Professional Documents
Culture Documents
Peripheral Cemento-Ossifying Fibroma - A Case Report
Peripheral Cemento-Ossifying Fibroma - A Case Report
Uploaded by
cdcrioralpathOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Peripheral Cemento-Ossifying Fibroma - A Case Report
Peripheral Cemento-Ossifying Fibroma - A Case Report
Uploaded by
cdcrioralpathCopyright:
Available Formats
Peripheral Cemento-Ossifying Fibroma- A Case Report
PERIPHERAL CEMENTO-OSSIFYING FIBROMA- A CASE REPORT
Dr.V.Gopinath,1 Dr.V.Krishna,2 Dr.Pramod kumar3
1. Professor and Head, Department Of Periodontology, Department Of Periodontology,
Rungta College of Dental Sciences Bhilai, India
2. Professor and Head, Department Of Periodontology, Chhattisgarh Dental College and
Research Institute, Rajnandgaon, India
3. Reader, Department of Oral Pathology and Microbiology, Chhattisgarh Dental College and
Research Institute, Rajnandgaon, India
Address for Correspondence
Dr. V.Gopinath. M.D.S., M.B.A
Professor and Head, Department Of Periodontology, Department Of Periodontology, Rungta
College of Dental Sciences Bhilai, India.
Email id:gopivivek@yahoo.com
Mobile no-9840180899
Abstract
Peripheral cemento-ossifying fibroma (PCOF) is a reactive neoplasm. It occurs frequently in
anterior maxilla comprises 9% of all gingival growths and predominantly affects adolescents
and young adults. It most commonly arises from the periodontal ligament. A number of
factors have been implicated in the pathogenesis of PCOF including trauma and local
irritation. The definitive diagnosis of these lesions requires integration of its clinical,
radiological and histological features. In this article, we describe a case of PCOF with the
history of three months involving anterior region.
Keywords: Ossifying fibroma, tooth migration, periodontal ligament, epulis, calcifying
fibroblastic granuloma.
International Journal of Innovations in Dental Sciences / January 2018 / Vol 3 / Issue 1 31
Peripheral Cemento-Ossifying Fibroma- A Case Report
INTRODUCTION
Ossifying fibroma is a benign neoplasm arising in craniofacial bones, composed of
proliferating fibroblasts with osseous products that include bone and ovoid calcifications;
these lesions are well demarcated from the adjacent bone.1
There are two types of ossifying fibromas: the central type and the peripheral type. The
central type arises from the endosteum or the periodontal ligament adjacent to the root apex
and causes expansion of medullary cavity. The peripheral type occurs solely on the soft
tissues covering the tooth-bearing areas of the jaws.2
In 1872, Menzel first described ossifying fibroma; but only in 1927, Montgomery assigned a
terminology to it.3 So, the term, peripheral cemento-ossifying fibroma was coined by
Montgomery in1927. Peripheral cemento-ossifying fibroma accounts for 3.1% of all oral
tumors and 9.6% of the gingival lesions. About 60% of these tumors occur in maxilla and
more than 50% of all cases of maxillary POF are found in the incisors and canine areas.2
A potential of tooth migration due to the presence of peripheral cement ossifying fibroma
has been reported. The treatment of choice is surgical excision with removal of irritation
factors.
CASE REPORT
A 22-year old male patient had reported to the Department of Periodontics, with the
chief complaint of painless overgrowth in upper front region of jaw since 1 year. He gave
the history that the overgrowth was present from last 1 year which was small in the
earliest and gradually increases till 4-5 months and then it became constant. Bleeding was
detected by the patient only after brushing.
Intraoral examination revealed a well defined gingival overgrowth, ovoid in shape with
diffuse border in relation to 11 and 21 region extending from cervical margin of 11 and 21
International Journal of Innovations in Dental Sciences / January 2018 / Vol 3 / Issue 1 32
Peripheral Cemento-Ossifying Fibroma- A Case Report
(buccally) to 1.5 beyond cervical margin of 11 and 21 (palatally) of approximately 1.5 × 2 cm
in size(Figure1). It was firm in consistency. Tenderness seemed to be absent on palpating but
present while probing. Skin over the overgrowth is normal intermixed with erythematous
surface. Pseudopocket of 4-5mm was present in relation to 11 and 21. No other marked
deformity was noted extraorally or intraorally.
