomy: cutting off sympathetic nerve fibers to • Can develop in the ascending, transverse, or descending aorta
relieve symptoms in the early stage of advanced ischemia • Signs and symptoms:
• In ulceration or gangrene occur, the area may need to be → Chest pain – most frequent; perceived when patient is in a
amputated supine position
→ Cough
NURSING INTERVENTIONS
→ Dyspnea
• Collect data on effects of associated factors: emotional stress, → Hoarseness
exposure to cold, cigarette smoking → Dysphagia
• Prevent injury, promote circulation
• Provide comfort
• Teach patient on effects of smoking and advise to quit smoking
• Discuss wats to avoid exposure to cold
→ Wear adequate clothing to promoter warmth
→ Wear gloves and socks
→ Use caution when cleaning refrigerator and freezer
→ Wear gloves when handling frozen foods
• Avoid drugs that will cause vasoconstriction (birth control pills or
ergotamine)
• Suggest anti-inflammatory analgesics to promote comfort
ANEURYSM
• Localized or diffuse enlargement of an artery at some point along
its course ABDOMINAL AORTIC ANEURYSM
• Can occur the vessel becomes weakened from trauma, • Most common site for the formation of an aortic aneurysm
congenital vascular disease, infection, or atherosclerosis • Abdominal aorta below renal arteries
PATHOPHYSIOLOGY • Sign and Symptoms:
→ Presence of pulsatile abdominal mass on palpation
Enlargement of a segment of an artery → Pain or tenderness in the mid or upper abdomen
→ The aneurysm may extend to impinge on the renal, iliac,
Tunica media is damages or mesenteric arteries
→ Stasis of blood favors thrombus formation along the wall
Progressive dilation and degeneration of the vessel
• Rupture of the aneurysm: most feared complication that can
Risk of rupture occur if the aneurysm is large; can lead to death
• Treatment
• Most common site is the aorta → Surgery: resection of the lesion and replacement with a
• May develop in any blood vessel graft
ASILO, CHESKA LYKA | BSN 3-1 5
TRANS: MEDICAL SURGICAL NURSING (LECTURE)
• Monitor anticoagulant or fibrinolytic therapy and assess for signs
of bleeding: nose or gum bleeding, petechiae, ecchymosis, or
hematoma formation
• Avoid IM injections, use soft toothbrush, use electric razor rather
than razor blasé, avoid rectal thermometer
VII. VENOUS DISORDERS
• Alteration in the transport or flow of blood from the capillary back
to the heart
• Changes in smooth muscle and connective tissue make the
veins less distensible with limited recoil capacity
• Valves may malfunction, causing backflow of blood
• Virchow’s triad: blood stasis, vessel wall injury, and altered
blood coagulation
THROMBOPHLEBITIS
• Inflammation of the veins caused by thrombus or blood clot
ARTERIAL EMBOLISM • Factors with the development of thrombophlebitis
• Blood clots floating in the circulating arterial blood → Venous stasis
• The embolus is frequently a fragment of arteriosclerotic plaque → Damage to the vessel wall
loosened from the aorta → Hypercoagulability of the blood (oral contraceptive use)
• Emboli will tend to lodge in femoral or popliteal arteries = blood → Common to hospitalized patients who undergone major
flow is impaired and ischemia develops surgery (pelvic or hip surgery), myocardial infarction
• Signs and symptoms
→ Depends in the size of the embolus, the presence of
collateral circulation and is it is close to a major organ
→ Abrupt onset of severe pain from the sudden cessation of
