Professional Documents
Culture Documents
Neurolocalization 2021
Neurolocalization 2021
Uploaded by
Kaleab0 ratings0% found this document useful (0 votes)
9 views87 pagesCopyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
9 views87 pagesNeurolocalization 2021
Neurolocalization 2021
Uploaded by
KaleabCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 87
Introduction: principles of neurolocalization
The somatosensory pathways
The spinal cord
The cerebral hemispheres
Differential diagnosis in neurology is based on
two main components determined rom the
clinical history and physical examination:
The localization of the neuroanatomic origin(s) of
the patient’s symptoms and signs
The time course over which these symptoms and
signs have arisen and evolved
Localization is the process of determining
where in the nervous system the patient’s
disease process is occurring:
Is the problem in the CNS, the PNS, or both?
Within the CNS, is there a lesion in the brain, brainstem,
cerebellum, or spinal cord?
More precisely, where is the lesion within those
structures?
Within the PNS, is the lesion at the level of one or
more spinal roots, dorsal root ganglia, peripheral
nerves, muscles, or at the NMJ?
Time course in neurologic diagnosis: determining
what the problem is
The time course of symptom onset and evolution may be
described as
Sudden/hyperacute (over seconds to minutes): vascular
Acute (over hours to days): infections, inflammatory,
metabolic, etc
Subacute (over days to weeks to months): infections,
inflammatory, etc
Chronic (over months to years): neoplastic,
neurodegenerative diseases, etc
NB: metabolic abnormalities, drugs, and toxins can cause
neurologic dys unction over nearly any time course
The cerebral hemispheres are where the motor
pathways originate, and where the somatosensory
pathways terminate
The left cerebral hemisphere controls the motor
functions of the right side of the body, and vice
versa
Motor:
The corticospinal tracts send motor information from the
cortex to the spinal cord
Sensory :
The anterolateral (or spinothalamic) tracts and
The dorsal (or posterior) column pathways
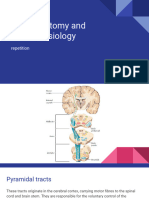
The Corticospinal Tracts (Pyramidal System)
The CST are the final output of the motor system
The convey the action plan to the alpha motor
neurons of the anterior horns of the spinal cord
The AHC, in turn, relay the signals to move the
muscles by way of peripheral nerves
Each CST begins in the motor cortex, which is
located in the precentral gyrus (anterior to the
central sulcus)
The motor cortex is organized by the region of the
body it controls
CST
Cortex (frontal lobe)
Corona radiata
Internal capsule
(posterior limb)
Brainstem: cerebral
peduncles of the
midbrain, basis pontis,
and medullary
pyramids
Cervicomedually
junction: Crosses to the
contralateral side at the
lower medulla (>85%)
Lateral CST
CST…
Synapse on alpha
motor neurons in the
AHC
Axons of the alpha
motor neurons leave
the ventral/anterior
spinal cord via
ventral roots and
enter peripheral
nerves to travel to
muscles
The pyarmidal motor system is a two-neuron
system
First-order neurons have their cell bodies in the
motor cortex
Their axons travel through the internal capsule,
brainstem, and spinal cord (CST)
Upper motor neurons
Second-order neurons have their cell bodies in the
AHC of the spinal cord
Their axons travel in peripheral nerves
Lower motor neurons
UMN: the neurons of the CNS component in
the brain/brainstem/ spinal cord (i.e., the CST)
LMN: the neurons of the PNS component
(AHC through the ventral roots into peripheral
nerves)
Lesions in the CST in the brain and brainstem
cause contralateral weakness
Lesions on one side of the spinal cord cause
ipsilateral weakness
UMN lesion LMN
Tone: increased Hyporeflexia or
(spastic) areflexia
DTR: increased Flaccid
(exaggerated) Atrophy (decreased
Plantar: extensor/up muscle bulk)
going/Babniski sign Fasciculation
present
Hoffmann sign
present
Pronator drift present
Pronator drift (can be present acutely)
The arms are held outstretched with the palms up
and fingers spread
The hand may begin to close and the arm may begin
to pronate and drift downward with UMN lesion
NB:
With parietal lesions, the affected arm may drift
upward due to impaired proprioception
UMN pattern of weakness (can be present
acutely)
The upper extremity extensors are weaker than the
flexors (DDx: radial nerve palsy)
I.e., the arm is stronger when flexing the elbow
compared to extending the elbow
The lower extremity flexors are weaker than the
extensors
I.e., the leg is stronger when extending the knee
compared to flexing the knee
The Corticobulbar Tracts
The muscles of the face, tongue, larynx, and
pharynx also have UMN and LMN
The upper motor neurons arise from the motor
cortex and travel with the CST as the corticobulbar
tracts
However, the corticobulbar fibers terminate in their
respective cranial nerve nuclei (c0ntralateral) in the
brainstem
The lower motor neurons arise in the cranial nerve
nuclei and travel in the cranial nerves
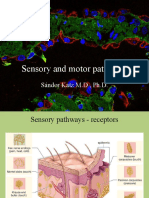
The sensory pathways begin in the periphery and
end in the brain
Sensory information from the skin (light touch,
pressure, pain, temperature, vibration) and from
the muscle spindles and the Golgi tendon organs
(proprioception) travels arrive in the dorsal root
ganglia
At the entrance to the spinal cord, somatosensory
information is “sorted” into two pathways:
The spinothalamic tracts (the anterolateral tracts): pain
and temperature information
The dorsal columns: proprioception and vibration
information
Light touch information travels in both pathways
Both sensory pathways
ascend through the
spinal cord and
brainstem to arrive at the
VPL nucleus of the
thalamus
The thalamus transmits
this somatosensory
information to the
somatosensory cortex in
the postcentral gyrus,
just posterior to the
motor strip
Sensory homunculus
Postcentral gyrus and
posterior part of the
paracentral lobule
NB: the location and
amount of cortex
assigned to the
