Professional Documents
Culture Documents
AAD BF Non TB Cutaneous Mycobact Infections
AAD BF Non TB Cutaneous Mycobact Infections
Uploaded by
kahkashanahmed065Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
AAD BF Non TB Cutaneous Mycobact Infections
AAD BF Non TB Cutaneous Mycobact Infections
Uploaded by
kahkashanahmed065Copyright:
Available Formats
DermWorld
directions in residency A Publication of the American Academy of Dermatology | Association
boards fodder
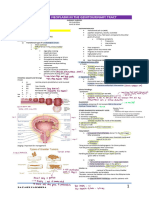
Non-tuberculous cutaneous mycobacterial infections
by Brooks David Kimmis, MD
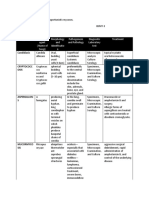
Organism Clinical Histopathology Laboratory Treatment Comments
features evaluation
M. ulcerans Firm, non- Extensive PCR Surgical exci- Transmission mode
(Buruli Ulcer) tender, mobile, necrosis and sion for ulcers unknown (related
subcutaneous obliteration of Culture at is treatment of to exposure to river
nodule that nerves and 32°C choice if feasible mud or water, ponds,
eventually forms vasculature or swamps)
a painless ulcer Local heating to
Granulomas can 40º C
Ulcer can develop during
expand exten- healing Hyperbaric
sively, even as oxygen
much as 15 cm Ziehl-neelsen
in diameter shows acid WHO
fast bacteria in recommended
Often on legs clumps antibiotic
regimen:
Can involve Rifampicin and
nearby and clarithromycin
underlying struc- for 8 weeks
tures (streptomycin if
clarithromycin
unavailable)
M. marinum Single Nonspecific PCR Empiric treatment Inoculation often
(Fish Tank erythema- histology findings with seen resultant from
Granuloma) tous nodule Culture at clarithromycin a combination of
or pustule Acute or chronic 31°C (must while awaiting trauma and aquatic
at the site of inflammatory and notify lab if sensitivities exposure (fish tank,
inoculation infiltrative chang- suspicious natural body of
which can es +/- granulo- for this For severe water, etc)
ulcerate, form mas organism, infection:
an abscess, or because clarithromycin + Sporotrichoid spread
develop Fibrinoid or case- most myco- rifampin or mnemonic
verrucous ation necrosis can bacteria are ethambutol CAT N SPLAT
epidermal occur cultured at • Cat scratch
changes 37°C) • Atypical
Organisms dif- mycobacteria
Brooks David
Can undergo ficult to find in • TB
Kimmis, MD,
is a PGY-3 at sporotrichoid immunocompe- • Nocardia
University of Kansas spread (of tent individuals • Sporotrichosis
Medical Center. all atypical • Phaeohyphyo-
mycobacterial mycosis or other
infections, M. deep fungal
marinum is most • Leishmaniasis
likely to have • Anthrax
sporotrichoid • Tularemia
distribution)
p. 1 • Fall 2020 www.aad.org/DIR
boards fodder
Non-tuberculous cutaneous mycobacterial infections
by Brooks David Kimmis, MD
Organism Clinical Histopathology Laboratory Treatment Comments
features evaluation
M. kansasii Verrucous Similar to TB PCR very IDSA guidelines Inoculation is usually
plaques, nod- (tuberculoid helpful, for pulmonary traumatic
ules or ulcers granulomas) difficult to infections
grow on (no specific Lung is major site of
Can have culture cutaneous infection
sporotrichoid guidelines exist):
spread
Rifampicin,
ethambutol, and
isoniazid or
macrolide
for at least 12
months (in the
past it was
recommended
12 months after
negative sputum
culture)
Fortuitum Most Neutrophilic Culture Often resistant to These organisms are
Complex common microabscesses is very anti-TB drugs grouped together
(Includes M. cutaneous and granuloma helpful due to similar clinical
fortuitum, M. pattern is formation +/- (unlike Often clarithro- presentations
chelonae, M. multiple necrosis other mycin-sensitive
abscessus) subcutaneous mycobac- Cutaneous infection
nodules on teria, these +/- excision uncommon
distal limbs organisms
grow within Cutaneous infection
Can show 7 days and usually results after
sporotrichoid can also surgeries, procedures
distribution grow on (Botox, fillers, lipo-
routine suction, others) trau-
Less bacte- ma, implant place-
commonly: rial culture ment, or tattoos
cellulitis, media,
abscesses, such as
papulopustules, sheep
sinus formation, blood or
ulceration chocolate
agar)
PCR
M. avium Systemic Macrophages PCR IDSA pulmonary Most frequently seen
complex symptoms are with phagocy- infection in patients with AIDS
(Includes M. very common tosed bacilli Culture guidelines
avium and (fever, night (skin, recommend M. avium and M.
