Professional Documents
Culture Documents
Pi Is 0002937812001317
Pi Is 0002937812001317
Uploaded by
harold.atmajaCopyright:
Available Formats
You might also like
- Sample Food Inspection ReportDocument3 pagesSample Food Inspection ReportCityNewsToronto75% (4)
- Beach Lifeguard: ManualDocument72 pagesBeach Lifeguard: ManualLuis ZapataNo ratings yet
- Journal 4Document13 pagesJournal 4intan wahyuNo ratings yet
- Nursing Research PaperDocument24 pagesNursing Research Paperapi-455624162No ratings yet
- PIIS0002937813009320Document7 pagesPIIS0002937813009320harold.atmajaNo ratings yet
- Outcome of Teenage PregnancyDocument4 pagesOutcome of Teenage PregnancyMALIK MANASRAHNo ratings yet
- Calderon Margalit2009Document8 pagesCalderon Margalit2009Aulya ArchuletaNo ratings yet
- Adverse Birth Outcomes Women With ‘ - LoDocument12 pagesAdverse Birth Outcomes Women With ‘ - Loshubh cards bhilwara Wedding cardsNo ratings yet
- Ajmw 2016 10 4 169Document10 pagesAjmw 2016 10 4 169Faouz AbNo ratings yet
- Unintended Pregnancy, Prenatal Care, Newborn Outcomes, and Breastfeeding in Women With EpilepsyDocument10 pagesUnintended Pregnancy, Prenatal Care, Newborn Outcomes, and Breastfeeding in Women With EpilepsyasfwegereNo ratings yet
- Mental Health Impact On The Unmet Need For Family Planning and Fertility Rate in Rural Ethiopia: A Population-Based Cohort StudyDocument10 pagesMental Health Impact On The Unmet Need For Family Planning and Fertility Rate in Rural Ethiopia: A Population-Based Cohort Studydiya desaiNo ratings yet
- Nejme2032499 PDFDocument2 pagesNejme2032499 PDFBladimir CentenoNo ratings yet
- Association of Self-Reported Adherence and AntiretDocument2 pagesAssociation of Self-Reported Adherence and AntiretDavidNo ratings yet
- Articles: BackgroundDocument12 pagesArticles: BackgroundChristian YzaguirreNo ratings yet
- Bjo12636 PDFDocument9 pagesBjo12636 PDFLuphly TaluvtaNo ratings yet
- Artikel 2 DheaDocument16 pagesArtikel 2 Dheadayana nopridaNo ratings yet
- Depression Among CD and VDDocument7 pagesDepression Among CD and VDnoam tiroshNo ratings yet
- A Case Control Study of Risk Factors and Neonatal Outcomes of Preterm BirthDocument5 pagesA Case Control Study of Risk Factors and Neonatal Outcomes of Preterm BirthSarahí SosaNo ratings yet
- ArticleDocument8 pagesArticleAstrid Abrahams PakelNo ratings yet
- Promoting Safe Prescribing in Primary Care With A Contraceptive Vital Sign: A Cluster-Randomized Controlled TrialDocument7 pagesPromoting Safe Prescribing in Primary Care With A Contraceptive Vital Sign: A Cluster-Randomized Controlled TrialDookNo ratings yet
- D'Souza-2019-Maternal Body Mass Index and PregDocument17 pagesD'Souza-2019-Maternal Body Mass Index and PregMARIATUL QIFTIYAHNo ratings yet
- Muest RaDocument13 pagesMuest RaBruno LinoNo ratings yet
- Chapter 2 Burden of Reproductive Ill HealthDocument38 pagesChapter 2 Burden of Reproductive Ill HealthFakhira Adzkiya SalsabilaNo ratings yet
- HHS Public Access: Child Neurodevelopmental Outcomes by Prepregnancy Body Mass Index and Gestational Weight GainDocument18 pagesHHS Public Access: Child Neurodevelopmental Outcomes by Prepregnancy Body Mass Index and Gestational Weight GainAndres GallegosNo ratings yet
- Hunt-Gibbon SUM 2019Document34 pagesHunt-Gibbon SUM 2019fatimaNo ratings yet
- Best 1Document7 pagesBest 1Wondwosen AsegidewNo ratings yet
- Pregnancy Complications and Outcomes in Women With Epilepsy: Mirzaei Fatemeh, Ebrahimi B. NazaninDocument5 pagesPregnancy Complications and Outcomes in Women With Epilepsy: Mirzaei Fatemeh, Ebrahimi B. NazaninMentari SetiawatiNo ratings yet
- PDF MaternityCarePtEngagementStrategiesIHADocument29 pagesPDF MaternityCarePtEngagementStrategiesIHAv_ratNo ratings yet
- Pregnancy and Childbirth Outcomes Among Adolescent Mothers: A World Health Organization Multicountry StudyDocument9 pagesPregnancy and Childbirth Outcomes Among Adolescent Mothers: A World Health Organization Multicountry StudyMahyudin SimarokoNo ratings yet
- Disrupting The Pathways of Social Determinants ofDocument10 pagesDisrupting The Pathways of Social Determinants ofIGA ABRAHAMNo ratings yet
- Piis0002937809020031 PDFDocument6 pagesPiis0002937809020031 PDFRaisa AriesthaNo ratings yet
- BMJ Open-2014-LiDocument16 pagesBMJ Open-2014-LiMarianaafiatiNo ratings yet
- The Conext of Unintended Pregnancy Among Married WDocument11 pagesThe Conext of Unintended Pregnancy Among Married WRose RoseNo ratings yet
- Depression Among Pregnant Women and Associated Factors in Hawassa City, Ethiopia: An Institution-Based Cross-Sectional StudyDocument6 pagesDepression Among Pregnant Women and Associated Factors in Hawassa City, Ethiopia: An Institution-Based Cross-Sectional Studyevita juniarNo ratings yet
- Emergency Contraception: Knowledge and Attitudes of Family Physicians of A Teaching Hospital, Karachi, PakistanDocument6 pagesEmergency Contraception: Knowledge and Attitudes of Family Physicians of A Teaching Hospital, Karachi, PakistanNaveed AhmadNo ratings yet
- The Worldwide Incidence of Preterm Birth: A Systematic Review of Maternal Mortality and MorbidityDocument8 pagesThe Worldwide Incidence of Preterm Birth: A Systematic Review of Maternal Mortality and MorbidityAnalia ZeinNo ratings yet
- Koren. Fetal Safety of DYD in 1st Trimester PregnancyDocument5 pagesKoren. Fetal Safety of DYD in 1st Trimester PregnancyRuth RachmawatyNo ratings yet
- 33873-Article Text-121761-1-10-20170831Document6 pages33873-Article Text-121761-1-10-20170831AnggaNo ratings yet
- Factors Influencing Contraceptive Uptake Among Lactating Mothers (6-24 Months) - A Case Study of 2medical Reception Station (2MRS)Document7 pagesFactors Influencing Contraceptive Uptake Among Lactating Mothers (6-24 Months) - A Case Study of 2medical Reception Station (2MRS)NanaKarikariMintahNo ratings yet
- Mental HealthDocument7 pagesMental HealthMirjana14No ratings yet
- Exploring Women Knowledge of Newborn Danger Signs: A Case of Mothers With Under Five ChildrenDocument8 pagesExploring Women Knowledge of Newborn Danger Signs: A Case of Mothers With Under Five ChildrenJohnjohn MateoNo ratings yet
- JAMA Ophthalmology Volume Issue 2018 (Doi 10.1001 - Jamaophthalmol.2018.2753) Binenbaum, Gil Bell, Edward F. Donohue, Pamela Quinn, Graham - Development of Modified Screening Criteria For Retinop PDFDocument7 pagesJAMA Ophthalmology Volume Issue 2018 (Doi 10.1001 - Jamaophthalmol.2018.2753) Binenbaum, Gil Bell, Edward F. Donohue, Pamela Quinn, Graham - Development of Modified Screening Criteria For Retinop PDFKarthik CNo ratings yet
- Risk Factors For Neonatal Asphyxia Occurrence at General Hospital Dr. M. Soewandhie, SurabayaDocument6 pagesRisk Factors For Neonatal Asphyxia Occurrence at General Hospital Dr. M. Soewandhie, SurabayaFatimah FadilahNo ratings yet
- Pi Is 0002937813005139Document5 pagesPi Is 0002937813005139fenskaNo ratings yet
- Antenatal Dexamethasone For Early Preterm Birth in Low-Resource CountriesDocument12 pagesAntenatal Dexamethasone For Early Preterm Birth in Low-Resource CountriesMemento MoriNo ratings yet
- 2018-BJOG An International Journal of Obstetrics & GynaecologyDocument40 pages2018-BJOG An International Journal of Obstetrics & GynaecologyBagusHibridaNo ratings yet
- 80 (11) 871 1 PDFDocument5 pages80 (11) 871 1 PDFMahlina Nur LailiNo ratings yet
