Professional Documents
Culture Documents
Pseudotumor Deltoideus Touch Me Not Lesion of The
Pseudotumor Deltoideus Touch Me Not Lesion of The
Uploaded by
neelimagooglyOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Pseudotumor Deltoideus Touch Me Not Lesion of The
Pseudotumor Deltoideus Touch Me Not Lesion of The
Uploaded by
neelimagooglyCopyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/369965024
Pseudotumor Deltoideus: Touch Me Not Lesion of the Humerus
Article in Cureus · April 2023
DOI: 10.7759/cureus.37427
CITATIONS READS
0 45
3 authors, including:
Michael Chirayath
St. John's National Academy of Health Sciences
19 PUBLICATIONS 0 CITATIONS
SEE PROFILE
All content following this page was uploaded by Michael Chirayath on 09 May 2023.
The user has requested enhancement of the downloaded file.
Open Access Case
Report DOI: 10.7759/cureus.37427
Pseudotumor Deltoideus: Touch Me Not Lesion of
the Humerus
Review began 03/26/2023
Michael Chirayath 1 , Stallon Sebastian 1 , Arun George 1
Review ended 04/08/2023
Published 04/11/2023 1. Radiology, St. John's Medical College Hospital, Bangalore, IND
© Copyright 2023
Chirayath et al. This is an open access Corresponding author: Michael Chirayath, michaelchirayath@gmail.com
article distributed under the terms of the
Creative Commons Attribution License CC-
BY 4.0., which permits unrestricted use,
distribution, and reproduction in any
medium, provided the original author and Abstract
source are credited.
Pseudotumor deltoideus is a localized region of irregular cortical thickening at the deltoid insertion that
causes a diagnostic quandary for radiologists due to its unusual radiological characteristics. It is benign in
origin, with the potential to act as a tumor stimulator, and has a variety of anatomic variants. The lesions
can be characterized on an X-ray by an area of lucency at or around the deltoid tuberosity and a cortical
irregularity or nearby eccentric marrow abnormality on computed tomography (CT)/magnetic resonance
imaging (MRI). The presence of cortical thickening and lucency at the deltoid insertion are unusual
radiological findings that provide a diagnostic challenge. In this article, we provide cases of shoulder pain
together with radiological imaging to make this previously underappreciated condition more
understandable. Further evaluation with CT/MRI should be performed in all cases of shoulder pain with
conventional radiographic findings of cortical thickening and intracortical lucency. The diagnosis of the
condition is aided by the presence of elongated lucency on CT and T2 hyperintensity in the cortex of the
proximal humerus. The clinical and imaging characteristics are important in the diagnosis of this condition.
It must not be confused for infection or malignancy, and a biopsy must never be attempted.
Categories: Radiology, Orthopedics, Sports Medicine
Keywords: humerus lucency, t2 isointense, t1 isointense, benign, pseudotumor deltoideus, deltoid lucency, cortical
thickening
Introduction
Morgan et al. first used the term “pseudotumor deltoideus” in 2001 after they published a study on
individuals who had shoulder pain and observed similar radiological clues at the deltoid insertion [1,2]. It is
well-recognized that deltoid muscle insertion is the site of a few benign skeletal anatomical abnormalities
that appear as irregular cortical thickening [1]. Similar cortical irregularity and thickening at the deltoid
insertion were also brought on by chronic avulsion damage to the deltoid tubercle and the pectoralis major
insertion in the proximal humerus. As a result, the presence of such skeletal abnormalities, combined with
pain and impairment, can mimic some cancers or infections. Therefore, these lesions are most often
misdiagnosed and subjected to unnecessary investigations [1]. This article illustrates three cases and aims to
better understand the radiological clues of this unusual variant known as pseudotumor deltoideus, a lesser-
known cause of shoulder pain.