Intraoral periapical radiograph in relation to 11 and 21 showed radio-opaque shadow on
coronal portion of 11 and 21 suggestive of orthodontic brackets and wires. Interdental
moderate crystal bone loss in relation to 11 and 21 upto the cervical third of radicular portion
was also seen(Figure 2)
A provisional diagnosis of pyogenic granuloma was made. The differential diagnosis
included peripheral cemento- ossifying fibroma, traumatic fibroma and peripheral giant cell
granuloma. The patient underwent complete blood investigation prior to surgery and was
found to be normal.
The patient didn’t reveal of any systemic problem, and the surgery was performed 7 days
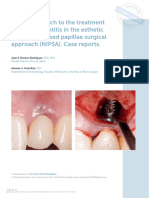
after complete oral prophylaxis. Under local anesthesia, the lesion was excised followed by
curettage of the area and scaling of the involved teeth (Figure 3). Periodontal dressing was
placed and patient was recalled after 7 days for removal of pack and re- evaluation. The
excised tissue was sent for histopathological examination.
HISTOPATHOLOGY
Histopathological report revealed Para-keratinized stratified squamous epithelium with long
and narrow rete ridges overlying connective tissue stroma. Underlying connective tissue
stroma is fibro-cellular composed of dense bundles of collagen fibres, fibroblasts, numerous
blood vessels containing RBCs and chronic inflammatory cell infiltrate composed of
lymphocytes and plasma cells. At places concentrically laminated calcified bodies resembling
cementum and bony trabeculae lined by osteoblast cells were also observed. A final diagnosis
of Peripheral Cemento-Ossifying Fibroma was made (Figure5,6,7).
International Journal of Innovations in Dental Sciences / January 2018 / Vol 3 / Issue 1 33
Peripheral Cemento-Ossifying Fibroma- A Case Report
DISCUSSION
Peripheral cement-Ossifying Fibroma is a non–neoplastic enlargement of the gingiva with
randomly distributed calcifications, immature bone and osteoid. It is found exclusively on the
gingiva and does not arise in other oral mucosal location.7
Peripheral cemento-ossifying fibroma( PCOF) has been given many synonyms, such as
epulis, calcifying fibroblastic granuloma, peripheral cementifying fibroma, peripheral
fibroma with cementogenesis, peripheral cemento-ossifying fibroma, ossifying fibro
epithelial polyp and peripheral fibroma with osteogenesis.8,9
The etiopathogenesis of PCOF is unclear, trauma or local irritants such as subgingival plaque
and calculus, dental appliances, poor-quality dental restorations, microorganism, masticatory
forces, food lodgement and iatrogenic factors are known to influence the development of the
lesion.
An origin from cells of periodontal ligament has been suggested because of exclusive
occurrence of PCOF from interdental papilla, the proximity of gingiva to PDL, the presence
of oxytalan fibers within the mineralized matrix of some lesions, the age distribution, and the
fibro cellular response similar to other reactive gingival lesions of periodontal ligament
origin.10
Approximately 60% of PCOFs occur in the maxilla and they are found more often in the
anterior region, with 55- 60% presenting in the incisor-cuspid region.
The peripheral cemento-ossifying fibroma clinically presents as a pedunculated or sessile
exophytic mass, about <2 cm in diameter (occasionally >10 cm), with a color similar to that
of the mucosa, unless the surface is ulcerated.
In our case the lesion was seen in the maxillary region involving the incisors, in a male
patient aged 22 with a mild supragingival stains and interdental bone loss. It measures
approximately 1.5x2.0 cm, sessile mass with well-defined margins and pebbled surface.
International Journal of Innovations in Dental Sciences / January 2018 / Vol 3 / Issue 1 34
Peripheral Cemento-Ossifying Fibroma- A Case Report
Postoperative infection is an uncommon complication of periodontal surgery. It appears that
infection is more likely to occur in association with bone exposure, flap displacement, where
periodontal lesions are the result of pulp degeneration. In association with sutures and
particles of impacted debris, in areas of tissue laceration and impaired vascularization add
calculus and bacterial plaque have been accidently impacted into the tissues. Aspects of
wound healing were considered before the start of the procedure.
