Professional Documents
Culture Documents
Article
Article
Uploaded by
Dino LjesnjaninCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Article
Article
Uploaded by
Dino LjesnjaninCopyright:
Available Formats
Spermatocele
A spermatocele is a benign, painless cystic mass that is filled with
seminal fluid and may also contain sperm. It is usually located above
or behind the testicle, but it is palpably separate from the testicle.
Spermatocele occurs in men of any age, the size is usually up to 10 mm,
but some can be significantly larger. The cause of its formation is not
clear, it is assumed that it arises from the expansion of the tubules with
subsequent fluid retention.
Clinical picture
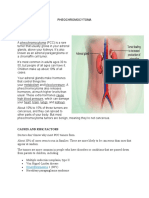
In most cases, spermatocele is asymptomatic , it can be detected during Ultrasound imaging of the spermatocele: the
testis is homogeneously echogenic, the fluid
palpation. A larger formation can cause a feeling of heaviness and
in the spermatocele is anechoic (black)
pressure in the scrotum, patients can feel a larger spermatocele
themselves.
Diagnostics and differential diagnosis
The basis of diagnosis is anamnesis. We ask the patient about the duration, we are interested in whether the
formation arose in connection with inflammation or trauma. We examine the scrotum by palpation standing and
lying down, we find a palpable mass. We use an ultrasound examination to confirm the spermatocele.
In the differential diagnosis we must distinguish between hydrocele, varicocele and cancer in the area of the
testicle or epididymis. The hardness of the testicle indicates a tumorous finding, the more elastic the formation, the
greater the probability that it is a spermatocele. Oncological origin is more suspected in younger men, in whom the
incidence of testicular tumors is higher. Pain is not a typical symptom of either a tumor or a spermatocele.
Tumor markers will also help us differentiate - we collect alfa-fetoprotein, β-hCG, we are also interested in the
value of lactate dehydrogenase (serum concentration of LDH is suitable for monitoring the growth and
regression of various malignancies) [1].
Therapy
In therapy, we choose between conservative and operative solutions. In asymptomatic patients with a smaller
spermatocele, we usually just observe the finding. Aspiration of the contents of the cyst is possible, but the fluid
usually replenishes over time.
Symptomatic spermatoceles are indicated for surgical treatment, we perform simple enucleation from the
scrotal approach. The procedure takes place under general or spinal anesthesia and takes approximately thirty
minutes. After opening the testicles, we remove the entire cystic formation.
We choose therapy individually for infertile men with azoospermia. The contents of the spermatocoel may be the
last possible source of sperm that we could obtain for assisted reproduction methods.
The main complications of surgery are testicular atrophy and recurrence of spermatocele.
Links
Related articles
Hydrocele
Varicocele
Reference
1. ABRAHÁMOVÁ, Jitka. Testicular tumors. Postgraduate medicine [online]. 2003, y. 5, vol. 6, p. 599-
615, Available from <https://zdravi.euro.cz/clanek/postgradualni-medicina/nadory-varlat-156493>.
Recommended literature
HANUŠ, Tomáš – MACEK, Petr, et al. Urology for medical professionals. 1. edition. 2015. 305 pp. ISBN
9788024630083.
1. Doporučené postupy pro praktické lékaře, Hydrokéla, varikokéla, spermatokéla. 2002. pp. 2-3. Available
from <www.cls.cz/dokumenty2/os/t178.rtf>.
