Professional Documents
Culture Documents
Midterms
Midterms
Uploaded by
Steph CaronanOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Midterms
Midterms
Uploaded by
Steph CaronanCopyright:
Available Formats
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
which describes the loss of sodium
I. FLUID VOLUME DISTURBANCES from the extracellular space (i.e.,
(Hypovolemia, Hypervolemia)
intravascular and interstitial fluid) that
II. ELECTROLYTE IMBALANCES (Sodium,
occurs during gastrointestinal
Potassium, Calcium, Magnesium Imbalance,
Phosphorus, Chloride) hemorrhage, vomiting, diarrhea, and
III. ACID–BASE DISTURBANCES (Metabolic diuresis;
Acidosis, Metabolic Alkalosis, Respiratory Dehydration
Acidosis, Respiratory Alkalosis , Mixed Acid– which refers to the loss of
Base Disorders) intracellular water (and
IV. PARENTERAL FLUID THERAPY (Purpose, total body water) that
Types of Intravenous Solutions, Nursing ultimately causes cellular
Management of the Patient Receiving desiccation and elevates
Intravenous Therapy the plasma sodium
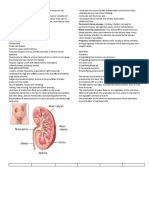
V. KIDNEY DISORDERS (Chronic Kidney concentration and
Disease, Nephrotic Syndrome , Acute osmolality.
Kidney Injury, End-Stage Kidney Disease or
Chronic Kidney Disease) ALTERATIONS IN HEALTH (DIAGNOSIS)
VI. RENAL REPLACEMENT THERAPIES
(Dialysis, Hemodialysis Dialyzers,
Fluid volume deficit
Continuous Renal Replacement Therapies,
Peritoneal Dialysis)
CAUSES
VII. INFECTIONS OF THE URINARY TRACT
(Lower Urinary Tract Infections)
ADULT VOIDING DYSFUNCTION (Urinary Commonly caused by dysfunction of various organs,
VIII.
Incontinence, Urinary Retention, Neurogenic such as Congestive Heart Failure or Kidney
Bladder) Failure.
Rarely, neurological disorders, particularly those
affecting the hormones that regulate kidney
functioning can also cause hypovolemia.
FLUID VOLUME DISTURBANCES Dehydration, which may result from excessive water
evaporating from the skin in extreme heat or when
experiencing a fever. Dehydration can also result
HYPOVOLEMIA from continuous vomiting or diarrhea without
sufficient fluid intake, usually associated with
FVD, or hypovolemia, occurs when loss of ECF infections that cause gastroenteritis.
(extracellular fluid) volume exceeds the intake of It may also result from excessive accumulation of
fluid. It occurs when water and electrolytes are lost in fluids within the interstitial space, between cells.
the same proportion as they exist in normal body For instance, when an infection becomes severe,
fluids, thus the ratio of serum electrolytes to water sepsis can occur, which is a life-threatening condition
remains the same. FVD should not be confused with in which the individual's response to the infection
dehydration, which refers to loss of water alone, with leads to organ dysfunction and systemic
increased serum sodium levels. FVD may occur inflammation.
alone or in combination with other imbalances. Other conditions that can cause fluids to exit blood
Unless other imbalances are present concurrently, vessels include pancreatitis, pericarditis, burns,
serum electrolyte concentrations remain essentially and nutritional hypoalbuminemia.
unchanged. Sudden blood loss due to a trauma, like a motor
o Two distinct disorders: vehicle accident or a fall from a height. External or
Volume Depletion internal bleeding may occur and, if not identified
quickly, can be life-threatening.
SIGNS & SYMPTOMS
Severity:
Dizziness when standing.
Dry skin and dry mouth.
Feeling tired (fatigue) or weak.
Muscle cramps.
Unable to pee (urinate) or the color of your urine is
darker than normal.
BSN 3A | PBL GROUP 1 1
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
Severe: your symptoms, especially if you get
dizzy when you’re upright, which is a
Confusion. sign of hypovolemia.
Difficulty breathing or fast breathing.
Excessive sweating. CLINICAL MANIFESTATION
Losing consciousness.
Low blood pressure.
Low body temperature.
Pale skin tone or a blue tone to the skin and lips
(cyanosis).
COMPLICATIONS
Hypoxia
Hypovolemic Shock
Dysrhythmias
Acute Kidney Failure
PATHOPHYSIOLOGY
FVD results from loss of body fluids and occurs more
rapidly when coupled with decreased fluid intake.
FVD can also develop with a prolonged period of
inadequate intake. Causes of FVD include abnormal
fluid losses, such as those resulting from vomiting,
diarrhea, GI suctioning, and sweating; decreased
intake, as in nausea or lack of access to fluids; and
third-space fluid shifts, or the movement of fluid from
the vascular system to other body spaces (e.g., with
edema formation in burns, ascites with liver
dysfunction). Additional causes include diabetes
insipidus (a decreased ability to concentrate urine
owing to a defect in the kidney tubules that interferes
with water reabsorption), adrenal insufficiency,
osmotic diuresis, hemorrhage, and coma.
ASSESSMENT AND DIAGNOSTIC FINDINGS
LABORATORY TESTS
o Elevated Potassium and BUN
o Urine Specific Gravity
o Urine Sodium Concentration
o Creatinine
o Blood Test:
CBC
Chemistry Panels
o UTZ or Echocardiogram
DIAGNOSTIC PROCEDURES
o Skin and Mucous Membrane
During a physical exam, your provider
will examine your skin and the mucous
membranes in your mouth, tongue, and
nose for dryness, which is a sign of the
condition.
o Pulse, body temperature and blood pressure:
Your provider will test your vitals while
you’re sitting and while you’re MEDICAL MANAGEMENT
standing to monitor changes. During
this process when you change your Fluid Resuscitation
posture, your provider will examine o to increase the amount of fluid volume in your
body via fluid replacement (fluid resuscitation).
BSN 3A | PBL GROUP 1 2
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
During this procedure, an IV (intravenous) tube Accurate and Frequent assessment of I&O, weight,
injects fluids into your vein vital signs, central venous pressure, level of
Isotonic Electrolyte Solution (e.g. consciousness, breath sounds, and skin color
lactated Ringer’s solution, 0.9% o should be performed to determine when
sodium chloride) is frequently the first- therapy should be slowed to avoid volume
line choice to treat the hypotensive overload. The rate of fluid administration is
patient with FVD because they expand based on the severity of loss and the
plasma volume patient’s hemodynamic response to volume
Hypotonic electrolyte solution (e.g., replacement
0.45% sodium chloride) is often used to Fluid Challenge Test
provide both electrolytes and water for o When is not excreting enough urine and to
renal excretion of metabolic wastes. determine whether the depressed renal
o Function is caused by reduced renal blood
flow secondary to FVD (prerenal azotemia)
or, more seriously, by acute tubular
necrosis from prolonged FVD
o During a fluid challenge test, volumes of
fluid are administered at specific rates and
intervals while the patient’s hemodynamic
response to this treatment is monitored (i.e.,
vital signs, breath sounds, orientation
status, central venous pressure, urine
output).
o An example of a typical fluid challenge test
involves administering 100 to 200 mL of
normal saline solution over 15 minutes. The
goal is to provide fluids rapidly enough to
attain adequate tissue perfusion without
compromising the cardiovascular system.
The response by a patient with FVD but
normal renal function is increased urine
output and an increase in blood pressure
and central venous pressure.
Note:
Shock can occur when the volume of fluid lost exceeds 25%
of the intravascular volume or when fluid loss is rapid.
NURSING MANAGEMENT
Monitors and measures fluid I&O at least every 8
hours, and sometimes hourly
o As FVD develops, body fluid losses exceed
fluid intake through excessive urination
(polyuria), diarrhea, vomiting, or other
mechanisms.
o Once FVD has developed, the kidneys
attempt to conserve body fluids, leading to
a urine output of less than 1 mL/kg/h in an
adult.
Daily body weights monitored
o an acute loss of 0.5 kg (1 lb) represents a
fluid loss of approximately 500 mL (1L of
Oxygen Therapy fluid weighs approximately 1 kg, or 2.2 lb)
o to alleviate the adverse effects of hypoxemia (Crawford & Harris, 2011c).
and tissue hypoxia Vital Signs are closely monitored
BSN 3A | PBL GROUP 1 3
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
o The nurse observes for a weak, rapid pulse should be implemented to control diarrhea and
and orthostatic hypotension (i.e., a replacement fluids administered. This includes
decrease in systolic pressure exceeding 20 administering antidiarrheal medications and small
mm Hg when the patient moves from a lying volumes of oral fluids at frequent intervals.
to a sitting position) (Weber & Kelley, 2010).
o A decrease in body temperature often CORRECTING HYPOVOLEMIA
accompanies FVD, unless there is a
concurrent infection. When possible, oral fluids are administered to help
Skin and tongue turgor are monitored on a regular correct FVD, with consideration given to the patient’s
basis. likes and dislikes. The type of fluid the patient has
o In a healthy person, pinched skin lost is also considered, and fluids most likely to
immediately returns to its normal position replace the lost electrolytes are appropriate. If the
when released (Weber & Kelley, 2010). patient is reluctant to drink because of oral
o This elastic property, referred to as turgor, discomfort, the nurse assists with frequent mouth
is partially dependent on interstitial fluid care and provides nonirritating fluids. The patient
volume. In a person with FVD, the skin may be offered small volumes of oral rehydration
flattens more slowly after the pinch is solutions (e.g., Rehydralyte, Elete, Cytomax). These
released. solutions provide fluid, glucose, and electrolytes in
o In a person with severe FVD, the skin may concentrations that are easily absorbed. If nausea is
remain elevated for many seconds. present, an antiemetic may be needed before oral
o Tissue turgor is best measured by fluid replacement can be tolerated. If the deficit
pinching the skin over the sternum, inner cannot be corrected by oral fluids, therapy may need
aspects of the thighs, or forehead. Tongue to be initiated by an alternative route (enteral or
turgor is not affected by age (see previous parenteral) until adequate circulating blood volume
Gerontologic Considerations), and and renal perfusion are achieved. Isotonic fluids are
evaluating this may be more valid than prescribed to increase ECF volume (Crawford &
evaluating skin turgor. In a normal person, Harris, 2011c).
the tongue has one longitudinal furrow.
o In the person with FVD, there are additional HYPERVOLEMIA
longitudinal furrows and the tongue is
smaller because of fluid loss. The degree of Hypervolemia is a medical condition when you have
oral mucous membrane moisture is also too much fluid in your body, also described as having
assessed; a dry mouth may indicate either excess water retention or fluid overload. Healthy
FVD or mouth breathing. people have a certain amount of fluid in their bodies.
Urine concentration is monitored by measuring the When you have too much excess fluid, it can cause
urine specific gravity health complications such as swelling, high blood
o In a volume-depleted patient, the urine pressure, heart problems, and more.
specific gravity should be greater than Hypervolemia is common among people with chronic
1.020, indicating healthy renal conservation kidney disease (CKD) and renal failure because their
of fluid. kidneys aren't working to remove excess fluid as
Hemodynamic monitoring healthy kidneys would. The good news is, once the
o Mental function is eventually affected, causes of your hypervolemia are understood, there
resulting in delirium in severe FVD as a are treatments that can help control it.
result of decreasing cerebral perfusion.
ALTERATIONS IN HEALTH (DIAGNOSIS)
Decreased peripheral perfusion can result
in cold extremities. In patients with relatively
Fluid Volume Excess
normal cardiopulmonary function, a low
central venous pressure is indicative of CAUSES
hypovolemia.
o Patients with acute cardiopulmonary Kidney failure. Your kidneys are responsible for
decompensation require more extensive removing excess fluid from your body. When your
hemodynamic monitoring of pressures in kidneys aren’t working well, fluid can build up.
both sides of the heart to determine if
Congestive heart failure. When your heart is not
hypovolemia exists.
pumping enough blood, your kidneys aren’t able to
work as well, leaving excess fluid in your body.
PREVENTION
Liver failure or cirrhosis. Your liver processes
To prevent FVD, the nurse identifies patients at risk nutrients and filters toxins. When your liver isn’t
and takes measures to minimize fluid losses. For working as it should, fluid can build up in your
example, if the patient has diarrhea, measures abdomen.
BSN 3A | PBL GROUP 1 4
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
Hormonal changes. Women may experience mild factors can include heart failure, renal failure, and
fluid retention as a normal part of premenstrual cirrhosis of the liver. Another contributing factor is the
syndrome (PMS) or pregnancy. Excessive fluid consumption of excessive amounts of table or other
retention related to hormonal changes may be a sign sodium salts. Excessive administration of sodium-
of high blood pressure and should be checked out by containing fluids in a patient with impaired regulatory
a doctor. mechanisms may predispose him or her to a serious
IV fluids. Receiving too much IV fluid, especially if FVE as well
there are other health conditions present, can lead to
fluid overload and swelling. ASSESSMENT AND DIAGNOSTIC FINDINGS
Salt (Sodium). Too much salt (sodium) in your body
Laboratory data useful in diagnosing FVE include
causes hypervolemia. Salt is an essential mineral in
BUN and hematocrit levels.
your body. Your body manages the amount of salt
In FVE, both of these values may be decreased
you eat with water. If you eat food that contains too
because of plasma dilution, low protein intake, and
much sodium, your body will use water to balance it
anemia.
back to a normal level. This is why you might feel
In chronic renal failure, both serum osmolality and
thirsty after eating a lot of salty foods.
the sodium level are decreased owing to excessive
Note: retention of water.
The urine sodium level is increased if the kidneys are
If you’re living with CKD: you may be at risk for attempting to excrete excess volume.
hypervolemia—especially in later stages as kidney function A chest x-ray may reveal pulmonary congestion.
declines. After a diagnosis of kidney failure, dialysis Hypervolemia occurs when aldosterone is
treatments replace some kidney function to help to remove chronically stimulated (i.e., cirrhosis, heart failure,
excess fluid from your body and get you as close to your “dry and nephrotic syndrome). Therefore, the urine
weight” as possible. Dry weight is your “ideal weight”—the sodium level does not increase in these conditions.
weight your care team determines you would be without the
excess fluid in your body. MEDICAL MANAGEMENT
If you’ve never been diagnosed with CKD: your doctor may Pharmacological Therapy
perform several tests to help determine the cause of your fluid o Diuretics
overload. You’ll probably be given a test to determine the are prescribed when dietary restriction
amount of sodium in your blood. You’ll likely also get a urine of sodium alone is insufficient to reduce
test to help the doctor determine whether your hypervolemia edema by inhibiting the reabsorption of
is being caused by a kidney issue. Further testing for kidney sodium and water by the kidneys.
function can help your doctor decide which steps to take next. The choice of diuretic is based on the
severity of the hypervolemic state, the
SIGNS & SYMPTOMS degree of impairment of renal function,
and the potency of the diuretic.
Rapid weight gain Thiazide diuretics
Noticeable swelling (edema) in your arms, legs, and o block sodium
face reabsorption in the distal
Swelling in your abdomen tubule, where only 5% to
Cramping, headache, and stomach bloating 10% of filtered sodium is
Shortness of breath reabsorbed.
High blood pressure o Generally, thiazide
Heart problems, including congestive heart failure diuretics, such as
hydrochlorothiazide
COMPLICATIONS (HydroDIURIL) or
chlorthalidone
Pericarditis (Thalitone), are
HF prescribed for mild to
Delayed wound healing moderate hypervolemia
Tissue Breakdown and loop diuretics for
Decreased bowl function severe hypervolemia
(Karch, 2012).
PATHOPHYSIOLOGY Loop diuretics
o such as furosemide
FVE may be related to simple fluid overload or (Lasix), bumetanide
diminished function of the homeostatic mechanisms (Bumex), or torsemide
responsible for regulating fluid balance. Contributing (Demadex), can cause a
BSN 3A | PBL GROUP 1 5
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
greater loss of both decreasing sodium intake. Lemon
sodium and water juice, onions, and garlic are
because they block excellent substitute flavorings,
sodium reabsorption in although some patients prefer salt
the ascending limb of substitutes. Most salt substitutes
Henle’s loop, where 20% contain potassium and must
to 30% of filtered sodium therefore be used cautiously by
is normally reabsorbed. patients taking potassium-sparing
Electrolyte imbalances may result from the effect of diuretics (e.g., spironolactone,
the diuretic. Hypokalemia can occur with all diuretics triamterene [Dyrenium], amiloride
except those that work in the last distal tubule of the [Midamor]). They should not be
nephrons. Potassium supplements can be used at all in conditions
prescribed to avoid this complication. associated with potassium
Hyponatremia occurs with diuresis owing to retention, such as advanced renal
increased release of ADH secondary to a reduction disease. Salt substitutes
in circulating volume. Decreased magnesium levels containing ammonium chloride
occur with the administration of loop and thiazide can be harmful to patients with
diuretics due to decreased reabsorption and liver damage
increased excretion of magnesium by the kidney. In some communities, drinking
High uric acid levels (hyperuricemia) can also occur water may contain too much
from increased reabsorption and decreased sodium for a sodium-restricted
excretion of uric acid by the kidneys diet. Depending on its source,
Dialysis water may contain as little as 1 mg
o If renal function is so severely impaired that or more than 1,500 mg of sodium
pharmacologic agents cannot act efficiently, per quart. Patients may need to
other modalities are considered to remove use distilled water if the local water
sodium and fluid from the body. supply is very high in sodium.
o Hemodialysis or peritoneal dialysis may be Bottled water can have a sodium
used to remove nitrogenous wastes and content that ranges from 0 to
control potassium and acid–base balance, 1,200 mg/L; therefore, if sodium is
and to remove sodium and fluid. restricted, the label must be
Continuous renal replacement therapy may carefully examined for sodium
also be required. content before purchasing and
Nutritional Therapy drinking bottled water. Also,
o Restriction of sodium. patients on sodium-restricted diets
An average daily diet not restricted should be cautioned to avoid
in sodium contains 6 to 15 g of water softeners that add sodium to
salt, whereas low-sodium diets water in exchange for other ions,
can range from a mild restriction to such as calcium. Protein intake
as little as 250 mg of sodium per may be increased in patients who
day, depending on the patient’s are malnourished or who have low
needs. serum protein levels in an effort to
A mild sodium-restricted diet increase capillary oncotic
allows only light salting of food pressure and pull fluid out of the
(about half the usual amount) in tissues into vessels for excretion
cooking and at the table, and no by the kidneys.
addition of salt to commercially
prepared foods that are already NURSING MANAGEMENT
seasoned
Foods high in sodium must be Measures I&O at regular intervals to identify
avoided. It is the sodium salt excessive fluid retention
(sodium chloride) rather than Monitored weight daily and rapid weight gain is noted
sodium itself that contributes to o The patient is weighed daily, and rapid
edema. Therefore, patients are weight gain is noted. An acute weight gain
instructed to read food labels of 1 kg (2.2 lb) is equivalent to a gain of
carefully to determine salt content. approximately 1 L of fluid
About half of ingested sodium is in Breath sounds are assessed at regular intervals in
the form of seasoning, seasoning at-risk patients, particularly if parenteral fluids are
substitutes can play a major role in being administered
monitors the degree of edema in
BSN 3A | PBL GROUP 1 6
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
the most dependent parts of the body, such as the oncotic pressure, causing expansion of the interstitial
feet and ankles in ambulatory fluid compartment
patients and the sacral region in patients confined to Edema can be localized (e.g., in the ankle, as in
bed rheumatoid arthritis) or generalized (as in cardiac
o Pitting edema is assessed by pressing a and renal failure). Severe generalized edema is
finger into the affected part, creating a pit or called anasarca.
indentation that is evaluated on a scale of Burns and infection are examples of conditions
1+ (minimal) to 4+ (severe). associated with increased interstitial fluid volume.
o Peripheral edema is monitored by Obstruction to lymphatic outflow, a plasma albumin
measuring the circumference of the level less than 1.5 to 2 g/dL, or a decrease in plasma
extremity with a tape marked in millimeters oncotic pressure contributes to increased interstitial
(Weber & Kelley, 2010). fluid volume.
