Professional Documents
Culture Documents
LOW Back Pain
LOW Back Pain
Uploaded by
Maya Vil100%(3)100% found this document useful (3 votes)
329 views111 pagesLow back pain is a costly burden that affects about 40% of people within a 6 month period. While most episodes are mild and resolve without treatment, the prevalence and costs associated with back pain have increased over the past 30 years likely due to social factors rather than changes in underlying medical conditions. Common causes of back pain include mechanical back pain, lumbar disc disease, spondylolysis, and spinal fractures. Back pain can be classified as acute, subacute, or chronic depending on its duration and associated symptoms.
Original Description:
Low Back Pain Physical Therapy
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentLow back pain is a costly burden that affects about 40% of people within a 6 month period. While most episodes are mild and resolve without treatment, the prevalence and costs associated with back pain have increased over the past 30 years likely due to social factors rather than changes in underlying medical conditions. Common causes of back pain include mechanical back pain, lumbar disc disease, spondylolysis, and spinal fractures. Back pain can be classified as acute, subacute, or chronic depending on its duration and associated symptoms.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
100%(3)100% found this document useful (3 votes)
329 views111 pagesLOW Back Pain
LOW Back Pain
Uploaded by
Maya VilLow back pain is a costly burden that affects about 40% of people within a 6 month period. While most episodes are mild and resolve without treatment, the prevalence and costs associated with back pain have increased over the past 30 years likely due to social factors rather than changes in underlying medical conditions. Common causes of back pain include mechanical back pain, lumbar disc disease, spondylolysis, and spinal fractures. Back pain can be classified as acute, subacute, or chronic depending on its duration and associated symptoms.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 111
LOW BACK PAIN
BY : MYRA LESLIE S. VILORIA
LOW BACK PAIN
Has become a costly burden to society and leading cause and loss of productivity.
About 40 % of people say that they have a low back pain within the past 6 months.
Studies have shown a lifetime prevalence as high as 84% . Onset usually begins in the
ten to early 40s . Most patients have short attacks of pain that are mild or moderate and
do not limit activities but these tend to reusr over many years. Most episodes resolve
without treatment.
The perventage of patients displayed by backpain as well as cot of lowback pain has
steadily increased during the past 30 years. This appears to be more from social cases
that from a change in the conditions that cause low back pain. The most commonly cited
factors are the increasing societal acceptance of back pain as a reason to become disbled
and changes in the social system that pay benefits with back pain .
Clinical Anatomy
Vertebral Column:
Cervical Spine:
Lordotic curvature
Greatest ROM
Most vulnerable to injury
Thoracic Spine:
Greatest protection
Least ROM
Lumbar Spine:
Balance between
protection/ROM
Clinical Anatomy
Vertebral Column:
Functions:
Transmits weight of the trunk to
the lower limbs
Surrounds/protects spinal cord
Attachment point for the ribs and
muscles of neck and back
Clinical Anatomy
Vertebral Column: Major
Supporting Ligaments
Anterior Longitudinal
Ligament runs vertically
along anterior surface of
vertebral bodies
Neck - Sacrum
Attaches strongly to both
vertebrae and intervertebral
discs (very wide)
Prevents back
hyperextension
Clinical Anatomy
Vertebral Column:
Major Supporting
Ligaments
Posterior Longitudinal
Ligament - runs vertically
along posterior surfaces of
vertebral bodies
Narrower, weaker
Attaches to intervertebral
discs
Prevents hyperflexion
Clinical Anatomy
Vertebral Column: Major
Supporting Ligaments
Ligamentum Flavum - strong
ligament that connects the
laminae of the vertebrae
Protects the neural elements
and the spinal cord
Stabilizes the spine to prevent
excessive vertebral body motion
Strongest of the spinal
ligaments
Forms the posterior wall of the
spinal canal with the laminae
Stretches with forward bending
/ recoils in erect position
Clinical Anatomy
Vertebral Column:
Supporting Ligaments
Intertransverse
Ligament - located
between the transverse
processes
Cervical region: consist of
a few irregular, scattered
fibers
Thoracic region: rounded
cords connected with deep
muscles of the back
Lumbar region: thin and
membranous
Clinical Anatomy
Vertebral Column: Supporting
Ligaments
Interspinal Ligament - connect
spinous processes (spans the
entire process)
Meets the ligamentum flavum in
front and the supraspinal ligament
behind
Clinical Anatomy
Vertebral Column:
Supporting Ligaments
Supraspinal Ligament -
connects together the
apexes of the spinous
processes
Extends from 7th cervical
vertebra to sacrum
Strong fibrous cord
At points of attachment
(tips of the spinous
processes) fibrocartilage is
developed in the ligament
Supraspinal
Ligament
Clinical Anatomy
Facet Joints:
Articulations between
superior articular facet
(bottom vertebrae) and
inferior articular facet
(above vertebrae)
Contribute to ROM
Weight-bearing stress
through vertebral body
and disc
Synovial joints
Clinical Anatomy
Pars Interarticularis:
Area between the
superior and inferior
facets
Common site for stress
fractures (lumbar spine)
Spondylolysis - refers to
the defect (black arrows)
present when the pars
interarticularis (green
arrow) is fractured
Clinical Anatomy
Intervertebral Foramen:
Space where spinal nerve
roots exit the vertebral
column
Size variable due to
placement, pathology,
spinal loading, and posture
Can be occluded by arthritic
degenerative changes and
space-occupying lesions
(tumors, spinal disc
herniations)
Clinical Anatomy
SI Ligaments:
Anterior Sacroiliac Ligament:
Connects the anterior surface of the
lateral part of the sacrum to the
ilium
Note: Black Arrow
Clinical Anatomy
SI Ligaments:
Posterior Sacroiliac
Ligament:
Forms the chief bond of
union between the bones
Upper part: (short PSL)
Nearly horizontal in
direction
Ilium to upper sacrum
Lower part: (long PSL)
Oblique in direction
Lower sacrum to PSIS
Short PSL Long PSL
Clinical Anatomy
SI Ligaments:
Sacrotuberous
Ligament:
Arises from ischial
tuberosity to blend in
with inferior fibers of
posterior SI ligaments
Ischial Tuberosity
Sacrotuberous
Ligament
Clinical Anatomy
SI Ligaments:
Sacrospinous Ligament:
Originates from the ischial spine and
attaches to the coccyx
Sacrospinous
Ligament
Clinical Anatomy
Intervertebral Discs:
23 intervertebral discs
No disc between skull and C1 or
between C1-C2
Discs are thickest in the lumbar
vertebrae and cervical regions
(enhances flexibility)
Functions:
Shock absorbers
walking, jumping, running
Allow spine to bend
At points of compression, the
discs flatten out and bulge out a
bit between the vertebrae
Clinical Anatomy
Nucleus Pulposus: Core
Gelatinous, acts like a
rubber ball (enables spine to
absorb compressive forces)
60-70% water
Annulus Fibrosus: Outer
rings
Multilayered fibers (cross
from opposite directions)
Rings absorb compressive
forces themselves
Clinical Anatomy
Intervertebral Discs: Dehydration Process
Collectively, the discs make up about 25% of the height of the
vertebral column
Nucleus pulposus becomes dehydrated during course of day
Flattens out (height is 1-2 centimeters less at night than when we awake in
morning)
Aging Process = Permanent dehydration (ages 40 60)
Decreased ROM
Narrowing intervertebral foramen
LOW BACK PAIN
DEFINITION ( DeLisa)
LBP as a diagnosis instead of being merely a
symptom.
( Braddom )
LBP is a symptom , not a disease and has many
causes.
Described as pain bet. The costal and gluteal folds.
TYPES OF LOW BACK PAIN
By Delisa
1.) Acute Low Back Pain
2.) Subacute Low Back Pain
3.) Chronic Low Back Pain
By Braddom and Magee
Mechanical Back Pain
TYPES OF LOW OF BACK PAIN
DEFINITION OF TERMS
1.) ALBP
defined as pain or discomfort in the lumbar region, on one or both sides
eventually irradiating to the buttocks and lasting no more than a month
No known cause
Does not Involve the bones and main nerves
. Instead, soft tissues are the main actors (muscles, ligaments,
apophyseal joints), together with discs eventually and/or vessels, and/or
the sympathetic nervous system.
2.) SLBP
SALBP is defined as pain or discomfort in the lumbar region,
on one or both sides, eventually irradiating to the buttocks
and lasting more than 1 month but less than 6 months
Some authors distinguish a subacute phase (1 to 3 months)
and a subchronic phase (4 to 6 months), but there is neither
epidemiological proof nor a real clinical decision based on
that distinction
3.) CLBP
CLBP is a pain with or without functional limitation in the
posterior region, including the area between the inferior limit
of the costal arch and the inferior buttock fold that lasts more
than 6 months.
4.) Secondary Back Pain
This section considers the spinal diseases that are recognized as causes of LBP.
It must be clearly stated that there is a big difference between imaging diagnosis
and clinical diagnosis.
According to the actual literature, the clinical diagnosis of secondary LBP should
be defined when there are symptoms and signs confirming that the imaging is
meaningful and strictly related to the clinical picture.
If this is not the case, the best interpretation of the imaging is the presence of
specific risk factors for the problems. In contrast, the worst interpretation of the
imaging finding is giving to the patient a diagnostic label (165,166) that can
propel him toward
chronicization.
CAUSES OF LBP
1.) Differential Dx: Back Pain Greater than Leg Pain
2.) Differential Dx: Leg Pain Greater than Back Pain
3.) Vertebral Deformities
4.) Nonlumbar Spine Causes of Radicular Symptoms
BACK PAIN GREATER THAN LEG PAIN
1.) Mechanical Back Pain
2.)Lumbar Disk Disease :
A.) Internal Disk Disruption
B.) Disc Degeneration
C.) DH
3.) Spondolysis
4.) Spondylolisthesis
6.) Other Spinal Fracture
7.) Cancer and LBP
LEG PAIN GREATER THAN BACK PAIN
Lumbosacral Radiculopathy
Lumbar Spinal Stenosis
Joint d/o
Soft tissue d/o
Cauda Equina Syndrome
BACK PAIN GREATER
THAN LEG PAIN
CAUSES OF LBP
1.) Back Pain Greater than Leg Pain
A.) Mechanical Back Pain :
85 % of those who seek medical care for LBP do not receive
specific dx
Causes: deconditioning , poor muscle recruitement, emotional
stress, changes associated with aging and injury such as disk
degeneration, arthritis and ligamentous hypertrophy.
2.) Lumbar Disk Disease
Diskogenic pain can be described as bandlike and exacerbated
lumbar flexion. It can be unilateral, , can radiate to the buttock,
can be even worsed by extension or side bending.
