Professional Documents
Culture Documents
jcdr-8-MD06_240610_185657
jcdr-8-MD06_240610_185657
Uploaded by
Gisela PieniakCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
jcdr-8-MD06_240610_185657
jcdr-8-MD06_240610_185657
Uploaded by
Gisela PieniakCopyright:
Available Formats
DOI: 10.7860/JCDR/2014/8991.
4711
Case Report
Visual loss in Takayasu Arteritis –
Internal Medicine
Section
Look Beyond the Eye
Jayanthi Peter1, George Joseph2, Vivek Mathew3, John Victor Peter4
ABSTRACT
Patients with Takayasu arteritis often present with reduced vision related either to the disease per se or due to complications of therapy.
We report a patient with Takayasu arteritis who developed acute onset bilateral visual loss 6wks following percutaneous revascularization of
occluded aortic arch branches. No ocular cause for the visual loss was evident. The reason for visual loss in this patient was an extraocular
cause. Ocular and extraocular causes of visual loss in Takayasu arteritis are discussed.
Keywords: Ischemia, Takayasu arteritis, Visual loss
Case report A single hemorrhage was seen in the left eye retinal periphery. The
A 32-year-old woman with history of inflammatory arthritis, absence of significant ocular findings despite severe visual loss and
presented with transient right focal seizures followed by blurred the presence of sensory symptoms suggested a lesion along the
vision that resolved completely, two months prior to presentation visual pathway.
to our hospital. A further short, self-limiting episode occurred two Magnetic resonance imaging (MRI) of the brain showed a large sub-
weeks later. On examination both upper limb blood pressures acute occipital bleed on the right side and a chronic occipital infarct
were not recordable. Systemic examination was otherwise normal. on the left side [Table/Fig-2a,b] without mass effect or features of
Erythrocyte sedimentation rate was 45mm at one hour, C-reactive raised intracranial pressure. She was reviewed by the neurosurgeons
protein was 10.4mg/L and anti-nuclear antibody was negative. who advised to stop anti-platelet drugs and start phenytoin. On
Magnetic resonance angiogram revealed bilateral subclavian and review 15d later, vision had improved to 4/60 in both eyes. She was
common carotid artery stenosis, consistent with a diagnosis of subsequently lost to follow up.
Type I Takayasu arteritis. She underwent percutaneous transluminal
angioplasty with stenting of the right subclavian and right common Discussion
carotid arteries. She was advised mycophenolate, tapering doses The initial presentation with right focal seizures and transient ocular
of prednisolone, aspirin, clopidogrel, fenfibrate and atorvastatin and symptoms suggested left cerebral and posterior circulation ischemia
sent for eye examination. respectively as the likely cause for the symptoms. The MRI finding
Best corrected visual acuity was 6/6 in both eyes. The anterior of a chronic infarct of the left occipital cortex may explain the visual
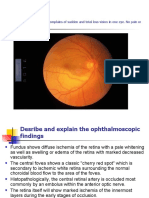
segment was normal. Dilated fundus examination revealed few symptoms. The subsequent presentation of acute onset blindness
retinal hemorrhages not involving the fovea [Table/Fig-1]. No specific of both eyes may be attributed to the new hemorrhage in the right
ophthalmic intervention was advised. occipital cortex on the background of pre-existing chronic infarct in
the left occipital cortex. The ischemic event is likely due to occlusion
She returned two months later with sudden onset visual loss in both
of the aortic arch branches while the hemorrhage may have been
eyes associated with multiple episodes of vomiting and reduced
due to antiplatelet therapy or cerebral aneurysms. Angioplasty
sensation in the right side of the body that occurred two weeks
related artery to artery embolization and re-perfusion injury due to
earlier. Visual acuity was perception of light in the right eye and hand
cerebral hyperperfusion was considered as alternative aetiological
movements in the left eye. Anterior segment was within normal
possibilities. However, these were less likely in view of the long
limits. Pupils were normal and reacting with no relative afferent
lag-period (6wks) between procedure (angioplasty) and symptom
pupillary defect. Fundus examination was normal in the right eye.
onset.
