Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
6 viewsVascular System
Vascular System
Uploaded by
CHRISTINE M. SALIGANThe vascular system consists of two circulatory systems - pulmonary and systemic. It is composed of arteries, veins, capillaries, and lymphatic vessels. Arteries carry oxygenated blood away from the heart while veins carry deoxygenated blood back to the heart. Capillaries allow for the exchange of nutrients and waste. The lymphatic system collects fluid from tissues and returns it to the bloodstream. Assessment of peripheral vascular disease involves evaluating symptoms, blood flow, and imaging arteries and veins.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You might also like
- Anatomy and Physiology Science Olympiad 2024 Cheat SheetDocument3 pagesAnatomy and Physiology Science Olympiad 2024 Cheat Sheetgfzmrtqj54No ratings yet
- Lymphatic System and Immunity - Seeleys - NotesDocument9 pagesLymphatic System and Immunity - Seeleys - NotesLol lol100% (2)
- Saluran Dan Peredaran DarahDocument75 pagesSaluran Dan Peredaran DarahAcecuwa ZaidenNo ratings yet
- 2013 34 216 Shashi Sahai: Pediatrics in ReviewDocument14 pages2013 34 216 Shashi Sahai: Pediatrics in ReviewcarlospinopedNo ratings yet
- Lecture 4 Cardiovascular System 2Document42 pagesLecture 4 Cardiovascular System 2hafiz patahNo ratings yet
- The Mammali An Circulator y SystemDocument21 pagesThe Mammali An Circulator y SystemFern BaldonazaNo ratings yet
- Physics of Blood FlowDocument59 pagesPhysics of Blood FlowsomethingNo ratings yet
- Cardiovascular 3Document71 pagesCardiovascular 3Balkis HumairohNo ratings yet
- Week 14: Peripheral Circulation and RegulationDocument112 pagesWeek 14: Peripheral Circulation and RegulationHuffy PotterNo ratings yet
- 2024-Nursing-Arterial and Venous SystemDocument38 pages2024-Nursing-Arterial and Venous SystemSyed Husnain Ali ShahNo ratings yet
- HemodynamicsDocument40 pagesHemodynamicsBravo HeroNo ratings yet
- Cardiovascular System (Blood Vessels and Circulation) : Roger Joseph II R. Jecino, R.N., M.DDocument53 pagesCardiovascular System (Blood Vessels and Circulation) : Roger Joseph II R. Jecino, R.N., M.DIan MendezNo ratings yet
- Cardiovascular SystemDocument50 pagesCardiovascular SystemMarbahun Jala KharbhihNo ratings yet
- Dr. Aaijaz Ahmed Khan Sr. Lecturer in Anatomy PPSP, UsmDocument38 pagesDr. Aaijaz Ahmed Khan Sr. Lecturer in Anatomy PPSP, UsmeliseudesafateNo ratings yet
- Circulatory SystemDocument30 pagesCirculatory SystemFiraol DiribaNo ratings yet
- Lect 17, Chapter 21 Peripheral Circulation and RegulationDocument69 pagesLect 17, Chapter 21 Peripheral Circulation and RegulationShaker MahmoodNo ratings yet
- Vascular PhysiologyDocument39 pagesVascular Physiologysultan khabeebNo ratings yet
- Blood Vessels: Cardio-Vascular SystemDocument38 pagesBlood Vessels: Cardio-Vascular SystemNermeinKhattabNo ratings yet
- Human Cardiovascular System: Introduction ToDocument76 pagesHuman Cardiovascular System: Introduction ToJunje SemeonNo ratings yet
- Circulation J Pressure J Flow and Resistance of by YasirDocument47 pagesCirculation J Pressure J Flow and Resistance of by Yasiryasir ishaqNo ratings yet
- Blood VesselsDocument48 pagesBlood VesselsGrape JuiceNo ratings yet
- Blood Vessel Heart StructureDocument26 pagesBlood Vessel Heart StructureRiya NarangNo ratings yet
- Arterial, Arteriolar, Capillary, Venous & Lymphatic Circulations Feyitimi AaDocument67 pagesArterial, Arteriolar, Capillary, Venous & Lymphatic Circulations Feyitimi Aaintarebatinya32No ratings yet
- Vascular System: - Arteries Arterioles - Capil ExchDocument35 pagesVascular System: - Arteries Arterioles - Capil ExchMikaelle GasparNo ratings yet
- محاضرة فسلجة 6 رقم 638097619114528622Document26 pagesمحاضرة فسلجة 6 رقم 638097619114528622محمد عليNo ratings yet
- Dynamics of Blood & Lymph FlowDocument35 pagesDynamics of Blood & Lymph FlowVera Arista100% (1)
