Professional Documents
Culture Documents
CD Hepatitis - Dr. Yapendon 2014
CD Hepatitis - Dr. Yapendon 2014
Uploaded by
jeccomOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
CD Hepatitis - Dr. Yapendon 2014
CD Hepatitis - Dr. Yapendon 2014
Uploaded by
jeccomCopyright:
Available Formats
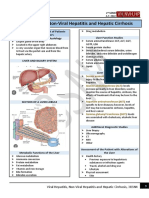
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
HEPATITIS pruritus, pedal edema, esophageal and intestinal varices,
encephalopathy
Injury to the liver characterized by inflammation and impaired liver
function PRESENTATION OF PATIENTS WITH HEPATITIS
Usually caused by viral infection Cirrhotic habitus – Ascites
Other causes are alcohol, drugs, toxin, autoimmune, alpha 1
antitrypsin deficiency, metabolic disorders like Wilson disease,
hemochromatosis, glycogenosis – pwede silang differential
diagnosis ng hepa
HEPATITIS VIRUS
A, B, C, D, E – 95% of viral infection
Enteral (A & E) or parenteral group (B, C, D)
Other causes of viral infection are HS, CMV, EBV, YFV, adenovirus,
mumps virus, rubella virus, rubeola, coxackie B
F(?), G Ascites grading:
Can be acute or chronic hepatitis 1. Mild, only visible on ultrasound
Chronic hepatitis – B, C, D (not seen in A and E) 2. Detectable with flank bulging and shifting dullness
3. Directly visible, confirmed with fluid thrill
Phases of hepatitis:
Incubation phase or period – period between actual infection and Caput medusa
presence of SSx
Preicteric phase – non specific ssx
Icteric phase – icteresia/ jaundice
Convalescent phase
ACUTE VIRAL HEPATITIS
Clinical Characteristics of acute viral infection are the same (all
hepa viruses)
Mild to fulminant
Asymptomatic in younger patients
Initially present as nonspecific flu-like symptoms: fever, N/V, Due to opening of the round ligament secondary to increased
diarrhea, malaise (95%), myalgia, arthralgia, diarrhea not all pressure
these symptoms are present in one patient Esophageal varices
Later present with anorexia, abdominal pain, dark colored urine,
jaundice (33%)
Tender hepatomegaly (10%)
Splenomegaly and lymphadenopathy (5%)
May present as:
1. Subclinical – does not present any ssx, or very minor (loss of
appetite)
2. Anicteric – no jaundice, but with nonspecific ssx, and elevation
of liver enzymes and billirubin
3. Fulminant hepatitis – jaundice, very high liver enzymes,
hepatic encephalopathy, death Icteric sclera
CHRONIC VIRAL HEPATITIS
FOR HEPA B, C AND B&D
Asymptomatic (incidental finding) or mild symptoms some have
return of acute symptoms
Usually discovered by abnormal blood test: abnormal LFT, presence
of relevant serologic markers, viral isolation
May present signs and symptoms of cirrhosis
Loss of weight, abdominal discomfort
May develop to liver tumor/hepatocellular Ca, secondary to
chronic viral hepatitis
6 months and above
Hepatosplenomegaly, ascites, spider nevi, esophageal varices, low
grade fever, weight loss, gynecomastia, easy bruisability, jaundice,
Magno Opere Somnia Dura Page 1 of 13 rye
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
Spider nevi & palmar erythema 3 PATTERNS OF ABNORMAL LIVER FUNCTION TEST
1. Hepatocellular
Inc. serum transaminases (AST,ALT)
2. Cholestatic
Inc. Alkaline phosphatase
Inc. GGT
3. Impaired synthetic function
Inc. protime
Dec. albumin
ALT - primarily found in the liver, indicates liver parenchymal injury
Gynecomastia AST – found in other parts of the body, kidneys, brain, muscles, heart
*mas reliableang ALT/SGPT
*in practice, both are requested
High levels of liver enzymes do not always reveal the degree of
liver inflammation or damage or prognosis
It only measures liver damage at one point in time – di sya
reliable.
AST:ALT Ratio –
o >2.0 – alcoholic hepatitis
o <1.0 – viral hepatitis
Macronodular Cirrhosis (walang picture) - >3mm, caused
by hepatitis & C (most common), but it can also be caused
SERUM TRANSAMINASES
by wilson’s disease, and alpha-1-AT deficiency.
Major elevations (>1000 IU/L)
o Toxic damage
o Acute viral hepatitis
o Autoimmune hepatitis
o Ischemic liver injury
Moderate elevations (100-300 IU/L)
o Alcoholic hepatitis
o NASH
o Autoimmune hepatitis
o Wilson’s disease
Minor elevations (<100 IU/L)
o Chronic hepatitis B&C
o Hemochromatosis
HEPATIC ENCEPHALOPATHY STAGES: o Fatty liver
CHOLESTASIS
Increase in ALKALINE PHOSPHATASE
Most common cause: biliary obstruction
Other causes: stone, tumor, lymph node enlargement
Very high alkaline phosphatase (2000 and above) – consider
hepatic infiltration, with malignancy or granulomatous lesion (TB,
sarcoidosis, etc.
Alkaline phosphatase: not exclusively produced by biliary tree,
SPLEEN meron din sa bones, kidney, intestines and placenta.
“Sugar icing / hyaline perisplenitis”
Itching in absence of jaundice, consider:
EXCESS ESTROGEN Primary biliary cirrhosis (PBC)
- Gynecomastia Primary sclerosing cholangitis (PSC)
- Inc in estradiol – due to increase of peripheral conversion of
androgen to androstinedione and testosterone GAMMA GLUTAMYL TRANSFERASE
- Testicular atrophy if elevated, there is a pathology in the biliary system
- Spider nevi
- Palmar erythema
Magno Opere Somnia Dura Page 2 of 13 rye
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
CHOLESTATIC VARIANT HEPATITIS A HEPATITIS A
Where, Hepa A positive and there is an increase in Alkaline -most common cause of hepatitis worldwide
phosphatase -highly endemic in developing countries
Commonly caused by large duct biliary obstruction -outbreaks of hep A are commonly seen in child care centers, illicit
And is also caused by: drug users, schools especially in the Philippines.
