Professional Documents
Culture Documents
Guillen Barre Syndrom
Guillen Barre Syndrom
Uploaded by
Vanquish Vein0 ratings0% found this document useful (0 votes)
26 views26 pagesGuillain-Barré syndrome (GBS) is an acute immune-mediated neuropathy that results in progressive muscle weakness. It has an annual incidence of 0.6 to 2.4 cases per 100,000 people and is the most common cause of acute flaccid paralysis. The pathogenesis involves peripheral nerve demyelination mediated by humoral and cell-mediated immune responses. Clinical features include ascending limb weakness over hours to weeks, areflexia, and possible autonomic dysfunction. Treatment includes plasmapheresis or intravenous immunoglobulin, which hasten recovery. The prognosis is generally good, with 30% residual weakness possible after 3 years and a 3% mortality rate.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentGuillain-Barré syndrome (GBS) is an acute immune-mediated neuropathy that results in progressive muscle weakness. It has an annual incidence of 0.6 to 2.4 cases per 100,000 people and is the most common cause of acute flaccid paralysis. The pathogenesis involves peripheral nerve demyelination mediated by humoral and cell-mediated immune responses. Clinical features include ascending limb weakness over hours to weeks, areflexia, and possible autonomic dysfunction. Treatment includes plasmapheresis or intravenous immunoglobulin, which hasten recovery. The prognosis is generally good, with 30% residual weakness possible after 3 years and a 3% mortality rate.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
0 ratings0% found this document useful (0 votes)
26 views26 pagesGuillen Barre Syndrom
Guillen Barre Syndrom
Uploaded by
Vanquish VeinGuillain-Barré syndrome (GBS) is an acute immune-mediated neuropathy that results in progressive muscle weakness. It has an annual incidence of 0.6 to 2.4 cases per 100,000 people and is the most common cause of acute flaccid paralysis. The pathogenesis involves peripheral nerve demyelination mediated by humoral and cell-mediated immune responses. Clinical features include ascending limb weakness over hours to weeks, areflexia, and possible autonomic dysfunction. Treatment includes plasmapheresis or intravenous immunoglobulin, which hasten recovery. The prognosis is generally good, with 30% residual weakness possible after 3 years and a 3% mortality rate.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
Download as pptx, pdf, or txt
You are on page 1of 26
Guillain Barre Syndrome
dr. Rohmania Setiarini
It has an annual incidence of 0.6 to 2.4 cases per
100,000 population and occurs at all ages and in
both sexes
With the marked decline in the incidence of polio,
Guillain-Barr syndrome is now the most
common cause of acute flaccid paralysis in healthy
people
Guillain-Barr syndrome:
is a rare immune mediated neuropathy characterized
by progressive muscle weakness
PATHOGENESIS
Peripheral nerve demyelination in Guillain-Barr
syndrome is believed to be immunologically
mediated
Humoral factors and cell-mediated immune
phenomena have been implicated in the damage of
myelin and/or the myelin-producing Schwann
cells
Clinical feature
Two-thirds of patients develop the neurologic symptoms 2-
4 weeks after what appears to be a benign respiratory or
gastrointestinal infection
The initial symptoms are fine paresthesias in the toes and
fingertips, followed by lower extremity weakness that may
ascend over hours to days to involve the arms, cranial
nerves, and in severe cases the muscles of respiration
Clinical feature
Weakness in lower extremities progresses
over hours to weeks and peaks in 14 days.
Muscles of the distal extremities are severely
affected.
Common sx include: hypotonia (reduced
muscle tone) and areflexia (lack of reflexes).
Autonomic disturbances
Physical Examination
Symmetric limb weakness with diminished or absent
reflexes
Minimal loss of sensation despite paresthesias
Signs of autonomic dysfunction are present in 50 percent
of patients, including
Cardiac dysrhythmias (asystole, bradycardia, sinus
tachycardia, and atrial/ventricular tachyarrhythmias)
Orthostatic hypotension
Transient or persistent hypertension
Paralytic ileus
Bladder dysfunction
Abnormal sweating
Diagnose
Based on pt hx and clinical manifestations.
Lumbar puncture for CSF is normal or low
protein. After 7 days protein is high.