- Introduction To Circulatory SystemDocument27 pagesIntroduction To Circulatory SystemHinKNo ratings yet
- Vasodilatasi, Vasokontriksi Dan Regulasi Tekanan Darah: DR Tanjung Subrata, MreproDocument43 pagesVasodilatasi, Vasokontriksi Dan Regulasi Tekanan Darah: DR Tanjung Subrata, MreproSeptia AnggaswariNo ratings yet
- Circulatory SystemDocument84 pagesCirculatory SystemAprille CastroNo ratings yet
- (03des) Slide Artery and VenaDocument30 pages(03des) Slide Artery and VenaAbigaleNo ratings yet
- 10) Circulatory SysDocument60 pages10) Circulatory SysyohdeforemostNo ratings yet
- CH 20 NotesDocument26 pagesCH 20 NotesFatimah AlkhafajiNo ratings yet
- The Histology of The Cardiovascular SystemDocument59 pagesThe Histology of The Cardiovascular SystemNifemi BorodeNo ratings yet
- Blood CirculationDocument58 pagesBlood CirculationSabashnee GovenderNo ratings yet
- Micro A - Heart & BV'sDocument85 pagesMicro A - Heart & BV'sarellanokristelleNo ratings yet
- Cardiovascular SystemDocument40 pagesCardiovascular SystemLouise TanNo ratings yet
- Unit 06 Blood VesselsDocument101 pagesUnit 06 Blood VesselsJohnykutty JosephNo ratings yet
- MF-local Circulation 2016Document61 pagesMF-local Circulation 2016OnSolomonNo ratings yet
- Chapter 9Document36 pagesChapter 9HC GamerNo ratings yet
- Blood VesselsDocument13 pagesBlood VesselsRalph Rezin MooreNo ratings yet
- Circulatory System Latest3Document67 pagesCirculatory System Latest3Gosego SepengNo ratings yet
- Cardiac Vascular SystemDocument51 pagesCardiac Vascular SystemYasir Altaf WaniNo ratings yet
- 4mgdskmlswg6dvazveij Signature Poli 150701080131 Lva1 App6892 PDFDocument42 pages4mgdskmlswg6dvazveij Signature Poli 150701080131 Lva1 App6892 PDFsaurabh chaturvediNo ratings yet
- GA&E 7 - Intro To Circulatory SystemDocument66 pagesGA&E 7 - Intro To Circulatory SystemSu ZikaiNo ratings yet
- 2.2 Circulation MNRDocument30 pages2.2 Circulation MNRAnonymous u7cQyr3QYNo ratings yet
- CardioDocument10 pagesCardioMonica SabarreNo ratings yet
- Structure and Functions of The Major Types of Blood VesselsDocument6 pagesStructure and Functions of The Major Types of Blood VesselsCharls DeimoyNo ratings yet
- K.5 CVS-K5 - Dynamics of Blood & Lymph Flow - EditedDocument36 pagesK.5 CVS-K5 - Dynamics of Blood & Lymph Flow - EditedWinson ChitraNo ratings yet
- Blood Pressure.Document49 pagesBlood Pressure.Sally PujaNo ratings yet
- Lecture - Circulatory SystemDocument38 pagesLecture - Circulatory SystemJanith VimukthiNo ratings yet
- Animal Circulatory Systems: Chapter 42 Pp. 867-879Document46 pagesAnimal Circulatory Systems: Chapter 42 Pp. 867-879Dhea Rafsaloka UtomoNo ratings yet
- IB Biology HL: 6.2 The Blood System - Human PhysiologyDocument12 pagesIB Biology HL: 6.2 The Blood System - Human PhysiologypetraNo ratings yet
- Pressure and Flow in Blood VesselsDocument51 pagesPressure and Flow in Blood VesselsDagmawe ZewengelNo ratings yet
- Histology of Circulatory SystemDocument156 pagesHistology of Circulatory SystemErmiyas BeletewNo ratings yet
- Bio Form5 Chapter1 Transport 1-2aDocument11 pagesBio Form5 Chapter1 Transport 1-2aWati WatakNo ratings yet
- Essential Idea: The Blood System Continuously Transports Substances ToDocument55 pagesEssential Idea: The Blood System Continuously Transports Substances Toormatt100% (1)
- Circulatory System PDFDocument5 pagesCirculatory System PDFNibshian Dela RosaNo ratings yet
- Blood Flow, Blood Coagulation and The Control of Blood PressureDocument83 pagesBlood Flow, Blood Coagulation and The Control of Blood Pressurecharuss.394No ratings yet
- Histology of The Circulatory SystemDocument39 pagesHistology of The Circulatory SystemkhyuiiohiohNo ratings yet
- Frog Circulatory SystemDocument43 pagesFrog Circulatory Systembawcock100% (5)
- The Cardiovascular System: Blood VesselsDocument71 pagesThe Cardiovascular System: Blood VesselsAdi ParamarthaNo ratings yet
- Blood VesselsDocument32 pagesBlood Vesselsabdullahwajd530No ratings yet