- Intl J Eating Disorders - 2013 - Linna - Reproductive Health Outcomes in Eating DisordersDocument8 pagesIntl J Eating Disorders - 2013 - Linna - Reproductive Health Outcomes in Eating Disordersdarkleaf03No ratings yet
- Weight Gain and Menstrual Abnormalities Between Users of Depo-Provera and NoristeratDocument6 pagesWeight Gain and Menstrual Abnormalities Between Users of Depo-Provera and NoristeratMauricio Lopez MejiaNo ratings yet
- E011705 FullDocument11 pagesE011705 Fullhellen-borgesNo ratings yet
- Geist 2006Document5 pagesGeist 2006Marifer EstradaNo ratings yet
- Maternal, Labor, Delivery, and Perinatal Outcomes Associated With Placental Abruption: A Systematic ReviewDocument23 pagesMaternal, Labor, Delivery, and Perinatal Outcomes Associated With Placental Abruption: A Systematic ReviewasfwegereNo ratings yet
- 2016 Article 211Document25 pages2016 Article 211agus fetal mein feraldNo ratings yet
- Cardiovascular Risk in Hypertension Open Question 13Document2 pagesCardiovascular Risk in Hypertension Open Question 13Nurulhuda RashidNo ratings yet
- Grant ProposalDocument34 pagesGrant Proposalapi-547026973No ratings yet
- Scientrfic Basis For The Content of Routine Antenatal CareDocument14 pagesScientrfic Basis For The Content of Routine Antenatal CareRusdySpotrNo ratings yet
- Lit Review NealeDocument9 pagesLit Review Nealeapi-726948535No ratings yet
- Baru 7Document17 pagesBaru 7Lissaberti AmaliahNo ratings yet
- Provision of No-Cost, Long-Acting Contraception and Teenage PregnancyDocument8 pagesProvision of No-Cost, Long-Acting Contraception and Teenage PregnancyFaza HaitamiNo ratings yet
- Manual Interventions For Musculoskeletal Factors in Infants With Suboptimal Breastfeeding: A Scoping ReviewDocument12 pagesManual Interventions For Musculoskeletal Factors in Infants With Suboptimal Breastfeeding: A Scoping ReviewPaula Belén Rojas CunazzaNo ratings yet
- Far Eastern UniversityDocument5 pagesFar Eastern UniversityCherry WineNo ratings yet
- Preconception Health and Care: A Life Course ApproachFrom EverandPreconception Health and Care: A Life Course ApproachJill ShaweNo ratings yet
- Physics A: Unit: G484: The Newtonian WorldDocument9 pagesPhysics A: Unit: G484: The Newtonian Worldptscribd941No ratings yet
- Actinomyces OdontolyticusDocument4 pagesActinomyces OdontolyticusLiviu Athos TamasNo ratings yet
- 2 Lane Widening With Paved ShouldersDocument147 pages2 Lane Widening With Paved ShouldersyedidiNo ratings yet
- OPTCL Safety Manual 2015 (Latest)Document136 pagesOPTCL Safety Manual 2015 (Latest)SARAVANANo ratings yet
- Cp-Vnc-B4K-Vm: 4K Ultra-HD Network Box CameraDocument5 pagesCp-Vnc-B4K-Vm: 4K Ultra-HD Network Box Camerarama1870No ratings yet
- Recipe Name: Yield/Servings: 1 Quantity Unit Ingredients Market Price Price Per Qty UnitDocument3 pagesRecipe Name: Yield/Servings: 1 Quantity Unit Ingredients Market Price Price Per Qty UnitQueenie AmoraNo ratings yet
- 09-06-2021 HMB EnglishDocument51 pages09-06-2021 HMB EnglishKiran SNNo ratings yet
- Optical Fiber Fabricated From 3D Printed Silica PreformsDocument8 pagesOptical Fiber Fabricated From 3D Printed Silica PreformsMahmudur Rahman RashaNo ratings yet
- 12 Biology Notes Ch06 Molecular Basis of InheritanceDocument6 pages12 Biology Notes Ch06 Molecular Basis of InheritanceInderpal SinghNo ratings yet
- CJ4 Avionics 1.01Document36 pagesCJ4 Avionics 1.01Jose Otero De Santiago100% (1)
- WattsBox Insulated Enclosures Specification SheetDocument4 pagesWattsBox Insulated Enclosures Specification SheetWattsNo ratings yet
- Organic Farming and Medicinal PlantDocument43 pagesOrganic Farming and Medicinal PlantAbraham100% (4)
- C O / C - S,, Y V: /Itdversions/19.3.0.1/Itdstart - Aspx?Svc 3F50C3C0-1874-400E-Af3A-5036E 79Dec9FDocument201 pagesC O / C - S,, Y V: /Itdversions/19.3.0.1/Itdstart - Aspx?Svc 3F50C3C0-1874-400E-Af3A-5036E 79Dec9FharshiniNo ratings yet
- Community Technology Development Trust: Our VisionDocument2 pagesCommunity Technology Development Trust: Our VisiondanielNo ratings yet
- Sudden DeathDocument26 pagesSudden DeathAbang AzharNo ratings yet
- Effective Utilization of Various Industrial Wastes in Concrete For Rigid Pavement Construction - A Literature ReviewDocument9 pagesEffective Utilization of Various Industrial Wastes in Concrete For Rigid Pavement Construction - A Literature ReviewIJIRSTNo ratings yet
- ReikiDocument2 pagesReikiSumeet SunnyNo ratings yet
- Product Data Sheet: Tesys Vario - Emergency Stop Switch Disconnector - 63 A - On DoorDocument3 pagesProduct Data Sheet: Tesys Vario - Emergency Stop Switch Disconnector - 63 A - On DoorBNCHNo ratings yet
- Total RNA Isolation and CDNA Synthesis From Bixa Orellana BarkDocument5 pagesTotal RNA Isolation and CDNA Synthesis From Bixa Orellana BarkIzzatizyanHamdanNo ratings yet
- Man and The Wild An Ecocritical ReadingDocument4 pagesMan and The Wild An Ecocritical ReadingExoplasmic ReticulumNo ratings yet
- B S T Year 5Document9 pagesB S T Year 5INCREASE & ABUNDANT SCHOOLSNo ratings yet
- Science and Technology and Nation BuildingDocument21 pagesScience and Technology and Nation BuildingQuizon, James Anthony R.No ratings yet
- ASUG QM Session 1 QM 101 Introduction To SAP Quality Management Module PDFDocument41 pagesASUG QM Session 1 QM 101 Introduction To SAP Quality Management Module PDFStorm100% (1)
- HMI & SCADA Catalogue ProductsDocument14 pagesHMI & SCADA Catalogue Productss_chendryNo ratings yet
- Vectors - Past Paper Questions: Cambridge IGCSEDocument12 pagesVectors - Past Paper Questions: Cambridge IGCSElilly lordNo ratings yet
- Hayat Intsituyte of Nursing Education Kamal Tower, Amerigog, 9 Mile, Kamrup (M) Articles Required For Newly Formed Advanced Nursing Practical LabDocument3 pagesHayat Intsituyte of Nursing Education Kamal Tower, Amerigog, 9 Mile, Kamrup (M) Articles Required For Newly Formed Advanced Nursing Practical LabDebika DasNo ratings yet
- Assigment - 2: Brains and GendersDocument2 pagesAssigment - 2: Brains and GendersThư Nguyễn100% (1)
- Fat Content Determination Methods: Infrared SpectrometryDocument8 pagesFat Content Determination Methods: Infrared SpectrometryFastabiqul KhairatNo ratings yet
Pi Is 0002937812001317
Pi Is 0002937812001317
Uploaded by
harold.atmajaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Pi Is 0002937812001317
Pi Is 0002937812001317
Uploaded by
harold.atmajaCopyright:
Available Formats
Research www. AJOG.
org
OBSTETRICS
The effect of CenteringPregnancy group prenatal care
on preterm birth in a low-income population
Amy H. Picklesimer, MD, MSPH; Deborah Billings, PhD; Nathan Hale, PhD;
Dawn Blackhurst, DrPH; Sarah Covington-Kolb, MSPH, MSW
OBJECTIVE: The purpose of this study was to evaluate the impact of 12.7%; P ⫽ .01), as was delivery at ⬍32 weeks’ gestation (1.3% vs
group prenatal care on rates of preterm birth. 3.1%; P ⫽ .03). Adjusted odds ratio for preterm birth for participants in
group care was 0.53 (95% confidence interval, 0.34 – 0.81). The racial
STUDY DESIGN: We conducted a retrospective cohort study of 316
disparity in preterm birth for black women, relative to white and His-
women in group prenatal care that was compared with 3767 women in tra-
panic women, was diminished for the women in group care.
ditional prenatal care. Women self-selected participation in group care.
