Professional Documents
Culture Documents
Comparison of The Reliability of 17 Celiac Disease
Comparison of The Reliability of 17 Celiac Disease
Uploaded by
siddhi divekarOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Comparison of The Reliability of 17 Celiac Disease
Comparison of The Reliability of 17 Celiac Disease
Uploaded by
siddhi divekarCopyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/314654635
Comparison of the Reliability of 17 Celiac Disease Associated Bio-Markers to
Reflect Intestinal Damage
Article in Journal of Clinical & Cellular Immunology · January 2017
DOI: 10.4172/2155-9899.1000486
CITATIONS READS
9 136
4 authors, including:
Aaron Lerner Wusterhausen Patricia
Technion - Israel Institute of Technology AESKU.KIPP Institute
107 PUBLICATIONS 1,212 CITATIONS 10 PUBLICATIONS 222 CITATIONS
SEE PROFILE SEE PROFILE
Torsten Matthias
120 PUBLICATIONS 2,014 CITATIONS
SEE PROFILE
Some of the authors of this publication are also working on these related projects:
The Industrial View project
Celiac disease and environment View project
All content following this page was uploaded by Torsten Matthias on 12 July 2017.
The user has requested enhancement of the downloaded file.
l & Cellula
ca
ni
Journal of Lerner et al., J Clin Cell Immunol 2017, 8:1
rI
urnal of Cli
mm
DOI: 10.4172/2155-9899.1000486
unolog
Clinical & Cellular Immunology
Jo
y
ISSN: 2155-9899
Research Article
Research Article Open
OMICS Access
International
Comparison of the Reliability of 17 Celiac Disease Associated Bio-Markers to
Reflect Intestinal Damage
Aaron Lerner1,2*, Patricia Jeremias2, Sandra Neidhöfer2 and Torsten Matthias2
1
Rappaport School of Medicine, Technion-Israel Institute of Technology, Haifa, Israel
2
ESKU.KIPP Institute, Wendelsheim, Germany
Abstract
In view of the increasing importance of serological biomarkers for screening and diagnosing celiac disease (CD)
and the lack of back-to-back comparison of their differential performance to their reliability to reflect the intestinal
damage in children with CD, their performances were evaluated.
95 pediatric CD patients (mean age 8.3), 45 nonspecific abdominal pain children (AP) (mean age 7.3), 99 normal
children (NC) (mean age 8.5) were tested with following ELISAs (detecting IgA, IgG or both, IgA and IgG (check)):
AESKULISA® Gliadin (AGA), AESKULISA® DGP (DGP), AESKULISA® tTg “New Generation” (Neo-epitope tTg
complexed to gliadin=tTg-neo), tTg (for in house research purpose only), AESKULISA® mTg neo-epitope and mTg
(RUO). Anti-endomysial antibodies (EMA) were checked via immunofluorescence test. Results were compared to
the degree of intestinal injury, using the revised Marsh criteria. Scatter diagrams and regression analysis comparing
the 17 antibodies’ activities to the degree of the intestinal damage were performed.
Most of the assays were able to discriminate patients with low and high degree of intestinal damage. Comparing
the different correlations of CD associated IgA and IgG antibodies’ isotypes, the tTg-neo IgA (r2=0.6165, p<0.0001)
and tTg-neo check (r2=0.6492, p<0.0001) stood out, significantly, as the best indicators for intestinal damage in CD.
EMA-IgA, tTg, DGP checks and mTg-neo IgG correlated closely to the mucosal injury.
The highest optical densities (medium 2.94 ± 1.2, p<0.0001) were measured in the tTg-neo IgA ELISA of patients
with Marsh 3c.
As a conclusion, it is suggested that tTg-neo IgA/IgG antibodies should be used preferably to closely reflect
intestinal damage during screening and diagnosing childhood CD. EMA-IgA, tTg and DGP checks and mTg-neo
IgG titers followed the tTg-neo check performance. mTg-neo IgG may present a new serological biomarker for CD.
Keywords: Celiac disease; Neo-epitope tissue transglutaminase; changes make reliance on symptomatology more remote and therefore
Tissue transglutaminase; Microbial transglutaminase; Deamidated diagnosis of the disease more difficult [6]. Recent, major improvements
gliadin peptide; Antibodies; Serology; Bio-markers; Intestine; Pathology in serological markers performance, with sensitivities and specificities
above 90%, are an additional reason why serological screening of CD
Introduction has achieved prime importance [1].
Celiac disease (CD) is a small intestine inflammatory autoimmune In the beginning of 2012 the European Society of Pediatric
disorder in genetically susceptible individuals, triggered by digestion Gastroenterology, Hepatology and Nutrition (ESPGHAN) released
of prolamins contained in wheat, barley, rye and partially in oat. The a new set of guidelines for the diagnosis of CD, based on both: the
accepted incidence in Western countries is 1-1.5%. The majority significant progress in the development of specific antibody tests and
of patients are still under-diagnosed, but increasing awareness and the understanding of the high prevalence of specific HLA haplotypes
improved serological performances, raise the diagnostic yield. In [7]. These advances were the base of updated guidelines for CD
contrast, in high-risk populations the average risk of CD can reach diagnosis in symptomatic and asymptomatic children, where, in
5-10% [1]. In the last decades CD frequency is increasing, joining the certain circumstances, small bowel biopsy can be omitted. Contrasting,
surge in autoimmune disease incidence and prevalence worldwide multiple adult guidelines still advocate serological screening followed
[2,3]. by obligatory intestinal biopsies for the diagnosis.
CD is a life-long multi-faced condition with an increased risk of Since only the tip of the CD iceberg is above the waterline and
complications. Hematological and gastrointestinal malignancies, a much larger portion remains under water undetected, it can be
osteoporosis/penia and other extraintestinal manifestations, decreased
height, malnutrition and nutritional deficiencies, fertility impairment,
stillbirth, dismaturity, hypercoagulability, psychosocial compromise, *Corresponding author: Aaron Lerner. AESKU.KIPP Institute. Mikroforum Ring
impairment of quality of life and-if left untreated-increased mortality 2, Wendelsheim 55234, Germany, Tel: 49-6734-9622-1010; Fax: 49-6734-9622-
2222; E-mail: aaronlerner1948@gmail.com
and additional autoimmune conditions, to name a few [4]. The
epidemiology and phenotype of CD are constantly changing, early Received: October 18, 2016; Accepted: January 24, 2017; Published: January
27, 2017
diagnosis and subsequent adherence to a gluten-free diet is highly
recommended. It has been shown that the classic intestinal clinical Citation: Lerner A, Jeremias P, Neidhöfer S, Matthias T (2017) Comparison of
picture of malnutrition, chronic diarrhea and nutritional deficiencies the Reliability of 17 Celiac Disease Associated Bio-Markers to Reflect Intestinal
Damage. J Clin Cell Immunol 8: 486. doi: 10.4172/2155-9899.1000486
are disappearing and extraintestinal presentations are emerging.
