Professional Documents
Culture Documents
Nur 092
Nur 092
Uploaded by
Lee NP0 ratings0% found this document useful (0 votes)
3 views5 pagesYEs
Original Title
NUR-092
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentYEs
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
3 views5 pagesNur 092
Nur 092
Uploaded by
Lee NPYEs
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 5
Cleaning ➢ Reduces incidence of muscle strain
- Removal of visible dirt Gravity and Friction – The greater the
- Reducing levels of harmful surface area the greater the friction
microorganisms
➢ Gravity – invisible force that
Risk-Based Environmental Cleaning pulls objects toward each other
Frequency Principles ➢ Friction – is a force that occurs in
a direction to oppose movement
- Probability of Contamination
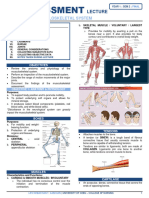
- Vulnerability of Patients to Infection Skeletal System
- Potential for Exposure to pathogens
➢ Provides attachments for muscles and
Cleaner to Dirtier Cleaning Strategy – ligaments
prevent the further spreading of dirt and ➢ Supporting framework as it allows
microorganisms movement of the body
o Ligaments – white, shiny,
1. Shared equipment and common
flexible bands of tissue that
surfaces
bind joints together, connect
2. Items touched during patient care
bones and cartilages, and aid
3. Patients and direct contact items
joint flexibility and support
o Tendons – are white,
➢ Techniques
glistening, fibrous bands of
o Terminal cleaning (low touch
tissue that connect muscle to
vs b4 high touch)
bone and are strong, flexible
o Patient zone b4 toilets
and inelastic
o Top to bottom (prevent dirt
o Cartilage – non-vascular,
and microorganisms from
supportive connective tissue
contaminating already
located chiefly in the joints
cleaned areas)
and thorax, trachea, larynx,
o Methodical/Systematic
nose and ear
Manner (avoids missing
areas) Nervous System – regulates movement and
posture
Postural Abnormalities – congenital or
Damp Dusting – is the removal of dirt and
acquired postural abnormalities affect the
bacteria from hard, flat surfaces, with a damp
efficiency of the musculoskeletal system and
cloth or sponge
body alignment, balance, and appearance.
➢ Low dusting – easily reached by
1. Torticollis – inclining head to
standing; done everyday
affected side
➢ High dusting – areas over windows,
2. Lordosis – exaggeration of anterior
pipes, wall and ceiling
convex curvature of lumbar spine
➢ Varnished – do not use soap
3. Kyphosis - increases convexity in
➢ Unvarnished – do not use mineral oil
curvature of thoracic spine
4. Scoliosis – lateral- S or C – shaped
spinal column with vertebral rotation
Body Mechanics – coordinated efforts of the 5. Congenital Hip Dysplasia – hip
musculoskeletal system and NS to maintain instability with limited adduction
balance, posture and body alignment during contractures
lifting, bending, moving and performing 6. Knock-knee (genu valgum) – legs
ADL’s; application of mechanical laws curved inward so knees come
Alignment and Balance together
7. Bowlegs (genu varum) – one or both
➢ Positioning of the joints, tendons, legs bent outward at knew; normal
ligaments, and muscles while until 2-3 years of age
standing, sitting, and lying 8. Clubfoot – 95% medial deviation and
➢ To keep the body aligned, the plantar flexion; 5% lateral deviation
individuals center of gravity should 9. Foot drop – inability to dorsiflex and
always be stable invert foot
10. Pigeon toes – internal rotation of ➢ Protect the acutely ill, infants, and
forefoot/entire foot; common in older adults from drafted by ensuring
infants that they are dressed adequately and
covered with a lightweight blanket
Muscle Abnormalities – injury and disease
➢ Always empty and rinse commodes,
lead to numerous alterations in
bedpans and urinals promptly