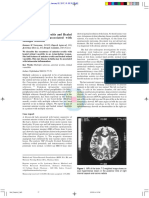
[Table/Fig-2]: Magnetic resonance imaging (MRI) of the brain: [A] T2 weighted
axial images of brain showing subacute hemorrhage in the right occipital lobe,
[Table/Fig-1]: Fundus photograph with the arrow pointing to a small hemorrhage and a chronic infarct in the left calcarine cortex; [B] T1 weighted images showing
in the right eye hyperintensity suggestive of subacute hemorrhage
6 Journal of Clinical and Diagnostic Research. 2014 Aug, Vol-8(8): MD06-MD07
www.jcdr.net Jayanthi Peter et al., Blindness in Takayasu Arteritis
Ocular causes Vascular events (ischemia or hemorrhage) involving the occipital
Anterior Segment Posterior segment of the eye
cortex, as in this patient, are extra-ocular causes for acute visual
of the eye loss.
Neovascular Amaurosis fugax (1) Chronic visual loss in Takayasu arteritis may be due to Takayasu
Disease related glaucoma (6) Central or branch retinal artery
Uveitis (7) occlusion (2, 3)
or hypertensive retinopathy [1,5], ocular ischemic syndrome [1],
Cataract Central or branch retinal vein neovascular glaucoma [6], uveitis [7], cataract [1] and sclerokeratitis
Sclerokeratitis (8) occlusion (4) [8]. Treatment for Takayasu arteritis with disease modifying agents
Anterior ischaemic optic neuropathy
(5) may also result in reduced vision due to complications such as
Vitreous haemorrhage steroid induced cataract, glaucoma and central serous retinopathy
Ocular ischaemia (1)
Macular oedema (1) [1].
Exudative retinal detachment (5)
Conclusion
Treatment related Steroid induced Glaucomatous optic neuropathy (1) Visual loss is the most common ocular symptom in Takayasu
Cataract (1) Steroid induced central serous
Steroid induced retinopathy arteritis. Since a variety of causes may result in reduced vision
Glaucoma (1) in Takayasu arteritis, a proper history and search for a cause is
Extra-ocular causes warranted. In some situations, such as highlighted in this case
Anterior circulation Posterior circulation who had sensory symptoms along with visual loss at the time of
Disease related Anterior circulation Posterior circulation stroke† presentation, the cause for visual loss was not in the eye per se. A
stroke* careful history is thus important to ascertain the cause of visual loss
Treatment related Reperfusion injury in Takayasu arteritis patients to reduce unnecessary investigations
[Table/Fig-3]: Causes of visual loss in takayasu arteritis and referrals.
* Anterior circulation stroke may occur due to infarction as a result of occlusion of
the aortic arch vessels or as a result of haemorrhage - visual loss as a result of
involvement of the optic tract along its pathway; †Visual loss in posterior circulation
References
[1] Peter J, David S, Danda D, Peter JV, Horo S, Joseph G. Ocular manifestations of
stroke is due a lesion in the occipital lobe as a result of infarction or haemorrhage
Takayasu arteritis: a cross-sectional study. Retina. 2011;31:1170-78.
[2] Peter J, David S, Joseph G, Horo S, Danda D, Peter JV. Rare retinal manifestations
in Takayasu arteritis. J Rheumatol. 2013; 40:1404-05.
Reduced vision is common in Takayasu arteritis [1] and may be [3] Noel N, Butel N, Le Hoang P, et al. Small vessel involvement in Takayasu’s
arteritis. Autoimmun Rev. 2013;12:355-62.
acute or chronic, transient or permanent, partial or complete or [4] Conrath J, Hadhadj E, Serratrice J, Ridings B. Branch retinal vein occlusion
related to the disease per se or due to treatment [Table/Fig-3]. Acute reveals Takayasu’s arteritis. J Fr Ophthalmol. 2004;27:162-65.
unilateral transient complete loss of vision,termed amaurosis fugax, [5] Peter J, David S, Joseph G, Horo S, Danda D. Hypoperfusive and hypertensive
ocular manifestations in Takayasu arteritis. Clin Ophthalmol. 2010;4:1173.
is due to emboli to the retinal artery. Acute onset of visual symptoms [6] Zhou B, Ye P, Wei S. Preliminary clinical analysis of neovascular glaucoma
with permanent visual loss may occur with embolic occlusion of the secondary to carotid artery disease. Clin Exp Optom. 2011;94:207-11.
