Professional Documents
Culture Documents
ATOWTutorial 509
ATOWTutorial 509
Uploaded by
caioaccorsiOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
ATOWTutorial 509
ATOWTutorial 509
Uploaded by
caioaccorsiCopyright:
Available Formats
INTENSIVE CARE Tutorial 509
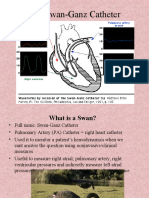
The Pulmonary Artery Catheter
Dr Gillian Crowe1†, Dr Carrie Murphy2, Dr Ian Conrick-Martin3
1
Specialist Registrar in Anaesthesia, Mater Misericordiae University Hospital, Dublin, Ireland
2
Fellow in Intensive Care Medicine, Mater Misericordiae University Hospital, Dublin, Ireland
3
Consultant Intensivist, Mater Misericordiae University Hospital, Dublin, Ireland
Edited by: Dr Julia Weinkauf
†
Corresponding author email: gcrowe@tcd.ie
Published 7 November 2023
KEY POINTS
• Pulmonary artery catheters (PACs) may be used to measure key physiological variables, including cardiac output,
and provide an estimate of left ventricular preload.
• Insertion of a PAC is not without risk and requires knowledge of right heart pressures.
• Evidence for the use of PACs in terms of mortality benefit has been conflicting, but in the correct clinical context, they
can provide essential information to guide changes in management of vasoactive supports and fluid therapies.
INTRODUCTION
The pulmonary artery catheter (PAC) is a versatile monitoring device capable of direct, simultaneous measurement of pulmo-
nary and cardiac pressures and oxygen saturation, and indirect calculation of a wide array of haemodynamic parameters
including cardiac output (CO) and systemic and pulmonary vascular resistance.
HISTORY
Right heart catheterisation was first described in humans in 1929 by Dr Werner Forssman, who performed it on himself using a
4 French ureteric catheter via his antecubital fossa. Subsequent investigators described the use of right heart catheterisation
to measure intracardiac pressures, including pulmonary capillary wedge pressure (PCWP), which was found to correlate
closely with pressure in the left atrium (LA). The 1956 Nobel Prize for Medicine was shared between Werner Forssmann and
Columbia University’s Cournand and Richards who estimated CO using mixed venous and arterial blood oxygen content,
employing right heart catheters for sampling. Dye and thermodilution techniques using the Fick principle were subsequently
employed during the 1960s to approximate CO.1
Catheterisation of the right heart was mostly limited to the cardiac catheterisation lab as it required fluoroscopic assistance
until the development of the balloon-tipped, flow-directed PAC by Swan and Ganz in 1970.2 This catheter could be rapidly
inserted at the bedside, and advanced into the wedge position for estimation of LA pressure. Furthermore, it could be left in
situ for serial measurements allowing physicians to measure and adjust preload and vascular resistance and immediately eval-
uate the response to therapy.
Unfortunately, the benefits of the PAC as a monitoring device have not translated into improved mortality in the majority of
patients. Although the popularity of PACs has declined significantly in recent years, there still exist several important indica-
tions for their use. A knowledge of their insertion and potential complications, as well as interpretation of PAC measurements,
is still essential for the anaesthetist and intensivist.
An online test is available for self-directed continuous medical education (CME). It is estimated to take 1 hour
to complete. Please record time spent and report this to your accrediting body if you wish to claim CME points. TAKE ONLINE TEST
A certificate will be awarded upon passing the test. Please refer to the accreditation policy here.
Subscribe to ATOTW tutorials by visiting https://resources.wfsahq.org/anaesthesia-tutorial-of-the-week/
ATOTW 509 — The Pulmonary Artery Catheter (7 November 2023) Page 1 of 8
STRUCTURE OF THE PAC CATHETER
Standard PACs for use in adults (Figure 1) are 5 to 8 French and 100 to 110 cm long. They are usually inserted via a short,
wide-bore PAC introducer sheath. The catheters are marked at 10-cm intervals to facilitate identification of catheter depth. A
plastic sheath with a locking mechanism allows for the catheter to remain sterile as it is moved in and out during wedging.
PACs have between 3 and 5 lumens depending on the model.
Lumens
Pulmonary Artery (PA) Pressure Transducer/Sampling Lumen (Yellow)
The tip of the catheter has a single open lumen which is used to transduce pulmonary artery (PA) pressures and to take PA
blood samples.
Balloon Inflation Lumen (Red)
This lumen is used to inflate and deflate the balloon found at the tip of the catheter with 1.5 ml of air to allow wedging. Usually,
a specialised volume-limited syringe is supplied which prevents inflation above this volume to avoid trauma to the PA.
Thermistor Lumen/Connector
The third lumen contains two insulated wires leading to a thermistor that is approximately 3.7 cm from the catheter tip. This
measures the change in temperature of the blood as it flows past during thermodilution measurement of CO.
Some PACs may have a thermal heating filament to allow for continuous thermodilution CO monitoring. These models have
an additional connector to power the heating filament.
