Professional Documents
Culture Documents
Develop Med Child Neuro - 2021 - Chaovalit - Sit To Stand Training For Self Care and Mobility in Children With Cerebral
Develop Med Child Neuro - 2021 - Chaovalit - Sit To Stand Training For Self Care and Mobility in Children With Cerebral
Uploaded by
zizee61Original Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Develop Med Child Neuro - 2021 - Chaovalit - Sit To Stand Training For Self Care and Mobility in Children With Cerebral
Develop Med Child Neuro - 2021 - Chaovalit - Sit To Stand Training For Self Care and Mobility in Children With Cerebral
Uploaded by
zizee61Copyright:
Available Formats
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE
Sit-to-stand training for self-care and mobility in children with
cerebral palsy: a randomized controlled trial
SIRAWEE CHAOVALIT 1,2 | KAREN J DODD 1,3 | NICHOLAS F TAYLOR 1,4
1 School of Allied Health, Human Services and Sport, La Trobe University, Melbourne, Victoria, Australia. 2 Faculty of Medicine, Prince of Songkla University, Hat Yai,
Thailand. 3 College of Health and Biomedicine, Victoria University, Melbourne, Victoria; 4 Allied Health Clinical Research Office, Eastern Health, Melbourne, Victoria,
Australia.
Correspondence to Sirawee Chaovalit, School of Allied Health, Human Services and Sport, La Trobe University, Melbourne, Vic. 3086, Australia. E-mail: s.chaovalit@latrobe.edu.au
PUBLICATION DATA AIM To investigate if a sit-to-stand exercise programme for children with cerebral palsy (CP)
Accepted for publication 1st June 2021. would improve self-care and mobility.
Published online 11th July 2021. METHOD Thirty-eight children with CP (19 males, 19 females; mean age 8y 0mo, SD 2y 4mo,
age range 4y 0mo–12y 4mo) classified in Gross Motor Function Classification System
ABBREVIATIONS (GMFCS) levels III and IV and their caregivers were randomly allocated to sit-to-stand training
FTSST Five Times Sit-to-Stand Test plus routine physiotherapy (balance and gait training) or routine physiotherapy only
MCSI Modified Caregiver Strain Index (controls). Task-specific sit-to-stand training was completed five times a week for 6 weeks
WeeFIM Functional Independence under physiotherapist (twice weekly) and caregiver (three times weekly) supervision. Blinded
Measure for Children outcome assessments at week 7 were the self-care and mobility domains of the Functional
Independence Measure for Children, Five Times Sit-to-Stand Test (FTSST), and Modified
Caregiver Strain Index (MCSI).
RESULTS The sit-to-stand group self-care increased by 2.2 units (95% confidence interval [CI]
1.3–3.1) and mobility increased by 2.2 units (95% CI 1.4–3.0) compared to the control group.
In the sit-to-stand group, the FTSST was reduced by 4.0 seconds (95% CI 4.7 to 3.2) and
the MCSI was reduced by 0.8 units (95% CI 1.2 to 0.4) compared to the control group.
INTERPRETATION A sit-to-stand exercise programme for children with CP classified in GMFCS
levels III and IV improved sit-to-stand performance and resulted in small improvements in
self-care and mobility, while reducing caregiver strain.
Children with cerebral palsy (CP) who are classified in which is consistent with the principles of motor learning6
levels III and IV of the Gross Motor Function Classifica- and task-specific training,7 whereby a systems approach
tion System (GMFCS) often have difficulty changing body involves adaptation of the brain to solve movement prob-
position by transferring from sitting to standing efficiently, lems.6 Therapy for children with CP commonly incorpo-
safely, and independently.1,2 This is a concern because rates task-specific training. Consistent with the criteria for
being able to sit-to-stand is an important component of functional therapy,8 this involves the goal-directed, repeti-
many everyday activities, such as standing up to prepare tive practice of a whole task or part of a task often modi-
for walking and to complete self-care activities, such as fied to suit a child’s abilities and practised under different
dressing, washing oneself, and toileting.1–3 Therefore, conditions consistent with the context under which the task
improvements in sit-to-stand might lead to greater inde- will be performed in daily activities.4–7,9
pendence for the child and in turn may reduce caregiver Although repetitive practice improved sit-to-stand per-
strain by reducing the level of assistance required for self- formance, a further meta-analysis in the review3 found no
care and mobility. For these reasons, optimizing the ability evidence that sit-to-stand exercise programmes improved
to sit-to-stand for these children may be a focus of ther- other functional activities, including mobility. A possible
apy. reason for changes not being detected in other outcomes
One systematic review3 of eight randomized controlled was that the prescribed exercise dose may have been inade-
trials investigated the effects of sit-to-stand exercise train- quate for motor learning. Exercise doses were typically
ing programmes on children and adults with physical similar to those associated with progressive resistance
impairments. Two of the trials included children with training regimens, that is, three sets of 10 repetitions three
CP.4,5 A meta-analysis within the review suggested that times a week for 6 weeks, with some progression of resis-
there was moderate-quality evidence that sit-to-stand exer- tance/intensity. While progressive resistance exercises
cise programmes can improve sit-to-stand performance. increase muscle strength in people with CP, there is evi-
This improvement was likely due to repetitive practice, dence that increases in strength do not carry over into
1476 DOI: 10.1111/dmcn.14979 © 2021 Mac Keith Press
14698749, 2021, 12, Downloaded from https://onlinelibrary.wiley.com/doi/10.1111/dmcn.14979 by Nat Prov Indonesia, Wiley Online Library on [20/02/2024]. See the Terms and Conditions (https://onlinelibrary.wiley.com/terms-and-conditions) on Wiley Online Library for rules of use; OA articles are governed by the applicable Creative Commons License
increased activity.10,11 A small case series reported that What this paper adds
more than 750 sit-to-stand repetitions throughout the • Sit-to-stand training improved independence in self-care and mobility for
intervention may be required to achieve independence in children with cerebral palsy (CP).
sit-to-stand and carry over to improvement in walking for • Home-based sit-to-stand training programmes for children with CP can
people with chronic stroke.12 Most trials in the systematic reduce the burden on supervising caregivers.
review, including the two trials that focused on children
consecutively numbered, sealed opaque envelopes. After
with CP,4,5 did not complete that number of sit-to-stand
written informed consent had been obtained and baseline
repetitions. So it remains possible that implementation of
testing was completed, the trial coordinator allocated the
programmes for children with CP that are more consistent
children by opening the next sealed envelope.
with the principles of motor learning and task-specific
training may improve not only sit-to-stand performance
Participants
but also carry over to improvements in mobility and self-
Children were included if they had any type of CP (e.g. spas-
care functions that are typically performed in an upright
tic, athetoid, ataxic) classified in GMFCS levels III and IV,
stance.
