Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
2 viewsAsma Kerja
Asma Kerja
Uploaded by
anggitasilambiparkeling
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You might also like
- Pathology For The Physical Therapist Assistant e Book 2nd Edition Ebook PDFDocument62 pagesPathology For The Physical Therapist Assistant e Book 2nd Edition Ebook PDFrobert.short87298% (53)
- Lehnes Pharmacotherapeutics For Advanced Practice Providers Ebook PDFDocument39 pagesLehnes Pharmacotherapeutics For Advanced Practice Providers Ebook PDFmarilyn.llamas494100% (42)
- Bronchial Asthma in Acute Exacerbation Case StudyDocument43 pagesBronchial Asthma in Acute Exacerbation Case Studyroseanne parkNo ratings yet
- Work-Related Asthma - Pulmonary Disorders - MSD Manual Professional EditionDocument6 pagesWork-Related Asthma - Pulmonary Disorders - MSD Manual Professional Editionpeterpavel112No ratings yet
- Asthma: Home OSH Answers Diseases, Disorders & InjuriesDocument7 pagesAsthma: Home OSH Answers Diseases, Disorders & InjuriesNashon_AsekaNo ratings yet
- Occupational Asthma 2Document7 pagesOccupational Asthma 2drunkpunchloveNo ratings yet
- Description of AsthmaDocument14 pagesDescription of AsthmaManayu WidaswariNo ratings yet
- Occupational Asthma Occupational Asthma: Sri Handayani LubisDocument19 pagesOccupational Asthma Occupational Asthma: Sri Handayani LubisdonkeyendutNo ratings yet
- Astm ErsDocument9 pagesAstm ErsAdrian RomanNo ratings yet
- Asthma InformationDocument10 pagesAsthma InformationSheen aballeNo ratings yet
- Bronchial Asthma: Made By: Sonakshi Chauhan Rollno. 81 BATCH: 2015-2016Document14 pagesBronchial Asthma: Made By: Sonakshi Chauhan Rollno. 81 BATCH: 2015-2016anshul100% (1)
- ASTHMA IllnessDocument8 pagesASTHMA IllnessJM MARQUEZNo ratings yet
- Asthma: Signs and SymptomsDocument6 pagesAsthma: Signs and Symptomstresdos09No ratings yet
- Asthma 2Document8 pagesAsthma 2Evangelist Stephen NziokaNo ratings yet
- Asthma: Prepared By: Genesis T. Consigna. BSN-3Document10 pagesAsthma: Prepared By: Genesis T. Consigna. BSN-3Digital ExpressNo ratings yet
- UAS Inggris (Final Test)Document2 pagesUAS Inggris (Final Test)Iga AmandaNo ratings yet
- AsthmaDocument43 pagesAsthmaPriyanka PNo ratings yet
- 4 Bronchial AsthmaDocument9 pages4 Bronchial Asthmashanfiza_92No ratings yet
- Occupational Bronchitis Asthma enDocument47 pagesOccupational Bronchitis Asthma enel spin artifactNo ratings yet
- AEBA QUESTIONS-WPS OfficeDocument2 pagesAEBA QUESTIONS-WPS OfficeMarj Castor LisondraNo ratings yet
- Asthma: Asthma (From The GreekDocument2 pagesAsthma: Asthma (From The GreekSteffiDoNo ratings yet
- Concept Map DraftsDocument9 pagesConcept Map DraftsFc CrisostomoNo ratings yet
- The Bronchial AsthmaDocument5 pagesThe Bronchial AsthmaKathleen Anne CajandingNo ratings yet
- Presentation Copd Asthma 2022Document65 pagesPresentation Copd Asthma 2022Pwani aquaponicsNo ratings yet
- Dental Management of Patients With Respiratory Disease: (Copd)Document12 pagesDental Management of Patients With Respiratory Disease: (Copd)Fahd AlahaidebNo ratings yet
- Occupational Airways Disease: Key PointsDocument4 pagesOccupational Airways Disease: Key PointsAlba D'kiferz EvridNo ratings yet