CONCLUSION: Among low-risk women, participation in group care im-
RESULTS: Risk factors for preterm birth were similar for group prenatal
proves the rate of preterm birth compared with traditional care, espe-
care vs traditional prenatal care: smoking (16.9% vs 20%; P ⫽ .17),
cially among black women. Randomized studies are needed to elimi-
sexually transmitted diseases (15.8% vs 13.7%; P ⫽ .29), and previ-
nate selection bias.
ous preterm birth (3.2% vs 5.4%; P ⫽ .08). Preterm delivery (⬍37
weeks’ gestation) was lower in group care than traditional care (7.9% vs Key words: CenteringPregnancy, disparity, prenatal care, preterm birth
Cite this article as: Picklesimer AH, Billings D, Hale N, et al. The effect of CenteringPregnancy group prenatal care on preterm birth in a low-income population.
Am J Obstet Gynecol 2012;206:415.e1-7.
P reterm birth is a serious, international
public health issue. In the short term,
preterm infants require more medical ment ranges from antibiotics and photo-
gestation. There is also a tremendous ra-
cial/ethnic disparity in rates of prematu-
rity; 19.7% of non-Hispanic black women
treatment than full-term infants; the treat- therapy to mechanical ventilation and total deliver preterm compared with 12.7% of
parenteral nutrition. Other complications of non-Hispanic white women and 13.0% of
prematurity, such as cerebral palsy and reti- Hispanic women.8 The Greenville Hospi-
nopathy, can lead to life-long handicap.1,2 tal System Obstetrics Center, located in
From the Departments of Obstetrics and
The annual cost of treatment for these and Greenville, SC, provides prenatal care pri-
Gynecology (Dr Picklesimer and Ms
Covington-Kolb) and Quality Management other complications that arise from preterm marily to medically underserved women.
(Dr Blackhurst), Greenville Hospital System birth has been estimated at ⬎26 billion dol- Given the vulnerability of the population
University Medical Center, Greenville, and lars in the United States alone.3 that is served, historic rates of premature
the Department of Health Promotion, Risk factors for spontaneous preterm birth among women in this practice
Education, and Behavior (Dr Billings) and the
Center for Health Services and Policy
delivery are well described and include a (16.4%) are markedly higher than both
Research (Dr Hale), Arnold School of Public history of previous preterm birth, multiple state and national averages.
Health, University of South Carolina, gestation, vaginal bleeding, low prepreg- In an effort to address this long-standing
Columbia, SC. nancy weight, systemic and genital tract in- issue, the Greenville Hospital System Ob-
Received Nov. 28, 2011; revised Jan. 19, fection, maternal smoking, and non-white stetrics Center began to offer Centering-
2012; accepted Jan. 31, 2012.
race among others.4,5 Although prescrip- Pregnancy group prenatal care in March
The authors report no conflict of interest.
tion of 17 alpha-hydroxyprogesterone 2009. CenteringPregnancy is a national
Presented as a poster at the 32nd annual caproate has led to reductions in the rates model of group prenatal care that has
meeting of the Society for Maternal-Fetal
Medicine, Dallas, TX, Feb. 6-11, 2012. of recurrent preterm delivery, there is no shown promise in reducing the rates of
The racing flag logo above indicates that this
similarly effective means of primary pre- preterm birth.8-12 The originators drew on
article was rushed to press for the benefit of the vention for women who are otherwise at basic adult learning theories that highlight
scientific community. low risk for preterm birth.6 Instead, clini- the importance of group work and partic-
Reprints not available from the authors. cians focus on symptom-based screening ipatory processes to develop the model, al-
0002-9378/free and physical examination, and treatment though no single theory of health behavior
© 2012 Mosby, Inc. All rights reserved. is aimed at arresting the labor process after was central to their design.
doi: 10.1016/j.ajog.2012.01.040
it has begun.7 The Centering Healthcare Institute (Bos-
For Editors’ Commentary, see South Carolina has one of the highest ton, MA) maintains the curriculum and
Contents rates of preterm birth in the country; evaluates and approves sites that offer this
14.3% of women deliver at ⬍37 weeks’ trademarked model of group prenatal
MAY 2012 American Journal of Obstetrics & Gynecology 415.e1
Research Obstetrics www.AJOG.org
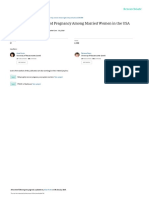
FIGURE
Study population of all singleton live-births during the study period
339 9291
group care traditional care
participants participants
12 women 4020 women
Not eligible for Not eligible for
Mediciad Mediciad
6 women 1398 women
Late entry to prenatal Late entry to prenatal
care (>16 wks) care (>16 weeks)
3 women 68 women
Pregestational Pregestational
diabetes, chronic diabetes, chronic
hypertension hypertension
2 women 38 women
More than 1 birth More than 1 birth
during study period during study period
(second birth (second birth
excluded) excluded)
316 3767
group care traditional care
final cohort final cohort
Exclusions are noted.
Picklesimer. Group prenatal care and preterm birth. Am J Obstet Gynecol 2012.
care. Participation typically is limited to result in improved social support for the The purpose of this study was to con-
low-risk women and excludes women with group members. In most settings, groups duct a retrospective cohort study to deter-
preexisting medical conditions or high- are led by certified nurse-midwives or mine the impact of the CenteringPreg-
risk pregnancies, such as multiple gesta- nurse-practitioners. nancy model of group prenatal care on
tions. Groups of up to 8-12 pregnant To date, only one large randomized rates of preterm birth for women who are
women at approximately the same gesta- controlled trial that evaluated pregnancy enrolled in group care compared with
tional age are brought together 10 times outcomes for women who were enrolled women who receive care in traditional pre-
over 6 months. Physical assessment by a in group prenatal care has been con- natal care. This study will contribute the
credentialed medical care provider occurs ducted.13 The authors found that the rate literature by examining the effectiveness of
within the group space, and women ac- of preterm birth among women in group this evidence-based model outside of a
tively participate in their own medical care care was 33% lower than the rate of pre- highly structured clinical trial setting, with
by taking responsibility for measuring term birth for women in the traditional a large enough sample to document any
their weight and blood pressure. Each prenatal care control group (9.8% vs observed changes in birth outcomes.
2-hour session follows an educational cur- 14.8%). The subsample of black women
riculum that includes information about demonstrated a 41% difference in the
health and nutrition, childbirth prepara- rate of preterm delivery (10.1% in group M ETHODS
tion, stress reduction, relationships, and care vs 15.9% in traditional care). Re- During the implementation of group pre-
parenting. Facilitated group discussion en- ductions in the rates of prematurity and natal care in our practice, we developed
courages active participation. There is an low birthweight have been inconsistent guidelines that limited eligibility for group
emphasis on relationship building that can in smaller matched cohort studies.9,14,15 participation to low-risk patients and that
415.e2 American Journal of Obstetrics & Gynecology MAY 2012
www.AJOG.org Obstetrics Research
was consistent with both the scope of prac-
tice of the nurse-practitioners and nurse- TABLE 1
midwives who were providing care in Demographic characteristics of women in group
the groups and the CenteringPregnancy care compared with women in traditional care
model design. Exclusion criteria for partic- Entire cohort
ipation in group care included, but were
Group care Traditional care
not limited to, pregestational diabetes mel- Characteristic (n ⴝ 316) (n ⴝ 3767) P valuea
litus, chronic hypertension, multiple ges-
Maternal age, yb 23.1 ⫾ 4.6 25.1 ⫾ 5.6 ⬍ .001
tation, obesity (defined by body mass ..............................................................................................................................................................................................................................................
index ⬎45 kg/m2), severe psychiatric dis- Maternal race/ethnicity, n (%) ⬍ .001
.....................................................................................................................................................................................................................................
ease, untreated drug or alcohol addiction, White 107 (33.9) 1725 (45.8)
.....................................................................................................................................................................................................................................
and other medical complications of preg- Black 107 (33.9) 961 (25.5)
.....................................................................................................................................................................................................................................
nancy that require higher levels of surveil-
Hispanic 55 (17.4) 835 (22.2)
lance, such as HIV infection and maternal .....................................................................................................................................................................................................................................
cardiac or renal disease. Beginning in Other 47 (14.9) 246 (6.5)
..............................................................................................................................................................................................................................................