musculoskeletal function
➢ Room deodorizers help remove any
➢ Direct trauma to the musculoskeletal unpleasant odors but before using
– results in bruises, contusions, deodorizers, determine first if the
sprains and fractures patient is not allergic or sensitive to
➢ Damage to the CNS – results in the deodorizer
impaired body alignment, balance ➢ Ill patients seem to be more sensitive
and mobility to noises and lighting commonly
found in health care settings
Hand Washing ➢ Try to lower the noise level;
5 Moments for Hand Hygiene
especially when a patient is trying to
1. Before touching the patient
2. Before an aseptic task/procedure sleep
3. After body fluid exposure ➢ Explain the source of unfamiliar
4. After touching the patient noises such as an IV pump or pulse
5. After touching patient surrounding oximeter alarms
➢ Proper lighting provides safety and
Bed Making - Attempt to make patients comfort
room as comfortable as home. It needs to be
Room Equipment’s
safe and large enough to allow the patient and
visitors to move about freely. Removal of 1. Over-bed table
barriers along walkways reduces risk of falls. 2. Bedside stand
Control room temperature, ventilation, noise 3. Chairs
and doors. Keeping the room nest and orderly 4. Patient’s Bed - seriously ill patients
also contributes to the patient’s sense of well- often remain in bed for a long time.
being Because a bed is the piece of
equipment used most by a
➢ To provide patients comfort
hospitalized patient. It is designed for
➢ To provide a clean environment for
comfort, safety and adaptability for
the clients
changing positions. A typical hospital
➢ To provide a smooth, wrinkle free bed
bed has a firm mattress on a metal
foundation, thus minimizing sources
frame that you can raise and lower
of skin irritation
horizontally
➢ To conserve a client’s energy and
maintain current healthy status Types of Linens
➢ To prevent and avoid microorganism
1. Bottom Sheet – used to cover the bed
to come intact with the patients
after mattress cover
Maintaining Comfort 2. Rubber Sheet – used to protect the
bottom sheet from soothing due to
➢ What makes a comfortable
patient secretions. It is usually placed
environment depends on a patient’s
over the center of the bottom sheet
age, severity of illness and level of
3. Cotton Draw Sheet – a piece of cloth
normal daily activity. Depending on
spread over the rubber sheet and is
age and physical condition,
used to absorb moisture
maintaining room temp between 20
4. Top sheet – used to cover the patient
and 23 degrees Celsius (68 to 73.4
to provide warmth, made of thick
degrees Fahrenheit). Infants, older
cotton, thermal material
adults and the acutely ill often need a
5. Blanket – a large piece of cloth soft,
warmer room
wooden and is used for warmth as a
Points to Remember: bed cover
➢ An effective ventilation system keeps Instructions for Folding Linens
stale air and odor from lingering in a
room
➢ Bed Spread and Blanket – fold linen Patient Transferring and Positioning
lengthwise; wrong side out
Ankle-foot Orthotic (AFO) – device that
➢ Top Sheet – fold linen lengthwise;
helps maintain dorsiflexion
right side out and the wider hem
should always be on the head part Patient Transferring:
➢ Draw and Rubber Sheet - fold
crosswise at the center; wrong side 1. Trochanter Roll – prevents external
out rotation of the hips when patient is in
➢ Bottom Sheet – fold lengthwise; a supine position. Under buttocks
wrong side out counterclockwise
➢ Pillow Case – fold linen crosswise; 2. Trapeze Bar – is a triangular device
wrong side out that hangs down from a securely
fastened overhead bar that is attached
2 Types of Bed to the bed frame. Allows patient to
pull with the upper extremities.
1. Occupied Bed – made when the
patient is unable to or not permitted to Patient Positioning
get out of bed.
