Professional Documents
Culture Documents
Female Physiology
Female Physiology
Uploaded by
MZ Lim0 ratings0% found this document useful (0 votes)
11 views10 pages1) The female reproductive cycle begins with the development of primordial follicles containing immature oocytes in the ovaries during fetal development.
2) At puberty, FSH and LH stimulation causes some primordial follicles to develop into primary, secondary, and antral follicles with multiple layers of granulosa cells surrounding the oocyte.
3) During each menstrual cycle, FSH causes several antral follicles to further develop and mature, with only one follicle typically ovulating and releasing an oocyte.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document1) The female reproductive cycle begins with the development of primordial follicles containing immature oocytes in the ovaries during fetal development.
2) At puberty, FSH and LH stimulation causes some primordial follicles to develop into primary, secondary, and antral follicles with multiple layers of granulosa cells surrounding the oocyte.
3) During each menstrual cycle, FSH causes several antral follicles to further develop and mature, with only one follicle typically ovulating and releasing an oocyte.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
11 views10 pagesFemale Physiology
Female Physiology
Uploaded by
MZ Lim1) The female reproductive cycle begins with the development of primordial follicles containing immature oocytes in the ovaries during fetal development.
2) At puberty, FSH and LH stimulation causes some primordial follicles to develop into primary, secondary, and antral follicles with multiple layers of granulosa cells surrounding the oocyte.
3) During each menstrual cycle, FSH causes several antral follicles to further develop and mature, with only one follicle typically ovulating and releasing an oocyte.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 10
Guyton and Hall Textbook of Medical Physiology 13Ed Once these primordial germ cells reach the germinal
(Chap 82) epithelium, they migrate into the substance of the
ovarian cortex and become oogonia/primordial ova
Female Physiology Before Pregnancy and Female
primordial ovum then collects around it a layer of
Hormones
spindle cells from the ovarian stroma causes
Female reproductive functions can be divided into them to take epithelioid-like cells/granulosa cells
two major phases: ovum surrounded by a single layer of granulosa cells
o (1) preparation of the female body for is called a primordial follicle ovum is still
conception and pregnancy immature and is called a primary oocyte
o (2) period of pregnancy itself oogonia in the embryonic ovary complete mitotic
PHYSIOLOGICAL ANATOMY OF THE FEMALE SEXUAL replication and the first stage of meiosis by the 5th
ORGANS month of fetal development
Reproduction begins with the development of ova At birth the ovary contains about 1 to 2 million
in the ovaries primary oocytes
In middle of each monthly sexual cycle, a single first meiotic division of the oocyte occurs after
ovum is expelled near fimbriated ends of 2 fallopian puberty
tubes oocyte divides into secondary oocyte and small first
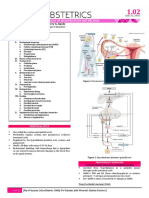
Figure 82-2 show the principal organs of the human polar body that contain 23 duplicated chromosomes
female reproductive tract polar body disintegrates and the other one
undergoes second meiotic division
after the sister chromatids separate, there is a
pause in meiosis
sister chromatids in the ovum go to separate cell
Half of the sister chromatids remain in the fertilized
ovum and the other half are released in a second
polar body
OOGENESIS AND FOLLICULAR DEVELOPMENT IN THE When the ovary releases the ovum (ovulation) and
OVARIES if the ovum is fertilized, the final step in meiosis
developing egg (oocyte) differentiates into a mature occurs
egg (ovum) through a series of steps called At puberty, only about 300,000 oocytes remain in
oogenesis (Figure 82-3) the ovaries, and only a small percentage of these
oocytes become mature
between about 13 and 46 years of age, only 400 to
500 of the primordial follicles develop enough to
expel their ova—one each month
remainder degenerate or become atretic
FEMALE HORMONAL SYSTEM
hypothalamic releasing hormone, called
gonadotropin-releasing hormone (GnRH)
anterior pituitary sex hormones, FSH and LH, both
of which are secreted in response to the release of
GnRH from the hypothalamus
primordial germ cells from the dorsal endoderm of ovarian hormones, estrogen and progesterone,
the yolk sac migrate along the mesentery of the which are secreted by the ovaries in response to the
hindgut to the outer surface of the ovary, which is two female sex hormones
covered by a germinal epithelium Figure 82-4 shows the approximate changing
During this migration, the germ cells divide concentrations of the anterior pituitary
repeatedly gonadotropic hormones FSH and LH and of the
ovarian hormones estradiol (estrogen) and Figure 82-5 shows the progressive stages of
progesterone follicular growth in the ovaries
GnRH secreted in short pulses averaging once every When a female child is born, the ovum is with single
90 minutes granulosa cell sheath = primordial follicle
granulosa cells are believed to provide nourishment
for ovum and to secrete an oocyte maturation
inhibiting factor that keeps the ovum suspended in
its primordial state in prophase stage of meiotic
division
after puberty, when FSH and LH begin to be
secreted, ovaries begin to grow
first stage of follicular growth is moderate
MONTHLY OVARIAN CYCLE; FUNCTION OF THE
enlargement of the ovum
GONADOTROPIC HORMONES
stage is followed by growth of additional layers of
normal reproductive years of the female are
granulosa cells forms primary follicles
characterized by monthly rhythmical changes
¤ Development of Antral and Vesicular Follicles
rhythmical pattern is called the female monthly
On first few days of each monthly female sexual
sexual cycle or menstrual cycle = 28 days
cycle, FSH and LH increase slightly to moderately
may be as short as 20 days or as long as 45 days in
