Professional Documents
Culture Documents
Respiratory Assessment
Respiratory Assessment
Uploaded by
Scott HalOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Respiratory Assessment
Respiratory Assessment
Uploaded by
Scott HalCopyright:
Available Formats
Respiratory
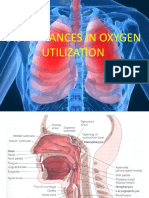
Assessment of the Respiratory System Anatomy and physiology review Upper respiratory tract Lower respiratory tract Lungs Accessory muscles of respiration Respiratory changes associated with aging
Role of the respiratory system Oxygenation and tissue perfusion
Organs/tissues important in meeting the need
Lungs Heart Blood vessels/RBC Patient history Target items for respiratory - Family, personal, smoking, drug use, allergies, travel, place of residence, dietary, occupational, and socioeconomic level Smoking pack years of smoking = number of packs smoked per day multiplied by the number of years the patient has smoked Current health problems cough, sputum production, chest pain, dyspnea Nutritional status
Physical assessment Lungs and thorax Other indicators clubbing, weight loss, unevenly developed muscles, skin & mucous membrane changes, general appearance, and endurance
Psychosocial Stress level Chronic issues family support, social activity, financial constraints, disability Coping mechanisms Access to support services
Care of Patients with Noninfectious Lower Respiratory Problems Chronic Airway Limitations (CAL) Asthma Chronic bronchitis Pulmonary emphysema Chronic Obstructive Pulmonary Disease (COPD) Emphysema & Chronic bronchitis Characterized by bronchospasm & dyspnea (what is this term?) Tissue damage is not reversible & increases in severity, eventually leading to respiratory failure
Asthma Intermittent disease Reversible airflow obstruction and wheezing
Pathophysiology Bronchial asthma is an intermittent and reversible airflow obstruction affecting only the airways, not the alveoli Airway obstruction occurs by: o Inflammation o Airway hyper-responsiveness Etiology Classified based on trigger events Inflammation response to specific o Allergens o General irritants o Microorganisms o Aspirin Hyper-responsiveness occurs with o Exercise o URI o Unknown reasons Genetic Genetic variation of a gene controls synthesis and activity of betaadrenergic receptors Inflammation caused by allergen binding to immunoglobulin E (IgE) Bronchospasm as a result of airway hyper-responsiveness ASA & other NSAIDS can trigger asthma in some people
Older adults Change in sensitivity of beta-adrenergic receptors Teach how to prevent asthma attacks Women 35% higher incidence Teach correct use of preventive and rescue drugs Collaborative management Assessment History Physical & clinical manifestations o Audible wheeze and increased resp rate o Increased cough o Use of accessory muscles o Barrel chest from air trapping o Long breathing cycle o Cyanosis o Hypoxemia Laboratory Assessment ABGs o Arterial oxygen level may be decreased in acute attack o Arterial carbon dioxide may decrease early in attach and increase later, indicating poor gas exchange Pulmonary Function Tests (PFTs) o Most accurate measures using spirometry Forced vital capacity (FVC) Forced expiratory volume in the first second (FEV1) Peak expiratory flow rate (PEFR) Interventions Patient education disease often intermittent; guided self-care to co-manage disease with goal of increasing symptom free periods and decreasing the number & severity of attacks Peak flow twice daily Personal drug therapy plan Drug therapy Based on the step category for severity and treatment Preventive Rx used daily regardless of symptoms Rescue drugs stop attack once it has started