Radiographically PCOF varies from completely no changes to areas of calcification
depending upon the degree of mineralization. Superficial bone loss, cupping defect and focal
areas calcification have been reported in some cases11. Present case shows intra-crestal bone
loss.
The reported gingival overgrowth has been clearly diagnosed as peripheral cemento-ossifying
fibroma after histopathologic examination. Clinical picture of less vascular growth rules out
the possibility of pyogenic granuloma.
The treatment of choice for PCOF is excision of the mass with removal of peripheral and
deep margins including both the periodontal ligament and the affected periosteal component
following a thorough scaling & root planning.12 Long term postoperative follow-up is
extremely important because of the high growth potential of incompletely removed lesion and
a relatively high recurrence rate of approximately 20%.
CONCLUSION
The diagnosis of peripheral cemento-ossifying fibroma based only on clinical aspects can be
difficult and therefore histopathological examination of the surgical specimen obtained by
excisional biopsy is mandatory for an accurate diagnosis.
International Journal of Innovations in Dental Sciences / January 2018 / Vol 3 / Issue 1 35
Peripheral Cemento-Ossifying Fibroma- A Case Report
Figure.1. Photograph showing gingival
overgrowth in relation to 11 & 21.
Figure.2. Intra oral Peri Apical showing
crestal bone loss in relation to 11 & 21.
Figure.3. Photograph showing excised tissue.
International Journal of Innovations in Dental Sciences / January 2018 / Vol 3 / Issue 1 36
Peripheral Cemento-Ossifying Fibroma- A Case Report
Figure.4. Photograph showing postoperative
view at 3 months.
Figure.5. Low power photomicrograph showing
epithelium overlying connective tissue
component (H & E stain, X 10)
Figure.6. High power photomicrograph
showing fibrocellular connective tissue
stroma along with cementum like masses
(H & E stain, 40x).
International Journal of Innovations in Dental Sciences / January 2018 / Vol 3 / Issue 1 37
Peripheral Cemento-Ossifying Fibroma- A Case Report
Figure.7. High power photomicrograph
showing bony trabeculae with peripheral
osteoblastic rimming in a fibrocellular
connective tissue stroma. (10x)
REFERENCES:
1.Eversole LR. Craniofacial fibrous dysplasia and ossifying fibroma. Oral Maxillofac Surg
Clin North Am 1997;9:632.
2.Keluskar V, Byakodi R, Shah N. Peripheral ossifying fibroma. J Indian Acad Oral Med
Radiol 2008;20:546.
3.Martins Junior JC, Keim FS, Kreibich MS. Peripheral Ossifying Fibroma of the Maxilla:
Case Report. Int Arch Otorhino-laryngol 2008;12:295-9.
4.Delbem A, Cunha R, Silva J, Soubhia A. Peripheral cementoossifying fibroma in child. a
follow-up of 4 years. Report of a case. Eur J Dent 2008;2:134-7.
5.Kenney JN, Kaugars GE, Abbey LM. Comparison between the peripheral ossifying
fibroma and peripheral odontogenic fibroma. J Oral Maxillofac Surg 1989;47:378-82.
6.Walters JD, Will JK, Hatfield RD, Cacchillo DA, Raabe DA.Excision and repair of the
peripheral ossifying fibroma: a report of 3 cases. J Periodontol 2001;72:939-44.
7.Orkin DA, Amaidas VD. Ossifying fibrous epulis—an abbreviated case report. Oral Surg
Oral Med Oral Pathol 1984;57:147-148.
International Journal of Innovations in Dental Sciences / January 2018 / Vol 3 / Issue 1 38
Peripheral Cemento-Ossifying Fibroma- A Case Report
8.Neville BW, Damm DD, Allen CM, Bouquot JE. Oral and Maxillofacial Pathology. 3rd ed.
St. Louis, MO: Elsevier; 2009:451-452.
9. Priyavadhana P, Julius A, et al. Wound Healing in Periodontics BIOSCIENCES
BIOTECHNOLOGY RESEARCH ASIA, August 2014. Vol. 11(2), 791-796.
