Professional Documents
Culture Documents
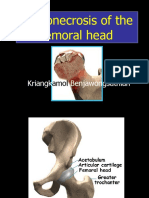
Avascular Necrosis of The Hip
Avascular Necrosis of The Hip
Uploaded by
bjpalmer100%(2)100% found this document useful (2 votes)
831 views22 pages1) Avascular necrosis (AVN) is the death of bone tissue due to a lack of blood supply. It most commonly affects the hip bone.
2) MRI is the most sensitive imaging method for diagnosing AVN. It can detect early changes in bone marrow signal and the pathognomonic "double line sign" on T2-weighted images.
3) AVN is staged based on radiographic and MRI findings, from Stage 0 showing just marrow edema to Stage 4 where the femoral head has collapsed, requiring joint replacement surgery.
Original Description:
Original Title
Avascular Necrosis
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document1) Avascular necrosis (AVN) is the death of bone tissue due to a lack of blood supply. It most commonly affects the hip bone.
2) MRI is the most sensitive imaging method for diagnosing AVN. It can detect early changes in bone marrow signal and the pathognomonic "double line sign" on T2-weighted images.
3) AVN is staged based on radiographic and MRI findings, from Stage 0 showing just marrow edema to Stage 4 where the femoral head has collapsed, requiring joint replacement surgery.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
Download as ppt, pdf, or txt
100%(2)100% found this document useful (2 votes)
831 views22 pagesAvascular Necrosis of The Hip
Avascular Necrosis of The Hip
Uploaded by
bjpalmer1) Avascular necrosis (AVN) is the death of bone tissue due to a lack of blood supply. It most commonly affects the hip bone.
2) MRI is the most sensitive imaging method for diagnosing AVN. It can detect early changes in bone marrow signal and the pathognomonic "double line sign" on T2-weighted images.
3) AVN is staged based on radiographic and MRI findings, from Stage 0 showing just marrow edema to Stage 4 where the femoral head has collapsed, requiring joint replacement surgery.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
Download as ppt, pdf, or txt
You are on page 1of 22
MRI
Avascular Necrosis of the Hip
Edward C. Fritsch, D.C.
Overview
• Avascular necrosis (AVN) is cellular death of the components
of bone, including bone marrow, due to impaired blood supply.
• AVN occurs in a number of conditions.
• AVN usually involves the epiphysis of long bones.
– Called bone infarct if in diaphysis or metaphysis
• AVN of the hip is the most common encountered in clinical
practice.
• Early diagnosis and appropriate intervention can delay the need
for joint replacement.
• Patients on corticosteroids and organ transplant recipients are
particularly at risk of developing AVN.
Pathophysiology:
• AVN is due to blood supply disruption, and it
affects bones with single terminal blood supply.
– Mechanical interruption of blood supply.
– Thrombotic or embolic occlusion of blood vessel.
– Injury to vessel wall
– Pressure on vessel wall
– Mechanism unknown (eg, high dose corticosteroids,
alcoholism, primary AVN)
Etiology
• SLE
• Rheumatoid arthritis
• Pancreatitis
Fracture / dislocation
• Gaucher's disease
• Steroid use • Polycythemia vera
• Alcoholism • Pregnancy
• Sickle cell disease • Septic emboli
• Fadiation
• Idiopathic
• Dysbarism (caisson
disease): scuba diver
surfacing too fast
• Thermal trauma (burns,
frostbite)
• Cushing's disease
Frequency
– Frequency depends on the site involved.
– The most common site is the hip, and other locations
include the carpals, talus, and humerus.
– US approximately 15,000 new cases are reported each
year.
– AVN accounts for >10% of total hip replacement
surgeries performed in the United States.
Patient Profile
• Sex: Depends on the underlying cause, the overall male-
to-female ratio is 8:1.
• Age: Age at onset depends on the underlying cause.
Primary AVN most often occurs during the forth or fifth
decade, and it is bilateral in 40-80% of cases. On
average, women present almost 10 years later than men.