The kidneys retain sodium and water when there is
PREVENTING HYPERVOLEMIA
decreased ECF volume as a result of decreased
require sodium-restricted diets in some form, and cardiac output from heart failure. A thorough
adherence to the prescribed diet is encouraged medication history is necessary to identify any
medications that could cause edema, such as
instructed to avoid over-the-counter (OTC)
nonsteroidal anti-inflammatory drugs (NSAIDs),
medications without first checking with a health care
estrogens, corticosteroids, and antihypertensive
provider, because these substances may contain
agents.
sodium.
o Ascites is a type of edema in which fluid
If fluid retention persists despite adherence to a
accumulates in the peritoneal cavity; it
prescribed diet, hidden sources of sodium, such as
results from nephrotic syndrome, cirrhosis,
the water supply or use of water softeners, should be
and some malignant tumors. The patient
considered.
commonly reports shortness of breath and
DETECTING AND CONTROLLING HYPERVOLEMIA a sense of pressure because of pressure on
the diaphragm.
Promote rest, restrict sodium intake, monitor The goal of treatment is to preserve or restore the
parenteral fluid therapy, and administer appropriate circulating intravascular fluid volume. Thus, in
medications. addition to treating the cause of the edema, other
Regular rest periods may be beneficial because bed treatments may include diuretic therapy, restriction of
rest favors the diuresis of fluid. fluids and sodium, elevation of the extremities,
Sodium and fluid restriction should be instituted as application of anti-embolism stockings, paracentesis,
indicated. dialysis, and continuous renal replacement therapy
Patients with FVE require diuretics, the patient’s in cases of renal failure or life-threatening fluid
response to these agents is monitored. volume overload
The rate of parenteral fluids and the patient’s ELECTROLYTE IMBALANCES
response to these fluids are also closely monitored
If dyspnea or orthopnea is present, the patient is An electrolyte imbalance occurs when certain
placed in a semi-Fowler’s position to promote lung mineral levels in your blood get too high or too low.
expansion. The patient is turned and repositioned at This imbalance may be a sign of a problem
regular intervals because edematous tissue is more like kidney disease.
prone to skin breakdown than normal tissue. Electrolytes are minerals that give off an electrical
charge when they dissolve in fluids like blood and
Note: urine. Our body makes electrolytes.
Electrolytes in blood, tissue, urine and other body
conditions predisposing to FVE are likely to be fluids play a critical role in balancing body fluids,
chronic, patients are taught to monitor their response regulating your heart rhythm and supporting nerve
to therapy by documenting fluid I&O and body weight and muscle function.
changes. The importance of adhering to the Our kidneys and liver, as well as other organs and
treatment regimen is emphasized. tissue, continually move electrolytes in and out of
cells to adjust fluid levels within the compartments.
EDUCATING PX ABOUT EDEMA Certain health conditions can affect our body’s ability to
move and balance electrolytes. When fluid compartments
gives special attention to edema when instructing the have too many or too few electrolytes, it can develop to an
patient with FVE. Edema can occur as a result of electrolyte imbalance.
increased capillary fluid pressure, decreased
capillary oncotic pressure, or increased interstitial
BSN 3A | PBL GROUP 1 7
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
COMPONENTS OF ELECTROLYTES COMPLICATIONS
Sodium controls fluid levels and aids nerve and A significant electrolyte imbalance (either too high or too low)
muscle function. can cause serious, life-threatening problems. These
Potassium supports heart, nerve and muscle
complications include:
functions. It also moves nutrients into cells and
waste products out of them while supporting your Coma.
metabolism. Seizures.
Calcium helps blood vessels contract and expand Sudden cardiac death (sudden cardiac arrest).
to stabilize blood pressure. It also secretes
hormones and enzymes (proteins) that help the
nervous system send messages. CLINICAL MANIFESTATIONS
Chloride helps maintain healthy blood levels, blood
pressure and body fluids. Symptoms of an electrolyte imbalance vary depending on the
Magnesium aids nerve and muscle function. It also severity and electrolyte type. A slight electrolyte imbalance
promotes the growth of healthy bones and teeth. may not cause noticeable changes. When problems occur,
Phosphate supports the skeletal system, as well as
you may experience:
nerve and muscle function.
Bicarbonate helps balance acids and basic alkaline Confusion and irritability.
compounds (bases) in blood (pH balance). Diarrhea or constipation.
Bicarbonate also helps move carbon dioxide (a Fatigue.
waste product) through your bloodstream. Headaches.
TYPES OF ELECTROLYTES Irregular or fast heart rate (arrhythmia).
High electrolyte imbalances include: Muscle cramps, muscle spasms or weakness.
Nausea and vomiting.
Sodium: Hypernatremia. Numbness or tingling in limbs, fingers and toes.
Potassium: Hyperkalemia.
Calcium: Hypercalcemia.
Chloride: Hyperchloremia. DIAGNOSTIC TEST
Magnesium: Hypermagnesemia.
Phosphate: Hyperphosphatemia. An electrolyte panel is a blood test that measures electrolyte
Bicarbonate: Alkalosis (low alkaline base). levels. Healthcare providers often order an electrolyte panel
if you:
Low electrolytes or electrolyte deficiencies include: Need blood tests for a routine physical exam.
Are in the hospital.
Sodium: Hyponatremia. Have certain health conditions.
Potassium: Hypokalemia. Experience disease symptoms.
Calcium: Hypocalcemia.
Chloride: Hypochloremia.
Magnesium: Hypomagnesemia. MEDICAL MANAGEMENT
Phosphate: Hypophosphatemia.
Bicarbonate: Acidosis (high acid levels). Treatment depends on the specific electrolyte
RISK FACTORS imbalance and cause. Some imbalances will correct
without treatment.
Certain conditions can also throw off your body’s electrolyte To treat dehydration, your provider may recommend
levels. You may be more likely to develop an electrolyte rehydrating with electrolyte drinks or an oral
imbalance if you have: rehydration salt (ORS) solution. Medical provider
can tell the correct amount of sugar, salt and water
Burns. to make this solution at home. Or can buy ORS
Cancer. packets at a drugstore.
Cardiovascular disease, heart failure or high blood Medical treatments for electrolyte imbalances
pressure. include:
Dehydration due to not drinking enough liquids or IV fluids like sodium chloride to rehydrate our
from excessive vomiting, diarrhea, sweating body.
(hyperhidrosis) or fever. IV medicines to restore a healthy electrolyte
Overhydration or water intoxication (drinking too balance.
much water). Medications or supplements to replace lost
Eating disorders. electrolytes.
Kidney disease. Hemodialysis to correct electrolyte imbalances
Liver disease like cirrhosis. caused by kidney failure or severe kidney
Substance use disorder. damage.
Proper hydration can help our body maintain a
healthy level of electrolytes. It’s especially
BSN 3A | PBL GROUP 1 8
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
important to drink enough fluids if experience CLINICAL MANIFESTATIONS
prolonged diarrhea, vomiting or sweating.
The clinical presentation depends on the underlying etiology.
Symptoms may include:
ACID–BASE DISTURBANCES
Kussmaul respirations (slow, deep breathing)
Diarrhea
Ketoacidosis:
ACUTE AND CHRONIC METABOLIC ACIDOSIS Polyuria
(BASE BICARBONATE DEFICIT) Polydipsia
Epigastric pain
The renal system is responsible for eliminating the Vomiting
daily load of non-volatile acids, which is
Renal failure:
approximately 70 millimoles per day. This daily load Nocturia
comes primarily from anaerobic metabolism, Polyuria
absorption of acids, and excretion of bases from the Pruritis
GI system. Metabolic acidosis occurs when there is
Methanol poisoning: visual symptoms (photophobia,
an increase in the levels of new non-volatile acids
scotomata, blindness)
(e.g., lactic acid), renal loss of HCO3-, or ingestion of
Salicylate overdose:
toxic alcohols. Respiratory compensation occurs
Tinnitus
very quickly (within minutes) and mitigates changes
Blurred vision
in pH. In the acute period, metabolic disorders can
Vertigo
cause severe symptoms. Management is aimed at
correcting the underlying etiology. ASSESSMENT AND DIAGNOSTIC FINDINGS
Metabolic acidosis is the process that results in the
gain of hydrogen ions (H+) or the loss of HCO3-. In ABG measurements are used in the diagnosis of
primary metabolic acidosis, arterial blood gas will acid–base imbalances such as metabolic acidosis.
show: Expected ABG changes include a low bicarbonate
pH < 7.4 level (less than 22 mEq/L) and a low blood pH (less
HCO3- < 24 mEq/L than 7.35). The cardinal feature of metabolic acidosis
Partial pressure of arterial CO2 (PCO2) < 40 is a decrease in the serum bicarbonate level. In
mm Hg conditions of acidosis there is elevated H+ and the
sodium–potassium cellular pump brings H+ into the
PATHOPHYSIOLOGY cells in place of K+. Therefore, high K+ accumulates
in the bloodstream in metabolic acidosis as a result
Normal anion gap metabolic acidosis results from the
direct loss of bicarbonate, as in diarrhea, lower of the shift of potassium out of the cells (Theodore,
intestinal fistulas, ureterostomies, use of diuretics, 2019). Later, when the acidosis is corrected and pH
early renal insufficiency, excessive administration of normalized, the cellular pump causes potassium to
chloride, and the administration of parenteral move back into the cells and hypokalemia may
nutrition without bicarbonate or occur. Blood levels of potassium need to be closely
bicarbonateproducing solutes (e.g., lactate) (Emmett monitored. ECG monitoring is recommended as
& Szerlip, 2018). changes of potassium in the bloodstream can cause
High anion gap metabolic acidosis occurs when arrhythmias (Palmer & Clegg, 2016a).
In metabolic acidosis, the lungs compensate for the
there is an excessive accumulation of acids. High
high H+ through hyperventilation to decrease the
anion gap occurs in lactic acidosis, salicylate
CO2 level, which in turn reduces H+ (see carbonic
poisoning (acetylsalicylic acid), renal failure,
acid equation). Calculation of the anion gap is helpful
methanol, ethylene or propylene glycol toxicity, DKA,
in determining the cause of metabolic acidosis.
and ketoacidosis that occurs with starvation. The
There are certain conditions that cause high anion
high amount of hydrogen ions due to the acids
gap metabolic acidosis and others that cause normal
present are neutralized and buffered by HCO3−
anion gap metabolic acidosis
causing the bicarbonate concentration to fall and
become exhausted. Other anions in the bloodstream
are called upon to neutralize the high acid in the
blood. In all of these instances, abnormally high
levels of anions are used to neutralize the H+, which
increases the anion above normal limits (high anion
gap) (Emmett & Szerlip, 2019).
BSN 3A | PBL GROUP 1 9
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
(within minutes) and mitigates changes in pH from
the primary metabolic disorder. Management is
aimed at correcting the underlying etiology.
Metabolic alkalosis is the process that results in the
loss of hydrogen ions (H+) or the gain of HCO3-. In
primary metabolic alkalosis, arterial blood gas will
show:
pH > 7.4
Partial pressure of CO2 (PCO2) > 40 mm Hg
HCO3- > 28 mEq/L
PATHOPHYSIOLOGY
A common cause of metabolic alkalosis is severe
vomiting or gastric suction that causes loss of
stomach HCl (hydrogen and chloride ions). The
MEDICAL MANAGEMENT disorder also occurs in pyloric stenosis, in which only
gastric fluid is lost. Gastric fluid has an acid pH
Treatment is directed at correcting the metabolic (usually 1 to 3), and loss of this highly acidic fluid
imbalance. If the problem results from excessive pulls H+ ions from the bloodstream to replenish the
intake of chloride, treatment is aimed at eliminating gastric acid. As a result, the bloodstream loses H+
the source of the chloride. When necessary, ions and becomes alkalotic. Other situations
bicarbonate is given; however, the administration of predisposing to metabolic alkalosis include those
sodium bicarbonate during cardiac arrest can result associated with loss of potassium, such as diuretic
in paradoxical intracellular acidosis. Hyperkalemia therapy that promotes excretion of potassium (e.g.,
may occur with acidosis and hypokalemia with thiazides, furosemide), and ACTH secretion (as in
reversal of the acidosis and subsequent movement hyperaldosteronism and Cushing’s syndrome)
of potassium back into the cells. Therefore, the (Emmett & Szerlip, 2017a; Norris, 2019).
serum potassium level is monitored closely, and Hypokalemia produces alkalosis in two ways: (1)
hypokalemia is corrected as acidosis is reversed when the bloodstream is low in K+, the nephrons
(Mount, 2017c) reabsorb K+ into the bloodstream and secrete H+
In chronic metabolic acidosis, low serum calcium into the tubule fluid which is excreted in the urine and
levels are treated before the chronic metabolic (2) when the bloodstream is low in K+, intracellular
acidosis is treated to avoid tetany resulting from an potassium moves out of the cells into the ECF, and
increase in pH and a decrease in ionized calcium. as potassium ions leave the cells, hydrogen ions
Alkalizing agents may be given. Treatment must enter to maintain electroneutrality (Mount,
modalities may also include hemodialysis or 2017c). Excessive alkali ingestion from antacids
peritoneal dialysis (Goltzman, 2019b) containing bicarbonate or from the use of sodium
bicarbonate during cardiopulmonary resuscitation
ACUTE AND CHRONIC METABOLIC ALKALOSIS can also cause metabolic alkalosis (Emmett &
(BASE BICARBONATE EXCESS) Szerlip, 2017b).
Chronic metabolic alkalosis can occur with long-term
The renal system is responsible for eliminating the diuretic therapy (thiazides or furosemide), villous
daily load of non-volatile acids, which is adenoma in the GI tract, external drainage of gastric
approximately 70 millimoles per day. This daily load
fluids, significant potassium depletion, cystic fibrosis,
comes primarily from anaerobic metabolism,
and the chronic ingestion of milk and calcium
absorption of acids, and excretion of base from the
carbonate (Emmett & Szerlip, 2017b).
GI system. Metabolic alkalosis develops when there
is an increase in serum HCO3- levels. Metabolic
alkalosis also occurs when there is an increased loss
of acid, either renally or through the upper GI tract
(e.g., vomiting), increased intake of HCO3-, or a
reduced ability to secrete HCO3- when needed.
Respiratory compensation occurs very quickly
BSN 3A | PBL GROUP 1 10
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
CLINICAL MANIFESTATIONS - Licorice ingestion (glycyrrhizic acid)
- Liddle syndrome
- Bartter and Gitelman syndromes
o Severe hypokalemia (K+ < 2)
Other tests:
Basic metabolic panel (BMP):
o Allows assessment of HCO3-
o Important for managing electrolytes,
especially K+
Arterial blood gas
The clinical presentation is dependent on the underlying Testing relevant to the suspected underlying
etiology. Symptoms may include: etiology
Vomiting
BP abnormalities: MEDICAL MANAGEMENT
Hypertension (primary mineralocorticoid
excess) Treatment is aimed at the underlying etiology.
Hypotension (↓ effective circulating volume) Attempt to improve renal HCO3- excretion to resolve
Hypokalemia alkalosis:
Hypocalcemia: In patients without edema (true volume
depletion): volume repletion with isotonic
saline
Tetany In patients with ↓ effective circulating volume
Chvostek sign: contraction of facial muscles (e.g., heart failure):
when the facial nerve is tapped o Potassium chloride
Trousseau sign: carpopedal spasm with o K+-sparing diuretics (e.g., amiloride)
inflation of the BP cuff
Changes in mental status/seizures o Avoid isotonic saline as it will worsen
symptoms without improving alkalosis.
Findings consistent with a prerenal state:
Congestive heart failure: Correct electrolyte abnormalities, especially:
K+
-Chest pain
Cl-
-Dyspnea on exertion
-↑ Jugular venous distension Na+ (through fluid management)
-Pulmonary edema(crackleson lung exam) Consider dialysis in patients with CKD.
-Peripheral edema ACUTE AND CHRONIC RESPIRATORY ACIDOSIS
Cirrhosis: (CARBONIC ACID EXCESS)
Jaundice
Ascites The respiratory system is responsible for eliminating
Hepatomegaly with/without splenomegaly the volatile acid carbon dioxide (CO2), which is
Telangiectasias produced via aerobic metabolism. The body
produces approximately 15,000 mmol of CO2 daily,
DIAGNOSTIC FINDINGS
which is the majority of daily acid production; the
The etiology of metabolic alkalosis is usually remainder of the daily acid load (only about 70 mmol
ascertainable from the history alone. Urine Cl- can of nonvolatile acids) is excreted through the kidneys.
be helpful in cases in which the patient is reluctant to In the setting of hypoventilation, this acid load is not
provide a full history (e.g., self-induced vomiting in adequately blown off, and respiratory acidosis
eating disorders) or for less common etiologies (e.g., occurs. Renal compensation occurs after 3–5 days,
Conn, Bartter, and Gitelman syndromes). as the kidneys attempt to increase the serum
bicarbonate levels. Patients are often asymptomatic,
Urine chloride: or they may present with neuropsychiatric
Urine Cl- < 20 mEq/L: body Cl- is also manifestations or mild dyspnea. Diagnosis is made
depleted, typically in volume depletion: with arterial blood gas measurement. Management
involves treating the underlying etiology, stabilizing
o Vomiting
the patient, and avoiding respiratory sedatives.
o Nasogastric suction
Urine Cl- > 20 mEq/L: Body Cl- level is Respiratory acidosis is the process that results in an
normal, typically in patients with volume accumulation of carbon dioxide (CO2) due to
expansion: abnormal gas exchange in the lungs. In primary
respiratory acidosis, the arterial blood gas will show:
o Mineralocorticoid excess:
- Cushing's syndrome (hypercortisolism) pH < 7.35
-Conn syndrome (primary hyperaldosteronism)
BSN 3A | PBL GROUP 1 11
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
PCO2 (partial pressure of carbon dioxide) > other diagnostic measures include monitoring of
45 mm Hg (i.e., hypercapnia) serum electrolyte levels, chest x-ray for determining
respiratory infection or other disease, and a drug
PATHOPHYSIOLOGY screen if an overdose is suspected. ECG monitoring
is recommended to identify any cardiac involvement
Respiratory acidosis is due to inadequate excretion as a result of COPD (Feller-Kopman &
of CO2 with inadequate ventilation, resulting in Schwartzstein, 2017).
elevated plasma CO2 concentrations and,
consequently, increased levels of carbonic acid. In MEDICAL MANAGEMENT
addition to an elevated PaCO2, inadequate
ventilation usually causes a decrease in PaO2. Acute Assess the ABCs:
respiratory acidosis occurs in emergency situations, Ensure that the airway is secure.
such as acute pulmonary edema, aspiration of a Administer supplemental O2.
foreign object, atelectasis, pneumothorax, and Ventilatory support as needed
overdose of sedatives, as well as in nonemergent Treat the underlying etiology; examples include:
situations, such as sleep apnea associated with COPD exacerbation: bronchodilators and
severe obesity, severe pneumonia, and acute corticosteroids
respiratory distress syndrome. Respiratory acidosis Pneumonia in neuromuscular disorders:
commonly occurs in patients with severe chronic antibiotics
obstructive pulmonary disease (COPD) when Avoid respiratory sedatives.
patients acutely decompensate due to respiratory
infection or heart failure. Respiratory acidosis can ACUTE AND CHRONIC RESPIRATORY ALKALOSIS
also occur in diseases that impair respiratory muscle (CARBONIC ACID DEFICIT)
function and cause hypoventilation. These disorders
include severe scoliosis, muscular dystrophy, The respiratory system is responsible for eliminating
multiple sclerosis, myasthenia gravis, and Guillain- the volatile acid carbon dioxide (CO2), which is
Barré syndrome (Feller-Kopman & Schwartzstein, produced via aerobic metabolism. The body
2017). produces approximately 15,000 mmol of CO2 daily,
which is the majority of daily acid production; the
CLINICAL MANIFESTATIONS remainder of the daily acid load (only about 70 mmol
of nonvolatile acids) is excreted through the kidneys.