o CBD stone
o Chronic pancreatitis HEPATITIS A Virus
o Pancreatic Ca Non enveloped Single stranded positive-sense linear RNA virus
o Cholangio Ca Picornaviridae family
o PBC Can live outside the body for months in fresh and salt water
o PSC Killed by heat 85 degrees centigrade and chlorinated water
o Intrahepatic cholestasis of sepsis 4 human genotypes that are antigenically closely related
o Drug induced One genotype confers immunity to other genotype
Present in liver, bile, stool and blood- patient is communicable
Liver infiltration can also cause cholestasis – sarcoid, amyloid,
before the onset of symptoms and later part of the disease
granuloma, liver mets
CASE DEFINITION
IMPAIRED LIVER FUNCTION
Discrete symptoms of acute viral infection
Pro time: acute or chronic
Jaundice or increase liver enzymes (ALT & AST) in the serum
Important predictor of outcome
Serologic test positive for HAV IgM – even without signs and
May rise up to >50secs in acute liver failure
symptoms
In cirrhosis, 2-5 secs
Most common cause of viral hepatitis worldwide
>20 secs, poor outcome
Albumin
TRANSMISSION
Measures chronic condition of liver, because albumin has long
half life (20-30 days) hence, not a good indicator of acute liver Person to person transmission through oral-fecal route – usually by
injury close personal contact with an infected household member or
You have to rule out first other non hepatic cause, ex: sexual partner
proteinuria, malutrition Intake of fecal contaminated food and drinks – common source of
Jaundice outbreaks and sporadic cases
Prehepatic Replicates exclusively in the liver, pass thru the biliary tree and
O Inc. In the rate of hemolysis shed in the feces 1-2 weeks before & at least 1 week after the
O Malaria, HUS, sickle cell anemia, thalassemia, G6PD def onset of illness – Period communicability
Hepatic Vertical transmission – rare but documented
O Acute and chronic hepatitis, hepatotoxicity, autoimmune
hepatitis, PATHOPHYSIOLOGY
Post hepatic Ingested virus enters mucosa into the bloodstream infect and
O Obstruction, stones, strictures multiply in the hepatocytes biliary tree feces (1-2 weeks
before, and 1 week after illness)
LABORATORY TEST AND FINDINGS
Elevated liver enzymes ALT AST PATHOLOGY
Elevated bilirubin Liver
Prolonged prothrombin time (decrease in platelets, Inflammation and necrosis
thrombocytopenia) due to increase in production of Increased cellularity at portal areas due to immune response
thrombopoietin
Abnormal imaging: high resolution ultrasound, CT scan, MRI CLINICAL COURSE
Decrease in serum albumin Incubation period 15- 50 days (28-30 days)
Serologic test, PCR, viral isolation Generally associated with abrupt onset of illness and fever for a
few days
As ictericia ensues other symptoms improve and ictericia usually
last for less than 2 weeks
Symptoms usually last for less than 2 months
No chronic case
No reinfection because of HAV IgG which give lifelong immunity
Relapsing or biphasic hepatitis occurs in 1.5 -11.9% (10-15) with an
interval 4-15 weeks. (same as typhoid, may relapse)
The enterohepatic cycling of the virus may contribute in such case
Cholestatic variant occurs 8% of cases characterized by severe
pruritus, diarrhea, weight loss, malabsorption
Magno Opere Somnia Dura Page 3 of 13 rye
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
DIFFERENTIAL DIAGNOSIS It consists of viral envelope and a core particle made of
Gall bladder diseases nucleocapsid protein, polymerase protein and viral genome
Gastroenteritis (circular/partially double stranded)
Drug induced hepa Can survive outside the body for at least 7 days and still be capable
Enteric bacterial infection of infecting
LABORATORY TESTS HBV MUTANT
Inc. AST ALT (4-100x)- peaks 3-10days Mutation in the HbSAg failure to detect and
Inc. serum billirubin – peaks 1-2wks treatment/immunity
Inc. ProTime Diagnostic failure – with Hepa B but has negative screening test
Dec. in albumin
(+) serology (HAV-IgM) disappear 4-6mo TRANSMISSION
Imaging not needed, used to rule out other pathologies Sex with an infected partner
Liver biopsy not indicated Injection drug use that involves sharing needles, syringes or drug-
preparation equipment
TREATMENT Birth to an infected mother
Supportive Contact with blood or open sores of an infected person, contact to
No specific drug therapy intact mucosa, buccal cavity, talsik ng dugo
Resistant to most current antiviral Needle sticks or sharp instrument exposures
Hospitalization – if with consistent vomiting or suspected fulminant Sharing items such as razors or toothbrushes with an infected
hepatitis or with encephalopathy person
PROGNOSIS HIGH RISK INDIVIDUALS
Good prognosis with a case fatality rate of 0.4% IV drug users
Clinical severity is proportional to age MSM
Younger patients have milder clinical form Heterosexual contact with multiple partners
Fulminant hepatitis is rare in hepatitis A Household contact with multiple partners
Persons with hemophilia
PREVENTION Patients/staff in hemodialysis centers
Sanitation Occupational exposure
Active immunization – mainstay Patients receiving immunosuppressants
PEP-HAV immunoglobulin within 2 weeks after exposure is > 85% Infants born on infected mothers
protective Persons with chronic elevations of liver enzymes
For high risk people – MSM, occupational, travel
.02 ml/kg BWT PATHOGENESIS
HAV inactivated vaccine (0-16) Cytotoxic T cells lyse infected hepatocytes, involve CD4 and NK
Cells, and will generate Antibody production.
HEPATITIS B Hepa B does not have cytopathic effect
Can survive outside the body and can be a source of infection until Direct cytopathic effect will show at heavy viral loads
7 days Produce little or no cytopathic effect viral amino acids are
Highly communicable loaded to MHC class I and transported to liver cell surface
May cause hepatocellular Ca recognized and destroyed by virus specific cytotoxic T
lymphocytes viral clearance if failed, will result to chronic
EPIDEMIOLOGY infection activation of crucial host genes that will result to
350 million people are infected with hepatitis B hepatocellular Ca
5% of world population, with chronic Hep B
Genotypes: MOLECULAR PATHOGENESIS
o A & D – predominant in the US and Europe HBV replicates its DNA genome via reverse transcription of
o Asia – Genotype B & C predominates pregenomic RNA
o Genotype B has better prognosis than Genotype C HBV is not generally cytopathic to hepatocytes
If hepB is acquired in the prenatal period, the baby has a high Host immune responses (generally inadequate and/or
chance to develop chronic HepB inappropriate) are responsible for the liver disease of chronic
If 1-5yo, 20-50% hepatitis B
If adults, less than 5% Two therapeutic approaches: (i) direct antiviral agents, (ii) immune
modulation: interferon alpha
HEPATITIS B VIRUS
Double-shelled, 42 nm DNA virus DETERMINANTS OF CHRONIC INFECTION
Hepadnavirus Number of infected cells at time of immune response
8 genotypes (A-H) o HBV cells low self limited
4 serotypes (adr, adw, ayr, ayw) Strength of immune response at time of infection
Magno Opere Somnia Dura Page 4 of 13 rye
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
COVALENTLY CLOSED CIRCULAR DNA (cccDNA) Interpretation unclear; four possibilities:
Partially double stranded viral DNA Resolved infection (most common)
Remains permanently in the nucleus False-positive anti-HBc, thus susceptible
Used as template in producing hepatitis B virus “Low level” chronic infection
Resolving acute infection
EXTRAHEPATIC SITES OF HEPATITIS B
HBe Antigen
Lymph nodes Associated with higher rate of viral replication
Bone marrow Enhance infectivity
Lymphocytes During the natural course it may be cleared with the rise in Anti-
Spleen HBe and associated with dramatic decline in viral replication
Pancreas
These are sites where the virus may hide and may result to
recurrence after liver transplant
SEROLOGIC MARKERS
Hepatitis B surface antigen (HBsAg): a protein on the surface of
HBV; it can be detected in high levels in serum during acute or
chronic HBV
Hepatitis B surface antibody (anti-HBs): indicative of recovery and
immunity from HBV infection. Anti-HBs also develop in a person
who has been successfully vaccinated against hepatitis B.
