Professional Documents
Culture Documents
Uploads-Lectureforum-Jomi 17 4 Cooper
Uploads-Lectureforum-Jomi 17 4 Cooper
Uploaded by
Daniel AtiehOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Uploads-Lectureforum-Jomi 17 4 Cooper
Uploads-Lectureforum-Jomi 17 4 Cooper
Uploaded by
Daniel AtiehCopyright:
Available Formats
Immediate Mandibular Rehabilitation with
REPRODUCED OR TRANSMITTED IN ANY FORM WITHOUT WRITTEN PERMISSION FROM THE PUBLISHER.
COPYRIGHT © 2002 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY. NO PART OF THIS ARTICLE MAY BE
Endosseous Implants: Simultaneous Extraction,
Implant Placement, and Loading
Lyndon F. Cooper, DDS, PhD1/Amin Rahman, BDS, MPH2/John Moriarty, DDS, MS2/
Nancy Chaffee, DDS, MS3/Debra Sacco, DDS, MS4
Purpose: This report of a clinical patient series indicates the relative safety and illustrates the proce-
dures involved in the extraction of remaining teeth followed by immediate implant placement and load-
ing with a simple acrylic resin fixed denture. Materials and Methods: Ten consecutive patients who
selected tooth extraction and implant-supported fixed denture rehabilitation of the mandible were
treated using a 1-visit approach for extraction, implant placement, and restoration. Healthy individuals
(10 women) were treated under local anesthesia. Fifty-four implants were placed in 10 patients. Five
or 6 Astra Tech implants (11 or 13 mm long) were placed into the edentulous parasymphyseal region
of the mandible. Four to 6 implants (48 of 54) were immediately loaded by the fabrication of a simple
acrylic resin fixed denture. The criterion for loading was clinical judgment of primary stability, ie, the
absence of axial or lateral mobility with physical resistance to rotation. Patients were recalled at 1, 3,
and 12 weeks. At 12 weeks, impressions were made for the fabrication of a screw-retained fixed den-
ture. The fixed dentures were completed using conventional fabrication and prosthetic techniques.
Results: After a period of 6 to 18 months, all 54 implants had survived and were considered 100%
successful by independent testing of mobility and radiographic evidence of osseointegration. There
were no surgical complications. Fracture and debonding of the acrylic resin provisional denture
occurred for 1 patient during the first 12 weeks of treatment. Discussion: Advantages to extraction
with simultaneous replacement include the maintenance of vertical dimension, elimination of reline
procedures and interim denture therapy, and potential improvement of soft tissue healing. Conclu-
sion: This therapeutic approach simplifies patient care without apparent additional risk. (INT J ORAL
MAXILLOFAC IMPLANTS 2002;17:517–525)
Key words: dental implants, dental prosthesis, immediate loading, immediate placement, mandible
T here are 25 to 45 million edentulous individu-
als in the United States. In some regions, the
prevalence of edentulism among individuals over 65
years of age approaches 50%.1 The available data
concerning endosseous implant utilization indicate
that fewer than 500,000 edentulous individuals have
had implants placed. Irrespective of the experimen-
1Associate Professor, Department of Prosthodontics, University of tal successes for endosseous implants, which repeat-
North Carolina School of Dentistry Bone Biology and Implant
edly exceed 95% in the parasymphyseal mandible,2–6
Therapy Laboratory, Chapel Hill, North Carolina.
2Associate Professor, Department of Periodontics, University of the public health care utilization of implant treat-
North Carolina School of Dentistry Bone Biology and Implant ment of mandibular edentulism may not exceed 5%.
Therapy Laboratory, Chapel Hill, North Carolina. One possible explanation for the disparity between
3Assistant Professor, Department of Prosthodontics, University of
the high success rate of this therapy and its low uti-
North Carolina School of Dentistry Bone Biology and Implant
lization may be the possible perception of low value
Therapy Laboratory, Chapel Hill, North Carolina.
4Assistant Professor, Department of Oral and Maxillofacial Surgery, of a therapy that requires many months for comple-
University of North Carolina School of Dentistry Bone Biology and tion and involves considerable expense.
Implant Therapy Laboratory, Chapel Hill, North Carolina. A growing body of data demonstrates that when
implants are placed with primary stability in the
Reprint requests: Dr Lyndon F. Cooper, Department of Prostho-
dontics, University of North Carolina, 404 Brauer Hall,
edentulous parasymphyseal mandible, immediate
CB #7450, Chapel Hill NC 27599. Fax: 919-966-3821. loading of the implants can be highly successful
E-mail: Lyndon_Cooper@dentistry.unc.edu (Table 1). Given the growing acceptance of 1-stage
The International Journal of Oral & Maxillofacial Implants 517
COOPER ET AL
REPRODUCED OR TRANSMITTED IN ANY FORM WITHOUT WRITTEN PERMISSION FROM THE PUBLISHER.
COPYRIGHT © 2002 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY. NO PART OF THIS ARTICLE MAY BE
Table 1 Summary of Published Immediate Loading Experience
Scope (no. Time to No. of implants/ Implant
Authors of patients) loading Location prosthesis type survival (%)
De Bruyn7 20 4 to 53 days* Edentulous mandible 3/FD 90
Grunder8† 10 24 hours Edentulous maxilla 4 or 5/FD 87.5
Edentulous mandible 97.26
Chow9 27 At surgery Edentulous mandible 5 to 8/FD 98.3
Chiapasco10 20 0 to 20 days Edentulous mandible 4/OD 97.5
Colomina11 13 2 weeks Edentulous mandible 5/FD 96.7
Brånemark et al12 50 At surgery Edentulous mandbile 3/FD 98
Horiuchi et al13 17 At surgery 12 mandibles/5 maxillae 8 to 10/FD 97.2
Jaffin et al14 27 At surgery 21 mandibles/6 maxillae 5 to 6/FD 97‡
Gatti et al15 21 2 to 20 days Edentulous mandible 4/OD 96
Cooper et al16 60 At surgery Edentulous mandible 2/OD 96.7
Randow et al17§ 16 20 days Edentulous mandible 5 to 6/FD 100
Chiapasco et al18 226 0 to 20 days Edentulous mandible 4/OD 96.9
Tarnow19 10 At surgery 6 mandibles/4 maxillae 5 of 10 loaded/FD 97.1
Balshi and Wolfinger20 10 At surgery Edentulous mandible 3 of 8 loaded/FD 84.7
Schnitman et al21 10 At surgery Edentulous mandbile 4 of 7 loaded/FD 96
Salama et al22 2 At surgery Edentulous mandible 5/FD 95
*Implants were loaded immediately after surgery by relined denture.
†Included 66 of 99 implants placed immediately after tooth extraction.
‡Excluding machined implants.
§Comparative study: 16 immediately loaded cases versus 11 conventionally loaded cases.