central or branch retinal artery [2,3], venous occlusion [4], anterior [7] Kausman JY, Walker A, Piper S. Acute panuveitis and Takayasu’s arteritis. Arch
Dis Child. 2003;88:938-39.
ischemic optic neuropathy [5] and vitreous hemorrhage due to [8] Arya SK, Nahar R, Narang S, Jain R, Kalra N, Sood S. Sclerokeratitis in Takayasu’s
bleeding from new vessels in proliferative Takayasu retinopathy. arteritis: a case report. Jpn J Ophthalmol. 2005; 49:548-50.
PARTICULARS OF CONTRIBUTORS:
1. Assistant Professor, Department of Ophthalmology, Christian Medical College, Vellore, India.
2. Professor and Head, Department of Cardiology Unit I, Christian Medical College, Vellore, India.
3. Professor, Department of Neurology, Christian Medical College, Vellore, India.
4. Associate Professor, Department of Medicine, Christian Medical College, Vellore, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR:
Dr. Jayanthi Peter,
Schell Eye Hospital, Christian Medical College,Vellore 632004, India. Date of Submission: Feb 23, 2014
Phone : +91 9994067762, E-mail : peterjohnvictor@yahoo.com.au Date of Peer Review: Jul 01, 2014
Date of Acceptance: Jul 09, 2014
Financial OR OTHER COMPETING INTERESTS: None. Date of Publishing: Aug 20, 2014
Journal of Clinical and Diagnostic Research. 2014 Aug, Vol-8(8): MD06-MD07 7
You might also like
- UWorld Notes NeurologyDocument6 pagesUWorld Notes NeurologysarahNo ratings yet
- Canon Oct HS100Document26 pagesCanon Oct HS100emoboysliveNo ratings yet
- Ophthalmology For The Primary Care PhysicianDocument393 pagesOphthalmology For The Primary Care PhysicianCatana TudorNo ratings yet
- Vitreous MicrosurgeryDocument271 pagesVitreous Microsurgerybajo0550% (2)
- Gunes-2014-Vision Loss and RNFL Thinning AfterDocument2 pagesGunes-2014-Vision Loss and RNFL Thinning Afterdr_jrcNo ratings yet
- A Case of Neovascular Glaucoma Secondary To Ocular IschemiaDocument5 pagesA Case of Neovascular Glaucoma Secondary To Ocular IschemiaAvila RaeNo ratings yet
- Anterior Ischemic Optic Neuropathy and Central.20Document3 pagesAnterior Ischemic Optic Neuropathy and Central.20Prasad HewawasamNo ratings yet
- Perebaikan DG Mandala - Terapi Cermin Kasus BRAO New 20 OktoberDocument9 pagesPerebaikan DG Mandala - Terapi Cermin Kasus BRAO New 20 OktoberAriandindi AriandiNo ratings yet
- Arterial & Venous DisordersDocument33 pagesArterial & Venous Disorderseiuj497No ratings yet
- Case 1: 70-Yr Man Complains of Sudden and Total Loss Vision in One Eye. No Pain or Other SymptomsDocument17 pagesCase 1: 70-Yr Man Complains of Sudden and Total Loss Vision in One Eye. No Pain or Other SymptomsCherry TamNo ratings yet
- (10920684 - Neurosurgical Focus) Mechanisms of Visual Loss in PapilledemaDocument8 pages(10920684 - Neurosurgical Focus) Mechanisms of Visual Loss in PapilledemaYusuf BrilliantNo ratings yet
- fneur-13-988825Document8 pagesfneur-13-988825adinda.larastitiNo ratings yet
- Macular Edema As Unusual Presentation of Non-Arteritic Ischemic Optic Neuropathy (Naion)Document9 pagesMacular Edema As Unusual Presentation of Non-Arteritic Ischemic Optic Neuropathy (Naion)IJAR JOURNALNo ratings yet
- Mandala - Terapi Cermin Kasus BRAO (DG)Document9 pagesMandala - Terapi Cermin Kasus BRAO (DG)Ariandindi AriandiNo ratings yet
