Professional Documents
Culture Documents
Urinary Elimination
Urinary Elimination
Uploaded by
ryamonamourofficial0 ratings0% found this document useful (0 votes)
10 views6 pagesCopyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
10 views6 pagesUrinary Elimination
Urinary Elimination
Uploaded by
ryamonamourofficialCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 6
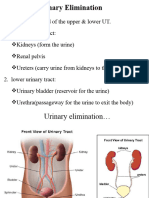
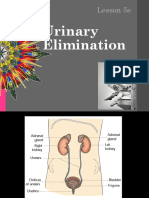
URINARY ELIMINATION Problems in Urinary elimination:
The major role is to maintain homeostasis by A. Altered Urine composition
maintaining body fluid composition and RBC Hematuria
volume. WBC Urinary
Tract
Micturition- is the act of expelling urine from
thebladder. ( also called urination or voiding). Pus Pyuria Infection
Bacteria Bacteriuria
- Refers to the process of emptying the urinary Albumin Albuminuria
bladder. Urine collects in the bladder until Protein Proteinuria
pressure stimulates special sensory nerve Casts Cylindriuria
endings in the bladder wall called the stretch Glucose Glycosuria
receptors. Ketones ketonuria Diabetic
ketoacidosis
The parasympathetic nervous system initiates
voiding. Whereas, the sympathetic nervous B. Altered Urine Production:
system inhibits voiding. The micturition reflex is 1. Polyuria – the production of excessive
involuntary, but it can be inhibited by higher amount of urine, such as more than
brain centers. 100ml/hr or 25,000 ml/ day ( also called
diuresis)
Factors affecting voiding:
2. Oliguria – the production of decreased
1. Developmental factors amount of urine, such as less than 30
a. infants- ml/hr or less than 500 ml/24 hours
b. preschoolers 3. Anuria – the absence of production of
c. school-age children urine by the kidneys such as 0 to 10
d. elders ml/hour ( also called urinary
2. Psychological factors- ex. Nurses-ignore the suppression
urge to void until they are able to have a break
C. Altered Urinary Frequency
3. Fluid and food intake- can change the color of
1. Frequency – voiding at frequent intervals that
the urine
is more than 4 to 6 times per day
4. Medications- diuretics- increase urine
2. Nocturia - increased frequency at night
formation; may alter color of the urine
3. Urgency – the strong feeling that the person
5. Muscle tone-
wants to void
6. Pathologic conditions-urinary stone- may
4. Dysuria – voiding that is either painful or
obstruct a ureter, blocking urine flow from
difficult
kidney to the bladder
5. Enuresis – repeated involuntary voiding
7. Surgical and diagnostics procedures-
beyond 4-5 years of age
cystoscopy
6. Pollakuria – frequent, scanty urination
Normal Characteristics of the Urine: 8. Urinary Incontinence:
Amount in 24hrs: 1,200-1500 ml a. Total urinary incontinence- a
Color: amber/straw continuous and unpredictable loss of
Odor: aromatic upon voiding urine
Transparency: Clear b. Stress urinary incontinence – the
Ph: slightly acidic (ranges: 4.6-8; average of 8) leakage of less than 50 ml of urine as a
Specific gravity: 1.010-1.025 (this is measured result of a sudden increase in intra-
by urinometer abdominal pressure
Glucose/ketone bodies (acetone)/blood: Not c. Urge urinary incontinence – follows a
Present sudden strong desire to urinate and
leads to involuntary detrusor
contraction ( overactive bladder ( Bethanecol) as ordered
syndrome) Last resort: Urinary catheterization .
d. Functional incontinence – the This is the last resort because it is one
involuntary unpredictable passage of of the most causes of nasocomial
urine infection. It is the introduction of a
e. Reflex incontinence – is an involuntary loss of catheter into the urinary bladder.