FSH cause accelerated growth of 6 to 12 primary
some women
follicles each month
abnormal cycle length is frequently associated with
initial effect is rapid proliferation of the granulosa
decreased fertility
cells, giving rise to many more layers of these
female sexual cycle has two significant results
spindle cells derived from the ovary interstitium
o only a single ovum is normally released
collect in several layers outside the granulosa cells
from the ovaries each month
forms second mass of cells called the theca
o uterine endometrium is prepared in
theca interna, the cells take on epithelioid
advance for implantation of the fertilized
characteristics similar to those of the granulosa cells
ovum at the required time of the month
and develop the ability to secrete additional
GONADOTROPIC HORMONES AND THEIR EFFECTS ON
estrogen and progesterone
THE OVARIES
theca externa, develops into a highly vascular
ovarian changes depend completely on FSH and LH
connective tissue capsule that becomes the capsule
Both FSH and LH are small glycoproteins that have
of developing follicle
molecular weights of about 30,000
after early proliferative phase of growth, mass of
At age 9-12 years, the pituitary begins to secrete
granulosa cells secretes a follicular fluid that
progressively more FSH and LH leading to onset
contains a high concentration of estrogen
of normal monthly sexual cycles beginning between
Accumulation of this fluid causes an antrum to
ages of 11-15 years = puberty; when menarche
appear within mass of granulosa cells (Figure 82-5)
starts
cyclical variations cause cyclical ovarian changes
FSH and LH stimulate their ovarian target cells
activated receptors increase the cells’ rates of
secretion all these stimulatory effects result from
activation of the cyclic adenosine monophosphate
second messenger system causes the formation
of protein kinase and multiple phosphorylations of
key enzymes that stimulate sex hormone synthesis early growth of the primary follicle up to the antral
OVARIAN FOLLICLE GROWTH—THE FOLLICULAR PHASE stage is stimulated mainly by FSH alone
OF THE OVARIAN CYCLE
Greatly accelerated growth then occurs leading allowing a more viscous fluid, which has occupied
to vesicular follicles caused by following the central portion of the follicle, to evaginate
mechanisms: outward
o Estrogen is secreted into the follicle and viscous fluid carries with it the ovum surrounded by
causes the granulosa cells to form a mass of several thousand small granulosa cells
increasing numbers of FSH receptors called corona radiata
causing granulosa cells to be more sensitive A Surge of Luteinizing Hormone Is Necessary for
to FSH Ovulation
o pituitary FSH and the estrogens combine to LH is necessary for final follicular growth and
promote LH receptors on the original ovulation, without this, follicle will not progress to
granulosa cells, thus allowing LH stimulation the stage of ovulation
to occur in addition to FSH stimulation and About 2 days before ovulation the rate of secretion
creating an even more rapid increase in of LH by the anterior pituitary gland increases
follicular secretion markedly & peaking about 16 hours before
o increasing estrogens from the follicle plus ovulation
the increasing LH from the anterior pituitary FSH and LH act synergistically to cause rapid
gland act together to cause proliferation of swelling of the follicle during last few days before
the follicular thecal cells and increase their ovulation
secretion LH also has a specific effect on the granulosa and
Once the antral follicles begin to grow, ovum also theca cells, converting them mainly to
enlarges giving a total ovum diameter increase up progesterone-secreting cells
to 10-fold, or a mass increase of 1000-fold It is in this environment of (1) rapid growth of the
As follicle enlarges, ovum remains embedded in a follicle, (2) diminishing estrogen secretion after a
mass of granulosa cells located at one pole of prolonged phase of excessive estrogen secretion,
follicle and (3) initiation of secretion of progesterone that
¤ Only One Follicle Fully Matures Each Month, and ovulation occurs
the Remainder Undergo Atresia Initiation of Ovulation (Figure 82-6)
After a week or more of growth, one of the follicles
begins to outgrow all the others, and the remaining
5 to 11 developing follicles involute atresia
Atresia is likely caused by large amounts of estrogen
from the most rapidly growing follicle act on the
hypothalamus to depress FSH secretion
largest follicle continues to grow because of its
intrinsic positive feedback effects, while all the
other follicles stop growing and actually involute
process of atresia is important because it normally
allows only one of the follicles to grow (mature
LH causes rapid secretion of follicular steroid
follicle) large enough each month to ovulate
hormones that contain progesterone and 2 events
¤ Ovulation
occur necessary to ovulate
Ovulation in a woman who has a normal 28-day
These two effects cause plasma transudation and
female sexual cycle occurs 14 days after the onset
contributes to follicle swelling
of menstruation
o theca externa begins to release proteolytic
before ovulation the protruding outer wall of the
enzymes from lysosomes, and these
follicle swells rapidly, and a small area in the center
enzymes cause dissolution of the follicular
of the follicular capsule, called the stigma,
capsular wall and consequent weakening of
protrudes like a nipple after 30 mins, fluid begins
the wall, resulting in further swelling of the
to ooze from the follicle through the stigma, and
about 2 minutes later, the stigma ruptures widely,
entire follicle and degeneration of the enlargement, (3) secretion, (4) degeneration in
stigma about 12 days
o rapid growth of new blood vessels into the chorionic gonadotropin can act on the corpus
follicle wall, and at the same time, luteum to prolong its life for first 2 to 4 months of
prostaglandins (cause vasodilation) are pregnancy
secreted into the follicular tissues ¤ Involution of the Corpus Luteum and Onset of the
combination of follicle swelling and simultaneous Next Ovarian Cycle.
