Professional Documents
Culture Documents
maleek BPH
maleek BPH
Uploaded by
Abdul maleek rex0 ratings0% found this document useful (0 votes)
1 views28 pagesBENIGN PROSTATE HYPERTROPHY
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentBENIGN PROSTATE HYPERTROPHY
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
1 views28 pagesmaleek BPH
maleek BPH
Uploaded by
Abdul maleek rexBENIGN PROSTATE HYPERTROPHY
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 28
Benign prostate hyperplasia
Moro abdul malik
Outline
• introduction
• brief anatomy
• Definition
• Epidemiology
• Aetiology /pathophysiology
• Clinical evaluation :history/ physical exam/investigation
• Management
• Complication
Introduction
• Benign prostatic hyperplasia (BPH) is a common condition
encountered in aging men and a common cause of lower urinary
tract symptoms. Histological prevalence of BPH is common, and
disease progression is associated with bladder outflow
obstruction, this may present clinically in both the emergency
surgical and outpatient clinical settings
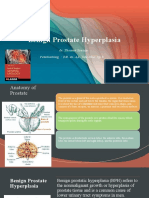
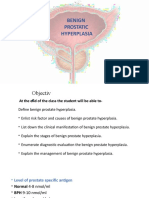
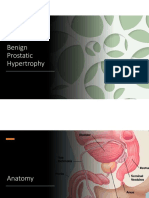
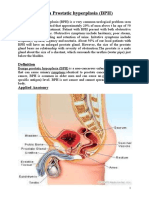
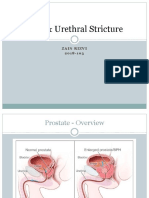
Brief anatomy
Definitions related to BPH
• Benign prostatic hyperplasia (BPH) refers to the non-malignant
growth or hyperplasia of prostate tissue and is a common cause
of lower urinary tract symptoms in men.
• BPE:) describes the increased size of the gland (usually
secondary to BPH)
• BOO: bladder outlet obstruction as a result of BPE
Epidemiology
• Age is a significant predictor of both development of BPH and
subsequent LUTS, with 50% of men over the age of 50 shown to
have evidence of BPH and the association with the development
of LUTS shown to increase with age in a linear fashion
• BPH is a common problem affecting the quality of life of approximately
1/3 of men older than 50 .it is histologically present in up to 90% of
men over the age of 85.world wide about 30million men have
symptoms of BPH
• The prevalence is similar in all races however African Americans have
a more severe and progressive symptoms ,possibly due to higher
androgen levels .
Aetiolgy/pathophysiolgy
• The aetiology of BPH is thought to due to an altered equilibrium
between cell proliferation and apoptosis .the aetiological factors are
complex .prostatic enlargement depends on the potent androgen
DHT from the metabolism of testosterone by type II 5-alpha-
reductase in the prostate. DHT acts locally and binds to androgen
receptors the prostate ,potentially leading to BPH.
• Other factors in the aetiology include ,metabolic
syndrome,hyperinsulinemia,norepinephrine ,angiotensin II,insulin like
growth factors
• Studies have shown that there is a large number of alpha-adrenergic
receptors located in the smooth muscle of the stroma and capsule as
well as the bladder neck. stimulation of these receptors causes an
increase in smooth muscle tone which worsens the symptoms of
BPH(LUTS)
• BPH is microscopically characterized by a hyperplastic process, this
may result in restriction of the flow of urine from the bladder >
manifestation of symptoms
Clinical presnetation
LUTS can be grouped into :
Storage/irritative symptoms
• Urinary frequency
• Nocturia
• Urinary urgency
• Voiding/obstructive symptoms
• Hesitency
• Straining
• Weak stream,intermittency,dribbling,incomplete bladder emptying ,retention
• The clinician must rule out other conditions that can present with LUTS
• DM
• Ca prostate
• UTIs
Cauda equina syndrome (can present with acute retention)
Prostatitis
Neurogenic bladder (can be secondary to Parkinson's, Multiple sclerosis, etc.)