Proximal Lumens(s) (Blue/White)
The proximal lumen should open in the right atrium (RA), being positioned about 26 to 30 cm from the catheter tip. It is used to
administer the cold injectate during cardiac output measurement. A second, more proximal, lumen designated as the ‘venous
infusion port’ (VIP) may be present for drug infusions depending on the catheter design.
Figure 1. Structure of the pulmonary artery catheter. VIP indicated venous infusion port.
Subscribe to ATOTW tutorials by visiting https://resources.wfsahq.org/anaesthesia-tutorial-of-the-week/
ATOTW 509 — The Pulmonary Artery Catheter (7 November 2023) Page 2 of 8
Additional Features
Some catheters also have an optical sensor for continuous mixed venous oxygen saturation readings and pacing wires.
RIGHT HEART PRESSURES AND PCWP
The pressure waveform transduced from the tip of the PAC changes in a predictable manner as the catheter is advanced through
the chambers of the right heart and into the PA (Figure 2). The PCWP is obtained by inflating the balloon on the tip of the catheter
and advancing until the pulsatile PA wave disappears, being replaced by an atrial waveform.
When the balloon is wedged, flow through the pulmonary circulation distal to the balloon is stopped. Thus, there is a static column
of blood between the catheter tip, through the pulmonary capillary bed and into the LA, and PCWP should therefore be equivalent
to LA pressure. Under normal conditions (and in particular normal transmitral flow), the LA pressure should equal the left ventricu-
lar end diastolic pressure (LVEDP), which may act as a surrogate measure of left ventricular end diastolic volume (LVEDV) and
thus left ventricular preload.
Limitations of PCWP
PCWP may not reliably represent LVEDP in the following situations:
Non-West Zone 3 Catheter Tip Position
PCWP may only represent LA pressure (and thus LVEDP) when there is an uninterrupted column of blood between the wedged
catheter and the LA. This will only occur in the West zone 3 where pulmonary capillary pressure is greater than alveolar pressure.
Practically speaking, this is below the level of the LA or behind it in the supine position. Of note, high intrathoracic pressures (eg
high positive end-expiratory pressure) and hypovolaemia may produce a similar non–zone 3 effect, with an artificially low PCWP.
Mitral Regurgitation and Poor Left Ventricular Compliance
Large regurgitant pressure waves (visible on the PCWP trace as ‘v’ waves), or high pressures generated during atrial systole
to fill a poorly compliant left ventricle may result in high mean atrial pressures above actual LVEDP.
Mechanical Obstruction
Pulmonary venous obstruction, mechanical atrial obstruction or a poorly compliant atrium can result in PCWP in excess of
actual LA (and thus LVEDP) pressure.
Figure 2. Pressure waveforms encountered on advancing the pulmonary artery catheter through the right heart.
Subscribe to ATOTW tutorials by visiting https://resources.wfsahq.org/anaesthesia-tutorial-of-the-week/
ATOTW 509 — The Pulmonary Artery Catheter (7 November 2023) Page 3 of 8
It is also important to note that LVEDP is not always a reliable estimate of LVEDV. LVEDV may be reduced with deceptively
normal LVEDPs in the context of cardiac tamponade or a poorly compliant left ventricle.
ESTIMATING CO
CO is estimated with a PAC using thermodilution, which can be classified as an indicator-dilution method.3 Indicator-dilution
methods are based on the premise that when an indicator is added to flowing liquid in a closed circuit, the flow is related the
average change in concentration measured at a distal site. Specifically, the flow in the system is inversely proportional to the
area under the concentration-time curve, which is described by the Stewart-Hamilton equation (Figure 3).
In thermodilution, the indicator used is a bolus of cold fluid of known temperature and volume, while the concentration change
is a change in temperature from baseline. A 5- to 10-mL bolus of cold liquid (usually 5% dextrose at 58C; saline may also be used
depending on the density constant used to calculate CO) is injected into the RA, causing a drop in temperature of the blood enter-
ing the PA. The rate of blood flow is inversely proportional to the mean change in temperature (represented by the area of the
temperature time curve, the AUC). The Stewart-Hamilton equation also describes this relationship; however, it is modified to take
the temperature, specific heat, and specific gravity of the injectate and blood into account (Figure 4).
Both indicator-dilution and thermodilution methods produce a similar curve, with an initial sharp deflection followed by a slower
return to baseline as the blood dilutes and carries out the cold indicator. The CO is inversely proportional to the area under this
curve, thus the shape of these curves is altered with varying cardiac output (Figure 5).
Limitations
Thermodilution CO measurement accuracy can be adversely affected by several factors listed in Table 1.
INSERTION AND COMPLICATIONS4
1. Under strict asepsis and ultrasound guidance, the PA sheath is inserted into the internal jugular vein using the Seldinger
technique. Other central veins (femoral, subclavian) may also be used.
2. The distal port of the PAC is attached to a pressure transducer zeroed at the level of the patient’s heart.
3. The catheter is inserted into the sheath and advanced to approximately 15 cm, after which the tip will exit the sheath and the
balloon may be inflated using the volume-limited syringe.