Case Presentation
Case I
A 54-year-old male presented with a complaint of chronic left shoulder pain with mild restriction of
movements. There was no history of trauma, significant weightlifting, or sports participation. On
examination, there was pain associated with abduction and internal rotation of the nondominant left
shoulder. Imaging revealed irregular cortical thickening, intracortical lucencies, and hyperintense T2-
weighted lesion at the site of the deltoid muscle insertion. Based on these clinical and radiological findings,
the diagnosis of pseudotumor deltoideus was made, and conservative treatment was advised. The patient
was started on nonsteroidal anti-inflammatory drugs (NSAIDs), as well as regular physiotherapy and hot
fomentation, and was then called for a follow-up appointment. The severity of the shoulder pain had
significantly decreased at the two-month follow-up evaluation, and the complete range of motion had been
restored. The follow-up X-ray, however, revealed no change.
How to cite this article
Chirayath M, Sebastian S, George A (April 11, 2023) Pseudotumor Deltoideus: Touch Me Not Lesion of the Humerus. Cureus 15(4): e37427. DOI
10.7759/cureus.37427
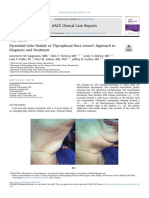
FIGURE 1: X-ray, CT, and MRI evaluation of the left shoulder. (a) Frontal
radiograph of the left shoulder shows an ill-defined area of cortical
thickening and sclerosis at the deltoid insertion. (b) Coronal CT of the
left humerus shows well-defined cortical thickness, mild irregularity,
and intracortical lucencies along the endosteal cortex. (c) Axial T2WI
shows small hyperintense foci in the endosteal region along the
anteromedial aspect of the humerus at the insertional site of the deltoid.
CT, computed tomography; MRI, magnetic resonance imaging; T2WI, T2-weighted image
Case II
A 39-year-old female presented to OPD with a six-week history of left shoulder pain and difficulty with
overhead movement. On physical examination, there was a mild restriction of overhead abduction. She was
right-hand dominant with no associated history of trauma. Imaging revealed similar irregular cortical
thickening and intracortical lucent lesion. She was managed conservatively and showed significant symptom
resolution.
FIGURE 2: X-ray and CT evaluation of the left shoulder. (a) Frontal
radiograph of the left humerus shows endosteal and cortical thickening
laterally at the level of the deltoid insertion. (b) Axial CT of the left
humerus shows thickened lateral cortex and radiolucent center of the
lesion.
CT, computed tomography
Case III
A 27-year-old right-hand-dominant female presented with a long-standing history of right upper and mid-
2023 Chirayath et al. Cureus 15(4): e37427. DOI 10.7759/cureus.37427 2 of 4
arm pain. There was no associated history of trauma or sports-related injury. The physical examination of
the patient revealed pain with internal and external shoulder rotation. Computed tomography (CT) and
magnetic resonance imaging (MRI) evaluation revealed an intracortical lucent lesion with T1 hypointense
and T2 hyperintense signal changes suggestive of pseudotumor deltoideus. He was managed conservatively,
and the follow-up showed a resolution of symptoms.
FIGURE 3: CT and MRI evaluation of the right shoulder. (a) Coronal T1WI
shows an isointense area of cortical thickening. (b and c) Axial T2 STIR
and T1WI hyperintense area of cortical thickening compared to the
normal cortical bone signal intensity at the region of the deltoid
insertion in the right humerus with no evidence of adjacent marrow and
soft tissue edema. (d) Axial CT shows well-defined cortical thickening,
expansion, and mild irregularity on the endosteal surface with irregular
intracortical lucency at the deltoid muscle attachment area.
CT, computed tomography; MRI, magnetic resonance imaging; T1WI, T1-weighted image; T2 STIR, T2-weighted
short-tau inversion recovery
Discussion
When an individual with a history of shoulder pain is observed in conjunction with imaging features such as
irregular cortical thickening and intracortical lucency in the proximal humerus, it can lead to an unneeded
biopsy or investigations based on the assumption of a malignant disease [1-3]. To add to the confusion
further, both musculoskeletal malignancy and sports-related injuries affect young patients, and their
symptoms frequently overlap [4]. However, imaging investigations of these lesions revealed no underlying
malignancy, and a clinical follow-up indicates that the process is inactive. Hence, “pseudotumor deltoideus”
is a term used to describe an anatomical variant at the deltoid insertion.