2. Unoccupied Bed – when there is no 1. Fowler’s Position – head of the bead
patient confined in bed, while the is elevated
patient is I the bathroom or waiting a. Low Fowler – 15-30 degrees
for a newly admitted patient arriving b. Semi Fowler – 30-45 degrees
from the ER c. Standard Fowler – 45-60
a. Open Bed – the top covers are degrees
folded back so the patient can d. High Fowler – 80-90
easily get back into bed degrees; best for eating
b. Closed Bed – the top sheet 2. Supine Position – for sleeping; after
blankets and bed spreads are operation (2 hours); on the back
drawn up to the head of the 3. Prone Position – face or chest down
mattress and under the pillow; 4. Sim’s Position – patient places
this is prepared before a new weight on the anterior ileum,
patient is admitted to the room humerus, and clavicle; used for rectal
c. Post-operative/ Surgical exam
Bed – Aka recovery 5. Side-lying Position – patient rest on
bed/anesthetic bed the side with the major portion of
bodyweight on the dependent hip and
Definition of Terms shoulder. For pressure ulcers, 30-
degree lateral is recommended.
➢ Bed Making – the technique of
6. Logrolling – for transferring the
preparing different types of bed,
patient from bed to stretcher and vice
making patients/clients comfortable
versa; for patient’s who have spinal
➢ Fan Folding – folding the edge of the
injury or recovering from neck, back,
sheet 6-8 inches outwards
or spinal surgery. Repositioning is
➢ Mitered Corner – anchoring the
done every 2 hours, without it patient
sheet on mattress
will develop ulcers
➢ Top Pleat – a fold made in the sheets
7. Orthopneic Position – client sits in
that allows a patient in bed move his
bed on a high fowler position; best for
feet
patients who have difficulty breathing
➢ Foot Drop – plantar flexion of the
since it allows for maximum lung
foot with permanent contracture of
expansion.
the calf muscle
8. Lithotomy Position – in supine, both
➢ Foot Board – used to support the
knees are flexed and placed close to
immobilized client’s foot in a normal
the hips, widely separated; used for
right angle to the legs to prevent
vaginal exanimation or labor
plantar flexion contractures
9. Knee Chest (Genupectoral)
➢ Intravenous Rods – usually made of
Position – patients kneel on the bed
metal, support intravenous (IV)
then leans forward with the hips in the
containers while fluid is being
air; used for procedure in the spine or
administered
rectal
10. Trendelenburg Position – pt is in development
supine, head of the bed is down (in of pressure
reverse the foot is down) and entire ulcers
body frame is tilted downwards. ➢ Smooth linen
11. Jackknife of Bozeman Position – out to remove
prone position, hip directly over the sources of
mechanical
break in the table
irritation
12. yung pang check ng hernia
➢ Remove rings
and bracelets
to not injure
Skin the patient’s
skin
➢ Functions as protection, secretion,
➢ Water is not
excretion, body temp regulation, and excessively
cutaneous sensation hot/cold
➢ Primary layers: epidermis and dermis. 3.Temp Regulation
Just beneath the skin is the ➢ Radiation ➢ Wala
subcutaneous tissue (Hypodermis) (electromagnetic
radiation),
Function/Description Implications for Care
evaporation
1.Protection (water vapor),
➢ Relatively ➢ Weakening conduction
impermeable occurs by (transfer), and