- Urinary System Test BankDocument30 pagesUrinary System Test BankVinz TombocNo ratings yet
- WEEK 6 LM#2 LymphaticsDocument5 pagesWEEK 6 LM#2 LymphaticsClyde Tan100% (1)
- Exam Questions Pediatric OMF Surgery V Eng 2021-2022 (Repaired)Document53 pagesExam Questions Pediatric OMF Surgery V Eng 2021-2022 (Repaired)Beni KelnerNo ratings yet
- Anatomy Lymphatic SystemDocument46 pagesAnatomy Lymphatic SystemJenise MuLatto Franklin100% (2)
- Test Bank For Medical Terminology An Accelerated Approach by Jones Full DownloadDocument67 pagesTest Bank For Medical Terminology An Accelerated Approach by Jones Full DownloadandrewlopezetosfzigkjNo ratings yet
- Lymphatic System 2Document31 pagesLymphatic System 2cardos cherryNo ratings yet
- Llymphatic SystemDocument14 pagesLlymphatic SystemfauziharunNo ratings yet
- Lymphatic and Endocrine SystemDocument5 pagesLymphatic and Endocrine Systemshanelhello1No ratings yet
- Anatomy of The Lymphatic SystemDocument27 pagesAnatomy of The Lymphatic SystemAntonio Lima Filho100% (2)
- ANP 1105 The Lymphatic SystemDocument23 pagesANP 1105 The Lymphatic SystemMathios TigerosNo ratings yet
- Lymphatic System MCQsDocument3 pagesLymphatic System MCQsNimra80% (10)
- Chang-Ming Huang, Chao-Hui Zheng (Eds.) - Laparoscopic Gastrectomy For Gastric Cancer - Surgical Technique and Lymphadenectomy-Springer Netherlands (2015)Document357 pagesChang-Ming Huang, Chao-Hui Zheng (Eds.) - Laparoscopic Gastrectomy For Gastric Cancer - Surgical Technique and Lymphadenectomy-Springer Netherlands (2015)Jaldo Freire100% (1)
- Fundamentals of Anatomy Physiology 11th Edition Ebook PDFDocument61 pagesFundamentals of Anatomy Physiology 11th Edition Ebook PDFwilliam.dailey153100% (55)
- Lymph Drainage For DetoxificationDocument8 pagesLymph Drainage For DetoxificationJay JonesNo ratings yet
- Sistem LimfatikDocument27 pagesSistem LimfatikVani Taah GNo ratings yet
- Circulatory System HandoutsDocument4 pagesCirculatory System HandoutsCzarae VillanuevaNo ratings yet
- Evolution of The Circulatory SystemDocument47 pagesEvolution of The Circulatory SystemWwwanand111No ratings yet
- Chapter 13 - Blood Vessels and CirculationDocument14 pagesChapter 13 - Blood Vessels and CirculationIrene BuenaNo ratings yet
- Chap13 Lymphatic System PPT LecDocument68 pagesChap13 Lymphatic System PPT LecThea Gornez100% (1)
- Chapter 29 Lymphatic System PDFDocument24 pagesChapter 29 Lymphatic System PDFMACON824No ratings yet
- Anatomical and Physiological Features of The Skin and Subcutaneous Fat in ChildrenDocument12 pagesAnatomical and Physiological Features of The Skin and Subcutaneous Fat in ChildrenOmar DawdiahNo ratings yet
- Department of Education: Republic of The PhilippinesDocument5 pagesDepartment of Education: Republic of The PhilippinesMarc Joseph NillasNo ratings yet
- Wiley LymphaticDocument38 pagesWiley LymphaticphilipNo ratings yet
- Human Anatomy and Physiology Course OutlineDocument16 pagesHuman Anatomy and Physiology Course OutlineDEVORAH CARUZNo ratings yet
- Lymphatic System N Body DefenseDocument23 pagesLymphatic System N Body Defensehafiz amriNo ratings yet
- Tabark Radhi - Benign Breast NeoplasmDocument19 pagesTabark Radhi - Benign Breast NeoplasmAhmed AliNo ratings yet
- Approach To Lymphadenopathy in ChildrenDocument39 pagesApproach To Lymphadenopathy in Childrenmrs raamNo ratings yet
Vascular System
Vascular System
Uploaded by
CHRISTINE M. SALIGAN0 ratings0% found this document useful (0 votes)
6 views34 pagesThe vascular system consists of two circulatory systems - pulmonary and systemic. It is composed of arteries, veins, capillaries, and lymphatic vessels. Arteries carry oxygenated blood away from the heart while veins carry deoxygenated blood back to the heart. Capillaries allow for the exchange of nutrients and waste. The lymphatic system collects fluid from tissues and returns it to the bloodstream. Assessment of peripheral vascular disease involves evaluating symptoms, blood flow, and imaging arteries and veins.