Nowadays, we are witnessing an epidemiological shift in the disease Copyright: © 2017 Lerner A, et al. This is an open-access article distributed under
the terms of the Creative Commons Attribution License, which permits unrestricted
phenotype toward a more advanced age, and increased prevalence of use, distribution, and reproduction in any medium, provided the original author and
latent, hyposymptomatic or asymptomatic presentations [5]. All these source are credited.
J Clin Cell Immunol, an open access journal
ISSN: 2155-9899 Volume 8 • Issue 1 • 1000486
Citation: Lerner A, Jeremias P, Neidhöfer S, Matthias T (2017) Comparison of the Reliability of 17 Celiac Disease Associated Bio-Markers to Reflect
Intestinal Damage. J Clin Cell Immunol 8: 486. doi: 10.4172/2155-9899.1000486
Page 2 of 8
expected that prevalence of the disease will increase continuously. Celiac disease was diagnosed according to the revised criteria of
Therefore, presenting symptoms will continue to change towards a-/ the European Society for Pediatric Gastroenterology and nutrition,
hyposymptomatic, supporting the need for improved serological based on specific serology (anti-tissue transglutaminase antibodies,
screening methods. There are multiple serological tests on the by ELISA) and duodenal biopsies [17]. All participants were on gluten
market: IgA anti-endomysial antibody (EMA), IgA and/or IgG tissue containing diet and had physical examination, laboratory work-up and
transglutaminase (tTg), IgA and/or IgG deamidated gliadin peptide celiac serology. On the day of endoscopy, 5 ml of peripheral blood was
(DGP), whereby IgA-tTg is the most frequently used and ESPGHAN’s withdrawn, centrifuged at 5000 c/sec for 10 minutes and the serum was
recommended one. Several combination tests are available too: DGP kept in -80° Celsius until used in serology assays.
IgA+G, tTg IgA+G, Gliadin IgA+G (check), CeliCheck IgA, IgG or Group 3: 99 normal children, recruited from a normal school,
IgA+IgG (autoantibodies against the cross-linked complex of tTg and mean age 8.5 ± 4.2 years, F\M 1:0.7, served as a normal control group
gliadin peptides (tTg neo-epitope) and the recently described IgG and/ (NC).
or IgA or IgG+IgA combined mTg neo-epitope and mTg (AESKULISA®
mTg neo-epitope and mTg, RUO) [1]. Being a new serological The study was approved by the Carmel Medical Center Helsinki
biomarker of CD mTg neo-epitope deserves some background committee and participants or legal guardians signed an informed
information. Microbial transglutaminase (mTg) is capable of cross- consent.
linking numerous molecules (including gliadin), thereby creating an Antibody determination by ELISA
mTg-gliadin neo-complex. This post-translational modification of
gliadin imitates its family member (human tTg) involved in CD. The following ELISAs, detecting IgA, IgG separated or combined
IgA and IgG (check) were used: AESKULISA® Gliadin (AGA), tTg (tTg;
For the last 26 years, numerous studies evaluated only one RUO (for in house research use only)), AESKULISA® DGP (DGP),
serological marker in relation to intestinal pathology, mainly EMA AESKULISA® tTg New Generation (tTg neo-epitope), AESKULISA®
and later on, tTg [8,9]. Fewer studies checked two antibodies, mainly mTg neo-epitope and mTg (RUO), according to the manufacturer
IgA-tTg and IgA-EMA, the latest being in 2012-13 [10-13]. Only in instructions.
two Israeli studies, 5 different antibodies’ levels were correlated to the
mucosal damage [14,15]. Parizade M. et al. found that high antibody Antibody determination by IFA
concentrations were predictive of villous atrophies for IgA+IgG-tTg, AESKUSLIDES® EMA (endomysium antibodies) were used
IgA+IgG-DGP and IgA-EMA [14], where EMA and IgA-tTg stood for indirect fluorescent IgA and IgG determination of human anti-
out to be the best. The second multi-marker study evaluated IgA- endomysium antibodies, according to the manufacturer instruction.
tTg, IgA+G-DGP, and IgA+G-EMA were the last one had the best
correlation [15]. The present study extended the serological repertoire The endomysium is the supporting, conective structure that
and checked, for the first time, 17 sub-types of the most frequently used surrounds the smooth fibers, located in the middle third of the
antibodies to screen in order to diagnose CD. esophagus. A representative positive EMA is shown in Figure 1.
In view of the increasing importance of serological biomarkers for Statistics
screening and diagnosis of CD, their differential performance, and the
Statistical analyses were performed using the Software MedCalc® (V
lack of back to back comparison, we undertook the task to evaluate the
15.6.1). Normally distributed values were expressed as mean ± standard
reliability of those individual or combined antibodies (ABs) to reflect
deviation (SD) and were compared by the Student`s t test. Correlations
the intestinal histological injury in CD children.
were assessed by the Pearson correlation test. p<0.05 was considered as
Material and Methods significant.
Patient populations Scatter diagrams and regression analysis comparing the 17
antibodies’ OD activities to the degrees of the intestinal damage were
Three groups of patients were investigated: correlated. Antibody results were compared to the degree of intestinal
injury, using revised Marsh criteria.
Group 1: 95 pediatric CD patients (CD), mean age 8.3 ± 4.4 years,
F/M (1/0.9). The CD group was divided according to the degree of Results
intestinal injury, using Marsh criteria, to 6 groups M0, MI, MII, MIII
a/b/c. With M0 representing a normal intestinal biopsy and MIII c total The performance of the different tests for the 99 pediatric CD, were
villous atrophy [16]. Those CD sub-groups contained MI=7, MII=13, compared to 45 pathological controls with AP and 99 normal control
MIII a=41, MIII b=27, MIII c=7 children, respectively. children, with similar age and sex ratio. All antibodies were detected via
ELISA, except for EMA which was checked via immunofluorescence.
Group 2: 45 children with nonspecific abdominal pain (AP), mean
age 7.3 ± 5.1 years, F\M 1:0.9, served as a pathological control group A general overview of the different IgA and IgG antibodies’ U/ml
(Marsh criteria=M0). titers is shown in Figure 2. All CD associated mean antibody’s levels
were above the cut-off levels. IgA isotype (Figure 2A) levels were higher
The CD and the AP groups underwent esophago-gastro- than of IgG isotypes (Figure 2B), except for the DGP-IgA and mTg-neo
duodenoscopy using GIF-xp 20 endoscope (pentax, Tokyo, Japan). At IgA, here IgG dominated. The tTg neo-epitope IgA test had the highest
least 5 biopsies were obtained: 4 from the second part of the duodenum immunoreactivity (P<0.0001) and tTg neo-epitope IgG had a higher
and 1 from the antrum, for the diagnosis or exclusion of CD. The immunoreactivity compared to single tTg-IgG. The following Figures
biopsies were immediately fixed in buffered formalin and embedded
3-6 correlate the various ABs activities to the degree of intestinal
on edge in paraffin. Sections were stained with hematoxylin-eosin and
damage, as characterized by Marsh criteria.