Clinical presentation of hypercapnia: When hyperventilation occurs, excess carbon
Neurologic: dioxide is blown off and respiratory alkalosis
o Anxiety/paranoia
o Headaches develops. The kidneys respond by decreasing serum
o Somnolence bicarbonate (HCO3–) through increased HCO3–
o Delirium
excretion or decreased excretion of H+. Patients
o Coma
present with an increased respiratory rate, dyspnea,
Pulmonary: dyspnea (usually mild)
light-headedness and potentially psychologic
Diagnosis: primarily with an arterial blood gas (ABG):
symptoms. Diagnosis involves a thorough history, an
Acute respiratory acidosis:
exam, and an arterial blood gas measurement.
o pH < 7.35
Management focuses on addressing the underlying
o PaCO2 > 45 mm Hg
abnormalities, stabilizing patients in acute distress,
o Normal HCO3–
and potentially a small dose of short-acting
Chronic respiratory acidosis (compensated):
benzodiazepines.
o pH < 7.4 (low or near-normal)
o PaCO2 > 45 mm Hg Respiratory alkalosis refers to the process that
o HCO3– elevated results in a decreased level of carbon dioxide (CO2)
within the blood.
ASSESSMENT AND DIAGNOSTIC FINDINGS PATHOPHYSIOLOGY
In respiratory acidosis, ABG analysis reveals a pH Respiratory alkalosis is caused by hyperventilation,
less than 7.35, a PaCO2 greater than 45 mm Hg, and which causes excessive loss or “blowing off” of CO2
variation in the bicarbonate level, depending on the and, hence, there is a decrease in the plasma
duration of the acute respiratory acidosis. When carbonic acid concentration (see carbonic acid
compensation occurs over a prolonged period and equation). Causes include extreme anxiety such as
renal retention of bicarbonate has fully occurred, the panic disorder, hypoxemia, salicylate intoxication,
bicarbonate neutralizes the acidosis. Arterial pH is gram-negative sepsis, and inappropriate ventilator
within the lower limits of normal (e.g., pH 7.35). settings.
Depending on the cause of respiratory acidosis,
BSN 3A | PBL GROUP 1 12
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
Chronic respiratory alkalosis results from chronic MIXED ACID–BASE DISORDERS
hypocapnia which leads to decreased serum H+ ion,
resulting in alkalosis. Chronic hepatic insufficiency Patients can simultaneously experience two or more
and cerebral tumors can cause chronic independent acid–base disorders. A normal pH in the
hyperventilation that leads to chronic respiratory presence of changes in the PaCO2 and plasma
alkalosis (Schwartzstein, Richards, Edlow, et al., HCO3− concentration immediately suggests a mixed
2018) disorder. An example of a mixed disorder is the
simultaneous occurrence of metabolic acidosis due
CLINICAL MANIFESTATIONS to lactic acid accumulation and respiratory acidosis
due to hypoventilation. Both of these disorders result
Tachypnea in excessive acid accumulation in the bloodstream
Dyspnea due to respiratory failure and cardiac arrest (Emmett
Dizziness/light-headedness & Palmer, 2018b).
Paresthesias (perioral, hands/feet) due to decreased
ionized calcium COMPENSATION
Psychologic symptoms:
Anxiety Generally, the pulmonary and renal systems
Fear compensate for each other to return the pH to
Impending doom normal. In a single acid–base disorder, the system
Highly variable presentation, based on underlying not causing the problem tries to compensate by
etiology; for example: returning the ratio of bicarbonate to carbonic acid to
High-altitude illness: findings consistent with the normal 20:1. The lungs compensate for
pulmonary and/or cerebral edema metabolic disturbances by changing CO2 excretion;
Sepsis: fever, hypotension, findings hypoventilation accumulates CO2, hyperventilation
consistent with originating infection (e.g., causes loss of CO2. The kidneys compensate for
cough or dysuria) respiratory disturbances by altering bicarbonate
Pulmonary embolism: calf pain, unilateral reabsorption and H+ secretion (Norris, 2019;
lower-extremity edema Theodore, 2019).
In respiratory acidosis, excess hydrogen in the blood
DIAGNOSTIC FINDINGS is excreted in the urine in exchange for bicarbonate
ions which are conserved. In respiratory alkalosis,
Diagnosing a respiratory alkalosis typically requires a the renal excretion of bicarbonate increases, and
thorough history and exam and an arterial blood gas hydrogen ions are retained. In metabolic acidosis,
measurement. the lungs compensate by increasing the ventilation
Arterial blood gas: rate and the kidneys retain bicarbonate. In metabolic
Acute respiratory alkalosis (uncompensated): alkalosis, the respiratory system compensates by
o pH > 7.45 decreasing ventilation to conserve CO2 and increase
o PaCO2 < 35 mm Hg the PaCO2, which in turn increases carbonic acid.
o Normal HCO3– Because the lungs respond to acid–base disorders
Chronic respiratory alkalosis (compensated): within minutes, compensation for metabolic
imbalances occurs faster than renal compensation
o pH > 7.4 (slightly high or near-normal) for respiratory imbalances (Norris, 2019; Theodore,
o PaCO2 < 35 mm Hg 2019).
o HCO3– decreased
Electrolytes: Abnormalities are common and may BLOOD GAS ANALYSIS
lead to complications.
Basic metabolic panel Blood gas analysis is often used to identify the
Magnesium specific acid–base disturbance and the degree of
Phosphate compensation that has occurred. The analysis is
Chest X-ray: to rule out other causes of tachypnea usually based on an arterial blood sample; however,
if an arterial sample cannot be obtained, a mixed
MEDICAL MANAGEMENT venous sample may be used (Theodore, 2019).
Results of ABG analysis provide information about
Assess and address the ABCs (airway, breathing, alveolar ventilation, oxygenation, and acid–base
and circulation) if patient is in acute distress.
balance. It is necessary to evaluate the
Attempt to correct the underlying abnormality. concentrations of serum electrolytes (e.g., sodium,
Small dose of short-acting benzodiazepine potassium, chloride) along with ABG data because
electrolytes are commonly affected by acid–base
imbalances. The health history, physical
examination, previous blood gas results, and serum
BSN 3A | PBL GROUP 1 13
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
electrolytes should always be part of the assessment
used to determine the cause of the acid–base
disorder (Larkin & Zimmanck, 2015). Responding to
isolated sets of blood gas results without these data
can lead to serious errors in interpretation. Treatment
of the underlying condition usually corrects acid–
base disorders.
PARENTERAL FLUID THERAPY
When patients cannot take oral fluid or oral feedings,
their status is termed NPO (nil per os), meaning
nothing by mouth.
In patients who are NPO, parenteral fluid therapy,
also termed IV fluid therapy, is used to administer
fluids. IV fluid therapy can be initiated to replace
fluids in various clinical settings such as hospitals,
outpatient diagnostic and surgical settings, clinics,
and home health care. IV fluids can also be used to
administer medications and provide nutrients.
PURPOSE
The choice of an IV solution depends on the purpose
of its administration. Generally, IV fluids are given to
achieve one or more of the following goals:
To provide water, electrolytes, and nutrients to
meet daily requirements.
To replace water and correct electrolyte
deficits.
To administer medications and blood
products.
BSN 3A | PBL GROUP 1 14
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
IV solutions contain dextrose and/or electrolytes NORMAL SALINE SOLUTION
mixed in various proportions with water. Pure,
electrolyte-free water can never be given by IV Normal saline (0.9% sodium chloride) solution
because it rapidly enters RBCs and causes them to contains water, sodium, and chloride.
rupture Because the osmolality is entirely contributed by
electrolytes, the solution remains within the ECF and
TYPES OF INTRAVENOUS SOLUTIONS expands the intravascular volume.
For this reason, normal saline solution is often used
IV solutions are categorized as isotonic, hypotonic,
to correct an extracellular volume deficit but is not
or hypertonic, according to whether their total
identical to ECF.
osmolality is the same as, less than, or greater than
It is used with administration of blood transfusions
that of blood, respectively.
and to replace large sodium losses, such as in burn
Electrolyte solutions are considered isotonic if the
injuries.
total electrolyte content (anions + cations) is between
It should not be used in heart failure, pulmonary
250 and 375 mEq/L, hypotonic if the total electrolyte
edema, renal impairment, or sodium retention.
content is less than 250 mEq/L, and hypertonic if the
Normal saline does not supply calories.
total electrolyte content is greater than 375 mEq/L.
OTHER ISOTONIC SOLUTION
ISOTONIC FLUIDS
Several other solutions contain ions in addition to
Fluids that are classified as isotonic have a total
sodium and chloride and are somewhat similar to the
osmolality close to that of the ECF and do not cause
ECF in composition.
cells to shrink or swell.
Lactated Ringer’s solution contains potassium and
When isotonic fluids are administered they expand
calcium in addition to sodium chloride.
the ECF volume.
It is used to correct dehydration, blood loss, and
An isotonic solution is a crystalloid solution (water
sodium depletion and to replace GI losses.
containing soluble mineral salts).
Plasma is a colloidal solution. A colloidal solution is
a mixture of fluid containing insoluble large particles, HYPOTONIC SOLUTIONS
such as proteins.
Colloidal solutions exert oncotic pressure; One purpose of hypotonic solution is to replace fluid,
crystalloids do not exert oncotic pressure because it is hypotonic compared with plasma.
Another purpose of hypotonic solution is to provide
Note: It is important for the nurse to recognize that in free water. At times, hypotonic sodium solutions are
blood loss, 3 L of isotonic fluid (crystalloid solution) used to treat hypernatremia and other hyperosmolar
is needed to replace 1 L of conditions.
blood (colloidal solution). Half-strength saline (0.45% sodium chloride) solution
is frequently used.
Isotonic fluids expand the water volume in the Patients with any type of cardiac implantable
intravascular space, patients with heart failure or electronic device need to be screened to determine
hypertension who receive isotonic solutions should if they can safely undergo MRI.
be carefully monitored for signs of fluid overload. The nurse should educate the patient regarding what
to expect during and after the procedure.
D5W The patient should be prepared to lie on a cold, hard
table that slides into an enclosed small tube.
A solution of D5W is unique in that it may be both The nurse should inform the patient that they will
isotonic and hypotonic. hear noises, including periodic banging and popping
It is essential to consider this action of D5W, sounds.
especially if the patient is at risk for increased Patients with claustrophobia may be prescribed a
intracranial pressure. sedative prior to the procedure.
During fluid resuscitation, this solution should not be Patients should be instructed to close their eyes
used because hyperglycemia can result. before entering the tube, and to keep them closed,
Therefore, D5W is used mainly to supply water and as this may decrease claustrophobic symptoms.
to correct an increased serum osmolality.
About 1 L of D5W provides less than 170 kcal and is
HYPERTONIC FLUIDS
a minor source of the body’s daily caloric
requirements.
Hypertonic fluids include 3% NaCl and IV mannitol.
BSN 3A | PBL GROUP 1 15
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
If a patient is sodium depleted, a hypertonic sodium FLUID OVERLOAD
IV solution might be used.
If a patient is experiencing acute cerebral edema, IV Overloading the circulatory system with excessive IV
mannitol is often used fluids causes increased blood pressure and central
Hypertonic solutions pull water from the interstitial venous pressure.
and intracellular compartments into the bloodstream. Signs and symptoms of fluid overload include moist
These solutions draw water out of intracellular crackles on auscultation of the lungs, cough,
compartments causing cellular dehydration. restlessness, distended neck veins, edema, weight
Normal saline and lactated Ringer’s solution are gain, dyspnea, and rapid, shallow respirations.
considered isotonic solutions. When 5% dextrose Its treatment includes decreasing the IV rate,
(D5W) is added to normal saline solution or lactated monitoring vital signs frequently, assessing breath
Ringer’s solution, the total osmolality exceeds that of sounds, and placing the patient in a high Fowler
the ECF. position.
Saline solutions are also available in osmolar The primary provider is contacted immediately. This
concentrations greater than that of the ECF. complication can be avoided by using an infusion
These solutions draw water from the ICF to the ECF pump and by carefully monitoring all infusions.
and cause cells to shrink.
As a result, these solutions must be given cautiously
and usually only when the serum osmolality has AIR EMBOLISM
decreased to dangerously low levels.
It is most often associated with cannulation of central
Hypertonic solutions exert an osmotic pressure
veins and directly related to the size of the embolus
greater than that of the ECF.
and the rate of entry.
Air entering into central veins gets to the right
OTHER INTRAVENOUS THERAPIES ventricle, where it lodges against the pulmonary
valve and blocks the flow of blood from the ventricle
When the patient is unable to tolerate food, into the pulmonary arteries.
nutritional requirements are often met using the IV Treatment calls for immediately clamping the
route. cannula and replacing a leaking or open infusion
Solutions may include high concentrations of glucose system, placing the patient on the left side in the
(such as 50% dextrose in water), protein, or fat to Trendelenburg position, assessing vital signs and
meet nutritional requirements. breath sounds, and administering oxygen.
Many medications are also delivered by the IV route, Air embolism can be prevented by using locking
either by continuous infusion or by intermittent bolus adapters on all lines, filling all tubing completely with
directly into the vein. solution, and using an air detection alarm on an IV
Because IV medications enter the circulation rapidly, infusion pump.
administration by this route is potentially hazardous
Note: The nurse must assess the patient for a history PHLEBITIS
of allergic reactions to medications. Although
obtaining drug allergy information is important when Phlebitis, or inflammation of a vein, can be
administering any medication, categorized as chemical, mechanical, or bacterial;
however, two or more of these types of irritation often
occur simultaneously.
It is especially critical with IV administration, because Phlebitis can be prevented by using aseptic
the medication is delivered directly into the technique during insertion, using the appropriate
bloodstream. This can trigger an immediate size cannula or needle for th vein, considering the
hypersensitivity reaction. composition of fluids and medications when
selecting a site, observing the site hourly for any
NURSING MANAGEMENT OF THE PATIENT RECEIVING complications, anchoring the cannula or needle well,
INTRAVENOUS THERAPY and changing the IV site according to agency policy
and procedures.
In many settings, the ability to perform venipuncture
to gain access to the venous system for
administering fluids and medication is an expected THROMBOPHLEBITIS
nursing skill.
This responsibility includes selecting the appropriate Thrombophlebitis refers to the presence of a clot plus
venipuncture site and type of cannula and being inflammation in the vein.
proficient in the technique of vein entry. Treatment includes discontinuing the IV infusion;
applying a cold compress first to decrease the flow
BSN 3A | PBL GROUP 1 16
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
of blood, followed by a warm compress; elevating the based on measures of kidney function and urine
extremity; and restarting the line in the opposite tests, and it is classified into stages based on the
extremity. level of kidney damage and the degree of reduction
If the patient has signs and symptoms of in the glomerular filtration rate (GFR). The condition
thrombophlebitis, the IV line should not be flushed can be caused by a variety of factors, including
(although flushing may be indicated in the absence diabetes, high blood pressure, and certain genetic or
of phlebitis to ensure cannula patency and to prevent autoimmune disorders. Treatment may include
mixing of incompatible medications and solutions). medications, lifestyle changes, and in severe cases,
dialysis or kidney transplantation.
HEMATOMA PATHOPHYSIOLOGY
Hematoma results when blood leaks into tissues Chronic kidney disease (CKD) is a progressive and
surrounding the IV insertion site. irreversible deterioration in renal function, with the
Leakage can result if the vein wall is perforated loss of nephrons, the functional unit of the kidney,
during venipuncture, the needle slips out of the vein, over time. The pathophysiology of CKD involves
a cannula is too large for the vessel, or insufficient complex interactions between different factors,
pressure is applied to the site after removal of the including genetic, environmental, and metabolic
needle or cannula. factors. The most common causes of CKD are
Treatment includes removing the needle or cannula diabetes and hypertension, which can lead to
and applying light pressure with a sterile, dry damage to the small blood vessels and the nephrons
dressing; applying ice for 24 hours to the site to avoid in the kidneys. Other causes include
extension of the hematoma; elevating the extremity glomerulonephritis, polycystic kidney disease, and
to maximize venous return, if tolerated; assessing obstructive uropathy. As the nephrons are damaged,
the extremity for any circulatory, neurologic, or motor the kidneys' ability to filter waste products and
dysfunction; and restarting the line in the other excess fluid from the blood is reduced, leading to a
extremity if indicated. build-up of toxic substances in the body. This can
cause a variety of symptoms, including fatigue,
weakness, nausea, and fluid retention. In addition to
CLOTTING AND OBSTRUCTION the loss of renal function, CKD can also lead to a
number of other complications, including anemia,
Blood clots may form in the IV line as a result of bone disease, and cardiovascular disease. These
kinked IV tubing, a very slow infusion rate, an empty complications are thought to be related to a
IV bag, or failure to flush the IV line after intermittent combination of factors, including inflammation,
medication or solution administrations. oxidative stress, and altered hormone levels. Overall,
If blood clots in the IV line, the infusion must be CKD is a complex and multifactorial condition that
discontinued and restarted in another site with a new requires ongoing management and monitoring to
cannula and administration set. prevent further kidney damage and to manage its
The tubing should not be irrigated or milked. Neither associated complications.
the infusion rate nor the solution container should be
raised, and the clot should not be aspirated from the RISK FACTORS
tubing.
Clotting of the needle or cannula may be prevented Diabetes: Diabetes is the leading cause of CKD.
by not allowing the IV solution bag to run dry, taping High blood sugar levels can damage blood vessels
the tubing to prevent kinking and maintain patency, in the kidneys, making them less effective at filtering
maintaining an adequate flow rate, and flushing the waste.
line after intermittent medication or other solution High blood pressure: High blood pressure damages
administration. the blood vessels in the kidneys and can lead to
CKD.
KIDNEY DISORDERS Family history of kidney disease: If you have a family
history of kidney disease, you may be at increased
risk of developing CKD.
CHRONIC KIDNEY DISEASE
Age: The risk of CKD increases as you get older.
Chronic kidney disease (CKD) is a long-term Smoking: Smoking damages blood vessels
condition in which the kidneys are damaged and throughout the body, including those in the kidneys,
cannot filter blood as effectively as they should. This and can increase the risk of CKD.
leads to a build-up of waste and fluid in the body, Obesity: Being overweight or obese can increase the
which can cause a range of symptoms and risk of CKD.
complications over time. CKD is typically diagnosed
BSN 3A | PBL GROUP 1 17
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
Cardiovascular disease: People with cardiovascular conducted to check for protein or blood in the urine,
disease are at increased risk of developing CKD. which can be a sign of kidney damage.
Certain ethnic groups: African Americans, Native Imaging tests: Imaging tests, such as an ultrasound,
Americans, and Hispanics are at higher risk of CT scan, or MRI, may be conducted to check the size
developing CKD than other ethnic groups. and shape of the kidneys and to detect any
Prolonged use of certain medications: Some abnormalities or blockages.
medications, such as nonsteroidal anti-inflammatory Kidney biopsy: A kidney biopsy may be performed to
drugs (NSAIDs), can damage the kidneys if used for obtain a sample of kidney tissue for analysis if the
long periods. cause of CKD is uncertain.
CLINICAL MANIFESTATIONS MANAGEMENT AND TREATMENT
Fatigue and weakness: As the kidneys become less Medications: Medications may be prescribed to treat
effective at removing waste products, toxins can conditions that can cause kidney damage, such as
build up in the body, causing fatigue and weakness. high blood pressure, diabetes, and high cholesterol.
Fluid retention: The kidneys play a key role in Medications may also be used to control symptoms
regulating the body's fluid balance. As they become associated with CKD, such as anemia and bone
damaged, fluid can build up in the body, leading to disease.
swelling in the legs, ankles, feet, and face. Dietary changes: A diet low in sodium, protein, and
High blood pressure: The kidneys are also involved phosphorus can help reduce the workload on the
in regulating blood pressure. When they are kidneys and prevent further damage. It is also
damaged, blood pressure can rise. important to consume enough calories to maintain a
Decreased urine output: As CKD progresses, the healthy weight and to limit the intake of fluids.
kidneys may produce less urine or stop producing Blood pressure control: High blood pressure is a
urine altogether. common complication of CKD and can worsen
Changes in urine: Urine may be foamy or contain kidney damage. Controlling blood pressure through
blood or protein as a result of kidney damage. medication, lifestyle changes, and regular monitoring
Anemia: The kidneys produce a hormone called is essential to prevent further damage.
erythropoietin that stimulates the production of red Blood sugar control: For people with diabetes,
blood cells. As the kidneys become damaged, they maintaining tight control of blood sugar levels is
produce less erythropoietin, leading to anemia. essential to prevent or slow the progression of CKD.