4. The catheter may be advanced to enter the RA, followed by the right ventricle (RV), pulmonary artery and finally into the
wedge position (see Table 2 for typical depths and pressures). Mean RA pressure, RV/PA systolic, diastolic and mean pres-
sures and finally the end expiratory PCWP should be measured.
5. The balloon is deflated and a PA trace should be observed. If not, the catheter should be withdrawn until a PA trace
appears.
6. The catheter depth should be noted and then may be secured in the plastic sheath.
Following the insertion of PAC, a chest radiograph should be performed to identify catheter misplacement or pneumothorax.
The tip of the catheter should not be more than 1 cm lateral to the mediastinal margin, or beyond the pulmonary hilum on chest
x-ray, to avoid trauma to distal branches of the PA and vascular obstruction causing pulmonary infarction. Other complications
associated with PAC insertion include ventricular arrhythmias, PA or myocardial perforation, and pulmonary embolus.
Figure 3. The Stewart-Hamilton equation.
Figure 4. The modified Stewart-Hamilton equation.
Subscribe to ATOTW tutorials by visiting https://resources.wfsahq.org/anaesthesia-tutorial-of-the-week/
ATOTW 509 — The Pulmonary Artery Catheter (7 November 2023) Page 4 of 8
Figure 5. Typical concentration-time curves observed in normal, high, and low cardiac output states. The area under the curve is calculated from
the extrapolated curve (denoted by the dotted lines), as the observed curve demonstrates a negative exponential decline due to recirculation.
Overestimation of CO
Source of Inaccuracy Correction
Injectate Too small volume of injectate producing low Use standardised volume and temperature
amplitude and low AUC of injectate for each measurement
Intracardiac shunt Right-to-left shunt: cold injectate escapes to ...
left heart without being measured
Underestimation of CO
Source of Inaccuracy Correction
Injectate Excessive volume of injectate producing Use standardised volume and temperature
large amplitude change and large AUC of injectate for each measurement
Injectate too cold, causing reduction in CO
due to direct effect on myocardium or
arrhythmia
Concurrent infusions Rapid flowing of intravenous fluid causing Avoid concurrent rapid fluid administration through
reduction in blood temperature line while measurements are taking place
Catheter tip position West zone 1: alveolar pressure exceeds PA Catheter should be positioned in West zone 3
pressure resulting in low/no blood flow and
dead space
West zone 2: alveolar pressure exceeds
pulmonary vascular pressure, blood flow
varies with respiration
Tricuspid regurgitation Some cold injectate regurgitated back into ...
right atrium, resulting in slow flow past
thermistor and large AUC
Intracardiac shunt Left-to-right shunt: cold injectate recirculates ...
back to right heart producing second peak
and large AUC
Other Effects
Source of Inaccuracy
Respiratory cycle May cause both under- and overestimation of Take all measurements at end expiration
CO depending on stage of respiratory cycle
and whether the patient is mechanically or
spontaneously ventilating
Abnormal haematocrit Haematocrit determines specific heat and
specific gravity of blood, which is used in
Stewart-Hamilton equation to calculate CO
Table 1. Factors Affecting Accuracy of cardiac output (CO) Measurement Using Thermodilution Techniques With Pulmonary
Artery Catheters. AUC indicates area under the curve; PA, pulmonary artery
Subscribe to ATOTW tutorials by visiting https://resources.wfsahq.org/anaesthesia-tutorial-of-the-week/
ATOTW 509 — The Pulmonary Artery Catheter (7 November 2023) Page 5 of 8
Catheter Location Depth From Skin (cm) Pressures (mm Hg)
RA 15-20 cm 2-6
RV 30 cm 25/4
PA 40 cm 25/10
PCWP 50 cm 8-12
Table 2. Typical Chamber Depth and Pressures Encountered on Inserting a
Pulmonary Artery Catheter. PA indicates pulmonary artery; PCWP, pulmonary
capillary wedge pressure; RA, right atrium; RV, right ventricle
PAC insertion should be avoided in the context of endocarditis, right-sided heart masses (clot or tumour) or prosthesis at risk
of damage or dislodgement, high-grade right-sided valvular disease, and severe coagulopathy. Caution should be observed in
patients with LBBB in whom catheter passage may induce complete heart block. The risk of myocardial perforation is also
increased in patients who have a severely dilated or thinned RA or RV.
NORMAL VALUES AND INTERPRETATION
Normal measured and derived values which can be obtained from a PAC are found in Table 3. These values are deranged in
distinct patterns with cardiovascular pathology, common examples of which are found in Table 4.
INDICATIONS AND EVIDENCE FOR USE
PACs may be inserted at the bedside and can yield valuable measurements of stroke volume, CO, mixed venous oxygen satura-
tions, and intracardiac pressures, as well as providing data for several derived variables to guide diagnosis and management.
