Professional Documents
Culture Documents
Eent Compiled
Eent Compiled
Uploaded by
Althea Franz DuoCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Eent Compiled
Eent Compiled
Uploaded by
Althea Franz DuoCopyright:
Available Formats
EENT
LESSON 1: INTRODUCTION TO EENT CONCEPT (EYES, EARS, NOSE, AND THROAT)
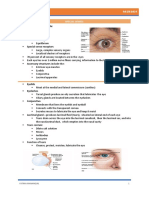
EYES EXTERNAL LAYER
It is a sensory organ, part of the sensory nervous system, Sclera
that reacts to visible light and allows us to use visual o Opaque white tissue
information for various purposes including seeing things, Cornea
keeping our balance, and maintaining circadian rhythm. o Dense transparent layer
o The “window” of the eye
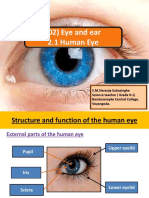
PARTS OF THE EYE Corneoscleral Junction
Eyelids and eyelashes o Transitional zone through which aqueous humor
Conjunctiva leaves the eyes.
o Palpebral conjunctiva o Also known as “LIMBUS”
Pink; lines inner surface of eyelids
o Bulbar conjunctiva MIDDLE LAYER
White with small blood vessels; covers anterior
Choroid
sclera
o Dark brown
Lacrimal Apparatus
o Lines most sclera and is attached to the retina
o Consists of lacrimal glands and ducts
o Contains many blood vessels
Meibomian glands
Ciliary body
Ciliary glands o Connects the choroid with the iris
o Secretes aqueous humor
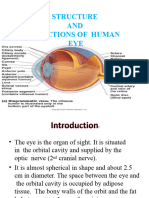
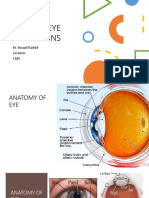
ANATOMY OF THE EYE Iris
o Colored portion of the eye
o Located behind the cornea and in front of the lens
o Has a central opening called “PUPIL”
Pupil
o controls the amount of light that enters the eye
Dark - dilate (mydriasis)
Light - constrict (miosis)
o Lens
Flexible, biconvex, transparent disc, lies behind
the iris
Bends the rays of light from entering through the
pupil
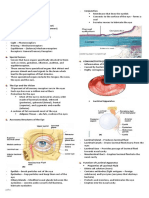
INNER LAYER
Retina
o Made of sensory receptors that transmit impulses to
the optic nerve
LAYERS OF THE EYE o Contains blood vessels and 2 types of photoreceptors
External Layer Rods
o Sclera - opaque white tissue work at low light and for peripheral visions
o Cornea - dense transparent layer; the window of the Cones
eye active at bright levels and provide color and
o Corneoscleral junction - transitional zone through central visions
which aqueous humor leaves the eyes; also known as Macula - yellow spot near the center of the retina
“Limbus” (responsible for central vision)
Problems: astigmatism (mismatch in the curvature Fovea - small pit; an indentation in the center of
of the eyes) the macula
Middle Layer Optic disk - creamy pink to white depressed area
o Choroid in the retina, “blind spot”
Dark brown Vitreous humor - jell-like substance that maintains
Lines most sclera and is attached to the reitan the shape of the eye
Contains many blood vessels
o Ciliary body MUSCLES OF THE EYE
connects the choroids with the iris External Muscles
Secretes aqueous humor Rectus muscles (CN 6- abducens) - medial, superior,
Inner Layer inferior
o Retina o Superior rectus - eyes move up and out (CN 3)
o Lateral rectus - eyes move laterally (CN 6)
o Medial rectus - eyes move medially (CN 3)
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 1
3rd CONCEPT: OPHTHALMOLOGY AND OTORHINOLARYNGOLOGY
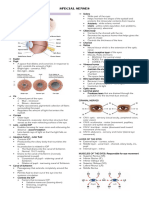
Oblique muscles (CN 4- trochlear) - superior and inferior o Snellen’s Chart
o Superior oblique - down and in (CN 4) Set patient at 20 ft
o Inferior oblique - up and in (CN 3) 20/20 normal vision
o Note: LR6 SO4; the rest CN 3 20/50 the client is able to read at 20 ft what a
Levator palpebrae healthy eye can read at 50 ft.
20/200 legally blind
If patient cannot see (1st line)
Set at 10 ft then 5 ft
E.g. 10/100
*1 - 20/200 legally blind
Top - Distance where client stands from the chart
Bottom - Distance where a normal person could
read the line
If patient still can't see. Proceed to do:
Counting fingers (CF) - if (-)
Hand movement (HM) - if (-)
Light perception (LP) - if (-), write NLP
(negative light perception)
Extraocular Muscle Function
NERVES OF THE EYE
Cranial nerve II - optic nerve
Cranial nerve III, IV, VI - innervate the muscles around the
eye Test for Color Vision
o Ishihara Chart
FUNCTIONS OF THE EYE Use of polychromatic plates
Refraction - the process of bending light rays to focus an Each eye is tested separately
image in the brain Sensitive for the diagnosis of red/green blindness
Accommodation - ability of the eye to focus specifically for o TEST:
close objects o https://www.color-blindness.com/ishihara-38-plates-
Pupillary constriction - ability of the pupils of the eye to cvd-
regulate light that enters the eye o RESULT:
https://picassciences.files.wordpress.com/2015/01/ish
ASSESSMENT ihara38.pdf
Inspection
o Exophthalmos - proptosis; protrusion of the eyeball DIAGNOSTIC TESTS FOR THE EYE
o Enophthalmos - sunken eyeballs, posterior FUNDOSCOPY
displacement of the eye Used to examine the health of the retina and vitreous humor
o Ptosis - drooping of upper eyelids Pupils should be dilated prior to the procedure
o Entropion - inversion of the lid margin o Administer pre-meds to dilate eyes (mydriatic agents)
o Ectropion - eversion of the lower lid
Set ophthalmoscope 6 inches away from the patient’ eyes
o Scleral Icterus - yellowish pigmentation of the sclera
Look for red reflex that indicates reflection of light in retina
Pupil
o Check for similarity of shape, size, and reaction
o Isocoria - equal pupil size TONOMETRY
o Anisocoria - 1 pupil larger than the other Measures IOP by determining the amount of force needed
o PERRLA - Pupil equally round and reactive to light and to the indent a portion of the anterior globe
accommodation Principle: A soft eye is easier to indent than a hard eye
Visual Acuity Normal IOP: 11-21 mmHg
o Measures the client’s distance and near vision
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 2
3rd CONCEPT: OPHTHALMOLOGY AND OTORHINOLARYNGOLOGY
SLIT LAMP Teach the patient or a family member the correct technique
Allows examination of the anterior ocular structures under for drug administration
microscopic magnification Emphasize that patients should never share eye
Help detect disorders of the anterior portion of the eye medications
CORNEAL STAINING
Consist of placing fluorescein or other topical dye into
conjunctival sac
A blue light is directed in the eye
The dye outlines the corneal irregularities that are not
visible
Normal eye: green color is uniformly scattered
Abnormal: green color accumulates on a certain area
COMMON PHARMACOLOGIC AGENTS
MYADRIATIC AGENTS
Cause pupillary dilation
Used in conditions requiring pupil to be dilated e.g.