Urinary tract stones (bladder stones)
Urethral stricture
Physical exam and evaluation
• A general exam should be performed first (anemia,edema ,
BP,hydration),
• IPSS
• the examination should include abdominal examination (looking for
a palpable bladder/loin pain) and examination of external genitalia
(meatal stenosis or phimosis). The examination should then conclude
with a digital rectal examination making a note in particular of the
size, shape (how many lobes), and consistency
(smooth/hard/nodular) of the prostate (BPH is characterized by a
smoothly enlarged prostate).
investigations
Urinalysis
• Appearance,Dipstick,Urine microscopy,Urine culture/ sensitivity(MSU)
Prostate specific antigen (normal value=0-4.0ng/ml)
Blood tests
• Fbc,RFT-serum creatinine ,BUE,blood urea and electrolytes
Ultrasound,CT/MRI urogram,retrograde urethro-cystography
Cystoscopy/urethroscopy
Biopsy
Treatment / management
Men with BPH may present acutely with urinary retention at the
ER, a transurethral catheter should be passed to relieve the
retention or a suprapubic catheterization if the transurethral
approach fails (in the absence of contraindications)
Treatment modalities include
Watchful waiting
Medical therapy
surgery
Watchful waiting
• Patients are adequately assessed to rule out malignancy. usually
offered to patients with an IPSS < 8 who are not troubled by
symptoms of BPH
• lifestyle advice. Examples include weight loss, reducing caffeine
intake or reducing fluid intake in the evening, and avoiding
constipation are given to patients.
• 3 monthly reassessment
• Contraindicated if there is
• Acute/chronic retention 2.recurrent UTIs,haematuria,signs of renal
impairment.
Medical treatment
Both static and dynamic components contribute to the
pathophysiology of BPH. Medical therapy aims to address both of
these components. For those with IPSS<19
1.Alpha-blockers=blocks alpha-adrenergic receptors in the
stromal smooth muscles of the prostate>smooth muscle
relaxation and improving urine flow
• Tamsulosin (400mcg once daily)
• Alfuzosin (10mg once daily)
• 5 alpha-reductase inhibitors:addresses the static component by
prevention the conversion of testosterone to DHT causing the
shrinkage of the prostate by about 25%. It takes about 6 months
for effects to be seen
• finasteride (5mg once daily) ##loss of libido and erectile
dysfuction are some adverse effects.
• dutasteride
• Anticholinergics detrusor muscle stability (solifenacin, tolterodine, and
oxybutynin)
• Phosphodiesterase-5 enzyme inhibitors; mediate smooth muscles
relaxation in the lower urinary tract (tadalafil)
• Alpha blocker+ a 5 alpha-reductase inhibitor= combination therapy
Surgery
• Guidelines for the indications for surgery in BPH as outlined by the European Association of Urology
(EAU) are as follows:[
Refractory urinary retention
Recurrent urinary infections
Haematuria refractory to medical treatment (other causes excluded)
Renal insufficiency
Bladder stones
Increased post-void residual
• High-pressure chronic retention (absolute indication
TURP
• Transurethral resection surgery focuses on debulking the
prostate to produce an adequate channel for urine to flow. This
is achieved using diathermy to produce a high-frequency
current that allows the cutting of tissue. By resecting all
obstructing prostatic tissue, an adequate channel can be created
to allow urine to flow. Bipolar diathermy has largely replaced
monopolar diathermy techniques for TURP, with increased
benefits such as resection in saline and reduced risk of "TUR
syndrome
HOLEP(Holmium laser enucleation of the
prostate)
• Previously, open prostatectomy allowed adenoma to be
removed or enucleated off its capsule. This can now be achieved
with laser enucleation, referred to as HoLEP (Holmium laser
enucleation of the prostate). Meta-analysis has shown improved
Qmax (flow rate), reduction in post-void residual, and IPSS
compared to TURP.
