Professional Documents
Culture Documents
270 Full
270 Full
Uploaded by
leegutierrez9023Copyright:
Available Formats
You might also like
- The Third RomeDocument52 pagesThe Third Romejoedoedoedoe100% (1)
- Zeng 2019Document3 pagesZeng 2019Andrei MarianNo ratings yet
- Primary HyperparathyroidismDocument9 pagesPrimary HyperparathyroidismJamesNo ratings yet
- Clinicopathological Correlates of HyperparathyroidismDocument18 pagesClinicopathological Correlates of HyperparathyroidismmaryNo ratings yet
- Rachel I Gafni Hypoparathyroidism 2019Document10 pagesRachel I Gafni Hypoparathyroidism 2019Ibrahim SabraNo ratings yet
- Journal of Internal Medicine - 2018 - Nilsson - Primary Hyperparathyroidism Should Surgery Be Performed On All PatientsDocument16 pagesJournal of Internal Medicine - 2018 - Nilsson - Primary Hyperparathyroidism Should Surgery Be Performed On All PatientsPryangka Viana MartinsNo ratings yet
- HyperparathyroidismDocument15 pagesHyperparathyroidismMuhamad ZulfiqarNo ratings yet
- Parathyroid Gland and Other Endocrine GlandsDocument35 pagesParathyroid Gland and Other Endocrine GlandsDrRahma Ali HeissNo ratings yet
- Surgical Management of Parathyroid Disease: Endocrine SurgeryDocument7 pagesSurgical Management of Parathyroid Disease: Endocrine SurgeryNiatazya Mumtaz SagitaNo ratings yet
- Primary HyperparathyroidismDocument16 pagesPrimary HyperparathyroidismHamza AhmedNo ratings yet
- A Case of Primary Hyperparathyroidism Secondary To Parathyroid Adenoma in A Pediatric PatientDocument4 pagesA Case of Primary Hyperparathyroidism Secondary To Parathyroid Adenoma in A Pediatric PatientTimothy supitNo ratings yet
- CA A Cancer J Clinicians - 2011 - Lewis - Oncologic Emergencies Pathophysiology Presentation Diagnosis and TreatmentDocument28 pagesCA A Cancer J Clinicians - 2011 - Lewis - Oncologic Emergencies Pathophysiology Presentation Diagnosis and TreatmentUtami DewiNo ratings yet
- New Directions in The Treatment of HypoparathyroidismDocument6 pagesNew Directions in The Treatment of Hypoparathyroidismmiguel saba sabaNo ratings yet
- The Diagnosis and Management of Inpatient HyponatrDocument7 pagesThe Diagnosis and Management of Inpatient Hyponatrbn3172005No ratings yet
- Naranjo 2017Document13 pagesNaranjo 2017enriquegarciagalianaNo ratings yet
- Parathyroid ImagingDocument6 pagesParathyroid ImagingjeffsunilNo ratings yet
- Jurnal 6Document21 pagesJurnal 6onisNo ratings yet
- Propofol Infusion Syndrome PDFDocument3 pagesPropofol Infusion Syndrome PDFPGI AnaesthesiaNo ratings yet
- Parathyroid Exploration For Primary Hyperparathyroidism - Uptodate 2022Document42 pagesParathyroid Exploration For Primary Hyperparathyroidism - Uptodate 2022juanrangoneNo ratings yet
- Jurnal PKDocument7 pagesJurnal PKGrace Yuni Soesanti MhNo ratings yet
- Hypoparathyroidism NEJM 2019 PDFDocument10 pagesHypoparathyroidism NEJM 2019 PDFalejandro toro riveraNo ratings yet
- ACFrOgAPsgsrLSMj4KGZ7fNxUWKzqWnBnsjwt-EBEWZ2RmyLwyzk7 w176irtJOx 3tL3bzlDNXU8IWMle9y-XqupqwUwc2hUjaAL5FY1kgteii33Z6eaOw Dn7q9q6DiyPs5X00vTqtQV6CoZ6lDocument7 pagesACFrOgAPsgsrLSMj4KGZ7fNxUWKzqWnBnsjwt-EBEWZ2RmyLwyzk7 w176irtJOx 3tL3bzlDNXU8IWMle9y-XqupqwUwc2hUjaAL5FY1kgteii33Z6eaOw Dn7q9q6DiyPs5X00vTqtQV6CoZ6lEmanuel D. Bejarano LiraNo ratings yet
- Disorders of Calcium, Magnesium, and Phosphate BalanceDocument20 pagesDisorders of Calcium, Magnesium, and Phosphate BalanceMarcela HincapiéNo ratings yet
- Parathyroid Gland Diseases: Classification of Diseases of PTGDocument11 pagesParathyroid Gland Diseases: Classification of Diseases of PTGgashbin latifNo ratings yet
- Propofol Infusion Syndrome ContinDocument3 pagesPropofol Infusion Syndrome Continzidni fatayanNo ratings yet
- IDK HiperparatiroidDocument23 pagesIDK HiperparatiroidWidya GladiantariNo ratings yet
- Hungry Bone Syndrome After Parathyroidectomy For Primary Hyperthyroidism 2161 1076 4 168Document5 pagesHungry Bone Syndrome After Parathyroidectomy For Primary Hyperthyroidism 2161 1076 4 168oki harisandiNo ratings yet
- Bilezikian 2017Document11 pagesBilezikian 2017Widya Arina WinataNo ratings yet
- HiperparatiroidDocument23 pagesHiperparatiroidrahmaNo ratings yet
- 1-7 BaileysDocument7 pages1-7 BaileysAura NirwanaNo ratings yet
- 4 EctDocument9 pages4 EctFebri Dwi HaryonoNo ratings yet
- Parathyroid, HyperparathyroidismDocument4 pagesParathyroid, Hyperparathyroidismjamil aoudeNo ratings yet
- Parathyroid DisordersDocument44 pagesParathyroid DisordersBIAN ALKHAZMARI100% (1)
- Anesthetic Management in Conn's Syndrome and PheochromocytomaDocument35 pagesAnesthetic Management in Conn's Syndrome and PheochromocytomaShashikant RamNo ratings yet
- Propofol Infusion Syndrome: Ne-Hooi Will Loh Mbbs Edic Frca Fficm Priya Nair Mbbs Frca FficmDocument3 pagesPropofol Infusion Syndrome: Ne-Hooi Will Loh Mbbs Edic Frca Fficm Priya Nair Mbbs Frca FficmAlexandra CojocaruNo ratings yet
- Actualizaciones Oaragangliomas Sociedad EndocrinoDocument9 pagesActualizaciones Oaragangliomas Sociedad EndocrinoCharly FlowNo ratings yet
- SD Nefrotico en AdultosDocument6 pagesSD Nefrotico en AdultosSebastian Ignacio Vega GonzalezNo ratings yet
- Pituitary Apoplexy Pathophysiology Diagnosis and MDocument6 pagesPituitary Apoplexy Pathophysiology Diagnosis and MlathifatulNo ratings yet