processing of sensory
information from a
particular part of the
body
Two systems:
Dorsal columns (convey joint position sense,
vibration sense, and light touch senses)
Spinothalamic tracts (convey pain, temperature, and
crude touch senses)
Both cross to transmit sensory information
from one side of the body to the contralateral
cerebral hemisphere
However, the sites of crossing differ
The dorsal column system
crosses in the medulla, just
superior to the crossing of the
CST
Unilateral lesions of the dorsal
column pathway from the upper
medulla and superiorly affect
contralateral sensation
Unilateral lesions from the lower
medulla through the spinal cord
affect ipsilateral sensation
This pattern essentially mirrors
that of the corticospinal tracts
The anterolateral tracts cross
immediately after entering the
spinal cord (they actually
cross over the course of a few
spinal levels)
Unilateral lesions anywhere in
this pathway affect contralateral
sensation
A small patch of ipsilateral pain/
temperature loss involving the
spinal levels over which the tract
crosses may also be observed)
Brainstem
In the brainstem, the corticospinal tracts
travel in the anterior (ventral) portion,
whereas the sensory pathways are
predominantly dorsolateral
Brainstem lesions can cause crossed
signs:
Weakness and/or sensory changes in the
face ipsilateral to the lesion but in the
contralateral body
NB: Nearly all cranial nerves control
ipsilateral functions in the head
Crossed signs: since brainstem lesions
affect the not-yet-crossed CST and the
already-crossed ascending sensory tracts
Lamination of the long tracts in
the spinal cord
The arrangement of fibers within a
pathway
For the corticospinal, anterolateral,
and dorsal column pathways, this
refers to where the arm, leg, and torso
fibers run
CST
As the corticospinal tracts descend from
the brainstem, arm fibers synapse on
LMN in the cervical cord before leg
fibers
Hence, the CST fibers are laminated
such that the arm fibers are medial and
the leg fibers are lateral
The dorsal column fibers from
the feet and legs enter the
spinal cord at the lumbar and
sacral levels, and are pushed
medially by the addition of
trunk and arm fibers as the
tracts ascend
The dorsal columns are thus
laminated with the legs medial
and the arms lateral
The spinothalamic tracts’ feet
and leg fibers cross to the
contralateral side and are pushed
laterally as subsequent crossing
fibers or the trunk and arms
push them aside and layer more
medially
The spinothalamic tracts are thus
laminated with the arms medial and
the legs lateral like the corticospinal
tracts (similar to CST)
Brown-Séquard
(Hemicord) Syndrome
Ipsilateral weakness
below the level of the
lesion
Ipsilateral loss of
vibration sense and
proprioception below
the level of the lesion
Contralateral loss of
pain and temperature
sensation below the
level o the lesion
Anterior Cord Syndrome
Involves nearly the entire
cross sectional area of the
spinal cord with the
exception of the dorsal
columns
Motor function and pain and
temperature sensation are
impaired below the level of
the lesion
Both upper and lower motor
neuron signs may be seen
Occurs most commonly due
to infarction in the territory
of the anterior spinal artery
Central Cord Syndrome
Occurs most commonly
due to syrinx- usually in
the cervical spinal cord
The closest structure to
the central canal is the
anterior commissure
where the anterolateral
tracts cross
The upper extremity
spinothalamic fibers
affected first
“Cape-like” distribution
of sensory deficits
(dissociated sensory loss)
Subacute Combined
Degeneration
Selective involvement of
the dorsal columns and
CST
Most commonly caused by
vitamin B12 deficiency;
other causes include
copper in the setting of
excess zinc ingestion ;
vacuolar myelopathy
Concurrent myelopathy
and neuropathy
Tabes dorsalis in syphilis
affects the dorsal column
and dorsal roots
Spinal Cord Pathways For Bowel And Bladder Control
The pathways for bowel and bladder control also pass through
the spinal cord
Acute spinal cord pathology causes flaccidity of the bowel and
bladder (as well as in cauda equina syndrome)
Urinary retention with overflow incontinence
Constipation due to decreased bowel motility and incontinence
due to decreased rectal tone
Spasticity develops over time with chronic spinal cord lesions
Bladder becomes spastic/hyperrefexic: it contracts too much,
leading to urgency and incontinence
Increased bowel and rectal tone- leading to constipation
(generally requiring physical stimulation of the rectum for a
bowel movement to occur)
The hemisphere contralateral to the side o
handedness is considered the dominant
hemisphere
The hemisphere ipsilateral to the side o
handedness is considered the nondominant
hemisphere
Most patients are right-handed, so their left
hemisphere is the dominant hemisphere
Language dysunction is most commonly due to
lesions in the dominant (usually left) hemisphere,
whereas neglect is most commonly due to lesions
in the nondominant (usually right) hemisphere
(causing left -sided neglect)
Arterial Supply Of The Cerebral Hemispheres
Paired internal carotid arteries (the anterior
circulation) and
Arise from the CCA
The right CCA arise from the brachiocephalic trunk and
directly from the aortic arch on the left
Each carotid artery ultimately gives rise to MCA and
ACA
Each internal carotid artery also gives rise to an
ophthalmic artery (supplies the retina) and an anterior
choroidal artery (supplies the posterior thalamus and
internal capsule)
Paired vertebral arteries (the posterior circulation)
Arise from the subclavian arteries
Join to form the basilar artery at around the level of the
pontomedullary junction
End by giving off the posterior cerebral arteries (PCAs)
at the level of the upper midbrain
PCAs supply the occipital lobes and inferior and
medial temporal lobes
Before giving rise to the PCAs, the vertebrobasilar
system gives off three paired circumferential arteries
that supply the lateral brainstem and cerebellum: SCA,
AICA, and PICA.