- The Hyperacute Vestibular Syndrome Ear or BrainDocument2 pagesThe Hyperacute Vestibular Syndrome Ear or BrainDea CantikNo ratings yet
- 9t4YwxZMqkZRd3DCCjVvJ7m 4Document4 pages9t4YwxZMqkZRd3DCCjVvJ7m 4رغد القرنيNo ratings yet
- Main PDFDocument3 pagesMain PDFanton MDNo ratings yet
- CorrespondenceDocument2 pagesCorrespondenceRiyanda FurqanNo ratings yet
- American Journal of Ophthalmology Case ReportsDocument3 pagesAmerican Journal of Ophthalmology Case ReportsElison Jaya PanggaloNo ratings yet
- Limb-Shaking Transient Ischemic Attack Associated With Focal Electroencephalography Slowing: Case ReportDocument3 pagesLimb-Shaking Transient Ischemic Attack Associated With Focal Electroencephalography Slowing: Case Reportkun avriadyNo ratings yet
- Reporting A Case of Spontaneous Ocular Hypotony After The Neurosurgical ProcedureDocument3 pagesReporting A Case of Spontaneous Ocular Hypotony After The Neurosurgical Procedurebijnn journalNo ratings yet
- 0410RT Feature BennettDocument4 pages0410RT Feature BennettRaissaNo ratings yet
- OpticIschemia BiousseDocument9 pagesOpticIschemia BiousseyetyningsyNo ratings yet
- Austin Biomarkers & DiagnosisDocument3 pagesAustin Biomarkers & DiagnosisAustin Publishing GroupNo ratings yet
- Nefropatías ÓpticasDocument9 pagesNefropatías Ópticasgabyc164No ratings yet
- Layout+39-45 Successfully+Procedure+Endovascular+C 240204 101818Document6 pagesLayout+39-45 Successfully+Procedure+Endovascular+C 240204 101818niaasyahabNo ratings yet
- NCP Rheum 0268Document9 pagesNCP Rheum 0268drheriNo ratings yet
- Multiple Sclerosis With Ophthalmologic Onset - Case ReportDocument5 pagesMultiple Sclerosis With Ophthalmologic Onset - Case ReportVannyNo ratings yet
- fimmu-12-791278 (2)_240610_185401Document16 pagesfimmu-12-791278 (2)_240610_185401Gisela PieniakNo ratings yet
- 852-Article Text-1602-1-10-20190613Document12 pages852-Article Text-1602-1-10-20190613anidar1245No ratings yet
- Peeping Painless ProptosisDocument3 pagesPeeping Painless ProptosisPutri YingNo ratings yet
- Foster Kennedy Syndrome: A Case ReportDocument3 pagesFoster Kennedy Syndrome: A Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Visual Anosognosia (Anton-Babinski Syndrome) : Report of Two Cases Associated With Ischemic Cerebrovascular DiseaseDocument5 pagesVisual Anosognosia (Anton-Babinski Syndrome) : Report of Two Cases Associated With Ischemic Cerebrovascular DiseaseHanna EnitaNo ratings yet
- Ischemic Optic Neuropathy: CE@HomeDocument7 pagesIschemic Optic Neuropathy: CE@HomeSiti Rokoyah Rezkylia SaktiNo ratings yet
- A Patient With Recent Visual DisturbancesDocument30 pagesA Patient With Recent Visual DisturbancesHeminNo ratings yet
- Anterior Ischemic Optic NeuropathyDocument4 pagesAnterior Ischemic Optic NeuropathyGading AuroraNo ratings yet
- Pathology of Ischemic Optic Neuropathy: Resident Short ReviewDocument5 pagesPathology of Ischemic Optic Neuropathy: Resident Short ReviewyetyningsyNo ratings yet
- Typical Optic Neuritis RevDocument6 pagesTypical Optic Neuritis RevAdhi AmertajayaNo ratings yet
- Foster Kennedy Synd 2Document3 pagesFoster Kennedy Synd 2Anonymous k4F8sAs25No ratings yet
- Oclusion LlaDocument5 pagesOclusion LlaGabriela Heredia AyardeNo ratings yet
- 個案報告:游離齒突小骨導致後循環復發性中風Document6 pages個案報告:游離齒突小骨導致後循環復發性中風王湘淇No ratings yet