OD = overdenture; FD = fixed denture.
surgery and the published success for immediate patients seeking care at the University of North
loading, the process of rehabilitation of the edentu- Carolina Department of Prosthodontics during the
lous mandible can be considered in the context of period of September 1998 to December 2000. All
individuals who face extraction of remaining teeth, patients were in good general health and were able
interim complete dentures, and subsequent implant to undergo dental extraction and implant placement
therapy. While the staging of implant therapy using under local anesthesia. Because of the presence of
interim partial dentures and subsequent implant existing teeth, all mandibles were of sufficient bone
placement into extraction sockets is possible, the volume (greater than 15 mm inferior-superior
further possibility of extraction and simultaneous height) and sufficient bone density.
implant placement with immediate loading must
also be considered. Treatment Planning
It was the aim of this clinical patient series to Each patient underwent a comprehensive oral
define the limitations for treatment, refine the pros- examination and review of medical and dental his-
thetic procedures for immediate loading using a tory. A panoramic radiograph was obtained and
simple acrylic resin fixed denture, and evaluate the diagnostic casts were made. Additional tomograms
relative safety and efficacy of this approach to were made in select cases at the request of individ-
mandibular dental rehabilitation. It was a further ual surgeons. A final cast for a complete maxillary
goal to use existing implant components and instru- denture or an immediate complete maxillary den-
ments and to limit the total number of implants to 5 ture was mounted on a semiadjustable articulator
or 6, thereby allowing the immediate loading of 4 to using a facebow transfer, and the mandibular diag-
6 primarily stable implants. In this manner, interim nostic cast was mounted with a centric relation
removable denture use is avoided. record utilizing a stabilized record base. The com-
plete denture was fabricated and a mandibular fixed
denture extending from the left mandibular second
MATERIALS AND METHODS premolar to the right mandibular second premolar
was processed (Fig 1). A polyvinylsiloxane interoc-
Patient Selection clusal index was made to record the articulation of
Ten patients, all women ranging in age from 32 to the maxillary complete denture and the mandibular
73 years, were identified in the screening of new fixed denture prior to processing.
518 Volume 17, Number 4, 2002
COOPER ET AL
Surgical Procedures Immediate Loading Procedures
REPRODUCED OR TRANSMITTED IN ANY FORM WITHOUT WRITTEN PERMISSION FROM THE PUBLISHER.
COPYRIGHT © 2002 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY. NO PART OF THIS ARTICLE MAY BE
After obtaining informed consent, patients were For 9 of the 10 implant prostheses, a newly fabri-
given a loading dose of amoxicillin (2 g stat) and 800 cated denture bearing the second left premolar to
mg of ibuprofen prior to the procedure. All proce- second right premolar teeth was hollowed using an
dures were performed using local anesthesia. Teeth acrylic bur and oriented to the transmucosal abut-
were extracted with care to limit socket expansion or ments by occlusion and intimate contact with the
cortical bone fracture. Mucoperiosteal flaps posterior residual alveolar ridges (Figs 4a to 4c).
extended distal to the left and right mental foram- With the denture stabilized by the patient’s occlu-
ina. Alveolectomies to reduce the residual sockets sion, autopolymerizing acrylic resin was used to
and to provide sufficient dimension for abutment register the position of the abutments. The denture
and prosthesis placement were performed with flanges were trimmed away and the posterior seg-
rongeurs and dental burs. Standard dental implant ments removed, and the reline procedure was
osteotomies were created using drilling sequences refined to capture the margins of the transmucosal
recommended for placement of Astra Tech dental abutments (Fig 4d). Rubber dam was applied clini-
implants (3.5 or 4.0 mm; Astra Tech, Lexington, cally to shield the suture line and tissues from the
MA). Special attention was directed toward achiev- acrylic resin. The relined denture was trimmed to
ing inter-implant parallelism to facilitate the subse- provide access for cleaning, and the occlusion was
quent restoration. Implants were placed to the level verified to provide bilaterally equivalent contacts in
of the residual alveolar crest. Two dehiscences were
treated with autogenous bone harvested during the
alveolectomy and resorbable membranes (Biomend;
Sulzer Dental, Carlsbad, CA). Cover screws were
placed into any implants lacking primary stability
and requiring bone augmentation, and these were
left to heal beneath the mucosa (Fig 2). In 2
instances, an implant lacked resistance to further
rotation but was axially stable, and healing abut-
ments were placed without loading of the implant.
In all other implants, 6-mm healing abutments
(modified to accept cemented prostheses) were
screwed to place with finger pressure and the
mucoperiosteum was adapted to the transmucosal
abutment and sutured with Gore sutures (W. L. Fig 1 Articulated casts with diagnostic denture tooth waxing.
Gore, Flagstaff, AZ) or 4-0 chromic gut sutures. The planning for immediate placement and loading following
tooth extraction is dependent upon precise tooth location relative
More recently, solid abutments of prepared configu- to existing tooth sockets and subsequent implant placement.
ration have been made available for the purpose of Planning requires that accurate diagnostic casts be mounted at a
providing a restorative platform for cemented verified vertical dimension of occlusion using stabilized record
bases for mounting in maximum intercuspation or centric rela-
restorations (Fig 3). A panoramic radiograph was tion. The mandibular molars are not included in the interim pros-
made following the procedure. thesis and the occlusion is balanced.
Figs 2a and 2b Implants placed into and between extraction sockets. Note that 1 implant in the canine extraction socket attained pri-
mary stability but is within a significant residual defect. In such cases, the implant site was grafted with autogenous bone from the alve-
olectomy or a suitable bone-grafting substitute. Such implants were not loaded but left to heal in a transmucosal healing position using a
healing abutment as shown (arrow).
The International Journal of Oral & Maxillofacial Implants 519
COOPER ET AL
centric relation and to provide balance, if occluding
REPRODUCED OR TRANSMITTED IN ANY FORM WITHOUT WRITTEN PERMISSION FROM THE PUBLISHER.
COPYRIGHT © 2002 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY. NO PART OF THIS ARTICLE MAY BE
a new complete denture. Attention at implant place-
ment avoided parallelism problems that could not
be reconciled by minor extraoral adjustment of the
abutment. Care was taken to avoid tissue exposure
to heat associated with exothermic setting of the
acrylic resin material. In a similar manner, one den-
ture was connected to the implants bearing 20-
degree uni-abutments using a reline procedure to
pick up titanium interim cylinders (Fig 5). This
prosthesis was retained with 6 gold screws.
All patients were asked to limit their diet to liquids
for the first week following therapy. A 0.2% chlorhex-
Fig 3 Evaluation of implant and abutment placement for imme- idine gluconate mouthrinse was prescribed for the
diate loading following extraction of remaining teeth. When more
teeth and a more significant alveolectomy were involved, tissue first 3 weeks. During the second and third weeks,
redundancy could be observed. Here, new solid abutments with a patients were asked to avoid any hard breads or foods
machined restorative surface offer an expanding conical form to requiring excessive tearing or incising in their diet.
maintain this tissue below the restorative margins and a slight
tapered axial wall to promote and simplify the reline procedure Following the 21-day evaluation, patients were unre-
involved in provisional denture fabrication. stricted in their diet. Hygiene was reinforced and a
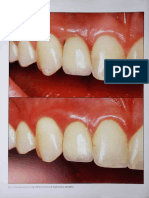
Figs 4a to 4d Stepwise conversion of a custom-made immediate denture. The processed denture for immediate loading has full exten-
sion without molar teeth.