The anterior circulation and posterior
circulation are linked by the posterior
communicating arteries
The ACAs are linked by the anterior
communicating artery
These connections form the circle of Willis on
the inferior surface of the brain
Not all patients have a complete circle of Willis,
and some patients have anatomic variants
The Vascular Territories of the ACA, MCA, and
PCA
The PCAs supply the occipital lobes, inferior medial
temporal lobes, and the thalami
The MCAs supply the lateral surface of the frontal,
temporal, and parietal lobes
The ACAs supply the medial surface of the frontal
and parietal lobes
Watershed
(Borderzone)
Territories
They are the regions at
the border of two
arterial territories
The common teaching
is that borderzone in
arction is due to
hypoperfusion; other
causes include emboli
arriving at the end-
arterial territories
Infarction in the Watershed (Borderzone)
Territories
Infarction in the MCA-ACA borderzone can cause
proximal arm and leg weakness with preserved
strength distally in the hands and feet
If bilaterally, it causes what is called the “person in a
barrel” syndrome
Bilateral infarction in the MCA-PCA watershed
region results in deficits in visual attention (e.g.,
Balint’s syndrome: optic ataxia, ocular apraxia, and
simultanagnosia)
Clinical Syndromes Associated With Cerebral
Vascular Territories
MCA Territory Infarction
The MCA territory includes the majority of the cerebral
hemisphere
The functional regions supplied by the MCA include
the motor and premotor regions, somatosensory cortex,
the frontal eye fields, the language areas, parietal
regions responsible for spatial attention, and the
superior and inferior radiations of the visual pathways
as they pass through the parietal and temporal lobes,
respectively
MCA strokes cause contralateral face and arm weakness
much more so than leg weakness
Left MCA syndrome: right hemiplegia and hemisensory
loss, aphasia, gaze deviation toward the left, and right
homonymous hemianopia
Right MCA syndrome: left hemiplegia and hemisensory
loss, left-sided neglect, gaze deviation to the right, and
left-sided homonomyous hemianopia
The MCA stem gives off the lenticulostriate penetrating
branches that supply the basal ganglia and internal
capsule
Complete contralateral hemiparesis (pure motor lacunar
syndrome
ACA Territory Infarction
ACA strokes cause contralateral leg weakness and
sensory loss more so than face and arm weakness
and sensory loss
Cognitive changes such as abulia
Occlusion o both ACAs simultaneously can cause
acute paraplegia
Azygous ACA: both ACAs arise from a common
trunk
The ACAs can also be compromised by subfalcine
herniation
Recurrent Artery of Huebner Territory
Infarction
A branch of the ACA that supplies the head of the
caudate and the adjacent internal capsule
Contralateral hemiparesis and/or movement
disorder
Anterior Choroidal Artery Territory Infarction
Arises directly from the ICA and supplies the
posterior thalamus and the internal capsule
Contralateral visual field defects, contralateral
hemiparesis, and/or contralateral hemisensory loss,
and can also cause cortical signs
PCA Territory Infarction
Contralateral homonymous hemianopia or superior
quadrantanopia, impaired short-term memory, inability
to read with spared ability to write (alexia without
agraphia- left inferior temporal lesion), decreased ability
to recognize faces (prosopagnosia- right inferior temporal
lesion), and/or changes in cognition and/or level of
arousal if thalamic is affected
PCA territory strokes are generally considered posterior
circulation strokes
Fetal PCA: when one or both PCAs arise from the ICAs
rather than the top of the basilar artery (anterior
circulation)
Artery of Percheron: when both thalami are both supplied
by a single artery that arises from the PCA
Lacunar Strokes
Caused by occlusion of small penetrating arteries affecting the
subcortical white matter (internal capsule), subcortical gray
matter (BG, thalamus), or anterior pons
Pure motor stroke: unilateral hemiparesis/hemiplegia due to
involvement of the posterior limb of the internal capsule or the
anterior pons
Pure sensory stroke: unilateral hemisensory loss due to
involvement of the VPL/VPM nuclei of the thalamus
Ataxia-hemiparesis: unilateral hemiparesis/hemiplegia (due to
involvement of the corticospinal tract) with ataxia in the weak
limb(s) due to lacunar stroke in either the internal capsule or
the anterior pons
Dysarthria–clumsy hand: dysarthria and unilateral upper limb