• Benefits include a lower transfusion rate with no increase in
complications compared to TURP. However, limitations include
specialized equipment required making it less readily available
Urolift
• Tissue-sparing approaches, such as Urolift, have also been
developed. This can help minimize the risk of bleeding in co-
morbid patients and the associated risks of more invasive
surgery (such as anesthesia risk, prolonged surgery time, etc.).
By compressing prostate lobes, the channel can be widened in
the prostatic urethra, improving LUTS. Studies have shown
benefits, including the possibility of day-case surgery, preserved
sexual function, and improved symptom scores (IPSS), and flow
rates (QMax
Other surgical options
• Intra urethral stents
• High intensity focused ultrasound(HIFU)
• Trans urethral vaporization of the prostate
• Trans urethral needle ablation (TUNA)
• Trans urethral laser therapy
• Transurethral balloon dilatation
• Open simple prostatectomy
Common Complications of BPH
Urinary retention
Chronic retention
Urinary tract infection (due to incomplete emptying)
Haematuria
Bladder calculi
BOO > reflux of urine into the ureters and kidney> renal impairment
Thank you
You might also like
- Environmental Impact Assessment ModuleDocument39 pagesEnvironmental Impact Assessment ModuleJoshua Landoy100% (2)
- Afar 2 - Summative Test (Consolidated) Theories: Realized in The Second Year From Upstream Sales Made in Both YearsDocument23 pagesAfar 2 - Summative Test (Consolidated) Theories: Realized in The Second Year From Upstream Sales Made in Both YearsVon Andrei Medina100% (1)
- Benign Prostatic HyperplasiaDocument34 pagesBenign Prostatic Hyperplasiaanwar jabari100% (1)
- Benign Prostate HyperplasiaDocument49 pagesBenign Prostate HyperplasiaRohani TaminNo ratings yet
- 1 BPHDocument27 pages1 BPHVikrant GholapNo ratings yet
- Benign Prostatic Hyperplasia (BPH)Document8 pagesBenign Prostatic Hyperplasia (BPH)miftah ar rahmahNo ratings yet
- Medscape BPHDocument41 pagesMedscape BPHEugenia ShepanyNo ratings yet
- BPH 180828154943Document42 pagesBPH 180828154943Amandeep SinghNo ratings yet
- Bladder Outlet Obstruction & Obstructive Uropathy BPHDocument73 pagesBladder Outlet Obstruction & Obstructive Uropathy BPHSisay FentaNo ratings yet
- Benign prostate hyperplasia (BPH) : Reporter: FM R1 余明謙 Supervisor: VS 張德宇Document53 pagesBenign prostate hyperplasia (BPH) : Reporter: FM R1 余明謙 Supervisor: VS 張德宇余明謙No ratings yet
- Benign Prostatic Hyperplasia CausesDocument4 pagesBenign Prostatic Hyperplasia CausesDae Young SeoNo ratings yet
- ImplementationDocument3 pagesImplementationSittie Hafsah L. MasbodNo ratings yet
- Benign Prostatic Hyperplasia (BPH) : Eman Shaker 20182348Document85 pagesBenign Prostatic Hyperplasia (BPH) : Eman Shaker 20182348زهرة الدوارNo ratings yet
- Urogenital SystemDocument32 pagesUrogenital SystemLove & Humanity100% (1)