3 Categories :
A.) Degenerative disk disease
B.) Internal disk Disruption
A condition in w.c the internal architecture of the disk ins
interrupted but its external surface remains essentially normal
It can be characterized by degradation of the nucleus pulposus and
radial fissure that extend to the outer third of the annulus.
Herniation :a general term used when there is any change in the shape of
the annulus that causes it to bulge beyond its normal perimeter
Protrusion: nuclear material is contained by the outer layers of the annulus
and supporting ligamentous structures
Prolapse: frank rupture of the nuclear material into the vertebral canal.
Extrusion: extension of nuclear material beyond confines of the posterior
longitudinal ligament or above and below the disk space, as detected on
magnetic resonance imagine (MRI), but still in contact
Free sequestration: the extruded nucleus has separated from the disk and
moved away from the prolapsed area
SPONDYLOSIS
Is a defect of the pars interarticularis and is acommon cause of back pain and
adolosecents.
Repetitve hyperextension loading in the immature spine
Common in adolescent gymnast and football linemen
Pars defect: result from a combination of heridatary dysplasia of the pars and
repetitive stressing of the spien byh walking and extension loading
Spondylolysis:
Defect in pars interarticularis (area between inferior
and superior articular facets)
MOI repetitive stress
Unilateral or bilateral defects
Listhesis:
Posterior portion of the vertebrae, laminae,
inferior articular surfaces, spinous process
separates from vertebral body
Collared Scotty dog deformity
Symptoms:
Localized mow back pain ( during/after
activity)
Pain with extension
Spondylolisthesis:
Progression of spondylolysis separation of
vertebrae (superior vertebrae slides anteriorly on the
one below it)
Decapitated Scotty dog deformity:
Head of the dog (anterior element of vertebrae)
has become detached from body (posterior
element)
Severity amount of anterior displacement
Epidemiology:
Most prevalent in women and adolescents
Young gymnasts
LEG PAIN GREATER THAN
BACK PAIN
. Instability
defined as an abnormal response to applied loads, characterized kinematically by
abnormal movement in the motion. Segment beyond normal constraints (336). This
abnormal
Movement can be explained in terms of damage to the restraining structures
(i.e., facet joints, disks, ligaments, and muscles) that, if damaged or lax, will
encourage altered equilibrium and thus . instability (335).
LSI is considered to represent one of the potential conditions causing nonspecific
LBP
Cauda Equina Syndrome:
Anatomy: spinal cord ends at the lower edge of the 1st
lumbar vertebra
Lumbar and sacral nerve roots form a bundle within
the spinal canal below the conus medullaris
CES nerves within the spinal canal have been damaged;
nerves supplying muscles of legs, bladder, bowel and
genitals do not function properly
Numbness, loss of sensation (damage usually
permanent)
Congenital causes:
Spina bifida (abnormality in closure of spinal canal)
Tumors of the cauda equina
Acquired causes of Cauda Equina Syndrome:
Injury (spinal fractures)
Secondary to medical procedures
LSS is defined as any type of narrowing of the lumbar
spinal canal, causing compression of its content . This
narrowing causes direct mechanical compression
on the neural elements or on their blood supply, which may
lead to symptoms
The symptoms can decrease the patients quality of life
and cause him or her to seek treatment.
LSS may occur at different places in the spinal canal,
sometimes in more than one location at the same time. In
central canal stenosis, the nerve Roots in the cauda equina
may be
compressed.
Lateral recess stenosis and foraminal stenosis may cause
compression of the nerve
roots leaving the spine
NON LUMBAR SPINE CAUSES
OF RADICULAR LEG
SYMPTOMS
Soft tissue d/o
A.) Greater trochanter pain syndrome :
Regional pain syundrome focused about greater trochanter , buttock, gluteal
folds.
Often dx with trochanteric bursitis
B. Iliotibeal band syndrome :
Can be confused with an L4 or L5 radiculopathy
Presents lateral knee pain but it can also present with more proximal lateral
thigh pain or radiate distally to the calf .
Joint Disorder
Sacroiliac joint pain :
Potential pain generator that can refer pain into the lower
limb
Substance P can be found in the posterior iliac joint
Sources of pain : articular cartilage, the capsule,
ligamentous structure , muscular support of sacroiliac joint
VERTEBRAL DEFORMITIES
Vertebral Deformities in Adults
Definition
The ageing spine might develop two characteristic deformities:
scoliosis and FP.
Scoliosis in the adult is a disorder that involves a convergence of
deformity and degenerative Disease in the spine. It is defined as a
spinal deformity in a skeletally
Mature patient .
FP is defined by thoracic kyphosis, protrusion of the head,
and in more severe cases, knee flexion. The
pathophysiology of FP in the elderly is most likely
multifactorial: low bone mineral density, vertebral fractures,
intervertebral disk degeneration, and back extensor
strength, which decreases with age, are the most
frequently encountered factors
OTHER CAUSES OF LBP
Low back in Pregnancy
2 categories :
a.) LBP in pregnancy : Hx of backpain, previous pregnancy r/t back pain , LBP
during menses
B.) Pelvic girdle pain ( pain below the iliac crest, SI joint pain ) :
Hormonal changes alter the lumbopelvic ligaments which influences the stability
of the lumbosacral spines and make it more vulnerable to loading .
