Professional Documents
Culture Documents
Asthma in Adults: Jessica Lo - MS3, SUNY Downstate May 2014
Asthma in Adults: Jessica Lo - MS3, SUNY Downstate May 2014
Uploaded by
superpickle870 ratings0% found this document useful (0 votes)
47 views22 pagesThis document discusses asthma in adults. It begins by providing statistics on asthma prevalence and costs in the US. It then describes asthma as a chronic inflammatory disease of the airways causing reversible airflow obstruction. The pathophysiology of asthma involves both intrinsic and extrinsic mechanisms. Extrinsic mechanisms are immune-related and involve mast cell activation by allergens. Clinical features of asthma include respiratory symptoms triggered by various factors that resolve with treatment. Diagnosis involves assessing symptoms, physical exam findings, and pulmonary function testing. Asthma is classified by severity to guide initial treatment and management. The document reviews various asthma medications and their mechanisms of action. It concludes by discussing management of asthma exacerbations in urgent care settings.
Original Description:
asthma powerpoint
Original Title
Asthma in Adults
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses asthma in adults. It begins by providing statistics on asthma prevalence and costs in the US. It then describes asthma as a chronic inflammatory disease of the airways causing reversible airflow obstruction. The pathophysiology of asthma involves both intrinsic and extrinsic mechanisms. Extrinsic mechanisms are immune-related and involve mast cell activation by allergens. Clinical features of asthma include respiratory symptoms triggered by various factors that resolve with treatment. Diagnosis involves assessing symptoms, physical exam findings, and pulmonary function testing. Asthma is classified by severity to guide initial treatment and management. The document reviews various asthma medications and their mechanisms of action. It concludes by discussing management of asthma exacerbations in urgent care settings.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
47 views22 pagesAsthma in Adults: Jessica Lo - MS3, SUNY Downstate May 2014
Asthma in Adults: Jessica Lo - MS3, SUNY Downstate May 2014
Uploaded by
superpickle87This document discusses asthma in adults. It begins by providing statistics on asthma prevalence and costs in the US. It then describes asthma as a chronic inflammatory disease of the airways causing reversible airflow obstruction. The pathophysiology of asthma involves both intrinsic and extrinsic mechanisms. Extrinsic mechanisms are immune-related and involve mast cell activation by allergens. Clinical features of asthma include respiratory symptoms triggered by various factors that resolve with treatment. Diagnosis involves assessing symptoms, physical exam findings, and pulmonary function testing. Asthma is classified by severity to guide initial treatment and management. The document reviews various asthma medications and their mechanisms of action. It concludes by discussing management of asthma exacerbations in urgent care settings.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 22
Asthma in Adults
Jessica Lo MS3, SUNY Downstate
May 2014
Introduction
1 in 12 people in the U.S. have asthma = 25 million people (CDC 2011)
7 million are children
$56 billion per year in medical costs, missed school days and missed work
days
>3000 deaths due to asthma in the U.S. (2010)
Numbers growing every year
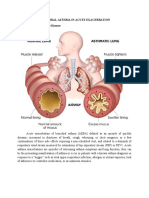
What is Asthma?
Chronic inflammatory disease of the airways causing airflow obstruction
Obstructive lung disease
Bronchial hyperresponsiveness
Symptoms typically wax and wane
REVERSIBLE (at least partially)
Triad of:
Bronchoconstriction
Inflammation and edema of airway walls
Mucus production/plugging
Asthma - Pathophysiology
2 mechanisms
Intrinsic non-immune related, caused by vagal stimulation (e.g. viral
infection, exercise, cold air)
Extrinsic immune-related, caused by mast cell activation and
degranulation (e.g. allergens)
Asthma - Pathophysiology
Extrinsic
Allergens bound by dendritic cells
and presented to T- and B-cells
T-cells secrete cytokines causing B-
cell production of IgE
IgE coats mast cells; cross-linking
causes mast cell degranulation
and release of histamine,
leukotrienes, and inflammatory
cytokines
Asthma - Pathophysiology
2 phases of asthma attack
Early phase
Within several minutes
Allergen exposure by sensitized individual causes mast cell degranulation and release
of histamines, prostaglandins, leukotrienes, etc.