were aged 4 to 12 years (inclusive), were able to sit-to-stand
Inspection of the two trials that included children with
with or without the assistance of caregiver or furniture with-
CP4,5 also showed that the effects of sit-to-stand exercise
out falling, and could follow simple verbal instruction, such
programmes for children classified in GMFCS levels III
as ‘Stand up, please’. Children were excluded if they had
and IV who, by definition of their disability, have quite
undergone an orthopaedic intervention, selective dorsal rhi-
severe difficulty moving from sit-to-stand independently, is
zotomy, or botulinum neurotoxin A injection to the lower
unknown. This is because both previous trials recruited
limbs within the previous 6 months or had any orthopaedic
children with relatively mild disability (GMFCS levels I
problems or medical conditions, such as osteogenesis imper-
and II with only a few classified in level III), who typically
fecta, arthrogryposis multiplex congenita, or spinal muscular
have little difficulty moving from sitting to standing inde-
atrophy that prevented participation in intensive exercise
pendently. It is assumed that relatively close caregiver
training. The primary caregivers of these children were
supervision of the children would be required for comple-
included if they spoke Thai fluently.
tion of a sufficient number of sit-to-stand repetitions for
effective task-specific training. The amount of supervision
required plus changes in the interaction between parent Intervention
and child during training could lead to increased caregiver Both groups received routine physiotherapy for 30 minutes
strain, particularly within a demanding programme.13,14 five times a week for 6 weeks. Two of these sessions were
Accordingly, our primary aim was to investigate the conducted in a quiet private training room and were super-
effects of sit-to-stand exercise training on self-care function vised by one of two registered physiotherapists and three
and independent upright mobility for children with CP in sessions were conducted at home and supervised by the
GMFCS levels III and IV. The secondary aims were to child’s primary caregiver. The routine physiotherapy pro-
evaluate the effects of the training on sit-to-stand perfor- gramme consisted of balance and gait training with the assis-
mance and caregiver strain. tive device orthosis that the child normally wore. In
addition, at each exercise session the experimental group
METHOD received 30 minutes of a sit-to-stand training programme
Design according to the principles of task-specific training focusing
A single-blind randomized controlled trial was conducted on three phases: repetition of part of the sit-to-stand task
using two parallel groups with one-to-one allocation. The (e.g. foot placement, forward weight shift); repetition of all
trial was conducted at a rehabilitation centre and physio- the sit-to-stand movement along with feedback; and repeti-
therapy unit in Thailand from 28th November 2019 to tion of the sit-to-stand movement applied within the context
27th March 2020 with a home exercise component of self-care tasks (e.g. standing and reaching for a toy)
included. Ethical approval was obtained from La Trobe (Fig. 1). The training duration of 6 weeks was chosen to
University and Prince of Songkla University Human ensure that an adequate number of repetitions of sit-to-
Research Ethics committees. Children with CP were stand could be completed to transfer to improved activity,12
invited to provide their own verbal assent in addition to while taking account of the need to optimize adherence. To
their caregivers providing written informed consent for control for this additional time, the control group partici-
themselves and their child to participate. The study was pants received 30 minutes of hot pack application and
registered prospectively with the Australian New Zealand lower-limb stretching. A full description of the interven-
Clinical Trials Registry (ACTRN12619001525178) and tions, according to the template for intervention description
reported consistent with the Consolidated Standards of and replication,16 can be viewed in Tables 1 and 2.
Reporting Trials (CONSORT) checklist.15
An independent researcher prepared the random alloca- Outcome measures
tion sequence using permuted blocks, with children strati- All outcomes were measured at weeks 0 and 7 by an
fied by GMFCS level. Allocations were placed in accredited assessor blinded to group allocation.
Sit-to-Stand Exercise for Children with CP Sirawee Chaovalit et al. 1477
14698749, 2021, 12, Downloaded from https://onlinelibrary.wiley.com/doi/10.1111/dmcn.14979 by Nat Prov Indonesia, Wiley Online Library on [20/02/2024]. See the Terms and Conditions (https://onlinelibrary.wiley.com/terms-and-conditions) on Wiley Online Library for rules of use; OA articles are governed by the applicable Creative Commons License
(a) (b)
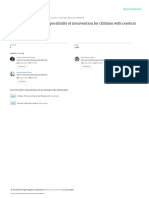
Figure 1: Examples of the sit-to-stand training. (a) Phase 1 repetition of part of the sit-to-stand task: forward weight shift. (b) Phase 2 repetition of all
the sit-to-stand movement along with feedback.
Table 1: Intervention: experimental group
TIDieR criteria Experimental group
Name Sit-to-stand exercise programme
Why Improving mobility and self-care functions
What Children received 1 hour of physiotherapy:
30 minutes of routine physiotherapy: 15 minutes of balance training in sitting and standing with progressions
including changing the base of support, increasing the time maintained, and superimposing movement while
maintaining balance; 15 minutes of overground walking training with the assistive device orthosis that the child
usually uses. Progressions included increasing distance and walking with reduced support
30 minutes of sit-to-stand training (three phrases): (1) repetition of part of the sit-to-stand task (e.g. foot placement,
forward weight shift); (2) repetition of all the sit-to-stand movement along with feedback; (3) progression: repeti-
tion of all the sit-to-stand movement applied within the context of self-care tasks (e.g. sit-to-stand with reaching
for a toy)
Who provided it Two physiotherapists experienced in working with children with cerebral palsy for more than 10 years at the unit
where the study was conducted; child’s caregiver for the home programme
How Individually, face to face, one physiotherapist per one child; individually, face to face, one caregiver per one child
Where Two days a week in a quiet private training room located in the physiotherapy unit in Thailand; 3 days a week at the
child’s home
When and how Training duration: 6 weeks;
much Frequency of training: five times per week;
One hour per day, 2 days a week for the hospital-based sessions;
One hour per day, 3 days a week (on days not training with the physiotherapist) for the home-based programme;
Session length, 60 minutes (30 minutes of regular physiotherapy and 30 minutes of sit-to-stand training);
Total number of sessions: 30 sessions;
Intensity and volume:
Phase 1: practised until part-task completed;
Phase 2: three sets of 25 repetitions of sit-to-stand, resting 2–3 minutes between each set;
Phase 3: individualized according to ability
Tailoring Details of the balance and walking training were individualized depending on each child’s abilities; the progression of
the sit-to-stand task from phases 1 to 3 with increasing difficulty was implemented according to each child’s ability
Modifications The intervention was not modified during the study
How well An independent physiotherapist monitored treatment once weekly to ensure that treatment was implemented as
planned; an exercise diary was provided to therapists and caregivers to record data about: total number of sessions,
reasons for any non-attendance, occurrence of any adverse events, number of repetitions of sit-to-stand completed
in phase 2 in each exercise session. An updated video recording of the sit-to-stand home programme was provided
to the caregiver once each week
TIDieR, template for intervention description and replication.