Scopolamine (Isopto Hyoscine); Cyclopentolate (Cyclogyl);
Tropicamide (Mydriacyl); Phenylephrine (AK-Dilate,
Mydfrin)
Nursing interventions: Wear sunglasses (patient), teach to
administer properly and put pressure on lacrimal sac so that
medication will stay
MIOTIC AGENTS
Cause intense miosis and contraction of the ciliary muscle
Decrease intraocular pressure
Used for treatment of glaucoma
Eg. Acetylcholine (Miochol); Carbachol (ISO carbachol,
Niostat); Pilocarpine (Pilocar, Isopto Carpine)
OSMOTIC DIURETICS
Used for reduction of IOP or before ocular surgery
e.g. Mannitol (Osmitol)l Glycerin (Glycerol)
OPHTHALMIC ANTI-INFECTIVES
Used for treatment of ophthalmic infections
Eg. Tobramycin (Tobramycin, Tobrex); Gentamycin
(Garamycin, Genoptic); Bacitracin (AK-Tracin)
OPHTHALMIC STEROID ANTI-INFLAMMATORIES
To relieve pain; suppress other inflammatory processes of
the conjunctiva, cornea lid, and interior segment of the
globe
Dexamethasone (Maxidrex, Decadron); Flourometholone
(FML, Flarex)
CARBONIC ANHYDRASE INHIBITORS
Used in combination regimen to treat glaucoma and
postoperative rise in IOP
Acetazolamide (Diamox); Methazolamide (Neptazane)
GENERAL CONSIDERATIONS:
Advise the patient to follow the directions exactly
If the condition worsens or does not improve, notify the
physician
If multiple drugs are ordered. Wait 5 minutes between them
After administering ophthalmic solutions, apply gentle
pressure to inner canthus for approximately 1 minute to
decrease absorption and systemic effects.
If patient has both an ophthalmic drops and ointment, instill
first the drops before the ointment.
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 3
EENT
LESSON 2: EYE DISORDERS
EYE DISORDERS Instruct the child to avoid rubbing the eye
Impairment of health or a condition of abnormal functioning D/C use of contact lenses and to obtain new lenses to
of the organ of sight. eliminate the chance of re-infection
Instruct patient that eye make-up should be discarded and
INFECTIOUS AND INFLAMMATORY CONDITIONS OF replaced
THE EYE
CORNEAL DYSTROPHIES
CONJUNCTIVITIS Rare condition in which the cornea is altered without the
presence of any inflammation, infection or other eye
Inflammatory disease
o d/t allergens
Runs in families
o Non contagious
Types
o Treated with vasoconstrictors / corticosteroids
o Epithelial
Infectious
o Stromal
o d/t staph, chlamydia, neisseria
o Endothelium
o Contagious
Signs and symptoms
o Treated with broad spectrum antibiotics
o Cloudy or blurry vision
S/sx:
o Watery eyes
o Itching
o Dry eyes
o Burning or scratchy eyelids
o Glare
o Redness
o Photophobia
o Conjunctival edema
o Pain
o Excessive tearing
o Foreign body sensation
o Discharge
o Corneal erosions
Nursing Interventions encourage to wear sunglasses,
Management
children should not go to school until symptoms have
Hypertonic eye drops/ ointment
disappeared within 3-7 days, discontinue contact lens use
o Antibiotic
and buy a new pair
o Special contact lenses
bandage contact lenses
BLEPHARITIS AND HORDEOLUM Rigid contact lenses
Blepharitis o Surgery
o Inflammation of the eyelid margins o Corneal transplant
o S/sx: itchy, red, burning eyes, flicking, purulent o Phototherapeutic keratectomy (PTK)
discharges o *slit lamp - used dx test
o Tx: topical/eye drops antibiotics
o Do warm compress EPITHELIAL DYSTROPHIES
Hordeolum (stye)
Meesman - occasional “foreign body” sensation
o Chalazion
Cogan’s - most common type
o Acute suppurative infection of the follicle of an eyelash
o d/t staph Reis buckler - painful foreign body sensation
o S/sx: redness and pain, lump/swelling of the eyelid,
purulent discharges STROMAL DYSTROPHIES
o Tx: antibiotics. I&D Granular - greyish dots can be seen through a microscope.
o Do warm compress 4-5x a day Vision may be lost at 50 yrs old
Macular - irregular, cloudy areas appear in both corneas
KERATITIS which gradually merge together. Light sensitive, sight lost
Inflammation of the cornea at 20-30 yrs old
S/Sx: pain, reduced vision, cloudy cornea, photophobia, Lattice - “foreign body” sensation and a slight deterioration
difficulty opening the eye, abrasion, ulceration on vision. Under a microscope, very fine, overlapping lines
Tx: Antibiotics, keratoplasty can be seen in the camera.
Wear pritective eye shield, frequent handwashing …
ENDOTHELIUM DYSTROPHIES
NURSING CONSIDERATIONS: Innermost layer of the cornea
o Fuch’s
Instruct infection control measures
More common in women, unlikely to be inherited
Administer antibiotic or antiviral
Begins at 40 painless deteriorations of vision and
Administer antihistamines glare
Child should be kept home from school until antibiotic eye Next stage, painful episodes due to tiny blisters on
drops have been administered for 24 hours the cornea, which will gradually disappear as the
Instruct in the use of cool compresses vision gets worse
Wear dark glasses for photophobia
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 1
3rd CONCEPT: OPHTHALMOLOGY AND OTORHINOLARYNGOLOGY
o Keratoconus
Conical or cone-shaped cornea Nursing Management
Rarely appears until puberty or older o Assess how visual impairment can affect normal
Cornea becomes stretched and thins at its center functioning
o Provide emotional support for recent visual impairment
AMETROPIA o Orient to the environment
A state where refractive error is present or when distant o Sight guide technique (eg. contact and grasp)
points are no longer focused properly to the retina
Etiology: corneal curvature, length of the eye, strength of CATARACTS
the lens Is an opacity or cloudiness of the normally transparent
Types of Refractive Errors crystalline lens
o Myopia Lens protein dried out and forms crystals
o Hyperopia Causes
o Astigmatism o Senile - associated with aging
o Presbyopia o Congenital - may be hereditary
Surgical Management o Traumatic - associated with injury
o Lasik o Secondary - sequelae of systemic disease, drug
Laser in situ Keratomileusis ingestion
Uses an excimer laser to cut/reshape the cornea Diagnostic Exams
o ICR Intrastromal Corneal Ring o Standard ophthalmic exam
are small devices implanted to correct vision o Visual acuity test
o Phacik Intraocular Lens o Eye movement and peripheral vision
Lens that are made of plastic/silicone; implanted o Color blindness
permanently o Pupil dilation
o Tonometry
MYOPIA o Slit-lamp exam
Near-sightedness Medical Examination
Has excessive refractive strength o Extracapsular cataract extraction (ECCE)
Focuses light in front of the retina Manual expression
Treat with concave lens Phacoemulsification
o Intracapsular cataract extraction (ICCE)
HYPEROPIA Lens is removed through it capsule by incision to correct the
vision of patient
Far-sightedness
Focuses light at the back of the retina Nursing Management
Treat with CONVEX LENS Pre-op Nursing Care
Clear sa malayo, blurry sa malapit o Instruct measures to prevent increased IOP
Administer pre-op eye medication including
ASTIGMATISM mydriatics and cycloplegics as prescribed (e.g.