Although several theories have been proposed to explain this phenomenon, it is uncertain what really
caused it. A few possible explanations include an anatomic variant, erosions associated with tendinitis,
secondary changes at the deltoid insertion due to burned-out neoplasm, and avulsive cortical
irregularities [2]. Similar-looking bone erosions may occasionally be associated with calcific tendinitis, but
they are characterized by calcium deposits in the adjacent soft tissues [5,6].
Chronic avulsion injury of the deltoid also can present with similar clinical and imaging characteristics,
posing a dilemma for the radiologist. MRI is helpful with features such as prominent thickness and
irregularity of the cortex, increased T2-weighted signal intensity in the tendon insertion, and edema in the
adjacent soft tissue directing towards avulsive injury [5]. The presence of increased T2-weighted signal
intensity in the tendon and surrounding adjacent soft tissue is an indicator for both acute and chronic
avulsive injuries of the deltoid tubercle. The absence of such T2 hyperintensity favors the presence of
pseudotumor deltoideus.
Neoplasm should be excluded during the evaluation of bone abnormality. Due to their eccentric position,
two benign neoplasms, fibrous cortical defects and non-ossifying fibromas, are given special consideration
as differentials [7,8]. They differ from pseudotumor deltoideus, in that they occur mostly in immature
2023 Chirayath et al. Cureus 15(4): e37427. DOI 10.7759/cureus.37427 3 of 4
skeletons, are metaphyseal, and rarely manifest symptoms unless associated with pathologic fracture [7].
View publication stats
In this article, cortical thickening and intracortical lucency were observed at the site of the deltoid insertion.
The radiological imaging findings were consistent with both pseudotumor deltoideus and chronic avulsion
injury of the deltoid. There was no bony fragment, and MRI revealed no edema in the soft tissue adjacent to
the deltoid insertion. The diagnosis of pseudotumor deltoideus was made after considering the patient's age,
symptoms, a lack of history of injury from sports or other strenuous activity, and imaging findings. The same
was confirmed during a two-month follow-up following physiotherapy, NSAIDs, and conservative care that
resulted in symptom remission. Few studies have found a link between arm dominance and the prevalence
of pseudotumor deltoideus [1]. In our cases, only one appeared on the dominant arm, implying that there
was no relationship with arm dominance.
Various studies such as those of Singh and Tanwar, Morgan et al., and Adiguzel et al. described similar
radiological clues of pseudotumor deltoideus [1,2,9]. Symptomatic individuals presented with an area of
cortical thickening and intracortical lucency at the site of deltoid attachment detected in both conventional
radiography and CT. In addition, MRI reveals T1- and T2-weighted hyperintense signal changes in the cortex
with no associated soft tissue and marrow edema. In previous studies, pseudotumor deltoideus in patients,
which resembled our symptomatic cases, was seen in their dominant arm [1,2]. The definitive diagnosis of
pseudotumor deltoideus is based on clinical and radiographic evidence, particularly when the differentials
have been ruled out.
Conclusions
A diagnosis of pseudotumor deltoideus should be taken into consideration in patients with shoulder pain
when imaging reveals cortical thickening of the proximal humerus at the site of the deltoid insertion
accompanied with irregularity and intracortical lucency on CT and T2 hyperintensity on MRI without any
surrounding soft tissue changes. Unwanted biopsies should be avoided, and MRI is useful in the differential
diagnosis.
Additional Information
Disclosures
Human subjects: Consent was obtained or waived by all participants in this study. Conflicts of interest: In
compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services
info: All authors have declared that no financial support was received from any organization for the
submitted work. Financial relationships: All authors have declared that they have no financial
relationships at present or within the previous three years with any organizations that might have an
interest in the submitted work. Other relationships: All authors have declared that there are no other
relationships or activities that could appear to have influenced the submitted work.