- Visual Field Defects in Vascular Lesions The Lateral GeniculateDocument4 pagesVisual Field Defects in Vascular Lesions The Lateral GeniculateMarion FernandaNo ratings yet
- IndianJOphthalmol51177-524492 143409Document3 pagesIndianJOphthalmol51177-524492 143409novywardanaNo ratings yet
- Detection of Pre-Clinical Involvement of The Second Eye in Viral Acute Retinal Necrosis Using Optical Coherence TomographyDocument4 pagesDetection of Pre-Clinical Involvement of The Second Eye in Viral Acute Retinal Necrosis Using Optical Coherence TomographyEdgar Azael GarciaNo ratings yet
- Medicine: Sumatriptan-Induced Angle-Closure GlaucomaDocument4 pagesMedicine: Sumatriptan-Induced Angle-Closure GlaucomanidaNo ratings yet
- Anterior Ischemic Optic NeuropathyDocument9 pagesAnterior Ischemic Optic NeuropathyRifqi FathendraNo ratings yet
- American Journal of Emergency Medicine: Dietrich Jehle Mary Claire Lark, Clay O'BrienDocument3 pagesAmerican Journal of Emergency Medicine: Dietrich Jehle Mary Claire Lark, Clay O'BrienGufront MustofaNo ratings yet
- A Rare Case of Terson Syndrome With Subarachnoid HemorrhageDocument12 pagesA Rare Case of Terson Syndrome With Subarachnoid HemorrhageNinaNo ratings yet
- Biousse 2017Document7 pagesBiousse 2017elmon patadunganNo ratings yet
- 1 s2.0 S2049080121010128 MainDocument5 pages1 s2.0 S2049080121010128 MainNabita AuliaNo ratings yet
- Bagheri 2015Document15 pagesBagheri 2015Juliana Valentina CedeñoNo ratings yet
- Approaching Acute Vertigo With Diplopia - A Rare Skew Deviation in Vestibular NeuritisDocument7 pagesApproaching Acute Vertigo With Diplopia - A Rare Skew Deviation in Vestibular NeuritisRudolfGerNo ratings yet
- Visual Loss As A Complication of Non-Ophthalmologic Surgery: A Review of The LiteratureDocument8 pagesVisual Loss As A Complication of Non-Ophthalmologic Surgery: A Review of The LiteratureIda MaryaniNo ratings yet
- Traumatic Optic Neuropathy and Central Retinal Artery Occlusion Following Blunt Trauma To The EyebrowDocument2 pagesTraumatic Optic Neuropathy and Central Retinal Artery Occlusion Following Blunt Trauma To The EyebrowMiftahurrahmah GmsNo ratings yet
- Observations On Time Course Changes of The CherryDocument16 pagesObservations On Time Course Changes of The CherryAndi Tiara S. AdamNo ratings yet
- Bilateral Radiation Retinopathy 17 Years Following.62Document3 pagesBilateral Radiation Retinopathy 17 Years Following.62ShivcharanLalChandravanshiNo ratings yet
- Clinical CasesDocument49 pagesClinical Casesnorfitri hadeyNo ratings yet
- Complete Occlusion of Extracranial Internal Carotid Artery: Clinical Features, Pathophysiology, Diagnosis and ManagementDocument5 pagesComplete Occlusion of Extracranial Internal Carotid Artery: Clinical Features, Pathophysiology, Diagnosis and ManagementAndreea Raluca CimpoiNo ratings yet
- Posterior Reversible Encephalopathy Syndrome After Lumbar PunctureDocument2 pagesPosterior Reversible Encephalopathy Syndrome After Lumbar PunctureMedtext PublicationsNo ratings yet
- Central Retinal Vein Occlusion Revealing Anti Phospholipid Antibody Syndrome Case ReportDocument4 pagesCentral Retinal Vein Occlusion Revealing Anti Phospholipid Antibody Syndrome Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Case Report: Contrast-Induced Encephalopathy Following Cerebral Angiography in A Hemodialysis PatientDocument4 pagesCase Report: Contrast-Induced Encephalopathy Following Cerebral Angiography in A Hemodialysis PatientAnaNo ratings yet