Unequal curvature of the cornea Atropine)
Treat with special lenses o No carrying of heavy objects
o No bending below the waist
PRESBYOPIA o Don't read
Post-op Nursing Care
Old sight
o CATARATA
Inability to accommodate for near vision due to loss of Clean post-operative eye
elasticity of the crystalline lens Analgesics
Treat with bifocal lens TobraDex (Tobramycin/dexamethasone)
Avoid lying on operative side
BLINDNESS Report complications
A condition of lacking visual perception Avoid bending and stooping
Defined ad a BCVA (Best Corrected Visual Acuity) of The use of eyeshield
20/400 to no light perception Advise hygiene
Types Of Blindness o Turn the client to the back or inoperative side
o Total blindness - no light perception and no usable o Give antibiotic-steroids (tobradex and acetaminophen)
vision o No aspirin due to clotting effects
o Functional blindness- has light perception but no o Instruct measures to prevent or decrease IOP
usable vision o Wear glasses during the day until the pupils responds
o Legally blindness - central vision acuity for distance of to light
20/20 o Eye shield at night or while sleeping
Etiology o For minor pain; use ice or heat as prescribed
o Common to adult 40 yrs old and above o Shower or bathing is allowed
o Diabetic retinopathy o Care of the dressings
o Macular degeneration o Stool softeners
o Glaucoma o Instruct to report pain with nausea and vomiting
o Cataract
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 2
3rd CONCEPT: OPHTHALMOLOGY AND OTORHINOLARYNGOLOGY
GLAUCOMA Signs and Symptoms
A group of disorder that all have IOP, leading to damage to o Early
the optic nerve structure with resulting visual field loss. Elevated IOP
Maybe caused by ocular inflammation or injury, trauma, Diminished accommodation
infection, hereditary predisposition o Late
Progressive loss of peripheral vision ”tunnel -
Normal IOP: 12-20 mmHg (determined by the rate of the
vision” followed by loss of central vision
aqueous production)
Vision worsening in the evening with difficulty
Two types:
adjusting to dark rooms
o Open-Angle Glaucoma
Blurred vision
Aka: chronic simple or wide-angle glaucoma
Halos around white lights
Most common
Frontal headaches
Bilateral and asymptomatic in early stage
Photophobia
Reduced outflow of AH
Increased lacrimation
The fluid cannot leave the eye at the same time it
Diagnostic Tests
is produced, IOP gradually increases
o Tonometry,
First s/sx is cloudy vision, lessened
o Ophthalmoscopy,
accommodation, loss of peripheral vision
o Visual field testing,
o Closed-Angle Glaucoma
o Gonioscopy (it checks the drainage angle)
AKA: Narrow-angle glaucoma or acute glaucoma
Less common Management
Movement of the iris against the cornea narrows o For acute glaucoma: treat as medical emergency
or closes the chamber angle, o Administer medications as prescribed to lower IOP
obstructing the outflow of the AH causing sudden Miotics (e.g. Pilocarpine) - constrict the pupils,
onset of unilateral eye pain with when it is constricted there will be contraction of
BOV and possibly nausea and vomiting. ciliary muscle so increase outflow of aqueous
IOP of 40-65 mmHg humor
Largest chance that the patient will get blind Carbonic anhydrase inhibitors (e.g.
Less Common Acetazolamide) - decreased the production of
aqueous humor
Beta-blockers (e.g. Timolol, betaxolol ) - use
cautiously to patient with asthma and CHF,
decreases the production of aqueous humor
Sympathomimetics (drug of choice to patient with
asthma and CHF; e.g, epinephrine) - reduce
aqueous humor output
o Surgery: peripheral iridectomy, trabeculectomy,
iridotomy
Peripheral Iridectomy- typically a laser
procedure that allows aqueous humor to flow from
the posterior to anterior chamber through an
excision of a small part of the iris.
Trabeculectomy- Partial thickness scleral
resection with small part of trabecular meshwork
removed.
Laser Iridotomy- Multiple laser incisions to the iris
to create openings for aqueous humor flow.
o Nursing Management
Monitor on CBR
Administer meds as ordered
Assist according to degree of visual impairment
Provide emotional support
Avoid mydriatics
Prepare patient for surgery
RETINAL DETACHMENT
Occurs when the layers of the retina separate because of
accumulation of fluid between them
Also occurs when both retinal layers elevate away from the
choroid as a result of a tumor.
Types:
o Partial Retinal Detachment
Initial detachment may be localized but without
rapid treatment
initial detachment that may be localized but
without rapid treatment
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 3
3rd CONCEPT: OPHTHALMOLOGY AND OTORHINOLARYNGOLOGY
o Complete Retinal Detachment
The entire retina may be detached; a serious eye Forms of AMD
condition needing immediate diagnosis and often o Dry (non-exudative)
urgent eye surgery (*entire retinal detachment*). Abnormal accumulation of yellowish colored
Causes: extracellular deposits “drusen” in the retinal
o Degenerative changes in the retina or vitreous. pigment of epithelium
o Trauma, inflammation, tumor Slow onset
o Diabetic Nephropathy Macular cells start to atrophy
o Myopia and loss of lens from a cataract Drusen= Are small yellow deposits of fatty proteins
Signs and Symptoms (lipids) that accumulate under the retina
o Sense of curtain (eye detachment) being drawn o Wet (exudative)
o Flashes of light Growth of new blood vessels from the choroid to
o - Black spots or floaters retinal epithelium
o - Blurred vision Rapid onset
o - Loss of a portion of the visual field Development of abnormal blood vessels around
Diagnostic Exams the macula
o Ophthalmoscopy Manifestations
o Slit-Lamp Exam o Blurred or darkened vision
Slit Lamp is a microscope with a bright light used o Scotomas (blind spots in visual fields)
during an eye exam. It gives the ophthalmologist a o Metamorphospia (distortion of vision)
closer look at the different structures at the front of Diagnostic Exam
the eye and inside the eye. It is a key tool in o Amster grid test: a diagnostic test that aids in detection
determining the health of the eyes and detecting of central visual disturbance; …
eye disease. o A pattern of intersecting lines with a black dot in the
o Gonioscopy middle. The central black dot is used for fixation (a
A painless exam your ophthalmologist uses to place for the eye to stare of)
check a part of your eye called the drainage angle. Management
Immediate Nursing Care o Laser macular photocoagulation
o Provide bedrest o Photodynamic therapy (PDT)
o Cover both eyes with patches to prevent further o Pegaptanib
detachment o Ranibizumab
o Speak to the client before approaching o Green leafy vegetables with lutein (spinach…)
o Position the client’s head as prescribed Nursing Interventions
o Protect the client from injury o Discuss strategies/modifications to carry out usual
o Avoid jerky head movements activities
o Minimize eye stress o Assist with self-care activities
o Prepare the client for surgical procedure as prescribed o Engage support people in assistance with patient
Goal: To prevent injury through further detachment activity
Surgical Management o Advise patient to memorize environment while some
o Sealing retinal breaks by cryosurgery vision is intact
A cold probe applied to the sclera to stimulate an o Use side rails as needed and make sure that patient
inflammatory response leading to adhesions can call help if needed
o Diathermy o Rest eyes as needed
the use of electrode needle & heat through the
sclera to stimulate an inflammatory response STRABISMUS
leading to adhesions Called “Squint Eye” or “crossed eye”
o Laser Therapy A condition in which the eyes are not aligned because of
to stimulate an inflammatory response to seal lack of muscle coordination of the extraocular muscles
small retinal tears before the detachment occurs Manifestations
o Scleral Buckling o Crossed eyes
to hold the choroid and retina together with a splint o Double vision
until scar tissue forms closing the tear o Uncoordinated eye movements
o Loss of depth perception
MACULAR DEGENERATION
Age-related macular degeneration CAUSES:
o Is a medical condition that results in loss of vision in the Children
center of the visual fields (the macula) because of o Unknown
damage to the retina o Congenital rubella
o The most common cause of irreversible central vision o Cerebral palsy
loss in persons over 60 o Retinopathy of prematurity
Risk Factors o Traumatic brain injury
o Related to retinal aging o Hemangioma near the eye
o Affected by genetics Adults
o Long term exposure to UV lights o Diabetes
o Hyperopia o Traumatic brain injury
o Cigarette smoking o Injury to the eye
o Stroke
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 4
3rd CONCEPT: OPHTHALMOLOGY AND OTORHINOLARYNGOLOGY
DIAGNOSTICS & TREATMENT CHEMICAL BURNS
Diagnostic Exams Immediately flush eye with water, normal saline or
o Retinal exam ophthalmic irrigation solution for a minimum of 15-20
o Ophthalmic exam minutes
o Visual acuity Using fingers to keep eye open as wide as possible
o Neurological exam
Treatment FOREIGN BODIES
o Glasses Never rub a speck or particle in the eye
o Eye patch Have the client look upward, expose the lower lid, wet a
o Eye muscles exercise cotton-tipped applicator with sterile normal saline and
o Surgery gently twist the swab over the particle and remove it.