degeneration of the stigma causes follicle rupture, lutein cells secrete small amounts of the hormone
with discharge of the ovum inhibin, the same as the inhibin secreted by the
CORPUS LUTEUM—THE LUTEAL PHASE OF THE Sertoli cells of the male testes
OVARIAN CYCLE inhibin depresses FSH secretion by the anterior
after expulsion of the ovum from the follicle, the pituitary gland
remaining granulosa and theca interna cells change loss of FSH and LH, corpus luteum degenerate
rapidly into lutein cells completely = process called involution
lutein cells enlarge in diameter two or more times Final involution normally occurs at the end of
and become filled with lipid inclusions that give almost exactly 12 days of corpus luteum life, around
them a yellowish appearance = luteinisation the 26th day of the normal female sexual cycle, 2
total mass of cells together is called the corpus days before menstruation begins
luteum with well-developed vascular supply sudden cessation of secretion of estrogen,
granulosa cells in the corpus luteum develop progesterone, and inhibin by the corpus luteum
extensive intracellular smooth endoplasmic reticula removes the feedback inhibition of the anterior
that form large amounts of progesterone pituitary gland, allowing it to begin secreting
theca cells form mainly the androgens increasing amounts of FSH and LH again
androstenedione and testosterone rather than paucity of secretion of progesterone and estrogen
female sex hormones these hormones are also at this time also leads to menstruation by the uterus
converted by the enzyme aromatase in the SUMMARY
granulosa cells into estrogens About every 28 days, gonadotropic hormones cause
corpus luteum reaching stage of development 7 to 8 8 to 12 new follicles to begin to grow in the ovaries
days after ovulation then begins to involute and Ovulation is on the 14th day of the cycle
eventually loses its secretory function and its secretory cells of the ovulating follicle develop into
yellowish, lipid characteristic about 12 days after a corpus luteum
ovulation, becoming the corpus albicans During growth of the follicles, estrogen is mainly
corpus albicans is replaced by connective tissue and secreted
over months is absorbed secretory cells of the ovulating follicle develop into
¤ Luteinizing Function of Luteinizing Hormone a corpus luteum that secretes estrogen,
change of granulosa and theca interna cells into progesterone
lutein cells is dependent mainly on LH secreted by After another 2 weeks, the corpus luteum
the anterior pituitary gland degenerates, whereupon the ovarian hormones
Luteinization “yellowing” also depends on extrusion estrogen and progesterone decrease greatly and
of the ovum from the follicle menstruation begins new cycle begins
luteinization-inhibiting factor seems to hold the FUNCTIONS OF THE OVARIAN HORMONES—
luteinization process in check until after ovulation ESTRADIOL AND PROGESTERONE
¤ Secretion by the Corpus Luteum: An Additional two types of ovarian sex hormones are the
Function of Luteinizing Hormone. estrogens and the progestins
Corpus luteum secreting large amounts of both most important of the estrogens is the hormone
progesterone and estrogen estradiol, and by far the most important progestin is
lutein cells seem to be programmed to go through a progesterone
preordained sequence of (1) proliferation, (2)
estrogens mainly promote proliferation and growth
of specific cells in the body that are responsible for
secondary sexual characteristics of female
progestins function mainly to prepare the uterus for
pregnancy and the breasts for lactation
CHEMISTRY OF THE SEX HORMONES
Estrogens
in nonpregnant female, estrogens are secreted in Estrogens and Progesterone Are Transported in the
significant quantities only by the ovaries Blood Bound to Plasma Proteins
Only three estrogens are present in significant estrogens and progesterone bound mainly with
quantities in the plasma of the human female β- plasma albumin and with specific estrogen- and
estradiol, estrone, and estriol progesterone-binding globulins
principal estrogen secreted by the ovaries is β- binding between these hormones and the plasma
estradiol proteins is loose rapidly released to the tissues
estrone is mostly formed in the peripheral tissues over a period of 30 minutes
from androgens secreted by the adrenal cortices Functions of the Liver in Estrogen Degradation
and by ovarian thecal cells liver conjugates the estrogens to form glucuronides
Estriol is a weak estrogen oxidative product and sulfates excreted in bile and urine
derived from both estradiol and estrone, with the liver converts potent estrogens estradiol and
conversion occurring mainly in the liver estrone into the almost totally impotent estrogen
β-estradiol is considered the major estrogen, estriol
although the estrogenic effects of estrone are not diminished liver function actually increases the
negligible activity of estrogens in the body hyperestrinism
Progestins Fate of Progesterone
small amounts of another progestin, 17-α- progesterone is degraded to other steroids that
hydroxyprogesterone, are secreted along with have no progestational effect
progesterone and have essentially the same effects major end product of progesterone degradation is
nonpregnant female, progesterone is usually pregnanediol
secreted by corpus luteum in significant amounts FUNCTIONS OF THE ESTROGENS— THEIR EFFECTS ON
only during the latter half of each ovarian cycle THE PRIMARY AND SECONDARY FEMALE SEX
Synthesis of the Estrogens and Progestins CHARACTERISTICS