10.Verdine Virginia Antony, Rahamathulla Khan. Peripheral Cemento- Ossifying Fibroma–A
Case Report. IOSR Journal of Dental and Medical Sciences Volume 6, Issue 3.May- Jun.
2013: 34-37.
11.G Sujatha, G Sivakumar, J Muruganandhan, J Selvakumar, M Ramasamy. Peripheral
Ossifying Fibroma-Report of a case. Indian Journal of Multidisciplinary Dentistry, vol.2,
Issue 1:Nov2011 - Jan2012.
International Journal of Innovations in Dental Sciences / January 2018 / Vol 3 / Issue 1 39
You might also like
- The Cure For All DiseasesDocument631 pagesThe Cure For All DiseasesMirna98% (100)
- Translation of A Paper Entitled Die Schizoiden Psychopathien Im Kindersalten - GE Ssucharewa 1926-By S Wolff 1996Document14 pagesTranslation of A Paper Entitled Die Schizoiden Psychopathien Im Kindersalten - GE Ssucharewa 1926-By S Wolff 1996Leonardo Alvarez50% (2)
- The Vagina Bible by Jennifer Gunter, MDDocument11 pagesThe Vagina Bible by Jennifer Gunter, MDsimas100% (1)
- Lesson Plan DepressionDocument7 pagesLesson Plan DepressionAnnapurna Dangeti50% (2)
- Dental Journal: Peripheral Ossifying Fibroma of The Anterior Maxillary GingivaDocument5 pagesDental Journal: Peripheral Ossifying Fibroma of The Anterior Maxillary Gingivaanugraha GanendraNo ratings yet
- Peripheral Cemento-Ossifying Fibroma - A Case Report With A Glimpse On The Differential DiagnosisDocument5 pagesPeripheral Cemento-Ossifying Fibroma - A Case Report With A Glimpse On The Differential DiagnosisnjmdrNo ratings yet
- Odontoma Vaka RaporuDocument4 pagesOdontoma Vaka RaporutasbetulNo ratings yet
- JOralMaxillofacRadiol3270-5211945 142839Document6 pagesJOralMaxillofacRadiol3270-5211945 142839Ankit SahaNo ratings yet
- Case Report Massive Radicular Cyst in The Maxillary Sinus As A Result of Deciduous Molar Tooth Pulp NecrosisDocument5 pagesCase Report Massive Radicular Cyst in The Maxillary Sinus As A Result of Deciduous Molar Tooth Pulp NecrosisSarah Ariefah SantriNo ratings yet
- Peripheral Ossifying Fi Broma: ASE EportDocument4 pagesPeripheral Ossifying Fi Broma: ASE Eporterr3sNo ratings yet
- Exophytic Gingival LesionsDocument8 pagesExophytic Gingival LesionsAlexandra ElenaNo ratings yet
- Marsupialização Tracionamento CistodentigeroDocument10 pagesMarsupialização Tracionamento CistodentigeroLucas SantiagoNo ratings yet
- A Parulis-Like Soft Tissue Tumor in Relation With A Dental Implant: Case ReportDocument3 pagesA Parulis-Like Soft Tissue Tumor in Relation With A Dental Implant: Case ReportDr. AtheerNo ratings yet
- Odontogenic FibromaDocument5 pagesOdontogenic FibromaGowthamChandraSrungavarapuNo ratings yet
- Apical Approach To The Treatment of Peri-Implantitis in The Esthetic Zone - Nonincised Papillae Surgical Approach (NIPSA) - Case ReportsDocument13 pagesApical Approach To The Treatment of Peri-Implantitis in The Esthetic Zone - Nonincised Papillae Surgical Approach (NIPSA) - Case ReportsCentro Dental IntegralNo ratings yet
- IJRID28Document10 pagesIJRID28Saurabh SatheNo ratings yet
- Surgical and Endodontic Management of Large Cystic Lesion: AbstractDocument5 pagesSurgical and Endodontic Management of Large Cystic Lesion: AbstractanamaghfirohNo ratings yet
- Article-PDF-Vajendra Joshi Kalwa Pavan Kumar Shalini Joshi Sujatha Gopal-177Document3 pagesArticle-PDF-Vajendra Joshi Kalwa Pavan Kumar Shalini Joshi Sujatha Gopal-177sagarjangam123No ratings yet