The primary outcome measures were the 11 items of complete independence, with scores summed for each
the self-care and mobility domains of the Functional domain.17 The minimum clinically important differences
Independence Measure for Children (WeeFIM).17 There for children classified in GMFCS level III were 3.3 units
are six items for self-care and five items for mobility. The for the WeeFIM self-care and 2.7 units for mobility.18
WeeFIM assesses the amount of assistance required from The minimum clinically important differences for large
a helper to complete all of the task components; a score effects were 5.2 units for self-care and 4.3 units for
of 1 is defined as total assistance and 7 is defined as mobility.18
1478 Developmental Medicine & Child Neurology 2021, 63: 1476–1482
14698749, 2021, 12, Downloaded from https://onlinelibrary.wiley.com/doi/10.1111/dmcn.14979 by Nat Prov Indonesia, Wiley Online Library on [20/02/2024]. See the Terms and Conditions (https://onlinelibrary.wiley.com/terms-and-conditions) on Wiley Online Library for rules of use; OA articles are governed by the applicable Creative Commons License
Table 2: Intervention: control group
TIDieR criteria Control group
Name Routine physiotherapy programme
Why Improving mobility and self-care functions
What Children received 1 hour of physiotherapy:
30 minutes of routine physiotherapy: 15 minutes of balance training in sitting and standing with progressions
including changing the base of support, increasing time maintained, and superimposing movement while main-
taining balance; 15 minutes of walking training with the assistive device orthosis that the individual child usually
uses. Progressions included increasing distance and walking with reduced support
In addition, to account for the time receiving the intervention in the experimental group children received: 15 min-
utes of a hot pack applied to both lower limbs; 15 minutes of stretching to both lower limbs
Who provided it Two physiotherapists experienced in working with children with cerebral palsy for more than 10 years at the unit
where the study was conducted; child’s caregiver for the home programme
How Individually, face to face, one physiotherapist per one child; individually, face to face, one caregiver per one child
Where Two days a week in a quiet private training room located in the physiotherapy unit in Thailand; 3 days a week at the
child’s home
When and how Training duration: 6 weeks;
much Frequency of training: five times per week;
One hour per day, 2 days a week for the hospital-based sessions;
One hour per day, 3 days a week (on days not training with the physiotherapist) for the home-based programme;
Session length: 60 minutes (30 minutes of regular physiotherapy and 30 minutes of hot pack and stretching);
Total number of sessions: 30
Tailoring Details of the balance training and walking training were individualized dependent on each child’s abilities
Modifications The intervention was not modified during the study
How well An independent physiotherapist monitored treatment once weekly to ensure that treatment was implemented as
planned;
An exercise diary was provided to the therapists and the caregivers to record data about: the total number of
sessions, the reasons for any non-attendance, occurrence of any adverse events
TIDieR, template for intervention description and replication.
Secondary outcomes were sit-to-stand performance covariance is robust to violations of the assumption of nor-
assessed using the time taken to stand up and sit down mality.22 Consistent with the principle of intention to
from a chair five times as quickly as possible (Five Times treat, all available data were analysed according to group
Sit-to-Stand Test [FTSST])19 and the 13-item Modified allocation, without adjusting for the level of adherence.
Caregiver Strain Index (MCSI),20 with caregiver responses Between-group differences were reported as mean differ-
on a 0 to 2 scale summed to provide a score out of 26, ences with 95% confidence intervals (CIs). Statistical sig-
with higher scores being indicative of higher levels of nificance was set at a=0.05. Data analysis was completed
strain associated with caregiving. The minimum clinically using SPSS v25.0 (IBM Corp., Armonk, NY, USA).
important differences for the FTSST and MCSI were Attendance was expressed as the percentage of sessions
based on 0.5 of the baseline standard deviation (SD) of the attended (ratio of the number of training sessions attended
control group.21 Attendance at training sessions, adherence to the total number of sessions prescribed multiplied by
to training protocols during sessions, and adverse events 100); reasons for non-attendance were also recorded.
for both home and rehabilitation centre sessions were Adherence to exercise prescription within sessions was cal-
recorded. The results of a qualitative analysis of caregiver culated as the number of repetitions of sit-to-stand com-
perceptions of the sit-to-stand training programme will be pleted in each session as a proportion of the number
reported elsewhere. prescribed by the physiotherapist. Adverse events were cat-
egorized as serious or non-serious. Non-serious events
Data analysis were defined as those not needing medical attention and
A sample size of 42 participants (21 in each group) was not causing children to miss exercise sessions. Serious
required to detect a large clinically important difference adverse events were defined as events (such as a serious
(d=0.8) in the self-care (5.2 units/42) and mobility (4.3 fall) that resulted in injury and resulted in missed training
units/35) domains of the WeeFIM18 at a type I error rate sessions.
of 0.05 and power (1 – type II error rate) of 0.7.
Descriptive statistics were used to describe the demo- RESULTS
graphic characteristic of participants (Table 3). Analysis of Participant characteristics
covariance was used to compare the main outcomes of the Forty children with CP and their caregivers were identified
primary and secondary continuous outcomes between con- for possible participation. Two children were excluded
trol and experimental groups at week 7 using the baseline because they had received botulinum neurotoxin A injec-
value as the covariate. Inspection of data and Shapiro– tions to their lower limbs within the previous 6 months.
Wilks tests (p>0.05) confirmed that the distributions did Therefore, 38 children with CP (19 males, 19 females;
not violate the assumption of normality. Analysis of mean age 8y 0mo, SD 2y 4mo, age range 4y 0mo–12y
Sit-to-Stand Exercise for Children with CP Sirawee Chaovalit et al. 1479
14698749, 2021, 12, Downloaded from https://onlinelibrary.wiley.com/doi/10.1111/dmcn.14979 by Nat Prov Indonesia, Wiley Online Library on [20/02/2024]. See the Terms and Conditions (https://onlinelibrary.wiley.com/terms-and-conditions) on Wiley Online Library for rules of use; OA articles are governed by the applicable Creative Commons License
Table 3: Baseline demographic characteristics of participants
self-care (3.1 units) was close to but still less than the min-
imum clinically significant difference of 3.3 units. The
Randomized and com- upper band of the 95% CI for mobility (3.0 units)
pleted the study (n=38)
exceeded the minimum clinically significant difference of
Exp-STS Controls 2.7 units.