M. intracel- sweats, bone Macrophages blood, 3-drug regimen intracellulare are
lulare) pain, weight may have spindle or lymph with macrolide closely related and
loss) cell transforma- node) (azithromycin> cause similar clinical
tion clarithromycin) findings
Papulopustules and ethambutol.
and purulent leg Can resemble Third drug vari- Traumatic inocula-
ulcers lepromatous lep- able but may tion is possible, but
rosy or spindle include rifampin dissemination in an
Can have cell neoplasm immunocompro-
sporotrichoid mised host is more
spread common
p. 2 • Fall 2020 www.aad.org/DIR
boards fodder
Non-tuberculous cutaneous mycobacterial infections
by Brooks David Kimmis, MD
Organism Clinical Histopathology Laboratory Treatment Comments
features evaluation
M. Single blue-red, Suppurative and Culture Rifampin and Generally, is an
haemophilum tender pus- granulomatous (from tissue clarithromycin infection of
tule, papule, or inflammation or synovial (Resistant to immunosuppressed
plaque which fluid) many anti-TB individuals (more
can form an Globi may be requires medications than half reported in
abscess or ulcer present similar source of other than patients with AIDS)
to lepromatous iron and rifampin and but may also affect
Can also be leprosy tem- rifabutin) healthy children, or
multiple lesions, perature following tattooing/
favoring skin between +/- Excision acupuncture
overlying joints 30-32°C
In children, the PCR
infection usu-
ally manifests as
lymphadenitis
M. Local Abscess forma- Culture Excision of lymph Typically infects
scrofulaceum lymphadenitis, tion in lymph of skin, node is preferred children via inhalation
slowly enlarging nodes or skin sputum, or ingestion
lymph nodes or lymph +/- Isoniazid and
that ulcerate and May be dif- nodes rifampin Primary cutaneous
drain with fistula ficult to dis- disease is rare
formation tinguish from
Scrofuloderma
Can be
sporotrichoid in Bacilli can be
distribution found within
involved lymph
nodes
References:
1. Bolognia J, Schaffer J, Cerroni L, et al. Dermatology. Philadelphia: Elsevier/Saunders, 2018. 4th edition.
Print.
2. Treatment of Mycobacterium Ulcerans Disease (Buruli Ulcer): Guidance for Health Workers. WHO. 2012.
ISBN: 978 92 4 150340 2
3. Wansbrough-Jones M. Report from the Meeting of the Buruli Ulcer Technical Advisory Group World Health
Organization, Headquarters, Geneva, Switzerland. 2017
4. DeStefano M, Shoen C, Cynamon M. Therapy for Mycobacterium kansasii infection: Beyond 2018. Frontiers
in Microbiology. 2018: 9:2271.
5. Daley, C, Iacacarino J, Lange C, et al. Treatment of Nontuberculous Mycobacterial Pulmonary disease: An
Official ATS/ERS/ESCMID/IDSA Clinical Practice Guideline. Clinical Infectious Diseases. 2020. Ciaa241.