OCULAR MELANOMA HYPHEMA
is a rare type of eye cancer that affects vision specifically
the choroid, ciliary body, and the iris. Choroidal melanoma is a pooling or collection of blood inside the anterior
is the most common. It is often discovered on a retinal chamber of the eye
examination and can be mistaken as a nevus/mole in its Management bedrest is semi fowler’s position
early stage; primarily occurs in adults. Avoid sudden movements for 3-5 days
Melanocytes produce the dark-colored pigment melanin Eye patch and shields
Found in the places in our body, including the skin, hair and If may resolve in 5-7 days
lining of the internal organs including the eye. Cycloplegic medications to rest the eye injured
Etiology
o Unknown
o Ultraviolet rays
o Dysplasic naevus syndrome
a condition that causes abnormal moles
o Ocular melanocytosis
a rare condition that causes crease and abnormal
pigmentation of the eye and skin around the eye.
MANIFESTATIONS
Blurred vision
Flashing lights and shadows
Change in iris color
Red and painful eye
Loss of peripheral vision
DIAGNOSTIC EXAMS
Ophthalmoscopy
Ultrasound
MRI/CT scan
MANAGEMENT
Radiotherapy
Surgery (Enucleation)
o Removal of the entire eye part of the optic nerve.
o An artificial ocular eye prosthesis can be created which
will maintain the contour of the eye
Transpupillary thermotherapy
o Is a method of delivering heat through the dilated pupil
into the posterior segment of the eye using a diiodide
laser.
OCULAR EMERGENCIES
An eye emergency is defined as a condition requiring
prompt medical attention due to a sudden change in ocular
health or vision. Eye trauma, foreign objects in the eye,
chemical exposure to the eyes, and ocular infections are all
considered eye emergencies and should be treated
immediately.
BLOW TO THE EYE
Apply cold compress for about 15 minutes to reduce
swelling and pain and help prevent bleeding.
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 5
EENT
LESSON 3: EARS
o Normal: sound is heard equally in both ears
EAR o Conductive hearing loss: affected ear
• It is a sensory organ that is responsible for hearing and o Sensorineural hearing loss: unaffected ear
equillibrium. ▪ * if malakas both ears (normal)
• *left conductive deafness (mas malakas si left ear)
DIVISION OF THE EAR • *left sensorineural deafness (mas malakas si right
OUTER (EXTERNAL) EAR ear)
• *right conductive deafness (malakas right ear)
• Auricle (Pinna)- collects sound waves
• *right sensorineural deafness (malakas si left)
• External Auditory Canal
• * weber’s right or left
o Glands secrete cerumen which provides protection
o Transmits sound waves to tympanic membrane. • *check for the lateralization; identify kong ano ang
o Tympanic Membrane side na mas malakas
▪ Barrier between external ear and middle ear • *N: same ang sound
▪ Transmit vibrations to middle ear • *Affected ear: yun yung mas malakas so it means
pt has conductive hearing loss
MIDDLE EAR *unaffected ear: mas malakas so si pt kay may
sensorineural hearing loss.
• Ossicles • Rinne Test
o Contains 3 small bones: o Useful in distinguishing between conductive and
▪ Malleus (hammer) sensorineural hearing loss
▪ Incus (anvil) ▪ (+) rinne test = air conduction > bone conduction
▪ Stapes (Stirrup) (normal)
• Oval window: an opening between the middle and inner ear ▪ (-) rinne test = bone conduction > air conduction
• Eustachian tube ▪ (+) conductive hearing loss
o Connects nasopharynx and middle ear ▪ *rinne under the pinne (pinna; mastoid)
o Equalizes pressure on both sides of the eardrum; ▪ * dapat mas malakas si bone conduction kesa sa
drainage channel air conduction
▪ *distinguish which is louder, either air or bone
INNER EAR conduction (normally mas loud si air conduction)
• Filled with perilymph and endolymph ▪ *(-) rinne test: conductive hearing loss (N: (+)
• Vestibule hearing loss)
o Entrance space next to oval window
• Cochlea IVESTIBULAR ASSESSMENT OF THE EAR
o Has the organ of corti, the receptor and organ of • Romberg’s test
hearing o Is a screening test for balance
o Contains hair cells that detect vibration from sound and ▪ (-) romberg: clent remains erect with slight
stimulate the 8th cranial nerve swaying
o Hearing ▪ (+) romberg: presence of significant swaying
• Semicircular canals • *let pt stand and close the eyes: if pt sway
o Organ of balance a lot (+) romberg’s test
o Bony tubes that form the inner part of the ear
o Balance DIAGNOSTIC TESTS
AUDIOMETRY
ASSESSMENTS
• Measure hearing acuity
VOICE TEST (WHISPER TEST) o The patient wears earphones and signals to the
• Ask the client to block one external canal audiologist when a tone is heard
• The examiner stands 1-2 ft away and quickly whispers a o Audiometric evaluations are performed in a soundproof
statement room
• The client is asked to repeat the whispered statement o Responses are plotted on a graph known as an
• Each ear is tested separately audiogram
o Mechanical Sound Transmission (middle ear function)
WATCH TEST o Neural Sound Transmission (cochlear function)
o Speech Discrimination (central integration)
• A ticking watch is used to test high-frequency sounds
• The examiner holds a ticking watch about 5 inches from
each ear and asks the client if the ticking is heard OTOSCOPIC EXAM
• Guidelines:
TUNING FORK TEST o The speculum is never blindly introduces into the
external canal
• Weber Test
o Tilt the head slightly away and golf the otoscope upside
o Uses bone conduction to test lateralization of sound
down as if it were a large pen
o Useful in detecting unilateral hearing loss
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 1
3rd CONCEPT: OPHTHALMOLOGY AND OTORHINOLARYNGOLOGY
o Visualize the external canal while slowly inserting the
speculum • Manifestations
o Normal: o Sound is perceived as distant or faint (decreased
▪ External canal - colored, intact, without lesions sensitivity)
▪ Eardrum - shiny, transparent, opaque or pearly o Complain that hearing is worse while eating crisp or
gray; mobile crunchy foods
• Diagnostic Tests:
ELECTRONYSTAGMOGRAPHY (ENG) o Weber test = lateralization on affected ear
o Electroencephalographic recording of eye movements o Rinne test = BC > AC
that provide objective documentation of induced and
spontaneous nystagmus SENSOURINAL HEARING LOSS
o Used to evaluate the oculomotor and vestibular • Results from damage to the inner ear and/or auditory nerve
systems to differentiate the cause of • Sensitivity to sounds/discrimination to sounds are impaired
o vertigo, tinnitus, and hearing loss of unknown origin • Irreversible
o C/I if patient has had prior neck injury • Etiology
o Exposure to nose
NURSING CONSIDERATIONS o Presbycusis
• Avoid a heavy meal before the procedure o Meningitis
• Avoid caffeine and/or alcohol - 48 hours before the o Ototoxic drugs (Aminoglycosides, Loop diuretics)
procedure o Acoustic neuroma
• Medications that may affect the vestibular system o Syphilis
(sedatives, anti anxiety agents, antihistamines, and o Diabetes mellitus
medications ordered for dizziness) - w/held for up to 5 days o Meniere’s disease
before the procedure. o Acoustic trauma
o Barotrauma/Ear Squeeze
EAR DISORDERS o Vascular diseases
• Manifestations
HEARING LOSS o Sound is distorted and faint
• Hearing loss is any degree of impairment of the ability to o Sounds “f” “s” and “z” are not heard
apprehend sound o High tones are less audible
• Disruption of the wave path • Diagnostic Tests
• Decibel (DB) - unit of measuring loudness o Weber test = lateralization on unaffected ear
• Types of hearing loss o Rinne test = AC > BC in affected ear
o Conductive
o Sensorineural MIXED HEARING LOSS
o Mixed • Client has both sensorineural and conductive hearing loss
o Presbycusis • Etiology
o Encephalitis
o Stroke
o Neoplasm in the brain
PESBYCUSIS
• Associated with aging
• Leads to degeneration or atrophy of the ganglionic cells in
the cochlea and a loss of elasticity of the basilar
membranes
• Leads to compromise of the vascular supply to the inner ear
• Bilateral hearing loss especially high frequency tones
• Etiology
o Age related changes
o Lifelong exposure to loud noises
o Ototoxic drugs
CONDUCTIVE HEARING LOSS o Disease process
• Occurs when sound waves are blocked to the inner ear • Common Manifestations:
fibers because of external ear or middle ear disorders o Complaints that their hearing is good but others
• Reversible mumble
• Etiology : o Leaning of turning one ear toward the speaker
o Otosclerosis o May fail to follow directions, speak while others are
o Changes in eardrum such as bulging speaking, or turn the radio/TV up very loud.