- An Assignment On Pathophysiology and Drug Therapy of Respiratory Disorders. byDocument34 pagesAn Assignment On Pathophysiology and Drug Therapy of Respiratory Disorders. byShaik ShoaibNo ratings yet
- Ecologic Model AsthmaDocument3 pagesEcologic Model AsthmaJaneth Cambronero CayetanoNo ratings yet
- RITS. Bronchial AsthmaDocument56 pagesRITS. Bronchial AsthmaRita100% (1)
- Connections and Differences Between Early-Onset Allergic Asthma and Xiao-ChuanDocument9 pagesConnections and Differences Between Early-Onset Allergic Asthma and Xiao-ChuaniomastNo ratings yet
- Upper Respiratory DisordersDocument37 pagesUpper Respiratory DisordersClaire Maurice JuaneroNo ratings yet
- AsthmaDocument5 pagesAsthmaThe SawggerNo ratings yet
- Asthma tiếng AnhDocument36 pagesAsthma tiếng Anh98lehaidangNo ratings yet
- Presented by Group 1Document62 pagesPresented by Group 1Gillian Miguel CanonoNo ratings yet
- Chronic Obstructive Pulmonary DiseaseDocument17 pagesChronic Obstructive Pulmonary DiseaseMark Adrian Jintalan ManzanoNo ratings yet
- CC C C C C CCC CCCCCCCCCCCC CCC C C C C C C C C C C C C C C C C CCCCCCCCCCCCCCCCCC C CCCCCCCCCCCCCCCCCCCCCCCCCCC CDocument7 pagesCC C C C C CCC CCCCCCCCCCCC CCC C C C C C C C C C C C C C C C C CCCCCCCCCCCCCCCCCC C CCCCCCCCCCCCCCCCCCCCCCCCCCC CAndreea PanteaNo ratings yet
- Asthma PDFDocument27 pagesAsthma PDFjeff homeres100% (1)
- Trivedi, 2017 - Occupational Asthma - Diagnostic Challenges and Management DilemmasDocument7 pagesTrivedi, 2017 - Occupational Asthma - Diagnostic Challenges and Management DilemmasAditya IbrahimNo ratings yet
- Asma KakakDocument3 pagesAsma KakakRozita DeramanNo ratings yet
- Content On Pediatric Asthma: Submitted To Mrs. Rupinder Kaur Lecturer Submitted by Anu George MSC Nsg. 1 YearDocument11 pagesContent On Pediatric Asthma: Submitted To Mrs. Rupinder Kaur Lecturer Submitted by Anu George MSC Nsg. 1 YeargopscharanNo ratings yet
- Case 1 Asthma QuestionareDocument3 pagesCase 1 Asthma QuestionareEduard GarchitorenaNo ratings yet
- Asthma: EpidemiologyDocument22 pagesAsthma: EpidemiologyananNo ratings yet
- Bronchial Asthma I. Objectives: A. U: - Espiratory InfectionsáDocument5 pagesBronchial Asthma I. Objectives: A. U: - Espiratory InfectionsáEnah EvangelistaNo ratings yet
- Disease Occupational OshaDocument6 pagesDisease Occupational OshabotakzxcNo ratings yet
- Asuhan Keperawatan Asma BronkhialDocument31 pagesAsuhan Keperawatan Asma BronkhialIndra PutraNo ratings yet
- AsthmaDocument5 pagesAsthmaabenezer isayasNo ratings yet
- Asthm ADocument3 pagesAsthm ADebbi YuniseraniNo ratings yet
- Lau, 2019 - Update On The Management of Occupational Asthma and Work-Exacerbated AsthmaDocument13 pagesLau, 2019 - Update On The Management of Occupational Asthma and Work-Exacerbated AsthmaAditya IbrahimNo ratings yet
- Management Work-Related AsthmaDocument7 pagesManagement Work-Related AsthmaSteven AndriieNo ratings yet
- Asthma (Christine Claire Caguimbay BSN III-D)Document1 pageAsthma (Christine Claire Caguimbay BSN III-D)Christine Claire CaguimbayNo ratings yet
- Is Asthma A Psychological Disorder?Document2 pagesIs Asthma A Psychological Disorder?putripardosiNo ratings yet