Original Description:
Original Title
VASCULAR-SYSTEM
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe vascular system consists of two circulatory systems - pulmonary and systemic. It is composed of arteries, veins, capillaries, and lymphatic vessels. Arteries carry oxygenated blood away from the heart while veins carry deoxygenated blood back to the heart. Capillaries allow for the exchange of nutrients and waste. The lymphatic system collects fluid from tissues and returns it to the bloodstream. Assessment of peripheral vascular disease involves evaluating symptoms, blood flow, and imaging arteries and veins.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
6 views34 pagesVascular System
Vascular System
Uploaded by
CHRISTINE M. SALIGANThe vascular system consists of two circulatory systems - pulmonary and systemic. It is composed of arteries, veins, capillaries, and lymphatic vessels. Arteries carry oxygenated blood away from the heart while veins carry deoxygenated blood back to the heart. Capillaries allow for the exchange of nutrients and waste. The lymphatic system collects fluid from tissues and returns it to the bloodstream. Assessment of peripheral vascular disease involves evaluating symptoms, blood flow, and imaging arteries and veins.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 34
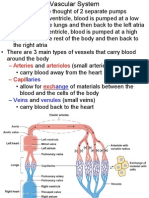
VASCULAR SYSTEM
TWO INTERDEPENDENT SYSTEM
1.Pulmonary circulation
2.Systemic circulation
Vascular system composition:
• Arteries-
• Capillaries
• Arterioles and venules
• Lymphatic vessel
Composition of vascular system
comparison
arteries veins
• Thick walled structure that • Walls o are thin and less
carries oxygenated blood muscular-allowing them to
distend that allows large
from the heart to the blood volume to remain in the
tissues veins under low pressure
• Some vein have valves (lower
extremity)-prevent blood from
seeping backward as it is
propelled toward the heart
• Competency of the valve
depends on the integrity of
the vein wall
arterioles
• small arteries and arterioles have much less
elastic tissue
• Smooth muscles in the media controls the
diameter of the vessel by contracting and
relaxing. ( chemical, neuronal, hormonal
activity of the body)
• Arterioles (resistance vessels)- they offer
resistance to blood flow
arterioles
• Regulate the volume and pressure in the
arterial system and the rate of blood flow to
the capillaries
capillaries
• Walls lack smooth muscle and
adventitia
• Composed of single layer of
endothelial cells
• Thin-walled structure permits
rapid and efficient transport of
nutrients to the cells and
removal of metabolic waste
• Diameter is very small-
• Changes in the capillary
diameter –passive- influenced by
contractile changes in the blood
vessels that carry blood to and
from it.
capillaries
Veins and venule
• Capillaries join to form a larger vessel known
as venules which joins to form veins
Lymphatic vessel
• Are a complex network of thin-walled vessels
similar to the blood capillaries
• Collects lymphatic fluids from tissues and
organs and transports the fluid to the venous
circulation
• Two main structure:
1. Lymphatic duct
2. Thoracic duct
• Peripheral lymphatic vessel joins larger lymph
vessels and pass through regional lymph nodes
before entering the venous circulation
• Lymph nodes filter foreign particles
• Lymphatic vessels are permeable to large
molecules and provides the only means by
which interstitial protein can return to the
venous system
Function of the vascular system
• Circulatory needs of tissue- vessels dilate and
constrict depending on the tissues metabolic
need
• Blood flow
-unidirectional blood flow cause by a pressure
difference that exist bet. The venous and arterial
system
-Arterial pressure= 100mmhg
-Venous pressure =40mmhg
• In long smooth blood vessel- blood flow is
laminar or streamlike- blood in the center of
the vessel moving slightly faster than the blood
near the vessel wall
• Laminar flow becomes turbulent when:
-blood flow rate increases
- Diameter of the vessel becomes greater than
normal
- Segments of the vessel are narrowed or
constricted.