• Race: No racial predilection exists except for AVN
associated with sickle cell disease and hemoglobin S and
SC disease, which predominantly occur in people of
African and Mediterranean descent.
Methods of Imaging
Imaging Findings Time to Comments
Method Diagnosis
X-Ray Osteopenia Months Sensitivity poor
Reactive sclerosis Specificity good
Subchondral Collapse (late)
CT Reactive sclerosis Weeks to Sensitivity poor
Subchondral collapse Months Specificity OK
Bone Scan Decreased uptake early Weeks Sensitivity good
Increased uptake late Specificity poor
MRI Change of signal in Days Sensitivity excellent
marrow pattern Specificity good
MRI Diagnosis of AVN
• MRI is the most
sensitive noninvasive
method for diagnosis
of AVN.
• Diagnosis involves
detection of marrow
foci of decreased signal
on T1-weighted images
and the characteristic
double line sign on T2-
weighted images.
(only condition that
will do the double line)
MRI Diagnosis of AVN - T1
• AVN is diagnosed when a
peripheral band of low
signal intensity is present
on all imaging sequences,
typically in the superior
portion of the femoral
head, outlining a central
area of marrow.
• This peripheral band is
most apparent on T1-
weighted sequences.
MRI Diagnosis of AVN - T2
• On conventional T2
sequences, the inner
border of the peripheral
band shows high signal in
80% of cases.
• This is called the "double
- line" sign of avascular
necrosis, and is considered
to be pathognomonic.
MRI Findings
T2 with Fat Supression
• Fat suppression is current
state of the art.
• Dark, peripheral band of
AVN that is not seen in
contrast to the inner high
signal band of AVN.
• Early edema of marrow
allowed MR to surpass
bone scans in early
diagnosis.
MRI Findings – Joint Effusions
• Increased joint fluid is
commonly associated with
AVN, and its presence
does not indicate a septic
joint effusion.
• The frequent presence of
joint effusions has led to
the hypothesis that
patients are presenting
with pain due to their
effusion, rather than the
long-standing process of
AVN.
Staging AVN
Ficat and Arlet Staging of AVN: (Radiographic staging)
Stage X-Ray MRI Bone Scan
0 Negative Marrow edema Maybe positive
Accidental finding
1 Osteopenia (hindsight) + bone necrosis Positive
Missed here and #2 s picture
perfect technique
2 Diffuses osteoporosis and sclerosis + joint edema Positive
on plain films. A reactive shell of
bone delimits the infarct. Spherical
femoral head.
3 Crescent sign (radiolucency) under + articular Positive
the subchondral bone representing cartilage
a fracture. Joint space preserved involvement
4 Femoral head collapse. Joint space + specificity of Positive
narrowing – OA joint
NEED SURGERY HERE AND 3 destruction
Stage 0
Stage 1
Stage 2
Stage 3 (crescent sign in frogleg)
Stage 4
Last Case
• 45 year old male
• Chronic LBP & hip
pain
• No response to
conservative care after
two weeks.