- Prostate Hyperplasia, Benign: Author: Raymond J Leveillee, MD, FRCS (Glasg), Professor of Clinical Urology, RadiologyDocument36 pagesProstate Hyperplasia, Benign: Author: Raymond J Leveillee, MD, FRCS (Glasg), Professor of Clinical Urology, RadiologyGerald FilomenoNo ratings yet
- BPH PDFDocument7 pagesBPH PDFJody FelizioNo ratings yet
- Practice Essentials: Signs and SymptomsDocument4 pagesPractice Essentials: Signs and Symptomsyeni62No ratings yet
- BPH (Benign Prostatic Hyperplasia)Document11 pagesBPH (Benign Prostatic Hyperplasia)AviZhafiraNo ratings yet
- SL No Content NODocument12 pagesSL No Content NOPdianghunNo ratings yet
- Benign Prostatic HypertrophyDocument45 pagesBenign Prostatic Hypertrophyjitendra magarNo ratings yet
- Benign Prostatic Hyperplasia (BPH) and Bladder Outlet Obstruction (BOO)Document73 pagesBenign Prostatic Hyperplasia (BPH) and Bladder Outlet Obstruction (BOO)Swe Zin NaingNo ratings yet
- BPH - TextDocument7 pagesBPH - TextSomesh GuptaNo ratings yet
- BPH - TextDocument7 pagesBPH - TextSomesh GuptaNo ratings yet
- Lecture 5.05 - Lower Urinary Tract Symptoms and Benign Prostatic Hyperplasia (BPH)Document41 pagesLecture 5.05 - Lower Urinary Tract Symptoms and Benign Prostatic Hyperplasia (BPH)splider5000sNo ratings yet
- Benign Prostate HyperthropyDocument3 pagesBenign Prostate Hyperthropyzmae23No ratings yet
- Benign Prostatic Hyperplasia (BPH) : By, Ms. Ekta. S. Patel, I Yr M.SC NursingDocument71 pagesBenign Prostatic Hyperplasia (BPH) : By, Ms. Ekta. S. Patel, I Yr M.SC NursingannisanabilaasNo ratings yet
- Benign Prostatic HyperthropyDocument54 pagesBenign Prostatic HyperthropyPrawira Buntara PutraNo ratings yet
- Disorders of The Prostate: Dr.M.Galuh Richata, SpuDocument32 pagesDisorders of The Prostate: Dr.M.Galuh Richata, SpuEmallia Phypiet FitrianiNo ratings yet
- Incontinentia Urine Kuliah Uniba 6-11-12. ADocument53 pagesIncontinentia Urine Kuliah Uniba 6-11-12. AHumaira AzmiNo ratings yet
- Benign Prostatic HyperplasiaDocument28 pagesBenign Prostatic HyperplasiaFedrick MasatuNo ratings yet
- Benign Prostatic Hypertrophy: Pathophysiology and EtiologyDocument4 pagesBenign Prostatic Hypertrophy: Pathophysiology and EtiologyErnestomalamionNo ratings yet
- Benign Prostat HiperplasiaDocument17 pagesBenign Prostat HiperplasiahawhawnurNo ratings yet
- BPH DefinitionDocument5 pagesBPH DefinitionMadhu Sudhan PandeyaNo ratings yet
- BPH Case PresentationDocument15 pagesBPH Case PresentationxxandraNo ratings yet
- Benign Prostatic HyperplasiaDocument9 pagesBenign Prostatic Hyperplasiaanju rachel joseNo ratings yet
- BPHDocument20 pagesBPHHerly KakaNo ratings yet
- BPH by SamuelDocument33 pagesBPH by SamuelIan Smith AkampuriraNo ratings yet
- Pharmacotherapy of - Benign Prostatic HyperplasiaDocument4 pagesPharmacotherapy of - Benign Prostatic HyperplasiaBaarid HamidiNo ratings yet
- BPH and Urethral StrictureDocument25 pagesBPH and Urethral Stricturezaminazz100% (1)
- Canuuc - Prostate Disease 1 Benign May 2017Document29 pagesCanuuc - Prostate Disease 1 Benign May 2017dktkaNo ratings yet