- Primary HyperparathyroidismDocument50 pagesPrimary HyperparathyroidismKate ClarksonNo ratings yet
- Hyperparathyroidism Main Jan 2020Document20 pagesHyperparathyroidism Main Jan 2020paingmyint100% (1)
- Cancer and CarcenoidDocument8 pagesCancer and Carcenoidmm7--No ratings yet
- Management of Perinatal AsphyxiaDocument4 pagesManagement of Perinatal AsphyxiaBharath Reddy DNo ratings yet
- 10 1001@jama 2020 0538Document2 pages10 1001@jama 2020 0538Julio Alberto VásquezNo ratings yet
- Acute Porpyria Management GuidelineDocument24 pagesAcute Porpyria Management GuidelineGPNNo ratings yet
- HypercalcemiaDocument6 pagesHypercalcemiajamil aoudeNo ratings yet
- Chapter 5: Electrolyte and Acid - Base Disorders in MalignancyDocument7 pagesChapter 5: Electrolyte and Acid - Base Disorders in MalignancyPratita Jati PermatasariNo ratings yet
- TMP 9 EFADocument5 pagesTMP 9 EFAFrontiersNo ratings yet
- Hypercalcemia: Etiology and Management: Amanda Demauro Renaghan and Mitchell H. RosnerDocument3 pagesHypercalcemia: Etiology and Management: Amanda Demauro Renaghan and Mitchell H. RosnerbabiNo ratings yet
- Afp 20180601 P 741Document9 pagesAfp 20180601 P 741Deni IrwandiNo ratings yet
- FERRET - Evaluating and Stabilizing The Critical FerretDocument7 pagesFERRET - Evaluating and Stabilizing The Critical Ferrettaner_soysurenNo ratings yet
- Pattern of Electrolyte Imbalance in Hospitalized Diabetic Patients: Experience in A Tertiary Care HospitalDocument5 pagesPattern of Electrolyte Imbalance in Hospitalized Diabetic Patients: Experience in A Tertiary Care HospitalSyed Shakil AhmedNo ratings yet
- Nejmcp 2113128Document9 pagesNejmcp 2113128Jordi Piñeros AriasNo ratings yet
- Para ThyroidDocument41 pagesPara ThyroidAdham YounesNo ratings yet
- Manejo Medico Hiperpoara Primario Mayo Clinic 2007Document5 pagesManejo Medico Hiperpoara Primario Mayo Clinic 2007Kenia LopezNo ratings yet
- Pe 08044Document4 pagesPe 08044Ro KohnNo ratings yet
- Calcium Metabolism-Board Questions 2018: Azar Khosravi April 2018Document55 pagesCalcium Metabolism-Board Questions 2018: Azar Khosravi April 2018Abdullah SiddiqiNo ratings yet
- 1 s2.0 S0085253815518541 MainDocument6 pages1 s2.0 S0085253815518541 MainaripNo ratings yet
- Paraneoplastic Hypercalcemia: Philip J. BergmanDocument3 pagesParaneoplastic Hypercalcemia: Philip J. BergmanYaya LaurenceNo ratings yet
- Nephrotic SyndromeDocument27 pagesNephrotic Syndromemerzi farooq ahmadkhanNo ratings yet
- Updates On Medical Management of HyperkalemiaDocument8 pagesUpdates On Medical Management of Hyperkalemiapaulina naranjoNo ratings yet
- Pilot Testing, Monitoring and Evaluating The Implementation of The CurriculumDocument34 pagesPilot Testing, Monitoring and Evaluating The Implementation of The CurriculumJoshua Dela Cruz Rogador100% (2)
- The Relational Attitude in Gestalt Therapy Theory and PracticeDocument15 pagesThe Relational Attitude in Gestalt Therapy Theory and PracticeAvtandilGogeshvili100% (1)
- Final ImmersionDocument14 pagesFinal ImmersionKzyrelle Aeyni Aparri PalañaNo ratings yet
- Stacey Bess: Nobody. After Bess Published Her First Book and Gained The Support of The Utah CommunityDocument2 pagesStacey Bess: Nobody. After Bess Published Her First Book and Gained The Support of The Utah CommunityRandom Thoughts - Baskar ArumugamNo ratings yet
- RS 1803 HFS BP Enterprise Artificial Intelligence (AI) Services 2018Document70 pagesRS 1803 HFS BP Enterprise Artificial Intelligence (AI) Services 2018pantmukulNo ratings yet
- Definition of Good GovernanceDocument3 pagesDefinition of Good GovernanceHaziq KhanNo ratings yet
- Migraine CorrectedDocument97 pagesMigraine CorrectedPranesh Peter100% (1)
- Nurse Entrepreneur: Name: Alex Kate C. Dela Year & Section: BSN 3-ADocument6 pagesNurse Entrepreneur: Name: Alex Kate C. Dela Year & Section: BSN 3-Akassy yeonNo ratings yet
- Marimba Grips AnalysisDocument16 pagesMarimba Grips Analysislewopxd100% (3)
- S3 Proofreading Answer 1-10Document10 pagesS3 Proofreading Answer 1-10Edwin FongNo ratings yet
- XIIBSTCh6S17082023014050 0Document13 pagesXIIBSTCh6S17082023014050 0Abdullah KhanNo ratings yet
- Dathathreya Stotras and Avadhootha GitaDocument138 pagesDathathreya Stotras and Avadhootha Gitaaditya kalekarNo ratings yet
- Define RX Path ImbalanceDocument4 pagesDefine RX Path Imbalancemedham100% (2)
- Lateral ThinkingDocument6 pagesLateral ThinkingKrengy TwiggAlinaNo ratings yet
- EEE 209 Presentation 1 IntroductionDocument8 pagesEEE 209 Presentation 1 IntroductionMert YılmazNo ratings yet
- Ipw WRDocument176 pagesIpw WRMay FaroukNo ratings yet
- HW 5Document15 pagesHW 5ottoporNo ratings yet
- Sense of BelongingnessDocument25 pagesSense of BelongingnessSrirrangam MathewNo ratings yet
- ReportDocument28 pagesReportQuincy PhiriNo ratings yet
- Review of Mcpherson Strut Suspension (Courtesy of Science Direct)Document4 pagesReview of Mcpherson Strut Suspension (Courtesy of Science Direct)Srikar ChinmayaNo ratings yet
- CPS MotorolaDocument92 pagesCPS MotorolaAbdelilah CharboubNo ratings yet
- 2014 - Design Thinking Research - Building Innovation Eco-Systems PDFDocument254 pages2014 - Design Thinking Research - Building Innovation Eco-Systems PDFABDIEL ADRIAZOLA MURIELNo ratings yet
- The Bobo Doll ExperimentDocument23 pagesThe Bobo Doll ExperimentManiya Dianne ReyesNo ratings yet
