Professional Documents
Culture Documents
Venipuncture: From Wikipedia, The Free Encyclopedia
Venipuncture: From Wikipedia, The Free Encyclopedia
Uploaded by
ishinaki28Original Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Venipuncture: From Wikipedia, The Free Encyclopedia
Venipuncture: From Wikipedia, The Free Encyclopedia
Uploaded by
ishinaki28Copyright:
Available Formats
Venipuncture
From Wikipedia, the free encyclopedia
Jump to: navigation, search This article needs additional citations for verification. Please help improve this article by adding citations to reliable sources. Unsourced material may be challenged and removed. (October 2007)
Venipuncture using the BD Vacutainer system. This picture shows a multiple-use BD Vacutainer device that is no longer used. It has been replaced by a single use BD Vacutainer device. In medicine, venipuncture, venopuncture or venepuncture is the process of obtaining intravenous access for the purpose of intravenous therapy or for blood sampling of venous blood. This procedure is performed by medical laboratory scientists, medical practitioners, some EMTs, paramedics, phlebotomists, dialysis technicians and other nursing staff. In veterinary medicine, the procedure is performed by veterinarians and veterinary technicians. Venipuncture is one of the most routinely performed invasive procedures and is carried out for any of five reasons: 1) to obtain blood for diagnostic purposes; 2)to monitor levels of blood components (Lavery & Ingram 2005); 3) to administer therapeutic treatments including medications, nutrition or chemotherapy; 4) to remove blood due to excess levels of iron or erythrocytes (red blood cells); 5) to collect blood for later use in patients requiring transfusions. Blood analysis is one of the most important diagnostic tools available to clinicians within healthcare. Its data is relied upon in the clinical setting for interpretation of a myriad of clinical signs and symptoms and developing skills in venepuncture can facilitate holistic and timely treatment. Blood is most commonly obtained from the median cubital vein, which lies within the cubital fossa anterior to the elbow. This vein lies close to the surface of the skin, and there is not a large nerve supply. Minute quantities of blood may be taken by fingersticks sampling and collected from infants by means of a heel stick or from scalp veins with a winged infusion needle. Phlebotomy (incision into a vein) is also the treatment of certain diseases such as hemochromatosis and primary and secondary polycythemia.
Contents
[hide]
1 Equipment o 1.1 Additives and order of draw
o 1.2 Venipuncture with evacuated or vacuum tubes 2 Venipuncture in children o 2.1 Venipuncture with needle and syringe 3 Blood cultures 4 Taking blood samples from animals 5 Blood alcohol tests 6 See also 7 References 8 External links
[edit] Equipment
There are many ways in which blood can be drawn from a vein. The best method varies with the age of the patient, equipment available and tests required. Most blood collection in the US and UK is done with an evacuated tube system, (two common systems are Vacutainer (Becton, Dickinson and company) and Vacuette (Greiner Bio-One GmBH). The equipment consisting of a plastic hub, a hypodermic needle, and a vacuum tube. Under certain circumstances, a syringe may be used, often with a butterfly needle, which is a plastic catheter attached to a short needle. In the developing world, a needle and syringe are still the most common method of drawing blood.
[edit] Additives and order of draw
The tubes in which blood is transported back to the laboratory contain a variety of additives or none at all. It is important to know which tube the individual laboratory requires for which test as reagents vary between laboratories and may be affected by different additives. In general whole blood needs to be mixed with EDTA which chelates calcium to prevent it clotting, unless the clotting time is the test to be measured in which citrates are used. The majority of biochemistry tests are performed on serum and so either a plain tube or a clotting accelerator is used. This clotting accelerator can interfere with some assays and so a plain tube is recommended in these cases but will obviously delay the result. Some assays may also require whole blood but are interfered with by EDTA and in this case Lithium Heparin is an alternative. With the vacuum tube system, the needle pierces the top of the sample tube and will potentially come into contact with the additives in the tube. As it is a hollow needle some of this can be carried into the next tube and contaminate it. The most likely additive to cause trouble is EDTA which will affect the coagulation time assays and by chelating some of the metal ions may interfere with some of the biochemistry results(especially potassium). Thus EDTA samples should be drawn last in most cases and plain tubes drawn first.