Characteristic (n=19) (n=19)
Children (n=38) Secondary outcomes: FTSST and MCSI
Mean age (SD), y:mo 7:2 (2:1) 8:8 (2:5) The sit-to-stand group reduced their FTSST by a mean of
Sex, male 10 (53) 9 (47)
GMFCS level (III/IV), n 8/11 8/11
4.0 seconds (95% CI 4.7 to 3.2) and reduced their
Type of CP MCSI by a mean of 0.8 units (95% CI 1.2 to 0.4) com-
Unilateral spastic 1 (5) 2 (11) pared to the control group (Table 4). The upper band of
Bilateral spastic 17 (90) 15 (79)
Ataxic 0 (0) 1 (5)
the 95% CI of the FTSST (4.7s) exceeded the minimum
Dyskinetic 1 (5) 0 (0) clinically significant difference of 4.2 seconds. The upper
Mixed 0 (0) 1 (5) band of the 95% CI of the MCSI (1.2 units) was less than
Primary caregivers (n=38)
Mean age (SD), y:mo 39:6 (8:4) 40:3 (8:1)
the minimum clinically significant difference (1.8 units)
Sex, female 17 (90) 18 (95) (Table 4).
Education Attendance was excellent in both groups: 93% (mean
High school 4 (21) 4 (21)
Diploma 5 (26) 6 (32)
27.8 out of 30 sessions) for the experimental group and
Bachelor’s degree 10 (53) 9 (48) 90% (mean 26.9 out of 30 sessions) for the control group.
Master’s degree – – There was 100% attendance at the scheduled 12 sessions
Doctoral or professional degree – –
Occupation
supervised by the physiotherapists in both groups but chil-
Home duties 12 (63) 10 (53) dren in the control group missed more scheduled home-
Farmer 4 (21) 5 (27) based sessions (p=0.033). The caregiver being busy was the
Childcare worker – 2 (11)
Other (self-employed, retired 3 (16) 2 (11)
main reason for missed sessions, both in the control (32
government staff) sessions) and experimental groups (40 sessions). Other rea-
sons for non-attendance were illness (experimental n=3 ses-
Data are n (%) unless otherwise stated. Exp-STS, experimental sit-
to-stand group; GMFCS, Gross Motor Function Classification Sys- sions, control n=2), the child refusing to participate due to
tem; CP, cerebral palsy. boredom or fatigue (experimental n=2 sessions, control
n=12), and clashes with other appointments (experimental
4mo) classified in GMFCS levels III and IV and their care- n=4 sessions, control n=5). The mean number of sit-to-
givers were included (Table 3 and Fig. S1, online support- stand repetitions completed within each session in the
ing information). No one dropped out and everyone experimental group was 65.7 (SD 2.5). The average num-
completed the follow-up assessment at week 7 (Fig. S1). ber of repetitions of sit-to-stand completed when the ses-
The two groups were similar in age, sex, and distribution sion was supervised by a physiotherapist was 67.8 (SD 2.3)
of GMFCS levels. compared with an average of 64.1 (SD 2.8) when the ses-
sion was supervised by the caregiver. The mean number of
Primary outcomes: self-care and mobility domain of the sit-to-stand repetitions completed over the 6-week pro-
WeeFIM gramme was 1960.3 (SD 76.1).
The sit-to-stand group improved self-care by a mean of No serious adverse events, such as falls, were reported in
2.2 units (95% CI 1.3–3.1) and improved mobility by a either group. Only non-serious adverse events were
mean of 2.2 units (95% CI 1.4–3.0) compared to the con- reported in a mean of 13.1 sessions out of 30 for the
trol group (Table 4). The upper band of the 95% CI for experimental group and 10.1 sessions out of 30 sessions for
Table 4: Mean (SD) of groups, mean (SD) difference within groups, and mean (95% CI) between-group difference
Difference within
Groups groups Difference between groups
Week 0 Week 7 Week 7 minus week 0 Week 7 minus week 0
Outcomes Exp (n=19) Controls (n=19) Exp (n=19) Controls (n=19) Exp Controls Exp minus controls
WeeFIM self-care (6–42) 18.5 (4.7) 17.3 (4.4) 21.0 (5.0) 17.7 (4.3) 2.5 (1.9) 0.4 (0.6) 2.2 (1.3–3.1)
WeeFIM mobility (5–35) 14.4 (4.5) 14.3 (4.8) 17.1 (5.0) 14.7 (4.8) 2.6 (1.4) 0.4 (1.0) 2.2 (1.4–3.0)
Total WeeFIM (11–77) 32.9 (8.5) 31.6 (8.9) 38.1 (9.5) 33.0 (8.9) 5.2 (2.5) 1.3 (2.6) 3.8 (2.1–5.5)
FTSST (s) 32.0 (7.4) 36.9 (8.5) 28.9 (7.7) 38.0 (9.2) 3.2 (1.1) 1.1 (1.2) 4.0 ( 4.7 to 3.2)
MCSI (0–26) 11.84 (3.0) 14.11 (3.7) 11.0 (2.9) 14.1 (3.5) 0.9 (0.5) 0.1 (0.5) 0.8 ( 1.2 to 0.4)
CI, confidence interval; Exp, experimental group; WeeFIM, Functional Independence Measure for Children; FTSST, Five Time Sit-to-Stand
Test; MCSI, Modified Caregiver Strain Index.
1480 Developmental Medicine & Child Neurology 2021, 63: 1476–1482
14698749, 2021, 12, Downloaded from https://onlinelibrary.wiley.com/doi/10.1111/dmcn.14979 by Nat Prov Indonesia, Wiley Online Library on [20/02/2024]. See the Terms and Conditions (https://onlinelibrary.wiley.com/terms-and-conditions) on Wiley Online Library for rules of use; OA articles are governed by the applicable Creative Commons License
the control group. The most common non-serious event physical strain of caring on caregivers. It is also possible
reported was fatigue. that being actively involved in their child’s therapy may
have reduced the emotional strain contributing to caregiver
DISCUSSION burden. This is a positive finding for therapists since it
This trial demonstrated that a 6-week sit-to-stand exercise provides reassurance that prescribed exercise programmes
programme led to small improvements in the indepen- can be implemented at home without risk of increasing
dence of self-care and mobility of children with CP (classi- caregiver strain.