Fig 4a The first step requires hollowing of the denture to clear Fig 4b The denture is relined to capture the position of the
the abutments and fully seat it along the unaffected posterior abutments in polymerized acrylic resin, and the flanges are
edentulous ridges. removed.
Fig 4c The interim fixed denture is refined by relining and con- Fig 4d The completed denture is polished and cemented to
touring. provide a cleansible form and surface (shown here at 6 weeks
after cementation).
520 Volume 17, Number 4, 2002
COOPER ET AL
REPRODUCED OR TRANSMITTED IN ANY FORM WITHOUT WRITTEN PERMISSION FROM THE PUBLISHER.
COPYRIGHT © 2002 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY. NO PART OF THIS ARTICLE MAY BE
Figs 5a and 5b Fabrication of a screw-retained interim fixed denture on immediately placed implants. (Left) After placement of 20-
degree uni-abutments, temporary titanium cylinders were placed with gold screws. (Right) Using autopolymerizing acrylic resin, the tempo-
rary titanium cylinders were then indexed within a hollowed-out purpose-made interim denture and carefully contoured and polished.
Table 2 Patient Data
No. of No. of
Patient implants implants loaded Opposing
no. Age placed at surgery dentition Complications
ILD001 50 6 4 Complete denture None
ILD002 57 5 5 Complete denture None
ILD003 73 5 4 Natural dentition Fractured provisional,
debonded
ILD004 70 5 5 Fixed partial denture/ None
removable partial denture
ILD005 67 6 5 Complete denture Fractured provisional,
debonded
ILD006 55 6 6 Complete denture None
ILD007 71 6 5 Implant prosthesis None
ILD008 55 6 6 Natural dentition None
ILD009 71 5 4 Immediate complete None
denture
ILD010 32 4 4 Implant prosthesis Fractured acrylic tooth
water irrigation device was recommended along with implants were placed directly into extraction sites.
proximal brushes and superfloss. After 3 months of Forty-eight implants achieved primary stability fol-
healing, 20-degree uni-abutments were placed and lowing placement (Table 2). All patients tolerated
fixed dentures were fabricated using gold cylinders surgery well and proceeded to controlled prosthetic
cast into gold alloy frameworks that were veneered loading immediately after panoramic radiography.
with acrylic resin and acrylic resin denture teeth. Stan- Patients were dismissed with good hemostasis in the
dard clinical and laboratory procedures were used. absence of direct pressure on the suture line. None
of the patients experienced pain or discomfort dur-
ing the extended prosthetic aspect of this single-visit
RESULTS therapy. Patients reported no uncontrolled pain or
discomfort during the first 72 hours or thereafter.
For 10 consecutively treated patients, 54 implants Limited swelling and ecchymosis were observed at
were placed into the parasymphyseal mandible the 7-day visit. All patients showed excellent pri-
immediately following extraction. Thirty-four mary wound healing at the 21-day follow-up visit.
The International Journal of Oral & Maxillofacial Implants 521
COOPER ET AL
REPRODUCED OR TRANSMITTED IN ANY FORM WITHOUT WRITTEN PERMISSION FROM THE PUBLISHER.
COPYRIGHT © 2002 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY. NO PART OF THIS ARTICLE MAY BE
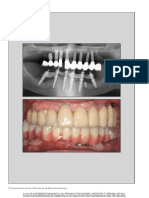
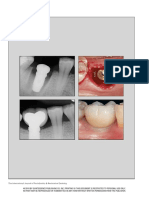
Figs 6a to 6c Radiographic history of immediate implant placement and loading following extraction of intact remaining teeth.
Fig 6a Preoperative image. Fig 6b Immediate postoperative image with abutments placed
for cement-retained provisional restoration.
(1) have meaning of significance to patients and (2)
have meaning that is relevant to biology. It is pro-
posed that the term immediate loading should refer to
situations where implant placement with primary
stability and prosthetic loading with a provisional
prosthetic tooth occur at the same clinical visit.
Immediate loading is temporally irrelevant with
respect to osseointegration. Biologically, primary
stability is essential. Loading should occur immedi-
ately following (hours and not days) implant place-
ment to eliminate possible disruption of the blood
Fig 6c Six-month posttreatment image. Note that the level of clot during the important early stages of healing.
bone is maintained at the implant-abutment interface. Note the Early loading refers to implants placed with primary
healing around the left implant. Arrows indicate maintained crest-
al bone. stability and loaded with a provisional prosthesis at a
subsequent clinical visit prior to attaining osseointe-
gration. Early loading should not perturb initial heal-
ing (blot clot formation, cellular infiltration, epithe-
At the 3-month visit, all 54 implants were individu- lialization). Early loading should also follow the onset
ally tested and shown to fulfill the criteria estab- of osteogenesis, because current biologic knowledge
lished for implant success.23 To date, these implants suggests that bone formation is enhanced by mechani-
loaded by a conventional metal/acrylic resin fixed cal stimulation. Therefore, early loading should occur
denture remain asymptomatic and successful. only after approximately 3 weeks of healing.
The radiographic surveys completed by If implants are not immediately loaded or loaded
panoramic radiography revealed good healing of early, then conventional-loading or delayed-loading
bone within the extraction sites and at the implant protocols are invoked. Conventional loading refers to
interface. The cortical bone levels appeared to be implant placement (typically achieving primary sta-
maintained at the machined cortical bevel that bility) and healing for 3 to 6 months in a sub-
approximates the implant-abutment interface (Fig merged or non-submerged mucosal orientation.
6). Thus, bone responses to the implants placed and This time frame reflects the requirement for osteo-
loaded immediately are similar to the responses genesis and woven bone remodeling to load-bear-
measured at unsplinted, rapidly loaded implants ing lamellar bone and acknowledges the original
placed by a 1-stage procedure 16,24 and implants recommendations of Brånemark or Schroeder.26,27
placed and restored using a 2-stage approach.25 More recently, suggestions of 6 to 8 weeks healing
at topographically enhanced surface implants have
been put forth.28,29
DISCUSSION Delayed-loading protocols are an important aspect
of implant therapy. Delayed loading refers to
Temporal aspects of dental implant loading require extended healing periods (more than 3 months)
clear definition. It is important that these definitions invoked when implants are placed without primary
522 Volume 17, Number 4, 2002
COOPER ET AL
stability, into bone of low density, into extraction immediate loading of the edentulous mandible.
REPRODUCED OR TRANSMITTED IN ANY FORM WITHOUT WRITTEN PERMISSION FROM THE PUBLISHER.
COPYRIGHT © 2002 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY. NO PART OF THIS ARTICLE MAY BE
sockets without significant primary bone-to-implant Bone density of the edentulous mandible favors
contact, or with a simultaneous bone regeneration osseointegration, and there appears to be high suc-
procedure. There are few guidelines for these pro- cess when any of the various surface topographies
cedures, but recommendations typically range from are used for conventional implant therapy.