- Nasopalatine Duct Cyst - A Delayed Complication To Successful Dental Implant Placement - Diagnosis and Surgical Management - As Published in The JOIDocument6 pagesNasopalatine Duct Cyst - A Delayed Complication To Successful Dental Implant Placement - Diagnosis and Surgical Management - As Published in The JOIHashem Motahir Ali Al-ShamiriNo ratings yet
- Periodontal Plastic Surgery To Improve AestheticsDocument7 pagesPeriodontal Plastic Surgery To Improve AestheticsElizabet KalmykovaNo ratings yet
- Case Report: Surgical Management of Compound Odontoma Associated With Unerupted ToothDocument7 pagesCase Report: Surgical Management of Compound Odontoma Associated With Unerupted ToothDame rohanaNo ratings yet
- Dentigerous Cyst With Recurrent Maxillary Sinusitis A Case Report With Literature ReviewDocument4 pagesDentigerous Cyst With Recurrent Maxillary Sinusitis A Case Report With Literature ReviewAnne LydellNo ratings yet
- Jurnal Asli JR Radiologi - Unusual Giant Complex Odontoma A Case ReportDocument4 pagesJurnal Asli JR Radiologi - Unusual Giant Complex Odontoma A Case ReportAliaNo ratings yet
- Dentigerous Cyst Associated With An Upper Permanent Central Incisor: Case Report and Literature ReviewDocument6 pagesDentigerous Cyst Associated With An Upper Permanent Central Incisor: Case Report and Literature ReviewLucas SantiagoNo ratings yet
- Compound Odontoma Associated With Impacted Maxillary Anterior Teeth A Case ReportDocument4 pagesCompound Odontoma Associated With Impacted Maxillary Anterior Teeth A Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Maillet 2011 PDFDocument5 pagesMaillet 2011 PDFIsmaelFelixNo ratings yet
- 15l8m04Document4 pages15l8m04chd9r5hr5kNo ratings yet
- Management of A Large Cyst in Maxillary Region: A Case ReportDocument11 pagesManagement of A Large Cyst in Maxillary Region: A Case ReportAry NohuNo ratings yet
- 4phase II Periodontal TherapyDocument76 pages4phase II Periodontal TherapyKaraz StudiosNo ratings yet
- Saudi Journal of Pathology and Microbiology (SJPM) : Case ReportDocument3 pagesSaudi Journal of Pathology and Microbiology (SJPM) : Case ReportSuman ChaturvediNo ratings yet
- RecessionsDocument68 pagesRecessionsmaryamNo ratings yet
- Benign Cementoblastoma Associated With Primary Mandibular Second MolarDocument9 pagesBenign Cementoblastoma Associated With Primary Mandibular Second Molarcahya satriaNo ratings yet
- A Novel Technique For Retention of Obturator Following Maxillectomy in Mucormycosis-A Case ReportDocument4 pagesA Novel Technique For Retention of Obturator Following Maxillectomy in Mucormycosis-A Case ReportBalwantNo ratings yet
- Odonto MaDocument5 pagesOdonto MaashariNo ratings yet
- Gingival Recession and Various Root Coverage ProceduresDocument6 pagesGingival Recession and Various Root Coverage ProceduresKhalid G. AzouniNo ratings yet
- Conversion of Questonable AbutmentsDocument25 pagesConversion of Questonable Abutmentskavya ravuriNo ratings yet
- Lateral Periodontal Cysts Arising in Periapical Sites: A Report of Two CasesDocument5 pagesLateral Periodontal Cysts Arising in Periapical Sites: A Report of Two CasesTrianita DivaNo ratings yet
- Exostosis MandibularDocument6 pagesExostosis MandibularCOne Gomez LinarteNo ratings yet
- Benign Cementoblastoma Associated With Primary Mandibular Second MolarDocument9 pagesBenign Cementoblastoma Associated With Primary Mandibular Second Molarcahya satriaNo ratings yet
