Professional Documents
Culture Documents
The P-Wave, PR Interval and PR Segment
The P-Wave, PR Interval and PR Segment
Uploaded by
llocopoloOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
The P-Wave, PR Interval and PR Segment
The P-Wave, PR Interval and PR Segment
Uploaded by
llocopoloCopyright:
Available Formats
ECG
Friday, January 29, 2021 2:59 PM
PR interval and PR segment
The P-wave
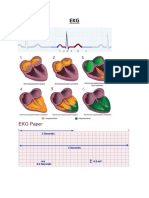
The PR interval starts at the onset of the P-wave and ends at the onset of the QRS complex ( Figure 1 ). It
ECG interpretation usually starts with an assessment of the P-wave. The P-wave is a small, positive and reflects the time interval from the start of atrial depolarization to the start of ventricular depolarization.
smooth wave. It is small because the atria make a relatively small muscle mass. If the rhythm is sinus The PR interval is assessed in order to determine whether impulse conduction from the atria to the
rhythm (i.e under normal circumstances) the P-wave vector is directed downwards and to the left in the ventricles is normal in terms of speed. The PR interval must not be too long nor too short. A normal PR
frontal plane and this yields a positive P-wave in lead II ( Figure 2 , right-hand side). The P-wave is interval ranges between 0.12 seconds to 0.22 seconds.
always positive in lead II during sinus rhythm. This is rather easy to understand because lead II is angled
alongside the P-wave vector, and the exploring electrode is located in front of the P-wave vector The flat line between the end of the P-wave and the onset of the QRS complex is called the PR segment
( Figure 2, right-hand side). and it reflects the slow impulse conduction through the atrioventricular node. The PR segment serves as
the baseline (also referred to as reference line or isoelectric line ) of the ECG curve. The amplitude of
The P-wave vector is slightly curved in the horizontal plane. It is initially directed forward but then turns any deflection/wave is measured by using the PR segment as the baseline.
left to activate the left atrium ( Figure 2 , left-hand side). Lead V1 might therefore display a biphasic
(diphasic) P-wave , meaning that the greater portion of the P-wave is positive but the terminal portion
is slightly negative (the vector generated by left atrial activation heads away from V1). Occasionally, the
negative deflection is also seen in lead V2. lead V5 only notes vectors heading towards the exploring
electrode (albeit with somewhat varying angles) and therefore displays a positive P-wave throughout.
The P-wave, PR interval and PR segment
ECG interpretation traditionally starts with an assessment of the P-wave. The P-wave reflects
atrial depolarization (activation). The PR interval is the distance between the onset of the P-
wave to the onset of the QRS complex. The PR interval is assessed in order to determine whether
impulse conduction from the atria to the ventricles is normal. The flat line between the end of
the P-wave and the onset of the QRS complex is called the PR segment and it reflects the slow
impulse conduction through the atrioventricular node. The PR segment serves as the baseline
(also referred to as reference line or isoelectric line ) of the ECG curve. The amplitude of any
deflection/wave is measured by using the PR segment as the baseline. Refer to Figure 1 .
The QRS complex
The QRS complex represents the depolarization (activation) of the ventricles. It is always
referred to as the “QRS complex” although it may not always display all three waves. Since the
electrical vector generated by the left ventricle is many times larger than the vector generated by
the right ventricle, the QRS complex is actually a reflection of left ventricular depolarization. QRS
duration is the time interval from the onset to the end of the QRS complex. A short QRS complex
is desirable as it proves that the ventricles are depolarized rapidly, which in turn implies that the
conduction system functions properly. Wide (also referred to as broad) QRS complexes indicate
that ventricular depolarization is slow, which may be due to dysfunction in the conduction
system.
The J point and the ST segment
The J point and the ST segment
The ST segment corresponds to the plateau phase (phase 2) of the action potential. The ST
segment must always be studied carefully since it is altered in a wide range of conditions. Many
of these conditions cause rather characteristic ST segment changes. The ST segment is of
particular interest in the setting of acute myocardial ischemia because ischemia causes deviation
of the ST segment ( ST segment deviation ). There are two types of ST segment deviations. ST
segment depression implies that the ST segment is displaced, such that it is below the level of
the PR segment. ST segment elevation implies that the ST segment is displaced, such that it is
above the level of the PR segment. The magnitude of depression/elevation is measured as the
height difference (in millimeters) between the J point and the PR segment. The J point is the
point where the ST segment starts. If the baseline (PR segment) is difficult to discern, the TP
interval may be used as the reference level.