Total hepatitis B core antibody (anti-HBc): appears at the onset of
symptoms in acute hepatitis B and persists for life. Indicates
previous or ongoing infection with HBV in an undefined time
frame.
IgM antibody to hepatitis B core antigen (IgM anti-HBc): positivity
indicates recent infection with HBV (<6 months). Its presence
indicates acute infection.
Hepatitis B e antigen (HBeAg): a secreted product of the OCCULT HEPATITIS
nucleocapsid gene of the HBV that is found in serum during acute HBV-DNA (+)
and chronic hepatitis B. Indicates that the virus is replicating and HBsAg (-)
the infected person has high levels of HBV. form of chronic hepa B associated with advanced fibrosis and
Hepatitis B e antibody (HBeAb or anti-HBe): produced by the decreased response to interferon
immune system temporarily during acute HBV infection or usually coinfected with hepatitis C
consistently during or after a burst in viral replication. Predictor of discovered in 2002
long-term clearance of HBV in patients undergoing antiviral
therapy and indicates lower levels of HBV. DISEASE PROGRESSION OF HEPATITIS B
HBsAg (-) Susceptible
Anti-HBc (-)
Anti-HBs (-)
HBsAg (-) Immune due to
Anti-HBc (+) natural
Anti-HBs (+) infection
HBsAg (-) Immune due to
Anti-HBc (-) vaccine
Anti-HBs (+)
HBsAg (+) Acute infection
Anti-HBc (+)
IgM anti-HBc(+)
Anti-HBs (-)
HBsAg(+) Chronic infection
Anti-HBc (+)
IgM anti-HBc(-)
Anti-HBs (-)
HBsAg (-)
Anti-HBc (+)
Anti-HBs (-)
Magno Opere Somnia Dura Page 5 of 13 rye
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
ACUTE HEPATITS B TREATMENT
CASE DEFINITION Antivirals are not generally recommended
Clinical case definition: 95% will recover because immune system is fully developed
Discrete onset of symptoms You can also give antivirals if patient has severe course,
Jaundice or elevated serum aminotransferase coagulopathy/bleeding tendency, marked jaundice >1-mg/dL,
Laboratory criteria: severe symptoms >4wks, immunocompromised, if with
AntiHBc positive concomitant Hepatitis C or D, elderly, hepatic encephalopathy
HBsAg positive Drugs: same as chronic hepatitis
Interferon is avoided in acute because it can worsen hepatic
CLINICAL COURSE necroinflammation – because interferon boost local immune
Incubation period – 60-150 days (90) response
Acute infection ranges from asymptomatic/mild disease to rarely When to hospitalize acute hepatitis B patients:
fulminant severe course, coagulopathy/bleeding tendency, marked
Case fatality rate 0.5-1% jaundice >1-mg/dL, severe symptoms >4wks,
Symptoms typically last for weeks (up to 6 months) immunocompromised, if with concomitant Hepatitis C or D,
Clearing of HBsAg within 6 months in most patients elderly, hepatic encephalopathy
If infected in the perinatal period, 90% of cases will progress from changes in sensorium, cannot tolerate oral feeding
acute to chronic hepatitis
If infected at the age of 1-5 years old 25-50% will be chronically CHRONIC HEPATITS B
infected CASE DEFINITION
If infected during adulthood less than 5% will progress to chronic (+) IgG
(95% will recover completely) Clinical case definition:
Approximately 25% of those who become chronically infected Asymptomatic/symptomatic
during childhood and 15% of those who become chronically Abnormal/normal LFT
infected after childhood die prematurely from cirrhosis or liver Laboratory criteria
cancer and the majority remain asymptomatic until onset of Anti-HBc IgM negative
cirrhosis or end-stage liver disease Positive it HBsag or HBeAg or HBV DNA
OR
Positve HBsag or HBV DNA or HBeAg 2x at least 6
months apart
FULMINANT HEPATITIS B
Very high liver enzymes, Jaundice, Hepatic encephalopathy
Massive lysis of infected hepatocytes HBsAg persisted >6mos
Some pt will have negative HbSAg – halos naubos na kaya magiging
false negative pati yung HBV-DNA PHASES OF CHRONIC HEPATITIS B
Immune tolerant
EXTRAHEPATIC MANIFESTATION OF HEPATITIS B o Virus can tolerate immune system because it is not fully
Serum Sickness like syndrome developed
o Immune complex reaction o Minimal hepatitis
o Deposition of HbsAg and Ab in tissue and blood vessel leading to o + HBV DNA, HBsAg, HBeAg
a complement reaction Immune clearance
Glomerulonephritis o Competent immune system, virus clear
Polyarteritis nodosa o Antibody response – enzymes elevated due to activation of
Essential mixed cryglobulinemia immune response, more inflammation
(pakibasa na lang daw yung manifestations nila) o Dec. or fluctuation of HBV DNA
Magno Opere Somnia Dura Page 6 of 13 rye
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
Immune inactive phase Recommendations: Whom to Treat (AASLD Guidelines 2007)
o Down immune system, patient serves as carrier Treatment indicated for “active” disease
o Subside liver inflammation, decrease liver enzymes ALT > 2 ULN
Reactivation of Active phase HBV DNA > 20,000 IU/ml
o Elevation of liver enzyme OR IF
o HBV DNA inc or fluctuate ALT 1-2 ULN and > age 40, consider biopsy and treat if
significant fibrosis or necroinflammation is present
FACTORS ASSOCIATED WITH DISEASE PROGRESSION
TREATMENT OPTIONS
Supportive
Interferon
AASLGD GUIDELINES: PERIODIC SCREENING FOR HCC o Interferon alpha 2b
At risk hepatitis B carriers o Pegylated interferon alpha 2a – once a week
Asian males > 40 years of age Nucleoside/nucleotide analog – NRTI
Asian females > 50 years of age o Lamivudine
All cirrhotic hepatitis B carriers o Adefovir
Family history of hepatocellular carcinoma o Entecavir
Africans > 20 years of age o Tenofovir
Those with high HBV DNA levels and those with o Telbivudine
ongoing hepatic inflammatory activity remain at o New – emtricitabine, clevudine
risk for hepatocellular carcinoma (HCC) Combination-NRTI+interferon
Liver ultrasound every 6 to 12 months Fulminant – ICU care
Liver transplant
TO IMPROVE QUALITY OF LIFE OF PATIENTS WITH CHB
Serovonversion of HBs to Anti HBs WHY CONSIDER COMBINATION THERAPY?