- Asthma: Vanessa T. Ucat, RN MSN 302 December 2015Document39 pagesAsthma: Vanessa T. Ucat, RN MSN 302 December 2015Vane UcatNo ratings yet
- B Inggris Halim NCP Asma BronchialDocument28 pagesB Inggris Halim NCP Asma BronchialAbdul HlmNo ratings yet
- Asma BronkialDocument18 pagesAsma BronkialLala SamosirNo ratings yet
- Primary Causes: Smoking, Alpha-1-Antitrypsin Deficiency and Air PollutionDocument10 pagesPrimary Causes: Smoking, Alpha-1-Antitrypsin Deficiency and Air PollutionLourdes DajonanNo ratings yet
- Bronchial AsthmaDocument17 pagesBronchial AsthmaUmidaNo ratings yet
- Case Study Bronchial-AsthmaDocument9 pagesCase Study Bronchial-AsthmaGabbii CincoNo ratings yet
- AsthmaDocument3 pagesAsthmaHardika Aurum PratiwiNo ratings yet
- Bronchial AsthmaDocument48 pagesBronchial AsthmaArum Ayu Kartika100% (1)
- AR and ComorbiditiesDocument17 pagesAR and ComorbiditiesHeena BhojwaniNo ratings yet
- Healthcare Quality Account 2021-22Document98 pagesHealthcare Quality Account 2021-22Adeuga ADEKUOYENo ratings yet
- Bleeding in Early Pregnancy Slide WorldDocument57 pagesBleeding in Early Pregnancy Slide Worlddashing_ritamNo ratings yet
- Eosinophilic Esophagitis in Adults: A Case Series and Literature ReviwDocument6 pagesEosinophilic Esophagitis in Adults: A Case Series and Literature ReviwIJAR JOURNALNo ratings yet
- "Sandwich" Bone Augmentation Technique-Rationale and Report of Pilot Cases PDFDocument14 pages"Sandwich" Bone Augmentation Technique-Rationale and Report of Pilot Cases PDFHector MurilloNo ratings yet
- Aahks 2019 PDFDocument36 pagesAahks 2019 PDFXiayi HuNo ratings yet
- Dengue FeverDocument8 pagesDengue FeverJay MagsaysayNo ratings yet
- Gayoso Position PaperDocument8 pagesGayoso Position PaperJayvee GayosoNo ratings yet
- Hrachovy 1989Document19 pagesHrachovy 1989YASMIN SALOMON OTERONo ratings yet
- Florence Nightingale - Environmental TheoryDocument6 pagesFlorence Nightingale - Environmental TheoryVictoria Castillo TamayoNo ratings yet
- Fdar Day 1 Psyche KarlDocument4 pagesFdar Day 1 Psyche KarlKristian Karl Bautista Kiw-is100% (1)
- Practical Hepatic Pathology A Diagnostic Approach 2Nd Edition Romil Saxena All ChapterDocument67 pagesPractical Hepatic Pathology A Diagnostic Approach 2Nd Edition Romil Saxena All Chapterpaul.wells767100% (6)
- Running Head: Evidence-Based Nursing Journal 2 1Document9 pagesRunning Head: Evidence-Based Nursing Journal 2 1rnrmmanphdNo ratings yet
- Hospital Waste ManagementDocument4 pagesHospital Waste ManagementMahrukh HaiderNo ratings yet
- JurnalDocument11 pagesJurnalNur Aliah BahmidNo ratings yet
- Brainsci 11 01171 v2Document25 pagesBrainsci 11 01171 v2Vaibhav BahelNo ratings yet
- Individual Assessment PaDocument8 pagesIndividual Assessment PaJoshua RoxasNo ratings yet
- GP Emergency Manual PDFDocument72 pagesGP Emergency Manual PDFRumana Ali100% (2)
- 30 Different Types of Doctors and What They DoDocument4 pages30 Different Types of Doctors and What They DoGemma C AlejagaNo ratings yet
- Executive SummaryDocument14 pagesExecutive SummaryDenmark LumacdayNo ratings yet
- Puncture Wound FactsDocument9 pagesPuncture Wound Factsbernard arcigaNo ratings yet
- Ahmar Metastasis Health JournalDocument9 pagesAhmar Metastasis Health JournalSyafaringga Dian oscarNo ratings yet