6 to 12 months. When considering immediate loading, implant
In the present study, the aforementioned defini- design may play a more important role. In the
tion of immediate loading was adopted, and every absence of controlled comparative clinical data, the
implant placed with primary stability was loaded at role of surface topography is presently acknowledged
the same clinical visit as the implant placement. A in facilitating osseointegration, in increasing the rate
sufficient number of implants were placed to permit of bone formation, and in assuring osteoconduction
immediate loading of a fixed denture, should 1 or 2 via improved blood clot retention.30 Surface rough-
implants not achieve primary stability. Significantly, ness also increases primary stability, as measured
this clinical patient series is the first report of using resonance frequency energy.31 In this study, the
immediate extraction and tooth replacement using implants used possess a titanium dioxide grit-blasted
immediately loaded dental implants. The requisite surface of defined biologic and clinical behavior. Pre-
alveolectomy (necessary to provide occlusogingival viously, a similar implant possessing the identical
dimension for tooth replacement and sufficient surface modification was used to achieve 96.2% suc-
labiolingual mandibular dimension for placement of cess following 1-stage placement and immediate
3.5-mm-diameter implants) prior to placement of loading beneath soft relined mandibular overden-
implants into extraction sockets following removal tures.16 Other topographically enhanced implant sur-
of mandibular incisors and first premolars often faces exist and have been shown to promote more
obliterated the extraction sockets if previous loss of rapid bone formation and greater bone-to-implant
periodontal attachment and bone resorption had contact at earlier times (see Cooper30). Chiapasco
occurred. In other cases, only 3 to 4 mm of the and associates18 demonstrated a high success rate
socket remained, and it was largely eliminated by when rapidly loading mandibular parasymphyseal
the osteotomy procedure or obliterated by a 3.5- implants via a bar overdenture. When sandblasted/
mm- or 4.0-mm-diameter implant. When canines acid-etched ITI implants (Straumann, Waldenburg,
were extracted or when dehiscences were present Switzerland) were used for treatment using a similar
following extraction, a significant portion of the protocol, Jaffin and colleagues reported similarly
implant did not achieve primary bone contact or high success rates. 14 Interestingly, the failures
primary stability. Sufficient autogenous bone was reported were for machined-surface implants. How-
available from the alveolectomy for direct augmen- ever, when loaded at 20 days versus conventional
tation; however, the implants that did not attain pri- therapy, machined-surface implants provided 100%
mary stability were not immediately loaded. success.17 When 6 to 10 machined-surface implants
This report, like that of Randow and coworkers,17 were used, often with implants placed distal to the
sought to limit the number of implants used in mandibular foramina and with assurance of fixation
immediate therapy instead of expanding the com- exceeding 40 Ncm, immediate loading was highly
plexity and cost of treatment by use of additional successful.13
implants during the immediate loading period. In The protocol illustrated in this report integrated
this manner, a test of the immediate loading concept the use of 2-component implants for a 1-stage,
with respect to conventional implant therapy could immediate loading protocol. The use of 2-compo-
be approximated, although it fails to replicate the nent systems (implant + abutment) was intentional
rigorous clinical comparison of Randow and cowork- and was based on 2 clinical possibilities. The first
ers. This limitation of implant number during ther- clinical variable that favors the use of a 2-component
apy is congruent with an overall goal to expedite and system is the possible absence of bone for primary
simplify treatment so as to increase the general use stability. When using a 2-component system, the
of implants in mandibular dental rehabilitation. implant can (1) remain unloaded in a transmucosal
Several other reports have used as many as 10 position using a healing abutment or (2) be placed in
implants for immediate loading protocols. Both a submucosal position using a cover screw. This flex-
studies using 10 implants used threaded implants ibility was viewed as a positive aspect of the protocol
exclusively or as a large segment of the study group. and limited the need for detailed radiographic inter-
Given the role of surface roughness in favoring pretations when addressing the parasymphyseal
osseointegration, the authors speculate that more mandible. The second clinical variable that favors
conventional numbers of implants may be used for the use of a 2-component system for 1-stage surgery
The International Journal of Oral & Maxillofacial Implants 523
COOPER ET AL
is the polymorphic nature of attached mucosa and term. However, whether or not the present results
REPRODUCED OR TRANSMITTED IN ANY FORM WITHOUT WRITTEN PERMISSION FROM THE PUBLISHER.
COPYRIGHT © 2002 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY. NO PART OF THIS ARTICLE MAY BE
gingiva. A 2-component system allows decisions may be extended to a larger population that
about abutment dimensions to solve discrepancies in includes systemically compromised individuals or
tissue/component relationships. In this report, a smokers merits careful consideration.
conus implant-abutment connection was used This protocol may directly address perceptions
specifically to facilitate the assembly of the compo- of long treatment times and the limited value of
nents at the surgical visit. The biomechanical nature expensive therapy by offering a single-visit solution
of the conus interface permits finger tightening to provisional replacement of a failed mandibular
without torque control or risk of disturbing the dentition by avoiding any mandibular complete
implant in place. The behavior of the conus inter- denture. The potential cost savings to patients can-
face further assures that the components will remain not be predicted; however, the reduced number of
in a stable relationship with one another during the patient visits, the reduced morbidity associated with
3-month healing phase. Finally, the solid nature of fewer surgical interventions, and the facilitated
the abutments used here precludes any accumulation functional rehabilitation offered by this protocol
of bacteria during the healing period. This may con- may represent important reductions to potentially
tribute to the excellent soft tissue healing response key barriers to accepting this therapy. When the
seen universally among the enrolled patients. expense of a fixed denture supported by 4 to 6
The introduction of a dedicated immediate-load- implants remains a limiting factor, treatment of
ing implant system for the edentulous mandible mandibular edentulism using an overdenture sup-
(Brånemark Novum; Nobel Biocare, Yorba Linda, ported by 2 implants placed by a 1-stage proce-
CA) further indicates great interest in this topic.12 dure 32 or by placement with immediate loading
The Novum System is well documented, with over using a soft reline material should be considered.24
70 consecutive cases reported to be successful. The
approach illustrated here differs considerably and
merits some comparison. First, the Novum requires CONCLUSION
a dedicated surgical instrumentation. Second, the
Novum system uses a unique 5.0-mm-diameter This report contributes to a growing body of litera-
implant. Third, the Novum system is presently ture that supports immediate loading of endosseous
available in 1 dimension. Related to this, it is not titanium screw-type implants as an expedited treat-
recommended for Class II or Class III maxillo- ment of mandibular edentulism. In selected healthy
mandibular skeletal relationships. Fourth, the patients, significant time and clinic visits may be
Novum system provides a definitive prosthesis the saved by simultaneous extraction, implant place-
day of surgery. In contrast, the present approach to ment, and restoration with a simple acrylic resin
immediate treatment of edentulism involves no provisional prosthesis. The use of existing compo-
additional instrumentation and can be adapted to an nents, surgical instrumentation, and simple provi-
extended spectrum of anatomies. This custom sional restoration techniques offers this opportunity
approach further requires a custom prosthodontic to clinicians and patients. The reduction in postop-
solution for each patient. The similarity of the 2 erative visits, an absence of postoperative complica-
approaches may be seen in the recognition of the tions, and the enthusiasm of patients who receive
biologic capacity of the parasymphyseal region of this treatment suggest that approaches to simplify-
the mandible and in the shared goal of increasing ing implant rehabilitation of the mandible may
the treatment of mandibular edentulism. increase patient acceptance of an extremely success-
At this time, the present clinical patient case ful, but currently poorly accepted, therapy.
series indicates good success for the first 10 sub-
jects. It may be impossible to conduct a clinical
study showing statistically different success rates for ACKNOWLEDGMENTS
this immediate procedure versus a conventional
approach (in that hundreds of age- and sex-matched The authors wish to thank the residents of the Graduate
individuals would require treatment in a controlled Prosthodontics and Graduate Periodontology programs of the
University of North Carolina for their assistance in patient
comparative clinical study, because there may be so treatment and documentation. This project was supported, in
few failures in either group). In additional subjects part, by the AstraTech Research Fellowship at the University of
treated since completion of this clinical patient North Carolina.
series, similar success has been observed in the short
524 Volume 17, Number 4, 2002
COOPER ET AL
REFERENCES
REPRODUCED OR TRANSMITTED IN ANY FORM WITHOUT WRITTEN PERMISSION FROM THE PUBLISHER.