Electromyogram (EMG) test shows that
nerve conduction is slower.
Electrocardiogram (ECG) test shows heart
irregularities.
Nerve biopsy can be done examining the
damaged nerve or axon.
Prognosis
The recovery ranges from 3 w to 3 y.
After 3 y, 30% of the pts will have residual
weakness. The mortality rate is 3% from
GBS.
Treatment
The main modalities of therapy for Guillain-Barr
syndrome include
Plasmapheresis
Administration of intravenous immune globulin
AANs
Class of evidence for therapy
Class I. High quality randomized controlled trials
(RCTs)
Class II. Prospective matched group cohort studies or
RCTs lacking adequate randomization
concealment or blinding, or potentially liable to
attrition or outcome ascertainment bias
Class
III.
Other studies such as natural history studies
Class
IV.
Uncontrolled studies, case series, or expert
opinion
AANs
Recommendation Levels
Level
A
Established as effective, ineffective or harmful,
or as useful/predictive or not useful/predictive
Level
B
Probably effective, ineffective or harmful, or as
useful/predictive or not useful/predictive
Level
C
Possibly effective, ineffective or harmful, or as
useful/predictive or not useful/predictive
Level
U
Data inadequate or conflicting; Treatment, test,
or predictor unproven
Conclusions (PE)
Plasma exchange hastens recovery in non-ambulant
patients with GBS who present within four weeks from the
onset of neuropathic symptoms (Class II evidence).
Plasma exchange also hastens recovery in ambulant
patients who present within two weeks but the evidence is
limited to one trial (Class II evidence).
The effects of plasma exchange and IVIg are equivalent in
patients requiring aid to walk(Class I evidence).
Treatment with CSF filtration has not been adequately
tested (Limited Class II evidence).
American Academy of Neurology
Recommendations
PE is recommended in non-ambulant patients
within four weeks from onset (Level A, Class II
evidence).
PE is recommended for ambulant patients within two
weeks from onset (Level B, limited Class II
evidence).
American Academy of Neurology
Iv immune globuline
Conclusions
Intravenous immunoglobulin has not been
adequately compared with placebo (limited Class II
evidence).
Such comparison is not now needed because, when
started within two weeks from the onset, IVIg has
equivalent efficacy to PE in hastening recovery from
patients with GBS who require aid to walk (Class I
evidence).
Multiple complications were significantly less
frequent with IVIg than with PE (Class I evidence).
There is no evidence concerning the relative efficacy
of PE and IVIg in patients with axonal forms of GBS.
American Academy of Neurology
Recommendations
IVIg is recommended for patients with GBS who
require aid to walk within two (Level A
recommendation) or four weeks from the onset of
neuropathic symptoms (Level B recommendation
derived from Class II evidence concerning PE
started within the first four weeks).
The effects of IVIg and plasma exchange are
equivalent. (Level B recommendation Class I
evidence concerning the comparisons between PE
and IVIg started within the first two weeks).
American Academy of Neurology
Analysis of the evidence
Combination treatments
One Class I trial showed that PE followed by IVIg
showed no significant benefit compared with PE
alone in any measured outcome.
Conclusions
Sequential treatment with PE followed by IVIg does
not have a superior effect to either treatment given
alone (Class I evidence).
Sequential treatment with immunoabsorption
followed by IVIg has not been adequately tested
(Limited Class IV evidence).
American Academy of Neurology
Recommendations
Sequential treatment with PE followed by IVIg is not
recommended (Level A recommendation, Class I
evidence).
Immunoabsorption followed by IVIg is not
recommended (Level U recommendation, Class IV
evidence).
American Academy of Neurology
Analysis of the evidence
Immunoabsorption
An alternative technique to PE, which removes
immunoglobulins.
Has the advantage of not requiring the use of a
human blood product as a replacement fluid.
In a prospective trial there were no differences in
outcome between 11 patients treated with PE and
13 treated with immunoabsorption
There is only limited Class IV evidence from a
single small non-randomized, unblinded study.
Conclusion
The evidence is insufficient to recommend the use of
immunoabsorption (Level U recommendation, Class IV
evidence).