fied in GMFCS levels III and IV) and increased sit-to- Strengths of this trial included its randomized design
stand performance. The training programme was safe, was conducted and reported according to the CONSORT
adhered to by children and their caregivers, and was associ- guidelines. Our trial was a single-blind randomized con-
ated with small reductions in caregiver strain. Consistent trolled trial, with an accredited assessor blinded to group
with previous trials, we found that repetitive and intensive allocation. Additionally, the exercise training programmes
practice of a skill, such as sit-to-stand, can improve sit-to- had excellent compliance and there was no loss to follow-
stand performance.5,23 In contrast to other trials, our find- up. However, there were limitations. First, we only exam-
ings show that such a training programme can also lead to ined the impacts on outcomes after a relatively short pro-
small improvements in self-care and mobility. gramme; it is still unknown if larger improvements may
One explanation for the positive results of our trial com- have been found after a longer training programme or if
pared to previous trials was that we targeted our interven- benefits are retained after training stops. Second, while
tion at those children who were most likely to benefit, that attendance and adherence to the programme was excellent
is, those classified in GMFCS levels III and IV. Most of in this group of Thai participants, generalizability to other
the participants of previous trials were children with CP cultures is unknown. To optimize attendance and adher-
who had a mild-to-moderate disability. These children ence, a number of features were incorporated into the pro-
could already independently sit-to-stand with little diffi- gramme, such as the use of an exercise diary and
culty, so further training might reasonably not be expected individualized video recordings of the sit-to-stand pro-
to improve their abilities. In addition to targeting children gramme and weekly physiotherapy review.25 In Thai cul-
who were most likely to benefit from the sit-to-stand train- ture, children are expected to do as their parents and those
ing, we prescribed a training dose consistent with the prin- in authority instruct without choice.26 Therefore, the gen-
ciples of task-specific training. The training dose of eralizability of the findings to other cultures where compli-
previous trials may not have been adequate for task-specific ance with medical and therapeutic advice might not be
training to improve gross motor functions and learning to embraced so willingly by caregivers, and where children
develop skills in children with CP.4,5 Participants in our might be less willing to comply with directions, certainly
trial programme completed an average of almost 2000 rep- over so many sessions, is unknown.
etitions of sit-to-stand, a number shown to be sufficient to
train a task.12 CONCLUSION
Despite the statistically significant results favouring the A relatively short 6-week sit-to-stand exercise programme
sit-to-stand group, the size of the effect on self-care and led to small improvements in children’s ability to complete
mobility was relatively small. Based on the confidence mobility and self-care tasks, which may be clinically rele-
bands around the between-group mean differences relative vant for mobility and can improve sit-to-stand performance
to the minimum clinically significant differences, our without increasing caregiver strain. Our results provide
results suggest that the observed change in self-care was partial support for the importance of sit-to-stand as a pre-
not clinically significant, while the changes in mobility may cursor skill for developing safe and independent mobility
be clinically significant. Therefore, our results only par- for these children. Sit-to-stand training could be a useful
tially support the view that training sit-to-stand may be focus of therapy in children with moderate and severe CP
important for children with moderate-to-severe disability. (i.e. GMFCS levels III and IV).
It is possible that sit-to-stand training may be more rele-
vant for mobility in this group because the ability to get to A CK N O W L E D G E M E N T S
and maintain an upright position is fundamental to upright SC is a PhD student funded by the Faculty of Medicine, Prince
gait.24 In contrast, many self-care activities, such as those of Songkla University, Thailand. The authors report no conflicts
completed in sitting (e.g. feeding), are not dependent on of interest.
the ability to transfer safely and independently from sitting
to standing. DATA AVAILABILITY STATEMENT
Despite the potential additional strain of supervising the Encourages data sharing – data openly available in a public
sit-to-stand programme three times a week for 6 weeks, repository that issues datasets with DOIs.
there were small reductions in the strain experienced by
caregivers. Consistent with the results of the primary out- SUPPORTING INFORMATION
come, it suggested that the children may have improved The following additional material may be found online:
enough in their self-care and mobility to reduce the Figure S1: Design and flow of participants through the trial.
Sit-to-Stand Exercise for Children with CP Sirawee Chaovalit et al. 1481
14698749, 2021, 12, Downloaded from https://onlinelibrary.wiley.com/doi/10.1111/dmcn.14979 by Nat Prov Indonesia, Wiley Online Library on [20/02/2024]. See the Terms and Conditions (https://onlinelibrary.wiley.com/terms-and-conditions) on Wiley Online Library for rules of use; OA articles are governed by the applicable Creative Commons License
REFERENCES
1. Palisano RJ, Rosenbaum P, Bartlett D, Livingston MH. 10. Taylor NF, Dodd KJ, Baker RJ, Willoughby K, responsiveness and minimum clinically important differ-
Content validity of the expanded and revised Gross Thomason P, Graham HK. Progressive resistance train- ences. Dev Med Child Neurol 2008; 50: 918–25.
Motor Function Classification System. Dev Med Child ing and mobility-related function in young people with 19. Wang T-H, Liao H-F, Peng Y-C. Reliability and valid-
Neurol 2008; 50: 744–50. cerebral palsy: a randomized controlled trial. Dev Med ity of the five-repetition sit-to-stand test for children
2. Hanna SE, Rosenbaum PL, Bartlett DJ, et al. Stability Child Neurol 2013; 55: 806–12. with cerebral palsy. Clin Rehabil 2012; 26: 664–71.
and decline in gross motor function among children 11. Ryan JM, Lavelle G, Theis N, et al. Progressive resis- 20. Thornton M, Travis SS. Analysis of the reliability of
and youth with cerebral palsy aged 2 to 21 years. Dev tance training for adolescents with cerebral palsy: the the Modified Caregiver Strain Index. J Gerontol B Psy-
Med Child Neurol 2009; 51: 295–302. STAR randomized controlled trial. Dev Med Child Neu- chol Sci Soc Sci 2003; 58: S127–32.
3. Chaovalit S, Taylor NF, Dodd KJ. Sit-to-stand exercise rol 2020; 62: 1283–93. 21. Norman GR, Sloan JA, Wyrwich KW. Interpretation
programs improve sit-to-stand performance in people 12. Boyne P, Israel S, Dunning K. Speed-dependent body of changes in health-related quality of life: the remark-
with physical impairments due to health conditions: a weight supported sit-to-stand training in chronic stroke: able universality of half a standard deviation. Med Care
systematic review and meta-analysis. Disabil Rehabil a case series. J Neurol Phys Ther 2011; 35: 178–84. 2003; 41: 582–92.