p. 3 • Fall 2020 www.aad.org/DIR
You might also like
- Mcq. SurgeryDocument132 pagesMcq. Surgeryمنتظر اللاميNo ratings yet
- Blood Pressure Levels For Boys by Age and Height PercentileDocument4 pagesBlood Pressure Levels For Boys by Age and Height PercentileNuzla EmiraNo ratings yet
- BLS PDFDocument6 pagesBLS PDFAyesha JadoonNo ratings yet
- AAD BF Cutaneous Mycobact Infections PDFDocument3 pagesAAD BF Cutaneous Mycobact Infections PDFkahkashanahmed065No ratings yet
- Wuolah Free Bacteria TableDocument11 pagesWuolah Free Bacteria TableELENA FERNANDEZNo ratings yet
- SGD 2Document1 pageSGD 2Thea PepitoNo ratings yet
- Jurnal Bakteriologi - Ni Nyoman Nami ArthisariDocument23 pagesJurnal Bakteriologi - Ni Nyoman Nami ArthisariNami ArthisariNo ratings yet
- Cryptoc Occus: Neoforman SisDocument5 pagesCryptoc Occus: Neoforman SisQueenie LeoncioNo ratings yet
- Opportunistic MycosesDocument3 pagesOpportunistic MycosesMary100% (1)
- MB Yeasts PassDocument1 pageMB Yeasts PassJulia IshakNo ratings yet
- Activity 2Document2 pagesActivity 2Cyril LumibaoNo ratings yet
- Micro-Para Practical Exam ReviewerDocument8 pagesMicro-Para Practical Exam ReviewerRA TranceNo ratings yet
- Branching, Aerobic, Partially Acid Fast and Non-Acid Fast Gram (+) BacilliDocument2 pagesBranching, Aerobic, Partially Acid Fast and Non-Acid Fast Gram (+) BacilliJustine Marie RevillaNo ratings yet
- Mycology Specimen CollectionDocument6 pagesMycology Specimen CollectionMaam ShaNo ratings yet
- Table of Bacteria BateriologyDocument6 pagesTable of Bacteria BateriologyTeresa Mae Dimen BautistaNo ratings yet
- Clinical Microbiology and Infection: C. Joron, B. Rom Eo, A. Le FL Eche-Mateos, C. Rames, Y. El Samad, F. HamdadDocument2 pagesClinical Microbiology and Infection: C. Joron, B. Rom Eo, A. Le FL Eche-Mateos, C. Rames, Y. El Samad, F. HamdadNatalie Sarah MoonNo ratings yet
- Para 2Document4 pagesPara 265O6O78 ฐิติพันธ์ เพชรกระจายแสงNo ratings yet
- Identification by Microimmunofluorescence Test: AKA "Woolster's Disease" Incubation For C. Anthrax Is 1-15 DaysDocument10 pagesIdentification by Microimmunofluorescence Test: AKA "Woolster's Disease" Incubation For C. Anthrax Is 1-15 DaysizzmichikoNo ratings yet
- Microbiology: Atypical Bacteria: Chlamydia, Mycoplasms, LegionellaDocument4 pagesMicrobiology: Atypical Bacteria: Chlamydia, Mycoplasms, LegionellaPatricia Mae de JesusNo ratings yet
- SparganosisDocument2 pagesSparganosisGeozel VivienneNo ratings yet
- S3 L5 ClostridiumDocument5 pagesS3 L5 Clostridium2013SecBNo ratings yet
- Gas Gangrene X-Ray InterpretationDocument18 pagesGas Gangrene X-Ray InterpretationarullNo ratings yet
- Bacteria's Short NotesDocument26 pagesBacteria's Short Notesphotosforshare0001No ratings yet
- 016 Trichinella Spiralis DracunculusDocument14 pages016 Trichinella Spiralis DracunculusAyop KhNo ratings yet
- 15 Miscellaneous Bacteria PDFDocument2 pages15 Miscellaneous Bacteria PDFAnne MorenoNo ratings yet
- MergedDocument17 pagesMergedJack Ortega PuruggananNo ratings yet
- Sexually-Transmitted Infections and Aids Control Program Sexually Transmitted InfectionsDocument5 pagesSexually-Transmitted Infections and Aids Control Program Sexually Transmitted InfectionsShaira Abigail AninoNo ratings yet
- (Doi 10.1016/B978!0!323-07909-9.00164-1) Buttaravoli, Philip - Minor Emergencies - Cutaneous Larva MigransDocument2 pages(Doi 10.1016/B978!0!323-07909-9.00164-1) Buttaravoli, Philip - Minor Emergencies - Cutaneous Larva MigransLink BuiNo ratings yet