Bone disease: CKD can lead to bone disease Regular monitoring: Regular check-ups with a
because the kidneys are involved in regulating healthcare provider are important to monitor kidney
calcium and phosphorus levels in the body. function and to adjust treatment plans as needed.
Itching: Build-up of waste products in the blood can Dialysis: In advanced stages of CKD, when the
cause skin itching. kidneys are no longer able to function properly,
Nausea and vomiting: As toxins build up in the body, dialysis may be necessary to filter waste products
it can cause nausea and vomiting. from the blood.
Shortness of breath: As fluid builds up in the lungs, it Kidney transplant: For some people with advanced
can cause shortness of breath. CKD, a kidney transplant may be an option. This
involves surgically implanting a healthy kidney from
ASSESSMENT AND DIAGNOSTIC FINDINGS a donor.
Medical history: A complete medical history is NURSING INTERVENTIONS
important in the diagnosis of CKD. Risk factors for
CKD, such as diabetes, high blood pressure, family Monitor and manage fluid and electrolyte balance:
history of kidney disease, and previous kidney CKD can affect the body's ability to regulate fluid and
infections or diseases, will be assessed. electrolyte levels, leading to imbalances. Nurses
Physical examination: A physical examination will be should monitor the patient's fluid intake and output,
conducted to check for signs of kidney disease, such assess for signs of fluid overload or dehydration, and
as high blood pressure, swelling in the legs or ankles, administer IV fluids and medications as needed to
and anemia. maintain electrolyte balance.
Blood tests: Blood tests, such as a complete blood Control blood pressure: High blood pressure is a
count (CBC), serum creatinine, and blood urea common complication of CKD and can further
nitrogen (BUN), will be conducted to measure the damage the kidneys. Nurses should monitor blood
levels of waste products in the blood. An abnormal pressure regularly and administer antihypertensive
result could indicate kidney damage or disease. medications as prescribed.
Urine tests: Urine tests, such as a urinalysis and
urine albumin-to-creatinine ratio (ACR), will be
BSN 3A | PBL GROUP 1 18
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
Administer medications as prescribed: Patients with and underlying medical conditions such as diabetes
CKD may require medications to manage symptoms, and lupus. When the glomeruli are damaged, they
control blood pressure, and reduce the risk of become more permeable to protein, allowing protein
complications. Nurses should ensure that patients to leak out of the blood and into the urine. This results
are taking their medications as prescribed and
monitor for any adverse reactions. in decreased levels of protein in the blood, leading to
Monitor and manage nutrition: Patients with CKD a drop in the oncotic pressure (the pressure that
may have specific dietary needs, such as limiting keeps fluid inside the blood vessels) and the
protein, phosphorus, and potassium intake. Nurses development of edema. The liver responds to the low
should work with a registered dietician to develop a protein levels by producing more proteins, including
nutrition plan that meets the patient's needs and cholesterol and triglycerides, leading to their
provide education on how to manage their diet. increased levels in the blood. In addition to
Manage anemia: CKD can lead to anemia, which can proteinuria, other common features of nephrotic
cause fatigue and weakness. Nurses should monitor syndrome include hypoalbuminemia (low levels of
the patient's hemoglobin levels and administer the protein albumin in the blood), hyperlipidaemia
erythropoietin-stimulating agents or iron (high levels of lipids such as cholesterol and
supplements as prescribed. triglycerides in the blood), and edema. Treatment of
nephrotic syndrome depends on the underlying
Educate patients on self-care: Patients with CKD
need to be involved in their care and understand how cause and may include medications to control blood
to manage their condition. Nurses should provide pressure, reduce proteinuria, and prevent
education on self-care, such as monitoring blood complications such as infections and blood clots.
pressure, managing medications, and following a
RISK FACTORS
renal diet.
Monitor and manage dialysis: Patients with Primary glomerular disease: This is the most
advanced CKD may require dialysis to filter waste common cause of nephrotic syndrome, and it occurs
and excess fluid from the blood. Nurses should when the small blood vessels in the kidneys become
monitor the patient during dialysis and assess for any inflamed and damaged. The primary glomerular
complications, such as infection or hypotension. diseases that can lead to nephrotic syndrome include
Assess and manage complications: CKD can lead to minimal change disease, focal segmental
a variety of complications, such as cardiovascular glomerulosclerosis (FSGS), and membranous
disease, anemia, and bone disease. Nurses should nephropathy.
assess for these complications and implement Secondary glomerular disease: This is a less
appropriate interventions to manage them. common cause of nephrotic syndrome, and it occurs
as a result of an underlying medical condition such
NEPHROTIC SYNDROME
as diabetes, lupus, or amyloidosis.
Infections: Certain infections, such as hepatitis B and
C, HIV, and malaria, can increase the risk of
Nephrotic syndrome is a condition characterized by developing nephrotic syndrome.
high levels of protein in the urine (proteinuria), low Medications: Some medications, such as
levels of protein in the blood, swelling (edema), and nonsteroidal anti-inflammatory drugs (NSAIDs),
high levels of cholesterol and triglycerides. It is antibiotics, and ACE inhibitors, can increase the risk
usually caused by damage to the tiny blood vessels of developing nephrotic syndrome.
in the kidneys, which can lead to the loss of large Genetic factors: Certain genetic mutations can
amounts of protein in the urine. The condition can be increase the risk of developing nephrotic syndrome,
caused by a variety of underlying health problems, such as mutations in the NPHS1, NPHS2, and WT1
such as diabetes, lupus, and certain infections or genes.
medications. Nephrotic syndrome is typically treated Age: Nephrotic syndrome is more common in
with medications that help reduce proteinuria and children than in adults.
inflammation, as well as other supportive measures Gender: Boys are more likely to develop nephrotic
such as dietary changes and rest. syndrome than girls.
Race and ethnicity: Nephrotic syndrome is more
PATHOPHYSIOLOGY common in people of African American, Hispanic,
and Asian descent than in Caucasians.
The pathophysiology of nephrotic syndrome involves
damage to the glomeruli, which are tiny blood CLINICAL MANIFESTATIONS
vessels in the kidneys responsible for filtering waste
products and excess fluid from the blood. This Edema: One of the most common clinical
damage may be due to various causes, such as manifestations of nephrotic syndrome is edema or
immune system disorders, infections, medications, swelling. It usually starts in the lower extremities,
BSN 3A | PBL GROUP 1 19
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
such as the ankles and feet, and can spread to other drugs are corticosteroids, such as prednisone, which
parts of the body, including the face and abdomen. help reduce inflammation and decrease proteinuria.
Proteinuria: Nephrotic syndrome is also Other medications that may be used include
characterized by proteinuria, which means that large diuretics, ACE inhibitors, and angiotensin receptor
amounts of protein are excreted in the urine. This blockers.
results in foamy urine and can lead to low protein Dietary changes: Dietary changes, such as reducing
levels in the blood. salt intake, may be recommended to help control
edema and hypertension, which are common
Hypoalbuminemia: As a result of proteinuria, the complications of nephrotic syndrome.
level of albumin, a protein made by the liver that Immunosuppressive therapy: If the underlying cause
helps to maintain the fluid balance in the body, of nephrotic syndrome is an autoimmune disorder,
decreases in the blood, leading to hypoalbuminemia. such as lupus or vasculitis, immunosuppressive
Hyperlipidaemia: Nephrotic syndrome can also therapy may be prescribed to suppress the immune
cause an increase in the level of lipids, such as system and reduce inflammation.
cholesterol and triglycerides, in the blood. Plasmapheresis: In some cases, plasmapheresis, a
Fatigue and weakness: Due to the loss of protein in procedure in which the plasma is removed from the
the urine, the body may not have enough protein to blood and replaced with a protein solution, may be
maintain muscle mass, leading to fatigue and recommended to remove excess antibodies and
weakness. other proteins from the blood.
Decreased urine output: In some cases, nephrotic Kidney transplant: If nephrotic syndrome is caused
syndrome can lead to decreased urine output or by irreversible kidney damage, a kidney transplant
oliguria. may be the best option for treatment.
Increased risk of infections: As a result of decreased
levels of immunoglobulin’s in the blood, patients with NURSING INTERVENTIONS
nephrotic syndrome are at an increased risk of
developing infections. Monitor fluid and electrolyte balance: Monitor the
patient's intake and output, assess the patient's fluid
ASSESSMENT AND DIAGNOSTIC FINDINGS status, and monitor for signs of electrolyte
imbalances such as hyperkalemia and hyponatremia.
Medical history: The healthcare provider will ask Administer medications: Administer medications as
about the patient's medical history, including any ordered by the healthcare provider, such as diuretics
past or present kidney problems, infections, or other to manage edema, angiotensin-converting enzyme
medical conditions. (ACE) inhibitors to lower blood pressure, and
Physical exam: The healthcare provider will perform immunosuppressant medications to manage
a physical exam to look for signs of swelling, inflammation.
particularly in the legs, feet, and ankles. They will Monitor vital signs: Monitor the patient's blood
also listen to the patient's lungs and heart to check pressure, pulse rate, and respiratory rate regularly,
for signs of fluid buildup. as hypertension is a common complication of
Urine tests: Urine tests are done to measure the nephrotic syndrome.
amount of protein in the urine. A 24-hour urine Assess for edema: Assess the patient for edema,
collection may be done to get an accurate particularly in the face, legs, and feet. Measure and
measurement of protein excretion. document the circumference of affected body parts,
Blood tests: Blood tests are done to measure the and monitor the patient's weight daily.
level of protein, cholesterol, and triglycerides in the Promote skin integrity: Keep the skin clean and dry,
blood. Blood tests may also be done to check for and apply moisturizing lotion to prevent cracking and
kidney function and to look for signs of infections or dryness.
other medical conditions. Provide education: Educate the patient on the
Kidney biopsy: A kidney biopsy is a procedure in importance of adhering to medication regimens,
which a small piece of kidney tissue is removed and following a low-sodium diet, and monitoring their fluid
examined under a microscope to look for signs of intake.
damage or disease. Monitor laboratory values: Monitor the patient's
Imaging tests: Imaging tests such as ultrasound, CT laboratory values, such as serum albumin levels,
scan, or MRI may be done to check for signs of serum creatinine levels, and urine output, and report
kidney damage or to look for other possible causes any abnormalities to the healthcare provider.
of the patient's symptoms.
ACUTE KIDNEY INJURY
MANAGEMENT AND TREATMENT
is a rapid loss of renal function due to damage to the
Medications: The mainstay of treatment for nephrotic kidneys.
syndrome is medication. The most commonly used
BSN 3A | PBL GROUP 1 20
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
Depending on the duration and severity of AKI, a wide
range of potentially life-threatening metabolic
complications can occur, including metabolic acidosis as
well as fluid and electrolyte imbalances.
problem seen in patients who are hospitalized and those
in outpatient settings.
The term acute kidney injury has replaced the term acute
renal failure because it better describes this syndrome,
in both those who require RRT and also in those patients
who experience minor changes in renal function.
NOTE: A widely accepted criterion for AKI is a 50% or greater
increase in serum creatinine above baseline (normal
creatinine is less than 1 mg/dL) (The Acute Dialysis Quality
Initiative, 2004). Urine volume may be normal, or changes
may occur including nonoliguria (greater than 800 mL/day), CATEGORIES OF ACUTE KIDNEY INJURY
oliguria (less than 400 mL/day or 0.5 mL/kg/h over 6 hours),
or anuria (less than 50 mL/day) (Odom, 2017). PRERENAL - hypoperfusion of kidney; occurs in
60% to 70% of cases, is the result of impaired blood
PATHOPHYSIOLOGY flow that leads to hypoperfusion of the kidney
commonly caused by volume depletion (burns,
Although the exact cause of AKI and oliguria is not
hemorrhage, GI losses), hypotension (sepsis,
always recognized, many people suffer from them.
shock), and obstruction of renal vessels, ultimately
There is sometimes a specific underlying cause.
leading to a decrease in the GFR (Odom, 2017).
Some of the risk factors may be reversible if they are
detected and treated early before kidney function is INTRARENAL - actual damage to kidney tissue; the
compromised. Hypovolemia, hypotension, reduced result of actual parenchymal damage to the
cardiac output and heart failure, obstruction of the glomeruli or kidney tubules.
kidney or lower urinary tract by tumor, blood clot, or Acute tubular necrosis (ATN), or AKI in which
kidney stone, and bilateral obstruction of the renal there is damage to the kidney tubules, is the most
arteries or veins are all examples of conditions that common type of intrinsic AKI. Characteristics of
reduce blood flow to the kidney and impair kidney ATN are intratubular obstruction, tubular back leak
function. Increased BUN and creatinine levels, (abnormal reabsorption of filtrate and decreased
oliguria, and other symptoms may be reversed if urine flow through the tubule), vasoconstriction, and
these diseases are treated and rectified before the changes in glomerular permeability. These
kidneys are irreparably damaged. Although renal processes result in a decrease of GFR, progressive
stones are not a prevalent cause of AKI, they do azotemia, and fluid and electrolyte imbalances.
occur on occasion. AKI risk may be increased. CKD, diabetes, heart failure, hypertension, and
Some inherited stone disorders, primary struvite cirrhosis can contribute to ATN.
stones, as well as infection-related urolithiasis. POSTRENAL - obstruction to urine flow; usually
Urinary tract anatomic and functional abnormalities, results from obstruction distal to the kidney by
as well as spinal cord damage, may occur conditions such as renal calculi, strictures, blood
and induce recurring obstructions as well as crystal- clots, benign prostatic hyperplasia, malignancies,
specific injury to tubular epithelial cells and and pregnancy. Pressure rises in the kidney
interstitial renal cells (Odom, 2017). tubules, and eventually the GFR decreases.
CLASSIFICATIONS OF ACUTE KIDNEY INJURY PHASES OF ACUTE KIDNEY INJURY
Classification criteria for AKI include assessment of INITIATION - begins with the initial insult and ends
three grades of severity and two outcome-level when oliguria develops.
classifications. This 5-point system is known as the OLIGURIA - is accompanied by an increase in the
RIFLE classification system. RIFLE stands for risk, serum concentration of substances usually excreted
injury, failure, loss, and ESKD (Bellomo et al., 2004). by the kidneys (urea, creatinine, uric acid, organic
Risk, injury, and failure are considered grades of acids, phosphorus, and the intracellular cations
AKI severity, whereas loss and ESKD are [potassium and magnesium]). In this phase, uremic
considered outcomes of loss that require some form symptoms first appear and life-threatening
of RRT, at least temporarily (Bellomo et al., 2004). conditions such as hyperkalemia develop.
DIURESIS - is marked by a gradual increase in urine
output, which signals that glomerular filtration has
started to recover. Laboratory values stabilize and
eventually decrease. Although the volume of urinary
BSN 3A | PBL GROUP 1 21
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
output may reach normal or elevated levels, renal PREVENTION
function may still be markedly abnormal since the
filtration of urea and creatinine has not yet Continually assess renal function (urine output, laboratory
commenced. values) when appropriate.
Because uremic symptoms may still be present, the Monitor central venous and arterial pressures and hourly
need for expert medical and nursing management urine output of patients who are critically ill to detect the
continues. The patient must be observed closely for onset of kidney dysfunction as early as possible.
dehydration during this phase; if dehydration occurs, Pay special attention to wounds, burns, and other
the uremic symptoms are likely to increase and an precursors of sepsis.
elevated serum BUN and creatinine will be noted. Prevent and treat infections promptly. Infections can
RECOVERY - signals the improvement of renal produce progressive kidney damage.
function and may take 3 to 12 months. Laboratory Prevent and treat hypotensive shock promptly with blood
values return to the patient’s normal level. Although and fluid replacement.
a permanent 1% to 3% reduction in the GFR may Provide adequate hydration to patients at risk for
occur, it is not clinically significant. However, in those dehydration, including:
patients with preexisting CKD, an episode of AKI Before, during, and after surgery
may necessitate beginning CRRT. Patients undergoing intensive diagnostic studies
requiring fluid restriction and contrast agents (e.g.,
CLINICAL MANIFESTATIONS
barium enema, IV pyelograms), especially older
The patient may appear critically ill and lethargic. patients who may have marginal renal reserve or
Central nervous system signs and symptoms include CKD.
drowsiness, headache, muscle twitching, and Patients with neoplastic disorders or disorders of
seizures. Table 48-3 summarizes common clinical metabolism (e.g., gout) and those receiving
characteristics in all three categories of AKI. chemotherapy with potential tumor lysis syndrome
Patients with skeletal muscle injuries (e.g., crush
injuries, compartment syndrome).
Patients with heat-induced illnesses (e.g., heat
stroke, heat exhaustion).
To prevent infections from ascending in the urinary tract,
give meticulous care to patients with indwelling catheters.
Remove catheters as soon as possible.
To prevent toxic drug effects, closely monitor dosage,
duration of use, and blood levels of all medications
metabolized or excreted by the kidneys.
MEDICAL MANAGEMENT
Treatment is aimed at replacing renal function temporarily to
minimize potentially lethal complications and reduce potential
causes of increased kidney injury with the goal of minimizing
long-term loss of renal function. Management includes
eliminating the underlying cause; maintaining fluid balance;
avoiding fluid excesses; and, when indicated, providing RRT.
ASSESSMENT AND DIAGNOSTIC FINDINGS Prerenal azotemia is treated by optimizing renal perfusion,
whereas postrenal failure is treated by relieving the
Assessment of the patient with AKI includes obstruction. Intrarenal or intrinsic azotemia is treated with
evaluation for changes in the urine, diagnostic tests supportive therapy, with removal of causative agents,
that evaluate the kidney contour, and a variety of aggressive management of pre- and postrenal failure, and
laboratory values. avoidance of associated risk factors.
ULTRASONOGRAPHY - a critical component of the
evaluation of patients with kidney disease. HEMODIALYSIS - a procedure that circulates the
SONOGRAM OR NONCONTRAST CT SCAN - may patient’s blood through an artificial kidney [dialyzer]
show evidence of anatomic changes. to remove waste products and excess fluid.
SERUM CREATININE LEVELS - useful in PERITONEAL DIALYSIS - a procedure that uses the
monitoring kidney function and disease progression patient’s peritoneal membrane (the lining of the
and increase with glomerular damage. peritoneal cavity) as the semipermeable membrane
to exchange fluid and solutes.
BSN 3A | PBL GROUP 1 22
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
CONTINOUS RENAL REPLACEMENT THERAPY - PATHOPHYSIOLOGY
methods used to replace normal kidney function by
circulating the patient’s blood through a hemofilter. As renal function declines, the end products of protein
metabolism (normally excreted in urine) accumulate
PHARMACOLOGIC THERAPY in the blood. Uremia develops and adversely affects
every system in the body. The greater the buildup of
SODIUM POLYSTYRENE SULFONATE - treats waste products, the more pronounced the symptoms.
elevated potassium levels by exchanging sodium The rate of decline in renal function and progression
ions for potassium ions in the intestinal tract. of ESKD is related to the underlying disorder, the
IV DEXTROSE 50%, INSULIN, AND CALCIUM urinary excretion of protein, and the presence of
REPLACEMENT - may be given to shift potassium hypertension. The disease tends to progress more
back into the cells. rapidly in patients who excrete significant amounts of
protein or have elevated blood pressure than in those
NURSING MANAGEMENT without these conditions (Mahaffey, 2017).
The nurse monitors for complications, participates in
CLINICAL MANIFESTATIONS
emergency treatment of fluid and electrolyte imbalances,
assesses the patient’s progress and response to Cardiovascular Disease
treatment, and provides physical and emotional support.
Peripheral Neuropathy
The nurse keeps family members informed about the
Severe pain and discomfort
patient’s condition, helps them understand the treatments,
Restless leg and burning feet
and provides psychological support.
The nurse continues to provide nursing care indicated for ASSESSMENT AND DIAGNOSTIC FINDINGS
the primary disorder (e.g., burns, shock, trauma,
obstruction of the urinary tract). GLOMERULAR FILTRATION RATE - As the GFR
The nurse monitors the patient’s serum electrolyte levels decreases (due to nonfunctioning glomeruli), the
and physical indicators of these complications during all creatinine clearance decreases, whereas the serum
phases of the disorder. creatinine and BUN levels increase. Serum creatinine
The nurse monitors fluid status by paying careful attention is a more sensitive indicator of renal function than
to fluid intake (IV medications should be given in the BUN. The BUN is affected not only by kidney disease
smallest volume possible), urine output, apparent edema, but also by protein intake in the diet, catabolism
distention of the jugular veins, alterations in heart sounds (tissue and RBC breakdown), parenteral nutrition, and
and breath sounds, and increasing difficulty in breathing. medications such as corticosteroids.