- Benign Prostatic HyperplasiaDocument10 pagesBenign Prostatic HyperplasiaRoshwill KingNo ratings yet
- Benign Prostatic Hyperplasia BPH: PathologyDocument9 pagesBenign Prostatic Hyperplasia BPH: Pathologyhussain Altaher0% (1)
- BPHDocument25 pagesBPHsurya mertayasaNo ratings yet
- Benign Prostatic Hyperplasia (BPH) : Jeselo Ouano GormeDocument60 pagesBenign Prostatic Hyperplasia (BPH) : Jeselo Ouano GormeMaddox EdeyajNo ratings yet
- Benign Prostate Hypertrophy NDocument43 pagesBenign Prostate Hypertrophy NAmjad AliNo ratings yet
- Powell 2020Document7 pagesPowell 2020kanaNo ratings yet
- Benign Prostatic HyperplasiaDocument6 pagesBenign Prostatic HyperplasiaAnonymous 9OkFvNzdsNo ratings yet
- Clinical Manifestations and Diagnostic Evaluation of Benign Prostatic Hyperplasia - UpToDateDocument13 pagesClinical Manifestations and Diagnostic Evaluation of Benign Prostatic Hyperplasia - UpToDateJhonnyJesùsHonorioEstelaNo ratings yet
- Benign prostatic hyperplasia يوازمحلا يلع دمحا.د: Epidemiology of BPHDocument8 pagesBenign prostatic hyperplasia يوازمحلا يلع دمحا.د: Epidemiology of BPHAli SafaaNo ratings yet
- Benign Prostatic HyperplasiaDocument4 pagesBenign Prostatic HyperplasiaAdelle Fortunato100% (2)
- BPH 2017Document14 pagesBPH 2017Andi MuftyNo ratings yet
- Benign Prostatic HyperplasiaDocument16 pagesBenign Prostatic HyperplasiaJood AL AbriNo ratings yet
- medical management of bepDocument41 pagesmedical management of bepyogendra devkotaNo ratings yet
- Dr. Mugalo E.LDocument32 pagesDr. Mugalo E.Lkhadzx100% (3)
- Clinical Manifestations and Diagnostic Evaluation of Benign Prostatic Hyperplasia - UpToDateDocument17 pagesClinical Manifestations and Diagnostic Evaluation of Benign Prostatic Hyperplasia - UpToDateMario Lopez CastellanosNo ratings yet
- Benign Prostatic HyperplasiaDocument19 pagesBenign Prostatic HyperplasiaEmmanuel MacheleleNo ratings yet
- Benign Prostatic HyperplasiaDocument36 pagesBenign Prostatic Hyperplasiamomodou s jallowNo ratings yet
- WONG Activity#9Document4 pagesWONG Activity#9Lecery Sophia WongNo ratings yet
- Urinary RetentionDocument28 pagesUrinary RetentionSchoeb MuhammadNo ratings yet
- Class Presentation ON BPH: Presented By: Ruchika Kaushal M.Sc. Nursing 1 YearDocument31 pagesClass Presentation ON BPH: Presented By: Ruchika Kaushal M.Sc. Nursing 1 YearRuchika KaushalNo ratings yet
- Benign Prostatic HyperplasiaDocument6 pagesBenign Prostatic HyperplasiaHenny HansengNo ratings yet
- Pelvic Dysfunction in Men: Diagnosis and Treatment of Male Incontinence and Erectile DysfunctionFrom EverandPelvic Dysfunction in Men: Diagnosis and Treatment of Male Incontinence and Erectile DysfunctionNo ratings yet
- Object Oriented Programming (OOP) - CS304 Power Point Slides Lecture 21Document49 pagesObject Oriented Programming (OOP) - CS304 Power Point Slides Lecture 21Sameer HaneNo ratings yet
- Domain Model Ppt-1updatedDocument17 pagesDomain Model Ppt-1updatedkhadija akhtarNo ratings yet
- GenMath Module 5 Week 5Document15 pagesGenMath Module 5 Week 5Immanuel CañecaNo ratings yet