COPYRIGHT © 2002 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY. NO PART OF THIS ARTICLE MAY BE
17. Randow K, Ericsson I, Nilner K, Petersson A, Glantz P-O.
Immediate functional loading of Brånemark dental implants.
1. Total tooth loss among persons aged greater than or equal to An 18-month clinical follow-up study. Clin Oral Implants
65 Years—Selected States, 1995-1997. Morb Mortal Wkly Res 1999;10:8–15.
Rep 1999 March 19;48(10):206–210. 18. Chiapasco M, Gatti C, Rossi E, Haefliger W, Markwalder
2. Spiekermann H, Jansen VK, Richter EJ. A 10-year follow- TH. Implant-retained mandibular overdentures with imme-
up study of IMZ and TPS implants in the edentulous diate loading. A retrospective multicenter study on 226 con-
mandible using bar-retained overdentures. Int J Oral Max- secutive cases. Clin Oral Implants Res 1997;8:48–57.
illofac Implants 1995;10(2):231–243. 19. Tarnow DP, Emtiaz S, Classi A. Immediate loading of
3. Lindquist LW, Carlsson GE, Jemt T. A prospective 15-year threaded implants at stage 1 surgery in edentulous arches:
follow-up study of mandibular fixed prostheses supported by Ten consecutive case reports with 1- to 5-year data. Int J
osseointegrated implants. Clinical results and marginal bone Oral Maxillofac Implants 1997;12:319–324.
loss. Clin Oral Implants Res 1996;7(4):329–336. 20. Balshi TJ, Wolfinger GJ. Immediate loading of Brånemark
4. Buser D, Mericske-Stern R, Bernard JP, et al. Long-term implants in edentulous mandibles: A preliminary report.
evaluation of non-submerged ITI implants. Part 1: 8-year life Implant Dent 1997;6:83–88.
table analysis of a prospective multi-center study with 2359 21. Schnitman PA, Wohrle PS, Rubenstein JE, DaSilva JD,
implants. Clin Oral Implants Res 1997;8(3):161–172 Wang NH. Ten-year results for Brånemark implants imme-
5. Arvidson K, Bystedt H, Frykholm A, von Konow L, diately loaded with fixed prostheses at implant placement.
Lothigius E. Five-year prospective follow-up report of the Int J Oral Maxillofac Implants 1997;12:495–503.
Astra Tech Dental Implant System in the treatment of eden- 22. Salama H, Rose LF, Salama M, Betts NJ. Immediate loading
tulous mandibles. Clin Oral Implants Res 1998;9(4):225–34. of bilaterally splinted titanium root-form implants in fixed
6. Deporter D, Watson P, Pharoah M, Levy D, Todescan R. prosthodontics—A technique reexamined: Two case reports.
Five- to six-year results of a prospective clinical trial using Int J Periodontics Restorative Dent 1995;15:344–361.
the ENDOPORE dental implant and a mandibular overden- 23. Roos J, Sennerby L, Lekholm U, Jemt T, Grondahl K,
ture. Clin Oral Implants Res 1999;10(2):95–102. Albrektsson T. A qualitative and quantitative method for
7. De Bruyn H, Kisch J, Collaert B, Linden U, Nilner K, evaluating implant success: A 5-year retrospective analysis of
Dvarsater L. Fixed mandibular restorations on three early- the Brånemark implant. Int J Oral Maxillofac Implants 1997;
loaded regular platform Brånemark implants. Clin Implant 12:504–514.
Dent Relat Res 2001;3:176–184. 24. Cooper L, Felton DA, Kugelberg CF, et al. A multicenter
8. Grunder U. Immediate functional loading of immediate 12-month evaluation of single-tooth implants restored 3
implants in edentulous arches: Two-year results. Int J Perio- weeks after 1-stage surgery. Int J Oral Maxillofac Implants
dontics Restorative Dent 2001;21:545–551. 2001;16:182–192.
9. Chow J, Hui E, Liu J, et al. The Hong Kong Bridge Proto- 25. Arvidson K, Bystedt H, Frykholm A, von Konow L,
col. Immediate loading of mandibular Brånemark fixtures Lothigius E. Five-year prospective follow-up report of the
using a fixed provisional prosthesis: Preliminary results. Clin Astra Tech Dental Implant System in the treatment of eden-
Implant Dent Relat Res 2001;3:166–174. tulous mandibles. Clin Oral Implants Res 1998;9:225–234.
10. Chiapasco M, Abati S, Romeo E, Vogel G. Implant-retained 26. Brånemark PI, Hansson BO, Adell R, et al. Osseointegrated
mandibular overdentures with Bånemark System MKII implants in the treatment of the edentulous jaw. Experience
implants: A prospective comparative study between delayed from a 10-year period. Scan J Plat Reconstr Surg Suppl
and immediate loading. Int J Oral Maxillofac Implants 1977;16:1–132.
2001;16:537–546. 27. Schroeder A, Pohler O, Sutter F. Gewebsreaktionauf ein
11. Colomina LE. Immediate loading of implant-fixed Titan-Hohlzylinder implantat mit Titan-Spritzschichtober-
mandibular prostheses: A prospective 18-month follow-up flache. Schweiz Mschr Zahnheilk 1976;862:16–23.
clinical study—Preliminary report. Implant Dent 2001;10(1) 28. Roccuzzo M, Bunino M, Prioglio F, Bianchi SD. Early load-
23–29. ing of sandblasted and acid-etched (SLA) implants: A prospec-
12. Brånemark P-I, Engstrand P, Ohrnell LO, et al. Brånemark tive split-mouth comparative study. Clin Oral Implants Res
Novum: A new treatment concept for rehabilitation of the 2001;12:572–578.
edentulous mandible. Preliminary results from a prospective 29. Lazzara RJ, Porter SS, Testori T, Galante J, Zetterqvist L. A
clinical follow-up study. Clin Implant Dent Relat Res 1999; prospective multicenter study evaluating loading of Osseo-
1(1):2–16. tite implants two months after placement: One-year results.