The T-wave
The T-wave reflects the rapid repolarization of contractile cells (phase 3) and T-wave changes
occur in a wide range of conditions. T-wave changes are frequently misunderstood in clinical
practice, which the discussion below will attempt to cure. The transition from the ST segment to
the T-wave should be smooth (and not abrupt). The normal T-wave is slightly asymmetric, with a
steeper downward slope.
The U-wave
The U-wave is seen occasionally. It is a positive wave occurring after the T-wave. Its amplitude is
generally one-fourth of the T-wave’s amplitude. The U-wave is most frequently seen in leads V2–
V4. Individuals with prominent T-waves, as well as those with slow heart rates, display U-waves
more often. The genesis of the U-wave remains elusive.
QT duration and QTc duration
QT duration reflects the total duration of ventricular depolarization and repolarization. It is
measured from the onset of the QRS complex to the end of the T-wave. The QT duration is
inversely related to heart rate; i.e the QT interval increases at slower heart rates and decreases at
higher heart rates. Therefore to determine whether the QT interval is within normal limits, it is
necessary to adjust for the heart rate. The heart rate-adjusted QT interval is referred to as the
corrected QT interval (QTc interval) . A long QTc interval increases the risk of ventricular
arrhythmias.
If an atrium becomes enlarged (typically as a compensatory mechanism) its contribution to the P-wave
will be enhanced. Enlargement of the left and right atria causes typical P-wave changes in lead II and
lead V1 ( Figure 3 ).
Enlargement of the right atrium is commonly a consequence of increased resistance to empty blood
into the right ventricle. This may be due to pulmonary valve stenosis, increased pulmonary artery
pressure etc . The right atrium must then enlarge (hypertrophy) in order to manage to pump blood
into the right ventricle. Right atrial enlargement (hypertrophy) leads to stronger electrical currents and
thus enhancement of the contribution of the right atrium to the P-wave. The P-wave will display higher
amplitude in lead II and lead V1. Such a P-wave is called P pulmonale because pulmonary diseases are
the most common causes ( Figure 3, P-pulmonale ).
If the left atrium encounters increased resistance (e.g due to mitral valve stenosis) it becomes enlarged
(hypertrophy) which amplifies its contribution to the P-wave. The second hump in lead II becomes
larger and the negative deflection in V1 becomes deeper. This is called P mitrale , because mitral valve
disease is a common cause ( Figure 25, P-mitrale ).
If the atria are depolarized by impulses generated by cells outside of the sinoatrial node (i.e by an
ectopic focus), the morphology of the P-wave may differ from the P-waves in sinus rhythm. If the
ectopic focus is located close to the sinoatrial node, the P-wave will have a morphology similar to the P-
wave in sinus rhythm. However, an ectopic focus may be located anywhere. If it is located near the
atrioventricular node, the activation of the atria will proceed in the opposite direction, which produces
an inverted (retrograde) P-wave .
