Professional Documents
Culture Documents
Git Phy
Git Phy
Uploaded by
Ketan PatelOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Git Phy
Git Phy
Uploaded by
Ketan PatelCopyright:
Available Formats
Chapter 18
The Digestive System
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Functions of the GI Tract
Motility:
Movement of of food through the GI tract.
Ingestion:
Taking food into the mouth. Chewing the food and mixing it with saliva. Swallowing the food. Rhythmic wave-like contractions that move food through GI tract.
Mastication:
Deglutition:
Peristalsis:
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Functions of the GI Tract
(continued)
Secretion:
Includes both exocrine and endocrine secretions.
Exocrine:
HCl, H20, HC03-, bile, lipase, pepsin, amylase, trypsin, elastase, and histamine are secreted into the lumen of the GI tract. Stomach and small intestine secrete hormones to help regulate the GI system.
Endocrine:
Gastrin, secretin, CCK, GIP, GLP-1, guanylin, VIP, and somatostatin.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Functions of the GI Tract
(continued)
Digestion:
Breakdown of food particles into subunits (chemical structure change). Process of the passage of digestion (chemical subunits) into the blood or lymph. Temporary storage and elimination of indigestible food.
Absorption:
Storage and elimination:
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
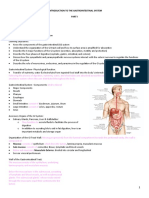
Digestive System (GI)
GI tract divided into:
Insert fig. 18.2
Alimentary canal. Accessory digestive organs.
GI tract is 30 ft long and extends from mouth to anus.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Layers of GI Tract
Composed of 4 tunics:
Mucosa. Submucosa.
Muscularis. Serosa.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Mucosa
Lines the lumen of GI tract.
Consists of simple columnar epithelium. Thin layer of connective tissue containing lymph nodules. Thin layer of smooth muscle responsible for the folds.
Lamina propria:
Muscularis mucosae:
Folds increase surface area for absorption.
Goblet cells:
Secrete mucus.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Submucosa
Thick, highly vascular layer of connective tissue. Absorbed molecules enter the blood and lymphatic vessels. Submucosal plexus (Meissners plexus):
Provide autonomic nerve supply to the muscularis mucosae.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Muscularis
Responsible for segmental contractions and peristaltic movement through the GI tract.
Inner circular layer of smooth muscle. Outer longitudinal layer of smooth muscle.
Contractions of these layers move food through the tract; pulverize and mix the food. Myenteric plexus located between the 2 muscle layers. Major nerve supply to GI tract.
Fibers and ganglia from both sympathetic and parasympathetic nervous systems.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Serosa
Binding and protective outer layer. Consists of areolar connective tissue covered with simple squamous epithelium.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Regulation of the GI Tract
Extrinsic innervation: Parasympathetic nervous system:
Vagus and spinal nerves: Stimulate motility and GI secretions. Postganglionic sympathetic fibers that pass through submucosal and myenteric plexuses and innervate GI tract: Reduce peristalsis and secretory activity.
Sympathetic nervous system:
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Regulation of the GI Tract
(continued)
Enteric nervous system:
Sites where parasympathetic fibers synapse with postganglionic neurons that innervate smooth muscle. Local regulation of the GI tract. Molecules acting locally. Secreted by the mucosa.
Submucosal and myenteric plexuses:
Paracrine secretion:
Hormonal secretion:
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
From Mouth to Stomach
Mastication (chewing):
Mixes food with saliva which contains salivary amylase.
Enzyme that can catalyze the partial digestion of starch.
Deglutition (swallowing):
Begins as a voluntary activity. Involves 3 phases:
Oral phase is voluntary. Pharyngeal and esophageal phases are involuntary.
Cannot be stopped.
Larynx is raised. Epiglottis covers the entrance to respiratory tract.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
From Mouth to Stomach
(continued)
Involuntary muscular contractions and relaxations in the mouth, pharynx, larynx, and esophagus are coordinated by the swallowing center in the medulla. Esophagus:
Connects pharynx to the stomach.