Bronchodilators o Short-acting beta2 agonists o Long-acting beta2 agonists o Cholinergic antagonists o Methylxanthines
Anti-inflammatory o Corticosteroids o NSAIDS o Leukotriene antagonists o Immunomodulators
Other treatments Exercise and activity recommended Oxygen therapy acute attacks Status asthmaticus Life-threatening; acute May lead to pneumothorax, cardiac or respiratory arrest Treatment: IV fluids, potent systemic bronchodilator, steroids, epi, and O2 Emphysema
Pathophysiology loss of lung elasticity & hyperinflation of the lung Airtrapping caused by loss of elastic recoil in the alveolar walls, overstretching, & enlargement of the alveoli into bullae, and collapse of small airways (bronchioles) Dyspnea; increased respiratory rate
Chronic Bronchitis Inflammation of bronchi and bronchioles caused by chronic exposure to irritants (i.e. tobacco smoke) Inflammation, vasodilation, congestion, mucosal edema, and bronchospasm Airway only affected, not the alveoli Thick mucus production
COPD Etiology Tobacco smoke Alpha1-antitrypsin (AAT) deficiency Air pollution
Complications Hypoxemia Acidosis Respiratory infections Cardiac failure Cardiac dysrhythmias Physical assessment & clinical manifestations History General appearance Respiratory changes Cardiac changes
Laboratory assessment ABGs Sputum samples CBC/Hemoglobin & Hematocrit Serum electrolytes Serum AAT Chest X-ray PFTs Nursing dx Impaired Gas Exchange
Ineffective Breathing Pattern
Ineffective Airway Clearance
Imbalanced Nutrition < Body
Anxiety
Activity Intolerance
Surgical management
Risks, esp. for older adult Pneumonia
Community Based Care Home care management
Health teaching
Care of Patients with Infectious Respiratory Problems Influenza highly contagious acute illness
Pneumonia Pathophysiology Excess fluid, inflammatory process Inflammation triggered by infectious organisms & inhalation of irritants Community acquired infections pneumonia (types of individuals most at risk?) Nosocomial (hospital-acquired) (types of patients most at risk?) Atelectasis Hypoxemia
Assessment History Physical assessment Clinical manifestations Psychosocial Laboratory
Community-based Care Home care management Health teaching Health care resources
Severe Acute Respiratory Syndrome (SARS) Infection of cells of the respiratory tract, triggers inflammatory response No known effective treatment Prevention Avian Influenza Bird Flu Virus Prevention
Pulmonary Tuberculosis Highly communicable Transmitted via aerosolization HIV high risk individuals on developing TB
Clinical manifestations Progressive fatigue Lethargy Nausea Anorexia Weight loss Irregular menses Low-grade fever, night sweats Cough, mucopurulent sputum, blood streaks
Assessment History Physical assessment Clinical manifestations
Diagnostics Manifestations of signs and symptoms Positive smear for acid-fast bacillus Confirmation of dx by sputum culture of M. tuberculosis Mantoux test (PPD) Induration of 10 mm or greater, indicative of exposure Does not mean active disease is present Interventions Combination drug therapy with strict adherence (education important) Negative sputum culture indicative of patient no longer being infectious (need results of three as negative)