- 5564 Quantitative TechniquesDocument8 pages5564 Quantitative TechniquesTalat RaniNo ratings yet
- Project Front PagesDocument7 pagesProject Front PagesbhaveshpipaliyaNo ratings yet
- En Banc (G.R. No. L-8964. July 31, 1956.) JUAN EDADES, Plaintiff-Appellant, vs. SEVERINO EDADES, ET AL., Defendants-AppelleesDocument21 pagesEn Banc (G.R. No. L-8964. July 31, 1956.) JUAN EDADES, Plaintiff-Appellant, vs. SEVERINO EDADES, ET AL., Defendants-AppelleesTetris BattleNo ratings yet
- OralComm Q2 W6 GLAKDocument20 pagesOralComm Q2 W6 GLAKCherryl GallegoNo ratings yet
- 3.imbalanced NutritionDocument8 pages3.imbalanced NutritionAgoenk PrabowoNo ratings yet
- The Neuroscience Joyful Education Judy Willis MDDocument6 pagesThe Neuroscience Joyful Education Judy Willis MDcecilitusNo ratings yet
270 Full
270 Full
Uploaded by
leegutierrez9023Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
270 Full
270 Full
Uploaded by
leegutierrez9023Copyright:
Available Formats
CME ENDOCRINOLOGY Clinical Medicine 2017 Vol 17, No 3: 270–3
Hypercalcaemia – presentation and management
Author: Jeremy J O Turner
Hypercalcaemia is a common disorder normally caused renal colic and abdominal pain related to constipation or peptic
ABSTRACT
by primary hyperparathyroidism (PHPT) or malignancy. ulceration. Symptomatic patients may also experience polyuria
A proportion of cases present as an emergency, which and polydipsia secondary to nephrogenic diabetes insipidus
carries a significant mortality. Emergency management of and intellectual obtundation. As the severity of hypercalcaemia
hypercalcaemia is based on intravenous rehydration with progresses, nausea, vomiting, QT shortening potentially
normal saline but when this is inadequate, bisphosphonate leading to ventricular fibrillation arrest, confusion and coma
therapy is used; more recently the novel anti-resorbtive may occur. Physical signs of hypercalcaemia are relatively few
agent denosumab has been shown to have a useful role in but include band keratopathy, although this is very rare, and
treatment. It is estimated that up to 10% of all cases of PHPT signs related to the aetiology of the hypercalcaemia. Classical
presenting under the age of 45 years have an underlying radiographic features of PHPT, although rarely seen, include
genetic predisposition; nine potentially causative genes are now resorption of the distal ends of the clavicles, sub periosteal
recognised and may be screened in routine clinical practice. erosions on the radial borders of the middle or terminal
Although parathyroidectomy is the only curative treatment for phalanges, brown tumours and ‘pepperpot skull’.
PHPT, this is indicated in a minority of cases. Many cases can be
adequately managed conservatively and guidance from the 4th Differential diagnosis
international workshop on the management of asymptomatic
PHPT has recently been updated in a consensus statement. The two commonest causes of hypercalcaemia are
PHPT and malignancy. Other causes include tertiary
hyperparathyroidism, granulomatous disorders (principally
Introduction sarcoidosis), thyrotoxicosis, drugs (principally thiazides but
Hypercalcaemia is a common disorder, accounting for poorly monitored therapy with alfacalcidol and calcitriol are
approximately 0.6% of all acute medical admissions.1 Its important causes of hypercalcaemia, and lithium therapy
prevalence in the general population is up to 1/1,000. It is may also be associated with hypercalcaemia due to Li-induced
most commonly due to primary hyperparathyroidism or PHPT), excessive ingestion of calcium carbonate (‘milk alkali
malignancy although there are numerous other causes.2 syndrome’), vitamin D toxicity, vitamin A intoxication,
The classical symptomatic presentation of hypercalcaemia is
seen relatively rarely in the developed world, the commonest
Key points
presentation being asymptomatic detection on biochemical
testing. Management of hypercalcaemia depends on the Nine potentially causative genes are now implicated in primary
presentation and underlying cause; while severe hypercalcaemia hyperparathyroidism (PHPT)
(>3.5 mmol/L) requires emergency management,3 a significant
proportion of asymptomatic mild hypercalcaemia is due to
Guidance on management of asymptomatic PHPT was recently
primary hyperparathyroidism (PHPT) and is amenable to
updated in the 4th international consensus guidelines
conservative management.
Cinacalcet is licensed for PHPT and its role is recognised in the
Presentation
4th international consensus guidelines
The commonest presentation is detection of a raised serum
calcium concentration on a biochemical screen. If symptoms Denosumab is recognised to have a role in the emergency
are present, classically they are ‘moans, bones, stones and management of hypercalcaemia
groans’ referring to depressed mood, musculoskeletal pain,
Pre-operative parathyroid imaging is increasingly being
performed by SPECT CT
Author: Consultant endocrinologist and clinical director,
Department of Diabetes & Endocrinology, Norfolk and Norwich KEYWORDS: Hypercalcaemia, hyperparathyroidism, malignancy,
University Hospital; honorary professor, Norwich Medical School; co parathyroidectomy, SPECT ■
director, NIHR CRN:Eastern Research Network, Norwich, UK .