Can also be through vagal stimulation by irritant
Bronchoconstriction via smooth muscle contraction, edema via blood vessel dilation
and increased permeability, and mucus production
Late phase
Hours later
Recruitment of other inflammatory and immune cells, e.g. eosinophils, basophils,
neutrophils, T-cells, monocytes, dendritic cells
Further release of inflammatory mediators
Clinical Features - History
Respiratory symptoms in presence of triggers that resolve with avoidance of
trigger or with asthma medication
E.g. allergens, exercise, cold air, smoke, infection, aspirin
Symptoms
Wheeze
Cough, often worse at night
Dyspnea
Chest tightness
Symptoms typically episodic and often worse at night
Personal or family history of asthma, allergies, or other atopic diseases
History of chronic cough, nighttime cough, or recurrent bronchitis as a child
Clinical Features Physical
Scattered, high-pitched musical wheezes
Commonly expiratory, but can also be inspiratory
Usually varies in tone and duration over time, starts and stops at different points of respiratory
cycle
Severe
Tachypnea
Tachycardia
Prolonged expiration (decreased I:E ratio)
Tripod position
Use of accessory muscles of respiration
Pulsus paradoxus (decrease in SBP >12mmHg during inspiration)
Absence of wheeze may indicate severe bronchoconstriction
Extra-pulmonary
Nares pale, swollen mucosa suggest of allergic rhinitis; nasal polyps suggest aspirin sensitivity
Skin atopic dermatitis
Nasal polyps
Diagnosis of Asthma
History
Physical exam
Spirometry
FEV1/FVC ratio <70%
Increase in FEV1 >12% or 200ml with
administration of short-acting bronchodilator
(e.g. albuterol)
Decrease in FEV1 >20% with
bronchoprovocation test (methacholine or
mannitol inhalation)
Peak expiratory flow
>20% variability over several recordings
Other Studies
CBC with diff may show eosinophilia (>15% or >1500/microL)
CXR
May show pneumonia (possible exacerbating factor)
Also used to rule out other causes of asthma-like symptoms
Poorly controlled asthma may have atelectasis due to mucus plugging
Allergy tests identify triggers
Total serum IgE when considering use of omalizumab as therapy
Classifying Asthma Severity
Intermittent
Symptoms 2 days/week
Nighttime awakenings 2x/month
Use of short-acting beta
2
-agonist 2 days/week
Mild persistent
Symptoms >2 days/week but less than daily
Nighttime awakenings 3-4x/month
Use of short-acting beta
2
-agonist >2 days/week but not daily and not >1x/week
Moderate persistent
Symptoms daily
Nighttime awakenings >1x/week but not nightly
Use of short-acting beta
2
-agonist daily
Severe persistent
Symptoms throughout the day
Nighttime awakenings often 7x/week
Use of short-acting beta
2
-agonist several times a day
Classifying Asthma Severity & Initial
Treatment
Management of Asthma by Severity
Reassessment and Adjusting Therapy
Asthma Medications
Asthma Medications Mechanisms of
Action
Asthma Medications
Short-acting beta
2
-agonists (SABA)
E.g. Albuterol, levalbuterol, pirbuterol, metaproterenol
Use: PRN
Mechanism: bronchial smooth muscle relaxation
Side effects: increase HR, tremors, arrhythmias, irritability
Levalbuterol marketed to have fewer side effects
Long-acting beta-agonists (LABA)
E.g. salmeterol, formoterol, arformoterol
Use: usually added to treatment if moderate persistent asthma or worse.