- L5. Chemotheraputic Agents IIDocument16 pagesL5. Chemotheraputic Agents IIMoNo ratings yet
- BActe Chap 14Document6 pagesBActe Chap 14barbiegahibNo ratings yet
- Equine Bacterial DiseasesDocument9 pagesEquine Bacterial Diseasesakilesh hardowarNo ratings yet
- Finals - Gram Negative Zoonotic Bacteria and Cell Wall DefficientDocument11 pagesFinals - Gram Negative Zoonotic Bacteria and Cell Wall DefficientJaneNo ratings yet
- Mycology Laboratory DiagnosisDocument4 pagesMycology Laboratory Diagnosisfpura210000001823No ratings yet
- Protozoa-Gastrointestinal Infections: Giardia Lamblia GiardiasisDocument7 pagesProtozoa-Gastrointestinal Infections: Giardia Lamblia GiardiasisHanunNo ratings yet
- 5 Systemic-MycosesDocument2 pages5 Systemic-MycosesMariz MartinezNo ratings yet
- CHANCROIDDocument13 pagesCHANCROIDPradeep YarasaniNo ratings yet
- Hepatic Abscess: Clinical Concept MapDocument1 pageHepatic Abscess: Clinical Concept MapKeep smileNo ratings yet
- URO 3 - Neoplasm in The Genitourinary TractDocument8 pagesURO 3 - Neoplasm in The Genitourinary TractHa Jae kyeongNo ratings yet
- Concise Common Diseases TableDocument4 pagesConcise Common Diseases Tableanushkasingh300806No ratings yet
- Fungal Infection of The SkinDocument4 pagesFungal Infection of The SkinYna Joy B. LigatNo ratings yet
- Semi Final TransesDocument17 pagesSemi Final TransesCAÑADA, JOHANNELYN M.No ratings yet
- Aerobic Gram PositiveDocument14 pagesAerobic Gram PositiveMickey mg100% (1)
- Cestodes Worksheet No. 1Document5 pagesCestodes Worksheet No. 1Denika AlmazanNo ratings yet
- Lesson 17 ChlamydiaceaeDocument4 pagesLesson 17 ChlamydiaceaeLittle CloudNo ratings yet
- Ascaris Lumbricoides (Linneaus. 1758) : NEMATODES: IntestinalDocument21 pagesAscaris Lumbricoides (Linneaus. 1758) : NEMATODES: IntestinalPatricia CabisonNo ratings yet
- Lesson 6 - Coccidian PDFDocument11 pagesLesson 6 - Coccidian PDFAnya IgnacioNo ratings yet
- Table of Lower Genital Tract Infections: Disease Etiology Pathogenesis SSX Diagnosis TreatmentDocument3 pagesTable of Lower Genital Tract Infections: Disease Etiology Pathogenesis SSX Diagnosis TreatmentMonique Angela Turingan GanganNo ratings yet
- Lec 15mycology SPPDocument35 pagesLec 15mycology SPPbujalkanNo ratings yet
- Parasitology Plasmodium SpeciesDocument9 pagesParasitology Plasmodium Speciespotatohart09No ratings yet
- Section 5: Chapter 17: Erysipelothrix, Lactobacilllus, and Similar OrganismsDocument13 pagesSection 5: Chapter 17: Erysipelothrix, Lactobacilllus, and Similar OrganismsPatricia CabisonNo ratings yet
- Clinical AND ADVANCE Pathology: TopicDocument7 pagesClinical AND ADVANCE Pathology: TopicNestley TiongsonNo ratings yet
- ECHINOCOCCUSDocument5 pagesECHINOCOCCUSGhina RizwanNo ratings yet
- Nematode Common Name Associated Disease Mode of Transmission Habitat Definitive Host Intermediate HostDocument5 pagesNematode Common Name Associated Disease Mode of Transmission Habitat Definitive Host Intermediate HostAnjelo PerenNo ratings yet
- Superficial and Cutaneous Mycoses: 2. Disease CharacteristicsDocument4 pagesSuperficial and Cutaneous Mycoses: 2. Disease CharacteristicsMA. ANGELI DELA CRUZNo ratings yet
- Blood and Tissue Protozoa (Con't) : DR - Mehru Nisha Mehrunisha@unikl - Edu.myDocument35 pagesBlood and Tissue Protozoa (Con't) : DR - Mehru Nisha Mehrunisha@unikl - Edu.myNida RidzuanNo ratings yet