- MC&OB Unit 4Document17 pagesMC&OB Unit 4Tanya MalviyaNo ratings yet
- Capitalisation AssignmentDocument5 pagesCapitalisation AssignmentFayis FYSNo ratings yet
- Class 12 Sample PaperDocument6 pagesClass 12 Sample PaperAaditya Vignyan VellalaNo ratings yet
- A Short Version of The Big Five Inventory (BFI-20) : Evidence On Construct ValidityDocument22 pagesA Short Version of The Big Five Inventory (BFI-20) : Evidence On Construct ValidityBagas IndiantoNo ratings yet
- Types of ParentingDocument13 pagesTypes of ParentingViseshNo ratings yet
- Alarm Security Pic - Google ShoppingDocument1 pageAlarm Security Pic - Google Shoppingleeleeleebc123No ratings yet
- Title: Relationship Between PH and Chemiluminescence of Luminol Author: Rolando Efraín Hernández RamírezDocument2 pagesTitle: Relationship Between PH and Chemiluminescence of Luminol Author: Rolando Efraín Hernández RamírezEfraínNo ratings yet
- Arithmetic 1Document15 pagesArithmetic 1arman malikNo ratings yet
- Occupational Safety and Health Aspects of Voice and Speech ProfessionsDocument34 pagesOccupational Safety and Health Aspects of Voice and Speech ProfessionskaaanyuNo ratings yet
- PCA TIME SAVING DESIGN AIDS - Two-Way SlabsDocument7 pagesPCA TIME SAVING DESIGN AIDS - Two-Way SlabsvNo ratings yet
- Teacher: Diana Marie V. Aman Science Teaching Dates/Time: Quarter: SecondDocument6 pagesTeacher: Diana Marie V. Aman Science Teaching Dates/Time: Quarter: SecondDiana Marie Vidallon AmanNo ratings yet
- Comm 130 PortfolioDocument23 pagesComm 130 PortfolioSami MossNo ratings yet
- Tuyển Sinh 10 - đề 1 -KeyDocument5 pagesTuyển Sinh 10 - đề 1 -Keynguyenhoang17042004No ratings yet
- Unit 1 - Task 3 - Reader Guru Adventure! - Evaluation Quiz - Revisión Del IntentoDocument7 pagesUnit 1 - Task 3 - Reader Guru Adventure! - Evaluation Quiz - Revisión Del IntentoNelson AbrilNo ratings yet
- Final Simple Research (BS CRIM. 1-ALPHA)Document5 pagesFinal Simple Research (BS CRIM. 1-ALPHA)Julius VeluntaNo ratings yet
- Toward The Efficient Impact Frontier: FeaturesDocument6 pagesToward The Efficient Impact Frontier: Featuresguramios chukhrukidzeNo ratings yet
- Applications Guide 2021 Covering LettersDocument8 pagesApplications Guide 2021 Covering LettersLALUKISNo ratings yet
- Factory Physics PrinciplesDocument20 pagesFactory Physics Principlespramit04100% (1)
- Semantically Partitioned Object Sap BW 7.3Document23 pagesSemantically Partitioned Object Sap BW 7.3smiks50% (2)
- Questionnaire For Technical AssistantDocument4 pagesQuestionnaire For Technical AssistantHabtamu Ye Asnaku LijNo ratings yet
- The Ezekiel Cycle of 500 YearsDocument1 pageThe Ezekiel Cycle of 500 YearsOtis Arms100% (1)
- Cvp-Analysis AbsvarcostingDocument13 pagesCvp-Analysis AbsvarcostingGwy PagdilaoNo ratings yet
- Bydf3 ElectricDocument61 pagesBydf3 ElectricIvan Avila100% (1)
- Sword of DestinyDocument435 pagesSword of DestinyJailouise Perez100% (1)
- Adamco BIFDocument2 pagesAdamco BIFMhie DazaNo ratings yet