You might also like
- EFSET (B2 Upper Intermediate)Document3 pagesEFSET (B2 Upper Intermediate)chandran_witts100% (1)
- (GUS 2) Bladder, Prostat, TestisDocument42 pages(GUS 2) Bladder, Prostat, TestisArifin SiregarNo ratings yet
- Testicular Cancer Is A Disease in Which Cells Become Malignant (Cancerous) inDocument5 pagesTesticular Cancer Is A Disease in Which Cells Become Malignant (Cancerous) inAngel CastroNo ratings yet
- SpermatoceleDocument6 pagesSpermatoceleDae AhmadNo ratings yet
- Testicle UltrasoundDocument5 pagesTesticle UltrasoundJan Karl Roelhsen AngelesNo ratings yet
- Diagnostic Work Up of Ovarian CystsDocument13 pagesDiagnostic Work Up of Ovarian Cystsririn selagalasNo ratings yet
- GUS2-K8-scrotal SwellingDocument35 pagesGUS2-K8-scrotal SwellingYohanna SinuhajiNo ratings yet
- Rangkuman TeratomaDocument22 pagesRangkuman TeratomaFelicia Fernanda IskandarNo ratings yet
- Testicular Torsion - StatPearls - NCBI BookshelfDocument6 pagesTesticular Torsion - StatPearls - NCBI Bookshelfwijana410No ratings yet
- DIQUE Polypectomy Possible Endometrial SamplingDocument5 pagesDIQUE Polypectomy Possible Endometrial Samplingmarjorie Dela CruzNo ratings yet
- Endometriosis: by Jane LyttletonDocument8 pagesEndometriosis: by Jane Lyttletonitsik12886No ratings yet
- Imaging of Adnexal Masses123Document41 pagesImaging of Adnexal Masses123Tsega HagosNo ratings yet
- Pathophysiology: Each Month, Normally Functioning Ovaries Develop SmallDocument9 pagesPathophysiology: Each Month, Normally Functioning Ovaries Develop SmallAl-nazer Azer Al100% (1)
- Group 4 Anatomy Assignment SubmissionDocument24 pagesGroup 4 Anatomy Assignment SubmissionGraceNo ratings yet
- Subject Date Professor Sbobinatore: (Armando Muro) ReviewerDocument10 pagesSubject Date Professor Sbobinatore: (Armando Muro) ReviewerÁngel Parra CominoNo ratings yet
- Testicular CancerDocument3 pagesTesticular CancerSherief MansourNo ratings yet
- ROLE OF FNAC TESTIS IN MALE INFERTILITY by SpandanaDocument61 pagesROLE OF FNAC TESTIS IN MALE INFERTILITY by SpandanaDineshprakash GovindhrajNo ratings yet
- Disorders of Testicles & ScrotumDocument10 pagesDisorders of Testicles & ScrotumAli SafaaNo ratings yet
- Benign and Malignat Ovarian TumorsDocument67 pagesBenign and Malignat Ovarian TumorsZEMENAY TRUNEHNo ratings yet
- Bladder CancerDocument3 pagesBladder CancerGhea Jovita SinagaNo ratings yet
- Benign Ovarian Tumors-1Document45 pagesBenign Ovarian Tumors-1abdulghani100% (1)
- SM 1Document12 pagesSM 1welinNo ratings yet
- Abnormalities of The EndometriumDocument3 pagesAbnormalities of The EndometriumDymas R SyahputraNo ratings yet
- Ovarian Germ Cell Tumors TreatmentDocument6 pagesOvarian Germ Cell Tumors TreatmentSoleh SundawaNo ratings yet
- Women Health Presentation (Ovarian Cyst)Document17 pagesWomen Health Presentation (Ovarian Cyst)Lim Su-WeiNo ratings yet
- Case6. ERISGRUPtesticularcancerDocument3 pagesCase6. ERISGRUPtesticularcancerJardee DatsimaNo ratings yet
- Perimenopausal Bleeding and Bleeding After MenopauseDocument5 pagesPerimenopausal Bleeding and Bleeding After MenopauseAnonymous KwWTUPjXNo ratings yet
- Scrotal SwellingDocument34 pagesScrotal SwellingViviViviNo ratings yet
- EndometriosisDocument46 pagesEndometriosisManoj Ranadive0% (1)