Long term suppression of viral production Sequential monotherapy with nucleoside/tide analogs has led to
o cHB patients – eradication of virus is not possible because of HBV resistance
presence of cccDNA persistence of production mechanism There may be special populations in whom combination is
recommended:
TREATMENT ENDPOINTS Cirrhotics in whom development of resistance may have
irreversible severe consequences
Sustain suppression of HBV replication indicated by: loss of HBsAg
HIV/HBV coinfected
& HBeAg, decrease in HBV DNA
Changing to another nucleoside/tide after failure increases chance
Remission of disease indicated by: normal ALT, improvement of
of poor or nonresponse and of resistance to next drug, (ex. ETV)
liver histology
Multidrug-resistant mutants described after sequential
monotherapy
TREATMENT Resistance has been low with combination therapy
Chronic HBV is a dynamic disease May lead to better long-term outcomes
Regular monitoring needed to determine timing of treatment At present no FDA-approved indications for use of combination
and other interventions therapy in patients with chronic HBV infection and no synergy in
Primary determinant of treatment initiation are HBV DNA decline noted
HBV DNA level > 20,00 IU/ml Use in cirrhotic patients especially those with preexisting YMDD
ALT level > 2 ULN mutations and in HIV/HBV patients appears warranted
+Histological finding severity of disease
Assessment of histology is most helpful in borderline ALT and HBV
DNA cases
Cirrhotics: lower thresholds to treat
Magno Opere Somnia Dura Page 7 of 13 rye
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
HBV THERAPY
HBV replication is closely linked to the lifetime risk of disease
outcomes (HCC, ESLD)
New treatment paradigm = long-term control of HBV replication:
↓ Hepatic inflammation and fibrosis
↓ risk of hepatic decompensation and/or HCC
First-line therapy – high potency/low resistance
Peg-IFN
Tenofovir
Entecavir
Combination antiviral therapy?
Type 1 Interferon
Achieve their potent antiviral effects through the regulation of
hundreds of IFN-stimulated genes (ISGs)
ISG encoded proteins establish a general antiviral state within the
cell
LIVER DECOMPENSATION
Peg-IFN for Chronic HEPATITIS B Abnormal clearance of proteins absorbed through the intestinal
Finite duration tract, leading to ammonia retention and hepatic encephalopathy
No resistance Abnormal excretion, leading to an accumulation of bilirubin in the
Higher rates of seroconversion blood, producing jaundice
Poor tolerance Ascites: increased sinusoidal pressure, as with severe inflammation
SQ injection or scarring of the liver, leads to fluid accumulation in the abdomen
High ALT activity that becomes more difficult to control with progressive liver
Low baseline serum HBV DNA concentration decompensation
Genotype A or B Portal hypertension: scarred liver tissue acts as a barrier to blood
Absence of comorbidities flow and causes increased portal blood pressure. A major
No cirrhosis consequence is the rapture of esophageal varices, causing massive
No decompensated liver disease and potentially fatal bleeding.
MANAGEMENT OF CHRONIC HBV INFECTION CLINICAL CONSEQUENCES OF DRUG RESISTANT HBV
Flares in serum ALT
Reduced HBeAg seroconversion
Histological progression of liver disease
Increased recurrence post-OLT
Changes in HBsAg envelope antigenicity
Transmission of drug resistant HBV
POPULATIONS WITH INCREASED RISK OF BECOMING INFECTED
WITH HBV
Infants born to infected mothers
Sex partners of infected persons
Sexually active persons who are not in a long-term, mutually
monogamous relationship (ex. > 1 sexual partner during the
previous 6 months)
Men who have sex with men
Injection drug users
Magno Opere Somnia Dura Page 8 of 13 rye
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
MANAGING RESPONSE IN THE TREATMENT OF CHB DELTA HEPATITIS AGENT
HEPATITIS D – HDV
Small circular defective RNA virus that requires HBsAg for
structural integrity
Enveloped hybrid particle w/ HBsAg coat and HDV core
Propagate only in the presence of HBV
EPIDEMIOLOGY
Worldwide distribution
With 3 epidemiologic pattern
Nonendemic:
o USA & northern Europe
o Percutaneous exposure to blood and blood products
Endemic
o Southern Europe, Northern Africa, Middle east
o Non-percutaneous ex close contact
TRANSMISSION
Percutaneous exposure to blood
PREVENTION o E.g: injection drug usage
Sexual transmission
Vaccination – pre-exposure
o Much less efficient than for HBV
Sanitation - use 1:10 dilution of household bleach (chlorine) w/
Perinatal transmission is rare
water to disinfect spilled fresh or even dried blood and other
contaminated body fluids. Incubation period 30-180d (60-90)
Acute
Used of disposable cutting or pricking instrument and dispose them
o Onset is insidious or acute
properly
Proper disinfection of non disposable hospital instrument Chronic
o Common in HDV
Strict compliance to standard precaution by health workers
Pre-exposure of vaccination (CDC 2006) CLINICAL SITUATION
0, 1 & 6 mos * intramuscular-deltoid Co-infection
0, 1 & 4 mos o Simultaneous infection w/ HBV and HDV
0, 2, & 4 mos Super-infection
0, 1, 2, 12 mos o HDV infection occurs in an already HBV infected patient
CO-INFECTION
Persons who are HBsAg-positive should: Severe acute hepatitis w/ high mortality > than HBV alone
Have their sexual contacts vaccinated Rarely result in chronic infection than HBV infection alone
Use barrier protection during sexual intercourse if partner is not Both anti-HDV IgM and IgG are detectable plus markers of active
vaccinated or naturally immune infection
SUPERINFECTION
Don’t share toothbrushes or razors