urine occuring at some what predictable
intervals when specific bladder volume is URINARY CATHETERIZATION
reached. Single catheterization: straight /nelaton
catheter
9. Urinary retention – the accumulation of urine Retention catheterization: 2 way Foley catheter
in the bladder with associated inability of the Continuous Bladder irrigation( Cystoclysis): 3
bladder to empty itself way Foleys Catheter
- 250-450 ml of urine in the bladder triggers PURPOSES:
micturition reflex 1. To relieve bladder distention
2. To instill medications into the bladder.
Clinical signs of urinary retention
3. To irrigate the bladder.
Discomfort in the pubic area 4. To measure hourly urine output
Bladder distention ( palpation and 5. To obtain a sterile urine specimen.
percussion) 6. To measure residual urine. Residual urine
- smooth, firm, ovoid mass at the suprapubic is the amount of urine retained in the bladder
area after forceful voiding.
- mass arising out of the pelvis 7. To manage incontinence when other
- dullness on percussion measures have failed
Inability to void or frequent voiding of 8. To promote healing of the genito-urinary
small structures post-operatively.
volumes ( 25-50 ml at a time) 9. To empty the bladder in preparation for
Disproportionately small amount of diagnostic procedures and surgery.
output in relation to fluid intake
Increasing restlessness and feeling of Equipments for Catheterization:
need to void
Sterile catheter of appropriate size
Nursing Interventions to induce Voiding:
Sizes: adult - #14, #16
Provide privacy. This is the most
children- #8 or #10
effective nursing measure to induce
Catheterization kit:
voiding.
1-2 pairs of sterile gloves
Provide fluids to drink.
sterile drapes
Assist the patient in the anatomical
antiseptic solution, cleansing balls, forceps,
position of voiding.
lubricant, sterile urine specimen container
Serve clean, warm and dry bedpan
(female) or urinal (male)
BOWEL ELIMINATION
Allow the patient to listen to the sound
of running water • DEFECATION – is the expulsion of feces
Dangle fingers in warm water. from the anus and rectum. It is also
Pour warm water over the perineum. called the bowel movement.
Promote relaxation
Provide adequate time for voiding Normal characteristic of the stool:
Perform Crede’s maneuver as ordered. Color: yellow or golden brown (due to the
This is done by applying pressure on the bile pigment derivative known as the stercobilin
suprapubic area. or fecal urobilinogen)
Administer cholinergics e.g. Urecholine Odor: aromatic upon defecation
Amount: depends on the bulk of the food Bulk Formers – they increase the bulk of the
intake. Approximately 150-300 g per day feces, increasing mechanical pressure and
Consistency: soft, formed distention of the intestine, thereby, increasing
Shape: cylindrical peristalsis e.g. Metamucil
Frequency: variable; usual range 1-2 per day
to 1 every 2-3 days • Stool softeners – they soften the stool
and facilitate its expulsion e. g. Colace
Alterations on the Characteristic of Stool:
• Osmotic agents – they attract fluids
• Acholic stool – gray, pale or clay- from the intestinal capillaries to the
colored stool due to absence of stool e.g. Milk of magnesia, Duphalac
stercobilin caused by biliary obstruction
2. FECAL IMPACTION – is the mass or collection
• Hematochezia – passage of stool with of hardened, putty-like feces in the folds of the
bright red blood due to lower rectum. The stool lodged or stuck in the rectum,
gastrointestinal bleeding the person is unable to voluntarily evacuate the
stool
• Melena – passage of black, tarry stool
due to upper gastrointestinal bleeding Nursing interventions to relieve Fecal
Impaction:
• Steatorrhea – greasy, bulky, foul Manual extraction or fecal disimpaction
smelling stool due to present of as ordered
undigested fats like in hepatobiliary- Increase fluid intake
pancreatic obstruction/disorder Sufficient bulk in diet
Common Fecal Elimination Problems: Adequate activity and exercise
1. CONSTIPATION – refers to the passage 3. DIARRHEA – refers to frequent evacuation of
of small, dry, hard stools or the passage watery stools. It is associated with increased
of no stool for a period of time. gastrointestinal motility, and a rapid passage of
fecal contents through the lower
• Nursing interventions to prevent and gastrointestinal tract
relieve constipation:
Adequate fluid intake Nursing interventions to relieve Diarrhea;
High fiber diet to provide bulk to the Replace fluid and electrolyte losses
stool Provide good perianal care. Diarrhea
Establish regular pattern of defecation stool is often times highly acidic which
Respond immediately to the urge to causes anal soreness and irritation in
defecate the perianal care.