The nurse takes steps to reduce the patient’s metabolic SODIUM AND WATER RETENTION - The kidney
rate. Fever and infection, both of which increase the cannot concentrate or dilute the urine normally in
metabolic rate and catabolism, are prevented and treated ESKD. Appropriate responses by the kidney to
promptly; blood, urine and wound cultures are ordered as changes in the daily intake of water and electrolytes,
indicated. therefore, do not occur. Some patients retain sodium
Attention is given to pulmonary function, and the patient is and water, increasing the risk for edema, heart failure,
assisted to turn, cough, and take deep breaths frequently and hypertension. Hypertension may also result from
to prevent atelectasis and respiratory tract infection. activation of the renin–angiotensin–aldosterone axis
Drowsiness and lethargy may prevent the patient from and the concomitant increased aldosterone secretion.
moving and turning without encouragement and Other patients have a tendency to lose sodium and
assistance. run the risk of developing hypotension and
Asepsis is essential with invasive lines and catheters to hypovolemia. Vomiting and diarrhea may cause water
minimize the risk of infection and increased metabolism. depletion, which may worsen the uremic state.
An indwelling urinary catheter is avoided whenever ACIDOSIS METABOLIC - acidosis occurs in ESKD
possible due to the high risk of UTI associated with its use, because the kidneys are unable to excrete increased
but may be required to provide ongoing data required to loads of acid. Decreased acid secretion results from
accurately monitor fluid I&O. the inability of the kidney tubules to excrete ammonia
(NH3 −) and to reabsorb sodium bicarbonate (HCO3
END-STAGE KIDNEY DISEASE OR CHRONIC KIDNEY
−). There is also decreased excretion of phosphorus
DISEASE
and other organic acids.
When a patient has sustained enough kidney damage ANEMIA - Anemia develops as a result of inadequate
to require RRT on a permanent basis, the patient has erythropoietin production, the shortened lifespan of
moved into the fifth or final stage of CKD, also referred RBCs, nutritional deficiencies, and the patient’s
to as ESKD. tendency to bleed, particularly from the GI tract.
Erythropoietin, a substance normally produced by the
kidneys, stimulates bone marrow to produce RBCs. In
ESKD, erythropoietin production decreases and
BSN 3A | PBL GROUP 1 23
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
profound anemia results, producing fatigue, angina, cannot maintain a reasonable quality of life with
and shortness of breath (Evans, 2017). conservative treatment.
CALCIUM AND PHOSPHORUS IMBALANCE -
Another abnormality seen in ESKD is a disorder in PHARMACOLOGIC THERAPY
calcium and phosphorus metabolism. Serum calcium
and phosphate levels have a reciprocal relationship in CALCIUM AND PHOSPHORUS BINDERS -
the body: As one increases, the other decreases. With Hyperphosphatemia and hypocalcemia are treated
a decrease in filtration through the glomerulus of the with medications that bind dietary phosphorus in the
kidney, there is an increase in the serum phosphorus GI tract. Binders such as calcium carbonate or
level and a reciprocal or corresponding decrease in calcium acetate are prescribed, but there is a risk of
the serum calcium level. The decreased serum hypercalcemia. This medication binds dietary
calcium level causes increased secretion of phosphorus in the intestinal tract; one to four tablets
parathormone from the parathyroid glands. However, are given with the first bite of food to be effective.
in kidney disease, the body cannot respond normally ANTIHYPERTENSIVE AND CARDIOVASCULAR
to the increased secretion of parathormone. As a AGENTS - Hypertension is managed by intravascular
result, calcium leaves the bone, often producing bone volume control and a variety of antihypertensive
changes and bone disease as well as calcification of agents. Heart failure and pulmonary edema may also
major blood vessels in the body. In addition, the active require treatment with fluid restriction, low-sodium
metabolite of vitamin D (1,25- diets, diuretic agents, inotropic agents, and dialysis.
dihydroxycholecalciferol) normally manufactured by The metabolic acidosis of ESKD usually produces no
the kidney decreases as kidney disease progresses symptoms and requires no treatment. However,
(Brooks, 2017). sodium bicarbonate supplements or dialysis may be
needed to correct the acidosis if it causes symptoms.
COMPLICATIONS ERYTHROPOIETIN - Anemia associated with ESKD
is treated with erythrocyte-stimulating agents
ANEMIA due to decreased erythropoietin production, (recombinant human erythropoietin).
decreased RBC lifespan, bleeding in the GI tract from
irritating toxins and ulcer formation, and blood loss in NURSING MANAGEMENT
the dialysis circuit and dialyzer after HD has been
completed. Nursing care is directed toward assessing fluid status
BONE DISEASE AND METASTATIC AND and identifying potential sources of imbalance,
VASCULAR CALCIFICATIONS due to retention of working with a renal dietitian to implement a dietary
phosphorus, low serum calcium levels, and abnormal program to ensure proper nutritional intake within the
vitamin D metabolism. limits of the treatment regimen, and engaging the
HYPERKALEMIA due to decreased excretion, patient by encouraging increased self-care and
metabolic acidosis, catabolism, and excessive greater independence. It is extremely important to
potassium intake from diet, medications, or IV provide explanations and information to the patient
solutions. and family concerning ESKD, treatment options, and
HYPERTENSION due to sodium and water retention potential complications. A great deal of emotional
and malfunction of the renin–angiotensin–aldosterone support is needed by the patient and family because
system. of the numerous changes experienced. A social
PERICARDITIS, PERICARDIAL EFFUSION, AND worker is also a vital part of the interprofessional care
PERICARDIAL TAMPONADE due to retention of at the dialysis center. Specific interventions, along
uremic waste products and inadequate dialysis. with rationale and evaluation criteria, are presented in
more detail in the plan of nursing care for the patient
MEDICAL MANAGEMENT with ESKD.
The goal of management is to maintain kidney RENAL REPLACEMENT THERAPIES
function and homeostasis for as long as possible.
Management is accomplished primarily with Renal replacement therapy is a term used to
medications and diet therapy, although dialysis may encompass life-supporting treatments for renal
also be needed to decrease the level of uremic waste failure. Renal replacement therapy replaces
products in the blood and to control electrolyte nonendocrine kidney function in patients with renal
balance. The close collaboration of a renal dietitian is failure. Techniques include intermittent
essential in dietary therapy. hemodialysis, continuous hemofiltration and
hemodialysis, and peritoneal dialysis. All modalities
DIALYSIS The patient with increasing symptoms of
exchange solute and remove fluid from the blood,
kidney disease is referred to a dialysis and
using dialysis and filtration across permeable
transplantation center early during progressive kidney
membranes.
disease. Dialysis is usually initiated when the patient
BSN 3A | PBL GROUP 1 24
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
Dialysis and filtration can be done intermittently or Detecting cardiac and respiratory
continuously. Continuous therapy is used exclusively Complications
for acute renal failure; benefits over intermittent Controlling electrolyte levels and Diet
therapy are improved tolerability as a result of slower Managing discomfort and pain
removal of solute and water. Monitoring BP
Preventing infection
DIALYSIS
Caring for the catheter site
Dialysis is a treatment for individuals whose kidneys Administering medications
are failing. When you have kidney failure, your Providing psychological support -pt andfamily
kidneys don’t filter blood the way they should.
Dialysis does the work of your kidneys.
PRESCRIPTION MANAGEMENT
WHO NEEDS DIALYSIS Understand your medications
Keep your medications organized
People who have kidney failure end- stage Stick with your treatment plan
renal disease (ESRD) Take all the medication you were prescribed.
Tell your doctor if you’re having side effects.
Injuries and conditions like high blood Check with your doctor first before you stop taking
pressure, diabetes and lupus can damage your medication.
kidneys, leading to kidneydisease. Ask your doctor if your prescription needs to be
refilled.
TWO TYPES OF DIALYSIS ACTIVITY RESTRICTION WHILE ON DIALYSIS
Hemodialysis Limit exercise or certain physical activities when the
Peritoneal Dialysis abdomen fills with dialysis solution. Otherwise,
exercise is typically OK for people on dialysis.
HEMODIALYSIS You should ask your provider about participating in
specific activities or sports.
With hemodialysis, a machine removes blood
from your body, filters it through a dialyzer NOTE: Dialysis only replaces part of your kidney function.
(artificial kidney) and returns thecleaned blood Hemodialysis and peritoneal dialysis allow people with
to your body. This 3- to 5-hour process may kidney failure to feel better and continue doing the things
take place in a hospitalor a dialysis center three they enjoy, but neither replaces all the jobs that healthy
times a week. kidneys do.
You can also do hemodialysis at home. You HEMODIALYSIS DIALYZERS
may need at-home treatments four to seven
times per week for fewer hourseach session. HEMODIALYSIS
PERITONEAL DIALYSIS It is used for patients who are acutely ill and require
short-term dialysis for days to weeks until kidney
With peritoneal dialysis, tiny blood vessels function resumes, as in patients with AKI, and for
inside the abdominal lining (peritoneum) filter patients with advanced CKD and ESKD who
blood through the aid of a dialysis solution. This require long-term or permanentRRT.
solution is a type of cleansing liquid that Prevents death but does not cure kidney disease
contains water, salt, and other additives. and does not compensate for the loss of endocrine
or metabolic activities of the kidneys.
Two ways to do this treatment: The objectives of HD are to extract toxic
nitrogenous substances from the blood and to
Automated peritoneal dialysis uses amachine
remove excess fluid.
called a cycler.
Continuous ambulatory DIALYZERS
peritoneal dialysis (CAPD) takes place
manually. Also referred to as an artificial kidney.
Hollow-fiber devices containing thousands oftiny
capillary tubes that carry the blood through the
NURSING RESPONSIBILITIES: HOSPITALIZED PATIENT artificial kidney.
Dialyzers have undergone many technologic
Protecting the vascular access changes in performance and biocompatibility.
Precautions during, I.V therapy
Monitoring symptoms of uremia
BSN 3A | PBL GROUP 1 25
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
VASCULAR ACCESS Other complications of dialysis may include the
following:
Access to the patient’s vascular system must be o Episodes of shortness of breath
established to allow blood to be removed, o Hypotension
cleansed, and returned to the patient’s vascular o Painful muscle cramping
system at the rapid rates of 300 and 500 mL/min. o Exsanguination
Several types of access can be surgically created
o Arrhythmias
or placed during procedures performed in
interventional radiology suites or at the bedside. o Air embolism
o Chest pain
o Dialysis disequilibrium
VASCULAR ACCESS DEVICES
Immediate access to the patient’s circulation for NURSING MANAGEMENT
acute HD is achieved by inserting a double- lumen,
noncuffed, large-bore catheter into the right or left The nurse in the dialysis unit has an important
internal jugular or femoral vein of either leg by the role in monitoring, supporting, assessing, and
physician, nurse practitioner, or physician educating the patient.
assistant.
This method of vascular access involves some risk
(e.g., hematoma, bleeding, pneumothorax, PHARMACOLOGICAL THERAPY
infection, thrombosis of the vein, inadequate flow).
The catheter is removed when no longer needed. Many medications are removed from the blood
during HD.
Medications that are water soluble are readily
ARTERIOVENUS FISTULA removed during HD treatment, and those that are fat
soluble or adhere to other substances (like albumin)
The preferred method of permanent vascular are not dialyzed out very well.
access for dialysis. Patients undergoing HD who require medications
This is created surgically (usually in theforearm) (e.g., cardiac glycosides, antibiotic agents,
by anastomosing (joining) an artery to a vein, antiarrhythmic medications, antihypertensive
either side to side or end to side. agents) are monitored closelyto ensure that blood
Needles are inserted into the vessel to obtain and tissue levels of these medications are
blood flow which is adequate to pass through the maintained without toxic accumulation.
dialyzer.
Many medications that are taken once daily should
The patient is encouraged to perform hand be administered after the dialysistreatment.
exercise.
NUTRITIONAL AND FLUID THERAPY
ARTERIOVENUS GRAFT
Diet is important for patients on HD.
Can be created by subcutaneously interposing a
biologic, semi biologic, or synthetic graft material Restriction of fluid is also part of the dietary
between an artery and vein. prescription because fluid accumulation may
occur, leading to fluid volume excess, heart failure,
Patients with compromised vascular systems
and pulmonary edema.
(e.g., from diabetes) often require a graft because
With the initiation of HD, the patient usually
their native vessels may not be suitable for
requires some restriction of dietary sodium,
creation of an AVF.
potassium, phosphorus, and fluid intake.
Stenosis, infection, and thrombosis are the most
common complications of this access. The goal for patients on HD is to keep their
interdialytic (between dialysis treatments) weight
gain less than 4% of their estimated dryweight
COMPLICATIONS (Gonyea, 2017).
Although HD can prolong life, it does not alter the MEETING PSYCHOLOGICAL NEEDS
natural course of the underlying CKD, nor does it
completely replace kidney function. The CKD
complications previously discussed will continue to Patients requiring long-term HD, as theyengage in
worsen and require treatment. psychosocial adaptation, tend to feelmired in a
cyclical routine (Lin, Han, & Pan, 2015).
Many people undergoing HD experience major The regimented lifestyle that frequents dialysis
sleep problems that further complicate their overall treatments and restrictions in food and fluid intake
impose can be demoralizing to the patient and
health status. Early-morning or late-afternoon
family.
dialysis may bea risk factor for developing sleep
Dialysis alters the lifestyle of the patient and
disturbances. family.
BSN 3A | PBL GROUP 1 26
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
The nurse needs to give the patient and family the functional status, and quality of life (Browne &
opportunity to express feelings of anger and Johnstone, 2017).
concern about the limitations that the disease and Many patients with CKD can resume relatively
treatment impose, possible financial problems, normal lives, doing the things that are important to
and job insecurity.
them: traveling, exercising, working, or actively
participating in family activities.
PROMOTING HOME, COMMUNITY-BASED, AND
Outcome goals for renal rehabilitation include
TRANSITIONAL CARE
employment for those able to work, improved
physical functioning of all patients, improved
High-quality transitional care is especially
important for older adults with multiple chronic understanding about adaptation and options for living
conditions and complex therapeutic regimens, as well, increased control over the effects of kidney
well as for their family caregiver. disease and dialysis, and resumption of activities
Communication about prognosis and patientgoals by enjoyed before dialysis.
a dedicated team with time and expertise leads to
CONTINUOUS RENAL REPLACEMENT THERAPY
decision making, clarity of the care plan, and
consistent follow-through.
CRRT is a method used to replace normalkidney
function in patients who are hemodynamically
EDUCATING PATIENTS ABOUT SELF-CARE
unstable by circulating thepatient’s blood through a
hemofilter and returning it to the patient.
Preparing a patient for HD is essential.
Continuous renal replacement therapy (CRRT)is a
Assessment helps identify the learning needs of the
method of slower, continuous dialysis to allow solute
patient and family members.
and fluid homeostasis. There are different
The diagnosis of ESKD and the need for dialysis
techniques of CRRT that aredistinguished by their
is a big adjustment for the patient and family.
method of solute removal,each detailed below. The
Many patients with ESKD have clinical
choice of CRRT is primarily based on provider
depression, and chronic uremia contributes to a
preference insteadof specific patient characteristics
shortened attention span, a decreased level of
or outcome data. This activity details the principles,
concentration, and altered perception.
indications, and complications of CRRT, and it
The nurse needs to convey a nonjudgmental
discusses when to consider initiating CRRT andwhen
attitude to enable the patient and family to discuss
options and their feelings about those options. to discontinue it. It highlights the role of the inter-
professional team in managing patients on CRRT.
HOME HEMODIALYSIS CRRT may be indicated for patients with acute or
chronic kidney disease who are too clinicallyunstable
Most patients who undergo HD do so in an for traditional HD, for patients with fluid overload
outpatient setting, but home HD is an option for secondary to oliguric (low urine output) kidney
some. disease, and for patients whose kidneys cannot
Home HD requires a highly motivated patient who handle their acutely high metabolic or nutritional
is willing to take responsibility for the needs. Some forms of CRRT may not require dialysis
procedure and can adjust each treatment to meet machines or dialysis personnel to carry out the
the body’s changing needs.
procedures and can be initiated quickly in the critical-
The health care team never forces a patient to use
home HD, because this treatment requires care unit. The methods are similar, as they require
changes in the home and family. access to the circulation and blood to pass through
The patient undergoing home HD and the an artificial filter. A hemofilter (an extremely porous
caregiver assisting that patient must be trained to blood filter containing a semipermeable membrane)
prepare, operate, and disassemble the dialysis is used in all types.
machine; maintain and clean the equipment;
administer medications (e.g., heparin) into the SEVERAL TYPES OF CRRT
machine lines; and handle emergency problems
(HD dialyzer rupture, electrical or mechanical
problems, hypotension, shock, and seizures) These are available and widely used incritical-
(Harwood & Dominski, 2017). care units.
Before home HD is initiated, the home
environment, household and community
resources, and ability and willingness of the
patient and family to carry out this treatment are
assessed.
CONTINUING AND TRANSITIONAL CARE
The health care team’s goal in treating patients with
CKD is to maximize their vocational potential,
BSN 3A | PBL GROUP 1 27
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
Devices for administering continuous renal embolization, and blood loss that occurs with the
replacement therapy (CRRT) offer an integrated filter or circuit changes.
fluid warmer for the heating of infusion and
dialysate fluids, a weighing or volumetric HOW CRRT WORKS?
measuring system to reduce the possibility of
error in assessing fluid balance, and a battery CRRT does some of the work normally done by
backup that allows treatments to continue when healthy kidneys. It gently filters and cleans your
the patient is moved. child’s blood by removing waste products and extra
The involvement of specialists external to fluid. This keeps chemicals and electrolytes, like
conventional intensive care staff with expertise potassium and phosphorus, in your child’s blood
in critically ill patients is not a new practice. The balanced. CRRT does not actually improve your
following is a list of external groups involved in child’s kidney function, but instead it keeps
the interprofessional management of patients
everything in line in your child’s body until the
on CRRT:
kidneys recover function.
o Respiratory care practitioners
o Nutritional support team A central venous catheter (CVC) is placed in one of
o Clinical pharmacology your child’s large veins. This is usually in the neck or
o Diagnostic and interventional radiology groin.
o Cardiology The CVC is connected to a machine that circulates
o Rehabilitation and physiotherapy some of your child’s blood in a loop outside the body.
After the blood has been filtered and cleaned, it is
sent back into the body. Nationwide Children’s
COMPLICATIONS Hospital uses 2 types of machines for CRRT:
PrisMax™ and Aquadex®.
As with every procedure, CRRT has risks, and these
should be communicated to the patient or family BEFORE CRRT
when considering initiation. Firstly, the risks
associated with intravascular lines include Placement of the dialysis catheter (CVC) is a sterile
hemorrhage, AV fistula, infection, or thrombosis. procedure. It is done by an intensive care unit (ICU)
The risks of the therapy itself include electrolyte doctor or a radiology doctor skilled in catheter
disturbances, clearance of trace elements or placement. The doctor placing the catheter will
antibiotics, hypothermia, and hypotension. decideif the parents may stay during the procedure.
Although hypotension should occur less commonly
than in IHD, hypotension may occur if the net DURING CRRT
ultrafiltration rate exceeds the intravascular filling
Your child will be connected to the CRRT machine thewhole
rate. Monitoring of electrolytes and acid-base
time. The machine is run by specially trained nurses in the
statusshould be done every 6 to 12 hours when
ICU.
starting CRRT. If remaining stable after the first 24
to 48 hours, the interval may be increased to 12 to The machine works best if your child doesn’t move
24 hours. The exception, as discussed above, is a lot. They may be given medicines, called
when using citrate as regional anticoagulation sedatives, to keep them still so the CRRT goes
because this requires frequent monitoring of smoothly.
ionized calcium levels. There are situations when your child will be taken
The removal of medications during CRRT is off(disconnected) from the CRRT machine. These
variable, and so it is advised to check the dose of include:
required drugs when on CRRT. This practice is If they need to have a test or a procedure. The
critical when it comesto administering antibiotics, as machine will be restarted afterward.
the troughconcentrations of these medications will Routine change of the tubing and filter to keep the
system operating well. This only requires a short
determine their bacteriocidal or bacteriostatic
time off the machine.
effectiveness. Most affected are water-soluble
Sometimes small blood clots get in the filter and
antimicrobials, aminoglycosides, and beta-lactam tubing and stop the machine from working well. A
antibiotics. Many patients who meet indications for nurse will change the tubing and filter if this
CRRT will do so because of sepsis, meaning that happens.
appropriate antibioticdosage is vital. The machine’s alarm may go off during CRRT.
