Professional Documents
Culture Documents
Female Pelvis
Female Pelvis
Uploaded by
palleti renuka0 ratings0% found this document useful (0 votes)
10 views7 pagesOriginal Title
female pelvis
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
10 views7 pagesFemale Pelvis
Female Pelvis
Uploaded by
palleti renukaCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 7
MUSCLES OF FEMALE PELVIS
The muscles of the female pelvis play crucial roles in
supporting pelvic organs, maintaining urinary and fecal
continence, and facilitating childbirth. Here’s an overview:
1.Levator ani muscles: These are a group of muscles that form
the pelvic floor. They include:
Pubococcygeus muscle: Runs from the pubis to the coccyx
and supports the pelvic organs.
Puborectalis muscle: Forms a sling around the rectum and
helps maintain fecal continence.
Iliococcygeus muscle: Extends from the ischial spine to the
coccyx and supports the pelvic organs.
2.Coccygeus muscle (Ischiococcygeus): Located posterior to
the levator ani muscles, it helps support the pelvic organs and
assists in maintaining fecal continence.
3.Obturator internus muscle: Originates from the pelvis and
inserts into the greater trochanter of the femur. It assists in the
external rotation of the thigh and stabilizes the hip joint.
4.Piriformis muscle: Runs from the sacrum to the greater
trochanter of the femur. It helps in the external rotation and
abduction of the hip joint.
5.Urogenital diaphragm muscles: These muscles are located in
the anterior part of the pelvis and include:
External urethral sphincter: Surrounds the urethra and helps
control urinary flow.
Deep transverse perineal muscle: Located below the external
urethral sphincter, it supports the pelvic floor and assists in
urinary continence.
6.Psoas major and minor muscles: These muscles originate
from the lumbar vertebrae and insert into the femur. They flex
the hip joint and contribute to stabilizing the pelvis.
7.Rectus abdominis muscle: While not specifically within the
pelvis, it plays a role in stabilizing the pelvis and trunk,
especially during activities like childbirth and heavy lifting.
These muscles work together to support the pelvic organs,
maintain continence, facilitate childbirth, and stabilize the
pelvis during movement. Dysfunction or weakness in these
muscles can lead to pelvic floor disorders such as urinary
incontinence, fecal incontinence, and pelvic organ prolapse.
Physical therapy and pelvic floor exercises are often
prescribed to strengthen these muscles and improve their
function.
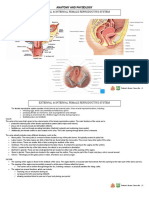
REPRODUCTIVE ORGANS IN FEMALE PELVIS
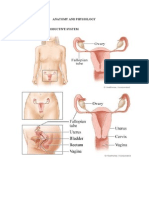
The female reproductive organs in the pelvis include:
Ovaries: Paired organs responsible for producing eggs (ova)
and hormones like estrogen and progesterone.
Fallopian Tubes (Uterine Tubes): Tubes that transport eggs
from the ovaries to the uterus. Fertilization typically occurs in
the fallopian tubes.
Uterus (Womb): A pear-shaped organ where a fertilized egg
implants and develops into a fetus during pregnancy.
Cervix: The lower portion of the uterus that connects it to the
vagina. It produces mucus that changes consistency
throughout the menstrual cycle to facilitate or prevent sperm
passage.
Vagina: A muscular canal that connects the uterus to the
outside of the body. It serves as the birth canal during delivery
and receives sperm during intercourse.
Vulva: The external genitalia, which includes the mons pubis,
labia majora, labia minora, clitoris, and vestibule (which
contains the openings of the urethra and vagina).
These organs work together in the female reproductive system
to facilitate ovulation, fertilization, pregnancy, and childbirth.
FEMALE PELVIC FLOOR
The female pelvic floor refers to a complex network of
muscles, ligaments, and connective tissues that support the
organs within the pelvis, including the bladder, uterus, and
rectum. It plays a crucial role in various bodily functions such
as supporting pelvic organs, maintaining urinary and fecal
continence, and facilitating sexual function.
1.Anatomy: The pelvic floor consists of several muscles
arranged in layers. The deepest layer includes the Levator ani
muscles, which include the pubococcygeus, iliococcygeus,
and puborectalis muscles. These muscles form a sling-like
structure that supports the pelvic organs.
2.Function: The pelvic floor muscles play a crucial role in
various bodily functions, including:
Supporting the pelvic organs and maintaining continence
(control over bladder and bowel movements).
Providing stability to the pelvis and spine.
Assisting in sexual function and childbirth by contracting
during orgasm and relaxing during childbirth.
3.Pelvic Floor Disorders: Dysfunction of the pelvic floor
muscles can lead to various conditions, including:
.Urinary incontinence: Involuntary leakage of urine.