• Turbulent blood flow- bruit
Function of the vascular system
• Capillary filtration and reabsorption-
-fluid exchange in across capillary wall is
continuous( interstitial fluid)
-the equilibrium between hydrostatic forces and
osmotic forces of the blood and interstitium, as
well as capillary permeability, determines the
fluid movement across the capillary
• Hydrostatic pressure- is a driving
pressure that is generated by the
blood pressure
• Osmotic pressure is the pulling
force created by plasma proteins
• Arterial end of the
capillary- high hydrostatic
pressure-drive fluid out
of the capillary and into
the tissue spaces.
-osmotic pressure tends to
pull back the fluid into the
capillary but can’t overcome
the high hydrostatic
pressure
• venous end of the capillary- lower hydrostatic
pressure
-pulling back of fluid into the capillaries by
osmotic pressure
-osmotic forces predominates over the low
hydrostatic pressure
Reabsorption of fluid from the tissue space into
the capillary
• This process help maintains tissue fluid
volume, and removing tissue waste and debris
• Sometimes fluids filtered out greatly exceeds
the amount reabsorbed and carried away by
the lymphatic vessel- due:
✓ Damage to capillary walls-increase
permeability
✓ Obstruction of lymphatic drainage
✓ Elevation of venous pressure
✓ Decrease plasma protein osmotic force
Peripheral vascular regulating mechanism
• Sympathetic ( adrenergic) –innervates all blood
vessels except the capillary and precapillary
sphincter- vasoconstriction (norepinephrine)
• Hormonal substance-
-epinephrine-acts like the nor epinephrine
(vasoconstriction) but low dose cause
vasodilation in skeletal muscles, heart and brain
Angiotensin
• Reduce blood flow through peripheral blood
vessel characterizes all peripheral vascular
disease:
• Pump failure- inadequate peripheral blood
flow
• Alteration in blood and lymphatic vessels-
damage arteries, thromboembolus occluding
the vein, incompetent venous valve, reduction
in the effectiveness of the pumping action of
the surrounding muscles
ASSESSMENT
• Intermittent claudication- muscular, cramp-like pain
in the extremities- peripheral arterial insufficient
• Cool and pale extremities
-rubor-20sec to 2 minutes after extremity is place in
dependent position
-cyanosis
• Reduced nutrient supply to tissues:
-Hair loss
-Brittle nails
-Dry and scaly skin
-Atrophy and
-Ulcerations
• Gangrenous changes- appear after prolonged,
severe ischemia
• Absent pulses
Diagnostic evaluation
• Doppler ultrasound flow studies-hand held
device that emits a continuous signal through
the patients tissues.