circulation
→ Muscular weakness and burning, aching pain occur
→ Distal pulses are absent and extremity becomes cold,
numb, and pale
→ Symptoms of shock may develop if the embolus blocks a
large artery
PATHOPHYSIOLOGY
• Develops in both deep and superficial veins of the lower
extremities
• Deep veins: femoral, popliteal, small calf veins
• Superficial veins: saphenous vein
• Thrombus: form in the veins from accumulation of platelets,
fibrin, white blood cells, and red blood cells
DEEP VEIN THROMBOSIS (DVT)
• Tends to occur at bifurcations of the deep veins, which are sites
of turbulent blood flow
MEDICAL MANAGEMENT • A major risk during acute phase of thrombophlebitis is
• Bed rest dislodgement of the thrombus = embolus
• Anticoagulants: prolong the clotting time of the blood to prevent • Pulmonary embolus: serious complication arising from DVT of
clot extension and new clot formation the lower extremities
→ Heparin – inhibits thrombin action = prevent clotting CLINICAL MANIFESTATIONS
✓ IV or SQ
✓ Antidote – Protamine sulfate • Pain and edema of the extremity – obstruction of venous blood
→ Warfarin sodium (Coumadin) – inhibits Vitamin K flow
dependent clotting factor = decreased prothrombin activity • Increased circumference of the thigh or calf
✓ Oral (10-15 mg/day) • (+) Homan’s sign – dorsiflexion of the foot produces calf pain
✓ Antidote – Vitamin K → Do not check for Homan’s sign if DVT is already known to
• Fibrinolytics or thrombolytics: useful for dissolving existing be present = ↑ risk of embolus formation
thrombus or clot when rapid dissolution of the clot is required to • If superficial veins are affected, signs of inflammation may be
preserve organ and limb function noted
→ Streptokinase and Urokinase → Redness
✓ IV → Warmth
✓ Side effect: bleeding → Tenderness
• Embolectomy: surgical removal of blood clot when large → Veins feel hard and thready and sensitive to pressure
arteries are obstructed
→ Must be performed within 6-10 hours to prevent muscle
necrosis and loss of extremity
NURSING MANAGEMENT
• Monitor the patient during acute phase for changes of color and
temperature of the extremity distal to the clot
• Assess for increasing pallor, cyanosis, or coldness, of the skin
• Keep the extremity warm, but do not apply heat
• Avoid chilling
• Monitor peripheral pulses for quality (weak or absent)
• Keep affected extremity flat or lightly dependent position to
promote circulation
ASILO, CHESKA LYKA | BSN 3-1 6
TRANS: MEDICAL SURGICAL NURSING (LECTURE)
MEDICAL MANAGEMENT • Give analgesic and anti-inflammatory agents to promote comfort
SUPERFICIAL THROMBOPHLEBITIS
CHRONIC VENOUS INSUFFICIENCY
• Bed rest with legs elevated • Results from obstruction of venous valves in legs or reflux of
• Apply moist heat blood back through the valves
• NSAIDs – aspirin • Venous ulceration is serious complication
DEEP VEIN THROMBOSIS • Pharmacological therapy is antibiotics for infections
• Requires hospitalization • Debridement to promote healing
• Bed rest with leg elevated to 15-20 degrees above heart level • Topical therapy may be used with cleansing and debridement
• Application of warm moist heat to reduce pain, promotes
VARICOSE VEINS
venous return
• Elastic stocking or bandage
• Abnormally dilated veins with incompetent veins, occurring
mostly in the lower extremities
• Anticoagulants, initially with IV heparin then coumadin
• Usually affect women ages 30-50 years old