[edit] Venipuncture with evacuated or vacuum tubes
Vacuum tubes were first marketed by U.S. company BD (Becton, Dickinson and Company) under the trade name Vacutainer tubes. Today, many companies sell vacuum tubes as the patent for this device is in the public domain. Some models are a type of test tube that contains a vacuum that automatically aspirates blood into itself. The tubes are made of glass or plastic. The tubes are attached to a needle and hub. Multiple vacuum tubes can be attached to and removed in turn from a single needle, allowing multiple samples to be obtained from a single procedure. This is possible due to a Japanese invention called the multiple sample sleeve, which is basically a plastic cap fitting over the posterior end of the needle cannula, thus keeping blood from draining onto both health care worker and patient. BD used this invention to create a system that included the vacuum pressurized sleeve, and a cannula with sleeve attached to a holder that holds the needle/sleeve combination, and guides the negatively pressured collection vial that is inserted once the needle is in the patient. Unfortunately, the sleeve that stops blood from moving until its seal is perforated by the collection tube's insertion, also prevents flashback, the tell-tale sign the vein has been entered properly. If the phlebotomist chooses to use a butterfly needle, the "flash" is still present, and easily visible to the phlebotomy tech as well as the patient. They are commonly used in US, UK, and Australian hospitals, private doctors' offices and community labs, and are available in various sizes to suit the age of the patient and the type of sample needed. There are several sized needles for a phlebotomist to choose from. The most commonly used are as follows: a 21g (green top) needle, a 22g (black top) needle, a 21g (green label) butterfly needle, a 23g (blue label) butterfly needle, and a 25g (orange label) butterfly needle (however this needle is only used in pediatrics or extreme cases as it is so small that it can often result in hemolizing the blood sample, thereby invalidating the test). Most lay people are under the impression that using a butterfly needle is easier on their veins and less painful. Using a finer needle is less painful. However, the hazard of using butterfly needles lies in the fact that as the blood flows through the rubber tubing, it cools significantly, thereby clotting faster. In clotting in the tube, it stops up and reduces or as in most cases, completely stops. When this happens, it is necessary to re-stick a patient in order to obtain the blood sample. This is not the case when using the more common needles. Since the tubing is not a part of the needle, the blood goes through the needle directly into the tube. This method results in a faster, cleaner sample with less chance of haemolysis. (When a blood sample is hemolyzed, it means the red cells have ruptured to the extent that they impart a pink/red color to the blood plasma, which is normally pale yellow.)[1]
[edit] Venipuncture in children
Use of Lidocaine Iontophoresis is an effective method for reducing pain and alleviating distress during venipuncture in pediatric patients. Rapid dermal anesthesia can be achieved by local anesthetic infiltration, but it may evoke anxiety in children frightened by needles or distort the skin, making vascular access more difficult and increasing the risk of needle exposure to health
care workers. Dermal anesthesia can also be achieved without needles by the topical application of local anesthetics (e.g., EMLA, ASTRA Pharmaceutical, Sodertalje, Sweden) or by lidocaine iontophoresis. By contrast, noninvasive dermal anesthesia can be established in 515 min without distorting underlying tissues by lidocaine iontophoresis, where a direct electrical current facilitates dermal penetration of positively charged lidocaine molecules when placed under the positive electrode. One study did conclude that the iontophoretic administration of lidocaine was safe and effective in providing dermal anesthesia for venipuncture in children 617 years old. This technique may not be applicable to all children. Future studies may provide information on the minimum effective iontophoretic dose for dermal anesthesia in children and the comparison of the anesthetic efficacy and satisfaction of lidocaine iontophoresis with topical anesthetic creams and subcutaneous infiltration.[2]
[edit] Venipuncture with needle and syringe
Some health care workers prefer to use a syringe-needle technique for Venipuncture. Sarstedt manufactures a blood-drawing system S-Monovette that uses this principle. This method can be preferred on elderly patients, oncology patients, severely burned patients, obese patients or patients with unreliable or fragile veins. Because syringes are manually operated, the amount of suction applied may be easily controlled. This is particularly helpful with patients that have small veins that collapse under the suction of an evacuated tube. In children or other circumstances where the quantity of blood gained may be limited it can be helpful to know how much blood can be obtained before distributing it amongst the various additives that the laboratory will require.
