Professional Documents
Culture Documents
Acute Coronary Syndrome (ACS) - At
Acute Coronary Syndrome (ACS) - At
Uploaded by
Ayush TamangCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Acute Coronary Syndrome (ACS) - At
Acute Coronary Syndrome (ACS) - At
Uploaded by
Ayush TamangCopyright:
Available Formats
Acute Coronary Syndrome
(ACS)
Study
Tags Cardiovascular
Ayush Tamang, NAIHSCOM; Last updated: 8/24/2020
Table of Contents
Introduction
Etiology
Pathophysiology
Clinical Features
Diagnostics
Management
Prevention
Prognosis
References
Introduction
Acute coronary syndrome ACS refers to acute myocardial ischemia
and/or infarction due to partial or complete occlusion of a coronary artery
Myocardial Infarction MI: myocardial cell death (necrosis) caused by
prolonged ischemia
Overview
3 clinical entities grouped under ACS unstable angina pectoris (UA),
non-ST-segment elevation myocardial infarction (NSTEMI), and ST
segment elevation myocardial infarction (STEMI)
Acute Coronary Syndrome ACS 1
There are 32.4 million myocardial infarctions and strokes
worldwide every year. WHO
Incidence: ∼ 1.5 million cases of myocardial infarction per year in
the US; ♂ > ♀ 31
Etiology
Risk Factors: (refer Coronary Heart Disease CHD)
Increasing age; Male gender; Personal history of angina and/or known
coronary artery disease
Family history of CAD; Diabetes mellitus; Systolic hypertension;
Tobacco use; Hyperlipidemia
Etiology
Most common cause: coronary artery atherosclerosis
Less common:
Coronary artery dissection
Coronary artery vasospasm (e.g., Prinzmetal angina, cocaine use)
Takotsubo cardiomyopathy
Myocarditis
Thrombophilia (e.g., polycythemia vera)
Coronary artery embolism (e.g., due to prosthetic heart valve, atrial
fibrillation)
Vasculitis (e.g., polyarteritis nodosa, Kawasaki syndrome)
Myocardial oxygen supply-demand mismatch
Hypotension
Acute Coronary Syndrome ACS 2
Severe anemia
Hypertrophic cardiomyopathy
Severe aortic stenosis
Pathophysiology
ACS is most commonly due to unstable plaque formation and subsequent
rupture
Plaque formation & rupture (refer CHD, atherosclerosis)
Stable atherosclerotic plaque: manifests as stable angina (symptomatic
during exertion)
Acute Coronary Syndrome ACS 3
Unstable plaques are lipid-rich and covered by thin fibrous caps →
high risk of rupture
Inflammatory cells in the plaque (e.g., macrophages) secrete matrix
metalloproteinases → breakdown of extracellular matrix → weakening
of the fibrous cap → minor stress → rupture of the fibrous cap →
exposure of highly thrombogenic lipid core → thrombus formation →
coronary artery occlusion
Coronary artery occlusion
Partial coronary artery occlusion
Decreased myocardial blood flow → supply-demand mismatch →
myocardial ischemia
Usually affects the inner layer of the myocardium (subendocardial
infarction)
Typically manifests clinically as unstable angina and/or NSTEMI
Complete coronary artery occlusion
Impaired myocardial blood flow → sudden death of myocardial
cells (if no reperfusion occurs)
Usually affects the full thickness of the myocardium (transmural
infarction)
Typically manifests clinically as STEMI
Acute Coronary Syndrome ACS 4
Ischemia/Reperfusion injury
Reperfusion may occur spontaneously or, most commonly, after
percutaneous coronary intervention PCI or thrombolytic (fibrinolytic)
therapy
Reperfusion may limit the size of the infarction by restoring blood
flow (and thus oxygen supply) to previously ischemic tissue.
Reperfusion may have deleterious effects if ischemic myocardial
cells that were not irreversibly injured are damaged by reperfusion
(called reperfusion injury). Up to 50% of infarction size may be
secondary to reperfusion injury.
Effects of reperfusing ischemic tissue depend on when reperfusion
occurs.