2020; 42: 1202–11. 13. Novak I. Parent experience of implementing effective 22. Vickers AJ. Parametric versus non-parametric statistics
4. Liao H-F, Liu Y-C, Liu W-Y, Lin Y-T. Effectiveness home programs. Phys Occup Ther Pediatr 2011; 31: 198– in the analysis of randomized trials with non-normally
of loaded sit-to-stand resistance exercise for children 213. distributed data. BMC Med Res Methodol 2005; 5: 35.
with mild spastic diplegia: a randomized clinical trial. 14. Beckers LWME, Smeets RJEM, van der Burg JJW. 23. Tung F-L, Yang Y-R, Lee C-C, Wang R-Y. Balance
Arch Phys Med Rehabil 2007; 88: 25–31. Therapy-related stress in parents of children with a outcomes after additional sit-to-stand training in sub-
5. Kumban W, Amatachaya S, Emasithi A, Siritaratiwat physical disability: a specific concept within the con- jects with stroke: a randomized controlled trial. Clin
W. Effects of task-specific training on functional ability struct of parental stress. Disabil Rehabil 2021; 43: 1185– Rehabil 2010; 24: 533–42.
in children with mild to moderate cerebral palsy. Dev 92. 24. Chou S-W, Wong AMK, Leong C-P, Hong W-S,
Neurorehabil 2013; 16: 410–7. 15. Schulz KF, Altman DG, Moher D, CONSORT Group. Tang F-T, Lin T-H. Postural control during sit-to
6. Schmidt RA. Motor Control and Learning. 5th edn. CONSORT 2010 statement: updated guidelines for stand and gait in stroke patients. Am J Phys Med Rehabil
Champaign, IL: Human Kinetics, 2005. reporting parallel group randomised trials. BMJ 2010; 2003; 82: 42–7.
7. Hubbard IJ, Parsons MW, Neilson C, Carey LM. 340: c332. 25. Taylor NF, Dodd KJ, McBurney H, Graham HK. Fac-
Task-specific training: evidence for and translation to 16. Hoffmann TC, Glasziou PP, Boutron I, et al. Better tors influencing adherence to a home-based strength-
clinical practice. Occup Ther Int 2009; 16: 175–89. reporting of interventions: template for intervention training programme for young people with cerebral
8. Geijen M, Ketelaar M, Sakzewski L, Palisano R, description and replication (TIDieR) checklist and palsy. Physiotherapy 2004; 90: 57–63.
Rameckers E. Defining functional therapy in research guide. BMJ 2014; 348: g1687. 26. Earde PT, Praipruk A, Rodpradit P, Seanjumla P.
involving children with cerebral palsy: a systematic 17. Msall ME, DiGaudio K, Rogers BT, et al. The Func- Facilitators and barriers to performing activities and
review. Phys Occup Ther Pediatr 2020; 40: 231–46. tional Independence Measure for Children (WeeFIM). participation in children with cerebral palsy: caregivers’
9. Toovey R, Bernie C, Harvey AR, McGinley JL, Spittle Conceptual basis and pilot use in children with devel- perspective. Pediatr Phys Ther 2018; 30: 27–32.
AJ. Task-specific gross motor skills training for ambu- opmental disabilities. Clin Pediatr 1994; 33: 421–30.
lant school-aged children with cerebral palsy: a system- 18. Oeffinger D, Bagley A, Rogers S, et al. Outcome tools
atic review. BMJ Paediatr Open 2017; 1: e000078. used for ambulatory children with cerebral palsy:
1482 Developmental Medicine & Child Neurology 2021, 63: 1476–1482
You might also like
- Metaboost Shopping List RecipesDocument38 pagesMetaboost Shopping List Recipesserpico7188% (16)
- Physical Education and Health 3 Grade 12 Module 1Document24 pagesPhysical Education and Health 3 Grade 12 Module 1Dame Iris Zamora95% (20)
- PBS PrintDocument20 pagesPBS Printlisa ekaNo ratings yet
- Occt643 - Cat Paper Systematic ReviewDocument10 pagesOcct643 - Cat Paper Systematic Reviewapi-293182319No ratings yet
- 21 Day Fat Loss Nutrition Program Book PDFDocument89 pages21 Day Fat Loss Nutrition Program Book PDFJohnDNo ratings yet
- Willoughby Et Al. (2010)Document7 pagesWilloughby Et Al. (2010)ع الNo ratings yet
- Entrenamiento de resistencia progresiva y función relacionada con la movilidad en jóvenes con parálisis cerebral un ensayo controlado aleatorioDocument7 pagesEntrenamiento de resistencia progresiva y función relacionada con la movilidad en jóvenes con parálisis cerebral un ensayo controlado aleatorioEnrique Benavente AliagaNo ratings yet
- Develop Med Child Neuro - 2014 - Dewar - Exercise Interventions Improve Postural Control in Children With Cerebral Palsy ADocument17 pagesDevelop Med Child Neuro - 2014 - Dewar - Exercise Interventions Improve Postural Control in Children With Cerebral Palsy AEvelyn_D_az_Ha_8434No ratings yet
- The Effects of Therapeutic Taping On Gross Motor Function in Children With Cerebral PalsyDocument8 pagesThe Effects of Therapeutic Taping On Gross Motor Function in Children With Cerebral PalsyDenise PereiraNo ratings yet
- Gates Et Al. (2012)Document35 pagesGates Et Al. (2012)ع الNo ratings yet
- Effects of A Supported Speed Treadmill Training Exercise Program On Impairment and Function For Children With Cerebral PalsyDocument9 pagesEffects of A Supported Speed Treadmill Training Exercise Program On Impairment and Function For Children With Cerebral PalsyKimum KimúmNo ratings yet
- Strength Training Adolescent Learners With Cerebral Palsy: Randomized ControlledDocument9 pagesStrength Training Adolescent Learners With Cerebral Palsy: Randomized ControlledtiaraaaindahNo ratings yet
- Exercise Interventions Improve Postural Control in Children With Cerebral Palsy: A Systematic ReviewDocument17 pagesExercise Interventions Improve Postural Control in Children With Cerebral Palsy: A Systematic ReviewEmad Eldin Mohamed AbdelatiefNo ratings yet
- 5a21 PDFDocument15 pages5a21 PDFekaNo ratings yet
- In Home Mobility Training With A Portable Body.27Document7 pagesIn Home Mobility Training With A Portable Body.27dr Harien LestariNo ratings yet
- Características Asociadas Con La Actividad Física Entre Niños y Adolescentes Con Parálisis Cerebral Unilateral Que Caminan de Forma IndependienteDocument8 pagesCaracterísticas Asociadas Con La Actividad Física Entre Niños y Adolescentes Con Parálisis Cerebral Unilateral Que Caminan de Forma IndependienteKimum KimúmNo ratings yet