- REMS Dermatology July 2022Document19 pagesREMS Dermatology July 2022vanisaezukuseNo ratings yet
- Defeats With ... : Infections PerfectlyDocument1 pageDefeats With ... : Infections PerfectlyMohammed shamiul ShahidNo ratings yet
- Anthrax: Koch's PostulateDocument25 pagesAnthrax: Koch's Postulatejamal nasir100% (1)
- Para Lect Prelims (Reviewer) : Lumbricoides Is An Example of A/anDocument17 pagesPara Lect Prelims (Reviewer) : Lumbricoides Is An Example of A/anJ Pao Bayro - LacanilaoNo ratings yet
- Candida SPP.: Dr. Mahesh AdhikariDocument13 pagesCandida SPP.: Dr. Mahesh Adhikarijeevan ghimireNo ratings yet
- Electrical Burn: Xantipphy Mae IbrahimDocument32 pagesElectrical Burn: Xantipphy Mae IbrahimMinette EmmanuelNo ratings yet
- Dermatology Notes for Medical StudentsFrom EverandDermatology Notes for Medical StudentsRating: 4 out of 5 stars4/5 (5)
- Facial Anatomy and The Application of Fillers andDocument12 pagesFacial Anatomy and The Application of Fillers andkahkashanahmed065No ratings yet
- Sandeep Kodali ppk-2Document6 pagesSandeep Kodali ppk-2kahkashanahmed065No ratings yet
- DIR Summer 2023 BF Atypical FibroxanthomaDocument2 pagesDIR Summer 2023 BF Atypical Fibroxanthomakahkashanahmed065No ratings yet
- DownloadDocument9 pagesDownloadkahkashanahmed065No ratings yet
- AAD BF Retinoid Biology 2Document2 pagesAAD BF Retinoid Biology 2kahkashanahmed065No ratings yet
- AAD BF Chemotherapy Specific Cutaneous ReactionsDocument3 pagesAAD BF Chemotherapy Specific Cutaneous Reactionskahkashanahmed065No ratings yet
- Quiz Review Exam ETASDocument183 pagesQuiz Review Exam ETASkahkashanahmed065No ratings yet
- DIR Fall 2023 BF Ticks ONLINEDocument3 pagesDIR Fall 2023 BF Ticks ONLINEkahkashanahmed065No ratings yet
- AAD BF Paisley Tie DiagnosisDocument2 pagesAAD BF Paisley Tie Diagnosiskahkashanahmed065No ratings yet
- AAD BF Cutaneous Mycobact Infections PDFDocument3 pagesAAD BF Cutaneous Mycobact Infections PDFkahkashanahmed065No ratings yet
- AAD BF Head and Neck Lesions InfantDocument2 pagesAAD BF Head and Neck Lesions Infantkahkashanahmed065No ratings yet
- AAD BF Herbal Supplements in DermatologyDocument2 pagesAAD BF Herbal Supplements in Dermatologykahkashanahmed065No ratings yet
- AAD BF Cutaneous Manifestations of HIV InfectionsDocument2 pagesAAD BF Cutaneous Manifestations of HIV Infectionskahkashanahmed065No ratings yet
- AAD BF Bones Eyes NailsDocument5 pagesAAD BF Bones Eyes Nailskahkashanahmed065No ratings yet
- Female Androgenetic Alopecia A Risk Factor For.4Document6 pagesFemale Androgenetic Alopecia A Risk Factor For.4kahkashanahmed065No ratings yet
- AAD BF HistiocytosisDocument2 pagesAAD BF Histiocytosiskahkashanahmed065No ratings yet
- Etas 2022-1Document1,135 pagesEtas 2022-1kahkashanahmed065No ratings yet
- Public Gdcmassbookdig Standardbookofet00ster Standardbookofet00sterDocument264 pagesPublic Gdcmassbookdig Standardbookofet00ster Standardbookofet00sterkahkashanahmed065No ratings yet
- RoutledgesManualofEtiquette 10001646Document264 pagesRoutledgesManualofEtiquette 10001646kahkashanahmed065No ratings yet
- Genetic Disorders of PigmentationDocument58 pagesGenetic Disorders of Pigmentationkahkashanahmed065No ratings yet
- NarmadhadeviDocument127 pagesNarmadhadevikahkashanahmed065No ratings yet
- IJD - Volume 1 - Issue 2 - Pages 22-23Document2 pagesIJD - Volume 1 - Issue 2 - Pages 22-23kahkashanahmed065No ratings yet