layer that scraping or convection (air)
prevents stripping its
4-5. Excretion and
entrance of surface
Secretion
microorganisms. ➢ Excessive
➢ Sweat promotes ➢ Perspiration
Relative dryness dryness causes
heat loss by and oil harbor
of surface of cracks and
evaporation. microorganism
skin inhibits breaks where
Sebum ➢ Bathing
bacterial growth. bacteria can
lubricates skin removes
Sebum removes enter
and hair excess body
bacteria from ➢ Constant
secretions; of
hair follicles exposure of
excessive it
skin to
causes dry skin
moisture
causes
softening, Epidermis
interrupting
dermal ➢ Outermost layer of the skin
integrity, ➢ Comprises of several thin layers of
promoting epithelial cells (protects the skin
ulcer and against water loss and injury and
bacterial prevent entry of disease providing
growth microorganisms)
➢ Keep bed linen
and clothing
dry
Bathing and Skin Care
➢ Misuse of
chemicals Hygiene – science that deals with the
causes preservation of health/science of health and
chemical its maintenance
irritation
2.Sensation Hygienic Care – promotes cleanliness,
➢ Skin contains ➢ Minimize provides for comfort and relaxation,
sensory organs friction to improves self-image and promotes healthy
for touch, pain, avoid loss of skin
heat, cold and stratum
pressure corneum,
which results
in
Early Morning Care (AM Care) ➢ To stimulate circulation to the skin
➢ To promote a sense of well-being
➢ Nursing personnel on the night shift
➢ To produce relaxation and comfort
provide basic hygiene to patients
➢ To prevent and eliminate unpleasant
getting ready for breakfast, scheduled
body odors
tests, or early morning surgery
➢ Offering a bedpan or urinal if the 2 General Baths
patient is not ambulatory (able to
1. Cleaning bath – provided as routine
walk around), washing the hands and
client care; main purpose is patient’s
face, helping with oral care
hygiene
Routine Morning Care (Complete AM o Complete Bed Bath
Care) ▪
o Partial Bed Bath
➢ After breakfast, offer bedpan/urinal;
o Sponge Bath
provide a full or partial bath or a
o Tub Bath
shower, including perineal care and
o Shower
oral, foot, nail, and hair care; give a
o Bag Bath (Travel Bath)
back rub; change gowns/pajamas; bed
o Chlorohexidine Gluconate
making is performed; and straighten
Bath (CHG Bath)
the patient’s bedside unit and room
2. Therapeutic Bath
Afternoon Care
➢ Hospitalized patients often undergo
exhausting diagnostic tests or
procedures in the morning. In
rehabilitation centers, patients
participate in physical therapy in the
morning. Afternoon hygiene care
includes washing the hands and face,
helping with oral care, offering a
bedpan or urinal, and straightening
the linen
Evening Care (PM Care)
➢ Before bedtime after personal
hygiene care that helps patients relax
and promotes sleep
➢ Changing solid linens, gowns, or
pajamas; helping patients wash the
face and hands; providing oral
hygiene; giving a back massage and
offering the bed bedpan or urinal
4 Types of Urinals and Bedpan
1. Fracture Bedpan
2. Bedpan
3. Female Urinal
4. Male Urinal
Bed bath – is given to provide cleanliness
and comfort who is unable to get out of bed
because of physical or mental limitations
Purpose:
➢ To remove transient microorganisms,
body secretions and excretions and
dead skin cells
You might also like