CRRT will result in amino acid, micronutrient, and Most of the alarms are not because of an
water-soluble vitamin loss. Patients are also often in emergency. They are usually meant to alert the
asubstantial negative nitrogen balance. Appropriate nurse(s) to changesolution bags. The machine may
caloric and protein intake with supplementation of also alarm to let the nurse know to change your
water-soluble vitamins should be ensured. child’s position or check the catheter to help the
Finally, the risks associated with the extracorporeal treatment run smoothly.
circuit include hypersensitivity to the circuit, air
BSN 3A | PBL GROUP 1 28
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
AFTER CRRT The peritoneal catheter can be inserted in
interventional radiology, in the operating room, or,
As your child gets better, the team may try some rarely, at the bedside.
time off CRRT. This is to see how well your child’s
kidneys work. If kidney support is still needed, Preparing the Equipment
CRRT may need to be restarted, or they may be
The nurse consults with the physician to determine
changed to a less frequent type of dialysis called
the concentration of dialysate to be used and the
hemodialysis. This is done for shorter periods of
medications to be added.
time (3 to 5 days perweek).
o Heparin may be added to prevent fibrin
If you have questions about your child’s kidney formation and resultant occlusion of the
functionor the CRRT treatment, please talk to your peritoneal catheter.
child’s kidney doctor (nephrologist). o Potassium chloride may be prescribed to
PERITONEAL DIALYSIS prevent hypokalemia.
o Antibiotic agents may be added to treat
Peritoneal dialysis (PD) is one type of dialysis treatment for peritonitis (inflammation of the peritoneal
kidney failure. It uses a fluid that you put in your belly and membrane) caused by infection.
then remove to clean your blood. It can be done at home.
o Insulin is rarely added to PD fluid due to
The goals of PD are to remove toxic substances and widespread use of subcutaneous insulin
metabolic wastes and to reestablish normal fluid and pumps and sliding scales.
electrolyte balance. In a hospital setting, to prevent contamination, a
PD may be the treatment of choice for patients with pharmacist generally adds all medications to the
kidney disease who are unable or unwilling to dialysate bags in the pharmacy under a laminar flow
undergo HD or kidney transplantation. hood.
Patients with diabetes or cardiovascular disease, In the home setting, the nurse instructs the patient or
many older patients, and those who may be at risk family on how to aseptically add medications to PD
for adverse effects of systemic heparin are likely fluid.
candidates for PD. The dialysate is warmed to body temperature to
Severe hypertension, heart failure, and pulmonary prevent patient discomfort and abdominal pain and
edema not responsive to usual treatment regimens to dilate the vessels of the peritoneum to increase
have been successfully treated with PD. urea clearance.
Immediately before initiating dialysis, using aseptic
In PD, the peritoneal membrane that covers the abdominal technique, the nurse assembles the dialysate with
organs and lines the abdominal wall serves as the attached tubing and drainage bag.
semipermeable membrane. Sterile dialysate fluid, containing All PD dialysate fluid, tubing, and drainage bags are
dextrose and electrolytes, is introduced into the peritoneal manufactured as closed systems and no spiking of
cavity through an abdominal catheter at established intervals. solution is needed.
Once the sterile solution is in the peritoneal cavity, uremic The tubing is primed with the prepared dialysate to
toxins such as urea and creatinine begin to be cleared from prevent air from entering the catheter and peritoneal
the blood. cavity, which would cause abdominal discomfort and
interfere with instillation and drainage of the fluid.
PROCEDURE
Inserting the Catheter
Preparing the Patient
The peritoneal catheter is inserted in the operating
Assess the patient’s physical and psychological
room or radiology suite to maintain surgical asepsis
status, mental status, previous experience with
and minimize the risk of contamination.
dialysis, and understanding of and familiarity with the
Catheters for long-term use are usually soft and
procedure.
flexible and made of silicone with a radiopaque strip
The nurse and surgeon or interventional radiologist
to permit visualization on x-ray.
or nephrologist explains the procedure to the patient.
These catheters have three sections:
The nurse assists the provider in obtaining signed
o an intraperitoneal section, with numerous
consent for insertion of the catheter. Baseline vital
openings and an open tip to allow dialysate
signs, weight, and serum electrolyte levels are
to flow freely.
recorded.
o a subcutaneous section that passes from
The patient is instructed to empty the bladder and the peritoneal membrane and tunnels
bowel to reduce the risk of puncture of internal through muscle and subcutaneous fat to the
organs during the insertion procedure. skin.
A prophylactic antibiotic agent will be given to
prevent infection.
BSN 3A | PBL GROUP 1 29
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
o an external section for connection to the o The first sign of peritonitis is cloudy
manufacturer specific transfer set which dialysate effluent. Diffuse abdominal pain
then connects to the dialysate tubing with and rebound tenderness often occur later.
attached dialysate. Hypotension and other signs of shock may
Most adult catheters have 2 cuffs made of Dacron also occur with advancing infection.
polyester. o The patient with peritonitis may be treated
The cuffs stabilize the catheter, limit movement, as an inpatient or outpatient (most
prevent leaks, and provide a barrier against common), depending on the severity of the
microorganisms. infection and the patient’s clinical status.
One cuff is placed just distal to the peritoneum, and o Antibiotic therapy continues for 14 to 21
the other cuff is placed subcutaneously. The days.
subcutaneous tunnel (5 to 10 cm long) further o During an episode of peritonitis, the patient
protects against bacterial infection. loses large amounts of protein through the
peritoneal membrane due to inflammation
Performing the Exchange and increased permeability.
o Attention must be given to educating the
All types of PD involve a series of exchanges or cycles. An patient to detect and promptly seek
exchange is the entire cycle including drainage of the effluent treatment for peritonitis.
(fluid), instillation of the dialysate, and dwell. This cycle is
repeated throughout the course of the dialysis. Leakage: leakage of dialysate through the catheter
site may occur even after a healing period.
The dialysate is infused by gravity into the peritoneal
o Usually, the leak stops spontaneously when
cavity. A period of about 10 minutes is usually dialysis is withheld for several days, giving
required to infuse 2 to 3 L of fluid. the tissue the opportunity to heal around the
A sterile cap is applied to the transfer set and the catheter cuffs and to seal the insertion
patient can perform ADLs. tunnel.
The prescribed dwell, or equilibration time, allows o It is important to reduce factors that might
diffusion and osmosis to occur. delay healing, such as undue abdominal
At the end of the prescribed dwell, the patient muscle activity (bending, lifting over 5 lb)
performs hand hygiene, dons a mask, removes the and straining during bowel movements.
sterile cap, unclamps the transfer set, and the o In many cases, leakage can be avoided by
solution drains from the peritoneal cavity by gravity using small volumes (500 mL) of dialysate,
through a closed system. gradually increasing the volume up to 2000
Drainage is usually completed in 20 to 30 minutes. to 3000 mL.
The drainage fluid is normally colorless or straw-
colored and should not be cloudy. Bloody or pink- Bleeding: Bleeding is also common during the first
colored drainage may be seen in the first few few exchanges after a new catheter insertion
exchanges after insertion of a new catheter, but because some blood enters the abdominal cavity
should not occur after that time. following insertion. The bleeding most often clears up
after several exchanges.
The number of cycles or exchanges and their frequency are o Most often, bleeding stops in 1 to 2 days
prescribed based on monthly laboratory values and the and requires no specific intervention.
presence of uremic symptoms. o More frequent exchanges and the addition
of heparin to the dialysate during this time
The exchanges can be performed manually during the waking
may be necessary to prevent blood clots
hours by the patient (continuous ambulatory peritoneal
from obstructing the catheter.
dialysis [CAPD]) or via the use of a PD machine (cycler) that
automatically performs exchanges, usually while the patient is LONG-TERM COMPLICATIONS
sleeping at night (continuous cycling peritoneal dialysis
[CCPD]). Hypertriglyceridemia, likely due to the use of glucose
containing dialysate, is common in patients on long-
COMPLICATIONS term PD.
Other complications that may occur with long-term
Most complications of PD are often minor; however, several, PD include abdominal hernias (incisional, inguinal,
if unattended, can have serious consequences. diaphragmatic, and umbilical), likely resulting from
ACUTE COMPLICATIONS continuously increased intra-abdominal pressure.
The persistently elevated intra-abdominal pressure
Peritonitis: is the most common and serious also aggravates symptoms of hiatal hernia and
complication of PD. hemorrhoids.
BSN 3A | PBL GROUP 1 30
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
Mechanical problems occasionally occur and may the tubing set, disconnects the tubing set, and
interfere with instillation or drainage of the dialysate. applies a new sterile cap to the transfer set, making
Formation of clots and fibrin in the peritoneal it a closed system.
catheter and constipation are factors that may
contribute to these problems. Complications
APPROACHES To reduce the risk of peritonitis, the patient (and all
caregivers) must use meticulous aseptic care to
ACUTE INTERMITTENT PERITONEAL DIALYSIS avoid contaminating the catheter, fluid, or tubing and
to avoid accidentally disconnecting the catheter from
Indications for acute intermittent PD, a variation of the tubing.
PD, include uremic signs and symptoms (nausea, Whenever a connection or disconnection is made,
vomiting, fatigue, altered mental status), fluid hand hygiene must be performed and a mask worn
overload, acidosis, and hyperkalemia. by anyone within 6 ft of the area to avoid
Exchange times range from 30 minutes to 2 hours. contamination with airborne bacteria.
Acute intermittent PD is not indicated for long-term Excess manipulation should be avoided, and
patient management, but for specific situations such meticulous care of the catheter exit site is provided
as patients who are referred late in the course of using a standardized protocol.
CKD (CKD stage 5) and require immediate dialysis. At home, a patient is taught to use clean technique
The nurse uses a flow sheet on paper or within the for exit site care.
electronic health record to document each exchange In the hospital, due to the increased risk of infection,
and records vital signs, dialysate concentration, sterile technique is employed by the nurse and
medications added, exchange volume, dwell time, patient.
dialysate fluid balance for each exchange (fluid lost
or gained), and cumulative fluid balance.
The nurse also carefully assesses skin turgor and CONTINUOUS CYCLIC PERITONEAL DIALYSIS
mucous membranes to evaluate fluid status and
It uses a machine called a cycler to provide the fluid
monitor the patient for edema. Daily weight is the
exchanges. It is programmed to deliver an
most accurate indicator of fluid volume status
established amount of PD solution that will dwell in
The nurse must ensure that the PD catheter remains
the peritoneal cavity for a programmed period of time
secure and that the dressing remains dry and is
before it drains from the peritoneal cavity via gravity.
changed on a routine basis.
CCPD may combine overnight intermittent PD with a
The patient and family are educated about the
prolonged dwell time during the day.
procedure and are kept informed about progress
Every evening, the patient connects the peritoneal
(fluid loss, weight loss, laboratory values).
catheter to tubing on the cycler machine, usually just
CONTINUOUS AMBULATORY PERITONEAL DIALYSIS before the patient goes to sleep for the night.
(CAPD) Because the machine is very quiet, the patient can
sleep, and the extra-long tubing allows the patient to
This works on the same principles as other forms of move and turn normally.
PD: diffusion and osmosis. Less extreme fluctuations In the morning, the patient disconnects from the
in the patient’s laboratory values occur with CAPD cycler. This process is done every day to achieve the
than with intermittent PD or HD because the dialysis effects of dialysis required.
is constantly in progress. The serum electrolyte CCPD has a lower infection rate than other forms of
levels often remain in the normal range PD because there are fewer opportunities for
contamination with bag changes and tubing
Procedure
disconnections.
The patient performs exchanges four or five times a It also allows the patient to be free from exchanges
day, 24 hours a day, 7 days a week, at intervals throughout the day, making it possible to engage in
scheduled throughout the day. work and activities of daily living more freely.
A closed Y-shaped system is most commonly used.
NURSING MANAGEMENT
To perform an exchange, the patient (or person
doing the exchange) washes their hands, dons a MEETING PSYCHOSOCIAL NEEDS
mask, and then removes the cap from the transfer
set while maintaining sterility. Patients who elect to do PD may experience altered
The open end of the “Y” set is connected to the end body image because of the presence of the
of the transferset and the dialysate is drained into the abdominal catheter, bag, tubing, and cycler. The
attached empty sterile bag (effluent) (over about 20 nurse may arrange for the patient to talk with other
to 30 minutes). Then the attached dialysate is patients who have adapted well to PD.
infused, the patient clamps off the transfer set and
BSN 3A | PBL GROUP 1 31
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
Patients undergoing PD may also experience altered The nurse continues to reinforce and clarify
sexuality patterns and sexual dysfunction. The education about PD and ESKD and assesses the
patient and partner may be reluctant to engage in patient’s and family’s progress in coping with the
sexual activities, partly because of the catheter being procedure.
psychologically “in the way” of sexual performance.
Questions by the nurse about concerns related to INFECTIONS OF THE URINARY TRACT
sexuality and sexual function often provide the caused by pathogenic microorganisms in the
patient with a welcome opportunity to discuss these urinary tract
issues and a first step toward assisting in their
NORMAL URINARY TRACT: sterile above urethra
resolution
Classified by location
PROMOTING HOME, COMMUNITY-BASED, AND LOWER URINARY TRACT: bladder & structures
TRANSITIONAL CARE below bladder
UPPER URINARY TRACT: kidneys & ureters
Patients are educated as inpatients or outpatients to second most common infection in the body
perform PD once their condition is medically stable. CATHETER-ASSOCIATED URINARY TRACT
Education generally takes 5 days to 2 weeks. INFECTIONS (CAUTI): hospital acquired infection
Patients are taught according to their own learning o associated with indwelling urinary
ability and knowledge level and only as much at one catheters.
time as they can handle without feeling o UTI that occurs while the patient had an
uncomfortable or becoming saturated. indwelling urinary catheter in place for
Because of protein loss with PD, the patient is more than 2 calendar days on the day that
instructed to eat a highprotein (1.2 to 1.3g/kg/day), the infection was detected.
low phosphorus, nutritious diet (NKF KDOQI, 2000).
The patient is also encouraged to increase their daily LOWER URINARY TRACT INFECTION
fiber intake to help prevent constipation, which can
Bladder & structures below the bladde
impede the flow of dialysate into or out of the
Bladder: sterile
peritoneal cavity.
Mechanisms that protects the sterility of the
Patients may gain 3 to 5 lb within a month of initiating
bladder:
PD, so they may be asked to limit their carbohydrate
o physical barrier of the urethra assists in
intake to avoid weight gain. keeping bacteria away from the bladder
Potassium and fluid restrictions are not usually o antibacterial enzymes and antibodies
necessary. Patients commonly lose at least 1 to 2 L o antiadherent effects mediated by the
of fluid over and above the volume of dialysate mucosal cells of the bladder
infused into the abdomen during a 24-hour period, LOWER UTIs include:
permitting a moderate fluid intake. o BACTERIAL CYSTITIS: inflammation of
urinary bladder
CONTINUING AND TRANSITIONAL CARE
o BACTERIAL PROSTATITIS: inflammation
Follow-up care through phone calls, visits to the of prostate gland
dialysis clinic, outpatient department, and continuing o BACTERIAL URETHRITIS: inflammation
home care assists patients in the transition to home of the urethra
and promotes their active participation in their own
PATHOPHYSIOLOGY
health care.
Patients often check with the nurse to see if they are For infection to occur, bacteria must gain access to
making the correct choices about dialysate or control the bladder, attach to and colonize the epithelium of
of blood pressure, or simply to discuss a problem. the urinary tract to avoid being washed out with
If a referral is made for home care, the home health voiding, evade host defense mechanisms, and
nurse assesses the home environment and suggests initiate inflammation. Many UTIs result from fecal
modifications to accommodate the equipment and organisms ascending from the perineum to the
facilities needed to carry out PD. urethra and the bladder and then adhering to the
The nurse assesses the patient’s and family’s mucosal surfaces.
understanding of PD and evaluates their technique
in performing PD. RISK FACTORS
Assessments include checking for changes related
to kidney disease; any complications such as Female gender
peritonitis; medication management; and treatment Diabetes
related problems such as heart failure, inadequate Pregnancy
drainage, and weight gain or loss. Neurologic disorders
BSN 3A | PBL GROUP 1 32
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
Gout o bacteria (often from fecal contamination)
Altered states caused by incomplete emptying of colonize the periurethral area and
the bladder and urinary stasis subsequently enter the bladder by means
Decreased natural host defenses or of the urethra
immunosuppression increased incidence of UTI to those who engage in
Inability or failure to empty the bladder completely penile-vaginal intercourse
Inflammation or abrasion of the urethral mucosa o due to short urethra
Instrumentation of the urinary tract (e.g.,
CLINICAL MANIFESTATIONS
catheterization, cystoscopic procedures)
Obstructed urinary flow caused by: UNCOMPLICATED UTI
o Congenital abnormalities
o Urethral strictures burning on urination
o Contracture of the bladder neck urinary frequency (more than every 3 hrs)
o Bladder tumors urinary urgency
o Calculi (stones) in the ureters or kidneys
nocturia
o Compression of the ureters
incontinence
BACTERIAL INVASION OF THE URINARY TRACT suprapubic or pelvic pain
hematuria
Bacterial removal: due to increased normal slow back pain
shedding of bladder epithelial cells
Glycosaminoglycan (GAG): hydrophilic protein; COMPLICATED UTI
attracts water forming a water barrier that serves as
defensive layer between bladder & urine asymptomatic bacteriuria to gram-negative sepsis
with shock
Urinary immunoglobulin A (IgA): provides barrier to
bacteria
GERONTOLOGIC CONSIDERATIONS
REFLUX
Bacteriuria increases with age and disability
URETHROVESICAL REFLUX: obstruction of free- women are affected more frequently than men
flowing urine In older adults, structural abnormalities secondary
o Backward flow of urine from urethra to the to decreased bladder tone, neurogenic bladder
bladder (dysfunctional bladder) secondary to stroke, or
o COUGHING, SNEEZING, OR autonomic neuropathy of diabetes may prevent
STRAINING: the bladder pressure complete emptying of the bladder and increase the
increases, which may force urine from the risk of UTI
bladder into the urethra ABSENCE OF ESTROGEN: postmenopausal
o caused by dysfunction of the bladder neck women are susceptible to colonization & increased
or urethra adherence of bacteria to vagina & urethra
o When the ureterovesical valve is impaired o Oral or topical estrogen has been used
by congenital causes or ureteral incidence of bacteriuria also increases in men with
abnormalities, the bacteria may reach the confusion, dementia, or bowel or bladder
kidneys and eventually destroy them incontinence.
URETHROVESICAL ANGLE AND URETHRAL BACTERIAL PROSTATITIS: common cause of
CLOSURE PRESSURE: altered w/ menopause recurrent UTI in older males
(increased infection in postmenopausal women) o Resection of prostate gland (management)
UROPATHOGENIC BACTERIA FACTORS THAT CONTRIBUTE TO UTI IN OLDER
ADULTS
BACTERIURIA: presence of bacteria in the urine.
a clean-catch midstream urine specimen is the Cognitive impairment
measure used to establish bacteriuria. Frequent use of antimicrobial agents
High incidence of multiple chronic medical
ROUTES OF INFECTION conditions
Immune compromised
3 ways:
Immobility and incomplete emptying of bladder
o Transurethral route (ascending infection)
Low fluid intake and excessive fluid loss
o Bloodstream (hematogenous spread)
o Fistula from the intestine (direct extension) Obstructed flow of urine (e.g., urethral strictures,
TRANSURETHRAL: most common route of neoplasms, clogged
infection indwelling catheter)
BSN 3A | PBL GROUP 1 33
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
Poor hygiene practices CELLULAR STUDIES
Escherichia coli: most common seen in OLDER Pyuria: WBC in urine
patients in COMMUNITY or HOSPITAL o Seen with renal calculi, interstitial nephritis
Proteus, Klebsiella, Pseudomonas, or & renal tuberculosis
Staphylococcus: seen in px w/ INDWELLING
CATHETERS OTHER STUDIES
Enterococcus: seen in px who are
PREVIOUSLY TREATED w/ ANTIBIOTICS multiple-test dipstick often includes testing for
WBCs, known as the leukocyte esterase test, and
nitrite testing
SIGNS & SYMPTOMS IN POSTMENOPAUSAL WOMEN & X-ray images, computed tomography (CT) scan,
OLDER ADULTS ultrasonography, and kidney scans are useful
diagnostic tools.