Upper third contains skeletal muscle. Middle third contains a mixture of skeletal and smooth muscle. Terminal portion contains only smooth muscle.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Esophagus
Peristalsis:
Produced by a series of localized reflexes in response to distention of wall by bolus.
Insert 18.4a
Wave-like muscular contractions:
Circular smooth muscle contract behind, relaxes in front of the bolus. Followed by longitudinal contraction (shortening) of smooth muscle.
Rate of 2-4 cm/sec.
After food passes into stomach, LES constricts.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Stomach
Most distensible part of GI tract.
Empties into the duodenum.
Functions of the stomach: Stores food. Initiates digestion of proteins. Kills bacteria. Moves food (chyme) into intestine.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Stomach
(continued)
Contractions of the stomach churn chyme.
Insert fig. 18.5
Mix chyme with gastric secretions. Push food into intestine.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Stomach
(continued)
Gastric mucosa has gastric pits in the folds. Cells that line the folds deeper in the mucosa, are gastric glands.
Insert fig. 18.7
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Gastric Glands
Secrete gastric juice:
Goblet cells: mucus. Parietal cells: HCl and intrinsic factor. Chief cells: pepsinogen. Enterochromaffin-like cells (ECL): histamine and serotonin. G cells: gastrin. D cells: somatostatin. Stomach: ghrelin.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
HCl Production
Parietal cells secrete H+ into gastric lumen by primary active transport, through H+/ K+ ATPase pump. Parietal cells basolateral membrane takes in Cl- against its electrochemical gradient, by coupling its transport with HC03-.
Insert fig. 18.8
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
HCl Production
(continued)
HCl production is stimulated:
Indirectly by gastrin. Indirectly by ACh.
ACh and gastrin stimulate release of histamine.
Histamine:
Stimulates parietal cells to secrete HCl.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
HCl Functions
Makes gastric juice very acidic.
Denatures ingested proteins (alter tertiary structure) so become more digestible.
Insert fig. 18.9
Activates pepsinogen to pepsin.
Pepsin is more active at pH of 2.0.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Digestion and Absorption in the Stomach
Proteins partially digested by pepsin. Carbohydrate digestion by salivary amylase is soon inactivated by acidity. Alcohol and aspirin are the only commonly ingested substances absorbed.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Gastric and Peptic Ulcers
Peptic ulcers:
Erosions of the mucous membranes of the stomach or duodenum produced by action of HCl.
Ulcers of the duodenum are produced by excessive gastric acid secretions. Bacterium that resides in GI tract that may produce ulcers. Histamine released by tissue damage and inflammation stimulate further acid secretion.
Zollinger-Ellison syndrome:
Helicobacter pylori:
Acute gastritis:
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Protective Mechanisms of Stomach
Parietal and chief cells impermeable to HCl. Alkaline mucus contains HC03-. Tight junctions between adjacent epithelial cells. Rapid rate of cell division (entire epithelium replaced in 3 days). Prostaglandins inhibit gastric secretions.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Small Intestine
Each villus is a fold in the mucosa. Covered with columnar epithelial cells interspersed with goblet cells. Epithelial cells at the tips of villi are exfoliated and replaced by mitosis in crypt of Lieberkuhn. Lamina propria contain lymphocytes, capillaries, and central lacteal.
Insert fig. 18.12
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Absorption in Small Intestine
Duodenum and jejunum:
Carbohydrates, amino acids, lipids, iron, and Ca2+. Bile salts, vitamin B12, electrolytes, and H20.
Ileum:
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Intestinal Enzymes
Microvilli contain brush border enzymes that are not secreted into the lumen.
Brush border enzymes remain attached to the cell membrane with their active sites exposed to the chyme.
Absorption requires both brush border enzymes and pancreatic enzymes.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Intestinal Contractions and Motility
2 major types of contractions occur in the small intestine:
Insert fig. 18.14
Peristalsis:
Slow movement. Pressure at the pyloric end of small intestine is greater than at the distal end.