If reperfusion occurs 3 hours after cessation of blood flow,
there is a greater chance of salvaging ischemic but not
irreversibly damaged tissue.
Salvaged tissue is biochemically altered, which may
interfere with normal function for several days or longer
(called myocardial stunning) and predispose tissue to
reperfusion dysrhythmias.
Acute Coronary Syndrome ACS 5
Reperfusion of previously irreversibly damaged cells results
in their death and the formation of contraction bands due
to the entry of Ca2 into the cytosol, causing
hypercontraction of the myocytes Fig. 115; Link 1119.
If reperfusion occurs 3 hours, there is a much greater chance
that previously ischemic cells are irreversibly damaged (called
reperfusion injury). Overall size of the infarction will increase.
Mechanism of irreversible myocardial injury
Superoxide free radicals (FRs) are locally produced by xanthine
oxidase and irreversibly damage myocytes
Acute inflammation occurs with an infiltration of tissue by
neutrophils
Neutrophils occlude capillary lumens, which decreases blood
flow to the ischemic tissue.
Neutrophils release proteolytic enzymes and increase the
production of reactive O2 species
Other factors that contribute to irreversible myocardial injury
include apoptosis as well as platelet and complement system
activation
Acute Coronary Syndrome ACS 6
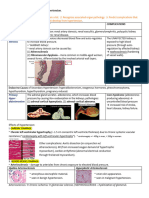
Histopathology
Acute Coronary Syndrome ACS 7
Acute Coronary Syndrome ACS 8
Complications
Clinical Features
Classical Presentation
Acute Coronary Syndrome ACS 9
Acute retrosternal chest pain
Typically described as dull, squeezing pressure and/or tightness
Commonly radiates to left chest, arm, shoulder, neck, jaw, and/or
epigastrium
Precipitated by exertion or stress
The peak time of occurrence is usually in the morning 811 a.m.)
More common in inferior wall infarction
Acute Coronary Syndrome ACS 10
Epigastric pain (maybe mistaken for reflux esophagitis)
Bradycardia (inferior wall infarction mostly due to occlusion to RCA,
which also supplies the conduction system of the heart → arrhythmia)
Clinical triad in right ventricular infarction: Hypotension, elevated
jugular venous pressure, clear lung fields
Atypical presentation: minimal to no chest pain
more likely in elderly, diabetic individuals, and women
Autonomic symptoms (e.g., nausea, diaphoresis) are often the chief
complaint.
In patients with diabetes, chest pain may be completely absent (e.g.,
silent MI due to polyneuropathy
STEMI classically manifests acutely with more severe symptoms, while
unstable angina/NSTEMI has a continuous course with milder symptoms.
Diagnostics
EKG should be performed immediately once ACS is suspected, followed by
measurement of cardiac biomarkers. Further diagnostic workup (e.g.,
echocardiography) depends on the results of initial evaluation and further
risk stratification (e.g., GRACE score, TIMI score)
EKG (refer Basics of EKG )
12-lead ECG is the best initial test if ACS is suspected
Dynamic changes require serial ECG evaluation
Compare to prior ECGs (if available)
ECG changes in STEMI
Acute Coronary Syndrome ACS 11
Acute stage: myocardial damage ongoing
Hyperacute T waves ("peaked T wave")
ST elevations in two contiguous leads with reciprocal ST
depressions
Intermediate stage: myocardial necrosis present
Absence of R wave
T-wave inversions
Pathological Q waves
Chronic stage: permanent scarring
Persistent, broad, and deep Q waves
Often incomplete recovery of R waves
Permanent T wave inversion is possible
The sequence of EKG changes over several hours to days:
hyperacute T wave → ST elevation → pathological Q wave → T
wave inversion → ST normalization → T-wave normalization
An acute LBBB + symptoms of ACS = STEMI because ST elevations
cannot be adequately assessed in the setting of an LBBB.
ECG changes in NSTEMI/unstable angina
No ST elevations present
Nonspecific changes may be present.