Giemsa, analyzed by the pathologist and graded according to Marsh
criteria, as previously described [16]. All assays were able to differentiate between patients of low and
J Clin Cell Immunol, an open access journal
ISSN: 2155-9899 Volume 8 • Issue 1 • 1000486
Citation: Lerner A, Jeremias P, Neidhöfer S, Matthias T (2017) Comparison of the Reliability of 17 Celiac Disease Associated Bio-Markers to Reflect
Intestinal Damage. J Clin Cell Immunol 8: 486. doi: 10.4172/2155-9899.1000486
Page 3 of 8
high degree intestinal damage. Comparing the different correlations Our own experience [16,18,19] and that of many others [1] favors
between CD associated IgA and IgG antibodies’ isotypes, EMA-IgA, combination tests to screen for CD. The main single antigen ELISA kit
tTg-neo IgA and tTg-neo check, stood out significantly as the best candidates are anti-tTg IgA and anti-DGP IgG, competing with the new
indicators of CD caused intestinal damage. The highest OD values CeliCheck combination of IgA and IgG thus omitting screening for IgA
(mean 2.94 ± 1.2, p<0.0001) were achieved using the tTg-neo IgA deficiency [16,18-21]. However, when reflection of intestinal pathology
ELISA with Marsh 3c patients (Figure 3). The correlations, as well as is concerned, single isotype Test are preferable, mainly the tTg-neo IgA.
their corresponding statistical significance of each AB isotype, are
The tTg-neo IgA kit uses a neo-epitope formed by complexing tTg
summarized (in increasing order) in Table 1.
and gliadin, the main antigens in CD. The basic idea is that tTg not
Since EMA testing is performed via immunofluorescence (Figure only able to deamidate gliadin peptides but also to cross-link with a
1), which is semi quantitative and operator-depended, it is shown high catalytic rate [22-24]. In the latter case, tTg/gliadin complexes
separately in Figure 6. The IgA and not the IgG isotype reflects the are formed, resulting in the formation of new epitopes (neo-epitopes),
intestinal pathology best. evidence has been shown in-vitro. More so, formation of the tTg-DGP
complex was suggested to involve epitope spreading from gliadin to tTg
For better comparison of diagnostic reliability, Table 1 lists various [21]. The antibodies against neo-epitopes of the tTg-gliadin complex
ABs’ activities of 5 combined (checks) and 12 single isotypes associated provide a new screening and diagnostic test in CD. Multiple studies
with CD. Many of the antibodies had high specificity and low sensitivity. have exhibited diagnostic sensitivities of 95% and specificities of 97% or
Combining the specificity and sensitivity by analyzing the AUC, tTg- more, when compared with those of traditional antibody assays [25,26].
neo IgA and EMA-IgA, in the single isotype, and tTg-neo check, in The neo-tTg/DGP complex is potentially able to drive the development
the combined isotype, stood out as best performers. Similarly, tTg-neo of newly formed epitopes derived from the cross-linkage between the
check and EMA-IgA reflect best the intestinal damage (p<0.005, Table enzyme and the substrate. It is foreseeable that the autoantibodies
1). Of note, mTg-neo IgG and not the IgA isotype, had a high AUC (0.95) generated against the neo-epitope may represent the best means for
and reflected significantly the intestinal histology in the CD group. screening populations, diagnosing high-risk groups and identify silent
or latent patients. In fact, several studies have shown the superiority
Discussion of screening for CD using the neo-tTg/DGPs complex strategy in the
The present study explored 15 ELISA kits encompassing 5 different general population [26,27] or in high-risk groups’ subjects [16,18,19,28-
families of antigens (gliadin, tTg, DGP and tTg neo-epitope and mTg 30]. The present results go along this serological diagnostic strategy and
neo-epitope) for specific IgA, IgG, combined IgA+G reactivities and add the aspect of intestinal damage reflection.
2 immunofluorescence EMA kits. The performances of all Kits were Several debates and disagreements exist in the literature concerning
assessed with the same blood sample, and then compared against the the cross talks between serological markers and reflection of the
rigid criterion of the corresponding biopsy-demonstrated duodenal intestinal pathology in CD.
histology, further enhancing the uniformity of the study. The analysis
On the pathological aspect a concern exists that intestinal
showed that antibody levels were well correlated to the duodenal
biopsy is the gold standard for diagnosis. Recently incorrect biopsy
damage degree in CD children, but there was a hierarchy among the
interpretation causing under diagnosis [31], lack of uniformity in
evaluated tests. The tTg neo-epitope IgA Kit occupied the first place in
the use of Marsh-Oberhuber classification [32] and unrecognized,
the IgA isotype group, DGP-IgG and tTg neo-epitope IgG shared the
misleading pathological features that are positively associated with
first place of IgG isotype Tests. The combined IgA+IgG isotypes had low
more advanced stages of the disease were described [33]. More so, even
correlations to intestinal histology, except for the tTg-neo check, which the cut-off for the intraepithelial lymphocyte count, a hallmark of CD
showed better performance than tTg-neo IgG or IgA kits . Concerning intestinal pathology, is debatable [34-35]. In the serological domain
the differential performance of Kit groups, IgA Kits surpassed IgG assays uniformity, lack of standardization, plethora of commercial
in reflecting intestinal damage, except for the mTg-neo IgG, which immune fluorescent and ELISA kits with variable cut-off levels are some
showed better performance than the mTg-neo IgA kit.
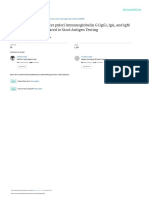
Figure 1: EMA IFA positive results as shown on the upper third esophageal slide. On the left positive-EMA IgG sera and on the right- positive EMA IgA sera, with a
total magnification of 40x.
J Clin Cell Immunol, an open access journal
ISSN: 2155-9899 Volume 8 • Issue 1 • 1000486
Citation: Lerner A, Jeremias P, Neidhöfer S, Matthias T (2017) Comparison of the Reliability of 17 Celiac Disease Associated Bio-Markers to Reflect
Intestinal Damage. J Clin Cell Immunol 8: 486. doi: 10.4172/2155-9899.1000486
Page 4 of 8
Figure 2: Comparison of A. IgA and B. IgG celiac disease associated antibody activities.
Figure 3: Correlations between IgA antibody activities and intestinal injury in celiac disease.