270 © Royal College of Physicians 2017. All rights reserved.
CMJv17n3-Turner.indd 270 15/05/17 1:12 PM
CME Endocrinology
> True ectopic production of PTH is very rare. Of course, a
Table 1. Genes potentially implicated in primary
diagnosis of carcinoma does not rule out the simultaneous
hyperparathyroidism presence of PHPT, which is common.
Disorder Gene
MEN1 MEN1 Investigations
MEN2 RET It is assumed throughout that calcium levels are adjusted for the
MEN4 CDKN1B albumin concentration according to the widely used formula:
HPT-JT CDC73 Adjusted calcium = Total calcium – 0.02 (40–Albumin)
FIHPT MEN1, CDC73, CASR, CDKN1A, CDKN2B, CDKN2C where calcium is measured in mmol/L and albumin in g/L.
NSPHPT CASR There is, however, some debate as to whether this formula
is universally appropriate or whether individual labs should
nsPHPT PTH
derive local adjustment formulae.7
MEN1/2/4 = multiple endocrine neoplasia type 1/2/4; HPT-JT = Broadly speaking, if PTH is detectable in the presence
hyperparathyroidism jaw tumour syndrome; FIHPT = familial isolated
of hypercalcaemia then the cause of the hypercalcaemia is
hyperparathyroidism; NSPHPT = neonatal severe primary hyperparathyroidism;
nsPHPT = non syndromic primary hyperparathyroidism. usually primary (sometimes tertiary) hyperparathyroidism.
Conversely, if the PTH level is suppressed, then the cause is
likely malignancy, although consideration of other PTH-
immobilisation, familial hypocalciuric hypercalcaemia (FHH) independent pathologies should be undertaken. However, two
and untreated Addison's disease. caveats to this approach should be considered. Firstly, while
Tertiary hyperparathyroidism occurs in the context of most laboratories will quote a reference range for PTH in the
long-standing secondary hyperparathyroidism where some region of 1.6–6.9 pmol/L, the lower limit of this reference range
degree of autonomy of parathyroid function arises and thus is very close to the lower limit of detection of the assay and
the calcium level rises inappropriately. FHH is a rare inherited therefore results at the lower end of the range require careful
disorder of calcium metabolism in which the set point for interpretation, specifically asking if the result is appropriate
serum calcium concentration is elevated, usually due to an for the clinical presentation. When in doubt, repeating the
inactivating mutation of the calcium sensing receptor gene,4 assay, discussing with the local laboratory and proceeding with
leading to lifelong and usually asymptomatic elevation of other investigations to rule out other possible pathology are all
serum calcium with normal or slightly elevated PTH levels and reasonable approaches. Secondly, FHH and PHPT may have
reduced urinary calcium excretion. indistinguishable serum biochemistry and conventionally,
the only way to separate these two conditions is by urinary
Primary hyperparathyroidism biochemistry – specifically, the calcium to creatinine clearance
ratio (FHH<0.01 versus PHPT>0.01). This is calculated from
Approximately 85% of all PHPT arises because of a solitary simultaneous measurements of urine and plasma calcium and
parathyroid adenoma, 1% are due to parathyroid carcinoma creatinine concentrations using the following formula:
and the remainder are due to multiple adenomata or
multi-gland hyperplasia.5 Although the majority of PHPT CaCl/CrCl = (urine calcium × plasma creatinine)/(plasma
is sporadic, a proportion arises on the background of a calcium × urine creatinine)
familial predisposition and abnormalities in a number of
potential genes are now recognised (Table 1).6 Thus, during The plasma creatinine concentration needs to be converted to
clinical assessment of PHPT, a family history should always the same units as the other parameters (mmol/L).
be sought and the physician should remain vigilant for other The 25 OH vitamin D level should be measured when
endocrinopathies as may be seen in, for example, multiple investigating hypercalcaemia. This allows the detection
endocrine neoplasia (MEN)1. Occurrence of PHPT at a young of vitamin D toxicity and, more importantly, vitamin D
age (approximately <45 years) and/or presence of multi-gland deficiency, which is common in PHPT and should be corrected
disease should also prompt consideration of this possibility. as part of the management.
Other investigations should be performed depending on the
results of the initial investigations, as follows:
Malignancy
1 Parathyroid localisation should be carried out if surgical
Up to 20% of all cases of carcinoma will be affected by
management is appropriate, but it should be noted that the
hypercalcaemia at some point during their clinical course.2
purpose of such imaging is not to confirm the diagnosis of
Several mechanisms account for hypercalcaemia due to
PHPT but rather to localise the target gland pre-operatively.
malignancy:
Conventional practice has been to perform ultrasound and
> Humoral hypercalcaemia of malignancy arises because of Sesta-MIBI nuclear imaging, although the literature gives
secretion of PTHrP. wide ranges for sensitivity for these, with typical values
> Osteolytic metastases. often in the region of 50–70%,8 and concordance between
> A limited range of neoplasms express 1 alpha hydroxylase and these modalities is suboptimal. When scans are concordant,
are able to activate vitamin D to the active 1,25 dihydroxylated parathyroidectomy will often be performed as a day case
form and drive hypercalcaemia. Lymphomas are the procedure, as minimal neck dissection is required. Where
commonest tumour in this category. there is non-concordance or complete failure of localisation,
© Royal College of Physicians 2017. All rights reserved. 271
CMJv17n3-Turner.indd 271 15/05/17 1:12 PM
CME Endocrinology
A (ESR), immunoglobulins, protein electrophoresis, urinary
Bence Jones proteins and/or serum free light chains, as well
as CXR, liver function tests (LFTs), bone scans, abdominal
ultrasound etc as indicated by presenting symptoms and
signs. Although many cases of malignancy-associated
hypercalcaemia are due to tumoural PTHrP secretion, it is
rarely necessary to assay PTHrP levels and indeed this test is
not widely available. Conversely, if the clinical presentation
raises the possibility of sarcoidosis then chest X-ray, serum
angiotensin-converting enzyme, 1,25 (OH)2 vitamin D levels
and biopsy of appropriate tissue will usually be indicated.