ST depression
Inverted T wave
Loss of R wave
EKG localization of MI
Acute Coronary Syndrome ACS 12
Cardiac Biomarkers
Creatine kinase (CKMB) and troponins T (Tn-T) and I (Tn-I) are the
first to rise, followed by aspartate aminotransferase (AST) and then
lactate (hydroxybutyrate) dehydrogenase (LDH).
Acute Coronary Syndrome ACS 13
Additional Lab findings
Elevated inflammatory markers: ↑ WBC, CRP
Elevated BNP especially in heart failure
Elevated LDH
Elevated AST SGOT
Coronary Angiography
Best test for definitive diagnosis of acute coronary occlusion
Can be used for concurrent intervention (e.g., PCI with stent
placement)
Can identify site and degree of vessel occlusion
Indications include: Acute STEMI, Other high-risk ACS (see TIMI score
below), See also cardiac catheterization
The most commonly occluded coronary arteries (descending order):
left anterior descending artery, right coronary artery, circumflex artery.
Additional studies
Transthoracic echocardiogram
Identification of any wall motion abnormalities and to assess LV
Acute Coronary Syndrome ACS 14
function
Important for risk assessment: In STEMI, the best predictor of survival
is LVEF.
Evaluation for complications: aneurysms, mitral valve regurgitation,
pericardial effusion, free wall rupture
Cardiac CT
May be considered as an alternative to invasive coronary angiography
in patients with an intermediate risk of ACS (based on TIMI score)
Allows for noninvasive visualization of the coronary arteries
Contraindication: arrhythmias, tachycardia
Risk Stratification
Thrombolysis in Myocardial Infarction TIMI score
Acute Coronary Syndrome ACS 15
The GRACE score Global Registry of Acute Coronary Events)
Differential Diagnosis
also refer DDx of chest pain
Acute Coronary Syndrome ACS 16
DDx of increased troponin
Cardiac causes
Myocarditis
Decompensated congestive heart failure
Pulmonary embolism
Cardiac arrhythmia, tachycardia
Cardiac trauma
Takotsubo cardiomyopathy
Noncardiac causes
Renal failure
Stroke
Critical illness (e.g., sepsis)
DDx of ST-elevations on ECG
Early repolarization
LBBB
Brugada syndrome
Myocarditis
Pericarditis
Pulmonary embolism
Hyperkalemia
Acute Coronary Syndrome ACS 17
Tricyclic antidepressant use
Poor ECG lead placement
Management
Summary
All patients
Acute Coronary Syndrome ACS 18
Monitoring
Serial 12-lead ECG
Continuous cardiac monitoring
Serial serum troponin measurement
Pharmacologic therapy
Sublingual or intravenous nitrate (nitroglycerin or ISDN
For symptomatic relief of chest pain
Does not improve prognosis
Contraindications: inferior wall infarct (due to risk for
hypotension), hypotension, and/or PDE 5 inhibitor (e.g.,
sildenafil) taken within last 24 hours
Morphine IV or SC 35 mg)
Only if the patient has severe, persistent chest pain or severe
anxiety related to the myocardial event
Administer with caution due to increased risk of complications
(e.g., hypotension, respiratory depression) and adverse events
Beta blocker
Recommended within the first 24 hours of admission
Avoid in patients with hypotension, features of heart failure,
and/or risk of cardiogenic shock (e.g., large LV infarct, low
ejection fraction).
Statins: early initiation of high-intensity statin (such as atorvastatin
80 mg) regardless of baseline cholesterol, LDL, and HDL levels
Loop diuretic (e.g., furosemide) if the patient has flash pulmonary
edema or features of heart failure
Supportive care
Intravenous fluids (e.g., normal saline): in patients with an inferior
MI that causes RV dysfunction
Acute Coronary Syndrome ACS 19
Oxygen: only in case of cyanosis, severe dyspnea, or SpO2 < 90%
(< 95% in STEMI
Primary interventions of MI treatment include “MONA”: Morphine,
Oxygen, Nitroglycerin, and Aspirin. But remember: Morphine, oxygen,
and nitroglycerine are not necessarily indicated for every patient (see
indications above).