March 2009, all women with low-risk Marital status, n (%) ⬍ .001
.....................................................................................................................................................................................................................................
pregnancies seeking prenatal care in the Married 75 (23.7) 1314 (34.9)
.....................................................................................................................................................................................................................................
first trimester were given the option of re-
Unmarried, Father not named 99 (31.3) 1000 (26.6)
ceiving care in the group prenatal care .....................................................................................................................................................................................................................................
model. Patients were recruited for groups Unmarried, Father named 141 (44.6) 1433 (38.0)
.....................................................................................................................................................................................................................................
at the time of their first prenatal care visit Unknown 1 (0.3) 20 (0.5)
..............................................................................................................................................................................................................................................
by either a nurse-practitioner or a nurse- Education, n (%) .266
.....................................................................................................................................................................................................................................
midwife, and the final determination
⬍High school 114 (36.1) 1532 (40.7)
regarding eligibility was made by the .....................................................................................................................................................................................................................................
provider. High school diploma/GED 105 (33.2) 1176 (31.3)
.....................................................................................................................................................................................................................................
All groups were conducted according ⬎High school 97 (30.7) 1055 (28.0)
..............................................................................................................................................................................................................................................
to the trademarked CenteringPregnancy Month prenatal care began, n (%) ⬍ .001
.....................................................................................................................................................................................................................................
curriculum, which has been described in
0-2 mo 181 (57.3) 1288 (34.2)
previous publications.9,11-13 Participa- .....................................................................................................................................................................................................................................
tion in group care was not randomized, 3-4 mo 135 (42.7) 2479 (65.8)
..............................................................................................................................................................................................................................................
but rather left to the discretion of the in- Kotelchuck Index, n (%) ⬍ .001
.....................................................................................................................................................................................................................................
dividual patient. Patients in group care Inadequate 16 (5.1) 182 (4.8)
.....................................................................................................................................................................................................................................
had the option of accessing additional
Intermediate 17 (5.4) 380 (10.1)
visits in a traditional individual care set- .....................................................................................................................................................................................................................................
ting as needed if health problems arose. Adequate 114 (36.1) 1786 (47.4)
.....................................................................................................................................................................................................................................
Typical monthly enrollment in group Adequate ⫹ 169 (53.5) 1419 (37.7)
..............................................................................................................................................................................................................................................
care ranged between 30 – 45 patients. A Tobacco use during pregnancy, n (%) .166
.....................................................................................................................................................................................................................................
log of all participants was maintained to
No 263 (83.2) 3012 (80.0)
track the outcomes of these patients for .....................................................................................................................................................................................................................................
ongoing quality control. Participation Yes 53 (16.8) 753 (20.0)
..............................................................................................................................................................................................................................................
c
was defined as attendance at even 1 Sexually transmitted disease infection, n (%) .287
.....................................................................................................................................................................................................................................
group session, and the total number of No 266 (84.2) 3252 (86.3)
.....................................................................................................................................................................................................................................
groups attended was recorded for each
Yes 50 (15.8) 515 (13.7)
participant. Women were permitted to ..............................................................................................................................................................................................................................................
withdraw from group care and continue Parity, n (%) ⬍ .001
.....................................................................................................................................................................................................................................
with traditional care if desired; this was 0 199 (63.0) 1549 (41.1)
.....................................................................................................................................................................................................................................
also recorded for each participant. Med- ⱖ1 117 (37.0) 2218 (58.9)
..............................................................................................................................................................................................................................................
ical care in groups was provided by
Previous preterm birth, n (%) .082
nurse-midwives and nurse-practitio- .....................................................................................................................................................................................................................................
ners. After the first 8 months of imple- No 306 (96.8) 3562 (94.6)
.....................................................................................................................................................................................................................................
mentation, many groups also included a Yes 10 (3.2) 205 (5.4)
..............................................................................................................................................................................................................................................
medical student, a resident physician in GED, general equivalency degree.
obstetrics and gynecology, or a resident a
Maternal age comparison was made with t test; the comparison of the remainder was made with 2; b Data are given as mean ⫾ SD;
c
physician in family medicine. Nesseria gonorrhea, Chlamydia tracho matis, Herpes simplex.
Picklesimer. Group prenatal care and preterm birth. Am J Obstet Gynecol 2012.
In December 2010, institutional re-
view board approval was granted by the
MAY 2012 American Journal of Obstetrics & Gynecology 415.e3
Research Obstetrics www.AJOG.org
of 2 analysis for categoric data and the
TABLE 2 Student t test for continuous data. Mul-
Birth outcomes for women in group care compared tiple logistic regression analysis was used
with women in traditional care to obtain adjusted odds ratios for pre-
Entire cohort, n (%) term birth for patients who were en-
rolled in group care vs the control group
Group care Traditional care
Characteristic (n ⴝ 316) (n ⴝ 3767) P valuea of women who participated in tradi-
tional prenatal care; adjustment was
Gestational age at delivery, wk .034
..................................................................................................................................................................................................................................... made for known risk factors and group
⬍32 4 (1.3) 118 (3.1) differences. Significance level was set at
.....................................................................................................................................................................................................................................
32-36 21 (6.7) 359 (9.5)
.....................................................................................................................................................................................................................................
the probability level of .05. All statistical
ⱖ37 291 (92.1) 3290 (87.3) analyses were performed with SAS statis-
..............................................................................................................................................................................................................................................
tical software (version 9.2; SAS Institute
Birthweight, g .265
..................................................................................................................................................................................................................................... Inc, Cary, NC).
⬍1500 5 (1.6) 112 (3.0)
.....................................................................................................................................................................................................................................
1500-2400 23 (7.3) 318 (8.4)
.....................................................................................................................................................................................................................................
ⱖ2500 288 (91.1) 3337 (88.6) R ESULTS
..............................................................................................................................................................................................................................................
During the study period, there were 9630
Admission to neonatal intensive care unit .082
..................................................................................................................................................................................................................................... singleton live-born deliveries at Green-
No 294 (93.0) 3391 (90.0) ville Memorial Hospital; 339 of these
.....................................................................................................................................................................................................................................
Yes 22 (7.0) 376 (10.0)
..............................................................................................................................................................................................................................................
women participated in group prenatal
Breastfed .099 care. After exclusions, the final study pop-
.....................................................................................................................................................................................................................................
ulation consisted of 4083 women: 316
No 111 (35.1) 1501 (39.9)
..................................................................................................................................................................................................................................... women in group care and 3767 women in
Yes 205 (64.9) 2266 (60.1) traditional care (Figure). Women in the
..............................................................................................................................................................................................................................................
a
test.
2
group care cohort attended a median of 7
Picklesimer. Group prenatal care and preterm birth. Am J Obstet Gynecol 2012. (interquartile range, 5– 8) sessions of the
10 scheduled group sessions. Forty-eight
Greenville Hospital System University age at delivery. Women are categorized women (15%) withdrew from the group
Medical Center for a retrospective cohort as receiving “inadequate” care if they en- care program after a median of 1 (range,
study to evaluate program outcomes. De- ter prenatal care after the month 4 of 1–5) sessions, but their pregnancy out-
mographic information and pregnancy pregnancy (16 weeks’ gestational age) or comes were evaluated with the group care
outcomes were obtained from the elec- receive ⬍50% of the expected visits. All cohort in an intent-to-treat analysis.
tronic birth certificate database that is other categories require entry to care in Maternal demographic characteristics
maintained by the hospital. Preterm birth months 1-4. The “intermediate” cate- were significantly different between
was considered as any delivery at ⬍37 gory requires attendance at 50-79% of groups (Table 1). Women who enrolled
weeks’ gestational age by the best obstetric the expected visits; the “adequate” cate- in group prenatal care were younger,
estimate of gestational age at delivery, gory requires attendance at 80-109% of more likely to be a minority, and nullip-
which was collected in accordance with the the expected visits; and the “adequate ⫹” arous, and to have entered prenatal care
Centers for Disease Control and Preven- category requires attendance at ⬎110% earlier in comparison with women in
tion’s National Center for Health Statistics of the expected visits. traditional care. Risk factors for preterm
Handbook and the 2003 revision of the US The study cohort consisted of women birth such as the presence of sexually
Standard Certificate of Live Birth.16-18 who delivered live-born singleton in- transmitted infections, tobacco use dur-
Adequacy of prenatal care was deter- fants between March 2009 and Decem- ing pregnancy, and history of previous
mined with standard scoring on the Ko- ber 2010, who received Medicaid cover- preterm birth were similar for both
telchuck Adequacy of Prenatal Care Uti- age at the time of delivery, who entered groups.