EVALUATION AND DIAGNOSTIC TOOLS
Clinical Evaluation
Test for Patient Malingering:
Malingering medical and psychological
terms that refers to an individual
fabricating/exaggerating their level of
symptoms
Financial compensation (fraud)
Avoiding work
Obtaining drugs
Attract attention or sympathy
Clinical Evaluation
Test for Patient Malingering:
Hoover Test:
Test Position:
Patient supine
Examiner at feet of patient with hands cupping the calcaneous of each leg
Action:
Patient attempts to actively straight leg raise on the involved side
Positive Findings:
Patient does not attempt to lift the leg and examiner does NOT sense pressure from the
uninvolved leg pressing down on the hand
Patient is not attempting to perform the test
Clinical Evaluation
Test Note: Examiner should be standing at feet of patient with their
hands cupping the heels of each leg
SLUMP TEST
What is this test for ?
Neurological test for the Lumber Spine
How do you perform the test?
The patient is seated on the edge of the examining table with the legs
supported, the hips in neutral position (i.e no rotation, abduction, or
adduction), and the hand behind the back (Fig. 9-49
STRAIGHT LEG RAISING TEST
Also known as Lasegue's test, the straight leg raising test (Fig. 9 - 51)
is done by the examiner with the patient completely relaxed.
What is this test for ?
It is a neurological tests of the lower limb. It is a passive test, and
each leg is tested individually with the normal leg being tested first
How do you perform the
test?
With the patient in the
supine position, the hip
medially rotated and
adducted, and the knee
extended, the examiner
flexes the hip until the
patient complains of pain
or tightness in the back
or back of back of leg.
WHAT WOULD A POSITIVE TEST INDICATE?
If the pain is primarily back pain, it is more likely a disc herniation or
the pathology causing the pressure is more central. If pain is primarily
in the leg, it is more likely that the pathology causing the pressure on
neurological tissues is more lateral.
Disc herniations or pathology causing pressure between the two
extremes are more likely to cause pain in both areas
FOR PATIENTS WHO HAVE DIFFICULTY
LYING SUPINE
Modified straight leg raising test
What is this test for ?
For patients who have difficulty lying supine.
How do you perform the test ?
The patient is in a side lying position with the test leg uppermost
and the hip and knee at 90. The lumbosacral spine is in neutral but
may be positioned in slight flexion or extension if this is more
comfortable for the patient. The examiner then passively extends the
patient's knee.
What would a positive test indicate?
pain, resistance, and reproduction of the patient's symptoms for a
positive test for neurological problem in the lumbar spine.
BILATERAL STRAIGHT LEG RAISING
What is this test for ?
Its a test for neurological test for Lumbar Spine.
How do you perform the test?
With the patient relaxed in the supine position and knees
extended, the examiner lifts both of the legs by flexing the
patient's hips until the patient complains of pain or
tightness. Because both legs are lifted the pelvis is not
stabilized (as it would be by one leg in unilateral straight leg
raise), so on hip flexion the pelvis is "freer" to rotate thereby
decreasing the stress or the neurological tissue.
What would a positive test
indicate ?
If the test causes pain
before 70 of hip flexion,
the lesion is probably in the
sacroiliac joints; if the test
causes pain after 70, the
lesion is probably in the
lumbar spine area.
Figure 9-64
H and I stability tests. (A) H test-side flexion. (B) H test-side flexion followed by
forward flexion. (C) H test-side flexion followed by extension. (D) I test-forward
flexion. (E) I test-forward flexion and side flexion. (F) I test-extension. (G) I
test-extension and side flexion
Specific Lumbar Spine Torsion Test.
What is this test for?
This test designed to stress specific levels of the lumbar spine.
To do this, the specific level must be rotated and stressed. An example would
be testing the integrity of left rotation on L5- S1
The patient is placed in a right side lying position with the
lumbar spine in slight extension (slight lordosis). Rotation
and side bending are achieved by the examiner grasping
the right arm and pulling it upward and forward at a 45
angle until movement is felt at the L5 spinous process. This
"locks" all the vertebrae above L5. The examiner then
stabilizes the L5 spinous process by holding the left
shoulder back with the examiner's elbow while rotating the
pelvis and sacrum forward until Sl starts to move (Fig. 9-
65) with the opposite hand. Minimal movement should
occur and a normal capsular tissue stretch should be felt
when L5-Sl is stressed by carefully pushing the shoulder
back ,with the elbow and rotating the pelvis forward with
the other arm/hand. This test position is a common position
used to manipulate the spine so the examiner should take
care not to "overstress" the rotation during assessment
Tests for Joint Dysfunction
One-Leg Standing (Stork Standing) Lumbar
ExensionTest.
The patient stands on one leg and extends the spine while
balancing on the leg (Fig.-72). The test is repeated with the
patient standing in the opposite leg. A positive test is
indicated by pain the back and is associated with a pars
interarticularistress fracture (spondylolisthesis). If the
stress fracture unilateral, standing on the ipsilateral leg
causes more pain. If rotation is combined with extension
and pain results, it 'is an indication of possible facet joint
.pathology on the side to which rotation occurs.