both synthesized in the ovaries mainly from primary function of the estrogens is to cause
cholesterol derived from the blood and acetyl cellular proliferation and growth of the tissues of
coenzyme A the sex organs and other tissues related to
mainly progesterone and androgens (testosterone reproduction
and androstenedione) are synthesized first ¤ Effect of Estrogens on the Uterus and External
during the follicular phase of the ovarian cycle, all Female Sex Organs
the androgens & much progesterone are converted ovaries, fallopian tubes, uterus, and vagina all
into estrogens by enzyme aromatase in granulosa increase several times in size
cells external genitalia enlarge, with deposition of fat in
theca cells lack aromatase, they cannot convert the mons pubis and labia majora and enlargement
androgens to estrogens BUT androgens diffuse out of the labia minora
of the theca cells and converted to estrogens by estrogens change the vaginal epithelium from a
aromatase via FSH (Figure 82-8) cuboidal into a stratified type, which is considerably
more resistant to trauma and infection
o Vaginal infections in children can often be
cured by the administration of estrogens
increase in uterus size are the changes that take osteoporosis can greatly weaken the bones and lead
place in the uterine endometrium under the to bone fracture, especially fracture of the
influence of estrogens vertebrae,
increased development of the endometrial glands, ¤ Estrogens Slightly Increase Protein Deposition
which will later aid in providing nutrition to the Estrogens cause a slight increase in total body
implanted ovum protein, which is evidenced by a slight positive
¤ Effect of Estrogens on the Fallopian Tubes nitrogen balance cause growth promoting effect
cause the glandular tissues of this lining to enhanced protein deposition caused by
proliferate testosterone is much more general and much more
they cause the number of ciliated epithelial cells powerful than that caused by estrogens
that line the fallopian tubes to increase ¤ Estrogens Increase Body Metabolism and Fat
activity of the cilia that beat toward the uterus is Deposition
enhanced Estrogens increase the whole-body metabolic rate
¤ Effect of Estrogens on the Breasts slightly, increased quantities of fat in the
masculine breast during the first 2 decades of life subcutaneous tissues
can develop sufficiently to produce milk in the same percentage of body fat in the female body is
manner as the female breast considerably greater than that in the male body,
Estrogens cause (1) development of the stromal which contains more protein
tissues of the breasts, (2) growth of an extensive estrogens cause the deposition of fat in the
ductile system, and (3) deposition of fat in the buttocks and thighs
breasts ¤ Estrogens Have Little Effect on Hair Distribution
lobules and alveoli of the breast develop to a slight Estrogens do not greatly affect hair distribution
extent under the influence of estrogens alone IT hair does develop in the pubic region and in the
IS THE PROGESTERONE cause the ultimate growth axillae after puberty due to female adrenal
estrogens initiate growth of the breasts and of the glands after puberty
milk-producing apparatus BUT do not complete the ¤ Effect of Estrogens on the Skin
job of converting breasts into milk-producing organs Estrogens cause the skin to develop a texture that is
¤ Effect of Estrogens on the Skeleton soft and usually smooth
Estrogens inhibit osteoclastic activity in the bones Estrogens also cause the skin to become more
and therefore stimulate bone growth vascular, which is often associated with increased
stimulation of osteoprotegerin, which is also called warmth of the skin and also promotes greater
osteoclastogenesis inhibitory factor, a cytokine that bleeding of cut surfaces
inhibits bone resorption ¤ Effect of Estrogens on Electrolyte Balance
estrogen cause uniting of the epiphyses with the Estrogens, like aldosterone, cause sodium and
shafts of the long bones water retention by the kidney tubules
estrogen in the female is much stronger than the The effect is slight and rarely of significance, but
similar effect of testosterone in the male during pregnancy the tremendous formation of
female eunuch who is devoid of estrogen estrogens by the placenta may contribute to body
production usually grows several inches taller than fluid retention
a normal mature female because her epiphyses do FUNCTIONS OF PROGESTERONE
not unite at the normal time major function of progesterone is to promote
¤ Osteoporosis of the Bones Caused by Estrogen secretory changes in the uterine endometrium
Deficiency in Old Age during the latter half of monthly female sexual cycle
After menopause, almost no estrogens are secreted preparing the uterus for implantation
by the ovaries that leads to (1) increased progesterone decreases the frequency and intensity
osteoclastic activity in the bones, (2) decreased of uterine contractions, thereby helping to prevent
bone matrix, and (3) decreased deposition of bone expulsion of the implanted ovum
calcium and phosphate ¤ Effect of Progesterone on the Fallopian Tubes
It promotes increased secretion by the mucosal Secretory Phase (Progestational Phase) of the
lining of the fallopian tubes Endometrial Cycle, Occurring After Ovulation
secretions are necessary for nutrition of the on latter half of the monthly cycle, after ovulation
fertilized, dividing ovum as it traverses the fallopian has occurred, progesterone and estrogen together