• Fibrinolytic to resolve the thrombus
• Causes:
• Vasodilator if needed to control vessel spasm and improve → Congenital absence of valve
circulation → Incompetent valves due to external pressure on the veins
SURGERY from pregnancy, ascites, or abdominal tumors
→ Sustained increase in venous pressure due to CHF,
• If the thrombus is recurrent and extensive, or it the patient is at cirrhosis
high risk for pulmonary embolism
• Prevention:
• Thrombectomy: incising the common femoral vein in the groin → Wear elastic stockings during activities that require long
and extracting the clots standing or when pregnant
• Vena cava interruption: transvenous placement of a grid or → Moderate exercise
umbrella filler in the vena cava to block the passage of the emboli → Elevation of legs
ASSESSMENT
PATHOPHYSIOLOGY
• Characteristic of the pain
• Onset and duration of symptoms • The great and small saphenous veins are most often involved
• History of thrombophlebitis or venous disorders Weakening of the vein wall
• Color temperature of the extremity
• Edema of calf or thigh – use a tape measure and measure both Does not withstand normal pressure
legs for comparison
Veins dilate, pooling of blood
NURSING INTERVENTIONS
PREVENTIVE CARE Veins become stretched and incompetent
• Prevent long periods of standing or sitting that impair venous
return Accumulation of blood in the veins
• Elevate legs when sitting, dorsiflex feet at regular intervals to
prevent venous pooling CLINICAL MANIFESTATIONS
• If edema occurs, elevate above heart level • Primary varicosities
• Regular exercise program to promote circulation → Gradual onset and affect superficial veins
• Avoid crossing legs at the knees → Appearance of dark tortuous veins
→ Signs and symptoms: dull aches, muscle cramps,
• Avoid wearing constrictive clothing such as tight bands around
pressure, heaviness or fatigue arising from reduced blood
socks or garters
flow to the tissues
• Use elastic stocking on affected leg
• Secondary varicosities
• Do leg exercises during periods of enforced immobility such as → Affect the deep veins
after surgery → Occur due to chronic venous insufficiency or venous
NURSING MANAGEMENT thrombosis
ACUTE CARE → Signs and symptoms: edema, pain, changes in skin color,
ulcerations may occur from venous stasis
• Explain purpose of bed rest and leg elevation
• Use elastic stockings
• Monitor patient on anticoagulant and fibrinolytic therapy for signs
of bleeding
• Monitor for signs of pulmonary embolism – sudden onset of
chest pain, dyspnea, rapid breathing, tachycardia
AFTER SURGERY OF VENA CAVAL INTERRUPTION
• Assess insertion site for bleeding, hematoma, apply pressure
over the site and inform physician
• Keep patient on bed rest for the 1st 24 hours then encourage
ROM exercises to promote venous return
• Assis patient in ambulation when permitted, elevate legs when
sitting
• Keep elastic bandage
• Avoid rubbing or massaging the affected extremity
ASILO, CHESKA LYKA | BSN 3-1 7
You might also like
- Perioperative Management of Anticoagulant andDocument14 pagesPerioperative Management of Anticoagulant andIlija Kosić100% (2)
- Prometric Questions OrthoDocument13 pagesPrometric Questions OrthoFaisal Mushtaq67% (12)
- Emergency Nursing Notes 2Document14 pagesEmergency Nursing Notes 2pauchanmnl100% (3)
- Blood VesselsDocument5 pagesBlood Vesselsdelemos.sahmaeNo ratings yet
- Chapter 13 - Blood Vessels and CirculationDocument21 pagesChapter 13 - Blood Vessels and CirculationGabriel CastenNo ratings yet