Minimize stress To promote rest; to reduce peristalsis
Adequate activity and exercise promote Diet: small amount of bland diet
muscle tone and facilitate peristalsis Low fiber diet
Assume sitting or semi-squatting BRAT diet (banana, rice am, apple,
position toast
Administer laxatives as ordered Avoid excessive hot or cold fluids, these
are stimulants
Types of laxatives: Potassium rich foods and fluid e.g.
banana, gatorade
Chemical irritants – they provide chemical
Antidiarrheal mediations as ordered:
stimulation to intestinal wall, thereby increasing
perisitalsis, e.g. Dulcolax, castor oil,senakot • Demulcents – mechanically coat the
irritated bowel and act as protectives
Stool lubricants – they lubricate feces and
facilitate the expulsion e.g. mineral oil • Absorbents – absorbs gas or toxic
substances from the bowel
• Astringents – shrink swollen or Enema – is a solution introduced into the
inflamed tissues in the bowel rectum and large intestine. The action of the
enema is to distend the intestine sometimes to
CAUTION: Do not administer antidiarrheal at irritate the intestinal mucosa , thereby increase
the start of diarrhea. peristalsis and excretion of feces and flatus.
4. FLATULENCE – is the presence of excessive TYPES:
gas in the intestines, this may be due to 1. Cleansing enema
swallowed air, bacterial action in the large 2. Carminative enema
intestine and diffusion from blood 3. Retention enema
Common causes of flatulence: 4. Return- flow enema
• Constipation PURPOSES:
• Codeine, barbiturates and other 1. To relieve constipation
medications that decrease intestinal 2. To relieve flatulence
motility 3. To administer medication
• Anxiety 4. To evacuate feces in preparation for
• Eating gas forming foods e.g. cabbage, diagnostic procedure or surgery
legumes, root crops
• Rapid food or fluid ingestion CONTRAINDICATION:
• Excessive drinking of carbonated 1. Appendicitis
beverages 2. Intestinal obstruction
• Improper use of straw 3. Increase intracranial pressure
• Gum chewing, candy sucking, smoking
• Abdominal surgery- causes decreased TYPES
peristalsis 1. Cleansing enema – intended to remove
feces, stimulates peristalsis by irritating
Nursing Interventions: the colon and rectum and or by
• Avoid gas forming foods distending the intestine with the
• Provide warm fluids to drink- increase volume of fluid introduced. It is given
peristalsis chiefly to:
• Adequate activity and exercise Prevent the escape of feces during
• Limit carbonated beverages, use of surgery
straws and chewing gums Prepare the intestine for certain
• Rectal tube insertion as ordered. Place diagnostic tests such as x-ray or
client in left lateral position. Insert 3-4 visualization test ( colonoscopy)
inches of the lubricated rectal tube, Remove feces in instances of
gently in rotating motion. Use rectal constipation and impaction.