ataxia; localization is the same as or ataxia-hemiparesis
Spatial Attention and Praxis
Attention
The parietal lobe plays roles in awareness of the body
in space, spatial reasoning, and mathematical
processing
The projection from the occipital lobe superiorly to the
parietal lobe (the dorsal stream)- the “where” pathway:
Visual information is processed here to determine where
things are in space with respect to the body
Lesions here can cause neglect: the patient is unaware of
one half of the world
Neglect is more common with lesions in the nondominant
parietal lobe (the right parietal lobe) causing left sided
neglect
Unilateral neglect:
The loss of conscious awareness for the left side of
the perceptual and mental space
Different, but simple bedside paper-and-pencil tests:
Ask to bisect a line segment
They misbisect it to the right of the objective midpoint;
Ask to cross out line segments printed on a sheet of
paper (Albert’s test)
They omit to cross out a number of left-side segments;
Ask to draw a clock face
They omit, misarrange, or distort left-side details
Examination findings in patients with neglect may
include
Simultagnosia (extinction) of the contralateral side
The mildest manifestation of a right parietal lesion
Primary sensory modalities are intact
The patient fails to appreciate the stimulus on the involved
side or fails to see the stimulus in the involved visual
hemifield
Tactile agnosia (astereognosia)
Lesion: posterior–inferior portion of the parietal lobe
(postcentral gyrus).
Lack of awareness of deficits (e.g., not acknowledging that a
paretic limb is weak), and inability to recognize the neglected
body parts as one’s own in severe cases
Gerstmann’s syndrome:
Due to lesions in the
angular gyrus of the left
parietal lobe can cause
Characterized by left-
right confusion, inability
to count (acalculia),
inability to name the
fingers (finger agnosia),
and inability to write
(agraphia)
Praxis
Apraxia: parietal lesions can cause difficulty
performing a complex learned action
There are several types of apraxia:
Limb-kinetic apraxia: loss of dexterity in performing
actions
Ideational apraxia: inability to conceive of the idea of
how to accurately perform an action (caused by lesions
of the left parietal lobe)
Ideomotor apraxia: inability to convert an idea about
how to do something into a motor plan (caused by
lesions of the left parietal lobe)
Recognition Memory
Memories are internal representations of sensory
experiences
Lesions of the medial temporal lobes can cause amnesia
The flow of visual information inferiorly to the temporal
lobe (the ventral stream)- the “what pathway:”
Visual information is processed here to determine what
things are (recognition memory)
The dominant inferior temporal lobe houses the visual word
form area necessary for reading (alexia- inability to read)
The nondominant inferior temporal lobe houses the face
recognition area (prosopagnosia- inability to recognize
familiar faces)
In the most severe cases patients cannot even recognize their
own face in the mirror
Ventral (occipitotemporal) stream: fusiform and lingual gyri; involved in the
analysis of color and shape of the object.
Unilateral lesions: ontralateral hemiachromatopsia (loss of color perception in
the contralateral visual hemifield)
Bilateral (or rarely right-sided) lesions: visual agnosia (prosopagnosia and
object agnosia)
The inferior frontal gyrus houses Broca’s area for
speech production
Wernicke’s area for speech recognition lies at the
junction of the auditory cortex (superior temporal
gyrus) and the parietal cortex
However, in some patients, language may localize
to the right hemisphere
Dominant hemisphere
Situated on the left side of the brain in > 90% of right
handed people and also in about two-third of left handed
people
Lesions in and around Broca’s and Wernicke’s
areas lead to speech disturbances (aphasia)
The aphasias can be categorized based on the
patient’s ability to produce speech, comprehend
speech, and repeat words and phrases
Broca’s aphasia (nonfluent, expressive, or motor
aphasia)
The primary deficit is in production of speech
I.e., effortful speech with frequent errors
Comprehension is largely preserved
In the most severe Broca’s aphasias, the patient is mute
The patient cannot repeat phrases stated by the examiner
but can comprehend (transcortical motor aphasia-
repetition is preserved)
Wernicke’s aphasia (receptive, fluent or
sensory aphasia)