American Academy of Neurology
Recommendation
A 17-year-old male developed flu-like symptoms, severe diarrhoea and
abdominal pain 4 days after attending a dinner party at which he had eaten a
chicken. Three other people who had attended the same party developed
gastrointestinal symptoms. These symptoms settled within a few days. Stool
cultures taken from all four individuals grew Campylobacter jejuni. About 10
days after the onset of diarrhoea, he developed diffuse aching around his
shoulders and buttocks and pins and needles in his hands and feet. Over the
next week the sensory changes worsened and spread to involve his arms and
legs. His limbs became progressively weaker and 8 days after the onset of
neurological symptoms he could not hold a cup or stand unaided. He was
admitted to hospital and found to have severe symmetrical distal limb
weakness and glove and stocking sensory loss to the elbows and knees.
Nerve conduction studies showed evidence of a mixed motor and sensory
neuropathy and examination of his cerebrospinal fluid (CSF) showed a very
high total protein level at 4g/l but without any increase in the number of cells
in the CSF. High titres of IgM and IgG antibodies to Campylobacter jejuni
were found in his peripheral blood.
Case
You might also like
- Sample Questions For Emstrex 2012Document6 pagesSample Questions For Emstrex 2012Dr.2020100% (1)
- Lesson Plan DETAILED HAZARD AND RISKDocument13 pagesLesson Plan DETAILED HAZARD AND RISKMelanie Delgado Magsino ReyesNo ratings yet
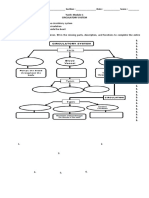
- Yunit 1 Module 1 Activity Circulatory System RevisedDocument2 pagesYunit 1 Module 1 Activity Circulatory System RevisedJan Ice100% (1)
- Guillain Barré SyndromeDocument21 pagesGuillain Barré SyndromebagusNo ratings yet
- Guillain-Barré SyndromeDocument21 pagesGuillain-Barré SyndromeZulkarnainBustamamNo ratings yet
- Jose B. Lingad Memorial General Hospital: Guillain-Barre Syndrome in Pregnancy - A Case ReportDocument8 pagesJose B. Lingad Memorial General Hospital: Guillain-Barre Syndrome in Pregnancy - A Case ReportRei MisakiNo ratings yet
- Asian Journal of Pharmaceutical and Health SciencesDocument4 pagesAsian Journal of Pharmaceutical and Health Sciencesfariska amanizataNo ratings yet
- Clinical Course of An Acute Motor Axonal Neuropathy Patient With Some Prognostic Factors Treated With Low Dose Intravenous ImmunoglobulinDocument1 pageClinical Course of An Acute Motor Axonal Neuropathy Patient With Some Prognostic Factors Treated With Low Dose Intravenous Immunoglobulinyeremias setyawanNo ratings yet
- Asbury - Assesment of Current Diagnostic Criteria For GBSDocument4 pagesAsbury - Assesment of Current Diagnostic Criteria For GBSMarcelo BedoyaNo ratings yet
- Aidp Post CovDocument4 pagesAidp Post CovJanki KotiyaNo ratings yet
- 2019 IteDocument188 pages2019 IteBHNo ratings yet
- Recurrent Guillain-Barre Syndrome-A Case Report.: Dilesha WL, Weerawansa MRP, Siribaddana SHDocument3 pagesRecurrent Guillain-Barre Syndrome-A Case Report.: Dilesha WL, Weerawansa MRP, Siribaddana SHjonniwal sanusiNo ratings yet
- What To Do, When Gbs PT Fails To Respond To TreatmentDocument4 pagesWhat To Do, When Gbs PT Fails To Respond To Treatmentidno1008No ratings yet
- Case of Celiac's Disease Mimicking ALSDocument4 pagesCase of Celiac's Disease Mimicking ALSfakbikNo ratings yet