tube before implantation are secreted in large quantities by the corpus
¤ Progesterone Promotes Development of the luteum
Breasts estrogens cause slight additional cellular
causing the alveolar cells to proliferate, enlarge, and proliferation in this phase
become secretory progesterone causes marked swelling and secretory
progesterone does not cause the alveoli to secrete development of the endometrium
milk but milk is secreted only after the prepared glands increase in tortuosity, and an excess of
breast is further stimulated by prolactin from the secretory substances accumulates in the glandular
anterior pituitary gland epithelial cells
Progesterone also causes the breasts to swell cytoplasm of the stromal cells increases, lipid and
MONTHLY ENDOMETRIAL CYCLE AND MENSTRUATION glycogen deposits increase greatly in the stromal
cells, and the blood supply also increases
at peak of the secretory phase, about 1 week after
ovulation, the endometrium has thickness of 5-6
mm
purpose to produce a highly secretory
endometrial cycle in the lining of the uterus endometrium that contains large amounts of stored
operates through the following stages: (1) nutrients to provide for the fertilized ovum
proliferation of the uterine endometrium; (2) ovum enters the uterine cavity from the fallopian
development of secretory changes in the tube (which occurs 3 to 4 days after ovulation) until
endometrium; and (3) desquamation of the the time the ovum implants (7 to 9 days after
endometrium, which is known as menstruation ovulation) uterine secretions, called “uterine
Proliferative Phase (Estrogen Phase) of the milk,” provide nutrition for the early dividing ovum
Endometrial Cycle, Occurring Before Ovulation. once the ovum implants in the endometrium, the
beginning of each cycle, most of the endometrium trophoblastic cells on the surface of the implanting
has been desquamated by menstruation ovum begin to digest the endometrium and absorb
After menstruation, only a thin layer of endometrial the endometrial stored substances
stroma remains and the only epithelial cells Menstruation
remaining in the deeper portions of the glands and if ovum is not fertilized, about 2 days before end of
crypts of the endometrium the monthly cycle, the corpus luteum involutes and
Under the influence of estrogens during the first the ovarian hormones decrease menstruation
part of the monthly ovarian cycle, the stromal cells Menstruation is caused especially by progesterone,
and the epithelial cells proliferate rapidly at the end of the monthly ovarian cycle
endometrial surface is re-epithelialized within 4 to 7 tortuous blood vessels leading to the mucosal layers
days after the beginning of menstruation of the endometrium become vasospastic
during the next week, endometrium increases vasospasm, loss of hormonal stimulation initiate
greatly in thickness, due to increasing numbers of necrosis in the endometrium blood at first seeps
stromal cell, endometrial glands and new blood into the vascular layer and the hemorrhagic areas
vessels into the endometrium grow rapidly over a period of 24 to 36 hours
at time of ovulation, endometrium is 3-5mm thick about 48 hours, all the superficial layers of the
endometrial glands, especially those of the cervical endometrium have desquamated
region, secrete thin, stringy mucus mass of desquamated tissue and blood in the
mucus strings actually align themselves along the uterine cavity, plus contractile effects of
length of the cervical canal, forming channels that prostaglandins initiate uterine contractions that
help guide sperm expel the uterine contents
During normal menstruation, approximately 40 abrupt surge in LH secretion is not known but some
milliliters of blood and an additional 35 milliliters of suggest estrogen has a peculiar positive feedback
serous fluid are lost effect of stimulating pituitary secretion of LH
menstrual fluid is normally nonclotting because a contrast to the normal negative feedback effect of
fibrinolysin is released along with the necrotic estrogen during the remainder of the female
endometrial material monthly cycle
If excessive bleeding occurs from the uterine FEEDBACK OSCILLATION OF THE HYPOTHALAMIC-
surface, the quantity of fibrinolysin is not enough PITUITARY-OVARIAN SYSTEM
presence of clots during menstruation is often
clinical evidence of uterine disease
Within 4 to 7 days after menstruation starts, the
loss of blood ceases because endometrium has
become re-epithelialized
There is large numbers of leukocytes are released
along with the necrotic material and blood
As a result of these leukocytes, uterus is highly
resistant to infection during menstruation, even
though the endometrial surfaces are denuded
REGULATION OF THE FEMALE MONTHLY RHYTHM—
INTERPLAY BETWEEN THE OVARIAN AND
HYPOTHALAMIC-PITUITARY HORMONES feedback oscillation that controls the rhythm of the
secretion of most of the anterior pituitary female sexual cycle in 3 events:
hormones is controlled by “releasing hormones” by o postovulatory secretion of the ovarian
way of the hypothalamic-hypophysial portal system hormones and depression of the pituitary
hypothalamus does not secrete GnRH continuously gonadotropins
but instead secretes it in pulses lasting 5 to 25 o follicular growth phase = negative feedback
minutes that occur every 1 to 2 hours effect, mainly of estrogen and sudden,
pulsatile release of GnRH also causes intermittent marked increase in the secretion of LH
output of LH secretion about every 90 minutes o preovulatory surge of LH and FSH causes