- Laboratory Corporation of AmericaDocument156 pagesLaboratory Corporation of AmericaJohn CollinsNo ratings yet
- 4 Edition: Guidelines For The Prevention, Treatment and Rehabilitation of Brain AttackDocument128 pages4 Edition: Guidelines For The Prevention, Treatment and Rehabilitation of Brain AttackVina EmpialesNo ratings yet
- Candida Infection in The NicuDocument78 pagesCandida Infection in The NiculordofthewebNo ratings yet
- BMC Dermatology: The Treatment of Melasma by Silymarin CreamDocument13 pagesBMC Dermatology: The Treatment of Melasma by Silymarin CreamAnna Listyana DewiNo ratings yet
- Ovarian Cancer Case StudyDocument46 pagesOvarian Cancer Case StudyAmriati100% (3)
- Diagnosis Pneumonia: M Sidhartani ZainDocument28 pagesDiagnosis Pneumonia: M Sidhartani ZainApriany Fitri SangajiNo ratings yet
- By: Kris Traver and Nitin JainDocument14 pagesBy: Kris Traver and Nitin JainMahesh BhagwatNo ratings yet
Asma Kerja
Asma Kerja
Uploaded by
anggitasilambi0 ratings0% found this document useful (0 votes)
2 views1 pageparkeling
Original Title
Asma Kerja (1)
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentparkeling
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
2 views1 pageAsma Kerja
Asma Kerja
Uploaded by
anggitasilambiparkeling
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 1
Occupational Asthma
When should someone suspect occupational asthma?
Work-related asthma is not uncommon but may be less well known. There are many explanations for
this. First, the relationship between asthma symptoms and work may not be obvious to patients.
Second, a doctor may not think to ask specifically about any work-related symptoms. Third, a
clinician may not feel confident in assessing work-related asthma. Lastly, there is limited information
regarding occupational asthma and its causes in international asthma guidelines.
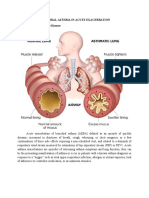
There are two main types of work-related asthma. Occupational asthma is caused by exposure to air in
the work environment. Meanwhile, in asthma that is exacerbated by work, various non-specific
factors in the workplace can worsen asthma symptoms, but the asthma is not caused by work. The
characteristics of these two conditions are not easy to distinguish from each other. Work-exacerbated
asthma is common and is estimated to affect one-fifth of working asthma patients.
Recognizing occupational asthma is challenging in many ways. For one thing, the observation that
symptoms may worsen at work (or improve afterwards) may not be possible. In addition, work-related
factors can cause asthma (either de novo or due to asthma) or can worsen pre-existing asthma
symptoms. A clinician should consider the possibility of a diagnosis of occupational asthma in
working-age patients who have new symptoms of asthma, reappearance of asthma in childhood,
worsening of asthma control, or when unexplained airflow obstruction is detected (table 1). Suspicion
will be higher if the patient works in a high-risk job or is exposed to asthma-causing agents at work
(table 2). Based on the underlying mechanisms, there are two types of occupational asthma with
different clinical features which are summarized in the following section and in table 3.