Clinical Evaluation
Nerve Root Impingement Tests:
Valsalva Test:
Test Position:
Patient seated, examiner standing next to patient
Action:
Subject takes a deep breath and holds while bearing down as if having a bowel movement
Positive Finding:
Increased spinal or radicular pain due to intrathecal pressure
May be secondary to a space-occupying lesion (i.e. herniated disc, tumor, osteophyte in
lumbar canal)
Comments:
Increase in intrathecal pressure may result in pulse, venous return, venous pressure
(dizziness and/or fainting)
Clinical Evaluation
Nerve Root Impingement Tests:
Milgram Test:
Test Position:
Patient supine, examiner at feet of the patient
Action:
Patient performs a bilateral straight leg raise to the height of 2 to 6 inches and is asked to hold
the position for 30 seconds
Positive Finding:
Patient unable to hold position, cannot lift the leg, or has pain with test
Implications:
Intrathecal or extrathecal pressure causing an intervertebral disc to place pressure on a lumbar
nerve root
Clinical Evaluation
Nerve Root Impingement Tests:
Kernigs Test:
Test Position:
Patient supine, examiner at side of patient
Action:
Patient performs a unilateral active straight leg raise with the knee extended until pain occurs
After pain occurs, the patient flexes the knee
Positive Finding:
Pain in the spine and possibly radiating into lower extremity
Pain relieved when patient flexes the knee
Implications:
Nerve root impingement secondary to bulging of the intervertebral disc or bony entrapment;
irritation of dural sheath; irritation of meninges
Clinical Evaluation
Nerve Root
Impingement Tests:
Kernig/Brudzinski Test:
Patient actively flexes the
cervical spine (lifts the
head)
Hip unilaterally flexed (no
more than 90
0
)
Knee than flexed to no
more than 90
0
(+) pain with neck and
hip flexion; pain relieved
when knee is flexed
Clinical Evaluation
Nerve Root Impingement Tests:
Unilateral Straight Leg Raise Test (Lasegue
Test):
Test Position:
Patient supine, examiner standing at tested side with the
distal hand around the subjects heel and proximal hand on
subjects distal thigh (anterior) maintains knee extension
Action:
Examiner slowly raises the leg until pain/tightness noted or
full ROM is obtained
Slowly lower the leg until the pain or tightness resolves, at
which point dorsiflex the ankle and have subject flex the
neck
TREATMENT AND REHABILATION
APPROACHES
TREATMENT APPROACH IN ALBP
ALBP should be treated mainly by general practitioners (GPs), both to
reduce costs and increase clinical long-term result.
The main objective and therapy in ALBP is, in fact, to reassure the
patient and provide accurate preventive
information. PO treatment is useful but secondary, even in the eyes of
patients . Specialists should reinforce the role of the GPs and
eventually offer them an educational support
.
REHABILITATION APPROACH IN ALBP
The key recommendation is to remain as active as possible and to
avoid
bed rest.
Caring for a patient suffering from ALBP should, however, take into
account two important factors related to prevention simultaneously:
avoiding chronicity and regaining any fitness lost during the period of
acute pain which may open the way to frequent relapses
TREATMENT AND REHABILITATION
APPROACH TO SLBP
TX AND REHABILITATION APPROACH OF
MECHANICAL BACK PAIN
a.) Reassurance and Patient and Education :
Explaination
Provide empathy and support and impart message
Reassurance that there is no serious underlying pahtylogy, that
the prognosis is good and that the patient can stay active and get
on with life despite the pain and can help counter megative
thoughts and misinformation that the patient might have about the
back pain
Back Schools:
Group classes that provide education about back pain
Exercise:
Individualized regimen learned and performed under
supervision that includes stretching and strethening.
Specific Exercise :
Lumbar stabilization and core strengthening exercises that
strengthen the muscles that support the spine are most widely
used to treat low back pain
Extension Exercise for Low back pain
Using principles of Mckinze, this therapy approach divides
into 3 categories : derangememnt, dysfunction and
postural syndrome.
The most common are that centralize the pain that is
move the pain from the leg or buttock into low back pain
Aerobic Activity
Low-impact aerobics with strengthening and stretching floor
exercises can be as effective in reducing pain and increasing
disability as individualized physical therapy and strengthening
with weight machines.
Aquatic Exercises for Mechanical Low back pain
Water can also decrease the pain vi the gate theory in which
the sensory input from the water temperatue, hydrostatic
pressure and turbulent cause the patient might also be
decreased in warm water.
MEDICATION :
1.) Muscle Relaxant : benzodiazepine, nonbenzodiazepines (
antispasmodic and antispaticity
Antidepressant: TCA
OPOIDS
Anticonvulsant
Tramadol
Herbal Medicinew : Capsicum frutescens ( cayenne) , Salix albab
INJECTIONS AND NEEDLE THERAPY FOR
MLBP
Acupuncture
Manual Mobilization or Manipulation
Traction
Lumbar Support
Complementary Movement Therapies:
Yoga: promote relaxation, acceptance, breathing
Pilates: core strengthening , that stress aligbnement and proper form +
Alexander technique
TX AND REHABILITATION APPROACH IN
SPONDYLOLISTHESIS
Conservative Mgt
Avoidance of activities that increase with pain
If tolerable, encourage client to do aeroboic activities to avoid
deconditioning
Patient should master core stabilization
For patient w/ CLBP and pars spondylolysis, according to OSullivan,
specific exercise focused on training the lumbar multifidie and deep
abdominal muscle
Surgical Mgt is rarely indicated
TX FOR SPINAL INFECTIONS
It is important to dx and tx spinal infection quickly to prevent increased morbidity
and mortality and to prevent complications such as epidural abscesses.
Usually a 4-6-week course of intravenous antibiiotics.
Sensitiivty can often be determined by blood culturues. But if these are negative
samples from a bone biopsy might be necessary.
TX AND REHABILITATION FOR LBP IN
PREGNANCY
Individualized physical therapy
Water aerobics
Acupuncture
Massage therapy
RESOURCES
1.) Braddom, Randall. Physical Medicine and Rehabilitation. 4
th
edition. Pp
871-906
2.) Colby and Kisner. Therapeutic Exercises 5
th
and 6
th
edition.