¤ Hypothalamic Centers for Release of Gonadotropin ovulation = high level of estron cause a
Releasing Hormone positive feedback stimulatory effect LH
neuronal activity that causes pulsatile release of surge
GnRH in mediobasal hypothalamus, arcuate Anovulatory Cycles—Sexual Cycles at Puberty
nuclei ovulation will not occur and the cycle is said to be
it is believed that these arcuate nuclei control most “anovulatory” if LH is insufficient
female sexual activity lack of ovulation causes failure of development of
NEGATIVE FEEDBACK EFFECTS OF ESTROGEN AND the corpus luteum, progesterone
PROGESTERONE TO DECREASE LH AND FSH SECRETION cycle is shortened by several days but rhythm
Estrogen in small amounts has a strong inhibitory continues
effect on the production of both LH and FSH first few cycles after the onset of puberty are
inhibin, which is secreted along with the steroid sex usually anovulatory
hormones by the granulosa cells of the ovarian PUBERTY AND MENARCHE
corpus luteum Puberty means the onset of adult sexual life, and
POSITIVE FEEDBACK EFFECT OF ESTROGEN BEFORE menarche means the beginning of the cycle of
OVULATION—THE PREOVULATORY LUTEINIZING menstruation
HORMONE SURGE period of puberty beginning in about the eighth
increased amounts of LH for 1 to 2 days beginning year of life or between ages 11 and 16 years in girls
24 to 48 hours before ovulation (average, 13 years)
it is now believed that the onset of puberty is FEMALE SEXUAL ACT
initiated by some maturation process that occurs successful performance of the female sexual act
elsewhere in the brain, perhaps somewhere in the depends on both psychic stimulation and local
limbic system sexual stimulation
Thinking sexual thoughts can lead to female sexual
desire that is based on psychological and
physiological drive
Desire also changes during the monthly sexual
cycle, reaching a peak near the time of ovulation
massage and other types of stimulation of the vulva,
vagina, and other perineal regions can create sexual
Figure 82-13 shows (1) increasing levels of estrogen sensations
secretion at puberty, (2) cyclical variation during the glans of the clitoris is especially sensitive for
monthly sexual cycle, (3) further increase in initiating sexual sensations
estrogen secretion during the first few years of sexual signals are transmitted to the cerebrum
reproductive life, (4) progressive decrease in local reflexes integrated in the sacral and lumbar
estrogen secretion toward the end of reproductive spinal cord are at least partly responsible for some
life, and, finally, (5) almost no estrogen or of the reactions in the female sexual organs
progesterone secretion beyond menopause Located around the introitus and extending into the
MENOPAUSE clitoris is erectile tissue almost identical to the
40 to 50 years, the sexual cycle usually becomes erectile tissue of the penis
irregular and ovulation often fails to occur Erectile tissue is controlled by the parasympathetic
period during which the cycle ceases and the female nerves that pass through the nervi erigentes from
sex hormones diminish to almost none is called the sacral plexus to the external genitalia
menopause early phases of sexual stimulation, parasympathetic
cause of menopause is “burning out” of the ovaries signals dilate the arteries of the erectile tissue, due
about 400 of the primordial follicles grow into to release of acetylcholine, nitric oxide, and VIP
mature follicles and ovulate, and hundreds of allows rapid accumulation of blood in the erectile
thousands of ova degenerate tissue so that the introitus tightens around the
at 45 years, only a few primordial follicles remain to penis, which aids the male in his attainment of
be stimulated by FSH and LH sufficient sexual stimulation for ejaculation to occur
When estrogen production falls below a critical Bartholin glands located beneath the labia minora
value, the estrogens can no longer inhibit the and cause them to secrete mucus immediately
production of the gonadotropins thus increase in inside the introitus
FSH and remaining primordial follicles become lubrication is necessary during intercourse to
atretic establish a satisfactory massaging sensation rather
loss of estrogens often causes marked physiological than an irritative sensation
changes in the function of the body, including (1) massaging sensation constitutes the optimal
“hot flushes” characterized by extreme flushing of stimulus for evoking the appropriate reflexes that
the skin, (2) psychic sensations of dyspnea, (3) culminate in both the male and female climaxes
irritability, (4) fatigue, (5) anxiety, and (6) decreased Female Orgasm
strength and calcification of bones When local sexual stimulation reaches maximum
When ovaries are absent from birth or when they intensity, reflexes are initiated that cause the
become nonfunctional before puberty, female female orgasm, also called the female climax
eunuchism occurs human female is known to be somewhat more
In hypothyroidism, the ovarian cycle often does not fertile when inseminated by normal sexual
occur normally intercourse
rare granulosa cell tumor can develop in an ovary; during the orgasm, the perineal muscles of the
developing after menopause female contract rhythmically
possible that these reflexes increase uterine and
fallopian tube motility during the orgasm
orgasm seems to cause dilation of the cervical canal
for up to 30 minutes, thus allowing easy transport
of the sperm
copulation causes the posterior pituitary gland to