Cardio Page 1
You might also like
- The 12-Lead Electrocardiogram for Nurses and Allied ProfessionalsFrom EverandThe 12-Lead Electrocardiogram for Nurses and Allied ProfessionalsNo ratings yet
- ECG/EKG Interpretation: An Easy Approach to Read a 12-Lead ECG and How to Diagnose and Treat ArrhythmiasFrom EverandECG/EKG Interpretation: An Easy Approach to Read a 12-Lead ECG and How to Diagnose and Treat ArrhythmiasRating: 5 out of 5 stars5/5 (2)
- Cardiologia - EletrocardiografiaDocument40 pagesCardiologia - EletrocardiografiaDANIEL ALEJANDRONo ratings yet
- Ecg 2Document106 pagesEcg 2hammad992No ratings yet
- ECG Interpretation TheoryDocument4 pagesECG Interpretation TheorySteph PiperNo ratings yet
- A Typical ECG Tracing of The Cardiac CycleDocument3 pagesA Typical ECG Tracing of The Cardiac CycleMhiyciel UyNo ratings yet
- Dr. Deep PantDocument39 pagesDr. Deep PantArnav gooswamiNo ratings yet
- 007 - Cardiovascular Physiology) MASTER ECGDocument8 pages007 - Cardiovascular Physiology) MASTER ECGSWATHIKA L100% (1)
- How Procedure Is Performed: ElectrocardiogramDocument10 pagesHow Procedure Is Performed: ElectrocardiogramJonathan AlvarezNo ratings yet
- Electrocardiography (Ii) Morphological Description of The ElectrocardiogramDocument8 pagesElectrocardiography (Ii) Morphological Description of The ElectrocardiogramAisleenHNo ratings yet
- FeatureDocument2 pagesFeatureLilian KrishnaNo ratings yet
- ECG InerpretitionDocument12 pagesECG InerpretitionMended_Heart100% (6)
- Strong's EKG Chamber Enlargement - DraftDocument12 pagesStrong's EKG Chamber Enlargement - DraftMonica GonzalezNo ratings yet
- 2017 - Pocket Guide ECG InterpretationDocument21 pages2017 - Pocket Guide ECG Interpretationmaria0% (1)
- ECG TerminologyDocument66 pagesECG TerminologyblndfflNo ratings yet
- ABC of Clinical Electrocardiography - Introduction. II-Basic Terminology - PMCDocument11 pagesABC of Clinical Electrocardiography - Introduction. II-Basic Terminology - PMCRuban RichardNo ratings yet
- Electrofisiologia Cardiaca Guia Viasual 2 PDFDocument82 pagesElectrofisiologia Cardiaca Guia Viasual 2 PDFMiguel LizarragaNo ratings yet
- Interpretasi ElektrokardiogramDocument36 pagesInterpretasi ElektrokardiogramendahNo ratings yet
- E Lectrocardiography ECG: Practical Physiology 2020-2021 LabDocument8 pagesE Lectrocardiography ECG: Practical Physiology 2020-2021 LabBushra AlkaqaniNo ratings yet
- Aaa Ejempl TraductDocument8 pagesAaa Ejempl TraductJm GamaNo ratings yet
- ECG Normal Values and InterpretationsDocument6 pagesECG Normal Values and InterpretationsAlexandryaHaleNo ratings yet
- Premature Atrial Complexes: Feature Description DurationDocument3 pagesPremature Atrial Complexes: Feature Description DurationRicky Marion ManaloNo ratings yet
- ECG PracticalDocument48 pagesECG PracticalbvkjtzrvnyNo ratings yet
- Nelec 2: Acute and Critical Care Nursing: Unit Learning OutcomeDocument4 pagesNelec 2: Acute and Critical Care Nursing: Unit Learning Outcomeyas minNo ratings yet
- 35 7-PDF EcDocument1 page35 7-PDF EcLwin Maung Maung ThikeNo ratings yet
- 02 - ECG - General Approach and Normal Aspects 2Document18 pages02 - ECG - General Approach and Normal Aspects 2hussain alkhrsanyNo ratings yet
- Basic ECG InterpretationDocument62 pagesBasic ECG Interpretationmohannadalkwiese3No ratings yet
- Significance of The Various Waveforms + Chamber EnlargementDocument45 pagesSignificance of The Various Waveforms + Chamber EnlargementKai Zi (凯)No ratings yet