They have been utilised extensively in the intensive care setting with the wealth of haemodynamic information provided guiding
vasoactive, inotropic, and diuretic therapy. Unfortunately, evidence for a mortality benefit was not borne out in several large trials
and subsequent metanalyses (Table 5) and as such most societies’ guidelines have moved away from recommending the routine
use of PACs in critically ill patients.
Measured Values Derived Values
CO: 4-8 L/min SV: 50-100 mL
CI: 2.5-4 L/min SVI: 25-45 mL/m2
CVP: 2-6 mm Hg SVR: 900-1300 dynes-sec/cm5
PCWP: 8-12 mm Hg SVRI: 1900-2400 dynes-sec/cm5
PA pressure: 25/10 mm Hg PVR: 40-150 dynes-sec/cm5
SvO2: 65-70% PVRI: 120-200 dynes-sec/cm5
Temperature
Table 3. Measured and Derived Pulmonary Artery Catheter Values. CI indicates
cardiac index; CVP, central venous pressure; PVR, pulmonary vascular resistance;
PVRI, pulmonary vascular resistance index; SV, stroke volume; SVI, SV index;
SVR, systemic vascular resistance; SVRI, SVR index
Pathology CVP PCWP CI SVR PVR
Right heart failure High ... Low ... High
Left heart failure High High Low High ...
Pericardial tamponade High High Low High ...
Hypovolaemia Low Low Low High ...
Cardiogenic shock High High Low High ...
Distributive shock Low Low High Low ...
Table 4. Typical Haemodynamic Patterns Observed in Common Cardiovascular
Pathology. CI indicates cardiac index; CVP, central venous pressure; PCWP, pul-
monary capillary wedge pressure; PVR, pulmonary vascular resistance; SVR, sys-
temic vascular resistance
Subscribe to ATOTW tutorials by visiting https://resources.wfsahq.org/anaesthesia-tutorial-of-the-week/
ATOTW 509 — The Pulmonary Artery Catheter (7 November 2023) Page 6 of 8
Trial Study Description Findings
SUPPORT5 Multicentre prospective observational cohort Increased 30-day mortality in PAC group
study Increased resource utilisation in PAC group
Patient group: critically ill ICU patients (n ¼ 5753)
PAC-Man6 Multicentre randomised control trial comparing No difference in in-hospital mortality between
management with or without PAC in ICU groups
patients
Patient group: critically ill ICU patients
(n ¼ 1041)
FACCTS7 Multicentre randomised trial comparing PAC No difference in 60-day mortality between
versus central venous catheter to guide groups
treatment of acute lung injury No difference in length of stay or organ
Patient group: Patients admitted to ICU with dysfunction between groups
acute lung injury (n ¼ 1000) More catheter-related complications in the
PAC group
Canadian critical care Multicentre randomised control trial comparing No difference in in-hospital, 6-month or
trials group8 goal-directed therapy guided by a PAC with 12-month mortality or length of stay
standard care without the use of a PAC in between groups
high-risk surgical patients Increased risk of pulmonary embolus in PAC
Patient group: 1994 elderly, ASA3-4 patients group
undergoing elective or emergency surgery
requiring post-operative ICU admission
French PAC Study Multicentre randomised control trial comparing No difference in 14-, 28-, or 90-day mortality
Group9 management with or without a PAC in ICU No difference in organ supports or dysfunction
patients with shock, ARDS, or both between groups
Patient group: ICU patients with shock, ARDS Similar duration of mechanical ventilation and
or both (n ¼ 676) length of stay in ICU
Cochrane review(10) Meta-analysis of 13 studies (5686 patients) Use of a PAC did not alter the mortality,
2013 including general ICU and high-risk surgical general ICU or hospital length of stay,
patients or cost for adult patients in ICU
Table 5. Key Studies Involving the Use of Pulmonary Artery Catheters (PACs). ARDA indicates acute respiratory distress syn-
drome; ICU, intensive care unit
PAC insertion is still indicated in certain situations, and there have been calls in recent years to reconsider the evidence
against their use, which may be less conclusive than is apparent from headline results. Many of the studies investigating PAC
use in general intensive care unit (ICU) patients are subject to significant limitations. The SUPPORT study was one of the first
to signal a worrying lack of mortality benefit with PAC use; however, it was not designed for this purpose.5 This observational
study only included patients with an estimated 6-month mortality risk of > 50% from a heterogenous group of severe disease
categories, the outcomes of which would be highly unlikely to be modified by using a PAC. The PAC-Man study, one of the
largest randomised clinical trials involving ICU patients, showed no in-hospital mortality benefit; however, it is important to
note that it was designed to detect a 10% absolute change in this outcome.6 Very few ICU therapies, let alone a monitoring
device, are capable of changing mortality rates by 10%. A Cochrane review conducted in 2013 noted that many of the
included studies were highly heterogenous in their interventions, with a lack of standardisation of therapies based on PAC
information.10
PACs continue to be used regularly in cardiothoracic surgery where the evidence for benefit is mixed. Recent large observa-
tional studies suggest that routine PAC insertion in uncomplicated cardiac surgery may not confer a mortality benefit.11,12 The
literature suggests that the advantages of PAC monitoring are likely to be seen in more complex patients, such as those with
severe left ventricular failure, those undergoing cardiac transplant, multivalvular operations, and ventricular assist device inser-
tion, all of which have been variously excluded from historical PAC studies. Thus PACs do not appear to add benefit for ‘rou-
tine’ or low-risk cardiac surgery, but in appropriate patients with more complex pathology may yield invaluable information for
the clinician.