STEMI
Immediate revascularization: Revascularization is the most important
step in the management of acute STEMI and initiation of further therapies
(e.g., DAPT, anticoagulation) should not delay this step in management)
Emergent coronary angiography: with percutaneous coronary
intervention (PCI)
Preferred method of revascularization
Balloon dilatation with stent implantation (see cardiac
catheterization)
Ideally, door-to-PCI time should be < 90 minutes. It should not
exceed 120 minutes.
Thrombolytic therapy: tPA, reteplase, or streptokinase
Indications:
If PCI cannot be performed < 120 minutes after onset of
STEMI
If PCI was unsuccessful
No contraindications to thrombolysis
Contraindications:
Any prior intracranial bleeding
Recent large GI bleeding
Recent major trauma, head injury, and/or surgery
Ischemic stroke within the past 3 months
Hypertension (> 180/110 mm Hg)
Acute Coronary Syndrome ACS 20
Known coagulopathy
Timing
Symptom onset was within the past 312 hours
Should be administered within < 30 minutes of patient
arrival to the hospital
Contraindicated if > 24 hours after symptom onset
PCI should be performed even if lysis is successful
Coronary artery bypass grafting
not routinely recommended for acute STEMI
Indications
If PCI is unsuccessful
If coronary anatomy is not amenable to PCI
If STEMI occurs at the time of surgical repair of a
mechanical defect
Medical therapy
Dual antiplatelet therapy: start as soon as possible
Aspirin loading dose 162 mg–325 mg
PLUS ADP receptor inhibitor: prasugrel, ticagrelor, or
clopidogrel
Dual antiplatelet therapy should be continued for at least 12
months after PCI with DES.
GP IIb/IIIa receptor antagonist (e.g., eptifibatide or tirofiban):
should be considered in precatheterization setting
Anticoagulation
Heparin or bivalirudin recommended
Continue until PCI is performed or for 48 hours after a
fibrinolytic is given.
Acute Coronary Syndrome ACS 21
"Time is muscle": Revascularization should occur as soon as possible in
patients with STEMI!
Unstable angina/NSTEMI
Dual antiplatelet therapy: start as soon as possible
Aspirin loading dose
Plus ADP receptor inhibitor: clopidogrel or ticagrelor
Dual antiplatelet therapy should be continued for at least 12
months if PCI with DES was performed.
Anticoagulation
Heparin or enoxaparin
Continue for the duration of hospitalization or until PCI is
performed.
Immediate vs. delayed revascularization
The indication for and timing of revascularization depends on the
mortality risk (e.g., TIMI score).
In patients with therapy-resistant chest pain, a TIMI score ≥ 3, ↑
troponin, and/or ST changes > 1 mm
Consider the addition of a GPIIb/ IIIa inhibitor (e.g., tirofiban or
eptifibatide)
Plan for revascularization within 72 hours (e.g., angiography
with PCI or CABG
Fibrinolytic treatment is not recommended in patients with unstable
angina or NSTEMI.
For Acute Management Checklist for ACS, refer AHA guidelines
MI in old age
Acute Coronary Syndrome ACS 22
Prevention
Primary prevention
Treatment/avoidance of modifiable risk factors for atherosclerosis
(e.g., smoking cessation, treatment of hypertension, etc.)
Healthy, plant-based diet
Regular physical activity and exercise
Low-dose aspirin is beneficial for certain high-risk groups. The choice
to prescribe it should be made on an individual basis.
Secondary prevention
Lifestyle modification and treatment of modifiable risk factors (see
“Primary prevention” above and treatment of diseases caused by
atherosclerosis)
Acute Coronary Syndrome ACS 23
Platelet-aggregation inhibitors
Lifelong low-dose aspirin 75100 mg/day
DAPT Dual Antiplatelet therapy) with the addition of an ADP receptor
inhibitor (e.g., prasugrel, ticagrelor, or clopidogrel) is recommended for
12 months for all patients who have undergone PCI.
Glycoprotein IIb/IIIa antagonists (e.g., abciximab) may be considered
but are not used routinely.