Fecal incontinence: Involuntary leakage of stool.
Pelvic organ prolapse: Descent of one or more pelvic organs
(bladder, uterus, rectum) into the vaginal canal due to
weakened pelvic floor muscles.
Pelvic pain: Discomfort or pain in the pelvic region, often due
to muscle tension or dysfunction.
4.Causes of Dysfunction: Pelvic floor disorders can result
from several factors, including pregnancy and childbirth,
aging, hormonal changes, obesity, chronic constipation,
repetitive heavy lifting, and certain medical conditions or
surgeries.
5.Diagnosis and Treatment: Diagnosis of pelvic floor
disorders often involves a physical examination, medical
history review, and sometimes imaging tests like MRI or
ultrasound. Treatment options may include pelvic floor
muscle exercises (Kegels), lifestyle modifications, behavioral
therapies, medications, and in severe cases, surgery.
6.Preventive Measures: Maintaining a healthy lifestyle,
practicing pelvic floor exercises, maintaining a healthy
weight, and addressing any underlying medical conditions can
help prevent pelvic floor dysfunction.
7.Pelvic Floor Physical Therapy: Specialized physical therapy
can help strengthen and rehabilitate the pelvic floor muscles,
improve muscle coordination, and alleviate symptoms
associated with pelvic floor disorders.
Interdisciplinary Approach: Managing pelvic floor disorders
often requires a multidisciplinary approach involving
healthcare providers such as gynecologists, urologists,
colorectal surgeons, physical therapists, and psychologists to
address the complex nature of these conditions.
Overall, the female pelvic floor is a critical anatomical
structure with various functions, and maintaining its health is
essential for overall well-being and quality of life.
You might also like
- Transformation Leadership in A Digital Era: EY StrategyDocument24 pagesTransformation Leadership in A Digital Era: EY StrategyakashNo ratings yet
- Chapter 06 - Behind The Supply CurveDocument90 pagesChapter 06 - Behind The Supply CurveJuana Miguens RodriguezNo ratings yet
- Base PlateDocument45 pagesBase PlateMuhammed Ali60% (5)
- Female Pelvis111Document1 pageFemale Pelvis111palleti renukaNo ratings yet
- Peer-Tutorials Surgery I - 5Document21 pagesPeer-Tutorials Surgery I - 5mashe1No ratings yet
- Female PelvisDocument15 pagesFemale Pelvispalleti renukaNo ratings yet
- Pelvic Floor DysfunctionDocument17 pagesPelvic Floor DysfunctionLenny SucalditoNo ratings yet
- Vaginal TighteningDocument4 pagesVaginal TighteningnathanNo ratings yet
- Document Intro To Female PelvisDocument2 pagesDocument Intro To Female Pelvispalleti renukaNo ratings yet
- External StructuresDocument7 pagesExternal StructuressittizhainabNo ratings yet
- CBL 2Document20 pagesCBL 2Hammad AkramNo ratings yet
- Pandapatan Paler AnaPhyDocument3 pagesPandapatan Paler AnaPhyShara Lailanie A. AzisNo ratings yet
- The Bony Pelvi1Document3 pagesThe Bony Pelvi1jonaNo ratings yet
- Function: 1 Function 2 Clinical Significance 3 See Also 4 Additional Images 5 References 6 External LinksDocument3 pagesFunction: 1 Function 2 Clinical Significance 3 See Also 4 Additional Images 5 References 6 External LinksAmulya ShettyNo ratings yet
- Clinical OBGDocument33 pagesClinical OBGVarshiniNo ratings yet
- Definition of The DiseaseDocument17 pagesDefinition of The DiseaseLucille Jane Onlos CalibadanNo ratings yet
- Case StudyDocument23 pagesCase StudyLucero HyacinthNo ratings yet
- Hemorroid Shin2015Document9 pagesHemorroid Shin2015agusNo ratings yet
- Pelvic Floor ExercisesDocument5 pagesPelvic Floor ExercisesRaj MohanNo ratings yet
- Anatomi Panggul, Sistem Hormonal Dan Konsepsi: Ns. Dina Mariyana.,S.KepDocument56 pagesAnatomi Panggul, Sistem Hormonal Dan Konsepsi: Ns. Dina Mariyana.,S.KepAna KareniaNo ratings yet
- Question No 01: PART A) Define Pelvis?Document5 pagesQuestion No 01: PART A) Define Pelvis?aminaNo ratings yet