[edit] Blood cultures
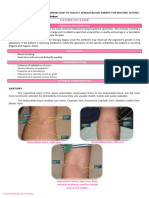
There are times where a patient may require a blood culture collection. The culture will determine if the patient has pathogens in the blood. Normally blood is sterile. When drawing blood from cultures using a sterile solution such as Betadine rather than alcohol. Using sterile gloves, do not wipe away the surgical solution, touch the puncture site, or in any way compromise the sterile process. It is vital that the procedure is performed in as sterile a manner as possible as the persistent presence of skin commensals in blood cultures could indicate endocarditis but they are most often found as contaminants. It is encouraged to use an abrasive method of skin preparation. This removes the upper layers of dead skin cells along with their contaminating bacteria. Povidone-iodine has traditionally been used but in the UK a 2% chlorhexidine in 70% ethanol or isopropyl alcohol solution is preferred and time must be allowed for it to dry. The tops of any containers used when drawing a blood culture should also be disinfected using a similar solution. Some labs will actively discourage iodine use where iodine is thought to degrade the rubber stopper through which blood enters the bottle, thus allowing contaminates to enter the container. The blood is collected into special transport bottles, which are like vacuum tubs but shaped differently. The blood culture bottle contains transport media to preserve any microorganisms
present while they are being transported to the laboratory for cultures. Because it is unknown whether the pathogens are anaerobic (living without oxygen) or aerobic (living with oxygen), blood is collected to test for both. The aerobic bottle is filled first, and then the anaerobic bottle is filled. However if the collection is performed using a syringe, the anaerobic bottle is filled first. If a butterfly collection kit is used, the aerobic bottle is filled first, so that any air in the tubing is released into the oxygen-containing bottle. Specially designed blood culture collection bottles eliminate the need for either the syringe or butterfly collection method. These specially designed bottles have long necks that fit into the evacuated tubes holders that are use for regular Venipuncture collection. These bottles also allow for collection of other blood specimens via evacuated tubes, to be collected without additional Venipuncture. The amount of blood that is collected is critical for the optimal recovery of microorganisms. Up to 10mL of blood is typical, but can vary according to the recommends of the manufacturer of the collection bottle. Collection from infants and children are 1 to 5 mL. If too little blood is collected, the ratio of blood to-nutrient broth will inhibit the growth of microorganisms. If too much blood is collected from the patient, the patient risks a hospital-induced anemia and the ratio of blood-to-nutrient broth will tilt in the opposite direction, which also is not conductive to optimal growth. The bottles are then incubated in specialized units for 24 hours before a lab technician studies and/or tests it. This step allows the very small numbers of bacteria (potentially 1 or 2 organisms) to multiply to a level which is sufficient for identification +/-antibiotic resistance testing. Modern blood culture bottles have an indicator in the base which changes color in the presence of bacterial growth and can be read automatically by machine. (For this reason the barcoded stickers found on these bottles should not be removed as they are used by the laboratorys automated systems.)