tube Fr. 22-30. Retain rectal tube for a
maximum of 30 minutes Commonly used solutions:
• Carminative enema as ordered Hypertonic – saline
• administer cholinergics s ordered e.g. Hypertonic enema – fleet phosphate enema
prostigmin Hypotonic – tap water
Isotonic – normal saline
5. FECAL INCONTINENCE is the involuntary Soap suds –irritates mucosa, distends colon
elimination of bowel contents; often associated Mineral oil – lubricates the feces and the
with neurologic, mental, or emotional colonic mucosa
impairments due to dysfunction of the anal Catminative enema
sphincter e.g. spinal cord injury clients-
impaired nerve supply to the rectum & A. High enema – is given to cleanse as
sphincter much of the colon as possible , client
should be in left lateral position to the
ADMINISTERING ENEMAS: dorsal recumbent then to the right
lateral so that the solution can follow NON-RETENTION ENEMA
the large intestine; 1000 ml 0f solution Solutions used are as follows:
o Tap water (500-1000 ml)
B. low enema – is used to clean the
o Soap suds ( 9 20 ml of castile soap in
rectum and sigmoid colon only; client
500-1000 ml of water)
maintains left lateral position during
o Normal Saline solution ( 9 ml of NaCl to
administration. 500ml of solution is
1000 ml of water)
introduced
o Hypertonic solution /fleet enema (90-
The force of flow is governed by: 120 ml)
Height of solution
a. Height of solution container – 30 to 49 o 18 inches above the rectum
cm (12 to 18 in) – the higher the faster Temperature of solution
o 115°-125° F
b. Size of the tubing- larger size, the faster
Time of retention
c. Viscosity of the fluid- thicker, slower o 5-10 minutes for better cleansing effect
d. Resistance of the rectum -+= slower RETENTION ENEMA
Solutions
2. Carminative enema – to expel flatus
o Carminative enema
- The solution instilled into the rectum o Oil (90-120 ml of mineral oil, olive oil or
releases gas, which in turn distends the cottonseed oil)
rectum and the colon thus stimulating Height of solution
peristalsis. For an adult, 60-80 ml of o 12 inches above the rectum
fluid is instilled Temperature of solution
o 105˚-110˚ F
3. Retention enema – introduces oil or Time of retention
medication into the rectum and sigmoid colon; o 1-3 hours until desired therapeutic
oil is retained in 1-3 hours, acts to soften the effect is obtained
feces and lubricates the rectum and anal canal,
facilitate passage of feces GUIDELINES FOR ADMINISTERING ENEMA:
4. Return-flow enema – is used occasionally Suggested Maximum Volumes
used to expel flatus Infant 150 to 250 ml
Toddler 250 to 350ml
• Harris Flush/ Colonic Irrigation School –age 300 to 500 ml
• 100-200 ml of fluid is introduced into Adolescent 500 to 750 ml
and out of the large intestine to Adult 750 to 1000 ml
stimulate peristalsis and to promote Suggested temperature of Solution
expulsion of flatus
Child 37.7 C (105 to 110 F)
• The solution container is lowered so
that the fluid backs out through the Adult 40-43 C ( 105 to 110 F)
rectal tube into the container.
Retention Enema 33 C ( 91 F )
• The inflow –outflow process is repeated
Suggested Rectal Tube Size
5-6 times
Infant/ Small Children 10 – 12 Fr
• Replace the solution several times
during the procedure as it becomes Child 12-18 Fr
thick with feces
Adult 22-30 Fr
• May take 15-20 minutes to be effective
Length of Insertion
Infant 1-1.5 inches
Child 2-3 inches
Adult 3-4 inches