- General: Determination of Heart Rate and Rhythm Determination of The Heart RateDocument14 pagesGeneral: Determination of Heart Rate and Rhythm Determination of The Heart RatedanradulescuNo ratings yet
- Lab 4 ECG Dan HuynhDocument13 pagesLab 4 ECG Dan Huynhdhdan27No ratings yet
- Batch-7 Bme Fap WordDocument5 pagesBatch-7 Bme Fap Wordofficial6705No ratings yet
- 118 Skills Lab-Week 2-ECG TakingDocument8 pages118 Skills Lab-Week 2-ECG TakingKeisha BartolataNo ratings yet
- Thinking About Ecgs (Garcia)Document9 pagesThinking About Ecgs (Garcia)Filip IonescuNo ratings yet
- Chapter 03Document13 pagesChapter 03matsliuNo ratings yet
- Basic ECG and Arrhythmia FINALDocument16 pagesBasic ECG and Arrhythmia FINALCharlotte James100% (5)
- 26A. ECG tutorial _ Basic principles of ECG analysis - UpToDate_101216Document23 pages26A. ECG tutorial _ Basic principles of ECG analysis - UpToDate_101216johundaphNo ratings yet
- Tugas Ep: Jerry Marisi H MarbunDocument21 pagesTugas Ep: Jerry Marisi H MarbunMaruliNo ratings yet
- Unit 1Document29 pagesUnit 1SasikumarNo ratings yet
- DYSRHYTMIASDocument16 pagesDYSRHYTMIASVictor StevenNo ratings yet
- 01 - Basic Principles of ECG Analysis - UpToDateDocument22 pages01 - Basic Principles of ECG Analysis - UpToDateElmer MoscosoNo ratings yet
- 5hypertrophy and MIDocument116 pages5hypertrophy and MIsamooanatenaNo ratings yet
- Deconstructing The ECG Curve - The Components of The Tracing: Key ConceptsDocument117 pagesDeconstructing The ECG Curve - The Components of The Tracing: Key ConceptsdrynwhylNo ratings yet
- 11 Steps of ECG - Ali Alnahari PDFDocument16 pages11 Steps of ECG - Ali Alnahari PDFBìnhNo ratings yet
- ElectrocardiogramDocument3 pagesElectrocardiogramgaratoh099No ratings yet
- Project 2 Electrocardiography: Practical TasksDocument16 pagesProject 2 Electrocardiography: Practical TasksFahad ShahidNo ratings yet
- EKGDocument11 pagesEKGTivano PaembonanNo ratings yet
- Clinical Demonstration: Topic: Electrocardiogram (ECG)Document24 pagesClinical Demonstration: Topic: Electrocardiogram (ECG)soniya josephNo ratings yet
- Sut Ams Medical College, TVMDocument7 pagesSut Ams Medical College, TVMDIVYA R.S100% (1)
- ECG TutorialDocument40 pagesECG TutorialAnonymous HAbhRTs2TfNo ratings yet
- Arrhythmias: M. Lacombe Mdfmr/Unecom July 22, 2009Document210 pagesArrhythmias: M. Lacombe Mdfmr/Unecom July 22, 2009Kent MaravillosaNo ratings yet
- Basic ECG InterpretationDocument8 pagesBasic ECG Interpretationamesb100% (1)
- EKG Interpretation Lecture 1 - Identifying The Squiggles, Developing A System For ReadingDocument6 pagesEKG Interpretation Lecture 1 - Identifying The Squiggles, Developing A System For Readingkcargen100% (1)
- 23 7-PDF EcDocument1 page23 7-PDF EcLwin Maung Maung ThikeNo ratings yet
- Rhythm 101-The Normal Rhythm - Fact SheetDocument3 pagesRhythm 101-The Normal Rhythm - Fact SheetReza MajidiNo ratings yet
- How To Read EcgDocument3 pagesHow To Read EcgAlloy Trixia BaguioNo ratings yet
- EKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookFrom EverandEKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookNo ratings yet
- Buku FKDocument1 pageBuku FKllocopoloNo ratings yet
- PF EndocrineDocument3 pagesPF EndocrinellocopoloNo ratings yet
- Changes in PregnancyDocument2 pagesChanges in PregnancyllocopoloNo ratings yet
- LantusDocument25 pagesLantusllocopoloNo ratings yet
- Emergencias Neurologicas Durante El EmbarazoDocument22 pagesEmergencias Neurologicas Durante El Embarazodora cuastumalNo ratings yet