References
1. Singh S, Tanwar A: Pseudotumor deltoideus: an underreported and misinterpreted cause of shoulder pain .
Indian J Radiol Imaging. 2020, 30:233-6. 10.4103/ijri.IJRI_407_19
2. Morgan H, Damron T, Cohen H, Allen M: Pseudotumor deltoideus: a previously undescribed anatomic
variant at the deltoid insertion site. Skeletal Radiol. 2001, 30:512-8. 10.1007/s002560100387
3. Hanna S, Al-Hindi B, Khaja A: Pseudotumor deltoideus case report: an incidental finding after a proximal
humerus fracture. Acta Sci Orthop. 2020, 30:59-62.
4. Damron TA, Morris C, Rougraff B, Tamurian R: Diagnosis and treatment of joint-related tumors that mimic
sports-related injuries. Instr Course Lect. 2009, 58:833-47.
5. Donnelly LF, Helms CA, Bisset GS 3rd: Chronic avulsive injury of the deltoid insertion in adolescents:
imaging findings in three cases. Radiology. 1999, 211:233-6. 10.1148/radiology.211.1.r99mr03233
6. Anderson SE, Hertel R, Johnston JO, Stauffer E, Leinweber E, Steinbach LS: Latissimus dorsi tendinosis and
tear: imaging features of a pseudotumor of the upper limb in five patients. AJR Am J Roentgenol. 2005,
185:1145-51. 10.2214/AJR.04.1247
7. Bullough PG, Walley J: Fibrous cortical defect and non-ossifying fibroma . Postgrad Med J. 1965, 41:672-6.
10.1136/pgmj.41.481.672
8. Bowers LM, Cohen DM, Bhattacharyya I, Pettigrew JC Jr, Stavropoulos MF: The non-ossifying fibroma: a
case report and review of the literature. Head Neck Pathol. 2013, 7:203-10. 10.1007/s12105-012-0399-7
9. Adiguzel E, Ata E, Demir Y, Tok F, Tan AK: A rare cause of shoulder pain: pseudotumor deltoideus . Am J
Phys Med Rehabil. 2015, 94:e96-7. 10.1097/PHM.0000000000000341
2023 Chirayath et al. Cureus 15(4): e37427. DOI 10.7759/cureus.37427 4 of 4
You might also like
- Chapter 06 - Behind The Supply CurveDocument90 pagesChapter 06 - Behind The Supply CurveJuana Miguens RodriguezNo ratings yet
- NEC SV8100 System Admin GuideDocument13 pagesNEC SV8100 System Admin GuideLuis AlvarezNo ratings yet
- PosterDocument1 pagePosterRaif RizqullahNo ratings yet
- Giant Cell Tumor of The Thoracal Spine Case Report 2020Document4 pagesGiant Cell Tumor of The Thoracal Spine Case Report 2020Ignatius Rheza SetiawanNo ratings yet
- Extra Renal Rhabdoid Tumor in An Adult Presentin 2024 International JournalDocument5 pagesExtra Renal Rhabdoid Tumor in An Adult Presentin 2024 International JournalRonald QuezadaNo ratings yet
- Spinal Tuberculosis: Imaging Features On MRIDocument6 pagesSpinal Tuberculosis: Imaging Features On MRIEster JuanitaNo ratings yet
- Paglia 2019Document6 pagesPaglia 2019idarNo ratings yet
- Lhermitte Duclos Disease - A Case Report: Ramya C, Renuka IV, Durga Prasad B, Pratyusha NDocument4 pagesLhermitte Duclos Disease - A Case Report: Ramya C, Renuka IV, Durga Prasad B, Pratyusha NajmrdNo ratings yet
- Contiguous Spinal Metastasis Mimicking Infectious SpondylodiscitisDocument5 pagesContiguous Spinal Metastasis Mimicking Infectious SpondylodiscitisCosmin RusneacNo ratings yet
- MSK UltrasoundDocument11 pagesMSK UltrasoundsafaNo ratings yet
- Cureus 0012 00000008855 PDFDocument11 pagesCureus 0012 00000008855 PDFAlberto BrahmNo ratings yet