-signals are reflected by “echo off” the moving
blood cells and are received by the device
-the filtered-output doppler signal is then
transmitted to a loud speaker or headphones
where it can be heard for interpretation
• Exercise testing- ankle systolic BP is taken-little
or no drop in BP is normal
• Duplex ultrasonography- imaging of the tissue,
organs and blood vessels and permits
estimation of velocity changes by the use of a
pulsed doppler
• Computed tomography-provides images of the
soft tissue and visualize the area of volume
changes to an extremity and the compartment
where changes takes place
• MRI- useful in pts with impaired renal function
• Angiography- arteriogram-to confirm the
diagnosis of occlusive arterial disease. Contrast
agent is injected into the vascular system to
visualize the vessel
• Contrast phlebography- also known as
venography
-injects contrast agent into the venous system to
check for thrombus
-injection of contrast media cause brief pain and
inflammation of the vein
• Lymph angiography- provides a way of
detecting lymph node involvement
- Lymph vessel in each foot is injected with
contrast media, then series of x-rays will be taken
after 24 hours and periodically thereafter
• Lymphoscintigraphy- a radioactively labelled
colloid is injected subcutaneously in the
second interdigital space. The extremity is then
exercised to facilitate uptake of the colloid by
the lymphatic system and serial images are
obtained at preset interval
You might also like
- Anatomy and Physiology Science Olympiad 2024 Cheat SheetDocument3 pagesAnatomy and Physiology Science Olympiad 2024 Cheat Sheetgfzmrtqj54No ratings yet
- Lymphatic System and Immunity - Seeleys - NotesDocument9 pagesLymphatic System and Immunity - Seeleys - NotesLol lol100% (2)
- Saluran Dan Peredaran DarahDocument75 pagesSaluran Dan Peredaran DarahAcecuwa ZaidenNo ratings yet
- 2013 34 216 Shashi Sahai: Pediatrics in ReviewDocument14 pages2013 34 216 Shashi Sahai: Pediatrics in ReviewcarlospinopedNo ratings yet
- Lecture 4 Cardiovascular System 2Document42 pagesLecture 4 Cardiovascular System 2hafiz patahNo ratings yet
- The Mammali An Circulator y SystemDocument21 pagesThe Mammali An Circulator y SystemFern BaldonazaNo ratings yet
- Physics of Blood FlowDocument59 pagesPhysics of Blood FlowsomethingNo ratings yet
- Cardiovascular 3Document71 pagesCardiovascular 3Balkis HumairohNo ratings yet
- Week 14: Peripheral Circulation and RegulationDocument112 pagesWeek 14: Peripheral Circulation and RegulationHuffy PotterNo ratings yet
- 2024-Nursing-Arterial and Venous SystemDocument38 pages2024-Nursing-Arterial and Venous SystemSyed Husnain Ali ShahNo ratings yet
- HemodynamicsDocument40 pagesHemodynamicsBravo HeroNo ratings yet
- Cardiovascular System (Blood Vessels and Circulation) : Roger Joseph II R. Jecino, R.N., M.DDocument53 pagesCardiovascular System (Blood Vessels and Circulation) : Roger Joseph II R. Jecino, R.N., M.DIan MendezNo ratings yet
- Cardiovascular SystemDocument50 pagesCardiovascular SystemMarbahun Jala KharbhihNo ratings yet
- Dr. Aaijaz Ahmed Khan Sr. Lecturer in Anatomy PPSP, UsmDocument38 pagesDr. Aaijaz Ahmed Khan Sr. Lecturer in Anatomy PPSP, UsmeliseudesafateNo ratings yet
- Circulatory SystemDocument30 pagesCirculatory SystemFiraol DiribaNo ratings yet
- Lect 17, Chapter 21 Peripheral Circulation and RegulationDocument69 pagesLect 17, Chapter 21 Peripheral Circulation and RegulationShaker MahmoodNo ratings yet
- Vascular PhysiologyDocument39 pagesVascular Physiologysultan khabeebNo ratings yet
- Blood Vessels: Cardio-Vascular SystemDocument38 pagesBlood Vessels: Cardio-Vascular SystemNermeinKhattabNo ratings yet
- Human Cardiovascular System: Introduction ToDocument76 pagesHuman Cardiovascular System: Introduction ToJunje SemeonNo ratings yet
- Circulation J Pressure J Flow and Resistance of by YasirDocument47 pagesCirculation J Pressure J Flow and Resistance of by Yasiryasir ishaqNo ratings yet