• MRI recommended
patient wanted to
wait…
The End
You might also like
- Gonstead Tech Study SheetDocument10 pagesGonstead Tech Study Sheetbjpalmer100% (3)
- DXR Clinician Quick ReferenceDocument2 pagesDXR Clinician Quick Referencebjpalmer100% (3)
- Orthopedics 2 Test NotesDocument6 pagesOrthopedics 2 Test Notesbjpalmer100% (1)
- Complication of FractureDocument38 pagesComplication of FractureAshok BalwadaNo ratings yet
- Amputasi Bellow KneeDocument29 pagesAmputasi Bellow KneeMolgen PanjaitanNo ratings yet
- Contraindications To Tourniquet UseDocument1 pageContraindications To Tourniquet UseSeti Aji H100% (1)
- Medical MnemonicsDocument256 pagesMedical MnemonicssitalcoolkNo ratings yet
- DR - Rieva Kuliah 7 November - 2018Document38 pagesDR - Rieva Kuliah 7 November - 2018Nisrina100% (1)
- Osteonecrosis of The Femoral Head: Kriangk BenjawongsathianDocument65 pagesOsteonecrosis of The Femoral Head: Kriangk Benjawongsathianryc0% (1)
- Avascular Necrosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandAvascular Necrosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsRating: 4 out of 5 stars4/5 (2)
- Discrimination of Metastatic From Acute Osteoporotic Compression Spinal Fractures With MRIDocument9 pagesDiscrimination of Metastatic From Acute Osteoporotic Compression Spinal Fractures With MRIChow Tat SingNo ratings yet
- Fdocuments - in - Chapter 10 Shoulder InjuriesDocument45 pagesFdocuments - in - Chapter 10 Shoulder Injuriespt.mahmoudNo ratings yet
- Lecture 11aDocument40 pagesLecture 11aElliya Rosyida67% (3)
- Menisectomy Case StudyDocument3 pagesMenisectomy Case StudyMiggy SikatNo ratings yet
- AOT Pri Absolute Stability BiomechanicsDocument21 pagesAOT Pri Absolute Stability BiomechanicsAbdullah Al Mamun Choudhury100% (1)
- Amputation: Sites of Amputation: UEDocument6 pagesAmputation: Sites of Amputation: UEChristine PilarNo ratings yet
- Spondylosis2 PDFDocument13 pagesSpondylosis2 PDFdrwarigitNo ratings yet
- Intravenous TherapyDocument48 pagesIntravenous TherapyFrancr ToledanoNo ratings yet
- Classification of Bone TumoursDocument3 pagesClassification of Bone TumoursMalueth AnguiNo ratings yet
- Tendon Transfers and Upper Limb Disorders: Aws KhanfarDocument41 pagesTendon Transfers and Upper Limb Disorders: Aws KhanfarRaghu Nadh100% (1)
- Tuberculosis of Knee: Presented By: DR Dipendra Maharjan 2 Yr Resident, MS Orthopaedics NAMS, Bir HospitalDocument25 pagesTuberculosis of Knee: Presented By: DR Dipendra Maharjan 2 Yr Resident, MS Orthopaedics NAMS, Bir HospitalshravaniNo ratings yet
- Ski Injuries To The Upper ExtremitiesDocument93 pagesSki Injuries To The Upper ExtremitiesBiba MijeeNo ratings yet
- Pelvic FractureDocument89 pagesPelvic FractureAndreas RendraNo ratings yet
- Rough DraftDocument12 pagesRough Draftapi-248853282No ratings yet
- Bahan Kuliah Fractures in ElderlyDocument27 pagesBahan Kuliah Fractures in ElderlyhazelelNo ratings yet
- Bones and Joints TBDocument19 pagesBones and Joints TBmichaelcylNo ratings yet
- Therapeutic Management of Knee Osteoarthritis: BY PT H N AbdullateefDocument96 pagesTherapeutic Management of Knee Osteoarthritis: BY PT H N AbdullateefMaida FitrianiNo ratings yet
- SPONDYLOLISTHESISDocument50 pagesSPONDYLOLISTHESISAnuj ShresthaNo ratings yet