o Obstructed external ear canal o Irritability and even hostility not unusual
o Perforated tympanic membrane o Some become very suspicious of other because they
o Dislocated ossicle cannot hear what is being said
o Otitis media o Otalgia (ear pain), dizziness, and tinnitus with certain
o Otitis externa types of disorders
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 2
3rd CONCEPT: OPHTHALMOLOGY AND OTORHINOLARYNGOLOGY
MANAGEMENT MANAGEMENT
• Hearing aids - are battery operated instruments that make • E - Ear wicking
sounds louder • X - Surgery; debridement
o B - battery check • T - Thorough cleaning
o U - u have to clean the earpiece • E - Steroids
o N - not in use turn it off • R - Relieve edema
o G - go away from high or extreme temperature • N - NSAID’s
o O - oil cosmetics are CI • A – Antibiotics
o L - lowest setting adjustment • Showering or swimming use an ear plug (one that is
• Cochlear implants - permits direct neural stimulation of designed to keep water out), or use
auditory nerve, bypassing damaged hair cells • cotton with Vaseline on the outside.
• Surgery • Cotton swabs should be avoided
o Tympanoplasty: reconstruction of diseased or
• Hearing aids should be left out as much as possible until
deformed middle ear components
swelling and discharge stops.
o Stapedectomy: removal of footplate of stapes and
• Suctioning of the ear canal helps to keep it open, remove
insertion of graft or prosthesis.
debris, and decrease bacterial counts.
POSTOPERATIVE NURSING MANAGEMENT
OTITIS MEDIA
• Antibiotic as prescribed • Infection of the middle ear occurring as a result of a blocked
• Bed rest may be maintained for the first 24 hours or longer eustachian tube, which prevents normal drainage.
• Analgesics, antiemetics, and antihistamines are given as • A common complication of an acute respiratory infection
needed • Primary causative agents: H. Influenzae, Strep, Staph,
• The patient is positioned to promote drainage but maintain E.coli
some immobility • Infants and children are more prone
• Elevate head of bed • Main Causes:
• Encourage the patient to move slowly o Allergy
• Wash hands before ear care, and instruct patient not to o Infection
touch ear o Blockage of the eustachian tube and nutritional
• Take care not to get dressing or ear wet deficiency
• Packing may be removed up to 6 days postoperatively
• Report and teach patient to report any manifestations of SIGN AND SYMPTOMS:
infections • Bulging and immobile tympanic membrane
• Fullness in the ear
OTITIS EXTERNA • With slight hearing loss
• Ineffective inflammatory or allergic responses involving the • Vertigo
strictures of the external auditory canal or the auricles.
• Pain: usually the first symptom
• Swimmer’s ear”
• Fever
• More common in children and adolescents
o primary cause: ear pain
MANAGEMENT
o *cause: bacteria
• M - Measures to open eustachian tube/ Myringotomy
CAUSES • E - Eradicate the case
• D - Decongestant and antihistamine
• Causative agents: bacteria (Pseudo, proteus, E.coli, staph)
and Fungi (candida and aspergillus) • I - Instruct to avoid colds and barotraumas
• “Swimmer’s ear” : water collects in the ear canal • A - Analgesics (for pain)
• Cuts or abrasions in the lining of the ear canal (e.g. cotton
swab injury) NURSING CARE
• Dermatologic conditions (seborrhea, eczema, and contact • Apply heat locally for 20 minutes 3x a day
dermatitis) • Administer analgesics, antipyretics, antibiotics (Amoxicillin,
• *NOTE: moisture and irritation will prolong the course of the Clarithromycin, Cefuroxime)
problem • Ears should be kept clean and dry
• Use earplugs for swimming
SIGNS AND SYMPTOMS • Instruct the client that irritating agents such as hair products
• First symptom: the ear will feel full, and it may itch or headphones should be discontinued
• Pain • Prepare for myringotomy
• Skin becomes red, swollen and tender
• Yellowish discharge MASTOIDITIS
• Fever • Infection of the mastoid air cells
• Lymphadenopathy • Secondary disorder resulting from untreated otitis media
• Excessive swelling of the canal lead to conductive hearing • Caused by strep, pneumoniae and H. Influenzae
loss • Most often affects children
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 3
3rd CONCEPT: OPHTHALMOLOGY AND OTORHINOLARYNGOLOGY
• Endolymphatic drainage and Insertions of the Shunt (First-
SIGNS AND SYMPTOMS line surgical approach)
• Dull, post-auricular pain swelling • Labyrinthectomy (for severe, or inability to make use of the
• Cellulitis of area involved organ)
• Low grade fever
• Anorexia NURSING CARE
• Tender and enlarged lymph nodes • Help patients recognize the aura so the patient has time to
prepare for an attack.
DIAGNOSTIC EXAMS • Encourage the patient to lie down during attack, in a safe
place, and lie still.
• Otoscopic exam: reddened, dull, thick, immobile tympanic
membrane with OR without perforation • Place a pillow on each side of head.
• Xray: shows bone destruction • Have patients close eyes if this lessens symptoms.