- Investigeting The Effects of Standing Training On Body Functions and Activity For Nonambulatory Children With MyelomeningoceleDocument6 pagesInvestigeting The Effects of Standing Training On Body Functions and Activity For Nonambulatory Children With MyelomeningoceleMutiarahmiNo ratings yet
- Plyometric Training Effectiveness and Optimal.3Document11 pagesPlyometric Training Effectiveness and Optimal.3LeonardoValenzuelaNo ratings yet
- Develop Med Child Neuro - 2015 - Kruijsen Terpstra - Efficacy of Three Therapy Approaches in Preschool Children WithDocument9 pagesDevelop Med Child Neuro - 2015 - Kruijsen Terpstra - Efficacy of Three Therapy Approaches in Preschool Children Withkitten 25No ratings yet
- The Use of Dynamic Weight Support With Principles of Infant Learning in A Child With Cerebral Palsy: A Case ReportDocument11 pagesThe Use of Dynamic Weight Support With Principles of Infant Learning in A Child With Cerebral Palsy: A Case ReportomenpkuNo ratings yet
- Brazilian Journal of Physical TherapyDocument11 pagesBrazilian Journal of Physical TherapyshodhgangaNo ratings yet
- Kassim 2022Document12 pagesKassim 2022ع الNo ratings yet
- A Comparison Between Single Task Versus Dual Task Condition Balance Training in Older Adults With Balance ImpairmentDocument6 pagesA Comparison Between Single Task Versus Dual Task Condition Balance Training in Older Adults With Balance ImpairmentDhiyo Areza PrastyatamaNo ratings yet
- Interventions To Promote Physical Activity in Young ChildrenDocument5 pagesInterventions To Promote Physical Activity in Young ChildrenJhonnyNogueraNo ratings yet
- Effect of Core Stability Exercises and Treadmill Training On Balance in Children With Down Syndrome - Randomized Controlled TrialDocument10 pagesEffect of Core Stability Exercises and Treadmill Training On Balance in Children With Down Syndrome - Randomized Controlled TrialGayuh Candra BuanaNo ratings yet
- August I JN 2018Document10 pagesAugust I JN 2018Alyce RodriguesNo ratings yet
- Develop Med Child Neuro - 2011 - SAKZEWSKI - Randomized trial of constraint‐induced movement therapy and bimanual trainingDocument8 pagesDevelop Med Child Neuro - 2011 - SAKZEWSKI - Randomized trial of constraint‐induced movement therapy and bimanual trainingrishivivek55No ratings yet
- Develop Med Child Neuro - 2021 - Jackman - Interventions To Improve Physical Function For Children and Young People WithDocument14 pagesDevelop Med Child Neuro - 2021 - Jackman - Interventions To Improve Physical Function For Children and Young People WithBruna SalvadorNo ratings yet
- A Novel Sensorimotor Movement and Walking Intervention To Improve Balance and Gait in WomenpdfDocument6 pagesA Novel Sensorimotor Movement and Walking Intervention To Improve Balance and Gait in WomenpdfCarmen LlerenasNo ratings yet
- Physiotherapy: J o U R N A L o FDocument10 pagesPhysiotherapy: J o U R N A L o FImran TarmiziNo ratings yet
- Exoskeleton SCIDocument11 pagesExoskeleton SCIsana siddiqueNo ratings yet
- Refinement, Reliability, and Validity of The Segmental Assessment of Trunk ControlDocument12 pagesRefinement, Reliability, and Validity of The Segmental Assessment of Trunk ControlBeverly IgartuaNo ratings yet
- PC Bobtah EfectosDocument7 pagesPC Bobtah EfectosConstanzza Arellano LeivaNo ratings yet
- Neurodesarrollo Bobath PDFDocument7 pagesNeurodesarrollo Bobath PDFCarol SanchezNo ratings yet
- Effectiveness of Proprioceptive Training Over Strength Training in Improving The Balance of Cerebral Palsy Children With Impaired BalanceDocument14 pagesEffectiveness of Proprioceptive Training Over Strength Training in Improving The Balance of Cerebral Palsy Children With Impaired BalanceDr. Krishna N. SharmaNo ratings yet
- The Association Between Functional Movement and Overweight and Obesity in British Primary School ChildrenDocument8 pagesThe Association Between Functional Movement and Overweight and Obesity in British Primary School ChildrenHanna RikaswaniNo ratings yet
- Effectiveness of Physiotherapy For Children With Spastic Diplegic Cerebral Palsy A Case Report FUL9Document3 pagesEffectiveness of Physiotherapy For Children With Spastic Diplegic Cerebral Palsy A Case Report FUL9ammarsalama997No ratings yet
- Influence of Sequential vs. Simultaneous Dual-Task Exercise Training On Cognitive Function in Older AdultsDocument10 pagesInfluence of Sequential vs. Simultaneous Dual-Task Exercise Training On Cognitive Function in Older AdultsSamara DiasNo ratings yet
- The Trunk Control Measurement Scale: Reliability and Discriminative Validity in Children and Young People With Neuromotor DisordersDocument7 pagesThe Trunk Control Measurement Scale: Reliability and Discriminative Validity in Children and Young People With Neuromotor DisordersDesak AgungNo ratings yet
- BMC PediatricsDocument11 pagesBMC PediatricsMica FrediNo ratings yet
- Cimt in Children WTH CP: Sample Measures/ FindingsDocument6 pagesCimt in Children WTH CP: Sample Measures/ Findingsapi-253994356No ratings yet
- Aricol IMC Si EscaladaDocument5 pagesAricol IMC Si EscaladacristinaelenazahariaNo ratings yet
- ASSIGNEMNT2Document5 pagesASSIGNEMNT2Jessica SebastianNo ratings yet
- Develop Med Child Neuro - 2014 - Curtis - The Central Role of Trunk Control in The Gross Motor Function of Children WithDocument7 pagesDevelop Med Child Neuro - 2014 - Curtis - The Central Role of Trunk Control in The Gross Motor Function of Children WithAmr Mohamed GalalNo ratings yet
- Educational Perspectives: Educational Strategies To Improve Outcomes From Neonatal ResuscitationDocument13 pagesEducational Perspectives: Educational Strategies To Improve Outcomes From Neonatal ResuscitationDian RahmawatiNo ratings yet