- 713full 221024 135448Document8 pages713full 221024 135448Olga Manco GuzmánNo ratings yet
- Microcirculation: From Bench to BedsideFrom EverandMicrocirculation: From Bench to BedsideMaria DorobantuNo ratings yet
- CBLM CaregiverDocument162 pagesCBLM Caregiverrichardjuanito.estarisNo ratings yet
- AntidoteDocument51 pagesAntidoteAravind Rajeev50% (2)
- Jurnal MataDocument11 pagesJurnal MataNovi RatnaNo ratings yet
- GlaucomaDocument23 pagesGlaucomasanjivdas100% (2)
- Glaucoma OverviewDocument4 pagesGlaucoma OverviewSurya Cahyadi JunusNo ratings yet
- GlaucomaDocument18 pagesGlaucomaOncología CdsNo ratings yet
- Lattice Corneal DystrophyDocument7 pagesLattice Corneal DystrophyPhilip McNelsonNo ratings yet
- MicroPulse - P3 Rev 2 - Cyan MedicaDocument6 pagesMicroPulse - P3 Rev 2 - Cyan MedicaMischell Lázaro OrdonioNo ratings yet
- Iridex Endo ProbesDocument8 pagesIridex Endo ProbeslatentheatNo ratings yet
- NCS GlaucomaDocument47 pagesNCS GlaucomaDan Floyd FernandezNo ratings yet
- 1 2 2018 Lens Induced Glaucoma Bhuvan PDFDocument50 pages1 2 2018 Lens Induced Glaucoma Bhuvan PDFDara AprillyantiNo ratings yet
- Ijmrhs Vol 2 Issue 4Document321 pagesIjmrhs Vol 2 Issue 4editorijmrhsNo ratings yet
- Optometry Guidelines For Use of Scheduled MedicinesDocument11 pagesOptometry Guidelines For Use of Scheduled MedicinesJLoNo ratings yet
- Yag PiDocument2 pagesYag PiSamatha BiotechNo ratings yet
- Central Corneal Thickness: Ultrasound Pachymetry Verus Anterior Segment Optical Coherence TomographyDocument5 pagesCentral Corneal Thickness: Ultrasound Pachymetry Verus Anterior Segment Optical Coherence TomographybasharatNo ratings yet
- COMPLICATIONS of CATARACT SURGERY (Capsular Opacification and Contraction and Hemorrhage)Document30 pagesCOMPLICATIONS of CATARACT SURGERY (Capsular Opacification and Contraction and Hemorrhage)Hikban Fiqhi100% (1)
- Prevalence of Glaucoma in India: A Review: Ronnie George, Lingam VijayaDocument5 pagesPrevalence of Glaucoma in India: A Review: Ronnie George, Lingam VijayaprinceamitNo ratings yet
- 2009-Use of Novel Devices For Control of Intraocular PressureDocument7 pages2009-Use of Novel Devices For Control of Intraocular PressureReza NaghibiNo ratings yet
- GlaucomaDocument25 pagesGlaucomaChris Paguio100% (3)
- Jarvis Physical Assessment Chapter 14Document19 pagesJarvis Physical Assessment Chapter 14Giorgia Adams100% (2)
- Concept MapDocument4 pagesConcept MapCasison Mark ArrysonNo ratings yet
- Glaucoma Surgery - Open Angle GlaucomaDocument155 pagesGlaucoma Surgery - Open Angle GlaucomaWilsonNo ratings yet
- SOLIX Essential BrochureDocument12 pagesSOLIX Essential BrochureHaag-Streit UK (HS-UK)No ratings yet
- Anterior Chamber Angle Assessment Technique - CH 17Document20 pagesAnterior Chamber Angle Assessment Technique - CH 17riveliNo ratings yet
- Prevalence and Geographical Variations: Section 1 Glaucoma in The WorldDocument10 pagesPrevalence and Geographical Variations: Section 1 Glaucoma in The WorldGuessNo ratings yet
- Special SensesDocument5 pagesSpecial SensesggukNo ratings yet
- Oet Reading Part A Additional - GlucomaDocument8 pagesOet Reading Part A Additional - Glucomaafacean22% (9)