3.) Magee David. OPA. 5
th
edition.
4.) Delisa. Physical Medicine and Rehabilitation. Volume 1. 5
th
edition.
You might also like
- C6 Student Assessment Booklet Final 2012 - Case Study 1Document9 pagesC6 Student Assessment Booklet Final 2012 - Case Study 1Nan Hoareau0% (1)
- 19 Century Neoclassicism: History of Architecture - VDocument22 pages19 Century Neoclassicism: History of Architecture - Vvinit gupta100% (1)
- Best Exercises For Low Back PainDocument32 pagesBest Exercises For Low Back Painscribd_jr50% (4)
- Review of Related LiteratureDocument6 pagesReview of Related LiteratureMaya Vil0% (1)
- Evening Primrose OilDocument100 pagesEvening Primrose Oiladext100% (3)
- Low Back PainDocument100 pagesLow Back Painchandrusai100% (1)
- Low Back PainDocument8 pagesLow Back PainLev KalikaNo ratings yet
- Low Back Pain and SciaticaDocument24 pagesLow Back Pain and SciaticaOVVCMOULINo ratings yet
- Hip Impingement FaiDocument8 pagesHip Impingement FaiLev KalikaNo ratings yet
- Structure and Function of The Vertebral Column: Your Subtitle Goes HereDocument54 pagesStructure and Function of The Vertebral Column: Your Subtitle Goes HereJohn DoeNo ratings yet
- William C. Cottrell, MD AbstractDocument4 pagesWilliam C. Cottrell, MD AbstractmalaNo ratings yet
- Low Back PainDocument113 pagesLow Back Painpidutsam100% (2)
- Shockwave Therapy & ICDDocument44 pagesShockwave Therapy & ICDNQorianaNo ratings yet
- Examination of The Upper Cervical Spine PDFDocument22 pagesExamination of The Upper Cervical Spine PDFiikemNo ratings yet
- Shoulder Rehabilitation: - Anatomy Review - Muscle Testing Review - Common Problems - TreatmentDocument29 pagesShoulder Rehabilitation: - Anatomy Review - Muscle Testing Review - Common Problems - TreatmentStefan VladNo ratings yet
- PostureDocument2 pagesPostureNader MorrisNo ratings yet
- Rotator Cuff Tears IhoqkuDocument2 pagesRotator Cuff Tears IhoqkuKeefe TanNo ratings yet
- Chiropractic: An Introduction: Key PointsDocument6 pagesChiropractic: An Introduction: Key Pointsblackhole93No ratings yet
- 5 Studies Every Chiropractor Should HaveDocument28 pages5 Studies Every Chiropractor Should HaveDavid LamsonNo ratings yet
- Rotator Cuff InjuryDocument29 pagesRotator Cuff InjuryArko duttaNo ratings yet
- Examination of Bone and Joint PathologyDocument89 pagesExamination of Bone and Joint PathologyMuhammad Thahir100% (1)
- Computer Aided Diagnosis System For Lumbar Spinal Stenosis Using X-Ray ImagesDocument45 pagesComputer Aided Diagnosis System For Lumbar Spinal Stenosis Using X-Ray Imagesroky100% (1)
- Physiotherapy Management in Scars, Wound and Ulcers 2Document23 pagesPhysiotherapy Management in Scars, Wound and Ulcers 2VybhavaNo ratings yet
- 03 RehabilitationDocument42 pages03 RehabilitationAlexandra ComanNo ratings yet
- Hallux Valgus PDFDocument26 pagesHallux Valgus PDFDeny EvanderNo ratings yet
- Achilles TendonDocument30 pagesAchilles TendonMeldianaNo ratings yet
- Handand Wrist ExammasterDocument91 pagesHandand Wrist ExammasterjothiNo ratings yet
- Hip Joint: 5 December 2016 Anatomy Lecture By: DR Anita RaniDocument38 pagesHip Joint: 5 December 2016 Anatomy Lecture By: DR Anita RaniDr'Dinesh MishraNo ratings yet
- Tendon Problems in Athletic IndividualsDocument15 pagesTendon Problems in Athletic IndividualsMuhammadskNo ratings yet
- 9 Pregnancy Stretches For The Whole Body 4 Pager Apr17 v3Document4 pages9 Pregnancy Stretches For The Whole Body 4 Pager Apr17 v3LeiltonNo ratings yet
- SCOLIOSIS Straightening Is Possible - DR Jan Polak - Ebook PDFDocument40 pagesSCOLIOSIS Straightening Is Possible - DR Jan Polak - Ebook PDFLuigi PolitoNo ratings yet
- The Road To Good Health: Discover ChiropracticDocument17 pagesThe Road To Good Health: Discover ChiropracticFioravanti AlessandroNo ratings yet
- Golfers Elbow Trigger Point Therapy TreatmentDocument35 pagesGolfers Elbow Trigger Point Therapy TreatmentYes ZamNo ratings yet
- Achilles RuptureDocument23 pagesAchilles RupturePhysiotherapist AliNo ratings yet
- I. Etiology Primary Adhesive Capsulitis Secondary Adhesive CapsulitisDocument8 pagesI. Etiology Primary Adhesive Capsulitis Secondary Adhesive CapsulitisVanessa Yvonne Gurtiza100% (1)
- Soft Tissue Mobilization IntroDocument33 pagesSoft Tissue Mobilization IntroasloocltNo ratings yet