- Post Extraction Lingual Mucosal Ulceration With Bone NecrosisDocument4 pagesPost Extraction Lingual Mucosal Ulceration With Bone Necrosisandrianiputri916No ratings yet
- Periapical Cemento-Osseous Dysplasia Clinicopathological FeaturesDocument4 pagesPeriapical Cemento-Osseous Dysplasia Clinicopathological FeaturesCindyNo ratings yet
- The Preternatural First Premolar: A Ground Section Tooth Case ReportDocument3 pagesThe Preternatural First Premolar: A Ground Section Tooth Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Clinical: Idiopathic Gingival Fibromatosis Associated With Generalized Aggressive Periodontitis: A Case ReportDocument5 pagesClinical: Idiopathic Gingival Fibromatosis Associated With Generalized Aggressive Periodontitis: A Case Reportchakriy9No ratings yet
- Cementoblastoma Jinak Sebuah Laporan Kasus Yang Jarang Terjadi Dengan Kajian LiteraturDocument4 pagesCementoblastoma Jinak Sebuah Laporan Kasus Yang Jarang Terjadi Dengan Kajian LiteraturRayAdityaParipurnaNo ratings yet
- Dentigerous Cyst Associated With Transmigrated Mandibular Canine - A Case ReportDocument5 pagesDentigerous Cyst Associated With Transmigrated Mandibular Canine - A Case ReportIJAR JOURNALNo ratings yet
- Dens Evaginatus and Type V Canal Configuration: A Case ReportDocument4 pagesDens Evaginatus and Type V Canal Configuration: A Case ReportAmee PatelNo ratings yet
- Limte Do Recobrimento RadicularDocument8 pagesLimte Do Recobrimento RadicularGiovanna Lima Costa BarcelosNo ratings yet
- Adenomatoid Odontogenic Tumour of Maxilla A Case ReportDocument6 pagesAdenomatoid Odontogenic Tumour of Maxilla A Case ReportAthenaeum Scientific PublishersNo ratings yet
- Bony Ankylosis Mimicking Benign ChondromaDocument4 pagesBony Ankylosis Mimicking Benign ChondromaAnumita DekaNo ratings yet
- Dentigerous Cyst Associated With Permanent Maxillary Central Incisor: Report of Two CasesDocument4 pagesDentigerous Cyst Associated With Permanent Maxillary Central Incisor: Report of Two CasesAhmad MustafaNo ratings yet
- Case Report Dentigerous Cyst in Maxillary Sinus: A Rare OccurrenceDocument5 pagesCase Report Dentigerous Cyst in Maxillary Sinus: A Rare OccurrencemawarmelatiNo ratings yet
- Gingival Abscess Case ReportDocument4 pagesGingival Abscess Case ReportKrishan GuliaNo ratings yet
- Journal Occlusal 2Document4 pagesJournal Occlusal 2Felianda ThaliaNo ratings yet
- Management of Thin Gingival Biotype With Hard and Soft Tissue Augmentation Post Orthodontic TreatmentDocument6 pagesManagement of Thin Gingival Biotype With Hard and Soft Tissue Augmentation Post Orthodontic TreatmentAh-ragab HouseNo ratings yet
- Osseous Choristoma of The Periodontium: Case ReportDocument3 pagesOsseous Choristoma of The Periodontium: Case ReportAndykaYayanSetiawanNo ratings yet
- Jurnal Gilut 3Document3 pagesJurnal Gilut 3adintaNo ratings yet
- Fibrous Dysplasia of The Anterior Mandible A Rare HDocument6 pagesFibrous Dysplasia of The Anterior Mandible A Rare HyesikaichaaNo ratings yet
- Periapical Cemento-Osseous Dysplasia: Case ReportDocument13 pagesPeriapical Cemento-Osseous Dysplasia: Case ReportDha Dina SevofrationNo ratings yet
- Artigo 7Document25 pagesArtigo 7Júlia OliveiraNo ratings yet
- Dentigerous CystDocument6 pagesDentigerous CystZahid ManzoorNo ratings yet
- Treatment Planning and Seminars IDocument23 pagesTreatment Planning and Seminars Ialsakar26No ratings yet