Severe asthma triggered by sensitizers
Occupational asthma triggered by sensitizers is considered the most common type of occupational
asthma and is triggered by high molecular weight or low molecular weight agents . HMW agents are
(glyco)proteins of animal, plant, or microbial origin, which have the ability to cause sensitization
mediated by immunoglobulin (Ig) E. LMW agents are synthetic chemicals, metals, and other natural
agents that are thought to cause immunological reactions , however specific IgE antibodies are often
not detected (table 2). Occupational asthma triggered by sensitizers always requires repeated periods
of exposure to the allergen before the onset of symptoms. It is during this “latent period” that
sensitization and immunological responses develop. The latent period can vary from weeks to years,
but the highest risk of developing asthma is in the first 2 years after exposure.
Asthma symptoms that improve after leaving work also increase the likelihood of a diagnosis of
occupational asthma, but the relationship between symptoms and work is not always clear. Some
occupational asthma patients may report that their symptoms occur at work or while doing certain
jobs, while others may experience more pronounced symptoms in the afternoon or evening, that is,
outside the workplace. In addition, triggers outside of work, such as cigarette smoke, exercise, and
cold air, can worsen existing symptoms. The pattern of overt work-related symptoms generally
decreases with increasing duration of asthma. These features emphasize the importance of considering
the possibility of occupational asthma, even when the patient experiences few symptoms at work and
most symptoms outside the workplace. Occupational asthma caused by HMW agents is more
common in people with atopy and almost always occurs in conjunction with occupational rhinitis and
conjunctivitis. These symptoms may begin before, or at the same time as, asthma symptoms.
Therefore, any patient with work-related upper or lower respiratory symptoms should raise clinical
suspicion. Occupational asthma induced by LMW agents is less common in rhinitis, and usually has a
delayed asthmatic response, especially compared with asthma induced by HMW agents.
You might also like
- Pathology For The Physical Therapist Assistant e Book 2nd Edition Ebook PDFDocument62 pagesPathology For The Physical Therapist Assistant e Book 2nd Edition Ebook PDFrobert.short87298% (53)
- Lehnes Pharmacotherapeutics For Advanced Practice Providers Ebook PDFDocument39 pagesLehnes Pharmacotherapeutics For Advanced Practice Providers Ebook PDFmarilyn.llamas494100% (42)
- Bronchial Asthma in Acute Exacerbation Case StudyDocument43 pagesBronchial Asthma in Acute Exacerbation Case Studyroseanne parkNo ratings yet
- Work-Related Asthma - Pulmonary Disorders - MSD Manual Professional EditionDocument6 pagesWork-Related Asthma - Pulmonary Disorders - MSD Manual Professional Editionpeterpavel112No ratings yet
- Asthma: Home OSH Answers Diseases, Disorders & InjuriesDocument7 pagesAsthma: Home OSH Answers Diseases, Disorders & InjuriesNashon_AsekaNo ratings yet