- Case Report 30-09-2014Document5 pagesCase Report 30-09-2014zeeshan arshadNo ratings yet
- Undescended TestisDocument2 pagesUndescended TestisdyarraNo ratings yet
- SpermatoceleDocument2 pagesSpermatocelemrizkidm2301No ratings yet
- ChaptDocument8 pagesChaptmamaljonNo ratings yet
- PDF HematospermiaDocument7 pagesPDF HematospermiaBayu PramanaNo ratings yet
- Varicocele, Spermatocele, HydroceleDocument35 pagesVaricocele, Spermatocele, HydroceleSurya ArhNo ratings yet
- Acute Scrotum PDFDocument9 pagesAcute Scrotum PDFJody FelizioNo ratings yet
- Screening, Early Sign & Classification of CancerDocument50 pagesScreening, Early Sign & Classification of CancerVinay SahuNo ratings yet
- Benign Lesions of The OvariesDocument12 pagesBenign Lesions of The OvariesdocjosmaNo ratings yet
- Testicular Self ExaminationDocument17 pagesTesticular Self ExaminationKath Costiniano50% (4)
- Male Reproductive DisordersDocument5 pagesMale Reproductive DisorderslordwinjohnbernardoNo ratings yet
- Torsio TestisDocument55 pagesTorsio TestisAulia RizkiaNo ratings yet
- Yolk Sac Tumor EmedicineDocument5 pagesYolk Sac Tumor EmedicineUtiya Nur LailiNo ratings yet
- Myoma Uteri/Fibroids/ Leiomyomata: Symptoms of Uterine Myoma May IncludeDocument3 pagesMyoma Uteri/Fibroids/ Leiomyomata: Symptoms of Uterine Myoma May IncludeDiane MargretNo ratings yet
- Benign Gynecological LesionsDocument9 pagesBenign Gynecological LesionsLanceNo ratings yet
- Ovarian Teratom-WPS OfficeDocument15 pagesOvarian Teratom-WPS OfficeAbdulwahab NuraminNo ratings yet
- 2.2 Gyn Pathology OvaryDocument0 pages2.2 Gyn Pathology OvarydinapurpleloversNo ratings yet
- 2 2019 02 09!12 08 16 PMDocument34 pages2 2019 02 09!12 08 16 PMPrakask BalanNo ratings yet
- Testicular Cancer Charyl Jane C. Acut Central Mindanao University College of Nursing Theresa Linda Narreto-PinaganDocument4 pagesTesticular Cancer Charyl Jane C. Acut Central Mindanao University College of Nursing Theresa Linda Narreto-PinaganCyril Jane Caanyagan AcutNo ratings yet
- Assignment 1 (Cancer)Document8 pagesAssignment 1 (Cancer)Leo Aurelio MarcelinoNo ratings yet
- Anatomy and Physiology of PlacentaDocument5 pagesAnatomy and Physiology of PlacentaAmuNo ratings yet
- Anatomy and Physiology of PlacentaDocument5 pagesAnatomy and Physiology of PlacentaAdrianne Basa100% (1)
- Gynecology Adnexal MassDocument2 pagesGynecology Adnexal MassgeNo ratings yet
- DR Sankalpa R WankhedeDocument76 pagesDR Sankalpa R Wankhedechaitanya suryawanshiNo ratings yet
- Gynecology - Vaginal Bleeding 3Document2 pagesGynecology - Vaginal Bleeding 3Ansley MadalaNo ratings yet
- Postmenopausal Bleeding - StatPearls - NCBI BooksDocument11 pagesPostmenopausal Bleeding - StatPearls - NCBI BooksKalaivathanan VathananNo ratings yet
- Gynecology - Adnexal MassDocument2 pagesGynecology - Adnexal MassAnsley MadalaNo ratings yet
- Revised Reproductive SystemDocument26 pagesRevised Reproductive SystemJaded KaysarNo ratings yet
- What Is Osteosarcoma? A.K.A: Osteogenic SarcomaDocument5 pagesWhat Is Osteosarcoma? A.K.A: Osteogenic SarcomaDan Leo UnicoNo ratings yet
- Pheochromocytoma: Causes and Risk FactorsDocument4 pagesPheochromocytoma: Causes and Risk FactorsJohanna Recca MarinoNo ratings yet
- (LIT) LS90 LS110 LS160 BrochureDocument20 pages(LIT) LS90 LS110 LS160 BrochureJuan Carlos Reinhold Niembro SuchowitzkiNo ratings yet