lization index, which is also included in prenatal care within the first 16 weeks of The mean gestational age at delivery
the 2003 revision of the US Standard pregnancy, and who had no pregesta- was 38.8 ⫾ 2.2 (SD) weeks for women in
Certificate of Live Birth.19 This index is tional diabetes mellitus or hypertension. group prenatal care, which was greater
based on the American College of Obste- If women had ⬎1 birth during the study than for women in traditional care who
tricians and Gynecologists prenatal care period, only the first delivery was in- demonstrated a mean gestational age at
standards for uncomplicated pregnan- cluded to maintain independence. delivery of 38.3 ⫾ 2.7 weeks (P ⬍ .001).
cies and characterizes care into 1 of 4 cat- Bivariate group comparisons between Similarly, mean birthweight was 3245 ⫾
egories according to the timing of initia- women who received group care and 579 g for women in group care compared
tion of care, the total number of prenatal those in the control group who received with 3178 ⫾ 654 g for women in tradi-
care visits received, and the gestational traditional care were made with the use tional care (P ⫽ .05). Previous preterm
415.e4 American Journal of Obstetrics & Gynecology MAY 2012
www.AJOG.org Obstetrics Research
birth, maternal race, marital status, and
adequacy of prenatal care were associ- TABLE 3
ated with preterm delivery at ⬍37 weeks’ Multivariate logistic regression for risk of preterm delivery <37 weeks
gestation (P ⬍ .001 for all). Bivariate Adjusted odds ratio
comparisons of birth outcomes for all Characteristic (95% CI) P value
women in group care compared with all Maternal age 1.01 (0.99–1.03) .398
..............................................................................................................................................................................................................................................
women in traditional care are available Maternal race/ethnicity
.....................................................................................................................................................................................................................................
in Table 2.
White Referent —
The rate of preterm delivery at ⬍37 .....................................................................................................................................................................................................................................
weeks’ gestation was 7.9% for women in Black 1.20 (0.95–1.50) .122
.....................................................................................................................................................................................................................................
group care and 12.7% for women in tra- Hispanic 0.51 (0.38–0.69) ⬍ .001
.....................................................................................................................................................................................................................................
ditional care (P ⫽ .01). Rates of preterm Other 0.87 (0.59–1.28) .472
..............................................................................................................................................................................................................................................
delivery at ⬍32 weeks’ gestation were Marital status
also lower, with a rate of 1.3% for women .....................................................................................................................................................................................................................................
Married Referent —
in group care and 3.1% for women in .....................................................................................................................................................................................................................................
traditional care (P ⫽ .03). There was no Unmarried 1.09 (0.87–1.37) .449
..............................................................................................................................................................................................................................................
difference in rates of low infant birth- Kotelchuck Index
.....................................................................................................................................................................................................................................
weight ⬍2500 g (8.9% group care vs Inadequate/intermediate 1.12 (0.86–1.45) .405
11.4% traditional care; P ⫽ .20) or neo- .....................................................................................................................................................................................................................................
Adequate/adequate ⫹ Referent —
natal intensive care unit admission ..............................................................................................................................................................................................................................................
(7.0% group care vs 10.0% traditional Month prenatal care began
.....................................................................................................................................................................................................................................
care; P ⫽ .08). Multivariate regression 0-2 0.69 (0.57–0.84) ⬍ .001
.....................................................................................................................................................................................................................................
analysis that included maternal age, race, 3-4 Referent —
..............................................................................................................................................................................................................................................
marital status, nulliparity, early entry to Parity, n
prenatal care, adequacy of prenatal care, .....................................................................................................................................................................................................................................
0 Referent —
and history of previous preterm delivery .....................................................................................................................................................................................................................................
demonstrated that participation in group ⱖ1 0.86 (0.69–1.07) .169
..............................................................................................................................................................................................................................................
prenatal care was highly protective for Previous preterm birth
.....................................................................................................................................................................................................................................
preterm delivery (odds ratio [OR], 0.53; No Referent —
.....................................................................................................................................................................................................................................
95% confidence interval [CI], 0.34 –
Yes 2.54 (1.80–3.58) ⬍ .001
0.81; Table 3). ..............................................................................................................................................................................................................................................
To eliminate the potential confound- Participation in group care
.....................................................................................................................................................................................................................................
ing effect of previous preterm birth, sub- No Referent —
.....................................................................................................................................................................................................................................
group analysis was performed only with Yes 0.53 (0.34–0.81) .004
..............................................................................................................................................................................................................................................
nulliparous patients. There were persis- Picklesimer. Group prenatal care and preterm birth. Am J Obstet Gynecol 2012.
tent demographic differences between
the 2 cohorts in the nulliparous sub-
tions was not different between the 2
group. We continued to see a higher per- Nulliparous women in group care en-
centage of minority women participate rolled in prenatal care earlier than nullip- groups (13.1% in group care vs 14.1% in
in group prenatal care compared with arous women in traditional care; 58.8% traditional care; P ⫽ .699).
traditional care. Of the 199 nulliparous entered care at ⬍2 months’ gestation com- Pregnancy outcomes for this subgroup
women in group care, 33.2% were non- pared with 33.7% in the traditional cohort were similar to those of the larger cohort.
Hispanic white women; 33.2% were (P ⬍ .001). Nulliparous women in group The mean gestational age at delivery for
non-Hispanic black women; 16.6% were care were also less likely to receive inade- nulliparous women was 38.8 ⫾ 2.3 weeks
Hispanic women, and 17.1% of the quate or intermediate prenatal care and for women in group prenatal care com-
women were self-reported as other race/ more likely to demonstrate more adequate pared with women in traditional care who
ethnicity. The 1549 nulliparous women and adequate⫹ prenatal care, as measured demonstrated a mean gestational age at de-
who received traditional care were by the Kotelchuck Index (P ⫽ .011). livery of 38.4 ⫾ 2.9 weeks (P ⫽ .01). Simi-
49.8% non-Hispanic white, 25.8% non- Nulliparous women in group care were larly, mean birthweight was 3238 ⫾ 588 g
Hispanic black, and 18% Hispanic; 6.4% less likely to use tobacco during pregnancy, for women in group care compared with
women reported to be other race/ethnic- with only 12.6% of the women reporting 3131 ⫾ 669 g for women in traditional care
ity (P ⬍ .001) Other demographic char- any tobacco use during pregnancy com- (P ⫽ .02).
acteristics, including age, marital status, pared with 19.3% of the nulliparous The differences in rates of preterm de-
and educational level were not different women in traditional care (P ⫽ .022). The livery were persistent in this subgroup;
between these 2 groups. incidence of sexually transmitted infec- 8.0% of the nulliparous patients in group
MAY 2012 American Journal of Obstetrics & Gynecology 415.e5
Research Obstetrics www.AJOG.org
in both the matched cohort and the ran-
TABLE 4 domized controlled trial. Other authors
Comparisons for preterm delivery at <37 weeks’ have published smaller studies on ra-
gestation by race/ethnicity within groups cially and ethnically homogeneous pop-
Group care Traditional care ulations that included black and His-
panic women.10,15 Authors with more
Preterm Preterm
Mother’s race/ Subjects, delivery, Subjects, delivery, diverse study populations have been lim-
ethnicity n n (%) P valuea n n (%) P valuea ited by small sample sizes.14,20 Because of
White 107 7 (6.5) .63 1725 236 (13.7) ⬍ .01 the diverse population in our practice,
..............................................................................................................................................................................................................................................
we were able to evaluate the impact of
Black 107 8 (7.5) 961 155 (16.1)
.............................................................................................................................................................................................................................................. group care across racial and ethnic
Hispanic 55 4 (7.3) 835 58 (7.0) groups; our finding of an apparent de-
..............................................................................................................................................................................................................................................
Other 47 6 (12.8) 246 28 (11.4) crease in the racial/ethnic disparities in
..............................................................................................................................................................................................................................................
a
2 test. preterm birth is novel.