• Management • Teach about the medication therapy
o Antibiotics • Assist patient to identify specific triggers to control attacks
o Surgery (Myringotomy; Mastoidectomy) • Remind the patient to move slowly
• Complications: • Avoid noises and glaring, bright lights
o Facial Nerve Injury • If there is a tendency to allergic reactions to foods, eliminate
o Meningitis those foods from the diet.
o Brain Abscess
o Labyrinthitis OTOSCLEROSIS
• Is a genetic disorder in which repeated reabsorption
LABYRINTHITIS • More common in women; 15-45 y/o
• An infection of the inner ear structure called labyrinth
• Causes MANIFESTATIONS
o Usually follows a viral illness • Progressive hearing loss
o Trauma or injury to the head or ear • Paracusis willisii (patient hears better in a noisy
o Bacterial infection (otitis media) environment
o Allergies • w/ or w/out tinnitus
o Alcohol abuse • Pinkish discoloration (schwartze’s sign) of the tympanic
o A benign tumor of the middle ear membrane
o Certain medications taken in high doses … • Rinne’s test: BC better that AC
• Manifestations • Weber’s test: increased sound in affected ear
o Common Symptoms:
• Audiometry: conductive hearing loss or mixed loss
▪ Vertigo
▪ Tinnitus
▪ Sensorineural hearing loss MANAGEMENT:
o Other symptoms • Medical therapy
▪ Nystagmus o Sodium fluoride therapy for 1-2 years
o Calcium gluconate and Vit. D
NURSING CARE • Amplification - hearing aid
• Nursing Care (PRIORITY: SAFETY) • Surgery - partial stapedectomy or complete stapedectomy
• Avoid turning the head with prosthesis (fenestration)
• Place on bed rest
• Assist to cope with anxiety that may be present because of ACOUSTIC NEUROMA
the frustration surrounding hearing loss or loss of work • Slow-growing tumor of the nerve that connects the ear to
• Priority: Patient’s safety = side rails up, if blind, be there for the brain. This nerve is located behind the ear.
the patient, if patient wants to pee, put on a wheelchair. • - Non-cancerous
Avoid injuries and further injuries (complications) • - Vestibular Schwannoma
• - Affects both men and women
MENIERE’S SYNDROME • Etiology
• Manifestations o Genetics (neurofibromatosis type 2) in which the tumor
o Traid: tinnitus, unilateral sensorineural hearing loss forms on the nerves (brain or spine).
and vertigo
o Nausea and vomiting MANIFESTATIONS
o Depression • Common Symptoms
o Headache o Hearing loss (progressive)
• Management o Tinnitus
o Treatment o Vertigo
▪ Sodium restricted diet • Less Common
▪ Diuretics: hydrochlorothiazide to decrease o Difficulty understanding speech
pressure o Headache
▪ Vestibular suppressants: antihistamine, o Numbeness in face or one ear
tranquilizers, and anticholinergics o Pain in the face or one ear
▪ Avoid alcohol, caffeine and smoking o Sleepiness
▪ Stress therapy o Vision problems
o Weakness of the face
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 4
3rd CONCEPT: OPHTHALMOLOGY AND OTORHINOLARYNGOLOGY
DIAGNOSTIC EXAMS MANIFESTATIONS
• Head CT • Lacerations
• Audiogram • Contusion
• Auditory Brainstem Response • Hematoma
• Caloric test • Abrasion
• Erythema
MANAGEMENT • Blistering
• Surgical removal of the tumor (preserve the facial nerve) • Conductive hearing loss
• Stereotactic radiosurgery (focus on high powered x rays on • Repeated trauma to the ear can cause hypertrophy, also
the small area) (pts unable to perform brain surgery and for known as cauliflower ear (common with boxers)
small tumors) • Numbness, pain, and paresthesia of the auricle
IMPACTED CERUMEN DIAGNOSTIC EXAMS
• A condition wherein earwax has built up in the ear canal and • Imaging studies
cause blockage. • Audiometric
• The air conduction would be equal to the bone conduction • Whisper test
or bone conduction ang mas malakas • Rinne and weber test
RISK FACTORS NURSING DIAGNOSIS
• Improper cleaning • Acute pain related to inflammation or trauma
• Older adult • Disturbed sensory perception: auditory related to altered
• Patients with hearing aids sensory reception
• Bony growths secondary to osteophyte or osteoma • Risk for injury related to self-cleaning of external ear
• • Deficient knowledge related to the lack of information on
MANIFESTATIONS preventive ar care
• Hearing loss
• A feeling of fullness, or blocked ear if cerumen has become
impacted
• Tinnitus
• Otoscopic examination reveals cerumen blocking the ear
canal
DIAGNOSTIC EXAMS
• Audiometric testing
• Hearing activity
• Whisper Voice
FOREIGN BODIES
• Anything that may be lodged in the ear canal intentionally
or accidentally
• High risks (Adults: insects; 9 months and up children: small
objects)
• Managements
o Of object is visible: use tweezers
o If insect: instill 2 drops of mineral oil
o If not insect do not instill mineral oil
o Irrigation in contraindicated if eardrum is perforated;
foreign vegetable bodies; insects
• Don’ts
o Do not push finger into the ear when you suspect some
foreign body in the ear
o Do not put out into the ear unless you are sure the
foreign body is insect
o Do not shake the head of the child who has foreign
body in the ear
o Do not attempt to clean your ears with cotton swabs
sticks or the match sticks
EAR TRAUMA
• A blow to the head
o Automobile accidents
o Burns
o Foreign bodies lodged in the ear canal
o Cold temperatures
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 5
EENT
LESSON 4: NOSE AND THROAT
NOSE & THROAT MANAGEMENT
Consists of bone and cartilages; air enters through 2 Antihistamines
opening/nostrils (nares) Antipyretics
Functions Nasal decongestants
o Olfaction - (CN1) smelling Rest and hydration
o Air-conditioning - controlling air temperature and Desensitization (gradual exposure to triggers)
humidity; removing particles before air enters into the
trachea, bronchi.
SINUSITIS
Inflammation of the mucous membrane of 1 or more
ANATOMY OF THE SINUSES
sinuses
PARANASAL SINUSES May accompany or follow rhinitis
frontal, sphenoid, maxillary, ethmoid Caused by Diplococcus, Strep, H. Influenzae
Air-filled cavities lined with mucous membranes Acute (if <4 weeks)
Functions
o Reduce the weight of the skull MANIFESTATIONS
o To produce mucus
Nasal swelling
o To influence voice quality (resonating chambers)
Purulent nasal discharge
Fever
ANATOMY OF THE PHARYNX AND LARYNX
Facial pain
Pharynx
o Commonly called the throat Fatigue
o Divided into 3 regions- nasopharynx, oropharynx, Congestion
laryngopharynx. Headache
o Functions: Cough
Respiratory function - receives air from the nasal Ear pain
cavity Anosmia
Digestive function - receives air, food and fluids
from the oral cavity MANAGEMENT
Larynx Antibiotics (amoxicillin, sulfamethoxazole, azithromycin,
o Commonly called the voice box/glottis clarithromycin, ciprofloxacin)
o Passageway for air bet. The pharynx above and the Decongestants
trachea below Antihistamines
Function: essential in human speech Antral irrigation: Caldwell-Luc procedure - permanent