- Occupational Asthma 2Document7 pagesOccupational Asthma 2drunkpunchloveNo ratings yet
- Description of AsthmaDocument14 pagesDescription of AsthmaManayu WidaswariNo ratings yet
- Occupational Asthma Occupational Asthma: Sri Handayani LubisDocument19 pagesOccupational Asthma Occupational Asthma: Sri Handayani LubisdonkeyendutNo ratings yet
- Astm ErsDocument9 pagesAstm ErsAdrian RomanNo ratings yet
- Asthma InformationDocument10 pagesAsthma InformationSheen aballeNo ratings yet
- Bronchial Asthma: Made By: Sonakshi Chauhan Rollno. 81 BATCH: 2015-2016Document14 pagesBronchial Asthma: Made By: Sonakshi Chauhan Rollno. 81 BATCH: 2015-2016anshul100% (1)
- ASTHMA IllnessDocument8 pagesASTHMA IllnessJM MARQUEZNo ratings yet
- Asthma: Signs and SymptomsDocument6 pagesAsthma: Signs and Symptomstresdos09No ratings yet
- Asthma 2Document8 pagesAsthma 2Evangelist Stephen NziokaNo ratings yet
- Asthma: Prepared By: Genesis T. Consigna. BSN-3Document10 pagesAsthma: Prepared By: Genesis T. Consigna. BSN-3Digital ExpressNo ratings yet
- UAS Inggris (Final Test)Document2 pagesUAS Inggris (Final Test)Iga AmandaNo ratings yet
- AsthmaDocument43 pagesAsthmaPriyanka PNo ratings yet
- 4 Bronchial AsthmaDocument9 pages4 Bronchial Asthmashanfiza_92No ratings yet
- Occupational Bronchitis Asthma enDocument47 pagesOccupational Bronchitis Asthma enel spin artifactNo ratings yet
- AEBA QUESTIONS-WPS OfficeDocument2 pagesAEBA QUESTIONS-WPS OfficeMarj Castor LisondraNo ratings yet
- Asthma: Asthma (From The GreekDocument2 pagesAsthma: Asthma (From The GreekSteffiDoNo ratings yet
- Concept Map DraftsDocument9 pagesConcept Map DraftsFc CrisostomoNo ratings yet
- The Bronchial AsthmaDocument5 pagesThe Bronchial AsthmaKathleen Anne CajandingNo ratings yet
- Presentation Copd Asthma 2022Document65 pagesPresentation Copd Asthma 2022Pwani aquaponicsNo ratings yet
- Dental Management of Patients With Respiratory Disease: (Copd)Document12 pagesDental Management of Patients With Respiratory Disease: (Copd)Fahd AlahaidebNo ratings yet
- Occupational Airways Disease: Key PointsDocument4 pagesOccupational Airways Disease: Key PointsAlba D'kiferz EvridNo ratings yet
- An Assignment On Pathophysiology and Drug Therapy of Respiratory Disorders. byDocument34 pagesAn Assignment On Pathophysiology and Drug Therapy of Respiratory Disorders. byShaik ShoaibNo ratings yet
- Ecologic Model AsthmaDocument3 pagesEcologic Model AsthmaJaneth Cambronero CayetanoNo ratings yet
- RITS. Bronchial AsthmaDocument56 pagesRITS. Bronchial AsthmaRita100% (1)
- Connections and Differences Between Early-Onset Allergic Asthma and Xiao-ChuanDocument9 pagesConnections and Differences Between Early-Onset Allergic Asthma and Xiao-ChuaniomastNo ratings yet
- Upper Respiratory DisordersDocument37 pagesUpper Respiratory DisordersClaire Maurice JuaneroNo ratings yet
- AsthmaDocument5 pagesAsthmaThe SawggerNo ratings yet
- Asthma tiếng AnhDocument36 pagesAsthma tiếng Anh98lehaidangNo ratings yet
- Presented by Group 1Document62 pagesPresented by Group 1Gillian Miguel CanonoNo ratings yet
- Chronic Obstructive Pulmonary DiseaseDocument17 pagesChronic Obstructive Pulmonary DiseaseMark Adrian Jintalan ManzanoNo ratings yet