- MORANDocument3 pagesMORANCubillas P. DerNo ratings yet
- Operative Review TAHBSODocument22 pagesOperative Review TAHBSOGinger Enireht HTaibNo ratings yet
- Pelvic Floor: FunctionDocument4 pagesPelvic Floor: FunctionBéla JózsiNo ratings yet
- PUBOCOCCYGEUS: The Muscle of Sexual FunctionDocument8 pagesPUBOCOCCYGEUS: The Muscle of Sexual FunctionOspen Noah Sithole100% (1)
- Female Reproductive SystemDocument42 pagesFemale Reproductive SystemAhmie MarcosNo ratings yet
- Screenshot 2022-03-28 at 10.17.47 PMDocument127 pagesScreenshot 2022-03-28 at 10.17.47 PMqdvvqvxn7gNo ratings yet
- Reproductive SystemDocument34 pagesReproductive Systemsyifa alawiyahNo ratings yet
- Gender and Society CompileDocument32 pagesGender and Society Compileクイーンクイーン ロペスNo ratings yet
- Female Reproductive PresentationDocument70 pagesFemale Reproductive PresentationCristy Jean ApdianNo ratings yet
- Female Reproductive SystemDocument25 pagesFemale Reproductive SystemJay PornelaNo ratings yet
- Biology Assignment 1,2Document8 pagesBiology Assignment 1,2prasathindika312No ratings yet
- Anatomy and PhysiologyDocument8 pagesAnatomy and PhysiologyG3-PORTILLA John MartNo ratings yet
- Structure and Function of The Reproductive SystemDocument48 pagesStructure and Function of The Reproductive SystemJohnryl FranciscoNo ratings yet
- Share Anatomy and Physiology CASE STUDY (Edited)Document3 pagesShare Anatomy and Physiology CASE STUDY (Edited)Glyndee Marr JagonobNo ratings yet
- Group 4 - Nursing Care of The Pregnant Client - Pelvic Floor Diseases Written ReportDocument29 pagesGroup 4 - Nursing Care of The Pregnant Client - Pelvic Floor Diseases Written ReportJunghoon YangParkNo ratings yet
- Female Reproductive System (Human)Document21 pagesFemale Reproductive System (Human)RiazAhmedNo ratings yet
- The Human Reproductive System FinalDocument16 pagesThe Human Reproductive System FinalIlac Tristan BernardoNo ratings yet
- Female Reproductive System Anatomy and PhysiologyDocument5 pagesFemale Reproductive System Anatomy and PhysiologyIkea Balhon100% (3)
- Physiology 2024Document12 pagesPhysiology 2024Tawshiq HassanNo ratings yet
- How to Strengthen and Tone Your Pelvic Floor: A Comprehensive Guide for Vaginal HealthFrom EverandHow to Strengthen and Tone Your Pelvic Floor: A Comprehensive Guide for Vaginal HealthNo ratings yet
- Genito Urinary AssessmentDocument31 pagesGenito Urinary AssessmentMuskan RastogiNo ratings yet
- What Constitutes SexDocument9 pagesWhat Constitutes SexAlex GutierrezNo ratings yet
- Female PelvisDocument4 pagesFemale Pelvismuzammilsutar8No ratings yet
- 10FRSDocument27 pages10FRSWakanda ForeverNo ratings yet
- Female Reproductive System SlidesDocument30 pagesFemale Reproductive System SlidesNyakie MotlalaneNo ratings yet
- Lesson 4-Biomedical Perspective in Gender and SexualityDocument38 pagesLesson 4-Biomedical Perspective in Gender and SexualityDiana Hernandez100% (2)
- UterusDocument3 pagesUterusBernadette FlorendoNo ratings yet
- Anatomy of The Female Pelvis 1Document5 pagesAnatomy of The Female Pelvis 1DrPreeti Thakur ChouhanNo ratings yet
- Structure and Function of The Reproductive SystemDocument83 pagesStructure and Function of The Reproductive SystemMagy Tabisaura GuzmanNo ratings yet
- Male Reproductive Organs and Functions - The Online Physiology LibraryDocument3 pagesMale Reproductive Organs and Functions - The Online Physiology LibraryIsaac OnigbindeNo ratings yet
- Gender & Society Lo4Document6 pagesGender & Society Lo4Mark Eugene DeocampoNo ratings yet
- GENSOC M2 Lesson 4Document7 pagesGENSOC M2 Lesson 4cassy margaNo ratings yet
- Anatomy and PhysiologyDocument10 pagesAnatomy and PhysiologyBurni GuevaraNo ratings yet
- Gas Module 4 Lesson 1Document3 pagesGas Module 4 Lesson 1MARK 2020No ratings yet
- MCN NotesDocument71 pagesMCN NotesAbmil Ching TinggalongNo ratings yet