Beta blockers: Unless contraindicated, all patients should be started on
a beta blocker, which has been shown to confer a mortality benefit.
Statin: All patients should be started on a high-intensity statin (e.g.,
atorvastatin).
An aldosterone antagonist and ACE inhibitor/ARB are recommended for
all patients with ischemic cardiomyopathy and an LV ejection fraction
< 40% or symptoms of heart failure.
Acute Coronary Syndrome ACS 24
Prognosis
is related to the extent of residual myocardial ischemia, the degree of
myocardial damage and the presence of ventricular arrhythmias.
In almost one-quarter of all cases of MI, death occurs within a few
minutes without medical care. Half the deaths occur
within 24 hours of the onset of symptoms and about 40% of all affected
patients die within the first month.
Early death is usually due to an arrhythmia and is independent of the
extent of MI. However, late outcomes are determined by
the extent of myocardial damage, and unfavorable features include poor
left ventricular function, AV block and persistent
ventricular arrhythmias.
The prognosis is worse for anterior than for inferior infarcts. Bundle
branch block and high cardiac marker levels both indicate extensive
myocardial damage. Old age, depression and social isolation are also
associated with a higher mortality.
Of those who survive an acute attack, more than 80% live for a further
year, about 75% for 5 years, 50%
for 10 years and 25% for 20 years.
Acute Coronary Syndrome ACS 25
References
Davidson's Principle and Practice of Medicine 23rd edition Page 493501
First Aid for USMLE Step 1 2020 30th edition
https://www.amboss.com/us/knowledge/Acute_coronary_syndrome
Risk Stratification in ACS
Acute Coronary Syndrome ACS 26
https://www.healthline.com/health/timi-score
https://www.mdcalc.com/grace-acs-risk-mortality-calculator
2013 ACCF/AHA Guideline for the Management of STElevation Myocardial
Infarction: Executive Summary
2014 AHA/ACC Guideline for the Management of Patients With Non–ST
Elevation Acute Coronary Syndromes
Goljan's Rapid Review of Pathology 5th edition 2019, Pg 483
Robbins & Cotran's Pathological Basis of Diseases 9th edition 2015, Pg
540
Acute Coronary Syndrome ACS 27
You might also like
- Medicine in Brief: Name the Disease in Haiku, Tanka and ArtFrom EverandMedicine in Brief: Name the Disease in Haiku, Tanka and ArtRating: 5 out of 5 stars5/5 (1)
- Brief Family-Based Crisis Intervention (Cftsi) - Stephen BerkowitzDocument20 pagesBrief Family-Based Crisis Intervention (Cftsi) - Stephen Berkowitzapi-279694446No ratings yet
- JoiningInstructionsPGP2019 21 22062019Document20 pagesJoiningInstructionsPGP2019 21 22062019Aditya RajNo ratings yet
- Acute Coronary SyndromeDocument41 pagesAcute Coronary SyndromeShrests SinhaNo ratings yet
- Ischemic Heart DiseaseDocument5 pagesIschemic Heart DiseaseBert DivinagraciaNo ratings yet
- Cardio Dra. Deduyo: Ischemic Heart DiseaseDocument4 pagesCardio Dra. Deduyo: Ischemic Heart DiseaseIm SharaNo ratings yet
- Ischemic Heart DiseaseDocument6 pagesIschemic Heart DiseaseApril Joy Villacorta PonceNo ratings yet
- Acute Coronary Syndrome (Myocardial Infarction and Unstable Angina) (Clinical) - LecturioDocument36 pagesAcute Coronary Syndrome (Myocardial Infarction and Unstable Angina) (Clinical) - Lecturiokujtimepira2No ratings yet