Segmentation:
Major contractile activity of the small intestine. Contraction of circular smooth muscle.
Mix chyme.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Contractions of Intestinal Smooth Muscles
Occur automatically in response to endogenous pacemaker activity. Rhythm of contractions is paced by graded depolarizations called slow waves.
Insert fig. 18.15
Slow waves produced by interstitial cells of Cajal. Slow waves spread from 1 smooth muscle cell to another through nexuses.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Contractions of Intestinal Smooth Muscles
When slow waves above threshold, it triggers APs by opening of VG Ca2+ channels. Inward flow of Ca2+:
Produces the upward depolarization phase. Stimulates contraction of smooth muscle. VG K+ channels open.
Repolarization:
Slow waves decrease in amplitude as they are conducted.
May stimulate contraction in proportion to the magnitude of depolarization.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Cells and Electrical Events in the Muscularis
Insert fig. 18.16
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Large Intestine
Outer surface bulges outward to form haustra. Little absorptive function.
Absorbs H20, electrolytes, several vitamin B complexes, vitamin K, and folic acid.
Intestinal microbiota produce significant amounts of folic acid and vitamin K. Bacteria ferment indigestible molecules to produce short-chain fatty acids.
Does not contain villi.
Secretes H20, via active transport of NaCl into intestinal lumen.
Guanylin stimulates secretion of Cl- and H20, and inhibits absorption of Na+ (minor pathway).
Membrane contains Na+/K+ pumps.
Minor pathway.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Fluid and Electrolyte Absorption in the Intestine
Small intestine:
Most of the fluid and electrolytes are absorbed by small intestine.
Absorbs about 90% of the remaining volume.
Absorption of H20 occurs passively as a result of the osmotic gradient created by active transport.
Aldosterone stimulates NaCl and H20 absorption in the ileum.
Large intestine:
Absorbs about 90% of the remaining volume.
Absorption of H20 occurs passively as a result of the osmotic gradient created by active transport of Na+ and Cl-.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Defecation
Waste material passes to the rectum. Occurs when rectal pressure rises and external anal sphincter relaxes. Defecation reflex:
Longitudinal rectal muscles contract to increase rectal pressure.
Relaxation of internal anal sphincter.
Excretion is aided by contractions of abdominal and pelvic skeletal muscles.
Push feces from the rectum.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Structure of Liver
Liver largest internal organ.
Hepatocytes form hepatic plates that are 12 cells thick. Arranged into functional units called lobules. More permeable than other capillaries.
Plates separated by sinusoids.
Contains phagocytic Kupffer cells. Secretes bile into bile canaliculi, which are drained by bile ducts.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Structure of Liver
(continued)
Insert fig. 18.20
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Hepatic Portal System
Products of digestion that are absorbed are delivered to the liver. Capillaries drain into the hepatic portal vein, which carries blood to liver.
blood is deoxygenated. Hepatic vein drains liver.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Enterohepatic Circulation
Compounds that recirculate between liver and intestine.
Many compounds can be absorbed through small intestine and enter hepatic portal blood. Variety of exogenous compounds are secreted by the liver into the bile ducts.
Insert fig. 18.22
Can excrete these compounds into the intestine with the bile.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Major Categories of Liver Function
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Bile Production and Secretion
The liver produces and secretes 2501500 ml of bile/day. Bile pigment (bilirubin) is produced in spleen, bone marrow, and liver.
Derivative of the heme groups (without iron) from hemoglobin.
Free bilirubin combines with glucuronic acid and forms conjugated bilirubin.
Secreted into bile. Urobilogen is absorbed by intestine and enters the hepatic vein.
Converted by bacteria in intestine to urobilinogen.
Recycled, or filtered by kidneys and excreted in urine.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Metabolism of Heme and Bilirubin
Insert fig. 18.23
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Bile Production and Secretion
(continued)
Bile acids are derivatives of cholesterol.
Major pathway of cholesterol breakdown in the body. Cholic acid. Chenodeoxycholic acid.
Insert fig. 18.25
Principal bile acids are:
Combine with glycine or taurine to form bile salts.