- Guil LianDocument18 pagesGuil LianPdianghunNo ratings yet
- Aan ?event Print&disorder - Id 935: TreatmentDocument3 pagesAan ?event Print&disorder - Id 935: TreatmentclaudiaNo ratings yet
- Gbs HarshaDocument34 pagesGbs HarsharobyanaoktvNo ratings yet
- Acute Poliomyelitis: BY: Reojano, Jeriby R. Paroginog, CharisDocument35 pagesAcute Poliomyelitis: BY: Reojano, Jeriby R. Paroginog, CharisMarivic DianoNo ratings yet
- GB SyndromDocument5 pagesGB Syndromavinash dhameriyaNo ratings yet
- QuestionsDocument1 pageQuestionsChibueze AfugbuomNo ratings yet
- A Rare Presentation of Guillain-Barre Syndrome: Pharyngeal Cervical-Brachial VariantDocument2 pagesA Rare Presentation of Guillain-Barre Syndrome: Pharyngeal Cervical-Brachial VariantdzakiyahNo ratings yet
- Anestesi Pada GBSDocument4 pagesAnestesi Pada GBSyudhalantankNo ratings yet
- Guillain-Barre Syndrome Presenting With Sensory Disturbance Following A Herpes Virus Infection: A Case ReportDocument5 pagesGuillain-Barre Syndrome Presenting With Sensory Disturbance Following A Herpes Virus Infection: A Case ReportAsep MetrikaNo ratings yet
- What Is GuillainDocument1 pageWhat Is Guillainloveitornot28No ratings yet
- Question of The Week # 433: Archer Red 11:25 AM Links To This PostDocument34 pagesQuestion of The Week # 433: Archer Red 11:25 AM Links To This PostChristian JaraNo ratings yet
- CBD Guillian BarreDocument18 pagesCBD Guillian BarreNATTAPAT SANGKAKULNo ratings yet
- CBD-Guillian BarreDocument18 pagesCBD-Guillian BarreNATTAPAT SANGKAKULNo ratings yet
- Guillain Barre SyndromeDocument6 pagesGuillain Barre SyndromeErtania NirmalaNo ratings yet
- Levofloxacin in Typhoid FeverDocument4 pagesLevofloxacin in Typhoid FeverUsman HanifNo ratings yet
- Neuropathy After Malnutrition Is Copper Deficiency The Missed Diagnosis E. Dowling 9.16.2014Document3 pagesNeuropathy After Malnutrition Is Copper Deficiency The Missed Diagnosis E. Dowling 9.16.2014xzx xNo ratings yet
- Recurrent GBSDocument14 pagesRecurrent GBSkashif mansoorNo ratings yet
- J Neurol Neurosurg Psychiatry 2001 Kuwabara 560 2Document4 pagesJ Neurol Neurosurg Psychiatry 2001 Kuwabara 560 2M ZumrodinNo ratings yet
- Terapi GBS FKDocument49 pagesTerapi GBS FKIhda ParidahNo ratings yet
- Sindrome de KawasakiDocument6 pagesSindrome de KawasakiCHOQUE APAZA DIMARIT KEMYNo ratings yet
- Ptosis Without Ophthalmoplegia: A Rare Manifestation of Guillain-Barré SyndromeDocument5 pagesPtosis Without Ophthalmoplegia: A Rare Manifestation of Guillain-Barré SyndromeMosNo ratings yet
- An Approach To Acute Flaccid Paralysis in ChildrenDocument55 pagesAn Approach To Acute Flaccid Paralysis in Childrennowrin05273815No ratings yet
- Cases Scenario (Question)Document13 pagesCases Scenario (Question)elavarkuzhali2019No ratings yet
- Emergency Medicine EducationGuillain-Barré Syndrome - Third Time's The Charm - EmDOCs - Net - Emergency Medicine EducationDocument14 pagesEmergency Medicine EducationGuillain-Barré Syndrome - Third Time's The Charm - EmDOCs - Net - Emergency Medicine EducationPgmee KimsNo ratings yet
- The Patient With Rhabdomyolysis: Have You Considered Quail Poisoning?Document2 pagesThe Patient With Rhabdomyolysis: Have You Considered Quail Poisoning?andriopaNo ratings yet
- 8008 28295 2 PB PDFDocument10 pages8008 28295 2 PB PDFPrabuddha ThihawaNo ratings yet