- CC C C C C CCC CCCCCCCCCCCC CCC C C C C C C C C C C C C C C C C CCCCCCCCCCCCCCCCCC C CCCCCCCCCCCCCCCCCCCCCCCCCCC CDocument7 pagesCC C C C C CCC CCCCCCCCCCCC CCC C C C C C C C C C C C C C C C C CCCCCCCCCCCCCCCCCC C CCCCCCCCCCCCCCCCCCCCCCCCCCC CAndreea PanteaNo ratings yet
- Asthma PDFDocument27 pagesAsthma PDFjeff homeres100% (1)
- Trivedi, 2017 - Occupational Asthma - Diagnostic Challenges and Management DilemmasDocument7 pagesTrivedi, 2017 - Occupational Asthma - Diagnostic Challenges and Management DilemmasAditya IbrahimNo ratings yet
- Asma KakakDocument3 pagesAsma KakakRozita DeramanNo ratings yet
- Content On Pediatric Asthma: Submitted To Mrs. Rupinder Kaur Lecturer Submitted by Anu George MSC Nsg. 1 YearDocument11 pagesContent On Pediatric Asthma: Submitted To Mrs. Rupinder Kaur Lecturer Submitted by Anu George MSC Nsg. 1 YeargopscharanNo ratings yet
- Case 1 Asthma QuestionareDocument3 pagesCase 1 Asthma QuestionareEduard GarchitorenaNo ratings yet
- Asthma: EpidemiologyDocument22 pagesAsthma: EpidemiologyananNo ratings yet
- Bronchial Asthma I. Objectives: A. U: - Espiratory InfectionsáDocument5 pagesBronchial Asthma I. Objectives: A. U: - Espiratory InfectionsáEnah EvangelistaNo ratings yet
- Disease Occupational OshaDocument6 pagesDisease Occupational OshabotakzxcNo ratings yet
- Asuhan Keperawatan Asma BronkhialDocument31 pagesAsuhan Keperawatan Asma BronkhialIndra PutraNo ratings yet
- AsthmaDocument5 pagesAsthmaabenezer isayasNo ratings yet
- Asthm ADocument3 pagesAsthm ADebbi YuniseraniNo ratings yet
- Lau, 2019 - Update On The Management of Occupational Asthma and Work-Exacerbated AsthmaDocument13 pagesLau, 2019 - Update On The Management of Occupational Asthma and Work-Exacerbated AsthmaAditya IbrahimNo ratings yet
- Management Work-Related AsthmaDocument7 pagesManagement Work-Related AsthmaSteven AndriieNo ratings yet
- Asthma (Christine Claire Caguimbay BSN III-D)Document1 pageAsthma (Christine Claire Caguimbay BSN III-D)Christine Claire CaguimbayNo ratings yet
- Is Asthma A Psychological Disorder?Document2 pagesIs Asthma A Psychological Disorder?putripardosiNo ratings yet
- Asthma: Vanessa T. Ucat, RN MSN 302 December 2015Document39 pagesAsthma: Vanessa T. Ucat, RN MSN 302 December 2015Vane UcatNo ratings yet
- B Inggris Halim NCP Asma BronchialDocument28 pagesB Inggris Halim NCP Asma BronchialAbdul HlmNo ratings yet
- Asma BronkialDocument18 pagesAsma BronkialLala SamosirNo ratings yet
- Primary Causes: Smoking, Alpha-1-Antitrypsin Deficiency and Air PollutionDocument10 pagesPrimary Causes: Smoking, Alpha-1-Antitrypsin Deficiency and Air PollutionLourdes DajonanNo ratings yet
- Bronchial AsthmaDocument17 pagesBronchial AsthmaUmidaNo ratings yet
- Case Study Bronchial-AsthmaDocument9 pagesCase Study Bronchial-AsthmaGabbii CincoNo ratings yet
- AsthmaDocument3 pagesAsthmaHardika Aurum PratiwiNo ratings yet
- Bronchial AsthmaDocument48 pagesBronchial AsthmaArum Ayu Kartika100% (1)
- AR and ComorbiditiesDocument17 pagesAR and ComorbiditiesHeena BhojwaniNo ratings yet
- Healthcare Quality Account 2021-22Document98 pagesHealthcare Quality Account 2021-22Adeuga ADEKUOYENo ratings yet