- J Surneu 2007 07 059Document4 pagesJ Surneu 2007 07 059lucasnegromonte0001No ratings yet
- Interdisciplinary Neurosurgery: Technical Notes & Surgical TechniquesDocument5 pagesInterdisciplinary Neurosurgery: Technical Notes & Surgical TechniquesYovanka Naryai ManuhutuNo ratings yet
- Tuberculosis of The Patella, Report CaseDocument4 pagesTuberculosis of The Patella, Report CaseAnonymous AzXah9n0YNo ratings yet
- Superficial Radial Nerve Compression Due To Fibrom 2019 Acta Orthopaedica EtDocument3 pagesSuperficial Radial Nerve Compression Due To Fibrom 2019 Acta Orthopaedica EtanggiNo ratings yet
- Case Bezold AbscessDocument3 pagesCase Bezold AbscessCarimaGhalieNo ratings yet
- A Review of Lumbar Radiculopathy, Diagnosis, and TreatmentDocument7 pagesA Review of Lumbar Radiculopathy, Diagnosis, and TreatmentMatthew PhillipsNo ratings yet
- Primum Non Nocere - First Do No HarmDocument4 pagesPrimum Non Nocere - First Do No HarmSuci AprilyaNo ratings yet
- Surgical Management of Sacral Chordomas - Illustrative Cases and Current Management ParadigmsDocument7 pagesSurgical Management of Sacral Chordomas - Illustrative Cases and Current Management ParadigmsHugo JBNo ratings yet
- Diag DifDocument3 pagesDiag DifJulia LemboNo ratings yet
- Mi TsuyamaDocument8 pagesMi TsuyamatnsourceNo ratings yet
- A Review of Lumbar Radiculopathy, Diagnosis, and TreatmentDocument7 pagesA Review of Lumbar Radiculopathy, Diagnosis, and TreatmentZuraidaNo ratings yet
- Laryngeal Chondrosarcoma of The Thyroid Cartilage: Case ReportDocument5 pagesLaryngeal Chondrosarcoma of The Thyroid Cartilage: Case ReportelvirNo ratings yet
- Keithbidwell 1987Document5 pagesKeithbidwell 1987Ignatius Rheza SetiawanNo ratings yet
- Shoulder 2 Ada MriDocument4 pagesShoulder 2 Ada MriNirmalasari AnirNo ratings yet
- Review Article: Radiologic Mimics of Osteomyelitis and Septic Arthritis: A Pictorial EssayDocument18 pagesReview Article: Radiologic Mimics of Osteomyelitis and Septic Arthritis: A Pictorial EssayILham AKbarNo ratings yet
- The History of Clinical Musculoskeletal RadiologyDocument8 pagesThe History of Clinical Musculoskeletal RadiologyVALENTINA LOPEZ MARINNo ratings yet
- (10920684 - Neurosurgical Focus) Multiple Spinal Extradural Arachnoid Cysts Occurring in A ChildDocument4 pages(10920684 - Neurosurgical Focus) Multiple Spinal Extradural Arachnoid Cysts Occurring in A ChildRafael Mujica OreNo ratings yet
- Pediatric Gun Shot Injury An Increasing Problem in Sub-Saharan AfricaDocument5 pagesPediatric Gun Shot Injury An Increasing Problem in Sub-Saharan Africachidiebere peter echiehNo ratings yet
- JCM 11 00166 With CoverDocument29 pagesJCM 11 00166 With CoverBruno MañonNo ratings yet
- 434 FullDocument3 pages434 FullRajan PatelNo ratings yet
- Spinal Epidural Cavernous Hemangiomas in The 2024 International Journal of SDocument3 pagesSpinal Epidural Cavernous Hemangiomas in The 2024 International Journal of SRonald QuezadaNo ratings yet
- Journal of Oral and Maxillofacial Surgery, Medicine, and PathologyDocument7 pagesJournal of Oral and Maxillofacial Surgery, Medicine, and PathologyOMFS FKG UnimusNo ratings yet
- Case 7727Document7 pagesCase 7727hieu21032000No ratings yet
- FirbomatnedonDocument7 pagesFirbomatnedonAbiyoga PramanaNo ratings yet