- Acute Coronary SyndromeDocument12 pagesAcute Coronary SyndromeAnamaria SNo ratings yet
- 3 IschemicHeartDiseasesDocument17 pages3 IschemicHeartDiseasesHarsha Maheshwari100% (1)
- IHD Ema - 2020Document55 pagesIHD Ema - 2020Anastasia ApriliaNo ratings yet
- Acute Coronary Syndrome Myocardial Infarction and Unstable Angina Clinical St. Paul University Philippines Lecturio AcademyDocument44 pagesAcute Coronary Syndrome Myocardial Infarction and Unstable Angina Clinical St. Paul University Philippines Lecturio AcademyGen XNo ratings yet
- Acute Coronary SyndromesDocument5 pagesAcute Coronary SyndromesHutomo Budi Hasnian SyahNo ratings yet
- 3) Management of IHD (Notes)Document25 pages3) Management of IHD (Notes)Priyanka GosaiNo ratings yet
- Patogenesis ACSDocument124 pagesPatogenesis ACSsesraNo ratings yet
- Patogenesis ACSDocument124 pagesPatogenesis ACSHayaNo ratings yet
- Internal Medicine Case Studies BMHDocument4 pagesInternal Medicine Case Studies BMHParsaant SinghNo ratings yet
- Acute Coronary Syndrome Sindroma Koroner Akut: Toni Mustahsani Aprami, DR., SPPD, SPJPDocument57 pagesAcute Coronary Syndrome Sindroma Koroner Akut: Toni Mustahsani Aprami, DR., SPPD, SPJPrian susantoNo ratings yet
- Acute Myocardia L Infarction: Subtit LEDocument33 pagesAcute Myocardia L Infarction: Subtit LEGabiiGabriiela100% (1)
- Myocardial InfarctionDocument14 pagesMyocardial InfarctionAnandh PereraNo ratings yet
- StemiDocument7 pagesStemiAsri ParamythaNo ratings yet
- Aug 2014 Ce Angina Acute Mi StrokeDocument105 pagesAug 2014 Ce Angina Acute Mi Strokemohammed shafique ahmed hussainNo ratings yet
- Anti Ischemic DrugsDocument33 pagesAnti Ischemic Drugsdeepak askarNo ratings yet
- Acute Coronary Syndrome ACSDocument9 pagesAcute Coronary Syndrome ACSChen BrionesNo ratings yet
- Ischemic Heart DiseasesDocument26 pagesIschemic Heart DiseasesFavourNo ratings yet
- Myocardial Infarction: Seminar OnDocument17 pagesMyocardial Infarction: Seminar OnSuhas IngaleNo ratings yet
- 6 - Ischemic Heart DiseaseDocument38 pages6 - Ischemic Heart DiseaseHamzehNo ratings yet
- Anatomy Myocardial InfarctionDocument5 pagesAnatomy Myocardial InfarctionLyka Milo AvilaNo ratings yet
- Acute Coronary SyndromeDocument27 pagesAcute Coronary SyndromeSahr Anne Pilar B. ParreñoNo ratings yet
- Askep Pada Acute Coronary Syndrome AcsDocument62 pagesAskep Pada Acute Coronary Syndrome Acsdefi rhNo ratings yet
- Cardiovascular Disease: Coronary Heart Disease Refers To The Failure of The Coronary Circulation To Supply AdequateDocument4 pagesCardiovascular Disease: Coronary Heart Disease Refers To The Failure of The Coronary Circulation To Supply AdequateAnant Kumar SrivastavaNo ratings yet
- Chapter 14-Nervous System Disorders: Payton Kesselring Case Study 6Document3 pagesChapter 14-Nervous System Disorders: Payton Kesselring Case Study 6joseph100% (2)
- Acute Coronary SyndromeDocument84 pagesAcute Coronary SyndromeRinkita MallickNo ratings yet
- Coronary Artery Disease (Cad)Document4 pagesCoronary Artery Disease (Cad)Freddy PanjaitanNo ratings yet
- Konsep Tatalaksana Pada ImaDocument57 pagesKonsep Tatalaksana Pada Imariska silviaNo ratings yet