Height of Enema Container
High Enema 18 inches
Low enema 12 inches
Infant 3 inches
Position for administration
Adult Left side lying (sim’s) position
with right knee flexed
Child Dorsal recumbent
Clients with Bedpan in comfortable dorsal
poor sphincter recumbent position
control
You might also like
- Invention and Evolution Design in Nature and EngineeringDocument387 pagesInvention and Evolution Design in Nature and Engineeringphucborso1100% (1)
- Nursing Care PlanDocument2 pagesNursing Care Planmjoie_baby6568470100% (6)
- Shark Dichotomous KeyDocument5 pagesShark Dichotomous KeyReviroda AnsayNo ratings yet
- CARIOLOGYDocument77 pagesCARIOLOGYteklay100% (3)
- Types of Microscopes Comparison Chart 4 Linear Venn Edit Answer KeyDocument2 pagesTypes of Microscopes Comparison Chart 4 Linear Venn Edit Answer KeyKLRSantosNo ratings yet
- Urinary Elimination: (Midterm)Document14 pagesUrinary Elimination: (Midterm)Mina RacadioNo ratings yet
- EliminationDocument7 pagesEliminationRoldan Andaya RamosNo ratings yet
- Elimination NeedsDocument52 pagesElimination NeedsKhadija JaraNo ratings yet
- UrinaryDocument3 pagesUrinaryAlyssa Jade GolezNo ratings yet
- UrinaryDocument3 pagesUrinaryAlyssa Jade GolezNo ratings yet
- Elimination - Urinary and BowelDocument58 pagesElimination - Urinary and BowelAnn A.No ratings yet
- CatheterizationDocument14 pagesCatheterizationV_RNNo ratings yet
- EliminationDocument128 pagesEliminationhailye mitikeNo ratings yet
- Elimination Needs 04Document52 pagesElimination Needs 04Kishore RathoreNo ratings yet
- Urinary Elimination: Four Major Parts of Urinary SystemDocument17 pagesUrinary Elimination: Four Major Parts of Urinary SystemMabes100% (2)
- Funda SL FinalsDocument3 pagesFunda SL FinalsKarylle Joy ValenciaNo ratings yet
- Bladder & Bowel Elimination PDFDocument37 pagesBladder & Bowel Elimination PDFSwarna JayarathnaNo ratings yet
- Urinary Elimination: Ra'eda Almashaqba 1Document8 pagesUrinary Elimination: Ra'eda Almashaqba 1Suneel Kumar PrajapatiNo ratings yet
- TolitsDocument42 pagesTolitsAzela TuzonNo ratings yet
- Group Iv - Urinary Elimination PDFDocument96 pagesGroup Iv - Urinary Elimination PDFMeshezabel AsentistaNo ratings yet
- Benign Prostatic Hyperplasia. NCM 109Document16 pagesBenign Prostatic Hyperplasia. NCM 109Niña Jean Tormis AldabaNo ratings yet
- EliminationDocument20 pagesEliminationHasan A AsFour100% (2)
- B Inggris NurulDocument35 pagesB Inggris NurulUcokNo ratings yet
- Urinary Elimination: Ra'eda Almashaqba 1Document9 pagesUrinary Elimination: Ra'eda Almashaqba 1JP AtrashiNo ratings yet
- Urinary EliminationDocument64 pagesUrinary EliminationAbdurehman AyeleNo ratings yet
- Inkontinensia UrinDocument24 pagesInkontinensia UrinBenny Wegah Nulis100% (9)
- Concept of EliminationDocument42 pagesConcept of EliminationOpen UserNo ratings yet
- Urinary Elimination BY AMNA AZKA BSN NURSINGDocument26 pagesUrinary Elimination BY AMNA AZKA BSN NURSINGmuhammad abdullah javedNo ratings yet
- Fundamental of Nursing: Unit Eleven and TwelveDocument45 pagesFundamental of Nursing: Unit Eleven and Twelveጀኔራል አሳምነው ፅጌNo ratings yet
- Renal and Genitourinary ConditionsDocument139 pagesRenal and Genitourinary ConditionsjustinahorroNo ratings yet
- Urinary Elimination: Prepared By: Lemuel C. Macasa, RNDocument30 pagesUrinary Elimination: Prepared By: Lemuel C. Macasa, RNRoger ViloNo ratings yet