- Evaluation of The Patient With Hip PainDocument12 pagesEvaluation of The Patient With Hip PainannisaNo ratings yet
- Shockwave Therapy MZUEDocument21 pagesShockwave Therapy MZUELove & HumanityNo ratings yet
- IvdpDocument89 pagesIvdpFelix Sabu100% (1)
- Rotator Cuff Tears Orthoinfo - Aaos.org TopicDocument7 pagesRotator Cuff Tears Orthoinfo - Aaos.org TopicMontserrat LandaNo ratings yet
- Craig Liebenson SI Joint InstabilityDocument3 pagesCraig Liebenson SI Joint InstabilityrojexeNo ratings yet
- Chondromalacia Patella RehabDocument1 pageChondromalacia Patella Rehabjntownsend3404No ratings yet
- Anatomical Variation of Sciatic Nerve Course in Saudi Population A Magnetic Resonance Imaging StudyDocument8 pagesAnatomical Variation of Sciatic Nerve Course in Saudi Population A Magnetic Resonance Imaging StudyInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Low Back Pain: Nama Kelompok: 1.ludivika Helembo (1562030032) 2.pankrasius A.B Baklu (1562030034) 3.jessica (1562030036)Document10 pagesLow Back Pain: Nama Kelompok: 1.ludivika Helembo (1562030032) 2.pankrasius A.B Baklu (1562030034) 3.jessica (1562030036)Maria Lastiar AmbaritaNo ratings yet
- Performing Palpation TechniquesDocument49 pagesPerforming Palpation TechniquesTina TalmadgeNo ratings yet
- Mulligan Vs ART PDFDocument4 pagesMulligan Vs ART PDFwernsickleNo ratings yet
- Rehabilitation: Walking After Total Knee ReplacementDocument10 pagesRehabilitation: Walking After Total Knee ReplacementSandeep DhimanNo ratings yet
- 5.6 Muscle Energy Techniques For The Pelvis 167-171Document5 pages5.6 Muscle Energy Techniques For The Pelvis 167-171maricartiNo ratings yet
- The Spencer TechniqueDocument11 pagesThe Spencer TechniqueDavidAgelliNo ratings yet
- Joint Mobilizations PDFDocument1 pageJoint Mobilizations PDFErik TellezNo ratings yet
- Lumbar Herniated DiscDocument5 pagesLumbar Herniated DiscRinda AndreanditaNo ratings yet
- Tuberculosis of Hip JointDocument25 pagesTuberculosis of Hip JointYousra ShaikhNo ratings yet
- Achilles Tendon: Exercises: Your Kaiser Permanente Care InstructionsDocument4 pagesAchilles Tendon: Exercises: Your Kaiser Permanente Care InstructionsCamden VistainNo ratings yet
- Shoulder Assessment: Ayesha RazzaqDocument47 pagesShoulder Assessment: Ayesha Razzaqayesha100% (1)
- Assessment of Posture: Prepared By: Floriza P. de Leon, PTRPDocument17 pagesAssessment of Posture: Prepared By: Floriza P. de Leon, PTRPFloriza de Leon100% (1)
- Managing Lumbar Spinal StenosisDocument11 pagesManaging Lumbar Spinal StenosismudassarnatiNo ratings yet
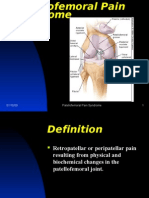
- Patellofemoral Pain SyndromeDocument24 pagesPatellofemoral Pain Syndromebjpalmer100% (3)
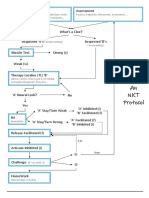
- NKT FlowChart - PDF Version 1 PDFDocument2 pagesNKT FlowChart - PDF Version 1 PDFJay SarkNo ratings yet
- ISMST GuidelinesDocument112 pagesISMST GuidelinesDhrubo TaraNo ratings yet
- Rotator Cuff Tear: Nurul Sahida Dina Fadhilah Monika MaghfiraDocument26 pagesRotator Cuff Tear: Nurul Sahida Dina Fadhilah Monika Maghfiradila_innongNo ratings yet
- Book of Abstracts Mulligan MCTA Porto Conference 2011Document89 pagesBook of Abstracts Mulligan MCTA Porto Conference 2011Michel BakkerNo ratings yet
- Extracorporeal Shockwave Therapy ESWT / EPAT.Document4 pagesExtracorporeal Shockwave Therapy ESWT / EPAT.Lev Kalika100% (1)
- Trochanteric Bursitis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandTrochanteric Bursitis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Basic Concepts of Computer Networks and Communications: Presented By: Joss Kendrick LiquidoDocument21 pagesBasic Concepts of Computer Networks and Communications: Presented By: Joss Kendrick LiquidoMaya VilNo ratings yet
- Grading Sheet (Title Defense)Document1 pageGrading Sheet (Title Defense)Maya VilNo ratings yet
- Berg Balance Scale: By: Myra Leslie S. ViloriaDocument5 pagesBerg Balance Scale: By: Myra Leslie S. ViloriaMaya VilNo ratings yet
- Cardiac RehabilitationDocument87 pagesCardiac RehabilitationMaya Vil100% (2)
- The School of Allied Health Sciences ofDocument1 pageThe School of Allied Health Sciences ofMaya VilNo ratings yet
- Postpartum Physical TherapyDocument10 pagesPostpartum Physical TherapyMaya VilNo ratings yet
- Sermon On The Ten Virgins - Parable of The Ten VirginsDocument4 pagesSermon On The Ten Virgins - Parable of The Ten VirginsMaya VilNo ratings yet