Cover open cuts and scratches Present as severe acute hepatitis in a previously asymptomatic hep
Clean blood spills w/ detergent or bleach B
Don’t donate blood, organ or sperms Results in chronic HDV infection (the rule)
>risk for cirrhosis and hepatocellular carcinoma compared to
Post exposure prophylaxis for Hepatitis B persons infected w/ HBV alone
<7 days for needlestick exposure Both anti-HDV IgM & IgG remain detectable plus HBV markers of
active infection
<14 days for sexual exposure
DIAGNOSIS
Post exposure prophylaxis w/ non occupational exposure
HB vaccine + HBIG HBsAg (+) source Anti-HDV
o During acute HDV infection anti-HDV igM predominates and
HBIG alone
detected 30-40days after the s/s
NAT-HDV RNA (PRC)
HB vaccine alone Unknown HBsAg
HBV/HDV
status
o Co-infection: IgM anti –HBC + anti HDV
o Superinfection: HBsAg & anti-HBC IgG+ anti-HDV
Post exposure prophylaxis for health care personnel
HBIG 0.06ml/kg IM asap (w/in 7days) + HB vaccine at different site
If vaccine is not started, repeat HBIG 1 month after
Magno Opere Somnia Dura Page 9 of 13 rye
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
PROGNOSIS CHRONIC HEPATITIS C
Good for acute infection Majority are asymptomatic or with mild nonspecific, intermittent
o Fulminant in 5% symptoms
o Fatigue
Poor for chronic infection o Mild right upper arm discomfort or tenderness (“liver pain”)
o Fulminant in 20% o Nausea
HDV + HBV infection has the highest mortality rate among the viral o Poor appetite
hepatitis o Muscle and joint pain
HDV + HBV has the greater chance of cirrhosis, liver
decompensation & HCC than HBV alone Clinical presentation of Chronic HCV
P.E is likely to be normal or show only mild enlargement of the liver
TREATMENT or tenderness
Some patient have vascular spider or palmar erythema
Supportive
ICU care for fulminant hepatitis
Extrahepatic Manifestation (1-2%)
Liver transplant
Cryoglobulinemia
Experimental: interferon & antiviral
o Skin rashes: purpura, vasculitis, urticaria
o Joint & muscle aches
PREVENTION o Kidney dse
HBV immunization o Neuropathy
o Cryoglobulins, rheumatoid factor & low-
HEPATITIS C complement levels in serum
Glomerulonephritis
Single-strand, positive sense RNA virus
Porphyria cutanea tarda
Genus hepacivirus
6 genotype (1-6) w/ >50 subtypes*
OUTCOME OF CHRONIC HCV
Family Flaviridae
Does not replicate via a DNA intermediate thus does not integrate 80% will develop mild scarring/cirrhosis or experience fatigue or
in the host genome depression
High mutation rate: interferes w/ effective humoral immunity 20-30% will develop sever scarring/cirrhosis
Does not induce lasting immunity 1-5% of those w/ cirrhosis will develop cancer
o Neutralizing antibody are short live 30% of those w/ cirrhosis are also at risk of hepatic
decompensation over 10 yrs
EPIDEMIOLOGY
Leading inindication for liver transplantation in the US ACCELERATED PROGRESSION TO CIRRHOSIS
180 million people are infected worldwide Older age
Mortality related to HCV infection will continue to increase over Obese
the next 2 decades Immunosuppresed (e.g: HIV co-infection)
o Liver failure Consumption of >50g of alcohol per day
o Hepatocellular carcinoma (HCC) “The optimal approach to detecting HCV infection is to screen
persons for history of risk of exposure to the virus and to test selected
TRANSMISSION individuals who have an identifiable risk factor”
Blood transfusion
Injection: drug use (sharing of needles) PATIENTS FOR HCV SCREENING
o Accident needle prick (2%risk)/razor
Persons who have injected illicit drugs in recent and remote past,
Hemodialysis
including those who injected only once and do not consider
Birth to an HCV positive mother (uncommon: 6%)
themselves to be drug users
High risk of sexual practice
Persons w/ conditions assoc w/ a high prevalence of HCV infection
including
ACUTE HEPATITIS C o Persons with HIV infection
Incubation period: 50-160d(50) o Persons w/ hemophilia who received clotting factor
Onset is insidious concentrates prior to 1987
Fulminant hepatitis is uncommon (0.1%) Persons who have ever been on hemodialysis
Progression to chronic is common (50-70%) 55-85% Persons w/ unexplained abnormal aminotranferase levels
Spontaneous resolution is common among infected infants and Prior recipients of transfusion or organ transplants prior to July
young women than among persons who are older when they 1992
develop acute hepatitis Children born to HCV-infected mother
Health care, emergency medical & public safety workers after a
needlestick injury or mucosal exposure to HCV-positive blood
Current sexual partners of HCV-infected persons
Magno Opere Somnia Dura Page 10 of 13 rye
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
Multiple sex partners EIA Anti-HCV (+), HCV RNA (-) RIBA (-)
o False positive
DIAGNOSIS o Recovery from hepatitis C
o Continued virus infection w/ levels of virus too low to be
HCV RNA is detectable w/in days to 8 weeks after infection
detected
o Titer fluctuates and maybe negative intermittently
Liver enzymes become elevated 6-12 wks after infection
TREATMENT
Anti-HCV become positive as early as 8 wks
5-10% of acute cases will have negative anti-HCV while >95% of Goal: prevent complications & death
chronic cases will be positive Drugs
Anti-HCV o Type 1 IFN (interferon) + Antiviral (rivabirin)
o Does not distinguish chronically infected and those cleared of HCV genotyping
infection o Should be performed prior to interferon-based treatment
Acute or Chronic??? Dosage & duration depends on the
o Difficult because anti-HCV and HCV RNA are present in both genotype
Negative Predictions of Response to Pegylated interferon &