- Infinitigeneralcatalog Compressed (1) CompressedDocument31 pagesInfinitigeneralcatalog Compressed (1) CompressedBilher SihombingNo ratings yet
- PSYC 1504 Discussion Forum Unit 5Document2 pagesPSYC 1504 Discussion Forum Unit 5keshanirathnayake745No ratings yet
- Word PartsDocument15 pagesWord PartsDr. Zakir HorizontalNo ratings yet
- Some Oral Chief Mate QuestionsDocument6 pagesSome Oral Chief Mate QuestionsKapil KhandelwalNo ratings yet
- 22 11 13 - Facility Water Distribution Piping PDFDocument11 pages22 11 13 - Facility Water Distribution Piping PDFmasoodaeNo ratings yet
- PandasDocument1,349 pagesPandasMichael GemminkNo ratings yet
- MCQ ObgDocument3 pagesMCQ ObgSahil sharma100% (1)
- Filipino American RelationshipDocument3 pagesFilipino American RelationshipSamuel Grant ZabalaNo ratings yet
- Speed Control of DC Motor Using Fuzzy PID ControllerDocument15 pagesSpeed Control of DC Motor Using Fuzzy PID Controllerthhluong.sdh232No ratings yet
- ICoMaSEdu Paper TemplateDocument6 pagesICoMaSEdu Paper TemplateRusly HidayahNo ratings yet
- Me 321: Fluid Mechanics-I: Dr. A.B.M. Toufique HasanDocument12 pagesMe 321: Fluid Mechanics-I: Dr. A.B.M. Toufique HasanankitaNo ratings yet
- Brunssen Onevoiceone 2017Document8 pagesBrunssen Onevoiceone 2017stephenieleevos1No ratings yet
- PCNE WorkbookDocument83 pagesPCNE WorkbookDaniel N Sherine FooNo ratings yet
- Petroleum & Petrochemicals Test Method Capabilities: Intertek Caleb Brett 1Document18 pagesPetroleum & Petrochemicals Test Method Capabilities: Intertek Caleb Brett 1Eng-sadeq HesseinNo ratings yet
- AFAR-09 (Separate & Consolidated Financial Statements)Document10 pagesAFAR-09 (Separate & Consolidated Financial Statements)Hasmin AmpatuaNo ratings yet
- ME - Paper 3 - Part B1 - Data FileDocument12 pagesME - Paper 3 - Part B1 - Data Filemmontagne1No ratings yet
- s7 200 Smart Pid ManualDocument37 pagess7 200 Smart Pid ManualSửa chữa Biến Tần - Servo - UPSNo ratings yet
- Comaroff, John L. Rules and Rulers. Political Processes in A Tswana ChiefdownDocument21 pagesComaroff, John L. Rules and Rulers. Political Processes in A Tswana ChiefdownDiego AlbertoNo ratings yet
- Confessions of Some High Ranking 1Document111 pagesConfessions of Some High Ranking 1Habilian AssociationNo ratings yet
- Kaise KB1218 - Hoja de DatosDocument2 pagesKaise KB1218 - Hoja de DatosGermanYPNo ratings yet
- Gis Prac1Document126 pagesGis Prac1Brijesh JavakeNo ratings yet
- Confined Space Hazards AwarenessDocument27 pagesConfined Space Hazards AwarenessNoor Fadilah Printis100% (1)
- 1) AISC Standards and PublicationsDocument6 pages1) AISC Standards and PublicationsJonatan MamaniNo ratings yet
- Common Law Pleading Regarding Name ChangesDocument54 pagesCommon Law Pleading Regarding Name ChangesgmsapiensNo ratings yet
- Hasegawa v. Giron, G.R. No. 184536, August 14, 2013Document6 pagesHasegawa v. Giron, G.R. No. 184536, August 14, 2013Braian HitaNo ratings yet
- Stress Concentrations at Holes in Thin Rotating Discs: ANG L. TANDocument3 pagesStress Concentrations at Holes in Thin Rotating Discs: ANG L. TANKris SmaczekNo ratings yet
- Chi-Square and Related DistributionDocument7 pagesChi-Square and Related DistributionMohammedseid AhmedinNo ratings yet
- Bio 1 SeriesDocument4 pagesBio 1 SerieskisesarevNo ratings yet