13. Horiuchi K, Uchida H, Yomanoto K, Sugimura M. Immedi- J Esthet Dent 1998;10:280–289.
ate loading of Brånemark system implants following place- 30. Cooper LF. A role for surface topography in creating and
ment in edentulous patients: A clinical report. Int J Oral maintaining bone at titanium endosseous implants. J Pros-
Maxillofac Implants 2000;15:824–830. thet Dent 2000;84:522–534.
14. Jaffin RA, Kumar A, Berman CL. Immediate loading of 31. Rasmusson L, Kahnberg KE, Tan A. Effects of implant
implants in partially and fully edentulous jaws: A series of 27 design and surface on bone regeneration and implant stabil-
case reports. J Periodontol 2000;71(5):833–838. ity: An experimental study in the dog mandible. Clin
15. Gatti C, Haefliger W, Chiapasco M. Implant-retained Implant Dent Relat Res 2001;3:2–8.
mandibular overdentures with immediate loading: A 32. Roynesdal AK, Amundrud B, Hannaes HR. A comparative
prospective study of ITI implants. Int J Oral Maxillofac clinical investigation of 2 early loaded ITI dental implants
Implants 2000;15:383–388. supporting an overdenture in the mandible. Int J Oral Max-
16. Cooper LF, Scurria MS, Lang LA, Guckes AD, Moriarty illofac Implants 2001;16:246–251.
JD, Felton DA. Treatment of edentulism using Astra Tech
implants and ball abutments to retain mandibular overden-
tures. Int J Oral Maxillofac Implants 1999;14:646–653.
The International Journal of Oral & Maxillofacial Implants 525
You might also like
- BPS Oncology Pharmacy Practice ExamDocument11 pagesBPS Oncology Pharmacy Practice Examiman100% (3)
- Crash Course Renal and Urinary System 4th - JonesDocument153 pagesCrash Course Renal and Urinary System 4th - JonesBiblioteca Libros de Nutricion100% (1)
- Professional Responsibility and AccountabilityDocument5 pagesProfessional Responsibility and Accountabilityjasdeepkaurnagra100% (2)
- Mini ImplantesDocument6 pagesMini ImplantesPablo GrossoNo ratings yet
- Panoramic Radiographs Made Before Complete Removable Dental Prostheses Fabrication A Retrospective Study of Clinical SignificanceDocument6 pagesPanoramic Radiographs Made Before Complete Removable Dental Prostheses Fabrication A Retrospective Study of Clinical Significance01 X A.A. Gede Reynata Putra XII MIPA 4No ratings yet
- Immediate Loading Implants With Mandibular Overdenture: A 48-Month Prospective Follow-Up StudyDocument6 pagesImmediate Loading Implants With Mandibular Overdenture: A 48-Month Prospective Follow-Up StudySung Soon ChangNo ratings yet
- Carga Inmediata Contra Tardia de Implantes Dentales en Alveolos Frescos Posextraccion en La Zona Estética Maxilar, Un Estudio Clínico ComparativoDocument6 pagesCarga Inmediata Contra Tardia de Implantes Dentales en Alveolos Frescos Posextraccion en La Zona Estética Maxilar, Un Estudio Clínico ComparativoKuro Aranda PlataNo ratings yet
- Becker2011 Provisional 1Document7 pagesBecker2011 Provisional 1Gabriel MoralesNo ratings yet
- Carl Misch Workshop Guidelines For Immediate Loading PDFDocument6 pagesCarl Misch Workshop Guidelines For Immediate Loading PDFyogananth100% (1)
- 11 B - All On Four Group 01 PDFDocument3 pages11 B - All On Four Group 01 PDFLuis Humberto BorgesNo ratings yet
- Telescopic Crowns As Attachments For Implant Supported Restorations A Case SeriesDocument15 pagesTelescopic Crowns As Attachments For Implant Supported Restorations A Case SeriesmaxNo ratings yet
- One Abutment at One Time: Non-Removalof An Immediate Abutment and Its Effecton Bone Healing Around Subcrestal TaperedimplantsDocument5 pagesOne Abutment at One Time: Non-Removalof An Immediate Abutment and Its Effecton Bone Healing Around Subcrestal TaperedimplantsRodrigo videiraNo ratings yet
- Implant Retained Overdenture: Splint Approach Using Copy DenturesDocument9 pagesImplant Retained Overdenture: Splint Approach Using Copy DenturesSorabh JainNo ratings yet
- 4th Article PDFDocument10 pages4th Article PDFSafu SalehNo ratings yet
- Cabello 2012Document7 pagesCabello 2012Vannia BautistaNo ratings yet
- Immediate Early Loading of Dental Implants. Clinical Documentation and Presentation of A Treatment ConceptDocument23 pagesImmediate Early Loading of Dental Implants. Clinical Documentation and Presentation of A Treatment ConceptDr.SnehalNo ratings yet
- Single Center Retrospective Analisys of 1001 Consecutevely Placed NobelActive Implants BABBUSH Et AlDocument8 pagesSingle Center Retrospective Analisys of 1001 Consecutevely Placed NobelActive Implants BABBUSH Et AlDr. Rafael OrroNo ratings yet
- Tilted Implants For A Mandibular Hybrid Prosthesis: James A. Rivers, DMD, MhsDocument4 pagesTilted Implants For A Mandibular Hybrid Prosthesis: James A. Rivers, DMD, MhsSummer HorneNo ratings yet
- Baroni JP 2006Document7 pagesBaroni JP 2006Sebastien MelloulNo ratings yet
- 5 PDFDocument8 pages5 PDFoskar ORTIZNo ratings yet
- Single ToothReplacementintheAnteriorMaxillaDocument14 pagesSingle ToothReplacementintheAnteriorMaxillaSteffany BernalNo ratings yet
- Clinical Implant Dentistry and Related Research Volume Issue 2019 (Doi 10.1111/cid.12854) Liu, Renzhang Yang, Zhen Tan, Jianguo Chen, Li Liu, Hanqing - Immediate Implant Placement For A SingleDocument11 pagesClinical Implant Dentistry and Related Research Volume Issue 2019 (Doi 10.1111/cid.12854) Liu, Renzhang Yang, Zhen Tan, Jianguo Chen, Li Liu, Hanqing - Immediate Implant Placement For A SingleliguojieNo ratings yet
- Clinical Outcome of Submerged vs. Non-Submerged Implants Placed in Fresh Extraction SocketsDocument8 pagesClinical Outcome of Submerged vs. Non-Submerged Implants Placed in Fresh Extraction SocketsLorenaCastanoGarzonNo ratings yet
- ImmedLoading IJRPD 23 1 03Document9 pagesImmedLoading IJRPD 23 1 03Fernando Letelier BaltierraNo ratings yet
- Arora2017 Implante Imediato Com RogDocument9 pagesArora2017 Implante Imediato Com RogAsafe RheinnickNo ratings yet
- Implant Supported OverdentureDocument5 pagesImplant Supported OverdentureFadil ObiNo ratings yet
- Orthopedic JournalDocument9 pagesOrthopedic JournalAdinarayana KashyapNo ratings yet