You might also like
- Phlebotomy NotesDocument2 pagesPhlebotomy NotesterenceMT89% (9)
- Quantitative Exam Sample For NMATDocument2 pagesQuantitative Exam Sample For NMATJenica YambsNo ratings yet
- Guided Wave System ComparisonDocument3 pagesGuided Wave System ComparisonsenthilndtNo ratings yet
- Exercise 2: Venipuncture Using Vacuum Collection System: ObjectivesDocument28 pagesExercise 2: Venipuncture Using Vacuum Collection System: ObjectivesFrieda CayabyabNo ratings yet
- HemodialysisDocument4 pagesHemodialysisQueen Factor VedraNo ratings yet
- Literature Review Intravenous TherapyDocument5 pagesLiterature Review Intravenous Therapygazqaacnd100% (1)
- Surgical Bed Side ProceduressDocument62 pagesSurgical Bed Side Proceduressdrhiwaomer100% (1)
- PMLS 1 Lab Activity 10Document21 pagesPMLS 1 Lab Activity 10Jey TeeNo ratings yet
- Unit - 4 Clinical Lab TechnologyDocument36 pagesUnit - 4 Clinical Lab Technologyyaswanthkalyan20No ratings yet
- Exercise 2: Venipuncture Using Vacuum Blood COLLECTION SYSTEM Skills 30 PointsDocument16 pagesExercise 2: Venipuncture Using Vacuum Blood COLLECTION SYSTEM Skills 30 PointsRue Wan UyNo ratings yet
- VCVBS - Transes SkillsDocument7 pagesVCVBS - Transes Skillsmaaisley.yebanNo ratings yet
- Catheterization of The Urinary Bladder (Foley Catheterization)Document8 pagesCatheterization of The Urinary Bladder (Foley Catheterization)Ilie DanielaNo ratings yet
- Phlebotomy Research Paper TopicsDocument4 pagesPhlebotomy Research Paper Topicsc9rbzcr0100% (1)
- Hemodialysis Shunt, Graft, and Fistula CareDocument11 pagesHemodialysis Shunt, Graft, and Fistula CareArjon Clint Reyes SulapasNo ratings yet
- Acesso Vascular EmergenciaDocument9 pagesAcesso Vascular EmergenciaSílvia TrindadeNo ratings yet
- DialysisDocument20 pagesDialysisSiwani rai100% (1)
- Module 5 ReviewerDocument8 pagesModule 5 ReviewerAnne Gabrielle EspadaNo ratings yet
- HEMODIALYSISDocument7 pagesHEMODIALYSISClarisse ReyesNo ratings yet
- IV TherapyDocument15 pagesIV Therapyprincessmonique_208609100% (2)
- Intravenous Therapy or IV TherapyDocument6 pagesIntravenous Therapy or IV TherapyMatt Razal TabliganNo ratings yet
- PG Lab 2 VenipunctureDocument26 pagesPG Lab 2 VenipunctureFlordabee Mercurio PaniaguaNo ratings yet
- NCCT Phlebotomy Answer KeyDocument122 pagesNCCT Phlebotomy Answer KeyArturo ColinNo ratings yet
- Case Study 2Document3 pagesCase Study 2Thesa Ray PadernalNo ratings yet
- Intravenous Therapy: Navigation Search List of ReferencesDocument12 pagesIntravenous Therapy: Navigation Search List of ReferencesPersia Kaye FabillarNo ratings yet
- HemodialysisDocument11 pagesHemodialysisjuan_sioNo ratings yet
- ACAreerSummer Fall2017Document4 pagesACAreerSummer Fall2017jelenaNo ratings yet
- Abdominal Paracentesis AnpDocument14 pagesAbdominal Paracentesis Anpesther100% (1)
- Complications of Ovariohysterectomy and Orchiectomy in Companion AnimalsDocument17 pagesComplications of Ovariohysterectomy and Orchiectomy in Companion AnimalsCarolina Soler GómezNo ratings yet
- Percutaneous Nephrostomy: Last Updated: January 3, 2003Document5 pagesPercutaneous Nephrostomy: Last Updated: January 3, 2003Alicia EncinasNo ratings yet
- The Blood Sampling: by Group 4 Anwar Mohungo Aziz Kurniawan Redo DalpaDocument10 pagesThe Blood Sampling: by Group 4 Anwar Mohungo Aziz Kurniawan Redo DalpaAnwar FauzyNo ratings yet
- IVTDocument34 pagesIVTWarrenPeaceNo ratings yet