Community-based Care Home care management Health teaching Health care resources
You might also like
- Nebdn National Diploma in Dental Nursing Practical Experience Record SheetDocument8 pagesNebdn National Diploma in Dental Nursing Practical Experience Record SheetCamila Walton100% (6)
- Caregiving Skill Evaluation TestDocument10 pagesCaregiving Skill Evaluation Testアビージョセフベンディホ ベロン100% (2)
- Case Study of AsthmaDocument6 pagesCase Study of Asthmabuzz Q100% (4)
- ASTHMADocument82 pagesASTHMAImmanuel100% (1)
- Mayo Clinic - Images in Internal MedicineDocument385 pagesMayo Clinic - Images in Internal Medicinemohammed97% (35)
- Bronchial AsthmaDocument34 pagesBronchial Asthmavowamik352No ratings yet
- Asthma and COPDDocument28 pagesAsthma and COPDShoaib PatelNo ratings yet
- Brochial Asthma EditedDocument40 pagesBrochial Asthma EditedMituran IshwarNo ratings yet
- AsthmaDocument8 pagesAsthmaLankeshwaraNo ratings yet
- Bronchial AsthmaDocument45 pagesBronchial Asthmamaggykariuki002No ratings yet
- Bronchial AsthmaDocument54 pagesBronchial AsthmaSehar162100% (2)
- Week 3 Obstructive DisorderDocument79 pagesWeek 3 Obstructive Disorderdelrosariojm87No ratings yet
- Asthma Diagnosis and TreatmentDocument16 pagesAsthma Diagnosis and TreatmentRabina PantaNo ratings yet
- 06 Respiratory03 Patho02Document46 pages06 Respiratory03 Patho02Divyajyoti DevaNo ratings yet
- NUR5703 Respiratory Advanced PathophysiologyDocument16 pagesNUR5703 Respiratory Advanced PathophysiologyLee MeyerNo ratings yet
- COPDDocument49 pagesCOPDArmoured SpartanNo ratings yet
- GP Reg - Asthma and Spirometry 2011Document114 pagesGP Reg - Asthma and Spirometry 2011minerva_stanciuNo ratings yet
- Pneumonia: Reporter: Cheren Cate BalogoDocument12 pagesPneumonia: Reporter: Cheren Cate BalogoCheren Cate BalogoNo ratings yet
- Nursing Care With PenumoniaDocument44 pagesNursing Care With PenumoniaFahmi SyarifNo ratings yet
- 418-M1-Cu 5 Resp. Emergencies 2Document12 pages418-M1-Cu 5 Resp. Emergencies 2Paradillo Regatuna LesterNo ratings yet
- Practice 2 - Chronic Bronchitis - AsthmaDocument22 pagesPractice 2 - Chronic Bronchitis - AsthmaVishtasb KhaliliNo ratings yet
- Copd 2022Document45 pagesCopd 2022Mubassir NisarNo ratings yet
- N24: Class #8 Obstructive and Inflammatory Lung Disease: Emphysema Chronic Bronchitis AsthmaDocument42 pagesN24: Class #8 Obstructive and Inflammatory Lung Disease: Emphysema Chronic Bronchitis Asthmadentist40No ratings yet
- COPD - Jindal Chest ClinicDocument31 pagesCOPD - Jindal Chest ClinicJindal Chest ClinicNo ratings yet
- Asthma and Cystic Fibrosis: Chinchu MDocument38 pagesAsthma and Cystic Fibrosis: Chinchu MChinchu MohanNo ratings yet
- Evaluationandtreatmentof Chroniccough: Genji Terasaki,, Douglas S. PaauwDocument13 pagesEvaluationandtreatmentof Chroniccough: Genji Terasaki,, Douglas S. PaauwRSU DUTA MULYANo ratings yet
- Bronchial Asthma in Acute Exacerbation - FinalDocument17 pagesBronchial Asthma in Acute Exacerbation - Finalmary_sulit_150% (2)
- 2010 Allergy and Immunology Board ReviewDocument132 pages2010 Allergy and Immunology Board Reviewgrahamabra50% (2)
- 2 Bronchial Asthma-2Document46 pages2 Bronchial Asthma-2mameekasim75No ratings yet
- Pedia Bronchial Asthma-1Document43 pagesPedia Bronchial Asthma-1MAHEJS HDNo ratings yet
- AsthmaDocument17 pagesAsthmaderarataye6No ratings yet
- Order ID 2001386 - Diagnostic Clinical & ReasoningDocument9 pagesOrder ID 2001386 - Diagnostic Clinical & ReasoningEdel MuneeNo ratings yet