- Abscesses of The Periodontium Article-PDF-bansi M Bhusari Rizwan M Sanadi Jayant R Ambulgeka-558Document4 pagesAbscesses of The Periodontium Article-PDF-bansi M Bhusari Rizwan M Sanadi Jayant R Ambulgeka-558Ferdinan PasaribuNo ratings yet
- Jpis 42 105Document5 pagesJpis 42 105Jean Pierre Alcántara VigoNo ratings yet
- Peri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentFrom EverandPeri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentNo ratings yet
- PAD vs. DVTDocument3 pagesPAD vs. DVTKrystel BatinoNo ratings yet
- Drug Education For Catch Up FridayDocument33 pagesDrug Education For Catch Up FridayCooleen100% (1)
- 2018 Surgical Rescue in Medical PatientsDocument11 pages2018 Surgical Rescue in Medical PatientsgiseladlrNo ratings yet
- E Maternal Adaptations To PregnancyDocument27 pagesE Maternal Adaptations To PregnancyGeraldine PatayanNo ratings yet
- Micro OBSDocument10 pagesMicro OBSMelchor Felipe SalvosaNo ratings yet
- Health Guard Brochure Print76Document22 pagesHealth Guard Brochure Print76fhnNo ratings yet
- Anemia in PregnancyDocument2 pagesAnemia in PregnancyAnonymous D0Eq9CZZONo ratings yet
- Inp Eval ExamDocument3 pagesInp Eval Examd1choosenNo ratings yet
- Apbd 1203 Topic 3Document56 pagesApbd 1203 Topic 3Anonymous wsqFdcNo ratings yet
- Antibacterial ActivityDocument31 pagesAntibacterial ActivityRatnesh SinghNo ratings yet
- Argumentative EssayDocument3 pagesArgumentative EssayJennie Del RosarioNo ratings yet
- Applsci 11 00816 v2Document16 pagesApplsci 11 00816 v2KhuleedShaikhNo ratings yet
- Global Practicesand Policiesof Organ Transplantationand Organ TraffickingDocument15 pagesGlobal Practicesand Policiesof Organ Transplantationand Organ TraffickingM Asif NawazNo ratings yet
- What To Do If Force VaccinatedDocument8 pagesWhat To Do If Force Vaccinated6bogota9100% (4)
- Chronic Liver Diseases & PLCCDocument56 pagesChronic Liver Diseases & PLCCibnbasheer100% (5)
- The Power of Physical ExerciseDocument5 pagesThe Power of Physical Exerciseapi-570993572No ratings yet
- Radical NephrectomyDocument3 pagesRadical NephrectomyBiggs JuntillaNo ratings yet
- Smile Reading ComprehensionDocument2 pagesSmile Reading ComprehensionAndrea Argoty100% (2)
- Apical: Elixir Terpin HydrateDocument3 pagesApical: Elixir Terpin Hydrateailene agustinNo ratings yet
- e97c7a82-8e5f-4cb6-bae0-6f90e5f1c198Document18 pagese97c7a82-8e5f-4cb6-bae0-6f90e5f1c198alex torresNo ratings yet
- Impaired Skin IntegrityDocument2 pagesImpaired Skin IntegrityVINCE ONATONo ratings yet
- Intrapartal Nursing Care 1 in The Delivery Room MrsDocument184 pagesIntrapartal Nursing Care 1 in The Delivery Room MrsRandy100% (2)
- Common and Uncommon Applications of Bowel Ultrasound With Pathologic Correlation in ChildrenDocument14 pagesCommon and Uncommon Applications of Bowel Ultrasound With Pathologic Correlation in Childrengrahapuspa17No ratings yet
- Hydrogel Dressings For Healing Diabetic Foot Ulcers (Review)Document56 pagesHydrogel Dressings For Healing Diabetic Foot Ulcers (Review)Alldila Hendy PsNo ratings yet
- (Download PDF) Gastrointestinal Emergencies 3Rd Edition Tony C K Tham Online Ebook All Chapter PDFDocument52 pages(Download PDF) Gastrointestinal Emergencies 3Rd Edition Tony C K Tham Online Ebook All Chapter PDFann.clabaugh151100% (14)
- Jamainternal Bosch 2023 Oi 230008 1678987522.54647-1Document9 pagesJamainternal Bosch 2023 Oi 230008 1678987522.54647-1Alirio Angulo QuinteroNo ratings yet