- An Intensive Virtual Reality Program Improves Functional Balance and Mobility of Adolescents With Cerebral PalsyDocument9 pagesAn Intensive Virtual Reality Program Improves Functional Balance and Mobility of Adolescents With Cerebral PalsyStephGrenNo ratings yet
- EBN Cerebral Palsy.1Document7 pagesEBN Cerebral Palsy.1chelle_asenjoNo ratings yet
- Gawel 2012Document9 pagesGawel 2012Leonardo MacedaNo ratings yet
- Tdcs Inglês 1Document8 pagesTdcs Inglês 1Augusto ManoelNo ratings yet
- Develop Med Child Neuro - 2020 - Ryan - Progressive Resistance Training For Adolescents With Cerebral Palsy The STARDocument12 pagesDevelop Med Child Neuro - 2020 - Ryan - Progressive Resistance Training For Adolescents With Cerebral Palsy The STARAkun NgasalNo ratings yet
- Haga2008Physiotherapy94253 9Document8 pagesHaga2008Physiotherapy94253 9Patrick ManatadNo ratings yet
- 09mjms2703 Oa6Document9 pages09mjms2703 Oa6BADLISHAH BIN MURAD MoeNo ratings yet
- Lowe 2015Document9 pagesLowe 2015ﻱﺪﺢ ﺁﻏﻦﻎNo ratings yet
- Develop Med Child Neuro - 2021 - Jackman - Interventions To Improve Physical Function For Children and Young People WithDocument14 pagesDevelop Med Child Neuro - 2021 - Jackman - Interventions To Improve Physical Function For Children and Young People WithMaria Alejandra MayaNo ratings yet
- The SCI Exercise Self-Efficacy Scale (ESES) : Development and Psychometric PropertiesDocument6 pagesThe SCI Exercise Self-Efficacy Scale (ESES) : Development and Psychometric PropertiesInês SacaduraNo ratings yet
- Enjoyment of Physical Activity-Not MVPA During Physical Education-Predicts Future MVPA Participation and Sport Self-Concept - 2021-MDPIDocument12 pagesEnjoyment of Physical Activity-Not MVPA During Physical Education-Predicts Future MVPA Participation and Sport Self-Concept - 2021-MDPIJoana CabralNo ratings yet
- (129 136) V9N5PTDocument8 pages(129 136) V9N5PTAqila NurNo ratings yet
- Computerizing WM TrainingDocument7 pagesComputerizing WM TrainingCynthia Torres-GonzálezNo ratings yet
- Nihms 105659 PDFDocument14 pagesNihms 105659 PDFGita TikihaiNo ratings yet
- Scholtes 2010Document7 pagesScholtes 2010Camille Louise LlaveNo ratings yet
- PREFIT MANUAL - Assessing FITness in PREschoolers - 14thsept2017Document34 pagesPREFIT MANUAL - Assessing FITness in PREschoolers - 14thsept2017Natalia GutierrezNo ratings yet
- DSC PositionDocument5 pagesDSC PositionKanhu Charan DigalNo ratings yet
- Assessing Neuromotor Readiness for Learning: The INPP Developmental Screening Test and School Intervention ProgrammeFrom EverandAssessing Neuromotor Readiness for Learning: The INPP Developmental Screening Test and School Intervention ProgrammeRating: 5 out of 5 stars5/5 (1)
- Physical Fitness - Prelim CoverageDocument13 pagesPhysical Fitness - Prelim CoverageFasra ChiongNo ratings yet
- 424-Psyconurobic Practice For Self HealingDocument15 pages424-Psyconurobic Practice For Self HealingZalinah Mohd YusofNo ratings yet
- Exercise and Disease Management Second Edition PDFDocument253 pagesExercise and Disease Management Second Edition PDFGajen Singh100% (1)
- Jhoanna Salve S. Bordeos - Final RequirementsDocument16 pagesJhoanna Salve S. Bordeos - Final RequirementsJhoanna BordeosNo ratings yet
- Pe Week 1 and 2Document36 pagesPe Week 1 and 2Czarina GenteroyNo ratings yet
- Treadmill Spacer 3501 Treadmill InstructionsDocument28 pagesTreadmill Spacer 3501 Treadmill InstructionsChris TwiggerNo ratings yet
- Ebn 1Document14 pagesEbn 1Faisal HarisNo ratings yet
- SHS Core - PE and Health CGDocument20 pagesSHS Core - PE and Health CGEthan Antoni Padua100% (1)
- Get Massive CompleteDocument26 pagesGet Massive CompleteDesitonic Gill100% (2)
- Maximum Aerobic Power Sample PDFDocument28 pagesMaximum Aerobic Power Sample PDFAdrianNo ratings yet
- Test Bank For Ebersole and Hess Gerontological Nursing and Healthy Aging 4th Edition TouhyDocument14 pagesTest Bank For Ebersole and Hess Gerontological Nursing and Healthy Aging 4th Edition Touhygrinting.creation4qlo100% (52)
- Physical Education. Physical Education Is "Education Through The Physical". It Aims ToDocument12 pagesPhysical Education. Physical Education Is "Education Through The Physical". It Aims Tokeanee simbajonNo ratings yet
- 1 STDocument5 pages1 STRyahNeil Bohol MoralesNo ratings yet
- The Importance of Regular Physical ActivityDocument23 pagesThe Importance of Regular Physical ActivityNagy KlaraNo ratings yet
- P.E. TestDocument1 pageP.E. TestAlbert Ian CasugaNo ratings yet
- Pe 8 - Curriculum - MapDocument2 pagesPe 8 - Curriculum - MapJohn Kenneth MejoradaNo ratings yet
- Chapter 1. Physical Activity and Exercise: Learning OutcomesDocument47 pagesChapter 1. Physical Activity and Exercise: Learning Outcomeszuong559No ratings yet
- Lecture 5 Kinesiology 2-2Document37 pagesLecture 5 Kinesiology 2-2Syeda Abida Hussain SheraziNo ratings yet
- City Schools Division Office of AntipoloDocument23 pagesCity Schools Division Office of AntipoloEnrico TzuNo ratings yet
- Module Physical Education G11 Lesson 1Document2 pagesModule Physical Education G11 Lesson 1chiarakim2428No ratings yet
- Aspects of The SelfDocument53 pagesAspects of The SelfNiña Mariel MendozaNo ratings yet
- Fourth Grading Exam in MAPEH-10Document3 pagesFourth Grading Exam in MAPEH-10Reymundo PenialaNo ratings yet
- Health Understanding Weight Loss 2021Document100 pagesHealth Understanding Weight Loss 2021svetlanaNo ratings yet
- Manual G9SDocument112 pagesManual G9SRafiHunJianNo ratings yet
- Discharge Planning and NCP SDocument8 pagesDischarge Planning and NCP SRainier RamosNo ratings yet
- Lesson 1: Understanding The Aerobics Exercise: College of Human KineticsDocument7 pagesLesson 1: Understanding The Aerobics Exercise: College of Human KineticsCamille CarengNo ratings yet
- Chapter 3 - Types of Physical ActivitiesDocument97 pagesChapter 3 - Types of Physical ActivitiesNicole CuteNo ratings yet