Picklesimer. Group prenatal care and preterm birth. Am J Obstet Gynecol 2012. This apparent decrease in racial dispari-
ties in preterm birth must be interpreted
with caution. Racial identity in this study
care and 12.9% of the nulliparous pa- parisons with 2 testing, we saw a signif- was self-reported on the mother’s work-
tients in traditional care delivered at ⬍37 icant difference in the rates of preterm sheet for the birth certificate; approxi-
weeks’ gestation (P ⫽ .05). Differences in delivery at ⬍37 weeks’ gestation by race/ mately 15% of the women in group care
the rate of preterm delivery at ⬍32 ethnicity for women in traditional care were self-identified as “other.” Based on
weeks’ gestation did not reach statistical (P ⬍ .01). For women in group care, this our familiarity with these women, we
significance: 1.5% for women (n ⫽ 3) in disparity in rates of preterm delivery at know that the majority are non-Hispanic
group care compared with 3.8% for ⬍37 weeks’ gestation by maternal race/ and biracial, white and black. Baseline rates
women (n ⫽ 59) in the control group ethnicity was no longer significant (P ⫽ of prematurity are not available for this
(P ⫽ .14). There was also no difference in .63; Table 4). group. The lower rates of preterm birth for
a low infant birthweight of ⬍2500 g Hispanic women in this study population
(8.5% group care vs 11.4% traditional; C OMMENT are evidence of the “Hispanic paradox,”
P ⫽ .10) or neonatal intensive care unit The 47% reduction in preterm birth for which is a well-described phenomenon
admission (7.5% group care vs 11.2% low-risk women in group care is consis- that seeks to explain the relatively positive
traditional care; P ⫽ .12). Multivariate tent with the previously published pro- health outcomes of recent Hispanic immi-
logistic regression modeling that con- spective randomized study of group pre- grants, a group with high rates of poverty
trolled for maternal race, marital status, natal care, and confirms that this model and limited access to medical care that may
tobacco use during pregnancy, early en- has the potential to deliver beneficial otherwise seem to be at risk for poor health
try to prenatal care, and adequacy of pre- outcomes outside of the clinical trial set- outcomes.21 Finally, although the current
natal care confirmed the protective effect ting.9,13 This finding persisted in the study sample is among the largest and
of participation in group care for reduc- subanalysis of nulliparous women. Fur- most diverse that has been reported, it is
ing the risk of preterm delivery at ⬍37 thermore, the racial/ethnic disparity in still relatively small, and the racial differ-
weeks’ gestation for nulliparous women rates of preterm birth seemed to dimin- ences in pregnancy outcome may diminish
(OR, 0.54; 95% CI, 0.31– 0.93). ish for the women who participated in when the number of patients who partici-
Because there was a higher percentage group care when compared with the pate in group care is larger.
of minority women in group care and control group of women in traditional Other study limitations are those in-
because non-Hispanic black race is asso- care. When considered as a “bench to herent to all retrospective cohort studies;
ciated with increased rates of preterm bedside” translational research project, the most significant is the potential for
delivery, we sought more information we can see that replication of group selection bias. Indeed, in bivariate anal-
about the influence of race in the cohort. care according to the guidelines that ysis, we do see a number of differences
Logistic regression modeling that con- were established by the Centering between women who elected to partici-
trolled for maternal age, marital status, Healthcare Institute delivers positive pate in group care compared with those
nulliparity, early entry to prenatal care, patient outcomes that are consistent who elected traditional prenatal care.
adequacy of prenatal care, and participa- with previously published prospective Many of the characteristics that are seen
tion in group care showed similar risks clinical trials. more frequently in group care patients,
for preterm delivery for black and white The principal strength of our study is however, would seem to confer an in-
women, with Hispanic women relatively the racial diversity of the study popula- creased risk for preterm delivery, such as
protected from preterm delivery (OR, tion. The 2 largest studies of group care a higher percentage of non-Hispanic
0.51; 95% CI, 0.38 – 0.69). When we per- published by Ickovics et al9,13 included a black women, younger maternal age, and
formed unadjusted within-group com- study population of 80% black women a higher number of unmarried women.
415.e6 American Journal of Obstetrics & Gynecology MAY 2012
www.AJOG.org Obstetrics Research
Finally, data collected from the elec- The possibility that group prenatal 8. National Center for Health Statistics. 2008 Final
tronic birth certificate database may be care could represent a form of primary natality data. Available at: www.marchofdimes.
com/peristats. Accessed Aug. 28, 2011.
less accurate and is less comprehensive prevention for preterm birth, particu-
9. Ickovics JR, Kershaw TS, Westdahl C, et al.
than data that could have collected from larly for nulliparous women, is intrigu- Group prenatal care and preterm birth weight:
a review of the medical records or in pa- ing. The mechanism that may explain results from a matched cohort study at public
tient interviews. The birth certificate the improved outcomes for participants clinics. Obstet Gynecol 2003;102:1051-7.
worksheets include only a very limited in group care is unclear. It may be that 10. Klima C, Norr K, Vonderheid S, Handler A.
number of risk factors in pregnancy the enhanced education that is provided Introduction of CenteringPregnancy in a public
during group sessions empowers women health clinic. J Midwifery Womens Health 2009;
(presence of diabetes mellitus, hyperten-
54:27-34.
sion, previous preterm birth, and “other to seek medical attention earlier when
11. Rising SS. Centering pregnancy: an inter-
poor pregnancy outcome”). The work- they are experiencing problems, and the disciplinary model of empowerment. J Nurse
sheets do not include information about improved relationship between patient Midwifery 1998;43:46-54.
the presence or absence of many of the and provider may ensure better compli- 12. Rising SS, Kennedy HP, Klima CS. Rede-
high-risk conditions that would have ex- ance with treatment recommendations. signing prenatal care through CenteringPreg-
cluded women from participation in our Relationships among patients that de- nancy. J Midwifery Womens Health 2004;49:
398-404.
group prenatal care program, such as velop in the context of the group provide
13. Ickovics JR, Kershaw TS, Westdahl C, et al.
maternal cardiac or renal disease. Reli- enhanced levels of social support, which Group prenatal care and perinatal outcomes: a
ance on this database also precluded our may help relatively low-resource women randomized controlled trial. Obstet Gynecol
assessment of other potential confound- with their levels of stress and coping. 2007;110:330-9.
ers, such as short cervical length, positive Stress reduction, in turn, may decrease 14. Grady MA, Bloom KC. Pregnancy out-
fetal fibronectin testing, or the adminis- the inflammatory mediators that con- comes of adolescents enrolled in a Centering-
tribute to the cascade of preterm labor. Pregnancy program. J Midwifery Womens
tration of 17-alpha hydroxyprogester-
Health 2004;49:412-20.
one caproate. We are also limited in our All of these theories are untested and will
15. Robertson B, Aycock DM, Darnell LA. Com-
ability to draw conclusions about rare be the source of future research in our parison of centering pregnancy to traditional
outcomes, such as preterm delivery at practice. f care in Hispanic mothers. Matern Child Health J
⬍32 weeks’ gestation, by the relatively 2009;13:407-14.
small numbers of women who partici- REFERENCES 16. Martin J. United States vital statistics and
1. Saigal S, Doyle LW. An overview of mortality the measurement of gestational age. Paediatr
pated in group care.
and sequelae or preterm birth from infancy to Perinat Epidemiol 2007;21(suppl 2):13-21.
The findings of our study are impor- 17. National Center for Health Statistics. Hos-
adulthood. Lancet 2008;371:261-9.
tant because implementation of group 2. Larroque B, Ancel PY, Marret S, et al. Neu- pitals’ and physicians’ handbook on birth reg-
care in a medical practice is a significant rodevelopmental disabilities and special care of istration and fetal death reporting. DHHS Pub-
commitment that requires changes to 5-year-old children born before 33 weeks ges- lication no. (PHS) 87-1107. Hyattsville, MD:
nearly every process in the office. There tation (the EPIPAGE study): a longitudinal co- National Center for Health Statistics, Public
hort study. Lancet 2008;371:813-20. Health Service, 1987. Available at: http://www.
are obvious differences in the provider-
3. Societal costs of preterm birth. In: Behrman cdc.gov/nchs/data/misc/hb_birth.pdf. Accessed
patient interaction, but changes are also RE, Butler AS, eds. Preterm birth: causes, con- Jan. 3, 2012.
required for registration, laboratory, as- sequences and prevention. Washington, DC: 18. National Center for Health Statistics. 2003
sessment of vital signs, physical configu- Institute of Medicine; 2007:398. Revision of the U.S. Standard Certificates of
ration of patient care areas, and dis- 4. Mercer BM, Goldenberg RL, Das A, et al. The Birth and Fetal Death. Items 29a, 29b, 30. 2003.
preterm prediction study: a clinical risk assess-
charge processes. Patients are also ment system. Am J Obstet Gynecol 1996;174:
Available at: http://www.cdc.gov/nchs/nvss/
required to make changes: a longer ap- vital_certificate_revisions.htm. Accessed Jan. 3,
1885-93.
2012.
pointment time, a loss of flexibility in 5. Goldenberg RL, Iams JD, Mercer BM, et al.