- Lumbar Herniated DiscDocument5 pagesLumbar Herniated DiscRinda AndreanditaNo ratings yet
- Spinal Tuberculosis IandIIDocument59 pagesSpinal Tuberculosis IandIIagisagitaNo ratings yet
- Articular Fractures PrinciplesDocument9 pagesArticular Fractures PrinciplesSylviany El NovitaNo ratings yet
- Colles FractureDocument89 pagesColles Fracturenur syafiqah kamaruzaman100% (1)
- De Quervain SyndromeDocument5 pagesDe Quervain SyndromePaula ZorziNo ratings yet
- Alians Proximal Humerus: Innovation Means MotionDocument8 pagesAlians Proximal Humerus: Innovation Means MotionDaniel G. A. C.No ratings yet
- BHTDocument18 pagesBHTNitesh KumawatNo ratings yet
- Low Back Pain - DR Herman GofaraDocument50 pagesLow Back Pain - DR Herman GofaragivenchyNo ratings yet
- Orthopedic SlidesDocument78 pagesOrthopedic SlidesAzry Mustapa100% (1)
- Degenerative Disorders of Lumbar SpineDocument54 pagesDegenerative Disorders of Lumbar Spineapi-19916399No ratings yet
- Shoulder Dislocation: Nguyen Phuoc Thanh - MDDocument71 pagesShoulder Dislocation: Nguyen Phuoc Thanh - MDThành NPNo ratings yet
- Plates and Screws: An Overview: Presented by DR Oteki MisianiDocument45 pagesPlates and Screws: An Overview: Presented by DR Oteki MisianiIan OrwaNo ratings yet
- Stage of Fracture HealingDocument5 pagesStage of Fracture HealingDimas AgungNo ratings yet
- Knee ReplacementDocument2 pagesKnee ReplacementpahumbleNo ratings yet
- Osteochondritis Dissecans: Vivek PandeyDocument25 pagesOsteochondritis Dissecans: Vivek PandeyRabin DasNo ratings yet
- TKR RehabilitationDocument1 pageTKR RehabilitationgursangeetNo ratings yet
- Salter Harris FracturesDocument22 pagesSalter Harris FractureskoxNo ratings yet
- Complications of Intravenous TherapyDocument37 pagesComplications of Intravenous TherapyCarl Elexer Cuyugan Ano100% (3)
- B 756 Vertebris GB III10Document44 pagesB 756 Vertebris GB III10Lukasz Bartochowski100% (1)
- Degenerative Disorders of JointsDocument48 pagesDegenerative Disorders of Jointsbaiq nining100% (1)
- Osteoarthritis & Rheumatoid ArthritisDocument60 pagesOsteoarthritis & Rheumatoid ArthritisSaya MenangNo ratings yet
- Fractures - Diagnosis and ManagementDocument28 pagesFractures - Diagnosis and ManagementdrthanallaNo ratings yet
- Erbs PalsyDocument9 pagesErbs PalsyVatsalVermaNo ratings yet
- Classificationofjoints 140413054157 Phpapp01 161023170805Document49 pagesClassificationofjoints 140413054157 Phpapp01 161023170805Adu-danquah StephenNo ratings yet
- ACL Tear InjuryDocument5 pagesACL Tear InjuryNicole VazNo ratings yet
- Fracture 01Document42 pagesFracture 01api-19916399No ratings yet
- OSTEOPOROSISDocument39 pagesOSTEOPOROSISHapsari Wibawani 'winda'No ratings yet
- Management of Bone Defects in Primary Knee Arthroplasty: A Case ReportDocument4 pagesManagement of Bone Defects in Primary Knee Arthroplasty: A Case ReportInternational Journal of Recent Innovations in Academic ResearchNo ratings yet
- Osteoarthritis of The Knee CopieDocument20 pagesOsteoarthritis of The Knee CopieNarcisYonutzNo ratings yet
- Congenital Talipes Equino-VarusDocument48 pagesCongenital Talipes Equino-VarusKojo DuncanNo ratings yet
- Malunion Delayed Union and Nonunion FracturesDocument31 pagesMalunion Delayed Union and Nonunion FracturesutisuryanjNo ratings yet