- Procedure-Central Venous Access Catheter InsertionDocument18 pagesProcedure-Central Venous Access Catheter Insertionmohamad dildarNo ratings yet
- Ventriculoperitoneal ShuntDocument5 pagesVentriculoperitoneal ShunttameemNo ratings yet
- Complications of Autogenous Arteriovenous Fistulas: February 2013Document15 pagesComplications of Autogenous Arteriovenous Fistulas: February 2013Tran Quyet TienNo ratings yet
- HemodialysisDocument7 pagesHemodialysisRandyNo ratings yet
- Capillary Blood Sampling National RecommDocument24 pagesCapillary Blood Sampling National RecommadrianaNo ratings yet
- Lenicek Krleza J Et Al Capillary Blood Sampling PDFDocument24 pagesLenicek Krleza J Et Al Capillary Blood Sampling PDFsinta purnama sariNo ratings yet
- Clinical Teaching On HaemodialysisDocument7 pagesClinical Teaching On HaemodialysisAnusha AkhilNo ratings yet
- Avoiding Common Errors in The Emergency Department-1281-1540Document260 pagesAvoiding Common Errors in The Emergency Department-1281-1540Hernando CastrillónNo ratings yet
- Guidelines On The Insertion and Management of CentralDocument18 pagesGuidelines On The Insertion and Management of CentralAgustina ItinNo ratings yet
- Blood Collection LectureDocument13 pagesBlood Collection LectureKatrina Cruz YambaoNo ratings yet
- Clinical Teaching On HaemodialysisDocument7 pagesClinical Teaching On HaemodialysisAnusha AkhilNo ratings yet
- Wound Drain FinalDocument16 pagesWound Drain Finaljosephnoon1100% (1)
- Iv TherapyDocument12 pagesIv TherapykatrinajoyjNo ratings yet
- CATHETERIZATIONDocument18 pagesCATHETERIZATIONZechariah NicholasNo ratings yet
- Venipuncture: Rajesh Mohess, CLTDocument32 pagesVenipuncture: Rajesh Mohess, CLTPuskesmas Sambirejo BanyuwangiNo ratings yet
- Urine CytologyDocument15 pagesUrine CytologyNaruto ShikamaruNo ratings yet
- Umbilical Vascular Catheterization: Videos in Clinical MedicineDocument3 pagesUmbilical Vascular Catheterization: Videos in Clinical MedicineStephanie RomeroNo ratings yet
- Cheek BleedingDocument5 pagesCheek BleedingRobbie WilliamsNo ratings yet
- Procedure AssignmentDocument12 pagesProcedure AssignmentMubarek UmerNo ratings yet
- Term Paper On Artificial Heart ValveDocument5 pagesTerm Paper On Artificial Heart Valvebeemwvrfg100% (1)
- Avian Blood Collection and Hematology - WSAVA 2015 Congress - VINDocument4 pagesAvian Blood Collection and Hematology - WSAVA 2015 Congress - VINMustafa AL-AsadsyNo ratings yet
- Sister Nivedita Govt. Nursing College Igmc, ShimlaDocument10 pagesSister Nivedita Govt. Nursing College Igmc, ShimlashivaniNo ratings yet
- LP QuizDocument8 pagesLP QuizsurainepNo ratings yet
- HemodialysisDocument123 pagesHemodialysismonabertNo ratings yet
- Urinary CatheterisationDocument26 pagesUrinary Catheterisationmadalina popaNo ratings yet
- Hemodialysis FinalDocument40 pagesHemodialysis Finalrose FolwersNo ratings yet
- 1 PBDocument4 pages1 PBrashmiNo ratings yet
- Percutaneous Surgery of the Upper Urinary Tract: Handbook of EndourologyFrom EverandPercutaneous Surgery of the Upper Urinary Tract: Handbook of EndourologyPetrisor Aurelian GeavleteRating: 5 out of 5 stars5/5 (1)
- Arteriovenous Access Surgery: Ensuring Adequate Vascular Access for HemodialysisFrom EverandArteriovenous Access Surgery: Ensuring Adequate Vascular Access for HemodialysisNo ratings yet