Comprehension is impaired
Nonsensical speech
Repetitions is impaired (transcortical sensory
aphasia- repetition is preserved)
Global aphasia
Both production and comprehension are impaired
Mixed transcortical aphasia- if repetition is
preserved
Global Aphasia
Conduction aphasia
A patient’s only language
deficit is repetition
Conduction between
Wernicke’s area and
Broca’s area (via the
arcuate fasciculus) is
disrupted
Most commonly due to
stroke in the left MCA
territory stroke
Other functions of the Frontal lobes
Executive functions including working memory, decision
making, abstract reasoning, and emotional processing
Frontal lobe lesions can cause
Abulia (decreased initiative, motivation, speech, and
emotional response),
Behavioral disinhibition, and/or impairments in any of the
above executive functions
Thalamus
The thalami are positioned on either side of the third
ventricle, just superior to the midbrain
The thalamus is a collection of nuclei
Four basic types of circuitry pass through thalamic
nuclei en route to the cortex:
A. Sensory pathways
All sensory pathways synapse in the thalamus, which
transmits sensory information to the respective
sensory cortices
Smell is the only sensory modality that reaches the
cortex before the thalamus
B. Motor control pathways
The ventral anterior (VA) and ventral lateral (VL) nuclei o
the thalamus participate in cortical–basal ganglia–cortical
loops and cerebellar–cortical pathways
C. Consciousness/arousal pathways
These pathways begin in the brainstem reticular
activating system and project to both thalami, which in
turn project diffusely throughout the cortex
D. Cognition/emotion pathways
Corticocortical loops pass through the thalamus, playing
roles in diverse cognitive functions
E.g., the circuit of Papez which participates in memory
and emotion: hippocampus→ fornix→mamillary
bodies→anterior nucleus of the thalamus→anterior
cingulate→entorhinal cortex→hippocampus
Lesions in the thalamus:
Contralateral sensory loss; contralateral
hemiparesis/hemiplegia
Larger lesions can cause decreased level of
consciousness
Generally, lesions of the thalamus can “do anything”
(i.e., cause any type of deficit), including causing
“cortical” signs (e.g., aphasia, neglect, cognitive
deficits) and eye movement abnormalities (in part
due to effects on nearby midbrain pathways or eye
movements)
Basal Ganglia
The BG include the caudate, putamen, globus
pallidus, and subthalamic nucleus
The striatum: caudate and putamen together
The lentiform nuclei: putamen and globus pallidus
together
The BG are part of circuits that initiate and
coordinate movements
BG dysfunction leads to movement disorders (e.g.,
Parkinson’s disease)
Disorders Of Visual Cognition
Visual information rom the primary visual cortex (at the
occipital pole) is transmitted superiorly to the parietal
lobe or spatial processing (the “where” pathway) and
transmitted inferiorly to the temporal lobe or object
identification/ recognition (the “what” pathway)
The left “what” pathway (inferior temporo-occipital
region )
Specialized for processing of visual word forms
Inability to read (alexia), alexia without agraphia
The right “what” pathway (inferior temporo-occipital
region )
Specialized for processing of faces
Inability to recognize faces (prosopagnosia)
Balint Syndrome
Lesions of the bilateral parieto-occipital junctions
This syndrome is characterized by a triad of signs
that are maniestations of deficits in visual attention:
Optic ataxia
Ocular apraxia
Simultanagnosia
Cortical Blindness and Anton Syndrome
Bilateral posterior cerebral artery strokes can lead to
cortical blindness: the eyes and optic nerves still work
I.e., normal pupillary light reflexes
However, the brain cannot decode visual information
Anton syndrome
Some patients with cortical blindness are unaware that
they are blind and may deny being unable to see
Charles Bonnet Syndrome
“Release” hallucinations in a patient with bilateral visual
loss of any cause
These hallucinations are generally of small people, are not
threatening to the patient, and the patient usually knows
they are not real
Overview Of Brainstem Anatomy
A “spinal cord or the head and neck”
In addition to somatic sensory information, the
brainstem also receives vestibular, auditory, taste,
and visceral sensory information
Motor functions of the brainstem include control of
ocular, pupillary, facial, laryngeal, pharyngeal, and
visceral musculature
There are five general categories of structures:
The descending motor pathways for the extremities and
torso (CST)
The ascending somatosensory pathways from the
extremities and torso (dorsal columns and spinothalamic
tracts)
The cranial nerve nuclei and associated structures
The cerebellar peduncles
The RAS and ascending neurotransmitter-specific
projection pathways: substantia nigra (dopamine), locus
coeruleus (norepinephrine), median raphe nuclei
(serotonin), pedunculopontine nuclei (acetylcholine)
The following principles apply at all three levels of
the brainstem
The CST run in the anterior (ventral) aspect of the
brainstem
The somatosensory pathways for the extremities and
torso are most often posterior (dorsal) within the
brainstem (except in the mid-medulla where the medial
lemnisci are medial and extend anteriorly
The cranial nerve nuclei are all posterior (dorsal)
The motor cranial nerve nuclei are closest to the midline, and
their cranial nerves emerge medially/anteriorly (except CN 4)
The motor cranial nerve nuclei innervating skeletal muscle
are at the midline: CNs 3, 4, 6, and 12
The motor cranial nerve nuclei innervating branchial muscles
are more lateral: CN 7, CN 5, and CNs 9 and 10
The sensory and special sensory cranial nerve nuclei
are all more lateral than the motor cranial nerve
nuclei: sensory nuclei of CN 5, vestibular and
cochlear nuclei (CN 8), and nucleus solitarius (for
taste and visceral sensation)
The cerebellar peduncles all arise from the
posterior/dorsal brainstem
The ascending neurotransmitter-specific projection
pathways are found throughout the brainstem, but
the RAS is at the level of the midbrain
The Cerebellar Peduncles
The inferior cerebellar peduncles connect the
medulla to the cerebellum
The middle cerebellar peduncles connect the pons to
the cerebellum
The superior cerebellar peduncles connect the
cerebellum to the upper pons
The Arterial Supply of the Brainstem
Brainstem has three levels
One pair of circumferential arteries per level of the
brainstem:
Superior cerebellar arteries (SCAs) or the midbrain
Anterior inferior cerebellar arteries (AICAs) or the
pons
Posterior inferior cerebellar arteries (PICAs) or the
medulla
The SCAs and AICAs
arise from the basilar
artery and the PICAs from
the vertebral arteries
The anterior spinal artery
ASA) arises from the
vertebral arteries and
supplies the medial
medulla and anterior
spinal cord
At the level of the pons
and midbrain, the midline
basilar artery supplies the
medial brainstem through
penetrating branches
Clinical Applications Of Basic Brainstem
Anatomy
Crossed Signs Due to Brainstem Lesions
Throughout most of the brainstem, lesions lead to
contralateral weakness and/or sensory symptoms in
the extremities
With the exception of CN 4, all cranial nerves project
ipsilaterally (hence, unilateral lesions cause ipsilateral
sensory and/or motor symptoms in the face
Medial Versus Lateral Brainstem Syndromes
The descending CST are anterior and medial throughout
the brainstem
The motor cranial nerve nuclei for skeletal muscle are
posterior and medial and their associated cranial nerves
exit anteriorly and medially except CN 4
The sensory and special sensory cranial nerve nuclei are
dorsolateral in the brainstem
Lesions of the medial brainstem cause predominantly
motor symptoms and signs
Lesions of the dorsolateral brainstem cause
predominantly sensory and special sensory symptoms
and signs; cerebellar symptoms
The cerebellar peduncles are positioned on the
dorsal/dorsolateral aspects of the brainstem
You might also like
- NeurologyDocument149 pagesNeurologyAimee100% (1)
- The Nervous SystemDocument71 pagesThe Nervous SystemDennis Limosnero MayorNo ratings yet
- 21-Spinal Cord TractsDocument23 pages21-Spinal Cord TractsALFAHRUL CAHYADINo ratings yet
- Correlative Neuroanatomy of The Sensory SystemDocument8 pagesCorrelative Neuroanatomy of The Sensory SystemJonathan Gorospe100% (2)
- Sistem Saraf 2: Ida Ayu Eka Widiastuti Bagian Fisiologi FK UnramDocument63 pagesSistem Saraf 2: Ida Ayu Eka Widiastuti Bagian Fisiologi FK UnramUpuUt Putrhie MinchuuetNo ratings yet
- Spinal Cord LesionsDocument110 pagesSpinal Cord Lesionsgtaha80100% (1)
- Ascending Spinal Tracts: Dr. Joachim Perera Joachim - Perera@imu - Edu.myDocument26 pagesAscending Spinal Tracts: Dr. Joachim Perera Joachim - Perera@imu - Edu.myZobayer AhmedNo ratings yet
- Somatosensory PathwaysDocument12 pagesSomatosensory PathwaysDimasBanyakRejekiNo ratings yet
- Sensory PathwayDocument31 pagesSensory PathwayAlma BaterinaNo ratings yet