- Telltale Signs of Skin Trespassers - Clues To Superficial MycosisDocument5 pagesTelltale Signs of Skin Trespassers - Clues To Superficial Mycosiskahkashanahmed065No ratings yet
- KamcoDocument27 pagesKamcoAnn JosephNo ratings yet
- Vashikaran Mantra For Love PDFDocument4 pagesVashikaran Mantra For Love PDFmustafaaldin0% (2)
- 11 SMAW Q4 Module 2Document11 pages11 SMAW Q4 Module 2Mark Johnson VillaronNo ratings yet
- Reference HelicoilDocument1 pageReference HelicoilPetrotrim ServicesNo ratings yet
- SOLON Black Blue 230 07 enDocument4 pagesSOLON Black Blue 230 07 enstulemanskiNo ratings yet
- Journal of Colloid and Interface Science: Michael P. Brandon, Deirdre M. Ledwith, John M. KellyDocument8 pagesJournal of Colloid and Interface Science: Michael P. Brandon, Deirdre M. Ledwith, John M. KellyCharles TayNo ratings yet
- Modul Science Form 1Document31 pagesModul Science Form 1Norafiza HashimNo ratings yet
- Pamphlet 21 (NCl3)Document210 pagesPamphlet 21 (NCl3)victorNo ratings yet
- The Effects of Electrical Muscle Stimulation Ems Towards Male Skeletal Muscle MassDocument10 pagesThe Effects of Electrical Muscle Stimulation Ems Towards Male Skeletal Muscle MassAnonymous N0vLeRxNo ratings yet
- Fuels LiquidDocument25 pagesFuels Liquidpranay639100% (1)
- Choose The Correct Answer by Crossing A, B, C, or D!: Test Chapter I: Greeting, Leave Taking, Thanking, and AppologizingDocument3 pagesChoose The Correct Answer by Crossing A, B, C, or D!: Test Chapter I: Greeting, Leave Taking, Thanking, and AppologizingFerdi AnsyahNo ratings yet
- Gobi ManchurianDocument3 pagesGobi ManchurianPriya JuligantiNo ratings yet
- GHB FactsheetDocument2 pagesGHB FactsheetABC Action NewsNo ratings yet
- Liber eDocument15 pagesLiber eFatimaNo ratings yet
- CP SYSTEM - DESIGN DOCUMENT (Rev.01)Document46 pagesCP SYSTEM - DESIGN DOCUMENT (Rev.01)suman ghosh100% (1)
- Reading b2 c1Document4 pagesReading b2 c1Karenza ThomasNo ratings yet
- Pooja Sharma ThesisDocument66 pagesPooja Sharma ThesissknagarNo ratings yet
- The Cardiovascular System: The Heart: Part B: Prepared by Barbara Heard, Atlantic Cape Community CollegeDocument80 pagesThe Cardiovascular System: The Heart: Part B: Prepared by Barbara Heard, Atlantic Cape Community CollegeBrianna PinchinatNo ratings yet
- Design Princples For Wood Burning Cook StovesDocument20 pagesDesign Princples For Wood Burning Cook Stoveshana temesegenNo ratings yet
- Funding Proposal: WebsiteDocument8 pagesFunding Proposal: Websitemajiamal99No ratings yet
- NYJC Prelim 2006 P2Document12 pagesNYJC Prelim 2006 P2miiewNo ratings yet
- High Sensitivity DNA Assay - DE72905431 - 2022-09-19 - 12-47-17Document15 pagesHigh Sensitivity DNA Assay - DE72905431 - 2022-09-19 - 12-47-17Sara SolimanNo ratings yet
- Module P&P (Specific Heat Capacity)Document11 pagesModule P&P (Specific Heat Capacity)Syazlina SamsudinNo ratings yet
- From Gathering To Growing Food: Neinuo's LunchDocument10 pagesFrom Gathering To Growing Food: Neinuo's Lunchsoumya KavdiaNo ratings yet
- 1.2 Safety & Rules in Biology LaboratoryDocument32 pages1.2 Safety & Rules in Biology LaboratoryasyuraNo ratings yet
- Food and FarmingDocument38 pagesFood and FarmingKevin LlorenteNo ratings yet
- Ateneo de Zamboanga University: Case Study (HOSPITAL)Document7 pagesAteneo de Zamboanga University: Case Study (HOSPITAL)Lyka SaysonNo ratings yet