- Bleeding in Early Pregnancy Slide WorldDocument57 pagesBleeding in Early Pregnancy Slide Worlddashing_ritamNo ratings yet
- Eosinophilic Esophagitis in Adults: A Case Series and Literature ReviwDocument6 pagesEosinophilic Esophagitis in Adults: A Case Series and Literature ReviwIJAR JOURNALNo ratings yet
- "Sandwich" Bone Augmentation Technique-Rationale and Report of Pilot Cases PDFDocument14 pages"Sandwich" Bone Augmentation Technique-Rationale and Report of Pilot Cases PDFHector MurilloNo ratings yet
- Aahks 2019 PDFDocument36 pagesAahks 2019 PDFXiayi HuNo ratings yet
- Dengue FeverDocument8 pagesDengue FeverJay MagsaysayNo ratings yet
- Gayoso Position PaperDocument8 pagesGayoso Position PaperJayvee GayosoNo ratings yet
- Hrachovy 1989Document19 pagesHrachovy 1989YASMIN SALOMON OTERONo ratings yet
- Florence Nightingale - Environmental TheoryDocument6 pagesFlorence Nightingale - Environmental TheoryVictoria Castillo TamayoNo ratings yet
- Fdar Day 1 Psyche KarlDocument4 pagesFdar Day 1 Psyche KarlKristian Karl Bautista Kiw-is100% (1)
- Practical Hepatic Pathology A Diagnostic Approach 2Nd Edition Romil Saxena All ChapterDocument67 pagesPractical Hepatic Pathology A Diagnostic Approach 2Nd Edition Romil Saxena All Chapterpaul.wells767100% (6)
- Running Head: Evidence-Based Nursing Journal 2 1Document9 pagesRunning Head: Evidence-Based Nursing Journal 2 1rnrmmanphdNo ratings yet
- Hospital Waste ManagementDocument4 pagesHospital Waste ManagementMahrukh HaiderNo ratings yet
- JurnalDocument11 pagesJurnalNur Aliah BahmidNo ratings yet
- Brainsci 11 01171 v2Document25 pagesBrainsci 11 01171 v2Vaibhav BahelNo ratings yet
- Individual Assessment PaDocument8 pagesIndividual Assessment PaJoshua RoxasNo ratings yet
- GP Emergency Manual PDFDocument72 pagesGP Emergency Manual PDFRumana Ali100% (2)
- 30 Different Types of Doctors and What They DoDocument4 pages30 Different Types of Doctors and What They DoGemma C AlejagaNo ratings yet
- Executive SummaryDocument14 pagesExecutive SummaryDenmark LumacdayNo ratings yet
- Puncture Wound FactsDocument9 pagesPuncture Wound Factsbernard arcigaNo ratings yet
- Ahmar Metastasis Health JournalDocument9 pagesAhmar Metastasis Health JournalSyafaringga Dian oscarNo ratings yet
- Laboratory Corporation of AmericaDocument156 pagesLaboratory Corporation of AmericaJohn CollinsNo ratings yet
- 4 Edition: Guidelines For The Prevention, Treatment and Rehabilitation of Brain AttackDocument128 pages4 Edition: Guidelines For The Prevention, Treatment and Rehabilitation of Brain AttackVina EmpialesNo ratings yet
- Candida Infection in The NicuDocument78 pagesCandida Infection in The NiculordofthewebNo ratings yet
- BMC Dermatology: The Treatment of Melasma by Silymarin CreamDocument13 pagesBMC Dermatology: The Treatment of Melasma by Silymarin CreamAnna Listyana DewiNo ratings yet
- Ovarian Cancer Case StudyDocument46 pagesOvarian Cancer Case StudyAmriati100% (3)
- Diagnosis Pneumonia: M Sidhartani ZainDocument28 pagesDiagnosis Pneumonia: M Sidhartani ZainApriany Fitri SangajiNo ratings yet
- By: Kris Traver and Nitin JainDocument14 pagesBy: Kris Traver and Nitin JainMahesh BhagwatNo ratings yet