Used as twice daily controller
Mechanism and side effects same as short-acting
Asthma Medications
Inhaled corticosteroids (ICS)
E.g. beclomethasone, budesonide, flunisolide, fluticasone, mometasone
Use: added for mild persistent or worse. Twice daily controller
Mechanism: decreases inflammation by inhibiting cytokine production
Side effects: dysphonia, thrush, reflex cough
Systemic corticosteroids
E.g. prednisone, prednisolone, methylprednisolone (IV)
Use: moderate to severe exacerbations. Usually given for 3-10 days to avoid
adrenal suppression
Side effects: adrenal suppression, leukocytosis, immune suppression, Cushings
syndrome, neuropsychiatric disturbance, osteoporosis, cataracts
Asthma Medications
Anticholinergics
E.g. ipratropium, tiotropium
Use: in combination with SABA for mild/moderate persistent asthma
Mechanism: inhibit muscarinic cholinergic receptors to reduce vagal tone bronchodilation
Side effects: dry mouth, blurred vision, urinary obstruction
Methylxanthines
E.g. theophylline
Use: add-on or alternative for moderate or severe persistent; used rarely
Mechanism: inhibits phosphodiesterase, leading to increased cAMP smooth muscle relaxation
Side effects: tachycardia, nausea/vomiting, sleep disturbance, arrhythmias and seizures in overdose;
narrow therapeutic index
Leukotriene modifiers
E.g. montelukast, zafirleukast, zileuton
Use: as alternative or add-on to ICS or LABA
Mechanism: leukotriene receptor antagonist (montelukast, zafirleukast) or leukotriene synthesis inhibitor
(zileuton). Leukotrienes responsible for eosinophil infiltration of airways
Side effects: elevated transaminases, hepatotoxicity (zileuton)
Asthma Medications
Mast cell stabilizers
E.g. cromolyn, nedocromil
Use: maintenance/controller. Add-on or alternate to ICS or LABA
Mechanism: prevents activation and degranulation of mast cell by membrane
stabilization (cromolyn) and prevents release of inflammatory mediators by by
neutrophils, eosinophils, monocytes, and macrophages (nedocromil)
Side effects: sore throat, unpleasant taste
Anti-IgE
E.g. Omalizumab
Use: moderate to severe persistent asthma. Good for patients with allergies.
Subcutaneous administration
Mechanism: prevents IgE binding to mast cells
Side effects: anaphylaxis
Urgent Care Setting
Assessment
Physical tachypnea, HR >120, diaphoresis, use of accessory muscles, inability to speak full
sentences, pulsus paradoxus
Peak flow meter PEF <200L/min or <50% of baseline
Pulse oximetry
ABG hypoxemia; normal or increased PaCO2 indicates worsening of exacerbation either
by severe airway narrowing or inspiratory muscle fatigue
Supplemental oxygen, albuterol, ipratropium, inhaled or IV steroids
Maintain O
s
sat >90%
Terbutaline drip or epinephrine
Magnesium sulfate IV if patient unimproved on conventional therapy
Bronchodilation by inhibition of calcium influx into smooth muscle cells
If all else fails - Intubation and mechanical ventilation
Methylxanthines, mast cell stabilizers, omalizumab, and LABAs are NOT effective in acute
exacerbations
References
UptoDate
FirstAid for USMLE Step 1
http://www.cdc.gov/nchs/fastats/asthma.htm
Clinical Guideline for the Diagnosis, Evaluation and Management of Adults
and Children with Asthma New York State Department of Health
You might also like