opening for drainage
DISORDERS OF THE NOSE
NURSING CARE
RHINITIS
Methods to promote drainage:
Inflammation of the nasal mucosa
o Inhaling steam, Increase fluid intake, and Applying
Types
local heat
o Acute viral rhinitis or common colds
Stress the importance of following the recommended
Due to rhinovirus, parainfluenza virus,
antibiotic regimen
coronavirus, respiratory syncytial virus (RSV),
influenza virus, and adenovirus Discourage swimming and diving while patient has URTI
o Allergic Rhinitis (hay fever) Avoid people who has URTI
Is the most common form of respiratory allergy Maintain strict hand washing habits
presumed to be mediated by an immediate
immunologic reaction EPISTAXIS
Maybe seasonal (pollens from grass, trees, A.K.A. Nosebleeding
flowers) or perennial (domestic animal, hair, wool, Causes:
house dust, foods, newspaper, tobacco, etc.) o Trauma, HPN, blood dyscrasias, tumor, inflammatory
Manifestations reactions, otic barotrauma, nasal sprays, vigorous
o Edema nose blowing and nose picking
o Headache Types
o Swelling of the nasal mucosa o Anterior - easier to treat
o Congestion o Posterior - more severe bleeding
o Fever MANAGEMENT
o Sneezing Apply direct pressure (Kiesselbach’s area)
o Rhinorrhea Cautery
o Cough and Itching
Nasal Packing
o Mucus production
Cotton Ball with epinephrine
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 1
3rd CONCEPT: OPHTHALMOLOGY AND OTORHINOLARYNGOLOGY
NURSING MANAGEMENT LARYNGITIS
Monitor vital signs and assist with control of bleeding Inflammation of the mucous membrane of the larynx
Provides tissues and an emesis basin to allow the patient Caused by viruses, exposure to irritating inhalants,
to expectorate ant excess blood pollutants, chemical agents, alcohol smoke, overuse of
Review ways to prevent epistaxis; avoiding forceful nose voice
blowing, straining, high altitudes. Manifestations
Adequate humidification to prevent drying of the nasal o Acute hoarseness
passages o Dry cough
Instruct the patient how to apply direct pressure to the nose o Dysphagia
in the case of a recurrent nosebleed o Aphonia (voice loss)
If recurrent bleeding cannot be stopped, the patient is o Fever
instructed to seek additional medical attention. Management
o Voice rest
o Steam inhalation
NASAL POLYPS
o Hydration
Benign, grape like clusters of mucous membrane and loose
o Lozenges
connective tissue
o Antibiotics
Most often seen in patients with allergic rhinitis
Forms gradually from recurrent swelling of the nasal
mucosa
Complication: airway obstruction
Manifestations
o Nose feeling blocked
o Anosmia
o Runny nose
o Headache or pain
o Rhinoscopy shows a grayish grape like mass in the
nasal cavity
o CT scan of the sinuses will show opaque (cloudy) spots
where the polyps are
Management
o Cortisone therapy
o Polypectomy
o Note: nasal polyps may recur (so avoid nasal blowing)
DISORDERS OF THE THROAT
TONSILITIS
Inflammation and infection of the tonsils
d/t strep, staph, H. influenzae
Prone to rheumatic fever
MANIFESTATIONS
Difficulty swallowing
Ear pain
Fever, chills
Headache
Sore throat
Tenderness of the jaw and throat
Redness and swelling of the tonsils and surrounding tissues
with patches upon inspections
Voice changes, loss of voice
MANAGEMENT
Antibiotic therapy, warm saline gargles, analgesics,
antipyretics
Apply ice collar to severe sore throat
Oral care
Soft/liquid diet, hydration
Discourage spicy/sweet foods
Bed rest with increase OFI
Tonsillectomy
BORROMEO, CUTA, DANGO, GELIG, MAGNANAO, SADAVA, VERAQUE | BSN 3A (21-22) 2
You might also like
- Eent + OrthoDocument87 pagesEent + OrthoKaris HemmingsNo ratings yet
- Assessing EyesDocument2 pagesAssessing Eyeshannahabigael.cajesNo ratings yet
- A. Eye Balls D. Lacrimal Glands: 1. External Structures of The EyeDocument7 pagesA. Eye Balls D. Lacrimal Glands: 1. External Structures of The EyebeayapNo ratings yet
- The Eye Is Made Up of THREE LayersDocument2 pagesThe Eye Is Made Up of THREE LayersMarissa AsimNo ratings yet
- Eyes Lecture 1Document4 pagesEyes Lecture 1Rue Cheng MaNo ratings yet
- NeuroSensory - Eye Part 2Document38 pagesNeuroSensory - Eye Part 2Zed P. EstalillaNo ratings yet
- Special SensesDocument8 pagesSpecial SensesdjiamaeduremdezNo ratings yet
- Eye PDFDocument11 pagesEye PDFManas kumarNo ratings yet
- EENT NotesDocument12 pagesEENT NotesMhae TabasaNo ratings yet
- External Layer: The Fibrous Tunic: Structure S Characteristics FunctionDocument23 pagesExternal Layer: The Fibrous Tunic: Structure S Characteristics FunctionTheodora IonescuNo ratings yet
- Eye LectureDocument38 pagesEye LectureAMR WALIDNo ratings yet
- Gross Eye AnatomyDocument48 pagesGross Eye AnatomyAzizan Hanny100% (3)
- Eye and Ear - 2019Document3 pagesEye and Ear - 2019Mr. RWord100% (1)
- Chapter 8Document8 pagesChapter 8Bea SeloterioNo ratings yet
- Senses BloodDocument16 pagesSenses BloodZucc mahnutNo ratings yet
- Chapter 8-SPECIAL SENSESDocument5 pagesChapter 8-SPECIAL SENSESRishelle Mae Miñoza Pilones100% (1)
- Special SensesDocument14 pagesSpecial SensesJude Del RosarioNo ratings yet
- The EyeDocument8 pagesThe Eyezyrine jhen100% (1)
- 2 2 Sensory OrgansDocument27 pages2 2 Sensory OrgansKeashi VelzyNo ratings yet
- Eye and VisisonDocument5 pagesEye and VisisonrazondiegoNo ratings yet
- OPTHALMOLOGYDocument17 pagesOPTHALMOLOGYSofia P. PanlilioNo ratings yet
- AP Senses Nerves ReflexesDocument4 pagesAP Senses Nerves ReflexesPrinceska Diane AlbertoNo ratings yet
- Special SensesDocument8 pagesSpecial SensesGiane Qeirr Osias TimmalogNo ratings yet
- A&P - 11. Vision, Taste & Smell (15p)Document15 pagesA&P - 11. Vision, Taste & Smell (15p)Gabriel StratulatNo ratings yet
- Eye and Colourful WorldDocument11 pagesEye and Colourful WorldutsavpihuNo ratings yet
- Human EyeDocument32 pagesHuman Eyekaruparthi sripravallikaNo ratings yet
- Histology of The Eye Lectured By: Dr. Gonzales Transcribed By: Angelo Louise A. Sayo Proofread By: Kaye Reyes & Erina ValdesDocument12 pagesHistology of The Eye Lectured By: Dr. Gonzales Transcribed By: Angelo Louise A. Sayo Proofread By: Kaye Reyes & Erina ValdesKaye NeeNo ratings yet
- Anaphy Special Senses NotesDocument6 pagesAnaphy Special Senses NotesThieza Mecca LucenaNo ratings yet
- NCM116 EyeDisordersAndEarDisorders SirBaguioDocument12 pagesNCM116 EyeDisordersAndEarDisorders SirBaguiobaraderoayyah41No ratings yet
- Eye and Ear 2.1 Human EyeDocument12 pagesEye and Ear 2.1 Human Eyechakshana kannangaraNo ratings yet
- Anatomyphysiology ReviewerDocument116 pagesAnatomyphysiology Reviewerrosekatekate929No ratings yet
- Eyes and Ears Maam JezDocument8 pagesEyes and Ears Maam JezJoana DupagonNo ratings yet
- Chapter 8-SPECIAL SENSESDocument5 pagesChapter 8-SPECIAL SENSESrishellemaepilonesNo ratings yet
- Assessing The EyesDocument61 pagesAssessing The EyessrslytrdNo ratings yet
- Chapter 8 Special SensesDocument5 pagesChapter 8 Special SensesEdralyn EgaelNo ratings yet