J Clin Cell Immunol, an open access journal
ISSN: 2155-9899 Volume 8 • Issue 1 • 1000486
Citation: Lerner A, Jeremias P, Neidhöfer S, Matthias T (2017) Comparison of the Reliability of 17 Celiac Disease Associated Bio-Markers to Reflect
Intestinal Damage. J Clin Cell Immunol 8: 486. doi: 10.4172/2155-9899.1000486
Page 5 of 8
Assay sensitivity specificity npv ppv AUC corr P
tTg IgG 13,13 98,99 53,26 92,86 0,56 0,2601 <0,0001
mTg neo IgA 64,65 98,99 73,68 98,46 0,82 0,3018 0,0003
Gliadin IgA 37,37 98,99 61,25 97,37 0,68 0,324 <0,0001
DGP IgA 66,67 98,99 74,81 98,51 0,83 0,359 <0,0001
Glia Check 57,58 98,99 70 98,28 0,78 0,3836 <0,0001
tTg IgA 60,61 98,99 71,53 98,36 0,80 0,4692 <0,0001
DGP IgG 70,71 98,99 77,17 98,59 0,85 0,4922 <0,0001
mTg neo Check 90,91 87,88 90,62 88,24 0,89 0,5127 <0,0001
Gliadin IgG 84,85 98,99 86,73 98,82 0,92 0,5181 <0,0001
tTg neo IgG 77,78 98 81,67 97,47 0,88 0,5334 <0,0001
mTg neo IgG 95,96 93,94 95,88 94,06 0,95 0,5633 <0,0001
DGP Check 82,83 98,99 85,22 98,78 0,91 0,5902 <0,0001
EMA IgG 55,7 99,3 N.D. N.D: 0,78 0,5996 <0,0001
tTg Check 79,8 98,99 83,05 98,75 0,89 0,6093 <0,0001
tTg neo IgA 88,89 98,99 89,91 98,88 0,94 0,6165 <0,0001
tTg neo check 97,98 98,99 98 98,98 0,98 0,6492 <0,0001
EMA IgA 90,2 94,1 N.D. N.D. 0,94 0,8094 <0,0001
Table 1: Antibodies diagnostic performances in pediatric celiac disease and their correlations between their activity and the degree of intestinal damage.
Figure 4: Correlations between IgG antibody titers and intestinal injury in celiac disease.
of the problematic aspects. On top of it, being on gluten containing 1. Much more CD associated antibodies were evaluated in a back-
diet, CD associated antibodies fluctuates or disappears spontaneously to-back experimental design (12 vs. 5).
in CD children [36]. Positive celiac serology coexists with normal 2. It is the first study to incorporate the neo-epitopes of tTg/mTg in
villous morphology [37]. Normalization of serology does not predict correlation to the intestinal injury.
normalization of intestinal histology [38]. A recent study from the UK
national external quality assessment service center (UK NEQAS) states 3. The group of AP is unique in composing pathological controls
that not all commercial available IgA-tTg kits are reliable and that the with normal intestinal biopsy.
ESPGHAN guidelines are not readily transferable to use in all centers 4. It is the only study that compared 17 CD associated serological
and should not be used in the UK [39]. Interestingly, even in the most markers, encompassing IgA, IgG and check isotypes.
recommended autoantibodies for CD diagnosis, multiple false positive
5. The addition of the IgA+IgG-AGA is important in reference to
and negative exist [40]. less recent historical data.
Screening some recent reviews and guidelines, comparing reliability 6. All determinations were done in the same laboratory, by the same
of the celiac specific serological markers, one sees the vast variability in person, under same conditions for better uniformity and comparability.
their sensitivity and specificities [1,7,41-43].
7. The antibodies’ activities were correlated to the same intestinal
The present study has several advantages: Marsh degree of atrophies.
J Clin Cell Immunol, an open access journal
ISSN: 2155-9899 Volume 8 • Issue 1 • 1000486
Citation: Lerner A, Jeremias P, Neidhöfer S, Matthias T (2017) Comparison of the Reliability of 17 Celiac Disease Associated Bio-Markers to Reflect
Intestinal Damage. J Clin Cell Immunol 8: 486. doi: 10.4172/2155-9899.1000486
Page 6 of 8
Figure 5: Correlations between IgA and IgG (check) antibody activities and intestinal injury in celiac disease.
Figure 6: Correlations between EMA-IgA and IgG activities and intestinal injury in celiac disease.
On the other hand, several limitations should be mentioned: mTg-neo isotypes compared to other ABs (but not to DGP and
EMA isotypes) [44] Since mTg-neo ABs isotypes are the newest
1. A multicenter study would have better represented the
published CD biomarkers of the 17 presently compared, in the
global clinical reality. Moreover, a multicenter-approach could have
following, some facts will be summarized. mTg-neo ABs isotypes are
normalized the potential biases encountered in one single center.
not autoimmune ABs, they are directed against neo-epitopes, formed
2. Comparing extended study populations would have increased during the conformational changes happening in the formation mTg/
the statistical power and the conclusion’s reliability. gliadin cross-link complex [22, 44-46]. Since mTg is heavily used by
the processed food industries, it is consumed daily [44,47]. mTg neo-
3. The present study represents only one aspect (intestinal pathology epitopes have, most recently, been shown to be immunogenic in active
reflection) in the decisional algorithm of the best serological marker for CD patients [44,46]. Presently, it represents a good reflector of CD
CD screening and diagnosis. intestinal atrophy, although, not the best one. CD is an IgA mediated
For transparency, some of the data were published separately: disease, so it is not astonishing that antibodies against tTg and tTg-
neo are of IgA isotype. Interestingly, the predominant antibody against
tTg IgA compared to tTg-neo isotypes [24] mTg-neo is of IgG isotype, reflecting the immune response against an
J Clin Cell Immunol, an open access journal
ISSN: 2155-9899 Volume 8 • Issue 1 • 1000486
Citation: Lerner A, Jeremias P, Neidhöfer S, Matthias T (2017) Comparison of the Reliability of 17 Celiac Disease Associated Bio-Markers to Reflect
Intestinal Damage. J Clin Cell Immunol 8: 486. doi: 10.4172/2155-9899.1000486
Page 7 of 8
following advantages over the single tTg-IgA ELISAs: 16. Rozenberg O, Lerner A, Pacht A Grinberg, M, Reginashvili D, et al. (2011) A
new algorithm for the diagnosis of celiac disease. Cellul molec Immunol 8: 146-
• Higher sera reactivity, Better reflection of intestinal pathology. 149.
17. Walker-Smith JA, Guandalini S, Schmitz J, Shmerling DH, Visakorpi JK (1990)
• Higher sensitivity, though comparable specificity, directed
Revised criteria for the diagnosis of celiac disease. Report of the working group
against different/new epitopes compared to the tTg antibody. of European Society of Pediatric Gastroenterology and nutrition. Arch Dis Child
65: 909911.
• It is suitable for IgA deficient patients, since it includes IgG
isotype. 18. Rozenberg O, Lerner A, Pacht A, Grinberg M, Reginashvili D, et al. (2012) A
novel algorithm for the diagnosis of celiac disease and a comprehensive review
In the hierarchy of the 17 bio-markers, the three autoantibodies of celiac disease diagnostics. Clin Rev Allergy Immunol 42: 331-341.
best reflecting CD intestinal damage, tTg-neo IgA, tTg-neo check and 19. Barak M, Rozenberg O, Froom P, Grinberg M, Reginashvili D, et al. (20132)
EMA IgA, won the competition. Therefore, it is suggested that tTg neo- Challenging our serological algorithm for celiac disease (CD) diagnosis by the
ESPGHAN guidelines. Clin Chem Lab Med 51: e257-259.
epitope antibodies should be preferably used to screen, diagnose and
monitor compliance in CD patients. The mTg neo-epitope IgG represent 20. Matthias T, Neidhöfer S, Pfeiffer S, Prager K, Reuter S, et al. (2011) Novel
a novel serological biomarker for CD. Its significance, pathogenic role, trends in celiac disease. Cell Mol Immunol 8: 121-125.
involvement in other autoimmune diseases or in non-celiac gluten 21. Matthias T, Pfeiffer S, Selmi C, Eric Gershwin M (2010) Diagnostic challenges
sensitivity, awaits further scientific explorations. in celiac disease and the role of the tissue transglutaminase-neo-epitope. Clin
Rev Allergy Immunol 38: 298-301.