If other causes are suspected then presenting clinical
features should alert the physician to these possibilities and
appropriate further investigations should be arranged.
3 Increasingly, genetic testing is becoming a routine part of the
investigation of a case of hypercalcaemia, specifically where
primary hyperparathyroidism is suspected to be part of an
inherited endocrinopathy or where the diagnosis is suspected
to be FHH. It is estimated that up to 10% of cases of PHPT
B
presenting below the age of 45 arise on the background of a
germline mutation and there are now nine genes recognised
to predispose to PHPT (Table 1).
Consideration of genetic testing is appropriate where a family
history of hypercalcaemia is apparent, where other features
of one of the above syndromes are present or where the age of
presentation is unusually low thereby raising the prior probability
of an abnormality in one of the causal genes. While the calcium
sensing receptor gene (CASR) is recognised as one of the causal
genes for FIHPT, it is also the causal gene for FHH1, wherein
inactivating mutations lead to an elevated set point for adjusted
serum calcium levels. Two other FHH variants and their causal
genes are also now recognised: FHH2 and FHH3, respectively
arising because of mutations in the GNA11 and AP2S1 genes.10
Management
Emergency management
Intravenous hydration with normal saline to restore calciuresis
should be the mainstay of management. In cases where this is
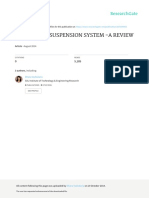
Fig 1. SPECT CT images of parathyroid adenoma. Fused (A) axial
and (B) coronal SPECT CT images showing a superior left parathyroid inadequate even after full and thorough rehydration (which
adenoma adjacent to the oesophagus posterior to the left lobe of thyroid. can take 24 hours or more), where there is no prospect of
Physiological uptake in the parotid glands is also seen. SPECT = single identification and definitive treatment of the underlying cause or
photon emission computerised tomography where attempts at definitive treatment would not be appropriate,
then the next step is usually intravenous bisphosphonate therapy
(pamidronate or zoledronate).3 Traditionally, other options for
the emergency management of hypercalcaemia have included
more extensive neck dissection will be required, with removal calcitonin, dialysis and mithramycin. However, more recently
of any enlarged or abnormal-appearing glands. However, the anti-resorbtive agent denosumab (licensed for treatment of
there is increasingly a move towards Single photon emission osteoporosis) is recognised as a useful adjunct in the emergency
computerised tomography (SPECT CT) scanning, which management of hypercalcaemia.11,12
combines both functional and cross sectional imaging into a
single investigation (Fig 1). This is a more efficient approach
PHPT
and provides sensitivity of up to 88%.9 It should be noted that
in genetic forms of PHPT pre-operative localisation is not The only curative treatment of hypercalcaemia due to
usually performed prior to a first neck exploration. hyperparathyroidism is parathyroidectomy, and where
2 If PHPT (and FHH) have been excluded then further patients are unequivocally symptomatic or markedly
tests will be required to elucidate whether the cause of hypercalcaemic there is usually little debate about proceeding
hypercalcaemia is associated with malignancy. In this to surgery. However, in cases of asymptomatic PHPT, where
scenario, PTH levels will be suppressed/undetectable and the hypercalcaemia is mild or where the patient may not have
further tests should include erythrocyte sedimentation rate long life expectancy or is unfit for surgery, other options
272 © Royal College of Physicians 2017. All rights reserved.
CMJv17n3-Turner.indd 272 15/05/17 1:12 PM
CME Endocrinology
and hypercalciura and relatively little evidence of benefit, on
Table 2. Recommended thresholds for consideration
balance expert opinion is therefore to do so cautiously.
of parathryoidectomy in management of Finally, although there are associations between PHPT and
asymptomatic PHPT cardiovascular risk and between PHPT and low quality of
Parameter Threshold for recommending surgery life, impaired cognition and other subtle neuro-cognitive
symptoms, the presence of these features should not be used as
Serum adjusted 0.25 mmol/L > upper limit of reference
indication for surgery until more definitive evidence of benefit
calcium range
is available. ■
Bone mineral density T score < –2.5 at lumbar spine, total
hip, femoral neck or distal 1/3 radius Conflicts of interest
Vertebral morphometry Presence of vertebral fracture detected The author has no conflicts of interest to declare.
by X-ray, CT, MRI or VFA
Creatinine clearance eGFR <60 mL/min/1.73m2 References
24-hour urine calcium >10 mmol/day by 24 hour urine 1 Dent DM, Miller JL, Klaff L, Barron J. The incidence and causes of
excretion analysis and increased stone risk by hypercalcaemia. Postgrad Med J 1987;63:745–50.
biochemical stone risk analysis 2 Goltzman D. Approach to Hypercalcemia. In: De Groot LJ,
Chrousos G, Dungan K et al (eds). Approach to Hypercalcemia.
Renal imaging Presence of nephrolithiasis or
South Dartmouth (MA): MDText.com, Inc.; 2000.
nephrocalcinosis on X-ray, USS or CT
3 Walsh J, Gittoes N, Selby P. Emergency management of acute
Age <50 years hypercalcaemia in adult patients. Endocr Connect 2016;5:G9-G11.
Thresholds given are according to consensus statement of fourth international
4 Pearce SH, Trump D, Wooding C et al. Calcium-sensing receptor
workshop on management of asymptomatic primary hyperparathyroidism.13 mutations in familial benign hypercalcemia and neonatal hyperpar-
Patients need only meet one of the above criteria for parathyroidectomy to athyroidism. J Clin Invest 1995;96:2683–92.
be indicated. CT = computerised tomography; eGFR = estimated glomerular 5 Marcocci C and Cetani F. Primary hyperparathyroidism. N Engl J
filtration rate; MRI = magnetic resonance imaging; USS = ultrasound scan; Med 2011; 365:2389–97.