19. Kotelchuck M. An evaluation of the Kessner
scheduling group appointments, and a The preterm prediction study: the value of new
Adequacy of Prenatal Care Index and a pro-
prohibition against bringing small chil- vs standard risk factors in predicting early and
posed Adequacy of Prenatal Care Utilization In-
all spontaneous preterm births: NICHD MFMU
dren to group. The data presented here Network. Am J Public Health 1998;88:233-8. dex. Am J Public Health 1994;84:1414-20.
show that offering group care to even a 6. Meis PJ, Klebanoff M, Thom E, et al. Preven- 20. Baldwin KA. Comparison of selected out-
portion of self-selected patients can tion of recurrent preterm delivery by 17 alpha comes of CenteringPregnancy versus tradi-
make a difference in pregnancy out- hydroxyprogesterone caproate: NICHD MFMU tional prenatal care. J Midwifery Womens
Network. N Engl J Med 2003;348:2379-85. Health 2006;51:266-72.
come. This may embolden providers and 21. Fuentes-Afflick E, Hessol NA, Perez-Stable
7. Iams JD, Romero R, Culhane JF, Goldenberg
practice managers to pursue the system RL. Primary, secondary and tertiary interven- EJ. Testing the epidemiologic paradox of low
redesign that is required to bring group tions to reduce the morbidity and mortality of birth weight in Latinos. Arch Pediatr Adolesc
care into their office. preterm birth. Lancet 2008;371:164-75. Med 1999;153:147-53.
MAY 2012 American Journal of Obstetrics & Gynecology 415.e7
You might also like
- Sample Food Inspection ReportDocument3 pagesSample Food Inspection ReportCityNewsToronto75% (4)
- Beach Lifeguard: ManualDocument72 pagesBeach Lifeguard: ManualLuis ZapataNo ratings yet
- Journal 4Document13 pagesJournal 4intan wahyuNo ratings yet
- Nursing Research PaperDocument24 pagesNursing Research Paperapi-455624162No ratings yet
- PIIS0002937813009320Document7 pagesPIIS0002937813009320harold.atmajaNo ratings yet
- Outcome of Teenage PregnancyDocument4 pagesOutcome of Teenage PregnancyMALIK MANASRAHNo ratings yet
- Calderon Margalit2009Document8 pagesCalderon Margalit2009Aulya ArchuletaNo ratings yet
- Adverse Birth Outcomes Women With ‘ - LoDocument12 pagesAdverse Birth Outcomes Women With ‘ - Loshubh cards bhilwara Wedding cardsNo ratings yet
- Ajmw 2016 10 4 169Document10 pagesAjmw 2016 10 4 169Faouz AbNo ratings yet
- Unintended Pregnancy, Prenatal Care, Newborn Outcomes, and Breastfeeding in Women With EpilepsyDocument10 pagesUnintended Pregnancy, Prenatal Care, Newborn Outcomes, and Breastfeeding in Women With EpilepsyasfwegereNo ratings yet
- Mental Health Impact On The Unmet Need For Family Planning and Fertility Rate in Rural Ethiopia: A Population-Based Cohort StudyDocument10 pagesMental Health Impact On The Unmet Need For Family Planning and Fertility Rate in Rural Ethiopia: A Population-Based Cohort Studydiya desaiNo ratings yet
- Nejme2032499 PDFDocument2 pagesNejme2032499 PDFBladimir CentenoNo ratings yet
- Association of Self-Reported Adherence and AntiretDocument2 pagesAssociation of Self-Reported Adherence and AntiretDavidNo ratings yet
- Articles: BackgroundDocument12 pagesArticles: BackgroundChristian YzaguirreNo ratings yet
- Bjo12636 PDFDocument9 pagesBjo12636 PDFLuphly TaluvtaNo ratings yet
- Artikel 2 DheaDocument16 pagesArtikel 2 Dheadayana nopridaNo ratings yet
- Depression Among CD and VDDocument7 pagesDepression Among CD and VDnoam tiroshNo ratings yet
- A Case Control Study of Risk Factors and Neonatal Outcomes of Preterm BirthDocument5 pagesA Case Control Study of Risk Factors and Neonatal Outcomes of Preterm BirthSarahí SosaNo ratings yet
- ArticleDocument8 pagesArticleAstrid Abrahams PakelNo ratings yet
- Promoting Safe Prescribing in Primary Care With A Contraceptive Vital Sign: A Cluster-Randomized Controlled TrialDocument7 pagesPromoting Safe Prescribing in Primary Care With A Contraceptive Vital Sign: A Cluster-Randomized Controlled TrialDookNo ratings yet
- D'Souza-2019-Maternal Body Mass Index and PregDocument17 pagesD'Souza-2019-Maternal Body Mass Index and PregMARIATUL QIFTIYAHNo ratings yet
- Muest RaDocument13 pagesMuest RaBruno LinoNo ratings yet
- Chapter 2 Burden of Reproductive Ill HealthDocument38 pagesChapter 2 Burden of Reproductive Ill HealthFakhira Adzkiya SalsabilaNo ratings yet
- HHS Public Access: Child Neurodevelopmental Outcomes by Prepregnancy Body Mass Index and Gestational Weight GainDocument18 pagesHHS Public Access: Child Neurodevelopmental Outcomes by Prepregnancy Body Mass Index and Gestational Weight GainAndres GallegosNo ratings yet
- Hunt-Gibbon SUM 2019Document34 pagesHunt-Gibbon SUM 2019fatimaNo ratings yet
- Best 1Document7 pagesBest 1Wondwosen AsegidewNo ratings yet
- Pregnancy Complications and Outcomes in Women With Epilepsy: Mirzaei Fatemeh, Ebrahimi B. NazaninDocument5 pagesPregnancy Complications and Outcomes in Women With Epilepsy: Mirzaei Fatemeh, Ebrahimi B. NazaninMentari SetiawatiNo ratings yet
- PDF MaternityCarePtEngagementStrategiesIHADocument29 pagesPDF MaternityCarePtEngagementStrategiesIHAv_ratNo ratings yet
- Pregnancy and Childbirth Outcomes Among Adolescent Mothers: A World Health Organization Multicountry StudyDocument9 pagesPregnancy and Childbirth Outcomes Among Adolescent Mothers: A World Health Organization Multicountry StudyMahyudin SimarokoNo ratings yet
- Disrupting The Pathways of Social Determinants ofDocument10 pagesDisrupting The Pathways of Social Determinants ofIGA ABRAHAMNo ratings yet
- Piis0002937809020031 PDFDocument6 pagesPiis0002937809020031 PDFRaisa AriesthaNo ratings yet
- BMJ Open-2014-LiDocument16 pagesBMJ Open-2014-LiMarianaafiatiNo ratings yet
- The Conext of Unintended Pregnancy Among Married WDocument11 pagesThe Conext of Unintended Pregnancy Among Married WRose RoseNo ratings yet
- Depression Among Pregnant Women and Associated Factors in Hawassa City, Ethiopia: An Institution-Based Cross-Sectional StudyDocument6 pagesDepression Among Pregnant Women and Associated Factors in Hawassa City, Ethiopia: An Institution-Based Cross-Sectional Studyevita juniarNo ratings yet
- Emergency Contraception: Knowledge and Attitudes of Family Physicians of A Teaching Hospital, Karachi, PakistanDocument6 pagesEmergency Contraception: Knowledge and Attitudes of Family Physicians of A Teaching Hospital, Karachi, PakistanNaveed AhmadNo ratings yet
- The Worldwide Incidence of Preterm Birth: A Systematic Review of Maternal Mortality and MorbidityDocument8 pagesThe Worldwide Incidence of Preterm Birth: A Systematic Review of Maternal Mortality and MorbidityAnalia ZeinNo ratings yet
- Koren. Fetal Safety of DYD in 1st Trimester PregnancyDocument5 pagesKoren. Fetal Safety of DYD in 1st Trimester PregnancyRuth RachmawatyNo ratings yet
- 33873-Article Text-121761-1-10-20170831Document6 pages33873-Article Text-121761-1-10-20170831AnggaNo ratings yet
- Factors Influencing Contraceptive Uptake Among Lactating Mothers (6-24 Months) - A Case Study of 2medical Reception Station (2MRS)Document7 pagesFactors Influencing Contraceptive Uptake Among Lactating Mothers (6-24 Months) - A Case Study of 2medical Reception Station (2MRS)NanaKarikariMintahNo ratings yet
- Mental HealthDocument7 pagesMental HealthMirjana14No ratings yet
- Exploring Women Knowledge of Newborn Danger Signs: A Case of Mothers With Under Five ChildrenDocument8 pagesExploring Women Knowledge of Newborn Danger Signs: A Case of Mothers With Under Five ChildrenJohnjohn MateoNo ratings yet