Bile salts aggregate as micelles.
95% of bile acids are absorbed by ileum.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Detoxification of the Blood
Liver can remove hormones, drugs, and other biologically active molecules from the blood by:
Excretion into the bile. Phagocytosis by Kupffer cells. Chemical alteration of the molecules.
Ammonia is produced by deamination of amino acids in the liver. Liver converts it into urea.
Excreted in urine.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Detoxification of the Blood
(continued)
Inactivation of steroid hormones and drugs.
Conjugation of steroid hormones and xenobiotics make them anionic.
Can be transported into bile by multispecific organic anion transport carriers.
Steroid and xenobiotic receptors stimulate production of cytochrome P450 enzymes.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Secretion of Glucose, Triglycerides and Ketones
Liver helps regulate blood glucose concentration by:
Glycogenesis and lipogenesis. Glycogenolysis and gluconeogenesis.
Contains enzymes required to convert free fatty acids into ketone bodies.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Production of Plasma Proteins
Albumin and most of the plasma globulins (except immunoglobulins) are produced by the liver. Albumin:
Constitutes 70% of the total plasma protein.
Contributes most to the colloid osmotic pressure in the blood.
Globulins:
Transport cholesterol and hormones. Inhibit trypsin. Produce blood clotting factors I, II, III, V, VII, IX, XI.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Gallbladder
Sac-like organ attached to the inferior surface of the liver. Stores and concentrates bile. When gallbladder fills with bile, it expands.
Contraction of the muscularis layer of the gallbladder, ejects bile into the common bile duct into duodenum.
When small intestine is empty, sphincter of Oddi closes.
Bile is forced up to the cystic duct to gallbladder.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Pancreas
Exocrine:
Acini:
Insert fig. 18.26
Secrete pancreatic juice.
Endocrine:
Islets of Langerhans:
Secrete insulin and glucagon.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Pancreatic Juice
Contains H20, HC03- and digestive enzymes.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Pancreatic Juice
Complete digestion of food requires action of both pancreatic and brush border enzymes.
Most pancreatic enzymes are produced as zymogens. Trypsin (when activated by enterokinase) triggers the activation of other pancreatic enzymes.
Fig. 18.29
Pancreatic trypsin inhibitor attaches to trypsin.
Inhibits its activity in the pancreas.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Neural and Endocrine Regulation
Neural and endocrine mechanisms modify the activity of the GI system. GI tract is both an endocrine gland, and a target for the action of hormones.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Regulation of Gastric Function
Gastric motility and secretion are automatic. Waves of contraction are initiated spontaneously by pacesetter cells. Extrinsic control of gastric function is divided into 3 phases:
Cephalic phase. Gastric phase. Intestinal phase.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Cephalic Phase
Stimulated by sight, smell, and taste of food. Activation of vagus: Stimulates chief cells to secrete pepsinogen. Directly stimulates G cells to secrete gastrin. Directly stimulates ECL cells to secrete histamine. Indirectly stimulates parietal cells to secrete HCl.
Continues into the 1st 30 min. of a meal.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Gastric Phase
Arrival of food in stomach stimulates the gastric phase. Gastric secretion stimulated by:
Distension. Chemical nature of chyme (amino acids and short polypeptides). Stimulates G cells to secrete gastrin. Stimulates chief cells to secrete pepsinogen. Stimulates ECL cells to secrete histamine. Histamine stimulates secretin of HCl. Positive feedback effect.
As more HCl and pepsinogen are secreted, more polypeptides and amino acids are released.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Gastric Phase
(continued)
Secretion of HCl is also regulated by a negative feedback effect:
Insert. Fig. 18.30
HCl secretion decreases if pH < 2.5. At pH of 1.0, gastrin secretion ceases. D cells stimulate secretion of somatostatin. Paracrine regulator to inhibit secretion of gastrin.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Intestinal Phase
Inhibits gastric activity when chyme enters the small intestine. Arrival of chyme increases osmolality and distension.