- 12 Spinal Cord TractsDocument39 pages12 Spinal Cord Tractssjs6r8wwv9No ratings yet
- Ascending TractsDocument44 pagesAscending Tractssalmankhan09215No ratings yet
- Somatosensory PathwaysDocument36 pagesSomatosensory PathwaysAnonymous w3vYureNo ratings yet
- Somatic Sensations IDocument23 pagesSomatic Sensations IjolilarmatarNo ratings yet
- Anatomy - Spinal Cord & Spinal NervesDocument32 pagesAnatomy - Spinal Cord & Spinal Nervesعهد زبنNo ratings yet
- Introduction To Nervous SystemDocument4 pagesIntroduction To Nervous SystemErnie G. Bautista II, RN, MD100% (1)
- Nerve Tract in Spinal CordDocument30 pagesNerve Tract in Spinal CordirfanzukriNo ratings yet
- Spinal Cord: Achmad AminuddinDocument29 pagesSpinal Cord: Achmad AminuddinSurajul AudaNo ratings yet
- Anatomia Si Localizare in Boli SpinaleDocument8 pagesAnatomia Si Localizare in Boli SpinaleHalit DianaNo ratings yet
- Lecture 5 p2Document51 pagesLecture 5 p2Ahmed G IsmailNo ratings yet
- Guyton Somatic SensesDocument2 pagesGuyton Somatic SensesJamie Ong100% (1)
- Neurology Final QuestionsDocument30 pagesNeurology Final QuestionsyiafkaNo ratings yet
- Sensory TractsDocument34 pagesSensory TractsMudassar RoomiNo ratings yet
- Spinalcord 181202085959Document95 pagesSpinalcord 181202085959gonzalesmailyn85No ratings yet
- Spinal CordDocument48 pagesSpinal CordDr.Saber - Ar - Raffi100% (1)
- MED (Neuro) - NeuroanatomyDocument6 pagesMED (Neuro) - NeuroanatomyFlora XuNo ratings yet
- Sensory PathwaysDocument17 pagesSensory PathwaysNabilah Ani SofianNo ratings yet
- Posterior Column-Medial Lemniscus PathwayDocument4 pagesPosterior Column-Medial Lemniscus PathwayRachmadina Basyarial BasyaruddinNo ratings yet
- Npte - Neuroanatomy Lec 2Document31 pagesNpte - Neuroanatomy Lec 2Densen Raphael C. Antonio100% (2)
- Neuroanatomy NotesDocument51 pagesNeuroanatomy NotesAditi MangalNo ratings yet
- Brainstem LesionsDocument10 pagesBrainstem LesionsKathleen CedilloNo ratings yet
- PY 10.3: Describe and Discuss Sensory TractsDocument34 pagesPY 10.3: Describe and Discuss Sensory TractsJiyaa PatelNo ratings yet
- Dorsal Root SyndromeDocument19 pagesDorsal Root SyndromeDerry HerdhimasNo ratings yet
- Sensory and Motor Pathways - DrKatzDocument24 pagesSensory and Motor Pathways - DrKatzWeli PermatasariNo ratings yet
- Ascending Descending TractsDocument46 pagesAscending Descending Tractsyasrul izad100% (4)
- Neuro AnatomyDocument26 pagesNeuro Anatomymeryclave345No ratings yet
- 1-NEU-Histology Lecture CNS (1, 2, 3, 4 & 5) 2021-2022Document16 pages1-NEU-Histology Lecture CNS (1, 2, 3, 4 & 5) 2021-2022Mohamed AbouzaidNo ratings yet
- MS NeurologyDocument30 pagesMS NeurologyAu CassieNo ratings yet
- Anat 6.3 GSA Appendix - EsguerraDocument4 pagesAnat 6.3 GSA Appendix - Esguerralovelots1234No ratings yet
- Tract Continues Down Spinal Cord: Input Location Notes Lesion MedullaDocument10 pagesTract Continues Down Spinal Cord: Input Location Notes Lesion MedullaherethemindNo ratings yet
- SI Week 1Document2 pagesSI Week 1Anonymous 2ABu0iNo ratings yet
- Descending Spinal Tracts: Dr. Joachim Perera Joachim - Perera@imu - Edu.myDocument28 pagesDescending Spinal Tracts: Dr. Joachim Perera Joachim - Perera@imu - Edu.myZobayer AhmedNo ratings yet
- NM Learning Outcomes 1-25Document113 pagesNM Learning Outcomes 1-25Kristin DouglasNo ratings yet
- Somatic Sensation & Pain: Prof. Yasmeiny Yazir Dr. Nuraiza MeutiaDocument23 pagesSomatic Sensation & Pain: Prof. Yasmeiny Yazir Dr. Nuraiza MeutiaAdi Trisno100% (1)
- Diseases of The Spinal CordDocument41 pagesDiseases of The Spinal CordMalueth AnguiNo ratings yet
- Motoric Central Nervous System: Dr. Ridwan Harrianto MHSC (Om) SP - Ok, PakDocument47 pagesMotoric Central Nervous System: Dr. Ridwan Harrianto MHSC (Om) SP - Ok, PakMahasiswa StrugleNo ratings yet
- Lo 1 Week 5 NeuroDocument36 pagesLo 1 Week 5 NeuroInna DamaNo ratings yet
- Sensory SystemDocument11 pagesSensory SystemAhmad Jazuli KaddumiNo ratings yet
- Spinal Cord: Navigation SearchDocument16 pagesSpinal Cord: Navigation SearchritzchoiNo ratings yet
- LECTURE Nervous SystemDocument4 pagesLECTURE Nervous SystemanonymousNo ratings yet
- BMS301, L11, Histology, Structure of White Matter of Spinal CordDocument38 pagesBMS301, L11, Histology, Structure of White Matter of Spinal Cordkareemosama9916No ratings yet
- DrMBA Medulla SpinalisDocument25 pagesDrMBA Medulla SpinalisAyu FadhilahNo ratings yet
- Biology ReportDocument3 pagesBiology ReportzyrianNo ratings yet