- JAMA Ophthalmology Volume Issue 2018 (Doi 10.1001 - Jamaophthalmol.2018.2753) Binenbaum, Gil Bell, Edward F. Donohue, Pamela Quinn, Graham - Development of Modified Screening Criteria For Retinop PDFDocument7 pagesJAMA Ophthalmology Volume Issue 2018 (Doi 10.1001 - Jamaophthalmol.2018.2753) Binenbaum, Gil Bell, Edward F. Donohue, Pamela Quinn, Graham - Development of Modified Screening Criteria For Retinop PDFKarthik CNo ratings yet
- Risk Factors For Neonatal Asphyxia Occurrence at General Hospital Dr. M. Soewandhie, SurabayaDocument6 pagesRisk Factors For Neonatal Asphyxia Occurrence at General Hospital Dr. M. Soewandhie, SurabayaFatimah FadilahNo ratings yet
- Pi Is 0002937813005139Document5 pagesPi Is 0002937813005139fenskaNo ratings yet
- Antenatal Dexamethasone For Early Preterm Birth in Low-Resource CountriesDocument12 pagesAntenatal Dexamethasone For Early Preterm Birth in Low-Resource CountriesMemento MoriNo ratings yet
- 2018-BJOG An International Journal of Obstetrics & GynaecologyDocument40 pages2018-BJOG An International Journal of Obstetrics & GynaecologyBagusHibridaNo ratings yet
- 80 (11) 871 1 PDFDocument5 pages80 (11) 871 1 PDFMahlina Nur LailiNo ratings yet
- Intl J Eating Disorders - 2013 - Linna - Reproductive Health Outcomes in Eating DisordersDocument8 pagesIntl J Eating Disorders - 2013 - Linna - Reproductive Health Outcomes in Eating Disordersdarkleaf03No ratings yet
- Weight Gain and Menstrual Abnormalities Between Users of Depo-Provera and NoristeratDocument6 pagesWeight Gain and Menstrual Abnormalities Between Users of Depo-Provera and NoristeratMauricio Lopez MejiaNo ratings yet
- E011705 FullDocument11 pagesE011705 Fullhellen-borgesNo ratings yet
- Geist 2006Document5 pagesGeist 2006Marifer EstradaNo ratings yet
- Maternal, Labor, Delivery, and Perinatal Outcomes Associated With Placental Abruption: A Systematic ReviewDocument23 pagesMaternal, Labor, Delivery, and Perinatal Outcomes Associated With Placental Abruption: A Systematic ReviewasfwegereNo ratings yet
- 2016 Article 211Document25 pages2016 Article 211agus fetal mein feraldNo ratings yet
- Cardiovascular Risk in Hypertension Open Question 13Document2 pagesCardiovascular Risk in Hypertension Open Question 13Nurulhuda RashidNo ratings yet
- Grant ProposalDocument34 pagesGrant Proposalapi-547026973No ratings yet
- Scientrfic Basis For The Content of Routine Antenatal CareDocument14 pagesScientrfic Basis For The Content of Routine Antenatal CareRusdySpotrNo ratings yet
- Lit Review NealeDocument9 pagesLit Review Nealeapi-726948535No ratings yet
- Baru 7Document17 pagesBaru 7Lissaberti AmaliahNo ratings yet
- Provision of No-Cost, Long-Acting Contraception and Teenage PregnancyDocument8 pagesProvision of No-Cost, Long-Acting Contraception and Teenage PregnancyFaza HaitamiNo ratings yet
- Manual Interventions For Musculoskeletal Factors in Infants With Suboptimal Breastfeeding: A Scoping ReviewDocument12 pagesManual Interventions For Musculoskeletal Factors in Infants With Suboptimal Breastfeeding: A Scoping ReviewPaula Belén Rojas CunazzaNo ratings yet
- Far Eastern UniversityDocument5 pagesFar Eastern UniversityCherry WineNo ratings yet
- Preconception Health and Care: A Life Course ApproachFrom EverandPreconception Health and Care: A Life Course ApproachJill ShaweNo ratings yet
- Physics A: Unit: G484: The Newtonian WorldDocument9 pagesPhysics A: Unit: G484: The Newtonian Worldptscribd941No ratings yet
- Actinomyces OdontolyticusDocument4 pagesActinomyces OdontolyticusLiviu Athos TamasNo ratings yet
- 2 Lane Widening With Paved ShouldersDocument147 pages2 Lane Widening With Paved ShouldersyedidiNo ratings yet
- OPTCL Safety Manual 2015 (Latest)Document136 pagesOPTCL Safety Manual 2015 (Latest)SARAVANANo ratings yet
- Cp-Vnc-B4K-Vm: 4K Ultra-HD Network Box CameraDocument5 pagesCp-Vnc-B4K-Vm: 4K Ultra-HD Network Box Camerarama1870No ratings yet
- Recipe Name: Yield/Servings: 1 Quantity Unit Ingredients Market Price Price Per Qty UnitDocument3 pagesRecipe Name: Yield/Servings: 1 Quantity Unit Ingredients Market Price Price Per Qty UnitQueenie AmoraNo ratings yet
- 09-06-2021 HMB EnglishDocument51 pages09-06-2021 HMB EnglishKiran SNNo ratings yet
- Optical Fiber Fabricated From 3D Printed Silica PreformsDocument8 pagesOptical Fiber Fabricated From 3D Printed Silica PreformsMahmudur Rahman RashaNo ratings yet
- 12 Biology Notes Ch06 Molecular Basis of InheritanceDocument6 pages12 Biology Notes Ch06 Molecular Basis of InheritanceInderpal SinghNo ratings yet
- CJ4 Avionics 1.01Document36 pagesCJ4 Avionics 1.01Jose Otero De Santiago100% (1)
- WattsBox Insulated Enclosures Specification SheetDocument4 pagesWattsBox Insulated Enclosures Specification SheetWattsNo ratings yet
- Organic Farming and Medicinal PlantDocument43 pagesOrganic Farming and Medicinal PlantAbraham100% (4)
- C O / C - S,, Y V: /Itdversions/19.3.0.1/Itdstart - Aspx?Svc 3F50C3C0-1874-400E-Af3A-5036E 79Dec9FDocument201 pagesC O / C - S,, Y V: /Itdversions/19.3.0.1/Itdstart - Aspx?Svc 3F50C3C0-1874-400E-Af3A-5036E 79Dec9FharshiniNo ratings yet
- Community Technology Development Trust: Our VisionDocument2 pagesCommunity Technology Development Trust: Our VisiondanielNo ratings yet
- Sudden DeathDocument26 pagesSudden DeathAbang AzharNo ratings yet
- Effective Utilization of Various Industrial Wastes in Concrete For Rigid Pavement Construction - A Literature ReviewDocument9 pagesEffective Utilization of Various Industrial Wastes in Concrete For Rigid Pavement Construction - A Literature ReviewIJIRSTNo ratings yet
- ReikiDocument2 pagesReikiSumeet SunnyNo ratings yet
- Product Data Sheet: Tesys Vario - Emergency Stop Switch Disconnector - 63 A - On DoorDocument3 pagesProduct Data Sheet: Tesys Vario - Emergency Stop Switch Disconnector - 63 A - On DoorBNCHNo ratings yet
- Total RNA Isolation and CDNA Synthesis From Bixa Orellana BarkDocument5 pagesTotal RNA Isolation and CDNA Synthesis From Bixa Orellana BarkIzzatizyanHamdanNo ratings yet
- Man and The Wild An Ecocritical ReadingDocument4 pagesMan and The Wild An Ecocritical ReadingExoplasmic ReticulumNo ratings yet
- B S T Year 5Document9 pagesB S T Year 5INCREASE & ABUNDANT SCHOOLSNo ratings yet
- Science and Technology and Nation BuildingDocument21 pagesScience and Technology and Nation BuildingQuizon, James Anthony R.No ratings yet
- ASUG QM Session 1 QM 101 Introduction To SAP Quality Management Module PDFDocument41 pagesASUG QM Session 1 QM 101 Introduction To SAP Quality Management Module PDFStorm100% (1)
- HMI & SCADA Catalogue ProductsDocument14 pagesHMI & SCADA Catalogue Productss_chendryNo ratings yet
- Vectors - Past Paper Questions: Cambridge IGCSEDocument12 pagesVectors - Past Paper Questions: Cambridge IGCSElilly lordNo ratings yet
- Hayat Intsituyte of Nursing Education Kamal Tower, Amerigog, 9 Mile, Kamrup (M) Articles Required For Newly Formed Advanced Nursing Practical LabDocument3 pagesHayat Intsituyte of Nursing Education Kamal Tower, Amerigog, 9 Mile, Kamrup (M) Articles Required For Newly Formed Advanced Nursing Practical LabDebika DasNo ratings yet
- Assigment - 2: Brains and GendersDocument2 pagesAssigment - 2: Brains and GendersThư Nguyễn100% (1)
- Fat Content Determination Methods: Infrared SpectrometryDocument8 pagesFat Content Determination Methods: Infrared SpectrometryFastabiqul KhairatNo ratings yet