- 10.1097@00008505 200204000 00013Document9 pages10.1097@00008505 200204000 00013boutebaaNo ratings yet
- Immediate DentureDocument4 pagesImmediate DenturenaomiNo ratings yet
- The International Journal of Periodontios & Restorative DentistryDocument11 pagesThe International Journal of Periodontios & Restorative DentistryAle ZuzaNo ratings yet
- Performance of Physics Forceps Vs Traditional Forceps A Review ArticleDocument3 pagesPerformance of Physics Forceps Vs Traditional Forceps A Review ArticleInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- The 2 X 4 Appliance McKeown Sandler PDFDocument4 pagesThe 2 X 4 Appliance McKeown Sandler PDFAgia Tessa AndrianiNo ratings yet
- Two Bilateral Zygomatic Implants Placed and Immediately Loaded A Retrospective Chart Review With Up-To-54-Month Follow-UpDocument5 pagesTwo Bilateral Zygomatic Implants Placed and Immediately Loaded A Retrospective Chart Review With Up-To-54-Month Follow-UpBagis Emre Gul100% (1)
- Conservative Endodontic Microsurgery To Protect Critical Anatomical Structures - Selective Curettage: A Case SeriesDocument12 pagesConservative Endodontic Microsurgery To Protect Critical Anatomical Structures - Selective Curettage: A Case SeriesClaudia Pérez LuisNo ratings yet
- Immediate Implant Loading Versus Delayed LoadingDocument27 pagesImmediate Implant Loading Versus Delayed LoadingAhmed GendiaNo ratings yet
- Defectos Óseos - Diagnóstico Radiográfico"Document101 pagesDefectos Óseos - Diagnóstico Radiográfico"Nucleo AlgodonesNo ratings yet
- Tanpa Judul PDFDocument7 pagesTanpa Judul PDFnadyashintakasihNo ratings yet
- Resonance Frequency Analysis Comparing Two Clinical InstrumentsDocument5 pagesResonance Frequency Analysis Comparing Two Clinical InstrumentsBagis Emre GulNo ratings yet
- Anitua 2016Document7 pagesAnitua 2016IsmaelNo ratings yet
- 2-Clinical Outcomes of Conventional and Immediate Placement-Sara - KHDocument12 pages2-Clinical Outcomes of Conventional and Immediate Placement-Sara - KHZiad RabieNo ratings yet
- Double Duplicate Technique For Cad Cam Full Arch Immediate Loading A Technical Description and Case ReportDocument9 pagesDouble Duplicate Technique For Cad Cam Full Arch Immediate Loading A Technical Description and Case ReportYuki MuraNo ratings yet
- Vertical Splitting of The Mandibular Body As An Alternative To Inferior Alveolar Nerve LateralizationDocument7 pagesVertical Splitting of The Mandibular Body As An Alternative To Inferior Alveolar Nerve Lateralizationr1comfupchNo ratings yet
- Cronin 1997Document13 pagesCronin 1997drg Triani UmaiyahNo ratings yet
- A Prospective, Multi Center Study Assessing Early Loading With Short Implants in Posterior Regions. A 3 Year Post Loading Follow Up StudyDocument9 pagesA Prospective, Multi Center Study Assessing Early Loading With Short Implants in Posterior Regions. A 3 Year Post Loading Follow Up StudyBagis Emre GulNo ratings yet
- Document PDFDocument4 pagesDocument PDFBagis Emre GulNo ratings yet
- Fragment Reattachment After Complicated Crown-Root Fractures of Anterior Teeth: A Systematic ReviewDocument16 pagesFragment Reattachment After Complicated Crown-Root Fractures of Anterior Teeth: A Systematic ReviewARUNA BharathiNo ratings yet
- Horizontal and Vertical Resistance Strength of Infrazygomatic Mini-ImplantsDocument5 pagesHorizontal and Vertical Resistance Strength of Infrazygomatic Mini-ImplantsHARITHA H.PNo ratings yet
- Hegde 2014Document4 pagesHegde 2014Harshitha RajannaNo ratings yet
- SwithcingDocument6 pagesSwithcingKyoko CPNo ratings yet
- 9230 Case ReportDocument3 pages9230 Case ReportrajaniNo ratings yet
- Long Term KIOSDocument6 pagesLong Term KIOSgattusoNo ratings yet
- A Comparative Evaluation of Immediate Implant Placement in Fresh Extraction Socket With and Without The Use of Platelet Rich Fibrin: A Clinical and Radiographic StudyDocument8 pagesA Comparative Evaluation of Immediate Implant Placement in Fresh Extraction Socket With and Without The Use of Platelet Rich Fibrin: A Clinical and Radiographic StudyShiva KalyanNo ratings yet
- Misch S Contemporary Implant Dentistry.4Document2 pagesMisch S Contemporary Implant Dentistry.4Dadi SindhuNo ratings yet
- 2023 - RL - Burashed - The Efficacy of Anterior Open Bite Closure W Invisa AttachmentsDocument6 pages2023 - RL - Burashed - The Efficacy of Anterior Open Bite Closure W Invisa Attachmentsdiego.mrodrigues11No ratings yet
- Immediate 1Document7 pagesImmediate 1rtyNo ratings yet
- Mozzati 2013Document9 pagesMozzati 2013Larissa RodovalhoNo ratings yet
- Zona Neutra Maxilofacial PacienteDocument6 pagesZona Neutra Maxilofacial Pacientemargarita de montenegroNo ratings yet
- Amato 1 (2018), Immediate Implant PlacementDocument8 pagesAmato 1 (2018), Immediate Implant PlacementPhương Thảo TrầnNo ratings yet
- TX External Fixator Unstable Pelvic FX Children Injury21Document5 pagesTX External Fixator Unstable Pelvic FX Children Injury21Antonio PáezNo ratings yet
- Journal of Clinical Orthopaedics and Trauma: Sourabh Kumar Sinha, Vineet Kumar, Ajai SinghDocument7 pagesJournal of Clinical Orthopaedics and Trauma: Sourabh Kumar Sinha, Vineet Kumar, Ajai SinghOtto NaftariNo ratings yet
- Module 2 PDFDocument23 pagesModule 2 PDFRui ViegasNo ratings yet
- Comparative Study Between Conventional En-Masse Retraction (Sliding Mechanics) and En-Masse Retraction Using Orthodontic Micro ImplantDocument9 pagesComparative Study Between Conventional En-Masse Retraction (Sliding Mechanics) and En-Masse Retraction Using Orthodontic Micro Implantdrgeorgejose7818No ratings yet
- The Immediacy Concept: Treatment Planning from Analog to DigitalFrom EverandThe Immediacy Concept: Treatment Planning from Analog to DigitalNo ratings yet
- Zirconium Fixed Prosthesis ReviewDocument8 pagesZirconium Fixed Prosthesis ReviewDaniel AtiehNo ratings yet
- Aesthetics and Ceramics Abutments InimplantDocument7 pagesAesthetics and Ceramics Abutments InimplantDaniel AtiehNo ratings yet
- Ejoi 2021 02 s0157Document24 pagesEjoi 2021 02 s0157Daniel AtiehNo ratings yet