- Notes by R.....Document14 pagesNotes by R.....gauravpscpatnaNo ratings yet
- Lab Act in Repro.Document4 pagesLab Act in Repro.Jhia TorreonNo ratings yet
- Biology Female-Rep ReportingDocument30 pagesBiology Female-Rep ReportingDeniseNo ratings yet
- Female Reproductive SystemDocument9 pagesFemale Reproductive Systembyata pausanosNo ratings yet
- Introduction To Women HealthDocument47 pagesIntroduction To Women HealthDarren LimNo ratings yet
- Uterine Prolapse: Presented By-Pooja Soni MSC Final Year Student Department of Obstetrics & GynecologyDocument39 pagesUterine Prolapse: Presented By-Pooja Soni MSC Final Year Student Department of Obstetrics & Gynecologyannu panchalNo ratings yet
- Pop QDocument45 pagesPop QObgyn Maret2016No ratings yet
- Sonic Drive inDocument1 pageSonic Drive inWXYZ-TV Channel 7 DetroitNo ratings yet
- Final Year Project ReportDocument27 pagesFinal Year Project ReportVaibhav BokareNo ratings yet
- Triple Compliant, Lightweight, Flexible ArmorDocument1 pageTriple Compliant, Lightweight, Flexible ArmorvictoriaNo ratings yet
- Concrete Discharge Time (ASCC)Document1 pageConcrete Discharge Time (ASCC)V. ManilalNo ratings yet
- PT Dago Energi Nusantara TIME SHEET BULANAN KARYAWAN (26 Mar 2022 SD 25 Apr 2022)Document7 pagesPT Dago Energi Nusantara TIME SHEET BULANAN KARYAWAN (26 Mar 2022 SD 25 Apr 2022)muchamad luthfi aliNo ratings yet
- Eee Lab Manual Part I PDFDocument26 pagesEee Lab Manual Part I PDFramNo ratings yet
- Afoem Sample Paper Stage B Written Exam Paper 7Document43 pagesAfoem Sample Paper Stage B Written Exam Paper 7Caity YoungNo ratings yet
- GSM To UMTSDocument551 pagesGSM To UMTSFelicito ManzanoNo ratings yet
- Cardholder Dispute Form 2022 - MCDocument3 pagesCardholder Dispute Form 2022 - MCBigo.wifeNo ratings yet
- Vision, Mission, School Map and History of OLRADocument4 pagesVision, Mission, School Map and History of OLRAJowel Mercado RespicioNo ratings yet
- Densit General BrochureDocument5 pagesDensit General BrochureMuhammad IqbalNo ratings yet
- 4 SubstractorDocument4 pages4 SubstractorYidnekachwe MekuriaNo ratings yet
- 2 Concept Plan - Myanmar Workshop - Final PDFDocument0 pages2 Concept Plan - Myanmar Workshop - Final PDFmaungohsiNo ratings yet
- Using A ComputerDocument30 pagesUsing A ComputerJEEHANDSOME RANDOMNo ratings yet
- Contemporary Issues On Cash Waqf: A Review of The LiteratureDocument26 pagesContemporary Issues On Cash Waqf: A Review of The LiteratureSharifah NurulhudaNo ratings yet
- Charotar 9789385039126Document4 pagesCharotar 9789385039126Jayapal Rajan0% (1)
- Fiber Glass Reinforced HDDDocument8 pagesFiber Glass Reinforced HDDGilvan SilvaNo ratings yet
- Wartung Assyst Plus 204 enDocument32 pagesWartung Assyst Plus 204 enKent Wai100% (1)
- Gr10 Tenses Chapter Test ICSEDocument1 pageGr10 Tenses Chapter Test ICSEanirahul jtNo ratings yet
- The Adoption of The Principles of Equity Jurisprudence Into The ADocument12 pagesThe Adoption of The Principles of Equity Jurisprudence Into The AAjinkya PatilNo ratings yet
- GENG 3130 Sec 01 02 Syllabus Full 2022Document14 pagesGENG 3130 Sec 01 02 Syllabus Full 2022pass wordNo ratings yet
- Grade 7&8 Week 2Document18 pagesGrade 7&8 Week 2RUSELLE HOROHORONo ratings yet
- Who Was Howard Bowles Talking To On 26 Feb 2015 Australian Time, Mastercardantitrust-HearingtranscriptDocument62 pagesWho Was Howard Bowles Talking To On 26 Feb 2015 Australian Time, Mastercardantitrust-HearingtranscriptSenateBriberyInquiryNo ratings yet
- C2a. Logic SimplificationDocument53 pagesC2a. Logic SimplificationNicolaas LimNo ratings yet
- My Future My WayDocument44 pagesMy Future My Wayapi-450865694No ratings yet
- Ha H. Change Management For SustainabilityDocument172 pagesHa H. Change Management For SustainabilitySentinelNo ratings yet
- Mec 422 Lecture 4Document37 pagesMec 422 Lecture 4Zhen LinNo ratings yet