Activates sensory neurons of vagus and produces an inhibitory neural reflex:
Inhibits gastric motility and secretion. In the presence of fat, enterogasterone inhibits gastric motility and secretion.
Hormone secretion:
Inhibit gastric activity:
Somatostatin, CCK, and GLP-1.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Enteric Nervous System
Submucosal and myenteric plexuses contain 100 million neurons. Include preganglionic parasympathetic axons, ganglion cell bodies, postganglionic sympathetic axons; and afferent intrinsic and extrinsic sensory neurons.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Enteric Nervous System
(continued)
Peristalsis: ACh and substance P stimulate smooth muscle contraction above the bolus. NO, VIP, and ATP stimulate smooth muscle relaxation below the bolus.
Insert fig. 18.31
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Paracrine Regulators of the Intestine
Serotonin (5-HT):
Stimulates intrinsic afferents, which send impulses into intrinsic nervous system; and activates motor neurons. Stimulates contraction of the duodenum and stomach antrum. Activates guanylate cyclase, stimulating the production of cGMP.
Motilin:
Guanylin:
cGMP stimulates the intestinal cells to secrete Cl- and H20.
Inhibits the absorption of Na+.
Uroguanylin:
May stimulate kidneys to secrete salt in urine.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Intestinal Reflexes
Intrinsic and extrinsic regulation controlled by intrinsic and paracrine regulators. Gastroileal reflex:
Increased gastric activity causes increased motility of ileum and movement of chyme through ileocecal sphincter. Distension of ileum, decreases gastric motility. Overdistension in 1 segment, causes relaxation throughout the rest of intestine.
Ileogastric reflex:
Intestino-intestinal reflex:
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Secretion of Pancreatic Juice
Secretion of pancreatic juice and bile is stimulated by: Secretin: Occurs in response to duodenal pH < 4.5. Stimulates production of HC03 by pancreas. Stimulates the liver to secrete HC03 into the bile. CCK: Occurs in response to fat and protein content of chyme in duodenum. Stimulates the production of pancreatic enzymes. Enhances secretin. Stimulates contraction of the sphincter of Oddi.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Digestion and Absorption of Carbohydrates
Salivary amylase:
Begins starch digestion. Digests starch to oligosaccharides. Oligosaccharides hydrolyzed by brush border enzymes.
Insert fig. 18.32
Pancreatic amylase:
Glucose is transported by secondary active transport with Na+ into the capillaries.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Digestion and Absorption of Protein
Digestion begins in the stomach when pepsin digests proteins to form polypeptides. In the duodenum and jejunum:
Endopeptidases cleave peptide bonds in the interior of the polypeptide: Trypsin. Chymotrypsin. Elastase. Exopeptidases cleave peptide bonds from the ends of the polypeptide: Carboxypeptidase. Aminopeptidase.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Digestion and Absorption of Protein
(continued)
Free amino acids absorbed by cotransport with Na+. Dipeptides and tripeptides transported by secondary active transport using a H+ gradient to transport them into the cytoplasm. Hydrolyzed into free amino acids and then secreted into the blood.
Insert fig. 18.33
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Digestion and Absorption of Lipids
Arrival of lipids in the duodenum serves as a stimulus for secretion of bile. Emulsification:
Bile salt micelles are secreted into duodenum to break up fat droplets.
Pancreatic lipase and colipase hydrolyze triglycerides to free fatty acids and monglycerides.
Colipase coats the emulsification droplets and anchors the lipase enzyme to them. Form micelles and move to brush border.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Digestion and Absorption of Lipids
(continued)
Free fatty acids, monoglycerides, and lysolecithin leave micelles and enter into epithelial cells.
Resynthesize triglycerides and phospholipids within cell.
Combine with a protein to form chylomicrons.
Secreted into central lacteals.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Transport of Lipids
In blood, lipoprotein lipase hydrolyzes triglycerides to free fatty acids and glycerol for use in cells. Remnants containing cholesterol are taken to the liver.
Form VLDLs which take triglycerides to cells. Once triglycerides are removed, VLDLs are converted to LDLs.