- Urinary Tract Changes in Older AdultDocument14 pagesUrinary Tract Changes in Older AdultMarens AfallaNo ratings yet
- MNT in Diseases of Kidney and UrinaryDocument38 pagesMNT in Diseases of Kidney and UrinaryJosephine A. Bertulfo100% (1)
- UriiiiiDocument24 pagesUriiiiiI-land fanNo ratings yet
- Chapter 44 - Urinary FrequencyDocument5 pagesChapter 44 - Urinary FrequencyJonalyn MejellanoNo ratings yet
- Urinary Elimination: Lesson 5eDocument33 pagesUrinary Elimination: Lesson 5eMikhaela Andree MarianoNo ratings yet
- Urinary EliminationDocument7 pagesUrinary EliminationwowsamanthaNo ratings yet
- Urinary Elimination: Lesson 5eDocument33 pagesUrinary Elimination: Lesson 5eMikhaela Andree MarianoNo ratings yet
- Disorders of The Genitourinary SystemDocument100 pagesDisorders of The Genitourinary SystemMurti GutoNo ratings yet
- Anatomy and PhysiologyDocument5 pagesAnatomy and PhysiologyAndrye Pelita ZamZam MubaroqNo ratings yet
- Fisiologi BerkemihDocument34 pagesFisiologi BerkemihTunik SugiantoNo ratings yet
- Chapter 45 Urinary EliminationDocument29 pagesChapter 45 Urinary EliminationKwenaNo ratings yet
- Computation of Urine OutputDocument4 pagesComputation of Urine OutputKassandra LabeNo ratings yet
- Detrusor InstabilityDocument7 pagesDetrusor Instabilityapi-3705046No ratings yet
- Bowel EliminationDocument3 pagesBowel EliminationPilacan KarylNo ratings yet
- MS Renal ReviewerDocument9 pagesMS Renal ReviewerSANCHEZ, BEA LYKA A.No ratings yet
- Neurogenic Bladder: Mobility Clinic Case-Based Learning ModuleDocument11 pagesNeurogenic Bladder: Mobility Clinic Case-Based Learning ModuleJamaicaNo ratings yet
- Urinary SystemDocument27 pagesUrinary Systemtareqhaddad123No ratings yet
- Urinary EliminationDocument101 pagesUrinary EliminationJade Giordano100% (1)
- Structures and Functions of Urinary SystemDocument6 pagesStructures and Functions of Urinary Systemمالك مناصرةNo ratings yet
- Urinary IncontineceDocument41 pagesUrinary IncontineceYazeed Asrawi100% (2)
- RENAL SYSTEM Handouts For IloiloDocument19 pagesRENAL SYSTEM Handouts For IloiloPrecious UncianoNo ratings yet
- WK4 - Urinary CatheterizationDocument6 pagesWK4 - Urinary Catheterizationkristelaaa guevarraNo ratings yet
- Group-5 NCM-107 NCPDocument4 pagesGroup-5 NCM-107 NCPbulok netflakes100% (1)
- Bladder Atony/Urinary RetentionDocument11 pagesBladder Atony/Urinary RetentionAngela CaguitlaNo ratings yet
- PEDIA 4.1 NephrologyDocument7 pagesPEDIA 4.1 NephrologyAngela CaguitlaNo ratings yet
- Urinary CatheterizationDocument17 pagesUrinary CatheterizationLeofe CorregidorNo ratings yet
- Triptico ITUDocument2 pagesTriptico ITUClaudi Tperez0% (1)
- UrinaryRetention 508Document8 pagesUrinaryRetention 508earldioborrinagaNo ratings yet
- Hematuria, (Blood in Urine) A Simple Guide to The Condition, Related Diseases And Use in Diagnosis of DiseasesFrom EverandHematuria, (Blood in Urine) A Simple Guide to The Condition, Related Diseases And Use in Diagnosis of DiseasesRating: 5 out of 5 stars5/5 (2)
- A Simple Guide To Nocturia, (Excessive Night Urination) Diagnosis, Treatment And Related ConditionsFrom EverandA Simple Guide To Nocturia, (Excessive Night Urination) Diagnosis, Treatment And Related ConditionsNo ratings yet
- Ascites, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandAscites, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- 9700 s07 QP 4Document24 pages9700 s07 QP 4CindyVortexNo ratings yet