- (Guzman, Ruben) - The Swimming Drill Book - 2º Edition (2017) PDFDocument370 pages(Guzman, Ruben) - The Swimming Drill Book - 2º Edition (2017) PDFEdi Fa Mendoza Rincon100% (2)
- Open Reduction Internal Fixation PPT With Nursing ResponsibilitiesDocument13 pagesOpen Reduction Internal Fixation PPT With Nursing ResponsibilitiesMiciola Mitch Tanquiamco100% (2)
- Bath House RomanDocument3 pagesBath House Romanapi-263482758No ratings yet
- PLUMBING DESIGN AND ESTIMATE by Max Fajardo PDFDocument175 pagesPLUMBING DESIGN AND ESTIMATE by Max Fajardo PDFeugene eugenio0% (2)
- Nur 092Document5 pagesNur 092Lee NPNo ratings yet
- Nur092 Lab Sas 1 10 PDFDocument3 pagesNur092 Lab Sas 1 10 PDFmaureensolano63No ratings yet
- Musculoskeletal DisordersDocument8 pagesMusculoskeletal DisordersMode Devi Publising IncorporatedNo ratings yet
- The Musculoskeletal HandoutsDocument3 pagesThe Musculoskeletal Handoutsseigelystic100% (11)
- Funda MidtermsDocument18 pagesFunda Midtermsjomari macasaetNo ratings yet
- 1st ExamDocument3 pages1st Examj UNo ratings yet
- Fracture Dislocation LesionsDocument14 pagesFracture Dislocation LesionsReichelle Reine LisingNo ratings yet
- Fracture MegDocument3 pagesFracture MegJhonny pingolNo ratings yet
- Prelim Midterm Rle NotesDocument12 pagesPrelim Midterm Rle NotesDaniela Crystal AbucayanNo ratings yet
- Auditory SystemDocument2 pagesAuditory SystemLyron GuemoNo ratings yet
- Med Surg LLDocument220 pagesMed Surg LLIbrahim Ahmed OsmanNo ratings yet
- TractionDocument20 pagesTractionCharinelle MolinaNo ratings yet
- Lecture Physical ExaminationDocument84 pagesLecture Physical ExaminationAdamNo ratings yet
- Peri-Op 1,2&3Document12 pagesPeri-Op 1,2&3nhmae gcabNo ratings yet
- Open Reduction and Internal Fixation (ORIF)Document13 pagesOpen Reduction and Internal Fixation (ORIF)Miciola Mitch Tanquiamco67% (3)
- Congenital Talipes Equinovarus (CTEV) : Nur Farhanah Binti Ariffin BJPA2019-0016 HSIDocument31 pagesCongenital Talipes Equinovarus (CTEV) : Nur Farhanah Binti Ariffin BJPA2019-0016 HSIfarhanah ariffinNo ratings yet
- Bedah 2 Batch 3 2018Document87 pagesBedah 2 Batch 3 2018Meiza Ihsan FakhriNo ratings yet
- Skeletal and Skin TractionDocument38 pagesSkeletal and Skin TractionCORROS JASMIN MARIE100% (1)
- DegenerativeDiskDisease (HNP) IDocument2 pagesDegenerativeDiskDisease (HNP) Iapi-3822433No ratings yet
- Management of FractureDocument20 pagesManagement of FractureHitesh RohitNo ratings yet
- MSK Ncm106lecDocument50 pagesMSK Ncm106lecJASTINE JOY PEREZNo ratings yet
- Medical Equipments 1. Scalpel Handle: 4. Bandage Scissors: 7. DeaverDocument4 pagesMedical Equipments 1. Scalpel Handle: 4. Bandage Scissors: 7. DeaverPhoebe CosteloNo ratings yet
- The Musculoskeletal Examination: Colon H - WilsonDocument5 pagesThe Musculoskeletal Examination: Colon H - WilsonAbdullah Bin SaeedNo ratings yet
- 3.1 AmputationDocument4 pages3.1 AmputationDiana CalderonNo ratings yet
- NCP Klippel Trenaunay SyndromeDocument3 pagesNCP Klippel Trenaunay SyndromePaola Marie VenusNo ratings yet
- Surgical Instrumentation: Iii. Grasping and HoldingDocument37 pagesSurgical Instrumentation: Iii. Grasping and Holdingkaren carpioNo ratings yet
- Illizarov and Principle of Distraction OsteogenesisDocument7 pagesIllizarov and Principle of Distraction OsteogenesisThiru MuruganNo ratings yet