LABORATORY TEST Ribavirin Therapy for Hepatitis C
Patient related factors Dse/viral-related factors
Serologic assays: detect specific antibody to hepatitis C virus (anti-
HCV) Non-white ethnicity HCV genotype 1
Molecular assays: detect viral nucleic acid High BMI Advanced fibrosis (stages 3-4)
Age over 40 yrs High baseline viral load (>/= 400,000
or >/= 600,000 IU/mL
Laboratory test
Male sex Steatosis on liver biopsy
EIA
Metabolic syndrome HCV/HIV co-infection
RIBA
Diabetes
NAT-qualitative and quantitative
Viral genotype
Use to guide treatment dose & duration TREATMENT RESPONSE FOR HCV
ALT-serial Defined by surrogate virological parameter rather than a clinical
Liver biopsy endpoint
Hepatitis B, D, HIV testing Short-term outcomes can be measured biochemically
o Normalization of serum ALT levels
EIA-enzyme immunosorbent assay
Virologic response
Detect antibody to core and structural gene of HCV
3
rd
generation EIA is 99% sensitive and specific in Absence of HCV RNA ffrom serum by sensitive PCR based assay
immunocompetent
Hemodialysis and immunodeficient patients rarely have false Histologic response
negative result 2 point improvement necroinflammatory score w/ no worsening in
Autoimmune disorder may have false positive result fibrosis score
RIBA-recombinant immunoblot assay Virologic response
Supplemental test w/ high specificity RVR (@ 4 wks)
Detect anti-HCV using HCV recombinant antigens & synthetic EVR (@ 12 wks)
peptide SVR (@6 mos)
Use in patients w/ positive EIA but negative for HCV RNA SVR: sustain viral response
NAT: HCV RNA Testing should be performed in Loss of detectable HCV RNA during treatment (<50 IU/mL) & its
Patients with a positive anti-HCV test continued absence for at least 6 months after stopping therapy
Patient for whom antiviral treatment is being considered, using a SVR is durable in 95% of patient
sensitive quantitative assay Probability of an SVR strongly depends on the early response to
Patient with unexplained liver dse whose anti-HCV test is negative treatment (EVR)
and who are immunocompromised or suspected of having acute
HCV infection EVR: early viral response
Defined as a declined of viral load by 2 log 10 after 12 wks (3mos)
INTERPRETATION OF TEST of therapy
Anti-HCV (+) HCV RNA (+) o Complete
o Acute or chronic o Partial
Anti-HCV (-) HCV RNA (+) Patients with an EVR have good chance of being cured, w/ 65% of
o Acute HCV them achieving SVR
o Chronic HCV in immunosuppressed
Anti-HCV (-) HCV RNA (-)
o Absence of HCV infection
Magno Opere Somnia Dura Page 11 of 13 rye
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
RVR: rapid viral response Ribavirin
Defined as serum HCV RNA undetectable after 4 wks (1mo) of Synthetic nucleoside analogue
treatment Monotherapy is not effective against CHC
Over 85% of w/ RVR will achieve SVR With pegylated interferon it helps stop making new HCV copies
Only <20% of patients w/ genotype 1 have RVR
60% of patients with genotype 2 and 3 show RVR Ribavirin Side effects
Anemia (hemolytic)
Treatment w/ peginterferon alfa 2a+ribavirin Fatigue and irritability
SVR is seen in 40-80% Itching
o SVR in genotype 2 & 3 is 80% Skin rash
o SVR in genotype 1 is 40% Nasal stuffiness, sinusitis, and cough
EVR
RVR During Therapy
Do CBC & liver enzymes
Before start therapy o At wk 1,2 & 4 and @ 4-8 wk intervals thereafter
Do a liver biopsy Reduce ribavirin (by 200mg @ a time)
Test for serum HCV RNA o If anemia occurs (hemoglobin less than 10g/dL or hematocrit
Test for HCV genotype (or serotype) <30%)
Measure blood counts and aminotransferase STOP ribavirin
Counsel the patient about the relative risks and benefits of o If severe anemia occurs (hemoglobin <8.5g/dL or hematocrit
treatment <26%)
DOSAGE Reduce peginterferon if there are intolerable side effects:
Genotype Peginterferon Ribavirin tabs Duration o Severer fatigue, depression, or irritability or
alfa 2a dose dose o Decrease in WBC (absolute neutrophil count below
Genotype 1,4 180 mcg <75kg=1000mg 48 wks 500cells/mm3) or
>75kg=1200mg 48 wks o Decrease platelet counts (dec below 30,000 cells/mm3)
With genotype 1, measure HCV RNA levels before therapy & again
Genotype 2,3 180 mcg 800 mg 24 wks
@ wk 12
o Stopped early if HCV RNA levels have not decreased by at least
Response to Definition SVR Duration of 2 log10 units
tx therapy (wks) o In situation where HCV RNA levels have not obtainable, repeat
Genotype 1 testing for HCV RNA by PCR (or TMA) should be done @ 24
RVR HCV RNA (-) @ tx wk 4 90% 24* - 48 wks and the therapy stopped if HCV RNA is still present, as a
cEVR HCV RNA (+) @ tx wk 70-80% 48 sustained response is unlikely
4 but HCV RNA Reinforce the need to practice strict birth control during therapy
negative @ tx wk 12 and for 6 mos thereafter
pEVR ≥2log decline in viral <30% Extend to 72
load from baseline but After Therapy
detectable viruse @ tx
Measure the liver enzymes every 2 mos for 6 mos
wk 12 & HCV RNA (-)
6 mos after stopping therapy, test for HCV RNA by PCR (or TMA)
by wk 21 (slow
If HCV RNA is still negative, the excellent for a long-term “cure” is
responder)
excellent
Nonresponse <2log decline in viral <2% Discontinue
o Relapse have rarely been reported after this point
load from baseline @
tx wk 12 or detectable
Future in treatment
virus @ tx wk 24
Studies are ongoing because the standard tx w/c is ribavirin +
interferon achieve only 40-50% chance of viral suppression
Interferon common side effects
New drugs
Fatigue Protease inhibitors: telaprevir & boceprevir
muscle aches
headache
Prognosis in HCV-HIV co-infection
nausea and vomiting
Spontaneous viral clearance < than mono infection
skin irritation at injection ste
More will develop fibrosis