- Enzyme Application in The Textile IndustryDocument14 pagesEnzyme Application in The Textile IndustryFie100% (1)
- When A Women Picks Up An Apple and Bits ItDocument1 pageWhen A Women Picks Up An Apple and Bits ItDanial2296No ratings yet
- Yarncraft and Cognition - Creativity and Cognition 2017Document2 pagesYarncraft and Cognition - Creativity and Cognition 2017Andrew Quitmeyer100% (1)
- Humastar300sr enDocument3 pagesHumastar300sr enNghi NguyenNo ratings yet
- 8725-300 Psa Xs Accubind Elisa Rev 0Document2 pages8725-300 Psa Xs Accubind Elisa Rev 0dr madhusudhan reddyNo ratings yet
- The Biological Revolution: Periodicals of Engineering and Natural Sciences Vol. 3 No. 1 (2015) Available Online atDocument2 pagesThe Biological Revolution: Periodicals of Engineering and Natural Sciences Vol. 3 No. 1 (2015) Available Online atAngel TaylorNo ratings yet
- Transport in PlantsDocument12 pagesTransport in PlantsMEME KA GHANTANo ratings yet
- Pex 08 01Document4 pagesPex 08 01Rafi SalimNo ratings yet
- Caplan Deron 201808 PHD CannabisDocument158 pagesCaplan Deron 201808 PHD CannabisMihai SimionNo ratings yet
- GCLP Guidelines 2020 FinalDocument78 pagesGCLP Guidelines 2020 FinalGyanuNo ratings yet
- Full Time Member, State Planning Commission, Government of Tamil NaduDocument5 pagesFull Time Member, State Planning Commission, Government of Tamil NadughurukumarNo ratings yet
- Gordon Research ConferencesDocument178 pagesGordon Research ConferencesMamadou Moustapha Sarr100% (1)
- Determination of Ibuprofen and Paraben in Pharmaceutical Formulations Using Flowinjection and Derivative SpectrophotometryDocument2 pagesDetermination of Ibuprofen and Paraben in Pharmaceutical Formulations Using Flowinjection and Derivative Spectrophotometrycamelia_ioana_14No ratings yet
- Relevance of Menarche, Menopause, and Other Bioevent To FertilityDocument3 pagesRelevance of Menarche, Menopause, and Other Bioevent To FertilitydattaniranjanNo ratings yet
- General Science Ability NotesDocument25 pagesGeneral Science Ability NotesZulfiqar Ali TunioNo ratings yet
- Histogenesis of Salivary Gland NeoplasmsDocument18 pagesHistogenesis of Salivary Gland Neoplasmsporkodi sudhaNo ratings yet
- Review: Zebrafish (Danio Rerio) Sebagai Model Obesitas Dan Diabetes Melitus Tipe 2Document12 pagesReview: Zebrafish (Danio Rerio) Sebagai Model Obesitas Dan Diabetes Melitus Tipe 2GREESTYNo ratings yet
- EcoCRM A Recombinant CRM197 Carrier ProteinDocument1 pageEcoCRM A Recombinant CRM197 Carrier ProteinRamakrishnaNo ratings yet
- Association Between Cortisol, Insulin Resistance and ZincDocument8 pagesAssociation Between Cortisol, Insulin Resistance and ZincEzard DavidNo ratings yet
- Short Takes On Three Books - American ScientistDocument6 pagesShort Takes On Three Books - American ScientistRay MondoNo ratings yet
- Free Download Human Aging Calogero Caruso Full Chapter PDFDocument51 pagesFree Download Human Aging Calogero Caruso Full Chapter PDFnola.rodriguez670100% (20)
- Southwick2017 Chapter LeadershipAndResilienceDocument19 pagesSouthwick2017 Chapter LeadershipAndResilienceUrsula MancusoNo ratings yet
- ID Identifikasi Jenis Alga Koralin Di PulauDocument4 pagesID Identifikasi Jenis Alga Koralin Di PulauEndoIeNo ratings yet
- نباتاتDocument2 pagesنباتاتhaneen refaeeNo ratings yet
- Intro - EstroG-100 Pres FullDocument60 pagesIntro - EstroG-100 Pres FulllilingNo ratings yet