- Myocardial Infarction AssignmentDocument23 pagesMyocardial Infarction AssignmentPums100% (6)
- Pathology+101 Complete)Document147 pagesPathology+101 Complete)Goh Kah Yong100% (2)
- Pathology of Acute Myocardial InfarctionDocument13 pagesPathology of Acute Myocardial InfarctionNaily Nuzulur RohmahNo ratings yet
- Angina Pectoris Myocardial Infarction: Bahuguna, Nimisha Imd-Batch 3Document19 pagesAngina Pectoris Myocardial Infarction: Bahuguna, Nimisha Imd-Batch 3Nimisha BahugunaNo ratings yet
- Myocardial InfarctionDocument6 pagesMyocardial InfarctionMaicie Rose Bautista VallesterosNo ratings yet
- Myocardial InfarctionDocument52 pagesMyocardial InfarctionAmad MirulNo ratings yet
- PATHO-II Unit V Cardiovascular DisordersDocument52 pagesPATHO-II Unit V Cardiovascular DisordersMuhammad ShayanNo ratings yet
- Cvspa04 Ihd and MiDocument8 pagesCvspa04 Ihd and MiRobert So JrNo ratings yet
- 5 Coronary Artery DiseasesDocument60 pages5 Coronary Artery Diseasesjyothi lekshmi sNo ratings yet
- Acute Coronary Sindromes 21046 61975Document28 pagesAcute Coronary Sindromes 21046 61975Simina ÎntunericNo ratings yet
- Treatment of NSTEMI Non-ST Elevation Myocardial inDocument12 pagesTreatment of NSTEMI Non-ST Elevation Myocardial inDavy JonesNo ratings yet
- Pathophysiology Worksheet MIDocument2 pagesPathophysiology Worksheet MIpjbedelNo ratings yet
- Lecture 2 Ischemic Heart DiseasesDocument19 pagesLecture 2 Ischemic Heart DiseasesOsama MalikNo ratings yet
- Acutecoronarysyndromeacs 180106041458Document82 pagesAcutecoronarysyndromeacs 180106041458Razvan SulaimanNo ratings yet
- Myocardial InfarctionDocument6 pagesMyocardial InfarctionAh LynNo ratings yet
- CardiologyDocument4 pagesCardiologyShatha AlgahtaniNo ratings yet
- Acute Coronary Syndrome Sindroma Koroner AkutDocument50 pagesAcute Coronary Syndrome Sindroma Koroner AkutWinda Ayu PurnamasariNo ratings yet
- Week 10 - Hypertension, Atherosclerosis, ArrhythmiaDocument14 pagesWeek 10 - Hypertension, Atherosclerosis, Arrhythmiashivani patel100% (1)
- Ischemic Heart Disease (IHD)Document37 pagesIschemic Heart Disease (IHD)Yowan SusantiNo ratings yet
- Ischaemic (Coronary) Heart DiseaseDocument4 pagesIschaemic (Coronary) Heart DiseasePrabhathNo ratings yet
- Myocardial Ischemia and Infarction, Part I ST Segment Elevation and Q Wave Syndromes, Goldberger's Clinical Electrocardiography PDFDocument19 pagesMyocardial Ischemia and Infarction, Part I ST Segment Elevation and Q Wave Syndromes, Goldberger's Clinical Electrocardiography PDFDavidNo ratings yet
- A Standardized and Comprehensive Approach To The Management of Cardiogenic Shock 2020Document13 pagesA Standardized and Comprehensive Approach To The Management of Cardiogenic Shock 2020gloriaNo ratings yet
- Infarction PDFDocument24 pagesInfarction PDFAmandeep Kaur ChabbraNo ratings yet
- Non Modifiable FactorsDocument2 pagesNon Modifiable FactorsColette Marie PerezNo ratings yet
- Comprehensive Insights into Acute Coronary Syndrome: Pathways, Interventions, and Holistic RecoveryFrom EverandComprehensive Insights into Acute Coronary Syndrome: Pathways, Interventions, and Holistic RecoveryNo ratings yet