- Pharmacy Services List of Drug That Contains Porcine, Bovine, Mixture of Both Bovine and Porcine, and Other Animal SourceDocument6 pagesPharmacy Services List of Drug That Contains Porcine, Bovine, Mixture of Both Bovine and Porcine, and Other Animal SourceKok Hui Diong100% (1)
- Pharma Anesth COMPILATIONDocument155 pagesPharma Anesth COMPILATIONDENTAL REVIEWER ONLYNo ratings yet
- Bronchial Asthma in Acute Exacerbation Case StudyDocument43 pagesBronchial Asthma in Acute Exacerbation Case Studyroseanne parkNo ratings yet
- ASTHMA TreatmentDocument27 pagesASTHMA TreatmentRho Vince Caño Malagueño0% (1)
- Pharmacology Questions RespiratoryDocument5 pagesPharmacology Questions Respiratoryasmakhadder86% (44)
- 6 Asthma and Copd HandoutDocument10 pages6 Asthma and Copd HandoutMd Sakil AminNo ratings yet
- AsthmaDocument95 pagesAsthmaMohiuddin AhmedNo ratings yet
- Clinpharm SGD Bronchial AsthmaDocument9 pagesClinpharm SGD Bronchial AsthmaBea SamonteNo ratings yet
- Nirmal Kumar Meena: Nursing Tutor, Aiims, JodhpurDocument42 pagesNirmal Kumar Meena: Nursing Tutor, Aiims, JodhpurmalathiNo ratings yet
- Asthma: Prepared By: DR - Habab AbdelrhmanDocument43 pagesAsthma: Prepared By: DR - Habab AbdelrhmanJdjshsbNo ratings yet
- ASTHMA AND COPD PharmacologyDocument42 pagesASTHMA AND COPD Pharmacologycarla osbourneNo ratings yet
- Concept Map DraftsDocument9 pagesConcept Map DraftsFc CrisostomoNo ratings yet
- Asthma Lesson PlanDocument29 pagesAsthma Lesson PlanRabiu Hassan Musa86% (7)
- AsthmaDocument7 pagesAsthmaSUSHIL KUMAR OLINo ratings yet
- Bronchial AsthmaDocument46 pagesBronchial AsthmaZahidul ZahidNo ratings yet
- Current Management of Asthma 2Document43 pagesCurrent Management of Asthma 2dan ekelemeNo ratings yet
- Lecture 14 - Pharmacology of Drugs Used in Bronchial Asthma L0 COPD - EditedDocument42 pagesLecture 14 - Pharmacology of Drugs Used in Bronchial Asthma L0 COPD - EditedAbdallah AlasalNo ratings yet
- Therapeutics I AsthmaDocument29 pagesTherapeutics I AsthmaManhal A AbdulkaderNo ratings yet
- !M !M !M !M !M !M !MDocument5 pages!M !M !M !M !M !M !MJazie Pitpitunge BognadonNo ratings yet
- Asthma Davidson + Osmosis + Step Up MedicineDocument2 pagesAsthma Davidson + Osmosis + Step Up MedicineElyas MehdarNo ratings yet
- Case Presentation GeriatricDocument35 pagesCase Presentation GeriatricNurdina AfiniNo ratings yet
- Definition:: AsthmaDocument7 pagesDefinition:: AsthmaMIchele LeongNo ratings yet
- Nursing Interventions: Asthma: PathoDocument4 pagesNursing Interventions: Asthma: Pathomische20No ratings yet
- Asthma ApproachDocument7 pagesAsthma ApproachpNo ratings yet
- Drugs Effecting Respiratory System (MSCN)Document63 pagesDrugs Effecting Respiratory System (MSCN)Irshad SahilNo ratings yet
- AsthmaDocument9 pagesAsthmaNiña Jemia CortezNo ratings yet
- AsthmaDocument57 pagesAsthmaVladanNo ratings yet
- ASTHMADocument5 pagesASTHMAabdulNo ratings yet
- Asthma: A Talk by Joe and MarvDocument13 pagesAsthma: A Talk by Joe and Marvmarv43No ratings yet
- Asthm ADocument3 pagesAsthm ADebbi YuniseraniNo ratings yet
- AsthmaDocument6 pagesAsthmaJay Hipulan QuiranteNo ratings yet
- Bronchial Asthma (BA) Vs Chronic Obstructive Pulmonary Disease (COPD)Document68 pagesBronchial Asthma (BA) Vs Chronic Obstructive Pulmonary Disease (COPD)Ooi Say TingNo ratings yet