- Chondrosarcoma of The Cervical Spine: C Ase ReportDocument3 pagesChondrosarcoma of The Cervical Spine: C Ase ReportChoirina Nur AzizaNo ratings yet
- PIIS1522294213000342Document11 pagesPIIS1522294213000342drcoraiuNo ratings yet
- Tail-End Troubles - Imaging of Soft-Tissue Buttock Tumours - Wijesekera2013Document12 pagesTail-End Troubles - Imaging of Soft-Tissue Buttock Tumours - Wijesekera2013yarumo1No ratings yet
- Otorhinolaryngology: Fibromatosis Colli or Pseudotumour of Sternocleidomastoid Muscle, A Rare Infantile Neck SwellingDocument3 pagesOtorhinolaryngology: Fibromatosis Colli or Pseudotumour of Sternocleidomastoid Muscle, A Rare Infantile Neck SwellingMohammedNo ratings yet
- Caso 1Document5 pagesCaso 1Jhomar QuinabandaNo ratings yet
- Radiology - Pathology Conference: Cutaneous Angiosarcoma of The LegDocument6 pagesRadiology - Pathology Conference: Cutaneous Angiosarcoma of The LegFrancisco ZurgaNo ratings yet
- Mano 4Document3 pagesMano 4juanNo ratings yet
- Atypical Atlanto Axial Subluxation - Yjocn - 4Document1 pageAtypical Atlanto Axial Subluxation - Yjocn - 4KaitlynHynes34No ratings yet
- 1647 Article p120Document4 pages1647 Article p120Santiago CeliNo ratings yet
- Ajr v8 Id1157Document2 pagesAjr v8 Id1157jenifer paathNo ratings yet
- Case Report: Iatrogenic Intraspinal Epidermoid CystDocument3 pagesCase Report: Iatrogenic Intraspinal Epidermoid CystWilda HanimNo ratings yet
- Ye 2015Document4 pagesYe 2015vernadskyiNo ratings yet
- Extra Cranial MetastasesDocument5 pagesExtra Cranial MetastasesJayendra Kumar AryaNo ratings yet
- RG 244035151Document21 pagesRG 244035151Radio ResidentNo ratings yet
- 1808 8694 Bjorl 86 s1 0s23Document3 pages1808 8694 Bjorl 86 s1 0s23VITOR PEREZNo ratings yet
- Tuberculous Osteomyelitis Mimicking A Lytic Bone Tumor: Report of Two Cases and Literature ReviewDocument5 pagesTuberculous Osteomyelitis Mimicking A Lytic Bone Tumor: Report of Two Cases and Literature ReviewazevedoNo ratings yet
- Solitary Intramuscular Cysticercosis of Right Elbow RegionDocument7 pagesSolitary Intramuscular Cysticercosis of Right Elbow RegionIJAR JOURNALNo ratings yet
- Tumor-Like Lesions of Bone and Soft TissuesDocument14 pagesTumor-Like Lesions of Bone and Soft TissuesFikri RamadhanNo ratings yet
- Raval PDFDocument5 pagesRaval PDFdebby claudiNo ratings yet
- AACE Clinical Case ReportsDocument3 pagesAACE Clinical Case ReportsSameerNo ratings yet
- Urology Case Reports: Abdullah, Junping XingDocument3 pagesUrology Case Reports: Abdullah, Junping XingHardiTariqHammaNo ratings yet
- Pediatric Thoracic Mass Lesions "Beyond The Common"Document10 pagesPediatric Thoracic Mass Lesions "Beyond The Common"Rifky ParmaNo ratings yet
- Imaging in RadiculopathyDocument17 pagesImaging in RadiculopathyFerdy DamaraNo ratings yet
- Tumor Celulas GigantesDocument7 pagesTumor Celulas GigantesGabyNo ratings yet
- SC 201543Document7 pagesSC 201543esinsubozatliNo ratings yet
- Malignant Mesothelioma of The Tunica Vaginalis Testis: Case ReportDocument2 pagesMalignant Mesothelioma of The Tunica Vaginalis Testis: Case ReportjamesyuNo ratings yet