- Chapter #5: The Spinal CordDocument4 pagesChapter #5: The Spinal CordRazvanNo ratings yet
- Neuroscience: Ascending and Descending TracDocument91 pagesNeuroscience: Ascending and Descending Trachazunga rayfordNo ratings yet
- UNIT III Disorders of Neurological SystemDocument7 pagesUNIT III Disorders of Neurological SystemAmmar BhattiNo ratings yet
- Dorsal Column-Medial Lemniscus Pathway - WikipediaDocument27 pagesDorsal Column-Medial Lemniscus Pathway - WikipediaCosplay AccountNo ratings yet
- Bioactivity study of modified curcumin loaded polymeric nanoparticlesFrom EverandBioactivity study of modified curcumin loaded polymeric nanoparticlesNo ratings yet
- Design Development and Analysis of a Nerve Conduction Study System An Auto Controlled Biofeedback ApproachFrom EverandDesign Development and Analysis of a Nerve Conduction Study System An Auto Controlled Biofeedback ApproachNo ratings yet
- Harpreet Kaur Gill SOP UKDocument2 pagesHarpreet Kaur Gill SOP UKSAHILPREET SINGHNo ratings yet
- The Gateway Experience®: Wave IV-AdventureDocument4 pagesThe Gateway Experience®: Wave IV-AdventureEvan SchowNo ratings yet
- Hydrofluoric Acid Scrubber SystemsDocument12 pagesHydrofluoric Acid Scrubber Systemsravichem823No ratings yet
- Lista de Precios 03 de DiciembreDocument33 pagesLista de Precios 03 de DiciembreRafael Kotty Cab TuzNo ratings yet
- Natural Blends Inc 1Document2 pagesNatural Blends Inc 1Álvaro Jurado0% (1)
- Tabel 1. Range Nilai Log SP, Resistivity Dan Gamma Ray No - Litologi Range Nilai Range Nilai Log Range Nilai LogDocument1 pageTabel 1. Range Nilai Log SP, Resistivity Dan Gamma Ray No - Litologi Range Nilai Range Nilai Log Range Nilai Logdody24No ratings yet
- Buthaina AlmamariDocument3 pagesButhaina Almamaributhin7heartNo ratings yet
- Note Semelles JumeléesDocument6 pagesNote Semelles JumeléeslionelNo ratings yet
- Search Help Exit How ToDocument18 pagesSearch Help Exit How Tobra_mxoNo ratings yet
- Definition of Research, Characteristics of Research, Research Process and Functions of Research Definition of ResearchDocument2 pagesDefinition of Research, Characteristics of Research, Research Process and Functions of Research Definition of ResearchNinda SNo ratings yet
- The Economic Consequences of Accounting Fraud in Product MarketsDocument37 pagesThe Economic Consequences of Accounting Fraud in Product MarketsJeiny ZambranoNo ratings yet
- Tl-Sg108pe Tl-Sg105pe Tl-Sg1210mpe IgDocument2 pagesTl-Sg108pe Tl-Sg105pe Tl-Sg1210mpe IgMaxNo ratings yet
- Materi & Tugas Bing Kelas 2 - Bab 5Document3 pagesMateri & Tugas Bing Kelas 2 - Bab 5Ronald WeleNo ratings yet
- Is 3786 1983 PDFDocument33 pagesIs 3786 1983 PDFsinegapriya100% (1)
- 2009 Tuffboom FlyerDocument2 pages2009 Tuffboom FlyerCarlos ReNo ratings yet
- EskimoDocument2 pagesEskimoabdul sorathiyaNo ratings yet
- Minnesota Timberwolves (17-28) vs. Indiana Pacers (22-22) : Probable StartersDocument23 pagesMinnesota Timberwolves (17-28) vs. Indiana Pacers (22-22) : Probable Starterstiwari_anunay1689No ratings yet
- 1117 33Document8 pages1117 33tm5u2rNo ratings yet
- Work in Team Environment Learning ModuleDocument3 pagesWork in Team Environment Learning ModuleNesri YayaNo ratings yet
- HDM Stuttgart Vorlage ThesisDocument5 pagesHDM Stuttgart Vorlage ThesisLuz Martinez100% (2)
- Patient Safety AjarDocument48 pagesPatient Safety AjarAngell YunitaNo ratings yet
- Ananya ROY: Software EngineerDocument1 pageAnanya ROY: Software EngineerAshishNo ratings yet
- Business Studies Project Class XIIDocument13 pagesBusiness Studies Project Class XIIKanishk Mehrotra67% (15)
- Assessing The Nature of Soil AcidityDocument8 pagesAssessing The Nature of Soil AcidityPartha DebRoyNo ratings yet
- 3:3Document15 pages3:3Nicholas CemenenkoffNo ratings yet
- Midterm Exam For Form 3 CompleteDocument8 pagesMidterm Exam For Form 3 CompleteCHRISTOPHER SCALENo ratings yet
- Gallbladder Mucocele A ReviewDocument6 pagesGallbladder Mucocele A ReviewThaís ChouinNo ratings yet
- 03 Spring Crochet Along BUNNY GBDocument2 pages03 Spring Crochet Along BUNNY GBkhuyên nguyễnNo ratings yet
- Electrostatic Respirator Filter Media Filter Efficiency and Most Penetrating Particle Size EffectsDocument10 pagesElectrostatic Respirator Filter Media Filter Efficiency and Most Penetrating Particle Size EffectsAdolfo OrozcoNo ratings yet
- A Detailed Study On Loss Processes in Solar CellsDocument11 pagesA Detailed Study On Loss Processes in Solar CellsFernando DiasNo ratings yet