- Guillain Barre SyndromDocument10 pagesGuillain Barre SyndromMiirnaawatii YalidaaNo ratings yet
- Quiz RheumDocument20 pagesQuiz RheumAzizan HannyNo ratings yet
- A Case of Successful Management of Guillainbarre Syndrome in PregnancyDocument3 pagesA Case of Successful Management of Guillainbarre Syndrome in PregnancyTias DiahNo ratings yet
- Vijay BhaiDocument35 pagesVijay BhaiRakesh LodwalNo ratings yet
- Simple Febrile SeizureDocument63 pagesSimple Febrile SeizureMary Ann SacramentoNo ratings yet
- Patient Case Presentation IIDocument7 pagesPatient Case Presentation IILangat IsaacNo ratings yet
- Pathology I Review 10Document30 pagesPathology I Review 10i_areinamoNo ratings yet
- Huma Mir-1Document51 pagesHuma Mir-1drw72409No ratings yet
- Guillain-Barré SyndromeDocument23 pagesGuillain-Barré SyndromeMahindra KumarNo ratings yet
- A Rare Neurological Complication of Typhoid FeverDocument2 pagesA Rare Neurological Complication of Typhoid FeverSuryati HusinNo ratings yet
- Guillain - Barre - SyndromeDocument18 pagesGuillain - Barre - SyndromeRAMNo ratings yet
- Inglés Clase 2Document189 pagesInglés Clase 2Steph OsNo ratings yet
- p191 PDFDocument7 pagesp191 PDFdessriyaNo ratings yet
- Guillain-Barre Syndrome: Practice EssentialsDocument16 pagesGuillain-Barre Syndrome: Practice EssentialsUKMBasketNo ratings yet
- Abuajela Sreh - St5 Gastroenterology - Sheffield Teaching Hospitals 1 4 / 0 1 / 2 0 2 2Document48 pagesAbuajela Sreh - St5 Gastroenterology - Sheffield Teaching Hospitals 1 4 / 0 1 / 2 0 2 2sryh2012No ratings yet
- Guillain Barre SyndromeDocument18 pagesGuillain Barre SyndromeRendy AndikaNo ratings yet
- Medicine: Systemic Lupus Erythematosus With Guillian - Barre SyndromeDocument5 pagesMedicine: Systemic Lupus Erythematosus With Guillian - Barre SyndromeShri RamNo ratings yet
- Pulmonary Tuberculosis As A Differential Diagnosis of PneumoniaDocument18 pagesPulmonary Tuberculosis As A Differential Diagnosis of PneumoniaKadek AyuNo ratings yet
- Guillane Barre SyndromeDocument8 pagesGuillane Barre SyndromeyasiraNo ratings yet
- Wernicke EncephalopathyDocument16 pagesWernicke Encephalopathyapi-286318965No ratings yet
- Guillain Barre Syndrome A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandGuillain Barre Syndrome A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Expert System For Diagnose Stomach Disease Using Fuzzy Logic and Certainty Factor MethodDocument16 pagesExpert System For Diagnose Stomach Disease Using Fuzzy Logic and Certainty Factor MethodVanquish VeinNo ratings yet
- Lampiran x4Document2 pagesLampiran x4Vanquish VeinNo ratings yet
- Lampiran x2Document2 pagesLampiran x2Vanquish VeinNo ratings yet
- Lampiran x1Document2 pagesLampiran x1Vanquish VeinNo ratings yet
- Homeostasis: Achmad AminuddinDocument49 pagesHomeostasis: Achmad AminuddinVanquish VeinNo ratings yet
- Skin Injury: Dr. Imam FirmansyahDocument28 pagesSkin Injury: Dr. Imam FirmansyahVanquish VeinNo ratings yet
- Embryology of The Cardiovascular SystemDocument59 pagesEmbryology of The Cardiovascular SystemVanquish VeinNo ratings yet
- If HP Cancer Guide br007 MriDocument13 pagesIf HP Cancer Guide br007 Mrirusgal8992100% (1)