secrete oxytocin; this effect is probably mediated
through the brain amygdaloid nuclei and then
through the hypothalamus to the pituitary
oxytocin causes increased rhythmical contractions
of the uterus = increased transport of the sperm
possible effects of the orgasm on fertilization, the
intense sexual sensations that develop during the
orgasm also pass to the cerebrum and cause intense
muscle tension throughout the body
tension gives way during the succeeding minutes to
a sense of satisfaction characterized by relaxed
peacefulness, an effect called resolution
You might also like
- Leonardo Da Vinci Anatomical DrawingsDocument170 pagesLeonardo Da Vinci Anatomical Drawingsmichael100% (8)
- Definition of EmbryologyDocument12 pagesDefinition of EmbryologyOmar BasimNo ratings yet
- Care of The Mother and The Fetus During Perinatal PeriodDocument11 pagesCare of The Mother and The Fetus During Perinatal PeriodMaria KawilanNo ratings yet
- Mammalian Reproductive SystemDocument50 pagesMammalian Reproductive SystemLeena MuniandyNo ratings yet
- Ch. 38 Human ReproductionDocument38 pagesCh. 38 Human ReproductionERIC ASAMAMLEH KLEMEHNo ratings yet
- Functions of Ovaries: Learning ObjectivesDocument9 pagesFunctions of Ovaries: Learning ObjectivesUloko ChristopherNo ratings yet
- Physiology of Non Pregnant FemaleDocument37 pagesPhysiology of Non Pregnant Femalephuyalaryan666No ratings yet
- MODULE 1-Lesson 2-3Document11 pagesMODULE 1-Lesson 2-3JOHN BRAINARD PEJONo ratings yet
- Module 6A Physiology of MenstruationDocument7 pagesModule 6A Physiology of MenstruationBroskiNo ratings yet
- NIH Public Access: Author ManuscriptDocument13 pagesNIH Public Access: Author ManuscriptDhikaNo ratings yet
- Physiology of OvulationDocument7 pagesPhysiology of OvulationAza Patullah ZaiNo ratings yet
- Dasar2 Biomolekuler Repro WanitaDocument51 pagesDasar2 Biomolekuler Repro WanitaFitriaNo ratings yet
- PEDIA-REVIEWER EditedDocument7 pagesPEDIA-REVIEWER EditedTO THE MOONNo ratings yet
- 057 - Endocrinology Physiology] OvulationDocument4 pages057 - Endocrinology Physiology] Ovulationmohsinafghan54No ratings yet
- Cervix Ca-Patho Initial DraftDocument17 pagesCervix Ca-Patho Initial Draftjam reparejoNo ratings yet
- NCM 107 Hands OutDocument15 pagesNCM 107 Hands OutErin SaavedraNo ratings yet
- 057 - Endocrinology Physiology) OvulationDocument4 pages057 - Endocrinology Physiology) Ovulationhasanatiya41No ratings yet
- ReproductionDocument6 pagesReproductionAbelle EnsuiNo ratings yet
- Menstrual Cycle: Pepino, Ricalde, Roxas 3PtDocument11 pagesMenstrual Cycle: Pepino, Ricalde, Roxas 3PtAlthea JacobNo ratings yet
- OvariesDocument5 pagesOvariesarpitsonone16No ratings yet
- Menstrual Cycle Embryonic Development PPT Group 5 1Document40 pagesMenstrual Cycle Embryonic Development PPT Group 5 1Alen ColiamNo ratings yet
- Pag 2Document1 pagePag 2Santiago TeixeiraNo ratings yet
- Mikes First Semester Embryology-1Document8 pagesMikes First Semester Embryology-1obianujuonyeka6No ratings yet
- Reproductive Processes: Chapter-34-Lesson-2 Page-961-966Document26 pagesReproductive Processes: Chapter-34-Lesson-2 Page-961-966JanaNo ratings yet
- FERTILIZATIONDocument73 pagesFERTILIZATIONSavita Hanamsagar100% (1)
- Dasar-Dasar Biomolekuler Reproduksi Wanita: Rahmatina B. HermanDocument29 pagesDasar-Dasar Biomolekuler Reproduksi Wanita: Rahmatina B. HermansilmiNo ratings yet
- 07.12.2019 Human Reproduction-Part 2Document32 pages07.12.2019 Human Reproduction-Part 2Ayisha AlamNo ratings yet
- Detailed EoT Coverage 9 ADVDocument50 pagesDetailed EoT Coverage 9 ADVNKANo ratings yet
- Nzary El 3maliDocument13 pagesNzary El 3maliGana KhaledNo ratings yet
- Female Reproductive System Study GuideDocument2 pagesFemale Reproductive System Study GuideRhea Jane SorillaNo ratings yet
- Kentuck IDocument44 pagesKentuck IdirinaNo ratings yet
- Fertilisation in HumansDocument47 pagesFertilisation in HumansVVS .b.s2126No ratings yet
- Overview of The Female Reproductive SystemDocument3 pagesOverview of The Female Reproductive SystemMonica J Ortiz PereiraNo ratings yet
- Fisiologia Sistema Genital Feminino (Resumo)Document3 pagesFisiologia Sistema Genital Feminino (Resumo)farmaciaNo ratings yet
- Menstruation FertilizationDocument2 pagesMenstruation FertilizationJamie Rose GarciaNo ratings yet
- Seminar 1Document8 pagesSeminar 1gatorssoccer1313No ratings yet
- Handout On ReproDocument4 pagesHandout On ReproJoe JosephNo ratings yet
- Ovulation & Menstrual Cycle Overview AtfDocument5 pagesOvulation & Menstrual Cycle Overview AtfAkeny AranyaNo ratings yet
- (TLOY) OB - Endometrial and Ovarian CycleDocument6 pages(TLOY) OB - Endometrial and Ovarian CycleJAMICA ROMAINE AMBIONNo ratings yet
- Life Sciences Teacher Booklet Saturdays Term 2 - 2024 For Level 1 & 2 LearnersDocument60 pagesLife Sciences Teacher Booklet Saturdays Term 2 - 2024 For Level 1 & 2 Learnersamyolisomdaka50No ratings yet
- 2003 EI KFER Pathophysiology of DUB - 01Document50 pages2003 EI KFER Pathophysiology of DUB - 01Hernita HuangNo ratings yet
- Group3 2Document53 pagesGroup3 2just myselfNo ratings yet
- OB 1 - 1.02 Physiology of Menstruation and Decidua PDFDocument11 pagesOB 1 - 1.02 Physiology of Menstruation and Decidua PDFMDreamerNo ratings yet
- Physiology of MenstruationDocument12 pagesPhysiology of MenstruationCharlz ZipaganNo ratings yet
- The Menstrual Cycle Ob - Gyn SecretsDocument4 pagesThe Menstrual Cycle Ob - Gyn Secretsleonardotorres1No ratings yet
- OogenesisDocument13 pagesOogenesisZerica JohnNo ratings yet