- Blood VesselsDocument48 pagesBlood VesselsGrape JuiceNo ratings yet
- Blood Vessel Heart StructureDocument26 pagesBlood Vessel Heart StructureRiya NarangNo ratings yet
- Arterial, Arteriolar, Capillary, Venous & Lymphatic Circulations Feyitimi AaDocument67 pagesArterial, Arteriolar, Capillary, Venous & Lymphatic Circulations Feyitimi Aaintarebatinya32No ratings yet
- Vascular System: - Arteries Arterioles - Capil ExchDocument35 pagesVascular System: - Arteries Arterioles - Capil ExchMikaelle GasparNo ratings yet
- محاضرة فسلجة 6 رقم 638097619114528622Document26 pagesمحاضرة فسلجة 6 رقم 638097619114528622محمد عليNo ratings yet
- Dynamics of Blood & Lymph FlowDocument35 pagesDynamics of Blood & Lymph FlowVera Arista100% (1)
- Introduction To Circulatory SystemDocument27 pagesIntroduction To Circulatory SystemHinKNo ratings yet
- Vasodilatasi, Vasokontriksi Dan Regulasi Tekanan Darah: DR Tanjung Subrata, MreproDocument43 pagesVasodilatasi, Vasokontriksi Dan Regulasi Tekanan Darah: DR Tanjung Subrata, MreproSeptia AnggaswariNo ratings yet
- Circulatory SystemDocument84 pagesCirculatory SystemAprille CastroNo ratings yet
- (03des) Slide Artery and VenaDocument30 pages(03des) Slide Artery and VenaAbigaleNo ratings yet
- 10) Circulatory SysDocument60 pages10) Circulatory SysyohdeforemostNo ratings yet
- CH 20 NotesDocument26 pagesCH 20 NotesFatimah AlkhafajiNo ratings yet
- The Histology of The Cardiovascular SystemDocument59 pagesThe Histology of The Cardiovascular SystemNifemi BorodeNo ratings yet
- Blood CirculationDocument58 pagesBlood CirculationSabashnee GovenderNo ratings yet
- Micro A - Heart & BV'sDocument85 pagesMicro A - Heart & BV'sarellanokristelleNo ratings yet
- Cardiovascular SystemDocument40 pagesCardiovascular SystemLouise TanNo ratings yet
- Unit 06 Blood VesselsDocument101 pagesUnit 06 Blood VesselsJohnykutty JosephNo ratings yet
- MF-local Circulation 2016Document61 pagesMF-local Circulation 2016OnSolomonNo ratings yet
- Chapter 9Document36 pagesChapter 9HC GamerNo ratings yet
- Blood VesselsDocument13 pagesBlood VesselsRalph Rezin MooreNo ratings yet
- Circulatory System Latest3Document67 pagesCirculatory System Latest3Gosego SepengNo ratings yet
- Cardiac Vascular SystemDocument51 pagesCardiac Vascular SystemYasir Altaf WaniNo ratings yet
- 4mgdskmlswg6dvazveij Signature Poli 150701080131 Lva1 App6892 PDFDocument42 pages4mgdskmlswg6dvazveij Signature Poli 150701080131 Lva1 App6892 PDFsaurabh chaturvediNo ratings yet
- GA&E 7 - Intro To Circulatory SystemDocument66 pagesGA&E 7 - Intro To Circulatory SystemSu ZikaiNo ratings yet
- 2.2 Circulation MNRDocument30 pages2.2 Circulation MNRAnonymous u7cQyr3QYNo ratings yet
- CardioDocument10 pagesCardioMonica SabarreNo ratings yet
- Structure and Functions of The Major Types of Blood VesselsDocument6 pagesStructure and Functions of The Major Types of Blood VesselsCharls DeimoyNo ratings yet
- K.5 CVS-K5 - Dynamics of Blood & Lymph Flow - EditedDocument36 pagesK.5 CVS-K5 - Dynamics of Blood & Lymph Flow - EditedWinson ChitraNo ratings yet
- Blood Pressure.Document49 pagesBlood Pressure.Sally PujaNo ratings yet
- Lecture - Circulatory SystemDocument38 pagesLecture - Circulatory SystemJanith VimukthiNo ratings yet
- Animal Circulatory Systems: Chapter 42 Pp. 867-879Document46 pagesAnimal Circulatory Systems: Chapter 42 Pp. 867-879Dhea Rafsaloka UtomoNo ratings yet
- IB Biology HL: 6.2 The Blood System - Human PhysiologyDocument12 pagesIB Biology HL: 6.2 The Blood System - Human PhysiologypetraNo ratings yet
- Pressure and Flow in Blood VesselsDocument51 pagesPressure and Flow in Blood VesselsDagmawe ZewengelNo ratings yet
- Histology of Circulatory SystemDocument156 pagesHistology of Circulatory SystemErmiyas BeletewNo ratings yet
- Bio Form5 Chapter1 Transport 1-2aDocument11 pagesBio Form5 Chapter1 Transport 1-2aWati WatakNo ratings yet
- Essential Idea: The Blood System Continuously Transports Substances ToDocument55 pagesEssential Idea: The Blood System Continuously Transports Substances Toormatt100% (1)