- Community Health Nursing Case Presentation: Bukidnon State University College of NursingDocument16 pagesCommunity Health Nursing Case Presentation: Bukidnon State University College of NursingAlmira GamaoNo ratings yet
- Assessment of Six Cardiovascular Risk Calculators...Document7 pagesAssessment of Six Cardiovascular Risk Calculators...Ale VillarNo ratings yet
- 63-Article Text-607-2-10-20200107Document9 pages63-Article Text-607-2-10-20200107benmarte2003No ratings yet
- Scenario StationsDocument17 pagesScenario StationsDaryl DunneNo ratings yet
- Pantoja Et Al. - 2019 - Prevalence of Degenerative Joint Disease of The TeDocument14 pagesPantoja Et Al. - 2019 - Prevalence of Degenerative Joint Disease of The TeMarco Saavedra BurgosNo ratings yet
- EPI Schedule-1Document2 pagesEPI Schedule-1sabbir.boss7333No ratings yet
- Society: Exercise Is For Every BodyDocument8 pagesSociety: Exercise Is For Every BodyFabiano HenriqueNo ratings yet
- How To Use This Module: Pre-TestDocument8 pagesHow To Use This Module: Pre-TestMarilou BitasoloNo ratings yet
- Neonatal Seizures: Lamiaa Mohsen, M.D Cairo UniversityDocument36 pagesNeonatal Seizures: Lamiaa Mohsen, M.D Cairo UniversityAdliah ZahiraNo ratings yet
- TB TreatmentDocument58 pagesTB TreatmentNdayisaba CorneilleNo ratings yet
- 2020 - Autism in Higher Education An Investigation of Quality of LifeDocument141 pages2020 - Autism in Higher Education An Investigation of Quality of LifeSilviaNo ratings yet
- AAFP 2015 Proceedings Book For WebDocument292 pagesAAFP 2015 Proceedings Book For WebPavel VokrouhlíkNo ratings yet
- Broilers &layers Yaras MaccharlesDocument38 pagesBroilers &layers Yaras MaccharlesNyasha VincentNo ratings yet
- 0960-0555 Sample MER Forms PDFDocument9 pages0960-0555 Sample MER Forms PDFAbhay SingaviNo ratings yet
- Research Paper About Effects of Air PollutionDocument7 pagesResearch Paper About Effects of Air Pollutionjtbowtgkf100% (1)
- OSHJ-CoP-16 First Aid at Work Version 1 EnglishDocument12 pagesOSHJ-CoP-16 First Aid at Work Version 1 EnglishsajinNo ratings yet
- OB-Reviewer With AlgorithmDocument29 pagesOB-Reviewer With Algorithmriczen mae vilaNo ratings yet
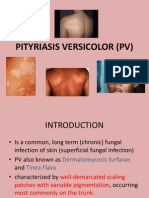
- Pityriasis Versicolor Part 1Document9 pagesPityriasis Versicolor Part 1Sopna Zenith0% (1)
- Assay Solutions: Vidas - Protocols - Units Vidas - ParametersDocument9 pagesAssay Solutions: Vidas - Protocols - Units Vidas - ParametersYonasNo ratings yet
- CDC Confirms COVID Vaccination Increases Risk of Autoimmune Heart Disease by 13200Document4 pagesCDC Confirms COVID Vaccination Increases Risk of Autoimmune Heart Disease by 13200WAYLOR MusicNo ratings yet
- Instruction Manual: M7 Intelli IT (HEM-7361T-EBK) X7 Smart (HEM-7361T-ESL)Document132 pagesInstruction Manual: M7 Intelli IT (HEM-7361T-EBK) X7 Smart (HEM-7361T-ESL)zabbizzoNo ratings yet
- Verrucous CarcinomaDocument12 pagesVerrucous Carcinomaanatomimanusia100% (1)
- #410 Heavy LiftDocument3 pages#410 Heavy LiftTolias EgwNo ratings yet
- TB of Genital TractDocument29 pagesTB of Genital TractKasi Krishna Raja100% (2)
- PFOonDocument3 pagesPFOonInternational Medical PublisherNo ratings yet
- Histamine H 2 Receptor Antagonists For DecreasingDocument10 pagesHistamine H 2 Receptor Antagonists For DecreasingYulian 53No ratings yet
- 2021 Essential Brain Hygiene EguideDocument26 pages2021 Essential Brain Hygiene EguideHector SolarNo ratings yet