References 22. Lerner A, Matthias T (2015) Possible association between celiac disease and
bacterial transglutaminase in food processing: a hypothesis. Nutr Rev 73: 544-
1. Lerner A (2014) Serological Diagnosis of Celiac Disease–Moving Beyond the 552.
Tip of the Iceberg. Internat J Celiac Dis 2: 64-66.
23. Lerner A, Neidhöfer S, Matthias T (2015) Transglutaminase 2 and anti
2. Lerner A, Jeremias P, Matthias T (2015) The world incidence of celiac disease transglutaminase 2 autoantibodies in celiac disease and beyond: Part A: TG2
is increasing: a review. Internat J Recent Scient Res 7: 5491-5496. double-edged sword: gut and extraintestinal involvement. Immunome Res 11:
101-105.
3. Lerner A, Jeremias P, Matthias T (2015) The world incidence and prevalence of
autoimmune diseases is increasing: A review. Internat J Celiac Dis 3: 151-155. 24. Lerner A, Jeremias P, Neidhöfer S, Matthias T (2016) Antibodies against neo-
epitope tTg complexed to gliadin are different and more reliable then anti-tTg
4. Lerner A, Agmon-Levin N, Shapira Y, Gilburd B, Reuter S, et al. (2013) The for the diagnosis of pediatric celiac disease. J Immunol Methods 429: 15-20.
thrombophilic network of autoantibodies in celiac disease. BMC Med 11: 89.
25. Bizzaro N, Tozzoli R, Villalta D, Fabris M, Tonutti E (2012) Cutting-edge issues
5. Lerner A (1994) Factors affecting the clinical presentation and time of diagnosis in celiac disease and in gluten intolerance. Clin Rev Allergy Immunol 42: 279-
of celiac disease: the Jerusalem and the West Bank-Gaza experience. Isr J 287.
Med Sci 30: 294-295.
26. Tozzoli R, Kodermaz G, Tampoia M, Visentini D, Tonutti E, et al. (2010)
6. Katz KD Rashtak S, Lahr BD, Melton LJ, Krause PK (2011) Screening for Detection of autoantibodies specific for transglutaminase-gliadin peptides
celiac disease in a North American population: sequential serology and complex: a new way to explore the celiac iceberg. It J Lab Med 6: 28-35.
gastrointestinal symptoms. Amer J Gastroentrol 106: 1333-1339.
27. Remes-Troche JM, Ramírez-Iglesias MT, Rubio-Tapia A, Alonso-Ramos A,
7. Husby S, Koletzko S, Korponay-Szabó IR, Mearin ML, Phillips A, et al. (2012) Velazquez A, et al. (2006) Celiac disease could be a frequent disease in Mexico:
European Society for Pediatric Gastroenterology Hepatology and Nutrition prevalence of tissue transglutaminase antibody in healthy blood donors. J Clin
guidelines for the diagnosis of coeliac disease. J Pediatr Gastroenterol Nutr Gastroenterol 40: 697-700.
54: 136-160.
28. Remes-Troche JM, Rios-Vaca A, Ramírez-Iglesias MT, Rubio-Tapia A,
8. Rossi TM, Kumar V, Lerner A, Heitlinger LA, Tucker N, et al. (1988) Relationship Andrade-Zarate V, et al. (2008) High prevalence of celiac disease in Mexican
of endomysial antibodies to jejunal mucosal pathology: specificity towards both Mestizo adults with type 1 diabetes mellitus. J Clin Gastroenterol 42: 460-465.
symptomatic and asymptomatic celiacs. J Pediatr Gastroenterol Nutr 7: 858-
863. 29. Tozzoli R, Kodermaz G, Porcelli B (2010) Clinical relevance and diagnostic
accuracy of new ELISA method for the detection of autoantibodies to gliadin-
9. Beltran L, Koenig M, Egner W, Howard, M, Butt A, et al. (2014) High-titre transglutaminase complex. Proceedings of the 7th International Congress on
circulating tissue transglutaminase-2 antibodies predict predict small bowel autoimmunity, Ljubljana: 5-9.
villous atrophy, but decision cut-off limits must be locally validated. Clin Exp
Immunol 176: 190-198. 30. Tonutti E, Visentini D, Fabris M (2010) Antibodies to the transglutaminase-
deamidated gliadin complex: a new serological approach to the diagnosis of
10. Mubarak A, Wolters VM, Gmelig-Meyling FH, Ten Kate FJ, Houwen RH celiac disease. Proceedings of the 7thInternational Congress on autoimmunity,
(2012) Tissue transglutaminase levels above 100 U/mL and celiac disease: a Ljubljana: 5-9.
prospective study. World J Gastroenterol 18: 4399-4403.
31. Arguelles-Grande C, Tennyson CA, Lewis SK, Green PH (2012) Variability
11. Licata A, Cappello M, Arini A, Florena AM, Randazzo C, et al. (2012) Serology in small bowel histopathology reporting between different pathology practice
in adults with celiac disease: limited accuracy in patients with mild histological settings: impact on the diagnosis of coeliac disease. J Clin Pathol 65: 242-247.
lesions. Intern Emerg Med 7: 337-342.
32. Picarelli A, Borghini R, Donato G, Di Tola M, Boccabella C, et al. (2014)
12. Alessio MG, Tonutti E, Brusca I, Radice A, Licini L et al. (2012) Correlation Weaknesses of histological analysis in celiac disease diagnosis: new possible
between IgA tissue transglutaminase antibody ratio and histological finding in scenarios. Scand J Gastroenterol 49: 1318-1324.
celiac disease. J Pediatr Gastroenterol Nutr 55: 44-49.
33. Brown IS, Smith J, Rosty C (2012) Gastrointestinal pathology in celiac disease:
13. Makovicky P, Rimarova K, Boor A, Makovicky P, Vodicka P, et al. (2013) a case series of 150 consecutive newly diagnosed patients. Am J Clin Pathol
Correlation between antibodies and histology in celiac disease: incidence of 138: 42-49.
celiac disease is higher than expected in the pediatric population. Mol Med
Rep 8: 1079-1083. 34. Siriweera EH, Qi Z, Yong JLC (2015) Validity of Intraepithelial Lymphocyte
Count in the Diagnosis of Celiac Disease: A Histopathological Study. Internat.
14. Parizade M, Bujanover Y, Weiss B, Nachmias V, Shainberg B (2009) J celiac Dis 3: 156-158
Performance of serology assays for diagnosing celiac disease in a clinical
setting. Clin Vaccine Immunol 16: 1576-1582. 35. Lerner A, Matthias T (2016) Intraepithelial Lymphocyte Normal Cut-off Level in
Celiac Disease: The Debate Continues. Internat. J of Celiac Dis 4: 4-6.