CONCLUSION
Despite the overall decline in their use, PACs and the variables which they measure underpin core physiological principles
central to the practice of intensive care and anaesthesia. In the appropriate clinical context, the PAC may provide essential
information to guide changes in management of vasoactive supports and fluid therapies.
Subscribe to ATOTW tutorials by visiting https://resources.wfsahq.org/anaesthesia-tutorial-of-the-week/
ATOTW 509 — The Pulmonary Artery Catheter (7 November 2023) Page 7 of 8
REFERENCES
1. Thakkar AB, Desai SP. Swan, Ganz, and their catheter: its evolution over the past half century. Ann Intern Med. 2018;
169(9):636-642.
2. Swan HJ, Ganz W, Forrester J, Marcus H, Diamond G, Chonette D. Catheterization of the heart in man with use of a flow-
directed balloon-tipped catheter. N Engl J Med. 1970;283(9):447-451.
3. Argueta EE, Paniagua D. Thermodilution cardiac output: a concept over 250 years in the making. Cardiol Rev. 2019;
27(3):138-144.
4. Kelly CR, Rabbani LE. Videos in clinical medicine. Pulmonary-artery catheterization. N Engl J Med. 2013;369(25):e35.
5. Connors AF, Speroff T, Dawson NV, et al. The effectiveness of right heart catheterization in the initial care of critically ill
patients. SUPPORT Investigators. JAMA. 1996;276(11):889-897.
6. Harvey S, Harrison DA, Singer M, et al. Assessment of the clinical effectiveness of pulmonary artery catheters in manage-
ment of patients in intensive care (PAC-Man): a randomised controlled trial. Lancet. 2005;366(9484):472-477.
7. Wheeler AP, Bernard GR, Thompson BT, et al. Pulmonary-artery versus central venous catheter to guide treatment of
acute lung injury. N Engl J Med. 2006;354(21):2213-2224.
8. Sandham JD, Hull RD, Brant RF, et al. A randomized, controlled trial of the use of pulmonary-artery catheters in high-risk
surgical patients. N Engl J Med. 2003;348(1):5-14.
9. Richard C, Warszawski J, Anguel N, et al. Early use of the pulmonary artery catheter and outcomes in patients with shock
and acute respiratory distress syndrome: a randomized controlled trial. JAMA. 2003;290(20):2713-2720.
10. Rajaram SS, Desai NK, Kalra A, et al. Pulmonary artery catheters for adult patients in intensive care. Cochrane Database
Syst Rev. 2013;2013(2):CD003408.
11. Shaw AD, Mythen MG, Shook D, et al. Pulmonary artery catheter use in adult patients undergoing cardiac surgery: a retro-
spective, cohort study. Perioper Med (Lond). 2018;7:24.
12. Brown JA, Aranda-Michel E, Kilic A, et al. The impact of pulmonary artery catheter use in cardiac surgery. J Thorac Cardiovasc
Surg. 2022;164(6):1965-1973.e6.
This work by WFSA is licensed under a Creative Commons Attribution-NonCommercial-NoDerivitives 4.0 International
License. To view this license, visit https://creativecommons.org/licenses/by-nc-nd/4.0/
WFSA Disclaimer
The material and content provided has been set out in good faith for information and educational purposes only and is not intended as a substi-
tute for the active involvement and judgement of appropriate professional medical and technical personnel. Neither we, the authors, nor other
parties involved in its production make any representations or give any warranties with respect to its accuracy, applicability, or completeness
nor is any responsibility accepted for any adverse effects arising as a result of your reading or viewing this material and content. Any and all lia-
bility directly or indirectly arising from the use of this material and content is disclaimed without reservation.