LDLs transport cholesterol to organs and blood vessels.
HDLs transport excess cholesterol back to liver.
Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display.
Absorption of Fat
Insert fig. 18.36
You might also like
- Anatomy and Physiology of Typhoid FeverDocument5 pagesAnatomy and Physiology of Typhoid FeverCharise Ligores67% (6)
- Gastrointestinal Anatomy and Physiology: The EssentialsFrom EverandGastrointestinal Anatomy and Physiology: The EssentialsJohn F. ReinusNo ratings yet
- Anatomy and Physiology DigestiveDocument7 pagesAnatomy and Physiology DigestiveFretzgine Lou ManuelNo ratings yet
- Physiology, Gastrointestinal Article - StatPearls PDFDocument5 pagesPhysiology, Gastrointestinal Article - StatPearls PDFThanh TrúcNo ratings yet
- Digestive System (Unit X)Document44 pagesDigestive System (Unit X)zahraNo ratings yet
- GIT 2020 MBCHBWeek SendDocument344 pagesGIT 2020 MBCHBWeek SendTino MapurisaNo ratings yet
- Digestive/Endocrine Answer KeyDocument10 pagesDigestive/Endocrine Answer KeykmulqsNo ratings yet
- The Endocrine Pancreas: Regulation of Carbohydrate MetabolismDocument61 pagesThe Endocrine Pancreas: Regulation of Carbohydrate MetabolismNona AsolaNo ratings yet
- Human Digestive System - Grade 11 & 12Document23 pagesHuman Digestive System - Grade 11 & 12Ishita SinghNo ratings yet
- Case Presentation (NCM 102)Document26 pagesCase Presentation (NCM 102)Ibs LimNo ratings yet
- Human Phyiology: The Digestive SystemDocument72 pagesHuman Phyiology: The Digestive SystemAnas Al DaragmehNo ratings yet
- Physiology of GIT NursingDocument87 pagesPhysiology of GIT NursingraphatoelNo ratings yet
- The Anatomy of The StomachDocument33 pagesThe Anatomy of The StomachVictor OmoloNo ratings yet
- Chapter 2 Gastrointestinal SystemDocument11 pagesChapter 2 Gastrointestinal SystemPersonne AnonymeNo ratings yet
- All About GIT PhysiologyDocument79 pagesAll About GIT PhysiologyHarshavardhan AmancherlaNo ratings yet
- Analisis de Heces CompletoDocument10 pagesAnalisis de Heces CompletoIvonne SVNo ratings yet
- Digestive System Best NoteDocument45 pagesDigestive System Best NoteVarsha Mol MohananNo ratings yet
- Basic Nutrition Chapt 1 2022Document59 pagesBasic Nutrition Chapt 1 2022a.joshuaNo ratings yet
- Answers Outcome 5Document4 pagesAnswers Outcome 5doaaNo ratings yet
- 21 DigestiveDocument23 pages21 DigestivesaqibNo ratings yet
- Digestive SystemDocument117 pagesDigestive SystemKBDNo ratings yet
- Lecture Outline: See Separate Powerpoint Slides For All Figures and Tables Pre-Inserted Into Powerpoint Without NotesDocument63 pagesLecture Outline: See Separate Powerpoint Slides For All Figures and Tables Pre-Inserted Into Powerpoint Without NotesJharaNo ratings yet
- IP Pre-Worksheet GIDocument6 pagesIP Pre-Worksheet GIstormigirl017No ratings yet
- The Digestive System: S.Kep, NS., M.KepDocument10 pagesThe Digestive System: S.Kep, NS., M.KepAuliya AlfaNo ratings yet
- Digestive System - MefloresDocument117 pagesDigestive System - MefloresJohnMichaelDominguezNo ratings yet
- Farko Cerna UTS + TugasDocument357 pagesFarko Cerna UTS + TugasAnnisa N RahmayantiNo ratings yet
- Digestion and NutritionDocument53 pagesDigestion and NutritionErwin Poblete AraraoNo ratings yet
- Fom 4.1Document8 pagesFom 4.1yelloweverglowNo ratings yet