- (BCA 1) Cardiac Physiology 1 - Dr. Valerio (2025)Document18 pages(BCA 1) Cardiac Physiology 1 - Dr. Valerio (2025)Carla PNo ratings yet
- Blood Vessels & CirculationDocument7 pagesBlood Vessels & CirculationCORONEL, SOPHIANo ratings yet
- 8 Transport in MammalsDocument4 pages8 Transport in MammalsTala AlkhawajaNo ratings yet
- AP10-Cardio-Blood VesselsDocument13 pagesAP10-Cardio-Blood VesselsPay per PrintNo ratings yet
- AP10 Cardio Blood VesselsDocument13 pagesAP10 Cardio Blood VesselsLyn YmiNo ratings yet
- Circulatory System PDFDocument5 pagesCirculatory System PDFNibshian Dela RosaNo ratings yet
- 2024-Nursing-Arterial and Venous SystemDocument38 pages2024-Nursing-Arterial and Venous SystemSyed Husnain Ali ShahNo ratings yet
- Circulatory SystemDocument42 pagesCirculatory SystemCenen de GuzmanNo ratings yet
- Cardiac Module - PVDDocument2 pagesCardiac Module - PVDMarie MNNo ratings yet
- Anaphy Blood Vessels Lab - HandoutDocument7 pagesAnaphy Blood Vessels Lab - HandoutAEGEL DARO TORRALBANo ratings yet
- Cardiovascular or Circulatory SystemDocument3 pagesCardiovascular or Circulatory SystemALEXIS MOIRAH CALIGAGANNo ratings yet
- Histology and Microtechniques Biology 160 Prof. Maria Luisa J. LandinginDocument2 pagesHistology and Microtechniques Biology 160 Prof. Maria Luisa J. LandinginDavid YapNo ratings yet
- Chap +5+Cardiovascular+SyDocument39 pagesChap +5+Cardiovascular+SySalman MasriNo ratings yet
- Circulatory System 1Document4 pagesCirculatory System 1Jhes D.No ratings yet
- CH 11 Vessels PDFDocument10 pagesCH 11 Vessels PDFIbra TutorNo ratings yet
- Intro On Circulatory System-UoC - 191123Document29 pagesIntro On Circulatory System-UoC - 191123Hidayah Mohamad raniNo ratings yet
- Circulatory System HandoutsDocument4 pagesCirculatory System HandoutsCzarae VillanuevaNo ratings yet
- Physio 1.7 Circulation - Blood Vessels Flow and Regulation Dr. UbinaDocument15 pagesPhysio 1.7 Circulation - Blood Vessels Flow and Regulation Dr. UbinapachayilstephanoseshintoNo ratings yet
- Cardiovascular System.Document37 pagesCardiovascular System.Wajahat FaizNo ratings yet
- Lesson 3: Animal Circulatory Systems PDFDocument5 pagesLesson 3: Animal Circulatory Systems PDFAli SighNo ratings yet
- Vascular SystemDocument218 pagesVascular SystemHeli MalivadNo ratings yet
- Circulatory System II Blood VesselsDocument7 pagesCirculatory System II Blood VesselsBrent ValdespinaNo ratings yet
- Cardiovascular SystemDocument8 pagesCardiovascular SystemChelsie NicoleNo ratings yet
- Cardiovascular System Blood: ObjectivesDocument4 pagesCardiovascular System Blood: ObjectiveschegleNo ratings yet
- Circulatory System REVIEWERDocument6 pagesCirculatory System REVIEWERClyde BaltazarNo ratings yet
- 4 - Blood Vessel AnatomyDocument23 pages4 - Blood Vessel AnatomyRashpal SidhuNo ratings yet
- The Mammali An Circulator y SystemDocument21 pagesThe Mammali An Circulator y SystemFern BaldonazaNo ratings yet
- Arterial, Arteriolar, Capillary, Venous & Lymphatic Circulations Feyitimi AaDocument67 pagesArterial, Arteriolar, Capillary, Venous & Lymphatic Circulations Feyitimi Aaintarebatinya32No ratings yet
- Circulatory SystemDocument2 pagesCirculatory SystemMiguel Christian SilvestreNo ratings yet
- CH13 BLOOD-VESSELS ByissaDocument8 pagesCH13 BLOOD-VESSELS ByissaRoeisa SalinasNo ratings yet