- Bronchial Asthma in Children For StudentsDocument89 pagesBronchial Asthma in Children For StudentsRasha Al MousaNo ratings yet
- PneumoniaDocument20 pagesPneumoniaFeizalNo ratings yet
- Asthmatic Attack: Miriti M.D Masters of Clinical Medicine Accidents and Emergency Facilitator: DR Simba DR MburuguDocument26 pagesAsthmatic Attack: Miriti M.D Masters of Clinical Medicine Accidents and Emergency Facilitator: DR Simba DR MburuguDennis MiritiNo ratings yet
- Asthma: Chronic Inflammation of The Airways. The Hyper-Responsive Airways Typical of AsthmaDocument7 pagesAsthma: Chronic Inflammation of The Airways. The Hyper-Responsive Airways Typical of AsthmaRaj PaulNo ratings yet
- Pediatric Critical CareDocument3 pagesPediatric Critical CareRem AlfelorNo ratings yet
- Asma Dan Penyakit Paru Obstruktif KronisDocument34 pagesAsma Dan Penyakit Paru Obstruktif KronisAtikah ArifahNo ratings yet
- Advance Clinical Nursing Presentation - SusanDocument40 pagesAdvance Clinical Nursing Presentation - SusanAbdul Hamid Al FarsiNo ratings yet
- Bronchial Asthma - HandoutDocument3 pagesBronchial Asthma - HandoutkimerellaNo ratings yet
- Bronchial AsthmaDocument95 pagesBronchial AsthmaBrian BrownNo ratings yet
- 3.pulmonary Alterations - Part 2Document37 pages3.pulmonary Alterations - Part 2Rawan AlotaibiNo ratings yet
- Asthma: Dr. Raed ShudifatDocument36 pagesAsthma: Dr. Raed ShudifatRema WaleedNo ratings yet
- Slides. Disturbances in Oxygen Utilization 2 1Document101 pagesSlides. Disturbances in Oxygen Utilization 2 1SHARMAINE ANNE POLICIOSNo ratings yet
- Bronchial Asthma 085523Document29 pagesBronchial Asthma 085523Satrumin ShirimaNo ratings yet
- Common Health ProblemDocument36 pagesCommon Health ProblemAmanda ScarletNo ratings yet
- Interventions For Critically Ill Patients With Respiratory Problems HandoutsDocument115 pagesInterventions For Critically Ill Patients With Respiratory Problems HandoutsDemuel Dee L. BertoNo ratings yet
- AsmaDocument31 pagesAsmaseptiman zebuaNo ratings yet
- CHD AsthmaDocument20 pagesCHD AsthmaRj MagpayoNo ratings yet
- Treatment of Bronchial AsthmaDocument50 pagesTreatment of Bronchial AsthmaJindal Chest ClinicNo ratings yet
- EmphysemaDocument21 pagesEmphysemaEdmund RufinoNo ratings yet
- Vestil - Case Study On AsthmaDocument7 pagesVestil - Case Study On Asthmaninachristenevestil25No ratings yet
- Infectious and Inflammatory DisordersDocument84 pagesInfectious and Inflammatory DisordersMariel OracoyNo ratings yet
- Asthma 1Document33 pagesAsthma 1Dalitso nkhomaNo ratings yet
- Bronchial Asthma (BA) Vs Chronic Obstructive Pulmonary Disease (COPD)Document68 pagesBronchial Asthma (BA) Vs Chronic Obstructive Pulmonary Disease (COPD)Ooi Say TingNo ratings yet
- ASTMA NisreenDocument19 pagesASTMA NisreenMuhd ShafiqNo ratings yet
- Acute Lower Respiratory Tract Infection (ALRTI)Document43 pagesAcute Lower Respiratory Tract Infection (ALRTI)yosephNo ratings yet
- Prepared By: Carrie Ann S. FernandezDocument15 pagesPrepared By: Carrie Ann S. FernandezAnn FernandezNo ratings yet
- Bronchial AsthmaDocument29 pagesBronchial AsthmaDrShaheen100% (5)
- Asthama & COPDDocument84 pagesAsthama & COPDAbdullah BhattiNo ratings yet
- Asthma 1. DefinitionDocument11 pagesAsthma 1. DefinitionKarl RobleNo ratings yet
- Asthma: History and Physical Findings: Ixsy Ramirez, MD, MPH Pediatric PulmonologyDocument32 pagesAsthma: History and Physical Findings: Ixsy Ramirez, MD, MPH Pediatric Pulmonologyfurr singhNo ratings yet