- Ncm107j Weekly NotesDocument11 pagesNcm107j Weekly NotesSHEENA MAE DE LOS REYESNo ratings yet
- Physiology of Women Reproduction SystemDocument52 pagesPhysiology of Women Reproduction Systemram kumarNo ratings yet
- Oogenesis Oogenesis Is The Process Whereby Oogonia Differentiate Into Mature Oocytes. It Starts in TheDocument7 pagesOogenesis Oogenesis Is The Process Whereby Oogonia Differentiate Into Mature Oocytes. It Starts in ThebarbacumlaudeNo ratings yet
- Chapter - 3 Human Reproduction - WatermarkDocument23 pagesChapter - 3 Human Reproduction - WatermarkDurgesh SainiNo ratings yet
- BIO ProjectDocument17 pagesBIO ProjectHârsh V ÎshwãkårmāNo ratings yet
- OB Dr. Rana (Chapter 5 & 6)Document26 pagesOB Dr. Rana (Chapter 5 & 6)Mich Therese AbejeroNo ratings yet
- 2 - Gametogenesis and Female CyclesDocument31 pages2 - Gametogenesis and Female CyclesMax DanhNo ratings yet
- Chapter 4 Reproduction and GrowthDocument11 pagesChapter 4 Reproduction and GrowthDeepa Manogaran100% (5)
- Science Quarter Iii: Prepared By: Magsino, Jallyna JaneDocument12 pagesScience Quarter Iii: Prepared By: Magsino, Jallyna Janellyna devillasNo ratings yet
- EOT - 9 Adv T3 - Yr 22-23Document83 pagesEOT - 9 Adv T3 - Yr 22-23NKANo ratings yet
- Reproductive System: Synopsis Menstrual Cycle Spermatogenesis Oogenesis Process of Reproduction Pregnancy ParturitionDocument57 pagesReproductive System: Synopsis Menstrual Cycle Spermatogenesis Oogenesis Process of Reproduction Pregnancy ParturitionBlack RoseNo ratings yet
- BiologyyyDocument2 pagesBiologyyyprecious siNo ratings yet
- 5.1 Female 2023 - JPDocument89 pages5.1 Female 2023 - JPtexasrepublican1976No ratings yet
- 10.1a Sexual Reproduction in HumanDocument31 pages10.1a Sexual Reproduction in HumanKA YAN YAPNo ratings yet
- B g8 Digestive SystemDocument3 pagesB g8 Digestive SystemnoorlailyNo ratings yet
- 19 Musculoskeletal System DR - FallerDocument27 pages19 Musculoskeletal System DR - FallerFranz Earl Niño AlbesaNo ratings yet
- Histology Exam I OutlineDocument76 pagesHistology Exam I OutlinePrinceNo ratings yet
- KIN 1AA3/1YY3/2YY3 EXAM BREAKDOWN Winter 2017: Lecture TopicsDocument1 pageKIN 1AA3/1YY3/2YY3 EXAM BREAKDOWN Winter 2017: Lecture TopicsMikayla RaeNo ratings yet
- Chapter 6 Outline: Hole's Human Anatomy and Physiology Shier, Butler & Lewis Twelfth EditionDocument5 pagesChapter 6 Outline: Hole's Human Anatomy and Physiology Shier, Butler & Lewis Twelfth EditionNOELLE BUTKEVICNo ratings yet
- Human Nutrition - 90 QPDocument16 pagesHuman Nutrition - 90 QPStephen AreriNo ratings yet
- Science6 ST1 Q2Document2 pagesScience6 ST1 Q2Cecilia TolentinoNo ratings yet
- ADocument40 pagesAapi-3826751No ratings yet
- 1000 Mcqs of FCPS Part 1Document35 pages1000 Mcqs of FCPS Part 1Sana Sheikh95% (21)
- Anatomy at A GlanceDocument327 pagesAnatomy at A GlanceANo ratings yet
- Vedicinals Spike Protein Detox and Long Covid - Joachim Gerlach-CompressedDocument162 pagesVedicinals Spike Protein Detox and Long Covid - Joachim Gerlach-CompressedvaikyumiNo ratings yet
- Staining Abnormalities of Dermal Collagen in Eosinophil - or Neutrophil-Rich Inflammatory Dermatoses of Horses and Cats As DemonstrateDocument6 pagesStaining Abnormalities of Dermal Collagen in Eosinophil - or Neutrophil-Rich Inflammatory Dermatoses of Horses and Cats As DemonstratejenNo ratings yet
- CRC Desk Reference For Allergy and AsthmaDocument401 pagesCRC Desk Reference For Allergy and AsthmaClaudio Luis VenturiniNo ratings yet
- Ear 1, 2Document9 pagesEar 1, 2Nnbbh HggyyNo ratings yet
- Caps HTMLDocument152 pagesCaps HTMLUchy Luph'milimiLy0% (1)
- Dr. Meidona - Development of Gastrointestinal System PDFDocument54 pagesDr. Meidona - Development of Gastrointestinal System PDFwkwkwkhhhhNo ratings yet
- Physiology Practical For 1st Year Institute Pharmacy StudentsDocument14 pagesPhysiology Practical For 1st Year Institute Pharmacy StudentsSnipper HunterNo ratings yet
- Enhanced Hybrid Module S9 Q1 M1 WEEK 1 2.edited 2Document16 pagesEnhanced Hybrid Module S9 Q1 M1 WEEK 1 2.edited 2Ryzza Claire Montes AurinoNo ratings yet
- Five Element DiagnosisDocument2 pagesFive Element Diagnosisalex100% (1)
- Leopold's Maneuvers - PPTMDocument26 pagesLeopold's Maneuvers - PPTMDencel BarramedaNo ratings yet
- Ashtanga Primary Series BenefitsDocument2 pagesAshtanga Primary Series BenefitsTest4DNo ratings yet
- Conventional Methods of Incision and The Cosmetic Autopsy Incision: Its AdvantagesDocument5 pagesConventional Methods of Incision and The Cosmetic Autopsy Incision: Its AdvantagesAleena AyoubNo ratings yet
- Spine Structure and FunctionDocument19 pagesSpine Structure and Functionakhil dattaNo ratings yet
- Systema Lymphaticum: Lymphatic SystemDocument38 pagesSystema Lymphaticum: Lymphatic SystemGeorge GeorgeNo ratings yet
- Grade 9 Module WK 1-2Document8 pagesGrade 9 Module WK 1-2Llena Grace GloryNo ratings yet
- Oral Mucous MembraneDocument36 pagesOral Mucous MembraneFourthMolar.com100% (1)
- Pathology-1 (Introduction To Pathology)Document87 pagesPathology-1 (Introduction To Pathology)Durge Raj Ghalan67% (6)
- Plant AnatomyDocument22 pagesPlant AnatomyYogesh Bagad100% (1)
- Anatomical Study of Coronary Arteries and Its Braching Pattern in Costal Andhra Pradesh PopulationDocument17 pagesAnatomical Study of Coronary Arteries and Its Braching Pattern in Costal Andhra Pradesh PopulationIJAR JOURNALNo ratings yet













![057 - Endocrinology Physiology] Ovulation](https://imgv2-1-f.scribdassets.com/img/document/747968057/149x198/f0d2a0e435/1720123448?v=1)