- The Digestive System: Dr. Ali EbneshahidiDocument46 pagesThe Digestive System: Dr. Ali EbneshahidiNirmala BandooNo ratings yet
- Homoestatic Mechanisms Regulate An Animal's Internal Environment. TheDocument19 pagesHomoestatic Mechanisms Regulate An Animal's Internal Environment. TheGabbie CruzNo ratings yet
- SLCC Anatomy CH 26-Digestive System: Study Online atDocument3 pagesSLCC Anatomy CH 26-Digestive System: Study Online atBrendaJooYeeNo ratings yet
- Anatomy and Physiology of Human Digestive System: The Mouth and PharynxDocument9 pagesAnatomy and Physiology of Human Digestive System: The Mouth and Pharynxitachi278No ratings yet
- Digestion Is The Breaking Down of Chemicals in The Body, Into A Form That Can Be Absorbed. It IsDocument10 pagesDigestion Is The Breaking Down of Chemicals in The Body, Into A Form That Can Be Absorbed. It IsSean McleanNo ratings yet
- Digestion 20240208 125021 0000Document21 pagesDigestion 20240208 125021 0000khandurreshahwar14No ratings yet
- Physio 5. Digestive System 5Document17 pagesPhysio 5. Digestive System 5Xena XenaNo ratings yet
- Esophages and Stomach ...........Document65 pagesEsophages and Stomach ...........Gebrie DinkayehuNo ratings yet
- Anatomy Digestive SystemDocument57 pagesAnatomy Digestive SystempabitraNo ratings yet
- Lect V Hormonal Regulation of MetabolismDocument61 pagesLect V Hormonal Regulation of Metabolismhou Diing HouNo ratings yet
- Р.8.OPERATION ON THE STOMATH AND DUODENUMDocument47 pagesР.8.OPERATION ON THE STOMATH AND DUODENUMMahmood SalahNo ratings yet
- Biopharmaceutics-01 AssignmentDocument14 pagesBiopharmaceutics-01 AssignmentRA TanvirNo ratings yet
- Part I: Anatomy and Physiology of The Digestive SystemDocument6 pagesPart I: Anatomy and Physiology of The Digestive SystemLleana TanNo ratings yet
- The Digestive SystemDocument23 pagesThe Digestive SystemJenderal Yohanes100% (1)
- Presentation On The Digestive SystemDocument48 pagesPresentation On The Digestive SystemOsman Saidu Sesay0% (1)
- AP Biology Guided Reading Chapter 41: Adapted From L. Miriello by S. SharpDocument6 pagesAP Biology Guided Reading Chapter 41: Adapted From L. Miriello by S. SharpPerla Villarreal100% (2)
- 7 Gastrointestinalsystemfull 120226085536 Phpapp01Document11 pages7 Gastrointestinalsystemfull 120226085536 Phpapp01didikekoNo ratings yet
- Lea 417 510 2011Document121 pagesLea 417 510 2011Oliver TalipNo ratings yet
- The Digestive SystemDocument44 pagesThe Digestive SystemJoy NatividadNo ratings yet
- Digestive System 2022-23Document28 pagesDigestive System 2022-23Fady Fady100% (1)
- Chapter 17 About Digestive SystemDocument4 pagesChapter 17 About Digestive SystemArash DhillonNo ratings yet
- Structure Appearance FunctionDocument6 pagesStructure Appearance FunctionKennee Eve CantilNo ratings yet
- Anatomy:: Basic StructureDocument7 pagesAnatomy:: Basic StructureCharish Dwayne Bautista PondalesNo ratings yet
- Digestive SystemDocument17 pagesDigestive SystemHana Sherif ElelamiNo ratings yet
- Introduction To The Gastrointestinal SystemDocument10 pagesIntroduction To The Gastrointestinal Systemjaninesimbol24No ratings yet
- Introduction To The Gastrointestinal SystemDocument10 pagesIntroduction To The Gastrointestinal Systemjaninesimbol24No ratings yet