Subscribe to ATOTW tutorials by visiting https://resources.wfsahq.org/anaesthesia-tutorial-of-the-week/
ATOTW 509 — The Pulmonary Artery Catheter (7 November 2023) Page 8 of 8
You might also like
- ACCP ASHP Cardiology Pharmacy Preparatory Review (2022)Document793 pagesACCP ASHP Cardiology Pharmacy Preparatory Review (2022)Faris Firas100% (2)
- Assignment 1Document4 pagesAssignment 1mp1757100% (1)
- Nursing Care Plan: Mrs Rajbr Kaur Lecturer OBGDocument20 pagesNursing Care Plan: Mrs Rajbr Kaur Lecturer OBGKavi rajput92% (25)
- STL2C6 - Support The Health and Safety of Children and Young PeopleDocument3 pagesSTL2C6 - Support The Health and Safety of Children and Young PeopleMarcela Coid100% (1)
- Swan GanzDocument35 pagesSwan Ganzdrivaner1No ratings yet
- Cateteres Arteriaes, Central y Arteria PulmonarDocument13 pagesCateteres Arteriaes, Central y Arteria PulmonarmmsNo ratings yet
- PIIS1053077021002081Document3 pagesPIIS1053077021002081DON TVNo ratings yet
- CVP Evaluation Interpretation PDFDocument3 pagesCVP Evaluation Interpretation PDFMegan LewisNo ratings yet
- Cardiopulmonary Bypass: Learning ObjectivesDocument5 pagesCardiopulmonary Bypass: Learning ObjectivesAnonymous zPwXqwNo ratings yet
- Intra-Aortic Balloon Counterpulsation Therapy and Its Role in Optimizing Outcomes in Cardiac SurgeryDocument31 pagesIntra-Aortic Balloon Counterpulsation Therapy and Its Role in Optimizing Outcomes in Cardiac SurgeryHendrik AbrahamNo ratings yet
- PAM Metas Terapéuticas y Soporte FarmocológicoDocument9 pagesPAM Metas Terapéuticas y Soporte FarmocológicoHernando CastrillónNo ratings yet
- CCPACatheter Basics 07 MedicineDocument44 pagesCCPACatheter Basics 07 MedicinerinbijoyNo ratings yet
- Bootsma2021 Article TheContemporaryPulmonaryArteryDocument11 pagesBootsma2021 Article TheContemporaryPulmonaryArteryElenaCondratscribdNo ratings yet
- Swan Ganz Catheterization: Prepared By: Rashmita Byanju Shrestha Nursing Incharge Sicu and HduDocument24 pagesSwan Ganz Catheterization: Prepared By: Rashmita Byanju Shrestha Nursing Incharge Sicu and HduArchana Maharjan100% (1)
- 9 IABP and Plasmapheresis (4 Files Merged)Document48 pages9 IABP and Plasmapheresis (4 Files Merged)Alaa OmarNo ratings yet
- PIIS0733862720300729Document15 pagesPIIS0733862720300729Hames SeguraNo ratings yet
- Gilbert - Cardiac Output MeasurementDocument7 pagesGilbert - Cardiac Output MeasurementCaos_123100% (1)
- Hepatology - 2004 - Colle - Diagnosis of Portopulmonary Hypertension in Candidates For Liver Transplantation A ProspectiveDocument9 pagesHepatology - 2004 - Colle - Diagnosis of Portopulmonary Hypertension in Candidates For Liver Transplantation A ProspectiveYasin DeveliogluNo ratings yet
- Cap 5 - Monitorización CardiovascularDocument53 pagesCap 5 - Monitorización CardiovascularMonserrath ReséndizNo ratings yet
- Perioperativehemodynamic Monitoring: An Overview of Current MethodsDocument16 pagesPerioperativehemodynamic Monitoring: An Overview of Current MethodsjayjayshrigokuleshNo ratings yet
- Basics of ECMO Part 2Document6 pagesBasics of ECMO Part 2corinna.ongaigui.gsbmNo ratings yet
- NCMB 418 Hemodynamics Week 7Document34 pagesNCMB 418 Hemodynamics Week 7Jennifer Ambrosio100% (1)
- Jurnal HemodinamikDocument16 pagesJurnal HemodinamikFauziatul RiyadaNo ratings yet
- Hour Pathophysiologic Approach To The Golden: Review of A Major Pulmonary EmbolismDocument31 pagesHour Pathophysiologic Approach To The Golden: Review of A Major Pulmonary EmbolismSilvio SillitanoNo ratings yet
- Balon CP AJ Cardiol 2006Document8 pagesBalon CP AJ Cardiol 2006drcarlos.romero.umichNo ratings yet
- Swan Ganz CathetersDocument27 pagesSwan Ganz CatheterschadchimaNo ratings yet
- CVPDocument3 pagesCVPAudreySalvadorNo ratings yet
- Eacvi Recommendations Valvular Regurgitation SummaryDocument34 pagesEacvi Recommendations Valvular Regurgitation SummaryWilli SotoNo ratings yet
- Extracorporeal Membrane Oxygenation (ECMO) System.: Atrial Septal DefectDocument10 pagesExtracorporeal Membrane Oxygenation (ECMO) System.: Atrial Septal DefectDhina KaranNo ratings yet