VFA = vertebral fracture assessment. 6 Eastell R, Brandi ML, Costa AG et al. Diagnosis of asympto-
matic primary hyperparathyroidism: proceedings of the Fourth
International Workshop. J Clin Endocrinol Metab 2014;99:3570–9.
including conservative and medical management should be 7 Hughes D, Doery JCG, Choy KW, Flatman R. Calculated chemistry
considered. parameters – do they need to be harmonised? Clin Biochem Rev
There is now good guidance on when to operate and when to 2016;37:131–4.
consider conservative management in the consensus statement 8 Purcell GP, Dirbas FM, Jeffrey RB et al. Parathyroid localization
from the fourth international workshop on management of with high-resolution ultrasound and technetium Tc 99m sestamibi.
Arch Surg 1999;134:824–8.
asymptomatic primary hyperparathyroidism.13 These are
9 Treglia G, Sadeghi R, Schalin-Jäntti C et al. Detection rate of (99m)
summarised in Table 2. There is also now an evidence base on Tc-MIBI single photon emission computed tomography (SPECT)/
conservative management of primary hyperparathyroidism14. CT in preoperative planning for patients with primary hyperparathy-
In brief, this shows that the calcimimetic cinacalcet works in roidism: a meta-analysis. Head Neck 2016;38(Suppl 1):E2159–72.
mild to moderate hypercalcaemia to normalise serum calcium 10 Nesbit MA, Hannan FM, Howles SA et al. Mutations affecting
in approximately 70% of cases. It should be noted that it has G-protein subunit α11 in hypercalcemia and hypocalcemia. N Engl J
no beneficial effect on bone mineral density, although it does Med 2013;368:2476–86.
reduce urinary calcium excretion. The oral bisphosphonates 11 Karuppiah D, Thanabalasingham G, Shine B et al. Refractory
have good evidence for protecting bone mineral density but no hypercalcaemia secondary to parathyroid carcinoma: response to
evidence for fracture risk reduction in PHPT and no consistent high-dose denosumab. Eur J Endocrinol 2014;171:K1–5.
12 Adhikaree J, Newby Y, Sundar S. Denosumab should be the treat-
evidence for reduction of hypercalcaemia in PHPT.
ment of choice for bisphosphonate refractory hypercalcaemia of
Similarly, conservative management has also been shown to malignancy. BMJ Case Reports 2014;bcr2013202861.
be a relatively safe option so long as some degree of medical 13 Bilezikian JP, Brandi ML, Eastell R et al. Guidelines for the manage-
vigilance is maintained, although data now show that ment of asymptomatic primary hyperparathyroidism: summary
durations of conservative management in excess of 15 years statement from the fourth international workshop. J Clin Endocr
pose some risk with up to one third of cases progressing to Metab 2014;99:3561–9.
display overt features of the disease.15 Thus, monitoring for 14 Marcocci C, Bollerslev J, Khan AA, Shoback DM. Medical manage-
conservative management should include serum calcium ment of primary hyperparathyroidism: Proceedings of the Fourth
measurement annually, periodic DEXA scans, imaging if there International Workshop on the Management of Asymptomatic Primary
are symptoms (eg X-ray if height loss/back pain is experienced), Hyperparathyroidism. J Clin Endocrinol Metab 2014;99:3607–18.
15 Singh Ospina N, Maraka S, Rodriguez-Gutierrez R et al.
eGFR annually and, if stones are suspected, renal imaging.
Comparative efficacy of parathyroidectomy and active surveillance
With respect to DEXA scanning, the distal forearm may be in patients with mild primary hyperparathyroidism: a systematic
considered to be the most informative site for serial T-scores to review and meta-analysis. Osteoporos Int 2016;27:3395–407.
be measured as the predominantly cortical bone at this site is
most at risk of loss in PHPT. Address for correspondence: Professor Jeremy Turner, Norfolk
One other consideration in the management of and Norwich University Hospitals NHS Foundation Trust,
hypercalcaemia due to PHPT is vitamin D repletion: as Norwich NR4 7UY, UK.
there is a very small risk of exacerbating hypercalcaemia Email: jeremy.turner@nnuh.nhs.uk
© Royal College of Physicians 2017. All rights reserved. 273
CMJv17n3-Turner.indd 273 15/05/17 1:12 PM
You might also like
- The Third RomeDocument52 pagesThe Third Romejoedoedoedoe100% (1)
- Zeng 2019Document3 pagesZeng 2019Andrei MarianNo ratings yet
- Primary HyperparathyroidismDocument9 pagesPrimary HyperparathyroidismJamesNo ratings yet
- Clinicopathological Correlates of HyperparathyroidismDocument18 pagesClinicopathological Correlates of HyperparathyroidismmaryNo ratings yet
- Rachel I Gafni Hypoparathyroidism 2019Document10 pagesRachel I Gafni Hypoparathyroidism 2019Ibrahim SabraNo ratings yet
- Journal of Internal Medicine - 2018 - Nilsson - Primary Hyperparathyroidism Should Surgery Be Performed On All PatientsDocument16 pagesJournal of Internal Medicine - 2018 - Nilsson - Primary Hyperparathyroidism Should Surgery Be Performed On All PatientsPryangka Viana MartinsNo ratings yet
- HyperparathyroidismDocument15 pagesHyperparathyroidismMuhamad ZulfiqarNo ratings yet
- Parathyroid Gland and Other Endocrine GlandsDocument35 pagesParathyroid Gland and Other Endocrine GlandsDrRahma Ali HeissNo ratings yet