15. Hojsak I, Mozer-Glassberg, Segal Gilboa N, Weinberger R, Hartman C, et al.
(2012) Celiac disease screening assays for children younger than 3 years of 36. Simell S, Hoppu S, Hekkala A, Simell T, Ståhlberg MR, et al. (2007) Fate of five
age: the performance of three serological tests. Dig Dis Sci 57: 127-132. celiac disease-associated antibodies during normal diet in genetically at-risk
J Clin Cell Immunol, an open access journal
ISSN: 2155-9899 Volume 8 • Issue 1 • 1000486
Citation: Lerner A, Jeremias P, Neidhöfer S, Matthias T (2017) Comparison of the Reliability of 17 Celiac Disease Associated Bio-Markers to Reflect
Intestinal Damage. J Clin Cell Immunol 8: 486. doi: 10.4172/2155-9899.1000486
Page 8 of 8
children observed from birth in a natural history study. Amer J Gastroenterol 43. Rubio-Tapia A, Hill ID, Kelly CP, Calderwood AH, Murray JA, American College
102: 2026-2035. of Gastroenterology (2013) ACG clinical guidelines: diagnosis and management
of celiac disease. Am J Gastroenterol 108: 656-676.
37. Tanpowpong P, Broder-Fingert S, Katz AJ, Camargo CA Jr (2013)
Characteristics of children with positive coeliac serology and normal villous 44. Matthias T, Jeremias P, Neidhöfer S, Lerner A (2016) The industrial food
morphology: potential coeliac disease. APMIS 121: 266-271. additive microbial transglutaminase, mimics the tissue transglutaminase and is
38. Tursi A, Brandimarte G, Giorgetti GM (2003) Lack of usefulness of anti- immunogenic in celiac disease patients. Autoimm Rev 15: 1111-1119.
transglutaminase antibodies in assessing histologic recovery after gluten-free 45. Lerner A, Matthias T (2015) Food Industrial Microbial Transglutaminase in
diet in celiac disease. J Clin Gastroenterol 37: 387-391. Celiac Disease: Treat or Trick. Internat J Celiac Dis 3: 1-6.
39. Egner W, Shrimpton A, Sargur R, Patel D, Swallow K (2012) ESPGHAN
46. Lerner A, Matthias T (2015) Microbial transglutaminase is a potential
guidance on coeliac disease 2012: multiples of ULN for decision making do
environmental inducer of celiac disease. In: From Autoantibody Research
not harmonise assay performance across centres. J Pediatr Gastroenterol Nutr
55: 733-735. to Standardized Diagnostic Assays in the Management of Human Diseases.
Volume 10th, ed: K Conrad, Chan EKL, Andrade LEC, Steiner G, Pruijn GJM,
40. Lerner A, Jeremias P, Matthias T (2015) Outside of Normal Limits: False Y Shoenfeld. Page 227-23, Pabst Science Publishers, Lengerich, Germany,
Positive/Negative Anti TG2 Autoantibodies. Internat. J Celiac Dis 3: 87-90. e-pub.
41. Leffler DA, Schuppan D (2010) Update on serologic testing in celiac disease. 47. Lerner A, Matthias T (2015) Changes in intestinal tight junction permeability
Am J Gastroenterol 105: 2520-2524. associated with industrial food additives explain the rising incidence of
42. Guandalini S, Assiri A (2014) Celiac disease: a review. JAMA Pediatr 168: 272-278. autoimmune disease. Autoimm Rev 14: 479-489.
OMICS International: Open Access Publication Benefits &
Features
Unique features:
• Increased global visibility of articles through worldwide distribution and indexing
• Showcasing recent research output in a timely and updated manner
• Special issues on the current trends of scientific researche
Special features:
• 700+ Open Access Journals
• 50,000+ editorial team
• Rapid review process
• Quality and quick editorial, review and publication processing
• Indexing at major indexing services
• Sharing Option: Social Networking Enabled
Citation: Lerner A, Jeremias P, Neidhöfer S, Matthias T (2017) Comparison of • Authors, Reviewers and Editors rewarded with online Scientific Credits
• Better discount for your subsequent articles
the Reliability of 17 Celiac Disease Associated Bio-Markers to Reflect Intestinal Submit your manuscript at: http://www.omicsonline.org/submission
Damage. J Clin Cell Immunol 8: 486. doi: 10.4172/2155-9899.1000486
J Clin Cell Immunol, an open access journal
ISSN: 2155-9899 Volume 8 • Issue 1 • 1000486
View publication stats
You might also like
- Too Good To Be Truth PDFDocument84 pagesToo Good To Be Truth PDFivica_putNo ratings yet
- Urinary Tract Infection Case StudyDocument15 pagesUrinary Tract Infection Case StudyLeidi LheenNo ratings yet
- Office-Based Point of Care Testing (Iga/Igg-Deamidated Gliadin Peptide) For Celiac DiseaseDocument9 pagesOffice-Based Point of Care Testing (Iga/Igg-Deamidated Gliadin Peptide) For Celiac DiseasemarcosNo ratings yet
- Fecal Calprotectin in Combination With Standard Blood Tests in The Diagnosis of Inflammatory Bowel Disease in ChildrenDocument8 pagesFecal Calprotectin in Combination With Standard Blood Tests in The Diagnosis of Inflammatory Bowel Disease in ChildrenAngieda SoepartoNo ratings yet
- Accepted ManuscriptDocument29 pagesAccepted ManuscriptVlatka MartinovichNo ratings yet
- Akkermansia e AutismoDocument4 pagesAkkermansia e AutismoMariane MirandaNo ratings yet
- Applied and Environmental Microbiology-2011-Wang-6718.fullDocument4 pagesApplied and Environmental Microbiology-2011-Wang-6718.fullJorge AlvesNo ratings yet
- Office-Based Point of Care Testing (Iga/Igg-Deamidated Gliadin Peptide) For Celiac DiseaseDocument10 pagesOffice-Based Point of Care Testing (Iga/Igg-Deamidated Gliadin Peptide) For Celiac DiseaseGrecia BocuNo ratings yet
- WJG 19 2612Document9 pagesWJG 19 2612Tanima BiswasNo ratings yet
- Gene Expression of Adipokines and Inflammatory Cytokines in Peripheral Blood Mononuclear Cells of Obese DogsDocument7 pagesGene Expression of Adipokines and Inflammatory Cytokines in Peripheral Blood Mononuclear Cells of Obese DogsAna Luiza LeroyNo ratings yet
- RAS Dan AtopiDocument4 pagesRAS Dan AtopiDenker GailNo ratings yet
- Cow Milk AllergyDocument12 pagesCow Milk AllergyAbi ArifiNo ratings yet
- Faecal Calprotectin in Treated and Untreated Children With CoeliacDocument4 pagesFaecal Calprotectin in Treated and Untreated Children With CoeliacNejc KovačNo ratings yet