- Functional Histology - Heart Conduction and VesselsDocument41 pagesFunctional Histology - Heart Conduction and VesselsDrSanket HiwareNo ratings yet
- Vascular SystemDocument34 pagesVascular SystemCHRISTINE M. SALIGANNo ratings yet
- The Vascular SystemDocument7 pagesThe Vascular SystemMiguel GumatayNo ratings yet
- Circulatory StudentsDocument45 pagesCirculatory Studentsiananicole.b30No ratings yet
- Urinary System Functions: - Filtering of Blood Via Filtration, Reabsorption, Secretion. - Regulation ofDocument35 pagesUrinary System Functions: - Filtering of Blood Via Filtration, Reabsorption, Secretion. - Regulation ofmelissa_sunNo ratings yet
- Blood VesselsDocument13 pagesBlood VesselsRalph Rezin MooreNo ratings yet
- 10) Circulatory SysDocument60 pages10) Circulatory SysyohdeforemostNo ratings yet
- MTHISTO100 Lesson 2 Excretory SystemDocument9 pagesMTHISTO100 Lesson 2 Excretory SystemJaeri HuangNo ratings yet
- Cardiovascular System (Blood Vessels and Circulation) : Roger Joseph II R. Jecino, R.N., M.DDocument53 pagesCardiovascular System (Blood Vessels and Circulation) : Roger Joseph II R. Jecino, R.N., M.DIan MendezNo ratings yet
- Circulatory System PearsonsDocument16 pagesCirculatory System Pearsonsblando.shaneNo ratings yet
- Heart 2Document56 pagesHeart 2migas1996No ratings yet
- Lecture 4 Cardiovascular System 2Document42 pagesLecture 4 Cardiovascular System 2hafiz patahNo ratings yet
- HemodynamicsDocument40 pagesHemodynamicsBravo HeroNo ratings yet
- 013 Cardiovascular Physiology Blood Vessel CharacteristicsDocument3 pages013 Cardiovascular Physiology Blood Vessel CharacteristicsTtNo ratings yet
- Blood Vessels and Blood PressureDocument21 pagesBlood Vessels and Blood PressureIAhmad QasimNo ratings yet
- Anatomy Physiology Lecture Endterm ReviewerDocument34 pagesAnatomy Physiology Lecture Endterm ReviewerKristil ChavezNo ratings yet
- Lesson 3 Lymphatic System and Body DefensesDocument10 pagesLesson 3 Lymphatic System and Body DefensesJulio De GuzmanNo ratings yet
- Anatomy Finals ReviewerDocument21 pagesAnatomy Finals ReviewerNicole Faith L. NacarioNo ratings yet
- VII - Urinary SystemDocument2 pagesVII - Urinary SystemGael QuingNo ratings yet
- The Cardiovascular System: Blood Vessels and Hemodynamics: Principles of Human Anatomy and Physiology, 11e 1Document89 pagesThe Cardiovascular System: Blood Vessels and Hemodynamics: Principles of Human Anatomy and Physiology, 11e 1Izra Joy MerivelesNo ratings yet
- Anaphy Chapter 21 Blood Vessels and Circulatory Doran Mls 1 FDocument12 pagesAnaphy Chapter 21 Blood Vessels and Circulatory Doran Mls 1 FayenaNo ratings yet
- CardioDocument10 pagesCardioMonica SabarreNo ratings yet
- Lymphatic SystemDocument11 pagesLymphatic SystemPlacido Edgar MagaNo ratings yet
- V. Anat 121 Lecture 21-23Document5 pagesV. Anat 121 Lecture 21-23mjdangca0111No ratings yet
- Blood Vessels and Circulation - Chapter 13 Blood Vessels Artery and VeinDocument11 pagesBlood Vessels and Circulation - Chapter 13 Blood Vessels Artery and VeinLol lolNo ratings yet
- Histology of Circulatory SystemDocument156 pagesHistology of Circulatory SystemErmiyas BeletewNo ratings yet
- Human Body Book | Introduction to the Circulatory System | Children's Anatomy & Physiology EditionFrom EverandHuman Body Book | Introduction to the Circulatory System | Children's Anatomy & Physiology EditionNo ratings yet
- CHN Transes Week 1Document5 pagesCHN Transes Week 1cheskalyka.asilo100% (1)
- CHN LabDocument13 pagesCHN Labcheskalyka.asiloNo ratings yet