- Basic Surgery PerioDocument34 pagesBasic Surgery Perioade ismailNo ratings yet
- W2 - MEDSURG Guidelines For Nursing Interventions On Coma PatientsDocument6 pagesW2 - MEDSURG Guidelines For Nursing Interventions On Coma PatientsKyla L. Madjad100% (1)
- Health Reviewer (Q3)Document2 pagesHealth Reviewer (Q3)summer.pesaNo ratings yet
- Physical AssessmentDocument7 pagesPhysical AssessmentRodolph Sean FamasNo ratings yet
- Module 7 Techniques in Physical AssessmentDocument14 pagesModule 7 Techniques in Physical AssessmentCalvo AdrianNo ratings yet
- Groin Hernia Repair by Open SurgeryDocument1 pageGroin Hernia Repair by Open SurgeryAnnisa Fitri AnggrainiNo ratings yet
- The Tenosynovitis: Patient Has Wrist or HandDocument2 pagesThe Tenosynovitis: Patient Has Wrist or HandrobouNo ratings yet
- Management of Compromised Residual Ridge PDFDocument73 pagesManagement of Compromised Residual Ridge PDFmarwa100% (1)
- (H.a.) Chapter 14 - Musculoskeletal SystemDocument9 pages(H.a.) Chapter 14 - Musculoskeletal SystemLevi Sebastian T. CabiguinNo ratings yet
- Slide MANTAP BEDAH 2 PDFDocument203 pagesSlide MANTAP BEDAH 2 PDFIni DiaNo ratings yet
- 8 Tmu - JD - 044 PDFDocument4 pages8 Tmu - JD - 044 PDFLaras Dwi AyuningrumNo ratings yet
- Fact SheetDocument2 pagesFact Sheetapi-407402630No ratings yet
- Basic Consept of Assessment Back PageDocument13 pagesBasic Consept of Assessment Back PageZgama AbdulrahmanNo ratings yet
- Chapter 51. Nursing Care of The Child With A Musculoskeletal Disorder TermsDocument3 pagesChapter 51. Nursing Care of The Child With A Musculoskeletal Disorder TermsJœnríčk AzueloNo ratings yet
- Human TissueDocument6 pagesHuman TissueRence GuerraNo ratings yet
- VM1Document123 pagesVM1Mohamed Essmat100% (5)
- Ms. Elizabeth D. Cruz E.N., M.A.N.: 9.1 PathophysiologyDocument20 pagesMs. Elizabeth D. Cruz E.N., M.A.N.: 9.1 PathophysiologyAlfadz AsakilNo ratings yet
- FIX - Fracture and DislocationDocument80 pagesFIX - Fracture and DislocationWildan Hilmi AnsoriNo ratings yet
- HerniasDocument6 pagesHerniasYalin AbouhassiraNo ratings yet
- Iontophoresis Carpal Tunnel SyndromeDocument2 pagesIontophoresis Carpal Tunnel SyndromeIkre19No ratings yet
- PalpationDocument4 pagesPalpationLucy EkwunifeNo ratings yet
- MusculoeacDocument7 pagesMusculoeachehehe29No ratings yet
- List of InstrumentsDocument7 pagesList of Instruments11loeychanNo ratings yet
- Ha Lab MidtermDocument12 pagesHa Lab MidtermLexa CyNo ratings yet
- FlabbyDocument36 pagesFlabbyLedia EssamNo ratings yet
- (Mantap) Slide Materi Bedah-2 Batch 3 2018 PDFDocument200 pages(Mantap) Slide Materi Bedah-2 Batch 3 2018 PDFRonald Shields100% (1)
- Principles of Fracture FIXDocument63 pagesPrinciples of Fracture FIXAndi NurcahyantiNo ratings yet
- Principle of Fractures - Appley (PROF RPT)Document62 pagesPrinciple of Fractures - Appley (PROF RPT)Fuad AbdullahNo ratings yet
- The Body of the Horse, Its External Accidents and Diseases - With Information on Diagnosis and TreatmentFrom EverandThe Body of the Horse, Its External Accidents and Diseases - With Information on Diagnosis and TreatmentNo ratings yet
- DeQuervain Disease, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandDeQuervain Disease, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Hygiene NotesDocument60 pagesHygiene NotesDuchess Juliane Jose MirambelNo ratings yet