- Ejo/cjq 100Document7 pagesEjo/cjq 100Daniel AtiehNo ratings yet
- Ethics of Esthetic Dentistry: Quintessence International July 2004Document11 pagesEthics of Esthetic Dentistry: Quintessence International July 2004Daniel AtiehNo ratings yet
- Int J Dental Hygiene - 2022 - AL Omiri - Oral Health Status Oral Health Related Quality of Life and Personality FactorsDocument11 pagesInt J Dental Hygiene - 2022 - AL Omiri - Oral Health Status Oral Health Related Quality of Life and Personality FactorsDaniel AtiehNo ratings yet
- E 1 s2.0 S0022391302000112 MainDocument7 pagesE 1 s2.0 S0022391302000112 MainDaniel AtiehNo ratings yet
- Digital Cross-Mounting A New Opportunity in ProsthDocument10 pagesDigital Cross-Mounting A New Opportunity in ProsthDaniel AtiehNo ratings yet
- Implant-Supported Fixed Prostheses inDocument9 pagesImplant-Supported Fixed Prostheses inDaniel AtiehNo ratings yet
- Esophegus and StomachDocument24 pagesEsophegus and StomachDaniel AtiehNo ratings yet
- Comparing The Perception of Dentists and Lay People To Altered Dental EstheticsDocument14 pagesComparing The Perception of Dentists and Lay People To Altered Dental EstheticsDaniel AtiehNo ratings yet
- 4280-Article Text-9949-10452-10-20220608Document5 pages4280-Article Text-9949-10452-10-20220608Daniel AtiehNo ratings yet
- 50-D21 1492 Rawan Abu Zaghlan JordanDocument11 pages50-D21 1492 Rawan Abu Zaghlan JordanDaniel AtiehNo ratings yet
- Hyaluronic Acid Hope of Light To Black TrianglesDocument4 pagesHyaluronic Acid Hope of Light To Black TrianglesDaniel AtiehNo ratings yet
- Admin, Journal Manager, 17-23-IJDR - 31531Document7 pagesAdmin, Journal Manager, 17-23-IJDR - 31531Daniel AtiehNo ratings yet
- Interdental Papilla Length and The Perception of AestheticsDocument10 pagesInterdental Papilla Length and The Perception of AestheticsDaniel AtiehNo ratings yet
- Developments in Resin-Based Composites: GeneralDocument6 pagesDevelopments in Resin-Based Composites: GeneralDaniel AtiehNo ratings yet
- Pharmaceutics 12 00644 v2Document15 pagesPharmaceutics 12 00644 v2Daniel AtiehNo ratings yet
- SJ BDJ 2018 172Document8 pagesSJ BDJ 2018 172Daniel AtiehNo ratings yet
- Types: Different of Foods Experimental AnimalsDocument11 pagesTypes: Different of Foods Experimental AnimalsDaniel AtiehNo ratings yet
- Complete Dentures: The Principles of Visual Perception and Their Clinical Application To Denture EstheticsDocument25 pagesComplete Dentures: The Principles of Visual Perception and Their Clinical Application To Denture EstheticsDaniel AtiehNo ratings yet
- Unit 1: Leisure ActivitiesDocument4 pagesUnit 1: Leisure ActivitiesThao Nguyen ThuNo ratings yet
- ACTH - IMMULITE 2000 Systems - Rev 19 DXDCM 09017fe9804e1ae9-1604005323094Document29 pagesACTH - IMMULITE 2000 Systems - Rev 19 DXDCM 09017fe9804e1ae9-1604005323094tawfiq bouyahiaNo ratings yet
- Awareness of Epilepsy in Pharmacy Students in Different Universities of Karachi, PakistanDocument6 pagesAwareness of Epilepsy in Pharmacy Students in Different Universities of Karachi, PakistanSyeda Eshaal JavaidNo ratings yet
- Material Safety Data Sheet Mad Artist ResinDocument5 pagesMaterial Safety Data Sheet Mad Artist ResinjoshNo ratings yet
- Breathing ExcersizeDocument35 pagesBreathing Excersizebbmoksh100% (1)
- 01 - 05 - Referat General - Uzura Dentara2017Document10 pages01 - 05 - Referat General - Uzura Dentara2017Simu MedaNo ratings yet
- What Is ReliabilityDocument3 pagesWhat Is ReliabilitysairamNo ratings yet
- Medical TourismDocument14 pagesMedical TourismSangeetha SNo ratings yet
- Technology Life CycleDocument11 pagesTechnology Life Cyclechenri1318No ratings yet
- Surveillance AssignmentDocument8 pagesSurveillance AssignmentPalwasha KhanNo ratings yet
- RPL 5363 OmDocument31 pagesRPL 5363 OmmiguelNo ratings yet
- Skin Rashes and EczemaDocument17 pagesSkin Rashes and EczemaStar WiseNo ratings yet
- Writing A Position Paper Part OneDocument7 pagesWriting A Position Paper Part OnePandinuela, Sean Kerby NatividadNo ratings yet
- Theme: National Digital Transformation: Sharing and ConnectingDocument9 pagesTheme: National Digital Transformation: Sharing and ConnectingthanhNo ratings yet
- Laser in Fixed ProsthodonticsDocument6 pagesLaser in Fixed Prosthodontics2oclock0% (1)
- Fit/Function KPC:: Special Characteristics 11.1 Key Product Characteristic (KPC) DefinitionsDocument3 pagesFit/Function KPC:: Special Characteristics 11.1 Key Product Characteristic (KPC) Definitions57641No ratings yet
- Ancient Liver Remedy Ebook PDFDocument16 pagesAncient Liver Remedy Ebook PDFRadu Savu100% (1)
- Probiotics Good Choice Remission IBDDocument13 pagesProbiotics Good Choice Remission IBDreadalotbutnowisdomyetNo ratings yet
- Resume Scarlet CarpenterDocument2 pagesResume Scarlet Carpenterapi-444441802No ratings yet
- Students' Perception of Medical School Stress and TheirDocument8 pagesStudents' Perception of Medical School Stress and TheirPamela Francisca Bobadilla BurgosNo ratings yet
- Katigraha ManagementDocument4 pagesKatigraha Managementmilind0% (1)
- SWM Ho Icm 70 10 08 2023Document24 pagesSWM Ho Icm 70 10 08 2023Thukaram McaNo ratings yet
- Medical Termination of Pregnancy (MTP) Amendment Act, 2021: Why in NewsDocument4 pagesMedical Termination of Pregnancy (MTP) Amendment Act, 2021: Why in NewsVivek GiriNo ratings yet
- Shinde Et Al. - 2021 - Synthesis of Chitosan Coated Silver Nanoparticle Bioconjugates and Their Antimicrobial Activity Against MultidDocument18 pagesShinde Et Al. - 2021 - Synthesis of Chitosan Coated Silver Nanoparticle Bioconjugates and Their Antimicrobial Activity Against MultidRevathi RajagopalNo ratings yet
- Self Management SkillsDocument7 pagesSelf Management SkillsAnuj HalderNo ratings yet
- Syllabus - Anatomy and Physiology IIDocument2 pagesSyllabus - Anatomy and Physiology IIapi-57781915No ratings yet
- Goods Procurement Contract Awards in Health SectorDocument2,562 pagesGoods Procurement Contract Awards in Health SectorvdvedNo ratings yet