- Paediatric Nursing Dissertation ExamplesDocument4 pagesPaediatric Nursing Dissertation ExamplesCustomCollegePaperUK100% (1)
- Case StudyDocument41 pagesCase StudyAubrey Ann FolloscoNo ratings yet
- CiteScore Rank2020 ScopusDocument16 pagesCiteScore Rank2020 ScopusPhu NguyenNo ratings yet
- اسئلة طفيليات MCQ مهمة جدا PDFDocument15 pagesاسئلة طفيليات MCQ مهمة جدا PDFفواطم صائب عباس فاضلNo ratings yet
- A Review On Nutraceuticals: Classification and Its Role in Various DiseaseDocument10 pagesA Review On Nutraceuticals: Classification and Its Role in Various DiseasePrakash RoyNo ratings yet
- Apoptosis: MBBS, FCPS, M.Phil. Histopathology Department of Pathology CMHLMCDocument42 pagesApoptosis: MBBS, FCPS, M.Phil. Histopathology Department of Pathology CMHLMCAiza AnwarNo ratings yet
- Derived PositionDocument7 pagesDerived PositionChristl Jan Tiu100% (1)
- Functions and Anatomy of Human Body GK Notes in PDFDocument14 pagesFunctions and Anatomy of Human Body GK Notes in PDFreenajoseNo ratings yet
- ARBs (Angiotensin II Receptor Blockers) NCLEXDocument15 pagesARBs (Angiotensin II Receptor Blockers) NCLEXSameerQadumi100% (1)
- Acupuncture PDFDocument2 pagesAcupuncture PDFAyu SudiantariNo ratings yet
- Biochem 322-Final 2005Document1 pageBiochem 322-Final 2005api-3763291No ratings yet
- IugrDocument5 pagesIugrvincentsharonNo ratings yet
- NBL ReviewerDocument6 pagesNBL ReviewerNovie Carla GayosaNo ratings yet
- CLOZAPINEDocument5 pagesCLOZAPINEMar OrdanzaNo ratings yet
- Pharm MGT NotesDocument62 pagesPharm MGT NotesMOHAMMED B KAMARANo ratings yet
- M1 MAY 2022 With Per Brgy BreakdownDocument408 pagesM1 MAY 2022 With Per Brgy BreakdownLaura Grace DecanoNo ratings yet
- Jurnal Carpal Tunnel SyndromeDocument11 pagesJurnal Carpal Tunnel SyndromeArjuna MarzaNo ratings yet
- Molecular Biology BT401: BiotechnologyDocument12 pagesMolecular Biology BT401: BiotechnologyVivek GuptaNo ratings yet
- Hyperbaric Oxygen Therapy Descriptive Review Of.52Document8 pagesHyperbaric Oxygen Therapy Descriptive Review Of.52drhestrellaNo ratings yet
- Near DrowningDocument36 pagesNear DrowningSheila Rose SalesNo ratings yet
- Grade 8-Q1-LMDocument85 pagesGrade 8-Q1-LMJoseph R. GallenoNo ratings yet
- Stability Indicating RP-HPLC Method For The Determination of Terbutaline Sulphate, Guaifenesin, Ambroxol Hydrochloride and Preservatives Content in Liquid FormulationsDocument6 pagesStability Indicating RP-HPLC Method For The Determination of Terbutaline Sulphate, Guaifenesin, Ambroxol Hydrochloride and Preservatives Content in Liquid FormulationsHanimi ReddyNo ratings yet
- (Iv) Osteomyelitis: Mini-Symposium: PathologyDocument14 pages(Iv) Osteomyelitis: Mini-Symposium: PathologyFiska FianitaNo ratings yet
- Uia 16 MCQ QUESTIONSDocument7 pagesUia 16 MCQ QUESTIONSsofian ashourNo ratings yet
- Cardiovascula R Imaging: Dept. of Diagnostic Radiology Diponegoro Univ./Dr - Kariadi General HospitalDocument85 pagesCardiovascula R Imaging: Dept. of Diagnostic Radiology Diponegoro Univ./Dr - Kariadi General HospitalvaniaNo ratings yet
- Reproduction 8 QP 5090Document10 pagesReproduction 8 QP 5090sunflower rantsNo ratings yet
- Biology Lab Report 1Document2 pagesBiology Lab Report 1JhiGz Llausas de GuzmanNo ratings yet
- Usa 2Document6 pagesUsa 2Aiman ArifinNo ratings yet