low-grade fever
More than 2x the chance of developing cirrhosis & in a shorter
weight loss
period (10 yrs)
irritability
Greater chance of developing cancer
depression
6x the risk of liver decompensation
mild bone marrow suppression
hair loss (reversible)
Magno Opere Somnia Dura Page 12 of 13 rye
HEPATITIS 2014 -2015
Dr. Yapendon Communicable Diseases
Prevention
Avoid situations in w/c others will be exposed to patients blood
o Do not donate blood, body organs, other tissue or semen
o Do not share toothbrushes, dental appliances, razors, home
therapy items that might have blood on them
No pre-exposure and post exposure immunization or antiviral drug
is currently recommended
Feature HAV HBV HCV HDV HEV
Incubation (days) 15-45, mean 30 30-180, mean 60- 15-160, mean 50 30-180, mean 60- 14-60, mean 40
90 90
Onset Acute Insidious or acute Insidious Insidious or acute Acute
Age preference Children, young Young adults Any age but more Any age (similar Young adults (20-
adult (sexual & common in adults to HBV) 40 yrs)
percutaneous),
babies, toddlers
Transmission
Fecal-oral +++ - - - +++
Percutaneous Unusual +++ +++ +++ -
Perinatal - +++ + + -
Magno Opere Somnia Dura Page 13 of 13 rye
You might also like
- Acute Liver Failure Group 3Document16 pagesAcute Liver Failure Group 31S VILLEGAS GabrielNo ratings yet
- Liver - Dr. Allam 2021 PDFDocument70 pagesLiver - Dr. Allam 2021 PDFMohammedNo ratings yet
- Arcipe Iccu Case 5Document98 pagesArcipe Iccu Case 5Maria Charis Anne Indanan100% (1)
- 9a Pathology PDFDocument47 pages9a Pathology PDFDianne GalangNo ratings yet
- Approach To Elevated LFTDocument42 pagesApproach To Elevated LFTAnant PachisiaNo ratings yet
- Validation & Interpretation of Hepatitis Testing Results MF18092022Document90 pagesValidation & Interpretation of Hepatitis Testing Results MF18092022Laila NihayaNo ratings yet
- Hepatobiliary Disorders: Katrina Saludar Jimenez, R. NDocument42 pagesHepatobiliary Disorders: Katrina Saludar Jimenez, R. NKatrinaJimenezNo ratings yet
- Hepatobiliary Disorders: Katrina Saludar Jimenez, R. NDocument42 pagesHepatobiliary Disorders: Katrina Saludar Jimenez, R. NreykatNo ratings yet
- Pathophysiology: Adobe Stock, Licensed To Teachmeseries LTDDocument6 pagesPathophysiology: Adobe Stock, Licensed To Teachmeseries LTDNestaNo ratings yet
- Chronic Liver Disease (Tutorial)Document44 pagesChronic Liver Disease (Tutorial)Hannah HalimNo ratings yet
- Alcoholism and HepatitisDocument15 pagesAlcoholism and HepatitisTom MallinsonNo ratings yet
- Harriet Lane Handbook 21st Ed 2018-401-600Document200 pagesHarriet Lane Handbook 21st Ed 2018-401-600nguyễn vjNo ratings yet
- Hepatic AbscessesDocument6 pagesHepatic Abscessesmohamed mowafeyNo ratings yet
- Slides DR Ashgar Approach To LFTs 12.12.2021Document47 pagesSlides DR Ashgar Approach To LFTs 12.12.2021Maryam OmarNo ratings yet
- Dr. Brendalyn A. Gallebo Department of Histopath and LaboratoriesDocument216 pagesDr. Brendalyn A. Gallebo Department of Histopath and LaboratoriesFelyne Angelique C. GanoticeNo ratings yet
- Interpreting Liver Function TestsDocument1 pageInterpreting Liver Function TestskarenmstamNo ratings yet
- Revision Notes Dr. A. MowafyDocument222 pagesRevision Notes Dr. A. MowafyMohammed RisqNo ratings yet
- Viral HepatitisDocument7 pagesViral Hepatitisadrian kristopher dela cruzNo ratings yet
- Jaundice: Seminar Under The Guidance Of-Dr. Shiva NarangDocument47 pagesJaundice: Seminar Under The Guidance Of-Dr. Shiva NarangMiguel MansillaNo ratings yet
- Abdominal PainDocument86 pagesAbdominal PainThitanun TungchutworakulNo ratings yet
- Jaundice 160318164012Document47 pagesJaundice 160318164012Ritik MishraNo ratings yet
- RNA VirusesDocument11 pagesRNA VirusesKate Alyssa CatonNo ratings yet
- JaundiceDocument47 pagesJaundiceShiv PatelNo ratings yet
- Type of Enzyme Location of The E Normal Value Abnorma L Values InterpretationDocument4 pagesType of Enzyme Location of The E Normal Value Abnorma L Values InterpretationvisiniNo ratings yet
- 0304 ConsultantoncallDocument4 pages0304 Consultantoncallnessimmounir1173No ratings yet
- Cpliver 1Document4 pagesCpliver 1isahNo ratings yet
- Drugstudy 2Document5 pagesDrugstudy 2Westley RubinoNo ratings yet
- 2 Approach To Elevated LFTDocument59 pages2 Approach To Elevated LFTparik2321No ratings yet
- Medical School GI Notes 2Document71 pagesMedical School GI Notes 2cusom34No ratings yet
- CH 49 MedsurgDocument18 pagesCH 49 MedsurgJiezl Abellano AfinidadNo ratings yet
- Pathologi Klinik Edited by MememeDocument11 pagesPathologi Klinik Edited by MememeReynaldi FernandesNo ratings yet
- 431 2023 Article 4825Document9 pages431 2023 Article 4825Rizqan Fahlevvi AkbarNo ratings yet
- Review: Liver Dysfunction in Critical IllnessDocument17 pagesReview: Liver Dysfunction in Critical IllnessRoger Ludeña SalazarNo ratings yet
- BethametasoneDocument3 pagesBethametasoneWestley RubinoNo ratings yet
- Ikd 10 Case 2Document11 pagesIkd 10 Case 2Senggol NgekNo ratings yet
- Parameter 1 2 3: Serum Bilirubin Serum Albumin Prothrombin Time Ascites Hepatic EncelopathyDocument3 pagesParameter 1 2 3: Serum Bilirubin Serum Albumin Prothrombin Time Ascites Hepatic EncelopathyFirst LastNo ratings yet
- 1-4-3 Liver Cirrhosis - Group 3Document35 pages1-4-3 Liver Cirrhosis - Group 3Maica LectanaNo ratings yet
- Patho - Hepatobiliary System AtfDocument21 pagesPatho - Hepatobiliary System AtfGaurav ThapaNo ratings yet
- What? Who?: DR - Mabel Sihombing Sppd-Kgeh DR - Ilhamd SPPD Dpertemen Ilmu Penyakit Dalam Rs - Ham/Fk-Usu MedanDocument45 pagesWhat? Who?: DR - Mabel Sihombing Sppd-Kgeh DR - Ilhamd SPPD Dpertemen Ilmu Penyakit Dalam Rs - Ham/Fk-Usu MedanM Rizky Assilmy LubisNo ratings yet