- Ulcer: DR - Sunil Kumar Asst - Professor Dept - of Gen - Surgery MNR Medical College Sangareddy 01-05-2019Document83 pagesUlcer: DR - Sunil Kumar Asst - Professor Dept - of Gen - Surgery MNR Medical College Sangareddy 01-05-2019Aashmi ChandrikaaNo ratings yet
- TBWDocument45 pagesTBWveedee cikalNo ratings yet
- Chest Wall DeformitiesDocument34 pagesChest Wall DeformitiesadharshNo ratings yet
- 05 - Spinal Cord InjuryDocument92 pages05 - Spinal Cord InjurywaqarsuparcoNo ratings yet
- Carpal Tunnel Syndrome Fact SheetDocument6 pagesCarpal Tunnel Syndrome Fact SheetTissa RanatungeNo ratings yet
- Systems 1 Test 4Document59 pagesSystems 1 Test 4bjpalmer100% (2)
- DXR Clinician Student User ManualDocument13 pagesDXR Clinician Student User Manualbjpalmer100% (2)
- SettingsDocument2 pagesSettingsbjpalmer100% (3)
- Physiotherapy 3Document8 pagesPhysiotherapy 3bjpalmerNo ratings yet
- Shortwave Diathermy: 2 Types of Short Wave Diathermy (SWD)Document19 pagesShortwave Diathermy: 2 Types of Short Wave Diathermy (SWD)bjpalmer100% (2)
- PhysiotherapyDocument53 pagesPhysiotherapybjpalmer100% (2)
- PostcompsynDocument3 pagesPostcompsynbjpalmer100% (2)
- B&E (5) Medical BillingDocument4 pagesB&E (5) Medical Billingbjpalmer100% (2)
- ICD Code ChartDocument1 pageICD Code ChartbjpalmerNo ratings yet
- X-Ray-Positioning Spine Dr. FritschDocument62 pagesX-Ray-Positioning Spine Dr. Fritschbjpalmer100% (3)
- Tarsal Tunnel SyndromeDocument7 pagesTarsal Tunnel Syndromebjpalmer100% (2)
- Arthritide Notes OnlyDocument156 pagesArthritide Notes Onlybjpalmer100% (2)
- Lower Leg: Four Fascial CompartmentsDocument24 pagesLower Leg: Four Fascial Compartmentsbjpalmer100% (2)
- Patellofemoral Pain SyndromeDocument24 pagesPatellofemoral Pain Syndromebjpalmer100% (3)
- Chondromalacia PatellaDocument5 pagesChondromalacia Patellabjpalmer100% (3)
- Ankle ExaminationDocument16 pagesAnkle Examinationbjpalmer100% (2)
- Knee PainDocument32 pagesKnee Painbjpalmer100% (5)
- Vascular Disorders and Miscellaneous: Jeffrey R. Thompson, DC, DACBRDocument43 pagesVascular Disorders and Miscellaneous: Jeffrey R. Thompson, DC, DACBRbjpalmer100% (2)
- SPINEFXDocument68 pagesSPINEFXbjpalmer100% (2)
- Arthritide Notes OnlyDocument156 pagesArthritide Notes Onlybjpalmer100% (2)
- Review Assessment: Pre-Midterm Quiz - Skeletal ImagingDocument2 pagesReview Assessment: Pre-Midterm Quiz - Skeletal Imagingbjpalmer100% (2)
- Bone Infection Notes OnlyDocument34 pagesBone Infection Notes Onlybjpalmer100% (2)
- Skeletal Trauma-Plain Film Trauma Terminology ReviewDocument35 pagesSkeletal Trauma-Plain Film Trauma Terminology Reviewbjpalmer100% (3)
- Blue Writing Is What I Added To These Notes: RadiographyDocument46 pagesBlue Writing Is What I Added To These Notes: Radiographybjpalmer100% (2)
- Skeletal ImagingDocument1 pageSkeletal Imagingbjpalmer100% (2)
- 1) Vertebrobasilar Artery InsufficiencyDocument22 pages1) Vertebrobasilar Artery Insufficiencybjpalmer100% (6)
- Tivoli Storage Manager Operational Reporting Installation, Configuration and CustomizationDocument53 pagesTivoli Storage Manager Operational Reporting Installation, Configuration and CustomizationSABRINE KHNo ratings yet
- Naamlp 2002 ProceedDocument578 pagesNaamlp 2002 ProceedRussell HartillNo ratings yet
- SummaryDocument2 pagesSummaryRosida IdaNo ratings yet