- Critical Care in The Emergency Department: Monitoring The Critically Ill PatientDocument4 pagesCritical Care in The Emergency Department: Monitoring The Critically Ill PatientNurul Falah KalokoNo ratings yet
- Cap 2013 NejmDocument7 pagesCap 2013 NejmpaulaandreavargasbNo ratings yet
- Arterial LineDocument2 pagesArterial LineRaghav Goyal100% (1)
- Monitoreo Minimamente Invasive CCC 2015Document18 pagesMonitoreo Minimamente Invasive CCC 2015Ana Miryam Pérez ZavalaNo ratings yet
- Arterial and Venous Pressure Monitoring During Hemodialysis - Document - Gale Academic OneFileDocument10 pagesArterial and Venous Pressure Monitoring During Hemodialysis - Document - Gale Academic OneFileBryan FarrelNo ratings yet
- Analisis de Gases SanguineosDocument18 pagesAnalisis de Gases SanguineosDiana CarolinaNo ratings yet
- CVP MonitoringDocument24 pagesCVP MonitoringsofiamansoorNo ratings yet
- Potri Hafisah B. Macadaya Group 2 BSN 3Document26 pagesPotri Hafisah B. Macadaya Group 2 BSN 3Marivic Diano100% (2)
- Hepatopulmonary Syndrome - A Liver-Induced Lung Vascular DisorderDocument10 pagesHepatopulmonary Syndrome - A Liver-Induced Lung Vascular DisorderFlavio FLores CruzNo ratings yet
- Bia - EscDocument17 pagesBia - EscFábio MachadoNo ratings yet
- ECMO Sidebotham TW Et Al ECMODocument17 pagesECMO Sidebotham TW Et Al ECMONitesh GuptaNo ratings yet
- PulmCirc 005 407Document5 pagesPulmCirc 005 407Andreea KNo ratings yet
- ANMCO POSITION PAPER Role of Intra-Aortic BalloonDocument17 pagesANMCO POSITION PAPER Role of Intra-Aortic BalloonapipNo ratings yet
- Intra Aortic Balloon PumpDocument3 pagesIntra Aortic Balloon PumpNkk Aqnd MgdnglNo ratings yet
- De Nition: Chapter 16 Blood PressureDocument5 pagesDe Nition: Chapter 16 Blood PressureAdebayo WasiuNo ratings yet
- Pulmonary Artery Catheterization and MonitoringDocument31 pagesPulmonary Artery Catheterization and MonitoringVhince Norben PiscoNo ratings yet
- Arterial LinesDocument13 pagesArterial LinesYee LengNo ratings yet
- Hemodynamic MonitoringDocument39 pagesHemodynamic MonitoringNor Jeannah PolaoNo ratings yet
- Measuring Central Venous Pressure: Elaine ColeDocument8 pagesMeasuring Central Venous Pressure: Elaine ColednllkzaNo ratings yet
- ITU Handbook For Non-Anaesthetists 214Document23 pagesITU Handbook For Non-Anaesthetists 214AtikaNo ratings yet
- Piis0007091217459812 PDFDocument10 pagesPiis0007091217459812 PDFAnonymous 1uP0mbNo ratings yet
- Swan Ganz FinalDocument36 pagesSwan Ganz FinalDanial HassanNo ratings yet
- I1524-5012-16-3-243 IMPELLADocument7 pagesI1524-5012-16-3-243 IMPELLAzairakuri32No ratings yet
- Open Heart 1Document18 pagesOpen Heart 1mohamedNo ratings yet
- Collective Review: Cardiac OutputDocument27 pagesCollective Review: Cardiac Outputrandomized1234No ratings yet
- Physiologic Monitoring of A Surgical PatientDocument41 pagesPhysiologic Monitoring of A Surgical PatientAlna Shelah IbañezNo ratings yet
- Invasivo PDFDocument21 pagesInvasivo PDFVasFel GicoNo ratings yet
- Arterial LinesDocument13 pagesArterial LinesberhanubedassaNo ratings yet
- IPM NotesDocument4 pagesIPM NotesPreethi ShekarNo ratings yet
- Resumen Article IcDocument14 pagesResumen Article Icapi-689165620No ratings yet
- Assessing Volume StatusDocument12 pagesAssessing Volume StatusMoises Torres AlvarezNo ratings yet
- Influence of Cardiomegaly On Disordered Breathing During Exercise in Chronic Heart FailureDocument8 pagesInfluence of Cardiomegaly On Disordered Breathing During Exercise in Chronic Heart FailurenadiaNo ratings yet
- Blalock Taussig Shunt PDFDocument4 pagesBlalock Taussig Shunt PDFzuraini_mdnoorNo ratings yet
- Invasive Hemodynamic Monitoring in The Cardiac Intensive Care UnitDocument12 pagesInvasive Hemodynamic Monitoring in The Cardiac Intensive Care Unitqe202300No ratings yet
- Perfusion for Congenital Heart Surgery: Notes on Cardiopulmonary Bypass for a Complex Patient PopulationFrom EverandPerfusion for Congenital Heart Surgery: Notes on Cardiopulmonary Bypass for a Complex Patient PopulationRating: 5 out of 5 stars5/5 (2)