- 1) Environmental FactorsDocument7 pages1) Environmental FactorsAhmad Jamal HashmiNo ratings yet
- Presenter - Dr. Ashray - VDocument33 pagesPresenter - Dr. Ashray - VKhushbu JainNo ratings yet
- Common Pediatric Emergencies - A2Document46 pagesCommon Pediatric Emergencies - A2Ahmad JustNo ratings yet
- Bronchial AsthmaDocument45 pagesBronchial Asthmamuluken mulatieNo ratings yet
- 03 Asthma FinalDocument50 pages03 Asthma FinalG SNo ratings yet
- AsthmaDocument17 pagesAsthmaderarataye6No ratings yet
- Etiology & Triggers: AsthmaDocument6 pagesEtiology & Triggers: AsthmaNichole CollinsNo ratings yet
- Dr. Sak Indriyani, Spa, Mkes: Department of Child Health Rsu MataramDocument48 pagesDr. Sak Indriyani, Spa, Mkes: Department of Child Health Rsu MataramMuhammad Bilal Bin AmirNo ratings yet
- Asthma: Rochelle M. Nolte, MD CDR Usphs Family MedicineDocument56 pagesAsthma: Rochelle M. Nolte, MD CDR Usphs Family MedicineJoan Marie Lechado InoviaNo ratings yet
- Drugs Used in AsthmaDocument135 pagesDrugs Used in AsthmaDR. MUSICNo ratings yet
- Practice Essentials: Signs and SymptomsDocument49 pagesPractice Essentials: Signs and SymptomsRhahima SyafrilNo ratings yet
- Asthma For PTDocument52 pagesAsthma For PTAnn SibyNo ratings yet
- Asthma: Chronic Inflammation of The Airways. The Hyper-Responsive Airways Typical of AsthmaDocument7 pagesAsthma: Chronic Inflammation of The Airways. The Hyper-Responsive Airways Typical of AsthmaRaj PaulNo ratings yet
- Inhalers in Pediatric AsthmaDocument53 pagesInhalers in Pediatric AsthmaKishore Chandki100% (2)
- Integrated Therapeutics IiiDocument91 pagesIntegrated Therapeutics IiiSalahadinNo ratings yet
- Status Asthmaticus DR Divya JainDocument45 pagesStatus Asthmaticus DR Divya JainParvathy R NairNo ratings yet
- Pediatric Asthma: Signs and SymptomsDocument34 pagesPediatric Asthma: Signs and SymptomsAngie Orillac De ObaldiaNo ratings yet
- AsthmaDocument8 pagesAsthmahusainozelNo ratings yet
- AsthmaDocument55 pagesAsthmaAlessandra CruzNo ratings yet
- Child Hood Asthma: Kussia .A (MD)Document45 pagesChild Hood Asthma: Kussia .A (MD)Yemata HailuNo ratings yet
- Treatment of AsthmaDocument22 pagesTreatment of AsthmaMedranoReyesLuisinNo ratings yet
- Asthma EditedDocument42 pagesAsthma EditedSurgicalgownNo ratings yet
- Content On Pediatric Asthma: Submitted To Mrs. Rupinder Kaur Lecturer Submitted by Anu George MSC Nsg. 1 YearDocument11 pagesContent On Pediatric Asthma: Submitted To Mrs. Rupinder Kaur Lecturer Submitted by Anu George MSC Nsg. 1 YeargopscharanNo ratings yet
- ASTHMADocument48 pagesASTHMAifcrstarsNo ratings yet
- CHD AsthmaDocument20 pagesCHD AsthmaRj MagpayoNo ratings yet
- Case Study HIEDocument8 pagesCase Study HIERoxanne MariÑas DelvoNo ratings yet
- Bronchial AsthmaDocument46 pagesBronchial AsthmaKhor Kee GuanNo ratings yet
- Asthma COPDDocument9 pagesAsthma COPDemmaazizNo ratings yet
- Definition & Pathogenesis (Ngân) : Asthma - Current Medical Diagnosis and Treatment 2015Document4 pagesDefinition & Pathogenesis (Ngân) : Asthma - Current Medical Diagnosis and Treatment 2015everydayisagift9999No ratings yet
- Asthma: Wassim Mehboobali NooranyDocument12 pagesAsthma: Wassim Mehboobali NooranyMalueth AnguiNo ratings yet