- Surgical Management of Parathyroid Disease: Endocrine SurgeryDocument7 pagesSurgical Management of Parathyroid Disease: Endocrine SurgeryNiatazya Mumtaz SagitaNo ratings yet
- Primary HyperparathyroidismDocument16 pagesPrimary HyperparathyroidismHamza AhmedNo ratings yet
- A Case of Primary Hyperparathyroidism Secondary To Parathyroid Adenoma in A Pediatric PatientDocument4 pagesA Case of Primary Hyperparathyroidism Secondary To Parathyroid Adenoma in A Pediatric PatientTimothy supitNo ratings yet
- CA A Cancer J Clinicians - 2011 - Lewis - Oncologic Emergencies Pathophysiology Presentation Diagnosis and TreatmentDocument28 pagesCA A Cancer J Clinicians - 2011 - Lewis - Oncologic Emergencies Pathophysiology Presentation Diagnosis and TreatmentUtami DewiNo ratings yet
- New Directions in The Treatment of HypoparathyroidismDocument6 pagesNew Directions in The Treatment of Hypoparathyroidismmiguel saba sabaNo ratings yet
- The Diagnosis and Management of Inpatient HyponatrDocument7 pagesThe Diagnosis and Management of Inpatient Hyponatrbn3172005No ratings yet
- Naranjo 2017Document13 pagesNaranjo 2017enriquegarciagalianaNo ratings yet
- Parathyroid ImagingDocument6 pagesParathyroid ImagingjeffsunilNo ratings yet
- Jurnal 6Document21 pagesJurnal 6onisNo ratings yet
- Propofol Infusion Syndrome PDFDocument3 pagesPropofol Infusion Syndrome PDFPGI AnaesthesiaNo ratings yet
- Parathyroid Exploration For Primary Hyperparathyroidism - Uptodate 2022Document42 pagesParathyroid Exploration For Primary Hyperparathyroidism - Uptodate 2022juanrangoneNo ratings yet
- Jurnal PKDocument7 pagesJurnal PKGrace Yuni Soesanti MhNo ratings yet
- Hypoparathyroidism NEJM 2019 PDFDocument10 pagesHypoparathyroidism NEJM 2019 PDFalejandro toro riveraNo ratings yet
- ACFrOgAPsgsrLSMj4KGZ7fNxUWKzqWnBnsjwt-EBEWZ2RmyLwyzk7 w176irtJOx 3tL3bzlDNXU8IWMle9y-XqupqwUwc2hUjaAL5FY1kgteii33Z6eaOw Dn7q9q6DiyPs5X00vTqtQV6CoZ6lDocument7 pagesACFrOgAPsgsrLSMj4KGZ7fNxUWKzqWnBnsjwt-EBEWZ2RmyLwyzk7 w176irtJOx 3tL3bzlDNXU8IWMle9y-XqupqwUwc2hUjaAL5FY1kgteii33Z6eaOw Dn7q9q6DiyPs5X00vTqtQV6CoZ6lEmanuel D. Bejarano LiraNo ratings yet
- Disorders of Calcium, Magnesium, and Phosphate BalanceDocument20 pagesDisorders of Calcium, Magnesium, and Phosphate BalanceMarcela HincapiéNo ratings yet
- Parathyroid Gland Diseases: Classification of Diseases of PTGDocument11 pagesParathyroid Gland Diseases: Classification of Diseases of PTGgashbin latifNo ratings yet
- Propofol Infusion Syndrome ContinDocument3 pagesPropofol Infusion Syndrome Continzidni fatayanNo ratings yet
- IDK HiperparatiroidDocument23 pagesIDK HiperparatiroidWidya GladiantariNo ratings yet
- Hungry Bone Syndrome After Parathyroidectomy For Primary Hyperthyroidism 2161 1076 4 168Document5 pagesHungry Bone Syndrome After Parathyroidectomy For Primary Hyperthyroidism 2161 1076 4 168oki harisandiNo ratings yet
- Bilezikian 2017Document11 pagesBilezikian 2017Widya Arina WinataNo ratings yet
- HiperparatiroidDocument23 pagesHiperparatiroidrahmaNo ratings yet
- 1-7 BaileysDocument7 pages1-7 BaileysAura NirwanaNo ratings yet
- 4 EctDocument9 pages4 EctFebri Dwi HaryonoNo ratings yet
- Parathyroid, HyperparathyroidismDocument4 pagesParathyroid, Hyperparathyroidismjamil aoudeNo ratings yet
- Parathyroid DisordersDocument44 pagesParathyroid DisordersBIAN ALKHAZMARI100% (1)
- Anesthetic Management in Conn's Syndrome and PheochromocytomaDocument35 pagesAnesthetic Management in Conn's Syndrome and PheochromocytomaShashikant RamNo ratings yet
- Propofol Infusion Syndrome: Ne-Hooi Will Loh Mbbs Edic Frca Fficm Priya Nair Mbbs Frca FficmDocument3 pagesPropofol Infusion Syndrome: Ne-Hooi Will Loh Mbbs Edic Frca Fficm Priya Nair Mbbs Frca FficmAlexandra CojocaruNo ratings yet
- Actualizaciones Oaragangliomas Sociedad EndocrinoDocument9 pagesActualizaciones Oaragangliomas Sociedad EndocrinoCharly FlowNo ratings yet
- SD Nefrotico en AdultosDocument6 pagesSD Nefrotico en AdultosSebastian Ignacio Vega GonzalezNo ratings yet
- Pituitary Apoplexy Pathophysiology Diagnosis and MDocument6 pagesPituitary Apoplexy Pathophysiology Diagnosis and MlathifatulNo ratings yet
- Primary HyperparathyroidismDocument50 pagesPrimary HyperparathyroidismKate ClarksonNo ratings yet
- Hyperparathyroidism Main Jan 2020Document20 pagesHyperparathyroidism Main Jan 2020paingmyint100% (1)
- Cancer and CarcenoidDocument8 pagesCancer and Carcenoidmm7--No ratings yet
- Management of Perinatal AsphyxiaDocument4 pagesManagement of Perinatal AsphyxiaBharath Reddy DNo ratings yet
- 10 1001@jama 2020 0538Document2 pages10 1001@jama 2020 0538Julio Alberto VásquezNo ratings yet
- Acute Porpyria Management GuidelineDocument24 pagesAcute Porpyria Management GuidelineGPNNo ratings yet
- HypercalcemiaDocument6 pagesHypercalcemiajamil aoudeNo ratings yet
- Chapter 5: Electrolyte and Acid - Base Disorders in MalignancyDocument7 pagesChapter 5: Electrolyte and Acid - Base Disorders in MalignancyPratita Jati PermatasariNo ratings yet
- TMP 9 EFADocument5 pagesTMP 9 EFAFrontiersNo ratings yet