- 2017 Article 141 Part2Document5 pages2017 Article 141 Part2Karina MonasaNo ratings yet
- Fped 06 00350Document19 pagesFped 06 00350Jake DagupanNo ratings yet
- Aging and Periodontium PDFDocument8 pagesAging and Periodontium PDFsania jamilNo ratings yet
- Dinardo 2018Document7 pagesDinardo 2018Elaine IllescasNo ratings yet
- Brottveit 2013Document9 pagesBrottveit 2013posclinicaarquivoNo ratings yet
- Effect of N-Acetylcysteine On Inflammation Biomarkers in Pediatric Acute PyelonephritisDocument9 pagesEffect of N-Acetylcysteine On Inflammation Biomarkers in Pediatric Acute Pyelonephritisstrawberry cheesecakeNo ratings yet
- WJG 18 4470Document4 pagesWJG 18 4470Link BuiNo ratings yet
- Intestinal Barrier Breakdown and Mucosal Microbiota Disturbance in Neuromyelitis Optical Spectrum DisordersDocument15 pagesIntestinal Barrier Breakdown and Mucosal Microbiota Disturbance in Neuromyelitis Optical Spectrum DisordersmagarciacastilloNo ratings yet
- Gingivita Din Ciclul MenstrualDocument10 pagesGingivita Din Ciclul MenstrualRamonaNo ratings yet
- Artigo Global-Prevalence-Of-Celiac-DiseaseDocument16 pagesArtigo Global-Prevalence-Of-Celiac-DiseasesergiorizeteNo ratings yet
- Kidney Research and Clinical Practice: Jürgen FloegeDocument8 pagesKidney Research and Clinical Practice: Jürgen FloegeAnita PrastiwiNo ratings yet
- Clinical Guidelines Secondary Prevention of Gastric CancerDocument1 pageClinical Guidelines Secondary Prevention of Gastric Cancerhenrique.uouNo ratings yet
- Autoimmune Gastritis in Pediatrics A Review of 3.24Document6 pagesAutoimmune Gastritis in Pediatrics A Review of 3.24henrique.uouNo ratings yet
- Recommendations For Uniform Definitions Used in Newborn Screening For Severe Combined ImmunodeficiencyDocument9 pagesRecommendations For Uniform Definitions Used in Newborn Screening For Severe Combined ImmunodeficiencyZ. Raquel García OsornoNo ratings yet
- Efficiency of Direct Microscopy of Stool Samples Using An Antigen-Specific Adhesin Test For Entamoeba HistolyticaDocument5 pagesEfficiency of Direct Microscopy of Stool Samples Using An Antigen-Specific Adhesin Test For Entamoeba HistolyticaNoraine Princess TabangcoraNo ratings yet
- Medical Science: Gjra - Global Journal For Research Analysis X 4Document3 pagesMedical Science: Gjra - Global Journal For Research Analysis X 4ZulhamNo ratings yet
- Biosensors 08 00055 v2Document12 pagesBiosensors 08 00055 v2RedhaLavNo ratings yet
- Safety and Preliminary Efficacy On Cognitive Performance and Ada 2022 GenetiDocument10 pagesSafety and Preliminary Efficacy On Cognitive Performance and Ada 2022 Genetironaldquezada038No ratings yet
- Serologic Diagnosis of Tuberculosis Using A Simple Commercial Multiantigen AssayDocument6 pagesSerologic Diagnosis of Tuberculosis Using A Simple Commercial Multiantigen AssayTanveerNo ratings yet
- Effect of Lactobacillus Sakei Supplementation in Children With Atopic Eczema - Dermatitis SyndromeDocument6 pagesEffect of Lactobacillus Sakei Supplementation in Children With Atopic Eczema - Dermatitis SyndromePutri Halla ShaviraNo ratings yet
- Some Serum Cytokines in Celiac Disease, Non-CeliacDocument10 pagesSome Serum Cytokines in Celiac Disease, Non-CeliacCentral Asian StudiesNo ratings yet
- Ige in Infants With Laryngomalacia: Risk For Asthma Impact of Asa and Body Mass Index in Pediatric TonsillectomyDocument1 pageIge in Infants With Laryngomalacia: Risk For Asthma Impact of Asa and Body Mass Index in Pediatric TonsillectomyshoviNo ratings yet
- Recommendations For Appropriate Sublingual Immunotherapy Clinical TrialsDocument6 pagesRecommendations For Appropriate Sublingual Immunotherapy Clinical TrialstitatNo ratings yet
- Case-Finding in Primary Care For Coeliac Disease: Accuracy and Cost-Effectiveness of A Rapid Point-Of-Care TestDocument11 pagesCase-Finding in Primary Care For Coeliac Disease: Accuracy and Cost-Effectiveness of A Rapid Point-Of-Care TestmarcosNo ratings yet
- Association of Antioxidants and Vitamin D Level With Inflammation in Children With Atopic DermatitisDocument6 pagesAssociation of Antioxidants and Vitamin D Level With Inflammation in Children With Atopic DermatitisaditiarrtuguNo ratings yet
- Tear Levels of Interleukin (IL) 2 &4 in Patients With Allergic Conjunctivitis (Levels of Cytokines in Tear)Document5 pagesTear Levels of Interleukin (IL) 2 &4 in Patients With Allergic Conjunctivitis (Levels of Cytokines in Tear)International Journal of Innovative Science and Research TechnologyNo ratings yet
- Digest: Predictors of Failure of Pneumatic Dilatation in AchalasiaDocument3 pagesDigest: Predictors of Failure of Pneumatic Dilatation in AchalasiaDian Eka PermataNo ratings yet
- Fped 09 801955Document9 pagesFped 09 801955YandiNo ratings yet
- Samahsamir@hotmail Co UkDocument9 pagesSamahsamir@hotmail Co UkYuosra Amer AlhamadanyNo ratings yet
- IgM Pada ThypoidDocument4 pagesIgM Pada ThypoidririlibertiNo ratings yet
- 2019 Glomerulonefritis Pos-Inf Pedi Clin NADocument14 pages2019 Glomerulonefritis Pos-Inf Pedi Clin NA0511821012 KATHERIN YULEIMA CAMACHO MARIN ESTUDIANTE ACTIVONo ratings yet
- Pi Is 0016508522011921Document15 pagesPi Is 0016508522011921NaveedNo ratings yet
- Jurnal PedetDocument6 pagesJurnal PedetDesna Datu RaraNo ratings yet
- Gene Therapy Clinical Trials Worldwide To 2017 An UpdateDocument16 pagesGene Therapy Clinical Trials Worldwide To 2017 An UpdateLeonardo Sandi SalazarNo ratings yet
- Assessment of A Test For The Screening and Diagnosis of Celiac DiseaseDocument6 pagesAssessment of A Test For The Screening and Diagnosis of Celiac DiseasekameliasitorusNo ratings yet
- Comparision of 6 Diffrent Assays For CalprotectinDocument8 pagesComparision of 6 Diffrent Assays For CalprotectinrjgsmxyppbNo ratings yet