- 5 Special SensesDocument8 pages5 Special SensesEdel GapasinNo ratings yet
- 1.1 and 1.2 Eye Anatomy - Examination (Eneganiron) 2Document153 pages1.1 and 1.2 Eye Anatomy - Examination (Eneganiron) 2charmaine.admanaNo ratings yet
- ASSESSMENT-OF-THE-EYEDocument7 pagesASSESSMENT-OF-THE-EYEvenezuelatrishamae22No ratings yet
- Special SensesDocument5 pagesSpecial SensesKathrene Angel GumilaoNo ratings yet
- Eye & EarDocument15 pagesEye & EarfatimasulaimanishereNo ratings yet
- EENTDocument21 pagesEENTMary Beth AbelidoNo ratings yet
- Finals EyesDocument11 pagesFinals EyesMonica JubaneNo ratings yet
- ATENGCO - Activity11 The Sense OrgansDocument8 pagesATENGCO - Activity11 The Sense OrgansJoann Mae PudaderaNo ratings yet
- The Sensory Organs: Anatomy Department Hasanuddin UniversityDocument117 pagesThe Sensory Organs: Anatomy Department Hasanuddin UniversityamiraNo ratings yet
- Ophthalmology Final TransDocument51 pagesOphthalmology Final TransPatryk Dionisio100% (1)
- 1group 1 - Compiled Topics-MergedDocument376 pages1group 1 - Compiled Topics-Mergedwhiskers qtNo ratings yet
- Iris Muscle - (Most Anterior Extension: EyeballDocument8 pagesIris Muscle - (Most Anterior Extension: EyeballBianx Flores DosdosNo ratings yet
- 27 Physiology of Visual AnalyzerDocument39 pages27 Physiology of Visual Analyzersiwap34656No ratings yet
- Ophthalmology 1st SessionDocument26 pagesOphthalmology 1st SessionWais samarNo ratings yet
- Eye PDFDocument16 pagesEye PDFhasbshahNo ratings yet
- Anatomy of The EyesDocument2 pagesAnatomy of The EyesTricia De TorresNo ratings yet
- Anatomy and PhysiologyDocument86 pagesAnatomy and PhysiologyAshinoyaaa JaehyungkookNo ratings yet
- Special SensesDocument16 pagesSpecial SensesAlther LorenNo ratings yet
- Special Senses NotesDocument3 pagesSpecial Senses NotesChelsa LeyritanaNo ratings yet
- Anatomy and Physiology of The EyeDocument18 pagesAnatomy and Physiology of The EyeMargaretha AdhiningrumNo ratings yet
- DISORDERS of The EYE and EARDocument8 pagesDISORDERS of The EYE and EARAnna Carmela P. MelendezNo ratings yet
- Special Senses 1Document14 pagesSpecial Senses 1Juan Miguel TevesNo ratings yet
- Introduction To Eye-Anatomy and PhysiologyDocument63 pagesIntroduction To Eye-Anatomy and Physiologyyi.limNo ratings yet
- Low Vision: Assessment and Educational Needs: A Guide to Teachers and ParentsFrom EverandLow Vision: Assessment and Educational Needs: A Guide to Teachers and ParentsNo ratings yet
- A Simple Guide to the Eye and Its Disorders, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to the Eye and Its Disorders, Diagnosis, Treatment and Related ConditionsNo ratings yet
- LEC Orthopedic NursingDocument31 pagesLEC Orthopedic NursingAlthea Franz DuoNo ratings yet
- Case Scenario GERDDocument9 pagesCase Scenario GERDAlthea Franz DuoNo ratings yet
- RIZALDocument1 pageRIZALAlthea Franz DuoNo ratings yet
- The Ambivalence of Filipino Traits and Values - For Quipper TaskDocument12 pagesThe Ambivalence of Filipino Traits and Values - For Quipper TaskAlthea Franz DuoNo ratings yet
- MS Cardiac SurgeryDocument99 pagesMS Cardiac SurgeryFazeela Naveen100% (1)
- Formulation and Pharmacological Evaluation of Cissus Quadrangularis Herbal Gel For Wound Healing ActivityDocument68 pagesFormulation and Pharmacological Evaluation of Cissus Quadrangularis Herbal Gel For Wound Healing ActivitydaniyaNo ratings yet
- Transdermal Drug Delivery: Endang Diyah IkasariDocument19 pagesTransdermal Drug Delivery: Endang Diyah IkasariZulfa SalsabellaNo ratings yet
- 1.2 Cardinal Manifestations of Renal Disease DR MoraDocument36 pages1.2 Cardinal Manifestations of Renal Disease DR MoraJewelNo ratings yet
- Case Analysis PaperDocument2 pagesCase Analysis PaperKukugirl DavisNo ratings yet
- Ledderhose Disease: Pathophysiology Diagnosis and ManagementDocument3 pagesLedderhose Disease: Pathophysiology Diagnosis and ManagementLeandro PolancoNo ratings yet
- Nursing Care of Children-QuestionsDocument11 pagesNursing Care of Children-QuestionsRamon Carlo AlmiranezNo ratings yet
- Principles of MicrobiologyDocument301 pagesPrinciples of MicrobiologyBenjamin A. Ujlaki76% (17)
- Interleukin 31 A New Cytokine Involved in Inflammation of The SkinDocument220 pagesInterleukin 31 A New Cytokine Involved in Inflammation of The SkinRemaja IslamNo ratings yet
- Germs Are Not For Sharing - CompressDocument22 pagesGerms Are Not For Sharing - CompressWanda GroenewaldNo ratings yet
- Algorithm 1 Algorithm 2Document51 pagesAlgorithm 1 Algorithm 2Zimm RrrrNo ratings yet
- Thyroid Eye Disease: Aka Thyroid Associated OphthalmopathyDocument25 pagesThyroid Eye Disease: Aka Thyroid Associated OphthalmopathyYuriko FerisNo ratings yet
- Postpartum CollapseDocument54 pagesPostpartum Collapsemedical chroniclesNo ratings yet
- Principles of Inheritance and VariationDocument81 pagesPrinciples of Inheritance and VariationRayan100% (2)
- Surah Al Baqarah (2:153) - Medical and Psychological Benefits of Salat and SabrDocument5 pagesSurah Al Baqarah (2:153) - Medical and Psychological Benefits of Salat and SabrMuhammad Awais Tahir100% (1)
- Herbal Infused Oils & Salves 2Document8 pagesHerbal Infused Oils & Salves 2Chelsea McGowanNo ratings yet
- Blanche GrubeDocument21 pagesBlanche GrubesangroniscarlosNo ratings yet
- B.Sc. Nuclear Medicine16 17 - 2516Document20 pagesB.Sc. Nuclear Medicine16 17 - 2516Bipun patelNo ratings yet
- HANDOUT MTP019 Thyroid DisordersDocument31 pagesHANDOUT MTP019 Thyroid DisordersShyama SharmaNo ratings yet
- Hodgkin's LymphomaDocument18 pagesHodgkin's LymphomaWilson Tiang Ko-PingNo ratings yet
- Organizational Structure at Various Levels of Care: DR K.R. AdewoyeDocument17 pagesOrganizational Structure at Various Levels of Care: DR K.R. AdewoyeKevia HartNo ratings yet
- A StudyDocument12 pagesA StudyNichchanun LertnuwatNo ratings yet
- Communicable and Non-Communicable DiseaseDocument44 pagesCommunicable and Non-Communicable DiseaseSajida Bibi NoonariNo ratings yet
- Jelena Kleut: ABSTRACT: Starting From The Observation That The COVID-19 Pandemic IsDocument21 pagesJelena Kleut: ABSTRACT: Starting From The Observation That The COVID-19 Pandemic IsTran Yen MinhNo ratings yet
- Protocollo Fazio CovidDocument12 pagesProtocollo Fazio CoviddonNo ratings yet
- Mitochondria and The Future of Medicine - Table of ContentsDocument3 pagesMitochondria and The Future of Medicine - Table of ContentsChelsea Green Publishing50% (2)
- PrepGenie GAMSAT Full Length TestDocument77 pagesPrepGenie GAMSAT Full Length TestRebekahNo ratings yet
- Effective Ways To Stop SnoringDocument32 pagesEffective Ways To Stop SnoringKwadwo Baah TiekuNo ratings yet
- Health Surveillance Affirmative and Negative - Michigan7 2015Document323 pagesHealth Surveillance Affirmative and Negative - Michigan7 2015Davis HillNo ratings yet
- Exam and KeysDocument24 pagesExam and KeyslirEcEnt WaldNo ratings yet