- Metastatic Spine Disease: A Guide to Diagnosis and ManagementFrom EverandMetastatic Spine Disease: A Guide to Diagnosis and ManagementRex A. W. MarcoNo ratings yet
- 02 Security Market Indices and Market Efficiency PDFDocument27 pages02 Security Market Indices and Market Efficiency PDFNgân Hà NguyễnNo ratings yet
- Product Life Cycle of Lux SoapDocument66 pagesProduct Life Cycle of Lux SoapAbhimita GaineNo ratings yet
- Archies LTD Imc Assignment: Group No 04, IMC - BDocument6 pagesArchies LTD Imc Assignment: Group No 04, IMC - BNirmal KumarNo ratings yet
- Business Form Three Term 3 Holiday AssignmentDocument4 pagesBusiness Form Three Term 3 Holiday Assignmentbalozi training InstituteNo ratings yet
- Unit 5 Air CompressorDocument15 pagesUnit 5 Air Compressormadhume01No ratings yet
- CALP Glossary 2023 ENDocument41 pagesCALP Glossary 2023 ENHendra WijayaNo ratings yet
- Adjusting For Bad DebtsDocument16 pagesAdjusting For Bad DebtssamahaseNo ratings yet
- Electricity ExamDocument4 pagesElectricity Examjorolan.annabelle100% (1)
- 2011 2030 CLUP Annex 03 Growth CentersDocument31 pages2011 2030 CLUP Annex 03 Growth Centersautumn moonNo ratings yet
- OneTravel - Booking ConfirmationDocument2 pagesOneTravel - Booking ConfirmationRizky AlfianNo ratings yet
- People Vs ObsaniaDocument2 pagesPeople Vs Obsaniaminri721No ratings yet
- Experiment #4 Title: Testing of Reinforcing Steel BarsDocument9 pagesExperiment #4 Title: Testing of Reinforcing Steel BarsAnne Kristel Dela RosaNo ratings yet
- Powers and Functions of Registrar Under Trade Union ActDocument20 pagesPowers and Functions of Registrar Under Trade Union ActJagriti SaikiaNo ratings yet
- Tec Recruitment 2021Document5 pagesTec Recruitment 2021RAJ MENo ratings yet
- Cleveland Resume PortfiloDocument1 pageCleveland Resume Portfiloapi-273069439No ratings yet
- History of 3D PrintingDocument4 pagesHistory of 3D PrintingCristina Palacios AllcaNo ratings yet
- Back Stepping - Wikipedia, The Free EncyclopediaDocument9 pagesBack Stepping - Wikipedia, The Free EncyclopediaMario RossiNo ratings yet
- AGA Dry Ice Brochure A4 UK - tcm639-101282Document20 pagesAGA Dry Ice Brochure A4 UK - tcm639-101282শুভঙ্করNo ratings yet
- TRTDocument4 pagesTRTHendrias SoesantoNo ratings yet
- 2 Classes and Objects2018-10-23 14 - 17 - 43Document71 pages2 Classes and Objects2018-10-23 14 - 17 - 43RiyaNo ratings yet
- (Download PDF) Business Psychology and Organizational Behaviour 6Th Edition Eugene Mckenna Online Ebook All Chapter PDFDocument42 pages(Download PDF) Business Psychology and Organizational Behaviour 6Th Edition Eugene Mckenna Online Ebook All Chapter PDFkurt.holland582100% (13)
- Industrial Marketing 5-6Document2 pagesIndustrial Marketing 5-6Mary Grace Ygot ParachaNo ratings yet
- Crim 4 Week 6Document2 pagesCrim 4 Week 6Rose Jane JuanNo ratings yet
- Hunter Color Lab UltraScan - PRO - ProspektusDocument4 pagesHunter Color Lab UltraScan - PRO - ProspektusSumeet KaurNo ratings yet
- Mixing and AgitationDocument84 pagesMixing and AgitationVikas MishraNo ratings yet
- CV 2013 NgouneDocument4 pagesCV 2013 NgouneNGOUNENo ratings yet
- Adp PDFDocument22 pagesAdp PDFSkill IndiaNo ratings yet
- Countryfocus KazakhstanDocument10 pagesCountryfocus KazakhstanDouglas FunkNo ratings yet