Malaise CT SCAN: detect pyelonephritis or abscesses
Nocturia ULTRASONOGRAPHY & KIDNEY SCANS:
Urinary incontinence detecting obstruction, abscesses, tumors, and cysts
Complain of foul-smelling urine
Burning, urgency, & fever MEDICAL MANAGEMENT
ONSET OF UTI: delirium & incontinence
DRUG CLASSES GENERIC MAJOR
ASSESSMENT AND DIAGNOSTIC FINDINGS NAME INDICATIONS
Anti-infective, Nitrofurantoin UTI
Bacterial colony counts urinary tract Cephalexin Genitourinary
Cellular studies Bactericidal Infection
Urine culture Cephalosporin Cefadroxil UTI
UNCOMPLICATED UTI: strain of bacteria Fluoroquinolone Ciprofloxacin UTI
determines antibiotic of choice Ofloxacin Pyelonephritis
Norfloxacin
URINE CULTURES Gatifloxacin
Fluoroquinolone levofloxacin Uncomplicated
useful for documenting a UTI and identifying the UTI
specific organism present. Penicillin ampicillin UTI—not
INFECTION: colony count >100,000 CFU/ml amoxicillin commonly used
alone due to
GROUPS OF PATIENTS SHOULD HAVE URINE
Escherichia coli
CULTURES OBTAINED WHEN BACTERIURIA IS resistance
PRESENT Pyelonephritis
o All children UTI—not
o All men (because of the likelihood of commonly used
structural or functional alone due to E.
o abnormalities) coli resistance
o Patients who have been recently Trimethoprim– Co-trimoxazole UTI
hospitalized or who live in longterm care sulfamethoxazole Pyelonephritis
facilities combination
o Patients who have undergone recent Urinary analgesic Phenazopyridine For relief of
instrumentation (including catheterization) agen burning, pain,
of the urinary tract and other
o Patients with diabetes symptoms
o Patients with prolonged or persistent associated with
symptoms UTI
o Patients with three or more UTIs in the
previous year
o Women who are postmenopausal NURSING MANAGEMENT
o Women who are pregnant
o Women who are sexually active To relieve pain:
o Women who have new sexual partners o Antispasmodic agents: relieving bladder
o Women with a history of compromised irritability and pain
immune function or renal o Analgesic agents and the application of
o Problem heat to the perineum help relieve pain and
spasm
BSN 3A | PBL GROUP 1 34
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
o Encouraged to drink liberal amounts of Acute pyelonephritis and chronic pyelonephritis
fluids (water and cranberry juice are the are thought to be the most likely type, with interstitial
best choices) to promote renal blood flow nephritis (inflammation of the kidney) and kidney
and to flush the bacteria from the urinary abscesses also a potential cause.
tract Upper UTIs are a common cause of urosepsis.
o Coffee, tea, citrus, spices, colas, alcohol Pyelonephritis is a bacterial infection of the renal
should be avoided pelvis, tubules, and interstitial tissue of one or both
o Void every 2 to 3 hours kidneys. Causes involve either the upward spread of
PREVENTING RECURRENT UTI bacteria from the bladder or spread from systemic
sources reaching the kidney via the bloodstream.
HYGIENE
o Shower rather than bathe in the tub ACUTE PYELONEPHRITIS
because bacteria in the bathwater may
usually leads to enlargement of the kidneys with
enter the urethra.
interstitial infiltrations of inflammatory cells.
o Clean the perineum and urethral meatus
from front to back after each bowel Abscesses may be noted on or within the renal
movement. This will help reduce capsule and at the corticomedullary junction.
concentrations of pathogens at the urethral Eventually, atrophy and destruction of tubules and
opening and, in women, the vaginal the glomeruli may result.
opening.
CLINICAL MANIFESTATIONS
FLUID INTAKE
o Drink liberal amounts of fluids daily to flush – Chills
out bacteria. It may be helpful to include at – Fever
least one glass of cranberry juice per day. – Leukocytosis
o Avoid coffee, tea, colas, alcohol, and other – Bacteriuria
fluids that are urinary tract irritants. – Pyuria
VOIDING HABITS – Low back pain
o Void every 2 to 3 hours during the day, – Flank pain
and completely empty the bladder. This – Nausea and vomiting
prevents overdistention of the bladder and – Headache
compromised blood supply to the bladder – Malaise
wall. Both predispose the patient to urinary – Painful urination
tract infection. Precautions expressly for – Lower urinary tract involvement, such as urgency
women include voiding immediately after and frequency, are common.
penile-vaginal intercourse.
INTERVENTIONS ASSESSMENT AND DIAGNOSTIC FINDINGS
o Take medication exactly as prescribed.
Special timing of administration may be – Ultrasound study or a CT scan may be performed
required. to locate an obstruction in the urinary tract.
o Keep in mind that if bacteria continue to – An IV pyelogram may be indicated if functional and
appear in the urine, long-term antimicrobial structural renal abnormalities are suspected.
therapy may be required to prevent – Radionuclide imaging with gallium citrate and
colonization of the periurethral area and indium-111 (111In)–labeled WBCs may be useful to
recurrence of infection. identify sites of infection that may not be visualized
o For recurrent infection, consider daily on CT scan or ultrasound.
consumption of cranberry juice or – Urine culture and sensitivity tests are performed
capsules. to determine the causative organism so that
o If prescribed, test urine for presence of appropriate antimicrobial agents can be prescribed.
bacteria following manufacturer’s and
health care provider’s instructions. MEDICAL MANAGEMENT
o Notify the primary provider if fever occurs
or if signs and symptoms persist. – Patients with acute uncomplicated pyelonephritis are
o Consult the primary provider regularly for most often treated on an outpatient basis if they are
follow-up. not exhibiting acute symptoms of sepsis,
dehydration, nausea, or vomiting.
UPPER URINARY TRACT INFECTIONS – For outpatients, a 2-week course of antibiotic agents
is recommended because renal parenchymal
Upper UTIs are much less common than those in the
disease is more difficult to eradicate than mucosal
lower urinary tract.
bladder infections. Commonly prescribed agents
BSN 3A | PBL GROUP 1 35
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
include many of the same medications prescribed for – Long-term use of prophylactic antimicrobial therapy
the treatment of UTIs. may help limit recurrence of infections and kidney
– Following acute pyelonephritis treatment, the patient scarring.
may develop a chronic or recurring symptomless – Impaired kidney function alters the excretion of
infection persisting for months or years. After the antimicrobial agents and necessitates careful
initial antibiotic regimen, the patient may need monitoring of kidney function, especially if the
antibiotic therapy for up to 6 weeks if a relapse medications are potentially toxic to the kidneys.
occurs.
– A follow-up urine culture is obtained 2 weeks after NURSING MANAGEMENT
completion of antibiotic therapy to document clearing
– The patient may require hospitalization or may be
of the infection.
treated as an outpatient.
– Hydration with oral or parenteral fluids is essential in
– When the patient requires hospitalization, fluid intake
all patients with UTIs when there is adequate kidney
and output are carefully measured and recorded.
function. Hydration helps facilitate “flushing” of the
Unless contraindicated, 3 to 4 L of fluids per day is
urinary tract and reduces pain and discomfort.
encouraged to dilute the urine.
– Decrease burning on urination
CHRONIC PYELONEPHRITIS – Prevent dehydration
– The nurse assesses the patient’s temperature every
— Repeated bouts of acute pyelonephritis may lead to 4 hours and administers antipyretic and antibiotic
chronic pyelonephritis. agents as prescribed.
— When pyelonephritis becomes chronic, the kidneys
become scarred, contracted, and nonfunctioning.
— Chronic pyelonephritis is a cause of chronic kidney ADULT VOIDING DYSFUNCTION
disease that can result in the need for renal
replacement therapy (RRT) such as transplantation
or dialysis.
URINARY INCONTINENCE
CLINICAL MANIFESTATIONS
sudden, intense urge to urinate followed by an
– No symptoms of infection unless an acute involuntary loss of urine
exacerbation occurs. unintentional passing of urine
– Fatigue loss of bladder control
– Headache
– Poor appetite TYPES/SYMPTOMS OF URINARY INCONTINENCE
– Polyuria
– Excessive thirst 1. Stress Incontinence: urine leaks out at times when
– Weight loss. bladder is under pressure (e.g. coughing or laughing)
– Persistent and recurring infection may produce 2. Urge Incontinence: urine leaks as an intense or
progressive scarring of the kidney, resulting in sudden urge to pee
chronic kidney disease. 3. Overflow Incontinence (chronic urinary
retention): unable to fully empty the bladder. There
ASSESSMENT AND DIAGNOSTIC FINDINGS is an obstruction or blockage in the bladder.
4. Total Incontinence: bladder cannot pass urine at all
– The extent of the disease is assessed by an IV
urogram. CAUSES OF URINARY INCONTINENCES
– Measurements of creatinine clearance, blood urea
nitrogen, and creatinine levels. Pregnancy or vaginal birth
Obesity
COMPLICATIONS
Family history
– End-stage kidney disease (from progressive loss of Increasing age
nephrons secondary to chronic inflammation and Urinary tract infection (UTI)
scarring). Constipation
– Hypertension Enlarged prostate
– Formation of renal calculi (from chronic infection with Neurological disorders (can interfere with nerve
urea-splitting organisms). signals involved in bladder control)
MEDICAL MANAGEMENT
– Bacteria, if detected in the urine, are eradicated if
possible.
BSN 3A | PBL GROUP 1 36
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
TREATMENT What was the time of the last voiding, and how much
urine was voided?
NON-SURGICAL Is the patient voiding small amounts of urine
frequently?
1. Lifestyle changes (losing weight, cutting down on
Is the patient dribbling urine?
caffeine or alcohol)
Does the patient complain of pain or discomfort in the
2. Pelvic floor exercises (strengthening pelvic floor
lower abdomen? (Discomfort may be relatively mild
muscles by squeezing them)
if the bladder distends slowly.)
3. Bladder training (learning ways to wait longer
Is the pelvic area rounded and swollen (could
between needing to urinate and passing urine)
indicate urine retention and a distended bladder)?
SURGICAL Does percussion of the suprapubic region elicit
dullness (possibly indicating urine retention and a
1. Sling procedure - used to reduce pressure on the distended bladder)?
bladder or strengthen the muscles that control Are other indicators of urinary retention present, such
urination as restlessness and agitation?
2. Enlarging the bladder or implanting a device that Does a postvoid bladder ultrasound test reveal
stimulates the nerve that controls the detrusor residual urine?
muscles. The patient may verbalize an awareness of bladder
fullness and a sensation of incomplete bladder
PREVENTION
emptying.
Maintain a healthy weight Signs and symptoms of UTI (hematuria, urgency,
Practice pelvic floor exercises frequency, and nocturia) may be present.
Avoid bladder irritants (such as caffeine, alcohol, A series of urodynamic studies may be performed to
acidic foods). identify the type of bladder dysfunction and to aid in
Eat more fiber, which can prevent constipation determining appropriate treatment.
A voiding diary can be used to provide a written
URINARY RETENTION record of the amount of urine voided and the
frequency of voiding.
Urinary retention is the inability to empty the bladder
completely during attempts to void. Postvoid residual urine may be assessed by using
Chronic urine retention often leads to overflow either straight catheterization or an ultrasound
incontinence bladder scanner is considered diagnostic of urinary
In a healthy adult younger than 60 years, complete retention.
bladder emptying should occur with each voiding, Normally, residual urine amounts to no more than 50
with no residual. mL in the middle-aged adult and less than 50 to 100
In adults older than 60 years, 50 to 100 mL of mL in the older adult
residual urine may remain after each voiding
because of the decreased contractility of the detrusor COMPLICATIONS
muscle.
Urinary retention can occur postoperatively in any The retention of urine can lead to chronic infections
patient, particularly if the surgery affected the that, if unresolved, predispose the patient to renal
perineal or anal regions and resulted in reflex spasm calculi (urolithiasis or nephrolithiasis), pyelonephritis,
of the sphincters. sepsis, or hydronephrosis.
General anesthesia reduces bladder muscle Urine leakage can lead to perineal skin breakdown,
innervation and suppresses the urge to void, especially if regular hygiene measures are
impeding bladder emptying. neglected.
NURSING MANAGEMENT
PATHOPHYSIOLOGY Strategies are instituted to prevent overdistention of
the bladder and to treat infection or correct
Urinary retention may result from diabetes, prostatic obstruction.
enlargement, urethral pathology (infection, tumor, The nurse explains to the patient why normal voiding
calculus), trauma (pelvic injuries), pregnancy, or is not occurring and monitors urine output closely.
neurologic disorders (e.g., stroke, spinal cord injury,
The nurse also provides reassurance about the
multiple sclerosis, Parkinson’s disease).
temporary nature of retention and successful
Some medications cause urinary retention either by management strategies.
inhibiting bladder contractility or by increasing Promoting Urinary Elimination [Nursing measures to
bladder outlet resistance encourage normal voiding patterns include providing
privacy, ensuring an environment and body position
ASSESSMENT AND DIAGNOSTIC FINDINGS conducive to voiding, and assisting the patient with
BSN 3A | PBL GROUP 1 37
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
the use of the bathroom or bedside commode, rather The two types of neurogenic bladder are spastic (or
than a bedpan, to provide a more natural setting for reflex) bladder and flaccid bladder.
voiding.] Spastic bladder is the more common type and is
If his condition allows, the male patient may stand caused by any spinal cord lesion above the voiding
beside the bed to use the urinal; most men find this reflex arc (upper motor neuron lesion). The result is
position more comfortable and natural. a loss of conscious sensation and cerebral motor
applying warmth to relax the sphincters (e.g., sitz control.
baths, warm compresses to the perineum, showers), A spastic bladder empties on reflex, with minimal or
giving the patient hot caffeine-free beverage and no controlling influence to regulate its activity.
offering encouragement and reassurance. Flaccid bladder is caused by a lower motor neuron
Simple trigger techniques, such as turning on the lesion, commonly resulting from trauma. This form of
water faucet while the patient is trying to void, may neurogenic bladder is also increasingly being
also be used. Other examples of trigger techniques recognized in patients with diabetes.
are stroking the abdomen or inner thighs, tapping The bladder continues to fill and becomes greatly
above the pubic area, and dipping the patient’s distended, and overflow incontinence occurs.
hands in warm water. The bladder muscle does not contract forcefully at
After surgery or childbirth, prescribed analgesic any time. Because sensory loss may accompany a
agents should be given because pain in the perineal flaccid bladder, the patient feels no discomfort.
area can make voiding difficult.
When the patient cannot void, bladder scanning is ASSESSMENT AND DIAGNOSTIC FINDINGS
used to assess for distention, then straight Evaluation for neurogenic bladder involves
catheterization (as prescribed) is used to prevent measurement of fluid intake, urine output, and
overdistention of the bladder residual urine volume; urinalysis; and assessment of
In the case of prostatic obstruction, attempts at sensory awareness of bladder fullness and degree of
catheterization (by the urologist) may not be motor control. Comprehensive urodynamic studies
successful, requiring insertion of a suprapubic are also performed.
catheter (catheter inserted through a small
abdominal incision into the bladder) COMPLICATIONS
After urinary drainage is restored, bladder retraining
is initiated for the patient who cannot void The most common complication of neurogenic
spontaneously. bladder is infection resulting from urinary stasis and
catheterization.
Other complications include renal calculi, impaired
Promoting Home, Community-Based, and skin integrity, and urinary incontinence or retention.
Transitional Care
modifications to the home environment can provide MEDICAL MANAGEMENT
simple and effective ways to assist in treating urinary Several long-term objectives appropriate for all types
incontinence and retention. For example, the patient of neurogenic bladders include preventing
may need to remove obstacles, such as throw rugs overdistention of the bladder, emptying the bladder
or other objects, to provide easy, safe access to the regularly and completely, maintaining urine sterility
bathroom. with no stone formation, and maintaining adequate
Other modifications that the nurse may recommend bladder capacity with no reflux.
include installing support bars in the bathroom; Specific interventions include continuous,
placing a bedside commode, bedpan, or urinal within intermittent, or self-catheterization (discussed later in
easy reach; leaving lights on in the bedroom and this chapter); the use of an external condomtype
bathroom; and wearing clothing that is easy to catheter; a diet low in calcium (to prevent calculi);
remove quickly. and encouragement of mobility and ambulation.
A liberal fluid intake is encouraged to reduce the
NEUROGENIC BLADDER
urinary bacterial count, reduce stasis, decrease the
Neurogenic bladder is a dysfunction that results from
concentration of calcium in the urine, and minimize
a disorder or dysfunction of the nervous system and
the precipitation of urinary crystals and subsequent
leads to urinary incontinence.
stone formation.
It may be caused by spinal cord injury, spinal tumor,
A bladder retraining program may be effective in
herniated vertebral disc, multiple sclerosis,
treating a spastic bladder or urine retention.
congenital disorders (spina bifida or
myelomeningocele), infection, or complications of The use of a timed, or habit, voiding schedule may
diabetes be established.
To further enhance emptying of a flaccid bladder, the
PATHOPHYSIOLOGY patient may be taught to “double void.” After each
BSN 3A | PBL GROUP 1 38
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
voiding, the patient is instructed to remain on the or tape, and the area around the catheter is covered
toilet, relax for 1 to 2 minutes, and then attempt to with a sterile dressing.
void again in an effort to further empty the bladder The catheter is connected to a sterile closed
drainage system, and the tubing is secured to
PHARMACOLOGIC THERAPY prevent tension on the catheter. This may be a
temporary measure to divert the flow of urine from
Parasympathomimetic medications, such as
the urethra when the urethral route is impassable
bethanechol, may help to increase the contraction of
(because of injuries, strictures, prostatic obstruction),
the detrusor muscle.
after gynecologic or other abdominal surgery when
SURGICAL MANAGEMENT bladder dysfunction is likely to occur, and
occasionally after pelvic fractures.
Surgery may be carried out to correct bladder neck A permanent indwelling suprapubic catheter may be
contractures or vesicoureteral reflux, or to perform a needed in the patient who is incontinent following a
urinary diversion procedure. spinal cord injury
Suprapubic bladder drainage may be maintained
URINARY CATHETERS continuously for several weeks.
When the patient’s ability to void is to be tested, the
When urine cannot be eliminated naturally and must catheter is clamped for 4 hours, during which time
be drained artificially, catheters may be inserted the patient attempts to void.
directly into the bladder, the ureter, or the renal pelvis
After the patient voids, the catheter is unclamped,
Catheterization is performed to achieve the following: and the residual urine is measured. If the amount of
residual urine is less than 100 mL on two separate
Assist with postoperative drainage in urologic and occasions (morning and evening), the catheter is
other surgeries usually removed.
Provide a means to monitor accurate urine output in if the patient complains of pain or discomfort, the
patients who are critically ill suprapubic catheter is usually left in place until the
Promote urinary drainage in patients with neurogenic patient can void successfully
bladder dysfunction, urine retention, or at end-of-life Patients can usually void sooner after surgery than
care those with urethral catheters, and they may be more
Prevent urinary leakage in patients with stage III to comfortable.
IV pressure injuries The catheter allows greater mobility, permits
Relieve urinary tract obstruction measurement of residual urine without urethral
instrumentation, and presents less risk of bladder
NOTE: An indwelling urinary catheter should be placed only if infection.
necessary because catheterization commonly leads to The suprapubic catheter is removed when it is no
CAUTI. longer required, and a sterile dressing is placed over
the site.