- Anatomy and Physiology of The StomachDocument7 pagesAnatomy and Physiology of The StomachEmmi Maliza HutagaolNo ratings yet
- Digestive System: Five Basic ActivitiesDocument5 pagesDigestive System: Five Basic ActivitiesCrystal MaidenNo ratings yet
- Exsc 223 Chapter 23 Practice ExamDocument5 pagesExsc 223 Chapter 23 Practice Examkimber brownNo ratings yet
- 1 Introduction To The Gastrointestinal SystemDocument7 pages1 Introduction To The Gastrointestinal SystemLinh Phan100% (1)
- Leaky Gut Syndrome Stop! - A Complete Guide To Leaky Gut Syndrome Causes, Symptoms, Treatments & A Holistic System To Eliminate LGS Naturally & PermanentlyFrom EverandLeaky Gut Syndrome Stop! - A Complete Guide To Leaky Gut Syndrome Causes, Symptoms, Treatments & A Holistic System To Eliminate LGS Naturally & PermanentlyNo ratings yet
- Sample Preservation - UrineDocument1 pageSample Preservation - UrinedewkmcNo ratings yet
- Laboratory Diagnosis of Parasitic InfectionsDocument50 pagesLaboratory Diagnosis of Parasitic InfectionsdewkmcNo ratings yet
- Arterial Blood Gas Analysis: TeachingDocument9 pagesArterial Blood Gas Analysis: TeachingdewkmcNo ratings yet
- Non-Communicable Diseases: Allied Health SciencesDocument20 pagesNon-Communicable Diseases: Allied Health SciencesdewkmcNo ratings yet
- SUBJECT: Histology Laboratory Research Specimen Submission GuidelinesDocument1 pageSUBJECT: Histology Laboratory Research Specimen Submission GuidelinesdewkmcNo ratings yet
- A) Research in Relation To Health Service DeliveryDocument7 pagesA) Research in Relation To Health Service DeliverydewkmcNo ratings yet
- The Importance of Breastfeeding: SearchDocument8 pagesThe Importance of Breastfeeding: SearchdewkmcNo ratings yet
- Sanitation: Allied Health Sciences - Batch 2012 Basic Community Health November 01, 2012Document32 pagesSanitation: Allied Health Sciences - Batch 2012 Basic Community Health November 01, 2012dewkmcNo ratings yet
- Disease Globally & Locally: Dr. N Sivarajah Faculty of Medicine, University of Jaffna August 09, 2012Document25 pagesDisease Globally & Locally: Dr. N Sivarajah Faculty of Medicine, University of Jaffna August 09, 2012dewkmcNo ratings yet
- Introduction To Health EducationDocument12 pagesIntroduction To Health EducationdewkmcNo ratings yet
- Care of Elders: Dr. N Sivarajah Faculty of Medicine, University of JaffnaDocument29 pagesCare of Elders: Dr. N Sivarajah Faculty of Medicine, University of JaffnadewkmcNo ratings yet
- Health & DiseaseDocument14 pagesHealth & DiseasedewkmcNo ratings yet
- Health Education Methods & AidsDocument23 pagesHealth Education Methods & AidsdewkmcNo ratings yet
- Endocrine Glands: Secretion and Action of HormonesDocument58 pagesEndocrine Glands: Secretion and Action of HormonesdewkmcNo ratings yet
- ReproductionDocument74 pagesReproductiondewkmcNo ratings yet
- 1Document21 pages1dewkmcNo ratings yet
- Physiology of The KidneysDocument65 pagesPhysiology of The KidneysdewkmcNo ratings yet
- Sensory PhysiologyDocument56 pagesSensory PhysiologydewkmcNo ratings yet
- Regulation of MetabolismDocument56 pagesRegulation of MetabolismdewkmcNo ratings yet
- Heart and CirculationDocument67 pagesHeart and CirculationdewkmcNo ratings yet
- The Nervous System: Neurons and SynapsesDocument54 pagesThe Nervous System: Neurons and SynapsesdewkmcNo ratings yet