- L550 19MY MB XC-EN V1j DX PDFDocument88 pagesL550 19MY MB XC-EN V1j DX PDFAnonymous gMgeQl1SndNo ratings yet
- Halimatus Islamiah Analisis Jurnal Internasional K3Document3 pagesHalimatus Islamiah Analisis Jurnal Internasional K3TussNo ratings yet
- VDRLDocument4 pagesVDRLfarazhussainkhanNo ratings yet
- Department of Mechanical Engineering: Final Year Mini Project PresentationDocument22 pagesDepartment of Mechanical Engineering: Final Year Mini Project PresentationNaresh DamaNo ratings yet
- Physical Pendulum - Angular SHM - Solved ProblemsDocument7 pagesPhysical Pendulum - Angular SHM - Solved ProblemsHomayoon GeramifarNo ratings yet
- A 182Document20 pagesA 182Thomas100% (1)
- Electro-Chemiluminescence Immunoassay (ECLIA) For The Quantitative Determination of CA 15-3 in Human Serum and PlasmaDocument2 pagesElectro-Chemiluminescence Immunoassay (ECLIA) For The Quantitative Determination of CA 15-3 in Human Serum and PlasmayantuNo ratings yet
- Bstem-5 4Document61 pagesBstem-5 4G-SamNo ratings yet
- The Road Not Taken: Bagrut Questions and AnswersDocument8 pagesThe Road Not Taken: Bagrut Questions and AnswersEstelle Nica Marie DunlaoNo ratings yet
- CyberbullyingDocument8 pagesCyberbullyingapi-433558817No ratings yet
- IIA IPPF PG - Quality Assurance and Improvement Program March 2012Document29 pagesIIA IPPF PG - Quality Assurance and Improvement Program March 2012Denilson MadaugyNo ratings yet
- Glass Configurator Datasheet 2023 03 27Document1 pageGlass Configurator Datasheet 2023 03 27Satrio PrakosoNo ratings yet
- Biophilic Design: ARC407 DissertationDocument4 pagesBiophilic Design: ARC407 DissertationAaryan JainNo ratings yet
- C C P S: Lalit KumarDocument3 pagesC C P S: Lalit KumarAbhishek aby5No ratings yet
- Chroma Bidirectional DC Power Supply Model 62000D SeriesDocument12 pagesChroma Bidirectional DC Power Supply Model 62000D SeriesaboofazilNo ratings yet
- Prayerbooklet 1st-EditionDocument16 pagesPrayerbooklet 1st-EditionRexelle Jane ManalaysayNo ratings yet
- Taylor Swift LyricsDocument2 pagesTaylor Swift LyricsElsie DomeNo ratings yet
- BDM SF 3 6LPA 2ndlisDocument20 pagesBDM SF 3 6LPA 2ndlisAvi VatsaNo ratings yet
- Name:: Nyoman Gede Abhyasa Class: X Mipa 2 Absent: 25 AnswersDocument2 pagesName:: Nyoman Gede Abhyasa Class: X Mipa 2 Absent: 25 AnswersRetrify - Random ContentNo ratings yet
- Chaliyama Steel Plant-Rungta Mines Limited Hazard Identification & Risk AssessmentDocument3 pagesChaliyama Steel Plant-Rungta Mines Limited Hazard Identification & Risk AssessmentCPP EI DSpNo ratings yet
- DAPA Teams Spider DiagramDocument2 pagesDAPA Teams Spider DiagramEduardoJaimeNo ratings yet
- Loads Table LV Power Panel Tag: 100-Dp-001Document1 pageLoads Table LV Power Panel Tag: 100-Dp-001Erwin CarrascoNo ratings yet
- 115 Ballard Tommelein 2021 LPS Benchmark 2020 2Document125 pages115 Ballard Tommelein 2021 LPS Benchmark 2020 2ATDNo ratings yet
- The Holy Spirit: A New LifeDocument2 pagesThe Holy Spirit: A New LifeKatu2010No ratings yet
- Geography P1 May-June 2023 EngDocument20 pagesGeography P1 May-June 2023 Engtanielliagreen0No ratings yet
- Mathematics Past Paper QuestionsDocument174 pagesMathematics Past Paper Questionsnodicoh572100% (2)
- Approach To Floppy InfantDocument44 pagesApproach To Floppy InfantNavya Hegde100% (2)