INDWELLING CATHETERS
The patient requires liberal amounts of fluid to
Use strict aseptic technique during insertion of the prevent encrustation around the catheter.
smallest catheter possible Other potential problems include the formation of
Secure the catheter to prevent movement bladder stones, acute and chronic infections, and
Frequently inspect urine color, odor, and consistency problems collecting urine.
Perform daily perineal care with soap and water A wound-ostomy continence (WOC) nurse may be
Maintain a closed system consulted to assist the patient and family in selecting
the most suitable urine collection system and to
Follow the manufacturer’s instructions when using
educate them about its use and care.
the catheter port to obtain urine specimens
Discontinue use as soon as feasible
NURSING MANAGEMENT
Assessing the Patient and the System: Patients at
high risk for CAUTI need to be identified and
SUPRAPUBIC CATHETERS monitored carefully.
They are observed for signs and symptoms of
Suprapubic catheterization allows bladder drainage
CAUTI: cloudy malodorous urine, hematuria, fever,
by inserting a catheter or tube into the bladder
chills, anorexia, and malaise. Any drainage and
through a suprapubic (above the pubis) incision or
excoriation in the area around the urethral orifice is
puncture
noted. Urine cultures provide the most accurate
The catheter or suprapubic drainage tube is then
means of assessing a patient for infection.
threaded into the bladder and secured with sutures
PREVENTING INFECTION
BSN 3A | PBL GROUP 1 39
NCM112 LECTURE
MEDICAL-SURGICAL NURSING
FLUID DISTRUBANCES, ELECTROLYTE IMBALANCES, RENAL AND KIDNEY DISORDERS
RETRAINING THE BLADDER WHEN AN INDWELLING,
Certain principles of care are essential to prevent
infection in patients with a closed urinary drainage urinary catheter is in place, the detrusor muscle
system does not actively contract the bladder wall to
Avoid contamination of the drainage spout. A stimulate emptying because urine is continuously
receptacle in which to empty the bag is provided for draining from the bladder. As a result, the detrusor
each patient. Avoid routine catheter changes. may not immediately respond to bladder filling
The catheter is changed only to correct problems when the catheter is removed, resulting in either
such as leakage, blockage, or encrustations. Avoid urine retention or urinary incontinence. This
unnecessary handling or manipulation of the condition, known as postcatheterization detrusor
catheter by the patient or staff. instability, can be managed with bladder retraining
Carry out hand hygiene before and after handling Immediately after the indwelling catheter is
the catheter, tubing, or drainage bag. removed, the patient is placed on a timed voiding
Ensure a free flow of urine to prevent infection. schedule, usually every 2 to 3 hours.
Improper drainage occurs when the tubing is At the given time interval, the patient is instructed
kinked or twisted, allowing pools of urine to collect to void. The bladder is then scanned using a
in the tubing loops. portable ultrasonic bladder scanner, and if the
Evaluate the benefit of placing an indwelling urinary bladder has not emptied completely, straight
catheter versus the risk of the patient developing a catheterization may be performed
catheter-associated urinary tract infection (CAUTI). After a few days, as the nerve endings in the
If the collection bag must be raised above the level bladder wall become resensitized to the bladder
of the patient’s bladder, clamp the drainage tube. filling and emptying, bladder function usually
This prevents backflow of contaminated urine into returns to normal. If the patient has had an
the patient’s bladder from the bag. indwelling catheter in place for an extended period
Monitor the patient’s voiding when the catheter is (e.g., greater than 1 month), bladder retraining will
removed. The patient must void within 8 hours; if take longer; in some cases, function may never
unable to void, the patient may require return to normal, and long-term intermittent
catheterization with a straight catheter. catheterization may become necessary.
Never disconnect the tubing to obtain urine ASSISTING WITH INTERMITTENT SELF-
samples, to irrigate the catheter, or to ambulate or CATHETERIZATION.
transport the patient.
Never irrigate the catheter routinely. If the patient is Intermittent self-catheterization provides periodic
prone to obstruction from clots or large amounts of drainage of urine from the bladder.
sediment, use a three-way system with continuous By promoting drainage and eliminating excessive
irrigation. Never leave the catheter in place longer residual urine, intermittent catheterization protects
than is necessary to decrease the risk of CAUTI. the kidneys, reduces the incidence of UTIs, and
Obtain a urine specimen for culture at the first sign improves continence.
of infection. It is the treatment of choice in some patients with
To prevent contamination of the closed system, spinal cord injury and other neurologic disorders,
never disconnect the tubing. The drainage bag such as multiple sclerosis, when the ability to
must never touch the floor. empty the bladder is impaired. Self-catheterization
The bag and collecting tubing are changed if promotes independence, results in few
contamination occurs, if urine flow becomes complications, and enhances self-esteem and
obstructed, or if tubing junctions start to leak at the quality of life.
connections.
To reduce the risk of bacterial proliferation, empty
the collection bag at least every 8 hours through
the drainage spout—more frequently if there is a
large volume of urine.
Use scrupulous aseptic technique during insertion
of the catheter. Use a preassembled, sterile, closed
urinary drainage system of the smallest catheter
size possible to minimize trauma.
Wash the perineal area with soap and water at
least twice a day; avoid a to-and-fro motion of the
catheter.
Dry the area well, but avoid applying powder
because it may irritate the perineum
BSN 3A | PBL GROUP 1 40
You might also like
- Midterms - Electrolyte Renal DisordersDocument40 pagesMidterms - Electrolyte Renal DisordersRachelle DelantarNo ratings yet
- Dialysis Hypotension Is The Result of AnDocument4 pagesDialysis Hypotension Is The Result of AnCathy ManicadNo ratings yet
- Electrolit ImbalanceDocument80 pagesElectrolit ImbalanceCherry LilacNo ratings yet
- Chapter 34 - PolyuriaDocument6 pagesChapter 34 - Polyuriajonalyn.mejellanoNo ratings yet
- Eca - Fluids and ElectrolytesDocument15 pagesEca - Fluids and ElectrolytesMelchora Lea Castro SorianoNo ratings yet
- Anaphy Lec IDocument3 pagesAnaphy Lec IKrishna LibrodoNo ratings yet
- Diabetes Insipidus: Nursing Care PlansDocument6 pagesDiabetes Insipidus: Nursing Care PlansSewyel GarburiNo ratings yet
- Anaphy Lec IiiDocument4 pagesAnaphy Lec IiiKrishna LibrodoNo ratings yet
- 110-Dehydration and Disorders of Sodium BalanceDocument5 pages110-Dehydration and Disorders of Sodium BalancepelinNo ratings yet
- Activity On Pituitary Disorders and Diabetes MellitusDocument8 pagesActivity On Pituitary Disorders and Diabetes MellitusSherlyn Miranda GarcesNo ratings yet
- POLON, THAGREED BSN3D - KIDNEY DISORDERSDocument4 pagesPOLON, THAGREED BSN3D - KIDNEY DISORDERSThagreed PolonNo ratings yet
- NCM 112 Fluid and ElectrolytesDocument2 pagesNCM 112 Fluid and ElectrolytesAngeline NavarroNo ratings yet
- PolyuriaDocument5 pagesPolyuriaKrisha Marie BadilloNo ratings yet
- Diarrhea PDFDocument14 pagesDiarrhea PDFabegail eliahNo ratings yet
- Electrolyte ImbalanceDocument1 pageElectrolyte ImbalanceJulia HermoginoNo ratings yet
- Chronic Renal Failure: PathophysiologyDocument1 pageChronic Renal Failure: PathophysiologyCindy Mae Dela Torre100% (2)
- Fluid Therapy: Adesola Odunayo, DVM, MS, DACVECCDocument6 pagesFluid Therapy: Adesola Odunayo, DVM, MS, DACVECCSamantha Orozco PinedaNo ratings yet
- Problems in Nutrition and EliminationDocument4 pagesProblems in Nutrition and EliminationBianca BautistaNo ratings yet
- MS1 DRUG CARDSDocument22 pagesMS1 DRUG CARDStheresefrancotuNo ratings yet
- Lesson 45: Fluid and Electrolyte ImbalancesDocument6 pagesLesson 45: Fluid and Electrolyte ImbalancesDarren BalbasNo ratings yet
- NCM112 LP1 Transes - RosalesDocument4 pagesNCM112 LP1 Transes - RosalesChristine CalleyNo ratings yet
- Urinary Tract Disease in Cattle: Karin MuellerDocument12 pagesUrinary Tract Disease in Cattle: Karin MuellerDavid Julian ClavijoNo ratings yet
- Fluid and Elec ImbalancesDocument19 pagesFluid and Elec ImbalancesswethashakiNo ratings yet
- Fluid ImbalancesDocument43 pagesFluid ImbalancesHarold DiasanaNo ratings yet
- Case Study On AGNDocument28 pagesCase Study On AGNArchana SahuNo ratings yet
- Quiz No.1Document5 pagesQuiz No.1Charina AubreyNo ratings yet
- HyponatremiaDocument9 pagesHyponatremiaFebe ChristiantoNo ratings yet
- Hyponatremia: Consultant On CallDocument5 pagesHyponatremia: Consultant On CallDanilo JimenezNo ratings yet
- Med Surg Study GuideDocument24 pagesMed Surg Study Guidekylie100% (4)
- Chapter 5, CARE OF OLDERDocument7 pagesChapter 5, CARE OF OLDERGracian Vel AsocsomNo ratings yet
- 6 Acute Renal Failure Nursing Care Plans - NurseslabsDocument11 pages6 Acute Renal Failure Nursing Care Plans - NurseslabsloshieloeNo ratings yet
- Intravenous SolutionsDocument10 pagesIntravenous SolutionsariestgNo ratings yet
- ElectrolyteDocument4 pagesElectrolyteRon Vien'sNo ratings yet
- Siadh Diabetes Insipidus Acute Renal Failure Chronic Renal FailureDocument6 pagesSiadh Diabetes Insipidus Acute Renal Failure Chronic Renal FailureRanusha AnushaNo ratings yet
- Chronic Kidney DiseaseDocument4 pagesChronic Kidney DiseaseImnot YouNo ratings yet
- Guia Implementacion Iso45001Document3 pagesGuia Implementacion Iso45001karelly molinaNo ratings yet
- Geriatric SyndromeDocument49 pagesGeriatric Syndromewita prabawatiNo ratings yet
- Vincristine Drug StudyDocument4 pagesVincristine Drug StudyNiziu BearsNo ratings yet
- Renal SystemDocument20 pagesRenal SystemRahul DasNo ratings yet
- Hemodynamic DisordersDocument10 pagesHemodynamic DisordersUshuaia Ira Marie L. GallaronNo ratings yet
- Final - CholeraDocument12 pagesFinal - CholeraCassey Cureg100% (1)
- Disorders-Of-Sodium-Balance - CAMBRIDGEDocument10 pagesDisorders-Of-Sodium-Balance - CAMBRIDGEDenisa Carmen ColiofNo ratings yet
- Hyper Nat Remi ADocument7 pagesHyper Nat Remi ALorenzo MacoNo ratings yet
- Drug Study & NCPDocument12 pagesDrug Study & NCPStephanie Mae Amoylen OdchigueNo ratings yet
- ShockDocument7 pagesShockLisa WiramasNo ratings yet
- Urinary and Renal DisordersDocument45 pagesUrinary and Renal DisordersHarper EppsNo ratings yet
- Please Answer The Following Questions. 1. What Are The Fuctions of Water?Document4 pagesPlease Answer The Following Questions. 1. What Are The Fuctions of Water?Rikkimae NaagNo ratings yet
- Drug Name Mecahnism of Action Indication Side Effects Generic NameDocument2 pagesDrug Name Mecahnism of Action Indication Side Effects Generic NamehahahaNo ratings yet
- Drug Study: Therapeutic EffectsDocument4 pagesDrug Study: Therapeutic Effectsunkown userNo ratings yet
- Dapus 30Document25 pagesDapus 30Titi SulistiowatiNo ratings yet
- تمريض الاطفال نظري 7Document42 pagesتمريض الاطفال نظري 7jadarcNo ratings yet
- Electrolytes TableDocument4 pagesElectrolytes TableMeg NoriegaNo ratings yet
- Unit Four Ateration in Body FluidDocument26 pagesUnit Four Ateration in Body Fluid555556666667777777No ratings yet
- Primary: Congenital Disease 2. Finnish Nephrotic Syndrome (Inherited) 3. Nephrotic Syndrome Minimal Change (The Most Common Type)Document6 pagesPrimary: Congenital Disease 2. Finnish Nephrotic Syndrome (Inherited) 3. Nephrotic Syndrome Minimal Change (The Most Common Type)Cici Novelia ManurungNo ratings yet
- Primary: Congenital Disease 2. Finnish Nephrotic Syndrome (Inherited) 3. Nephrotic Syndrome Minimal Change (The Most Common Type)Document6 pagesPrimary: Congenital Disease 2. Finnish Nephrotic Syndrome (Inherited) 3. Nephrotic Syndrome Minimal Change (The Most Common Type)Cici Novelia ManurungNo ratings yet
- Hypernatremia NEJM 2000Document8 pagesHypernatremia NEJM 2000BenjamÍn Alejandro Ruiz ManzanoNo ratings yet
- Diabetes Insipidu1Document11 pagesDiabetes Insipidu1Ham SotheaNo ratings yet
- Liver Cirrhosis Lesson Plan 2Document16 pagesLiver Cirrhosis Lesson Plan 2SuchitaNo ratings yet
- Mid3 - Methodology - Tools and InstrumentsDocument15 pagesMid3 - Methodology - Tools and InstrumentsSteph CaronanNo ratings yet
- Poyos FINALS 1 OutlineDocument15 pagesPoyos FINALS 1 OutlineSteph CaronanNo ratings yet
- Mental Health Status and Coping Mechanism Among College Students Basis for a Proposed Plan of Action FINAL PAPER EDITEDDocument166 pagesMental Health Status and Coping Mechanism Among College Students Basis for a Proposed Plan of Action FINAL PAPER EDITEDSteph CaronanNo ratings yet
- NCM 109 Finals Quiz 1Document5 pagesNCM 109 Finals Quiz 1Steph CaronanNo ratings yet
- Lia - Finals Quiz 1 NotesDocument18 pagesLia - Finals Quiz 1 NotesSteph CaronanNo ratings yet
- Finals Notes NiDocument11 pagesFinals Notes NiSteph CaronanNo ratings yet
- Answers RationaleDocument14 pagesAnswers RationaleSteph CaronanNo ratings yet
- NCM 112 Mock ExamDocument27 pagesNCM 112 Mock ExamSteph CaronanNo ratings yet
- MS Finals Reference For ReviewDocument5 pagesMS Finals Reference For ReviewSteph CaronanNo ratings yet
- Practice TestDocument15 pagesPractice TestSteph CaronanNo ratings yet
- PCRTDocument10 pagesPCRTSteph CaronanNo ratings yet
- Principle of Moral DiscernmentDocument14 pagesPrinciple of Moral DiscernmentSteph CaronanNo ratings yet
- The ICN Code of Ethics For NursesDocument19 pagesThe ICN Code of Ethics For NursesSteph CaronanNo ratings yet
- QUIZ 1 and 2Document12 pagesQUIZ 1 and 2Steph CaronanNo ratings yet
- Decision Making ProcessDocument16 pagesDecision Making ProcessSteph CaronanNo ratings yet
- World-Lit PoetryDocument6 pagesWorld-Lit PoetrySteph CaronanNo ratings yet
- Principle of Well-Formed ConscienceDocument14 pagesPrinciple of Well-Formed ConscienceSteph CaronanNo ratings yet
- NCM 102 Health EducDocument20 pagesNCM 102 Health EducSteph CaronanNo ratings yet
- Meaning and Service Value of Medical CareDocument15 pagesMeaning and Service Value of Medical CareSteph CaronanNo ratings yet
- Bioethics FINALSDocument10 pagesBioethics FINALSSteph CaronanNo ratings yet
- PDEVDocument7 pagesPDEVSteph CaronanNo ratings yet
- NCM110 Nursing Informatics FinalsDocument7 pagesNCM110 Nursing Informatics FinalsSteph CaronanNo ratings yet
- Sample AparmomDocument9 pagesSample AparmomSteph CaronanNo ratings yet
- Code 802Document8 pagesCode 802Steph CaronanNo ratings yet
- Risk ManagementDocument13 pagesRisk ManagementSteph CaronanNo ratings yet
- Diabetic NephropathyDocument62 pagesDiabetic Nephropathydevyani meshram100% (1)
- Dissertation On Blood Pressure and HypertensionDocument60 pagesDissertation On Blood Pressure and HypertensionHemant Kumar AhirwarNo ratings yet
- Irm1501 02 Mark090100Document9 pagesIrm1501 02 Mark090100Gideon MatthewsNo ratings yet
- Urinary Tract ReviewDocument12 pagesUrinary Tract ReviewJessica MooreNo ratings yet
- PathoPhysiology of Renal Failure (Overview)Document7 pagesPathoPhysiology of Renal Failure (Overview)Tiger Knee100% (3)
- Nclex Q'S Aki and CKDDocument18 pagesNclex Q'S Aki and CKDDENNROSE DECLARONo ratings yet
- Synopsis - Chronic-kidney-disease-prediction-usingMLDocument7 pagesSynopsis - Chronic-kidney-disease-prediction-usingMLKamran AnasNo ratings yet
- Therapeutic Diet Manual: DIRECTIVE #4311Document27 pagesTherapeutic Diet Manual: DIRECTIVE #4311DuNo ratings yet
- Thyroid Hormone Profile in Chronic Kidney DiseaseDocument6 pagesThyroid Hormone Profile in Chronic Kidney DiseaserefaNo ratings yet
- Reg Rujukan Eksternal 26 Juni-25 Juli 2021Document54 pagesReg Rujukan Eksternal 26 Juni-25 Juli 2021RuciNo ratings yet
- Cabrera Jorene AbstractDocument6 pagesCabrera Jorene Abstractjade cabreraNo ratings yet
- Renal Case StudyDocument4 pagesRenal Case Studydsaitta108No ratings yet
- Electrolyte Replacement - Critical Care ICU/PCU (30400716)Document7 pagesElectrolyte Replacement - Critical Care ICU/PCU (30400716)Lubna AliNo ratings yet
- CIRSG Manual EDocument30 pagesCIRSG Manual EBryanJermyHendrikNo ratings yet
- Group Health Insurance: Customercare@magma-Hdi - Co.inDocument34 pagesGroup Health Insurance: Customercare@magma-Hdi - Co.inKumar AbhiNo ratings yet
- Chronic Renal FailureDocument54 pagesChronic Renal Failuresanjivdas100% (3)
- Prof TestDocument13 pagesProf TestOlive NNo ratings yet
- Acute Renal FailureDocument2 pagesAcute Renal FailureKim GarciaNo ratings yet
- Journal Homepage: - : IntroductionDocument8 pagesJournal Homepage: - : IntroductionIJAR JOURNALNo ratings yet
- Course Description: 3. Communities (Community Service)Document35 pagesCourse Description: 3. Communities (Community Service)April Mae Magos LabradorNo ratings yet
- Side Effects of VancomycinDocument20 pagesSide Effects of VancomycinSiti Hajar Mohd ZaidiNo ratings yet
- Preoperative Care of Patients With Kidney DiseaseDocument13 pagesPreoperative Care of Patients With Kidney Disease84ghmynprvNo ratings yet
- MCN Oral RevalidaDocument11 pagesMCN Oral RevalidaADOLF FRUELAN HIDALGONo ratings yet
- Drug Use in Special Conditions - CLD and CKDDocument93 pagesDrug Use in Special Conditions - CLD and CKDadamu mohammadNo ratings yet
- Case PresentationDocument39 pagesCase PresentationAnni BarbaNo ratings yet
- Case Study Introduction CKDDocument6 pagesCase Study Introduction CKDRhajibNo ratings yet
- Managing and Treating Chronic Kidney Disease: ReviewDocument4 pagesManaging and Treating Chronic Kidney Disease: ReviewSheena CabrilesNo ratings yet
- HemodialysisDocument24 pagesHemodialysisLaurince Christian Faith Pineda100% (2)
- sglt2 Inhibitor - PDF 27Document7 pagessglt2 Inhibitor - PDF 27JaganNo ratings yet
- HEMODIALYSIS FinalDocument8 pagesHEMODIALYSIS Finalvineeta.ashoknagarNo ratings yet