- DopamineDocument11 pagesDopaminecaioaccorsiNo ratings yet
- AddictionDocument12 pagesAddictioncaioaccorsiNo ratings yet
- Laparoscopic SurgeryDocument4 pagesLaparoscopic SurgerycaioaccorsiNo ratings yet
- UIA 37 Paed Neuraxial AnaesDocument7 pagesUIA 37 Paed Neuraxial AnaescaioaccorsiNo ratings yet
- Atow 505 00 01Document8 pagesAtow 505 00 01caioaccorsiNo ratings yet
- ICU OnePager Perc TracheostomyDocument1 pageICU OnePager Perc TracheostomycaioaccorsiNo ratings yet
- Anestesia Transplat FigadoDocument7 pagesAnestesia Transplat FigadocaioaccorsiNo ratings yet
- Advanced Thermal Management of Diesel Engines: Knowledge LibraryDocument8 pagesAdvanced Thermal Management of Diesel Engines: Knowledge LibrarycaioaccorsiNo ratings yet
- AaaaaaaaaaaaaaaaaaaedfgDocument6 pagesAaaaaaaaaaaaaaaaaaaedfgcaioaccorsiNo ratings yet
- Literature Review On Herbal Medicine PDFDocument7 pagesLiterature Review On Herbal Medicine PDFfihum1hadej2100% (1)
- Daisy Ursino's Portfolio: Bruce RiddellDocument95 pagesDaisy Ursino's Portfolio: Bruce Riddellapi-404780243No ratings yet
- Science Investigatory Project: Universidad de ManilaDocument7 pagesScience Investigatory Project: Universidad de ManilaCassandra AgustinNo ratings yet
- Mycotoxins in Feed Ingredients PDFDocument8 pagesMycotoxins in Feed Ingredients PDFUmar ChaudharyNo ratings yet
- Passive Smoking: Oral and Dental Effects: Letter To The EditorDocument2 pagesPassive Smoking: Oral and Dental Effects: Letter To The EditordebsanNo ratings yet
- Aquate Shrimp Helps Provide Economic Benefit To Shrimp Farmers in HondurasDocument4 pagesAquate Shrimp Helps Provide Economic Benefit To Shrimp Farmers in HondurasInternational Aquafeed magazineNo ratings yet
- Unit 2 1-2 3Document5 pagesUnit 2 1-2 3api-282526559No ratings yet
- Cefalea LancetDocument2 pagesCefalea LancetJohana Zamudio RojasNo ratings yet
- Cough, Cold, and Allergy: AntitussivesDocument8 pagesCough, Cold, and Allergy: AntitussivesSalsabila RaniahNo ratings yet
- 1 s2.0 S0264410X13001369 MainDocument8 pages1 s2.0 S0264410X13001369 MainTuấn HuỳnhNo ratings yet
- Medical TerminologyDocument27 pagesMedical TerminologyXuan CarpentierNo ratings yet
- Infectious Diseases IIDocument57 pagesInfectious Diseases IIAhmad MakhloufNo ratings yet
- ISYS90069 - Week 3 Tutorial - Group 22Document4 pagesISYS90069 - Week 3 Tutorial - Group 22Kaylene SivNo ratings yet
- Neopedia-Day-1 (Milestones)Document17 pagesNeopedia-Day-1 (Milestones)Quevee CondezNo ratings yet
- Kalium KloratDocument6 pagesKalium KloratAnnisa Nur JNo ratings yet
- Protein Drug BindingDocument26 pagesProtein Drug BindingBandita DattaNo ratings yet
- Module 1 Gen EdDocument14 pagesModule 1 Gen EdPhilip Floro0% (1)
- Gecc 125 - Biodiversity and Healthy SocietyDocument24 pagesGecc 125 - Biodiversity and Healthy SocietyMARIA JEZZA LEDESMANo ratings yet
- Toxic Responses of The BloodDocument10 pagesToxic Responses of The BloodM. Joyce100% (2)
- Phytochemical Investigations of Tapinanthus Globiferus (Loranthaceae) From Two Hosts and The Taxonomic ImplicationsDocument4 pagesPhytochemical Investigations of Tapinanthus Globiferus (Loranthaceae) From Two Hosts and The Taxonomic ImplicationsAbraham YirguNo ratings yet
- 011ho10079 - Altatoyota Usa ProofDocument1 page011ho10079 - Altatoyota Usa ProofjoynahidNo ratings yet
- Bb3 WHO Classification of Tumors of Haemopoietic and Lymphoid Tissues 4th 2008 PGDocument422 pagesBb3 WHO Classification of Tumors of Haemopoietic and Lymphoid Tissues 4th 2008 PGLoredana Milea Ex Lefter100% (1)
- Pain Management Us PharmacistDocument78 pagesPain Management Us PharmacistMarfu'ah Mar'ah100% (1)
- Material Mini NetterDocument11 pagesMaterial Mini NetterVALENTINA ALBORNOZ BASTÍASNo ratings yet
- Acute and Chronic Whiplash Disorders - A Review: Ylva Sterner and Bjo RN GerdleDocument18 pagesAcute and Chronic Whiplash Disorders - A Review: Ylva Sterner and Bjo RN GerdleJeremi SetiawanNo ratings yet
- Astro-Diagnosis, A Guide To Healing, Chapters XXX - XXXIIIDocument14 pagesAstro-Diagnosis, A Guide To Healing, Chapters XXX - XXXIIIOmSilence2651100% (1)