- Hypercalcemia: Etiology and Management: Amanda Demauro Renaghan and Mitchell H. RosnerDocument3 pagesHypercalcemia: Etiology and Management: Amanda Demauro Renaghan and Mitchell H. RosnerbabiNo ratings yet
- Afp 20180601 P 741Document9 pagesAfp 20180601 P 741Deni IrwandiNo ratings yet
- FERRET - Evaluating and Stabilizing The Critical FerretDocument7 pagesFERRET - Evaluating and Stabilizing The Critical Ferrettaner_soysurenNo ratings yet
- Pattern of Electrolyte Imbalance in Hospitalized Diabetic Patients: Experience in A Tertiary Care HospitalDocument5 pagesPattern of Electrolyte Imbalance in Hospitalized Diabetic Patients: Experience in A Tertiary Care HospitalSyed Shakil AhmedNo ratings yet
- Nejmcp 2113128Document9 pagesNejmcp 2113128Jordi Piñeros AriasNo ratings yet
- Para ThyroidDocument41 pagesPara ThyroidAdham YounesNo ratings yet
- Manejo Medico Hiperpoara Primario Mayo Clinic 2007Document5 pagesManejo Medico Hiperpoara Primario Mayo Clinic 2007Kenia LopezNo ratings yet
- Pe 08044Document4 pagesPe 08044Ro KohnNo ratings yet
- Calcium Metabolism-Board Questions 2018: Azar Khosravi April 2018Document55 pagesCalcium Metabolism-Board Questions 2018: Azar Khosravi April 2018Abdullah SiddiqiNo ratings yet
- 1 s2.0 S0085253815518541 MainDocument6 pages1 s2.0 S0085253815518541 MainaripNo ratings yet
- Paraneoplastic Hypercalcemia: Philip J. BergmanDocument3 pagesParaneoplastic Hypercalcemia: Philip J. BergmanYaya LaurenceNo ratings yet
- Nephrotic SyndromeDocument27 pagesNephrotic Syndromemerzi farooq ahmadkhanNo ratings yet
- Updates On Medical Management of HyperkalemiaDocument8 pagesUpdates On Medical Management of Hyperkalemiapaulina naranjoNo ratings yet
- Pilot Testing, Monitoring and Evaluating The Implementation of The CurriculumDocument34 pagesPilot Testing, Monitoring and Evaluating The Implementation of The CurriculumJoshua Dela Cruz Rogador100% (2)
- The Relational Attitude in Gestalt Therapy Theory and PracticeDocument15 pagesThe Relational Attitude in Gestalt Therapy Theory and PracticeAvtandilGogeshvili100% (1)
- Final ImmersionDocument14 pagesFinal ImmersionKzyrelle Aeyni Aparri PalañaNo ratings yet
- Stacey Bess: Nobody. After Bess Published Her First Book and Gained The Support of The Utah CommunityDocument2 pagesStacey Bess: Nobody. After Bess Published Her First Book and Gained The Support of The Utah CommunityRandom Thoughts - Baskar ArumugamNo ratings yet
- RS 1803 HFS BP Enterprise Artificial Intelligence (AI) Services 2018Document70 pagesRS 1803 HFS BP Enterprise Artificial Intelligence (AI) Services 2018pantmukulNo ratings yet
- Definition of Good GovernanceDocument3 pagesDefinition of Good GovernanceHaziq KhanNo ratings yet
- Migraine CorrectedDocument97 pagesMigraine CorrectedPranesh Peter100% (1)
- Nurse Entrepreneur: Name: Alex Kate C. Dela Year & Section: BSN 3-ADocument6 pagesNurse Entrepreneur: Name: Alex Kate C. Dela Year & Section: BSN 3-Akassy yeonNo ratings yet
- Marimba Grips AnalysisDocument16 pagesMarimba Grips Analysislewopxd100% (3)
- S3 Proofreading Answer 1-10Document10 pagesS3 Proofreading Answer 1-10Edwin FongNo ratings yet
- XIIBSTCh6S17082023014050 0Document13 pagesXIIBSTCh6S17082023014050 0Abdullah KhanNo ratings yet
- Dathathreya Stotras and Avadhootha GitaDocument138 pagesDathathreya Stotras and Avadhootha Gitaaditya kalekarNo ratings yet
- Define RX Path ImbalanceDocument4 pagesDefine RX Path Imbalancemedham100% (2)
- Lateral ThinkingDocument6 pagesLateral ThinkingKrengy TwiggAlinaNo ratings yet
- EEE 209 Presentation 1 IntroductionDocument8 pagesEEE 209 Presentation 1 IntroductionMert YılmazNo ratings yet
- Ipw WRDocument176 pagesIpw WRMay FaroukNo ratings yet
- HW 5Document15 pagesHW 5ottoporNo ratings yet
- Sense of BelongingnessDocument25 pagesSense of BelongingnessSrirrangam MathewNo ratings yet
- ReportDocument28 pagesReportQuincy PhiriNo ratings yet
- Review of Mcpherson Strut Suspension (Courtesy of Science Direct)Document4 pagesReview of Mcpherson Strut Suspension (Courtesy of Science Direct)Srikar ChinmayaNo ratings yet
- CPS MotorolaDocument92 pagesCPS MotorolaAbdelilah CharboubNo ratings yet
- 2014 - Design Thinking Research - Building Innovation Eco-Systems PDFDocument254 pages2014 - Design Thinking Research - Building Innovation Eco-Systems PDFABDIEL ADRIAZOLA MURIELNo ratings yet
- The Bobo Doll ExperimentDocument23 pagesThe Bobo Doll ExperimentManiya Dianne ReyesNo ratings yet
- 5564 Quantitative TechniquesDocument8 pages5564 Quantitative TechniquesTalat RaniNo ratings yet
- Project Front PagesDocument7 pagesProject Front PagesbhaveshpipaliyaNo ratings yet
- En Banc (G.R. No. L-8964. July 31, 1956.) JUAN EDADES, Plaintiff-Appellant, vs. SEVERINO EDADES, ET AL., Defendants-AppelleesDocument21 pagesEn Banc (G.R. No. L-8964. July 31, 1956.) JUAN EDADES, Plaintiff-Appellant, vs. SEVERINO EDADES, ET AL., Defendants-AppelleesTetris BattleNo ratings yet
- OralComm Q2 W6 GLAKDocument20 pagesOralComm Q2 W6 GLAKCherryl GallegoNo ratings yet
- 3.imbalanced NutritionDocument8 pages3.imbalanced NutritionAgoenk PrabowoNo ratings yet
- The Neuroscience Joyful Education Judy Willis MDDocument6 pagesThe Neuroscience Joyful Education Judy Willis MDcecilitusNo ratings yet