- Restroom Monitoring Checklist: Safety Management System FormsDocument4 pagesRestroom Monitoring Checklist: Safety Management System FormsTJames PaulinNo ratings yet
- Pe7 q1 Mod3 Introduction To Individual Sports Running and Swimming v2Document37 pagesPe7 q1 Mod3 Introduction To Individual Sports Running and Swimming v2Mark Christian Patricio100% (1)
- Bathroom Vocabulary: Sink Drain FaucetDocument10 pagesBathroom Vocabulary: Sink Drain FaucetMbNo ratings yet
- UAS 1 Bahasa Inggris Wajib Kelas XDocument8 pagesUAS 1 Bahasa Inggris Wajib Kelas XFaiz MabruriNo ratings yet
- Toilet & Bath at Bedroom: Medicine Cabinet Counter Top Lavatory Installation Siphon Jet Water ClosetDocument1 pageToilet & Bath at Bedroom: Medicine Cabinet Counter Top Lavatory Installation Siphon Jet Water ClosetStephen Mark Garcellano DalisayNo ratings yet
- VignetteDocument3 pagesVignettegsekar74No ratings yet
- Tepid SpongebobDocument2 pagesTepid SpongebobSean Rene Duay100% (2)
- Basic Survival Skills in SwimmingDocument2 pagesBasic Survival Skills in SwimmingTinayNo ratings yet
- Results Sligo V Marlins Feb 13Document10 pagesResults Sligo V Marlins Feb 13sligoswimNo ratings yet
- Handicapped Toilet DetailDocument1 pageHandicapped Toilet DetailHung NguyentheNo ratings yet
- Backstroke or Back Crawl Is One of The Four Swimming Styles Used in Competitive Events Regulated by FINADocument4 pagesBackstroke or Back Crawl Is One of The Four Swimming Styles Used in Competitive Events Regulated by FINAANGELO DELA PEÑANo ratings yet
- PLUMBING UNIT - A Minimum Standard Quantity of Plumbing Fixtures That Discharge WastesDocument1 pagePLUMBING UNIT - A Minimum Standard Quantity of Plumbing Fixtures That Discharge WastesMark Ronald SuaisoNo ratings yet
- The Swimming ThingDocument6 pagesThe Swimming ThingKevin AdrianoNo ratings yet
- Hindware Bath Tub, Multi Function, Premium Tub MRP CATALOGUE PDFDocument15 pagesHindware Bath Tub, Multi Function, Premium Tub MRP CATALOGUE PDFPundlik ChoudhariNo ratings yet
- Luxushomes Bathroom Catalog Part 1 (27!08!21)Document33 pagesLuxushomes Bathroom Catalog Part 1 (27!08!21)TCL TNo ratings yet
- Preventive and Curative Method of Treatment Regimental Therapy A ReviewDocument7 pagesPreventive and Curative Method of Treatment Regimental Therapy A ReviewDr. Md. Shahab UddinNo ratings yet
- Plumbing Code - DFU Drainage - SumpDocument4 pagesPlumbing Code - DFU Drainage - SumpDina Moh El HadedyNo ratings yet
- Oyster Bath Price Books 2019Document72 pagesOyster Bath Price Books 2019pravirNo ratings yet
- Fitting CatalogDocument28 pagesFitting CatalognotreadyNo ratings yet
- Penn Manor Modified Locker RoomsDocument1 pagePenn Manor Modified Locker RoomsAlex GeliNo ratings yet
- Revised New MRP List of Bipl W.E.F. 10.07.2020Document32 pagesRevised New MRP List of Bipl W.E.F. 10.07.2020MEDICA ULTIMATENo ratings yet
- Starts: Rules of The GameDocument4 pagesStarts: Rules of The GameAvox EverdeenNo ratings yet
- What I Have Learn in This Weekly Topic?Document3 pagesWhat I Have Learn in This Weekly Topic?Julius CabinganNo ratings yet
- Written TestDocument7 pagesWritten TestAdrian Reyes CapalarNo ratings yet
- Ancient Roman BathingDocument4 pagesAncient Roman BathingCarl Stephen PerezNo ratings yet
- Breast StrokeDocument21 pagesBreast StrokeJohn Reg BrillantesNo ratings yet