- Mechanisms of Tolerance and Tachyphylaxis - Deranged PhysiologyDocument12 pagesMechanisms of Tolerance and Tachyphylaxis - Deranged Physiologydo leeNo ratings yet
- Seizure Disorder Case Study ClinicalDocument5 pagesSeizure Disorder Case Study Clinicalapi-546621912No ratings yet
- Immuno Multi Therapy and Prophylaxis Efficacy Against COVID 19Document9 pagesImmuno Multi Therapy and Prophylaxis Efficacy Against COVID 19Athenaeum Scientific PublishersNo ratings yet
- Master List 2019-20Document47 pagesMaster List 2019-20daizhussain004100% (1)
- Drug Study (Romel Cruz Hospital)Document35 pagesDrug Study (Romel Cruz Hospital)Djoan SamontañezNo ratings yet
- Aac 37 2 178Document5 pagesAac 37 2 178Marcelo salvador silva MacotoraNo ratings yet
- Study of Antibiotic-Resistance and Sensitivity Pattern in A Tertiary Care Teaching HospitalDocument8 pagesStudy of Antibiotic-Resistance and Sensitivity Pattern in A Tertiary Care Teaching HospitalIJAR JOURNALNo ratings yet
- Guided ImageryDocument28 pagesGuided ImageryDian Novita AnggraeniNo ratings yet
- Management of Orofacial Pain Other Than Trigeminal NeuralgiaDocument11 pagesManagement of Orofacial Pain Other Than Trigeminal NeuralgiaNahal HashirNo ratings yet
- United States Pharmacopeia (USP) PDFDocument229 pagesUnited States Pharmacopeia (USP) PDFHoneyNo ratings yet
- Modern PharmaceuticsDocument3 pagesModern PharmaceuticsRagulNo ratings yet
- 3a Competency Assessment - Patient Controlled AnalgesiaDocument2 pages3a Competency Assessment - Patient Controlled AnalgesiaQuijano GpokskieNo ratings yet
- PARIET 20mg - Summary of Product Characteristics (SMPC) - Print Friendly - (Emc)Document9 pagesPARIET 20mg - Summary of Product Characteristics (SMPC) - Print Friendly - (Emc)Abdullah Al MamunNo ratings yet
- Pencegahan & Tatalaksana Ulkus DiabetikumDocument60 pagesPencegahan & Tatalaksana Ulkus Diabetikumirham100% (1)
- Supporting Letter Evidence-CompressedDocument35 pagesSupporting Letter Evidence-CompressedHeena ShahNo ratings yet
- Module 1 & 2 - Teaching Materials PharmaDocument13 pagesModule 1 & 2 - Teaching Materials PharmaSamantha DiegoNo ratings yet
- Pricing Information of Vet Products..HarisDocument17 pagesPricing Information of Vet Products..HarisMirza Hassan75% (4)
- Neuroanesthesia Crisis ManualDocument56 pagesNeuroanesthesia Crisis ManualChrismas BangunNo ratings yet
- Model de CV EnglezaDocument3 pagesModel de CV EnglezaIoana TrîmbițașNo ratings yet
- PneumoniaDocument53 pagesPneumoniaAtif100% (1)
- Lithium NeurotoxicityDocument4 pagesLithium NeurotoxicityKimolli JamesNo ratings yet
- Assignment On-: "Pharmacokinetics of Drug Molecules in Different Disease Condition"Document19 pagesAssignment On-: "Pharmacokinetics of Drug Molecules in Different Disease Condition"Susmoy SinhaNo ratings yet
- Vitamin D DeficiencyDocument11 pagesVitamin D DeficiencyElvisNo ratings yet
- Illegal and Legal Substance Abuse Amongst Harm Reduction Program Users - A Case Study From CroatiaDocument18 pagesIllegal and Legal Substance Abuse Amongst Harm Reduction Program Users - A Case Study From CroatiamarijaNo ratings yet
- TARGETED THERAPY Pada Kanker ParuDocument13 pagesTARGETED THERAPY Pada Kanker Parudebby nirmasariNo ratings yet
- Antifolate Drugs 17970Document19 pagesAntifolate Drugs 17970TES SENNo ratings yet
- SGLT 2Document21 pagesSGLT 2Genix PharmaNo ratings yet