- Interpretation and implementation of the revised European Society for Paediatric Gastroenterology Hepatology and Nutrition (ESPGHAN) guidelines on pediatric celiac disease amongst consultant general pediatricians in Southwest of EnglandDocument8 pagesInterpretation and implementation of the revised European Society for Paediatric Gastroenterology Hepatology and Nutrition (ESPGHAN) guidelines on pediatric celiac disease amongst consultant general pediatricians in Southwest of EnglandJephte LaputNo ratings yet
- Neutrophil To Lymphocyte Ratio in Diagnosis of Complicated and Non-Complicated AppendicitisDocument7 pagesNeutrophil To Lymphocyte Ratio in Diagnosis of Complicated and Non-Complicated AppendicitisHamza AhmedNo ratings yet
- Faring It IsDocument8 pagesFaring It IsMuhammad sukronNo ratings yet
- Autoantibodies Against Complement C1q in Acute Post-Streptococcal GlomerulonephritisDocument6 pagesAutoantibodies Against Complement C1q in Acute Post-Streptococcal GlomerulonephritisRiasukmawatiNo ratings yet
- Acute Kidney Injury in ChildrenDocument8 pagesAcute Kidney Injury in ChildrenInfectologia ClinicaNo ratings yet
- Evaluation of Helicobacter Pylori Immunoglobulin GDocument4 pagesEvaluation of Helicobacter Pylori Immunoglobulin GRaffaharianggaraNo ratings yet
- Both Fecal Calprotectin and Imuno Test in Children IBDDocument13 pagesBoth Fecal Calprotectin and Imuno Test in Children IBDdichafrNo ratings yet
- IgA Nephropathy JournalDocument11 pagesIgA Nephropathy JournalerlisaNo ratings yet
- Amblyopia Risk Factors in Newborns With Congenital Nasolacrimal Duct ObstructionDocument5 pagesAmblyopia Risk Factors in Newborns With Congenital Nasolacrimal Duct ObstructionSyaiful UlumNo ratings yet
- 1471 230X 7 9 PDFDocument5 pages1471 230X 7 9 PDFivanhariachandraNo ratings yet
- Comparison Between Presepsin and Procalcitonin in Early Diagnosis of Neonatal SepsisDocument21 pagesComparison Between Presepsin and Procalcitonin in Early Diagnosis of Neonatal SepsisERIKA PAMELA SOLANO JIMENEZNo ratings yet
- Cathelicidin Level in Less in ARDocument6 pagesCathelicidin Level in Less in ARvishdubey777No ratings yet
- Endoscopy in Pediatric Inflammatory Bowel DiseaseFrom EverandEndoscopy in Pediatric Inflammatory Bowel DiseaseLuigi Dall'OglioNo ratings yet
- IFA Produktinfo Infectious Diseases GB 10.2015 SK 1Document28 pagesIFA Produktinfo Infectious Diseases GB 10.2015 SK 1siddhi divekarNo ratings yet
- HEV - Journal of Clinical Microbiology-2016-Norder-549.fullDocument7 pagesHEV - Journal of Clinical Microbiology-2016-Norder-549.fullsiddhi divekarNo ratings yet
- Chemiluminescence Immunoassay Clia Label Alkaline Phosphatase AlpDocument7 pagesChemiluminescence Immunoassay Clia Label Alkaline Phosphatase Alpsiddhi divekarNo ratings yet
- M3001-SNIBE Company Presentation-E150507-7mDocument62 pagesM3001-SNIBE Company Presentation-E150507-7msiddhi divekarNo ratings yet
- 1 s2.0 S0019483213000382 MainDocument10 pages1 s2.0 S0019483213000382 Mainsiddhi divekarNo ratings yet
- Behavior Intervention and Support Plan (BISP)Document5 pagesBehavior Intervention and Support Plan (BISP)api-379946201No ratings yet
- SICK BUILDING SYNDROME.17512001.Galih PDFDocument15 pagesSICK BUILDING SYNDROME.17512001.Galih PDFRezandi Zaki RizqiullahNo ratings yet
- Assessment of The EyesDocument32 pagesAssessment of The EyesArlyn MendenillaNo ratings yet
- 10 Msds Mepoxe ADocument4 pages10 Msds Mepoxe AAnto MaryadiNo ratings yet
- Ronald H. Roth, 1933-2005: in MemoriamDocument1 pageRonald H. Roth, 1933-2005: in MemoriamakanshaNo ratings yet
- CONSOL Form Oil WBDocument3 pagesCONSOL Form Oil WBimmanuel lumbantobingNo ratings yet
- Medical College List GujaratDocument1 pageMedical College List GujaratAjay Pal SinghNo ratings yet
- Office of The Family and Children'S OmbudsDocument79 pagesOffice of The Family and Children'S OmbudsKING 5 NewsNo ratings yet
- DNB Post MBBS Allotments - R2 2020 - State WiseDocument152 pagesDNB Post MBBS Allotments - R2 2020 - State WiseManeesh BalachandranNo ratings yet
- 2003 White PaperDocument26 pages2003 White PaperShreeNo ratings yet
- Assessment of Patients in Emergency DepartmentDocument22 pagesAssessment of Patients in Emergency DepartmentClaudine PadillonNo ratings yet
- Perpetua Nnamdi-Emmanuel's CVDocument4 pagesPerpetua Nnamdi-Emmanuel's CVAnyaogu PerpetuaNo ratings yet
- Orthodontics: Current Principles and Techniques, 5th EditionDocument1 pageOrthodontics: Current Principles and Techniques, 5th EditionHalley De Sousa AlvesNo ratings yet
- Georgia Pool Inspection FormDocument1 pageGeorgia Pool Inspection FormdivermedicNo ratings yet
- Additional Interview QuestionsDocument3 pagesAdditional Interview Questionsapi-347153077No ratings yet
- Pone 0245511Document13 pagesPone 0245511Dr-Akram HadiNo ratings yet
- TeksolDocument5 pagesTeksolniki fitraNo ratings yet
- d10 The Host-Parasite RelationshipDocument4 pagesd10 The Host-Parasite RelationshipMuhammad Bilal SaifulhaqNo ratings yet
- Group 10: 1. Describe The Journey of Shahnaz HussainDocument3 pagesGroup 10: 1. Describe The Journey of Shahnaz HussainShyamsunder SharmaNo ratings yet
- Biosafety SOPDocument4 pagesBiosafety SOPIsam SalehNo ratings yet
- Moving Stories - Chennai IEATSDocument14 pagesMoving Stories - Chennai IEATSAnshuma KshetrapalNo ratings yet
- Finance (Pay Cell) Department G.O.Ms - No.306, Dated 13 October 2017Document15 pagesFinance (Pay Cell) Department G.O.Ms - No.306, Dated 13 October 2017manikandan andiappanNo ratings yet
- Module 6-Key Attributes of Cost AnalysesDocument3 pagesModule 6-Key Attributes of Cost AnalysesLou CalderonNo ratings yet
- 06SMARTeZ Drug Stability Table Non USDocument2 pages06SMARTeZ Drug Stability Table Non USJessica Blaine BrumfieldNo ratings yet
- Changes To The Australian Government's Schools Chaplaincy ProgramDocument2 pagesChanges To The Australian Government's Schools Chaplaincy ProgramLatika M BourkeNo ratings yet
- Iecmd - November 2021Document97 pagesIecmd - November 2021Siti Hutami pratiwiNo ratings yet
- Bleaching With Without ReservoirsDocument8 pagesBleaching With Without ReservoirsBasil AlNo ratings yet
- MSDS Soda Ash DenseDocument14 pagesMSDS Soda Ash DenseNamanNo ratings yet