- Presented By: Myra Leslie S. ViloriaDocument10 pagesPresented By: Myra Leslie S. ViloriaMaya VilNo ratings yet
- Clinical Case Study GonadsDocument18 pagesClinical Case Study GonadsMaya VilNo ratings yet
- Adrenal Cortex Case StudyDocument21 pagesAdrenal Cortex Case StudyMaya Vil0% (1)
- Bilateral OsteoarthritisDocument58 pagesBilateral OsteoarthritisMaya VilNo ratings yet
- Traumatic Spinal Cord InjuryDocument60 pagesTraumatic Spinal Cord InjuryMaya Vil100% (1)
- Congenital Malformation of The Brain: By: Myra Leslie S. Viloria References: Neuroimaging - Clinical ApplicationsDocument32 pagesCongenital Malformation of The Brain: By: Myra Leslie S. Viloria References: Neuroimaging - Clinical ApplicationsMaya VilNo ratings yet
- Ankle and FootDocument188 pagesAnkle and FootMaya VilNo ratings yet
- Major Components of Social SciencesDocument18 pagesMajor Components of Social SciencesMaya VilNo ratings yet
- Sensory AssessmentDocument3 pagesSensory AssessmentMaya VilNo ratings yet
- Major Components of Social SciencesDocument27 pagesMajor Components of Social SciencesMaya VilNo ratings yet
- Gender and Development Made EasyDocument49 pagesGender and Development Made EasyMaya Vil100% (1)
- 1992 - Worlds of Consciousness and The Structure of ConsciousnessDocument43 pages1992 - Worlds of Consciousness and The Structure of ConsciousnessKátharsisNo ratings yet
- Cold Mail Samples For Non-STEM GraduatesDocument8 pagesCold Mail Samples For Non-STEM GraduatesKifayat HussainNo ratings yet
- LEA 5 Midterm Exam 2013Document2 pagesLEA 5 Midterm Exam 2013Ivy Maril De Guzman-ViernesNo ratings yet
- Mechanical PunchinelloDocument1 pageMechanical PunchinelloMarco FrascariNo ratings yet
- Gender and Development New Udsm Updated 1 1 1Document177 pagesGender and Development New Udsm Updated 1 1 1barakaathuman888No ratings yet
- L05 Dynamic Modelling Sequence DiagramDocument17 pagesL05 Dynamic Modelling Sequence DiagramPrachi ShishodiaNo ratings yet
- Ea 4 18 Inf Rev00 June 2010 RevDocument15 pagesEa 4 18 Inf Rev00 June 2010 RevBrandon EricksonNo ratings yet
- A Brief History of Kenya.20121109.224503Document2 pagesA Brief History of Kenya.20121109.224503anon_646668022No ratings yet
- Daniel: HISTORY - (Chapters 1-6)Document3 pagesDaniel: HISTORY - (Chapters 1-6)aweda142No ratings yet
- ch04Document62 pagesch04Liow Zhi XianNo ratings yet
- 2015 Eccentric or Concentric Exercises For The Treatment of Tendinopathies...Document11 pages2015 Eccentric or Concentric Exercises For The Treatment of Tendinopathies...Castro WeithNo ratings yet
- Web Hosting Server DetailsDocument11 pagesWeb Hosting Server DetailsTarun VBRSITNo ratings yet
- Certainty Equivalent FactorDocument2 pagesCertainty Equivalent FactorParth SahniNo ratings yet
- Sermon 3Document5 pagesSermon 3Clarry GruyalNo ratings yet
- Human Eye and EarDocument2 pagesHuman Eye and Earshathurjanan.jana5No ratings yet
- IAMGOLD Geotech Logging 20071101 PrintDocument42 pagesIAMGOLD Geotech Logging 20071101 PrintJoseph Mofat100% (1)
- SupriyaDocument15 pagesSupriyaprajwal karkiNo ratings yet
- CPBFI - 2.0 - Online - Lesson 7-Session 1Document11 pagesCPBFI - 2.0 - Online - Lesson 7-Session 1Mahima SonsareNo ratings yet
- Ifrs 9Document82 pagesIfrs 9kamal asgharNo ratings yet
- M e Demand Forecasting 100202064135 Phpapp02Document20 pagesM e Demand Forecasting 100202064135 Phpapp02Rahul ParabNo ratings yet
- Piano Sheet 12 Days of ChristmasDocument5 pagesPiano Sheet 12 Days of ChristmasSong Loi100% (1)
- Index 1 4Document13 pagesIndex 1 4Al LaiusNo ratings yet
- Naila KabeerDocument64 pagesNaila KabeerSangeeta SinghNo ratings yet
- Paradise Datacom Q-Flex-400 IP Satellite Modem Data Sheet 215635 12-11-2017Document6 pagesParadise Datacom Q-Flex-400 IP Satellite Modem Data Sheet 215635 12-11-2017arzeszutNo ratings yet
- These Beautiful Butterflies Up in The Sky, Send Valentine Wishes As They Flutter byDocument6 pagesThese Beautiful Butterflies Up in The Sky, Send Valentine Wishes As They Flutter byRaquel SilvaNo ratings yet
- Unity and Diversity in New Testament TheologyDocument9 pagesUnity and Diversity in New Testament Theologyseth Effah hillNo ratings yet
- Salaria v. Buenviaje G.R. No. L 45642 DIGESTDocument2 pagesSalaria v. Buenviaje G.R. No. L 45642 DIGESTMikee BornforThis MirasolNo ratings yet