- NLE: Community Health Nursing Exam 1: Text ModeDocument33 pagesNLE: Community Health Nursing Exam 1: Text ModeAngelica SorianoNo ratings yet
- Vesicovaginal Fistula RepaireDocument21 pagesVesicovaginal Fistula RepaireFlaviu Ionuț FaurNo ratings yet
- Diabetic KetoacidosisDocument10 pagesDiabetic KetoacidosisdhanasundariNo ratings yet
- HypoglycemiaDocument8 pagesHypoglycemianurizzah_885541No ratings yet
- Biofilm Related To Dental Implants8Document7 pagesBiofilm Related To Dental Implants8Isworo RukmiNo ratings yet
- Arterial Blood GasDocument55 pagesArterial Blood GasDharlyn MungcalNo ratings yet
- Pathophysiology Schistosomiasis: Table in New WindowDocument7 pagesPathophysiology Schistosomiasis: Table in New WindowKaren Leigh MagsinoNo ratings yet
- Drugs Used in Cardiac Failure (CCF)Document8 pagesDrugs Used in Cardiac Failure (CCF)Faria Islam Juhi100% (1)
- Application For LicenseDocument11 pagesApplication For LicenseSadaf RizwanhumayoonNo ratings yet
- Sgop CPG 2008 FinalDocument105 pagesSgop CPG 2008 FinalVia Alip100% (2)
- Treatment of Water Using Various Filtration Techniques: Review StudyDocument8 pagesTreatment of Water Using Various Filtration Techniques: Review StudysagarNo ratings yet
- Matriks MCU Tangguh PreEmp 28 8 18 PDFDocument1 pageMatriks MCU Tangguh PreEmp 28 8 18 PDFDont All C SNo ratings yet
- WS VDocument2 pagesWS VPrasetiyo WilliamNo ratings yet
- BERADocument19 pagesBERADr.shradhaNo ratings yet
- MannitolDocument8 pagesMannitolkristiandiorcapiliNo ratings yet
- Assessment and Management Women in PregnantDocument1 pageAssessment and Management Women in Pregnantanisah tri agustiniNo ratings yet
- Eliminate Papillomas and Warts at Home in 1 Treatment Course - PapiSTOP® PHDocument9 pagesEliminate Papillomas and Warts at Home in 1 Treatment Course - PapiSTOP® PHkiratuz1998No ratings yet
- PDF DocumentDocument40 pagesPDF DocumentBambie's recipe negosyo ideasNo ratings yet
- EBOOK Modern Nutrition in Health and Disease Modern Nutrition in Health Disease Shils 11Th Edition Ebook PDF Download Full Chapter PDF KindleDocument62 pagesEBOOK Modern Nutrition in Health and Disease Modern Nutrition in Health Disease Shils 11Th Edition Ebook PDF Download Full Chapter PDF Kindlecarla.robbins451100% (45)
- Chapter 21 Male ReproDocument34 pagesChapter 21 Male ReproIsfahan MasulotNo ratings yet
- ACE Inhibitors Vs ARBs Is One Class Better For HeaDocument7 pagesACE Inhibitors Vs ARBs Is One Class Better For HeaZul Qodri GintingNo ratings yet
- UrinalysisDocument10 pagesUrinalysisElvan Dwi WidyadiNo ratings yet
- 2019 Developmentofthe PMGQand Prevalenceof Mobile Gaming Addiction Among Adolescentsin Taiwan Cyberpsychol Behav Soc NetwDocument8 pages2019 Developmentofthe PMGQand Prevalenceof Mobile Gaming Addiction Among Adolescentsin Taiwan Cyberpsychol Behav Soc NetwJr BagaporoNo ratings yet
- Module 2 Handout CO2 Adverse Health Effects Fact SheetDocument1 pageModule 2 Handout CO2 Adverse Health Effects Fact Sheetdennis ovichNo ratings yet
- Pharma MneomicsDocument30 pagesPharma MneomicselanthamizhmaranNo ratings yet
- Trima-Accel Ver7Document8 pagesTrima-Accel Ver7Anil Kumar kakaraparthiNo ratings yet
- D G Model Making Sense of Clinical Examination of The Adult Patient Hands-On GuideDocument313 pagesD G Model Making Sense of Clinical Examination of The Adult Patient Hands-On GuidevaidyamNo ratings yet