- Ms CompreDocument19 pagesMs ComprenokolipNo ratings yet
- Nur 1210 Pedia Module #1 NewbornDocument43 pagesNur 1210 Pedia Module #1 NewbornJohn Raven GenetianoNo ratings yet
- IntralipidDocument3 pagesIntralipidGwyn RosalesNo ratings yet
- Radiology ExamDocument7 pagesRadiology Examayushbhardwaj181820No ratings yet
- Endocrine System NotesDocument8 pagesEndocrine System NotesShiela Mae SagayoNo ratings yet
- Deep Vein Thrombosis Causes and Consequences.4Document4 pagesDeep Vein Thrombosis Causes and Consequences.4zarozeNo ratings yet
- Isnaira A. Imam Bsn-Iii: Betty Neuman Health Care Systems Model (1982, 1989, 1992) Betty NeumanDocument5 pagesIsnaira A. Imam Bsn-Iii: Betty Neuman Health Care Systems Model (1982, 1989, 1992) Betty Neumanisnaira imamNo ratings yet
- Tachdjian 5Document8 pagesTachdjian 5Abrudan GabrielNo ratings yet
- GR 11 Life Sciences CAPS 3 in 1 ExtractsDocument14 pagesGR 11 Life Sciences CAPS 3 in 1 Extractskatlego.moimi05No ratings yet
- Dissertation Kurzendorfer TanjaDocument197 pagesDissertation Kurzendorfer TanjaASIK1144No ratings yet
- Nutritionreviews58 0001Document10 pagesNutritionreviews58 0001tanjossNo ratings yet
- Icd 10 Rajal Poli SarafDocument3 pagesIcd 10 Rajal Poli Sarafgrace efiliaNo ratings yet
- Auscultation of Lung Sounds and MurmursDocument8 pagesAuscultation of Lung Sounds and MurmursKarl RobleNo ratings yet
- Sans TitreDocument17 pagesSans TitrerollinpeguyNo ratings yet
- Full Download PDF of Conn's Current Therapy 2021 1st Edition - Ebook PDF All ChapterDocument69 pagesFull Download PDF of Conn's Current Therapy 2021 1st Edition - Ebook PDF All Chapterpetezadudy100% (5)
- Biomarkers in Progressive Chronic Kidney Disease. Still A Long Way To GoDocument13 pagesBiomarkers in Progressive Chronic Kidney Disease. Still A Long Way To GoconstanzanazarethNo ratings yet
- Mind Map Cardiovascular SystemDocument7 pagesMind Map Cardiovascular SystemaldyNo ratings yet
- Science Form 3 Chapter 2 - Blood Circulation PDFDocument4 pagesScience Form 3 Chapter 2 - Blood Circulation PDFFarah Sofea Razali91% (11)
- Connective Tissues ReviewDocument14 pagesConnective Tissues ReviewAlfonso Rafael AbayaNo ratings yet
- Hypertensive Heart DiseaseDocument33 pagesHypertensive Heart Diseaserini_adriani6817No ratings yet
- Science 9 ReviewerDocument22 pagesScience 9 ReviewerRio OrpianoNo ratings yet
- Management of Hypertensive Crisis (Diskusi RSUD)Document20 pagesManagement of Hypertensive Crisis (Diskusi RSUD)Kia AgusputraNo ratings yet
- Myocardial InfarctionDocument20 pagesMyocardial InfarctionRio Ramon HilarioNo ratings yet
- Dau Mabil Postmortem ExamDocument5 pagesDau Mabil Postmortem ExamAnthony WarrenNo ratings yet
- Macroscopic Diagnostic For Pathoanathomy and Cytopathology ExamDocument21 pagesMacroscopic Diagnostic For Pathoanathomy and Cytopathology Examkapil pancholiNo ratings yet
- SP 16Document1 pageSP 16ray72roNo ratings yet
- Clinical Application of Point of Care Ultrasound Gastric Examination in The Management of An Asa Class 3e Patient A Case ReportDocument4 pagesClinical Application of Point of Care Ultrasound Gastric Examination in The Management of An Asa Class 3e Patient A Case ReportkamounthNo ratings yet
- L9 - Pathogenesis of JaundiceDocument23 pagesL9 - Pathogenesis of JaundicetrcfghNo ratings yet
- Ksellybelly - MSK I Arthritis RheumDocument4 pagesKsellybelly - MSK I Arthritis RheumTricia Kaye IblanNo ratings yet