- CHALLENGES IN IMPLEMENTING A NEW SIGNALLING SYSTEM TO REPLACE AN EXISTING SIGNALLING SYSTEM WHILE MAINTAINING NORMAL TRAIN SERVICE-good ReferenceDocument47 pagesCHALLENGES IN IMPLEMENTING A NEW SIGNALLING SYSTEM TO REPLACE AN EXISTING SIGNALLING SYSTEM WHILE MAINTAINING NORMAL TRAIN SERVICE-good ReferencePulin ChaudhariNo ratings yet
- 8816 User Manual Iss6 5Document40 pages8816 User Manual Iss6 5Richard Ritchie MettensNo ratings yet
- Vendor Directory ICF - 2019-20 - Regular PDFDocument108 pagesVendor Directory ICF - 2019-20 - Regular PDFpadmanaban100% (1)
- Sample For Official Solution Manual Dynamics (8th Edition) by Meriam & KraigeDocument26 pagesSample For Official Solution Manual Dynamics (8th Edition) by Meriam & Kraigeomar burakNo ratings yet
- Bridge Axi AhbDocument22 pagesBridge Axi Ahbkrishnaav100% (1)
- Deep Learning: Huawei AI Academy Training MaterialsDocument47 pagesDeep Learning: Huawei AI Academy Training Materialsfadhil muhammad hanafiNo ratings yet
- Object-Oriented Programming, C++ and Power System SimulationDocument10 pagesObject-Oriented Programming, C++ and Power System SimulationjasonkinNo ratings yet
- Maintenance Kit (HB 4200-4200DP) SealsDocument4 pagesMaintenance Kit (HB 4200-4200DP) SealsdrmassterNo ratings yet
- BS 873-7 - 1984 Road Traffic Signs and Internally Illuminated Bollards Specification For Posts and FittingsDocument16 pagesBS 873-7 - 1984 Road Traffic Signs and Internally Illuminated Bollards Specification For Posts and Fittingspaul reyesNo ratings yet
- Nisarg CSCDocument34 pagesNisarg CSCNarendra MehtaNo ratings yet
- SLG Chem2 LG 4.9 BuffersDocument6 pagesSLG Chem2 LG 4.9 BuffersIman SontousidadNo ratings yet
- 7 Principles of An EagleDocument2 pages7 Principles of An EagleDhruti BotadraNo ratings yet
- Sankarabharanamu 2 PDFDocument7 pagesSankarabharanamu 2 PDFAdiNav PabKasNo ratings yet
- Science 3 1ST Monthly ExaminationDocument5 pagesScience 3 1ST Monthly ExaminationCarina BarandinoNo ratings yet
- Supplement Guide Healthy AgingDocument63 pagesSupplement Guide Healthy AgingJeff BanksNo ratings yet
- RAC FinalDocument15 pagesRAC FinalAbhishek AnandNo ratings yet
- DSTV PDFDocument4 pagesDSTV PDFEddy TangaNo ratings yet
- Rzasg-M2 (7) v1b Databook Eeden17 New DaikinDocument37 pagesRzasg-M2 (7) v1b Databook Eeden17 New DaikinTheEngineer - المهندسNo ratings yet
- Development of A Topical Gel Containing A Dipeptidyl Peptidase-4 Inhibitor For Wound Healing ApplicationsDocument15 pagesDevelopment of A Topical Gel Containing A Dipeptidyl Peptidase-4 Inhibitor For Wound Healing ApplicationsGlobal Research and Development ServicesNo ratings yet
- FF1. Unit 2, ToysDocument37 pagesFF1. Unit 2, ToysBội LaiNo ratings yet
- Schrack Accessories Industrial Power Relay RT: General Purpose RelaysDocument6 pagesSchrack Accessories Industrial Power Relay RT: General Purpose RelaysUlfran MedinaNo ratings yet
- Uk Erik Common Rail Nozzle Catalogue 2014 PDFDocument13 pagesUk Erik Common Rail Nozzle Catalogue 2014 PDFjeferson de castro souzaNo ratings yet
- Assessment and Transportation Risk-1Document7 pagesAssessment and Transportation Risk-1TanzeemNo ratings yet
- 4MA1 2HR Que 20220118Document32 pages4MA1 2HR Que 20220118Bruce RussellNo ratings yet
- Pioneer WoodlandsDocument38 pagesPioneer Woodlandsapi-249262419No ratings yet
- TM25RDocument2 pagesTM25Rphong nguyễn bá0% (1)
- Gacun SMPS Design TipsDocument19 pagesGacun SMPS Design TipsGerson PenalosaNo ratings yet
- Série 400 PDFDocument526 pagesSérie 400 PDFLeonardo OliveiraNo ratings yet