- Circulatory System PDFDocument5 pagesCirculatory System PDFNibshian Dela RosaNo ratings yet
- Blood Flow, Blood Coagulation and The Control of Blood PressureDocument83 pagesBlood Flow, Blood Coagulation and The Control of Blood Pressurecharuss.394No ratings yet
- Histology of The Circulatory SystemDocument39 pagesHistology of The Circulatory SystemkhyuiiohiohNo ratings yet
- Frog Circulatory SystemDocument43 pagesFrog Circulatory Systembawcock100% (5)
- The Cardiovascular System: Blood VesselsDocument71 pagesThe Cardiovascular System: Blood VesselsAdi ParamarthaNo ratings yet
- Blood VesselsDocument32 pagesBlood Vesselsabdullahwajd530No ratings yet
- Urinary System Test BankDocument30 pagesUrinary System Test BankVinz TombocNo ratings yet
- WEEK 6 LM#2 LymphaticsDocument5 pagesWEEK 6 LM#2 LymphaticsClyde Tan100% (1)
- Exam Questions Pediatric OMF Surgery V Eng 2021-2022 (Repaired)Document53 pagesExam Questions Pediatric OMF Surgery V Eng 2021-2022 (Repaired)Beni KelnerNo ratings yet
- Anatomy Lymphatic SystemDocument46 pagesAnatomy Lymphatic SystemJenise MuLatto Franklin100% (2)
- Test Bank For Medical Terminology An Accelerated Approach by Jones Full DownloadDocument67 pagesTest Bank For Medical Terminology An Accelerated Approach by Jones Full DownloadandrewlopezetosfzigkjNo ratings yet
- Lymphatic System 2Document31 pagesLymphatic System 2cardos cherryNo ratings yet
- Llymphatic SystemDocument14 pagesLlymphatic SystemfauziharunNo ratings yet
- Lymphatic and Endocrine SystemDocument5 pagesLymphatic and Endocrine Systemshanelhello1No ratings yet
- Anatomy of The Lymphatic SystemDocument27 pagesAnatomy of The Lymphatic SystemAntonio Lima Filho100% (2)
- ANP 1105 The Lymphatic SystemDocument23 pagesANP 1105 The Lymphatic SystemMathios TigerosNo ratings yet
- Lymphatic System MCQsDocument3 pagesLymphatic System MCQsNimra80% (10)
- Chang-Ming Huang, Chao-Hui Zheng (Eds.) - Laparoscopic Gastrectomy For Gastric Cancer - Surgical Technique and Lymphadenectomy-Springer Netherlands (2015)Document357 pagesChang-Ming Huang, Chao-Hui Zheng (Eds.) - Laparoscopic Gastrectomy For Gastric Cancer - Surgical Technique and Lymphadenectomy-Springer Netherlands (2015)Jaldo Freire100% (1)
- Fundamentals of Anatomy Physiology 11th Edition Ebook PDFDocument61 pagesFundamentals of Anatomy Physiology 11th Edition Ebook PDFwilliam.dailey153100% (55)
- Lymph Drainage For DetoxificationDocument8 pagesLymph Drainage For DetoxificationJay JonesNo ratings yet
- Sistem LimfatikDocument27 pagesSistem LimfatikVani Taah GNo ratings yet
- Circulatory System HandoutsDocument4 pagesCirculatory System HandoutsCzarae VillanuevaNo ratings yet
- Evolution of The Circulatory SystemDocument47 pagesEvolution of The Circulatory SystemWwwanand111No ratings yet
- Chapter 13 - Blood Vessels and CirculationDocument14 pagesChapter 13 - Blood Vessels and CirculationIrene BuenaNo ratings yet
- Chap13 Lymphatic System PPT LecDocument68 pagesChap13 Lymphatic System PPT LecThea Gornez100% (1)
- Chapter 29 Lymphatic System PDFDocument24 pagesChapter 29 Lymphatic System PDFMACON824No ratings yet
- Anatomical and Physiological Features of The Skin and Subcutaneous Fat in ChildrenDocument12 pagesAnatomical and Physiological Features of The Skin and Subcutaneous Fat in ChildrenOmar DawdiahNo ratings yet
- Department of Education: Republic of The PhilippinesDocument5 pagesDepartment of Education: Republic of The PhilippinesMarc Joseph NillasNo ratings yet
- Wiley LymphaticDocument38 pagesWiley LymphaticphilipNo ratings yet
- Human Anatomy and Physiology Course OutlineDocument16 pagesHuman Anatomy and Physiology Course OutlineDEVORAH CARUZNo ratings yet
- Lymphatic System N Body DefenseDocument23 pagesLymphatic System N Body Defensehafiz amriNo ratings yet
- Tabark Radhi - Benign Breast NeoplasmDocument19 pagesTabark Radhi - Benign Breast NeoplasmAhmed AliNo ratings yet
- Approach To Lymphadenopathy in ChildrenDocument39 pagesApproach To Lymphadenopathy in Childrenmrs raamNo ratings yet