- AMC MCQ Dermatology NotesDocument25 pagesAMC MCQ Dermatology NotesJenny FuNo ratings yet
- Organ Function Test: Assessment of Functions of The OrgansDocument39 pagesOrgan Function Test: Assessment of Functions of The OrgansSri Abinash MishraNo ratings yet
- Chronic Liver DiseaseDocument3 pagesChronic Liver DiseaseNikey LimNo ratings yet
- Nephrology: I. ProteinuriaDocument7 pagesNephrology: I. ProteinuriaBenjamin NgNo ratings yet
- How To Work-Up A Patient With JaundiceDocument6 pagesHow To Work-Up A Patient With JaundiceTatum CheneyNo ratings yet
- Drug StudyDocument2 pagesDrug StudyJIREH MAE NOTARTENo ratings yet
- Lecture 01 Hemorrh-Diat KaplanDocument53 pagesLecture 01 Hemorrh-Diat KaplanАбдул Насер МохаммадізмаелNo ratings yet
- Autoimmune HepatitisDocument41 pagesAutoimmune HepatitisMigi Pradysta100% (1)
- Hari-3 - 02 - Dr. Alindina - Demam TifoidDocument33 pagesHari-3 - 02 - Dr. Alindina - Demam TifoidmodrsbmNo ratings yet
- Drug Study For HepatitisDocument4 pagesDrug Study For Hepatitisunyokies100% (1)
- Interpretation of Liver Function TestsDocument14 pagesInterpretation of Liver Function TestsNirav SharmaNo ratings yet
- Autoimmune Liver DeseaseDocument4 pagesAutoimmune Liver DeseaseJankirk BacierraNo ratings yet
- Liver Function Tests (LFTS) : March 2010Document4 pagesLiver Function Tests (LFTS) : March 2010lavanyaNo ratings yet
- L8 - Hepatic EnzymesDocument30 pagesL8 - Hepatic Enzymesyouservezeropurpose113No ratings yet
- Liver Function Tests LFTsDocument4 pagesLiver Function Tests LFTsDr-Dalya ShakirNo ratings yet
- Skin ComplexionDocument51 pagesSkin Complexionomod415No ratings yet
- Metastatic Carcinoma of Prostate: AlkalineDocument2 pagesMetastatic Carcinoma of Prostate: AlkalineDjdjjd SiisusNo ratings yet
- Year 2: PBL 2: JaundiceDocument74 pagesYear 2: PBL 2: JaundiceyaneemayNo ratings yet
- Biochemical Alterations in Dengue Haemorrhagic Fever in Liver Function Test NewDocument46 pagesBiochemical Alterations in Dengue Haemorrhagic Fever in Liver Function Test Newraheemrahi089No ratings yet
- Name and Classification of DrugDocument3 pagesName and Classification of DrugAnicas, Ralph Joshua V.No ratings yet
- JaundiceDocument17 pagesJaundiceDarwithaNo ratings yet
- Urinary Tract Infection in Children - Classification, Diagnosis and TreatmentFrom EverandUrinary Tract Infection in Children - Classification, Diagnosis and TreatmentNo ratings yet
- Fast Facts: Acute and Recurrent Pancreatitis: Using evidence to support treatmentFrom EverandFast Facts: Acute and Recurrent Pancreatitis: Using evidence to support treatmentNo ratings yet
- Drug StudyDocument4 pagesDrug Studym100% (1)
- GoitreDocument2 pagesGoitresuggaplumNo ratings yet
- Breast SurgeryDocument6 pagesBreast SurgeryDeedee Rocha100% (1)
- Mnemonics and Acronyms For Nursing SchoolDocument20 pagesMnemonics and Acronyms For Nursing SchoolFaye G.100% (3)
- Case SheetDocument5 pagesCase SheetvisweswarkcNo ratings yet
- Clinical Biochemistry Lab 3 PDFDocument8 pagesClinical Biochemistry Lab 3 PDFNael NomanNo ratings yet
- B12 Deficiency Protocol 2013-09 PDFDocument8 pagesB12 Deficiency Protocol 2013-09 PDFariarcoirisNo ratings yet
- Neurology Lectures 1 4 DR - RosalesDocument20 pagesNeurology Lectures 1 4 DR - RosalesMiguel Cuevas DolotNo ratings yet
- PHENYLKETONURIADocument4 pagesPHENYLKETONURIAmarsiel03No ratings yet
- Ulcerative Colitis DiarrheaDocument2 pagesUlcerative Colitis DiarrheateuuuuNo ratings yet
- How I Treat Anemia in Pregnancy: Iron, Cobalamin, and FolateDocument11 pagesHow I Treat Anemia in Pregnancy: Iron, Cobalamin, and FolateAgungBudiPamungkasNo ratings yet
- Dipiro 9 (012-047) PDFDocument36 pagesDipiro 9 (012-047) PDFNingrumSindayaniNo ratings yet
- COPD - Jindal Chest ClinicDocument31 pagesCOPD - Jindal Chest ClinicJindal Chest ClinicNo ratings yet
- Adrenal 1 5Document41 pagesAdrenal 1 5Ditas ChuNo ratings yet
- EmergencyDocument86 pagesEmergencyyazzNo ratings yet
- Hepatic Embolotherapy in Interventional Oncology - Technology, Techniques, and ApplicationsDocument15 pagesHepatic Embolotherapy in Interventional Oncology - Technology, Techniques, and ApplicationsVeronica AlexanderNo ratings yet
- Acute Uncomplicated PyelonephritisDocument5 pagesAcute Uncomplicated PyelonephritisoreaNo ratings yet
- P300 in Patients With Epilepsy - The DifDocument241 pagesP300 in Patients With Epilepsy - The DifasasakopNo ratings yet
- Patologi GinjalDocument94 pagesPatologi GinjalDenoNo ratings yet
- Management of Menopause - A View Towards Prevention (Lobo y Gompel, 2022)Document14 pagesManagement of Menopause - A View Towards Prevention (Lobo y Gompel, 2022)Susana RoyNo ratings yet
- Management of DiplopiaDocument5 pagesManagement of Diplopiacahyati syhrilNo ratings yet
- Hyperosmolar Hyperglycemic StateDocument10 pagesHyperosmolar Hyperglycemic StateMirko S. León RguezNo ratings yet
- Gumboro Disease: Daissy Vanessa Diaz Guerrero - 542874Document10 pagesGumboro Disease: Daissy Vanessa Diaz Guerrero - 542874Ana Maria Vargas RuizNo ratings yet
- Metabolism of HemoglobinDocument46 pagesMetabolism of Hemoglobinlayla hitaNo ratings yet
- Carotid Cavernous FistulaDocument3 pagesCarotid Cavernous FistulaSadia GullNo ratings yet
- Burn PathophysiologyDocument14 pagesBurn PathophysiologyAgung Widya PramanaNo ratings yet
- Biology: Pearson Edexcel International Advanced LevelDocument4 pagesBiology: Pearson Edexcel International Advanced LevelAyesha GulzarNo ratings yet
- Continuous EEG Monitoring in The Intensive Care UnDocument7 pagesContinuous EEG Monitoring in The Intensive Care UnSara MendesNo ratings yet