- CHN Transes Week 2Document2 pagesCHN Transes Week 2cheskalyka.asiloNo ratings yet
- Medical Surgerical Nursing: Lecture / Nurs 13 Ppts / BookDocument4 pagesMedical Surgerical Nursing: Lecture / Nurs 13 Ppts / Bookcheskalyka.asiloNo ratings yet
- Nurs 13 Lec AbgDocument3 pagesNurs 13 Lec Abgcheskalyka.asiloNo ratings yet
- Clinical Periodontology and Implant Dentistry, 6th.2Document2 pagesClinical Periodontology and Implant Dentistry, 6th.2Reynante, Jeremy Eleison M.No ratings yet
- 05 - 26 - 22 TahbsoDocument29 pages05 - 26 - 22 TahbsoMa. Therese GarganianNo ratings yet
- Diagnosis and Plan of Implant PatientDocument35 pagesDiagnosis and Plan of Implant PatientShahbaz Saqib100% (1)
- Set, Laparotomy, Instruments: General InformationDocument2 pagesSet, Laparotomy, Instruments: General Informationiqbal meerNo ratings yet
- Thorax (2) 2Document86 pagesThorax (2) 2Hà Quang SơnNo ratings yet
- OET Practice Writing TestDocument2 pagesOET Practice Writing TestyazzNo ratings yet
- Dental Implants Treatment in Kerala, India - Novadent CareDocument16 pagesDental Implants Treatment in Kerala, India - Novadent CareNovadent CareNo ratings yet
- DMV Cipe Di AtriaDocument6 pagesDMV Cipe Di AtriaAngélica ContrerasNo ratings yet
- Colonoscopy: Dr. Aries Budianto, SPB (K) BDDocument52 pagesColonoscopy: Dr. Aries Budianto, SPB (K) BDRisal WintokoNo ratings yet
- Video Telescopic Operating Microscope - A Recent Development in Reptile MicrosurgeryDocument4 pagesVideo Telescopic Operating Microscope - A Recent Development in Reptile MicrosurgeryChecko LatteNo ratings yet
- Failed Hypospadias in Paediatric PatientsDocument11 pagesFailed Hypospadias in Paediatric PatientsJemy IkkiNo ratings yet
- Yanlin Ma Feb 3 PDFDocument2 pagesYanlin Ma Feb 3 PDFMitziNo ratings yet
- 9th Eng Ut2Document2 pages9th Eng Ut2officerscorrido1407No ratings yet
- Endoscopic Parathyroid Surgery: Results of 365 Consecutive ProceduresDocument5 pagesEndoscopic Parathyroid Surgery: Results of 365 Consecutive ProceduresEmilio SanchezNo ratings yet
- The Greatest Miracle On Earth Is The Human BodyDocument1 pageThe Greatest Miracle On Earth Is The Human Bodyapi-463277619No ratings yet
- BIO 302L Laboratory Report - Circulatory System - Group 5Document9 pagesBIO 302L Laboratory Report - Circulatory System - Group 5Jv Dela CruzNo ratings yet
- Self Correcting ANOMALIESDocument31 pagesSelf Correcting ANOMALIESDONA MARIAM SAMNo ratings yet
- Thoracic Surgery 1989Document500 pagesThoracic Surgery 1989cretu mihaiNo ratings yet
- Crosswalk From CMS DRGs To MS-DRGsDocument46 pagesCrosswalk From CMS DRGs To MS-DRGsswilliams6622No ratings yet
- CPT PCM NHSNDocument307 pagesCPT PCM NHSNYrvon RafaNo ratings yet
- CLABSI - Central Lines in ICUDocument28 pagesCLABSI - Central Lines in ICUChamika Madushan ManawaduNo ratings yet
- THE Electrocardiogram (ECG)Document13 pagesTHE Electrocardiogram (ECG)Bander Binjabaan Al-QahtaniNo ratings yet
- SRI 1 - 2020 Airway Management in Critical Illness An UpdateDocument11 pagesSRI 1 - 2020 Airway Management in Critical Illness An UpdateAlejandro OlivaNo ratings yet
- Angie ResumeDocument2 pagesAngie Resumeapi-270344093No ratings yet
- Iti Implant Course 2018 PDFDocument5 pagesIti Implant Course 2018 PDFShyam K MaharjanNo ratings yet
- Niyats Proposal DraftDocument35 pagesNiyats Proposal DraftrobelNo ratings yet
- Clinical EndodonticsDocument30 pagesClinical EndodonticsJemmy WendyNo ratings yet